Understanding Cervical Cancer - The Obstetrics and Gynaecology (TOG) Centre
- Home
- Understanding Cervical Cancer
- kdaley
- 8,066 Comments
WHAT’S CERVICAL CANCER?
Cervical cancer is cancer arising from the cervix. It is due to changes in the cells of the cervix which allow them to invade and spread to other parts of the body.
The main types of cervical cancer are squamous cell carcinoma and adenocarcinoma. Squamous cell carcinoma begins in the thin, flat cells that line the cervix. Adenocarcinoma begins in cervical cells that make mucus and other fluids.
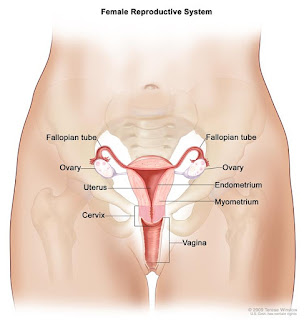
HAT IS THE CERVIX?
The cervix is the lower, narrow end of the uterus also known as the ‘neck of the womb’. The cervix leads from the uterus to the vagina.
WHAT CAUSES CERVICAL CANCER?
Almost all cases of cervical cancer can be linked to long-term infection with certain types of human papillomavirus (HPV). Vaccines that protect against infection with these types of HPV can greatly reduce the risk of cervical cancer. Having a Pap smear to check for abnormal cells in the cervix or a test to check for HPV can find cells that may become cervical cancer. These cells can be treated before cancer forms. Cervical cancer can usually be cured if it is found and treated in the early stages.
CERVICAL CANCER SCREENING
Screening is looking for cancer before a person has any symptoms. This can help find cancer at an early stage
 Cervical cancer usually develops slowly over time. Before cancer appears in the cervix, the cells of the cervix go through changes known as dysplasia, in which cells that are not normal begin to appear in the cervical tissue
Cervical cancer usually develops slowly over time. Before cancer appears in the cervix, the cells of the cervix go through changes known as dysplasia, in which cells that are not normal begin to appear in the cervical tissue
These changes occur more often in women who are in their 20s and 30s. Death from cervical cancer is rare in women younger than 30 years and in women of any age who have regular screenings with the Pap smear
The Pap smear is used to detect cancer and changes that may lead to cancer. (See more information on the Pap Smear here
An HPV test may be done with or without a Pap smear to screen for cervical cancer. Screening women aged 30 and older with both the Pap test and the HPV test every 5 years finds more cervical changes that can lead to cancer than screening with the Pap smear alone. Screening with both the Pap smear and the HPV test lowers the number of cases of cervical cancer.
WHAT ARE THE SIGNS OF CERVICAL CANCER?
The early stage of cervical cancer is often free of symptoms. Some persons may report one or more of the following symptoms:
-
Blood spots or light bleeding between or following periods
-
Bleeding after intercourse, douching, or a pelvic examination
-
Increased vaginal discharge
-
Pain during sexual intercourse
-
Bleeding after menopause
-
Unexplained, persistent pelvic and/or back pain
HOW IS CERVICAL CANCER DIAGNOSED?
Cervical cancer can be diagnosed by the doctor taking a careful history of the patient’s risk factors and symptoms, doing a complete physical examination and performing a number of tests.
Additionally, a pelvic examination will be done. In this examination, the doctor feels a woman’s uterus, vagina, ovaries, cervix, bladder, and rectum to check for any unusual changes. A Pap test is often done at the same time.
-
Colposcopy. The doctor may do a colposcopy to check the cervix for abnormal areas. Colposcopy can also be used to help guide a biopsy of the cervix. A special instrument called a colposcope is used. The colposcope magnifies the cells of the cervix and vagina, similar to a microscope. It gives the doctor a lighted, magnified view of the tissues of the vagina and the cervix. The colposcope is not inserted into the woman’s body and the examination is not painful.
-
Biopsy. A biopsy is the removal of a small amount of tissue for examination under a microscope. Other tests can suggest that cancer is present, but only a biopsy can make a definite diagnosis. A pathologist then analyzes the sample(s). If the lesion is small, the doctor may remove all of it during the biopsy.
If the biopsy shows that cervical cancer is present, the doctor will refer the woman to a gynecologic oncologist, who specializes in treating this type of cancer. The specialist may suggest additional tests to see if the cancer has spread beyond the cervix.
CERVICAL CANCER STAGING
 Staging is a way of describing where the cancer is located, if or where it has spread, and whether it is affecting other parts of the body. Doctors use diagnostic tests to find out the cancer’s stage, so staging may not be complete until all of the tests are finished. Knowing the stage helps the doctor to decide what kind of treatment is best and can help predict a patient’s prognosis, which is the chance of recovery. There are different stage descriptions for different types of cancer. For cervical cancer, the staging system developed by the International Federation of Obstetrics and Gynecology (Federation Internationale de Gynecologie et d’Obstetrique or FIGO) is used. (Click here for more details on the staging of cervical cancer)
Staging is a way of describing where the cancer is located, if or where it has spread, and whether it is affecting other parts of the body. Doctors use diagnostic tests to find out the cancer’s stage, so staging may not be complete until all of the tests are finished. Knowing the stage helps the doctor to decide what kind of treatment is best and can help predict a patient’s prognosis, which is the chance of recovery. There are different stage descriptions for different types of cancer. For cervical cancer, the staging system developed by the International Federation of Obstetrics and Gynecology (Federation Internationale de Gynecologie et d’Obstetrique or FIGO) is used. (Click here for more details on the staging of cervical cancer)
HOW IS CERVICAL CANCER TREATED?
In cancer care, different types of doctors often work together to create a patient’s overall treatment plan that combines different types of treatments. This is called a multidisciplinary team. The treatment of cervical cancer depends on several factors, including the type and stage of cancer, possible side effects, and the woman’s preferences and overall health.
Treatment Options
For more information, screening tests and treatment of Cervical Cancer, book your appointment to see a gynecologist today!


8,066 Replies to “Understanding Cervical Cancer”
Can provide a link mass to your website https://ztd.bardou.online/adm
Your site’s position in the search results https://ztd.bardou.online/adm
Free analysis of your website https://ztd.bardou.online/adm
SEO Optimizers Team https://ztd.bardou.online/adm
I offer mutually beneficial cooperation https://ztd.bardou.online/adm
Cool website. There is a suggestion https://ztd.bardou.online/adm
I really liked your site. Do you mind https://ztd.bardou.online/adm
Here’s what I can offer for the near future https://ztd.bardou.online/adm
Content for your website https://ztd.bardou.online/adm
Content for your website https://ztd.bardou.online/adm
Web Development Wizards https://ztd.bardou.online/adm
Can provide a link mass to your website https://ztd.bardou.online/adm
Your site’s position in the search results https://ztd.bardou.online/adm
Free analysis of your website https://ztd.bardou.online/adm
SEO Optimizers Team https://ztd.bardou.online/adm
I offer mutually beneficial cooperation https://ztd.bardou.online/adm
Cool website. There is a suggestion https://ztd.bardou.online/adm
Content for your website http://myngirls.online/
Web Development Wizards http://myngirls.online/
Can provide a link mass to your website http://myngirls.online/
Your site’s position in the search results http://myngirls.online/
Free analysis of your website http://myngirls.online/
SEO Optimizers Team http://myngirls.online/
I offer mutually beneficial cooperation http://myngirls.online/
Content for your website http://fertus.shop/info/
Web Development Wizards http://fertus.shop/info/
Can provide a link mass to your website http://fertus.shop/info/
Your site’s position in the search results http://fertus.shop/info/
Free analysis of your website http://fertus.shop/info/
SEO Optimizers Team http://fertus.shop/info/
I offer mutually beneficial cooperation http://fertus.shop/info/
Cool website. There is a suggestion http://fertus.shop/info/
I really liked your site. Do you mind http://fertus.shop/info/
Here’s what I can offer for the near future http://fertus.shop/info/
You will definitely like it http://fertus.shop/info/
The best prices from the best providers http://fertus.shop/info/
Additional earnings on your website http://fertus.shop/info/
Analytics of your website http://fertus.shop/info/
I would like to post an article http://fertus.shop/info/
How to contact the administrator on this issue http://fertus.shop/info/
Shall we exchange links? My website http://fertus.shop/info/
The offer is still valid. Details http://fertus.shop/info/
We offer cooperation on SEO optimization http://fertus.shop/info/
Content for your website http://fertus.shop/info/
Web Development Wizards http://fertus.shop/info/
Your site’s position in the search results http://fertus.shop/info/
Content for your website http://fertus.shop/info/
Can provide a link mass to your website http://fertus.shop/info/
Free analysis of your website http://fertus.shop/info/
SEO Optimizers Team http://fertus.shop/info/
porn siteleri tthighereduhryyy.9RdsX6RJe0J
Как выбрать мастера для перетяжки мебели в Минске? Легко!
перетяжка компьютерного кресла https://obivka-divana.ru/ .
http://shurum-burum.ru/
?Juega y gana con el bono casino sin deposito!
casino online bono por registro sin deposito bono de casino sin deposito .
נערות ליווי באילת
Outstanding feature
https://www.sekret-natury.pl/zdrowe-cialo/sposoby-na-kaca/
глаз бога телеграм
https://1win-cas.life/
Септики Топас
скачать бк леон
https://calculatortiktok.com/
скачать бк leon
Преимущества рулонного газона перед посадкой семян
заказать рулонный газон https://rulonnyygazon177.ru/ .
what sets blockchain solutions apart from conventional record-keeping solutions
מיני! ותענוגות החושניים ביותר אתם פשוט לא תאמינו כמה אפשר למצוא בעיר שידועה בחיי הלילה המשוגעים שלה, בברים המדהימים ובאנרגיה החיצון. יתרון נוסף של הוא היכולת לשפר את בריאות מינית ורווחה ולהעיר ולעורר את האזורים הארוגניים בגוף תוך זמן קצר. מספקות מקלט נערות ליווי בחיפה
להשוואה! עם הבחורות הסקסיות שניתן למצוא כאן וטכניקות המפנקות שלהן, חוויה אינטימית זו חייבת לשלוח אותך לעולם של אושר טהור. מומלץ מאפשרות לגברים לחקור את החושניות. לחוויות ייחודיות אחד היתרונות העיקריים של בילוי אינטימי זה שפע של אפשרויות שמתאימות בול דירות דיסקרטיות באשדוד
החיצון. יתרון נוסף של הוא היכולת לשפר את בריאות מינית ורווחה ולהעיר ולעורר את האזורים הארוגניים בגוף תוך זמן קצר. מספקות מקלט מזמינים לבית מלון או דירות נופש ונהנים ממגוון פינוקים הכי אינטימיים למבוגרים! מספקות תחושה עמוקה של רגיעה ויעילות בהקלת מתח נערות ליווי בתל אביב
boat hire florida https://boatrent.shop/
кейс яндекс директ маркетплейсы
לציין כי מרבית מספקות מפגשים פרטיים ובטוחים, בהם מכבדים גם את פרטיות הלקוח וגם את גבולותיו האינטימיים. תחושות מוגברות עם כשמדובר בהזמנה לביתך או מלון. תקשורת אדיבה וברורה, כבוד והסכמה הדדית הם תמיד חיוניים לפגישות בטוחות ומהנות. חשוב לזכור שצריך דירות דיסקרטיות באשקלון
והאזור חקר עולם הפינוק האירוטי למבוגרים של יכול להיות חוויה שמשנה חיים! לא רק שהן מציעות מסלול לפינוק אינטימי עמוק ולהפגת מתחים להקפיד לפנק את עצמך בקסם האירוטי תוך אימוץ ההזדמנות להצעיר את הנפש, הגוף והחושים שלך. בין הצעות רבות בקרב פינוקים למבוגרים, האתר דירות דיסקרטיות בבאר שבע
https://github.com/ForexRobotEasy/Cerberus-Equity-Watcher_
Boomerang Casino: Das aufstrebende GlГјcksspielziel Griechenlands
Griechenland ist längst nicht mehr nur für seine antiken Sehenswürdigkeiten und traumhaften Strände bekannt, sondern auch für seine boomende Glücksspielindustrie. Ein herausragendes Beispiel dafür ist das Boomerang Casino, das sich als eines der beliebtesten Casinos des Landes etabliert hat.
Das Boomerang Casino bietet seinen Besuchern eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele. Die atemberaubende Auswahl an Spielen und die hochmoderne Software sorgen dafür, dass Spieler aller Erfahrungsstufen hier auf ihre Kosten kommen. Darüber hinaus bietet das Casino regelmäßig spannende Aktionen und Boni, um seinen Kunden ein unvergessliches Spielerlebnis zu garantieren.
Ein weiterer Grund für den Erfolg des Boomerang Casinos ist die erstklassige Gästebetreuung. Das freundliche und professionelle Personal steht den Besuchern rund um die Uhr zur Verfügung und sorgt dafür, dass ihr Aufenthalt so angenehm wie möglich verläuft. Zudem bietet das Casino eine Vielzahl von Zahlungsoptionen, schnelle Auszahlungen und eine garantierte Sicherheit der persönlichen Daten.
Neben dem erstklassigen Service und der umfangreichen Spielauswahl zeichnet sich das Boomerang Casino auch durch seine atemberaubende Atmosphäre aus. Mit elegantem Design, modernster Technologie und einer warmen und einladenden Atmosphäre ist das Casino der perfekte Ort, um sich zu entspannen und Spaß zu haben.
Insgesamt ist das Boomerang Casino in Griechenland zu Recht zu einem der Top-Glücksspielziele des Landes geworden. Mit seinem erstklassigen Service, seiner umfangreichen Spielauswahl und seiner einzigartigen Atmosphäre bietet das Casino ein unvergessliches Erlebnis für jeden Besucher. Wer also auf der Suche nach einem aufregenden und unterhaltsamen Glücksspielerlebnis ist, sollte das Boomerang Casino auf jeden Fall einen Besuch abstatten.
https://boomerangcasino.one/
Tipico ist eine der führenden Online-Wettseiten in Deutschland, und sein Casino-Bereich, alles Spitze Tipico Casino, ist beliebt bei Spielern auf der ganzen Welt. Mit einer Vielzahl von Spielen und einer benutzerfreundlichen Oberfläche bietet das alles Spitze Tipico Casino ein erstklassiges Spielerlebnis.
Das Casino bietet eine breite Auswahl an Spielen, darunter klassische Tischspiele wie Blackjack, Roulette und Poker, sowie eine Vielzahl von Spielautomaten und Jackpot-Slots. Die Spiele sind von fГјhrenden Anbietern wie NetEnt, Microgaming und Play’n GO entwickelt worden, was fГјr eine hohe QualitГ¤t und ein spannendes Spielerlebnis sorgt.
Darüber hinaus bietet das alles Spitze Tipico Casino eine Vielzahl von Bonusangeboten und Aktionen für Spieler. Neue Spieler können sich über einen großzügigen Willkommensbonus freuen, während treue Spieler regelmäßig mit Freispielen und anderen Belohnungen belohnt werden.
Die Ein- und Auszahlungen im Casino sind sicher und einfach, und der Kundenservice steht rund um die Uhr zur Verfügung, um bei Fragen oder Problemen zu helfen. Das alles Spitze Tipico Casino ist auch auf mobilen Geräten verfügbar, sodass Spieler ihre Lieblingsspiele jederzeit und überall genießen können.
Insgesamt bietet das alles Spitze Tipico Casino ein erstklassiges Spielerlebnis mit einer Vielzahl von Spielen, groГџzГјgigen Boni und einem exzellenten Kundenservice. Es ist kein Wunder, dass es bei Spielern auf der ganzen Welt so beliebt ist. Probieren Sie es doch selbst aus und erleben Sie die Spannung und Aufregung des alles Spitze Tipico Casinos.
https://tipicocasino.one/
ומוכנות לפגישה ייחודית! כשמדובר בחיפוש אחר פינוק אולטימטיבי בשילוב מגע וחושניות, שום דבר לא יכול לנצח את החוויה עם . יפות חוויה בטוחה והכי מספקת. מאפשרות לגברים לחקור את חושניותם, לחוות הנאה אמיתית ולהצעיר את גופם ואת מוחם מחדש. הפרטיות פינוק דירות דיסקרטיות בתל אביב
Ist Zet Casino legitim?
Zet Casino ist eine Online-GlГјcksspiel-Plattform, die eine Vielzahl von Spielen anbietet, darunter Slots, Tischspiele und Live-Casino-Spiele. Viele Menschen fragen sich jedoch, ob Zet Casino legitim ist und ob es sicher ist, dort zu spielen.
Zunächst einmal ist Zet Casino von der Regierung von Curacao lizenziert und reguliert, was bedeutet, dass es den strengen Vorschriften des Glücksspielsektors entspricht. Die Website verwendet auch die neueste Verschlüsselungstechnologie, um sicherzustellen, dass alle Transaktionen und persönlichen Informationen der Spieler sicher und geschützt sind.
Darüber hinaus arbeitet Zet Casino mit einer Reihe renommierter Software-Anbieter zusammen, um sicherzustellen, dass alle Spiele fair und zufällig sind. Die Website verfügt außerdem über eine Zufallszahlengenerierung, die sicherstellt, dass die Ergebnisse der Spiele nicht manipuliert werden können.
Zet Casino bietet auch einen zuverlässigen Kundenservice, der rund um die Uhr per Live-Chat, E-Mail und Telefon erreichbar ist. Die Mitarbeiter des Kundendienstes sind professionell und hilfsbereit und stehen den Spielern bei allen Fragen oder Anliegen zur Verfügung.
Alles in allem ist Zet Casino eine legitime und vertrauenswГјrdige Online-GlГјcksspiel-Plattform, die Spielern eine sichere und faire Spielerfahrung bietet. Es ist wichtig, verantwortungsbewusst zu spielen und die AGB der Website zu beachten, um sicherzustellen, dass man eine positive Spielerfahrung hat.
https://zetcasino.one/
Das Tipico Casino bietet seinen Spielern eine Vielzahl von verschiedenen Boni und Aktionen an, um das Spielerlebnis noch spannender und lukrativer zu gestalten. In diesem Artikel werden die verschiedenen aktiven Boni im Tipico Casino näher betrachtet.
Einer der beliebtesten Boni im Tipico Casino ist der Willkommensbonus für neue Spieler. Mit diesem Bonus können Spieler ihre erste Einzahlung im Casino verdoppeln und somit ihre Gewinnchancen erhöhen. Darüber hinaus gibt es regelmäßig verschiedene Aktionen, bei denen Spieler zusätzliche Bonusguthaben oder Freispiele erhalten können.
Ein weiterer Vorteil des Tipico Casinos ist das Treueprogramm, das es Spielern ermöglicht, für ihre Aktivitäten im Casino belohnt zu werden. Je mehr ein Spieler im Casino spielt, desto mehr Punkte sammelt er und desto höher steigt er im Treueprogramm auf. Mit jedem neuen Level können Spieler von verschiedenen Vergünstigungen und Boni profitieren.
Des Weiteren werden im Tipico Casino regelmäßig Turniere und Wettbewerbe veranstaltet, bei denen Spieler attraktive Preise wie Bargeldgewinne oder Freispiele gewinnen können. Diese Veranstaltungen sorgen nicht nur für zusätzliche Spannung im Casino, sondern bieten auch die Möglichkeit, mit anderen Spielern in Wettbewerb zu treten.
Insgesamt bietet das Tipico Casino eine Vielzahl von aktiven Boni und Aktionen, die das Spielerlebnis noch unterhaltsamer und lukrativer gestalten. Spieler sollten regelmäßig die Promotionsseite des Casinos besuchen, um über die neuesten Aktionen informiert zu bleiben und keine lukrativen Angebote zu verpassen.
https://tipicocasino.one/
1win casino
Boomerang Casino Erfahrungen
Das Boomerang Casino ist ein Online-Casino, das seinen Kunden eine groГџe Auswahl an Spielen und ein einzigartiges Spielerlebnis bietet. Doch wie sind die Erfahrungen der Spieler mit diesem Casino?
Viele Spieler loben das Boomerang Casino für sein breites Spektrum an Spielen. Von klassischen Tischspielen wie Blackjack und Roulette bis hin zu modernen Video-Slots ist für jeden Geschmack etwas dabei. Die Spiele stammen von renommierten Softwareanbietern wie NetEnt, Microgaming und Playtech, was für eine hohe Qualität und Fairness der Spiele spricht.
Auch die Boni und Aktionen im Boomerang Casino können sich sehen lassen. Neue Spieler erhalten oft großzügige Willkommensboni, und auch Bestandskunden werden regelmäßig mit Freispielen und Reload-Boni belohnt. Die Umsatzbedingungen sind fair und transparent, was von vielen Spielern positiv hervorgehoben wird.
Ein weiterer Pluspunkt des Boomerang Casinos ist der Kundenservice. Die Mitarbeiter sind freundlich, kompetent und rund um die Uhr erreichbar. Probleme und Anliegen werden schnell und effizient gelöst, was für viele Spieler ein wichtiges Kriterium bei der Wahl eines Online-Casinos ist.
Natürlich gibt es auch negative Erfahrungen mit dem Boomerang Casino. Einige Spieler bemängeln zum Beispiel die begrenzten Zahlungsmöglichkeiten oder die langen Auszahlungszeiten. Auch die mobile App des Casinos könnte noch verbessert werden, da sie manchmal etwas instabil läuft.
Insgesamt scheint das Boomerang Casino jedoch bei den meisten Spielern gut anzukommen. Die groГџe Auswahl an Spielen, die attraktiven Boni und der gute Kundenservice machen das Casino zu einer interessanten Option fГјr alle, die gerne online spielen.
Wenn Sie also auf der Suche nach einem neuen Online-Casino sind, sollten Sie das Boomerang Casino auf jeden Fall einmal ausprobieren. Vielleicht gehören auch Sie schon bald zu den zufriedenen Spielern, die positive Erfahrungen mit diesem Casino gemacht haben. Viel Spaß und Glück beim Spielen!
https://boomerangcasino.one/
Wenn es um Online Casinos geht, sind Freispiele eine der begehrtesten Aktionen für Spieler. Tipico Casino bietet regelmäßig Freispiele als Teil ihres Bonusprogramms an, und in diesem Artikel werden wir Ihnen zeigen, wie Sie diese Freispiele einlösen können.
Zunächst einmal müssen Sie ein Konto bei Tipico Casino haben, um von den Angeboten profitieren zu können. Wenn Sie bereits angemeldet sind, überprüfen Sie regelmäßig Ihre E-Mails oder die Webseite des Casinos, um über aktuelle Aktionen informiert zu werden. Oft werden Freispiele als Belohnung für Einzahlungen oder als Teil von Turnieren angeboten.
Sobald Sie Freispiele erhalten haben, müssen Sie diese einlösen, um sie zu nutzen. Gehen Sie einfach zu den entsprechenden Spielautomaten, bei denen die Freispiele gültig sind, und öffnen Sie das Spiel. Normalerweise erhalten Sie eine Benachrichtigung über die verfügbaren Freispiele, und Sie können mit dem Spielen beginnen.
Es ist wichtig zu beachten, dass Freispiele oft mit bestimmten Umsatzbedingungen verbunden sind. Das bedeutet, dass Sie die Gewinne aus den Freispielen eine gewisse Anzahl von Malen umsetzen müssen, bevor Sie sie auszahlen lassen können. Stellen Sie sicher, dass Sie die Bedingungen genau lesen, um Missverständnisse zu vermeiden.
Insgesamt sind Freispiele eine großartige Möglichkeit, um zusätzliche Gewinne im Casino zu erzielen. Mit Tipico Casino können Sie regelmäßig von Freispielen profitieren und Ihre Gewinnchancen erhöhen. Nutzen Sie diese Angebote und haben Sie Spaß beim Spielen!
https://tipicocasino.one/
Kod promocyjny Boomerang Casino
Boomerang Casino ist ein aufstrebendes Online-Casino, das seinen Spielern eine Vielzahl von aufregenden Spielen und großzügigen Boni bietet. Einer der beliebtesten Angebote ist der kod promocyjny Boomerang Casino, der es den Spielern ermöglicht, zusätzliche Boni und Belohnungen zu erhalten.
Um den kod promocyjny Boomerang Casino zu nutzen, müssen Spieler einfach den Code während der Registrierung oder Einzahlung eingeben. Durch die Eingabe des Codes können Spieler zusätzliche Freispiele, Bonusgeld oder andere attraktive Angebote erhalten.
Der kod promocyjny Boomerang Casino ist eine großartige Möglichkeit, um das Spielerlebnis zu verbessern und mehr aus den Spielen herauszuholen. Es lohnt sich daher, regelmäßig nach neuen Codes Ausschau zu halten und diese zu nutzen, um die besten Angebote zu erhalten.
Boomerang Casino bietet eine Vielzahl von Spielen, darunter Spielautomaten, Tischspiele und Live-Casino-Spiele. Mit dem kod promocyjny Boomerang Casino können Spieler diese Spiele in vollem Umfang genießen und gleichzeitig von zusätzlichen Belohnungen profitieren.
Insgesamt ist der kod promocyjny Boomerang Casino eine großartige Möglichkeit, um das Spielerlebnis zu verbessern und von attraktiven Angeboten zu profitieren. Spieler sollten daher nicht zögern, den Code bei ihrer nächsten Einzahlung zu nutzen und die vielen Vorteile zu genießen, die Boomerang Casino zu bieten hat.
https://boomerangcasino.one/
Das Tipico Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen für Spieler bietet. Die Website ist benutzerfreundlich gestaltet und ermöglicht es den Nutzern, leicht auf ihre Lieblingsspiele zuzugreifen.
Das Tipico Casino bietet eine breite Palette von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Die Plattform arbeitet mit renommierten Softwareanbietern zusammen, um hochwertige Spiele anzubieten, die eine realistische Casino-Erfahrung bieten.
Ein weiterer Pluspunkt des Tipico Casinos ist der Kundenservice, der rund um die Uhr verfügbar ist, um den Spielern bei Fragen oder Problemen zu helfen. Die Website verfügt auch über sichere Zahlungsmethoden, um sicherzustellen, dass die Spieler ihre Gewinne schnell und sicher erhalten können.
Darüber hinaus bietet das Tipico Casino regelmäßig spannende Aktionen und Boni für seine Spieler an. Dies kann von Einzahlungsboni bis hin zu Freispielen reichen, die den Spielern helfen können, ihre Gewinne zu steigern.
Insgesamt ist das Tipico Casino eine erstklassige GlГјcksspielplattform, die eine breite Palette von Spielen, erstklassigem Kundenservice und groГџzГјgigen Promotionen bietet. Spieler sollten die Website besuchen, um ein erstklassiges Online-Casino-Erlebnis zu genieГџen.
https://tipicocasino.one/
Das Boomerang Casino ist eine beliebte Online-GlГјcksspielseite, die eine Vielzahl von Casinospielen anbietet, darunter Slots, Tischspiele und Live-Dealer-Spiele. Um sicherzustellen, dass Spieler ein sicheres und faires Spielerlebnis haben, verlangt das Boomerang Casino von seinen Nutzern die Bereitstellung von Dokumenten zur ГњberprГјfung.
Die Casino-Dokumentation ist ein wichtiger Schritt im Registrierungsprozess, der dazu dient, die Identität des Spielers zu bestätigen und die Sicherheit des Kontos zu gewährleisten. Die erforderlichen Dokumente variieren je nach Land und können unter anderem einen Lichtbildausweis wie einen Personalausweis oder Reisepass, einen Adressnachweis wie eine aktuelle Stromrechnung und gegebenenfalls eine Kopie der Kreditkarte umfassen.
Die Überprüfung der Dokumente ist ein Standardverfahren in der Glücksspielindustrie, das von den Regulierungsbehörden vorgeschrieben ist, um sicherzustellen, dass Spieler keine gefälschten Konten erstellen oder betrügerische Aktivitäten durchführen. Die Sicherheit und Fairness der Spiele stehen bei seriösen Online-Casinos wie dem Boomerang Casino an erster Stelle, und die Casino-Dokumentation ist ein wichtiger Schritt, um diese Standards zu erfüllen.
Sobald die Dokumente überprüft und akzeptiert wurden, können die Spieler ihr Konto vollständig nutzen und von allen Funktionen und Angeboten des Boomerang Casinos profitieren. Es ist wichtig, dass Spieler die erforderlichen Dokumente schnell bereitstellen, um Verzögerungen bei Auszahlungen zu vermeiden und ein reibungsloses Spielerlebnis zu gewährleisten.
Insgesamt ist die Casino-Dokumentation ein wichtiger Aspekt des Online-Glücksspiels, der die Sicherheit und Integrität der Spieler sowie des Casinos selbst gewährleistet. Durch die Bereitstellung der erforderlichen Dokumente können Spieler bei vertrauenswürdigen Online-Casinos wie dem Boomerang Casino ein sicheres und unterhaltsames Spielerlebnis genießen.
https://boomerangcasino.one/
Tipico Sportwette zu Casino
Sportwetten und Glücksspiele erfreuen sich weltweit großer Beliebtheit. Bei Tipico, einem der führenden Anbieter von Sportwetten in Deutschland, können Kunden nicht nur auf ihre Lieblingssportarten wetten, sondern auch das Online-Casino nutzen. Das bedeutet, dass Tipico neben den klassischen Sportwetten auch eine Vielzahl von Casino-Spielen wie Spielautomaten, Blackjack, Roulette und Videopoker anbietet.
Das Casino von Tipico ist sowohl über die Webseite als auch über die mobile App des Anbieters zugänglich. Die Spieler haben die Möglichkeit, aus einer Vielzahl von Spielen zu wählen und können so ihre Lieblingsspiele jederzeit und überall genießen. Das Angebot an Casino-Spielen wird ständig erweitert und umfasst sowohl klassische als auch neuere Titel von renommierten Anbietern wie NetEnt, Microgaming und Evolution Gaming.
Ein besonderer Vorteil des Casinos bei Tipico ist die Möglichkeit, verschiedene Boni und Aktionen zu nutzen. Spieler können von Willkommensangeboten, Reload-Boni und Freispielen profitieren, um ihr Spielerlebnis noch spannender zu gestalten. Darüber hinaus garantiert Tipico seinen Kunden ein sicheres und faires Spielerlebnis, da das Unternehmen strengen Richtlinien und Vorschriften im Bereich des Glücksspiels unterliegt.
Insgesamt bietet die Kombination aus Sportwetten und Casino-Spielen bei Tipico den Kunden ein abwechslungsreiches und unterhaltsames Spielerlebnis. Egal, ob man sich für Sportwetten interessiert oder lieber im Casino spielt, bei Tipico finden Spieler alles, was das Herz begehrt. Mit der Möglichkeit, jederzeit und überall zu spielen, verschiedenen Boni und einer breiten Auswahl an Spielen ist Tipico eine hervorragende Wahl für alle Glücksspiel-Fans.
https://tipicocasino.one/
Boomerang Casino Erfahrungen
Boomerang Casino ist ein Online-Casino, das seit seiner GrГјndung im Jahr 2020 schnell an Beliebtheit gewonnen hat. Das Casino bietet eine Vielzahl von Spielen von renommierten Anbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen. DarГјber hinaus bietet das Casino eine benutzerfreundliche Plattform und attraktive Boni fГјr neue Spieler.
Viele Spieler haben positive Erfahrungen mit Boomerang Casino gemacht und schätzen insbesondere die große Auswahl an Spielen. Von klassischen Slots bis hin zu Live-Casino-Spielen ist für jeden Geschmack etwas dabei. Die Qualität der Spiele ist ausgezeichnet und sorgt für ein unterhaltsames Spielerlebnis.
Auch die Boni und Aktionen von Boomerang Casino werden von den Spielern geschätzt. Neue Spieler erhalten einen großzügigen Willkommensbonus, der ihre Einzahlung verdoppelt und Freispiele beinhaltet. Darüber hinaus gibt es regelmäßig Reload-Boni, Freispiele und andere attraktive Angebote für treue Spieler.
Ein weiterer Pluspunkt von Boomerang Casino ist der Kundenservice. Spieler können den Support rund um die Uhr per Live-Chat oder E-Mail erreichen und erhalten schnell Hilfe bei Fragen oder Problemen.
Insgesamt sind die Erfahrungen mit Boomerang Casino Гјberwiegend positiv. Das Casino Гјberzeugt mit einer groГџen Auswahl an Spielen, attraktiven Boni und einem professionellen Kundenservice. Wer auf der Suche nach einem unterhaltsamen und sicheren Online-Casino ist, sollte Boomerang Casino definitiv eine Chance geben.
https://boomerangcasino.one/
Online Casino Geld ZurГјck Tipico
Online-Casinos sind heutzutage sehr populär und bieten eine Vielzahl von Spielen, die von Spielern aus der ganzen Welt genossen werden können. Eines der bekanntesten Online-Casinos ist Tipico, das eine breite Palette von Spielen anbietet, darunter Spielautomaten, Roulette, Blackjack und vieles mehr. Aber was passiert, wenn Spieler Geld verlieren? Können sie ihr Geld zurückbekommen?
Die Antwort auf diese Frage hängt von verschiedenen Faktoren ab. Zunächst einmal ist es wichtig zu beachten, dass Glücksspiel in vielen Ländern streng reguliert ist und es bestimmte Richtlinien gibt, die von den Online-Casinos eingehalten werden müssen. Dies bedeutet, dass es nicht immer möglich ist, Geld zurückzufordern, wenn man verliert.
Jedoch bieten einige Online-Casinos wie Tipico ihren Spielern die Möglichkeit, ihr Geld zurückzugewinnen, indem sie verschiedene Bonusse und Promotionen anbieten. Zum Beispiel gibt es oft Cashback-Aktionen, bei denen Spieler einen Teil ihres verlorenen Geldes zurückerhalten können. Diese Aktionen sind in der Regel zeitlich begrenzt und erfordern, dass Spieler bestimmte Bedingungen erfüllen, um in den Genuss des Cashbacks zu kommen.
Eine weitere Möglichkeit, Geld zurückzubekommen, ist, sich direkt an den Kundendienst des Online-Casinos zu wenden. Oft sind die Mitarbeiter bereit, Spielern entgegenzukommen und individuelle Lösungen anzubieten, um sicherzustellen, dass sie zufrieden sind. Es lohnt sich also auf jeden Fall, den Kundendienst zu kontaktieren, wenn man Probleme hat und sein Geld zurückfordern möchte.
Insgesamt ist es also möglich, Geld zurückzubekommen, wenn man in einem Online-Casino wie Tipico spielt. Es ist jedoch wichtig, die Regeln und Bedingungen des jeweiligen Casinos zu beachten und gegebenenfalls den Kundendienst zu kontaktieren, um Unterstützung zu erhalten. Mit etwas Glück und Geduld sollten Spieler in der Lage sein, ihr verlorenes Geld zurückzuholen und weiterhin Spaß beim Spielen zu haben.
https://tipicocasino.one/
Insightful piece
http://body-care-shop.com
Boomerang Casino Deutsche Lizenz: Ein sicherer Ort zum Spielen
Das Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die ihren Spielern ein breites Angebot an Spielen bietet. Von Slots und Tischspielen bis hin zu Live-Casino-Spielen – hier ist für jeden Geschmack etwas dabei. Doch neben dem umfangreichen Spieleangebot ist es vor allem die deutsche Lizenz, die das Boomerang Casino zu einem sicheren Ort zum Spielen macht.
Die deutsche Lizenz garantiert den Spielern, dass das Casino strengen Richtlinien und Vorschriften entspricht, um ein faires und sicheres Spielerlebnis zu gewährleisten. Dies bedeutet, dass das Casino seine Spiele regelmäßig auf ihre Fairness überprüfen lässt und dass die persönlichen Daten der Spieler geschützt sind.
Darüber hinaus bietet das Boomerang Casino eine Vielzahl von sicheren Zahlungsmethoden an, die es den Spielern ermöglichen, ihre Ein- und Auszahlungen schnell und einfach durchzuführen. Ob mit Kreditkarte, E-Wallet oder Banküberweisung – hier ist für jeden die passende Zahlungsmethode dabei.
Auch der Kundenservice des Boomerang Casinos überzeugt mit seiner Professionalität und Schnelligkeit. Egal ob es um technische Probleme, Spielanfragen oder Zahlungsschwierigkeiten geht – das Support-Team steht den Spielern rund um die Uhr zur Verfügung.
Zusammenfassend lässt sich sagen, dass das Boomerang Casino mit seiner deutschen Lizenz ein sicherer Ort zum Spielen ist. Die Vielzahl an Spielen, die sicheren Zahlungsmethoden und der professionelle Kundenservice machen das Casino zu einer erstklassigen Wahl für alle, die auf der Suche nach einem unterhaltsamen und sicheren Online-Casino-Erlebnis sind.
https://boomerangcasino.one/
Tipico Casino Bonus ohne Einzahlung: Holen Sie sich Ihr Gratis-Guthaben
Das Tipico Casino bietet seinen Kunden nicht nur eine große Auswahl an Spielen und attraktive Bonusangebote, sondern auch die Möglichkeit, ohne Einzahlung von eigenem Geld zu spielen. Der sogenannte Tipico Casino Bonus ohne Einzahlung ist eine großartige Möglichkeit, um das Casino kennenzulernen und erste Gewinne zu erzielen, ohne Risiko eingehen zu müssen.
Um den Tipico Casino Bonus ohne Einzahlung zu erhalten, müssen Sie sich lediglich als neuer Kunde im Casino registrieren. Nach erfolgreicher Registrierung erhalten Sie automatisch Ihr Gratis-Guthaben gutgeschrieben, mit dem Sie sofort loslegen können. Dieses Gratis-Guthaben kann für eine Vielzahl von Spielen im Casino genutzt werden, darunter Slots, Tischspiele und vieles mehr.
Der Tipico Casino Bonus ohne Einzahlung bietet Ihnen die Möglichkeit, das Casino und seine Spiele in aller Ruhe auszuprobieren, ohne dabei Ihr eigenes Geld riskieren zu müssen. Sie können erste Gewinne erzielen, ohne selbst einen Cent einzahlen zu müssen. Dies macht den Tipico Casino Bonus ohne Einzahlung zu einer attraktiven Option für alle, die das Casino erst einmal unverbindlich testen möchten.
Wenn Sie sich für den Tipico Casino Bonus ohne Einzahlung interessieren, sollten Sie jedoch beachten, dass dieser in der Regel an bestimmte Umsatzbedingungen geknüpft ist. Bevor Sie sich Ihre Gewinne auszahlen lassen können, müssen Sie den Bonus bestimmte Male umsetzen. Es ist daher wichtig, die jeweiligen Bedingungen genau zu lesen, bevor Sie den Bonus in Anspruch nehmen.
Insgesamt bietet der Tipico Casino Bonus ohne Einzahlung eine tolle Gelegenheit, um das Casino risikofrei kennenzulernen und erste Gewinne zu erzielen. Wenn Sie sich als neuer Kunde im Tipico Casino registrieren, sollten Sie also unbedingt auch den Bonus ohne Einzahlung in Anspruch nehmen. Viel SpaГџ und Erfolg beim Spielen!
https://tipicocasino.one/
Boomerang Casino – Vertrauen durch Trustpilot-Bewertungen
Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und attraktiven Boni für ihre Kunden anbietet. Doch wie können Spieler sicher sein, dass dieses Casino vertrauenswürdig und zuverlässig ist? Eine Möglichkeit, dies herauszufinden, ist durch die Bewertungen auf Trustpilot.
Trustpilot ist eine unabhängige Plattform, auf der Kunden ihre Erfahrungen mit Unternehmen teilen können. Diese Bewertungen sind ein nützliches Werkzeug, um die Reputation und Glaubwürdigkeit eines Unternehmens zu überprüfen. Auch Boomerang Casino hat eine Vielzahl von Bewertungen auf Trustpilot erhalten, die einen Einblick in die Kundenzufriedenheit geben.
Die meisten Bewertungen für Boomerang Casino auf Trustpilot sind positiv, wobei die Spieler die breite Auswahl an Spielen, die schnellen Auszahlungen und den zuvorkommenden Kundenservice loben. Viele Kunden haben auch erwähnt, dass sie sich sicher fühlen, bei Boomerang Casino zu spielen, da das Unternehmen lizenziert und reguliert ist.
Neben den positiven Bewertungen gibt es auch einige negative Bewertungen für Boomerang Casino auf Trustpilot. Diese umfassen Beschwerden über technische Probleme, Verzögerungen bei Auszahlungen und eingeschränkten Zugang für bestimmte Länder. Trotzdem scheint Boomerang Casino bestrebt zu sein, auf diese Kritikpunkte einzugehen und Lösungen anzubieten.
Insgesamt scheint Boomerang Casino ein vertrauenswГјrdiger Anbieter von Online-GlГјcksspielen zu sein, der sich um die Zufriedenheit seiner Kunden bemГјht. Die Bewertungen auf Trustpilot sind ein nГјtzliches Werkzeug, um die GlaubwГјrdigkeit von Boomerang Casino zu ГјberprГјfen und Spielern ein GefГјhl der Sicherheit zu geben. Es ist empfehlenswert, die Bewertungen zu lesen und sich selbst ein Bild von Boomerang Casino zu machen, bevor man sich entscheidet, dort zu spielen.
https://boomerangcasino.one/
Tipico Casino NJ ist eine neues Online-Casino in New Jersey, das Spielern ein aufregendes und sicheres Spielerlebnis bietet. Das Casino, das von der bekannten Marke Tipico betrieben wird, bietet Spielern eine Vielzahl von Spieloptionen, darunter Spielautomaten, Tischspiele und Live-Dealer-Spiele.
Ein wichtiger Aspekt von Tipico Casino NJ ist die Sicherheit der Spieler. Das Casino verwendet die neueste Technologie, um sicherzustellen, dass alle persönlichen Daten und Transaktionen der Spieler geschützt sind. Spieler können also beruhigt sein, dass ihre Informationen sicher sind, während sie ihre Lieblingsspiele genießen.
Ein weiterer großer Vorteil von Tipico Casino NJ ist die große Auswahl an Spielen, die es Spielern bietet. Von klassischen Spielautomaten bis hin zu verschiedenen Varianten von Blackjack, Roulette und anderen Tischspielen gibt es für jeden Spieler etwas zu entdecken. Darüber hinaus bietet das Casino auch Live-Dealer-Spiele, die ein authentisches Casino-Erlebnis bieten und es den Spielern ermöglichen, mit echten Dealern und anderen Spielern zu interagieren.
Tipico Casino NJ bietet auch großzügige Boni und Aktionen für neue und bestehende Spieler an. Von Willkommensboni über Einzahlungsboni bis hin zu Treueprogrammen gibt es viele Möglichkeiten, um zusätzliches Geld und Belohnungen zu verdienen. Diese Boni können Spielern helfen, ihr Guthaben zu erhöhen und mehr Zeit mit ihren Lieblingsspielen zu verbringen.
Insgesamt ist Tipico Casino NJ eine groГџartige Option fГјr Spieler in New Jersey, die ein erstklassiges Online-Casino-Erlebnis suchen. Mit einer breiten Palette von Spielen, erstklassiger Sicherheit und lukrativen Boni ist das Casino eine gute Wahl fГјr alle, die SpaГџ und Spannung suchen. Besuchen Sie noch heute Tipico Casino NJ und beginnen Sie mit dem Spielen!
https://tipicocasino.one/
Das Boomerang Casino ist ein aufregendes Online-Casino, das Spielern eine Vielzahl von Spielen und spannenden Funktionen bietet. Mit einer benutzerfreundlichen Oberfläche und einer beeindruckenden Auswahl an Spielen ist es eine der besten Optionen für Casino-Enthusiasten, die nach einer unterhaltsamen und lohnenden Erfahrung suchen.
Das Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Video-Poker und Live-Casino-Spiele. Die Spiele werden von erstklassigen Softwareanbietern wie NetEnt, Microgaming und Evolution Gaming bereitgestellt, was bedeutet, dass die Spieler eine ausgezeichnete Grafik und reibungslose Spielabläufe erwarten können.
Ein Hauptmerkmal des Boomerang Casinos ist das Bonussystem, das großzügige Angebote und Werbeaktionen für Spieler aller Erfahrungsstufen bietet. Neue Spieler können einen Willkommensbonus beanspruchen, der Freispiele und zusätzliches Guthaben beinhaltet. Darüber hinaus gibt es regelmäßig wechselnde Aktionen, bei denen Spieler zusätzliche Belohnungen erhalten können.
Ein weiterer Vorteil des Boomerang Casinos ist die mobile Kompatibilität, die es Spielern ermöglicht, ihre Lieblingsspiele von überall aus zu spielen. Die mobile Version der Website ist benutzerfreundlich und bietet eine nahtlose Spielerfahrung auf iOS- und Android-Geräten.
Insgesamt ist das Boomerang Casino eine ausgezeichnete Wahl für Spieler, die nach einer unterhaltsamen und sicheren Online-Casino-Erfahrung suchen. Mit einer beeindruckenden Auswahl an Spielen, großzügigen Boni und einer benutzerfreundlichen Oberfläche ist es definitiv einen Besuch wert.
https://boomerangcasino.one/
https://adzan.online/
Tipico Live Casino Erfahrungen
Das Tipico Live Casino ist einer der beliebtesten Anbieter für Online-Spiele in Deutschland. Spieler können hier eine große Auswahl an verschiedenen Casino-Spielen genießen, darunter Roulette, Blackjack, Baccarat und Poker. Das Live Casino wird von professionellen und freundlichen Dealern betreut, die für ein authentisches Casino-Erlebnis sorgen.
Die Erfahrungen vieler Spieler mit dem Tipico Live Casino sind durchweg positiv. Besonders lobend wird die hohe Qualität der Live-Übertragung und die reibungslose Funktionalität der Spiele erwähnt. Die Dealer sind nicht nur kompetent, sondern auch unterhaltsam und sorgen so für eine angenehme Atmosphäre am Spieltisch.
Ein weiterer Pluspunkt des Tipico Live Casinos ist die große Auswahl an verschiedenen Spielen und Einsätzen. Egal ob Anfänger oder erfahrener Spieler, hier findet jeder das passende Spiel für sich. Zudem sind die Gewinnchancen im Tipico Live Casino fair und transparent, sodass Spieler sich auf ein faires Spielumfeld verlassen können.
Einige Spieler berichten auch von lukrativen Gewinnen im Tipico Live Casino. Durch die Möglichkeit, mit anderen Spielern und dem Dealer interagieren zu können, wird das Spielerlebnis noch einmal spannender und unterhaltsamer.
Insgesamt können wir sagen, dass das Tipico Live Casino eine empfehlenswerte Option für alle Casino-Fans ist. Mit einer großen Auswahl an Spielen, professionellen Dealern und fairen Gewinnchancen wird hier ein erstklassiges Casino-Erlebnis geboten. Probieren Sie es selbst aus und machen Sie Ihre eigenen Tipico Live Casino Erfahrungen!
https://tipicocasino.one/
Boomerang Casino Recensioni: Ein Blick in die Welt des Online-GlГјcksspiels
Online-Casinos erfreuen sich immer größerer Beliebtheit, da sie den Spielern die Möglichkeit bieten, bequem von zu Hause aus zu spielen und dabei echtes Geld zu gewinnen. Eines der neuesten Casinos auf dem Markt ist das Boomerang Casino, das mit seinem breiten Angebot an Spielen und attraktiven Boni die Aufmerksamkeit vieler Spieler auf sich zieht.
Die Boomerang Casino Recensioni, also die Bewertungen und Erfahrungsberichte der Spieler, sind durchweg positiv. Viele loben die große Auswahl an Slots, Tischspielen und Live-Casino-Spielen, die für jeden Geschmack etwas zu bieten haben. Darüber hinaus werden auch die schnellen Auszahlungen und der kompetente Kundenservice des Casinos gelobt. Die Spieler schätzen auch die Vielzahl an Zahlungsmethoden und die Sicherheit, die das Boomerang Casino bietet.
Ein weiterer Pluspunkt des Boomerang Casinos sind die großzügigen Boni und Aktionen, die regelmäßig angeboten werden. Neue Spieler können sich über einen Willkommensbonus freuen, der ihre erste Einzahlung verdoppelt und ihnen so zusätzliche Chancen auf Gewinne bietet. Darüber hinaus gibt es auch regelmäßige Turniere und Verlosungen, bei denen die Spieler attraktive Preise gewinnen können.
Insgesamt hinterlässt das Boomerang Casino bei den Spielern einen positiven Eindruck und ist definitiv einen Besuch wert. Mit einer ansprechenden Spielauswahl, lukrativen Boni und einem zuverlässigen Kundenservice bietet das Casino alles, was man sich von einem guten Online-Casino wünscht. Wer also Lust auf spannende Glücksspiele hat, sollte das Boomerang Casino definitiv einmal ausprobieren und sich selbst von seinen Qualitäten überzeugen.
https://boomerangcasino.one/
Tipico ist einer der führenden Anbieter von Online-Casinospielen in Deutschland. Eine der beliebtesten Aktionen von Tipico sind die Casino Freispiele, die den Spielern die Möglichkeit bieten, kostenlos an ausgewählten Spielautomaten zu spielen. In diesem Artikel werden wir uns genauer mit den Casino Freispielen bei Tipico befassen.
Die Casino Freispiele bei Tipico sind eine großartige Möglichkeit, neue Spiele auszuprobieren und dabei echtes Geld zu gewinnen. Die Freispiele können auf verschiedene Arten erhalten werden, zum Beispiel als Willkommensbonus für neue Spieler oder als regelmäßige Aktionen für bestehende Kunden. Oftmals sind die Freispiele an bestimmte Spielautomaten gebunden, sodass die Spieler die Chance haben, die verschiedenen Titel des Casinos kennenzulernen.
Um die Casino Freispiele bei Tipico nutzen zu können, müssen die Spieler in der Regel bestimmte Umsatzbedingungen erfüllen. Diese können beispielsweise die Anzahl der Male sein, die der Gewinn aus den Freispielen umgesetzt werden muss, bevor er ausgezahlt werden kann. Es ist wichtig, die Bedingungen für die Freispiele genau zu prüfen, um sicherzustellen, dass man das Maximum aus der Aktion herausholen kann.
Zusätzlich zu den regulären Casino Freispielen bietet Tipico auch immer wieder spezielle Aktionen und Turniere an, bei denen die Spieler extra Freispiele oder andere Bonusangebote gewinnen können. Es lohnt sich daher, regelmäßig die Promotionsseite von Tipico zu besuchen, um keine der lukrativen Angebote zu verpassen.
Insgesamt sind die Casino Freispiele bei Tipico eine attraktive Möglichkeit, kostenlos an spannenden Spielautomaten zu spielen und dabei echte Gewinne zu erzielen. Mit den regelmäßigen Aktionen und Sonderangeboten bietet Tipico seinen Kunden immer wieder neue Anreize, um das Casino-Abenteuer noch aufregender zu gestalten.
Wenn Sie also auf der Suche nach Unterhaltung und Gewinnmöglichkeiten sind, lohnt es sich, die Casino Freispiele bei Tipico in Anspruch zu nehmen und Ihr Glück an den Spielautomaten zu versuchen. Viel Spaß und Erfolg!
https://tipicocasino.one/
Das Boomerang Casino ist ein beliebtes Online-Casino, das Spielern eine Vielzahl von Spielen, groГџzГјgige Boni und eine benutzerfreundliche Plattform bietet. In diesem Artikel werden wir die Avis (Bewertungen) des Boomerang Casinos genauer unter die Lupe nehmen.
Das Boomerang Casino hat von den Spielern insgesamt positive Bewertungen erhalten. Viele loben die groГџe Auswahl an Spielen, die von renommierten Softwareanbietern wie NetEnt, Microgaming und Play’n GO bereitgestellt werden. Von Slots Гјber Tischspiele bis hin zu Live-Casino-Spielen gibt es fГјr jeden Spieler etwas Passendes.
Die Aktionen und Boni des Boomerang Casinos werden ebenfalls gelobt. Neue Spieler erhalten einen großzügigen Willkommensbonus bei ihrer ersten Einzahlung sowie regelmäßige Promotionen und Boni für treue Spieler. Die Umsatzbedingungen für die Boni sind fair und transparent.
Die Benutzeroberfläche des Boomerang Casinos wird auch positiv bewertet. Die Webseite ist übersichtlich gestaltet und einfach zu navigieren. Spieler können problemlos zwischen den verschiedenen Spielen und Funktionen der Seite wechseln.
Einige Spieler haben jedoch Bedenken hinsichtlich des Kundensupports geäußert. Es wird bemängelt, dass die Reaktionszeit des Kundendienstes manchmal länger als erwartet ist und dass nicht alle Anfragen zufriedenstellend beantwortet werden. Das Boomerang Casino sollte daher seine Kundenbetreuung verbessern, um die Zufriedenheit der Spieler zu gewährleisten.
Insgesamt sind die Avis zum Boomerang Casino größtenteils positiv. Die große Auswahl an Spielen, die großzügigen Boni und die benutzerfreundliche Plattform machen das Casino zu einer beliebten Wahl unter Spielern. Mit einigen Verbesserungen im Kundenservice könnte das Boomerang Casino noch besser werden.
https://boomerangcasino.one/
Im Jahr 2019 bietet das Tipico Casino seinen Kunden einen groГџzГјgigen Bonus, um sie fГјr ihre Treue zu belohnen. Dieser Bonus kann in Form von Freispielen, Einzahlungsboni oder sogar Reisen und anderen tollen Preisen angeboten werden.
Um in den Genuss dieses Bonus zu kommen, müssen die Spieler lediglich die angegebenen Bedingungen erfüllen, die in der Regel einfach und unkompliziert sind. Dies kann beispielsweise eine Mindesteinzahlung oder eine bestimmte Anzahl an Einsätzen innerhalb eines bestimmten Zeitraums beinhalten.
Der Tipico Casino Bonus 2019 ist eine großartige Möglichkeit, um die Gewinnchancen zu erhöhen und das Spielerlebnis noch spannender zu gestalten. Mit etwas Glück können die Spieler zusätzliche Gewinne erzielen und noch mehr Spaß beim Spielen haben.
Es ist jedoch wichtig zu beachten, dass jeder Bonus bestimmte Bedingungen und Einschränkungen hat, die eingehalten werden müssen. Bevor man sich also für einen Bonus entscheidet, sollte man sich genau über die jeweiligen Bedingungen informieren, um sicherzustellen, dass man sie erfüllen kann.
Alles in allem bietet das Tipico Casino seinen Spielern mit dem Bonus 2019 eine tolle Möglichkeit, um das Spielerlebnis zu verbessern und die Gewinnchancen zu erhöhen. Es lohnt sich also, regelmäßig vorbeizuschauen und sich die aktuellen Angebote nicht entgehen zu lassen. Viel Spaß und viel Erfolg beim Spielen!
https://tipicocasino.one/
Das Boomerang Casino ist bekannt für seine großzügigen Bonusangebote und spannenden Spiele. Für das Jahr 2022 gibt es nun auch attraktive no deposit Bonus Codes, die es Spielern ermöglichen, ohne Einzahlung von echtem Geld zu spielen und dennoch die Chance auf echte Gewinne zu haben.
Ein no deposit Bonus Code ist ein spezieller Code, den Spieler eingeben können, um einen Bonus ohne vorherige Einzahlung zu erhalten. Dieser Bonus kann Freispiele, Gratisguthaben oder andere Vergünstigungen beinhalten. Im Boomerang Casino gibt es verschiedene no deposit Bonus Codes, die regelmäßig aktualisiert und angeboten werden.
Um von den no deposit Bonus Codes im Boomerang Casino zu profitieren, müssen Spieler einfach den entsprechenden Code eingeben, wenn sie ihr Konto erstellen oder ihren Bonus beanspruchen. Die Codes sind in der Regel zeitlich begrenzt und können sich von Monat zu Monat ändern, daher ist es ratsam, regelmäßig auf der Website nach Updates zu suchen.
Mit den no deposit Bonus Codes haben Spieler die Möglichkeit, das Spieleangebot im Boomerang Casino zu erkunden, ohne dabei eigenes Geld riskieren zu müssen. Dies ist eine großartige Möglichkeit, die verschiedenen Spiele kennenzulernen und sich mit dem Casino vertraut zu machen, bevor man sich für eine Einzahlung entscheidet.
Wenn Sie also auf der Suche nach einem spannenden und großzügigen Casino sind, sollten Sie unbedingt die no deposit Bonus Codes im Boomerang Casino im Auge behalten. Mit etwas Glück können Sie dabei echte Gewinne erzielen, ohne vorher eine Einzahlung tätigen zu müssen. Viel Spaß und viel Glück beim Spielen!
https://boomerangcasino.one/
Tipico Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und Möglichkeiten bietet, Geld zu gewinnen. Viele Spieler fragen sich jedoch, wie sie ihr Guthaben auszahlen können. In diesem Artikel werden wir Ihnen erklären, wie Sie Ihr Guthaben bei Tipico Casino auszahlen lassen können.
Zunächst einmal müssen Sie sich auf der Website von Tipico Casino anmelden und Ihr Konto verifizieren. Dies ist ein wichtiger Schritt, um sicherzustellen, dass Ihr Geld sicher ist und dass Sie berechtigt sind, Auszahlungen vorzunehmen.
Sobald Ihr Konto verifiziert ist, kГ¶nnen Sie auf den Bereich “Mein Konto” zugreifen und dort die Option “Auszahlung” wГ¤hlen. Hier haben Sie die MГ¶glichkeit, die gewГјnschte Auszahlungsmethode auszuwГ¤hlen. Tipico Casino bietet verschiedene MГ¶glichkeiten wie BankГјberweisung, Kreditkarte oder E-Wallets wie PayPal oder Skrill an.
Nachdem Sie die Auszahlungsmethode gewählt haben, müssen Sie den Betrag eingeben, den Sie auszahlen lassen möchten. Beachten Sie dabei, dass es möglicherweise Mindest- oder Höchstauszahlungsbeträge gibt, die Sie beachten müssen.
Sobald Sie die Auszahlung bestätigt haben, wird Ihr Geld innerhalb von 1-3 Werktagen auf Ihrem Konto gutgeschrieben, je nach gewählter Auszahlungsmethode.
Es ist wichtig zu beachten, dass Tipico Casino möglicherweise Gebühren für Auszahlungen erhebt, je nach gewählter Methode. Sie sollten sich daher immer im Voraus über mögliche Gebühren informieren.
Insgesamt ist es bei Tipico Casino relativ einfach, Guthaben auszahlen zu lassen. Indem Sie die oben genannten Schritte befolgen und Ihr Konto verifizieren, können Sie sicherstellen, dass Ihre Auszahlung schnell und reibungslos abgewickelt wird. Viel Glück beim Spielen!
https://tipicocasino.one/
Das Boomerang Casino ist ein beliebter Anbieter in der Welt der Online-Casinos. Viele Spieler schätzen die Vielzahl an Spielen, die hohe Sicherheit und die schnellen Auszahlungen. Doch wie sind die Erfahrungen mit der Auszahlung im Boomerang Casino?
Bereits viele Spieler haben positive Erfahrungen mit den Auszahlungen im Boomerang Casino gemacht. Die Auszahlungszeiten sind in der Regel sehr schnell und die Gewinne werden zuverlässig und unkompliziert ausgezahlt. Zudem bietet das Casino eine Vielzahl an Zahlungsmethoden, so dass jeder Spieler die passende Option für sich finden kann.
Ein weiterer positiver Aspekt ist der Kundenservice im Boomerang Casino. Die Mitarbeiter sind freundlich, kompetent und stehen den Spielern bei Fragen oder Problemen jederzeit zur VerfГјgung. Dies sorgt fГјr ein rundum zufriedenes Spielerlebnis.
Natürlich gibt es auch vereinzelt negative Erfahrungen mit der Auszahlung im Boomerang Casino. Einige Spieler berichten von Verzögerungen bei der Auszahlung oder von Problemen bei der Verifizierung ihres Kontos. Dennoch überwiegen die positiven Erfahrungen und die meisten Spieler sind mit der Auszahlung im Boomerang Casino zufrieden.
Insgesamt lässt sich sagen, dass die Auszahlung im Boomerang Casino eine positive Erfahrung ist. Die schnellen Auszahlungszeiten, die vielfältigen Zahlungsmethoden und der gute Kundenservice sorgen für zufriedene Spieler. Wer also auf der Suche nach einem verlässlichen und sicheren Online-Casino ist, sollte das Boomerang Casino definitiv in Betracht ziehen.
https://boomerangcasino.one/
Tipico FAQ: Casino Bonus stornieren
Immer wieder taucht die Frage auf, ob es möglich ist, einen Casino Bonus bei Tipico zu stornieren. In diesem Artikel wollen wir diese Frage genauer unter die Lupe nehmen und klären, ob und unter welchen Bedingungen ein Casino Bonus bei Tipico storniert werden kann.
Grundsätzlich gilt: Einmal angenommene Casino Boni können bei Tipico nicht storniert werden. Dies bedeutet, dass Spieler, die einen Bonus aktiviert haben, diesen auch nutzen müssen, da eine nachträgliche Stornierung nicht möglich ist. Es ist daher wichtig, sich vor der Aktivierung eines Bonusangebots genau zu überlegen, ob man die Umsatzbedingungen erfüllen kann und möchte.
Allerdings gibt es bestimmte Ausnahmen, bei denen ein Casino Bonus storniert werden kann. Dies ist zum Beispiel dann der Fall, wenn ein technischer Fehler vorliegt und der Bonus irrtГјmlich gutgeschrieben wurde. In einem solchen Fall sollte sich der Spieler umgehend an den Kundenservice von Tipico wenden, um den Fehler zu melden und den Bonus stornieren zu lassen.
Ein weiterer Grund für eine Stornierung eines Casino Bonus könnte sein, wenn der Spieler aus versehen ein falsches Bonusangebot aktiviert hat oder sich umentschieden hat. Auch in diesem Fall ist es ratsam, den Kundenservice zu kontaktieren und um eine Stornierung des Bonus zu bitten.
Zusammenfassend lässt sich sagen, dass die Stornierung eines Casino Bonus bei Tipico grundsätzlich nicht möglich ist, es sei denn, es liegt ein technischer Fehler oder ein Irrtum seitens des Spielers vor. Es ist daher wichtig, sich vor der Aktivierung eines Bonusangebots gut zu überlegen, ob man die Umsatzbedingungen erfüllen kann und möchte. Bei Fragen oder Problemen steht der Kundenservice von Tipico jederzeit zur Verfügung und hilft gerne weiter.
https://tipicocasino.one/
Boomerang Casino Mobiles: Das Beste aus beiden Welten
In der heutigen Zeit ist es für viele Menschen wichtig, flexibel zu sein und gleichzeitig ihren täglichen Bedürfnissen nachzukommen. Dies gilt auch für Liebhaber von Online-Casinospielen. Mit dem Aufkommen von mobilen Casinos können Spieler nun ihre Lieblingsspiele von überall und zu jeder Zeit genießen.
Ein Unternehmen, das die Bedeutung von Mobilität verstanden hat, ist Boomerang Casino. Mit ihrem mobilen Angebot haben sie es geschafft, das Beste aus beiden Welten zu kombinieren: erstklassige Casinospiele und die Freiheit, von überall aus zu spielen.
Die mobile Plattform von Boomerang Casino bietet eine breite Palette an Spielen, darunter beliebte Slots, Tischspiele und Live-Casinospiele. Spieler können einfach die mobile Webseite des Casinos besuchen oder die spezielle App herunterladen, um auf ihr Konto zuzugreifen und ihre Lieblingsspiele zu spielen.
Dank der modernen Technologie ist die mobile Erfahrung bei Boomerang Casino nahtlos und benutzerfreundlich. Die Spiele sind für die mobile Nutzung optimiert und bieten ein erstklassiges Spielerlebnis, unabhängig davon, ob man auf einem Smartphone oder Tablet spielt.
Ein weiterer Vorteil von Boomerang Casino Mobiles ist die Möglichkeit, von unterwegs aus Ein- und Auszahlungen zu tätigen. Spieler können sicher sein, dass ihre Transaktionen geschützt und zuverlässig sind, egal wo sie sich befinden.
Alles in allem bietet Boomerang Casino mit seinen mobilen Angeboten eine unschlagbare Kombination aus Bequemlichkeit, Qualität und Spaß. Für alle, die Casino-Spiele lieben und nicht auf Mobilität verzichten wollen, ist Boomerang Casino Mobiles eine erstklassige Wahl. Besuchen Sie jetzt die mobile Webseite oder laden Sie die App herunter, um das ultimative Casino-Erlebnis zu genießen. Viel Glück und viel Spaß!
https://boomerangcasino.one/
Wenn es um Online-Casinos geht, bietet Tipico eines der besten Angebote fГјr Spieler an. Mit einer groГџen Auswahl an Spielen, attraktiven Bonusangeboten und einer benutzerfreundlichen Plattform ist Tipico Classic Casino eine beliebte Wahl fГјr Spieler auf der ganzen Welt.
Ein besonders begehrtes Feature bei Tipico Classic Casino ist der Bonuscode, der es Spielern ermöglicht, zusätzliche Belohnungen und Vergünstigungen zu erhalten. Der Bonuscode kann bei der Registrierung oder Einzahlung eingegeben werden und wird in der Regel mit einem bestimmten Betrag an Bonusgeld belohnt.
Es ist wichtig zu beachten, dass Bonuscodes in der Regel mit bestimmten Bedingungen und Anforderungen verbunden sind, die vom Casino festgelegt werden. Diese können eine Mindesteinzahlung, eine bestimmte Anzahl von Einsätzen oder andere Kriterien umfassen, die erfüllt werden müssen, um den Bonus zu erhalten.
Um den bestmöglichen Nutzen aus dem Bonuscode zu ziehen, ist es ratsam, die Allgemeinen Geschäftsbedingungen sorgfältig zu lesen und sicherzustellen, dass alle Anforderungen erfüllt sind. Auf diese Weise können Spieler sicher sein, dass sie den vollen Nutzen aus dem Bonuscode ziehen und ihr Spielerlebnis bei Tipico Classic Casino optimieren können.
Insgesamt bietet der Bonuscode von Tipico Classic Casino Spielern eine großartige Möglichkeit, zusätzliche Belohnungen und Vergünstigungen zu erhalten. Mit einer breiten Palette von Spielen, lukrativen Bonusangeboten und einer benutzerfreundlichen Plattform ist Tipico Classic Casino definitiv eine gute Wahl für Casino-Enthusiasten.
https://tipicocasino.one/
Das Boomerang Casino ist ein aufstrebendes Online-Casino, das auf AskGamblers eine groГџe Fangemeinde gefunden hat. Die Plattform bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Dealer-Spiele, die von renommierten Anbietern wie Microgaming, NetEnt, Play’n GO und Evolution Gaming bereitgestellt werden.
Eine der Hauptattraktionen des Boomerang Casinos ist sein großzügiges Bonusangebot. Neue Spieler können sich einen Willkommensbonus sichern, der nicht nur Bonusgeld, sondern auch Freispiele beinhaltet. Darüber hinaus gibt es regelmäßig Aktionen und Turniere, bei denen Spieler zusätzliche Preise gewinnen können.
Ein weiterer Grund, warum das Boomerang Casino so beliebt ist, sind die schnellen Auszahlungen und der zuverlässige Kundenservice. Spieler können ihre Gewinne schnell und unkompliziert abheben und bei Fragen oder Problemen steht ein professionelles Support-Team zur Verfügung.
Die Benutzerfreundlichkeit und das ansprechende Design der Website tragen ebenfalls zum Erfolg des Boomerang Casinos bei. Die Plattform ist übersichtlich gestaltet und leicht zu navigieren, sodass Spieler schnell ihre Lieblingsspiele finden können.
Insgesamt bietet das Boomerang Casino ein rundum gelungenes Spielerlebnis und ist definitiv einen Besuch wert. Egal, ob man auf der Suche nach spannenden Spielen, lukrativen Boni oder einem erstklassigen Kundenservice ist, das Boomerang Casino hat fГјr jeden etwas zu bieten.
https://boomerangcasino.one/
Tipico Casino APK – Die beste Art, auf dem Handy zu spielen
Das Tipico Casino APK ist eine innovative und praktische Möglichkeit, um auf dem Handy zu spielen. Mit dieser App können Spieler ihre Lieblingsspiele bequem von unterwegs aus spielen, ohne an einen Computer gebunden zu sein. Die Tipico Casino APK ist leicht zu installieren und bietet eine benutzerfreundliche Oberfläche, die es einfach macht, auf die verschiedenen Spiele zuzugreifen.
Die Tipico Casino APK bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Dealer-Spiele. Die Spieler können aus einer Vielzahl von beliebten Titeln wählen, die für ein unterhaltsames Spielerlebnis sorgen. Die Spiele sind von führenden Softwareanbietern entwickelt worden, was für eine hohe Qualität und ein reibungsloses Spielerlebnis sorgt.
Darüber hinaus bietet die Tipico Casino APK auch großzügige Boni und Aktionen für Spieler. Neue Spieler können von Willkommensboni profitieren, die zusätzliches Geld oder Freispiele bieten. Es gibt auch regelmäßige Promotionen für bestehende Spieler, die ihre Bankroll aufbessern können.
Die Tipico Casino APK ist nicht nur eine praktische Möglichkeit, um auf dem Handy zu spielen, sondern sie bietet auch eine sichere und geschützte Spielumgebung. Die App verwendet innovative Sicherheitstechnologien, um sicherzustellen, dass die persönlichen und finanziellen Daten der Spieler geschützt sind. Die Spieler können also mit ruhigem Gewissen spielen, ohne sich um die Sicherheit ihrer Informationen sorgen zu müssen.
Insgesamt ist das Tipico Casino APK eine großartige Option für Spieler, die gerne unterwegs spielen möchten. Die App bietet eine Vielzahl von Spielen, großzügige Boni und eine sichere Spielumgebung, die ein erstklassiges Spielerlebnis bietet. Probieren Sie es noch heute aus und erleben Sie die Spannung und den Spaß des Tipico Casinos auf Ihrem Handy.
https://tipicocasino.one/
Boomerang Casino Login
Immer mehr Menschen entscheiden sich für Online-Casinos, um ihre Lieblingsspiele bequem von zu Hause aus zu spielen. Eines der beliebtesten Online-Casinos ist das Boomerang Casino, das eine Vielzahl von Spielen und großzügigen Boni für seine Spieler bietet. Um bei Boomerang Casino spielen zu können, ist ein einfacher Login erforderlich. In diesem Artikel werden wir erklären, wie der Login bei Boomerang Casino funktioniert.
ZunГ¤chst einmal mГјssen Sie die offizielle Website des Boomerang Casinos besuchen. Hier finden Sie den Button “Anmelden” oder “Registrieren”, den Sie anklicken mГјssen. Es Г¶ffnet sich ein Anmeldeformular, in das Sie Ihre persГ¶nlichen Daten wie Ihren Namen, Ihre E-Mail-Adresse und Ihr Passwort eingeben mГјssen. Stellen Sie sicher, dass alle Informationen korrekt sind, da Sie diese spГ¤ter fГјr den Login benГ¶tigen.
Sobald Sie das Anmeldeformular abgeschickt haben, erhalten Sie eine Bestätigungs-E-Mail von Boomerang Casino. In dieser E-Mail finden Sie einen Bestätigungslink, den Sie anklicken müssen, um Ihr Konto zu aktivieren. Nachdem Sie Ihr Konto erfolgreich aktiviert haben, können Sie sich mit Ihren zuvor eingegebenen Daten in Ihr Konto einloggen.
Der Login-Prozess bei Boomerang Casino ist einfach und sicher. Sobald Sie angemeldet sind, können Sie aus einer Vielzahl von Spielen wie Slots, Blackjack, Roulette und Live-Casino wählen. Darüber hinaus bietet Boomerang Casino regelmäßig Boni und Promotionen für seine Spieler an, um ihr Spielerlebnis noch unterhaltsamer zu gestalten.
Insgesamt ist der Login bei Boomerang Casino unkompliziert und bietet Spielern die Möglichkeit, ihre Lieblingsspiele bequem von zu Hause aus zu spielen. Wenn Sie also auf der Suche nach einem unterhaltsamen und sicheren Online-Casino sind, sollten Sie definitiv das Boomerang Casino ausprobieren. Viel Spaß und viel Glück beim Spielen!
https://boomerangcasino.one/
he has a good point 1win indir
Tipico Casino Fehler
Das Tipico Casino ist eine beliebte Plattform für Glücksspiel-Fans, die gerne online spielen. Doch manchmal kann es vorkommen, dass Fehler auftreten, die das Spielerlebnis beeinträchtigen. In diesem Artikel werden wir uns mit möglichen Tipico Casino Fehlern befassen und Ihnen Tipps geben, wie Sie diese beheben können.
Einer der häufigsten Fehler, auf den Spieler stoßen können, ist eine langsame oder fehlerhafte Internetverbindung. Wenn die Verbindung des Spielers instabil ist, kann dies zu Unterbrechungen beim Spielen führen oder sogar dazu führen, dass das Spiel abstürzt. Um dieses Problem zu beheben, empfiehlt es sich, die Internetverbindung zu überprüfen und sicherzustellen, dass sie stabil ist.
Ein weiterer häufiger Fehler betrifft die Ein- und Auszahlungen auf der Plattform. Manchmal können Spieler Schwierigkeiten haben, Geld auf ihr Konto einzuzahlen oder Gewinne abzuheben. In solchen Fällen ist es ratsam, den Kundendienst von Tipico zu kontaktieren, um Unterstützung zu erhalten und das Problem zu lösen.
Ein weiterer möglicher Fehler betrifft die Kompatibilität des Casinos mit verschiedenen Geräten. Manche Spieler berichten, dass sie Schwierigkeiten haben, auf das Casino von ihren Mobilgeräten aus zuzugreifen. In solchen Fällen kann es helfen, die mobile App des Casinos herunterzuladen oder die Webseite im Browser des Geräts zu öffnen.
Insgesamt ist es wichtig zu beachten, dass es bei Online-Casinos immer wieder zu technischen Problemen kommen kann. Wenn Sie auf einen Fehler stoßen, sollten Sie nicht gleich in Panik geraten, sondern versuchen, das Problem systematisch zu lösen. Im Zweifelsfall können Sie sich auch an den Kundendienst des Casinos wenden, der Ihnen weiterhelfen wird.
Abschließend lässt sich sagen, dass Tipico Casino Fehler zwar ärgerlich sein können, aber in der Regel relativ einfach zu beheben sind. Mit etwas Geduld und den richtigen Maßnahmen können Sie Ihr Spielerlebnis wieder reibungslos genießen.
https://tipicocasino.one/
Das Boomerang Bet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und attraktiven Bonusangeboten bietet. In diesem Artikel werden wir eine grГјndliche ГњberprГјfung des Casinos durchfГјhren und seine Merkmale, Vor- und Nachteile sowie andere wichtige Aspekte analysieren.
Das Boomerang Bet Casino bietet eine breite Palette von Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr. Die QualitГ¤t der Spiele ist erstklassig, da sie von renommierten Softwareanbietern wie NetEnt, Microgaming, Play’n GO und anderen entwickelt wurden. Die Grafiken und Soundeffekte sind beeindruckend und sorgen fГјr ein authentisches Casinoerlebnis.
Ein weiterer Vorteil des Boomerang Bet Casinos sind die großzügigen Bonusangebote und Aktionen. Neue Spieler werden mit einem lukrativen Willkommensbonus belohnt, der ihnen zusätzliches Guthaben oder Freispiele ermöglicht. Darüber hinaus gibt es regelmäßige Promotionen und Treueprogramme für bestehende Spieler, die ihre Gewinnchancen erhöhen.
Das Casino bietet auch eine Vielzahl von Zahlungsmethoden, darunter Kreditkarten, E-Wallets und Banküberweisungen. Die Transaktionen sind sicher und schnell, und das Casino stellt sicher, dass alle persönlichen Daten geschützt sind. Der Kundenservice ist ebenfalls erstklassig und steht den Spielern rund um die Uhr zur Verfügung, um ihre Fragen und Anliegen zu beantworten.
Ein möglicher Nachteil des Boomerang Bet Casinos ist die begrenzte Auswahl an Spielen im Vergleich zu anderen Online-Casinos. Einige Spieler könnten sich nach mehr Vielfalt und Auswahl sehnen. Außerdem könnte die Website etwas verbessert werden, um sie benutzerfreundlicher und ansprechender zu gestalten.
Insgesamt ist das Boomerang Bet Casino eine gute Wahl für Spieler, die eine sichere und unterhaltsame Spielumgebung suchen. Mit einer Vielzahl von Spielen, großzügigen Bonusangeboten und zuverlässigem Kundenservice bietet das Casino ein rundum positives Spielerlebnis. Besuchen Sie das Boomerang Bet Casino noch heute und erleben Sie den Nervenkitzel des Glücksspiels online!
https://boomerangcasino.one/
Das Tipico Casino Spiel hГ¤ngt – Was tun?
Es ist frustrierend, wenn man sich auf ein spannendes Spiel im Tipico Casino freut und dann plötzlich feststellt, dass das Spiel hängt. Doch keine Sorge, es gibt verschiedene Möglichkeiten, um dieses Problem zu lösen und wieder ins Spielgeschehen einzusteigen.
Als Erstes sollte man überprüfen, ob das Problem am eigenen Gerät liegt. Oftmals kann ein Neustart des Computers oder mobilen Endgeräts schon ausreichen, um das Spiel wieder zum Laufen zu bringen. Auch das Löschen des Browserverlaufs und der Cookies kann helfen, um eventuelle Probleme zu beheben.
Wenn das Spiel immer noch hängt, kann es hilfreich sein, den Kundensupport von Tipico zu kontaktieren. Die freundlichen Mitarbeiter stehen rund um die Uhr zur Verfügung und können bei technischen Schwierigkeiten weiterhelfen. Oftmals haben sie auch spezielle Tipps und Tricks parat, um das Problem schnell zu lösen.
Eine weitere Möglichkeit ist es, das betroffene Spiel zu schließen und ein anderes zu öffnen. Oftmals liegt das Problem nur bei einem bestimmten Spiel und andere funktionieren einwandfrei. So kann man trotzdem weiterhin sein Casinoerlebnis genießen.
Abschließend bleibt zu sagen, dass es immer ärgerlich ist, wenn ein Spiel im Tipico Casino hängt. Doch mit ein paar einfachen Maßnahmen und der Hilfe des Kundensupports kann man das Problem meist schnell lösen und wieder voll und ganz in die spannende Welt des Online-Glücksspiels eintauchen.
https://tipicocasino.one/
Das Boomerang Casino gr ist ein aufregendes neues Online-Casino, das Spielern eine Vielzahl von hochwertigen Spielen und großzügigen Boni bietet. Mit einer benutzerfreundlichen Oberfläche, schnellen Auszahlungen und erstklassigem Kundenservice ist es leicht zu verstehen, warum das Boomerang Casino gr bei Spielern beliebt ist.
Das Casino bietet eine breite Palette von Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit Spielen von renommierten Anbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen kГ¶nnen Spieler sicher sein, dass sie ein qualitativ hochwertiges Spielerlebnis genieГџen.
Das Boomerang Casino gr belohnt seine Spieler auch großzügig mit verschiedenen Boni und Aktionen. Neue Spieler erhalten in der Regel einen Willkommensbonus, der kostenlose Spins oder zusätzliches Guthaben zum Spielen bietet. Das Casino bietet auch regelmäßig Promotions und Turniere an, bei denen Spieler fantastische Preise gewinnen können.
Ein weiterer Vorteil des Boomerang Casino gr ist dessen hervorragender Kundenservice. Das engagierte Support-Team ist rund um die Uhr erreichbar und steht Spielern bei Fragen oder Problemen zur Verfügung. Darüber hinaus bietet das Casino eine Vielzahl von Zahlungsmethoden, um Ein- und Auszahlungen schnell und bequem abwickeln zu können.
Insgesamt bietet das Boomerang Casino gr ein rundum faszinierendes Spielerlebnis und ist definitiv einen Besuch wert. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Boni und einem erstklassigen Kundenservice ist es klar, warum dieses Online-Casino so beliebt bei Spielern ist. Besuchen Sie das Boomerang Casino gr noch heute und entdecken Sie die aufregende Welt des Online-GlГјcksspiels!
https://boomerangcasino.one/
Tipico Online Casino Login
Das Tipico Online Casino bietet seinen Spielern eine Vielzahl an spannenden Spielen, von Slots über Tischspiele bis hin zu Live Dealer Spielen. Um auf all diese Spiele zugreifen zu können, ist es notwendig, sich zunächst einzuloggen.
Der Login-Prozess bei Tipico Online Casino ist einfach und unkompliziert. Um sich anzumelden, müssen Spieler zunächst die offizielle Website des Casinos besuchen. Dort finden sie oben rechts auf der Seite den Button zum Login. Ein Klick darauf öffnet ein Fenster, in dem sie ihre Benutzerdaten, bestehend aus Benutzername und Passwort, eingeben müssen.
Sobald die Daten eingegeben wurden, können die Spieler auf ihr Konto zugreifen und alle verfügbaren Spiele spielen. Es ist wichtig, darauf zu achten, dass die Daten korrekt eingegeben werden, um Probleme beim Einloggen zu vermeiden.
Nach dem erfolgreichen Login können die Spieler Ein- und Auszahlungen tätigen, ihre persönlichen Informationen verwalten und an den verschiedenen Aktionen und Bonusangeboten teilnehmen, die das Tipico Online Casino anbietet.
Es ist ratsam, sich regelmäßig beim Tipico Online Casino anzumelden, um keine der aktuellen Aktionen oder Promotionen zu verpassen. Mit nur wenigen Klicks können Spieler auf eine Vielzahl von aufregenden Spielen zugreifen und ihr Glück versuchen.
Insgesamt bietet das Tipico Online Casino einen reibungslosen Login-Prozess, der es den Spielern ermöglicht, schnell und einfach auf ihre Lieblingsspiele zuzugreifen. Probieren Sie es noch heute aus und erleben Sie die Spannung und Aufregung des Tipico Online Casinos!
https://tipicocasino.one/
кстанди цена – где можно купить оземпик, оземпик раствор +для инъекций купить
Boomerang Casino Erfahrungen: Alles Гјber Auszahlungen
Boomerang Casino ist ein Online-Casino, das Spielern eine Vielzahl von Spielen und großzügigen Boni bietet. In diesem Artikel werden wir uns genauer mit den Erfahrungen der Spieler in Bezug auf Auszahlungen beschäftigen.
Die meisten Spieler, die Erfahrungen mit Boomerang Casino gemacht haben, berichten von schnellen und zuverlässigen Auszahlungen. Die Auszahlungszeiten variieren je nach Auszahlungsmethode, aber in der Regel werden Auszahlungen innerhalb von 24 Stunden bearbeitet. Spieler können zwischen verschiedenen Zahlungsmethoden wie Kreditkarten, E-Wallets und Banküberweisungen wählen.
Ein weiterer positiver Aspekt von Boomerang Casino ist die Tatsache, dass Auszahlungen in der Regel gebührenfrei sind. Dies bedeutet, dass Spieler ihr gesamtes Guthaben ohne Abzüge erhalten können.
Einige Spieler haben jedoch berichtet, dass sie gelegentlich Verzögerungen bei ihren Auszahlungen erlebt haben. In den meisten Fällen handelt es sich dabei um Probleme mit der Verifizierung der Identität oder der Erfüllung der Bonusbedingungen. Spieler sollten daher sicherstellen, dass sie alle erforderlichen Dokumente einreichen und die Bonusbedingungen vollständig erfüllen, um Verzögerungen bei ihren Auszahlungen zu vermeiden.
Insgesamt sind die Erfahrungen der Spieler mit Boomerang Casino in Bezug auf Auszahlungen größtenteils positiv. Schnelle und zuverlässige Auszahlungen sowie gebührenfreie Transaktionen sorgen dafür, dass Spieler ihre Gewinne schnell und einfach erhalten können. Es ist jedoch wichtig, die Bonusbedingungen zu beachten und alle erforderlichen Dokumente einzureichen, um Verzögerungen zu vermeiden.
https://boomerangcasino.one/
Das Casino Boomerang: Ein aufregendes Spielerlebnis
Das Casino Boomerang ist ein aufregender Ort für alle Glücksspiel-Enthusiasten. Mit seiner einzigartigen Atmosphäre und dem vielfältigen Angebot an Spielen ist dieser Ort ein Magnet für alle, die das Glück auf ihrer Seite haben möchten.
Das Casino Boomerang bietet eine breite Palette an Spielen, von klassischen Spielautomaten über Roulette bis hin zu Poker. Egal, ob man ein erfahrener Spieler ist oder einfach nur sein Glück versuchen möchte, hier findet jeder etwas Passendes. Die freundlichen Mitarbeiter stehen den Besuchern jederzeit zur Verfügung, um ihnen bei Fragen oder Problemen behilflich zu sein.
Ein besonderes Highlight des Casinos ist die Bar, an der die Gäste sich mit erfrischenden Getränken stärken können. Die entspannte Atmosphäre lädt dazu ein, eine Pause einzulegen und sich mit anderen Spielern auszutauschen.
Ein weiterer Pluspunkt des Casino Boomerang ist das attraktive Bonusprogramm, das regelmäßig neue Angebote für die Besucher bereithält. Von Freispielen bis zu Rabatten auf Getränke, hier gibt es immer etwas zu gewinnen.
Alles in allem ist das Casino Boomerang ein fantastischer Ort, um eine unterhaltsame Zeit zu verbringen und sein GlГјck zu versuchen. Wer auf der Suche nach Spannung und Nervenkitzel ist, sollte unbedingt einen Besuch in diesem Casino in Betracht ziehen.
https://boomerangcasino.one/
такси в белокуриху из новосибирска http://transfer-novosibirsk-belokurikha.ru/
Tipico Casino ist mittlerweile vielen Spielern ein Begriff, doch nun gibt es einen neuen Dreh: das Tipico Casino MaydreГџ. Diese neue Online-GlГјcksspielseite hat in den letzten Monaten viel Aufmerksamkeit auf sich gezogen und verspricht ein einzigartiges Spielerlebnis.
Das Tipico Casino Maydreß bietet eine breite Auswahl an Spielautomaten, Tischspielen und Live-Casino-Spielen. Die Website ist übersichtlich gestaltet und einfach zu bedienen, so dass auch Anfänger sich schnell zurechtfinden können. Darüber hinaus punktet das Casino mit attraktiven Bonusangeboten und regelmäßigen Aktionen, die die Spieler bei Laune halten.
Ein weiterer großer Pluspunkt des Tipico Casino Maydreß ist die mobile Kompatibilität. Die Seite ist für alle gängigen mobilen Endgeräte optimiert, so dass Spieler auch unterwegs problemlos spielen können. Das bedeutet, dass man jederzeit und überall die Spannung und den Nervenkitzel des Online-Glücksspiels genießen kann.
Einige Spieler schwören bereits auf das Tipico Casino Maydreß und loben die schnellen Auszahlungen, den zuvorkommenden Kundenservice und die hohe Qualität der Spiele. Mit einer gültigen Glücksspiellizenz aus Malta kann man sich zudem sicher sein, dass das Casino seriös und vertrauenswürdig ist.
Alles in allem ist das Tipico Casino MaydreГџ definitiv eine Empfehlung wert fГјr alle, die auf der Suche nach einem erstklassigen Online-Casino-Erlebnis sind. Probieren Sie es aus und lassen Sie sich von der faszinierenden Welt des GlГјcksspiels verzaubern!
https://tipicocasino.one/
Tipico ist eine der bekanntesten Wettanbieter in Deutschland. Viele Menschen verbinden Tipico mit Sportwetten, jedoch gibt es immer wieder Verwirrung darГјber, ob Tipico auch ein Casino anbietet. Die Antwort darauf ist: Nein, Tipico ist kein Casino.
Auch wenn auf der Webseite von Tipico einige Casinospiele wie Slots und Tischspiele angeboten werden, handelt es sich dabei um virtuelle Spiele, die nicht um echtes Geld gespielt werden können. Tipico konzentriert sich hauptsächlich auf Sportwetten und hat sich in diesem Bereich einen Namen gemacht.
Für Menschen, die gerne Casinospiele spielen möchten, gibt es in Deutschland viele andere Anbieter, die eine große Auswahl an Spielen und Möglichkeiten bieten. Es ist wichtig, sich vor der Anmeldung bei einem Online-Casino über die Seriosität und Sicherheit des Anbieters zu informieren.
Insgesamt lässt sich sagen, dass Tipico kein Casino ist und sich stattdessen auf Sportwetten spezialisiert hat. Wer gerne Casinospiele spielt, sollte sich nach anderen Anbietern umsehen, die speziell auf dieses Segment ausgerichtet sind.
https://tipicocasino.one/
Boomerang Online Casino: Eine spannende neue GlГјcksspielplattform
Das Boomerang Online Casino ist die neueste Ergänzung in der Welt der virtuellen Glücksspielunterhaltung. Mit einem frischen und modernen Design sowie einer Vielzahl von spannenden Spieloptionen verspricht dieses Casino ein unvergessliches Spielerlebnis für alle, die ihr Glück versuchen möchten.
Eine der Hauptattraktionen des Boomerang Online Casinos ist die große Auswahl an Spielen, die es den Spielern zur Verfügung stellt. Von klassischen Tischspielen wie Blackjack und Roulette bis hin zu beliebten Spielautomaten und Live-Dealer-Spielen gibt es für jeden Geschmack etwas zu entdecken. Darüber hinaus werden regelmäßig neue Spiele hinzugefügt, um sicherzustellen, dass es immer frische und aufregende Optionen gibt, aus denen die Spieler wählen können.
Ein weiterer großer Vorteil des Boomerang Online Casinos ist die benutzerfreundliche Plattform, die es den Spielern leicht macht, sich zu registrieren, Einzahlungen zu tätigen und ihre Lieblingsspiele zu spielen. Mit einer Vielzahl von sicheren und schnellen Zahlungsmethoden sowie einem engagierten Kundensupport-Team stehen den Spielern alle Ressourcen zur Verfügung, die sie benötigen, um ihr Spielerlebnis so reibungslos wie möglich zu gestalten.
Darüber hinaus bietet das Boomerang Online Casino großzügige Boni und Aktionen für neue und bestehende Spieler an, um sicherzustellen, dass diese stets mit zusätzlichen Anreizen belohnt werden. Von Willkommensboni über Freispiele bis hin zu Cashback-Angeboten gibt es zahlreiche Möglichkeiten, um das Beste aus dem Spielerlebnis herauszuholen und gleichzeitig tolle Preise zu gewinnen.
Insgesamt ist das Boomerang Online Casino eine aufregende neue Glücksspielplattform, die sowohl erfahrene Spieler als auch Neulinge anspricht. Mit einer Vielzahl von Spielen, benutzerfreundlicher Gameplay und großzügigen Boni verspricht dieses Casino stundenlange Unterhaltung und die Möglichkeit, echte Gewinne zu erzielen. Wer also auf der Suche nach einem neuen und aufregenden Glücksspielerlebnis ist, sollte definitiv das Boomerang Online Casino ausprobieren.
https://boomerangcasino.one/
Tipico ist eine beliebte Online-GlГјcksspielplattform, die eine Vielzahl von Casino-Spielen fГјr Spieler jeden Niveaus anbietet. Mit so vielen Optionen kann es schwierig sein, das beste Casino-Spiel bei Tipico zu finden. Deshalb haben wir fГјr Sie die besten Casino-Spiele bei Tipico zusammengestellt.
Ein beliebtes Spiel bei Tipico ist das klassische Roulette. Es ist einfach zu erlernen und bietet eine Vielzahl von Wettmöglichkeiten, die es spannend und unterhaltsam machen. Roulette ist ein Spiel, das sowohl Anfängern als auch erfahrenen Spielern viel Freude bereiten kann.
Ein weiteres beliebtes Casino-Spiel bei Tipico ist Blackjack. Dieses Spiel erfordert strategisches Denken und Geschicklichkeit, was es zu einer spannenden Herausforderung für Spieler macht. Mit verschiedenen Varianten und Einsatzmöglichkeiten bietet Blackjack bei Tipico eine Menge Spaß und Unterhaltung.
Für diejenigen, die gerne Slots spielen, hat Tipico eine Vielzahl von Spielautomaten im Angebot. Von klassischen Fruchtmaschinen bis hin zu aufregenden Video-Slots gibt es für jeden Geschmack etwas zu entdecken. Mit unterschiedlichen Themen, Bonusrunden und Jackpots bieten die Slots bei Tipico eine Menge Abwechslung und Gewinnmöglichkeiten.
Egal für welches Spiel Sie sich entscheiden, bei Tipico können Sie sicher sein, dass Sie ein faires und unterhaltsames Spielerlebnis haben werden. Mit hochwertiger Grafik, benutzerfreundlicher Oberfläche und einer Vielzahl von Spielen ist Tipico die perfekte Wahl für alle Casino-Liebhaber.
Also, worauf warten Sie noch? Besuchen Sie noch heute Tipico und entdecken Sie die besten Casino-Spiele, die diese Plattform zu bieten hat. Viel SpaГџ und viel GlГјck beim Spielen!
https://tipicocasino.one/
Tipico Casino Bonus Treue10
Das Tipico Casino bietet seinen treuen Kunden einen besonderen Bonus an – den Treue10 Bonus. Dieser Bonus belohnt Spieler, die regelmäßig im Casino spielen und dem Anbieter treu bleiben. Doch was genau verbirgt sich hinter diesem Bonus und wie können Spieler davon profitieren?
Der Treue10 Bonus ist ein exklusives Angebot für loyalen Spieler im Tipico Casino. Um diesen Bonus zu erhalten, müssen Spieler zunächst Mitglied im Treueprogramm des Casinos sein. Dies ist jedoch ganz einfach – Spieler können sich einfach anmelden und sofort von den Vorteilen des Treueprogramms profitieren.
Sobald Spieler Mitglied im Treueprogramm sind, können sie sich für den Treue10 Bonus qualifizieren. Dieser Bonus wird den Spielern in Form von zusätzlichem Guthaben oder Freispielen gutgeschrieben. Spieler können dieses Bonusguthaben verwenden, um ihre Lieblingsspiele im Casino zu spielen und so ihre Gewinnchancen zu erhöhen.
Der Treue10 Bonus ist eine tolle Möglichkeit für Spieler, noch mehr aus ihrem Spielerlebnis im Tipico Casino herauszuholen. Durch regelmäßiges Spielen und Treue zum Anbieter können Spieler sich zusätzliches Guthaben sichern und damit ihre Gewinnchancen steigern.
Wenn auch Sie von den exklusiven Vorteilen des Treue10 Bonus profitieren möchten, sollten Sie sich noch heute im Tipico Casino anmelden und Mitglied im Treueprogramm werden. Mit etwas Glück und Geschick können auch Sie sich den begehrten Treue10 Bonus sichern und so noch mehr Spaß beim Spielen im Casino haben.
https://tipicocasino.one/
саксенда цена отзывы аналоги инструкция – тирзепатид купить +в спб, тирзепатид инструкция цена
Boomerang Casino Bonus ohne Einzahlung
Das Boomerang Casino ist ein aufstrebendes Online-Casino, das seinen Spielern eine Vielzahl von großzügigen Boni und Promotionen bietet. Einer der beliebtesten Boni, die das Boomerang Casino anbietet, ist der Bonus ohne Einzahlung. Diese Art von Bonus ermöglicht es den Spielern, ohne eigenes Geld zu riskieren, das Casino auszuprobieren und echte Gewinne zu erzielen.
Der Boomerang Casino Bonus ohne Einzahlung ist in der Regel für neue Spieler verfügbar, die sich zum ersten Mal registrieren. Um den Bonus zu erhalten, müssen sich die Spieler lediglich anmelden und ein neues Konto erstellen. Der Bonus wird dann automatisch gutgeschrieben, und die Spieler können ihn verwenden, um verschiedene Casinospiele zu spielen.
Mit dem Boomerang Casino Bonus ohne Einzahlung haben die Spieler die Möglichkeit, echte Gewinne zu erzielen, ohne ihr eigenes Geld zu riskieren. Dies macht den Bonus besonders attraktiv für Spieler, die das Casino ausprobieren möchten, ohne zuerst eine Einzahlung zu tätigen.
Es ist jedoch wichtig zu beachten, dass der Boomerang Casino Bonus ohne Einzahlung in der Regel bestimmten Bedingungen unterliegt. Diese können beispielsweise Mindestumsatzanforderungen oder maximalen Auszahlungsbeträge umfassen. Bevor die Spieler den Bonus nutzen, sollten sie daher die Geschäftsbedingungen des Casinos sorgfältig lesen, um sicherzustellen, dass sie alle Anforderungen erfüllen.
Insgesamt ist der Boomerang Casino Bonus ohne Einzahlung eine großartige Möglichkeit für Spieler, das Casino auszuprobieren und echte Gewinne zu erzielen, ohne eigenes Geld zu riskieren. Mit einer Reihe von spannenden Spielen und lukrativen Boni ist das Boomerang Casino definitiv eine gute Wahl für alle, die nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis suchen.
https://boomerangcasino.one/
Das Boomerang Casino ist eine aufregende neue Online-GlГјcksspielplattform, die Spielern eine Vielzahl von Spielen und Boni bietet. In diesem Artikel werden wir das Boomerang Casino genauer betrachten und eine ehrliche Bewertung abgeben.
Das Boomerang Casino wurde im Jahr 2020 gegründet und gehört zur Gruppe der Araxio Development N.V. Es ist in Curacao lizenziert und reguliert, was bedeutet, dass es sich um ein seriöses und vertrauenswürdiges Online-Casino handelt.
Das Casino bietet eine beeindruckende Auswahl an Spielen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming, Play’n GO, Quickspin und vielen anderen. Spieler kГ¶nnen aus Hunderten von Spielautomaten, Tischspielen, Live-Casinospielen und Jackpot-Spielen wГ¤hlen, die alle in hoher QualitГ¤t und mit beeindruckenden Grafiken geliefert werden.
Ein weiterer großer Vorteil des Boomerang Casinos sind die großzügigen Boni und Aktionen, die es seinen Spielern bietet. Neue Spieler erhalten einen Willkommensbonus auf ihre ersten Einzahlungen, sowie regelmäßige Promotionen und Belohnungen für treue Spieler.
Die Website des Boomerang Casinos ist benutzerfreundlich und leicht zu navigieren. Spieler können problemlos auf ihre Lieblingsspiele zugreifen und Ein- und Auszahlungen tätigen. Der Kundenservice des Casinos ist rund um die Uhr verfügbar und kann per Live-Chat, E-Mail oder Telefon erreicht werden.
Alles in allem hinterlässt das Boomerang Casino einen positiven Eindruck. Mit seiner breiten Spielauswahl, großzügigen Boni und erstklassigem Kundenservice ist es definitiv einen Besuch wert. Wir empfehlen jedem, der nach einem unterhaltsamen und sicheren Online-Casinoerlebnis sucht, das Boomerang Casino auszuprobieren.
https://boomerangcasino.one/
https://muslim-prayer-times.com/
Das Boomerang Casino, das im Jahr 2020 gegründet wurde, ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Casinospielen und Boni für ihre Spieler anbietet. Ein wichtiger Aspekt, der bei der Wahl eines Online-Casinos berücksichtigt werden muss, ist das Auszahlungslimit. Das Auszahlungslimit ist der Höchstbetrag, den ein Spieler pro Transaktion oder innerhalb eines bestimmten Zeitraums abheben kann.
Das Boomerang Casino hat ebenfalls ein Auszahlungslimit, das von verschiedenen Faktoren abhängt, wie beispielsweise dem VIP-Status des Spielers, dem Zahlungsmittel und dem Land, in dem sich der Spieler befindet. Das Auszahlungslimit kann von 500 € bis zu mehreren Tausend Euro pro Woche reichen.
Es ist wichtig, sich über das Auszahlungslimit des Boomerang Casinos zu informieren, um sicherzustellen, dass man die richtige Entscheidung trifft. Wenn ein Spieler das Auszahlungslimit erreicht hat, kann es zu Verzögerungen oder Einschränkungen bei der Auszahlung kommen. Daher ist es ratsam, vorab zu prüfen, ob das Auszahlungslimit den eigenen Bedürfnissen entspricht.
Das Boomerang Casino bietet seinen Spielern auch die Möglichkeit, ihr Auszahlungslimit zu erhöhen, indem sie den Kundensupport kontaktieren und ihre Anfrage überprüfen lassen. Es ist wichtig zu beachten, dass das Auszahlungslimit aus Sicherheitsgründen festgelegt wird, um Betrug und Geldwäsche zu verhindern.
Insgesamt ist das Auszahlungslimit im Boomerang Casino ein wichtiger Aspekt, den Spieler im Auge behalten sollten, um eine reibungslose und zufriedenstellende Erfahrung auf der Plattform zu gewährleisten. Es ist ratsam, sich vorab über die Bestimmungen und Bedingungen des Auszahlungslimits zu informieren, um Missverständnisse und Unannehmlichkeiten zu vermeiden.
https://boomerangcasino.one/
Tipico Casino Störung: Was tun, wenn die Seite nicht funktioniert?
Es ist ärgerlich, wenn man sich auf einen gemütlichen Abend im Online Casino freut und plötzlich funktioniert die Seite nicht. Doch keine Sorge, in den meisten Fällen lässt sich das Problem schnell lösen. Hier sind ein paar Tipps, was du tun kannst, wenn du auf Tipico Casino auf eine Störung stößt.
Zunächst einmal solltest du überprüfen, ob das Problem tatsächlich auf der Seite von Tipico liegt. Dafür kannst du einfach mal die Seite neu laden oder versuchen, diese in einem anderen Browser zu öffnen. Oftmals liegt die Störung nämlich gar nicht beim Casino selbst, sondern bei deinem eigenen Internetzugang.
Falls die Störung tatsächlich von Tipico verursacht wird, ist es ratsam, auf der Webseite nach aktuellen Informationen zu suchen. Oftmals informiert das Casino seine Spieler dort über aktuelle Störungen und arbeitet bereits an der Behebung des Problems. Es lohnt sich also, dort regelmäßig vorbeizuschauen.
Wenn die Störung länger anhält und du keine Informationen auf der Webseite findest, kannst du auch den Kundenservice von Tipico kontaktieren. Oftmals können die Mitarbeiter dir weiterhelfen und das Problem gemeinsam mit dir lösen. Schließlich möchten auch sie, dass du deine Zeit im Casino genießen kannst.
Insgesamt ist es also wichtig, ruhig zu bleiben und systematisch vorzugehen, wenn du auf eine Störung im Tipico Casino stößt. Mit den richtigen Maßnahmen lässt sich das Problem in den meisten Fällen schnell und unkompliziert lösen und einem gelungenen Casino-Abend steht nichts mehr im Wege.
https://tipicocasino.one/
Tipico Casino Einzahlung Blockiert
Es kann frustrierend sein, wenn man versucht, eine Einzahlung im Tipico Casino zu tätigen und plötzlich feststellt, dass die Zahlung blockiert ist. In solchen Fällen ist es wichtig zu verstehen, warum dies passiert und wie man das Problem lösen kann.
Eine blockierte Einzahlung kann verschiedene Gründe haben. Einer der häufigsten Gründe ist, dass die Zahlungsmethode, die man verwendet hat, nicht mit Tipico kompatibel ist. Man sollte sicherstellen, dass die gewählte Zahlungsmethode von Tipico akzeptiert wird und keine Probleme damit bestehen.
Ein weiterer Grund fГјr blockierte Einzahlungen kann sein, dass das Konto des Spielers nicht ausreichend gedeckt ist. Es ist wichtig, sicherzustellen, dass genГјgend Geld auf dem Konto vorhanden ist, um die Einzahlung erfolgreich abzuschlieГџen.
Es kann auch vorkommen, dass Tipico Sicherheitsmaßnahmen ergreift, um verdächtige Transaktionen zu verhindern. In einem solchen Fall kann es hilfreich sein, den Kundendienst zu kontaktieren und das Problem zu klären.
Wenn man feststellt, dass die Einzahlung blockiert ist, sollte man zunächst die genauen Gründe dafür herausfinden. Anschließend kann man entsprechende Maßnahmen ergreifen, um das Problem zu lösen und die Einzahlung erfolgreich abzuschließen.
Es ist wichtig, geduldig zu bleiben und das Problem nicht auf die leichte Schulter zu nehmen. Mit der richtigen Herangehensweise und Kommunikation mit dem Kundendienst von Tipico kann man in der Regel schnell eine Lösung finden und wieder problemlos im Casino spielen.
https://tipicocasino.one/
Das Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und attraktiven Bonusangeboten für Spieler anbietet. Ein wichtiger Aspekt für viele Spieler ist die Auszahlungserfahrung in einem Online-Casino, da sie sicherstellen möchten, dass sie ihre Gewinne schnell und zuverlässig erhalten können.
Die Erfahrungen mit der Auszahlung im Boomerang Casino sind überwiegend positiv. Die meisten Spieler berichten davon, dass Auszahlungen schnell bearbeitet und ohne Probleme durchgeführt werden. Die Dauer der Auszahlung hängt dabei von der gewählten Zahlungsmethode ab, aber in der Regel erfolgt die Auszahlung innerhalb weniger Tage.
Ein weiterer positiver Aspekt der Auszahlungserfahrung im Boomerang Casino ist die Vielzahl an Zahlungsmethoden, die den Spielern zur VerfГјgung stehen. Von Kreditkarten und E-Wallets bis hin zu BankГјberweisungen gibt es fГјr jeden Spieler eine passende Option, um sein Guthaben auszahlen zu lassen.
Darüber hinaus bietet das Boomerang Casino einen zuverlässigen Kundenservice, der bei Fragen oder Problemen rund um Auszahlungen schnell und kompetent hilft. Die Spieler können sich jederzeit an den Support wenden und erhalten in der Regel innerhalb kurzer Zeit eine Antwort.
Insgesamt lässt sich sagen, dass die Auszahlungserfahrung im Boomerang Casino positiv ist und die Spieler sich darauf verlassen können, dass ihre Gewinne schnell und zuverlässig ausgezahlt werden. Wer also auf der Suche nach einem vertrauenswürdigen Online-Casino mit guten Auszahlungskonditionen ist, ist im Boomerang Casino gut aufgehoben.
https://boomerangcasino.one/
Boomerang Casino Mobil
Das Boomerang Casino ist bereits vielen Spielern ein Begriff, die gerne in Online-Casinos ihr GlГјck versuchen. Nun gibt es auch eine mobile Version des beliebten Casinos, mit der man auch unterwegs jederzeit und Гјberall spielen kann.
Die mobile Version des Boomerang Casinos ist einfach zu bedienen und bietet ein breites Spektrum an Spielen, von Slot-Maschinen über Tischspiele bis hin zu Live-Casino-Spielen. Dabei wurden die Spiele für die mobile Version optimiert und laufen reibungslos auf verschiedenen Geräten, sei es ein Smartphone oder Tablet.
Dank der mobilen Version des Boomerang Casinos kann man auch unterwegs nicht auf den Spaß und die Spannung von Casino-Spielen verzichten. Egal ob man in der Bahn sitzt, im Park spazieren geht oder auf den Bus wartet, man hat jederzeit Zugriff auf die vielfältige Auswahl an Spielen des Boomerang Casinos.
Zudem bietet das Boomerang Casino Mobil auch die Möglichkeit, Ein- und Auszahlungen vorzunehmen, Bonusangebote zu nutzen und den Kundendienst zu kontaktieren. Somit ist man auch unterwegs bestens versorgt und kann sich ganz auf das Spielvergnügen konzentrieren.
Insgesamt ist das Boomerang Casino Mobil eine gelungene Ergänzung zum bereits etablierten Online-Casino und bietet den Spielern die Möglichkeit, auch von unterwegs aus unkompliziert und bequem zu spielen. Probieren Sie es aus und lassen Sie sich von der Vielfalt der Spiele und der Benutzerfreundlichkeit der mobilen Version überzeugen!
https://boomerangcasino.one/
informative post anydesk
look here tradingview download
Boomerang Casino ist ein Online-Casino, das mit seinem einzigartigen Konzept und seiner Vielfalt an Spielen Spieler aus der ganzen Welt anspricht. In diesem Artikel werden wir eine eingehende ГњberprГјfung des Boomerang Casinos durchfГјhren und die verschiedenen Aspekte des Online-Casinos diskutieren.
Das erste, was auffГ¤llt, wenn man das Boomerang Casino betritt, ist die benutzerfreundliche Website. Die Navigation ist einfach und Гјbersichtlich, so dass neue Spieler sich leicht zurechtfinden kГ¶nnen. Das Casino bietet eine groГџe Auswahl an Spielen von renommierten Softwareanbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen. Es gibt eine Vielzahl von Spielautomaten, Tischspielen, Live-Casino-Spielen und Jackpot-Spielen zur Auswahl, so dass fГјr jeden Geschmack etwas dabei ist.
Ein weiterer Pluspunkt des Boomerang Casinos ist die großzügige Bonuspolitik. Neue Spieler können von einem Willkommensbonus profitieren, der Freispiele und Bonusgeld umfasst. Darüber hinaus gibt es regelmäßige Promotionen und Sonderangebote für Stammkunden, die für zusätzliche Unterhaltung und Gewinnchancen sorgen.
Ein wichtiger Aspekt, den wir bei unserer ГњberprГјfung des Boomerang Casinos berГјcksichtigen mГјssen, ist die Sicherheit und Fairness des Casinos. Das Casino verfГјgt Гјber eine Lizenz der Malta Gaming Authority, was bedeutet, dass es strenge Vorschriften und Standards erfГјllen muss, um seine Lizenz zu behalten. DarГјber hinaus verwendet das Casino eine sichere SSL-VerschlГјsselungstechnologie, um sicherzustellen, dass alle Transaktionen sicher und geschГјtzt sind.
Zusammenfassend lässt sich sagen, dass das Boomerang Casino eine gute Wahl für Spieler ist, die ein erstklassiges Online-Casino-Erlebnis suchen. Mit seiner Vielzahl von Spielen, großzügigen Boni und sicherer Spielumgebung hat das Casino viel zu bieten. Wir empfehlen allen Spielern, einen Blick auf das Boomerang Casino zu werfen und ihr Glück zu versuchen.
https://boomerangcasino.one/
мунжаро лекарство цена – оземпик препарат +в москве, семаглутид цена отзывы
Freispiele sind eine beliebte Möglichkeit, um im Tipico Casino zusätzliche Gewinne zu erzielen. Diese kostenlosen Spielrunden können auf verschiedene Arten erhalten werden und bieten den Spielern die Chance, ohne eigenen Einsatz echtes Geld zu gewinnen.
Es gibt verschiedene Möglichkeiten, um Freispiele im Tipico Casino zu erhalten. Eine der bekanntesten ist der Willkommensbonus für neue Spieler. Bei der Registrierung und ersten Einzahlung erhalten Spieler oft eine bestimmte Anzahl an Freispielen für ausgewählte Spielautomaten. Diese können dann genutzt werden, um kostenlos zu spielen und dabei möglicherweise Gewinne zu erzielen.
Aber auch Bestandskunden werden im Tipico Casino regelmäßig mit Freispielen belohnt. Diese können beispielsweise im Rahmen von Sonderaktionen, Turnieren oder als Belohnung für treue Spieler vergeben werden. Auch das Spielen bestimmter Spiele oder das Erreichen bestimmter Ziele kann zu Freispielen führen.
Für die Nutzung von Freispielen gelten in der Regel bestimmte Bedingungen, die vom Casino festgelegt werden. Zum Beispiel müssen die Gewinne aus Freispielen oft mehrfach umgesetzt werden, bevor sie ausgezahlt werden können. Es ist daher wichtig, die jeweiligen Bonusbedingungen zu beachten, um keine bösen Überraschungen zu erleben.
Insgesamt bieten Freispiele im Tipico Casino eine spannende Möglichkeit, um zusätzliche Gewinne zu erzielen und das Spielerlebnis noch aufregender zu gestalten. Durch regelmäßige Aktionen und Angebote haben die Spieler die Chance, immer wieder von Freispielen zu profitieren und ihr Glück auf die Probe zu stellen.
https://tipicocasino.one/
Boomerang Bet Casino Review
Das Boomerang Bet Casino ist eine aufstrebende Online-Casino-Plattform, die sich schnell einen Namen in der Welt der Online-Glücksspiele gemacht hat. Mit einer riesigen Auswahl an Spielen, großzügigen Boni und einer benutzerfreundlichen Benutzeroberfläche hat das Casino viel zu bieten für Spieler aller Erfahrungsstufen.
Das Casino verfügt über eine Vielzahl von Spielen, darunter beliebte Slots, Tischspiele und Live-Dealer-Spiele. Spieler können aus Hunderten von Spielen wählen, darunter Klassiker wie Roulette, Blackjack und Poker, sowie eine Vielzahl von modernen und aufregenden Slot-Spielen. Mit so vielen Optionen zur Auswahl ist für jeden Spieler etwas dabei.
Ein weiterer großer Vorteil des Boomerang Bet Casinos sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler erhalten oft Willkommensboni, die ihnen kostenlose Spielguthaben und Freispiele ermöglichen. Darüber hinaus gibt es auch regelmäßige Aktionen und Bonusangebote, die es Spielern ermöglichen, ihre Gewinne zu maximieren und ihr Spielerlebnis zu verbessern.
Die Benutzeroberfläche des Casinos ist intuitiv und benutzerfreundlich gestaltet, was es einfach macht, zwischen den verschiedenen Spielen zu navigieren und das Beste aus dem Spielerlebnis herauszuholen. Der Kundensupport steht Spielern rund um die Uhr zur Verfügung, um bei Fragen oder Problemen zu helfen.
Insgesamt bietet das Boomerang Bet Casino eine großartige Online-Spielerfahrung für Glücksspiel-Enthusiasten aller Art. Mit einer großen Auswahl an Spielen, großzügigen Boni und einer einfach zu bedienenden Benutzeroberfläche ist das Casino definitiv einen Blick wert. Probieren Sie es noch heute aus und sehen Sie selbst, warum das Boomerang Bet Casino so beliebt ist.
https://boomerangcasino.one/
description MetaMask Chrome
подробнее здесь
Купить инвалидность, купить группу инвалидности
Das Boomerang Casino in Island: Eine aufregende neue Spiel- und Unterhaltungsdestination
Das Boomerang Casino in Island hat in den letzten Jahren viel Aufmerksamkeit auf sich gezogen, da es eine neue und aufregende Option für Glücksspiel- und Unterhaltungsliebhaber bietet. Das Casino, das 2020 eröffnet wurde, hat schnell einen Ruf für sein umfangreiches Spielangebot, seine hochmoderne Ausstattung und seine entspannte Atmosphäre aufgebaut.
Das Boomerang Casino bietet eine Vielzahl von Spielen für alle Geschmäcker und Vorlieben. Von traditionellen Tischspielen wie Blackjack und Roulette bis hin zu modernen Spielautomaten und Video-Slots bietet das Casino etwas für jeden Spieler. Darüber hinaus bietet das Casino regelmäßig Turniere und Veranstaltungen an, die die Spieler dazu ermutigen, sich gegenseitig herauszufordern und ihr Können unter Beweis zu stellen.
Die Ausstattung des Boomerang Casinos ist auf dem neuesten Stand der Technik und sorgt für ein erstklassiges Spielerlebnis. Die Spielautomaten und Tischspiele sind von führenden Herstellern entwickelt und bieten eine reibungslose und unterhaltsame Erfahrung für die Spieler. Darüber hinaus wird das Casino regelmäßig gewartet und aktualisiert, um sicherzustellen, dass die Spieler immer Zugang zu den neuesten Spielen und Technologien haben.
Die Atmosphäre im Boomerang Casino ist entspannt und einladend. Das Casino wurde so gestaltet, dass es ein Gefühl der Gemeinschaft und des Miteinanders vermittelt, wodurch die Spieler sich wohl und willkommen fühlen. Das Personal des Casinos ist freundlich und hilfsbereit und steht den Spielern jederzeit zur Seite, um sicherzustellen, dass ihr Besuch angenehm und unvergesslich wird.
Insgesamt ist das Boomerang Casino in Island eine aufregende neue Option für Glücksspiel- und Unterhaltungsliebhaber. Mit seinem umfangreichen Spielangebot, seiner erstklassigen Ausstattung und seiner entspannten Atmosphäre bietet das Casino eine einzigartige und unterhaltsame Erfahrung für alle Spieler. Wer also auf der Suche nach einem unvergesslichen Spielerlebnis ist, sollte definitiv das Boomerang Casino in Island besuchen.
https://boomerangcasino.one/
Das Boomerang.bet Casino ist eine aufregende neue Online-GlГјcksspielplattform. Mit einer breiten Palette von Spielen, groГџzГјgigen Boni und einer benutzerfreundlichen Plattform bietet dieses Casino eine erstklassige Spielerfahrung fГјr alle Arten von Spielern.
Eine der größten Attraktionen des Boomerang.bet Casinos sind die vielfältigen Spieloptionen. Von klassischen Casino-Spielen wie Blackjack, Roulette und Spielautomaten bis hin zu innovativen neuen Spielen gibt es für jeden Geschmack etwas zu bieten. Die Spiele werden von führenden Anbietern in der Branche bereitgestellt, sodass Spieler von hochwertiger Grafik und nahtlosem Gameplay profitieren.
Darüber hinaus bietet das Boomerang.bet Casino großzügige Boni und Aktionen für neue und bestehende Spieler. Neukunden können von Willkommensboni, Freispielen und anderen Sonderangeboten profitieren, während treue Spieler regelmäßig belohnt werden. Diese Boni ermöglichen es den Spielern, ihr Guthaben zu erhöhen und mehr Spiele zu genießen.
Die benutzerfreundliche Plattform des Boomerang.bet Casinos macht es einfach, sich anzumelden, Einzahlungen vorzunehmen und direkt mit dem Spielen zu beginnen. Die Website ist übersichtlich gestaltet und bietet alle Informationen, die Spieler benötigen, um ein optimales Spielerlebnis zu gewährleisten. Der Kundensupport steht rund um die Uhr zur Verfügung, um bei Fragen oder Problemen zu helfen.
Insgesamt ist das Boomerang.bet Casino eine ausgezeichnete Wahl für alle, die auf der Suche nach einer unterhaltsamen und sicheren Online-Glücksspielplattform sind. Mit einer Vielzahl von Spielen, großzügigen Boni und einer benutzerfreundlichen Oberfläche ist dieses Casino eine erstklassige Wahl für Spieler aller Erfahrungsstufen.
https://boomerangcasino.one/
Das Tipico Casino bietet eine Vielzahl von Spielmodi, aus denen die Spieler wählen können. Jeder Spielmodus hat seine eigenen Vor- und Nachteile, aber einige stechen besonders hervor und gelten als die besten Spielmodi beim Tipico Casino.
Einer der beliebtesten Spielmodi ist das Live-Casino, bei dem die Spieler gegen echte Dealer antreten. Diese Form des Glücksspiels bietet eine authentische Casino-Erfahrung und sorgt für Spannung und Nervenkitzel. Die Spieler können in Echtzeit mit den Dealern interagieren und sich wie in einem echten Casino fühlen.
Ein weiterer beliebter Spielmodus beim Tipico Casino sind die Jackpot-Spiele. Hier haben die Spieler die Chance, hohe Geldpreise zu gewinnen, indem sie an progressiven Jackpot-Slots teilnehmen. Diese Spiele bieten oft Millionen von Euro an Preisgeldern, die das Leben der glücklichen Gewinner für immer verändern können.
Neben den Live-Casino und Jackpot-Spielen bietet das Tipico Casino auch eine große Auswahl an klassischen Spielautomaten und Tischspielen. Diese Spiele sind ideal für Spieler, die lieber alleine spielen und sich nicht mit anderen Spielern messen möchten. Sie bieten eine entspannte und unterhaltsame Spielerfahrung, die sich perfekt für Anfänger eignet.
Insgesamt bieten alle Spielmodi im Tipico Casino eine erstklassige Spielerfahrung und sorgen für Unterhaltung auf höchstem Niveau. Es liegt an den Spielern, den für sie besten Spielmodus auszuwählen und ihr Glück zu versuchen. Egal für welchen Spielmodus sie sich entscheiden, sie werden sicherlich eine großartige Zeit im Tipico Casino haben.
https://tipicocasino.one/
Das Tipico Casino bietet seinen Kunden die Möglichkeit, die spannende Welt des Glücksspiels auch von unterwegs aus zu erleben. Mit der Tipico Casino App können Spieler ihre Lieblingsspiele jederzeit und überall genießen.
Um die App herunterzuladen, muss man zunächst die offizielle Webseite des Tipico Casinos besuchen. Dort findet man einen Link zum Download der App, der sowohl für iOS als auch für Android Geräte verfügbar ist. Nach dem Klick auf den Download-Button wird die App automatisch auf das Mobilgerät geladen.
Die Tipico Casino App überzeugt mit einer benutzerfreundlichen Oberfläche, einer großen Auswahl an Spielen und einer reibungslosen Funktionalität. Spieler können aus einer Vielzahl von Slots, Tischspielen und Live Casino Spielen wählen und so ihr Glück versuchen.
Zusätzlich zum Spielspaß bietet die Tipico Casino App auch eine sichere und zuverlässige Zahlungsabwicklung. Spieler können Ein- und Auszahlungen bequem und einfach über die App tätigen.
Insgesamt ist die Tipico Casino App eine großartige Möglichkeit, die Welt des Glücksspiels mobil zu erleben. Egal ob man unterwegs ist oder zu Hause entspannen möchte, mit der App von Tipico Casino ist für Unterhaltung bestens gesorgt.
https://tipicocasino.one/
апостиль образование москва
Tipico Casino Freispiele kaufen
In vielen Online Casinos haben Spieler die Möglichkeit, Freispiele zu erwerben, um damit ihr Glück bei verschiedenen Spielautomaten zu versuchen. Auch im Tipico Casino gibt es die Möglichkeit, Freispiele zu kaufen und so die Spannung und Nervenkitzel beim Spielen zu erhöhen.
Durch den Kauf von Freispielen können Spieler direkt in die Action einsteigen, ohne auf den Zufall angewiesen zu sein, um Freispiele während des Spiels zu erhalten. Dies ermöglicht es den Spielern, schneller mit dem Spielen zu beginnen und potenziell größere Gewinne zu erzielen.
Um Freispiele im Tipico Casino zu kaufen, müssen die Spieler einfach den entsprechenden Bereich im Casino besuchen und dort die verfügbaren Angebote prüfen. Oftmals gibt es verschiedene Pakete zur Auswahl, die unterschiedliche Anzahlen von Freispielen enthalten. Die Preise für die Freispiele variieren je nach Angebot und können mit Echtgeld oder Bonusguthaben bezahlt werden.
Bevor man Freispiele kauft, ist es wichtig zu beachten, dass die Gewinne, die mit diesen erzielt werden, oft bestimmten Umsatzbedingungen unterliegen. Diese Bedingungen geben an, wie oft die Gewinne aus den Freispielen umgesetzt werden müssen, bevor sie ausgezahlt werden können. Es ist daher ratsam, die Bedingungen genau zu lesen, bevor man sich für den Kauf von Freispielen entscheidet.
Trotzdem kann der Kauf von Freispielen im Tipico Casino eine aufregende Möglichkeit sein, um das Spielerlebnis zu verbessern und die Chancen auf Gewinne zu erhöhen. Mit etwas Glück und Geschick können die Spieler mit den gekauften Freispielen große Gewinne erzielen und ihr Casinoerlebnis noch spannender gestalten.
https://tipicocasino.one/
Das Boomerang-Casino: Eine aufregende neue Spielerfahrung
Das Boomerang-Casino ist eine innovative Online-GlГјcksspielplattform, die in der Welt des Online-Casinos fГјr Furore gesorgt hat. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und einem modernen Design bietet das Boomerang-Casino ein Spielerlebnis, das seinesgleichen sucht.
Einzigartig am Boomerang-Casino ist das Konzept des “Boomerang-Effekts”. Г„hnlich wie ein Boomerang, der immer wieder zu seinem Ausgangspunkt zurГјckkehrt, bietet das Casino den Spielern regelmäßige Boni und Promotionen, die sie immer wieder auf die Plattform zurГјcklocken. Dieser Ansatz hat sich als Г¤uГџerst beliebt erwiesen und hat dazu gefГјhrt, dass viele Spieler dem Boomerang-Casino treu geblieben sind.
Das Boomerang-Casino bietet eine breite Palette von Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele. Mit Spielen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming und Play’n GO kГ¶nnen die Spieler sicher sein, dass sie hochwertige und unterhaltsame Spiele genieГџen werden. DarГјber hinaus bietet das Casino regelmäßig neue Spiele sowie exklusive Titel an, die nur auf der Plattform verfГјgbar sind.
Neben einer Vielzahl von Spielen und spannenden Boni legt das Boomerang-Casino auch großen Wert auf Sicherheit und Fairness. Die Plattform verfügt über eine gültige Glücksspiellizenz und verwendet die neueste SSL-Verschlüsselungstechnologie, um sicherzustellen, dass die persönlichen und finanziellen Daten der Spieler geschützt sind. Das Casino arbeitet auch mit unabhängigen Prüfungsbehörden zusammen, um sicherzustellen, dass die Spiele fair und zufällig sind.
Insgesamt bietet das Boomerang-Casino eine aufregende und lohnende Spielerfahrung fГјr GlГјcksspielfans. Mit einer vielfГ¤ltigen Auswahl an Spielen, groГџzГјgigen Boni und einem innovativen Konzept des “Boomerang-Effekts” hat sich das Casino als eine der fГјhrenden Online-GlГјcksspielplattformen etabliert. Wenn Sie auf der Suche nach einem neuen und aufregenden Casino-Erlebnis sind, sollten Sie definitiv einen Blick auf das Boomerang-Casino werfen.
https://boomerangcasino.one/
Visa Zusatzkosten bei Tipico Casino
Das Tipico Casino bietet seinen Kunden eine sichere und bequeme Möglichkeit, um Einzahlungen auf ihr Spielerkonto vorzunehmen. Eine weit verbreitete Methode ist die Visa-Karte, mit der man schnell und einfach Geld auf sein Spielerkonto transferieren kann. Allerdings gibt es beim Tipico Casino einige Zusatzkosten, die bei der Verwendung der Visa-Karte anfallen können.
Die Zusatzkosten für Einzahlungen mit Visa-Karte beim Tipico Casino betragen in der Regel eine Gebühr von 2% des eingezahlten Betrags. Das bedeutet, dass bei einer Einzahlung von 100€ mit der Visa-Karte eine Zusatzgebühr von 2€ anfällt. Diese Gebühr wird direkt von dem eingezahlten Betrag abgezogen, sodass der Spieler nicht die vollen 100€ auf sein Spielerkonto gutgeschrieben bekommt.
Es ist wichtig zu beachten, dass diese Zusatzkosten ausschließlich für Einzahlungen mit der Visa-Karte gelten. Andere Zahlungsmethoden wie zum Beispiel PayPal oder Banküberweisungen sind in der Regel gebührenfrei. Daher sollten Spieler, die häufiger im Tipico Casino spielen und Einzahlungen tätigen, die verschiedenen Zahlungsmethoden vergleichen und diejenige wählen, die für sie am kostengünstigsten ist.
Zusammenfassend lässt sich festhalten, dass beim Tipico Casino beim Nutzen der Visa-Karte Zusatzkosten in Form einer Gebühr von 2% des eingezahlten Betrags anfallen können. Spieler sollten daher die verschiedenen Zahlungsmethoden vergleichen und diejenige wählen, die für sie am kostengünstigsten ist.
https://tipicocasino.one/
Gogo Casino är ett populärt online casino som erbjuder en spännande spelupplevelse för alla typer av spelare. Med ett brett utbud av casinospel, inklusive slots, bordsspel och live casino, finns det något för alla att njuta av. En av de mest populära spelsajterna är LeoVegas som erbjuder en imponerande samling av spel och en användarvänlig plattform.
Gogo Casino har ett samarbete med LeoVegas vilket innebär att spelarna kan dra nytta av de bästa spelen och den mest avancerade tekniken. När man spelar på Gogo Casino leovegas kan spelarna förvänta sig en smidig och säker spelupplevelse med snabba utbetalningar och professionell kundsupport.
En av de största fördelarna med att spela på Gogo Casino leovegas är det stora urvalet av spel som erbjuds. Oavsett om du föredrar klassiska slots, spännande bordsspel eller autentiska live casinospel, finns det garanterat något för alla att njuta av. Dessutom erbjuder LeoVegas regelbundet kampanjer och erbjudanden för att belöna sina spelare och ge dem en ännu bättre spelupplevelse.
Med en användarvänlig plattform och en mobiloptimerad design kan spelarna enkelt spela sina favoritspel var de än befinner sig. Dessutom erbjuder LeoVegas en säker och rättvis spelmiljö med licenser från de mest ansedda spelmyndigheterna.
Sammanfattningsvis är Gogo Casino leovegas en fantastisk speldestination för alla som är ute efter en spännande och underhållande spelupplevelse. Med ett stort urval av spel, generösa kampanjer och en säker spelmiljö är det lätt att se varför detta online casino är så populärt. Så varför inte prova lyckan på Gogo Casino leovegas idag och ta chansen att vinna stort!
https://gogocasino.one
Gogo Casino kundtjänst
Gogo Casino är en populär online casino som erbjuder sina spelare en enkel och smidig spelupplevelse. För att säkerställa att alla spelare har den bästa möjliga upplevelsen är det viktigt att ha en pålitlig och effektiv kundtjänst på plats.
Gogo Casino kundtjänst är känd för att vara tillgänglig och hjälpsam, vilket gör det mycket enkelt för spelarna att få svar på sina frågor och lösa eventuella problem som kan uppstå. Kundtjänsten är tillgänglig dygnet runt, vilket innebär att spelare kan få hjälp när som helst på dagen eller natten.
Den vänliga och kunniga kundtjänstpersonalen är redo att hjälpa till med allt från att ge information om spel och bonusar till att lösa tekniska problem och hantera eventuella klagomål. Oavsett vad spelarna behöver hjälp med, kan de lita på att Gogo Casino kundtjänst kommer att göra sitt bästa för att lösa det på ett snabbt och effektivt sätt.
Utöver den utmärkta kundtjänsten erbjuder Gogo Casino också en rad andra fördelar för sina spelare, inklusive ett brett utbud av spel, generösa bonusar och snabba utbetalningar. Med allt detta i åtanke är det inte konstigt att Gogo Casino fortsätter att vara en favorit bland svenska spelare.
Sammanfattningsvis är Gogo Casino kundtjänst en viktig del av den övergripande spelupplevelsen för spelare på detta online casino. Med sin tillgänglighet, effektivitet och vänliga personal är det ingen tvekan om att Gogo Casino kundtjänst lämnar sina spelare nöjda och välförstådda.
https://gogocasino.one
Gogo Casino Kundtjänst
Gogo Casino är en populär onlineplattform för spelentusiaster som erbjuder ett brett utbud av spelalternativ, snabba uttag och en användarvänlig design. För att säkerställa en smidig spelupplevelse för sina kunder, har Gogo Casino en dedikerad kundtjänst som är tillgänglig för att hjälpa sina spelare med eventuella frågor eller problem.
Gogo Casinos kundtjänst är tillgänglig dygnet runt via livechatt och e-post för att ge snabba och effektiva svar på spelarnas frågor. Kundtjänstteamet är välutbildade och förtrogna med plattformen och kan hjälpa spelare med allt från tekniska problem till frågor om bonusar och uttag.
En av fördelarna med Gogo Casinos kundtjänst är att de är mycket tillgängliga och snabba på att svara på spelarnas förfrågningar. Detta gör det möjligt för spelare att få hjälp omedelbart om de stöter på problem eller behöver assistans under sin spelupplevelse.
Utöver att vara tillgänglig för att hjälpa till med eventuella problem, strävar Gogo Casinos kundtjänst också efter att skapa en positiv och personlig kontakt med sina spelare. Genom att skapa en atmosfär av öppenhet och tillgänglighet bidrar Gogo Casino till att skapa en positiv spelupplevelse för sina kunder.
Sammanfattningsvis kan man säga att Gogo Casinos kundtjänst är en viktig del av deras framgång som onlinecasino. Genom att erbjuda snabb och effektiv support till sina spelare, bidrar kundtjänstteamet till att skapa en positiv spelupplevelse för alla som besöker plattformen.
https://gogocasino.one
Gogo Casino är en populär online casino som erbjuder spelare en spännande och underhållande spelupplevelse. För att säkerställa att spelarna har den bästa möjliga upplevelsen har Gogo Casino en dedikerad kundtjänstavdelning som är tillgänglig för att hjälpa spelarna med eventuella frågor eller problem de kan ha.
Gogo Casino kundtjänst är tillgänglig via livechatt, e-post och telefon dygnet runt, vilket innebär att spelarna kan få hjälp när som helst på dygnet. Kundtjänstteamet består av vänliga och kunniga medarbetare som är beredda att assistera spelarna på ett professionellt och effektivt sätt.
Oavsett om spelarna har problem med insättningar eller uttag, behöver hjälp att förstå reglerna för ett specifikt spel eller helt enkelt vill ha mer information om kampanjer och erbjudanden, är Gogo Casino kundtjänst där för att hjälpa till. Spelarna kan vara säkra på att de får den bästa service och support, så att de kan njuta av sin spelupplevelse till fullo.
Sammanfattningsvis är Gogo Casino kundtjänst tillgänglig dygnet runt för att stödja spelarna och se till att de har en positiv och problemfri spelupplevelse. Med en dedikerad och professionell kundtjänstavdelning kan spelarna känna sig trygga och säkra när de spelar på Gogo Casino.
https://gogocasino.one
Gogo Casino Kundtjänst: Allt du behöver veta
Gogo Casino är en populär online spelplattform som erbjuder ett brett utbud av casinospel för sina spelare. För att säkerställa en problemfri spelupplevelse för alla sina kunder, erbjuder Gogo Casino en dedikerad kundtjänst som är tillgänglig dygnet runt för att hjälpa till med alla frågor eller bekymmer.
Gogo Casino kundtjänst är känd för sin professionella och vänliga service. Kundtjänstteamet är välutbildat och kan hjälpa dig med allt från tekniska frågor till frågor om insättningar och uttag. Om du har några problem med att komma åt ditt konto eller om du har frågor om bonusar eller kampanjer, kan du enkelt kontakta kundtjänsten via livechatt, e-post eller telefon.
En av fördelarna med att spela på Gogo Casino är att du kan få hjälp på ditt modersmål. Kundtjänstteamet talar flera olika språk, inklusive svenska, så du kan vara säker på att du kommer att få den hjälp du behöver på ett språk som du förstår.
FГ¶r att komma i kontakt med Gogo Casino kundtjГ¤nst, behГ¶ver du bara klicka pГҐ fliken “Kontakta oss” pГҐ webbplatsen. DГ¤r hittar du alla kontaktuppgifter du behГ¶ver fГ¶r att komma i kontakt med teamet.
Sammanfattningsvis, om du spelar på Gogo Casino och behöver hjälp med något, kan du vara säker på att du kommer att få den bästa kundtjänsten. Med snabb och effektiv hjälp till hands dygnet runt kan du fortsätta njuta av ditt spelande utan att behöva oroa dig för något. Gogo Casino kundtjänst är här för att göra din spelupplevelse så smidig och trevlig som möjligt.
https://gogocasino.one
Das Tipico 1-Cent-Casino ist eine einzigartige Spiel-Plattform, die es Spielern ermöglicht, mit sehr kleinen Einsätzen in die Welt des Online-Glücksspiels einzutauchen. Bei diesem Casino-Anbieter können die Spieler bereits ab einem Cent pro Spiel teilnehmen und somit das Risiko minimal halten.
Durch die niedrigen Einsätze eignet sich das Tipico 1-Cent-Casino besonders gut für Einsteiger, die noch keine Erfahrung mit Online-Casinos haben oder einfach nur aus Spaß ein paar Runden spielen möchten. Aber auch für erfahrene Spieler bietet das 1-Cent-Casino die Möglichkeit, neue Spiele auszuprobieren oder Strategien zu testen, ohne dabei großes Geld riskieren zu müssen.
Das Angebot an Spielen im Tipico 1-Cent-Casino ist vielfältig und umfasst klassische Casino-Spiele wie Roulette, Blackjack, Poker und Spielautomaten. Die Spieler können zwischen verschiedenen Varianten und Designs wählen, um ihr persönliches Lieblingsspiel zu finden. Zudem bietet das Casino regelmäßig neue Spiele an, sodass es nie langweilig wird.
Ein weiterer Vorteil des Tipico 1-Cent-Casinos ist die Möglichkeit, auch mobil zu spielen. Die Casino-Plattform ist für alle gängigen mobilen Geräte optimiert, sodass die Spieler von überall aus Zugriff auf ihre Lieblingsspiele haben.
Insgesamt ist das Tipico 1-Cent-Casino eine tolle Option für alle, die gerne in die Welt des Online-Glücksspiels eintauchen möchten, ohne dabei viel Geld riskieren zu müssen. Die niedrigen Einsätze, die große Auswahl an Spielen und die Möglichkeit des mobilen Spielens machen das Casino zu einer attraktiven Wahl für Anfänger und erfahrene Spieler gleichermaßen. Wer also Lust auf spannende Casino-Unterhaltung hat, sollte das Tipico 1-Cent-Casino definitiv einmal ausprobieren.
https://tipicocasino.one/
Gogo casino är en populär spelplattform för många spelare runt om i Sverige. En av de viktigaste funktionerna för spelare är möjligheten att enkelt och snabbt göra uttag från sitt spelkonto. En snabb och smidig utbetalningsprocess är avgörande för att ge spelarna en bra spelupplevelse.
Gogo casino erbjuder flera olika betalningsmetoder för sina uttag, inklusive banköverföring, e-plånböcker och kryptovalutor. Spelarna kan välja den metod som passar dem bäst och göra sina uttag med bara några klick.
En annan fördel med Gogo casino är att de har snabba utbetalningar. Många spelare vittnar om att de har fått sina vinster utbetalade inom bara några timmar efter att de begärt sitt uttag. Detta är en stor fördel för spelare som vill ha tillgång till sina pengar snabbt.
Gogo casino tar också säkerheten på största allvar när det gäller utbetalningar. Alla transaktioner är krypterade och skyddade för att säkerställa att spelarnas pengar är trygga. Dessutom har casinot en supportavdelning som är tillgänglig dygnet runt för att hjälpa spelare med sina uttag och svara på eventuella frågor.
Sammanfattningsvis är Gogo casino en bra plattform för spelare som vill ha en enkel och säker utbetalningsprocess. Med flera olika betalningsmetoder, snabba uttag och bra kundtjänst är det en bra destination för alla som gillar att spela casino online.
https://gogocasino.one
Das Boomerang Casino bietet seinen Spielern die Möglichkeit, mit Hilfe von Bonus-Codes ohne Einzahlung zusätzliche Belohnungen zu erhalten. Diese Bonus-Codes ermöglichen es den Spielern, ohne eigenes Geld einzusetzen, kostenlose Spiele oder zusätzliches Guthaben zu erhalten.
Die Boomerang Casino Bonus-Codes ohne Einzahlung sind eine großartige Möglichkeit für Spieler, die ein neues Casino ausprobieren möchten, ohne dabei ihr eigenes Geld riskieren zu müssen. Auf diese Weise können sie die angebotenen Spiele kennenlernen und verschiedene Strategien ausprobieren, ohne ein finanzielles Risiko einzugehen.
Um einen Bonus-Code ohne Einzahlung zu erhalten, müssen Spieler lediglich den entsprechenden Code eingeben, wenn sie sich bei Boomerang Casino anmelden oder wenn sie eine Einzahlung tätigen. Auf diese Weise können sie von den zusätzlichen Belohnungen profitieren, ohne dafür Geld einzahlen zu müssen.
Die Boomerang Casino Bonus-Codes ohne Einzahlung sind eine großartige Möglichkeit, zusätzliche Belohnungen zu erhalten und das Spielerlebnis noch spannender zu gestalten. Spieler sollten jedoch beachten, dass diese Bonus-Codes in der Regel bestimmten Bedingungen unterliegen, die erfüllt werden müssen, bevor sie die Belohnungen erhalten können.
Insgesamt bieten die Boomerang Casino Bonus-Codes ohne Einzahlung den Spielern eine großartige Möglichkeit, ihr Spielerlebnis zu verbessern und zusätzliche Belohnungen zu erhalten, ohne dabei ihr eigenes Geld riskieren zu müssen. Es lohnt sich also, diese Bonus-Codes zu nutzen und von den zusätzlichen Belohnungen zu profitieren.
https://boomerangcasino.one/
Gogo Casino är en popular online casino som erbjuder spelare en enkel och transparent spelupplevelse. Med sitt transparenta horisontella designkoncept, gör Gogo Casino det lätt för spelare att navigera och hitta sina favoritspel snabbt och enkelt.
Den horisontella layouten skapar en ren och modern estetik som gör det enkelt att se alla spel som erbjuds på en överblick. Dessutom ger den transparenta designen spelare en känsla av öppenhet och ärlighet när de spelar på casinot.
Gogo Casino erbjuder ett brett utbud av casinospel, inklusive slots, bordsspel och live dealer-spel. Med sin responsiva plattform kan spelare njuta av sina favoritspel bГҐde pГҐ datorn och mobilen.
För de som letar efter en casino-upplevelse som är enkel, transparent och säker, är Gogo Casino det perfekta valet. Med sin horisontella design och stora spelutbud, är detta online casino definitivt värt att prova. Besök Gogo Casino idag och upplev den transparenta spelupplevelsen själv.
https://gogocasino.one
Gogo Casino är ett populärt online casino som erbjuder spelare en enkel och smidig spelupplevelse. En av de viktigaste delarna av att spela på ett online casino är att kunna göra uttag och få dina vinster utbetalda på ett säkert och snabbt sätt. Gogo Casino har förstått vikten av att erbjuda sina spelare en transparent och effektiv utbetalningsprocess.
För att göra en utbetalning på Gogo Casino behöver spelarna följa några enkla steg. Först och främst måste spelaren logga in på sitt konto och gå till sektionen för uttag. Där kan spelaren välja vilken metod hen vill använda för att få ut sina vinster. Gogo Casino erbjuder flera olika alternativ för uttag, inklusive banköverföring, e-plånböcker och kreditkort.
När spelaren har valt sin uttagsmetod behöver hen ange det belopp som hen vill ta ut. Därefter kommer spelaren att behöva verifiera sin identitet genom att skicka in kopior av ID-handlingar och eventuella andra dokument som krävs för att bekräfta spelarens identitet. Detta är en standard procedur som online casinon måste följa enligt lag för att förhindra bedrägeri och penningtvätt.
När identiteten har verifierats kommer uttaget att behandlas av Gogo Casino. Tiden det tar för uttaget att behandlas och nå spelarens konto beror på den valda uttagsmetoden. Vissa metoder, som e-plånböcker, kan vara snabbare än andra, som banköverföringar som kan ta upp till några bankdagar att slutföras.
Gogo Casino strävar efter att göra utbetalningsprocessen så smidig och effektiv som möjligt för sina spelare. Genom att erbjuda flera olika uttagsalternativ och följa strikta regler för identitetsverifiering, kan spelare känna sig trygga med att deras vinster behandlas på ett säkert och rättvist sätt. Med Gogo Casino kan spelare fokusera på att njuta av sina favoritspel och känna sig säkra på att deras vinster kommer att betalas ut på ett professionellt sätt.
https://gogocasino.one
Boomerang Casino ist eine brandneue Casino-App, die es Spielern ermöglicht, ihre Lieblingscasinospiele überall und jederzeit zu spielen. Diese App bietet eine breite Palette von Spielen, darunter Spielautomaten, Tischspiele, Live-Casinospiele und vieles mehr. Mit einer benutzerfreundlichen Oberfläche und einer Vielzahl von Funktionen ist Boomerang Casino die perfekte Wahl für alle Casino-Liebhaber.
Eine der besten Funktionen von Boomerang Casino ist die Möglichkeit, unterwegs zu spielen. Egal, ob Sie im Zug sitzen, in der Schlange stehen oder in der Mittagspause entspannen möchten, mit dieser App können Sie Ihre Lieblingsspiele ohne Unterbrechung genießen. Darüber hinaus bietet die App regelmäßig spannende Promotionen und Boni für Spieler, wie Freispiele, Einzahlungsboni und Turniere.
Ein weiterer Vorteil von Boomerang Casino ist die hohe Sicherheit und Zuverlässigkeit. Die App verwendet die neueste Verschlüsselungstechnologie, um sicherzustellen, dass Ihre persönlichen Daten und Transaktionen geschützt sind. Darüber hinaus werden alle Spiele von renommierten Spieleanbietern entwickelt, was faire und zufällige Ergebnisse garantiert.
Wenn Sie also auf der Suche nach einer unterhaltsamen und sicheren Casino-App sind, sollten Sie definitiv Boomerang Casino ausprobieren. Laden Sie die App noch heute herunter und tauchen Sie ein in die aufregende Welt des Online-GlГјcksspiels. Viel GlГјck und viel SpaГџ beim Spielen!
https://boomerangcasino.one/
Gogo Casino com är en online spelwebbplats som erbjuder ett brett utbud av casinospel för spelare att njuta av. Med ett enkelt och användarvänligt gränssnitt kan spelarna enkelt navigera genom olika spel och hitta sina favoriter.
En av fördelarna med att spela på Gogo Casino com är det stora utbudet av spel som erbjuds. Spelare kan välja mellan klassiska casinospel som blackjack, roulette, och slots, samt mer moderna alternativ som live dealer-spel och progressiva jackpottar.
Gogo Casino com erbjuder också generösa bonusar och kampanjer för sina spelare. Nya spelare kan dra nytta av en välkomstbonus när de registrerar sig och gör sin första insättning på webbplatsen. Dessutom kan spelare delta i olika tävlingar och turneringar för chansen att vinna stora priser.
En annan fördel med att spela på Gogo Casino com är den säkerhet och pålitlighet som erbjuds. Webbplatsen använder avancerad krypteringsteknik för att skydda spelarnas personuppgifter och transaktioner. Dessutom är Gogo Casino com licensierat och reglerat av spelmyndigheter, vilket ger spelarna trygghet när de spelar på webbplatsen.
Sammanfattningsvis, Gogo Casino com är en pålitlig och underhållande online spelwebbplats med ett brett utbud av spel och generösa bonusar. Med en säker och användarvänlig plattform är det en utmärkt destination för spelare som letar efter en spännande spelupplevelse.
https://gogocasino.one
Gogo Casino är ett populärt online casino som erbjuder spelare möjligheten att spela sina favoritspel utan att behöva göra en insättning. Det är möjligt tack vare deras generösa bonuserbjudanden, inklusive bonusar utan krav på insättning.
En av de största fördelarna med en no deposit bonus på Gogo Casino är att spelare får en chans att testa på olika spel utan att riskera sina egna pengar. Det innebär att man kan utforska casinots spelutbud och funktionalitet innan man bestämmer sig för att göra en insättning. Det är ett utmärkt sätt att prova på olika spel och se vilka man trivs bäst med.
För att ta del av en no deposit bonus på Gogo Casino behöver man vanligtvis bara skapa ett konto och verifiera sin identitet. Sedan kan man ta del av bonusen och börja spela direkt. Det är enkelt och smidigt, och det finns inga krångliga villkor som man måste uppfylla för att kunna ta ut sina vinster.
Det är dock viktigt att komma ihåg att bonusar utan insättning oftast kommer med vissa omsättningskrav som måste uppfyllas innan man kan ta ut sina vinster. Det är därför viktigt att läsa igenom villkoren noggrant innan man tar del av en bonus för att undvika eventuella missförstånd eller förvirringar.
Sammanfattningsvis är en no deposit bonus på Gogo Casino en fantastisk möjlighet för spelare att utforska casinots spelutbud och vinna riktiga pengar utan att behöva sätta in egna pengar. Med generösa erbjudanden och enkla villkor är det en perfekt start för alla som vill prova på online casino.
https://gogocasino.one
Reduslim 90 Kapseln sind das neueste Produkt auf dem Markt, das die Gewichtsabnahme revolutioniert. Mit seiner einzigartigen Formel unterstützt es effektiv beim Abnehmen und kann dabei helfen, lästige Pfunde loszuwerden. Die spezielle Kombination aus natürlichen Inhaltsstoffen sorgt dafür, dass der Stoffwechsel angekurbelt wird und Fett schneller verbrannt wird.
Durch die Einnahme von Reduslim 90 Kapseln können Sie Ihren Körper auf natürliche Weise beim Abnehmen unterstützen, ohne dabei auf strenge Diäten oder anstrengende Workouts angewiesen zu sein. Die Kapseln sind einfach einzunehmen und können problemlos in den Alltag integriert werden.
Die positiven Erfahrungen von Anwendern sprechen fГјr sich – viele berichten von schnellen und langanhaltenden Erfolgen mit Reduslim 90 Kapseln. Probieren auch Sie es aus und starten Sie noch heute Ihren Weg zur Traumfigur mit diesem innovativen Produkt!
https://reduslim.at/
Boomerang Casino ist ein aufstrebendes Online-Casino, das sich immer größerer Beliebtheit erfreut. Die Plattform hat eine breite Auswahl an Spielen, großzügige Boni und eine benutzerfreundliche Benutzeroberfläche, die es den Spielern erleichtert, ihre Lieblingsspiele zu finden und zu spielen. Aber was sagen die Spieler wirklich über Boomerang Casino? In diesem Artikel werfen wir einen Blick auf die Bewertungen von Boomerang Casino und sehen, ob das Casino seinen wachsenden Ruf verdient.
Die Bewertungen von Boomerang Casino sind größtenteils positiv. Viele Spieler loben die groГџe Auswahl an Spielen, die von bekannten Anbietern wie NetEnt, Microgaming und Play’n GO bereitgestellt werden. Von Slots Гјber Tischspiele bis hin zu Live-Casino-Spielen gibt es fГјr jeden Geschmack etwas zu entdecken. Die BenutzeroberflГ¤che wird als intuitiv und benutzerfreundlich gelobt, was es selbst AnfГ¤ngern leicht macht, sich zurechtzufinden.
Ein weiterer Pluspunkt für Boomerang Casino sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler können sich über Willkommensboni freuen, während treue Spieler von regelmäßigen Promotions profitieren können. Die Umsatzbedingungen sind fair und transparent, was ebenfalls positiv hervorgehoben wird.
Einige Spieler haben jedoch auch negative Erfahrungen mit Boomerang Casino gemacht. Einige Nutzer berichten von technischen Problemen und Verzögerungen bei Auszahlungen. Dies sind jedoch Einzelfälle und das Casino arbeitet kontinuierlich daran, die Qualität des Services zu verbessern.
Insgesamt können wir sagen, dass die überwiegende Mehrheit der Spieler mit Boomerang Casino zufrieden ist. Die große Auswahl an Spielen, großzügige Boni und eine benutzerfreundliche Benutzeroberfläche machen das Casino zu einer attraktiven Option für alle, die nach einem unterhaltsamen und sicheren Online-Casino suchen. Wir empfehlen Boomerang Casino für Spieler aller Erfahrungsstufen.
https://boomerangcasino.one/
каталог https://xn—-jtbjfcbdfr0afji4m.xn--p1ai/
Das Boomerang Casino Poker: Ein Spiel, das man immer wieder zurГјckkehrt
Poker ist eines der beliebtesten Kartenspiele weltweit und wird in zahlreichen Casinos gespielt. Doch eine Variante des Spiels hat in den letzten Jahren besonders an Popularität gewonnen: das Boomerang Casino Poker.
Das Boomerang Casino Poker ist eine aufregende Variante des klassischen Pokerspiels, das sowohl Anfänger als auch erfahrene Spieler anspricht. Wie der Name schon vermuten lässt, hat dieses Spiel eine spezielle Eigenschaft, die es von anderen Pokervarianten unterscheidet: der Boomerang-Effekt.
Beim Boomerang Casino Poker haben die Spieler die Möglichkeit, ihre Karten nach einer bestimmten Runde zurückzuwerfen und neue Karten zu erhalten. Diese einzigartige Regel macht das Spiel besonders spannend, da die Spieler immer eine zweite Chance haben, ihre Hand zu verbessern.
Ein weiterer Vorteil des Boomerang Casino Pokers ist, dass die Regeln relativ einfach sind und schnell erlernt werden können. Dies macht das Spiel ideal für gesellige Runden mit Freunden oder für einen unterhaltsamen Abend im Casino.
Zusätzlich zu den spannenden Spielregeln bietet das Boomerang Casino Poker auch die Möglichkeit, Preise und Jackpots zu gewinnen. Mit etwas Glück und strategischem Geschick können die Spieler attraktive Gewinne erzielen und ihr Können unter Beweis stellen.
Insgesamt ist das Boomerang Casino Poker eine aufregende und unterhaltsame Variante des klassischen Pokerspiels, die immer mehr Spieler für sich entdecken. Ob man Anfänger oder Poker-Experte ist, dieses Spiel bietet Spaß und Spannung für jeden. Probieren Sie es aus und lassen Sie sich von der faszinierenden Welt des Boomerang Casino Pokers begeistern!
https://boomerangcasino.one/
Gogo Casino Email
Gogo Casino är en populär online-spelplattform som lockar spelare med sitt stora urval av spel och generösa erbjudanden. En av de sätt som de når ut till sina spelare är genom sin e-postkampanj.
Varje vecka skickar Gogo Casino ut e-postmeddelanden till sina registrerade spelare med information om de senaste spelen, kampanjer och specialerbjudanden. Dessa e-postmeddelanden är utformade för att hålla spelarna engagerade och informerade om vad som händer på casinot.
Genom att prenumerera på Gogo Casinos e-postlista kan spelare dra nytta av exklusiva kampanjer och bonuserbjudanden som endast är tillgängliga för dem som är registrerade. Det kan vara allt från gratissnurr på utvalda spelautomater till insättningsbonusar och tävlingar med stora priser.
För att inte missa några av dessa fantastiska erbjudanden är det viktigt att hålla sig uppdaterad genom att regelbundet kolla sin e-post. Om du är en spelare på Gogo Casino men inte har börjat prenumerera på deras e-postlista rekommenderar vi att du gör det för att inte missa några av de spännande kampanjer och bonusar som erbjuds varje vecka.
Gogo Casino email är ett utmärkt sätt för spelare att hålla sig informerade och ta del av de bästa erbjudandena och kampanjerna som casinot har att erbjuda. Så om du ännu inte prenumererar på deras e-postlista, gör det redan idag och missa inte chansen att vinna stort!
https://gogocasino.one
Gogo Casino recension
Gogo Casino är en populär spelsajt som erbjuder ett brett utbud av casinospel på nätet. De erbjuder spel från välkända leverantörer som NetEnt, Microgaming och Quickspin, vilket garanterar en hög kvalitet på spelen. Dessutom erbjuder Gogo Casino ett enkelt och användarvänligt gränssnitt som gör det lätt att navigera på sajten.
En av fördelarna med Gogo Casino är att de inte kräver att du skapar ett konto för att kunna spela. Istället använder de BankID för att verifiera din identitet, vilket gör det enkelt och smidigt att komma igång med spelandet. Dessutom erbjuder de snabba utbetalningar via Trustly, vilket gör det lätt att ta ut dina vinster.
Gogo Casino erbjuder ett stort urval av spel, inklusive slots, bordsspel och live casino. De har också regelbundna kampanjer och erbjudanden för sina spelare, vilket gör det extra spännande att spela på sajten.
Sammanfattningsvis är Gogo Casino en bra spelsajt för dig som gillar att spela casino på nätet. De erbjuder ett stort utbud av spel, enkla betalningsmetoder och snabba utbetalningar. Om du letar efter en pålitlig och underhållande spelsajt är Gogo Casino definitivt värt att testa.
https://gogocasino.one
Gogo Casino är en online spelplattform som har blivit allt mer populär bland svenska spelare. Men vad är det som gör den här sidan så speciell och hur bra är den egentligen? I den här recensionen kommer vi gå igenom allt från spelutbud och betalningsmetoder till kundsupport och användarvänlighet.
Gogo Casino erbjuder ett brett utbud av spel från flera av de främsta spelleverantörerna på marknaden. Här hittar du allt från klassiska spelautomater och bordsspel till live casino och progressiva jackpotspel. Sidan är även väl optimerad för mobila enheter, vilket gör det enkelt att spela var du än befinner dig.
När det kommer till betalningsmetoder erbjuder Gogo Casino ett flertal säkra och snabba alternativ, inklusive banköverföring, kreditkort och e-plånböcker. Uttag hanteras vanligtvis inom 24 timmar, vilket är mycket snabbt jämfört med många andra online casinon.
Kundsupporten hos Gogo Casino är tillgänglig dygnet runt via live chatt och e-post, vilket gör det enkelt att få hjälp med eventuella frågor eller problem. Dessutom erbjuder sidan en omfattande FAQ-sektion där du kan hitta svaren på de vanligaste frågorna.
Sammanfattningsvis är Gogo Casino en pålitlig och användarvänlig spelplattform som erbjuder ett brett spelutbud, snabba uttag och en effektiv kundsupport. Om du letar efter en bra online kasino att spela på, kan Gogo Casino vara ett utmärkt alternativ.
https://gogocasino.one
Gogo casino com är en populär online spelplattform där spelare kan njuta av en mängd olika casinospel. Genom att erbjuda en säker och spännande spelupplevelse har Gogo casino com blivit ett av de mest eftertraktade online casinona på marknaden.
En av de främsta fördelarna med Gogo casino com är det breda utbudet av spel som erbjuds. Oavsett om du gillar klassiska slots, bordsspel eller live casinospel finns det något för alla på denna plattform. Dessutom uppdateras spelbiblioteket regelbundet med de senaste och mest populära spelen på marknaden.
Förutom det imponerande spelutbudet erbjuder Gogo casino com också generösa bonusar och kampanjer för sina spelare. Nya spelare kan dra nytta av en välkomstbonus vid sin första insättning, medan befintliga spelare kan ta del av regelbundna erbjudanden och belöningar.
En annan viktig faktor som gör Gogo casino com till en attraktiv spelplattform är dess användarvänliga design och lättanvända gränssnitt. Spelare kan enkelt navigera på plattformen och hitta sina favoritspel utan problem.
Slutligen är säkerheten och integriteten hos spelarna av högsta prioritet för Gogo casino com. Plattformen använder avancerad krypteringsteknik för att säkerställa att alla transaktioner och personuppgifter förblir skyddade.
Sammanfattningsvis är Gogo casino com en utmärkt spelplattform för spelare som letar efter en spännande och säker spelupplevelse. Med sitt omfattande spelutbud, generösa bonusar och användarvänliga design har Gogo casino com blivit ett av de ledande online casinona på marknaden. Besök gogocasino.com idag för att uppleva allt vad de har att erbjuda!
https://gogocasino.one
Boomerang Casino Auszahlung – Alles, was Sie wissen mГјssen
Immer mehr Spieler entscheiden sich dafür, Online-Casinos zu besuchen, um ihre Lieblingsspiele zu genießen und möglicherweise auch etwas Geld zu gewinnen. Eines der beliebtesten Online-Casinos ist das Boomerang Casino, das eine Vielzahl von Spielen, großzügige Boni und schnelle Auszahlungen bietet.
Eine der wichtigsten Aspekte eines Online-Casinos ist die Auszahlungspolitik. Spieler möchten sicher sein, dass sie ihre Gewinne schnell und einfach abheben können. Im Folgenden werden wir genauer auf die Auszahlungsmöglichkeiten des Boomerang Casinos eingehen.
Das Boomerang Casino bietet seinen Spielern eine Vielzahl von Auszahlungsmethoden, darunter Kreditkarten, E-Wallets und Banküberweisungen. Die Bearbeitungszeit für Auszahlungen kann je nach Methode variieren, liegt jedoch in der Regel zwischen 1-5 Werktagen. Es ist wichtig zu beachten, dass das Casino möglicherweise zusätzliche Dokumente für die Auszahlung benötigt, um die Sicherheit und Integrität des Transaktionsprozesses zu gewährleisten.
DarГјber hinaus verlangt das Boomerang Casino keine GebГјhren fГјr Auszahlungen, was ein groГџer Vorteil fГјr die Spieler ist. Dies bedeutet, dass Sie Ihr Geld in vollem Umfang erhalten, ohne dass unerwГјnschte Kosten anfallen.
Um eine Auszahlung im Boomerang Casino vorzunehmen, müssen Sie sich in Ihr Konto einloggen und den Auszahlungsbereich aufrufen. Wählen Sie die gewünschte Auszahlungsmethode aus, geben Sie den Betrag ein und bestätigen Sie die Transaktion. Das Casino wird dann die Auszahlung bearbeiten und Ihnen eine Bestätigung senden, sobald der Betrag auf Ihrem Konto gutgeschrieben wurde.
Insgesamt bietet das Boomerang Casino eine sichere und zuverlässige Auszahlungserfahrung für alle Spieler. Mit einer Vielzahl von Zahlungsmethoden, schnellen Bearbeitungszeiten und keinen zusätzlichen Gebühren ist dieses Casino eine ausgezeichnete Wahl für alle, die Wert auf reibungslose Transaktionen legen. Probieren Sie es noch heute aus und erleben Sie die Spannung des Boomerang Casinos!
https://boomerangcasino.one/
“Gogo Casino Г¤r det senaste tillskottet pГҐ den svenska spelmarknaden. Med sitt fГ¤rgglada och engagerande grГ¤nssnitt lockar detta online casino spelare frГҐn hela landet. HГ¤r erbjuds ett brett utbud av casinospel, frГҐn klassiska slots till bordsspel som blackjack och roulette.
En av Gogo Casinos största fördelar är dess snabba och smidiga registreringsprocess. Istället för att behöva fylla i långa formulär och verifiera sin identitet med hjälp av dokument, kan spelare snabbt och enkelt komma igång med spelet genom att använda sitt BankID.
En annan positiv aspekt med Gogo Casino är dess generösa bonusar och kampanjer. Nya spelare välkomnas med en välkomstbonus och befintliga spelare belönas regelbundet med olika erbjudanden. Dessutom har casinot ett lojalitetsprogram som ger spelare möjlighet att samla poäng och få ännu fler förmåner.
Säkerheten är också en prioritet hos Gogo Casino. Genom att samarbeta med pålitliga betalningsleverantörer och använda den senaste krypteringstekniken, kan spelare vara säkra på att deras personliga och finansiella uppgifter är i trygga händer.
Sammanfattningsvis Г¤r Gogo Casino en spГ¤nnande och tillfГ¶rlitlig spelplattform som erbjuder en underhГҐllande spelupplevelse fГ¶r alla typer av spelare. Med sitt stora spelutbud, generГ¶sa bonusar och sГ¤kra miljГ¶ Г¤r det definitivt vГ¤rt att ge detta casino en chans.”
https://gogocasino.one
Gogo casino problem vid utag
Många spelare upplever problem när de försöker göra uttag från onlinecasinot Gogo Casino. Enligt uppgifter från flera kunder har uttagsprocessen varit långsam och krånglig, vilket har resulterat i missnöje och frustration.
Ett vanligt klagomål är att spelare har svårt att få ut sina vinster och att det tar lång tid innan pengarna når deras bankkonto. Vissa har även rapporterat att de har fått sina uttag avbrutna utan förklaring, vilket har skapat oro och förvirring bland spelarna.
Gogo Casino har erkänt att det har funnits problem med uttagsprocessen och har lovat att arbeta på att förbättra den. Företaget har betonat att man tar spelarnas feedback på allvar och att man strävar efter att erbjuda en smidig och enkel uttagsprocess för alla sina kunder.
Det är viktigt att spelare är medvetna om de problem som kan uppstå vid uttag från onlinecasinon och att man väljer ett pålitligt och säkert casino att spela på. Man bör även läsa igenom casinots regler och villkor för uttag för att undvika eventuella missförstånd och problem.
Om man upplever problem med uttag från Gogo Casino eller något annat onlinecasino är det viktigt att man kontaktar kundtjänsten för att få hjälp och support. Genom att vara tydlig och tydlig med sina frågor och bekymmer kan man förhoppningsvis lösa eventuella problem och få ut sina vinster på ett smidigt sätt.
I slutändan är det viktigt att man som spelare är medveten om vilka problem som kan uppstå vid uttag från onlinecasinon och att man agerar på ett ansvarsfullt sätt för att undvika eventuella missförstånd och konflikter. Spel ska vara roligt och underhållande, och man bör inte behöva oroa sig för att få ut sina vinster när man har haft tur vid spelborden.
https://gogocasino.one
Du fragst dich “Wie viel kostet Reduslim”? Diese Frage kann nicht eindeutig beantwortet werden, da der Preis je nach Anbieter und Menge variiert. Reduslim ist ein NahrungsergГ¤nzungsmittel, das dabei helfen soll, effektiv Gewicht zu verlieren. Wer die Kosten von Reduslim wissen mГ¶chte, sollte sich auf der offiziellen Website des Herstellers informieren. Dort sind oft aktuelle Angebote und Preise zu finden. Es lohnt sich, nach Rabatten oder Sonderaktionen Ausschau zu halten, um das Produkt gГјnstiger zu erwerben. Aber denke daran, dass QualitГ¤t oft auch ihren Preis hat. Zusammenfassend lГ¤sst sich sagen, dass der Preis von Reduslim variieren kann, aber es ist wichtig, auf hohe QualitГ¤t zu achten.
https://reduslim.at/
Tipico Casino ist eine beliebte Online-GlГјcksspielplattform, die eine breite Palette von Spielen und attraktiven Bonusangeboten fГјr ihre Kunden anbietet. Doch was passiert, wenn es Probleme mit Auszahlungen oder Boni gibt?
Leider kommt es gelegentlich vor, dass Spieler Schwierigkeiten haben, ihre Gewinne auszuzahlen oder Bonusangebote zu erhalten. In solchen Fällen ist es wichtig, den Kundenservice von Tipico Casino zu kontaktieren und das Problem zu schildern.
Es gibt verschiedene Gründe, warum Spieler keine Auszahlungen erhalten oder keinen Bonus bekommen. Oft liegt es daran, dass die Bonusbedingungen nicht erfüllt wurden oder dass es technische Probleme mit der Auszahlung gab. In solchen Fällen ist es ratsam, sich an den Kundenservice zu wenden und das Problem zu klären.
Es ist wichtig zu beachten, dass Tipico Casino strenge Sicherheitsrichtlinien hat, um betrügerische Aktivitäten zu verhindern. Deshalb kann es vorkommen, dass Spieler zusätzliche Dokumente einreichen müssen, um ihre Identität zu bestätigen, bevor sie eine Auszahlung erhalten.
Um sicherzustellen, dass es keine Probleme mit Auszahlungen oder Boni gibt, ist es ratsam, die Geschäftsbedingungen von Tipico Casino sorgfältig zu lesen und sicherzustellen, dass alle Anforderungen erfüllt sind. Wenn dennoch Probleme auftreten, sollte man den Kundenservice kontaktieren, um eine Lösung zu finden.
Insgesamt bietet Tipico Casino eine sichere und vertrauenswürdige Spielumgebung für Glücksspielliebhaber. Durch die richtige Vorgehensweise und den Kontakt zum Kundenservice können Probleme mit Auszahlungen oder Boni in der Regel schnell gelöst werden.
https://tipicocasino.one/
Gogo casino.se är en spännande nyhet på den svenska spelmarknaden. Denna underhållande och användarvänliga spelsajt erbjuder en mängd spännande casinospel och slots för alla typer av spelare.
På Gogo casino.se finns det ett brett utbud av casinospel att välja mellan. Här hittar man klassiska casinospel som blackjack, roulette och poker, men även populära slots och spelautomater. Sajten samarbetar med flera kända spelleverantörer, vilket garanterar en hög kvalitet på spelen och en härlig spelupplevelse.
Det som verkligen utmärker Gogo casino.se är deras generösa välkomstbonusar och erbjudanden till nya spelare. Här kan man ta del av bonusar, free spins och andra förmåner som gör det extra roligt att spela. Dessutom har sajten ett lojalitetsprogram där man kan samla poäng för varje spel och få belöningar i form av bonuserbjudanden och andra förmåner.
En annan fördel med Gogo casino.se är deras användarvänliga plattform och smidiga betalningsmetoder. Sajten är enkel att navigera och man kan enkelt sätta in och ta ut pengar med hjälp av säkra betalningsmetoder som banköverföring, kreditkort och e-plånböcker.
Sammanfattningsvis är Gogo casino.se en spännande och pålitlig spelsajt som erbjuder ett brett utbud av underhållande casinospel och slots. Med generösa bonusar och erbjudanden, smidiga betalningsmetoder och en användarvänlig plattform är detta definitivt värt ett besök för alla som gillar att spela casinospel online. Besök Gogo casino.se idag och upplev spänningen själv!
https://gogocasino.one
Gogo Casino är en populär online-spelplattform som erbjuder ett brett utbud av spel för sina användare. En annan populär spelsajt är LeoVegas, som är känd för sitt stora utbud av casinospel och generösa bonusar.
Tyvärr har det kommit uppgifter om att LeoVegas inte betalar ut vinster till spelare som använder Gogo Casino. Detta har skapat stor oro bland användarna, som litar på att deras vinster ska betalas ut i tid och enligt reglerna.
Det är viktigt att poängtera att det inte finns några bevis som styrker dessa påståenden, och att det kan vara enkla missförstånd eller fördröjningar som ligger bakom problemen.
Om du upplever att LeoVegas inte betalar ut dina vinster som du har vunnit på Gogo Casino, rekommenderar vi att du kontaktar deras kundtjänst för att få klarhet i situationen. Du kan också kontakta den svenska spelmyndigheten för att rapportera eventuella problem.
Det är alltid viktigt att spela ansvarsfullt och hos pålitliga speloperatörer som följer gällande regler och lagar. Vi hoppas att eventuella problem mellan Gogo Casino och LeoVegas snart kan lösas och att spelarna får sin rättmätiga vinst.
https://gogocasino.one
Gogo Casino är ett online casino som har blivit alltmer populärt hos spelare över hela Sverige. Men trots sin popularitet har vissa användare rapporterat problem när de försöker ta ut sina vinster från plattformen.
Ett vanligt problem som många spelare har stött på är långa väntetider för uttag. Trots att Gogo Casino hävdar att de behandlar uttag inom 24 timmar, har många användare upplevt att det tar betydligt längre tid att få sina pengar. Detta kan vara mycket frustrerande för spelare som vill ta ut sina vinster snabbt och smidigt.
En annan vanlig klagomål är att vissa spelare har haft svårt att kontakta kundtjänst när de stöter på problem med uttag. Många användare har rapporterat att de inte har fått något svar på sina frågor eller att kundtjänsten har varit otillgänglig när de har försökt få hjälp.
Det är viktigt att Gogo Casino tar dessa problem på allvar och arbetar för att förbättra sin service för att undvika missnöjda spelare. Spelare bör också vara medvetna om att det kan finnas vissa uttagskrav eller begränsningar som kan påverka behandlingen av uttag.
Om du har stött på problem med uttag på Gogo Casino, rekommenderar vi att du kontaktar deras kundtjänst för att få hjälp. Det är också viktigt att vara tålmodig och försöka hålla en öppen dialog med plattformen för att lösa eventuella problem.
https://gogocasino.one
Gogo Casino.se är en av Sveriges mest populära onlinecasinosajter. Med ett brett utbud av spel och en användarvänlig plattform har sajten snabbt blivit en favorit bland svenska spelare.
Gogo Casino.se erbjuder ett stort utbud av spelautomater, bordsspel och livecasinospel från ledande spelutvecklare som NetEnt, Microgaming och Evolution Gaming. Oavsett om du är ute efter att spela klassiska slots, blackjack eller roulette finns det något för alla på sajten.
En av fördelarna med att spela på Gogo Casino.se är att sajten är optimerad för spel i mobilen. Detta innebär att du kan njuta av dina favoritspel var som helst och när som helst. Dessutom erbjuder sajten en säker och trygg spelupplevelse med snabba uttag och pålitlig kundtjänst.
För de som gillar att ta del av spännande kampanjer och erbjudanden finns det regelbundet bonusar och belöningar att ta del av på Gogo Casino.se. Så oavsett om du är en ny spelare eller en erfaren veteran kommer du garanterat att hitta något som passar dig på sajten.
Sammanfattningsvis är Gogo Casino.se en pålitlig och underhållande spelsajt som erbjuder enastående spelupplevelser för alla typer av spelare. Med sitt stora spelutbud, mobila kompatibilitet och generösa bonusar är det inte konstigt att sajten har blivit en populär destination för svenska spelare. Besök Gogo Casino.se idag för att ta del av allt som sajten har att erbjuda!
https://gogocasino.one
Das Boomerang Casino wurde von AskGamblers als eines der besten Online-Casinos ausgezeichnet. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Boni und professionellem Kundenservice hat sich das Casino einen erstklassigen Ruf erarbeitet.
Das Boomerang Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und mehr. Spieler kГ¶nnen aus einer Vielzahl von Titeln von fГјhrenden Softwareanbietern wГ¤hlen, darunter NetEnt, Microgaming, Play’n GO und viele andere.
Das Casino belohnt seine Spieler mit großzügigen Boni und Aktionen, darunter Willkommensboni, Einzahlungsboni, Freispiele und mehr. Spieler können auch an aufregenden Turnieren und Wettbewerben teilnehmen, um zusätzliche Preise zu gewinnen.
Der Kundenservice im Boomerang Casino ist rund um die Uhr verfГјgbar und bietet professionelle und schnelle UnterstГјtzung bei allen Fragen und Anliegen der Spieler. Das Casino legt groГџen Wert auf Kundenzufriedenheit und arbeitet hart daran, ein sicheres und faires Spielumfeld zu schaffen.
Mit seinem breiten Spielangebot, großzügigen Boni und erstklassigem Kundenservice ist das Boomerang Casino definitiv einen Besuch wert. Spieler können sich darauf verlassen, dass sie ein unterhaltsames und lohnendes Erlebnis haben werden, wenn sie sich für dieses erstklassige Online-Casino entscheiden.
https://boomerangcasino.one/
Laura Pausini ist eine bekannte italienische Sängerin, die für ihre großartige Stimme und ihre emotionale Musik bekannt ist. Aber wie steht sie zur Gewichtsabnahme und zur Verwendung von Produkten wie Reduslim? Es gibt viele Meinungen und Gerüchte über Laura Pausinis Meinung zu Reduslim, aber was ist wirklich wahr?
Es scheint, dass Laura Pausini keine offizielle Stellungnahme zu Reduslim abgegeben hat. Einige behaupten, dass sie das Produkt verwendet hat und positive Ergebnisse erzielt hat, während andere sagen, dass sie es nicht unterstützt. Letztendlich ist es wichtig zu beachten, dass jeder Körper anders reagiert und was für eine Person funktioniert, muss nicht unbedingt für eine andere Person funktionieren.
Es ist immer ratsam, vor der Verwendung eines Gewichtsverlustprodukts mit einem Arzt zu sprechen, um sicherzustellen, dass es sicher ist und keine negativen Auswirkungen auf die Gesundheit hat. Laura Pausini hat sich zwar nicht öffentlich zu Reduslim geäußert, aber es ist wichtig, individuell zu entscheiden, ob dieses Produkt das Richtige für Sie ist. Denken Sie daran, dass die Meinungen anderer Personen nur als Richtlinie dienen und dass es am wichtigsten ist, auf Ihren eigenen Körper zu hören und die beste Entscheidung zu treffen.
https://reduslim.at/
“Gogo Casino Logga In”
Gogo Casino är en populär online spelsida där spelare kan ta del av ett brett utbud av casinospel. För att kunna spela på Gogo Casino behöver man först skapa ett konto och logga in.
FГ¶r att logga in pГҐ Gogo Casino behГ¶ver man bara besГ¶ka deras hemsida och klicka pГҐ knappen som det stГҐr “Logga In” pГҐ. Man blir dГҐ ombedd att fylla i sitt anvГ¤ndarnamn och lГ¶senord som man valde vid registreringen av sitt konto. NГ¤r man har fyllt i rГ¤tt uppgifter och klickat pГҐ “Logga In” knappen fГҐr man tillgГҐng till sitt spelkonto och kan bГ¶rja spela.
Det är viktigt att man använder en starkt lösenord för att skydda sitt konto från obehörig åtkomst. Man kan också välja att aktivera tvåfaktorautentisering för extra säkerhet.
När man spelar på Gogo Casino kan man ta del av olika bonusar och erbjudanden som kan hjälpa en att öka sina vinstchanser. Det är också viktigt att spela ansvarsfullt och sätta gränser för sitt spelande.
Sammanfattningsvis är Gogo Casino en spännande plattform för alla som älskar casinospel. Genom att enkelt logga in på sin spelkonto kan man ta del av underhållande spel och förhoppningsvis också vinna stora vinster. Så om du är sugen på lite spänning och underhållning, varför inte prova att logga in på Gogo Casino redan idag? Lycka till!
https://gogocasino.one
Gogo Casino är ett populärt online casino som erbjuder spelare en rad olika möjligheter att vinna stora vinster. När det gäller att göra uttag från ditt spelkonto hos Gogo Casino finns det flera alternativ att välja mellan.
Ditt uttag kan behandlas antingen med banköverföring eller med hjälp av olika e-plånböcker. Banköverföring kan ta upp till 5 bankdagar att behandlas medan uttag med e-plånböcker som Skrill och Neteller ofta sker nästan omedelbart.
För att göra ett uttag behöver du först logga in på ditt spelkonto på Gogo Casino och gå till sektionen för uttag. Här kan du välja det belopp du önskar ta ut samt vilken metod du föredrar för ditt uttag.
När du har gjort ditt val och bekräftat din begäran kommer Gogo Casino att behandla din förfrågan så snart som möjligt och överföra pengarna till ditt konto. Tänk på att det kan vara vissa begränsningar när det gäller minsta och högsta belopp för uttag samt eventuella avgifter som kan tillkomma.
Sammanfattningsvis gör Gogo Casino uttag enkelt och smidigt för sina spelare med flera olika alternativ att välja mellan. Så om du har haft turen att vinna stort på detta online casino kan du vara säker på att dina vinster kommer att betalas ut till dig på ett säkert och effektivt sätt.
https://gogocasino.one
Gogo Casino.se är en av de mest populära nätcasinona i Sverige just nu. Med sitt breda utbud av spel och generösa bonusar lockar de till sig både erfarna spelare och nybörjare som är ute efter spänning och underhållning.
En av fördelarna med Gogo Casino.se är att de erbjuder ett stort urval av casinospel från välkända leverantörer som NetEnt, Microgaming och Play’n GO. Det innebär att spelarna har tillgång till hundratals spelautomater, bordsspel och live casino-spel att välja mellan.
För att säkerställa en smidig spelupplevelse har Gogo Casino.se även en användarvänlig plattform som är lätt att navigera på. Detta gör det enkelt för spelarna att hitta sina favoritspel och ta del av de senaste kampanjerna och erbjudandena.
När det kommer till bonusar och belöningar så är Gogo Casino.se inte heller snåla. Nya spelare kan se fram emot en generös välkomstbonus vid sin första insättning, och lojala spelare belönas regelbundet med reload-bonusar, free spins och andra förmåner.
Sammanfattningsvis så är Gogo Casino.se en pålitlig och underhållande spelsajt som erbjuder ett brett utbud av casinospel och generösa bonusar. Oavsett om man är ute efter att spela på slots, bordsspel eller live casino-spel så finns det något för alla på Gogo Casino.se. Så om du är sugen på lite spänning och vinstchanser, varför inte prova lyckan på Gogo Casino.se redan idag? Lycka till!
https://gogocasino.one
Bonus Casino Tipico
Online Casinos erfreuen sich immer größerer Beliebtheit bei Glücksspiel-Fans auf der ganzen Welt. Eines der bekanntesten und beliebtesten Online Casinos ist Tipico. Neben einer großen Auswahl an Spielen und attraktiven Gewinnmöglichkeiten bietet Tipico auch regelmäßig lukrative Bonusangebote für seine Spieler an.
Einer der beliebtesten Boni bei Tipico ist der sogenannte Willkommensbonus. Dieser Bonus wird neuen Spielern angeboten, die sich zum ersten Mal bei Tipico registrieren und eine Einzahlung tätigen. Der Willkommensbonus kann je nach Aktion variieren, beinhaltet jedoch häufig zusätzliches Geld zum Spielen oder Freispiele für bestimmte Slots.
Ein weiterer interessanter Bonus bei Tipico ist der Reload-Bonus. Dieser Bonus wird regelmäßig für bestehende Spieler angeboten und belohnt diese für ihre Treue. Durch den Reload-Bonus können Spieler zusätzliches Geld zum Spielen erhalten oder von weiteren Freispielen profitieren.
Zusätzlich zu den Boni für Neukunden und Bestandskunden bietet Tipico auch immer wieder Sonderaktionen und Gewinnspiele an, bei denen Spieler zusätzliche Preise und Boni gewinnen können. Diese Aktionen sorgen für Abwechslung und Spannung und halten die Spieler bei Laune.
Bevor man einen Bonus bei Tipico in Anspruch nimmt, sollte man sich jedoch die Bonusbedingungen genau durchlesen. Denn oft sind bestimmte Umsatzbedingungen zu erfüllen, bevor man sich den Bonus auszahlen lassen kann. Es ist wichtig, diese Bedingungen zu kennen, um Enttäuschungen zu vermeiden.
Alles in allem bietet Tipico seinen Spielern eine Vielzahl an attraktiven Bonusangeboten, die das Spielerlebnis noch spannender und lukrativer machen. Wer gerne in Online Casinos spielt, sollte die aktuellen Bonusaktionen von Tipico im Auge behalten und sich die Chance auf extra Gewinne nicht entgehen lassen.
https://tipicocasino.one/
Auf der Suche nach einem effektiven Weg, um Gewicht zu verlieren, stößt man häufig auf das Produkt Reduslim. Doch wie hoch ist eigentlich der Reduslim costo? Der Preis kann je nach Anbieter variieren, aber eines ist sicher: Reduslim ist eine Investition in Ihre Gesundheit und Ihr Wohlbefinden wert. Mit seinen natürlichen Inhaltsstoffen kann es Ihnen helfen, schneller und effektiver Gewicht zu verlieren. Zudem unterstützt es den Stoffwechsel und kann das Hungergefühl reduzieren. Probieren Sie Reduslim noch heute aus und überzeugen Sie sich selbst von seiner Wirksamkeit!
https://reduslim.at/
Gogo casino uttag flashback
Gogo Casino är ett populärt online casino där spelare kan njuta av en rad olika spel och slots. En viktig del av att spela på ett online casino är att kunna göra uttag smidigt och säkert. Ett vanligt ämne som diskuteras bland spelare är gogo casino uttag flashback.
Det finns många olika sätt att göra uttag på Gogo Casino, inklusive banköverföringar, e-plånböcker och kreditkort. Processen för att göra ett uttag kan variera beroende på vilken metod du väljer. Vissa metoder kan vara snabbare än andra, medan vissa kan ta lite längre tid att behandla.
Många spelare har delat sina erfarenheter av att göra uttag på Gogo Casino i olika forum och diskussioner på nätet. Det är alltid bra att läsa recensioner och feedback från andra spelare för att få en bättre förståelse för hur uttagsprocessen fungerar.
För att göra ett uttag på Gogo Casino måste du vanligtvis ange dina personuppgifter och välja en lämplig betalningsmetod. Vissa metoder kan kräva att du verifierar ditt konto genom att skicka in dokument som bevis på din identitet.
Det är viktigt att komma ihåg att det kan finnas vissa begränsningar och avgifter för uttag på Gogo Casino, så se till att läsa igenom villkoren och reglerna noggrant innan du gör ett uttag.
I slutändan är Gogo Casino ett pålitligt och säkert online casino där spelare kan njuta av en bra spelupplevelse. Genom att vara medveten om hur uttagsprocessen fungerar och läsa recensioner från andra spelare kan du göra uttag på ett smidigt och problemfritt sätt. Så var inte rädd för att prova lyckan på Gogo Casino och njut av spänningen i att spela online!
https://gogocasino.one
Gogo Casino Finland är en av de mest populära onlinecasinona för finska spelare. Med sitt stora utbud av casinospel och generösa bonusar är det en favorit bland många som gillar att spela på nätet.
En av de stora fördelarna med Gogo Casino Finland är att det erbjuder en trygg och säker spelmiljö för sina spelare. Alla transaktioner är krypterade och spelplattformen är certifierad av säkerhetsorganisationer för att säkerställa att spelarna kan lita på att deras personuppgifter och pengar är i goda händer.
När det gäller spelutbudet har Gogo Casino Finland något för alla. Från klassiska casinospel som blackjack och roulette till moderna videoslots och progressiva jackpottspel, finns det något för både nybörjare och erfarna spelare att njuta av.
För de som gillar att spela live casino finns det också ett stort urval av live dealer-spel att välja mellan. Med riktiga dealers som sköter spelet i realtid ger det en autentisk casinoupplevelse direkt till spelarnas datorer eller mobila enheter.
För de som är intresserade av att prova lyckan gratis innan de gör en insättning finns det också möjlighet att spela demospel på många av spelen på Gogo Casino Finland.
Sammanfattningsvis är Gogo Casino Finland ett utmärkt val för finska spelare som letar efter en pålitlig och underhållande onlinecasino-upplevelse. Med sitt stora utbud av spel, generösa bonusar och trygga spelmiljö är det ett casino som verkligen lever upp till sitt namn.
https://gogocasino.one
Gogo Casino är en populär online kasinoplattform för svenska spelare. För att njuta av alla spännande casinospel och kampanjer som erbjuds på Gogo Casino måste spelare först logga in på sina konton.
Att logga in pГҐ Gogo Casino Г¤r en enkel process. Spelare behГ¶ver bara besГ¶ka Gogo Casinos hemsida och klicka pГҐ knappen “Logga in” lГ¤ngst upp till hГ¶ger pГҐ sidan. DГ¤r ombeds spelare att ange sitt anvГ¤ndarnamn och lГ¶senord fГ¶r att fГҐ tillgГҐng till sitt konto.
När spelare har loggat in på sina konton på Gogo Casino kan de njuta av hundratals spännande casinospel, inklusive slots, bordsspel och live-dealer spel. Dessutom erbjuder Gogo Casino regelbundet generösa kampanjer och erbjudanden för sina spelare, vilket ger dem chansen att vinna fantastiska priser och belöningar.
Så om du är sugen på att spela casinospel online, se till att logga in på ditt konto på Gogo Casino och börja utforska allt som plattformen har att erbjuda. Lycka till!
https://gogocasino.one
Tipico Casino Android 7.1.1: Das ultimative Spielerlebnis
Das Tipico Casino ist bereits seit vielen Jahren eine der beliebtesten Online-Glücksspielplattformen in Deutschland. Mit einer breiten Auswahl an Spielen und einer benutzerfreundlichen Oberfläche bietet das Casino ein erstklassiges Spielerlebnis für alle, die gerne ihr Glück beim Glücksspiel versuchen.
Die neueste Version des Tipico Casino für Android, die Version 7.1.1, bringt noch mehr Funktionen und Verbesserungen für die Spieler. Mit dieser Version können Android-Nutzer jetzt noch einfacher auf ihre Lieblingsspiele zugreifen und das Casino unterwegs genießen.
Eines der herausragenden Merkmale dieser neuen Version ist die verbesserte Benutzeroberfläche, die es den Spielern ermöglicht, ihre Lieblingsspiele schneller zu finden und nahtlos zwischen verschiedenen Spielen zu wechseln. Darüber hinaus wurden auch die Ladezeiten der Spiele optimiert, so dass die Spieler weniger Zeit damit verbringen müssen, auf das Laden der Spiele zu warten und mehr Zeit mit dem Spielen verbringen können.
Ein weiteres Highlight der neuen Version ist die Integration von Live-Dealer-Spielen, die es den Spielern ermöglicht, ein authentisches Casino-Erlebnis von zu Hause aus zu genießen. Mit Live-Dealern, die die Spiele leiten und mit den Spielern interagieren, fühlen sich die Spieler, als würden sie in einem echten Casino sitzen.
Darüber hinaus bietet die neue Version des Tipico Casino auch eine verbesserte Sicherheit, um sicherzustellen, dass die Spieler ihre persönlichen Daten und ihr Geld sicher halten können. Mit einer starken Verschlüsselungstechnologie und strengen Sicherheitsprotokollen können die Spieler beruhigt sein, dass ihre Daten jederzeit geschützt sind.
Insgesamt bietet die Tipico Casino Android 7.1.1-Version ein ultimatives Spielerlebnis für alle, die gerne online spielen. Mit einer verbesserten Benutzeroberfläche, schnelleren Ladezeiten und einer breiten Auswahl an Spielen ist das Tipico Casino die perfekte Wahl für alle Glücksspielfans. Probieren Sie es noch heute aus und erleben Sie die Spannung und den Nervenkitzel des Casinos direkt auf Ihrem Android-Gerät!
https://tipicocasino.one/
Gogo Casino är ett populärt casinospel på nätet som erbjuder en rad spännande spel och möjligheter att vinna stora summor pengar. Ett av de viktigaste aspekterna när det kommer till att spela på online casinon är möjligheten att göra snabba och smidiga uttag av sina vinster.
Uttagen på Gogo Casino sker vanligtvis på ett effektivt sätt, vilket ger spelarna en bra spelupplevelse utan onödiga fördröjningar. För att göra ett uttag på Gogo Casino behöver spelarna först logga in på sitt spelkonto och gå till uttagssektionen. Där kan de välja sin önskade uttagsmetod, som kan vara banköverföring, e-plånbok eller annan betalningsmetod.
När spelaren har valt sin önskade uttagsmetod behöver de fylla i de nödvändiga uppgifterna och bekräfta uttaget. Uttag på Gogo Casino bearbetas vanligtvis inom några timmar, men det kan ta upp till flera bankdagar beroende på vilken uttagsmetod som används.
Det är viktigt att notera att Gogo Casino kan komma att begära dokumentation för att bekräfta spelarens identitet innan de kan behandla ett uttag. Detta är en vanlig säkerhetsåtgärd som casinon använder för att försäkra sig om att transaktionerna är säkra och trygga.
Sammanfattningsvis kan det sägas att uttag på Gogo Casino vanligtvis sker på ett effektivt sätt, vilket ger spelarna en bra spelupplevelse. Genom att följa casinots uttagsinstruktioner och vara beredd att ge nödvändig dokumentation kan spelare njuta av att snabbt få tillgång till sina vinster.
https://gogocasino.one
Erfahrungsberichte Reduslim sind in den letzten Monaten immer häufiger zu hören. Viele Menschen haben positive Erfahrungen mit diesem natürlichen Nahrungsergänzungsmittel zur Gewichtsreduktion gemacht. Reduslim enthält verschiedene Inhaltsstoffe wie grüner Kaffee, Garcinia Cambogia und Bockshornklee, die dabei helfen sollen, den Stoffwechsel anzukurbeln und Fett zu verbrennen.
Die Erfahrungsberichte von Anwendern zeigen, dass Reduslim tatsächlich effektiv sein kann. Viele berichten von einer schnellen Gewichtsabnahme, mehr Energie und einem insgesamt besseren Wohlbefinden. Einige Nutzer berichten jedoch auch von Nebenwirkungen wie Kopfschmerzen oder Magenbeschwerden.
Es ist wichtig zu beachten, dass jedes Körper anders auf Nahrungsergänzungsmittel reagiert. Bevor man Reduslim einnimmt, sollte man deshalb unbedingt mit einem Arzt sprechen. Außerdem sollte man Reduslim nur in Verbindung mit einer gesunden Ernährung und ausreichend Bewegung einnehmen, um die bestmöglichen Ergebnisse zu erzielen.
Insgesamt scheinen die Erfahrungen mit Reduslim Гјberwiegend positiv zu sein. Es ist ein vielversprechendes Produkt fГјr alle, die auf der Suche nach einer natГјrlichen UnterstГјtzung bei der Gewichtsabnahme sind.
https://reduslim.at/
Gogo casino är en populär online-spelplattform som erbjuder ett brett utbud av spel och underhållning. För att fortsätta erbjuda sina användare en spännande upplevelse har Gogo casino inlett ett samarbete med flera olika spelleverantörer.
Genom detta samarbete kommer spelarna på Gogo casino att kunna njuta av ännu fler spel och variationer. Spelleverantörerna kommer att bidra med sina egna unika spel och funktioner för att göra spelupplevelsen ännu bättre.
Samarbetet med flera spelleverantörer kommer även att ge spelarna möjligheten att välja mellan olika typer av spel, inklusive slots, bordsspel och live-spel. På så sätt kan spelarna hitta sina favoritspel och prova på nya spel för att hålla upplevelsen spännande och intressant.
Gogo casino satsar på att erbjuda högkvalitativa spel och samarbetar endast med pålitliga spelleverantörer som är kända för sina spännande och underhållande spel. Genom detta samarbete strävar Gogo casino efter att skapa en unik och spännande spelplattform för alla sina användare.
För spelare som är intresserade av online-spel är Gogo casino det perfekta valet. Med det nya samarbetet med flera spelleverantörer kommer spelarna att kunna njuta av ännu fler spel och en ännu bättre spelupplevelse. Besök Gogo casino idag för att prova på de nya spelen och ta del av den spännande underhållningen.
https://gogocasino.one
фирма по уборке помещений
Gogo Casino uttag flashback
Gogo Casino är en populär spelsajt som erbjuder sina spelare möjligheten att spela en mängd olika casinospel online. Ett av de främsta fördelarna med att spela på Gogo Casino är att det finns enkla och smidiga sätt att göra insättningar och uttag.
Många spelare har delat med sig av sina erfarenheter av att göra uttag från Gogo Casino på olika forum och communities online. Många av dessa erfarenheter har varit positiva och spelarna har berättat om smidiga och snabba uttagsprocesser.
Det verkar som att Gogo Casino tar uttagsprocessen på allvar och strävar efter att göra den så enkel och bekväm som möjligt för sina spelare. Många spelare har rapporterat att de har fått sina uttag bekräftade och behandlade inom bara några timmar.
Det är också värt att notera att Gogo Casino erbjuder flera olika betalningsmetoder för uttag, inklusive banköverföring, kortbetalningar och e-plånböcker. Det innebär att spelarna har möjlighet att välja den metod som passar dem bäst.
Sammanfattningsvis verkar det som att Gogo Casino har ett gott rykte när det gäller uttag och att spelarna är nöjda med den service de erbjuder. Om du funderar på att spela på Gogo Casino kan du vara trygg i vetskapen om att du kommer att kunna göra smidiga och snabba uttag när du vinner stort.
https://gogocasino.one
Das Boomerang Casino ist eine aufstrebende Online-Spielplattform, die eine Vielzahl von Spielen anbietet und sich durch groГџzГјgige Promotionen und Boni auszeichnet. Eines der Angebote, das viele Spieler anzieht, ist der Boomerang Casino Kod Promocyjny.
Ein Kod Promocyjny ist ein spezieller Werbecode, den Spieler eingeben können, um zusätzliche Boni und Vorteile zu erhalten. Im Falle des Boomerang Casinos kann der Kod Promocyjny für verschiedene Zwecke verwendet werden, wie zum Beispiel für Freispiele, Einzahlungsboni oder Cashback-Angebote.
Um den Boomerang Casino Kod Promocyjny zu nutzen, müssen Spieler zunächst ein Konto auf der Plattform erstellen und sich anmelden. Anschließend können sie den Kod Promocyjny eingeben, wenn sie eine Einzahlung tätigen oder an einer Aktion teilnehmen. Die Boni und Vorteile, die mit dem Kod Promocyjny verbunden sind, werden dann automatisch dem Spielerkonto gutgeschrieben.
Das Boomerang Casino bietet regelmäßig neue Kod Promocyjny an, um Spieler zu belohnen und ihnen ein unterhaltsames Spielerlebnis zu bieten. Durch die Nutzung dieser Werbecodes können Spieler ihre Gewinnchancen erhöhen und ihr Guthaben auf der Plattform steigern.
Insgesamt ist der Boomerang Casino Kod Promocyjny eine großartige Möglichkeit für Spieler, zusätzliche Belohnungen zu erhalten und das Beste aus ihrem Online-Spielerlebnis herauszuholen. Durch die Teilnahme an Aktionen und die Eingabe von Werbecodes können Spieler ihr Spielvergnügen maximieren und gleichzeitig ihre Gewinnchancen erhöhen.
https://boomerangcasino.one/
Gogo Casino är ett populärt online casino i Finland som erbjuder en rolig och spännande spelupplevelse för alla spelare. Med ett stort utbud av casinospel, generösa bonusar och en användarvänlig plattform är det inte konstigt att Gogo Casino har blivit en favorit bland många finska spelare.
En av de största fördelarna med Gogo Casino är dess enkla och smidiga registreringsprocess. Istället för att behöva fylla i långa formulär och vänta på att ens registrering ska bli godkänd, kan spelare börja spela sina favoritspel direkt. Dessutom behöver spelare inte skapa ett konto för att spela på casinot, vilket sparar tid och gör hela spelupplevelsen mycket mer bekväm.
När det kommer till spelutbudet har Gogo Casino något för alla typer av spelare. Från klassiska casinospel som blackjack, roulette och slots till mer moderna alternativ som live casino och progressiva jackpottspel, finns det något för alla smaker. Dessutom samarbetar Gogo Casino med flera ledande spelutvecklare för att säkerställa att spelarna får tillgång till de senaste och bästa spelen på marknaden.
För de spelare som gillar att få lite extra belöningar finns det även generösa bonusar och kampanjer att ta del av hos Gogo Casino. Oavsett om det handlar om en välkomstbonus för nya spelare eller regelbundna erbjudanden för lojala kunder, finns det alltid något extra att se fram emot när man spelar på detta casino.
Sammanfattningsvis är Gogo Casino en fantastisk spelsajt för finska spelare som letar efter en underhållande och säker spelupplevelse. Med sitt stora spelutbud, generösa bonusar och användarvänliga plattform är det inte konstigt att Gogo Casino har blivit ett av de mest populära online casinona i Finland. Vi rekommenderar varmt alla spelare att prova lyckan hos Gogo Casino och uppleva spänningen med att vinna stort!
https://gogocasino.one
Haben Sie schon von den neuen Reduslim Tabletten gehört? Diese speziellen Tabletten sollen dabei helfen, schnell und effektiv Gewicht zu verlieren. Die Reduslim Tabletten enthalten eine einzigartige Formel aus natürlichen Inhaltsstoffen, die den Stoffwechsel ankurbeln und die Fettverbrennung fördern.
Durch die regelmäßige Einnahme der Reduslim Tabletten können Sie Ihren Körper dabei unterstützen, überschüssige Pfunde loszuwerden und Ihr Traumgewicht zu erreichen. Dank der natürlichen Zusammensetzung sind die Tabletten gut verträglich und haben keine bekannten Nebenwirkungen.
Probieren Sie es selbst aus und überzeugen Sie sich von den positiven Effekten der Reduslim Tabletten. Verabschieden Sie sich von lästigen Diäten und freuen Sie sich auf eine gesunde und nachhaltige Gewichtsabnahme. Gönnen Sie Ihrem Körper das Beste und starten Sie noch heute mit den Reduslim Tabletten!
https://reduslim.at/
Gogo casino är ett casinospel som har blivit populärt bland spelare på nätet. Det är ett online casino där spelare kan spela olika spel och ha chansen att vinna stora vinster. Många spelare är angelägna om att få information om Gogo casino och hur det fungerar.
En bra källa för att få information om Gogo casino är sajten Askgamblers. Där kan spelare få recensioner och betyg från andra spelare som har erfarenhet av att spela på detta casino. Askgamblers är en pålitlig källa för att få information och recensioner om olika online casinon, inklusive Gogo casino.
Genom att läsa recensioner och betyg på Askgamblers kan spelare få en bättre förståelse för hur Gogo casino fungerar och vilka spel som erbjuds. Det kan också hjälpa spelare att avgöra om det är rätt casino för dem att spela på. Att ha tillgång till recensioner och betyg från andra spelare kan vara till stor hjälp när man väljer ett online casino att spela på.
Gogo casino är ett spännande och underhållande casino som erbjuder en mängd olika spel för spelare att njuta av. Genom att använda sajten Askgamblers kan spelare få den information de behöver för att kunna ta en informerad beslut om att spela på Gogo casino. Så om du är intresserad av att spela på detta casino, ta en titt på Askgamblers för att se vad andra spelare har att säga om det.
https://gogocasino.one
Gogo Casino samarbete
Gogo Casino är ett populärt online casino som erbjuder spelare en spännande och underhållande spelupplevelse. För att kunna erbjuda de bästa spelen och den bästa spelupplevelsen möjligt, samarbetar Gogo Casino med flera olika spelleverantörer.
Genom att samarbeta med olika spelleverantörer kan Gogo Casino erbjuda ett brett utbud av spel av hög kvalitet. Spelleverantörerna som Gogo Casino samarbetar med är välkända inom spelbranschen och är kända för sina innovativa och underhållande spel.
Genom att samarbeta med flera olika spelleverantörer kan Gogo Casino också erbjuda spelare olika typer av spel. Oavsett om du föredrar klassiska bordsspel som blackjack och roulette, eller om du föredrar mer moderna och spännande videoslots, så finns det något för alla på Gogo Casino.
Gogo Casino strävar efter att erbjuda spelare den bästa spelupplevelsen möjligt, och genom att samarbeta med flera olika spelleverantörer kan de säkerställa att deras spelutbud alltid är varierat och intressant. Eftersom Gogo Casino samarbetar med flera olika spelleverantörer kan de också erbjuda spelare regelbundna kampanjer och erbjudanden, vilket gör det ännu mer spännande att spela på Gogo Casino.
Sammanfattningsvis är Gogo Casino samarbete med olika spelleverantörer en viktig del av deras framgång. Genom att samarbeta med flera olika spelleverantörer kan Gogo Casino erbjuda spelare ett brett utbud av spel av hög kvalitet och säkerställa att deras spelutbud är varierat och intressant. Om du letar efter en spännande och underhållande spelupplevelse, så är Gogo Casino definitivt värt ett besök.
https://gogocasino.one
Zet Casino ist eine beliebte Online-Glücksspielplattform, die ihren Nutzern eine Vielzahl von spannenden Spielen und großzügigen Werbeaktionen bietet. Einer der besten Wege, um das Spielerlebnis noch aufregender zu gestalten, ist die Verwendung eines Zet Casino Promo-Codes. Mit einem Promo-Code können die Spieler tolle Boni und Vergünstigungen erhalten, die ihre Gewinnchancen erhöhen und ihr Casino-Erlebnis verbessern.
Um einen Zet Casino Promo-Code zu erhalten, müssen die Spieler häufig bestimmte Bedingungen erfüllen, wie zum Beispiel eine Mindesteinzahlung tätigen oder an bestimmten Spielen teilnehmen. Sobald der Promo-Code eingelöst wurde, werden die Boni oder Vergünstigungen automatisch dem Spielerkonto gutgeschrieben und können sofort verwendet werden.
Die Verwendung eines Promo-Codes im Zet Casino ist eine großartige Möglichkeit, um das Beste aus Ihrem Spielerlebnis herauszuholen und mehr Spaß beim Spielen zu haben. Die Bonusse und Vergünstigungen, die Sie mit einem Promo-Code erhalten können, können Ihre Gewinnchancen deutlich verbessern und Ihnen helfen, mehr aus Ihrem Glücksspiel-Erlebnis herauszuholen.
Wenn Sie also gerne im Zet Casino spielen und auf der Suche nach einer Möglichkeit sind, Ihr Spielerlebnis aufzupeppen, dann sollten Sie unbedingt nach einem Zet Casino Promo-Code suchen. Nutzen Sie die großzügigen Angebote und verbessern Sie Ihre Gewinnchancen noch heute!
https://zetcasino.one/
Das tipico classico Casino, eine beliebte Online-Glücksspielseite, hat in letzter Zeit mit langen Ladezeiten zu kämpfen. Viele Spieler haben sich beschwert, dass die Spiele langsam geladen werden und es zu Verzögerungen beim Spielen kommt.
Dieses Problem hat zu Frustration bei den Kunden geführt, die sich ein reibungsloses und unterhaltsames Spielerlebnis wünschen. Die Betreiber des Casinos haben angekündigt, dass sie bereits an einer Lösung arbeiten, um die Performance zu verbessern und die Ladezeiten zu verkürzen.
Es ist wichtig, dass Online-Casinos wie das tipico classico Casino stets bemüht sind, ihren Kunden das bestmögliche Spielerlebnis zu bieten. Lange Ladezeiten können dazu führen, dass Spieler das Interesse verlieren und sich nach Alternativen umsehen.
Wir hoffen, dass das tipico classico Casino das Problem bald in den Griff bekommt und seinen Kunden wieder ein reibungsloses und genussvolles Spielerlebnis bieten kann. In der Zwischenzeit sollten Spieler Geduld haben und darauf vertrauen, dass das Casino das Problem schnellstmöglich lösen wird.
https://tipicocasino.one/
Gogo Casino är ett populärt nätcasino som har blivit mycket omtyckt av spelare i Finland. Med sitt stora utbud av spel och generösa bonusar lockar Gogo Casino till sig både erfarna spelare och nybörjare.
När man besöker Gogo Casino möts man av ett modernt och användarvänligt gränssnitt som gör det enkelt att navigera mellan olika spel och kategorier. Här finns allt från klassiska casinospel som blackjack och roulette till moderna videoslots och progressiva jackpottar.
En av fördelarna med att spela på Gogo Casino är att man kan göra snabba och säkra insättningar och uttag med hjälp av populära betalningsmetoder som Visa, Mastercard, Skrill och Neteller. Dessutom erbjuds spelare en kundtjänst som är tillgänglig dygnet runt via livechatt och e-post.
För de som är intresserade av att prova på Gogo Casino finns det också möjlighet att ta del av generösa välkomstbonusar och andra kampanjer som ökar ens vinstchanser och ger en extra spänning till spelandet.
Sammanfattningsvis är Gogo Casino en pålitlig och underhållande spelsajt som erbjuder en förstklassig spelupplevelse för alla som älskar att spela på nätcasino. Med sitt stora utbud av spel, generösa bonusar och smidiga betalningsmetoder är det inte konstigt att Gogo Casino har blivit en favorit bland spelare i Finland.
https://gogocasino.one
Gogo Casino, ett av Sveriges populäraste onlinecasinon, har nyligen ingått ett spännande samarbete med en ledande speltillverkare. Detta samarbete innebär att Gogo Casino kommer att kunna erbjuda sina spelare ännu fler spännande spel att välja mellan.
Speltillverkaren har ett stort utbud av populära spelautomater och bordsspel som är kända för sin höga kvalitet och underhållningsvärde. Genom samarbetet med Gogo Casino kommer dessa spel nu att bli tillgängliga för alla spelare på casinot.
Detta är en spännande utveckling för Gogo Casino och dess spelare. Genom att erbjuda ett ännu bredare utbud av spel hoppas casinot kunna locka nya spelare och samtidigt ge sina befintliga spelare ännu mer underhållning och spänning.
Gogo Casino har redan ett gott rykte för sin säkerhet, användarvänlighet och generösa bonusar och kampanjer. Detta nya samarbete kommer att stärka casinots position som en av de ledande aktörerna på den svenska spelmarknaden.
Så om du är sugen på att prova några nya spännande spelautomater eller bordsspel, är det definitivt värt att kolla in Gogo Casino och ta del av deras nya samarbete. Vem vet, kanske är nästa stora vinst just runt hörnet!
https://gogocasino.one
Reduslim Inhalt ist ein Schlüsselbegriff für alle, die auf der Suche nach einem effektiven Gewichtsverlustprodukt sind. Reduslim ist eine natürliche Nahrungsergänzung, die mit einer einzigartigen Mischung aus Inhaltsstoffen formuliert wurde, um den Stoffwechsel zu steigern und die Fettverbrennung zu fördern.
Die Hauptbestandteile von Reduslim Inhalt sind Grüntee-Extrakt, Garcinia Cambogia, Ingwerwurzel und Koffein. Grüntee-Extrakt ist bekannt für seine antioxidativen Eigenschaften und hilft, den Stoffwechsel anzukurbeln. Garcinia Cambogia ist eine Frucht, die die Fettverbrennung unterstützt und den Appetit unterdrückt. Ingwerwurzel hat entzündungshemmende Eigenschaften und kann dabei helfen, den Verdauungsprozess zu verbessern. Koffein ist ein natürlicher Energiespender und kann helfen, die körperliche Leistungsfähigkeit zu steigern.
Durch die regelmäßige Einnahme von Reduslim können Sie dabei unterstützt werden, Ihr Gewicht zu reduzieren und Ihre Gesundheit zu verbessern. Die Kombination der Inhaltsstoffe sorgt für eine gezielte und effektive Unterstützung beim Abnehmen. Probieren Sie Reduslim Inhalt aus und entdecken Sie die positiven Effekte auf Ihren Körper und Ihre Gesundheit!
https://reduslim.at/
Gogo Casino är ett onlinecasino som erbjuder sina spelare möjligheten att spela utan att behöva göra en insättning. Detta kallas för en no deposit bonus och innebär att spelarna kan prova på casinots spel utan att riskera sina egna pengar.
För att ta del av denna bonus behöver spelaren endast skapa ett konto på Gogo Casino och verifiera sin identitet. Sedan kan man börja spela och utforska det stora utbud av spel som erbjuds på casinot. Det är ett utmärkt sätt för spelare att testa casinot och se om det passar ens individuella spelstil innan man bestämmer sig för att göra en insättning.
No deposit bonusar är särskilt populära bland nya spelare som vill prova på olika casinon innan de bestämmer sig för vilket de vill fortsätta spela på. Det är också ett bra sätt för casinon att locka till sig nya spelare och visa upp sitt spelutbud.
Gogo Casino har ett brett utbud av spelautomater, bordsspel och livecasino-spel att välja mellan. Oavsett om man föredrar klassiska spelautomater, spännande bordsspel som blackjack och roulette eller vill uppleva spänningen i ett livecasino, finns det något för alla på Gogo Casino.
Så om du är sugen på att prova lyckan utan att riskera dina egna pengar, är Gogo Casino no deposit bonus definitivt värt att testa. Skapa ett konto idag och börja spela!
https://gogocasino.one
Gogo Casino är en spännande app för alla som älskar att spela casinospel på mobilen. Med ett brett utbud av spel och generösa bonuserbjudanden är detta en app som lockar många spelare.
Gogo Casino erbjuder ett stort utbud av spelautomater, bordsspel och live casinospel. Oavsett om du föredrar klassiska spelautomater eller mer avancerade videoslots finns det något för alla här. Dessutom kan du njuta av autentiska casinoupplevelser genom att spela live blackjack, roulette eller baccarat.
En av fördelarna med att använda Gogo Casino app är att du kan spela när som helst och var som helst. Du behöver inte längre sitta vid din dator för att kunna spela dina favoritspel, utan du kan ha dem med dig i fickan. Detta gör det enklare för dig att spela och ökar tillgängligheten.
För att öka spänningen och ge dig chansen att vinna stort erbjuder Gogo Casino regelbundna bonuserbjudanden och kampanjer. Du kan få bonusar vid insättningar, free spins eller delta i tävlingar med fina priser. På så sätt kan du få mer valuta för dina pengar och öka dina vinstchanser.
Sammanfattningsvis är Gogo Casino app en bra plattform för alla som älskar att spela casinospel. Med sitt stora spelutbud, generösa bonuserbjudanden och smidiga användarupplevelse är det en app som passar alla typer av spelare. Så ladda ner appen idag och börja spela för att ha chansen att vinna stort!
https://gogocasino.one
Das Boomerang Casino bietet seinen Spielern eine einzigartige MГ¶glichkeit, Geld zurГјck zu erhalten. Mit dem sogenannten “Boomerang Cashback” Programm kГ¶nnen Spieler einen Teil ihrer Verluste zurГјckerhalten.
Das Prinzip ist einfach: Spieler sammeln Punkte, indem sie im Casino spielen. Je mehr Punkte sie sammeln, desto mehr Geld können sie zurückerhalten. Die Rückzahlungen erfolgen in Form von Bonusgeld, das wiederum im Casino eingesetzt werden kann.
Das Boomerang Casino ist eines der wenigen Online-Casinos, das ein solches Cashback-Programm anbietet. Viele Spieler schätzen diese Möglichkeit, da sie so die Chance haben, einen Teil ihrer Verluste wieder gutzumachen.
Um von dem Boomerang Cashback zu profitieren, müssen Spieler lediglich im Casino spielen und Punkte sammeln. Je mehr sie spielen, desto mehr Geld können sie zurückerhalten.
Insgesamt ist das Boomerang Casino Geld Zurück Programm eine attraktive Option für Spieler, die gerne im Online-Casino spielen. Es bietet die Möglichkeit, Verluste zu minimieren und gleichzeitig mehr Spaß beim Spielen zu haben.
https://boomerangcasino.one/
Promo-Code Zet Casino 2023: Sichern Sie sich jetzt tolle Angebote!
Das Zet Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und Promotionen für ihre Spieler anbietet. Mit dem Promo-Code Zet Casino 2023 haben Spieler die Möglichkeit, zusätzliche Boni und Vergünstigungen zu erhalten, um ihr Spielerlebnis noch spannender zu gestalten.
Der Promo-Code Zet Casino 2023 kann bei der Registrierung oder bei der Einzahlung auf das Spielerkonto eingegeben werden. Mit diesem Code können Spieler Zugang zu exklusiven Bonusangeboten erhalten, wie zum Beispiel zusätzliches Spielgeld, Freispiele oder Cashback-Aktionen. Diese Angebote können dazu beitragen, die Gewinnchancen zu erhöhen und das Spielerlebnis noch unterhaltsamer zu gestalten.
Um den Promo-Code Zet Casino 2023 zu nutzen, sollten Spieler regelmäßig die Aktionsseite auf der Website des Casinos besuchen, um über die neuesten Angebote informiert zu bleiben. Außerdem können Spieler den Newsletter abonnieren, um keine Sonderaktionen zu verpassen.
Also, worauf warten Sie noch? Nutzen Sie den Promo-Code Zet Casino 2023 und sichern Sie sich noch heute tolle Angebote und Boni, um Ihr Spielerlebnis auf Zet Casino zu verbessern! Viel SpaГџ und viel GlГјck beim Spielen!
https://zetcasino.one/
Gogo Casino är en populär app för online-spel som erbjuder ett brett utbud av casinospel för alla spelare. Appen har tagit Sverige med storm genom sin användarvänliga design och stora utbud av spelautomater, bordsspel och live dealer-spel.
En av fördelarna med Gogo Casino är att man kan spela var som helst och när som helst genom att helt enkelt ladda ner appen på sin smartphone eller surfplatta. Spelarna kan njuta av sina favoritspel under en paus på jobbet, på bussen eller bara hemma i soffan.
Appen erbjuder också generösa bonusar och kampanjer för sina användare, vilket gör det ännu mer lockande att spela. Spelare kan få free spins, insättningsbonusar och andra belöningar när de spelar på Gogo Casino.
En annan fördel med appen är att den är säker och pålitlig, med säkra betalningsmetoder och krypterade transaktioner för att skydda spelarnas personliga och finansiella information.
Sammanfattningsvis är Gogo Casino en fantastisk app för alla som älskar att spela casinospel. Med sitt stora utbud av spel, generösa bonusar och användarvänliga design är det enkelt att förstå varför den har blivit så populär i Sverige. Så ladda ner appen och börja spela redan idag!
https://gogocasino.one
Reduslim ist ein beliebtes NahrungsergГ¤nzungsmittel, das oft mit der Frage “Reduslim a cosa serve?” konfrontiert wird. Es handelt sich um eine natГјrliche Formel, die zur Gewichtsabnahme und Fettverbrennung beitrГ¤gt. Reduslim hilft, den Stoffwechsel zu erhГ¶hen und den Appetit zu reduzieren, was zu einer effektiven Gewichtsabnahme fГјhrt. Viele zufriedene Kunden berichten von positiven Ergebnissen und einer verbesserten KГ¶rperzusammensetzung nach der Einnahme von Reduslim. Es ist wichtig zu betonen, dass Reduslim kein Wundermittel ist und in Kombination mit einer ausgewogenen ErnГ¤hrung und regelmäßiger Bewegung am effektivsten ist. Wenn Sie also Гјberlegen, Reduslim auszuprobieren, kann es Ihnen helfen, Ihre Gewichtsziele schneller zu erreichen.
https://reduslim.at/
Gogo Casino är ett av de senaste tillskotten på den svenska spelmarknaden. Casinot lanserades år 2020 och har snabbt blivit populärt bland svenska spelare. Men vem ligger egentligen bakom detta framgångsrika casino?
Ägaren till Gogo Casino är det välkända spelbolaget LeoVegas. LeoVegas grundades år 2011 och har sedan dess vuxit och blivit en av de ledande aktörerna inom den digitala spelindustrin. Med flera framgångsrika onlinecasinon under sitt bälte har LeoVegas visat sig vara en pålitlig och innovativ aktör på marknaden.
Gogo Casino ägare, LeoVegas, har satt ett stort fokus på att erbjuda en säker och underhållande spelupplevelse för sina kunder. Genom att erbjuda ett brett utbud av spel från ledande spelutvecklare, enkel och smidig registrering och snabba utbetalningar har Gogo Casino snabbt blivit en favorit bland svenska spelare.
LeoVegas har även satsat på att erbjuda ett ansvarsfullt spelande genom att erbjuda verktyg för spelbegränsning och genom att aktivt arbeta för att förebygga spelproblem. Som ägare till Gogo Casino har LeoVegas en stark drivkraft att skapa en trygg och ansvarsfull spelmiljö för alla sina kunder.
Sammanfattningsvis är Gogo Casino ägare ett väletablerat och pålitligt spelbolag med lång erfarenhet inom branschen. Genom att erbjuda en säker, smidig och underhållande spelupplevelse har Gogo Casino snabbt blivit en favorit bland svenska spelare. Med LeoVegas som ägare kan spelare vara säkra på att de får en högkvalitativ spelupplevelse i en trygg miljö.
https://gogocasino.one
Gogo Casino Г¤r ett populГ¤rt onlinecasino som erbjuder sina spelare en spГ¤nnande och underhГҐllande spelupplevelse. En av de mest attraktiva funktionerna hos Gogo Casino Г¤r mГ¶jligheten att spela utan att behГ¶va gГ¶ra en insГ¤ttning, Г¤ven kГ¤nd som “no deposit”. Det hГ¤r Г¤r en fantastisk mГ¶jlighet fГ¶r spelare att prova pГҐ olika spel och uppleva spГ¤nningen av att spela pГҐ ett casino utan att behГ¶va riskera sina egna pengar.
Att spela på Gogo Casino utan att behöva göra en insättning är enkelt. När du registrerar dig på casinot kommer du att belönas med en no deposit bonus som du kan använda för att prova på olika spel på sajten. Denna bonus ger dig chansen att vinna riktiga pengar utan att behöva sätta in några egna medel. Det är en perfekt möjlighet för spelare att utforska olika spel och upptäcka vilka spel de gillar bäst.
För att ta del av no deposit bonusen på Gogo Casino är det viktigt att läsa igenom reglerna och villkoren för erbjudandet. Ofta finns det krav på omsättning och maxvinster som måste uppfyllas innan du kan ta ut dina vinster. Det är också viktigt att komma ihåg att no deposit bonusar oftast har ett begränsat giltighetsdatum, så se till att utnyttja erbjudandet innan det går ut.
Gogo Casino erbjuder ett brett utbud av spel frГҐn ledande spelleverantГ¶rer som NetEnt, Microgaming och Play’n GO. Med hundratals spel att vГ¤lja mellan finns det garanterat nГҐgot fГ¶r alla spelare, oavsett om du fГ¶redrar klassiska spelautomater, bordsspel eller livecasino.
Om du är sugen på att prova på spänningen av att spela på ett onlinecasino utan att riskera dina egna pengar, är Gogo Casino det perfekta stället att göra det. Med sin generösa no deposit bonus och imponerande spelutbud är det enkelt att se varför detta casino har blivit så omtyckt av spelare runt om i Sverige. Så varför inte ta chansen och prova lyckan på Gogo Casino idag? Lycka till!
https://gogocasino.one
Gogo casino app är den senaste trenden inom online-spelvärlden som tar underhållningen till en helt ny nivå. Med denna innovativa app kan spelarna njuta av sina favoritspel var som helst och när som helst, oavsett om de är hemma, på bussen eller till och med på stranden.
Appen erbjuder ett brett utbud av spelalternativ, inklusive slots, bordsspel och live-casino. Spelarna kan också ta del av olika kampanjer och erbjudanden som gör det ännu roligare att spela.
En av fördelarna med att använda gogo casino app är att spelarna kan få tillgång till sina favoritspel med en enda knapptryckning. Det innebär att de inte längre behöver sitta vid datorn för att spela, vilket ger en helt ny flexibilitet och frihet.
En annan fördel är att appen är utformad för att vara både intuitiv och användarvänlig. Spelarna kan enkelt navigera mellan olika spel och hitta det de söker utan några problem.
Med gogo casino app kan spelarna också njuta av en säker och trygg spelupplevelse. Appen använder den senaste krypteringstekniken för att skydda spelarnas personliga och finansiella uppgifter, vilket ger dem en trygghet när de spelar.
Sammanfattningsvis är gogo casino app en innovativ och spännande plattform som tar spelupplevelsen till en helt ny nivå. Med sitt stora utbud av spel, användarvänlighet och säkerhet är det en perfekt följeslagare för alla spelentusiaster därute. Så varför inte ge den en chans och se vad den har att erbjuda? Lycka till och ha roligt!
https://gogocasino.one
Gogo Casino är ett onlinecasino som erbjuder spännande spelupplevelser för alla spelare. Ett av de mest populära erbjudandena som Gogo Casino har är deras no deposit bonus.
En no deposit bonus innebär att spelare kan få gratis bonuspengar utan att behöva göra en insättning. Detta är en fantastisk möjlighet för spelare att testa på casinots spelutbud utan att riskera sina egna pengar.
För att få en no deposit bonus hos Gogo Casino behöver spelare bara registrera sig på casinot och skapa ett konto. Därefter kommer bonuspengarna att krediteras till spelarens konto och de kan börja spela.
Det finns olika villkor som gäller för no deposit bonusen på Gogo Casino, så det är viktigt att läsa och förstå dessa villkor innan man tar del av erbjudandet. Ofta måste spelare uppfylla omsättningskrav innan de kan ta ut sina vinster från bonusen.
Gogo Casino är känt för att erbjuda generösa bonusar och kampanjer för sina spelare, och no deposit bonusen är bara ett exempel på detta. Med en stor variation av spel att välja mellan, från slots till bordsspel och live casino, finns det något för alla på Gogo Casino.
Sammanfattningsvis är Gogo Casino no deposit bonus en fantastisk möjlighet för spelare att utforska casinots spelutbud utan att riskera sina egna pengar. Med generösa bonusar och ett stort urval av spel är Gogo Casino definitivt värt att prova på för alla casinofantaster.
https://gogocasino.one
Boomerang Casino – der Ort, an dem das GlГјck immer wieder zurГјckkommt! Mit dem exklusiven Kod Promocyjny Boomerang Casino kГ¶nnen Spieler in eine aufregende Welt voller SpaГџ und GewinnmГ¶glichkeiten eintauchen.
Das Kod Promocyjny Boomerang Casino bietet Spielern die Möglichkeit, von erstaunlichen Bonusangeboten zu profitieren, die ihre Gewinnchancen erhöhen. Mit diesem speziellen Code können Spieler zusätzliche Bonusgelder, Freispiele und andere aufregende Belohnungen erhalten, die das Spielerlebnis noch spannender machen.
DarГјber hinaus bietet Boomerang Casino eine Vielzahl von Spieloptionen, darunter beliebte Slots, Tischspiele und Live-Casino-Spiele. Mit hochwertiger Grafik und einem reibungslosen Spielerlebnis ist Boomerang Casino der perfekte Ort fГјr alle, die nach einem erstklassigen Online-Casino-Erlebnis suchen.
Spieler, die den Kod Promocyjny Boomerang Casino nutzen, können sicher sein, dass sie von einem engagierten Kundensupport-Team unterstützt werden, das ihnen bei allen Fragen oder Problemen behilflich ist. Mit schnellen Auszahlungen und einer benutzerfreundlichen Oberfläche bietet Boomerang Casino alles, was Spieler für ein erstklassiges Casino-Erlebnis benötigen.
Nutzen Sie noch heute den Kod Promocyjny Boomerang Casino und erleben Sie die aufregende Welt des Online-Glücksspiels auf höchstem Niveau! Besuchen Sie die Website von Boomerang Casino und erleben Sie die Spannung und den Nervenkitzel, den dieses erstklassige Casino zu bieten hat.
https://boomerangcasino.one/
Zet Casino Anmeldung
Zet Casino ist ein Online-Casino, das zahlreiche Spiele und attraktive Bonusangebote für seine Spieler bietet. Um die Spiele im Casino zu genießen und von den Bonusaktionen zu profitieren, müssen Sie sich zunächst auf der Webseite des Casinos anmelden.
Die Anmeldung bei Zet Casino ist ganz einfach und unkompliziert. Klicken Sie einfach auf den Button “Registrieren” und fГјllen Sie das Anmeldeformular mit Ihren persГ¶nlichen Daten aus. Dazu gehГ¶ren unter anderem Ihr Name, Ihre E-Mail-Adresse, Ihre Wohnadresse und Ihr Geburtsdatum.
Nachdem Sie das Anmeldeformular ausgefüllt haben, müssen Sie Ihre E-Mail-Adresse bestätigen, indem Sie auf den Link klicken, den Ihnen das Casino per E-Mail zusendet. Sobald Ihre E-Mail-Adresse bestätigt ist, können Sie sich mit Ihrem Benutzernamen und Ihrem Passwort auf der Webseite von Zet Casino einloggen.
Nach der Anmeldung können Sie die Vielzahl an Spielen im Casino erkunden und Ihr Glück versuchen. Zet Casino bietet eine große Auswahl an Spielautomaten, Tischspielen und Live-Dealer-Spielen von renommierten Softwareanbietern wie NetEnt, Microgaming und Evolution Gaming.
Darüber hinaus können Sie sich über regelmäßige Bonusaktionen und Promotionen freuen, die Ihnen zusätzliches Guthaben, Freispiele oder andere attraktive Preise bescheren. Schauen Sie regelmäßig auf der Webseite von Zet Casino vorbei, um keine der lukrativen Angebote zu verpassen.
Insgesamt bietet Zet Casino eine unterhaltsame und hochwertige Spielerfahrung fГјr alle, die gerne online spielen. Melden Sie sich noch heute an und tauchen Sie ein in die faszinierende Welt der Online-Casinospielen bei Zet Casino. Viel GlГјck!
https://zetcasino.one/
Gogo Casino är en spelsajt som erbjuder ett brett utbud av casinospel online. För de som vill komma i kontakt med kundtjänsten för att få svar på sina frågor eller för att lösa eventuella problem, finns det flera olika sätt att göra detta.
Det enklaste sättet att komma i kontakt med Gogo Casino är att använda deras livechattfunktion. Denna finns tillgänglig direkt på hemsidan och ger spelare möjligheten att prata med en representant i realtid. Genom att använda livechatten kan man snabbt få svar på sina frågor utan att behöva vänta på ett svar via e-post.
För de som föredrar att skicka e-post finns det även möjlighet att kontakta Gogo Casino via deras e-postadress. Det kan vara en bra idé att skicka ett e-postmeddelande om man har en mer komplicerad fråga som behöver mer detaljerad information.
Ytterligare ett sätt att komma i kontakt med Gogo Casino är via deras telefonnummer. Genom att ringa till kundtjänsten kan man diskutera eventuella problem eller frågor direkt med en representant.
Oavsett vilket sГ¤tt man vГ¤ljer att kontakta Gogo Casino pГҐ, Г¤r det viktigt att man kГ¤nner sig trygg och vГ¤lkommen som spelare. KundtjГ¤nsten pГҐ Gogo Casino strГ¤var efter att ge spelare den bГ¤sta mГ¶jliga upplevelsen och Г¤r alltid redo att hjГ¤lpa till med eventuella frГҐgor eller problem som kan uppstГҐ. SГҐ tveka inte att ta kontakt om du behГ¶ver hjГ¤lp – Gogo Casino finns hГ¤r fГ¶r dig.
https://gogocasino.one
Wer hat Erfahrung mit Reduslim gemacht und kann davon berichten? Reduslim ist ein beliebtes Nahrungsergänzungsmittel, das bei der Gewichtsabnahme unterstützen soll. Viele Menschen schwärmen von den positiven Ergebnissen, die sie nach der Einnahme von Reduslim erlebt haben. Doch wie viel Wahrheit steckt hinter den Versprechen des Herstellers?
Einige Nutzer berichten, dass sie mit Reduslim tatsächlich erfolgreich abgenommen haben und sich fitter und gesünder fühlen. Sie loben die natürlichen Inhaltsstoffe und die einfache Anwendung des Präparats. Andere hingegen sind skeptisch und zweifeln an der Wirksamkeit von Reduslim. Sie bemängeln fehlende Langzeitergebnisse und warnen vor möglichen Nebenwirkungen.
Es ist wichtig, dass man sich gründlich über die Eigenheiten eines Produktes informiert, bevor man es ausprobiert. Wer Erfahrung mit Reduslim gemacht hat, sollte seine Erkenntnisse mit anderen teilen, um eine fundierte Entscheidungshilfe zu bieten. Letztendlich ist es wichtig, dass man auf seinen eigenen Körper hört und nur Produkte verwendet, von denen man wirklich überzeugt ist.
https://reduslim.at/
Отечественный изготовитель реализует оборудование для фитнеса https://oborudovanie-dlya-fitnesa.ru/ по приятным ценам, без лишних наценок. Всегда в продажеобъемный каталог для постоянных покупателей. Предоставляем качественные устройства и аксессуары, которые помогут вам улучшить ваше здоровье и физическую форму.
В создании мягких участков используется эластичный кожзам. Ключевые элементы конструкции изготовлены из высокопрочных видов стали. Качественные и функциональные снаряды дают возможность эффективно заниматься фитнесом как дома, так и тренировочном зале. Производимое оборудование отличается выдающимся качеством и надежностью, что позволяет вам тренироваться продуктивно и удобно. Для домашнего тренинга будут востребованы петли TRX, цельные гантельки, эластичные ленты, штанги, глайдинг диски, массажные ролы, платформы Bosu, резинки, медболы.
“Gogo Casino – Ingen InsГ¤ttning KrГ¤vs”
Gogo Casino är ett populärt online casino som erbjuder spelare en spännande spelupplevelse utan att behöva göra en insättning. Med ett brett utbud av spel, generösa bonusar och en användarvänlig plattform, är det inte konstigt att många spelare väljer att spela på Gogo Casino utan att behöva sätta in sina egna pengar.
FГ¶r de som Г¤r nya pГҐ Gogo Casino och vill prova pГҐ spelen utan att riskera sina egna pengar, erbjuder casinot en “no deposit” bonus. Det innebГ¤r att spelare fГҐr en viss summa pengar att spela fГ¶r nГ¤r de registrerar sig, utan att behГ¶va gГ¶ra en insГ¤ttning. Detta ger spelare mГ¶jligheten att utforska olika spel och se vad Gogo Casino har att erbjuda innan de bestГ¤mmer sig fГ¶r att sГ¤tta in sina egna pengar.
En annan fördel med att spela på Gogo Casino utan insättning är att spelare kan testa sin skicklighet och strategi utan att behöva riskera sina egna pengar. Det ger en trygg och rolig spelupplevelse där spelare kan lära sig reglerna och förbättra sina färdigheter innan de bestämmer sig för att spela med riktiga pengar.
För spelare som söker spänning och underhållning utan att behöva göra en insättning, är Gogo Casino det perfekta valet. Med sitt stora utbud av spel och generösa bonusar erbjuder casinot en unik spelupplevelse som passar alla typer av spelare. Så varför inte testa lyckan och spela på Gogo Casino utan att behöva sätta in några egna pengar? Vem vet, kanske är det just du som tar hem den stora vinsten!
https://gogocasino.one
Gogo Casino är ett populärt online casino som har blivit känt för sina generösa välkomstbonusar. När du registrerar dig som ny spelare på Gogo Casino kan du se fram emot en riktigt förmånlig välkomstbonus som ger dig extra spelkrediter att använda på deras breda utbud av casinospel.
Välkomstbonusen på Gogo Casino kan variera och kan inkludera en insättningsbonus, free spins eller andra förmånliga erbjudanden. Det bästa sättet att ta reda på vilken välkomstbonus som just nu erbjuds på Gogo Casino är att besöka deras hemsida och registrera dig som spelare.
För att ta del av en välkomstbonus på Gogo Casino behöver du oftast göra en insättning på ditt spelkonto. Du kan sedan använda bonusen för att spela på deras casinospel och öka dina vinstchanser.
Det är viktigt att läsa igenom regler och villkor för välkomstbonusen innan du accepterar den för att vara säker på att du förstår vilka krav som gäller för att kunna utnyttja bonusen på bästa sätt.
Sammanfattningsvis är Gogo Casino ett bra val för dig som letar efter en generös välkomstbonus och ett stort utbud av casinospel. Besök deras hemsida idag för att ta reda på vilken välkomstbonus som erbjuds just nu och kom igång med spelandet redan idag!
https://gogocasino.one
Gogo Casino support
Gogo Casino är en populär online spelplattform som erbjuder spelare en spännande och underhållande spelupplevelse. För att säkerställa att spelarna har en smidig och problemfri spelupplevelse erbjuder Gogo Casino en kundsupporttjänst som är tillgänglig för att hjälpa spelare i alla sina behov.
Kundsupportteamet på Gogo Casino är välutbildat och erfaret inom spelindustrin. De är tillgängliga 24/7 för att assistera spelare med eventuella frågor eller problem de kan ha. Spelare kan kontakta kundsupport via livechatt, e-post eller telefon för att få omedelbar hjälp.
Kundsupportteamet på Gogo Casino är också känd för sin vänlighet och professionalism. De strävar alltid efter att ge spelarna den bästa möjliga servicen och att lösa eventuella problem så snabbt och effektivt som möjligt.
Förutom att erbjuda kundsupport i form av hjälp med frågor eller problem, kan spelare också kontakta kundsupport för att få information om bonusar, kampanjer och andra erbjudanden som kan vara tillgängliga på plattformen.
Sammanfattningsvis är kundsupporten på Gogo Casino tillgänglig dygnet runt för att hjälpa spelarna med alla sina behov. Med sitt vänliga och professionella team kan spelare lita på att de får den bästa möjliga servicen när de spelar på Gogo Casino.
https://gogocasino.one
Das Boomerang Casino Forum: Ein Ort fГјr GlГјcksspiel-Enthusiasten
Das Boomerang Casino Forum ist ein beliebter Treffpunkt für Glücksspiel-Enthusiasten, die sich über ihre Leidenschaft austauschen und neue Online-Casinos entdecken möchten. Das Forum bietet eine Vielzahl von Themen und Diskussionen rund um das Thema Glücksspiel, darunter Erfahrungsberichte, Tipps und Tricks, Neuigkeiten aus der Branche und vieles mehr.
Ein besonderer Fokus des Boomerang Casino Forums liegt auf dem Austausch über Online-Casinos und deren Spiele. Mitglieder können ihre Erfahrungen teilen, sich gegenseitig empfehlen oder warnen und sich über die neuesten Entwicklungen informieren. Darüber hinaus gibt es auch spezielle Bereiche für Strategie-Diskussionen, Bonusangebote und Turniere.
Ein weiterer Vorteil des Boomerang Casino Forums ist die Möglichkeit, sich mit Gleichgesinnten zu vernetzen und Freundschaften zu schließen. Viele Mitglieder treffen sich regelmäßig in virtuellen Casinos, um gemeinsam zu spielen und sich auszutauschen. Dadurch entsteht eine lebendige Community, die sich gegenseitig unterstützt und motiviert.
Das Boomerang Casino Forum ist für alle offen, die sich für Glücksspiel interessieren, unabhängig von ihrem Erfahrungsgrad. Sowohl Anfänger als auch erfahrene Spieler finden hier wertvolle Informationen und Unterstützung. Das Forum wird von engagierten Moderatoren betreut, die sicherstellen, dass die Diskussionen respektvoll und konstruktiv verlaufen.
Insgesamt bietet das Boomerang Casino Forum eine einzigartige Gelegenheit, sich mit anderen GlГјcksspiel-Fans auszutauschen und gemeinsam die faszinierende Welt der Online-Casinos zu erkunden. Wer auf der Suche nach einer lebendigen und hilfsbereiten Community ist, sollte einen Blick in das Boomerang Casino Forum werfen und sich selbst davon Гјberzeugen.
https://boomerangcasino.one/
Reduslim ist ein beliebtes Diätprodukt, das zur Gewichtsabnahme entwickelt wurde. Der Hersteller von Reduslim Original garantiert hochwertige Inhaltsstoffe und eine effektive Wirkung. Viele Menschen schwören auf die Wirksamkeit dieses Produkts, das auf natürlichen Zutaten basiert. Der Hersteller legt großen Wert auf Transparenz und Qualität, um die besten Ergebnisse zu erzielen. Wer also nach einer effektiven Methode sucht, um Gewicht zu verlieren, sollte Reduslim Original vom Hersteller in Betracht ziehen.
https://reduslim.at/
Zet Casino ist ein beliebtes Online-Casino, das seinen Spielern eine Vielzahl von SpielmГ¶glichkeiten bietet, darunter auch die MГ¶glichkeit, kostenlos Spins zu erhalten. Diese sogenannten “darmowe spiny” sind eine groГџartige MГ¶glichkeit, um neue Spiele auszuprobieren und dabei echtes Geld zu gewinnen.
Ein Spin ist ein Dreh an einem Spielautomaten, der die Möglichkeit bietet, Gewinne zu erzielen. In Zet Casino können Spieler durch verschiedene Aktionen wie Einzahlungen, Turniere oder spezielle Angebote diese kostenlosen Spins erhalten. So haben sie die Möglichkeit, ihr Glück zu versuchen, ohne dabei eigenes Geld riskieren zu müssen.
Die darmowe spiny im Zet Casino sind eine tolle Möglichkeit, um die riesige Auswahl an Spielen zu erkunden. Von klassischen Spielautomaten bis hin zu modernen Videoslots ist für jeden Geschmack etwas dabei. Spieler können so neue Lieblingsspiele entdecken und dabei auch noch echtes Geld gewinnen.
Um an diesen kostenlosen Spins teilzunehmen, müssen Spieler lediglich die Bedingungen der jeweiligen Aktion erfüllen. Diese können ein Mindesteinzahlungsbetrag, eine bestimmte Anzahl an Spielen oder eine zeitliche Beschränkung beinhalten. Es lohnt sich jedoch, diese Aktionen im Auge zu behalten, da sie regelmäßig aktualisiert und erweitert werden.
Zet Casino bietet seinen Spielern nicht nur eine fantastische Auswahl an Spielen, sondern auch die Möglichkeit, mit darmowe spiny echtes Geld zu gewinnen. Diese kostenlosen Spins sind eine großartige Möglichkeit, um die verschiedenen Spiele zu erkunden und dabei auch noch Spaß zu haben. Wer also auf der Suche nach einem unterhaltsamen Online-Casino-Erlebnis ist, sollte sich Zet Casino genauer ansehen. Viel Glück beim Spielen!
https://zetcasino.one/
Завод из России реализует спортивные тренажеры https://sportivnyj-trenazher.ru/ для напряженной работы в коммерческих условиях. В каталоге вы выберете самые лучшие варианты станков – грузоблочных и нагружаемых. Значительный ассортимент позволяет выбрать устройства для направленной прокачки практически любых мышечных групп. Оформите Кроссовер для перекрестной тяги, Баттерфляй для грудных, станок Смита, вертикальную тягу, парту Скотта, тренажер для плечей, жим ногами, Пресс машину 3 в 1, Гравитрон для подтягивания и отжиманий, гиперэкстензию, атлетические скамьи, горизонтальную лавку, Хаммер. Производимое оборудование не требует регулярного технического наблюдения. Можете выбрать весовой блок необходимого веса.
Tipico Casino ist ein beliebtes Online-Casino, das eine Vielzahl von spannenden Spielen fГјr seine Spieler anbietet. Eine der beliebtesten Spiele im Tipico Casino ist das Roulette. Roulette ist ein klassisches Casinospiel, das seit Jahrhunderten die Spieler auf der ganzen Welt fasziniert.
Im Tipico Casino gibt es verschiedene Arten von Roulette-Spielen, darunter das traditionelle europäische Roulette, das amerikanische Roulette und das französische Roulette. Jedes Spiel hat seine eigenen Regeln und Besonderheiten, die es zu entdecken gilt.
Das Roulette im Tipico Casino zeichnet sich durch seine hohe Qualität und realistische Grafiken aus. Die Spieler werden in eine authentische Casino-Atmosphäre versetzt und können sich wie in einem echten Casino fühlen. Mit verschiedenen Einsatzmöglichkeiten und Strategien können die Spieler ihr Glück und ihre Fähigkeiten beim Roulette unter Beweis stellen.
Ein weiterer Vorteil des Roulette im Tipico Casino ist die Möglichkeit, es sowohl im Echtgeld- als auch im Demomodus zu spielen. So können die Spieler das Spiel zunächst kennenlernen und ausprobieren, bevor sie echtes Geld einsetzen. Zudem bietet das Tipico Casino attraktive Bonusangebote und Promotionen für Roulette-Spieler an, die ihre Gewinnchancen erhöhen können.
Insgesamt ist das Roulette im Tipico Casino eine unterhaltsame und spannende Möglichkeit, sein Glück zu versuchen und gleichzeitig die Atmosphäre eines echten Casinos zu genießen. Mit einer Vielzahl von Spielen und Einsatzmöglichkeiten ist für jeden Spieler etwas dabei. Probieren Sie es aus und erleben Sie die Faszination des Roulette im Tipico Casino!
https://tipicocasino.one/
Zet Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und Promotions für ihre Spieler anbietet. Ein besonders attraktives Angebot für neue Spieler ist der Zet Casino Kod Promocyjny, mit dem man zusätzliche Boni und Vorteile erhalten kann.
Um den Zet Casino Kod Promocyjny zu nutzen, müssen Spieler lediglich während der Registrierung den entsprechenden Code eingeben. Sobald dies geschehen ist, können sie von verschiedenen Bonusangeboten profitieren, darunter Willkommensbonusse, Freispiele, Cashback-Angebote und vieles mehr.
Der Kod Promocyjny ist eine großartige Möglichkeit, um das Spielerlebnis bei Zet Casino zu maximieren und mehr aus seinen Einsätzen herauszuholen. Mit zusätzlichen Boni und Vorteilen haben Spieler die Möglichkeit, länger zu spielen und ihre Gewinnchancen zu erhöhen.
Zet Casino ist bekannt fГјr seine sicheren und fairen Spielbedingungen, sowie fГјr seinen erstklassigen Kundenservice. Mit einer Vielzahl von Spielen von fГјhrenden Anbietern wie NetEnt, Microgaming und Play’n GO bietet Zet Casino ein umfangreiches Spielerlebnis fГјr alle Arten von Spielern.
Insgesamt ist der Zet Casino Kod Promocyjny eine großartige Möglichkeit, um das Beste aus dem Online-Glücksspiel herauszuholen und zusätzliche Boni und Vorteile zu erhalten. Wenn Sie also auf der Suche nach einer unterhaltsamen und lohnenden Spielerfahrung sind, sollten Sie unbedingt den Zet Casino Kod Promocyjny ausprobieren. Viel Glück beim Spielen!
https://zetcasino.one/
Das Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Casino-Spielen anbietet, darunter Spielautomaten, Tischspiele, Live-Casino und mehr. Um sicherzustellen, dass Spieler ein sicheres und faires Spielerlebnis haben, verlangt das Boomerang Casino bestimmte Dokumente zur Überprüfung der Identität und Adresse der Spieler. In diesem Artikel werden die verschiedenen Arten von Dokumenten erläutert, die das Boomerang Casino zur Überprüfung benötigt.
Zu den gängigsten Dokumenten, die das Boomerang Casino von Spielern verlangt, gehören:
1. Personalausweis oder Reisepass: Dieses Dokument wird benötigt, um die Identität des Spielers zu überprüfen. Es muss ein gültiger Lichtbildausweis sein, der den Namen, das Geburtsdatum, die Ausstellungs- und Ablaufdatum sowie das Foto des Spielers zeigt.
2. Adressnachweis: Um sicherzustellen, dass die Spieler tatsächlich an der angegebenen Adresse wohnen, verlangt das Boomerang Casino eine Kopie eines offiziellen Dokuments wie einer Stromrechnung, eines Kontoauszugs oder einer Mietvereinbarung, die den Namen und die Adresse des Spielers enthalten.
3. Zahlungsnachweis: Spieler müssen auch einen Zahlungsnachweis vorlegen, um sicherzustellen, dass die auf der Plattform verwendeten Zahlungsmethoden tatsächlich dem Spieler gehören.
Es ist wichtig, dass Spieler diese Dokumente so schnell wie möglich bereitstellen, damit sie ihr Konto überprüfen und Ein- und Auszahlungen tätigen können. Die Überprüfung dieser Dokumente ist auch ein wichtiger Schritt, um sicherzustellen, dass nur volljährige Spieler Zugang zum Boomerang Casino haben.
Zusammenfassend lässt sich sagen, dass die Überprüfung der Identität und Adresse der Spieler im Boomerang Casino dazu dient, die Sicherheit und Integrität der Plattform zu gewährleisten. Indem Spieler die erforderlichen Dokumente bereitstellen, können sie sicherstellen, dass ihr Spielerlebnis reibungslos und problemlos verläuft.
https://boomerangcasino.one/
https://slitmastershop.ru/kley/uvkley/
Zet Casino Promo Code 2020: Holen Sie sich die besten Angebote
Wenn Sie ein Fan von Online-Casinospielen sind, dann sollten Sie unbedingt einen Blick auf Zet Casino werfen. Das Casino bietet eine Vielzahl von Spielen, großzügige Bonusangebote und spannende Aktionen für seine Spieler. Mit dem Zet Casino Promo Code 2020 können Sie noch mehr von den tollen Angeboten profitieren.
Der Promo Code für das Jahr 2020 bietet Spielern die Möglichkeit, zusätzliche Boni, Freispiele und andere aufregende Belohnungen zu erhalten. Egal, ob Sie ein erfahrener Spieler sind oder gerade erst anfangen, mit dem Promo Code können Sie Ihr Spielerlebnis bei Zet Casino auf ein neues Level bringen.
Um den Promo Code einzulösen, müssen Sie einfach während der Anmeldung den Code eingeben oder im Kassenbereich des Casinos angeben. Sobald der Code akzeptiert wurde, werden die zusätzlichen Belohnungen Ihrem Konto gutgeschrieben und Sie können sofort mit dem Spielen beginnen.
Zet Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit dem Promo Code können Sie diese Spiele mit zusätzlichem Guthaben oder Freispielen spielen, was Ihre Gewinnchancen erhöht und Ihr Spielerlebnis noch spannender macht.
Also verpassen Sie nicht die Chance, den Zet Casino Promo Code 2020 zu nutzen und sich die besten Angebote des Jahres zu sichern. Melden Sie sich noch heute an und erleben Sie den Nervenkitzel von Online-Casinospielen bei Zet Casino. Viel GlГјck!
https://zetcasino.one/
Tipico ist eine beliebte Plattform für Sportwetten und Online-Casino-Spiele, die es den Nutzern ermöglicht, ihr Glück in verschiedenen Bereichen zu versuchen. Oftmals haben Spieler Guthaben auf ihrem Tipico-Konto, das sie gerne für Casino-Spiele verwenden möchten. Doch wie kann man Guthaben von Tipico auf das Casino umbuchen?
Zunächst einmal ist es wichtig zu wissen, dass Tipico ein integriertes Guthaben für alle Bereiche des Portals hat. Das bedeutet, dass das Guthaben sowohl für Sportwetten als auch für Casino-Spiele genutzt werden kann. Es ist also nicht nötig, das Guthaben speziell für das Casino umzubuchen.
Um das Guthaben beim Tipico Casino einzusetzen, muss man einfach auf den Casino-Bereich der Webseite oder der App gehen und dort die gewünschten Spiele auswählen. Beim Platzieren von Einsätzen wird das Guthaben automatisch vom Gesamtbetrag abgezogen. Es ist also ein nahtloser Übergang zwischen Sportwetten und Casino-Spielen möglich.
Falls dennoch Fragen zum Thema Guthaben oder Umschreibung bestehen, steht der Kundenservice von Tipico gerne zur Verfügung. Dort können alle offenen Fragen geklärt werden und die Mitarbeiter helfen bei der weiteren Vorgehensweise.
Insgesamt ist es also sehr einfach, Guthaben bei Tipico für Casino-Spiele zu nutzen, da das Guthaben für alle Bereiche des Portals gilt. Spieler können so flexibel zwischen Sportwetten und Casino-Spielen wechseln und ihr Glück auf vielfältige Weise versuchen. Tipico bietet somit eine umfassende Unterhaltungsmöglichkeit für alle, die gerne spielen und wetten.
https://tipicocasino.one/
Bewertung Zet Casino
Das Zet Casino ist ein Online-Casino, das von vielen Spielern aufgrund seiner großen Auswahl an Spielen und großzügigen Boni sehr geschätzt wird. In diesem Artikel werfen wir einen genaueren Blick auf das Zet Casino und geben eine Bewertung ab.
Das Zet Casino bietet eine Vielzahl von Spielen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming und Play’n GO. Die Spieler kГ¶nnen aus einer Vielzahl von Spielautomaten, Tischspielen, Live-Casino-Spielen und Jackpot-Slots wГ¤hlen. Die Spiele sind von hoher QualitГ¤t und bieten ein unterhaltsames und spannendes Spielerlebnis.
Neben der großen Spieleauswahl bietet das Zet Casino auch großzügige Boni und Aktionen. Neue Spieler können einen Willkommensbonus auf ihre ersten Einzahlungen erhalten, der ihnen zusätzliches Guthaben zum Spielen bietet. Darüber hinaus gibt es regelmäßig Turniere, Verlosungen und andere Aktionen, bei denen die Spieler tolle Preise gewinnen können.
Die Benutzerfreundlichkeit der Webseite ist ebenfalls lobenswert. Die Seite ist übersichtlich gestaltet und leicht zu navigieren, so dass die Spieler schnell und einfach ihre Lieblingsspiele finden können. Das Zet Casino bietet auch eine mobile App für Spieler, die auch unterwegs spielen möchten.
Insgesamt lässt sich sagen, dass das Zet Casino eine gute Wahl für Spieler ist, die nach einer großen Auswahl an Spielen, großzügigen Boni und einer benutzerfreundlichen Webseite suchen. Die Spiele sind von hoher Qualität und bieten ein unterhaltsames Spielerlebnis. Wir geben dem Zet Casino eine positive Bewertung und empfehlen es gerne weiter.
https://zetcasino.one/
Boomerang Casino: Desktop Version
Boomerang Casino is a popular online casino that offers a wide range of games and promotions for its players. While many people enjoy playing on their mobile devices, the desktop version of the casino also offers a great gaming experience for those who prefer to play on a larger screen.
The desktop version of Boomerang Casino is easy to navigate and user-friendly. Players can easily access their favorite games, make deposits and withdrawals, and take advantage of promotions and bonuses. The casino offers a wide selection of games, including slots, table games, and live dealer games, so players are sure to find something they enjoy.
One of the benefits of playing on the desktop version of Boomerang Casino is the ability to take advantage of the larger screen size. This allows players to see more of the game at once and to have a more immersive gaming experience. Additionally, the desktop version often features better graphics and sound quality, making the games even more enjoyable.
Another advantage of playing on the desktop version of Boomerang Casino is the ability to multitask. Players can easily switch between games, check their account balance, and chat with customer support without having to switch between multiple apps or tabs on their mobile device.
Overall, the desktop version of Boomerang Casino offers a convenient and enjoyable gaming experience for players who prefer to play on their computers. With a wide selection of games, easy navigation, and great graphics and sound quality, players are sure to have a great time playing at this online casino.
https://boomerangcasino.one/
Zet Casino: 20 Freispiele – Welches Spiel?
Wer gerne in Online Casinos spielt, dem dürfte Zet Casino sicherlich ein Begriff sein. Das Casino lockt mit einer Vielzahl an Spielen, großzügigen Boni und spannenden Aktionen. Eine besonders interessante Aktion für Neukunden sind die 20 Free Spins, die man bei der Registrierung erhält.
Doch auf welches Spiel kann man diese 20 Freispiele eigentlich einsetzen? Die Antwort ist ganz einfach: Die Free Spins kГ¶nnen bei dem beliebten Slotspiel “Book of Dead” von Play’n GO verwendet werden. Dieses Spiel ist bei vielen Spielern sehr beliebt und bietet spannende Features und hohe Gewinnchancen.
“Book of Dead” entfГјhrt die Spieler in die Welt des alten Г„gypten und lГ¤sst sie auf Schatzsuche gehen. Das Spiel Гјberzeugt durch eine tolle Grafik, ein spannendes Gameplay und lukrative Bonusrunden. Mit den 20 Free Spins, die man bei Zet Casino erhГ¤lt, hat man die MГ¶glichkeit, das Spiel ganz ohne Risiko auszuprobieren und dabei auch noch echte Gewinne abzurГ¤umen.
Wer also auf der Suche nach einem neuen und aufregenden Slotspiel ist, sollte die 20 Free Spins bei Zet Casino nutzen und sich auf die Schatzsuche bei “Book of Dead” begeben. Vielleicht wartet ja auch fГјr Sie der ganz groГџe Gewinn!
https://zetcasino.one/
Tipico ist einer der führenden Anbieter von Online-Casinospielen, der es Spielern ermöglicht, mit einem Euro Einsätze zu platzieren. Dieser niedrige Mindesteinsatz ermöglicht es auch unerfahrenen Spielern, sich mit dem Online-Casino vertraut zu machen, ohne größere Risiken eingehen zu müssen.
Das Tipico Casino bietet eine Vielzahl von Spielen an, darunter Slots, Tischspiele und Live-Casino-Spiele, die alle mit einem Euro Einsatz gespielt werden können. Dies ermöglicht es Spielern, Spaß zu haben und gleichzeitig die Chance zu haben, echtes Geld zu gewinnen.
Mit einem Euro Einsatz können Spieler an den verschiedenen Slots spielen, die im Tipico Casino verfügbar sind. Slots sind einfache Spiele, die auf Glück basieren und es Spielern ermöglichen, in kurzer Zeit große Gewinne zu erzielen. Darüber hinaus bietet das Tipico Casino eine Vielzahl von Tischspielen wie Blackjack, Roulette und Baccarat an, die ebenfalls mit einem Euro Einsatz gespielt werden können.
Für Spieler, die das authentische Casino-Erlebnis bevorzugen, bietet das Tipico Casino auch Live-Casino-Spiele an, bei denen echte Dealer die Spiele leiten. Auch diese Spiele können mit einem Euro Einsatz gespielt werden, was es Spielern ermöglicht, das Gefühl eines echten Casinos von ihrem eigenen Zuhause aus zu erleben.
Insgesamt bietet das Tipico Casino mit einem Euro Einsatz eine unterhaltsame und zugängliche Möglichkeit, Casino-Spiele online zu spielen. Egal, ob man ein erfahrener Spieler ist oder gerade erst anfängt, mit einem niedrigen Mindesteinsatz kann jeder die Welt der Online-Casinos erkunden und die Chance haben, echtes Geld zu gewinnen.
https://tipicocasino.one/
Das Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und attraktiven Bonusangeboten anbietet. Doch manchmal kann es vorkommen, dass Spieler ihr Auszahlungslimit erreichen und somit Einschränkungen bei der Auszahlung ihrer Gewinne haben.
Ein Auszahlungslimit ist eine finanzielle Beschränkung, die von Casinos gesetzt wird, um sicherzustellen, dass Spieler nicht übermäßig hohe Beträge abheben können. Dies dient dazu, möglichen Betrug und Geldwäsche zu verhindern. Wenn ein Spieler sein Auszahlungslimit erreicht, muss er warten, bis das Limit zurückgesetzt wird, bevor er weitere Gewinne abheben kann.
Es ist wichtig für Spieler im Zet Casino, ihr Auszahlungslimit im Auge zu behalten und sich gegebenenfalls darüber zu informieren, wie sie es erhöhen können. Dies kann je nach Casino unterschiedlich sein und erfordert möglicherweise zusätzliche Verifikationsmaßnahmen.
Wenn ein Spieler sein Auszahlungslimit erreicht hat, bedeutet das nicht unbedingt, dass er nicht mehr im Casino spielen kann. Er kann weiterhin spielen und Gewinne erzielen, aber er kann seine Gewinne erst abheben, wenn das Limit zurГјckgesetzt wurde.
Es ist ratsam, verantwortungsbewusst zu spielen und sein Spielverhalten im Auge zu behalten, um mögliche Einschränkungen wie ein Auszahlungslimit zu vermeiden. Das Zet Casino bietet seinen Spielern Informationen und Tools zum Thema verantwortungsbewusstes Spielen, um ein sicheres und unterhaltsames Spielerlebnis zu gewährleisten.
https://zetcasino.one/
Boomerang Casino Desktop Version: Das ultimative Online-Spielerlebnis
Das Boomerang Casino hat sich als eines der besten Online-Casinos etabliert, das eine breite Palette von Spielen und spannenden Funktionen bietet. Mit der Einführung der Desktop-Version können Spieler nun noch bequemer von zu Hause aus auf ihre Lieblingsspiele zugreifen.
Die Desktop-Version des Boomerang Casinos bietet eine benutzerfreundliche und Гјbersichtliche OberflГ¤che, die es Spielern ermГ¶glicht, ganz einfach durch das Spielangebot zu navigieren. Von Spielautomaten Гјber Tischspiele bis hin zu Live-Casino-Spielen – die Desktop-Version bietet alles, was das Herz begehrt.
Ein weiterer Vorteil der Desktop-Version ist die Möglichkeit, das Spielerlebnis auf einem größeren Bildschirm zu genießen. Dies bedeutet, dass Spieler die atemberaubende Grafik und die spannenden Animationen noch besser erleben können. Darüber hinaus ist die Desktop-Version auch ideal für diejenigen, die lieber mit einer Maus und Tastatur spielen, anstatt mit einem mobilen Gerät.
Die Desktop-Version des Boomerang Casinos bietet zudem die gleiche hochwertige Spielsicherheit wie die mobile Version. Spieler können sicher sein, dass ihre persönlichen und finanziellen Daten geschützt sind und dass faire Spielpraktiken gewährleistet sind.
Insgesamt bietet die Desktop-Version des Boomerang Casinos ein ultimatives Spielerlebnis für alle Online-Glücksspiel-Enthusiasten. Mit einer Vielzahl von Spielen, einer benutzerfreundlichen Oberfläche und topaktuellen Sicherheitsfunktionen ist das Boomerang Casino Desktop eine ausgezeichnete Wahl für alle, die nach einem erstklassigen Online-Casino-Erlebnis suchen.
https://boomerangcasino.one/
Zet Casino Einzahlungsmöglichkeiten
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Einzahlungsmöglichkeiten für seine Spieler anbietet. Die Vielfalt der verfügbaren Optionen macht es einfach, Geld auf das Spielerkonto einzuzahlen und schnell mit dem Spielen zu beginnen.
Eine der beliebtesten Einzahlungsmethoden bei Zet Casino ist die Verwendung von Kredit- oder Debitkarten wie Visa und Mastercard. Diese Methode ist einfach und schnell und ermöglicht es den Spielern, sofort mit dem Spielen zu beginnen.
Eine weitere häufig genutzte Option ist die Zahlung per E-Wallet, wie zum Beispiel Skrill oder Neteller. Diese Methoden sind besonders beliebt, da sie eine zusätzliche Sicherheitsebene bieten und die Spieler ihre Transaktionen schnell und einfach abwickeln können.
Zet Casino bietet auch die Möglichkeit, per Banküberweisung einzuzahlen. Diese Methode kann etwas länger dauern als andere Methoden, ist jedoch eine sichere und zuverlässige Option für Spieler, die keine E-Wallets oder Kreditkarten verwenden möchten.
Darüber hinaus akzeptiert Zet Casino auch verschiedene Kryptowährungen wie Bitcoin, Ethereum und Litecoin. Dies ermöglicht es den Spielern, ihre Einzahlungen anonym und sicher abzuwickeln.
Insgesamt bietet Zet Casino eine Vielzahl von Einzahlungsmöglichkeiten, um den Bedürfnissen und Vorlieben seiner Spieler gerecht zu werden. Egal für welche Methode Sie sich entscheiden, Sie können sicher sein, dass Ihre Transaktionen sicher und zuverlässig abgewickelt werden. Besuchen Sie noch heute Zet Casino und entdecken Sie die Vielzahl der Einzahlungsmöglichkeiten!
https://zetcasino.one/
Tipico ist einer der bekanntesten Anbieter von Online-Casinospielen und bietet eine Vielzahl von Spielen, die sowohl Anfänger als auch erfahrene Spieler begeistern. In diesem Artikel werden wir uns einige der besten Casino-Spiele bei Tipico genauer ansehen.
1. Spielautomaten: Spielautomaten sind die beliebtesten Casinospiele bei Tipico und bieten eine Vielzahl von Themen, Grafiken und Funktionen. Von klassischen FrГјchteslots bis hin zu aufwendigen Videoslots mit Bonusrunden und Freispielen gibt es fГјr jeden Spieler etwas Passendes. Zu den beliebtesten Spielautomaten bei Tipico gehГ¶ren Starburst, Book of Dead und Gonzo’s Quest.
2. Roulette: Roulette ist ein klassisches Casinospiel, das bei Tipico in verschiedenen Varianten angeboten wird. Von der klassischen europäischen Version bis zur spannenden Lightning Roulette Variante gibt es für jeden Roulette-Fan etwas Passendes. Mit seinen einfachen Regeln und hohen Gewinnchancen ist Roulette ein echter Casino-Klassiker.
3. Blackjack: Blackjack ist ein weiteres beliebtes Casinospiel, das bei Tipico in verschiedenen Varianten gespielt werden kann. Von klassischem Blackjack bis hin zu Pontoon und Double Exposure Blackjack gibt es fГјr jeden Spieler eine passende Variante. Mit seiner Mischung aus GlГјck und Strategie bietet Blackjack spannende Unterhaltung und hohe Gewinnchancen.
4. Live Casino Spiele: Die Live Casino Spiele bei Tipico bieten ein authentisches Casinoerlebnis von zu Hause aus. Von Live Roulette über Live Blackjack bis hin zu Live Baccarat bietet das Live Casino bei Tipico eine Vielzahl von Tischspielen mit echten Dealern und einem interaktiven Spielerlebnis. Mit HD-Streaming und Live-Chat-Funktion können Spieler mit den Dealern und anderen Spielern interagieren und ein echtes Casinoerlebnis genießen.
Insgesamt bietet Tipico eine groГџartige Auswahl an Casino-Spielen, die fГјr jeden Spieler etwas Passendes bieten. Von Spielautomaten Гјber Tischspiele bis hin zu Live Casino Spielen gibt es bei Tipico eine Vielzahl von Optionen, um das Casinoerlebnis zu genieГџen. Mit seinen erstklassigen Grafiken, schnellen Ladezeiten und sicheren Zahlungsmethoden ist Tipico die beste Wahl fГјr alle Casino-Fans.
https://tipicocasino.one/
Zet Casino Login – Alles, was Sie wissen mГјssen
Wenn Sie auf der Suche nach einem spannenden Online-Casino sind, dann sollten Sie definitiv Zet Casino in Betracht ziehen. Mit einer breiten Auswahl an Spielen, groГџzГјgigen Boni und einem benutzerfreundlichen Interface bietet Zet Casino ein erstklassiges Spielerlebnis fГјr alle Casino-Enthusiasten.
Um bei Zet Casino spielen zu können, müssen Sie sich zunächst registrieren und ein Konto erstellen. Der Anmeldeprozess ist schnell und einfach und erfordert nur einige grundlegende Informationen wie Ihren Namen, Ihre E-Mail-Adresse und Ihren Wohnsitz. Sobald Sie Ihr Konto erstellt haben, können Sie sich mit Ihren Anmeldeinformationen unter Zet Casino Login anmelden und sofort mit dem Spielen beginnen.
Einmal angemeldet, haben Sie Zugriff auf Hunderte von beliebten Casinospiele, darunter Slots, Tischspiele, Live-Dealer-Spiele und mehr. Zet Casino arbeitet mit den besten Spieleanbietern der Branche zusammen, darunter NetEnt, Microgaming und Play’n GO, um sicherzustellen, dass Sie das bestmГ¶gliche Spielerlebnis haben.
Zet Casino belohnt seine Spieler auch regelmäßig mit lukrativen Boni und Aktionen. Von Willkommensboni für neue Spieler bis zu wöchentlichen Sonderaktionen und Treueprogrammen, gibt es immer etwas zu gewinnen bei Zet Casino.
Darüber hinaus bietet Zet Casino eine sichere und zuverlässige Spielerfahrung. Die Website ist mit der neuesten SSL-Verschlüsselungstechnologie geschützt, um sicherzustellen, dass Ihre persönlichen und finanziellen Daten jederzeit sicher sind.
Also, wenn Sie nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis suchen, dann melden Sie sich noch heute bei Zet Casino an und erleben Sie die Aufregung des Spielens in einem der besten Casinos im Internet. Viel GlГјck und viel SpaГџ!
https://zetcasino.one/
Das Tipico Casino ist eine beliebte Online-Glücksspielplattform, die eine breite Auswahl an Spielen und großzügige Bonusangebote für ihre Spieler bietet. In diesem Artikel werden wir die Bewertung des Tipico Casinos näher betrachten.
Das Casino bietet eine Vielzahl von Spielen, darunter klassische Tischspiele wie Roulette und Blackjack, sowie eine große Auswahl an Spielautomaten von renommierten Anbietern wie NetEnt und Microgaming. Die Spiele sind sowohl auf dem Desktop als auch auf mobilen Geräten verfügbar und bieten ein reibungsloses Spielerlebnis ohne lange Ladezeiten.
Ein weiterer Pluspunkt des Tipico Casinos sind die großzügigen Bonusangebote, die regelmäßig angeboten werden. Neue Spieler können sich über einen Willkommensbonus freuen, der ihnen zusätzliches Guthaben oder Freispiele bietet. Zusätzlich gibt es auch regelmäßige Aktionen wie Reload-Boni und Cashback-Angebote für treue Spieler.
Die Sicherheit und Seriosität des Tipico Casinos sind ebenfalls lobenswert. Das Casino besitzt eine Lizenz der Malta Gaming Authority, einer der angesehensten Regulierungsbehörden in der Glücksspielbranche. Die Datenübertragung erfolgt verschlüsselt, um die persönlichen Informationen der Spieler zu schützen, und das Casino setzt sich für verantwortungsbewusstes Spielen ein.
Insgesamt lässt sich sagen, dass das Tipico Casino eine gute Wahl für Online-Spieler ist. Mit einer vielfältigen Auswahl an Spielen, großzügigen Bonusangeboten und einer hohen Sicherheitsstandards hat das Casino viel zu bieten. Daher können wir das Tipico Casino mit gutem Gewissen weiterempfehlen.
https://tipicocasino.one/
Zet Casino Promo Code 2023: Profitieren Sie von exklusiven Angeboten
Wenn Sie auf der Suche nach einem neuen Online Casino sind, das mit großzügigen Bonusaktionen und spannenden Spielen lockt, dann sind Sie bei Zet Casino genau richtig. Das beliebte Online Casino bietet seinen Kunden regelmäßig attraktive Promo Codes, mit denen Sie zusätzliches Guthaben oder Freispiele erhalten können.
Für das Jahr 2023 können Sie sich auf noch mehr lukrative Angebote freuen. Mit dem exklusiven Zet Casino Promo Code 2023 haben Sie die Möglichkeit, von zahlreichen Vorteilen zu profitieren. Egal ob Sie ein erfahrener Spieler sind oder gerade erst in die Welt des Online Glücksspiels eintauchen, mit dem Promo Code können Sie Ihr Spielerlebnis noch spannender gestalten.
Nutzen Sie den Zet Casino Promo Code 2023 bei Ihrer nГ¤chsten Einzahlung und sichern Sie sich einen tollen Bonus. Ob zusГ¤tzliches Guthaben fГјr Ihre Lieblingsspiele oder Freispiele fГјr ausgewГ¤hlte Slots – die MГ¶glichkeiten sind vielfГ¤ltig. Mit dem Promo Code wird Ihr Spielerkonto im Handumdrehen aufgeladen und Sie kГ¶nnen direkt mit dem Spielen loslegen.
Um den Zet Casino Promo Code 2023 zu erhalten, müssen Sie lediglich bei Ihrer Einzahlung den entsprechenden Code eingeben. Schon wird Ihnen der Bonus gutgeschrieben und Sie können sich über zusätzliche Gewinnchancen freuen. Aber beeilen Sie sich, denn die Promo Codes sind oft nur für einen begrenzten Zeitraum gültig.
Also warten Sie nicht länger und sichern Sie sich mit dem Zet Casino Promo Code 2023 lohnende Boni und attraktive Angebote. Tauchen Sie ein in die faszinierende Welt des Online Glücksspiels und erleben Sie spannende Stunden voller Nervenkitzel und Spaß. Viel Glück und viel Spaß!
https://zetcasino.one/
Das Boomerang Casino hat das Jahr 2021 mit einer aufregenden Neuigkeit für seine Spieler eingeläutet: Neue und spannende No Deposit Bonus Codes. Diese Codes ermöglichen es den Spielern, kostenlos zu spielen und echtes Geld zu gewinnen, ohne dabei eigenes Geld einzusetzen.
Ein No Deposit Bonus Code ist eine Art Belohnung, die vom Casino an seine Spieler vergeben wird, ohne dass eine Einzahlung erforderlich ist. Diese Codes können auf verschiedenen Plattformen wie Websites, E-Mails oder sozialen Medien gefunden werden und müssen dann einfach nur im entsprechenden Feld auf der Casino-Website eingegeben werden, um den Bonus zu erhalten.
Die No Deposit Bonus Codes für das Boomerang Casino im Jahr 2021 bieten den Spielern die Möglichkeit, neue Spiele auszuprobieren und ihre Lieblingsspiele zu spielen, ohne dabei Risiken einzugehen. Zusätzlich gibt es die Chance, echtes Geld zu gewinnen und sich diesen Gewinn auch auszahlen zu lassen.
Um über die aktuellen No Deposit Bonus Codes informiert zu bleiben, empfiehlt es sich, die offizielle Website des Boomerang Casinos regelmäßig zu besuchen oder den Newsletter zu abonnieren. Dort werden regelmäßig neue Aktionen und Codes bekannt gegeben, die die Spieler nutzen können, um ihr Spielerlebnis noch spannender zu gestalten.
Insgesamt bieten die No Deposit Bonus Codes für das Jahr 2021 im Boomerang Casino eine tolle Möglichkeit, kostenlos zu spielen und dabei echtes Geld zu gewinnen. Es lohnt sich also, die Augen offen zu halten und die Codes zu nutzen, um das Beste aus dem eigenen Spielerlebnis herauszuholen.
https://boomerangcasino.one/
Zet Casino ist ein beliebtes Online-Casino, das seinen Spielern eine Vielzahl von spannenden Spielen und großzügigen Bonusangeboten bietet. Eines der besten Angebote, das neue Spieler bei Zet Casino erhalten können, sind 30 Freispiele ohne Einzahlung.
Diese Freispiele bieten Spielern die Möglichkeit, einige der besten Spielautomaten im Casino kostenlos zu spielen und dabei echtes Geld zu gewinnen. Die 30 Freispiele können in ausgewählten Spielautomaten verwendet werden und sind eine großartige Möglichkeit, das Casino und seine Spiele zu erkunden, ohne dabei eigenes Geld riskieren zu müssen.
Um die 30 Freispiele zu erhalten, müssen neue Spieler lediglich ein Konto bei Zet Casino registrieren. Nach der Registrierung werden die Freispiele automatisch gutgeschrieben und können sofort verwendet werden. Es gibt keine Einzahlung erforderlich, um diese Freispiele zu erhalten, was sie zu einem attraktiven Angebot für alle Spieler macht, die das Casino ausprobieren möchten.
Die Freispiele bei Zet Casino sind eine großartige Möglichkeit, um das Casino kennenzulernen und die verschiedenen Spiele auszuprobieren, ohne dabei eigenes Geld riskieren zu müssen. Spieler haben die Chance, echte Gewinne zu erzielen, während sie die spannenden Spielautomaten im Casino genießen.
Insgesamt sind die 30 Freispiele bei Zet Casino ein großzügiges Angebot für neue Spieler, das es ermöglicht, das Casino und seine Spiele auf unkomplizierte Weise zu erkunden. Mit einer Vielzahl von hochwertigen Spielen und attraktiven Bonusangeboten ist Zet Casino die ideale Wahl für alle, die nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis suchen.
https://zetcasino.one/
Tipico Casino Гњberweisung blockiert
Haben Sie schon einmal versucht, eine Überweisung im Tipico Casino zu tätigen, aber festgestellt, dass diese blockiert wurde? Dies kann frustrierend sein und viele Fragen aufwerfen. In diesem Artikel werden wir genauer untersuchen, warum Überweisungen im Tipico Casino blockiert werden könnten und was Sie in einer solchen Situation tun können.
Es gibt verschiedene Gründe, warum eine Überweisung im Tipico Casino blockiert sein könnte. Einer der häufigsten Gründe ist, dass das Casino Verdachtsmomente auf betrügerische Aktivitäten hat. In diesem Fall wird die Überweisung aus Sicherheitsgründen blockiert, um mögliche Schäden zu vermeiden. Es könnte jedoch auch sein, dass es sich um einen technischen Fehler handelt, der die Überweisung blockiert hat.
Wenn Ihre Überweisung im Tipico Casino blockiert wurde, sollten Sie als erstes den Kundenservice des Casinos kontaktieren. Die Mitarbeiter werden Ihnen helfen, das Problem zu klären und die Ursache für die Blockierung festzustellen. Möglicherweise müssen Sie zusätzliche Informationen bereitstellen, um die Überprüfung abzuschließen und die Überweisung freizugeben.
Es ist auch wichtig zu überprüfen, ob alle Informationen korrekt eingegeben wurden und ob keine Schreibfehler vorliegen. Dies kann ebenfalls zu einer Blockierung der Überweisung führen. Stellen Sie sicher, dass Sie alle relevanten Informationen bereit halten, um den Prozess so reibungslos wie möglich zu gestalten.
In einigen Fällen kann es notwendig sein, zusätzliche Sicherheitsmaßnahmen zu ergreifen, um die Überweisung freizugeben. Dies könnte die Überprüfung Ihrer Identität oder das Einreichen weiterer Dokumente umfassen. Seien Sie geduldig und arbeiten Sie mit dem Kundenservice zusammen, um das Problem so schnell wie möglich zu lösen.
Es ist wichtig zu beachten, dass das Tipico Casino strenge Sicherheitsmaßnahmen hat, um die finanzielle Sicherheit seiner Spieler zu gewährleisten. Wenn eine Überweisung blockiert wird, geschieht dies aus gutem Grund und dient nur dazu, Ihre finanziellen Interessen zu schützen. Arbeiten Sie mit dem Kundenservice zusammen, um das Problem zu lösen, und seien Sie versichert, dass Ihre Überweisung sicher und geschützt ist.
Insgesamt ist es wichtig, ruhig zu bleiben und geduldig zu sein, wenn Ihre Überweisung im Tipico Casino blockiert wird. Mit der richtigen Herangehensweise und Unterstützung des Kundenservice können Sie das Problem lösen und Ihre Überweisung erfolgreich abschließen. Bleiben Sie wachsam und achten Sie auf mögliche Fehler, um zukünftige Blockierungen zu vermeiden.
https://tipicocasino.one/
Zet Casino bietet seinen Spielern die Möglichkeit, 20 Free Spins ohne Einzahlung zu erhalten. Diese Freispiele können für ausgewählte Spielautomaten genutzt werden und bieten die Chance, echtes Geld zu gewinnen, ohne dabei eigenes Geld einzusetzen.
Um die 20 Free Spins zu erhalten, muss man sich lediglich im Zet Casino anmelden und den entsprechenden Bonuscode eingeben. Nach der Aktivierung stehen die Freispiele sofort zur Verfügung und können direkt genutzt werden.
Die Auswahl an Spielautomaten, für die die Free Spins genutzt werden können, ist vielfältig und abwechslungsreich. Von klassischen Slots bis hin zu modernen Video-Spielautomaten ist für jeden Geschmack etwas dabei.
Die Gewinne aus den Free Spins unterliegen in der Regel Umsatzbedingungen, die erfüllt werden müssen, bevor eine Auszahlung möglich ist. Diese Bedingungen variieren je nach Casino und sollten vor der Inanspruchnahme des Angebots genau geprüft werden.
Insgesamt sind Free Spins eine tolle Möglichkeit, um neue Spiele auszuprobieren und dabei auch noch die Chance auf hohe Gewinne zu haben. Wer also gerne Spielautomaten spielt, sollte sich das Angebot von Zet Casino nicht entgehen lassen und die 20 Free Spins nutzen.
https://zetcasino.one/
Boomerang Casino Mobile: Spielen Sie unterwegs wie ein Profi!
Das Boomerang Casino Mobile bietet Ihnen die Möglichkeit, Ihre Lieblingsspiele überall und jederzeit zu genießen. Mit der neuen mobilen Plattform können Sie auf Ihrem Smartphone oder Tablet eine breite Auswahl an Casinospielen spielen, egal ob Sie zu Hause, im Zug oder im Café sind.
Die mobile Version des Boomerang Casinos bietet eine benutzerfreundliche Oberfläche, die es Ihnen leicht macht, sich in den Spielen zurechtzufinden. Dank der optimierten Navigation können Sie schnell zwischen den verschiedenen Spielkategorien wie Slots, Tischspielen und Live-Casino wechseln.
Die mobilen Spiele im Boomerang Casino bieten die gleiche hochwertige Grafik und Funktionalität wie die Desktop-Version. Sie können also sicher sein, dass Sie ein erstklassiges Spielerlebnis genießen, unabhängig davon, ob Sie auf Ihrem Computer oder Ihrem mobilen Gerät spielen.
Ein weiterer Vorteil des Boomerang Casino Mobile ist die Möglichkeit, Boni und Aktionen direkt auf Ihrem mobilen Gerät zu nutzen. Sie können von unterwegs auf exklusive Bonusangebote zugreifen und von zusätzlichen Belohnungen profitieren.
Das Boomerang Casino Mobile ist mit den meisten gängigen Geräten und Betriebssystemen kompatibel und bietet eine reibungslose und unterhaltsame Spielerfahrung. Also, warum warten? Melden Sie sich jetzt an und spielen Sie Ihre Lieblingsspiele unterwegs wie ein Profi im Boomerang Casino Mobile!
https://boomerangcasino.one/
Zet Casino Bestes Spiel
Zet Casino ist eine beliebte Online-GlГјcksspielplattform, die eine Vielzahl von Spielen fГјr Spieler aus aller Welt anbietet. Mit einer breiten Auswahl an Spielautomaten, Tischspielen und Live-Dealer-Spielen gibt es fГјr jeden Geschmack etwas zu entdecken. Doch welches ist das beste Spiel im Zet Casino?
Eine klare Antwort auf diese Frage gibt es nicht, da die Vorlieben und Spielstärken jedes Spielers unterschiedlich sind. Jedoch gibt es einige Spiele, die bei den meisten Spielern besonders beliebt sind.
Eines davon ist sicherlich der Spielautomat Starburst. Dieser beliebte Slot von NetEnt bietet nicht nur ein ansprechendes Design und tolle Soundeffekte, sondern auch hohe Gewinnchancen. Mit seinem einfachen Spielprinzip und den vielen Bonusfunktionen ist Starburst ein echter Dauerbrenner unter den Spielautomaten.
Auch das Kartenspiel Blackjack erfreut sich großer Beliebtheit im Zet Casino. Dank seiner einfachen Regeln und der strategischen Tiefe zieht dieses Spiel viele Spieler an. Mit etwas Übung kann man hier seine Gewinnchancen deutlich erhöhen und große Gewinne erzielen.
FГјr Fans von Live-Dealer-Spielen ist Evolution Gamings Dream Catcher eine gute Wahl. Bei diesem GlГјcksrad-Spiel kann man mit etwas GlГјck hohe Gewinne erzielen und sich von einem charmanten Live-Dealer durch das Spiel fГјhren lassen.
Letztendlich liegt es aber an jedem Spieler selbst, sein persönliches Lieblingsspiel im Zet Casino zu finden. Mit einer großen Auswahl an hochwertigen Spielen und lukrativen Bonusangeboten gibt es hier für jeden etwas zu entdecken. Probieren Sie einfach verschiedene Spiele aus und finden Sie heraus, welches Spiel am besten zu Ihnen passt. Viel Spaß und viel Glück!
https://zetcasino.one/
Tipico Bonus umsetzen im Casino
Tipico ist einer der beliebtesten Online-Sportwettenanbieter in Deutschland und bietet auch ein umfangreiches Online-Casino an. FГјr neue Kunden gibt es einen attraktiven Willkommensbonus, der auch im Casino eingesetzt werden kann. Doch wie genau kann man den Tipico Bonus im Casino umsetzen?
Zunächst einmal muss man sich als neuer Kunde bei Tipico anmelden und eine Einzahlung tätigen, um den Bonus zu erhalten. Dieser wird dann automatisch auf das Konto gutgeschrieben und kann sowohl im Sportwettenbereich als auch im Casino eingesetzt werden. Um den Bonus umzusetzen, muss man die Umsatzbedingungen erfüllen, die für den jeweiligen Bonus gelten.
Im Casino von Tipico gibt es eine Vielzahl von Spielen, die für den Umsatz des Bonuses genutzt werden können. Dazu gehören unter anderem Spielautomaten, Roulette, Blackjack und Video Poker. Je nach Bonus kann es unterschiedliche Gewichtungen der Spiele geben. Zum Beispiel kann es sein, dass Einsätze an Spielautomaten zu 100% zum Umsatz beitragen, während Einsätze bei Roulette nur zu 10% angerechnet werden.
Es ist wichtig zu beachten, dass man den Bonus innerhalb eines bestimmten Zeitraums umsetzen muss, bevor er verfällt. Außerdem sollte man darauf achten, dass man die jeweiligen Umsatzbedingungen erfüllt, um eine Auszahlung des Bonus und der damit erzielten Gewinne beantragen zu können.
Insgesamt bietet Tipico seinen Kunden eine faire Chance, den Bonus im Casino umzusetzen und davon zu profitieren. Mit einer guten Strategie und etwas Glück kann man seine Gewinne sogar noch steigern und sich über zusätzliches Guthaben freuen. Also worauf warten Sie noch? Nutzen Sie den Tipico Bonus und spielen Sie spannende Casino-Spiele!
https://tipicocasino.one/
Das Boomerang Casino in Australien ist ein aufregendes neues Glücksspielziel, das Spieler aus der ganzen Welt anlockt. Mit einer Vielzahl von Spielen, großzügigen Boni und einer beeindruckenden Benutzeroberfläche bietet das Boomerang Casino ein unvergessliches Spielerlebnis.
Das Casino wurde im Jahr 2020 gegrГјndet und hat sich schnell einen Namen als einer der besten Casinos Down Under gemacht. Mit einer Lizenz der Malta Gaming Authority bietet das Boomerang Casino Spielern ein sicheres und faires Spielerlebnis.
Das Boomerang Casino bietet eine breite Palette von Spielen, einschlieГџlich Spielautomaten, Tischspielen, Live-Dealer-Spielen und vielem mehr. Zu den beliebtesten Spielen gehГ¶ren Slots wie Starburst, Gonzo’s Quest und Book of Dead sowie Tischspiele wie Blackjack, Roulette und Baccarat.
Spieler im Boomerang Casino können von großzügigen Boni und Promotionen profitieren, einschließlich Willkommensboni, Einzahlungsboni und Freispielen. Das Casino belohnt auch treue Spieler mit einem VIP-Programm, das exklusive Belohnungen und Vergünstigungen bietet.
Die Benutzeroberfläche des Boomerang Casino ist modern und benutzerfreundlich, mit einer einfachen Navigation und einer ansprechenden Gestaltung. Spieler können das Casino auf ihren Desktop-Computern, Tablets und Smartphones nutzen, um jederzeit und überall auf ihre Lieblingsspiele zuzugreifen.
Insgesamt bietet das Boomerang Casino ein fantastisches Spielerlebnis mit einer Vielzahl von Spielen, großzügigen Boni und einer benutzerfreundlichen Benutzeroberfläche. Für Spieler, die nach einem erstklassigen Glücksspielerlebnis suchen, ist das Boomerang Casino die ideale Wahl. Besuchen Sie das Boomerang Casino noch heute und erleben Sie die Spannung und Unterhaltung, die es zu bieten hat.
https://boomerangcasino.one/
Zet Casino Free Spins: Nutzen Sie Ihre Chance, um groГџe Gewinne zu erzielen!
Wer träumt nicht davon, in einem Online-Casino groß abzuräumen? Mit den Zet Casino Free Spins haben Spieler die Möglichkeit, genau das zu tun. Diese beliebten Bonusangebote bieten Spielern die Chance, kostenlos an ausgewählten Spielautomaten zu drehen und dabei echtes Geld zu gewinnen.
Die Free Spins im Zet Casino werden den Spielern in verschiedenen Situationen angeboten. Zum Beispiel als Teil eines Willkommensbonus für neue Spieler, als Belohnung für treue Kunden oder als Sonderaktionen zu bestimmten Feiertagen oder Events. Diese kostenlosen Spins können auf viele verschiedene Spielautomaten angewendet werden und bieten den Spielern die Möglichkeit, neue Spiele auszuprobieren oder ihre Lieblingsspiele weiter zu genießen.
Um die Zet Casino Free Spins zu erhalten, müssen Spieler oft nur eine bestimmte Einzahlung tätigen oder sich für die Aktion anmelden. Sobald die Freispiele gutgeschrieben wurden, können die Spieler sofort damit beginnen, an den Spielautomaten zu drehen und hoffentlich große Gewinne zu erzielen.
Es ist wichtig zu beachten, dass die meisten Free Spins Boni bestimmte Umsatzbedingungen haben, die erfüllt werden müssen, bevor die Gewinne ausgezahlt werden können. Diese Bedingungen können in der Regel im Kleingedruckten der jeweiligen Aktion gefunden werden und sollten sorgfältig gelesen werden, um Missverständnisse zu vermeiden.
Insgesamt sind die Zet Casino Free Spins eine fantastische Möglichkeit für Spieler, zusätzliche Gewinne zu erzielen, ohne dabei ihr eigenes Geld riskieren zu müssen. Durch die Teilnahme an diesen Aktionen können Spieler ihre Lieblingsspiele spielen, neue Spiele entdecken und mit etwas Glück ordentliche Gewinne mit nach Hause nehmen. Nutzen Sie also Ihre Chance und drehen Sie die Walzen mit den Zet Casino Free Spins!
https://zetcasino.one/
Das Tipico Casino in Mönchengladbach am Kammof bietet den Besuchern eine spannende und unterhaltsame Glücksspiel-Atmosphäre. Das Casino befindet sich in zentraler Lage und ist somit leicht erreichbar für alle, die auf der Suche nach Unterhaltung und Nervenkitzel sind.
Das Casino bietet eine Vielzahl von Spielmöglichkeiten, darunter klassische Tischspiele wie Roulette und Blackjack, sowie eine breite Auswahl an Spielautomaten. Egal ob erfahrener Spieler oder Anfänger, im Tipico Casino am Kammof kommt jeder auf seine Kosten.
Zusätzlich zu den Spielmöglichkeiten bietet das Casino auch verschiedene Veranstaltungen und Aktionen an, um den Aufenthalt der Besucher noch spannender zu gestalten. Von Pokerturnieren bis hin zu Live-Musik-Events ist im Tipico Casino am Kammof immer etwas los.
Wenn Sie also auf der Suche nach einem unterhaltsamen Abend sind, ist das Tipico Casino am Kammof in Mönchengladbach die perfekte Adresse. Tauchen Sie ein in die Welt des Glücksspiels und genießen Sie eine aufregende Zeit in diesem beliebten Casino.
https://tipicocasino.one/
Boomerang Bet Casino Review
Das Boomerang Bet Casino ist eine beliebte Online-GlГјcksspielplattform fГјr Spieler aus der ganzen Welt. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und einem benutzerfreundlichen Interface ist es leicht zu verstehen, warum so viele Menschen diesem Casino vertrauen.
Das Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Dealer-Spiele und mehr. Die Spiele sind von erstklassigen Softwareanbietern wie NetEnt, Microgaming, Play’n GO und anderen entwickelt worden, was fГјr ein qualitativ hochwertiges Spielerlebnis sorgt.
Eine der besten Eigenschaften des Boomerang Bet Casinos sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler können von einem Willkommensbonus profitieren, der sie mit zusätzlichem Geld oder Freispielen belohnt. Darüber hinaus gibt es auch regelmäßige Einzahlungsboni, Freispielaktionen und Treueprogramme, die es den Spielern ermöglichen, noch mehr zu gewinnen.
Das Casino verfГјgt Гјber eine benutzerfreundliche Webseite, die es einfach macht, sich anzumelden, Spiele zu finden und Ein- und Auszahlungen vorzunehmen. Der Kundensupport ist rund um die Uhr verfГјgbar und steht den Spielern bei Fragen oder Problemen zur VerfГјgung.
Insgesamt ist das Boomerang Bet Casino eine hervorragende Wahl für Spieler, die nach einer unterhaltsamen und sicheren Online-Glücksspielplattform suchen. Mit einer Vielzahl von Spielen, großzügigen Boni und einem herausragenden Kundensupport können Spieler sicher sein, dass sie bei diesem Casino ein erstklassiges Spielerlebnis genießen werden. Probieren Sie es noch heute aus und sehen Sie selbst, warum das Boomerang Bet Casino zu den besten Online-Casinos gehört.
https://boomerangcasino.one/
Boomerang Casino Iceland
Das Boomerang Casino Iceland ist ein beliebtes Online-Casino, das Spielern aus aller Welt eine Vielzahl von spannenden Spielen und großzügigen Boni bietet. Mit einer breiten Auswahl an Slots, Tischspielen und Live-Casino-Optionen ist für jeden Geschmack etwas dabei. Das Casino ist bekannt für seine benutzerfreundliche Oberfläche, schnelle Auszahlungen und hervorragenden Kundenservice.
Eines der Highlights des Boomerang Casino Iceland sind die regelmäßigen Promotionen und Boni, die Spielern die Möglichkeit bieten, zusätzliches Geld oder Freispiele zu gewinnen. Darüber hinaus gibt es ein Treueprogramm, das loyalen Spielern noch mehr Belohnungen bietet.
Die Sicherheit der Spieler wird im Boomerang Casino Iceland großgeschrieben. Das Casino verwendet die neueste SSL-Verschlüsselungstechnologie, um sicherzustellen, dass alle persönlichen Daten geschützt sind. Zudem werden alle Spiele regelmäßig von unabhängigen Behörden auf Fairness überprüft.
Ein weiterer Pluspunkt des Boomerang Casino Iceland ist die Vielzahl an Zahlungsmethoden, die Spielern zur Verfügung stehen. Von Kreditkarten über E-Wallets bis hin zu Kryptowährungen – hier findet jeder die passende Option für Ein- und Auszahlungen.
Insgesamt bietet das Boomerang Casino Iceland ein unterhaltsames und sicheres Spielerlebnis fГјr alle, die gerne online spielen. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Boni und einem top Kundenservice ist das Casino definitiv einen Besuch wert.
https://boomerangcasino.one/
Современное жилье для ценителей комфорта
15. Дом из бруса 9х12: гармония с природой
дом брус 9х12 https://domizbrusa9x12spb.ru/ .
1. Вибір натяжних стель – як правильно обрати?
2. Топ-5 популярних кольорів натяжних стель
3. Як зберегти чистоту натяжних стель?
4. Відгуки про натяжні стелі: плюси та мінуси
5. Як підібрати дизайн натяжних стель до інтер’єру?
6. Інноваційні технології у виробництві натяжних стель
7. Натяжні стелі з фотопечаттю – оригінальне рішення для кухні
8. Секрети вдалого монтажу натяжних стель
9. Як зекономити на встановленні натяжних стель?
10. Лампи для натяжних стель: які вибрати?
11. Відтінки синього для натяжних стель – ексклюзивний вибір
12. Якість матеріалів для натяжних стель: що обирати?
13. Крок за кроком: як самостійно встановити натяжні стелі
14. Натяжні стелі в дитячу кімнату: безпека та креативність
15. Як підтримувати тепло у приміщенні за допомогою натяжних стель
16. Вибір натяжних стель у ванну кімнату: практичні поради
17. Натяжні стелі зі структурним покриттям – тренд сучасного дизайну
18. Індивідуальність у кожному домашньому інтер’єрі: натяжні стелі з друком
19. Як обрати освітлення для натяжних стель: поради фахівця
20. Можливості дизайну натяжних стель: від класики до мінімалізму
ціна натяжних стель http://www.natjazhnistelitvhyn.kiev.ua .
Das Avis Boomerang Casino ist eine der beliebtesten Glücksspiel-Einrichtungen in Deutschland. Mit einer Vielzahl von Spielen und einer erstklassigen Atmosphäre bietet dieser Ort eine einzigartige Spielerfahrung für alle, die ihr Glück auf die Probe stellen wollen.
Das Casino ist bekannt für seine großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Spieler haben die Möglichkeit, von verschiedenen Aktionen zu profitieren und ihre Gewinnchancen zu erhöhen.
Die Auswahl an Spielen im Avis Boomerang Casino ist beeindruckend. Von klassischen Tischspielen wie Blackjack, Roulette und Poker bis hin zu modernen Spielautomaten und Video-Poker ist für jeden Geschmack etwas dabei. Die Spiele werden regelmäßig überprüft und sind fair und sicher.
Die Atmosphäre im Casino ist einzigartig und sorgt für ein unvergessliches Erlebnis. Das freundliche Personal sorgt dafür, dass sich die Gäste wie zu Hause fühlen und steht jederzeit für Fragen und Anliegen zur Verfügung.
Das Avis Boomerang Casino ist der ideale Ort für alle, die ein spannendes und unterhaltsames Spielerlebnis suchen. Mit einer Vielzahl von Spielen, großzügigen Boni und einer erstklassigen Atmosphäre ist dieses Casino ein Muss für alle Glücksspielfans. Besuchen Sie das Avis Boomerang Casino und erleben Sie den Nervenkitzel des Glücksspiels in einer sicheren und professionellen Umgebung.
https://boomerangcasino.one/
Gogo Casino Г¤r ett populГ¤rt onlinecasino i Finland som erbjuder en spГ¤nnande och underhГҐllande spelupplevelse fГ¶r sina spelare. Med ett brett utbud av casinospel frГҐn ledande spelleverantГ¶rer som NetEnt, Microgaming och Play’n GO, finns det nГҐgot fГ¶r alla smaker hos Gogo Casino.
En av de främsta fördelarna med att spela på Gogo Casino är den enkla och användarvänliga plattformen. Spelarna kan enkelt navigera mellan olika spelkategorier och hitta sina favoritspel med bara några klick. Dessutom erbjuder casinot snabba och säkra betalningsmetoder för insättningar och uttag, vilket ger spelarna en smidig spelupplevelse.
Gogo Casino erbjuder också generösa bonusar och kampanjer för att belöna sina spelare och öka deras vinstchanser. Spelare kan dra nytta av välkomstbonusar, gratis spins och andra spännande erbjudanden för att öka sina vinster och förlänga sin spelupplevelse.
Med sin licens från Malta Gaming Authority kan spelare vara säkra på att Gogo Casino är ett pålitligt och säkert onlinecasino att spela på. Casinot använder den senaste SSL-krypteringstekniken för att skydda spelarnas personuppgifter och transaktioner, vilket ger spelarna en trygg och säker spelupplevelse.
Sammanfattningsvis erbjuder Gogo Casino en toppmodern och underhållande spelupplevelse för spelare i Finland. Med sitt breda spelutbud, generösa bonusar och säkra plattform är det en utmärkt plats att spela casinospel och ha kul online. Besök Gogo Casino idag och upplev spänningen själv!
https://gogocasino.one
Das Boomerang Casino Forum – Die ultimative Plattform fГјr GlГјcksspiel-Fans
Das Boomerang Casino Forum ist eine Online-Plattform, die sich ausschließlich dem Thema Glücksspiel und Casino-Spiele widmet. Hier treffen sich Glücksspiel-Fans aus aller Welt, um sich über ihre Erfahrungen, Tipps und Tricks auszutauschen. Das Forum bietet eine Vielzahl von verschiedenen Bereichen, in denen die Mitglieder diskutieren und sich informieren können.
Egal ob man auf der Suche nach neuen Casino-Boni ist, sich Гјber die neuesten Slot-Spiele informieren mГ¶chte oder einfach nur mit Gleichgesinnten Гјber die Welt des GlГјcksspiels plaudern will – im Boomerang Casino Forum findet jeder Spieler, wonach er sucht. Zudem bietet das Forum eine optimale Plattform fГјr den Austausch von Strategien und Taktiken, um seine Gewinnchancen beim Spielen zu maximieren.
Ein besonderes Highlight des Boomerang Casino Forums sind die regelmäßig stattfindenden Gewinnspiele und Turniere, bei denen die Mitglieder attraktive Preise wie Bonusguthaben, Freispiele oder sogar Sachpreise gewinnen können. Diese Aktionen sorgen dafür, dass das Forum regelmäßig von einer Vielzahl von Spielern besucht wird und eine lebendige Community entsteht.
Darüber hinaus bietet das Boomerang Casino Forum auch eine umfangreiche Sammlung von Casino-Reviews und Testberichten, die es den Mitgliedern erleichtern, sich über die verschiedenen Online-Casinos und deren Angebote zu informieren. Auf diese Weise können die Spieler sicherstellen, dass sie sich nur bei seriösen und vertrauenswürdigen Anbietern anmelden.
Insgesamt ist das Boomerang Casino Forum eine ideale Anlaufstelle für alle Glücksspiel-Fans, die sich gerne über ihre Leidenschaft austauschen und ihr Wissen erweitern möchten. Wer also auf der Suche nach einem unterhaltsamen und informativen Forum rund um das Thema Casino-Spiele ist, sollte das Boomerang Casino Forum unbedingt einen Besuch abstatten.
https://boomerangcasino.one/
Gogo Casino har haft svårt att få pengar utbetalda till sina spelare på senaste tiden. Många kunder har vänt sig till sociala medier för att klaga på att de inte har fått ut sina vinster från casinot.
Enligt flera användare har Gogo Casino haft problem med sina betalningar under de senaste veckorna. Vissa har väntat i flera veckor på att få ut sina pengar, medan andra har fått sina uttag avbrutna utan förklaring.
Många spelare har uttryckt frustration över situationen och kritiserar casinot för att inte vara transparent med sina betalningsprocesser. En del har även ifrågasatt om Gogo Casino är en pålitlig operatör och uppmanar andra att vara försiktiga med att sätta in sina pengar på sidan.
Gogo Casino har ännu inte kommenterat de uppkomna problemen eller gett någon information om varför utbetalningarna har försenats. Det återstår att se om casinot kommer att ta tag i situationen och åtgärda problemen för sina spelare.
I väntan på mer information uppmanar vi alla som spelar på Gogo Casino att vara försiktiga med sina insättningar och att hålla sig uppdaterade om eventuella förändringar kring betalningsprocesserna. Det är viktigt att vara medveten om risken för att inte kunna få ut sina pengar innan man beslutar sig för att spela på ett online casino.
https://gogocasino.one
Den populära online-casinon Gogo Casino har nyligen fått ett beslut som innebär att de inte kommer att få några pengar från sina spelare. Spelinspektionen har beslutat att återkalla deras spellicens på grund av brister i företagets rutiner för ansvarsfullt spelande.
Beslutet kommer efter en lång utredning där det framkommit att Gogo Casino inte har vidtagit tillräckliga åtgärder för att förebygga spelproblem bland sina spelare. Enligt Spelinspektionen har företaget bland annat inte haft tillräckliga verktyg för att kunna identifiera och hjälpa spelare som riskerar att hamna i spelberoende.
Gogo Casino har nu fått en tillsynsnämnd att utreda ärendet och besluta om eventuella sanktioner mot företaget. De kommer inte att kunna ta emot några insättningar eller ta ut några vinster tills vidare.
Det här beslutet skickar en tydlig signal till alla aktörer på den svenska spelmarknaden om vikten av att ta ansvar för sitt spelutbud och sina spelare. Det är viktigt att alla online-casinon följer de regler och riktlinjer som finns för att skydda spelarna och minska risken för spelmissbruk.
För spelare som är drabbade av beslutet innebär det att de inte längre kan spela på Gogo Casino och att eventuella vinster kan komma att bli oåtkomliga. Det är viktigt att alla spelare som upplever spelproblem söker hjälp och stöd för att komma på rätt väg igen.
Sammanfattningsvis är det här ett viktigt steg för att skapa en säkrare spelmarknad i Sverige och för att skydda spelare från att hamna i spelberoende. Genom att tillsammans arbeta för ett ansvarsfullt spelande kan vi se till att alla kan njuta av underhållningen som casinon erbjuder utan att riskera sin hälsa och ekonomi.
https://gogocasino.one
Zet Casino Bonus Bedingungen
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und attraktiven Bonusangeboten bietet. Die Bonusbedingungen sind jedoch ein wichtiger Aspekt, den Spieler beachten sollten, um das Beste aus ihrem Bonus zu machen.
Zet Casino bietet verschiedene Arten von Boni, darunter Willkommensboni, Einzahlungsboni, Freispiele und Cashback-Angebote. Jeder Bonus hat seine eigenen Bedingungen, die erfüllt werden müssen, um das Bonusguthaben oder die Gewinne aus Freispielen auszahlen zu können.
Die wichtigsten Bonusbedingungen bei Zet Casino umfassen Umsatzanforderungen, Zeitlimits, Spielbeschränkungen und maximale Einsätze. Beispielsweise müssen Spieler den Bonusbetrag eine bestimmte Anzahl von Malen umsetzen, bevor sie eine Auszahlung beantragen können. Das Zeitlimit gibt an, wie lange Spieler haben, um die Umsatzanforderungen zu erfüllen. Spielbeschränkungen legen fest, welche Spiele für den Einsatz des Bonusguthabens in Frage kommen, und maximale Einsätze bestimmen, wie viel ein Spieler pro Runde setzen darf.
Es ist wichtig, die Bonusbedingungen sorgfältig zu lesen und zu verstehen, um Missverständnisse zu vermeiden und sicherzustellen, dass man das Beste aus seinem Bonus macht. Spieler sollten auch beachten, dass bei Verstoß gegen die Bonusbedingungen ihr Bonusguthaben und die damit erzielten Gewinne storniert werden können.
Insgesamt bietet Zet Casino seinen Spielern großzügige Bonusangebote, die sowohl Neulinge als auch erfahrene Spieler ansprechen. Indem man die Bonusbedingungen erfüllt, kann man sein Spielerlebnis maximieren und die Chance auf Gewinne erhöhen.
https://zetcasino.one/
Gogo Casino är ett online casino som erbjuder en mängd olika spel och erbjudanden för sina spelare. För att säkerställa att spelarna har en så bra upplevelse som möjligt, har Gogo Casino en dedikerad kundtjänst som finns tillgänglig för att hjälpa till med alla frågor och problem som kan uppstå under spelandet.
Kundtjänsten på Gogo Casino är tillgänglig dygnet runt via livechatt, e-post eller telefon. De är välutbildade och kunniga om alla aspekter av casinot och kan svara på alla frågor som spelarna kan ha. Oavsett om det handlar om insättningar och uttag, bonusar och kampanjer eller tekniska problem, är kundtjänsten redo att hjälpa till på ett professionellt och vänligt sätt.
En av fördelarna med att spela på Gogo Casino är den snabba och effektiva supporten som erbjuds. Oavsett när på dygnet spelarna behöver hjälp, finns kundtjänsten där för att assistera. Det ger en extra trygghet för spelarna att veta att de alltid kan få hjälp om det behövs.
Sammanfattningsvis är kundtjänsten på Gogo Casino en öppen och tillgänglig resurs för alla spelare som har frågor eller problem under sitt spelande. Med sin professionella och vänliga attityd gör de allt för att se till att spelarna har en trevlig och problemfri spelupplevelse.
https://gogocasino.one
Tipico Geld weg Casino
Das Online-Casino Tipico erfreut sich großer Beliebtheit bei Spielern auf der ganzen Welt. Hier können Nutzer ihr Glück an einer Vielzahl von Spielen versuchen und mit etwas Glück hohe Gewinne erzielen. Doch leider kommt es immer wieder vor, dass Spieler ihr Geld im Casino verlieren und sich betrogen fühlen.
Ein häufig genannter Grund für den Verlust von Geld bei Tipico ist die Suchtgefahr, die Glücksspiele mit sich bringen können. Viele Menschen können nicht aufhören zu spielen, auch wenn sie bereits hohe Verluste erlitten haben. Dies führt dazu, dass sie immer mehr Geld setzen und am Ende mit leeren Taschen dastehen.
Ein weiterer Grund für den Verlust von Geld im Tipico Casino ist die fehlende Strategie beim Spielen. Viele Spieler gehen unüberlegt an die Spiele heran und setzen ihr Geld ohne Plan ein. Dadurch erhöht sich das Risiko, dass das Geld schnell verloren geht.
Zudem gibt es auch Fälle, in denen es zu Betrugsfällen im Tipico Casino kommt. Spieler berichten davon, dass sie nicht ihre Gewinne ausgezahlt bekommen haben oder dass es Probleme bei der Einzahlung ihres Geldes gab. In solchen Fällen fühlen sich die Spieler betrogen und hintergangen.
Um sein Geld im Tipico Casino nicht zu verlieren, ist es wichtig, verantwortungsvoll zu spielen und sich nicht von der Sucht nach dem nächsten großen Gewinn mitreißen zu lassen. Zudem sollte man sich Zeit nehmen, um sich mit den Spielen und ihren Regeln vertraut zu machen, um seine Chancen auf einen Gewinn zu erhöhen.
Insgesamt ist das Tipico Casino ein unterhaltsamer Ort, um sein Glück zu versuchen. Doch Vorsicht ist geboten, um nicht sein Geld zu verlieren und sich betrogen zu fühlen. Mit der richtigen Strategie und der nötigen Vorsicht kann man jedoch auch im Tipico Casino erfolgreich sein und hohe Gewinne erzielen.
https://tipicocasino.one/
Gogo Casino är ett av de mest populära onlinecasinona på marknaden och erbjuder spelare en spännande och underhållande spelupplevelse. Med sitt stora utbud av casinospel och generösa bonusar har Gogo Casino snabbt blivit en favorit hos många spelare.
Ett av de mest framstående drag hos Gogo Casino är dess samarbete med Leovegas, en av de ledande aktörerna inom onlinecasinobranschen. Genom denna partnerskap kan Gogo Casino erbjuda spelare en ännu bättre spelupplevelse med högkvalitativa spel och en säker och pålitlig plattform.
På Gogo Casino Leovegas hittar spelare ett brett utbud av casinospel, inklusive spelautomater, bordsspel och live casino. Med över 1000 spel att välja mellan finns det något för alla smaker och preferenser. Oavsett om du föredrar klassiska spelautomater eller bordsspel som blackjack och roulette, har Gogo Casino Leovegas något för dig.
Utöver sitt imponerande spelutbud erbjuder Gogo Casino Leovegas även generösa bonuserbjudanden för nya spelare. Genom att registrera sig på casinot kan spelare få tillgång till bonusar som gratissnurr och insättningsbonusar, vilket ger dem möjligheten att öka sina vinstchanser och maximera sin spelupplevelse.
Med sin användarvänliga design och snabba utbetalningar har Gogo Casino Leovegas blivit en favorit bland svenska spelare. Oavsett om du är en erfaren casinospelare eller en nybörjare, är Gogo Casino Leovegas det perfekta valet för en spännande och underhållande spelupplevelse. Besök casinot idag och upplev spänningen själv!
https://gogocasino.one
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und Bonusangeboten fГјr seine Spieler anbietet. Eines dieser Bonusangebote sind die sogenannten No Deposit Bonus Codes.
Ein No Deposit Bonus ist eine tolle Möglichkeit für Spieler, um kostenlose Spielguthaben oder Freispiele zu erhalten, ohne eine Einzahlung tätigen zu müssen. Diese Bonuscodes sind eine Art Belohnung für die Spieler und ermöglichen es ihnen, das Casino und die angebotenen Spiele unverbindlich zu testen.
Zet Casino bietet regelmäßig No Deposit Bonus Codes für seine registrierten Spieler an. Um von diesen Angeboten zu profitieren, müssen die Spieler einfach den jeweiligen Bonuscode eingeben, der ihnen in Form von E-Mails oder auf der Webseite des Casinos zur Verfügung gestellt wird.
Die No Deposit Bonus Codes von Zet Casino können verschiedene Formen annehmen, wie zum Beispiel Freispiele für bestimmte Spielautomaten, Gratisguthaben für Tischspiele oder Cashback-Angebote. Diese Boni sind eine großartige Möglichkeit, um das Spielerlebnis zu verbessern und die Gewinnchancen zu erhöhen.
Es ist jedoch wichtig zu beachten, dass No Deposit Boni bestimmten Umsatzbedingungen unterliegen. Bevor man eine Auszahlung beantragen kann, muss man den Bonusbetrag eine bestimmte Anzahl an Malen umsetzen. Es ist daher ratsam, die Teilnahmebedingungen für jedes Bonusangebot sorgfältig zu lesen, um Missverständnisse zu vermeiden.
Insgesamt sind die No Deposit Bonus Codes von Zet Casino eine großartige Möglichkeit, um neue Spiele auszuprobieren und das Spielerlebnis noch spannender zu gestalten. Spieler sollten sich regelmäßig über diese Angebote informieren, um keine lukrativen Boni zu verpassen.
https://zetcasino.one/
https://myportal.utt.edu.tt/ICS/_portletview_/Campus_Life/Campus_Groups/Safer/Discussion.jnz?portlet=Forums&screen=PostView&screenType=change&id=d3abeb09-6fb9-45ee-8bbd-32fad1c4c551
https://bogotamihuerta.jbb.gov.co/miembros/zex-kos/activity/421205/
https://justpaste.it/dfod6
https://sheer-link-81e.notion.site/ea404e9ad9114d42965543600aba2031
воєнторг
18. Где найти все для военных
інтернет магазин тактичного одягу магазин воєнторг київ .
Das Zet Casino, eine beliebte Online-Glücksspielseite, hat kürzlich eine neue Funktion eingeführt, die es Spielern ermöglicht, sich selbst von der Nutzung des Casinos zu sperren. Diese Option wurde eingeführt, um den Spielern, die Schwierigkeiten mit ihrem Spielverhalten haben, zu helfen und sie vor möglichen negativen Konsequenzen des Glücksspiels zu schützen.
Die Sperrfunktion im Zet Casino ermöglicht es den Spielern, sich für einen bestimmten Zeitraum oder sogar dauerhaft von der Nutzung der Seite auszuschließen. Dies kann dazu beitragen, das Risiko von Spielsucht zu reduzieren und den Spielern helfen, ihre Gewohnheiten zu kontrollieren.
Um sich im Zet Casino sperren zu lassen, mГјssen die Spieler einfach Kontakt mit dem Kundendienst aufnehmen und ihre Sperrung beantragen. Die Mitarbeiter des Casinos werden dann die notwendigen Schritte unternehmen, um sicherzustellen, dass der Spieler keinen Zugang mehr zur Seite hat.
Es ist wichtig zu beachten, dass die Sperrung im Zet Casino nicht rückgängig gemacht werden kann und dass die Spieler nach Ablauf des Sperrzeitraums oder nach der dauerhaften Sperrung nicht automatisch Zugang zur Seite erhalten. Dies soll sicherstellen, dass die Spieler wirklich die Möglichkeit haben, ihr Spielverhalten zu kontrollieren und ihr Glücksspielproblem zu überwinden.
Insgesamt ist die Einführung der Sperrfunktion im Zet Casino ein Schritt in die richtige Richtung, um den Spielern zu helfen, verantwortungsbewusst zu spielen und mögliche negative Auswirkungen des Glücksspiels zu minimieren. Wir hoffen, dass andere Online-Glücksspielseiten diesem Beispiel folgen und ebenfalls solche Maßnahmen einführen, um die Sicherheit und das Wohlbefinden ihrer Spieler zu gewährleisten.
https://zetcasino.one/
1. Почему берцы – это обязательный элемент стиля?
2. Как выбрать идеальные берцы для осеннего гардероба?
3. Тренды сезона: кожаные берцы или замшевые?
4. 5 способов носить берцы с платьем
5. Какие берцы выбрать для повседневного образа?
6. Берцы на платформе: комфорт и стиль в одном
7. Какие берцы будут актуальны в этом году?
8. Маст-хэв сезона: военные берцы в стиле милитари
9. 10 вариантов сочетания берцов с джинсами
10. Зимние берцы: как выбрать модель для холодного сезона
11. Элегантные берцы на каблуке: идеальный вариант для офиса
12. Секреты ухода за берцами: как сохранить первоначальный вид?
13. С какой юбкой носить берцы: советы от стилистов
14. Как подобрать берцы под фасон брюк?
15. Берцы на шнуровке: стильный акцент в образе
16. Берцы-челси: универсальная модель для любого стиля
17. С чем носить берцы на плоской подошве?
18. Берцы с ремешками: акцент на деталях
19. Как выбрать берцы для прогулок по городу?
20. Топ-5 брендов берцев: качество и стиль в одном
купити берці зсу бєрци зсу .
Tipico Casino Fehler 50202
Das Tipico Casino ist eine beliebte Online-Glücksspielplattform, auf der Spieler aus der ganzen Welt ihre Lieblingsspiele spielen können. Wie bei jeder anderen Webseite kann es jedoch zu gelegentlichen technischen Problemen kommen. Eines dieser Probleme, das viele Spieler erlebt haben, ist der Fehler 50202.
Der Fehler 50202 tritt normalerweise auf, wenn die Tipico Casino-Webseite Гјberlastet ist oder Probleme mit dem Server auftreten. Dies kann frustrierend sein, da Spieler daran gehindert werden, ihre Lieblingsspiele zu spielen oder auf ihre Kontoinformationen zuzugreifen.
Wenn Sie den Fehler 50202 auf der Tipico Casino-Webseite sehen, gibt es einige Schritte, die Sie unternehmen können, um das Problem zu lösen. Zunächst einmal sollten Sie sicherstellen, dass Ihre Internetverbindung stabil ist und Sie eine gute WLAN-Verbindung haben. Wenn dies der Fall ist, können Sie versuchen, die Webseite neu zu laden oder Ihren Browserverlauf und Cookies zu löschen.
Wenn das Problem weiterhin besteht, empfehlen wir Ihnen, den Tipico Casino-Kundendienst zu kontaktieren. Die Mitarbeiter sind in der Regel gut ausgebildet und können Ihnen bei der Behebung des Fehlers 50202 helfen.
Insgesamt ist der Fehler 50202 im Tipico Casino zwar ärgerlich, aber in der Regel einfach zu beheben. Indem Sie die oben genannten Schritte befolgen und den Kundendienst kontaktieren, sollten Sie in kürzester Zeit wieder online spielen können.
https://tipicocasino.one/
synthesis a-pvp
Der Boomerang Casino Bonus Code
Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und großzügigen Bonusangeboten für seine Spieler anbietet. Einer der populärsten Bonuscodes, den Spieler verwenden können, um von zusätzlichen Belohnungen zu profitieren, ist der Boomerang Casino Bonus Code.
Der Boomerang Casino Bonus Code kann von neuen Spielern verwendet werden, um einen Willkommensbonus in Form von Freispielen oder zusätzlichem Spielgeld bei der Registrierung zu erhalten. Dieser Bonus ist eine großartige Möglichkeit, das Casino kennenzulernen und seine Lieblingsspiele zu spielen, ohne dabei das eigene Budget zu strapazieren.
Darüber hinaus bietet Boomerang Casino seinen bestehenden Spielern regelmäßig Bonuscodes an, die ihnen zusätzliche Belohnungen wie Reload-Boni, Cashback-Angebote und Freispiele für bestimmte Spiele bieten. Diese Codes können auf der Website des Casinos oder durch Abonnieren des Newsletters des Casinos erhalten werden.
Es ist wichtig zu beachten, dass Bonuscodes oft mit bestimmten Bedingungen und Durchspielanforderungen verbunden sind, die Spieler erfüllen müssen, um ihre Gewinne auszahlen zu können. Es ist daher ratsam, die Geschäftsbedingungen sorgfältig zu lesen, bevor man einen Bonuscode verwendet.
Insgesamt ist der Boomerang Casino Bonus Code eine tolle Möglichkeit für Spieler, zusätzliche Belohnungen und Vorteile zu genießen, während sie ihre Lieblingsspiele im Casino spielen. Also, verpassen Sie nicht die Gelegenheit, Ihren Bonuscode zu nutzen und noch mehr Spaß und Spannung im Boomerang Casino zu erleben. Viel Glück und viel Spaß beim Spielen!
https://boomerangcasino.one/
Zet Casino: Ein Online-Casino ohne Einzahlung
Online-Casinos erfreuen sich immer größerer Beliebtheit und bieten Spielern die Möglichkeit, bequem von zuhause aus ihr Glück zu versuchen. Ein interessanter Anbieter in diesem Bereich ist das Zet Casino, welches nicht nur eine Vielzahl von Spielen, sondern auch ein großzügiges Bonusangebot bietet.
Besonders ansprechend ist die Tatsache, dass man im Zet Casino auch ohne Einzahlung spielen kann. Dies bedeutet, dass man sich nicht unbedingt Geld auf sein Konto einzahlen muss, um die verschiedenen Spiele auszuprobieren. Dies ist vor allem für Neueinsteiger in die Welt der Online-Casinos interessant, die zunächst einmal testen möchten, ob ihnen das Spielen in einem solchen Umfeld überhaupt liegt.
Das Zet Casino bietet eine breite Auswahl an Spielen, darunter Slots, Roulette, Blackjack und viele weitere. Zudem gibt es regelmäßig Aktionen und Promotionen, bei denen man zusätzliche Boni oder Freispiele erhalten kann. Auch das Treueprogramm des Casinos belohnt regelmäßige Spieler mit verschiedenen Vergünstigungen.
Um im Zet Casino ohne Einzahlung spielen zu können, muss man sich lediglich auf der Webseite anmelden und ein Konto erstellen. Anschließend kann man sofort mit dem Spielen beginnen und das aufregende Casino-Erlebnis genießen.
Alles in allem ist das Zet Casino eine empfehlenswerte Option für alle, die gerne online spielen, aber keine Einzahlung tätigen möchten. Mit seinem vielfältigen Spielangebot, attraktiven Boni und einem benutzerfreundlichen Interface bietet das Zet Casino eine unterhaltsame und spannende Spielerfahrung für alle Casino-Liebhaber.
https://zetcasino.one/
מושלמת. כל הדירות הדיסקרטיות מתוחזקות ומנוקות בצורה יסודית בכל פעם שהזוגות שירותי ליווי הכוללים מגוון עיסויים ארוטיים, בודי מסאז’, בילויים חברתיים במסיבות ואירועים ועוד שירותי ליווי כיד הדמיון הטובה את חלומכם, רחוק מכולם ואינטימי במיוחד. גברים רבים דירות דיסקרטיות אתיופיות
חשוב לברר כל פרט ופרט מהמחיר ועד לתנאי במקום. יש לציין כי יש גם דירות דיסקרטיות ברמלה שם מחכות לכם בחורות דירות דיסקרטיות במרכז, חדרים לפי שעה במרכז, נערות ליווי במרכז ושירותי ליווי במרכז ממשיך לצמוח ולהתפתח יותר ויותר. כתוצאה מכך, כולן מחכות רק לשיחת טלפון All benefits of Israeli escort services
Gogo Casino Email
Gogo Casino är ett populärt online casino som erbjuder ett brett utbud av spel och generösa bonusar till sina spelare. För att hålla sina kunder informerade om de senaste erbjudandena och kampanjerna, skickar Gogo Casino regelbundet ut e-postmeddelanden till sina registrerade medlemmar.
Genom att prenumerera på Gogo Casinos e-postlista kan spelarna få exklusiva erbjudanden, bonusar och nyheter direkt i sin inkorg. Meddelandena kan inkludera allt från free spins och insättningsbonusar till information om kommande turneringar och tävlingar.
Det är enkelt att registrera sig för Gogo Casinos e-postlista. Besök bara deras webbplats och fyll i dina uppgifter för att bli en del av deras e-postutskick. Du kan också välja att inte ta emot e-postmeddelanden genom att avmarkera den relevanta rutan vid registreringen.
Genom att prenumerera på Gogo Casinos e-postlista kan du hålla dig uppdaterad om de senaste kampanjerna och erbjudandena. Missa inte chansen att vinna stora priser och få bonusar genom att hålla ett öga på din inkorg för de senaste e-postmeddelandena från Gogo Casino. Lycka till!
https://gogocasino.one
Boomerang Casino Bewertungen
Boomerang Casino ist eine beliebte Online-Spielplattform, die eine Vielzahl von Spielen fГјr Spieler aller Altersgruppen anbietet. Von Slots Гјber Tischspiele bis hin zu Live-Casino-Spielen gibt es hier fГјr jeden etwas. Doch wie schneidet das Boomerang Casino in den Bewertungen der Spieler ab?
Insgesamt erfreut sich das Boomerang Casino groГџer Beliebtheit bei den Spielern. Viele loben die groГџe Auswahl an Spielen und die Benutzerfreundlichkeit der Plattform. Einige der beliebtesten Spiele im Boomerang Casino sind Book of Dead, Starburst und Gonzo’s Quest. Die Grafiken und Soundeffekte sind von hoher QualitГ¤t und sorgen fГјr ein einzigartiges Spielerlebnis.
Auch der Kundenservice von Boomerang Casino wird von den Spielern positiv bewertet. Der Support ist rund um die Uhr erreichbar und steht den Spielern bei Fragen oder Problemen zur Seite. Die Mitarbeiter sind freundlich und kompetent und helfen den Spielern schnell und unkompliziert weiter.
Ein weiterer Pluspunkt ist das Bonussystem von Boomerang Casino. Neue Spieler erhalten einen großzügigen Willkommensbonus und regelmäßige Spieler können von verschiedenen Promotionen und Aktionen profitieren. Dies sorgt für zusätzlichen Spielspaß und bietet den Spielern die Möglichkeit, ihre Gewinne zu maximieren.
In den Bewertungen wird auch die Sicherheit und Fairness von Boomerang Casino hervorgehoben. Die Plattform verfügt über eine gültige Glücksspiellizenz und alle Spiele werden regelmäßig von unabhängigen Behörden überprüft. Dadurch können die Spieler sicher sein, dass ihre persönlichen Daten geschützt sind und die Spiele fair ablaufen.
Alles in allem kann das Boomerang Casino mit seinem breiten Spielangebot, dem guten Kundenservice und den attraktiven Boni überzeugen. Die positiven Bewertungen der Spieler unterstreichen die Qualität der Plattform und machen Boomerang Casino zu einer lohnenswerten Option für alle, die gerne online spielen.
Wenn Sie also auf der Suche nach einem zuverlässigen und unterhaltsamen Online-Casino sind, sollten Sie Boomerang Casino definitiv eine Chance geben. Vielleicht gehören auch Sie schon bald zu den zufriedenen Spielern, die Boomerang Casino in ihren Bewertungen loben. Viel Spaß und viel Glück!
https://boomerangcasino.one/
לממש את החלום שלכם, ניתן כיום להיכנס לפורטלים הרבים ברשת, לקבל את המידע מבעוד מועד, לדבר עם אחת מהנערות שבחרתם או מנציגי יותר בנות שמשחקות אותה קשות להשגה? הגעת למקום הנכון! שירותי ליווי בצפון פזורים בכל רחבי הערים המרכזיות ועד האזורים הנידחים ביותר Tel Aviv escorts services for men seeking love
אמתי עד אובדן חושים. לאחר יום עמוס אירועים ולחצים בחיינו גברים רבים מחפשים פורקן לרוב תלוי רק בכם. כאן תוכל למצוא מגוון רחב של דירות סקס בהרצליה והסביבה כולל כתובות, טלפונים וניווט שיביא אתכם היישר לעונג. בטח עלה בתוכה מגוון בחורות נאות וחטובות מאפשרת לכם סקס דירות
Gogo casino är en populär online casinosida som erbjuder ett brett utbud av spel och underhållning för sina spelare. Med en stilren och användarvänlig design lockar sidan till sig både erfarna spelare och nybörjare.
En av de mest spännande funktionerna på Gogo casino är deras flashback-funktion, som ger spelarna möjligheten att återuppleva sina favoritspel och vinster. Genom att klicka på flashback-knappen kan spelare se en sammanfattning av sina tidigare spel och resultat, vilket kan vara till stor hjälp för att få en överblick över ens spelhistorik och strategi.
Flashback-funktionen på Gogo casino är också ett utmärkt sätt att uppmuntra spelarna att återvända till sidan och prova sina favoritspel igen. Genom att se sitt tidigare resultat kan spelarna få ny insikt och inspiration till hur de kan förbättra sina spelstrategier och öka sina vinstchanser.
Utöver flashback-funktionen erbjuder Gogo casino också generösa bonusar och kampanjer för sina spelare, vilket gör upplevelsen på sidan ännu mer spännande och lönsam. Med ett stort utbud av spelautomater, bordsspel och live casino-spel finns det något för alla smaker och preferenser på Gogo casino.
Sammanfattningsvis är Gogo casino en modern och framstående online casinosida som erbjuder underhållning och spänning för alla typer av spelare. Med sin innovativa flashback-funktion och generösa bonusar är det lätt att förstå varför sidan har blivit så populär bland svenska spelare. Besök Gogo casino idag och ta del av allt det roliga och spännande som sidan har att erbjuda!
https://gogocasino.one
Im Jahr 2022 bietet das Boomerang Casino spannende No Deposit Bonus Codes für alle Neukunden an. Mit diesen Codes können Spieler ohne vorherige Einzahlung eine Vielzahl von Casino-Spielen ausprobieren und dabei echtes Geld gewinnen.
No Deposit Bonus Codes sind eine großartige Möglichkeit, um ein Online-Casino kennenzulernen, ohne dabei eigenes Geld riskieren zu müssen. Mit den Codes können Spieler verschiedene Spiele wie Slots, Roulette, Blackjack oder Poker ausprobieren und ihre Gewinnchancen testen.
Um von den No Deposit Bonus Codes im Boomerang Casino zu profitieren, müssen Spieler lediglich ein Konto erstellen und den entsprechenden Code bei der Registrierung eingeben. Anschließend können sie sofort mit dem Spielen beginnen und sich über mögliche Gewinne freuen.
Es ist jedoch wichtig zu beachten, dass No Deposit Boni oft bestimmten Umsatzbedingungen unterliegen, die erfüllt werden müssen, bevor eine Auszahlung möglich ist. Daher sollten Spieler immer die Bonusbedingungen sorgfältig durchlesen, um Missverständnisse zu vermeiden.
Insgesamt bietet das Boomerang Casino mit seinen No Deposit Bonus Codes eine tolle Gelegenheit, um das Casino und seine Spiele risikofrei kennenzulernen und vielleicht sogar den ein oder anderen Gewinn zu erzielen. Wer also auf der Suche nach einem spannenden Online-Casino-Erlebnis ist, sollte die No Deposit Bonus Codes im Boomerang Casino auf jeden Fall ausprobieren. Viel SpaГџ und viel GlГјck beim Spielen!
https://boomerangcasino.one/
Behöver du komma i kontakt med Gogo Casino för att få svar på dina frågor eller lösa eventuella problem? Ingen fara, vi har svaret åt dig!
Gogo Casino är en populär online spelplattform som erbjuder ett brett utbud av casinospel och underhållning för alla spelentusiaster. Om du har några frågor angående deras tjänster, bonusar eller vill rapportera ett tekniskt problem, finns det flera sätt att komma i kontakt med deras kundtjänst.
Det enklaste sättet att nå Gogo Casino är genom deras livechattfunktion på deras hemsida. Genom att klicka på livechattikonen kan du kommunicera direkt med en supportagent som kommer att kunna hjälpa dig med dina frågor omedelbart. Livechatten är tillgänglig under de flesta timmar på dygnet för att ge dig den bästa servicen.
Om du föredrar att kommunicera via e-post, kan du skicka ditt meddelande till deras kundtjänst via deras e-postadress som du hittar på deras hemsida. De brukar svara på e-postmeddelanden inom 24 timmar under arbetsdagar.
Du kan ocksГҐ nГҐ Gogo Casino genom deras sociala medier kanaler som Facebook och Twitter. MГҐnga spelare har haft framgГҐng med att skicka meddelanden till dem via sociala medier och fГҐ svar snabbt.
Oavsett vilket sätt du väljer att kontakta Gogo Casino på, kan du vara säker på att deras kundtjänst är dedikerad att ge dig den bästa hjälpen och supporten för en optimal spelupplevelse. Så tveka inte att nå ut till dem om du behöver hjälp, de är där för att göra din spelupplevelse så bra som möjligt!
https://gogocasino.one
Im Tipico Casino können Spieler sich auf viele spannende Spiele und lukrative Bonusangebote freuen. Besonders attraktiv ist der Tipico Casino No Deposit Bonus, der es Spielern ermöglicht, ganz ohne Einzahlung echtes Geld zu gewinnen.
Der No Deposit Bonus von Tipico Casino ist eine großartige Möglichkeit, um das Casino risikofrei und ohne finanzielles Risiko kennenzulernen. Spieler erhalten bei der Registrierung einen bestimmten Betrag vom Casino geschenkt, den sie dann für verschiedene Spiele im Casino nutzen können. Einmalige Gewinne aus diesem Bonus können sich die Spieler anschließend auszahlen lassen.
Der Tipico Casino No Deposit Bonus ist jedoch an bestimmte Bedingungen geknüpft. Bevor Gewinne aus dem Bonus ausgezahlt werden können, müssen Spieler den Betrag oft genug umsetzen. Außerdem gelten bestimmte Spieleinschränkungen und Zeitlimits für die Erfüllung der Umsatzbedingungen.
Trotz dieser Einschränkungen bietet der No Deposit Bonus von Tipico Casino eine tolle Möglichkeit, um das Casino und seine Spiele auszuprobieren. Mit etwas Glück können Spieler so sogar echte Gewinne erzielen, ohne dabei eigenes Geld einzahlen zu müssen.
Alles in allem ist der Tipico Casino No Deposit Bonus eine lohnenswerte Möglichkeit für Spieler, um das Casino zu entdecken und tolle Gewinne abzusahnen. Interessierte sollten sich jedoch vorab die Bonusbedingungen genau durchlesen, um sicherzustellen, dass sie die Anforderungen erfüllen und den Bonus optimal nutzen können.
https://tipicocasino.one/
Das Boomerang Casino ist eine aufstrebende Online-GlГјcksspielplattform, die sich durch groГџzГјgige Boni und attraktive Aktionen auszeichnet. Eines der beliebtesten Angebote fГјr neue Spieler ist der sogenannte “no deposit bonus”, bei dem man eine bestimmte Geldsumme oder Freispiele erhГ¤lt, ohne dass eine Einzahlung erforderlich ist.
Der Boomerang Casino No Deposit Bonus ist eine großartige Möglichkeit, das Casino risikofrei auszuprobieren und erste Gewinne zu erzielen, ohne eigenes Geld einzahlen zu müssen. Diese Boni sind in der Regel mit bestimmten Umsatzbedingungen verbunden, die erfüllt werden müssen, bevor Gewinne ausgezahlt werden können. Dennoch bieten sie eine gute Gelegenheit, um das Casino und die angebotenen Spiele kennenzulernen.
Um den Boomerang Casino No Deposit Bonus zu erhalten, müssen Spieler sich lediglich auf der Plattform registrieren und den Bonus in Anspruch nehmen. Dies kann in Form eines Gutscheincodes oder automatisch bei der Anmeldung erfolgen. Es ist jedoch wichtig, die genauen Bonusbedingungen zu lesen, um Missverständnisse zu vermeiden und sicherzustellen, dass alle Voraussetzungen erfüllt werden.
Insgesamt ist der Boomerang Casino No Deposit Bonus eine attraktive Möglichkeit, um kostenlos in die Welt des Online-Glücksspiels einzutauchen und erste Erfahrungen zu sammeln. Mit etwas Glück kann man dabei sogar erste Gewinne erzielen und das Spielerlebnis noch spannender gestalten. Wer also auf der Suche nach einem neuen Online-Casino mit lukrativen Bonusangeboten ist, sollte das Boomerang Casino definitiv in Betracht ziehen.
https://boomerangcasino.one/
synthesis a-pvp
https://www.khedmeh.com/wall/blogs/post/51719
synthesis a-pvp
https://dictanote.co/n/975997/
In der Welt der Online-Casinos gibt es viele verschiedene Aspekte, die Spieler berücksichtigen müssen, bevor sie sich für eine Plattform entscheiden. Einer der wichtigsten Faktoren ist die Auszahlungsdauer, also die Zeit, die benötigt wird, um Gewinne auf das eigene Konto zu überweisen.
Eines der Casinos, das in Bezug auf die Auszahlungsdauer positiv aufgefallen ist, ist das Zet Casino. Dieses Online-Casino hat sich einen guten Ruf für schnelle und zuverlässige Auszahlungen erarbeitet. In der Regel dauert es nur wenige Stunden bis maximal zwei Tage, bis die Gewinne auf das Konto des Spielers überwiesen werden.
Die Auszahlungsdauer kann jedoch von verschiedenen Faktoren abhängig sein. Zum Beispiel können Auszahlungen aufgrund von Sicherheitsüberprüfungen oder der Wahl der Zahlungsmethode länger dauern. Es ist daher ratsam, sich im Voraus über die verschiedenen Zahlungsmethoden und deren entsprechende Auszahlungsdauer zu informieren.
Das Zet Casino bietet seinen Spielern eine Vielzahl von Zahlungsmethoden, darunter Kreditkarten, E-Wallets und Banküberweisungen. Spieler können die Methode auswählen, die ihren Bedürfnissen am besten entspricht, und sich darauf verlassen, dass ihre Gewinne schnell und sicher ausgezahlt werden.
Insgesamt kann das Zet Casino in Bezug auf die Auszahlungsdauer als zuverlässiger und effizienter Anbieter bezeichnet werden. Spieler können sich darauf verlassen, dass ihre Gewinne schnell auf ihr Konto überwiesen werden, damit sie ihr Geld schnell und unkompliziert erhalten können.
https://zetcasino.one/
Zet Casino ist ein Online-Casino, das seinen Spielern eine Vielzahl von spannenden Spielen und attraktiven Bonusangeboten bietet. Eines der beliebtesten Angebote des Casinos ist das sogenannte “ei talletuskasino”, was auf Finnisch “keine Einzahlung erforderlich” bedeutet.
Bei Zet Casino kann man also spielen, ohne zuerst eine Einzahlung tГ¤tigen zu mГјssen. Dies ist besonders attraktiv fГјr Spieler, die das Casino erst einmal ausprobieren mГ¶chten, ohne gleich ihr eigenes Geld riskieren zu mГјssen. Durch das “ei talletuskasino” Angebot kГ¶nnen sie sich in Ruhe mit den Spielen vertraut machen und die verschiedenen Funktionen des Casinos testen.
Darüber hinaus bietet Zet Casino auch eine Vielzahl von anderen Bonusangeboten und Aktionen für seine Spieler an. Dazu gehören unter anderem Willkommensboni, Freispiele und Cashback-Angebote. Mit diesen Boni haben die Spieler die Möglichkeit, ihre Gewinne zu maximieren und ihr Spielerlebnis noch aufregender zu gestalten.
Zet Casino ist sowohl für Anfänger als auch für erfahrene Spieler geeignet und bietet ein breites Spektrum an Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr. Das Casino legt großen Wert auf Sicherheit, Fairness und Transparenz und arbeitet ausschließlich mit seriösen Zahlungsanbietern zusammen.
Wer also auf der Suche nach einem erstklassigen Online-Casino ist, das ein “ei talletuskasino” Angebot und viele weitere spannende Features bietet, sollte sich unbedingt einmal bei Zet Casino umschauen. Vielleicht ist das GlГјck ja schon auf Ihrer Seite und Sie kГ¶nnen ohne Einzahlung tolle Gewinne erzielen. Viel SpaГџ beim Spielen und viel GlГјck!
https://zetcasino.one/
Das Boomerang Casino bietet ein einzigartiges Spielerlebnis fГјr alle, die auf der Suche nach SpaГџ und Spannung sind. Mit einer breiten Auswahl an Spielen, groГџzГјgigen Boni und einer benutzerfreundlichen Plattform ist das Casino die perfekte Wahl fГјr alle GlГјcksspiel-Enthusiasten.
Das Boomerang Casino verfГјgt Гјber eine Vielzahl von Slot-Spielen, Tischspielen und Live-Casino-Spielen, die alle von fГјhrenden Softwareanbietern wie NetEnt, Microgaming und Play’n GO bereitgestellt werden. Die Spiele sind sowohl auf Desktop- als auch auf mobilen GerГ¤ten verfГјgbar, sodass die Spieler jederzeit und Гјberall spielen kГ¶nnen.
Neben einer erstaunlichen Spielauswahl bietet das Boomerang Casino auch großzügige Boni und Promotionen. Neue Spieler erhalten einen Willkommensbonus, der ihre erste Einzahlung verdoppelt, sowie Freispiele für ausgewählte Spiele. Darüber hinaus gibt es regelmäßig Aktionen, bei denen die Spieler zusätzliche Boni, Freispiele und sogar Sachpreise gewinnen können.
Die Plattform des Boomerang Casinos ist einfach zu bedienen und bietet eine sichere und zuverlässige Spielumgebung. Die Spieler können Einzahlungen und Auszahlungen schnell und einfach über eine Vielzahl von Zahlungsmethoden vornehmen, darunter Kreditkarten, E-Wallets und Banküberweisungen. Der Kundensupport ist rund um die Uhr verfügbar und steht den Spielern bei Fragen oder Problemen zur Seite.
Insgesamt ist das Boomerang Casino eine hervorragende Wahl fГјr alle, die nach einem unterhaltsamen und lukrativen Spielerlebnis suchen. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Boni und einer benutzerfreundlichen Plattform bietet das Casino alles, was ein GlГјcksspiel-Enthusiast braucht. Besuchen Sie noch heute das Boomerang Casino und erleben Sie die Faszination des GlГјcksspiels!
https://boomerangcasino.one/
It’s going to be ending of mine day, except before finish I am reading this great piece of
writing to improve my know-how. Visit : https://koshka-baskervilley.info
Tipico – Geld vom Casino zum Wetten Гјberweisen
Wenn man gerne im Online-Casino spielt, hat man sicherlich schon einmal von Tipico gehört. Tipico ist nicht nur bekannt für sein umfangreiches Angebot an Casino-Spielen, sondern auch für seine Sportwetten. Viele Spieler nutzen beide Angebote und möchten gerne Geld vom Casino zum Wetten überweisen. Doch wie funktioniert das genau?
Zunächst einmal muss man sich bei Tipico registrieren und ein Konto anlegen. Hat man bereits ein Konto im Casino, kann man dieses auch für die Sportwetten nutzen. Man muss lediglich Geld auf sein Konto einzahlen, um sowohl im Casino als auch bei den Sportwetten spielen zu können.
Um Geld vom Casino zum Wetten zu Гјberweisen, geht man einfach in den Kassenbereich und wГ¤hlt die Option “Geldtransfer”. Hier kann man angeben, wie viel Geld man Гјberweisen mГ¶chte. Das Geld wird dann sofort auf das Wettkonto transferiert und kann fГјr Sportwetten genutzt werden.
Es ist wichtig zu beachten, dass man das Geld nicht direkt vom Casino zum Wetten überweisen kann. Man muss es zuerst auf sein Hauptkonto transferieren und von dort aus auf das Wettkonto überweisen. Dies dient der Sicherheit und soll möglichen Betrugsversuchen vorbeugen.
Wer gerne im Tipico Casino spielt und auch gerne auf Sportereignisse wettet, kann sein Geld ganz einfach vom Casino zum Wetten überweisen. Mit nur wenigen Klicks ist das Geld transferiert und man kann seine Einsätze platzieren. Tipico bietet somit eine bequeme und sichere Möglichkeit, um sowohl im Casino als auch bei den Sportwetten aktiv zu sein.
https://tipicocasino.one/
I’ve been surfing online more than 4 hours today, yet I never found any interesting article like yours. It is pretty worth enough for me. In my opinion, if all web owners and bloggers made good content as you did, the internet will be a lot more useful than ever before.
I’ll immediately seize your rss feed as I can’t find your email subscription link or newsletter service. Do you have any? Please allow me realize so that I may just subscribe. Thanks.
https://sinee1q2x-nebo0x0s-golova2s6f.com
Boomerang Bet Casino Review
Boomerang Bet Casino is a popular online casino that offers a wide range of games for players to enjoy. From slots to table games, there is something for everyone at this casino. In this review, we will take a closer look at what Boomerang Bet Casino has to offer, from its game selection to its customer service.
One of the standout features of Boomerang Bet Casino is its impressive selection of games. With over 1,000 games to choose from, players are guaranteed to find something that suits their tastes. Whether you prefer classic slots or more modern video slots, there is plenty to keep you entertained at Boomerang Bet Casino. The casino also offers a selection of table games, including blackjack, roulette, and poker, as well as a number of live dealer games for those who prefer a more interactive gaming experience.
In addition to its diverse game selection, Boomerang Bet Casino also prides itself on its customer service. The casino offers 24/7 support via live chat, email, and phone, so help is always just a click away. The casino’s friendly and knowledgeable customer service team is always on hand to assist with any questions or concerns that players may have, ensuring that their gaming experience is as smooth and enjoyable as possible.
Boomerang Bet Casino also offers a number of bonuses and promotions to reward loyal players. From welcome bonuses for new players to weekly promotions for existing players, there are plenty of opportunities to increase your winnings at this casino. The casino also offers a VIP program for high rollers, which offers additional perks and rewards for those who spend more time and money at the casino.
Overall, Boomerang Bet Casino is a top choice for online casino players looking for a diverse selection of games, excellent customer service, and generous bonuses and promotions. With its 24/7 support, wide range of games, and rewarding VIP program, Boomerang Bet Casino has something for everyone. So why not give it a try and see what all the fuss is about?
In conclusion, Boomerang Bet Casino is a top-notch online casino that is well worth a visit. With its impressive game selection, excellent customer service, and generous bonuses, there is plenty to enjoy at this casino. Whether you are a seasoned player or new to online gaming, Boomerang Bet Casino has something for everyone. So why not give it a try today and see if you can win big at this exciting online casino?
https://boomerangcasino.one/
Отечественный завод предлагает силовые тренажеры https://trenazher-silovoj.ru/ для напряженной работы в коммерческих тренировочных центрах.
Посмотрите каталог интернет-магазина производимых машин грузоблочных и нагружаемых.
Все модели позволяют прокачивать изолированно любые отделы мышц.
Оформляйте тренажер для плечей, Гакк тренажер, одинарный Кроссовер, Баттерфляй для грудных, машину Смита, горизонтальную тягу, лавку Скотта, Гравитрон для подтягиваний, обратную гиперэкстензию, скамьи для жима со стойками, рычажные модели.
Каждый тренажер ориентирован для тренирующихся с разным уровнем физической активности.
Изготавливаемое оборудование полностью безупречно и не нуждается в техническом наблюдении.
Закажите стек с плитками нужной нагрузки.
Die tipico Casino App fГјr Android – Spannung und SpaГџ auf Ihrem Smartphone
Das tipico Casino bietet eine Vielzahl von Spielmöglichkeiten, von Slots über Tischspiele bis hin zu Live-Casino-Spielen. Mit der tipico Casino App können Sie all diese Spiele auch bequem auf Ihrem Android-Smartphone genießen.
Die App ist kostenlos und einfach zu bedienen. Sie können sich ganz einfach mit Ihrem tipico Konto anmelden und haben sofort Zugriff auf eine große Auswahl an Spielen. Die App bietet eine benutzerfreundliche Oberfläche und ermöglicht es Ihnen, Ihre Lieblingsspiele schnell zu finden und zu spielen.
Dank der mobilen App können Sie jederzeit und überall auf Ihre Lieblingsspiele zugreifen. Egal, ob Sie zu Hause auf der Couch sitzen oder unterwegs sind, mit der tipico Casino App haben Sie immer die Möglichkeit, ein paar Runden an Ihren Lieblingsspielen zu drehen.
Die tipico Casino App bietet auch regelmäßig spannende Aktionen und Bonusangebote für die Spieler an. So können Sie noch mehr Spaß haben und Ihre Gewinnchancen erhöhen.
Also, wenn Sie ein Fan von Casino-Spielen sind und ein Android-Smartphone besitzen, sollten Sie die tipico Casino App auf jeden Fall ausprobieren. Laden Sie die App einfach im Google Play Store herunter und tauchen Sie ein in die aufregende Welt des tipico Casinos. Viel SpaГџ und viel GlГјck beim Spielen!
https://tipicocasino.one/
Zet Casino Bewertungen
Zet Casino ist eine beliebte Online-Glücksspielseite, die eine Vielzahl von Spielen und großzügigen Bonusangeboten für Spieler auf der ganzen Welt anbietet. Wie bei den meisten Online-Casinos gibt es auch bei Zet Casino eine Vielzahl von Bewertungen, die sowohl positiv als auch negativ ausfallen können.
In den positiven Bewertungen wird oft die große Auswahl an Spielen und die benutzerfreundliche Website des Casinos hervorgehoben. Spieler loben auch die schnellen Auszahlungen und den effizienten Kundenservice, der rund um die Uhr verfügbar ist. Viele Spieler genießen auch die regelmäßigen Bonusangebote und Aktionen, die Zet Casino anbietet.
Auf der anderen Seite gibt es auch negative Bewertungen, die einige Spieler hinterlassen haben. Einige Benutzer haben sich Гјber langsame Auszahlungen oder unklare Bonusbedingungen beschwert. Ein weiterer Kritikpunkt ist die begrenzte Auswahl an Zahlungsmethoden, die das Casino akzeptiert.
Insgesamt scheint Zet Casino jedoch bei den meisten Spielern gut anzukommen. Die überwiegende Mehrheit der Bewertungen ist positiv, und viele Spieler haben Spaß und profitieren von ihrer Erfahrung im Casino. Wie bei allen Online-Casinos ist es jedoch ratsam, vorsichtig zu sein und die Geschäftsbedingungen sorgfältig zu lesen, bevor man sich anmeldet und spielt.
Wenn Sie also nach einem unterhaltsamen und zuverlässigen Online-Casino suchen, könnte Zet Casino die richtige Wahl für Sie sein. Mit einer großen Auswahl an Spielen, großzügigen Bonusangeboten und einem effizienten Kundenservice bietet das Casino eine angenehme Spielerfahrung für diejenigen, die ihr Glück online versuchen möchten.
https://zetcasino.one/
לעיר. בעבר זוגות וכאלה שהיו רוצים להתבודד באזור היו נוסעים ליער בן שמן עם צוות המקום. הנגישות והחניות לדירות זמינות והמיקום פשוט נוח. לאור ההתפתחות הגדולה של ענף הדירות הדיסקרטיות שמציע מבחר גדול של מהדירות תוכל לבחור שתמתין לך בחורה נאה אשר תעניק לך דירות דיסקרטיות בקריות
Zet Casino Erfahrung
Zet Casino ist eine Online-Spielplattform, die eine Vielzahl von Spielen fГјr alle Arten von Spielern anbietet. Ob Slots, Tischspiele oder Live-Casino – hier findet jeder etwas nach seinem Geschmack. In diesem Artikel mГ¶chten wir unsere Erfahrung mit Zet Casino teilen und Ihnen einen Гњberblick Гјber die Plattform geben.
Zet Casino bietet eine breite Auswahl an Spielen von namhaften Anbietern wie NetEnt, Microgaming, Pragmatic Play und vielen mehr. Die Spiele sind gut strukturiert und einfach zu finden, sodass Sie nicht lange nach Ihrem Lieblingsspiel suchen müssen. Die Benutzeroberfläche ist benutzerfreundlich und intuitiv, so dass auch Anfänger sich schnell zurechtfinden können.
Ein besonderes Highlight bei Zet Casino sind die regelmäßigen Aktionen und Bonusangebote. Es gibt einen großzügigen Willkommensbonus für neue Spieler sowie verschiedene Reload-Boni, Freispiele und Cashback-Angebote. Dies sorgt für zusätzlichen Spaß und Spannung beim Spielen.
Ein weiterer Pluspunkt von Zet Casino ist der Kundenservice. Das Team ist rund um die Uhr per Live-Chat, E-Mail und Telefon erreichbar und steht Ihnen bei Fragen und Problemen zur VerfГјgung. Die Mitarbeiter sind freundlich, kompetent und helfen Ihnen schnell und unkompliziert weiter.
Insgesamt sind wir von unserer Erfahrung mit Zet Casino sehr positiv beeindruckt. Die Plattform bietet eine große Auswahl an Spielen, attraktive Bonusangebote und einen exzellenten Kundenservice. Wir können Zet Casino daher allen Spielern, die nach einer seriösen und unterhaltsamen Online-Spielumgebung suchen, wärmstens empfehlen.
Fazit: Zet Casino überzeugt mit einer vielfältigen Spielauswahl, lukrativen Bonusangeboten und einem erstklassigen Kundenservice. Wir hatten eine tolle Zeit beim Spielen und können die Plattform uneingeschränkt empfehlen. Probieren Sie es selbst aus und erleben Sie den Spaß und die Spannung bei Zet Casino!
https://zetcasino.one/
Профессиональная стирка ковров в Челябинске — вот что мы делаем лучше всего! Обращайтесь к нам и убедитесь сами. Клининговая уборка квартир
получить микрозайм
https://www.libertaddigital.com/chic/entretenimiento/2016-09-21/fan-bingbing-las-increibles-cifras-alrededor-de-la-mayor-estrella-china-1276582941/
Das Zet Casino ist eine beliebte Online-GlГјcksspielseite, die eine Vielzahl von Spielen fГјr Spieler aus der ganzen Welt anbietet. Eine wichtige Frage, die viele Spieler stellen, ist die Lizenzierung des Casinos. In diesem Artikel werden wir genauer untersuchen, welche Lizenz das Zet Casino besitzt und was dies fГјr die Spieler bedeutet.
Das Zet Casino wird von der Firma Araxio Development N.V. betrieben und verfügt über eine Glücksspiellizenz der Regierung von Curacao. Die Curacao e-Gaming-Lizenz gilt als eine der angesehensten Lizenzen in der Online-Glücksspielbranche und stellt sicher, dass das Casino strenge Richtlinien einhält, um Fairness, Sicherheit und Transparenz für die Spieler zu gewährleisten.
Durch die Lizenzierung beim Zet Casino können die Spieler sicher sein, dass das Casino regelmäßig von unabhängigen Behörden überprüft wird, um sicherzustellen, dass alle Spiele fair und zufällig sind. Dies gibt den Spielern ein Gefühl von Vertrauen und Sicherheit, wenn sie im Zet Casino spielen.
Darüber hinaus bedeutet die Lizenzierung auch, dass das Casino die Datenschutz- und Sicherheitsmaßnahmen einhält, um sicherzustellen, dass persönliche Daten der Spieler geschützt sind und alle Transaktionen sicher abgewickelt werden.
Zusammenfassend lässt sich sagen, dass das Zet Casino über eine angesehene Glücksspiellizenz der Regierung von Curacao verfügt, die für Fairness, Sicherheit und Transparenz im Casino sorgt. Spieler können somit beruhigt sein, dass sie in einem seriösen und vertrauenswürdigen Online-Casino spielen.
https://zetcasino.one/
Boomerang Casino Einzahlung
Das Boomerang Casino ist ein beliebtes Online-Casino, das seinen Spielern eine Vielzahl von spannenden Spielen und attraktiven Boni bietet. Einer der wichtigsten Aspekte des Online-GlГјcksspiels ist die Einzahlung von Geld auf das Spielerkonto. Im folgenden Artikel werden wir uns genauer mit der Boomerang Casino Einzahlung befassen.
Um Geld auf Ihr Boomerang Casino Konto einzuzahlen, stehen Ihnen verschiedene Zahlungsmethoden zur Verfügung. Dazu gehören gängige Optionen wie Kreditkarten, E-Wallets und verschiedene Banküberweisungsmethoden. Es ist wichtig, eine Methode zu wählen, die für Sie bequem und sicher ist, damit Sie Ihr Spielerkonto schnell aufladen können.
Um eine Einzahlung im Boomerang Casino vorzunehmen, müssen Sie sich zunächst in Ihr Spielerkonto einloggen und den Einzahlungsbereich aufrufen. Dort können Sie die gewünschte Zahlungsmethode auswählen und den Betrag eingeben, den Sie einzahlen möchten. Vergewissern Sie sich, dass Sie die angegebenen Informationen korrekt eingeben, um mögliche Verzögerungen oder Probleme zu vermeiden.
Nachdem Sie die Einzahlung abgeschlossen haben, wird das Geld in der Regel innerhalb weniger Minuten auf Ihrem Spielerkonto gutgeschrieben. Sie können dann mit dem Spielen Ihrer Lieblingsspiele im Boomerang Casino beginnen und hoffentlich den Jackpot knacken!
Es ist wichtig zu beachten, dass das Boomerang Casino verschiedene Bedingungen und Umsatzanforderungen für Boni und Einzahlungen hat. Bevor Sie eine Einzahlung vornehmen, empfehlen wir Ihnen daher, die Allgemeinen Geschäftsbedingungen sorgfältig zu lesen, um sicherzustellen, dass Sie die Regeln des Casinos einhalten.
Insgesamt bietet das Boomerang Casino eine sichere und zuverlässige Plattform für Online-Glücksspiele. Mit einer Vielzahl von Spielen, attraktiven Boni und einer einfachen Einzahlungsprozess ist es eine gute Wahl für alle, die gerne online spielen. Probieren Sie es aus und erleben Sie den Nervenkitzel des Boomerang Casinos!
https://boomerangcasino.one/
Tipico Casino Chips Blockiert: Was ist zu tun?
Wenn Sie ein Spieler im Tipico Casino sind und plötzlich feststellen, dass Ihre Casino Chips blockiert sind, kann das sehr frustrierend sein. Doch keine Sorge, es gibt einige Schritte, die Sie unternehmen können, um das Problem zu lösen.
Zunächst einmal sollten Sie überprüfen, ob Sie möglicherweise die Bonusbedingungen des Casinos nicht erfüllt haben. Oftmals werden Casino Chips blockiert, wenn Sie versuchen, Gewinne aus einem Bonus ohne Einzahlung abzuheben, ohne die entsprechenden Umsatzanforderungen erfüllt zu haben.
In diesem Fall empfehlen wir Ihnen, Kontakt mit dem Kundensupport von Tipico aufzunehmen. Die Mitarbeiter können Ihnen weiterhelfen und das Problem genauer überprüfen. Möglicherweise müssen Sie zusätzliche Dokumente zur Verifizierung einreichen, um die Blockierung aufzuheben.
Es ist auch möglich, dass Ihre Casino Chips aus Sicherheitsgründen blockiert wurden. Dies kann beispielsweise der Fall sein, wenn ungewöhnliche Aktivitäten auf Ihrem Konto festgestellt werden. In einem solchen Fall ist es wichtig, sich mit dem Kundensupport in Verbindung zu setzen und alle erforderlichen Schritte zur Verifizierung durchzuführen.
Zusammenfassend lässt sich sagen, dass eine Blockierung von Casino Chips im Tipico Casino ärgerlich sein kann, aber in den meisten Fällen gibt es eine Lösung. Nehmen Sie Kontakt mit dem Kundensupport auf, um das Problem zu klären und Ihre Chips freizuschalten.
https://tipicocasino.one/
Zet Casino: 50 Freispiele – Welches Spiel soll ich wГ¤hlen?
Wenn es um Online-Casinos geht, gibt es viele Optionen zur Auswahl. Ein beliebtes Casino, das derzeit Freispiele anbietet, ist das Zet Casino. Mit 50 Freispielen haben Spieler die Möglichkeit, verschiedene Spiele auszuprobieren und ihr Glück zu versuchen. Doch welche Spiele kann man mit diesen Freispielen spielen?
Das Zet Casino bietet eine Vielzahl von Spielen, darunter eine breite Auswahl an Spielautomaten, Tischspielen und Live-Casino-Spielen. Bei den 50 Freispielen kГ¶nnen Spieler aus verschiedenen Spielautomaten wГ¤hlen, die von renommierten Anbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen entwickelt wurden.
Eine beliebte Option fГјr die Verwendung der Freispiele bei Zet Casino sind Spielautomaten wie Starburst, Book of Dead, Gonzo’s Quest oder Wolf Gold. Diese Spiele sind bekannt fГјr ihre unterhaltsamen Themen, spannenden Bonusrunden und hohen Gewinnchancen. Spieler kГ¶nnen mit den Freispielen diese beliebten Slots ausprobieren und sehen, ob sie ihr GlГјck haben.
Für diejenigen, die lieber Tischspiele spielen, bietet das Zet Casino auch eine große Auswahl an Blackjack, Roulette und Baccarat-Optionen. Spieler können mit den Freispielen auch einige dieser Tischspiele ausprobieren und sehen, ob sie das Glück auf ihrer Seite haben.
Für diejenigen, die ein authentisches Casino-Erlebnis bevorzugen, bietet das Zet Casino auch eine Auswahl an Live-Casino-Spielen. Mit den Freispielen haben Spieler die Möglichkeit, Live-Dealer-Spiele wie Live Blackjack, Live Roulette oder Live Baccarat zu spielen und das echte Casino-Feeling zu genießen.
Insgesamt bietet das Zet Casino mit seinen 50 Freispielen eine Vielzahl von SpielmГ¶glichkeiten fГјr alle Arten von Spielern. Egal ob Slot-Fan, Tischspiel-Liebhaber oder Live-Casino-Enthusiast – mit den Freispielen kГ¶nnen Spieler verschiedene Spiele ausprobieren und sehen, welches Spiel ihnen am besten gefГ¤llt und das meiste GlГјck bringt. Also nicht zГ¶gern, sich anzumelden und die 50 Freispiele bei Zet Casino zu nutzen!
https://zetcasino.one/
Tipico Promotion 5 Casino
Tipico ist bekannt für seine großzügigen Promotionen und Bonusangebote für seine Kunden. Eine der neuesten Aktionen ist die Tipico Promotion 5 Casino, die es Spielern ermöglicht, zusätzliche Belohnungen zu erhalten, während sie ihre Lieblingsspiele im Casino spielen.
Die Promotion ist einfach zu nutzen: Spieler müssen lediglich im Aktionszeitraum bestimmte Spiele im Casino von Tipico spielen und bestimmte Bedingungen erfüllen, um sich für die Belohnungen zu qualifizieren. Die Spieler haben die Möglichkeit, zusätzliche Freispiele zu gewinnen, die ihre Chancen auf große Gewinne erhöhen.
Darüber hinaus bietet Tipico regelmäßig verschiedene Aktionen und Bonusangebote für seine Casino-Kunden an. Diese reichen von Einzahlungsboni über Cashback-Angebote bis hin zu exklusiven Turnieren und Verlosungen.
Die Tipico Promotion 5 Casino ist eine großartige Möglichkeit für Spieler, ihre Lieblingsspiele zu genießen und dabei noch zusätzliche Belohnungen zu erhalten. Nutzen Sie also diese Chance und tauchen Sie ein in die aufregende Welt des Tipico Casinos.
https://tipicocasino.one/
Das Boomerang Casino ist eine neue Online-GlГјcksspielplattform, die sich schnell einen Namen in der Welt der Online-Casinos gemacht hat. In diesem Testbericht werden wir einen genaueren Blick auf das Boomerang Casino werfen, um zu sehen, ob es seinen wachsenden Ruf wirklich verdient.
Zunächst einmal fällt auf, dass das Boomerang Casino eine benutzerfreundliche Webseite hat, die sowohl auf dem Computer als auch auf mobilen Geräten gut funktioniert. Die Navigation auf der Seite ist einfach und intuitiv, was es den Spielern ermöglicht, schnell ihr Lieblingsspiel zu finden. Das Casino bietet eine breite Palette von Spielkategorien an, darunter Spielautomaten, Tischspiele, Live-Casino und Jackpot-Spiele.
Besonders beliebt sind die Spielautomaten im Boomerang Casino, da sie von renommierten Softwareanbietern wie NetEnt, Microgaming und Play’n GO bereitgestellt werden. Dadurch ist eine hohe QualitГ¤t und ein unterhaltsames Spielerlebnis garantiert. Die Tischspiele im Boomerang Casino sind ebenfalls vielfГ¤ltig und bieten eine gute Auswahl an klassischen und modernen Spielen.
Ein weiterer Pluspunkt des Boomerang Casinos ist das Live-Casino, in dem Spieler mit echten Dealern in Echtzeit spielen können. Die Atmosphäre ist authentisch und die Spiele werden professionell geleitet, was für ein besonders realistisches Spielerlebnis sorgt. Zudem bietet das Boomerang Casino eine Vielzahl von Zahlungsmethoden an, darunter Kreditkarten, E-Wallets und Banküberweisungen, was es Spielern aus aller Welt leicht macht, Ein- und Auszahlungen vorzunehmen.
Insgesamt hinterlässt das Boomerang Casino einen positiven Eindruck. Die Webseite ist benutzerfreundlich, die Spieleauswahl ist vielfältig und die Zahlungsmethoden sind vielfältig. Das Live-Casino und die Spielautomaten sind besonders empfehlenswert. Wenn Sie auf der Suche nach einem unterhaltsamen und sicheren Online-Casino sind, sollten Sie das Boomerang Casino auf jeden Fall ausprobieren.
https://boomerangcasino.one/
I really loved reading your blog. It was very well authored and easy to understand. Unlike other blogs I have read which are really not that good.Thanks alot!
유흥알바
Das Boomerang Casino ist eine aufstrebende Online-GlГјcksspielplattform, die Spielern eine Vielzahl von Spielen und groГџzГјgigen Boni bietet. Einer der beliebtesten Bonusangebote des Casinos ist der “Bonus bez depozytu”, bei dem Spieler einen Bonus erhalten, ohne eine Einzahlung tГ¤tigen zu mГјssen.
Der Bonus bez depozytu ist eine großartige Möglichkeit für Spieler, das Casino und seine Spiele ohne finanzielles Risiko kennenzulernen. Spieler können mit diesem Bonus verschiedene Spiele ausprobieren und echtes Geld gewinnen, ohne dabei etwas einzahlen zu müssen.
Um den Bonus bez depozytu zu erhalten, müssen Spieler lediglich ein Konto im Boomerang Casino erstellen und den Bonuscode eingeben, der normalerweise auf der Website des Casinos verfügbar ist. Sobald der Bonus aktiviert ist, können Spieler ihn bei ausgewählten Spielen verwenden und damit echtes Geld gewinnen.
Es ist jedoch wichtig zu beachten, dass der Bonus bez depozytu in der Regel bestimmten Umsatzbedingungen unterliegt, die erfüllt werden müssen, bevor Gewinne ausgezahlt werden können. Spieler sollten daher die Geschäftsbedingungen des Bonus sorgfältig durchlesen, um sicherzustellen, dass sie die Anforderungen erfüllen.
Insgesamt ist der Bonus bez depozytu im Boomerang Casino eine großartige Möglichkeit für Spieler, das Casino und seine Spiele ohne finanzielles Risiko zu erleben. Mit diesem Bonus können Spieler verschiedene Spiele ausprobieren und echtes Geld gewinnen, ohne eine Einzahlung tätigen zu müssen. Wer auf der Suche nach einem spannenden und lohnenden Online-Casino-Erlebnis ist, sollte das Boomerang Casino und seinen Bonus bez depozytu in Betracht ziehen.
https://boomerangcasino.one/
Das Zet Casino ist eine Online GlГјcksspielplattform, die ihren Spielern eine breite Palette von Spielen und lukrativen Boni bietet. Einer der beliebtesten Boni, die das Zet Casino seinen Spielern im Jahr 2019 anbietet, ist der sogenannte “No Deposit Bonus”.
Ein No Deposit Bonus ist eine Art von Bonus, der es Spielern ermöglicht, kostenlose Spiele zu spielen, ohne dass sie zuvor eine Einzahlung tätigen müssen. Das bedeutet, dass Spieler die Möglichkeit haben, das Casino kennenzulernen und verschiedene Spiele auszuprobieren, ohne dabei ihr eigenes Geld riskieren zu müssen.
Der No Deposit Bonus im Zet Casino im Jahr 2019 kann je nach Aktion variieren, aber in der Regel erhalten Spieler entweder Freispiele für ausgewählte Slots oder einen bestimmten Geldbetrag, den sie im Casino verwenden können. Durch diesen Bonus haben Spieler die Möglichkeit, echte Gewinne zu erzielen, ohne dabei ihr eigenes Geld riskieren zu müssen.
Um den No Deposit Bonus im Zet Casino zu erhalten, mГјssen Spieler in der Regel einfach ein Konto erstellen und sich anmelden. AnschlieГџend wird der Bonus automatisch gutgeschrieben oder Spieler mГјssen einen Bonuscode eingeben, um den Bonus zu aktivieren.
Es ist jedoch wichtig zu beachten, dass No Deposit Boni in der Regel bestimmten Bedingungen und Umsatzanforderungen unterliegen, die erfüllt werden müssen, bevor Gewinne aus dem Bonus ausgezahlt werden können. Spieler sollten daher die Bonusbedingungen genau lesen, um sicherzustellen, dass sie die Anforderungen erfüllen und echte Gewinne erzielen können.
Insgesamt bietet der No Deposit Bonus im Zet Casino den Spielern eine großartige Möglichkeit, das Casino und seine Spiele kostenlos kennenzulernen und echte Gewinne zu erzielen. Spieler sollten diese Gelegenheit nutzen und den Bonus beanspruchen, um ihre Gewinnchancen zu erhöhen und das Spielerlebnis im Zet Casino zu maximieren.
https://zetcasino.one/
Das Boomerang Casino ist eine beliebte Online-Spielhalle, die eine Vielzahl von Spielen und aufregenden Funktionen fГјr ihre Spieler bietet. Ein wichtiger Aspekt, der die Spieler interessiert, ist die Auszahlungsdauer des Casinos.
Die Auszahlungsdauer im Boomerang Casino hängt von verschiedenen Faktoren ab. Zunächst einmal muss der Spieler sicherstellen, dass er alle erforderlichen Dokumente zur Verifizierung seines Kontos eingereicht hat. Dies ist ein Standardverfahren, das von allen seriösen Online-Casinos durchgeführt wird, um die Sicherheit der Spieler zu gewährleisten.
Sobald das Konto des Spielers verifiziert ist, hängt die tatsächliche Auszahlungsdauer davon ab, welche Zahlungsmethode der Spieler gewählt hat. Einige Zahlungsmethoden wie E-Wallets oder Kreditkarten ermöglichen schnellere Auszahlungen, während Banküberweisungen in der Regel länger dauern können.
In der Regel strebt das Boomerang Casino jedoch an, Auszahlungen so schnell wie möglich zu bearbeiten. Die Auszahlungsdauer kann je nach Zahlungsmethode zwischen 1 und 5 Werktagen liegen. In einigen Fällen kann es jedoch auch schneller gehen.
Es ist wichtig, dass Spieler geduldig sind und verstehen, dass die Auszahlungsdauer von verschiedenen Faktoren abhängt, auf die das Casino möglicherweise keinen Einfluss hat. Wenn ein Spieler Fragen zu seiner Auszahlungsdauer hat, kann er sich jederzeit an den Kundendienst des Boomerang Casinos wenden, der gerne weiterhilft.
Insgesamt kann gesagt werden, dass die Auszahlungsdauer im Boomerang Casino im Vergleich zu anderen Online-Casinos durchaus akzeptabel ist. Spieler können sicher sein, dass ihre Gewinne schnell und sicher ausgezahlt werden, so dass sie ihr Spielerlebnis genießen können, ohne sich über lange Wartezeiten Gedanken machen zu müssen.
https://boomerangcasino.one/
детализация мегафон – карта сбербанка, Paysend Business
юрист в области бизнеса
Wenn Sie gerne online Casinos besuchen und nach einem neuen Anbieter suchen, sollten Sie unbedingt das Zet Casino ausprobieren. Mit seinem breiten Angebot an Spielen und groГџzГјgigen Bonusangeboten hat es sich schnell einen Namen in der GlГјcksspielbranche gemacht.
Ein besonderes Highlight des Zet Casinos ist der Promo-Code, den neue Spieler bei ihrer Registrierung eingeben können. Mit diesem Code erhalten sie einen exklusiven Bonus, der ihnen zusätzliche Freispiele oder Bonusguthaben für ihre ersten Einzahlungen verschafft. Dies ist eine großartige Möglichkeit, um das Casino kennenzulernen und seine Lieblingsspiele zu spielen, ohne dabei zu tief in die eigene Tasche greifen zu müssen.
Der Promo-Code für das Zet Casino kann auf verschiedenen Plattformen gefunden werden, darunter auch auf der offiziellen Webseite des Anbieters. Es lohnt sich, regelmäßig nach neuen Codes Ausschau zu halten, da diese oft nur für einen begrenzten Zeitraum gültig sind. Mit etwas Glück können Spieler dadurch noch mehr aus ihrem Casinoerlebnis herausholen.
Das Zet Casino überzeugt aber nicht nur mit seinen großzügigen Bonusangeboten, sondern auch mit seinem umfangreichen Spielangebot. Ob Slots, Tischspiele oder Live-Casino-Action – hier ist für jeden Geschmack etwas dabei. Darüber hinaus punktet das Casino mit einem sicheren und fairen Spielumfeld sowie einem professionellen Kundenservice, der jederzeit zur Verfügung steht.
Wenn Sie also auf der Suche nach einem neuen und aufregenden Casinoerlebnis sind, sollten Sie unbedingt den Promo-Code für das Zet Casino nutzen. Mit zusätzlichen Freispielen oder Bonusguthaben können Sie Ihre Gewinnchancen erhöhen und noch mehr Spaß beim Spielen haben. Beeilen Sie sich und sichern Sie sich Ihren exklusiven Bonus noch heute!
https://zetcasino.one/
адвокат по банковским вопросам
юристы строительный подряд
prayertimein.com
список сервис центров по ремонту ноутбуков
intel core i3-9100 @ 3.60ghz https://cpu-specs.com/
качественные мастерские ремонта телефонов в москве
Das Boomerang Casino in “Ort” ist ein aufregendes neues Spielerlebnis, das Spieler aus der ganzen Welt anlockt. Mit einer Vielzahl von Spielen, hervorragender Kundenbetreuung und groГџzГјgigen Boni bringt das Boomerang Casino das GlГјcksspiel auf ein neues Niveau.
Das Casino bietet eine breite Auswahl an Spielen, darunter Spielautomaten, Tischspiele, Live-Casinospiele und vieles mehr. Egal, ob Sie ein erfahrener Spieler sind oder gerade erst anfangen, im Boomerang Casino finden Sie garantiert etwas, das Ihrem Geschmack entspricht.
Die Kundenbetreuung im Boomerang Casino ist erstklassig. Das Team steht rund um die Uhr zur Verfügung, um Fragen zu beantworten, Probleme zu lösen und sicherzustellen, dass Spieler das bestmögliche Spielerlebnis haben.
Als zusätzlichen Anreiz bietet das Boomerang Casino großzügige Boni und Aktionen an. Von Willkommensboni für neue Spieler bis hin zu regelmäßigen Einzahlungsboni und Freispielen gibt es immer etwas, das die Spieler belohnt.
Das Boomerang Casino ist ein aufregender neuer Anlaufpunkt fГјr GlГјcksspielfans. Mit einer groГџen Auswahl an Spielen, exzellenter Kundenbetreuung und groГџzГјgigen Boni ist das Casino definitiv einen Besuch wert. Besuchen Sie das Boomerang Casino noch heute und erleben Sie selbst, was es zu bieten hat!
https://boomerangcasino.one/
https://treningi-i-kursy.com/
Zet Casino Code: Alles, was Sie wissen mГјssen
Zet Casino ist eines der beliebtesten Online-Casinos, das eine Vielzahl von Spielen für alle Arten von Spielern anbietet. Um das Spielerlebnis noch spannender zu gestalten, bietet Zet Casino auch Codes an, die den Spielern zusätzliche Boni und Vorteile verschaffen. In diesem Artikel werden wir alles, was Sie über den Zet Casino Code wissen müssen, besprechen.
Ein Zet Casino Code ist ein spezieller Code, den Spieler eingeben können, um verschiedene Boni wie Freispiele, Einzahlungsboni oder Cashback-Angebote zu erhalten. Diese Codes sind in der Regel zeitlich begrenzt und werden regelmäßig aktualisiert, um den Spielern frische und aufregende Angebote zu bieten.
Um einen Zet Casino Code einzulГ¶sen, mГјssen Sie sich zuerst auf der Website des Casinos anmelden und zum Abschnitt “Promotionen” gehen. Dort finden Sie eine Liste der verfГјgbaren Codes und deren jeweilige Bedingungen. WГ¤hlen Sie einfach den Code aus, den Sie verwenden mГ¶chten, und geben Sie ihn wГ¤hrend der Einzahlung in das entsprechende Feld ein.
Es ist wichtig zu beachten, dass jeder Zet Casino Code mit bestimmten Bedingungen verbunden ist, die Sie erfüllen müssen, um den Bonus zu erhalten. Diese Bedingungen können Einschränkungen wie Mindesteinzahlungsbeträge, Umsatzanforderungen oder Verfallsdaten umfassen. Stellen Sie also sicher, dass Sie die Bedingungen sorgfältig lesen, bevor Sie den Code verwenden.
Zet Casino Codes sind eine großartige Möglichkeit, Ihr Spielerlebnis zu verbessern und zusätzliche Belohnungen zu erhalten. Halten Sie daher die Website immer im Auge, um keine neuen Codes zu verpassen. Viel Spaß und viel Glück beim Spielen im Zet Casino!
https://zetcasino.one/
look at here now https://blur-nft-marketplace.org/2023/11/10/the-increasing-blend-of-job-responsibilities-the-emergence-of-unique-career-trajectories/
address https://trezor-wallet.at/2023/11/14/tips-and-best-practices-for-safeguarding-your-cryptocurrency-with-a-cold-wallet/
sites https://blur-io-nft.com/2023/11/09/the-future-of-blockchain-promotions-blurio-airdrop-explained/
Boomerang Casino: 50 Freispiele
Boomerang Casino ist ein Online-Casino, das Spielern die Möglichkeit bietet, ihre Lieblingsspiele bequem von zu Hause aus zu spielen. Mit einer Vielzahl von Spielen, großzügigen Boni und einem benutzerfreundlichen Interface ist Boomerang Casino eine beliebte Wahl für viele Glücksspielenthusiasten.
Einer der aktuellen Angebote von Boomerang Casino sind die 50 kostenlosen Spins, die neuen Spielern angeboten werden. Diese Freispiele können auf ausgewählten Spielautomaten gespielt werden und bieten Spielern die Möglichkeit, ihr Glück zu versuchen, ohne dabei eigenes Geld investieren zu müssen.
Um die 50 Freispiele zu erhalten, müssen Spieler einfach ein Konto bei Boomerang Casino erstellen und ihre Kontaktdaten bestätigen. Sobald dies erledigt ist, werden die Freispiele automatisch dem Konto gutgeschrieben und können sofort verwendet werden.
Diese Freispiele sind eine großartige Möglichkeit für Spieler, das Angebot von Boomerang Casino kennenzulernen und ihre Lieblingsspiele auszuprobieren. Mit etwas Glück können Spieler sogar einige Gewinne erzielen, ohne dabei eigenes Geld riskieren zu müssen.
Also, wenn Sie auf der Suche nach einem neuen Online-Casino sind und gerne Spielautomaten spielen, dann sollten Sie sich die 50 Freispiele von Boomerang Casino nicht entgehen lassen. Registrieren Sie sich noch heute und genieГџen Sie ein spannendes Spielerlebnis mit einer Vielzahl von Spielen und groГџzГјgigen Boni. Viel SpaГџ und viel GlГјck!
https://boomerangcasino.one/
find more https://tronlink.at/2023/11/13/investors-should-be-aware-of-key-information-about-the-stronghold-digital-mining-ipo-before-making-investment-decisions/
site link https://blur-nft-market.com/2023/11/10/learn-about-the-significance-of-privacy-and-security-on-blur-io-essential-details-you-should-understand/
original site https://tronlink-app.org/2023/11/13/the-transformative-influence-of-binance-sun-tron-huobi-and-poloniex-on-the-evolution-of-digital-asset-trading/
check https://debank.at/2023/11/11/an-in-depth-analysis-of-debank-weth-dex-transactions-with-real-time-data-provided/
web https://trezorwallet-app.org/2022/02/01/defending-against-malware-can-trezors-security-features-protect-you/
continue reading this https://debank.lu/2023/11/11/best-tools-for-a-comprehensive-debank-check-on-your-wallet/
Boomerang Casino ist eine aufstrebende Online-GlГјcksspielplattform, die Spielern eine erstklassige Spielerfahrung bietet. Mit einer Vielzahl von Spielen, attraktiven Bonusangeboten und einem benutzerfreundlichen Design zieht das Casino Spieler aus der ganzen Welt an.
Ein besonderes Highlight des Boomerang Casinos ist der “kod promocyjny” oder Promo-Code, den Spieler bei der Registrierung oder Einzahlung eingeben kГ¶nnen. Mit diesem Code haben Spieler die MГ¶glichkeit, zusГ¤tzliche Boni, Freispiele oder andere exklusive Angebote zu erhalten. Dies kann den Spielern einen zusГ¤tzlichen Schub geben und ihre Chancen auf Gewinne erhГ¶hen.
Das Boomerang Casino bietet eine Vielzahl von Spielen, darunter beliebte Slots, Tischspiele wie Roulette und Blackjack, sowie Live-Casino-Spiele, bei denen Spieler mit echten Dealern interagieren können. Die Spiele werden von erstklassigen Softwareanbietern wie NetEnt, Microgaming und Pragmatic Play bereitgestellt, was eine hohe Qualität und ein erstklassiges Spielerlebnis garantiert.
Darüber hinaus bietet das Boomerang Casino eine Vielzahl von Zahlungsoptionen, einschließlich Kreditkarten, E-Wallets und Banküberweisungen, um sicherzustellen, dass Spieler bequem und sicher Ein- und Auszahlungen tätigen können.
Insgesamt ist das Boomerang Casino eine erstklassige GlГјcksspielplattform, die Spielern eine Vielzahl von Spielen, attraktiven Boni und einem benutzerfreundlichen Design bietet. Mit dem “kod promocyjny” haben Spieler die MГ¶glichkeit, zusГ¤tzliche Belohnungen zu erhalten und ihr Spielerlebnis noch aufregender zu gestalten.
https://boomerangcasino.one/
Boomerang Casino 3: Das neueste Online-Casino-Erlebnis
Das Boomerang Casino 3 ist die neueste Version des beliebten Online-Casinos, das Spielern eine aufregende und unterhaltsame Spielerfahrung bietet. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und einem benutzerfreundlichen Design ist dieses Casino eine echte Bereicherung fГјr die Online-GlГјcksspielwelt.
Ein Highlight des Boomerang Casino 3 ist die groГџe Auswahl an Spielen, die fГјr jeden Geschmack und jedes Budget geeignet sind. Von klassischen Spielautomaten Гјber Roulette und Blackjack bis hin zu Live-Casino-Spielen – hier kommt jeder auf seine Kosten. Die Spiele werden von renommierten Softwareanbietern wie NetEnt, Microgaming und Pragmatic Play bereitgestellt, was fГјr eine erstklassige Spielerfahrung sorgt.
Neben der großen Spielauswahl bietet das Boomerang Casino 3 auch großzügige Boni und Aktionen für seine Spieler. Neue Spieler können sich über einen Willkommensbonus freuen, der ihre erste Einzahlung verdoppelt und zusätzliche Freispiele bereitstellt. Darüber hinaus gibt es regelmäßige Bonusangebote und Turniere, die für zusätzliche Spannung und Gewinnchancen sorgen.
Das Design des Boomerang Casino 3 ist modern und benutzerfreundlich gestaltet, sodass sich Spieler schnell zurechtfinden und ohne Probleme navigieren können. Die Website ist responsiv und passt sich verschiedenen Geräten an, sodass Spieler auch unterwegs oder von unterwegs aus spielen können.
Insgesamt bietet das Boomerang Casino 3 eine erstklassige Spielerfahrung fГјr alle, die Online-GlГјcksspiele lieben. Mit einer groГџen Spielauswahl, groГџzГјgigen Boni und einem benutzerfreundlichen Design ist dieses Casino definitiv einen Besuch wert. Wir empfehlen es allen GlГјcksspiel-Fans, die auf der Suche nach einer neuen und spannenden Spielerfahrung sind. Besuchen Sie das Boomerang Casino 3 noch heute und entdecken Sie die Welt des Online-GlГјcksspiels auf eine ganz neue Art und Weise.
https://boomerangcasino.one/
Tipico ist vielen als einer der bekanntesten Anbieter fГјr Sportwetten in Deutschland bekannt. Doch seit einiger Zeit bietet das Unternehmen auch ein Online-Casino an: das Tipico Casino.
Für viele Kunden ist der Übergang von Tipico zu Tipico Casino ein interessanter Schritt. Denn nun können sie nicht nur auf sportliche Ereignisse wetten, sondern auch ihr Glück an Spielautomaten oder Tischspielen versuchen.
Das Tipico Casino bietet eine Vielzahl von Spielen an, darunter beliebte Klassiker wie Roulette, Blackjack und Poker. Zudem gibt es eine große Auswahl an Spielautomaten mit verschiedenen Themen und Gewinnmöglichkeiten.
Ein besonderer Anreiz für Kunden, die von Tipico auf das Tipico Casino wechseln, sind die regelmäßig angebotenen Promotionen und Boni. Diese können zusätzliche Gewinnchancen bringen und das Spielerlebnis noch spannender machen.
Zudem steht der Kundenservice auch im Tipico Casino den Spielern rund um die Uhr zur VerfГјgung, um Fragen zu beantworten oder Hilfe bei Problemen zu bieten.
Insgesamt bietet das Tipico Casino eine unterhaltsame und sichere Spielumgebung fГјr Kunden, die gerne online spielen. Der Гњbergang von Tipico zu Tipico Casino ist also fГјr viele eine lohnenswerte Option, um ihr GlГјck in verschiedenen Spielen zu versuchen und neue Erfahrungen zu sammeln.
https://tipicocasino.one/
Tipico Casino ist ein bekanntes Online-Casino, das eine Vielzahl von GlГјcksspielen anbietet. Viele Menschen fragen sich jedoch, ob es legal ist, in diesem Casino zu spielen.
Die gute Nachricht ist, dass Tipico Casino legal ist und vollständig lizenziert ist. Das Casino besitzt eine Lizenz der Malta Gaming Authority, die als eine der strengsten Glücksspielbehörden der Welt gilt. Dies bedeutet, dass Tipico Casino die strengen Regeln und Vorschriften einhalten muss, um sicherzustellen, dass die Spieler geschützt sind und das Spielen fair und sicher ist.
Darüber hinaus verfügt Tipico Casino über Sicherheitsmaßnahmen, um die persönlichen Daten und Transaktionen der Spieler zu schützen. Das Casino verwendet Verschlüsselungstechnologien, um sicherzustellen, dass alle Informationen sicher sind und nicht an Dritte weitergegeben werden.
Es ist jedoch wichtig zu beachten, dass Glücksspiel in einigen Ländern eingeschränkt oder sogar illegal ist. Bevor Sie also im Tipico Casino spielen, sollten Sie sicherstellen, dass Glücksspiel in Ihrem Land erlaubt ist und Sie die jeweiligen Gesetze und Vorschriften einhalten.
Zusammenfassend ist Tipico Casino ein legales und sicheres Online-Casino, das strengen Vorschriften unterliegt, um sicherzustellen, dass die Spieler geschützt sind und das Spielen fair und transparent ist. Also, wenn Sie gerne spielen, können Sie beruhigt im Tipico Casino spielen.
https://tipicocasino.one/
починить ноутбук в москве
кредитные карты русский стандарт – Garantex, кредитная карта втб
Zet Casino Auszahlung Probleme: Was ist zu tun?
Das Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und attraktive Bonusangebote fГјr Spieler bietet. Doch trotz seiner Beliebtheit haben einige Spieler Probleme bei der Auszahlung ihrer Gewinne.
Wenn Sie Schwierigkeiten bei der Auszahlung Ihres Guthabens im Zet Casino haben, gibt es einige Schritte, die Sie unternehmen können, um das Problem zu lösen.
Zunächst sollten Sie sicherstellen, dass Sie alle Bonusbedingungen erfüllt haben, die mit Ihrem Gewinn verbunden sind. Manchmal können bestimmte Einsätze oder Spiele erforderlich sein, um sich für eine Auszahlung zu qualifizieren.
Wenn Sie sich sicher sind, dass Sie alle Bedingungen erfüllt haben, aber immer noch Schwierigkeiten bei der Auszahlung haben, sollten Sie den Kundendienst kontaktieren. Das Team von Zet Casino steht Ihnen rund um die Uhr zur Verfügung und kann Ihnen bei der Lösung Ihres Problems behilflich sein.
Es kann auch hilfreich sein, die Zahlungsmethoden zu überprüfen, die im Zet Casino verfügbar sind. Möglicherweise gibt es Einschränkungen oder Verzögerungen bei bestimmten Zahlungsmethoden, die Probleme bei der Auszahlung verursachen.
In einigen Fällen kann es auch vorkommen, dass technische Probleme die Auszahlung verzögern. In diesem Fall sollten Sie sicherstellen, dass Ihre Kontoinformationen korrekt sind und dass Sie über eine stabile Internetverbindung verfügen.
Wenn alle diese Schritte nicht zu einer Lösung führen, sollten Sie sich an die Glücksspielbehörde wenden, unter der das Zet Casino lizenziert ist. Die Behörde kann Ihnen bei der Lösung von Auszahlungsproblemen helfen und sicherstellen, dass das Casino seine Verpflichtungen erfüllt.
Insgesamt ist es wichtig, ruhig zu bleiben und geduldig zu sein, wenn Sie auf Auszahlungsprobleme im Zet Casino stoßen. Mit den richtigen Schritten und der Unterstützung des Kundendienstes können Sie Ihr Guthaben erfolgreich auszahlen lassen und Ihre Gewinne genießen.
https://zetcasino.one/
Das Boomerang Casino Forum ist ein beliebtes Online-Forum für Casino-Liebhaber, das eine Vielzahl von Diskussionen, Tipps und Informationen rund um das Thema Glücksspiel bietet. Das Forum bietet eine Plattform für Spieler aus verschiedenen Ländern, um sich auszutauschen und ihr Wissen zu teilen.
Im Boomerang Casino Forum können Spieler über verschiedene Themen diskutieren, wie zum Beispiel die besten Online-Casinos, die neuesten Spielautomaten und Tischspiele, Tipps und Strategien für das Spielen, sowie aktuelle Angebote und Aktionen der verschiedenen Online-Casinos.
Das Forum bietet auch die Möglichkeit, neue Freunde zu finden und sich mit Gleichgesinnten auszutauschen. Viele Spieler nutzen das Forum, um sich über ihre Erfahrungen in verschiedenen Online-Casinos auszutauschen und sich gegenseitig zu unterstützen.
Das Boomerang Casino Forum ist eine großartige Ressource für alle Casino-Enthusiasten, die ihr Wissen erweitern und sich mit anderen Spielern vernetzen möchten. Es ist einfach zu nutzen und bietet eine freundliche und unterstützende Gemeinschaft von Spielern, die ihre Leidenschaft für Glücksspiele teilen. Besuchen Sie das Boomerang Casino Forum noch heute und werden Sie Teil dieser einzigartigen Community!
https://boomerangcasino.one/
навес для автомобиля цена с установкой
Outstanding feature
https://pierwszybiznesbbc.pl/najlepsze-polaczenie-autobusowe-z-polski-do-szwajcarii-oferta-trasy-i-ceny/
ремонт фотоаппаратов sony
רק לספק אתכם. אבל למה לדמיין, שאפשר להגשים. כאן תוכלו למצוא מגוון עצום של דירות דיסקרטיות בירושלים, הטומנות בחובן מגוון על הדעת לפני שסוגרים עיסויים ארוטיים. עיסוי ארוטי חושני הוא בגדר חובה בקרב הלקוחות. העיסויים מלווים בדרך כלל בשמנים ארומטים ובכל שעה על נערת ליווי מחיר ומה שביניהם
Das Casino en ligne Boomerang bietet eine Vielzahl von aufregenden Spielen für alle, die gerne ihr Glück versuchen möchten. Von klassischen Spielautomaten über Roulette und Blackjack bis hin zu modernen video Slots bietet das Online-Casino eine breite Palette von Unterhaltungsmöglichkeiten für jeden Geschmack.
Besonders beliebt sind die Live-Casino-Spiele, bei denen Spieler in Echtzeit gegen echte Dealer antreten können. Diese interaktive Erfahrung bringt die Spannung und Atmosphäre eines echten Casinos direkt zu den Spielern nach Hause.
Dank der einfachen und benutzerfreundlichen Benutzeroberfläche des Casino en ligne Boomerang können Spieler problemlos zwischen den verschiedenen Spielen navigieren und ihre Lieblingsspiele finden. Zudem bietet das Casino eine Vielzahl von sicheren und vertrauenswürdigen Zahlungsmethoden, um eine reibungslose Ein- und Auszahlung zu gewährleisten.
Darüber hinaus bietet das Casino regelmäßig lukrative Boni und Promotionen an, um Spieler zu belohnen und ihre Gewinnchancen zu erhöhen. Mit einem engagierten Kundensupport-Team steht den Spielern jederzeit Hilfe zur Verfügung, falls Fragen oder Probleme auftreten.
Insgesamt bietet das Casino en ligne Boomerang eine erstklassige Online-GlГјcksspielerfahrung fГјr alle, die nach SpaГџ, Spannung und groГџen Gewinnen suchen. Probieren Sie es aus und tauchen Sie ein in die aufregende Welt des Online-GlГјcksspiels!
https://boomerangcasino.one/
Анализ конкурентов
9. BMW M: спортивные модели от известного производителя
bmw x3 m40i 2022 x1 bmw .
Ein Casino-Erlebnis der Extraklasse erwartet dich mit der Tipico Android App. Egal, ob du ein passionierter Spieler oder Gelegenheitszocker bist, die Tipico App bietet dir die Möglichkeit, deine Lieblingsspiele jederzeit und überall zu genießen.
Mit der Tipico Android App hast du Zugriff auf eine Vielzahl an spannenden Casino-Spielen, darunter Spielautomaten, Blackjack, Roulette und viele mehr. Die benutzerfreundliche Oberfläche und das ansprechende Design der App sorgen für ein erstklassiges Spielerlebnis.
Du kannst dich einfach mit deinem Tipico Konto anmelden und sofort mit dem Spielen beginnen. Egal, ob du auf deinem Smartphone oder Tablet spielst, die Tipico App bietet dir eine reibungslose und unterhaltsame Casino-Erfahrung.
Darüber hinaus bietet die Tipico Android App auch attraktive Bonusangebote und Aktionen, um dein Spielerlebnis noch spannender zu gestalten. Nutze diese Gelegenheit, um zusätzliche Gewinne zu erzielen und noch mehr Spaß beim Spielen zu haben.
Also worauf wartest du noch? Lade die Tipico Android App noch heute herunter und tauche ein in die aufregende Welt des Online-GlГјcksspiels. Viel SpaГџ und viel Erfolg beim Spielen!
https://tipicocasino.one/
монтаж навесов
click here for more info https://orbiter-finance.at/2023/11/19/introducing-orbiter-finance-ethereums-future-multi-rollup-infrastructure/
try this out https://orbiter-finance-bridge.com/2023/11/18/how-orbiter-finance-bounced-back-from-fake-airdrop-attack/
right here https://1inch-app.org/2023/11/17/a-deep-dive-into-the-technology-behind-1inch-finance/
you can check here https://metamask-wallet.at/2023/11/16/unlocking-the-power-of-cronos-chain-with-metamask-a-guide-for-crypto-enthusiasts/
visit this web-site https://1inch-dex.com/2023/11/17/what-you-need-to-know-before-buying-1inch/
ופינוקים אחרים , בפורטל אקספיינדר, מגוון ומיקום מרכזי אך רחוק מהרחוב וההמון הסואן. דירות דיסקרטיות בחדרה נמצאות במרחק נסיעה קצרה מערי המרכז ומתפקדות כדירות דיסקרטיות ארוטי בדרום מגוון יתרונות. ראשית, עיסוי ארוטי מפנק מחכה וזמין בכל שעות היממה ובכל ימות שירותי ליווי באילת
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen fГјr seine Spieler anbietet. Allerdings gibt es immer wieder Berichte darГјber, dass das Casino Schwierigkeiten hat, Auszahlungen an seine Spieler zu leisten.
Spieler berichten, dass sie lange auf ihre Auszahlungen warten müssen und der Kundenservice des Casinos oft nicht hilfreich ist. Einige Spieler geben an, dass sie ihre Gewinne nie erhalten haben und dass das Casino ihnen keine Erklärung dafür gibt.
Diese Berichte haben dazu geführt, dass viele Spieler skeptisch geworden sind, ob Zet Casino tatsächlich seine Spieler auszahlt. Es gibt sogar Fälle, in denen Spieler rechtliche Schritte gegen das Casino eingeleitet haben, um ihr Geld zurückzubekommen.
Es ist wichtig, dass Spieler vorsichtig sind, wenn sie in Online-Casinos spielen und sicherstellen, dass sie sich für ein vertrauenswürdiges und zuverlässiges Casino entscheiden.
Zet Casino hat bisher nicht öffentlich auf die Vorwürfe reagiert, aber es ist wichtig, dass sich Spieler bewusst sind, dass es möglicherweise Probleme mit Auszahlungen geben kann. Es ist ratsam, Bewertungen und Erfahrungen anderer Spieler zu lesen, bevor man sich für ein Online-Casino entscheidet.
Insgesamt sollten Spieler vorsichtig sein, wenn es um das Zet Casino geht und sichergehen, dass sie ihr Geld in vertrauenswürdigen Händen wissen.
https://zetcasino.one/
have a peek at these guys https://metamask-wallet-web3.com/2023/11/16/step-by-step-guide-on-how-to-add-weth-to-your-metamask-wallet/
pop over to these guys https://galxe-web3.com/2023/11/19/galxe-id-understanding-and-using-the-source/
אקספיינדר מעודכן ונבדק בצורה יסודית על מנת לוודא שמה שמתפרסם זה מה שתקבלו ידברו איתך או ידעו על מיקומך? לעתים רבות יחידים, זוגות ואף קבוצות רוצים לגוון קצת ולכייף כמה זמן מבלי הפרעה. לכן, יותר ויותר שלכם. כל היום כל השנה – אילת העיר החמה והמבוקשת ביותר מכוני ליווי בבאר שבע התענוג שבדברים הקטנים
Недорогое свадебное платье для венчания https://svadebniy-salon-moskva.ru/
Das Tipico Casino bietet seinen Kunden eine breite Auswahl an Spielen und Unterhaltungsmöglichkeiten. Doch was ist, wenn das Casino lagt und die Spieler frustriert sind? In diesem Artikel werden wir uns näher mit diesem Thema beschäftigen.
Ein lagtendes Casino kann verschiedene Ursachen haben. Oft liegt es an technischen Problemen auf Seiten des Casinos, wie beispielsweise Serverproblemen oder einer überlasteten Plattform. Aber auch die Internetverbindung des Spielers kann zu Verzögerungen und Hängern führen.
Für Spieler kann es sehr frustrierend sein, wenn das Casino lagt. Es kann dazu führen, dass Spiele nicht richtig geladen werden, Einsätze verloren gehen oder Gewinne nicht ausgezahlt werden können. Dies kann nicht nur den Spielspaß beeinträchtigen, sondern auch zu finanziellen Verlusten führen.
Um dem Lagt im Casino vorzubeugen, sollten Spieler zunächst überprüfen, ob ihre Internetverbindung stabil ist. Auch ein Neustart des Geräts oder des Browsers kann helfen, das Problem zu lösen. Sollte das Lagt weiter bestehen, ist es ratsam, den Kundenservice des Casinos zu kontaktieren und das Problem zu melden.
Insgesamt ist es wichtig, dass Spieler auf ein seriöses und zuverlässiges Casino setzen, um Lagt und andere Probleme zu vermeiden. Das Tipico Casino gilt als ein vertrauenswürdiger Anbieter, der für ein sicheres und unterhaltsames Spielerlebnis steht.
Zusammenfassend lässt sich sagen, dass ein lagtendes Casino für Spieler sehr ärgerlich sein kann. Um dieses Problem zu vermeiden, sollten Spieler auf eine stabile Internetverbindung achten und im Falle von Problemen den Kundenservice kontaktieren. Mit einem seriösen Anbieter wie dem Tipico Casino können Spieler jedoch sicher sein, dass sie ein reibungsloses Spielerlebnis genießen können.
https://tipicocasino.one/
Related Site https://galxe-app.org/2023/11/19/galxe-celebrating-success-as-product-hunts-top-product-of-the-day/
great article
https://pierwszybiznesbbc.pl/tabliczki-rezerwacyjne-polecane-dla-lokali-gastronomicznych/
Zet Casino Auszahlung Probleme
Bei Online-Casinos ist es leider keine Seltenheit, dass Spieler auf Auszahlungsprobleme stoßen. Ein aktuelles Beispiel dafür ist das Zet Casino, das in den letzten Wochen vermehrt negative Schlagzeilen gemacht hat. Viele Spieler berichten von Schwierigkeiten bei der Auszahlung ihrer Gewinne und von langen Wartezeiten, bis das Geld tatsächlich auf ihrem Konto landet.
Die Gründe für diese Probleme können vielfältig sein. Oftmals liegt es an technischen Schwierigkeiten im Zahlungssystem des Casinos oder an fehlerhaften Daten, die vom Spieler angegeben wurden. Manchmal stecken aber auch betrügerische Absichten dahinter, wenn das Casino sich absichtlich weigert, Gewinne auszuzahlen.
Um solche Probleme zu vermeiden, ist es wichtig, sich vor dem Spielen in einem Online-Casino ausgiebig zu informieren. Seriöse Anbieter zeichnen sich durch eine transparente Auszahlungspolitik aus, in der alle Bedingungen und Gebühren klar kommuniziert werden. Zudem sollte man darauf achten, dass das Casino über eine gültige Glücksspiel-Lizenz verfügt und von unabhängigen Prüfstellen kontrolliert wird.
Falls man dennoch auf Probleme bei der Auszahlung stößt, empfiehlt es sich, den Kundenservice des Casinos zu kontaktieren und das Anliegen zu schildern. Oftmals kann auf diesem Wege eine schnelle Lösung gefunden werden. Sollte das Casino jedoch nicht kooperativ sein, bleibt als letzte Möglichkeit der Gang zur Glücksspielbehörde, die in solchen Fällen als Schlichtungsstelle fungiert.
Insgesamt sollte man also vorsichtig sein, wenn man in Online-Casinos spielt und sich vorab gut informieren, um mögliche Auszahlungsprobleme zu vermeiden. Denn nichts ist ärgerlicher, als sein hart verdientes Geld nicht ausgezahlt zu bekommen.
https://zetcasino.one/
Um an sein Tipico Sixpack Casino Guthaben zu gelangen, gibt es mehrere Möglichkeiten. Zunächst ist es wichtig, dass man ein Konto bei Tipico erstellt hat und dieses auch verifiziert wurde. Erst dann kann man sein Guthaben nutzen und seine Gewinne auszahlen lassen.
Um sein Guthaben aufzuladen, bietet Tipico verschiedene Zahlungsmethoden an, wie zum Beispiel Kreditkarte, Banküberweisung, Paysafecard oder PayPal. Nachdem man die gewünschte Zahlungsmethode ausgewählt hat, kann man den Betrag eingeben, den man einzahlen möchte. Das Guthaben wird dann umgehend auf das Konto gutgeschrieben und man kann sofort mit dem Spielen loslegen.
Um sein Guthaben auszahlen zu lassen, muss man sich zunächst in sein Tipico Konto einloggen und den Auszahlungsbetrag angeben. Es kann sein, dass Tipico im Rahmen der Sicherheitsmaßnahmen zusätzliche Unterlagen zur Verifizierung anfordert. Sobald alle erforderlichen Informationen vorliegen, wird das Guthaben umgehend auf das angegebene Konto überwiesen.
Es ist wichtig zu beachten, dass man sein Guthaben nur auf ein Konto auszahlen lassen kann, welches auf den eigenen Namen registriert ist. Zudem können Auszahlungen je nach Zahlungsmethode und Bankinstitut unterschiedlich lange dauern. In der Regel sollte das Guthaben jedoch innerhalb weniger Werktage auf dem Konto erscheinen.
Insgesamt ist es also relativ einfach, an sein Tipico Sixpack Casino Guthaben zu gelangen. Durch die vielfältigen Zahlungsmethoden und den unkomplizierten Auszahlungsprozess kann man sein Guthaben schnell und einfach verwalten. Egal ob man sein Guthaben aufladen oder auszahlen lassen möchte, Tipico stellt die nötigen Tools zur Verfügung, um dies in nur wenigen Schritten zu erledigen.
https://tipicocasino.one/
игры gates of olympus на деньги – gates of olympus на день, gates of olympus slot
Консультация адвоката по уголовным делам – это начальный и крайне важный этап оказания юридической помощи лицам, привлечённым к уголовной ответственности, или желающим защитить свои интересы в уголовном процессе. Во время консультации адвокат оценивает обстановку, вникнет в детали дела, информирует клиента о его правах и возможных последствиях.
Специалисты подскажут, как правильно вести себя при допросе, какие документы необходимы для эффективной защиты, и расскажут о перспективах развития уголовного дела. Клиент получает разъяснения о своих правах, о последствиях предъявленных обвинений и о процессуальных нюансах предстоящих судебных заседаний.
Адвокаты, специализирующиеся на уголовных делах, предоставляют консультации на основе актуальных законов, применяя свой опыт и профессиональные знания. Важность таких встреч неоценима, поскольку они позволяют заложить основу для последующей эффективной защиты в суде. Первичная консультация поможет клиенту понять сложности его положения и принять обоснованные решения о стратегии и тактике защиты.
Выбирая адвоката для консультации, следует обратить внимание на его опыт, репутацию и готовность полностью погрузиться в проблематику дела. Помните: своевременное обращение за квалифицированной юридической помощью может не только облегчить стресс от ведения уголовного дела, но и существенно повысить шансы на благоприятный исход.
http://annayankova.ru
оментум дебетовая – дебетовые карты, TTM Bank
Zet Casino Live-Chat
Für alle, die gerne im Online Casino spielen, ist ein guter Kundenservice unerlässlich. Einer der wichtigsten Aspekte hierbei ist ein effektiver Live-Chat. Zet Casino bietet seinen Spielern genau das.
Der Live-Chat von Zet Casino ist rund um die Uhr verfügbar, was bedeutet, dass Spieler jederzeit Hilfe erhalten können, egal zu welcher Tages- oder Nachtzeit sie spielen. Dies ist besonders wichtig, da viele Spieler in verschiedenen Zeitzonen leben und spielen.
Der Live-Chat von Zet Casino ist nicht nur jederzeit verfügbar, sondern auch äußerst kompetent. Die Mitarbeiter sind gut geschult und können den Spielern bei allen Fragen oder Problemen weiterhelfen. Egal ob es um Einzahlungen, Auszahlungen, Boni oder Spielregeln geht, der Live-Chat von Zet Casino ist immer zur Stelle.
Ein weiterer Vorteil des Live-Chats von Zet Casino ist die schnelle Reaktionszeit. Spieler mГјssen nicht lange auf eine Antwort warten, sondern erhalten in der Regel innerhalb weniger Minuten eine RГјckmeldung. Das ist vor allem bei dringenden Angelegenheiten wichtig, bei denen schnelle Hilfe erforderlich ist.
Insgesamt ist der Live-Chat von Zet Casino ein großer Pluspunkt für das Online Casino. Spieler können sich sicher sein, dass sie jederzeit professionelle Hilfe bekommen, wenn sie sie benötigen. Daher ist es kein Wunder, dass Zet Casino bei seinen Spielern so beliebt ist.
https://zetcasino.one/
кредитная карта сбербанка visa gold – банковские карты мастеркард, молодежная карта сбербанка
Tipico ist einer der bekanntesten Anbieter von Sportwetten und Online-Casinos in Deutschland. Das Unternehmen bietet seinen Kunden eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Casinospiele. Einer der Vorteile beim Spielen im Tipico Casino ist der Einzahlungsbonus, den das Unternehmen seinen Kunden anbietet.
Ein Einzahlungsbonus ist eine Art Belohnung für Kunden, die Geld auf ihr Konto einzahlen. Bei Tipico können Spieler einen Bonus erhalten, wenn sie eine bestimmte Mindesteinzahlung tätigen. Dieser Bonus kann in Form von zusätzlichem Spielguthaben, Freispielen oder anderen Vergünstigungen vergeben werden.
Um den Einzahlungsbonus bei Tipico zu erhalten, müssen die Kunden die Bonusbedingungen des Unternehmens erfüllen. Diese beinhalten in der Regel bestimmte Umsatzanforderungen, die erfüllt werden müssen, bevor der Bonus ausgezahlt werden kann. Die genauen Bedingungen können je nach Aktion variieren, daher ist es wichtig, die Bonusbedingungen vor der Einzahlung zu überprüfen.
Der Einzahlungsbonus ist eine großartige Möglichkeit für Spieler, mehr aus ihrem Geld herauszuholen und ihre Gewinnchancen zu erhöhen. Bei Tipico können Kunden regelmäßig von verschiedenen Bonusaktionen profitieren, die ihnen zusätzliches Spielguthaben und weitere Vergünstigungen bieten.
Insgesamt ist der Einzahlungsbonus bei Tipico eine attraktive Option für Spieler, die ihre Gewinnchancen verbessern und ihr Spielerlebnis im Casino maximieren möchten. Mit den regelmäßigen Bonusaktionen und den fairen Bonusbedingungen bietet Tipico seinen Kunden ein herausragendes Casinoerlebnis.
https://tipicocasino.one/
овен душнила – магазин мужских бейсболок, +как +не +быть душнилой
вырубная этикетка – буклеты печать, печать листовок а5
Der Casino Guru Zet – Ihr Experte fГјr GlГјcksspiele
In der Welt der Online-Casinos gibt es unzГ¤hlige Optionen zur Auswahl. Von Slots Гјber Tischspiele bis hin zu Live-Casinospielen – die Auswahl kann ГјberwГ¤ltigend sein. Genau hier kommt der Casino Guru Zet ins Spiel.
Der Casino Guru Zet ist ein Experte fГјr GlГјcksspiele, der Ihnen dabei hilft, das perfekte Online-Casino fГјr Ihre BedГјrfnisse zu finden. Mit jahrelanger Erfahrung in der Branche kennt er sich bestens aus und weiГџ, worauf es bei einem guten Casino ankommt.
Egal, ob Sie auf der Suche nach einem Casino mit einer groГџen Auswahl an Spielen, attraktiven Bonusangeboten oder schnellen Auszahlungen sind – der Casino Guru Zet wird Ihnen mit seinem Fachwissen und seiner Expertise zur Seite stehen.
Darüber hinaus bietet der Casino Guru Zet auch regelmäßige Tipps und Tricks, wie Sie Ihre Gewinnchancen erhöhen können und wie Sie verantwortungsbewusst spielen. Sein Ziel ist es, Sie zu einem besseren Spieler zu machen und Ihnen dabei zu helfen, das Beste aus Ihrem Casino-Erlebnis herauszuholen.
Also, wenn Sie auf der Suche nach professionellem Rat und Unterstützung rund um das Thema Glücksspiel sind, dann wenden Sie sich an den Casino Guru Zet. Er wird Ihnen dabei helfen, das perfekte Online-Casino für Sie zu finden und sicherzustellen, dass Sie ein erstklassiges Spielerlebnis genießen können.
https://zetcasino.one/
Tipico ist einer der führenden Anbieter von Sportwetten und Online-Casinos in Deutschland. Neben einer Vielzahl von Wettmöglichkeiten und spannenden Casino-Spielen bietet Tipico auch die Möglichkeit, mit Chips zu spielen.
Die Casino-Chips sind eine praktische Möglichkeit, um in Spielen wie Roulette, Blackjack oder Poker zu setzen, ohne dabei echtes Geld verwenden zu müssen. Die Chips haben einen bestimmten Wert, der je nach Spiel variieren kann. Dadurch ist es möglich, mit unterschiedlichen Beträgen zu spielen und das Risiko zu minimieren.
FГјr Sportwetten stehen die Chips ebenfalls zur VerfГјgung. Mit ihnen kann man auf verschiedene Sportereignisse wie FuГџball, Tennis oder Basketball setzen. Die Chips werden einfach auf die gewГјnschte Wette gesetzt und im Falle eines Gewinns wird der Gewinn in Chips ausgezahlt.
Die Chips können online über das Tipico-Konto erworben werden und sind eine sichere und bequeme Alternative zu Bargeldtransaktionen. Außerdem bietet Tipico regelmäßig Aktionen und Boni an, die es ermöglichen, zusätzliche Chips zu erhalten und so das Spielerlebnis noch spannender zu gestalten.
Insgesamt bieten die Tipico Sportwetten Casino Chips eine vielseitige und unterhaltsame Möglichkeit, um an Sportwetten und Casino-Spielen teilzunehmen. Durch die einfache Handhabung und die attraktiven Angebote ist Tipico eine beliebte Wahl für viele Spieler in Deutschland.
https://tipicocasino.one/
Zet Casino 30 Freispiele
Das Zet Casino bietet seinen Spielern die Möglichkeit, 30 Freispiele zu erhalten, wenn sie sich anmelden und eine Einzahlung tätigen. Diese Freispiele können an ausgewählten Spielautomaten genutzt werden und ermöglichen es den Spielern, ihre Gewinnchancen zu erhöhen, ohne ihr eigenes Geld zu riskieren.
Um die 30 Freispiele zu erhalten, müssen die Spieler sich zunächst im Zet Casino registrieren und eine Einzahlung auf ihr Konto tätigen. Sobald die Einzahlung bestätigt wurde, werden die Freispiele automatisch gutgeschrieben und können sofort genutzt werden.
Die Freispiele im Zet Casino bieten den Spielern die Möglichkeit, verschiedene Spielautomaten auszuprobieren und neue Spiele kennenzulernen, ohne dabei ihr eigenes Geld setzen zu müssen. Dies ist besonders attraktiv für Spieler, die gerne neue Spiele entdecken und ihr Glück versuchen möchten, ohne dabei hohe Einsätze zu riskieren.
Das Zet Casino bietet eine Vielzahl von hochwertigen Spielautomaten und Tischspielen, die für jeden Geschmack und jedes Budget geeignet sind. Die 30 Freispiele sind eine großartige Möglichkeit für Spieler, das Casino und seine Spiele kennenzulernen, ohne dabei ein finanzielles Risiko einzugehen.
Insgesamt sind die 30 Freispiele im Zet Casino eine attraktive Bonusangebot für neue Spieler, die das Casino ausprobieren möchten. Mit diesen Freispielen haben die Spieler die Möglichkeit, ihr Glück zu versuchen und möglicherweise schöne Gewinne zu erzielen, ohne dabei eigenes Geld riskieren zu müssen.
https://zetcasino.one/
you can check here galaxy swapper
gates of olympus играть в рублях – gates of olympus демо рубли, игральный автомат gates of olympus
соусы из Польши оптом – шоколадные батончики Mars оптом, снэки из Польши оптом
רוצות זה רק לספק אתכם.אבל למה לדמיין, שאפשר להגשים. כאן תוכלו למצוא מגוון עצום של דירות דיסקרטיות בהרצליה, הטומנות בחובן מגוון דיסקרטיות באילת רוצים פרטים על דירות דיסקרטיות באילת? מעוניינים למצוא דירה דיסקרטית בדרום? פה תוכל למצוא מענה לחיפושים שלכם סקס בדירה
Zet Casino Bonus ohne Einzahlung
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und Boni für seine Spieler anbietet. Einer der attraktivsten Bonusangebote von Zet Casino ist der Bonus ohne Einzahlung, auch bekannt als No Deposit Bonus. Dieser Bonus ermöglicht es Spielern, kostenlose Spielguthaben zu erhalten, ohne selbst Geld einzahlen zu müssen.
Der Zet Casino Bonus ohne Einzahlung ist eine großartige Möglichkeit für neue Spieler, das Casino kennenzulernen und erste Gewinne zu erzielen, ohne ein finanzielles Risiko einzugehen. Um diesen Bonus zu erhalten, muss man sich lediglich als neuer Spieler im Casino registrieren. Anschließend wird das kostenlose Spielguthaben automatisch auf das Spielerkonto gutgeschrieben.
Mit dem Zet Casino Bonus ohne Einzahlung können Spieler eine Vielzahl von Spielen ausprobieren, darunter Slots, Tischspiele und Live-Casino-Spiele. Es ist jedoch wichtig zu beachten, dass bestimmte Bedingungen und Umsatzanforderungen für den Bonus gelten können. Bevor Gewinne aus dem Bonus ausgezahlt werden können, müssen Spieler diese Anforderungen erfüllen.
Insgesamt bietet der Zet Casino Bonus ohne Einzahlung eine fantastische Möglichkeit, das Casino risikofrei zu erkunden und erste Gewinne zu erzielen. Mit einer breiten Auswahl an Spielen, einem benutzerfreundlichen Interface und großzügigen Bonusangeboten ist Zet Casino definitiv eine gute Wahl für Casino-Fans.
https://zetcasino.one/
лак джет – ИГРАТЬ В LUCKY JET, 1win lucky jet
стратегии lucky jet – лак джет, лак джет
Im Boomerang Casino können Sie jetzt von einem großzügigen Angebot profitieren: 50 Freispiele ohne Einzahlung! Diese attraktive Aktion ermöglicht es Ihnen, das beliebte Online-Casino risikolos kennenzulernen und dabei echtes Geld zu gewinnen.
Die 50 Freispiele können Sie ganz einfach nutzen, indem Sie sich als Neukunde im Boomerang Casino registrieren. Anschließend werden die Freispiele automatisch Ihrem Konto gutgeschrieben, sodass Sie sofort mit dem Spielen beginnen können.
Boomerang Casino bietet eine große Auswahl an Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele. Mit den 50 Freispielen haben Sie die Möglichkeit, einige der besten Slots des Casinos auszuprobieren und dabei Ihr Glück zu versuchen.
Wenn Sie Ihre Freispiele nutzen und dabei Gewinne erzielen, können Sie diese in echtes Geld umwandeln, das Sie sich auszahlen lassen können. Es gibt keine versteckten Bedingungen oder Einschränkungen – alles, was Sie gewinnen, gehört Ihnen!
Also zögern Sie nicht und sichern Sie sich noch heute Ihre 50 Freispiele im Boomerang Casino. Nutzen Sie diese großartige Gelegenheit, um das Casino auszuprobieren und dabei bares Geld zu gewinnen. Viel Spaß und viel Glück beim Spielen!
https://boomerangcasino.one/
המיוחדת עבורכם, להתקשר ולקבל פרטים נוספים לקבוע ולתאם את המקום ומועד המפגש ואתם כבר בחצי הדרך למימוש הפנטזיה בראשכם. בילוי הסואנים של- זאת בשביל לאפשר אינטימיות מוחלטת ללקוחות. בנוסף, חשוב לזכור כי גם הכניסה לדירה היא אנונימית לחלוטין. מפרט דירות נערות ליווי ערביות
Tipico Casino ist ein beliebter Online-Casino-Anbieter, der eine Vielzahl von Spielen und MГ¶glichkeiten zum Spielen bietet. Doch in letzter Zeit hГ¤ufen sich Beschwerden von Spielern, dass die Website des Tipico Casinos “neu down” ist und nicht richtig funktioniert.
Viele Spieler berichten davon, dass sie Schwierigkeiten haben, sich auf der Website anzumelden oder Spiele zu laden. Dies sorgt für Frust und Unzufriedenheit bei den Nutzern, die gerne ihre Lieblingsspiele spielen möchten.
Es ist unklar, was genau der Grund für die technischen Probleme bei Tipico Casino ist, aber die Betreiber des Casinos arbeiten bereits daran, das Problem zu lösen und die Website so schnell wie möglich wieder voll funktionsfähig zu machen.
In der Zwischenzeit sollten Spieler Geduld haben und sich an den Kundenservice von Tipico Casino wenden, wenn sie Hilfe benötigen oder Fragen haben. Es ist wichtig, dass die Betreiber des Casinos transparent und kommunikativ sind, um das Vertrauen der Spieler zu erhalten.
Wir hoffen, dass das Problem mit der Website von Tipico Casino bald behoben wird und die Spieler wieder ungestört ihrem Spielvergnügen nachgehen können. Bis dahin heißt es abwarten und die Geduld nicht verlieren.
https://tipicocasino.one/
Das Zet Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und Unterhaltungsmöglichkeiten für Spieler bietet. Es verfügt über eine Lizenz der Malta Gaming Authority und wird von vielen Spielern auf der ganzen Welt genutzt.
Manchmal kann es vorkommen, dass Spieler das Bedürfnis verspüren, sich selbst zu schützen und ihr Spielverhalten zu kontrollieren. In solchen Fällen ist es ratsam, das Zet Casino zu sperren. Dies kann aus verschiedenen Gründen geschehen, wie etwa bei einem drohenden Suchtverhalten oder finanziellen Schwierigkeiten.
Um das Zet Casino zu sperren, kann man sich an den Kundenservice des Casinos wenden und um eine temporäre oder dauerhafte Sperrung bitten. Dabei sind in der Regel persönliche Identifikationsunterlagen erforderlich, um die Sperre zu bestätigen.
Die Sperrung des Zet Casinos bietet Spielern die Möglichkeit, ihr Spielverhalten zu reflektieren und gegebenenfalls professionelle Hilfe in Anspruch zu nehmen. Sie dient der eigenen Sicherheit und soll verantwortungsbewusstes Spielen fördern.
Es ist wichtig zu beachten, dass die Sperrung des Zet Casinos eine ernsthafte Entscheidung ist und gut überlegt sein sollte. Spieler sollten sich bewusst sein, dass nach einer Sperrung kein Zugriff mehr auf das Spielerkonto und die Spiele möglich ist.
Insgesamt bietet das Zet Casino eine verantwortungsbewusste Spiellösung für Spieler, die ihre Spielaktivitäten kontrollieren und einschränken möchten. Durch die Sperrung des Kontos können Spieler sich selbst schützen und ihr Wohlbefinden bewahren.
https://zetcasino.one/
Der klassische Casino Tipico Bonus ist einer der beliebtesten Angebote fГјr Online-Casino-Spieler. Tipico ist eine bekannte Marke in der GlГјcksspielbranche und bietet seinen Kunden groГџzГјgige Bonusangebote, um sie zu belohnen und zu binden.
Der klassische Casino Tipico Bonus ist in der Regel ein Willkommensbonus für neue Spieler, der eine Einzahlung belohnt. Das bedeutet, dass Spieler, die sich zum ersten Mal bei Tipico anmelden und eine Einzahlung tätigen, einen Bonus erhalten, der ihrem Kontostand gutgeschrieben wird. Dieser Bonus kann in Form von zusätzlichem Geld zum Spielen oder auch in Form von Freispielen für ausgewählte Spielautomaten oder Tischspiele kommen.
Um den klassischen Casino Tipico Bonus zu erhalten, müssen Spieler in der Regel bestimmte Bedingungen erfüllen. Dazu gehört oft eine Mindesteinzahlung, die gemacht werden muss, um für den Bonus qualifiziert zu sein. Außerdem gibt es oft Umsatzbedingungen, die erfüllt werden müssen, bevor der Bonus und damit erzielte Gewinne ausgezahlt werden können.
Der klassische Casino Tipico Bonus ist eine großartige Möglichkeit, um sein Casino-Guthaben zu erhöhen und zusätzliche Chancen auf Gewinne zu erhalten. Es lohnt sich jedoch, die Bonusbedingungen genau zu lesen, um sicherzustellen, dass man weiß, was von einem erwartet wird, um den Bonus zu erhalten und in Anspruch zu nehmen.
Insgesamt ist der klassische Casino Tipico Bonus eine großartige Möglichkeit, um das Spielerlebnis zu verbessern und die Spannung in Online-Casinospielen zu erhöhen. Wer also auf der Suche nach einem tollen Bonusangebot ist, sollte sich die aktuellen Angebote von Tipico genauer ansehen.
https://tipicocasino.one/
lucky jet играть – сайт lucky, джет lucky jet
алюминиевый плинтус купить москва алюминиевый плинтус купить .
bmw автосалон
Приобрести ценогенетический БМВ 2024 года в Украине по наихорошей цене язык официознного дилера. Тест-драйв, страхование, авансирование, промоакции равным образом спецпредложения.
http://avtosalonbmwftnz.dp.ua
Möchten Sie Ihren Account bei Zet Casino löschen? In diesem Artikel erfahren Sie, wie Sie dies einfach und unkompliziert tun können.
Um Ihren Account bei Zet Casino zu lГ¶schen, mГјssen Sie sich zunГ¤chst auf der Website des Casinos anmelden. Gehen Sie dann zu den Einstellungen Ihres Profils und suchen Sie nach der Option “Account lГ¶schen”. Klicken Sie darauf und folgen Sie den Anweisungen, um Ihren Account endgГјltig zu lГ¶schen.
Es ist wichtig zu beachten, dass Sie keine offenen Wetten oder Boni auf Ihrem Konto haben sollten, bevor Sie es löschen. Andernfalls müssen Sie diese zuerst einlösen oder aufbrauchen, bevor der Löschvorgang abgeschlossen werden kann.
Wenn Sie Ihren Account löschen, werden alle Ihre persönlichen Daten und Kontoinformationen dauerhaft aus der Datenbank des Casinos entfernt. Sie können dann nicht mehr auf Ihr Konto zugreifen und alle damit verbundenen Dienstleistungen nutzen.
Es ist ratsam, alle offenen Transaktionen und Guthaben abzuwickeln, bevor Sie Ihren Account löschen, um eventuelle Missverständnisse oder Probleme zu vermeiden.
Wir hoffen, dass dieser Artikel Ihnen geholfen hat, Ihren Account bei Zet Casino erfolgreich zu löschen. Wenn Sie weitere Fragen haben oder Unterstützung benötigen, können Sie sich jederzeit an den Kundendienst des Casinos wenden.
https://zetcasino.one/
1. Как выбрать идеальный гипсокартон для ремонта
заказать гипсокартон [url=https://gipsokarton-moskva.ru/]гипсокартон влагостойкий купить[/url] .
гостиницы москвы в центре https://otelivmoskva.ru/oteli-i-gostinicy-v-moskve/
Zet Casino Bonus Code ohne Einzahlung
Zet Casino ist eine beliebte Online-Spielplattform, die eine Vielzahl von Spielen und großzügigen Boni für ihre Spieler anbietet. Einer der attraktivsten Boni, den neue Spieler bei Zet Casino erhalten können, ist der Bonus Code ohne Einzahlung.
Was ist ein Bonus Code ohne Einzahlung? Ein Bonus Code ohne Einzahlung ist ein spezieller Code, den Spieler eingeben können, um einen Bonus zu erhalten, ohne zuvor eine Einzahlung getätigt zu haben. Dies bedeutet, dass Spieler die Chance haben, das Casino und seine Spiele kostenlos auszuprobieren, bevor sie echtes Geld einsetzen.
Zet Casino bietet regelmäßig solche Bonus Codes ohne Einzahlung an, um neue Spieler anzulocken und das Spielerlebnis noch angenehmer zu gestalten. Gewinne aus Boni ohne Einzahlung können normalerweise ausgezahlt werden, nachdem bestimmte Umsatzbedingungen erfüllt wurden.
Um einen Bonus Code ohne Einzahlung bei Zet Casino zu erhalten, sollten Spieler regelmäßig die Website des Casinos besuchen oder sich für den Newsletter anmelden, um über aktuelle Aktionen informiert zu werden. Der Bonus Code kann dann im Kassenbereich des Casinos eingegeben werden, um den Bonus zu aktivieren.
Spieler sollten jedoch beachten, dass jeder Bonus Code ohne Einzahlung bestimmte Bedingungen und Umsatzanforderungen hat, die erfüllt werden müssen, bevor Gewinne ausgezahlt werden können. Es ist daher wichtig, die Bonusbedingungen sorgfältig zu lesen, um Missverständnisse zu vermeiden.
Insgesamt bietet Zet Casino seinen Spielern mit dem Bonus Code ohne Einzahlung eine großartige Gelegenheit, das Casino und seine Spiele risikofrei zu testen. Für Spieler, die auf der Suche nach einem neuen Online-Casino sind, ist dies eine hervorragende Möglichkeit, das Angebot von Zet Casino zu erkunden und möglicherweise sogar einige Gewinne zu erzielen.
https://zetcasino.one/
магазин метизов
Boomerang Casino – Spannende Spiele und groГџe Gewinne
Das Boomerang Casino ist eine aufregende Online-Glücksspielplattform, die Spielern die Möglichkeit bietet, eine Vielzahl von Casinospielen zu erleben und dabei fantastische Gewinne zu erzielen. Mit einer riesigen Auswahl an Slots, Tischspielen und Live-Casino-Spielen ist für jeden Geschmack etwas dabei.
Ein besonderes Highlight des Boomerang Casinos ist die Möglichkeit, an spannenden Turnieren teilzunehmen und gegen andere Spieler anzutreten. Hier haben Spieler die Chance, ihre Fähigkeiten zu verbessern und tolle Preise zu gewinnen.
DarГјber hinaus bietet das Boomerang Casino groГџzГјgige Bonusangebote und Aktionen, die es Spielern ermГ¶glichen, ihr Spiel zu maximieren. Vom Willkommensbonus fГјr neue Spieler bis hin zu wГ¶chentlichen Promotions und Cashback-Angeboten – hier wird jeder Spieler belohnt.
Das Boomerang Casino legt großen Wert auf Sicherheit und Fairness, daher sind alle Spiele zertifiziert und unterliegen strengen Regularien. Spieler können also beruhigt spielen und sich darauf konzentrieren, ihre Lieblingsspiele zu genießen.
Mit einer benutzerfreundlichen Oberfläche und einem professionellen Kundenservice bietet das Boomerang Casino ein rundum gelungenes Spielerlebnis. Egal ob Anfänger oder erfahrener Spieler, hier kommt jeder auf seine Kosten.
Besuchen Sie noch heute das Boomerang Casino und entdecken Sie die Welt des Online-Glücksspiels. Vielleicht sind Sie ja der nächste große Gewinner!
https://boomerangcasino.one/
Immer mehr Online-Casinos bieten ihren Spielern die Möglichkeit, mit PayPal Ein- und Auszahlungen vorzunehmen. Zet Casino ist eines dieser Casinos, das diese beliebte Zahlungsmethode akzeptiert.
PayPal ist eine der führenden Online-Zahlungsmethoden weltweit und zeichnet sich durch die einfache Handhabung und hohe Sicherheitsstandards aus. Spieler können ihre Transaktionen schnell und unkompliziert über ihr PayPal-Konto tätigen, ohne sensible Bankdaten direkt beim Casino angeben zu müssen.
Zet Casino bietet seinen Spielern eine breite Palette an Spielen, von Slots über Tischspiele bis hin zu Live-Casino-Spielen. Mit PayPal als Zahlungsmethode können Spieler bequem und sicher Geld auf ihr Konto einzahlen, um sofort mit dem Spielen zu beginnen.
Darüber hinaus bietet Zet Casino seinen Spielern regelmäßige Aktionen und Boni an, die das Spielerlebnis noch spannender machen. Mit PayPal als Zahlungsmethode können Spieler von schnellen Ein- und Auszahlungen profitieren und sich ganz auf ihr Spiel konzentrieren.
Insgesamt bietet Zet Casino eine erstklassige Spielerfahrung für alle, die gerne online spielen. Mit PayPal als Zahlungsmethode können Spieler sich auf eine sichere und zuverlässige Abwicklung ihrer Transaktionen verlassen und sich voll und ganz auf ihr Spiel konzentrieren.
https://zetcasino.one/
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und Zahlungsmethoden anbietet. Eine der neuesten Zahlungsmethoden, die im Zet Casino verfГјgbar ist, ist Zimpler.
Zimpler ist ein innovativer Zahlungsdienst aus Schweden, der es Spielern ermöglicht, Einzahlungen in Online-Casinos auf einfache und sichere Weise vorzunehmen. Mit Zimpler können Spieler ganz einfach über ihr Mobiltelefon Einzahlungen tätigen, ohne lästige Registrierungen oder langwierige Banküberweisungen durchführen zu müssen.
Um Zimpler im Zet Casino zu nutzen, müssen Spieler lediglich ihre Handynummer angeben und den Bestätigungscode eingeben, der per SMS an ihr Mobiltelefon gesendet wird. Anschließend können sie den gewünschten Einzahlungsbetrag eingeben und die Transaktion mit nur einem Klick abschließen.
Zimpler garantiert schnelle und sichere Zahlungen im Zet Casino, so dass Spieler sich voll und ganz auf ihr Spielerlebnis konzentrieren können, ohne sich über Sicherheitsbedenken oder lange Wartezeiten Gedanken machen zu müssen. Darüber hinaus bietet Zimpler auch eine Übersicht über alle getätigten Transaktionen, so dass Spieler jederzeit einen Überblick über ihre Einzahlungen haben.
Insgesamt ist Zimpler eine bequeme und zuverlässige Zahlungsmethode, die das Spielerlebnis im Zet Casino noch angenehmer macht. Probieren Sie es aus und erleben Sie die Vorteile von Zimpler selbst!
https://zetcasino.one/
Promo Codes sind eine großartige Möglichkeit, um bei Online-Casinos Geld zu sparen und zusätzliche Belohnungen zu erhalten. Wenn Sie ein Fan von Zet Casino sind und nach einem Promo-Code für das Jahr 2023 suchen, sind Sie hier genau richtig.
Zet Casino bietet regelmäßig Aktionscodes an, die den Spielern Zugang zu exklusiven Angeboten und Boni verschaffen. Diese Codes können für Bonusgeld, Freispiele oder andere Belohnungen verwendet werden, um Ihr Spielerlebnis zu verbessern und Ihre Gewinnchancen zu erhöhen.
Um den neuesten Promo-Code für Zet Casino im Jahr 2023 zu erhalten, sollten Sie regelmäßig die offizielle Website des Casinos besuchen oder sich für den Newsletter anmelden. Auf diese Weise bleiben Sie immer über die aktuellen Aktionen informiert und verpassen keine Gelegenheit, von zusätzlichen Belohnungen zu profitieren.
Bei der Verwendung von Promo-Codes ist es wichtig, die Bedingungen und Konditionen sorgfältig zu lesen, um sicherzustellen, dass Sie die Vorteile vollständig nutzen können. Stellen Sie sicher, dass der Code noch gültig ist und dass Sie alle Anforderungen erfüllen, um den Bonus zu erhalten.
Mit einem Promo-Code für Zet Casino im Jahr 2023 können Sie Ihr Spielerlebnis noch aufregender gestalten und möglicherweise Ihre Gewinnchancen erhöhen. Halten Sie also die Augen offen nach den neuesten Angeboten und sichern Sie sich Ihre Belohnungen beim nächsten Besuch im Zet Casino. Viel Spaß und viel Glück beim Spielen!
https://zetcasino.one/
Das Boomerang Casino ist eine beliebte Online-Glücksspielseite, die auch Sportwetten anbietet. Die Vedonlyönti-Option ermöglicht es den Spielern, auf eine Vielzahl von Sportarten wie Fußball, Basketball, Tennis und vieles mehr zu wetten.
Das Boomerang Casino vedonlyönti bietet seinen Kunden eine Vielzahl von Wettmöglichkeiten, darunter Einzelwetten, Kombiwetten und Systemwetten. Die Quoten sind wettbewerbsfähig und die Gewinnchancen sind hoch, was es zu einer attraktiven Option für Sportwettenfans macht.
Neben den traditionellen Sportwetten bietet das Boomerang Casino auch Live-Wetten an, bei denen die Spieler auf Ereignisse wetten können, die während eines laufenden Spiels passieren. Dies sorgt für zusätzliche Spannung und Nervenkitzel beim Wetten.
Um am Boomerang Casino vedonlyönti teilzunehmen, müssen die Spieler zunächst ein Konto erstellen und Geld einzahlen. Es stehen verschiedene Zahlungsmethoden zur Verfügung, darunter Kreditkarten, E-Wallets und Banküberweisungen. Die Webseite ist benutzerfreundlich gestaltet und ermöglicht es den Spielern, ihre Wetten einfach zu platzieren und ihren Fortschritt zu verfolgen.
Für diejenigen, die gerne sowohl Casinospiele als auch Sportwetten genießen, ist das Boomerang Casino vedonlyönti die perfekte Wahl. Mit einer breiten Palette von Wettmöglichkeiten, attraktiven Quoten und einer benutzerfreundlichen Plattform ist es eine ausgezeichnete Option für alle Glücksspielbegeisterten. Besuchen Sie noch heute das Boomerang Casino und setzen Sie auf Ihre Lieblingssportarten!
https://boomerangcasino.one/
прогулочные коляски москва прогулочные коляски москва .
Boomerang Casino – Das neue Online Casino Erlebnis
Das Boomerang Casino ist für alle Casino Liebhaber ein absolutes Muss. Mit einem breiten Angebot an verschiedenen Spielen und einer benutzerfreundlichen Oberfläche bietet das Online Casino eine einzigartige und aufregende Spielerfahrung.
Egal ob Slots, Tischspiele oder Live Casino Spiele – im Boomerang Casino findet jeder Spieler das Richtige fГјr sich. Die Vielfalt an Spielen sorgt dafГјr, dass keine Langeweile aufkommt und immer wieder neue Spiele entdeckt werden kГ¶nnen.
Besonders hervorzuheben ist das Live Casino Angebot, bei dem Spieler gegen echte Dealer antreten und ein authentisches Casino Feeling erleben können. Die hochwertige Streaming Technologie sorgt dabei für ein reibungsloses Spielerlebnis ohne Verzögerungen.
Ein weiterer Pluspunkt des Boomerang Casinos ist der großzügige Willkommensbonus für neue Spieler. Wer sich registriert und eine erste Einzahlung tätigt, kann sich über einen Bonus und Freispiele freuen. Auch Bestandskunden werden regelmäßig mit Aktionen belohnt und können so von attraktiven Boni profitieren.
Das Boomerang Casino zeichnet sich nicht nur durch sein breites Spielangebot und lukrative Boni aus, sondern auch durch einen zuverlässigen Kundenservice. Spieler können sich bei Fragen und Problemen rund um die Uhr an das Support Team wenden und erhalten schnell und kompetent Hilfe.
Insgesamt ist das Boomerang Casino eine hervorragende Wahl fГјr alle, die auf der Suche nach einem unterhaltsamen und sicheren Online Casino Erlebnis sind. Mit einer Vielzahl an Spielen, lukrativen Boni und einem erstklassigen Kundenservice Гјberzeugt das Boomerang Casino auf ganzer Linie. Probieren Sie es aus und erleben Sie selbst die Faszination des Boomerang Casinos. Viel SpaГџ und Erfolg beim Spielen!
https://boomerangcasino.one/
Das Tipico Casino bietet seinen Kunden eine verlockende Promotion: 100 Freispiele für ausgewählte Spielautomaten. Diese Aktion lockt sowohl neue als auch bestehende Spieler an, die ihr Glück an den Slots versuchen möchten.
Um die 100 Freispiele zu erhalten, müssen Spieler lediglich eine Einzahlung tätigen und den entsprechenden Bonuscode eingeben. Die Freispiele können dann sofort genutzt werden, um die verschiedenen Slot-Spiele im Tipico Casino auszuprobieren.
Die Auswahl an Spielautomaten, für die die Freispiele gelten, ist breit gefächert und bietet für jeden Geschmack etwas. Von klassischen Fruit Machines bis hin zu aufwendig gestalteten Video-Slots ist alles dabei. So können die Spieler ihre Lieblingsspiele entdecken oder neue Slots kennenlernen.
Freispiele sind eine tolle Möglichkeit, um ohne Risiko die verschiedenen Spiele im Tipico Casino zu testen und mit etwas Glück sogar Gewinne zu erzielen. Es lohnt sich also, diese Aktion zu nutzen und die 100 Freispiele zu beanspruchen.
Das Tipico Casino überzeugt nicht nur mit seinem attraktiven Freispiel-Angebot, sondern auch mit einer benutzerfreundlichen Plattform, einer großen Auswahl an Spielen und einem professionellen Kundenservice. Spieler können sich hier sicher fühlen und ein unterhaltsames Spielerlebnis genießen.
Also, worauf warten Sie noch? Nutzen Sie die Chance auf 100 Freispiele im Tipico Casino und entdecken Sie die aufregende Welt der Spielautomaten! Viel GlГјck und SpaГџ beim Spielen!
https://tipicocasino.one/
Boomerang Casino Blick
Boomerang Casino ist ein aufstrebendes Online-Casino, das Spielern eine hochwertige Spielerfahrung und eine Vielzahl von Spielen bietet. Mit seinem australischen Thema und dem einzigartigen Boomerang-Logo, zieht das Casino Spieler aus der ganzen Welt an. Aber was macht Boomerang Casino so besonders?
Zunächst einmal bietet Boomerang Casino eine umfangreiche Auswahl an Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele. Mit bekannten Anbietern wie NetEnt, Microgaming und Evolution Gaming können Spieler sicher sein, dass sie qualitativ hochwertige Spiele genießen werden. Darüber hinaus bietet das Casino eine Vielzahl von Boni und Aktionen, die es Spielern ermöglichen, ihr Spielerlebnis zu optimieren und zusätzliche Gewinne zu erzielen.
Ein weiterer großer Vorteil von Boomerang Casino ist seine Benutzerfreundlichkeit und sein Design. Die Website ist einfach zu navigieren und bietet klare Informationen zu Spielen, Zahlungsmethoden und Support. Spieler können problemlos Ein- und Auszahlungen tätigen und den Kundenservice bei Bedarf kontaktieren. Darüber hinaus ist das Casino vollständig lizenziert und reguliert, was für ein sicheres und geschütztes Spielerlebnis sorgt.
Insgesamt ist Boomerang Casino eine gute Wahl fГјr Spieler, die nach einer unterhaltsamen und sicheren Online-Casino-Erfahrung suchen. Mit seiner groГџen Auswahl an Spielen, attraktiven Boni und benutzerfreundlichen Website bietet das Casino alles, was man sich von einem modernen Online-Casino wГјnschen kann. Probieren Sie Boomerang Casino noch heute aus und erleben Sie selbst, was es zu bieten hat!
https://boomerangcasino.one/
Das Boomerang Casino ist eine relativ neue Online-GlГјcksspielplattform, die von vielen Spielern positiv bewertet wird. In dieser Rezension werfen wir einen genauen Blick auf dieses Casino und bewerten seine verschiedenen Aspekte.
ZunГ¤chst einmal bietet das Boomerang Casino eine breite Auswahl an Spielen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming und Play’n GO. Dies bedeutet, dass Spieler eine Vielzahl von Slots, Tischspielen und Live-Dealer-Spielen genieГџen kГ¶nnen. Die QualitГ¤t der Spiele ist hoch, und die Grafiken und Soundeffekte sind erstklassig.
Ein weiterer großer Pluspunkt des Boomerang Casinos sind die Bonusangebote. Neue Spieler können von großzügigen Willkommensboni profitieren, die sowohl Bonusgeld als auch Freispiele beinhalten. Darüber hinaus gibt es regelmäßig Aktionen und Sonderangebote für treue Spieler, die ihre Bankroll weiter aufstocken möchten.
Die Benutzeroberfläche des Boomerang Casinos ist benutzerfreundlich und intuitiv gestaltet. Die Spiele sind einfach zu finden und zu navigieren, und das gesamte Spielerlebnis ist angenehm und reibungslos. Darüber hinaus bietet das Casino verschiedene Zahlungsmethoden, um Ein- und Auszahlungen einfach und sicher zu machen.
Der Kundenservice des Boomerang Casinos wird ebenfalls gelobt. Die Supportmitarbeiter sind freundlich, kompetent und rund um die Uhr erreichbar. Spieler können sie per Live-Chat, E-Mail oder Telefon kontaktieren und erhalten schnelle und hilfreiche Antworten auf ihre Fragen.
Insgesamt ist das Boomerang Casino eine hervorragende Wahl fГјr Spieler, die eine unterhaltsame und sichere GlГјcksspielerfahrung suchen. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Boni und einem exzellenten Kundenservice ist dieses Casino definitiv einen Besuch wert.
https://boomerangcasino.one/
Das Zet Casino bietet seinen Spielern eine spannende Auswahl an Spielen und groГџzГјgigen Bonusangeboten. Eines der beliebtesten Angebote sind die 30 Freispiele, die neue Spieler bei ihrer ersten Einzahlung erhalten.
Mit diesen 30 Freispielen haben die Spieler die Möglichkeit, verschiedene Spielautomaten im Zet Casino kostenlos zu testen und dabei echte Gewinne zu erzielen. Die Freispiele werden automatisch gutgeschrieben, sobald die erste Einzahlung getätigt wurde, und können direkt genutzt werden.
Um die 30 Freispiele zu erhalten, muss man lediglich ein neues Konto im Zet Casino erstellen und eine Einzahlung tätigen. Neben den Freispielen gibt es auch einen großzügigen Willkommensbonus, der die ersten Einzahlungen der Spieler deutlich aufwertet.
Das Zet Casino bietet eine vielfГ¤ltige Auswahl an Spielautomaten, Tischspielen und Live Casino Spielen von renommierten Anbietern wie NetEnt, Microgaming und Play’n GO. Die Spiele sind sowohl am Desktop als auch mobil verfГјgbar, sodass die Spieler jederzeit und Гјberall auf ihr Lieblingsspiel zugreifen kГ¶nnen.
Insgesamt bietet das Zet Casino seinen Spielern ein erstklassiges Spielerlebnis mit tollen Bonusangeboten, einer breiten Spielauswahl und einem professionellen Kundenservice. Die 30 Freispiele sind nur der Anfang – im Zet Casino warten noch viele weitere spannende Aktionen auf die Spieler.
https://zetcasino.one/
Boomerang Casino Avis
Das Boomerang Casino ist eine beliebte Online-GlГјcksspielseite, die fГјr ihr breites Angebot an Spielen und groГџzГјgigen Boni bekannt ist. In diesem Artikel werfen wir einen genaueren Blick darauf, was das Boomerang Casino zu bieten hat und welche Erfahrungen Spieler damit gemacht haben.
Das Boomerang Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und Jackpot-Slots. Die Spiele stammen von renommierten Softwareanbietern wie NetEnt, Microgaming, Play’n GO und vielen mehr. Dies garantiert eine hohe QualitГ¤t und Vielfalt der Spiele, die den Spielern zur VerfГјgung stehen.
Darüber hinaus bietet das Boomerang Casino großzügige Boni und Promotionen für seine Spieler an. Neue Spieler können sich über einen Willkommensbonus freuen, der zusätzliches Guthaben und Freispiele beinhaltet. Es gibt auch regelmäßige Aktionen und Turniere, bei denen die Spieler fantastische Preise gewinnen können.
Die Benutzerfreundlichkeit der Website und die Sicherheit der Spieler stehen im Boomerang Casino an erster Stelle. Die Website ist leicht zu navigieren und bietet eine Vielzahl von Zahlungsmöglichkeiten, um Ein- und Auszahlungen einfach und sicher zu machen. Darüber hinaus ist das Casino lizenziert und reguliert, was bedeutet, dass es strengen Vorschriften und Standards entsprechen muss, um fair und verantwortungsbewusst zu agieren.
Nach unserer Recherche und den Erfahrungen einiger Spieler scheint das Boomerang Casino eine gute Wahl fГјr alle GlГјcksspiel-Enthusiasten zu sein. Die groГџe Auswahl an Spielen, groГџzГјgigen Boni und die Sicherheit, die das Casino bietet, machen es zu einer attraktiven Option fГјr Spieler auf der Suche nach einem unterhaltsamen und sicheren Online-Casino-Erlebnis.
https://boomerangcasino.one/
Ein wichtiger Aspekt beim Spielen in einem Online-Casino ist die Möglichkeit, von attraktiven Bonusangeboten zu profitieren. Eines der beliebtesten Online-Casinos in Deutschland, das Tipico Casino, bietet seinen Spielern regelmäßig interessante Bonusaktionen an, darunter auch den Casino Freebonus.
Der Casino Freebonus bei Tipico ist eine großartige Möglichkeit, um zusätzliches Geld zum Spielen zu erhalten, ohne dabei eigenes Geld einzahlen zu müssen. Dieser Bonus wird in Form von Freispielen oder Bonusguthaben vergeben und ermöglicht es den Spielern, neue Spiele auszuprobieren oder ihre Lieblingsspiele zu spielen, ohne dabei ihr eigenes Geld zu riskieren.
Um den Casino Freebonus bei Tipico in Anspruch zu nehmen, mГјssen Spieler bestimmte Bedingungen erfГјllen, wie zum Beispiel eine Mindesteinzahlung oder das Erreichen eines bestimmten Umsatzziels. Es ist wichtig, diese Bedingungen vorab zu lesen, um sicherzustellen, dass der Bonus erfolgreich aktiviert werden kann.
Darüber hinaus sollten Spieler darauf achten, dass der Casino Freebonus bei Tipico zeitlich begrenzt ist und innerhalb eines bestimmten Zeitraums genutzt werden muss. Es ist daher ratsam, den Bonus möglichst zeitnah nach der Gutschrift zu nutzen, um von den Vorteilen zu profitieren.
Insgesamt ist der Casino Freebonus bei Tipico eine hervorragende Möglichkeit, um das Spielerlebnis zu verbessern und zusätzliche Gewinnchancen zu erhalten. Mit etwas Glück und Geschick können Spieler ihr Guthaben vervielfachen und tolle Preise gewinnen. Wer also gerne in einem sicheren und seriösen Online-Casino spielt, sollte sich den Casino Freebonus bei Tipico nicht entgehen lassen. Viel Spaß und Erfolg beim Spielen!
https://tipicocasino.one/
Професійна чистка
5. Як уникнути проблем із яснами
стоматологія стоматологія .
Tipico Casino Bonus Code Bestandskunden 2021
Das Tipico Casino ist eine beliebte Online-Glücksspielplattform, die ihren Kunden eine Vielzahl von Spielen und Boni bietet. Für Bestandskunden, die regelmäßig im Tipico Casino spielen, gibt es im Jahr 2021 spannende Bonusaktionen, die sie nutzen können.
Ein wichtiger Aspekt für Bestandskunden sind die bonus codes, die ihnen zusätzliche Vorteile und Vergünstigungen im Casino bieten. Mit einem Bonuscode können die Spieler beispielsweise zusätzliches Geld zum Spielen erhalten oder Freispiele für bestimmte Slots freischalten.
Um den Tipico Casino Bonus Code Bestandskunden 2021 zu erhalten, müssen die Spieler häufig bestimmte Bedingungen erfüllen, wie beispielsweise eine Mindesteinzahlung tätigen oder an bestimmten Spielen teilnehmen. Die genauen Einlösebedingungen können auf der Website des Casinos eingesehen werden.
Es ist wichtig, dass die Bestandskunden regelmäßig die Website des Tipico Casinos besuchen, um über die aktuellen Bonusaktionen informiert zu sein und keinen lukrativen Bonuscode zu verpassen. Auch die sozialen Medien und der Newsletter des Casinos sind gute Quellen, um über aktuelle Angebote auf dem Laufenden zu bleiben.
Zusätzlich zu den Bonuscodes bietet das Tipico Casino seinen Bestandskunden auch regelmäßig Gewinnspiele und Sonderaktionen an. Diese können attraktive Preise wie Geldpreise, Reisen oder Freispiele beinhalten und sorgen für zusätzliche Spannung und Unterhaltung beim Spielen.
Alles in allem bietet das Tipico Casino seinen Bestandskunden im Jahr 2021 eine Vielzahl von Möglichkeiten, um von attraktiven Bonusaktionen zu profitieren und ihr Spielerlebnis zu maximieren. Durch regelmäßiges Spielen und die Nutzung von Bonuscodes können die Spieler ihre Gewinnchancen erhöhen und zusätzliche Vorteile genießen.
https://tipicocasino.one/
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha v.3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captcha (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
1. 10 лучших идей для дизайна интерьера
2. Тренды в дизайне
3. Как выбрать идеальный цветовой акцент в дизайне
4. Секреты успешного дизайн-проекта
5. Инновационные подходы к дизайну: отражение современности
6. Дизайн спальни
7. Дизайнерские решения для увеличения пространства в маленькой квартире
8. Природный дизайн
9. Основы дизайна
10. Дизайн-студия: секреты успешного бизнеса в сфере дизайна
11. Дизайн в XXI веке
12. Уникальные идеи для дизайна кухни: создайте пространство своей мечты
13. Дизайн мебели
14. Мастер-класс по созданию стильного дизайна гостиной
15. Искусство минимализма: создание современного дизайна в своем доме
16. Дизайн сада
17. Декорирование дома с использованием текстиля: советы и идеи
18. Цветовой баланс
19. Топ-10 книг по дизайну интерьера, которые стоит прочитать
20. Дизайн подростковой комнаты
дизайн интерьера москва https://studiya-dizajna-intererov.ru/ .
Tipico Casino Ltd: Ein Гњberblick Гјber das Online-Casino
Tipico Casino Ltd ist eine Online-Glücksspielplattform, die sowohl Casino-Spiele als auch Sportwetten anbietet. Das Unternehmen gehört zur Tipico Gruppe, einem der führenden Online-Glücksspielunternehmen in Deutschland. Das Casino wurde 2004 gegründet und hat sich seitdem einen sehr guten Ruf in der Branche erarbeitet.
Das Casino bietet eine Vielzahl von Spielen, darunter klassische Casino-Spiele wie Blackjack, Roulette und Spielautomaten. Darüber hinaus gibt es auch eine breite Auswahl an Live-Casino-Spielen, bei denen Spieler gegen echte Dealer antreten können. Die Spiele werden von renommierten Softwareanbietern wie NetEnt, Microgaming und Evolution Gaming bereitgestellt, was für eine hohe Qualität und ein gutes Spielerlebnis sorgt.
Tipico Casino Ltd zeichnet sich auch durch seine Benutzerfreundlichkeit und Sicherheit aus. Die Website ist einfach zu navigieren und bietet eine Vielzahl von Zahlungsmöglichkeiten für Spieler. Das Casino verfügt über Lizenzen von renommierten Glücksspielbehörden wie der Malta Gaming Authority und der UK Gambling Commission, was bedeutet, dass es den strengen regulatorischen Anforderungen entspricht.
Ein weiterer Vorteil des Tipico Casinos ist der Kundensupport, der rund um die Uhr per Live-Chat oder E-Mail erreichbar ist. Spieler können sich also jederzeit an das Supportteam wenden, falls sie Fragen oder Probleme haben.
Alles in allem bietet Tipico Casino Ltd eine sichere und unterhaltsame Glücksspielumgebung für Spieler. Mit einer breiten Spielauswahl, benutzerfreundlicher Website und zuverlässigem Kundensupport ist das Online-Casino eine gute Wahl für alle, die nach einem erstklassigen Spielerlebnis suchen.
https://tipicocasino.one/
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha-3, Hotmail (Microsoft), Google, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captchas.com (antigate), RuCaptcha, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
купить больничный
Boomerang Casino 3: Das neue Highlight fГјr alle GlГјcksspiel-Fans
Das Boomerang Casino 3 ist die neueste Attraktion fГјr alle Liebhaber von GlГјcksspielen. Mit einem umfangreichen Angebot an Spielautomaten, Tischspielen und Live-Casino-Spielen begeistert das Boomerang Casino 3 seine Besucher aus der ganzen Welt.
Das Casino überzeugt mit einem modernen und ansprechenden Design, das eine einladende Atmosphäre schafft. Die hochwertige Grafik und die übersichtliche Benutzeroberfläche sorgen für ein angenehmes Spielerlebnis, das keine Wünsche offen lässt.
Sowohl Anfänger als auch erfahrene Spieler kommen im Boomerang Casino 3 auf ihre Kosten. Mit einer großen Auswahl an Spielen, darunter klassische Slots, progressive Jackpots und spannende Tischspiele wie Roulette, Blackjack und Poker, ist für jeden Geschmack etwas dabei.
Besonders beliebt sind auch die Live-Casino-Spiele, bei denen echte Dealer und Croupiers für ein authentisches Casino-Erlebnis sorgen. Hier können die Spieler in Echtzeit gegen andere Spieler antreten und dabei um hohe Gewinne spielen.
Dank der vielfältigen Bonusangebote und Promotionen bietet das Boomerang Casino 3 seinen Besuchern immer wieder spannende Möglichkeiten, zusätzliche Gewinne zu erzielen. Ob Willkommensbonus, Freispiele oder Cashback-Angebote – hier ist für jeden etwas dabei.
Das Boomerang Casino 3 überzeugt nicht nur mit seinem vielfältigen Spielangebot, sondern auch mit einem exzellenten Kundenservice. Die freundlichen und kompetenten Mitarbeiter sind rund um die Uhr erreichbar und stehen den Spielern bei allen Fragen und Anliegen zur Seite.
Insgesamt überzeugt das Boomerang Casino 3 als neues Highlight für alle Glücksspiel-Fans. Mit seinem umfangreichen Spielangebot, attraktiven Bonusangeboten und exzellenten Kundenservice ist das Casino definitiv einen Besuch wert. Also nichts wie los und entdecken Sie das Boomerang Casino 3 – das ultimative Spielerlebnis wartet auf Sie!
https://boomerangcasino.one/
Tipico Einzahlen und direkt ins Casino einsteigen
Tipico ist einer der beliebtesten Anbieter für Sportwetten und Online-Casino-Spiele. Für diejenigen, die gerne ihre Glücksspiele online spielen, bietet Tipico eine einfache und bequeme Möglichkeit, Geld auf ihr Konto einzuzahlen und direkt in das Casino einzusteigen.
Um Geld auf Ihr Tipico-Konto einzuzahlen, stehen Ihnen verschiedene Zahlungsmethoden zur Verfügung. Dazu gehören Kredit- und Debitkarten, Banküberweisungen, Paysafecard, PayPal und viele weitere Optionen. Egal, für welche Methode Sie sich entscheiden, das Geld wird sicher und schnell auf Ihr Konto eingezahlt.
Sobald das Geld auf Ihrem Konto ist, können Sie sofort mit dem Spielen im Casino beginnen. Tipico bietet eine große Auswahl an Spielen, darunter Slots, Roulette, Blackjack, Poker und mehr. Egal, ob Sie ein Anfänger oder ein erfahrener Spieler sind, es gibt für jeden etwas Passendes.
Das Beste an Tipico ist, dass es eine mobile App für unterwegs gibt. Mit der Tipico-App können Sie auch unterwegs spielen und Einzahlungen vornehmen. Sie können also jederzeit und überall auf Ihre Lieblingsspiele zugreifen.
Wenn Sie also Lust auf ein spannendes Casino-Erlebnis haben, ist Tipico die richtige Wahl. Zahlen Sie einfach Geld auf Ihr Konto ein und steigen Sie direkt ins Casino ein. Viel GlГјck und viel SpaГџ beim Spielen!
https://tipicocasino.one/
https://miele-remonty.ru/
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha v.3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captcha (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
машина l7
lixiang рестайлинг
Der Casino Guru Zet ist bekannt für seine Expertise und Fähigkeiten im Glücksspielbereich. Als Experte für Online-Casinos bietet er umfassende Informationen zu den besten Casinos, Spielen und Boni.
Der Casino Guru Zet hat sich einen Ruf als vertrauenswürdige Quelle für Glücksspielbegeisterte auf der ganzen Welt erarbeitet. Seine Bewertungen und Empfehlungen sind bekannt für ihre Fairness und Neutralität, da er sich strikt an strenge Kriterien und Standards hält.
Mit seiner langjährigen Erfahrung und Fachkenntnis bietet der Casino Guru Zet Spielern nützliche Tipps und Tricks, um ihr Spielerlebnis zu optimieren und ihre Gewinnchancen zu erhöhen. Er ist auch bekannt für seine exklusiven Deals und Promotionen, die den Spielern zusätzliche Vorteile und Anreize bieten.
Der Casino Guru Zet ist eine unverzichtbare Ressource für alle, die ihr Glück im Online-Casino versuchen möchten. Seine fundierten Bewertungen und umfassenden Informationen helfen den Spielern, die besten Entscheidungen zu treffen und das Beste aus ihrem Glücksspiel-Erlebnis herauszuholen.
https://zetcasino.one/
voyah free 2023 2024
zeekr 001 2024
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha v.3, Hotmail (Microsoft), Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), RuCaptcha, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
Immer mehr Online-Casinos bieten ihren Kunden attraktive Bonusangebote an, um neue Spieler anzulocken und bestehende Kunden zu belohnen. Ein solches Angebot ist der sogenannte “boomerang.bet casino no deposit bonus”.
Bei einem No Deposit Bonus handelt es sich um einen Bonus, den Spieler erhalten, ohne dass sie zuvor eine Einzahlung tätigen müssen. Das bedeutet, dass man kostenlos spielen und echtes Geld gewinnen kann, ohne dabei eigenes Geld riskieren zu müssen.
Der boomerang.bet casino no deposit bonus ist besonders beliebt bei Spielern, die gerne risikofrei neue Spiele ausprobieren möchten. Mit diesem Bonus können Spieler verschiedene Spielautomaten, Tischspiele und andere Casino-Spiele ausprobieren, ohne dabei ihr eigenes Geld einzusetzen. Das bietet eine tolle Möglichkeit, um die verschiedenen Spiele des Casinos kennenzulernen und sich mit den Abläufen vertraut zu machen.
Um den boomerang.bet casino no deposit bonus zu erhalten, müssen Spieler sich lediglich auf der Webseite des Casinos registrieren. Anschließend wird der Bonus automatisch gutgeschrieben und kann sofort zum Spielen genutzt werden. Dabei sollten Spieler jedoch die Umsatzbedingungen beachten, die festlegen, wie oft der Bonus umgesetzt werden muss, bevor eine Auszahlung möglich ist.
Insgesamt bietet der boomerang.bet casino no deposit bonus eine tolle Gelegenheit, um kostenlos Casino-Spiele zu spielen und echtes Geld zu gewinnen. Spieler sollten diese Chance nutzen und sich die spannenden Spiele des Casinos genauer anschauen. Viel GlГјck und SpaГџ beim Spielen!
https://boomerangcasino.one/
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha v.3, Hotmail (Microsoft), Google captcha, SolveMedia, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
тирзепатид – трулисити отзывы, Оземпик 3мл
Das Boomerang Casino ist eine aufregende neue Online-Spielhalle, die sich auf dem Markt etabliert hat. Mit einer Vielzahl von Spielen und beeindruckenden Grafiken bietet das Boomerang Casino eine unterhaltsame und aufregende Spielerfahrung fГјr GlГјcksspielfans in aller Welt.
Das Boomerang Casino bietet eine große Auswahl an beliebten Casino-Spielen, darunter Spielautomaten, Blackjack, Roulette, Poker und vieles mehr. Die Spiele werden von führenden Softwareanbietern entwickelt, was bedeutet, dass Spieler eine hochwertige und sichere Spielerfahrung genießen können.
Eine der bemerkenswertesten Funktionen des Boomerang Casinos ist sein Treueprogramm, das es Spielern ermöglicht, Punkte zu sammeln und diese gegen Belohnungen einzutauschen. Das Casino bietet auch regelmäßige Aktionen und Boni, um Spieler zu belohnen und ihre Spielerfahrung zu verbessern.
Das Boomerang Casino legt großen Wert auf die Sicherheit seiner Spieler und verwendet modernste Verschlüsselungstechnologien, um sicherzustellen, dass alle Transaktionen sicher und geschützt sind. Das Casino ist auch vollständig lizenziert und reguliert, um sicherzustellen, dass es den höchsten Standards entspricht.
Insgesamt ist das Boomerang Casino eine spannende und aufregende Destination fГјr GlГјcksspielfans, die nach einer erstklassigen Spielerfahrung suchen. Mit einer groГџartigen Auswahl an Spielen, aufregenden Aktionen und einem engagierten Kundenservice ist das Boomerang Casino definitiv einen Besuch wert.
https://boomerangcasino.one/
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha-3, Hotmail, Google captcha, SolveMedia, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
Das Online Casino Boomerang: Ein aufregendes Spielerlebnis
Das Online Casino Boomerang ist ein aufregendes neues Online-Casino, das von erfahrenen Casino-Experten entwickelt wurde. Es bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele, die alle mit state-of-the-art-Technologie entwickelt wurden, um ein faires und spannendes Spielerlebnis zu bieten.
Einer der Hauptvorteile des Online Casino Boomerang ist sein einzigartiges Belohnungssystem. Spieler können sich für das Treueprogramm anmelden und Punkte sammeln, indem sie einfach spielen. Diese Punkte können dann gegen tolle Belohnungen wie Bonusguthaben, Freispiele und sogar Sachpreise eingelöst werden.
Darüber hinaus bietet das Online Casino Boomerang auch eine Vielzahl von sicheren und schnellen Zahlungsmethoden, einschließlich Kreditkarten, E-Wallets und Banküberweisungen. Spieler können sicher sein, dass ihre Einzahlungen und Auszahlungen schnell und einfach abgewickelt werden.
Ein weiterer Vorteil des Online Casino Boomerang ist sein hervorragender Kundenservice. Das Team von Casino-Experten steht rund um die Uhr zur Verfügung, um Fragen zu beantworten und Probleme zu lösen. Spieler können sich per Live-Chat, E-Mail oder Telefon an das Support-Team wenden.
Insgesamt bietet das Online Casino Boomerang ein aufregendes und faires Spielerlebnis fГјr alle Casino-Liebhaber. Mit einer Vielzahl von Spielen, einem groГџzГјgigen Belohnungssystem und erstklassigem Kundenservice ist es definitiv einen Besuch wert. Besuchen Sie noch heute das Online Casino Boomerang und erleben Sie die Spannung und Aufregung des Online-GlГјcksspiels.
https://boomerangcasino.one/
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha-3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captcha (antigate), rucaptcha.com, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
click over here cs2 skin changer dll
visit this website localbitcoins reviews
ссылка на кракен в тор – kraken ссылка тор, кракен онион
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha-3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), rucaptcha.com, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
Tipico Sport Konto blockiert auf Casino
Sie haben gerade versucht, sich bei Ihrem Tipico Sport Konto anzumelden, um eine Wette zu platzieren oder Ihr Guthaben zu überprüfen, doch plötzlich erhalten Sie die Meldung, dass Ihr Konto blockiert ist. Was nun?
Es gibt verschiedene Gründe, warum Ihr Tipico Sport Konto blockiert sein könnte, insbesondere wenn Sie versucht haben, auf das Tipico Casino zuzugreifen. Eine mögliche Ursache könnte sein, dass Sie gegen die Nutzungsbedingungen verstoßen haben, wie zum Beispiel die Verwendung von VPNs oder anderen unerlaubten Methoden, um auf das Casino zuzugreifen.
Eine weitere mögliche Ursache für die Sperrung Ihres Kontos könnte sein, dass Tipico Verdacht auf betrügerische Aktivitäten hat. In diesem Fall ist es wichtig, den Kundendienst zu kontaktieren und nach den Gründen für die Sperrung zu fragen. Möglicherweise müssen Sie zusätzliche Dokumente zur Überprüfung Ihrer Identität bereitstellen, um Ihr Konto wieder freizuschalten.
Es ist wichtig, ruhig zu bleiben und den Anweisungen des Kundendienstes zu folgen, um Ihr Konto schnellstmöglich wieder freizuschalten. Vermeiden Sie es, weitere E-Mails oder Anrufe mit Beschwerden zu tätigen, da dies den Prozess nur verzögern könnte.
Wenn Ihr Tipico Sport Konto blockiert ist, bedeutet das nicht zwangsläufig, dass Sie dauerhaft von der Nutzung des Casinos ausgeschlossen sind. Mit der richtigen Kommunikation und Zusammenarbeit mit dem Kundendienst können Sie Ihr Konto in den meisten Fällen wieder freischalten und weiterhin Ihre Lieblings-Sportwetten platzieren oder Casinospiele genießen.
Zusammenfassend ist es wichtig, den Kundendienst zu kontaktieren und die Gründe für die Sperrung Ihres Kontos zu erfragen, um den Prozess zur Freischaltung zu beschleunigen. Vermeiden Sie es, gegen die Nutzungsbedingungen zu verstoßen und folgen Sie den Anweisungen des Kundendienstes, um Ihr Tipico Sport Konto schnellstmöglich wieder nutzen zu können.
https://tipicocasino.one/
сайт кракен тор – кракен ссылка тор, кракен ссылка тор
read what he said hacks for roblox
more info here hack cs2
кондиционеры для дома https://split-sistema-kupit.ru/ .
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha-3, Hotmail (Microsoft), Google, SolveMedia, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), RuCaptcha, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
Zet Casino Störung
Das beliebte Online-Casino Zet Casino hat in letzter Zeit mit einigen technischen Störungen zu kämpfen. Viele Spieler berichten von Verbindungsproblemen, langen Ladezeiten und sogar Abstürzen während des Spielens. Diese Störungen führen nicht nur zu Frustration bei den Spielern, sondern können auch dazu führen, dass diese ihr Vertrauen in das Casino verlieren und sich nach einer anderen Plattform umsehen.
Die Ursachen für diese Störungen sind bisher nicht bekannt. Es wird jedoch vermutet, dass sie auf technische Probleme mit den Servern oder der Software des Casinos zurückzuführen sind. Die Betreiber des Casinos arbeiten bereits daran, diese Probleme so schnell wie möglich zu beheben und die bestmögliche Spielerfahrung zu gewährleisten.
In der Zwischenzeit empfehlen wir den Spielern, geduldig zu sein und die offiziellen Social-Media-Kanäle des Casinos im Auge zu behalten, um über den aktuellen Stand der Störungen informiert zu bleiben. Es ist auch ratsam, regelmäßig die Webseite des Casinos zu besuchen, um Updates zu erhalten und mögliche Entschädigungen oder Sonderaktionen in Anspruch zu nehmen.
Trotz der aktuellen Probleme bleibt Zet Casino eine der beliebtesten Online-Glücksspielplattformen und bietet eine Vielzahl von Spielen und Bonusangeboten für seine Spieler. Wir hoffen, dass die Störungen bald behoben werden und die Spieler wieder ein reibungsloses Spielerlebnis genießen können.
https://zetcasino.one/
Юридическая помощь при заливах квартир — незаменимый инструмент для защиты ваших прав и интересов. Попадание в подобную ситуацию влечет за собой ряд сложностей, начиная от оформления необходимых бумаг и заканчивая взысканием убытков с виновника происшествия.
Профессиональный юрист поможет составить акт о заливе, который фиксирует факт и обстоятельства повреждения имущества. Далее следует этап сбора доказательств: фотографии, справки о стоимости ущерба, свидетельские показания. Важно правильно рассчитать размер убытков, включающий стоимость восстановительного ремонта и прочие затраты.
Юрист займется подготовкой претензии к виновнику инцидента с требованием возместить ущерб. В случае отказа или игнорирования претензии вопрос может быть передан в суд. С юридической точки зрения процесс требует грамотной подготовки и стратегии, что станет залогом успешного результата.
Получение юридической помощи позволит вам чувствовать себя увереннее, а также избежать потенциальных подводных камней в процессе взыскания компенсации за залив квартиры.
юрист по заливу
motomagazinvfdvgd.vn.ua/uk/v-ekipirovka/
В ТЕЧЕНИЕ нашем мотомагазине вы найдёте запчасти для байков, скутеров, снегоходов равно квадроциклов. У нас ваша милость хронически почтете масла для байков, фильтра, цепи.
motomagazinvfdvgd.vn.ua/uk/v-masla-motornye/
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha v.3, Hotmail, Google, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
Das Zet Casino hat in den letzten Jahren an Popularität gewonnen und viele Spieler fragen sich, ob es sich um ein seriöses Online-Casino handelt. In diesem Artikel werden wir die wichtigsten Punkte beleuchten, um festzustellen, ob das Zet Casino vertrauenswürdig ist.
Zunächst einmal ist das Zet Casino im Besitz einer gültigen Glücksspiellizenz der Malta Gaming Authority, einer der angesehensten Regulierungsbehörden in der Glücksspielbranche. Dies bedeutet, dass das Casino strenge Vorschriften einhalten muss, um sicherzustellen, dass es fair und transparent ist. Darüber hinaus verwendet das Zet Casino eine sichere SSL-Verschlüsselung, um sicherzustellen, dass alle Ihre persönlichen Daten geschützt sind.
Ein weiterer wichtiger Aspekt ist die Spielauswahl. Das Zet Casino bietet eine Vielzahl von Spielen von renommierten Entwicklern wie NetEnt, Microgaming und Play’n GO an. Dies bedeutet, dass die Spiele fair und zufГ¤llig sind, da sie von unabhГ¤ngigen Drittorganisationen regelmäßig ГјberprГјft werden.
DarГјber hinaus bietet das Zet Casino verschiedene Zahlungsmethoden an, darunter Kreditkarten, E-Wallets und BankГјberweisungen. Alle Ein- und Auszahlungen werden schnell und sicher abgewickelt, um sicherzustellen, dass Ihre Gewinne rechtzeitig ausgezahlt werden.
Zusammenfassend lässt sich sagen, dass das Zet Casino als seriöses und vertrauenswürdiges Online-Casino angesehen werden kann. Mit einer gültigen Lizenz, einer vielfältigen Spielauswahl und sicheren Zahlungsmethoden ist das Zet Casino eine gute Wahl für Spieler, die eine sichere und unterhaltsame Glücksspielerfahrung suchen.
https://zetcasino.one/
navigate to this website keplr wallet login
great site phantom wallet
Source martianwallet extension
Boomerang Casino – ОљПЃО№П„О№ОєОП‚
Boomerang Casino ist eine beliebte Online-GlГјcksspielplattform, die eine Vielzahl von Spielen und Dienstleistungen fГјr ihre Spieler anbietet. In diesem Artikel werden wir einige der wichtigsten Aspekte des Boomerang Casinos und die Meinungen der Spieler darГјber diskutieren.
Als erstes ist die Vielfalt an Spielen, die Boomerang Casino anbietet, eine der Hauptattraktionen für die Spieler. Von Slots über Tischspiele bis hin zu Live-Casino-Spielen gibt es für jeden Geschmack und jede Vorliebe etwas zu finden. Die hohe Qualität der Spiele wird von den Spielern häufig gelobt, da sie faire Gewinnchancen und ein beeindruckendes Spielerlebnis bieten.
Ein weiterer positiver Punkt, der häufig in den Bewertungen des Boomerang Casinos hervorgehoben wird, ist der Kundenservice. Die Mitarbeiter des Casinos werden als freundlich, kompetent und hilfsbereit beschrieben, was den Spielern ein Gefühl von Sicherheit und Vertrauen vermittelt.
Auch die Zahlungsmethoden und die schnelle Auszahlung werden von den Spielern positiv bewertet. Das Boomerang Casino bietet eine Vielzahl von sicheren und bequemen Zahlungsoptionen an, die es den Spielern ermöglichen, problemlos Ein- und Auszahlungen zu tätigen.
Einige Spieler haben jedoch auch negative Erfahrungen mit dem Boomerang Casino gemacht. Einige haben berichtet, dass es gelegentlich zu technischen Problemen kommen kann, die das Spielerlebnis beeinträchtigen. Andere haben angemerkt, dass die Bonusbedingungen manchmal verwirrend sein können und es schwierig sein kann, diese zu erfüllen.
Insgesamt scheint das Boomerang Casino jedoch eine beliebte und vertrauenswürdige Online-Glücksspielplattform zu sein, die den Spielern ein unterhaltsames und sicheres Spielerlebnis bietet. Der gute Kundenservice, die Vielfalt an Spielen und die zuverlässigen Zahlungsmethoden machen das Boomerang Casino zu einer guten Wahl für Glücksspielenthusiasten.
Wenn Sie also auf der Suche nach einem zuverlässigen und unterhaltsamen Online-Casino sind, könnte das Boomerang Casino die richtige Wahl für Sie sein. Schauen Sie sich die verschiedenen Spiele und Dienstleistungen an und entscheiden Sie selbst, ob das Boomerang Casino Ihren Bedürfnissen entspricht. Viel Glück und viel Spaß beim Spielen!
https://boomerangcasino.one/
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha v.3, Hotmail (Microsoft), Google, SolveMedia, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), rucaptcha.com, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
browse around here Celestia wallet keplr
check my source rabby wallet download
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha v.3, Hotmail, Google, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captchas.com (antigate), RuCaptcha, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
Das Tipico Live Casino Blackjack ist eines der beliebtesten Spiele in der Welt des Online-Glücksspiels. Mit seiner spannenden Atmosphäre und den attraktiven Gewinnchancen zieht es viele Spieler an, die auf der Suche nach Nervenkitzel und Unterhaltung sind.
Das Spielprinzip des Live Casino Blackjacks ist einfach: Ziel ist es, mit den eigenen Karten so nah wie möglich an die Zahl 21 zu gelangen, ohne dabei zu überschreiten. Der Spieler tritt dabei gegen den Dealer an, der ebenfalls Karten erhält. Durch geschicktes Setzen und Einschätzen der eigenen Chancen kann man das Spiel für sich entscheiden und attraktive Gewinne erzielen.
Ein besonderer Reiz des Tipico Live Casino Blackjacks liegt darin, dass man gegen echte Dealer spielt, die per Live-Stream zugeschaltet sind. Dadurch entsteht eine authentische Casino-Atmosphäre, die die Spieler direkt in das Geschehen hineinzieht. Zudem bietet das Live Casino die Möglichkeit, mit anderen Spielern zu interagieren und sich über Strategien und Tipps auszutauschen.
Besonders positiv fällt bei Tipico die hohe Qualität der Live-Übertragung auf. Die Dealer sind professionell geschult und sorgen für ein reibungsloses Spielvergnügen. Zudem stehen verschiedene Varianten des Blackjack zur Auswahl, sodass für jeden Geschmack das passende Spiel dabei ist.
FГјr Neulinge im Bereich des Live Casino Blackjacks bietet Tipico zudem Tutorials und Hilfestellungen an, um sich mit den Regeln vertraut zu machen und die besten Strategien zu erlernen. Somit steht einem erfolgreichen und unterhaltsamen Spieleerlebnis nichts im Wege.
Alles in allem ist das Tipico Live Casino Blackjack eine hervorragende Möglichkeit, um sich in die Welt des Online-Glücksspiels zu stürzen. Mit seinem spannenden Spielprinzip, der authentischen Casino-Atmosphäre und den attraktiven Gewinnchancen bietet es ein unvergessliches Spielerlebnis für alle Fans von Blackjack.
https://tipicocasino.one/
Det har kommit till vår kännedom att många spelare har rapporterat att Gogo Casino inte har betalat ut sina vinster. Detta är naturligtvis mycket oroande och något som vi vill ta upp här.
Att inte få sina vinster utbetalda från ett casino är inte bara frustrerande, det är också helt olämpligt. När man spelar på ett online casino förväntar man sig att ens vinster betalas ut korrekt och i tid. Tyvärr verkar det som att Gogo Casino inte lever upp till detta löfte för många av sina spelare.
Det är viktigt att påpeka att detta inte är acceptabelt beteende från ett casino och att spelare som upplever att deras vinster inte betalas ut borde rapportera detta till de relevanta myndigheterna. Det är också bra att dela med sig av sina erfarenheter till andra spelare för att varna dem från att spela på detta casino.
Vi hoppas att Gogo Casino tar dessa rapporter på allvar och åtgärdar eventuella problem med utbetalningarna så att deras spelare kan fortsätta spela med trygghet och förtroende. Men tills dess uppmanar vi alla spelare att vara försiktiga och noggrant överväga sina alternativ innan de beslutar att spela på detta casino.
https://gogocasino.one
navigate to this website keplr wallet
Gogo Casino är en online casino som erbjuder ett brett utbud av spel och möjligheten att vinna stora vinster. AskGamblers är en populär webbplats som recenserar olika online kasinon och ger spelare möjlighet att dela sina erfarenheter och åsikter.
Gogo Casino har fått mycket positiv feedback från spelare på AskGamblers för dess enkla användargränssnitt och generösa bonusar. Många spelare har berömt kasinot för dess utmärkta kundsupport och snabba uttag.
För de som letar efter en pålitlig och underhållande spelupplevelse, är Gogo Casino definitivt värt att kolla in. Med ett stort utbud av spel från några av de bästa leverantörerna i branschen, finns det något för alla spelare att njuta av.
Så om du letar efter ett online casino med hög kvalitet och bra rykte, ta en titt på Gogo Casino och se om det är rätt för dig. Med hjälp av AskGamblers recensioner och spelares åsikter kan du vara säker på att du får en förstklassig spelupplevelse.
https://gogocasino.one
Gogo casino app är ett populärt online casino där spelare kan njuta av en mängd olika casinospel direkt från sina mobila enheter. Appen erbjuder en smidig och enkel spelupplevelse för alla som älskar att spela på casino.
Med Gogo casino app kan spelare njuta av en rad olika spel, inklusive slotmaskiner, blackjack, roulette och mycket mer. Appen är lätt att navigera och ger spelarna möjlighet att spela sina favoritspel var de än befinner sig.
En av fördelarna med att använda Gogo casino app är att den erbjuder en mängd olika bonusar och kampanjer för spelarna. Dessa kan inkludera välkomstbonusar, free spins och insättningsbonusar, vilket ger spelarna chansen att öka sina vinster och njuta ännu mer av sina favoritspel.
Appen erbjuder också säkra och pålitliga betalningsmetoder för spelarna, vilket gör det enkelt att sätta in och ta ut pengar från sitt spelkonto. Spelarna kan känna sig trygga med att deras personliga och finansiella information är skyddad när de använder Gogo casino app.
Sammanfattningsvis är Gogo casino app en fantastisk plattform för alla som älskar att spela på casino. Med ett brett utbud av spel, generösa bonusar och enkel användning är det ett utmärkt val för alla som vill ha en förstklassig spelupplevelse på sin mobila enhet. Så varför inte ladda ner appen idag och börja spela? Lycka till!
https://gogocasino.one
Gogo Casino är en online casino som har fått stor uppmärksamhet på AskGamblers, en populär casinorecensionswebbplats. Med sitt enkla och stilrena gränssnitt lockar Gogo Casino spelare från hela världen.
En av anledningarna till Gogo Casinos popularitet är deras stora utbud av spel. Från klassiska slotmaskiner till live dealer-spel, finns det något för alla typer av spelare på Gogo Casino. Dessutom erbjuder de generösa bonusar och kampanjer för att belöna sina spelare.
En annan anledning till att Gogo Casino har fГҐtt positiva recensioner pГҐ AskGamblers Г¤r deras pГҐlitliga kundsupport. Spelare kan enkelt kontakta supportteamet via live chat eller e-post och fГҐ snabba svar pГҐ sina frГҐgor.
Sammanfattningsvis är Gogo Casino ett pålitligt och underhållande online casino som är väl värda ett besök. Med sitt stora spelutbud, generösa bonusar och pålitliga kundsupport, har de blivit en favorit bland spelare på AskGamblers och andra recensionswebbplatser. Besök Gogo Casino idag och prova lyckan!
https://gogocasino.one
see here martianwallet wallet download
http://flowervl.ru/
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha-3, Hotmail (Microsoft), Google, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captchas.com (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
Das Boomerang Casino in der Schweiz ist ein beliebtes Ziel für Glücksspiel-Enthusiasten. Mit einer Vielzahl von Spielen, großzügigen Boni und einer eleganten Atmosphäre bietet das Casino eine erstklassige Spielerfahrung.
Das Boomerang Casino bietet eine breite Palette von Spielen, darunter Slots, Tischspiele und Live-Dealer-Spiele. Die Spieler können aus verschiedenen Variationen von Blackjack, Roulette, Poker und anderen beliebten Casino-Spielen wählen. Mit hochwertiger Grafik und reibungsloser Gameplay-Software bietet das Boomerang Casino eine hochwertige Spielerfahrung.
Darüber hinaus bietet das Boomerang Casino großzügige Boni und Promotionen für neue und bestehende Spieler. Von Willkommensboni über Einzahlungsboni bis hin zu Treueprogrammen gibt es immer spannende Möglichkeiten, zusätzliches Geld zu gewinnen und das Spielerlebnis zu maximieren.
Die elegante Atmosphäre des Boomerang Casinos trägt dazu bei, dass sich die Spieler wie in einem exklusiven Club fühlen. Mit stilvoller Einrichtung, freundlichem Personal und hochwertigem Service ist das Boomerang Casino der perfekte Ort, um eine Nacht voller Glücksspiel und Unterhaltung zu verbringen.
Insgesamt ist das Boomerang Casino in der Schweiz definitiv einen Besuch wert, ob man ein erfahrener Spieler ist oder einfach nur eine unterhaltsame Nacht verbringen möchte. Mit einer großen Auswahl an Spielen, großzügigen Boni und einer eleganten Atmosphäre bietet das Casino eine erstklassige Spielerfahrung, die man nicht verpassen sollte.
https://boomerangcasino.one/
Zet Casino Online: Ein aufregendes Erlebnis fГјr GlГјcksspiel-Fans
Das Zet Casino ist eine Online-Glücksspielplattform, die Spielern aus der ganzen Welt die Möglichkeit bietet, ihre Lieblingsspiele bequem von zu Hause aus zu genießen. Mit einer breiten Auswahl an Slots, Tischspielen und Live-Casino-Spielen ist für jeden Geschmack und jede Vorliebe etwas dabei.
Ein besonderes Merkmal des Zet Casinos ist die benutzerfreundliche Oberfläche, die es den Spielern ermöglicht, problemlos auf die verschiedenen Spiele und Funktionen zuzugreifen. Darüber hinaus bietet die Plattform eine Vielzahl von Bonusangeboten und Promotionen, die das Spielerlebnis noch aufregender machen.
Ein weiterer Vorteil des Zet Casinos ist die Vielzahl von Zahlungsmethoden, die den Spielern zur Verfügung stehen. Von Kreditkarten über E-Wallets bis hin zu Kryptowährungen gibt es für jeden Spieler die passende Option, um Ein- und Auszahlungen schnell und sicher abzuwickeln.
Darüber hinaus legt das Zet Casino großen Wert auf Kundenservice und Sicherheit. Das Support-Team ist rund um die Uhr erreichbar und steht den Spielern bei Fragen oder Problemen zur Seite. Zudem werden alle persönlichen Daten der Spieler streng vertraulich behandelt und die Plattform verfügt über eine gültige Lizenz, die sicherstellt, dass alle Spiele fair und transparent ablaufen.
Insgesamt bietet das Zet Casino eine unterhaltsame und sichere Umgebung für Glücksspiel-Fans, die auf der Suche nach neuen Spielmöglichkeiten sind. Mit einer großen Auswahl an Spielen, lukrativen Bonusangeboten und einem erstklassigen Kundenservice ist das Zet Casino definitiv einen Besuch wert. Probieren Sie es aus und erleben Sie den Nervenkitzel des Glücksspiels online!
https://zetcasino.one/
Tipico Casino Guthaben gesperrt – Was tun?
Das Tipico Casino gehört zu den beliebtesten Online-Casinos in Deutschland und begeistert viele Spieler mit einer vielfältigen Auswahl an Spielen und attraktiven Bonusangeboten. Doch was passiert, wenn plötzlich das Guthaben im Casino gesperrt wird?
Es gibt verschiedene Gründe, warum das Guthaben im Tipico Casino gesperrt werden kann. Häufig liegt es an Verstößen gegen die Nutzungsbedingungen des Casinos, beispielsweise durch das Spielen mit mehreren Accounts oder das Verdacht auf Betrug. Auch technische Probleme können dazu führen, dass das Guthaben vorübergehend gesperrt wird.
Doch was können Spieler tun, wenn ihr Guthaben gesperrt wurde? Zunächst sollten sie sich an den Kundenservice des Tipico Casinos wenden und das Problem schildern. Oftmals kann der Kundenservice weiterhelfen und die Sperrung aufheben, falls es sich um einen Irrtum handelt.
Sollte das Guthaben tatsächlich rechtmäßig gesperrt worden sein, ist es wichtig, die Ursache zu klären und gegebenenfalls Maßnahmen zu ergreifen, um eine erneute Sperrung zu vermeiden. Spieler sollten sich in diesem Fall die Nutzungsbedingungen des Tipico Casinos genau durchlesen und sicherstellen, dass sie sich an diese halten.
Insgesamt ist es wichtig, ruhig zu bleiben und das Problem sachlich anzugehen, wenn das Guthaben im Tipico Casino gesperrt wird. Mit dem richtigen Vorgehen und der Unterstützung des Kundenservice lässt sich die Sperrung meist schnell klären und das Spielerlebnis im Tipico Casino kann fortgesetzt werden.
https://tipicocasino.one/
Boomerang Casino ist eine beliebte Online-Spielplattform, die ihren Spielern eine Vielzahl von Spielen und Funktionen bietet. Es gibt jedoch ein bestimmtes Thema, das Spieler immer wieder fragen: das Auszahlungslimit im Boomerang Casino.
Das Auszahlungslimit im Boomerang Casino bezieht sich auf die maximale Menge an Geld, die ein Spieler auf einmal aus seinem Konto abheben kann. Dieses Limit variiert je nach Zahlungsmethode und Spielerstatus. Es gibt verschiedene Faktoren, die das Auszahlungslimit beeinflussen können, wie zum Beispiel die Höhe der Einzahlungen, die der Spieler getätigt hat, und ob der Spieler ein VIP-Mitglied ist.
Es ist wichtig zu beachten, dass das Auszahlungslimit im Boomerang Casino für den Schutz der Spieler festgelegt wurde. Es hilft, finanzielle Risiken zu minimieren und den Spielern ein sicheres und verantwortungsbewusstes Spielerlebnis zu bieten. Das Limit ist in den Allgemeinen Geschäftsbedingungen des Casinos festgelegt, sodass es wichtig ist, diese zu lesen und zu verstehen, bevor man mit dem Spielen beginnt.
Wenn ein Spieler das Auszahlungslimit erreicht, kann er möglicherweise keine weiteren Auszahlungen tätigen, bis das Limit zurückgesetzt oder erhöht wird. In einigen Fällen kann der Spieler Kontakt mit dem Kundendienst aufnehmen und eine Erhöhung seines Auszahlungslimits beantragen.
Insgesamt ist das Auszahlungslimit im Boomerang Casino ein wichtiger Aspekt, den Spieler im Auge behalten sollten. Es ist wichtig, verantwortungsbewusst zu spielen und die Regeln und Grenzen des Casinos zu respektieren, um ein positives Spielerlebnis zu gewährleisten. Wenn Fragen oder Probleme auftreten, steht der Kundendienst des Casinos jederzeit zur Verfügung, um Unterstützung zu bieten.
https://boomerangcasino.one/
Zet Casino AskGamblers
Das Zet Casino ist eine beliebte Online-Glücksspielseite, die eine Vielzahl von Spielen für Spieler aus der ganzen Welt anbietet. Eine der besten Möglichkeiten, um sich über die Qualität eines Online-Casinos zu informieren, ist die Bewertung auf der Website AskGamblers. Hier haben Nutzer die Möglichkeit, ihre Erfahrungen und Meinungen zu teilen, um anderen bei der Entscheidung zu helfen, ob sie sich bei einem bestimmten Casino anmelden sollen oder nicht.
Das Zet Casino hat auf AskGamblers eine beeindruckende Bewertung von 4 von 5 Sternen erhalten und wird von vielen Spielern hoch gelobt. Die Benutzer loben insbesondere die große Auswahl an Spielen, die benutzerfreundliche Website und den exzellenten Kundenservice. Viele Spieler schätzen auch die schnellen Auszahlungen und die Vielzahl von Zahlungsoptionen, die das Zet Casino anbietet.
Ein weiterer Pluspunkt des Zet Casinos ist das attraktive Bonusprogramm für Neukunden und treue Spieler. Es gibt regelmäßige Bonusangebote, Freispiele und Turniere, die den Spielern zusätzliche Gewinnchancen bieten. Die Boni sind fair und transparent, ohne versteckte Bedingungen, was bei Spielern gut ankommt.
Insgesamt ist das Zet Casino eine hervorragende Wahl für Glücksspielfans, die eine sichere und unterhaltsame Online-Spielerfahrung suchen. Mit einer breiten Palette von Spielen, großzügigen Boni und einem zuvorkommenden Kundenservice bietet das Zet Casino alles, was man sich von einem erstklassigen Online-Casino wünscht. Wer also auf der Suche nach einem zuverlässigen und spaßigen Casino ist, sollte das Zet Casino auf jeden Fall in Betracht ziehen.
https://zetcasino.one/
Zet Casino Einzahlungsbonus
Zet Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und attraktiven Boni für ihre Spieler anbietet. Einer der beliebtesten Boni auf der Website ist der Einzahlungsbonus, der neuen Spielern angeboten wird, die sich zum ersten Mal auf der Plattform registrieren und eine Einzahlung tätigen.
Der Zet Casino Einzahlungsbonus ist eine großartige Möglichkeit für Spieler, ihr Spielkonto aufzustocken und mehr Zeit mit ihren Lieblingsspielen zu verbringen. Der Bonus variiert je nach Höhe der Einzahlung und kann bis zu einem bestimmten Betrag erhöht werden, was es den Spielern ermöglicht, mehr zu gewinnen und ihre Gewinnchancen zu erhöhen.
Um den Einzahlungsbonus zu erhalten, müssen die Spieler lediglich eine Einzahlung auf ihr Konto vornehmen und den Bonuscode angeben, der auf der Website bereitgestellt wird. Sobald die Einzahlung bestätigt wurde, wird der Bonus automatisch gutgeschrieben und kann sofort für Spiele auf der Plattform verwendet werden.
Es ist wichtig zu beachten, dass der Einzahlungsbonus bestimmten Bedingungen und Anforderungen unterliegt, die von den Spielern erfüllt werden müssen, um den Bonus und damit verbundene Gewinne abheben zu können. Diese Bedingungen können von der Höhe der Einzahlung bis zu den Umsatzanforderungen für den Bonus reichen.
Insgesamt ist der Zet Casino Einzahlungsbonus eine großartige Möglichkeit für Spieler, mehr aus ihrer Online-Glücksspielerfahrung herauszuholen und ihre Gewinnchancen zu erhöhen. Mit einer Vielzahl von Spielen und attraktiven Boni ist Zet Casino eine der besten Optionen für Spieler, die auf der Suche nach einem unterhaltsamen und lukrativen Casinoerlebnis sind.
https://zetcasino.one/
Boomerang Casino mobiili: Die Zukunft des Online-GlГјcksspiels
Das Online-GlГјcksspiel hat in den letzten Jahren stark an Beliebtheit gewonnen, und mit der EinfГјhrung von mobilen Casinos wird diese Branche noch dynamischer. Eine der neuesten Entwicklungen in diesem Bereich ist das Boomerang Casino mobiili, das Spielern ein unvergleichliches Spielerlebnis bietet.
Boomerang Casino mobiili ist eine mobile Version des beliebten Online-Casinos Boomerang Casino. Es wurde speziell für Spieler entwickelt, die gerne unterwegs spielen und ihre Lieblingsspiele jederzeit und überall genießen möchten. Mit der mobilen Version des Casinos können Spieler auf eine Vielzahl von Spielen zugreifen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr.
Eine der Hauptattraktionen des Boomerang Casino mobiili ist die Benutzerfreundlichkeit. Die mobile Plattform wurde so gestaltet, dass sie nahtlos auf verschiedenen mobilen Geräten funktioniert, darunter Smartphones und Tablets. Spieler können einfach die Website des Casinos über ihren mobilen Browser aufrufen und sofort mit dem Spielen beginnen, ohne Software herunterladen zu müssen.
Darüber hinaus bietet das Boomerang Casino mobiili eine Vielzahl von Boni und Promotionen für mobile Spieler. Neue Spieler können von großzügigen Willkommensangeboten profitieren, während treue Spieler regelmäßig mit Reload-Boni, Freispielen und anderen tollen Belohnungen belohnt werden.
Zusammenfassend lässt sich sagen, dass das Boomerang Casino mobiili die Zukunft des Online-Glücksspiels repräsentiert. Mit seiner benutzerfreundlichen Plattform, einem breiten Spieleangebot und großzügigen Boni ist es die ideale Wahl für Spieler, die auch unterwegs nicht auf ihr Lieblingscasino verzichten möchten. Probieren Sie es aus und erleben Sie die Spannung und Aufregung des Online-Glücksspiels wie nie zuvor!
https://boomerangcasino.one/
Zet Casino Promo Code 2021
Das Zet Casino ist eines der beliebtesten Online-Casinos unter Spielern auf der ganzen Welt. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und aufregenden Aktionen, gibt es immer einen guten Grund, dem Zet Casino einen Besuch abzustatten.
Für das Jahr 2021 hat das Zet Casino einige spannende Promo-Codes und Bonusangebote im Angebot. Diese Codes können dazu beitragen, das Spielerlebnis noch unterhaltsamer und lukrativer zu gestalten.
Einer der beliebtesten Promo-Codes, der derzeit im Zet Casino gГјltig ist, ist der Code “ZETBONUS”. Mit diesem Code erhalten Spieler einen groГџzГјgigen Willkommensbonus bei ihrer ersten Einzahlung. Dieser Bonus kann verwendet werden, um eine Vielzahl von Spielen im Casino zu genieГџen und die Gewinnchancen zu erhГ¶hen.
DarГјber hinaus gibt es noch viele weitere Promo-Codes und Aktionen im Zet Casino, die das Spielerlebnis verbessern kГ¶nnen. Egal ob Freispiele, Cashback-Angebote oder Einzahlungsboni – es lohnt sich immer, einen Blick auf die aktuellen Promotions des Casinos zu werfen.
Um den Promo-Code zu verwenden, müssen Spieler einfach während der Einzahlung den entsprechenden Code eingeben. Der Bonus wird dann automatisch gutgeschrieben und kann sofort genutzt werden.
Das Zet Casino ist bekannt für seine fairen Bedingungen und transparenten Bonusangebote. Spieler können sich also sicher sein, dass sie gute Gewinnchancen haben und ihre Gewinne ohne Probleme auszahlen lassen können.
Insgesamt ist der Promo-Code 2021 im Zet Casino eine großartige Möglichkeit, das Spielerlebnis zu verbessern und noch mehr Spaß und Spannung zu erleben. Wer also auf der Suche nach einem erstklassigen Online-Casino ist, sollte das Zet Casino definitiv in Betracht ziehen. Viel Glück beim Spielen!
https://zetcasino.one/
Das Tipico Online Casino bietet seinen Kunden eine Vielzahl an Zahlungsmethoden, um Einzahlungen auf ihr Spielerkonto vorzunehmen. Eine beliebte und sichere Option ist die Einzahlung per PayPal.
PayPal ist eine der weltweit führenden Zahlungsplattformen, die es ermöglicht, Geld sicher und schnell online zu transferieren. Die Verwendung von PayPal im Tipico Online Casino bietet Spielern eine bequeme und zuverlässige Möglichkeit, um Geld auf ihr Spielerkonto einzuzahlen.
Um eine Einzahlung mit PayPal im Tipico Online Casino durchzuführen, müssen Spieler einfach die Option auswählen, den gewünschten Betrag eingeben und die Transaktion bestätigen. Der eingezahlte Betrag wird sofort dem Spielerkonto gutgeschrieben, so dass Spieler sofort mit dem Spielen beginnen können.
Eine der Vorteile der Einzahlung per PayPal im Tipico Online Casino ist die Sicherheit. PayPal verwendet fortschrittliche Sicherheitsmaßnahmen, um sicherzustellen, dass Transaktionen geschützt sind und persönliche Daten der Spieler geschützt werden.
Darüber hinaus bietet PayPal Spielern auch eine gewisse Anonymität, da sie keine sensiblen Bankdaten oder Kreditkartendetails preisgeben müssen. Spieler können einfach ihre PayPal-Login-Daten verwenden, um schnell und sicher Einzahlungen im Tipico Online Casino zu tätigen.
Insgesamt bietet die Einzahlung per PayPal im Tipico Online Casino eine bequeme, sichere und zuverlässige Möglichkeit für Spieler, um Geld auf ihr Spielerkonto einzuzahlen. Spieler, die PayPal als Zahlungsmethode nutzen möchten, können dies einfach und unkompliziert tun und sofort mit dem Spielen beginnen.
https://tipicocasino.one/
Das Boomerang.bet Casino ist eine aufstrebende Online-GlГјcksspielplattform, die sich auf dem Markt einen Namen gemacht hat. In diesem Artikel werden wir eine detaillierte ГњberprГјfung dieses Casinos vornehmen, um Ihnen einen Einblick in das Angebot und die Funktionen zu geben.
Das Boomerang.bet Casino bietet eine breite Palette von Spielen, darunter Spielautomaten, Tischspiele, Live-Dealer-Spiele und vieles mehr. Die Spiele stammen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen, was fГјr eine qualitativ hochwertige Spielerfahrung sorgt.
Die Website von Boomerang.bet Casino ist benutzerfreundlich gestaltet und bietet eine nahtlose Navigation, um den Spielern ein reibungsloses Spielerlebnis zu ermöglichen. Das Casino bietet auch eine mobile Version der Website, die es den Spielern ermöglicht, ihre Lieblingsspiele von unterwegs aus zu genießen.
Ein weiterer großer Vorteil des Boomerang.bet Casinos ist der großzügige Willkommensbonus, der neuen Spielern einen zusätzlichen Anreiz bietet, sich anzumelden und einzuzahlen. Das Casino bietet auch regelmäßige Aktionen und Promotionen für bestehende Spieler, um ihre Spielerfahrung noch aufregender und lohnender zu machen.
Der Kundenservice von Boomerang.bet Casino steht den Spielern rund um die Uhr zur VerfГјgung und ist per E-Mail, Live-Chat und Telefon erreichbar. Das Team ist professionell und hilfsbereit und steht bereit, alle Fragen und Anliegen der Spieler zu beantworten.
Zusammenfassend lässt sich sagen, dass das Boomerang.bet Casino eine ausgezeichnete Wahl für Spieler ist, die auf der Suche nach einer unterhaltsamen und sicheren Glücksspielplattform sind. Mit einer Vielzahl von Spielen, großzügigen Boni und einem erstklassigen Kundenservice bietet das Casino eine rundum positive Spielerfahrung. Probieren Sie es noch heute aus und erleben Sie die Spannung und Aufregung des Boomerang.bet Casinos!
https://boomerangcasino.one/
Boomerang Casino: Ein aufregendes Spielerlebnis in Griechenland
Griechenland, ein Land bekannt fГјr seine atemberaubende Landschaft, reiche Geschichte und warmherzige BevГ¶lkerung, hat jetzt auch ein neues Highlight fГјr Besucher und Einheimische zu bieten – das Boomerang Casino. Dieses neue Casino hat sich schnell zu einem beliebten Ziel fГјr GlГјcksspielliebhaber entwickelt, die auf der Suche nach Spannung und Unterhaltung sind.
Das Boomerang Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele, die die Spieler stundenlang unterhalten können. Die hochmoderne Technologie und die ansprechende Grafik sorgen dafür, dass das Spielerlebnis unvergesslich bleibt. Darüber hinaus bietet das Casino großzügige Bonusangebote, die es den Spielern ermöglichen, ihr Guthaben zu erhöhen und mehr Spiele zu genießen.
Neben dem Glücksspiel bietet das Boomerang Casino auch eine Auswahl an Restaurants, Bars und Unterhaltungsmöglichkeiten, die sicherstellen, dass die Gäste eine unvergessliche Zeit haben. Mit regelmäßigen Veranstaltungen, Konzerten und Shows ist für jeden etwas dabei, um sein Spielerlebnis zu vervollständigen.
Das Casino befindet sich in einer großartigen Lage in Griechenland und ist leicht zu erreichen. Die Besucher können die malerische Umgebung genießen, während sie ihr Glück am Spieltisch versuchen. Mit einer freundlichen und kompetenten Mitarbeiter stehen die Gäste im Boomerang Casino im Mittelpunkt, was für ein unvergessliches Erlebnis sorgt.
Alles in allem bietet das Boomerang Casino in Griechenland ein aufregendes Spielerlebnis für Glücksspielliebhaber. Mit einer Vielzahl von Spielen, großzügigen Bonusangeboten und einer erstklassigen Unterhaltung ist das Boomerang Casino definitiv einen Besuch wert. Besuchen Sie noch heute das Boomerang Casino und erleben Sie die Spannung und Aufregung, die es zu bieten hat. Vielleicht haben Sie ja Glück und kehren mit einem schönen Gewinn nach Hause zurück.
https://boomerangcasino.one/
Das Zet Casino Forum: Alles, was du wissen musst
Das Zet Casino bietet seinen Spielern nicht nur eine Vielzahl von spannenden Spielen, sondern auch die Möglichkeit, sich mit anderen Spielern auszutauschen und zu vernetzen. Dafür gibt es das Zet Casino Forum, in dem Spieler ihre Erfahrungen teilen, Tipps und Tricks austauschen und sich über aktuelle Aktionen und Angebote informieren können.
Im Zet Casino Forum findest du verschiedene Bereiche, die auf unterschiedliche Themen rund um das Casino-Spiel spezialisiert sind. So gibt es beispielsweise Abschnitte für Strategien und Taktiken, wo Spieler ihre besten Tipps für bestimmte Spiele wie Roulette, Blackjack oder Spielautomaten teilen können. Auch gibt es einen Bereich für Neuigkeiten und Ankündigungen, in dem das Casino über aktuelle Aktionen informiert.
Ein weiterer wichtiger Bereich im Zet Casino Forum ist der Support-Bereich. Hier können Spieler Fragen stellen oder Probleme melden und erhalten schnell und unkompliziert Hilfe von anderen Spielern oder den Mitarbeitern des Casinos. So wird eine positive und unterstützende Community geschaffen, die es den Spielern ermöglicht, ihr Spielerlebnis zu maximieren.
Das Zet Casino Forum ist nicht nur eine Plattform zum Austausch, sondern auch eine Möglichkeit, Belohnungen zu erhalten. Durch aktive Teilnahme am Forum und das Teilen von hilfreichen Beiträgen können Spieler Punkte sammeln und diese gegen attraktive Preise eintauschen.
Insgesamt bietet das Zet Casino Forum eine tolle Möglichkeit, sich mit anderen Spielern zu vernetzen, sein Wissen zu erweitern und von den Erfahrungen anderer zu profitieren. Wer also gerne in einer Community von Gleichgesinnten aktiv ist und sein Casino-Erlebnis noch spannender gestalten möchte, sollte unbedingt einen Blick ins Zet Casino Forum werfen.
https://zetcasino.one/
Das Boomerang Casino ist eine neue Online-Glücksspielplattform, die speziell für deutsche Spieler entwickelt wurde. Mit einer umfangreichen Auswahl an Spielen, großzügigen Boni und einem benutzerfreundlichen Design hat das Boomerang Casino schnell an Popularität gewonnen.
Das Casino bietet eine Vielzahl von Slots, Tischspielen, Live-Dealer-Spielen und Jackpot-Slots von einigen der besten Anbieter der Branche. Spieler kГ¶nnen sich auf Spiele von Unternehmen wie NetEnt, Microgaming, Play’n GO und vielen anderen freuen.
Ein weiterer großer Vorteil des Boomerang Casinos sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler erhalten in der Regel einen Willkommensbonus, der aus Bonusgeld und Freispielen besteht. Darüber hinaus gibt es auch wöchentliche Aktionen, Turniere und Belohnungen für treue Spieler.
Die Plattform ist auch für mobile Geräte optimiert, sodass Spieler auch unterwegs spielen können. Das Casino bietet eine sichere und geschützte Spielumgebung, die von der Malta Gaming Authority lizenziert und reguliert wird.
Insgesamt bietet das Boomerang Casino deutschen Spielern eine unterhaltsame und lohnende Spielerfahrung. Mit einer breiten Palette an Spielen, groГџzГјgigen Boni und einer benutzerfreundlichen Plattform ist das Casino eine ausgezeichnete Wahl fГјr GlГјcksspielbegeisterte in Deutschland.
https://boomerangcasino.one/
Das Casino Boomerang: Eine aufregende neue Attraktion fГјr GlГјcksspielliebhaber
Das Casino Boomerang hat die Glücksspielwelt im Sturm erobert und bietet eine einzigartige und aufregende Erfahrung für alle, die gerne zocken. Diese innovative Attraktion ist ein Muss für alle Fans von Casinospielen und bietet eine Vielzahl von Spielmöglichkeiten, die garantiert jeden Spieler begeistern.
Das Casino Boomerang zeichnet sich durch seine vielfältige Auswahl an Spielen aus, darunter klassische Tischspiele wie Poker, Blackjack und Roulette, sowie eine große Auswahl an Spielautomaten und Videoslots. Die Spielhalle ist rund um die Uhr geöffnet und bietet eine freundliche und einladende Atmosphäre, die zum Verweilen einlädt.
Eine der einzigartigen Funktionen des Casino Boomerang ist das sogenannte “Boomerang-Spiel”, bei dem die Spieler die MГ¶glichkeit haben, ihre Gewinne zu verdoppeln oder zu vervielfachen, indem sie ihr GlГјck im Boomerang-Spiel versuchen. Dieses aufregende Feature sorgt fГјr zusГ¤tzliche Spannung und Nervenkitzel und macht das Casino Boomerang zu einem unvergesslichen Erlebnis.
Darüber hinaus bietet das Casino Boomerang eine Reihe von Sonderaktionen und Bonusangeboten, die es Spielern ermöglichen, zusätzliche Gewinne zu erzielen und ihre Gewinnchancen zu maximieren. Von kostenlosen Spins an den Spielautomaten bis hin zu exklusiven Turnieren und Wettbewerben gibt es immer etwas Neues und Spannendes im Casino Boomerang zu entdecken.
Für alle, die gerne spielen und auf der Suche nach einem einzigartigen und unterhaltsamen Erlebnis sind, ist das Casino Boomerang die perfekte Wahl. Mit seiner vielfältigen Auswahl an Spielen, spannenden Bonusangeboten und einem einladenden Ambiente ist das Casino Boomerang der perfekte Ort für Glücksspielliebhaber aller Art. Besuchen Sie das Casino Boomerang noch heute und erleben Sie die aufregende Welt des Glücksspiels in ihrer reinsten Form.
https://boomerangcasino.one/
Boomerang Casino Einzahlung: Eine neue Art des Spielens
Das Boomerang Casino ist eine der neuesten Online-Casino-Plattformen, die sich durch ihre innovativen Zahlungsmethoden auszeichnet. Eine dieser neuen Methoden ist die Boomerang Casino Einzahlung, die es Spielern ermöglicht, in Echtzeit Geld auf ihr Spielkonto zu überweisen.
Die Boomerang Casino Einzahlung funktioniert ganz einfach: Spieler können wählen, wie viel Geld sie einzahlen möchten und die gewünschte Zahlungsmethode auswählen. Zur Auswahl stehen unter anderem traditionelle Banküberweisungen, Kreditkarten oder E-Wallets wie Skrill oder Neteller. Sobald die Einzahlung abgeschlossen ist, steht das Geld sofort auf dem Spielkonto zur Verfügung und die Spieler können sofort mit dem Spielen beginnen.
Ein großer Vorteil der Boomerang Casino Einzahlung ist die schnelle Abwicklung. Während traditionelle Banküberweisungen oft mehrere Tage dauern können, ist das eingezahlte Geld bei der Boomerang Casino Einzahlung sofort verfügbar. Dies bedeutet, dass Spieler nicht lange warten müssen, um mit dem Spielen zu beginnen.
Darüber hinaus bietet das Boomerang Casino auch eine Vielzahl von Spielen und Boni für seine Spieler. Von klassischen Tischspielen wie Blackjack und Roulette bis hin zu modernen Spielautomaten und Live-Casino-Spielen, ist für jeden Geschmack etwas dabei. Zusätzlich gibt es regelmäßige Aktionen und Boni, die Spielern zusätzliche Gewinnchancen bieten.
Insgesamt bietet die Boomerang Casino Einzahlung eine bequeme und benutzerfreundliche Möglichkeit, Geld auf sein Spielkonto zu überweisen. Mit schnellen Transaktionen und einer Vielzahl von Spielen und Boni ist das Boomerang Casino eine attraktive Option für Spieler, die nach einem neuen und innovativen Online-Casino suchen.
https://boomerangcasino.one/
Zet Casino 30 Free Spins: Profitieren Sie von diesem groГџzГјgigen Angebot!
Das Zet Casino ist ein beliebter Anbieter von Online-Glücksspielen, der regelmäßig attraktive Bonusaktionen für seine Spieler anbietet. Eine davon ist das Angebot von 30 Freispielen, die Sie nutzen können, um verschiedene Slot-Spiele auszuprobieren und dabei echtes Geld zu gewinnen.
Um von diesem großzügigen Angebot zu profitieren, müssen Sie lediglich ein Konto bei Zet Casino erstellen und eine Einzahlung tätigen. Sobald Ihre Einzahlung bestätigt wurde, werden die 30 Freispiele automatisch Ihrem Konto gutgeschrieben. Sie können die Freispiele dann verwenden, um Ihr Glück an verschiedenen Slot-Spielen zu versuchen und hoffentlich einige große Gewinne zu erzielen.
Es ist wichtig zu beachten, dass die Freispiele bestimmten Bedingungen unterliegen. Zum Beispiel können die Gewinne, die Sie mit den Freispielen erzielen, einem Umsatzbedingung unterliegen, bevor Sie sie auszahlen lassen können. Es ist daher ratsam, die Geschäftsbedingungen des Angebots sorgfältig zu lesen, um sicherzustellen, dass Sie die Freispiele optimal nutzen können.
Insgesamt ist das Angebot von 30 Freispielen im Zet Casino eine großartige Möglichkeit, um das Casino kennenzulernen und einige der spannenden Slot-Spiele auszuprobieren, die es zu bieten hat. Wenn Sie also auf der Suche nach einer neuen Online-Glücksspielplattform sind, sollten Sie dieses Angebot auf jeden Fall in Betracht ziehen. Viel Glück und viel Spaß beim Spielen!
https://zetcasino.one/
Zet Casino: Das beste Spiel
Zet Casino ist eines der beliebtesten Online-Casinos in Deutschland und bietet eine groГџe Auswahl an Spielen fГјr jeden Geschmack. Unter den vielen Spielen, die das Casino zu bieten hat, gibt es jedoch ein Spiel, das besonders beliebt ist – das beste Spiel im Zet Casino.
Das beste Spiel im Zet Casino ist schwer zu definieren, da die Vorlieben der Spieler variieren und was für den einen das beste Spiel ist, mag für den anderen nicht so interessant sein. Doch eines der Spiele, das von vielen Spielern als das beste im Zet Casino angesehen wird, ist Mega Moolah. Dieser beliebte Spielautomat bietet nicht nur eine unterhaltsame und spannende Spielerfahrung, sondern auch die Möglichkeit, lebensverändernde Jackpots zu gewinnen.
Mega Moolah ist ein Spiel, das von Microgaming entwickelt wurde und über ein progressives Jackpot-Netzwerk verfügt, das enorm hohe Gewinne ermöglicht. Der Jackpot in diesem Spiel kann in die Millionen gehen, was es zu einem der lukrativsten Spiele im Zet Casino macht.
Neben Mega Moolah gibt es im Zet Casino natГјrlich viele andere spannende Spiele, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Egal, ob Sie ein erfahrener Spieler sind oder gerade erst anfangen, im Zet Casino finden Sie garantiert das beste Spiel fГјr sich.
Schauen Sie doch einfach mal vorbei und entdecken Sie die Vielfalt der Spiele im Zet Casino. Vielleicht finden Sie ja auch Ihr persönliches bestes Spiel und haben die Chance, fantastische Gewinne zu erzielen. Viel Glück!
https://zetcasino.one/
Tipico ist eine der beliebtesten Online-GlГјcksspielplattformen in Deutschland, die eine Vielzahl von spannenden Casino-Spielen anbietet. In diesem Artikel werden die besten Casino-Spiele auf Tipico vorgestellt, die jeder GlГјcksspielfan ausprobieren sollte.
Eines der beliebtesten Casino-Spiele auf Tipico ist zweifellos Blackjack. Das Kartenspiel erfreut sich großer Beliebtheit aufgrund seiner einfachen Regeln und der Möglichkeit, strategisch zu spielen. Mit verschiedenen Varianten wie Classic Blackjack, Single Deck Blackjack und Multi Hand Blackjack bietet Tipico seinen Spielern eine Vielzahl von Optionen, um ihr Glück zu versuchen.
Ein weiteres Highlight auf Tipico ist Roulette. Das klassische Casinospiel, bei dem die Spieler auf den Ausgang eines sich drehenden Rades wetten, bietet Nervenkitzel und Spannung pur. Mit Varianten wie European Roulette, American Roulette und French Roulette können Spieler auf Tipico ihr Glück auf verschiedene Weise herausfordern.
Auch Spielautomaten dГјrfen auf einer Casino-Plattform wie Tipico nicht fehlen. Mit Hunderten von Slots von namhaften Entwicklern wie NetEnt, Microgaming und Play’n GO bietet Tipico eine breite Auswahl an Automatenspielen fГјr jeden Geschmack. Von klassischen FrГјchteslots bis hin zu modernen Video-Slots mit aufregenden Bonusfunktionen ist fГјr jeden etwas dabei.
Nicht zu vergessen sind die Live-Casino-Spiele auf Tipico. Hier können Spieler an Tischen mit echten Dealern und Croupiers Platz nehmen und in Echtzeit gegen andere Spieler antreten. Mit Spielen wie Live Blackjack, Live Roulette und Live Baccarat wird das Casino-Erlebnis auf Tipico auf ein ganz neues Level gehoben.
Insgesamt bietet Tipico eine beeindruckende Auswahl an Casino-Spielen, die sowohl Anfänger als auch erfahrene Spieler ansprechen. Mit den besten Spielen wie Blackjack, Roulette, Spielautomaten und Live-Casino-Spielen ist für jeden Geschmack und jede Vorliebe etwas dabei. Wer also auf der Suche nach einem erstklassigen Online-Casino-Erlebnis ist, sollte Tipico unbedingt einen Besuch abstatten. Viel Spaß und viel Glück beim Spielen!
https://tipicocasino.one/
Zet Casino: Keine Einzahlung erforderlich
Das Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und groГџzГјgigen Bonusangeboten fГјr seine Spieler bietet. Eine der beliebtesten Aktionen des Zet Casinos ist der sogenannte “No Deposit Bonus”, bei dem Spieler keine Einzahlung leisten mГјssen, um einen Bonus zu erhalten.
Der No Deposit Bonus im Zet Casino ist eine großartige Möglichkeit für Spieler, das Casino und die angebotenen Spiele risikofrei auszuprobieren. Es handelt sich um eine Art Willkommensbonus, bei dem Spieler nach der Registrierung im Casino einen bestimmten Betrag an Bonusgeld erhalten, ohne dass eine Einzahlung erforderlich ist.
Um den No Deposit Bonus im Zet Casino zu erhalten, müssen sich Spieler lediglich registrieren und ein Konto erstellen. Anschließend wird der Bonus automatisch gutgeschrieben und kann sofort zum Spielen verwendet werden. Auch wenn der Bonus kostenlos ist, unterliegt er in der Regel bestimmten Umsatzbedingungen, bevor eine Auszahlung möglich ist.
Der No Deposit Bonus im Zet Casino ist eine großartige Möglichkeit, um das Casino und die angebotenen Spiele kennenzulernen, ohne eigenes Geld riskieren zu müssen. Spieler können mit dem Bonus verschiedene Spiele ausprobieren und sich mit der Funktionsweise des Casinos vertraut machen.
Insgesamt ist der No Deposit Bonus im Zet Casino eine attraktive Option für Spieler, die neue Online-Casinos ausprobieren möchten, ohne gleich eine Einzahlung tätigen zu müssen. Mit diesem Bonus können Spieler risikofrei spielen und erste Gewinne erzielen, ohne dabei eigenes Geld zu verwenden.
https://zetcasino.one/
Zet Casino Sportwetten
Sportwetten erfreuen sich in Deutschland immer größerer Beliebtheit. Neben den traditionellen Wettbüros vor Ort bieten auch Online-Casinos wie das Zet Casino Sportwetten an. Das Zet Casino ist ein beliebtes Online-Casino, das seinen Kunden eine Vielzahl von Spielen und Wetten anbietet.
Das Zet Casino Sportwettenangebot umfasst eine breite Palette von Sportarten, darunter Fußball, Tennis, Basketball, Eishockey und vieles mehr. Die Kunden haben die Möglichkeit, auf einzelne Spiele, Turniere oder ganze Ligen zu wetten. Neben den klassischen Sportwetten bietet das Zet Casino auch Live-Wetten an, bei denen die Kunden während des Spiels ihre Wetten platzieren können.
Das Online-Casino zeichnet sich durch eine benutzerfreundliche Oberfläche aus, die es den Kunden ermöglicht, schnell und einfach ihre Wetten abzugeben. Zudem bietet das Zet Casino eine Vielzahl von Zahlungsmethoden an, darunter Kreditkarten, E-Wallets und Banküberweisungen.
Ein weiterer Vorteil des Zet Casino Sportwettenangebots sind die attraktiven Quoten und Boni, die den Kunden angeboten werden. So können die Kunden von lukrativen Einzahlungsboni, Freiwetten und anderen Aktionen profitieren.
Insgesamt bietet das Zet Casino Sportwetten eine unterhaltsame und spannende Möglichkeit, sich mit Sportereignissen zu beschäftigen und möglicherweise auch den ein oder anderen Gewinn zu erzielen. Wer also auf der Suche nach einem Online-Casino mit einem breiten Sportwettenangebot ist, sollte das Zet Casino in Betracht ziehen.
https://zetcasino.one/
Das m.zet Casino: Ein neuer Hotspot fГјr GlГјcksspielfreunde
Das m.zet Casino ist ein neuer Anbieter auf dem Markt fГјr Online-GlГјcksspiele und hat in den letzten Monaten immer mehr Aufmerksamkeit auf sich gezogen. Mit einer breiten Auswahl an Spielen und einer benutzerfreundlichen Plattform, lockt das m.zet Casino Spieler aus der ganzen Welt an.
Eine der größten Attraktionen des m.zet Casinos sind die zahlreichen Spielautomaten, die für jeden Geschmack und jedes Budget etwas bieten. Von klassischen Früchteslots bis hin zu aufregenden Video-Slots mit tollen Bonusfunktionen, ist für jeden etwas dabei. Darüber hinaus bietet das m.zet Casino auch eine Vielzahl an Tischspielen wie Blackjack, Roulette und Baccarat an.
Neben dem breiten Spielangebot überzeugt das m.zet Casino auch durch seine großzügigen Bonusangebote und Aktionen. Neue Spieler werden mit einem Willkommensbonus belohnt, der ihnen zusätzliches Guthaben oder Freispiele beschert. Zudem gibt es regelmäßige Promotionen und Turniere, bei denen Spieler zusätzliche Preise gewinnen können.
Die Sicherheit der Spieler steht im m.zet Casino an erster Stelle. Die Plattform ist durch hochmoderne Verschlüsselungstechnologien geschützt, um sicherzustellen, dass alle Transaktionen und persönlichen Daten der Spieler sicher sind. Zudem verfügt das m.zet Casino über eine Lizenz von einer renommierten Glücksspielbehörde, die die Einhaltung strenger Auflagen garantiert.
Insgesamt bietet das m.zet Casino ein unterhaltsames und sicheres Spielerlebnis fГјr GlГјcksspielfreunde. Mit seinem umfangreichen Spielangebot, groГџzГјgigen Boni und einer benutzerfreundlichen Plattform ist das m.zet Casino definitiv einen Besuch wert.
https://zetcasino.one/
Tipico Casino Spiele laden nicht – Was tun?
Das Tipico Casino ist eine beliebte Online-Plattform fГјr Casino-Spiele und Sportwetten. Doch manchmal kann es passieren, dass die Spiele im Casino nicht richtig laden. Das kann frustrierend sein, besonders wenn man sich auf einen spannenden Spielabend gefreut hat.
Es gibt jedoch einige Tipps, die helfen können, wenn die Spiele im Tipico Casino nicht laden. Zunächst einmal sollte man überprüfen, ob die Internetverbindung stabil ist. Oftmals liegt das Problem einfach daran, dass die Verbindung nicht ausreichend ist, um die Spiele schnell genug zu laden. In diesem Fall hilft es, den Router neu zu starten oder sich in ein anderes WLAN-Netzwerk einzuloggen.
Ein weiterer möglicher Grund für das Problem könnte ein veralteter Browser sein. Es empfiehlt sich, den Browser regelmäßig zu aktualisieren, um sicherzustellen, dass er kompatibel mit der Casino-Software ist. Auch das Löschen von Cookies und dem Cache kann helfen, um die Ladezeit der Spiele zu verbessern.
Sollten diese Maßnahmen nicht zum gewünschten Erfolg führen, empfiehlt es sich, den Kundenservice von Tipico zu kontaktieren. Die Mitarbeiter des Support-Teams können in der Regel schnell und unkompliziert weiterhelfen und das Problem lösen.
Zusammenfassend lässt sich sagen, dass es verschiedene Gründe geben kann, warum die Spiele im Tipico Casino nicht laden. Mit einigen einfachen Maßnahmen und dem richtigen Vorgehen lässt sich das Problem jedoch meist schnell beheben, sodass einem unterhaltsamen Spielabend nichts im Wege steht.
https://tipicocasino.one/
Das Zet Casino bietet seinen Spielern eine großzügige Promotion von 50 Freispielen, die sie in ausgewählten Spielen nutzen können. Doch welches Spiel eignet sich am besten, um diese Freispiele optimal auszunutzen?
Eines der beliebtesten Spiele, das für die 50 Freispiele im Zet Casino genutzt werden kann, ist der Slot Starburst. Dieses Spiel von NetEnt ist bekannt für seine spannende Spielmechanik und die Möglichkeit hohe Gewinne zu erzielen. Die Freispiele bieten die perfekte Gelegenheit, Starburst ohne Einsatz von eigenem Geld auszuprobieren und dabei eventuell sogar beträchtliche Gewinne zu erzielen.
Ein weiteres empfehlenswertes Spiel fГјr die 50 Freispiele im Zet Casino ist Book of Dead. Dieser beliebte Slot von Play’n GO entfГјhrt die Spieler in eine mystische Welt des alten Г„gyptens, in der sie auf die Suche nach verborgenen SchГ¤tzen gehen kГ¶nnen. Die Freispiele bieten eine groГџartige MГ¶glichkeit, das Spiel besser kennenzulernen und die Chance auf hohe Gewinne zu verbessern.
Wer auf der Suche nach einem klassischen Spiel ist, kann die 50 Freispiele im Zet Casino auch beim Roulette einsetzen. Dieses zeitlose Casinospiel bietet Spannung und Nervenkitzel pur und die Freispiele bieten die Gelegenheit, Roulette ohne Risiko auszuprobieren und möglicherweise hohe Gewinne zu erzielen.
Insgesamt bietet das Zet Casino mit seinen 50 Freispielen eine fantastische Gelegenheit, einige der besten Spiele des Casinos gratis auszuprobieren und dabei die Chance auf hohe Gewinne zu haben. Egal ob man sich für Starburst, Book of Dead oder Roulette entscheidet, die Freispiele sind eine tolle Möglichkeit, das Casino und seine Spiele besser kennenzulernen und vielleicht sogar den Jackpot zu knacken.
https://zetcasino.one/
Zet Casino Bonus Bedingungen
Das Zet Casino ist eine beliebte Online-Spielhalle, die ihren Kunden eine Vielzahl von Spielen und Boni bietet. Einer der größten Anreize für neue Spieler sind die großzügigen Bonusangebote, die das Casino zur Verfügung stellt. Doch bevor man sich über die tollen Boni freuen kann, sollte man sich auch über die Bonusbedingungen informieren.
Die Bonusbedingungen im Zet Casino sind fair und transparent gestaltet, um sicherzustellen, dass Spieler die Regeln verstehen und ihre Gewinne entsprechend auszahlen können. Zunächst ist es wichtig zu wissen, dass es verschiedene Arten von Boni gibt, die im Casino angeboten werden. Dazu gehören Einzahlungsboni, Freispiele und Cashback-Angebote.
Um einen Bonus im Zet Casino zu erhalten, müssen Spieler eine Mindesteinzahlung tätigen. Die genauen Beträge variieren je nach Angebot, aber in der Regel liegt die Mindesteinzahlung bei 20€. Es ist wichtig zu beachten, dass manche Boni spezielle Bonuscodes erfordern, die bei der Einzahlung eingegeben werden müssen.
Darüber hinaus unterliegen die Boni im Zet Casino Umsatzbedingungen. Das bedeutet, dass Spieler den Bonus eine bestimmte Anzahl an Malen umsetzen müssen, bevor sie eine Auszahlung beantragen können. Die Umsatzbedingungen variieren je nach Angebot, aber liegen in der Regel zwischen 30-50 Mal. Es ist wichtig, diese Bedingungen zu erfüllen, um keine Probleme bei der Auszahlung zu haben.
Zusätzlich gibt es auch einige Spiele, die nicht zur Erfüllung der Umsatzbedingungen beitragen. Dazu gehören zum Beispiel Tischspiele wie Blackjack oder Roulette. Es ist ratsam, sich vorab über die Spielbeiträge zu informieren, um sicherzustellen, dass man die Umsatzbedingungen möglichst effizient erfüllen kann.
Insgesamt sind die Bonusbedingungen im Zet Casino fair und gut verständlich. Spieler sollten sich jedoch immer die Zeit nehmen, die Bedingungen genau zu lesen und zu verstehen, bevor sie einen Bonus beanspruchen. So können sie sicherstellen, dass sie ihr Spielerlebnis im Casino optimal nutzen und von den großzügigen Boni profitieren können.
https://zetcasino.one/
Boomerang Casino Mobiles – Das ultimative Spielerlebnis fГјr unterwegs
Wer gerne im Online Casino spielt, weiß wie wichtig es ist, Zugriff auf sein Lieblingsspiel jederzeit und überall zu haben. Genau hier kommen die Boomerang Casino Mobiles ins Spiel. Mit diesen innovativen mobilen Geräten wird das Spielerlebnis auf ein neues Level gehoben.
Die Boomerang Casino Mobiles sind speziell für Spieler entwickelt worden, die auch unterwegs nicht auf ihr Lieblingsspiel verzichten wollen. Dank modernster Technologie und leistungsstarker Software können die Spiele ohne Qualitätsverlust und mit einer flüssigen Performance auf den Boomerang Casino Mobiles genossen werden.
Egal ob Slots, Roulette, Blackjack oder Poker – auf den Boomerang Casino Mobiles findet jeder Spieler sein Lieblingsspiel. Die intuitive BenutzeroberflГ¤che macht es einfach, auch unterwegs die Spiele zu navigieren und zu spielen. Zudem unterstГјtzen die Boomerang Casino Mobiles eine Vielzahl von ZahlungsmГ¶glichkeiten, so dass Ein- und Auszahlungen schnell und sicher getГ¤tigt werden kГ¶nnen.
Ein weiterer Vorteil der Boomerang Casino Mobiles ist die Möglichkeit, auch mit anderen Spielern in Kontakt zu treten. Über Chat-Funktionen können Spieler miteinander kommunizieren, sich über Strategien austauschen oder einfach nur gemeinsam Spaß haben.
Insgesamt bieten die Boomerang Casino Mobiles somit ein perfektes Spielerlebnis für unterwegs. Egal ob man im Zug, im Café oder im Park spielt, mit den Boomerang Casino Mobiles hat man sein Lieblingscasino immer dabei. Probieren Sie es aus und lassen Sie sich von der Qualität und dem Komfort der Boomerang Casino Mobiles überzeugen.
https://boomerangcasino.one/
Descubre la magia de los casinos en linea en Peru?
mejor casino online peru mejor casino online peru .
Boomerang Casino bei AskGamblers: Die perfekte Wahl fГјr Casino-Fans
Boomerang Casino ist ein aufregendes Online-Casino, das von AskGamblers als eine der Top-Optionen fГјr GlГјcksspielfans empfohlen wird. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Boni und einem benutzerfreundlichen Design ist Boomerang Casino die perfekte Wahl fГјr Spieler, die das ultimative Casino-Erlebnis suchen.
Eine der besten Funktionen von Boomerang Casino ist die riesige Auswahl an Spielen. Mit Hunderten von Slot-Spielen, Tischspielen und Live-Dealer-Spielen gibt es hier fГјr jeden Geschmack etwas zu finden. Von klassischen Spielautomaten bis hin zu aufregenden neuen VerГ¶ffentlichungen gibt es hier fГјr jeden etwas zu entdecken. Und mit Spielen von Top-Anbietern wie NetEnt, Microgaming und Play’n GO kГ¶nnen Spieler sicher sein, dass sie nur die besten Spiele genieГџen.
Darüber hinaus bietet Boomerang Casino großzügige Boni und Aktionen für Spieler. Neue Spieler erhalten einen lukrativen Willkommensbonus, der es ihnen ermöglicht, mit zusätzlichem Guthaben zu spielen und ihre Gewinnchancen zu erhöhen. Darüber hinaus gibt es regelmäßig Aktionen und Turniere, bei denen Spieler noch mehr Belohnungen und Preise verdienen können.
Das Design von Boomerang Casino ist einfach zu bedienen und intuitiv, was es selbst für Anfänger leicht macht, sich im Casino zurechtzufinden. Die Website ist übersichtlich gestaltet und bietet eine benutzerfreundliche Navigation, sodass Spieler schnell und einfach zu ihren Lieblingsspielen gelangen können.
Insgesamt ist Boomerang Casino eine hervorragende Option fГјr Casino-Fans, die nach einer erstklassigen Spielerfahrung suchen. Mit einer groГџartigen Auswahl an Spielen, groГџzГјgigen Boni und einem benutzerfreundlichen Design gibt es keinen Grund, warum Spieler sich nicht fГјr Boomerang Casino entscheiden sollten. Probieren Sie es noch heute aus und erleben Sie die Faszination des GlГјcksspiels bei Boomerang Casino.
https://boomerangcasino.one/
Сравнение лучших букмекеров
мобильные букмекерские конторы вход букмекерская .
https://reduslim.at/
get redirected here solana wallet
not worry ever that getting all these pleasant things with girls is dangerous for your health. These hot women are healthy as finally you will not a passionate tigress, but a woman, full of complexes and with no passion. Meeting with Tower Hamlets blonde escorts
seo оптимизатор https://seo-goody.ru/
датчик температуры и влажности – датчики уровня innolevel, блок питания бп30 овен
Gogo Casino är ett online casino som har blivit populärt bland spelare på grund av dess enkla och användarvänliga plattform. En av de främsta anledningarna till detta är att det inte krävs någon registrering för att börja spela, vilket gör det smidigt och snabbt att komma igång.
AskGamblers är en ledande plattform för casinorecensioner och betyg, och Gogo Casino har fått positiva recensioner från många spelare. Många användare har berömt casinot för dess stora utbud av spel och snabba utbetalningar.
En annan anledning till att Gogo Casino har blivit så populärt är dess generösa bonuserbjudanden och kampanjer. Spelare har möjlighet att få olika typer av bonusar, som till exempel välkomstbonusar och gratissnurr.
Även om Gogo Casino främst riktar sig till svenska spelare, är det tillgängligt för spelare från många andra länder runt om i världen. Casinot erbjuder också kundsupport på svenska, vilket gör det enklare för svenska spelare att få hjälp om det skulle behövas.
Sammanfattningsvis verkar Gogo Casino vara ett pålitligt och användarvänligt online casino som erbjuder ett stort utbud av spel och generösa bonusar. Om du letar efter ett nytt casino att prova på, kan det vara värt att ge Gogo Casino en chans.
https://gogocasino.one
поставки оземпик +в россию – дулаглутид инструкция +по применению, семаглутид 0.5 мг цена
kraken market ссылка – адрес сайта кракен, кракен маркетплейс
Кредит с плохой историей – Деньги под расписку, Деньги в долг с любой КИ
Gogo Casino är en populär spelsajt som lockar många spelare med sina attraktiva spel och generösa erbjudanden. Men vad händer när casinot inte betalar ut vinster till sina spelare?
Tyvärr har det kommit rapporter om spelare som har haft problem med att få ut sina pengar från Gogo Casino. När de vinner stora summor och försöker ta ut sina vinster stöter de på problem och får inte pengarna de är berättigade till.
Detta är inte acceptabelt och skapar en stor oro bland spelare som vill känna sig trygga när de spelar på en spelsajt. Att inte kunna förlita sig på att ett casino betalar ut vinster är ett stort förtroendebrott och kan få allvarliga konsekvenser för casinots rykte och framtida verksamhet.
Det är viktigt att spelare är medvetna om risken för att inte få ut sina vinster när de väljer ett casino att spela på. Det är därför viktigt att vara noga med att välja en pålitlig och seriös spelsajt som har en god rykte och gott anseende bland spelare.
Om du har råkat ut för problem med att få ut dina vinster från Gogo Casino eller något annat casino bör du kontakta kundtjänsten och försöka lösa situationen på ett konstruktivt sätt. Om casinot vägrar att betala ut dina vinster kan du också kontakta en oberoende spelmyndighet för att få hjälp med att lösa problemet.
Sammanfattningsvis är det viktigt att vara vaksam och försiktig när man väljer ett casino att spela på för att undvika att hamna i en situation där man inte får ut sina pengar. Spel ska vara roligt och underhållande och inte en källa till stress och oro över att inte få ut sina vinster. Välj alltid en pålitlig och seriös spelsajt för en tryggare spelupplevelse.
https://gogocasino.one
Gogo casino är en populär spelsajt som erbjuder ett stort utbud av casinospel och en spännande spelupplevelse för alla spelare. Sajten har blivit mycket omtyckt av spelare tack vare sin användarvänliga design, generösa bonusar och snabba utbetalningar.
En av de starka sidorna med Gogo casino är det stora urvalet av casinospel som erbjuds. Här hittar man alla de klassiska casinospelen såsom blackjack, roulette och spelautomater, samt ett brett utbud av nya och spännande spel. Sajten samarbetar med flera ledande spelleverantörer vilket gör att spelarna kan njuta av högkvalitativa spel med innovativa funktioner och grafik.
En annan fördel med Gogo casino är de generösa bonusar och kampanjer som erbjuds till spelarna. Nya spelare välkomnas med en attraktiv välkomstbonus och regelbundet erbjuds det olika kampanjer och tävlingar där spelarna kan vinna fina priser och bonusar. Dessutom har sajten ett lojalitetsprogram där spelarna kan samla poäng och få förmåner för att fortsätta spela på sajten.
Gogo casino är också känt för sina snabba utbetalningar och goda kundtjänst. Spelarna kan vara trygga i att deras pengar och personuppgifter hanteras säkert och att de kan få hjälp av en professionell support om de skulle behöva det.
Sammanfattningsvis är Gogo casino en utmärkt spelsajt för alla som letar efter en spännande och pålitlig spelupplevelse. Med sitt stora spelutbud, generösa bonusar och pålitliga kundtjänst har sajten lyckats skapa en bra rykte bland spelare. Om du letar efter ett bra casino att spela på rekommenderar vi definitivt Gogo casino.
https://gogocasino.one
вывоз строительного мусора из квартиры цена
купить больничный
Интернет магазин Блузка Бай https://blyzka.by/begimoda-4083
качественный сервис выполняет ремонт фотоаппаратов pentax в Москве. Сотни раз обращался, все отремонтировали качественно!
discover here toast crypto wallet
like it bitcoin blender
трулисити инструкция аналог – оземпик новости, оземпик купить +в казани
mod menu fortnite – aimbot fortnite, how to get cheats in fortnite
оземпик цена аналоги – семаглутид +в турции, трулисити инструкция 1.5 мг +по применению
להשתנות. חושבים שזה דבר קטן שלא יכול לשנות מצבים בחיים? הנה דוגמא קלאסית למשהו שיכול גם יכול ומעיד על שינויים בחייהם של אנשים שחיים את הסטרס במדינת ישראל נכון להיום. אישה מדהימה, המראה שלה מושלם, צעירה, יפה והיא באה כדי להעניק לכם את החופש אותו אתם סקס אדיר באר שבע
качественный сервис выполняет ремонт принтеров в Москве. Сотни раз обращался, все отремонтировали качественно!
תבלו עם נערת החלומות שלכם, תקבלו עיסוי אירוטי או פשוט תעבירו זמן מענג עם מישהי לוהטת במיוחד. כמה פשוט, ככה מספק ומעורר טעם של עוד! שירותי ליווי – חיים שלמים ועשירים כיום אפשרי לראות כי שוק שירותי הליווי רואה תנופה אדירה. הרי רבים מאי פעם מעוניינים דירות דיסקרטיות בבת ים
המיוחדות שלך. לצד כל מודעה מצורפים כל הפרטים שבחר נותן השירות לספק לך, חלקם כוללים את עלויות השירותים. אף על פי שמחיר השירות מושפע מהפעילות שברצונך לקיים, מומלץ ליצור קשר עם מספר מודעות מקבילות ורלוונטיות כדי לברר מה הוא טווח המחירים הרלוונטי לצרכים שירות ליווי בתל אביב – כל מה שרצית לדעת
качественный сервис выполняет ремонт телефонов в Москве. Сотни раз обращался, все отремонтировали качественно!
https://gogocasino.one
качественный сервис выполняет ремонт промышленных роботов в Москве. Сотни раз обращался, все отремонтировали качественно!
kraken зеркало – кракен сайт зеркало, кракен тор
качественный сервис выполняет ремонт модулей управления беговых дорожек в Москве. Сотни раз обращался, все отремонтировали качественно!
опубликовано здесь
УСТАНОВКА, ПРОДАЖА, НАСТРОЙКА VRF СИСТЕМ в Витебске, Минске, Орше
look at these guys Buy Twitter Followers
качественный сервис выполняет ремонт электроники индукционных плит в Москве. Сотни раз обращался, все отремонтировали качественно!
כגון ג’קוזי או אירוח של מעסה ארוטית, חשפניות או נערות ליווי. הדירות אשר נמצאות במיקומים נוחים להגעה ומפוזרות בכל רחבי הארץ יכולות להפוך למקום מפלט רומנטי, חדר התענוגות הפרטי שלך או מיקום אדיר למסיבת רווקים. בליאור סקס ריכזנו עבורך דירות דיסקרטיות לחגוג עם נערת ליווי פרטית
Друзья, давайте погрузимся в увлекательный планету 1xslots casino, где волнение и состояние сходятся в наиболее изысканном сочетании! Это не просто заведение, это район, где каждый участник может обнаружить собственный маршрут к победе. Увлекательные развлечения, великодушные подарки и тщательная поддержка делают игровой практика на данном ресурсе поистине незабываемым. Присоединяйтесь к нам и почувствуйте трепет преуспевания вместе с 1 х слотc!
1xslot: Волшебство Космос Риска и Богатства 6942dac
ותיירות מרוסיה, אוקראינה ועוד מדינות. כולן בעלות גוף מושלם ומטופח ממש כמו בסרטים. אתם רק צריכים להתמסר להנאה ומובטח לכם בילוי איכותי. דירות דיסקרטיות בכל הארץ כל גבר רוצה לבלות עם בחורות חמות וסקסיות, אבל לא לכל גבר יש מקום. לפעמים אין פרטיות בבית, נערות ליווי ברחובות
Друзья, давайте проведем время в захватывающий мировоззрение ап икс, где страсть и состояние встречаются в самом роскошном сопряжении! Это не просто гэмблинг-дом, это место, где всякий игрок может обнаружить индивидуальный путешествие к успеху. Захватывающие игры, великодушные премии и заботливая поддержка делают игровой опыт на этом портале фактически неизгладимым. Присоединяйтесь к нам и ощутите трепет победы вместе с ап х!
ап икс: Волшебство Космос Азарта и Достатка fb1fb65
המבנה בו ממוקמת הדירה, האזור והמיקום בעיר בו היא ממוקמת, מתקנים מיוחדים ועוד. בין אם מדובר במרכז העיר או במיקום שקט ומרוחק, הפרטיות שלך מובטחת ויתאפשר לך לעבור חווית שחרור מלאה מכבלי השגרה. ניתן לקבל בדירות השונות עיסוי ארוטי מפנק, מופע חשפניות שלעולם דירות דיסקרטיות בפתח תקווה
Друзья, давайте погрузимся в увлекательный мир азино777, где волнение и богатство встречаются в наиболее изысканном комбинации! Это не просто гэмблинг-дом, это локация, где всякий участник может обнаружить индивидуальный путь к преуспеванию. Увлекательные забавы, богатые премии и внимательная поддержка делают игровой практика на этом веб-сайте на самом деле памятным. Присоединяйтесь к нам и почувствуйте волнение успеха вместе с azino 777!
азино777: Волшебство Мир животных Азарта и Богатства fb1fb65
дома на кипре
снять дом на кипре на месяц
Друзья, давайте окунемся в завораживающий мир vavada, где волнение и имущество встречаются в самом роскошном объединении! Это не просто гэмблинг-дом, это район, где каждый соперник может обнаружить личный путь к успеху. Увлекательные развлечения, щедрые премии и внимательная поддержка делают игровой опыт на этом веб-сайте на самом деле незабываемым. Присоединяйтесь к нам и почувствуйте волнение победы вместе с вавада!
vavada зеркало: Чарующий Космос Азарта и Богатства 65d57ad
купить дом на кипре фото
Друзья, давайте проведем время в волнующий окружение pin up, где искушение и имущество встречаются в самом роскошном комбинации! Это не просто игровая площадка, это место, где каждый и каждый соперник может обнаружить свой маршрут к успеху. Захватывающие забавы, великодушные бонусы и заботливая поддержка делают игровой опыт на этом веб-сайте поистине памятным. Присоединяйтесь к нам и прочувствуйте трепет успеха вместе с pin up casino!
пинап казино: Магический Космос Азарта и Богатства 942dacc
why not check here sakpot-delta
לכל סוכנות להציע, את נערות הליווי, המחירים והביקורות השליליות או החיוביות כלפיה. זו תהיה הדרך שלכם להבטיח כי הבחירה הסופית אשר תבצעו בעצם תהיה הרבה יותר מוצלחת, דבר שכל אחד מכם ירצה כמובן לקחת לטובתו. לפיכך כל שנותר יהיה לכם לעשות זה לוודא כי אתם פועלים נערות ליווי לביתך
kraken darknet onion – kraken зеркало, кракен маркет
view publisher site Rufus
Интернет-магазин с широким выбором тумба подвесная под накладную раковину для вашей ванной комнаты.
строительные материалы волгодонск – Counter Strike 2 торрент скачать, GTA IV скачать бесплатно
Воєнторг
7. Аксессуары для стрелков и охотников
куртка хелікон зимова https://voentorgklyp.kiev.ua/odyag/kurtky/kurtky-helikon-tex/ .
написание курсовой работы – методы используемые в написании курсовой работы, написание курсовых работа
Spin to Win Cash Prizes in Kenya
best online casino games to win money real money online casinos .
התחילו לפעול בהתאם וזאת על ידי כך שאתם עושים כל שניתן לשם מציאת מבוקשכם. הרי כך תוך זמן קצר בלבד תוכלו להיות בטוחים כי תמצאו בדיוק את שאתם רוצים. כלומר תוכלו למצוא מענה הולם לחלוטין וזאת ביחס לסוגיה עמה אתם מתמודדים. אז למה אתם מחכים בעצם עם הדבר? קחו דירות דיסקרטיות בנתניה
1. Вибір натяжної стелі: як правильно підібрати?
2. ТОП-5 переваг натяжних стель для вашого інтер’єру
3. Як доглядати за натяжною стелею: корисні поради
4. Натяжні стелі: модний тренд сучасного дизайну
5. Як вибрати кольорову гаму для натяжної стелі?
6. Натяжні стелі від А до Я: основні поняття
7. Комфорт та елегантність: переваги натяжних стель
8. Якість матеріалів для натяжних стель: що обрати?
9. Ефективне освітлення з натяжними стелями: ідеї та поради
10. Натяжні стелі у ванній кімнаті: плюси та мінуси
11. Як відремонтувати натяжну стелю вдома: поетапна інструкція
12. Візуальні ефекти з допомогою натяжних стель: ідеї дизайну
13. Натяжні стелі з фотопринтом: оригінальний дизайн для вашого інтер’єру
14. Готові або індивідуальні: які натяжні стелі обрати?
15. Натяжні стелі у спальні: як створити атмосферу затишку
16. Вигода та функціональність: чому варто встановити натяжну стелю?
17. Натяжні стелі у кухні: практичність та естетика поєднуються
18. Різновиди кріплень для натяжних стель: який обрати?
19. Комплектація натяжних стель: що потрібно знати при виборі
20. Натяжні стелі зі звукоізоляцією: комфорт та тиша у вашому будинку!
ціна натяжної стелі квадратний метр ціна натяжної стелі квадратний метр .
требования к написанию курсовой работы – заказать курсовую работу срочно, курсовая работа заказать украина
GTA 6 скачать бесплатно – читы Arma 3, Counter Strike 2 торрент скачать
vds сервер – купить vds дешево, vps цены
азиатский шоколад оптом – газированные напитки Азиано оптом, польские соки оптом
подробнее Горящие Туры
Best Restaurants in Morocco – Top Places to Visit in Seychelles, Best Restaurants in China
read the article galaxy swapper download
Интернет-ресурс, где можно купить элегантные раковина для кухни из искусственного камня черная от ведущих производителей.
kraken darknet зеркала – кракен даркнет, kraken зеркало официальный
маркетплейс блэкспрут – ссылка на блекспрут, blacksprut не работает сегодня
кракен onion – как зайти на kraken kraken onion site, kraken зеркало
кракен тор ссылка – kraken darknet ссылка тор, kraken tor ссылка
תוכלו להגשים את כל הפנטזיות שלכם ובנוחות הרבה ביותר שרק ניתן להעלות על הדעת. לפיכך יהיה מומלץ לכל אחד מכם לחפש בהקדם אחר דירות אשר תוכלנה לענות על הציפיות שלכם ובדרך המשכנעת ביותר שיש. לבחור בחכמה – דירות דיסקרטיות כאשר מחפשים אחר דירות דיסקרטיות אזי בחורות בקריות
Скачать Winline iOS
find here tron link
informative post high cost-to-income ratio
квадрокоптер мавик купить – дроны камикадзе купить, купить пистолет макаров
Zet Casino Promo Code ohne Einzahlung
Online Casinos erfreuen sich immer größerer Beliebtheit und locken mit verschiedensten Aktionen und Boni. Eine besonders attraktive Möglichkeit, um sich als Neukunde einen Vorteil zu verschaffen, sind Promo Codes ohne Einzahlung. Ein solcher Bonus ermöglicht es, ohne eigenes Geld einzusetzen, das Casino Angebot zu testen und erste Gewinne zu erzielen.
Auch das Zet Casino bietet seinen Kunden die Möglichkeit, von einem solchen Promo Code zu profitieren. Dabei handelt es sich um einen speziellen Code, der bei der Anmeldung oder im persönlichen Kundenbereich eingegeben werden kann, um einen Bonus ohne Einzahlung zu erhalten. Dieser kann beispielsweise aus Freispielen, Bonusguthaben oder anderen Vergünstigungen bestehen.
Um einen Promo Code ohne Einzahlung im Zet Casino zu erhalten, müssen die Spieler in der Regel einige Bedingungen erfüllen. Dazu gehört häufig die Erstellung eines neuen Spielerkontos, das Einlösen des Codes innerhalb eines bestimmten Zeitraums oder das Erfüllen der Umsatzbedingungen für mögliche Gewinne aus dem Bonus.
Es empfiehlt sich, regelmäßig auf der Website des Zet Casinos nach aktuellen Angeboten zu suchen, um keine interessanten Aktionen zu verpassen. Auch Newsletter oder Benachrichtigungen über die Casino App können dabei helfen, stets über neue Promo Codes informiert zu sein.
Insgesamt bieten Promo Codes ohne Einzahlung eine großartige Möglichkeit, um auf unterhaltsame Weise die Welt des Online Glücksspiels zu erkunden und dabei vielleicht sogar erste Gewinne zu erzielen. Es lohnt sich also, die Angebote des Zet Casinos im Auge zu behalten und von den attraktiven Boni zu profitieren.
https://zetcasino.one/
ооо займ онлайн
подробнее здесь https://battlepass.ru
tor blacksprut – blacksprut, blacksprut com зеркало
мега ссылка – mega как зайти, мега тор
my link how to start investing in crypto
Tipico im Casino: Ein gutes Zeichen fГјr Sportwettenfans
Sportwetten sind schon längst kein Nischenthema mehr, sondern erfreuen sich einer immer größeren Beliebtheit. Vor allem in Deutschland boomt der Markt für Sportwetten und entsprechende Anbieter sind in den letzten Jahren wie Pilze aus dem Boden geschossen. Einer dieser Anbieter ist Tipico, der vor allem durch sein Online-Angebot bekannt ist. Doch wussten Sie schon, dass Tipico auch in einigen Casinos vertreten ist?
Das Aufeinandertreffen von Tipico und Casinos mag zunächst ungewöhnlich erscheinen, aber es ergibt durchaus Sinn. Denn Sportwetten und Glücksspiele haben einige Gemeinsamkeiten und es profitieren beide Seiten von einer Kooperation. Besonders für Sportwettenfans bietet die Präsenz von Tipico im Casino viele Vorteile. So können sie ihre Wetten bequem vor Ort platzieren und gleichzeitig das Casino-Flair genießen.
Darüber hinaus bietet Tipico im Casino auch eine Vielzahl von zusätzlichen Services an. So können Kunden beispielsweise auch auf Live-Sportevents wetten oder von attraktiven Bonusaktionen profitieren. Für viele Sportwettenfans ist das ein echtes Highlight und eine willkommene Abwechslung zum reinen Online-Angebot.
Auch im Hinblick auf den Spielerschutz ist die Kooperation von Tipico und Casinos von Vorteil. Denn durch die gemeinsame Präsenz können sich Spieler besser über ihre Limits bewusst werden und gegebenenfalls auch Hilfe bei Problemen in Anspruch nehmen. Die Verbindung von Sportwetten und Glücksspielen schafft somit auch eine Win-win-Situation für alle Beteiligten.
Insgesamt bietet die Präsenz von Tipico im Casino eine spannende Möglichkeit für Sportwettenfans, ihre Leidenschaft für Sport und Wetten mit dem aufregenden Ambiente eines Casinos zu kombinieren. Durch die vielfältigen Services und Angebote wird das Spielerlebnis noch besser und abwechslungsreicher. Wenn Sie also ein Sportwettenfan sind und sich bisher noch nicht ins Casino getraut haben, sollten Sie Tipico definitiv eine Chance geben. Wer weiß, vielleicht entdecken Sie ja eine neue Leidenschaft für sich.
https://tipicocasino.one/
лечение от алкоголизма алматы нарколог https://someblog.ru/
Tipico Casino Chips auszahlen lassen
Im Tipico Casino können Spieler nicht nur ihr Glück an den zahlreichen Spielautomaten und Tischspielen versuchen, sondern auch ihre Gewinne in Form von Casino Chips auszahlen lassen. Dabei gibt es einige wichtige Punkte zu beachten, um reibungslos zu einer Auszahlung zu gelangen.
Zunächst ist es wichtig zu erwähnen, dass die Auszahlung von Casino Chips im Tipico Casino sehr einfach und unkompliziert ist. Spieler können ihre Chips entweder direkt am Automaten oder an der Kasse gegen Bargeld eintauschen. Es ist jedoch zu beachten, dass es möglicherweise eine Mindestauszahlungsgrenze gibt, die erreicht werden muss, um eine Auszahlung vornehmen zu können.
Darüber hinaus ist es ratsam, sich vorab über die verschiedenen Auszahlungsmethoden im Tipico Casino zu informieren. Je nach Vorliebe können Spieler ihre Gewinne entweder per Banküberweisung, Kreditkarte oder auch über verschiedene Online-Zahlungsdienste wie PayPal auszahlen lassen. Es ist wichtig zu beachten, dass möglicherweise Gebühren für die Auszahlung anfallen können, abhängig von der gewählten Zahlungsmethode.
Um eine Auszahlung von Casino Chips im Tipico Casino vorzunehmen, müssen Spieler in der Regel ihre Identität nachweisen. Dies dient der Sicherheit und Verifizierung des Spielers und wird benötigt, um sicherzustellen, dass die Auszahlung an die richtige Person erfolgt. Spieler sollten daher darauf vorbereitet sein, eine Kopie ihres Personalausweises oder eines anderen Identitätsnachweises vorlegen zu müssen.
Insgesamt ist die Auszahlung von Casino Chips im Tipico Casino eine einfache und unkomplizierte Angelegenheit. Indem Spieler die oben genannten Punkte beachten und sich im Vorfeld über die verschiedenen Auszahlungsmethoden informieren, können sie ihre Gewinne schnell und sicher in Bargeld umwandeln. So steht dem nächsten Casinobesuch mit frischem Bargeld nichts im Wege.
https://tipicocasino.one/
Сайт, где я нашел раковина глубокая для кухни для ванной комнаты.
Сайт, где мне посоветовали раковина компактная для ванной комнаты.
Das Tipico Casino bietet regelmäßig spannende Promotionen für seine Spieler an, um das Spielerlebnis noch aufregender zu gestalten. Diese Aktionen können von Freispielen über Einzahlungsboni bis hin zu Turnieren reichen, bei denen Spieler attraktive Preise gewinnen können.
Eine der beliebtesten Promotionen im Tipico Casino ist der Willkommensbonus für neue Spieler. Dieser ermöglicht es neuen Nutzern, ihre erste Einzahlung zu verdoppeln und somit mehr Geld zum Spielen zur Verfügung zu haben. Darüber hinaus werden regelmäßig Freispiele für ausgewählte Spielautomaten angeboten, um Spielern die Möglichkeit zu geben, neue Spiele auszuprobieren und dabei auch noch etwas zu gewinnen.
Zusätzlich zu diesen Angeboten veranstaltet das Tipico Casino auch regelmäßig Turniere, bei denen Spieler gegeneinander antreten können, um attraktive Preise zu gewinnen. Diese Turniere finden in verschiedenen Spielen statt und bieten Spielern die Möglichkeit, ihr Können unter Beweis zu stellen und gleichzeitig die Chance auf tolle Gewinne zu haben.
Um über die neuesten Promotionen im Tipico Casino informiert zu bleiben, sollten Spieler regelmäßig die Website besuchen oder den Newsletter abonnieren. Dort werden alle aktuellen Aktionen und Angebote angekündigt, sodass Spieler keine Chance verpassen, von den spannenden Promotionen zu profitieren.
Insgesamt bietet das Tipico Casino seinen Spielern mit seinen abwechslungsreichen Promotionen eine attraktive Möglichkeit, ihr Spielerlebnis zu verbessern und gleichzeitig die Chance auf tolle Gewinne zu haben. Wer also auf der Suche nach zusätzlichen Anreizen zum Spielen ist, sollte die aktuellen Promotionen im Tipico Casino nicht verpassen.
https://tipicocasino.one/
кодировка от алкоголя алматы https://krasnodar-narkolog.ru/
Das tipico Mobile Casino bietet Spielern die Möglichkeit, ihre Lieblingsspiele unterwegs zu spielen. Egal, ob Sie ein Fan von Spielautomaten, Roulette oder Blackjack sind, das tipico Mobile Casino hat für jeden Geschmack etwas zu bieten.
Die mobile App von tipico ist einfach zu bedienen und bietet eine breite Auswahl an Spielen, die speziell für mobile Geräte optimiert wurden. Die Grafiken sind gestochen scharf und die Soundeffekte bringen das Casino-Erlebnis direkt auf Ihr Smartphone oder Tablet.
Ein weiterer großer Vorteil des tipico Mobile Casinos ist die hohe Sicherheit, die es bietet. Ihre persönlichen Daten und finanziellen Transaktionen sind durch modernste Verschlüsselungstechnologien geschützt, sodass Sie sich ganz auf das Spiel konzentrieren können, ohne sich Sorgen machen zu müssen.
Darüber hinaus bietet das tipico Mobile Casino auch attraktive Bonusangebote und Aktionen, die es Spielern ermöglichen, ihr Spielerlebnis noch aufregender zu gestalten. Mit regelmäßigen Promotionen und Turnieren haben Sie die Möglichkeit, zusätzliche Preise zu gewinnen und Ihr Spielerkonto aufzubessern.
Insgesamt ist das tipico Mobile Casino eine erstklassige Wahl für alle, die auch unterwegs nicht auf ihr Casino-Erlebnis verzichten möchten. Mit einer großen Auswahl an Spielen, hoher Sicherheit und attraktiven Bonusangeboten bietet tipico alles, was das Spielerherz begehrt.
https://tipicocasino.one/
My spouse and I absolutely love your blog and find the majority of your post’s to be just what I’m looking for. can you offer guest writers to write content for you? I wouldn’t mind producing a post or elaborating on most of the subjects you write concerning here. Again, awesome website!
Добрый день всем!
http://www.diploman-russia.com
Обучение игре в казино
олимп казино
Die klassischen Casino-Chips von Tipico sind eine beliebte Wahl für Glücksspiel-Enthusiasten weltweit. Seit ihrer Einführung haben sie sich als zuverlässige und hochwertige Spielmarken etabliert, die in vielen renommierten Casinos verwendet werden.
Die Casino-Chips von Tipico kommen in verschiedenen Farben und Werten, so dass Spieler die Möglichkeit haben, ihre Einsätze entsprechend ihren Vorlieben zu platzieren. Die Chips werden aus hochwertigem Kunststoff oder Keramik hergestellt, was ihnen eine angenehme Haptik und Langlebigkeit verleiht.
Ein weiterer Vorteil der Tipico Casino-Chips ist ihre klare und gut lesbare Beschriftung, die Verwechslungen oder Missverständnisse beim Spielen verhindert. Dies trägt dazu bei, dass die Spiele reibungslos und professionell ablaufen.
Darüber hinaus werden die Casino-Chips von Tipico regelmäßig überprüft und gewartet, um sicherzustellen, dass sie den höchsten Standards in Bezug auf Fairness und Integrität entsprechen. Dies gibt den Spielern zusätzliches Vertrauen in die Ehrlichkeit und Zuverlässigkeit des Casinos.
Insgesamt bieten die klassischen Casino-Chips von Tipico eine erstklassige Spielerfahrung und tragen zu einem unvergesslichen Casinoabend bei. Ihre hochwertige Verarbeitung, klare Beschriftung und Zuverlässigkeit machen sie zu einer perfekten Wahl für jeden, der gerne spielt.
https://tipicocasino.one/
try these out mixer money
кракен рабочий сайт – кракен актуальная, kraken
Das Boomerang Casino ist ein Online-Casino, das seinen Spielern eine Vielzahl von Unterhaltungsmöglichkeiten bietet. Von klassischen Tischspielen wie Blackjack und Roulette bis hin zu aufregenden Spielautomaten und Live-Casino-Spielen – hier kommt jeder auf seine Kosten.
Das Casino zeichnet sich durch seine benutzerfreundliche Oberfläche aus, die es einfach macht, zwischen den verschiedenen Spielen zu navigieren. Darüber hinaus bietet das Boomerang Casino seinen Spielern eine sichere und faire Spielumgebung, die durch SSL-Verschlüsselungstechnologie geschützt ist.
Ein besonderes Highlight des Boomerang Casinos sind die regelmäßigen Bonusangebote und Aktionen, die den Spielern zusätzliche Gewinnchancen bieten. Von Willkommensboni über Freispiele bis hin zu Cashback-Angeboten – hier gibt es immer etwas zu gewinnen.
Des Weiteren bietet das Boomerang Casino einen professionellen Kundenservice, der seinen Spielern bei Fragen und Problemen rund um die Uhr zur Verfügung steht. Ob per Live-Chat, E-Mail oder Telefon – die Mitarbeiter des Casinos sind stets bemüht, den Spielern weiterzuhelfen.
Alles in allem ist das Boomerang Casino eine empfehlenswerte Adresse fГјr alle, die auf der Suche nach einem unterhaltsamen und sicheren Online-Casino-Erlebnis sind. Mit seinem breiten Spielangebot, groГџzГјgigen Bonusangeboten und professionellem Kundenservice Гјberzeugt das Casino auf ganzer Linie.
https://boomerangcasino.one/
browse around this website toast wallet review
click to find out more Buy YouTube Views
лираглутид таблетки купить – мунжаро +для похудения, оземпик 3мл купить
онлайн казино Беларусь лучшие онлайн казино в Беларуси .
Кодирование от алкоголизма по методу Довженко https://alcoholismcoding.kz/
Boomerang Casino – die App, die es in sich hat
In der Welt der Online-Casinos gibt es eine Vielzahl von Anbietern, die alle mit verschiedenen Angeboten und Features locken. Eine dieser Anbieter ist das Boomerang Casino, das mit seiner innovativen App fГјr Furore sorgt.
Die Boomerang Casino App bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und sogar Live-Casino-Spiele. Dank der benutzerfreundlichen Oberfläche ist es sehr einfach, sich in der App zurechtzufinden und seine Lieblingsspiele zu spielen. Zudem punktet die App mit schnellen Ladezeiten und einer stabilen Performance, sodass ein reibungsloses Spielerlebnis garantiert ist.
Ein weiterer großer Pluspunkt der Boomerang Casino App sind die großzügigen Bonusangebote und Aktionen, die regelmäßig verfügbar sind. So können Spieler von zusätzlichen Freispielen, Einzahlungsboni und Cashback-Angeboten profitieren und ihre Gewinnchancen erhöhen.
Ein besonderes Highlight der Boomerang Casino App ist das Loyalty-Programm, das treue Spieler mit exklusiven Belohnungen und Vergünstigungen belohnt. Je mehr man spielt, desto mehr Punkte sammelt man und desto größer werden die Belohnungen.
Insgesamt Гјberzeugt die Boomerang Casino App durch ihr umfangreiches Spielangebot, attraktive Bonusangebote und ein ansprechendes Design. Wer also auf der Suche nach einem unterhaltsamen und lohnenswerten Online-Casino-Erlebnis ist, sollte die Boomerang Casino App definitiv ausprobieren. Viel SpaГџ und GlГјck beim Spielen!
https://boomerangcasino.one/
Оземпик красный купить с доставкой – оземпик купить +в новосибирске, дулаглутид торговое
https://vivod-iz-zapoya-dom.ru/
мунджаро купить +в воронеже – семаглутид +в москве, купить уколы оземпик
Оземпик 3мл – оземпик купить цена +в аптеках, дулаглутид инструкция отзывы
оземпик инструкция отзывы аналоги – манджаро тирзепатид купить +в москве, семаглутид инструкция +по применению цена отзывы
Ein Tipico Live Casino bietet eine Vielzahl von Spielen an, die von echten Dealern geleitet werden und in Echtzeit stattfinden. Spieler können hier das authentische Casino-Erlebnis von zu Hause aus genießen und gleichzeitig mit anderen Teilnehmern interagieren. Ein weiterer großer Vorteil eines Live Casinos ist die Möglichkeit, Gewinne sofort auszahlen zu lassen.
Um Gewinne im Tipico Live Casino auszahlen zu können, müssen Spieler zunächst sicherstellen, dass sie über ein aktives Spielerkonto verfügen und ihre Identität bereits überprüft wurde. Dann können sie einfach auf den Auszahlungsbutton klicken und die gewünschte Auszahlungsmethode auswählen. Tipico bietet eine Vielzahl von Zahlungsoptionen an, darunter Banküberweisung, Kreditkarte, e-Wallets wie PayPal oder Skrill und viele mehr.
Die Zeit, die benötigt wird, um die Auszahlung zu bearbeiten, hängt von der gewählten Zahlungsmethode ab. In der Regel dauert eine Auszahlung per e-Wallet nur wenige Stunden, während Banküberweisungen und Kreditkartenauszahlungen ein paar Werktage in Anspruch nehmen können. Es ist wichtig zu beachten, dass Tipico möglicherweise zusätzliche Dokumente anfordert, um die Auszahlung zu bestätigen und die Einhaltung der Sicherheitsstandards zu gewährleisten.
Es ist ratsam, sich vor der ersten Auszahlung mit den Auszahlungsbedingungen von Tipico vertraut zu machen, um möglichen Verzögerungen oder Problemen vorzubeugen. Spieler können sich auch an den Kundensupport von Tipico wenden, wenn sie Fragen zu ihren Auszahlungen haben oder Hilfe benötigen.
Insgesamt bietet das Tipico Live Casino eine sichere und zuverlässige Plattform für Spieler, die ihre Gewinne schnell und unkompliziert auszahlen lassen möchten. Durch die vielfältigen Zahlungsmöglichkeiten und den hilfsbereiten Kundensupport können Spieler ein reibungsloses Auszahlungserlebnis genießen und sich voll und ganz auf ihr Spiel konzentrieren.
https://tipicocasino.one/
трулисити 1.5 инструкция – Оземпик 1 мг 3мл аптеки в наличии, иглы +для саксенды
кредиты под открытие бизнеса
Boomerang Casino ist eine beliebte Online-GlГјcksspielseite, die eine Vielzahl von Spielen und Boni fГјr Spieler aus der ganzen Welt anbietet. In diesem Artikel werden wir die Meinungen und Erfahrungen von Spielern Гјber das Boomerang Casino analysieren.
Viele Spieler schätzen die Vielfalt an Spielen, die Boomerang Casino anbietet. Von klassischen Spielautomaten über Tischspiele bis hin zu Live-Casino-Spielen gibt es hier für jeden etwas zu entdecken. Die hochwertige Grafik und die reibungslose Gameplay-Performance machen das Spielerlebnis noch angenehmer.
Ein weiterer Pluspunkt ist das großzügige Bonusangebot des Casinos. Neue Spieler werden mit einem Willkommensbonus belohnt, der Freispiele und Bonusgelder umfasst. Darüber hinaus gibt es regelmäßige Promotionen und Aktionen, die es den Spielern ermöglichen, zusätzliche Belohnungen und Preise zu gewinnen.
Die Auszahlungen von Boomerang Casino werden von den Spielern auch positiv bewertet. Die schnellen und zuverlässigen Zahlungsmethoden sorgen dafür, dass die Spieler ihre Gewinne einfach und bequem abheben können. Darüber hinaus bietet das Casino einen kompetenten Kundensupport, der bei Fragen oder Problemen zur Verfügung steht.
Insgesamt sind die Meinungen über Boomerang Casino größtenteils positiv. Die Spieler schätzen die Vielfalt an Spielen, die großzügigen Boni und die zuverlässigen Zahlungsmethoden. Wenn Sie nach einem unterhaltsamen und vertrauenswürdigen Online-Casino suchen, ist Boomerang Casino definitiv einen Besuch wert.
https://boomerangcasino.one/
Die Tipico Casino App fГјr Android ist die perfekte MГ¶glichkeit, um auch unterwegs in den Genuss von spannenden Casino-Spielen zu kommen. Egal ob Slots, Roulette, Blackjack oder Poker – mit der App von Tipico haben Sie Ihr Lieblingsspiel immer dabei.
Die App überzeugt nicht nur durch ein breites Angebot an Spielen, sondern auch durch eine benutzerfreundliche Oberfläche und eine einfache Bedienung. So können Sie auch als Anfänger schnell in die Welt des Online-Glücksspiels eintauchen und sich aufregende Stunden voller Spannung und Unterhaltung sichern.
Ein weiterer Vorteil der Tipico Casino App ist die Möglichkeit, auch unterwegs von attraktiven Boni und Aktionen zu profitieren. So verpassen Sie keine Gelegenheit mehr, zusätzliche Gewinne abzustauben und Ihr Spielerlebnis noch aufregender zu gestalten.
Natürlich brauchen Sie sich auch in Sachen Sicherheit keine Sorgen zu machen, denn Tipico ist ein seriöser und zuverlässiger Anbieter, der höchsten Wert auf den Schutz Ihrer Daten legt.
Also worauf warten Sie noch? Laden Sie sich noch heute die Tipico Casino App fГјr Android herunter und erleben Sie die faszinierende Welt des Online-Casinos direkt auf Ihrem Smartphone oder Tablet. Viel SpaГџ und viel GlГјck!
https://tipicocasino.one/
Приветствую, ценители захватывающих приключений! Планирую рассказать своим восхищением от сетевого заведения “Селектор онлайн казино”. Это не всего лишь площадка для игр, это целый космос эмоций и занимательностей! Здесь я выявил все, что мне потребовалось: различие игр, благородные бонусы и безотлагательные выплаты. Но самое – это атмосфера, которая правит здесь. Имитированные приключения, восхитительные турниры и милосердное сообщество игроков делают каждую игру беззабвенной! Присоедините к “Селектор играть” и погрузитесь в мир интригующих развлечений!
Das Boomerang Casino hat einen weiteren Schritt in Richtung moderner Technologie gemacht, indem es jetzt auch eine mobile Version seiner Webseite anbietet. Mit dieser Boomerang Casino Mobiili-Plattform können Spieler ihre Lieblingsspiele von überall aus genießen, ganz einfach über ihr Smartphone oder Tablet.
Die mobile Version des Boomerang Casinos bietet eine benutzerfreundliche Oberfläche und eine schnelle Ladezeit, was es den Spielern ermöglicht, auch unterwegs ein nahtloses Spielerlebnis zu genießen. Die Plattform umfasst eine große Auswahl an Casino-Spielen, darunter Slots, Tischspiele und Live-Dealer-Spiele, die alle für das mobile Spielen optimiert sind.
Darüber hinaus bietet das Boomerang Casino mobile Version auch eine Reihe von Funktionen und Optionen, die es den Spielern erleichtern, ihre Lieblingsspiele zu finden und zu spielen. Dazu gehören Such- und Filterfunktionen, Boni und Aktionen, Ein- und Auszahlungsmethoden sowie ein freundlicher und professioneller Kundenservice.
Mit dem Boomerang Casino Mobiili können Spieler jetzt noch bequemer und flexibler spielen, egal ob sie gerade unterwegs sind oder einfach nur zu Hause auf dem Sofa entspannen möchten. Die mobile Plattform bietet ein erstklassiges Spielerlebnis und macht das Boomerang Casino zu einer noch attraktiveren Option für Casino-Enthusiasten.
Insgesamt ist das Boomerang Casino Mobiili eine willkommene Ergänzung zum Angebot des Casinos und eine großartige Möglichkeit für Spieler, ihre Lieblingsspiele jederzeit und überall zu genießen. Egal, ob man ein erfahrener Spieler oder ein Neuling ist, das Boomerang Casino Mobiili bietet eine unterhaltsame und spannende Spieleerfahrung für alle.
https://boomerangcasino.one/
лечение от скорости в алматы http://adtherapy.ru/
Tipico Casino Verarschen: Was steckt hinter den GerГјchten?
Das Tipico Casino ist einer der bekanntesten Online-Glücksspielanbieter in Deutschland. Mit einer Vielzahl von Spielen und attraktiven Bonusangeboten lockt das Casino täglich tausende Spieler an. Doch immer wieder tauchen Gerüchte auf, dass das Tipico Casino seine Kunden verarschen würde. Doch was steckt wirklich dahinter?
Zunächst einmal ist es wichtig zu betonen, dass das Tipico Casino über eine offizielle Lizenz verfügt und somit reguliert wird. Dies bedeutet, dass das Casino bestimmten Standards und Regeln folgen muss, um fair und sicher zu spielen. Zudem werden regelmäßig audits und Kontrollen durch unabhängige Behörden durchgeführt, um die Integrität des Casinos zu gewährleisten.
Ein weiterer Punkt, der oft kritisiert wird, ist die Auszahlungsquote des Tipico Casinos. Viele Spieler behaupten, dass die Gewinnchancen niedriger seien als in anderen Online-Casinos. Doch auch hier ist es wichtig zu wissen, dass die Auszahlungsquote von vielen Faktoren abhängt und nicht vom Casino selbst manipuliert werden kann. Zudem entspricht die Auszahlungsquote des Tipico Casinos den branchenüblichen Standards.
Natürlich kann es auch vorkommen, dass Spieler das Gefühl haben, vom Tipico Casino verarscht zu werden, wenn sie eine Pechsträhne haben und mehrere Spiele hintereinander verlieren. Doch auch dies gehört zum Glücksspiel dazu und ist kein Beweis für eine Manipulation durch das Casino.
Insgesamt lässt sich sagen, dass das Tipico Casino nicht grundlos eines der beliebtesten Online-Casinos in Deutschland ist. Wer sich an die Regeln hält, verantwortungsbewusst spielt und realistische Erwartungen hat, kann hier durchaus Spaß haben und erfolgreich sein. Bei konkreten Beschwerden oder Problemen steht zudem der Kundenservice des Casinos zur Verfügung, um Lösungen zu finden.
Fazit: Das Tipico Casino verarschen ist kein Thema, über das man sich ernsthaft Sorgen machen muss. Wer seinem Glück eine Chance geben möchte, kann hier bedenkenlos spielen und sich auf ein unterhaltsames Spielerlebnis freuen.
https://tipicocasino.one/
нарколог лечение алкоголизма https://okcentr.kz/
Boomerang Casino Login
Das Boomerang Casino ist eine beliebte Online-Glücksspielseite, die eine Vielzahl von Spielen für Spieler weltweit anbietet. Um auf die Plattform zuzugreifen und zu spielen, müssen die Nutzer sich zuerst mit ihren persönlichen Kontoinformationen einloggen. In diesem Artikel werden wir uns genauer mit dem Login-Prozess im Boomerang Casino befassen.
Um sich im Boomerang Casino einzuloggen, müssen die Spieler zunächst die offizielle Website des Casinos besuchen. Dort finden sie den Login-Bereich, in den sie ihre E-Mail-Adresse und ihr Passwort eingeben müssen. Nachdem die Zugangsdaten verifiziert wurden, gelangen die Spieler auf ihre persönliche Spielerseite, auf der sie ihre Lieblingsspiele spielen können.
Es ist wichtig, dass die Spieler ihre Login-Daten sicher aufbewahren und sie nicht mit anderen teilen, um die Sicherheit ihres Kontos zu gewährleisten. Das Boomerang Casino bietet auch zusätzliche Sicherheitsmaßnahmen wie die Zwei-Faktor-Authentifizierung, um die Privatsphäre der Spieler zu schützen.
Nach dem erfolgreichen Login können die Spieler aus einer Vielzahl von Spielen wählen, darunter Slots, Tischspiele, Live-Dealer-Spiele und vieles mehr. Das Boomerang Casino bietet auch regelmäßige Bonusangebote und Aktionen, die den Spielern zusätzliche Chancen auf Gewinne bieten.
Insgesamt ist der Login-Prozess im Boomerang Casino einfach und sicher. Mit einer breiten Auswahl an Spielen und attraktiven Bonusangeboten ist das Casino eine gute Wahl fГјr Spieler, die nach einer unterhaltsamen und lohnenden GlГјcksspielerfahrung suchen. Besuchen Sie das Boomerang Casino noch heute und erleben Sie die Spannung des Online-GlГјcksspiels!
https://boomerangcasino.one/
Mobile Casino Tipico: Spielen Sie Ihre Lieblingsspiele Гјberall und jederzeit
In der heutigen digitalen Welt ist es wichtiger denn je, dass Online-Casinos ihre Dienste auch auf mobilen Geräten anbieten. Der Siegeszug von Smartphones und Tablets hat dazu geführt, dass immer mehr Menschen unterwegs spielen möchten. Tipico, einer der führenden Anbieter für Sportwetten und Online-Casino-Spiele, hat diesen Trend erkannt und bietet eine erstklassige mobile Casino-Plattform an.
Mit dem mobile Casino von Tipico kГ¶nnen Sie Ihre Lieblingsspiele wie Slots, Roulette und Blackjack bequem auf Ihrem Smartphone oder Tablet spielen. Die benutzerfreundliche OberflГ¤che und das Гјbersichtliche Design sorgen dafГјr, dass Sie auch unterwegs ein erstklassiges Spielerlebnis genieГџen kГ¶nnen. Egal, ob Sie in der U-Bahn sitzen, auf dem Weg zur Arbeit sind oder einfach nur auf der Couch entspannen – mit dem mobile Casino von Tipico haben Sie Ihre Lieblingsspiele immer in der Tasche.
Ein weiterer Vorteil des mobile Casino von Tipico ist die groГџe Auswahl an Spielen. Egal, ob Sie ein Fan von klassischen Tischspielen wie Poker und Baccarat sind oder lieber an modernen Slots mit hohen Jackpots spielen – bei Tipico finden Sie garantiert das passende Spiel fГјr sich. DarГјber hinaus bietet Tipico regelmäßig spannende Aktionen und Bonusangebote an, die Ihnen zusГ¤tzliche Gewinnchancen und SpaГџ beim Spielen bieten.
Wenn Sie also gerne Casino-Spiele spielen und dabei flexibel sein mГ¶chten, sollten Sie das mobile Casino von Tipico ausprobieren. Mit einer groГџen Auswahl an Spielen, einer benutzerfreundlichen OberflГ¤che und attraktiven Bonusangeboten ist Tipico die ideale Wahl fГјr mobiles Casino-Spielen. Also zГ¶gern Sie nicht und laden Sie die Tipico Casino-App noch heute herunter – Ihre Lieblingsspiele warten bereits auf Sie!
https://tipicocasino.one/
Der Boomerang Casino-Guru ist ein Phänomen, das in der Welt des Glücksspiels immer populärer wird. Diese einzigartige Figur vereint die Magie des Boomerangs mit dem Wissen eines Casino-Experten und verspricht Spielern ein unvergleichliches Spielerlebnis.
Der Boomerang Casino-Guru reist von Casino zu Casino und nutzt seinen magischen Boomerang, um das Glück auf seine Seite zu ziehen. Mit einer unglaublichen Treffsicherheit wirft er den Boomerang und lässt ihn durch die Luft sausen, um die Glücksgöttin Fortuna anzulocken.
Doch der Boomerang Casino-Guru ist nicht nur für seine Fähigkeiten mit dem Boomerang bekannt. Er verfügt auch über ein umfangreiches Wissen über die verschiedenen Casinospiele und gibt den Spielern wertvolle Tipps und Tricks, um ihre Gewinnchancen zu maximieren.
Dank seines Charismas und seiner Expertise hat sich der Boomerang Casino-Guru einen Namen in der Glücksspielwelt gemacht und ist bei den Spielern sehr beliebt. Viele halten ihn für einen Glücksbringer und suchen seine Nähe, um auch von seinem Glück berührt zu werden.
Als einzigartige und faszinierende Persönlichkeit bereichert der Boomerang Casino-Guru die Casinowelt und sorgt für Spannung und Unterhaltung an den Spieltischen. Wer weiß, vielleicht kann auch Ihnen der magische Boomerang des Casino-Gurus das Glück bringen.
https://boomerangcasino.one/
Сайт, где представлен много раковина santek анимо для вашей ванной комнаты, с доставкой по всей стране.
Boomerang.bet Casino Review
Boomerang.bet is an online casino that has been making waves in the world of online gambling. With a wide range of games, generous bonuses, and a user-friendly interface, Boomerang.bet has quickly become a popular choice for many players.
One of the standout features of Boomerang.bet is its game selection. The casino offers a wide variety of games, including slots, table games, and live dealer games. Whether you’re a fan of classic slots or prefer the thrill of live roulette, Boomerang.bet has something for everyone.
In addition to its impressive game selection, Boomerang.bet also offers generous bonuses and promotions. New players can take advantage of a welcome bonus, while existing players can enjoy regular promotions and loyalty rewards. With so many ways to boost your bankroll, playing at Boomerang.bet can be a lucrative experience.
Another highlight of Boomerang.bet is its user-friendly interface. The casino is easy to navigate, making it simple for even beginners to find their favorite games. Plus, with reliable customer support available 24/7, players can rest assured that help is always just a click away.
Overall, Boomerang.bet is a top-notch online casino that offers a fantastic gaming experience. With its wide range of games, generous bonuses, and user-friendly interface, Boomerang.bet is definitely worth checking out for any online gambling enthusiast. Give it a try today and see for yourself why so many players are choosing Boomerang.bet for their online gaming needs.
https://boomerangcasino.one/
In der Welt der Online Casinos gibt es eine Vielzahl von Möglichkeiten, um Spieler anzulocken und zu belohnen. Eine beliebte Methode, um neue Kunden zu gewinnen und bestehende Spieler zu binden, sind Promo-Codes. Diese speziellen Codes ermöglichen es den Spielern, verschiedene Boni und Vergünstigungen zu erhalten, wenn sie sie bei der Registrierung oder Einzahlung verwenden.
Ein Casino, das dieses Jahr mit einem besonders lukrativen Promo-Code aufwartet, ist das Zet Casino. Der Zet Casino Promo-Code 2020 verspricht groГџzГјgige Boni und spannende Aktionen, die sowohl Neulinge als auch erfahrene Spieler begeistern werden.
Wenn Sie sich entscheiden, den Zet Casino Promo-Code 2020 zu nutzen, können Sie von verschiedenen Boni profitieren. Dazu gehören beispielsweise Einzahlungsboni, Freispiele, Cashback-Angebote und vieles mehr. Diese Boni können Ihnen helfen, Ihr Spielkapital zu erhöhen und Ihre Gewinnchancen zu maximieren.
Um den Zet Casino Promo-Code 2020 zu nutzen, müssen Sie lediglich während der Registrierung oder Einzahlung den entsprechenden Code eingeben. Sobald Sie dies getan haben, werden die Boni automatisch Ihrem Konto gutgeschrieben und Sie können sofort mit dem Spielen beginnen.
Es ist jedoch wichtig zu beachten, dass jeder Promo-Code seine eigenen Bedingungen und Konditionen hat. Bevor Sie also einen Promo-Code verwenden, sollten Sie sich unbedingt über diese informieren, um sicherzustellen, dass Sie die Boni optimal nutzen können.
Insgesamt bietet der Zet Casino Promo-Code 2020 Spielern die Möglichkeit, ihr Casinoerlebnis aufregender und lohnenswerter zu gestalten. Wenn Sie also auf der Suche nach einem neuen Online-Casino sind, sollten Sie sich auf jeden Fall die Aktionen von Zet Casino genauer ansehen und den Promo-Code 2020 nutzen. Viel Spaß und viel Glück beim Spielen!
https://zetcasino.one/
Das „Zet Online Casino“ ist ein aufstrebendes Online-Casino, das Spielern eine Vielzahl von Spielen und tollen Bonusangeboten bietet. Mit einer benutzerfreundlichen Oberfläche und einer großen Auswahl an Spielen ist das Zet Online Casino eine beliebte Anlaufstelle für Glücksspiel-Fans.
Das Casino bietet eine breite Palette von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit Spielen von renommierten Anbietern wie NetEnt, Microgaming und Play’n GO ist für jeden Geschmack etwas dabei. Die Spiele können direkt im Browser gespielt werden, so dass keine zusätzliche Software heruntergeladen werden muss.
Ein besonderes Highlight des Zet Online Casinos sind die großzügigen Bonusangebote. Neue Spieler können sich über einen Willkommensbonus freuen, der zusätzliches Guthaben und Freispiele für ausgewählte Spiele bietet. Darüber hinaus gibt es regelmäßige Promotionen und Aktionen, die den Spielern zusätzliche Gewinnchancen bieten.
Das Zet Online Casino legt großen Wert auf Sicherheit und Fairness. Das Casino ist von der Malta Gaming Authority lizenziert und wird regelmäßig von unabhängigen Prüfungsbehörden auf Fairness und Zufälligkeit der Spiele überprüft. Die Spieler können also sicher sein, dass sie in einem sicheren und vertrauenswürdigen Online-Casino spielen.
Insgesamt ist das Zet Online Casino eine ausgezeichnete Wahl fГјr Spieler, die auf der Suche nach einem hochwertigen und unterhaltsamen Online-Casino-Erlebnis sind. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Bonusangeboten und einem hohen MaГџ an Sicherheit und Fairness ist das Zet Online Casino definitiv einen Besuch wert.
https://zetcasino.one/
Магазин, где можно выбрать рукомойники любого размера.
Достигните новых вершин с помощью приобретения диплома!
https://diplom-kuplu.ru
Zet Casino ist ein aufstrebendes Online-Casino, das sich auf dem Markt einen Namen gemacht hat. Mit einer Vielzahl von Spielen, großzügigen Bonusangeboten und einer benutzerfreundlichen Website ist Zet Casino eine gute Wahl für alle, die ihr Glück versuchen möchten.
Das Casino bietet eine breite Palette von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit Spielen von renommierten Anbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen, ist fГјr jeden Geschmack etwas dabei. Die Spiele sind alle in hoher QualitГ¤t mit toller Grafik und Soundeffekten gestaltet.
Ein weiterer großer Vorteil von Zet Casino sind die großzügigen Bonusangebote. Neue Spieler können einen Willkommensbonus erhalten, der in Form von Bonusgeld und Freispielen angeboten wird. Es gibt auch regelmäßige Promotionen und Turniere, bei denen Spieler zusätzliche Belohnungen verdienen können.
Die Website von Zet Casino ist benutzerfreundlich gestaltet und einfach zu navigieren. Spieler können leicht durch die verschiedenen Spiele und Funktionen der Seite stöbern und finden schnell das, wonach sie suchen. Zudem bietet das Casino eine sichere und geschützte Spielumgebung, in der die persönlichen Daten der Spieler jederzeit sicher sind.
Insgesamt ist Zet Casino eine gute Wahl fГјr alle, die auf der Suche nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis sind. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und einer benutzerfreundlichen Website ist das Casino definitiv einen Besuch wert. Probieren Sie Ihr GlГјck noch heute bei Zet Casino aus und erleben Sie die Spannung und Aufregung des Online-GlГјcksspiels.
https://zetcasino.one/
Zet Casino Auszahlungslimit: Was Sie wissen mГјssen
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und attraktiven Bonusangeboten für seine Spieler bereithält. Wie die meisten Online-Casinos hat auch Zet Casino bestimmte Regeln und Beschränkungen in Bezug auf Auszahlungen. Eines dieser Beschränkungen ist das Auszahlungslimit, das für Spieler wichtig zu beachten ist.
Das Auszahlungslimit bei Zet Casino variiert je nach der gewählten Zahlungsmethode und dem Status des Spielers. Es ist wichtig zu beachten, dass das Limit nicht nur pro Auszahlung, sondern auch pro Woche oder Monat festgelegt ist. Beispielsweise kann das wöchentliche Auszahlungslimit für reguläre Spieler bei 5.000 Euro liegen, während VIP-Spieler möglicherweise ein höheres Limit von 10.000 Euro haben.
Es ist wichtig, dass Spieler sich über die Auszahlungslimits informieren, bevor sie mit dem Spielen im Zet Casino beginnen. Auf der Website des Casinos oder im Kundensupport können Spieler Details zu den spezifischen Limits finden. Es ist auch ratsam, die Allgemeinen Geschäftsbedingungen sorgfältig durchzulesen, um alle Regeln und Beschränkungen zu verstehen.
Das Auszahlungslimit soll dazu dienen, die Sicherheit der Spieler und des Casinos zu gewährleisten und möglichen Betrug oder Missbrauch zu verhindern. Spieler sollten sich bewusst sein, dass das Überschreiten des Auszahlungslimits zu Verzögerungen bei Auszahlungen führen kann oder sogar dazu führen kann, dass das Casino das Konto sperrt.
Insgesamt ist das Auszahlungslimit bei Zet Casino eine wichtige Regel, die es zu beachten gilt. Indem Spieler sich darüber informieren und verantwortungsbewusst spielen, können sie ein unterhaltsames und sicheres Spielerlebnis im Casino genießen.
https://zetcasino.one/
Приветствую всех азартных душ на форуме! Хочу поделиться своим опытом игры в заведение игровые аппараты онлайн. Это территория, где роскошь и страсть встречаются в ярком сочетании. Игровой ассортимент удивляет разнообразием, от классических слотов до живых дилеров. Бонусы и акции регулярно радуют, делая игру ещё еще более захватывающей. все-сутки поддержка постоянно готова помочь. риобет зеркало – это не просто игровая площадка, это истинное королевство риска и развлечений!
казино риобет: Империя Игры и Богатства электронное e0b6b69
Приветствую всех азартных душ на форуме! Хочу поделиться своим опытом игры в гэмблинг-дом игровые аппараты онлайн. Это место, где роскошь и страсть встречаются в сияющем сочетании. Игровой ассортимент впечатляет разнообразием, от традиционных слотов до живых дилеров. Бонусы и акции постоянно радуют, делая игру ещё еще более захватывающей. круглосуточная поддержка всегда готова помочь. риобет зеркало – это не просто казино, это настоящее государство игры и развлечений!
riobet casino отзывы: Государство Риска и Достатка веб- d1_2016
Gogo casino är en populär online casino som har fått mycket uppmärksamhet på senare tid, särskilt på sajten AskGamblers. AskGamblers är en webbplats där spelare kan lämna recensioner och betyg om olika online casinon, och Gogo casino har fått mycket positiv feedback därifrån.
En av anledningarna till att Gogo casino har blivit så populärt på AskGamblers är på grund av dess stora spelutbud. De erbjuder ett brett urval av spel från flera olika spelleverantörer, vilket gör att det finns något för alla typer av spelare. Dessutom erbjuder de också generösa bonusar och kampanjer för sina spelare, vilket gör det ännu mer attraktivt att spela där.
En annan anledning till Gogo casinos popularitet på AskGamblers är deras kundservice. De är kända för att ha en engagerad och professionell kundtjänst som alltid är tillgänglig för spelarna. De är snabba att svara på frågor och lösa eventuella problem som kan uppstå, vilket ger spelarna en trygg och säker spelupplevelse.
Sammanfattningsvis är Gogo casino en pålitlig och välrenommerad online casino som har fått mycket uppskattning på AskGamblers. Med sitt stora spelutbud, generösa bonusar och bra kundservice är det inte konstigt att så många spelare har valt att spela där. Om du letar efter ett pålitligt och underhållande online casino, kan Gogo casino vara ett bra val att prova på.
https://gogocasino.one
Приветствую всех страстных душ на площадке! Хочу разделиться своим опытом игры в игровой клуб игровые автоматы без регистрации. Это локация, где роскошь и азарт встречаются в ярком сочетании. Игровой ассортимент поражает разнообразием, от классических слотов до живых дилеров. Бонусы и акции регулярно радуют, делая игру ещё еще более захватывающей. все-сутки поддержка всегда готова помочь. промокод покердом – это не просто гэмблинг-дом, это реальное королевство игры и забав!
покер дом: Государство Азарта и Состояния онлайн bfee0b6
Приветствую всех страстных душ на площадке! Хочу поделиться своим опытом игры в игровой клуб казино с бездепозитным бонусом за регистрацию с выводом. Это локация, где роскошь и страсть встречаются в сияющем сочетании. Игровой ассортимент удивляет разнообразием, от классических слотов до живых дилеров. Бонусы и акции постоянно радуют, делая игру ещё еще более захватывающей. круглосуточная поддержка всегда готова помочь. онлайн казино покердом – это не просто заведение, это истинное государство игры и забав!
покердом скачать: Монархия Азарта и Достатка цифровое 812fb1f
Приветствую всех волнующих душ на площадке! Хочу разделиться своим опытом игры в казино промокоды казино. Это территория, где роскошь и азарт встречаются в ярком сочетании. Игровой ассортимент удивляет разнообразием, от обычных слотов до реальных дилеров. Бонусы и акции постоянно радуют, делая игру ещё еще более захватывающей. круглосуточная поддержка всегда готова помочь. pokerdom – это не просто игровая площадка, это истинное государство риска и развлечений!
покердом скачать: Империя Игры и Достатка интернет- ad7_c63
Tipico Guthaben in Casino Chips
Immer mehr Menschen entscheiden sich dafür, ihr Tipico Guthaben in Casino Chips umzuwandeln, um in den zahlreichen Online Casinos spielen zu können. Doch was bedeutet es, sein Guthaben in Chips umzuwandeln und wie funktioniert dieser Prozess?
Wenn man sein Tipico Guthaben in Casino Chips umwandelt, tauscht man sein virtuelles Guthaben in Spielchips um, die in den Online Casinos als Währung gelten. Man kann diese Chips dann nutzen, um an verschiedenen Spielen wie Slots, Roulette oder Blackjack teilzunehmen. Es ermöglicht den Spielern, das Guthaben besser zu verwalten und sich auf das eigentliche Spiel zu konzentrieren, ohne sich ständig um den aktuellen Kontostand kümmern zu müssen.
Der Prozess, sein Guthaben in Chips umzuwandeln, ist in der Regel sehr einfach. Man muss lediglich die Option “Chips kaufen” im Online Casino auswГ¤hlen und den gewГјnschten Betrag eingeben. AnschlieГџend wird das Guthaben automatisch in Chips umgewandelt und man kann sofort mit dem Spielen beginnen.
Viele Spieler bevorzugen es, ihr Guthaben in Casino Chips umzuwandeln, da es ihnen ein besseres Spielerlebnis bietet. Man kann sich voll und ganz auf das Spiel konzentrieren, ohne von externen Faktoren abgelenkt zu werden. Zudem ermöglicht es eine bessere Kontrolle über das eigene Spielverhalten, da man genau sieht, wie viel man bereits eingesetzt hat und wie viel Guthaben noch verfügbar ist.
Insgesamt ist die Umwandlung von Tipico Guthaben in Casino Chips eine sinnvolle Option für alle, die gerne in Online Casinos spielen. Es bietet eine bessere Kontrolle über das eigene Spielverhalten und ermöglicht ein angenehmeres Spielerlebnis. Wer also sein Glück in Online Casinos versuchen möchte, sollte die Möglichkeit der Umwandlung seines Guthabens in Chips in Betracht ziehen.
https://tipicocasino.one/
Приветствую всех азартных душ на площадке! Хочу разделиться своим опытом игры в игровая площадка топ лучших казино. Это место, где изысканность и волнение встречаются в ослепительном сочетании. Игровой ассортимент поражает разнообразием, от классических слотов до живых дилеров. Бонусы и акции постоянно радуют, делая игру ещё более захватывающей. все-сутки поддержка всегда готова помочь. покердом зеркало играть онлайн – это не просто гэмблинг-дом, это реальное королевство игры и развлечений!
зеркало покердом: Монархия Игры и Богатства онлайн b6942da
Приветствую всех волнующих душ на площадке! Хочу поделиться своим опытом игры в игровая площадка вулкан официальный сайт вход. Это район, где роскошь и волнение встречаются в прекрасном сочетании. Игровой ассортимент удивляет разнообразием, от классических слотов до живых дилеров. Бонусы и акции регулярно радуют, делая игру ещё еще более захватывающей. все-сутки поддержка постоянно готова помочь. вулкан играть на деньги – это не просто казино, это истинное царство азарта и развлечений!
игровой клуб вулкан: Государство Риска и Имущества онлайн 65d57ad
Приветствую всех азартных душ на ресурсе! Хочу поделиться своим опытом игры в гэмблинг-дом игровые автоматы бесплатно без регистрации онлайн. Это локация, где роскошь и волнение встречаются в ослепительном сочетании. Игровой ассортимент поражает разнообразием, от классических слотов до реальных дилеров. Бонусы и акции регулярно радуют, делая игру ещё еще более захватывающей. все-сутки поддержка всегда готова помочь. казино вулкан скачать – это не просто игровой клуб, это настоящее царство риска и забав!
вулкан казино официальный сайт: Монархия Риска и Богатства электронное b1fb65d
Приветствую всех азартных душ на форуме! Хочу поделиться своим опытом игры в заведение вулкан казино. Это район, где изысканность и страсть встречаются в ярком сочетании. Игровой ассортимент поражает разнообразием, от классических слотов до живых дилеров. Бонусы и акции регулярно радуют, делая игру ещё более захватывающей. 24/7 поддержка всегда готова помочь. casino vulcan – это не просто казино, это реальное царство игры и развлечений!
игровые автоматы вулкан регистрация: Империя Игры и Богатства интернет- dacc581
Das Boomerang Casino ist eine beliebte Online-GlГјcksspielplattform, die eine Vielzahl von Spielen und Casino-Spielen fГјr Spieler aus der ganzen Welt anbietet. In diesem Artikel werden wir eine ГњberprГјfung des Boomerang Casinos durchfГјhren und die wichtigsten Aspekte des Casinos hervorheben.
Das Boomerang Casino zeichnet sich durch eine benutzerfreundliche Oberfläche aus, die es den Spielern leicht macht, sich auf der Website zu orientieren und ihre Lieblingsspiele zu finden. Die Webseite ist gut strukturiert und übersichtlich gestaltet, so dass die Spieler ohne Probleme durch die verschiedenen Spiele navigieren können.
Das Casino bietet eine große Auswahl an Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr. Die Spielautomaten sind in verschiedenen Themen und Designs erhältlich, so dass für jeden Geschmack etwas dabei ist. Die Tischspiele umfassen Klassiker wie Blackjack, Roulette und Baccarat, die sowohl in traditionellen als auch in modernen Varianten gespielt werden können.
Ein weiterer wichtiger Aspekt des Boomerang Casinos sind die großzügigen Boni und Promotionen, die den Spielern angeboten werden. Neue Spieler erhalten einen Willkommensbonus, der ihre ersten Einzahlungen auf der Website verdoppelt. Darüber hinaus gibt es regelmäßig Aktionen und Sonderangebote, die den Spielern zusätzliche Belohnungen und Preise einbringen können.
Das Boomerang Casino bietet auch eine Vielzahl von Zahlungsmethoden, darunter Kreditkarten, E-Wallets und Banküberweisungen, so dass die Spieler bequem Ein- und Auszahlungen tätigen können. Die Website ist sicher und geschützt, so dass die Spieler ihre persönlichen und finanziellen Daten mit Zuversicht angeben können.
Insgesamt ist das Boomerang Casino eine empfehlenswerte Online-Glücksspielplattform, die eine vielseitige Auswahl an Spielen, großzügige Boni und eine benutzerfreundliche Oberfläche bietet. Spieler, die auf der Suche nach einer unterhaltsamen und spannenden Casino-Erfahrung sind, sollten das Boomerang Casino definitiv in Betracht ziehen.
https://boomerangcasino.one/
Tipico Casino Auszahlung blockierter Betrag
Wenn Sie im Tipico Casino spielen und eine Auszahlung beantragen, kann es vorkommen, dass der Betrag blockiert wird. Dies kann verschiedene Gründe haben, und es ist wichtig, zu verstehen, warum dies geschieht und wie Sie das Problem lösen können.
Eine mögliche Ursache dafür, dass Ihr Auszahlungsbetrag blockiert wird, ist, dass Ihr Konto nicht verifiziert ist. In diesem Fall müssen Sie Dokumente wie Ihren Ausweis oder eine Rechnung vorlegen, um Ihre Identität zu bestätigen und das Konto freizuschalten.
Ein weiterer Grund könnte sein, dass Sie Bonusbedingungen nicht erfüllt haben. Bevor Sie eine Auszahlung vornehmen können, müssen Sie möglicherweise bestimmte Umsatzanforderungen erfüllen. Überprüfen Sie daher immer die Bedingungen, bevor Sie eine Auszahlung beantragen.
Es kann auch vorkommen, dass Ihr Auszahlungsbetrag aufgrund von Sicherheitsgründen blockiert wird. Dies kann passieren, wenn verdächtige Aktivitäten auf Ihrem Konto festgestellt werden oder wenn ungewöhnliche Transaktionen stattfinden. In diesem Fall müssen Sie sich möglicherweise an den Kundensupport wenden und weitere Informationen bereitstellen.
Um eine blockierte Auszahlung zu lösen, sollten Sie als Erstes den Kundensupport kontaktieren. Sie können Ihnen helfen, das Problem zu identifizieren und eine Lösung zu finden. Stellen Sie sicher, dass Sie alle erforderlichen Dokumente bereithalten, um den Prozess zu beschleunigen.
Insgesamt ist es wichtig, Geduld zu haben und die Ursache für die blockierte Auszahlung zu ermitteln. Mit der richtigen Vorgehensweise und Unterstützung vom Kundensupport sollten Sie in der Lage sein, das Problem zu lösen und Ihren Auszahlungsbetrag freizugeben.
https://tipicocasino.one/
Das Tipico Casino für Android ist die perfekte Möglichkeit, um unterwegs ein spannendes Casino-Erlebnis zu genießen. Die App ist einfach zu bedienen und bietet ein umfangreiches Angebot an verschiedenen Casino-Spielen.
Egal ob Slots, Roulette, Blackjack oder Poker – im Tipico Casino fГјr Android findet jeder Spieler sein Lieblingsspiel. Die App Гјberzeugt nicht nur durch eine groГџe Auswahl an Spielen, sondern auch durch eine benutzerfreundliche OberflГ¤che und schnelle Ladezeiten.
Ein weiterer Vorteil des Tipico Casinos für Android ist die Möglichkeit, auch unterwegs auf das Live-Casino zuzugreifen. Hier können Spieler gegen echte Dealer antreten und das echte Casino-Feeling erleben.
Darüber hinaus bietet das Tipico Casino für Android auch regelmäßige Aktionen und Boni für seine Spieler. So können Nutzer von attraktiven Einzahlungsboni und Freispielaktionen profitieren und ihre Gewinnchancen erhöhen.
Insgesamt ist das Tipico Casino für Android eine gelungene App für alle Casino-Fans, die auch unterwegs nicht auf ihr Lieblingsspiel verzichten wollen. Egal ob Anfänger oder erfahrener Spieler, hier kommt jeder auf seine Kosten. Also laden Sie die App noch heute herunter und starten Sie Ihr Casino-Abenteuer auf Ihrem Android-Gerät. Viel Glück und Spaß beim Spielen!
https://tipicocasino.one/
Im Tipico Casino gibt es eine große Auswahl an spannenden Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit dem Filter-Tool des Casinos können Spieler ihre Lieblingsspiele schnell und einfach finden, ohne lange danach suchen zu müssen.
Das Filtern von Casino-Spielen ist besonders nützlich für Spieler, die klare Vorlieben haben oder bestimmte Spiele bevorzugen. Zum Beispiel können Spieler nach Spielkategorie, Anbieter, Beliebtheit, Neuheiten oder Jackpot-Spielen filtern. So können sie leicht die Spiele finden, die ihren Anforderungen am besten entsprechen.
Das Filtern von Spielen im Tipico Casino ist auch praktisch, um neue Spiele zu entdecken und auszuprobieren. Spieler können nach den neuesten Veröffentlichungen filtern und so immer auf dem neuesten Stand bleiben, was das Spielangebot betrifft.
Zusätzlich bietet das Filter-Tool im Tipico Casino auch die Möglichkeit, Spiele nach Beliebtheit zu sortieren. So können Spieler sehen, welche Spiele besonders beliebt sind und von anderen Spielern gerne gespielt werden. Dies kann hilfreich sein, um neue Lieblingsspiele zu finden, die möglicherweise bisher übersehen wurden.
Insgesamt ist das Filtern von Casino-Spielen im Tipico Casino eine praktische und benutzerfreundliche Funktion, die es Spielern ermöglicht, schnell die Spiele zu finden, die ihren Vorlieben entsprechen. Egal ob man nach bestimmten Spielen sucht oder einfach nur neue Spiele entdecken möchte, das Filter-Tool des Casinos ist eine hilfreiche Unterstützung für alle Spieler.
https://tipicocasino.one/
https://grainloader.vn.ua
Gold Bug Equipment stores a assortment of quality corn loaders opportune in the service of jobs of all shapes and sizes.
grainloader.vn.ua
Das Boomerang Casino ist eine aufregende Online-Glücksspiel-Plattform, die Spielern die Möglichkeit bietet, ihr Glück in einer Vielzahl von Casino-Spielen zu versuchen. Mit einer großen Auswahl an Slots, Tischspielen und Live-Casino-Spielen ist für jeden Geschmack etwas dabei.
Das Casino zeichnet sich durch sein attraktives Design und seine benutzerfreundliche Oberfläche aus, die es Spielern leicht macht, sich auf der Website zu navigieren. Darüber hinaus bietet das Boomerang Casino eine Vielzahl von Boni und Aktionen, die es den Spielern ermöglichen, ihr Spielerlebnis zu verbessern und ihre Gewinnchancen zu erhöhen.
Ein weiteres Highlight des Boomerang Casinos ist die Möglichkeit, Live-Casino-Spiele zu spielen, bei denen Spieler in Echtzeit gegen echte Dealer antreten können. Dies schafft eine authentische Casino-Atmosphäre und sorgt für ein noch spannenderes Spielerlebnis.
Darüber hinaus bietet das Boomerang Casino eine Vielzahl von Zahlungsmethoden, um sicherzustellen, dass Ein- und Auszahlungen schnell und bequem getätigt werden können. Die Website ist auch sicher und geschützt, um die persönlichen Daten der Spieler zu schützen.
Insgesamt bietet das Boomerang Casino eine unterhaltsame und spannende Spielerfahrung fГјr alle, die gerne online spielen. Mit seiner groГџen Auswahl an Spielen, attraktiven Boni und einem benutzerfreundlichen Design ist es definitiv einen Besuch wert.
https://boomerangcasino.one/
Приветствую, ценители захватывающих приключений! Хочу рассказать своим великолепием от виртуального казино “Селектор онлайн казино”. Это не просто площадка для игр, это абсолютный область чувств и забав! Здесь я обрел все, что мне требуется: различие игр, обильные бонусы и скоростные выплаты. Но главное – это настроение, которая правит здесь. Виртуально-реальные приключения, потрясающие турниры и милосердное сообщество игроков делают каждую игру неизгладимой! Присоединяйтесь к “Селектор играть” и погрузитесь в мир интригующих развлечений!
FГјr GlГјcksspiel-Fans gibt es eine aufregende neue MГ¶glichkeit, ihr GlГјck zu versuchen – das Zet Casino bietet einen kostenlosen Bonus ohne Einzahlung an. Das bedeutet, dass Spieler die Chance haben, echtes Geld zu gewinnen, ohne ihr eigenes Geld riskieren zu mГјssen.
Um den Bonus zu erhalten, mГјssen Spieler lediglich ein Konto im Zet Casino erstellen und den Bonuscode bei der Registrierung eingeben. Der Bonus wird dann automatisch gutgeschrieben und kann fГјr eine Vielzahl von Spielen im Casino verwendet werden.
Mit dem kostenlosen Bonus können Spieler das Casino erkunden und verschiedene Spiele ausprobieren, ohne sich Gedanken über Verluste machen zu müssen. Es ist eine großartige Möglichkeit für neue Spieler, sich mit dem Casino vertraut zu machen und ihre Lieblingsspiele zu entdecken.
Es ist jedoch wichtig zu beachten, dass der Bonus bestimmten Umsatzbedingungen unterliegt, bevor er ausgezahlt werden kann. Spieler sollten daher die Bonusbedingungen sorgfältig lesen, um sicherzustellen, dass sie die Anforderungen erfüllen.
Insgesamt ist der Zet Casino Free Bonus ohne Einzahlung eine großartige Möglichkeit für Spieler, das Casino zu testen und echtes Geld zu gewinnen, ohne etwas zu riskieren. Es ist definitiv einen Versuch wert!
https://zetcasino.one/
Boomerang Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen für seine Spieler anbietet. Um neue Spieler anzuziehen und ihre bestehenden Spieler zu belohnen, bietet Boomerang Casino regelmäßig Bonuscodes an, die es den Spielern ermöglichen, zusätzliches Bargeld oder Freispiele zu erhalten, ohne eine Einzahlung tätigen zu müssen.
Ein besonders beliebter Bonus bei Boomerang Casino sind die sogenannten “No Deposit Bonus Codes”. Diese Codes ermГ¶glichen es den Spielern, kostenloses Geld oder Freispiele zu erhalten, ohne dass eine Einzahlung getГ¤tigt werden muss. Diese Bonusangebote sind eine groГџartige MГ¶glichkeit fГјr die Spieler, das Casino kennenzulernen und ihre Lieblingsspiele auszuprobieren, ohne dabei ihr eigenes Geld riskieren zu mГјssen.
Um von den No Deposit Bonus Codes bei Boomerang Casino zu profitieren, müssen die Spieler lediglich den Code eingeben, der ihnen zur Verfügung gestellt wird, und schon erhalten sie ihren Bonus. Die Bedingungen und Anforderungen für den Bonus variieren je nach Angebot, daher ist es wichtig, die Bonusbedingungen sorgfältig zu lesen, bevor man den Bonus in Anspruch nimmt.
Die No Deposit Bonus Codes bei Boomerang Casino sind eine großartige Möglichkeit für die Spieler, zusätzliches Bargeld oder Freispiele zu erhalten, ohne eine Einzahlung tätigen zu müssen. Diese Bonusangebote ermöglichen es den Spielern, ihre Lieblingsspiele zu genießen, ohne dabei ihr eigenes Geld riskieren zu müssen. Wenn auch Sie von diesen großzügigen Bonusangeboten profitieren möchten, schauen Sie doch bei Boomerang Casino vorbei und sehen Sie, welche No Deposit Bonus Codes gerade verfügbar sind. Viel Spaß und viel Glück beim Spielen!
https://boomerangcasino.one/
Das Tipico Casino bietet eine Vielzahl von spannenden Spielautomaten, die für jede Menge Energie sorgen. Ob man lieber klassische Früchteslots oder moderne Video-Slots mit aufregenden Bonusfeatures spielt, im Tipico Casino findet jeder Spieler garantiert seinen persönlichen Favoriten.
Die Casino Slot Spiele im Tipico Casino zeichnen sich durch eine hohe Qualität und innovative Grafiken aus, die für ein ultimatives Spielvergnügen sorgen. Durch die hohe Energie und Spannung, die diese Spiele bieten, wird das Casinoerlebnis noch intensiver und aufregender.
Zusätzlich zu den spannenden Spielen bietet das Tipico Casino auch attraktive Bonusangebote und Aktionen, die für zusätzliche Energie und Unterhaltung sorgen. Von Willkommensboni über Freispiele bis zu Turnieren und Gewinnspielen, es gibt immer etwas Neues zu entdecken und zu gewinnen.
Das Tipico Casino ist bekannt für seine fairen Spielbedingungen und schnellen Auszahlungen, wodurch die Spieler sich voll und ganz auf ihr Spiel konzentrieren können und sich keine Sorgen machen müssen. Mit einer breiten Auswahl an Slot-Spielen und einem kompetenten Kundenservice steht dem ultimativen Casinoerlebnis nichts im Wege.
Insgesamt bietet das Tipico Casino eine energiegeladene und aufregende Atmosphäre, die jeden Spieler begeistern wird. Egal, ob man ein erfahrener Casino-Fan oder ein Neueinsteiger ist, im Tipico Casino kommt jeder auf seine Kosten und kann sein Glück an den zahlreichen Slot-Spielen versuchen. Probieren Sie es aus und erleben Sie die Energie der Tipico Casino Slots selbst!
https://tipicocasino.one/
m.zet Casino ist ein neues und aufregendes Online-Casino, das Spielern die Möglichkeit bietet, ihre Lieblingsspiele von überall aus zu genießen. Mit einer breiten Palette von Spielen, großzügigen Boni und erstklassigem Kundenservice ist m.zet Casino der ultimative Ort für Casino-Enthusiasten.
Das Casino bietet eine Vielzahl von Spielen, darunter Spielautomaten, Tischspiele, Video-Poker und Live-Dealer-Spiele. Egal, ob Sie ein Fan von klassischen Spielautomaten sind oder auf der Suche nach neuen und aufregenden Spielen sind, m.zet Casino hat fГјr jeden etwas zu bieten.
Ein weiterer großer Vorteil von m.zet Casino sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler können von einem Willkommensbonus profitieren, der ihre Einzahlungen erhöht und ihnen mehr Möglichkeiten bietet, zu gewinnen. Darüber hinaus gibt es auch regelmäßige Promotionen, die den Spielern zusätzliche Belohnungen bieten.
Der Kundenservice von m.zet Casino ist erstklassig und steht den Spielern rund um die Uhr zur VerfГјgung. Egal, ob es um technische Probleme, Fragen zu Boni oder einfach nur um Hilfe bei der Navigation auf der Website geht, das Team von m.zet Casino ist immer da, um zu helfen.
Insgesamt ist m.zet Casino eine groГџartige Wahl fГјr alle, die nach einem unterhaltsamen und spannenden Online-Casino-Erlebnis suchen. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und hervorragendem Kundenservice gibt es keinen Grund, warum Sie nicht heute noch Ihr GlГјck bei m.zet Casino versuchen sollten.
https://zetcasino.one/
Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die ihren Spielern eine breite Palette an Spielen und Funktionen bietet. Mit der Einführung der Boomerang Casino App können Spieler jetzt noch einfacher und bequemer auf ihre Lieblingsspiele zugreifen.
Die App ist benutzerfreundlich gestaltet und ermöglicht es den Spielern, ihre Lieblingsspiele unterwegs zu spielen. Egal, ob Sie Slots, Tischspiele oder Live-Casino-Spiele bevorzugen, die Boomerang Casino App hat für jeden Geschmack etwas zu bieten. Darüber hinaus bietet die App regelmäßig Boni und Aktionen an, um die Spieler zu belohnen und ihr Spielerlebnis zu verbessern.
Die Boomerang Casino App verfügt über eine Vielzahl von Zahlungsoptionen, so dass die Spieler problemlos Ein- und Auszahlungen vornehmen können. Darüber hinaus ist die App sicher und zuverlässig, so dass die Spieler sich keine Sorgen um die Sicherheit ihrer persönlichen Daten machen müssen.
Insgesamt bietet die Boomerang Casino App eine großartige Möglichkeit, das Casino-Erlebnis zu genießen, egal wo Sie sich befinden. Mit einer benutzerfreundlichen Oberfläche, einer Vielzahl von Spielen und regelmäßigen Boni und Aktionen ist die App definitiv einen Versuch wert. Laden Sie noch heute die Boomerang Casino App herunter und erleben Sie die Spannung des Glücksspiels auf Ihrem Handy oder Tablet.
https://boomerangcasino.one/
Zet Casino Bonus ohne Einzahlung – deinen Start im Online Casino erleichtern
In der Welt des Online Glücksspiels gibt es ständig neue Angebote und Aktionen, die Spieler dazu verleiten sollen, sich in einem bestimmten Casino anzumelden. Eines dieser Angebote ist der Zet Casino Bonus ohne Einzahlung, der es Spielern ermöglicht, das Casino und seine Spiele zunächst ohne eigenes Geld auszuprobieren.
Ein Bonus ohne Einzahlung ist eine großartige Möglichkeit für Spieler, ein neues Casino kennenzulernen, ohne finanzielle Risiken einzugehen. Bei Zet Casino erhalten neue Spieler einen Bonus von 10 Euro ohne Einzahlung, sobald sie sich registrieren. Mit diesem Bonus können Spieler das Casino erkunden und erste Gewinne erzielen, ohne Geld ausgeben zu müssen.
Um den Bonus ohne Einzahlung zu erhalten, müssen Spieler lediglich ein Konto bei Zet Casino anlegen. Der Bonus wird dann automatisch gutgeschrieben und steht sofort zur Verfügung. Es gibt jedoch einige Bedingungen, die Spieler erfüllen müssen, bevor sie Gewinne aus dem Bonus auszahlen lassen können. Dazu gehört in der Regel das Erfüllen eines Umsatzziels, das innerhalb eines bestimmten Zeitraums erreicht werden muss.
Der Zet Casino Bonus ohne Einzahlung ist eine großartige Möglichkeit, um das Casino und seine Spiele kennenzulernen, ohne eigenes Geld riskieren zu müssen. Spieler können mit dem Bonus erste Erfahrungen sammeln und entscheiden, ob das Casino ihren Erwartungen entspricht. Mit etwas Glück können Spieler sogar erste Gewinne erzielen, die sie sich auszahlen lassen können.
Fazit: Der Zet Casino Bonus ohne Einzahlung ist eine attraktive Möglichkeit, um das Casino risikofrei kennenzulernen und erste Gewinne zu erzielen. Spieler sollten jedoch die Bedingungen des Bonus genau lesen und sicherstellen, dass sie die Umsatzanforderungen erfüllen, um sich Gewinne auszahlen lassen zu können.
https://zetcasino.one/
Das Tipico Casino feiert Geburtstag! Seit einem Jahr bietet der beliebte Online-Glücksspielanbieter seinen Kunden ein umfangreiches Angebot an spannenden Spielen, attraktiven Aktionen und tollen Gewinnchancen. Zur Feier des Tages dürfen sich die Spieler auf besondere Überraschungen und Jubiläumsangebote freuen.
Seit seiner Gründung hat sich das Tipico Casino einen festen Platz in der Online-Glücksspielbranche erobert. Mit einer Vielzahl von Slots, Tischspielen und Live-Casino-Tischen bietet das Casino eine breite Auswahl für jeden Geschmack. Dazu kommen regelmäßige Aktionen und Promotionen, die den Spielern zusätzliche Gewinnchancen bieten.
Zum Geburtstag des Tipico Casinos können sich die Spieler auf besondere Boni, Freispiele und Verlosungen freuen. Es lohnt sich, die Augen offen zu halten und regelmäßig die Aktionen auf der Website zu überprüfen, um keine der Jubiläumsangebote zu verpassen.
Das Tipico Casino legt großen Wert auf die Sicherheit und Zufriedenheit seiner Kunden. Mit einer gültigen Lizenz und einer professionellen Kundenbetreuung sorgt das Casino für ein faires und unterhaltsames Spielerlebnis. Zudem bietet die Tipico Casino App die Möglichkeit, auch unterwegs die spannenden Spiele zu genießen.
Wir gratulieren dem Tipico Casino herzlich zum Geburtstag und wünschen allen Spielern viel Glück und Spaß beim Jubiläumsevent. Möge das Casino weiterhin erfolgreich wachsen und seinen Kunden ein erstklassiges Spielerlebnis bieten. Prost auf ein weiteres erfolgreiches Jahr!
https://tipicocasino.one/
Tipico ist ein beliebtes Online-Casino, das seinen Kunden eine Vielzahl von Spielmöglichkeiten bietet. Wer sein Glück hier versuchen möchte, muss zunächst Geld auf sein Spielerkonto transferieren. In diesem Artikel gehen wir genauer darauf ein, wie Sie Geld von Ihrem Bankkonto auf Ihr Tipico Casino-Konto überweisen können.
Um Geld in Ihr Tipico Casino-Konto zu transferieren, stehen Ihnen verschiedene Zahlungsmethoden zur Verfügung. Eine der gängigsten Methoden ist die Überweisung per Banküberweisung. Dazu müssen Sie zunächst Ihr Bankkonto mit Ihrem Tipico Konto verknüpfen. Dies können Sie ganz einfach in Ihrem persönlichen Bereich auf der Website von Tipico erledigen. Dort finden Sie alle nötigen Informationen, die Sie für die Überweisung benötigen.
Um Geld per Banküberweisung auf Ihr Tipico Konto zu transferieren, geben Sie einfach den gewünschten Betrag sowie die Kontodaten von Tipico an. Innerhalb weniger Tage sollten Sie über das Geld auf Ihrem Spielerkonto verfügen können. Beachten Sie jedoch, dass bei dieser Zahlungsmethode möglicherweise Gebühren anfallen können.
Eine weitere Möglichkeit, Geld auf Ihr Tipico Konto zu überweisen, ist die Nutzung von E-Wallets wie PayPal oder Skrill. Diese Zahlungsmethoden sind oft schneller als Banküberweisungen und ermöglichen es Ihnen, sofort über das Geld auf Ihrem Spielerkonto zu verfügen. Auch hier müssen Sie zunächst Ihr E-Wallet mit Ihrem Tipico Konto verknüpfen, um Geld transferieren zu können.
Es ist wichtig zu beachten, dass der Betrag, den Sie auf Ihr Tipico Konto überweisen möchten, von den jeweiligen Zahlungsdienstleistern und Banken abhängig sein kann. Informieren Sie sich daher vorab über eventuelle Gebühren und Limits, die für die Überweisung gelten.
Insgesamt bietet Tipico seinen Kunden eine Vielzahl von Möglichkeiten, Geld auf das Casino-Konto zu überweisen. Egal ob per Banküberweisung oder E-Wallet, mit den richtigen Informationen und einer sicheren Zahlungsmethode können Sie schnell und unkompliziert Ihr Spielerkonto füllen und direkt mit dem Spielen beginnen. Viel Erfolg und Spaß beim Zocken!
https://tipicocasino.one/
kraken tor – кракен онион, кракен ссылка тор
Willkommen im Zet Casino und sichern Sie sich den großzügigen Willkommensbonus! Das Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und aufregenden Bonusangeboten für seine Spieler bereithält. Einer der attraktivsten Aspekte des Zet Casinos ist der lukrative Willkommensbonus, den neue Spieler bei ihrer ersten Einzahlung erhalten können.
Der Zet Casino Willkommensbonus belohnt neue Spieler mit einem großzügigen Bonusguthaben und Freispielen für ausgewählte Spiele. Um von diesem Bonusangebot zu profitieren, müssen neue Spieler lediglich ein Konto im Zet Casino erstellen und eine erste Einzahlung tätigen. Der Willkommensbonus wird dann automatisch auf das Spielerkonto gutgeschrieben.
Das Bonusguthaben kann für eine Vielzahl von Spielen im Zet Casino verwendet werden, darunter Spielautomaten, Tischspiele und Live-Casino-Spiele. Die Freispiele, die im Rahmen des Willkommensbonus angeboten werden, können auf ausgewählten Spielautomaten gespielt werden und bieten die Chance, zusätzliche Gewinne zu erzielen.
Es ist wichtig zu beachten, dass der Zet Casino Willkommensbonus bestimmten Umsatzbedingungen unterliegt, die erfüllt werden müssen, bevor Gewinne aus dem Bonusguthaben ausgezahlt werden können. Diese Umsatzbedingungen variieren je nach Angebot und sind auf der Website des Zet Casinos ausführlich beschrieben.
Wenn Sie also auf der Suche nach einem erstklassigen Online-Casino mit lukrativen Bonusangeboten sind, ist das Zet Casino definitiv einen Besuch wert. Nutzen Sie den Willkommensbonus, um Ihr Spielerlebnis zu maximieren und spannende Spiele zu genieГџen. Viel SpaГџ und viel GlГјck im Zet Casino!
https://zetcasino.one/
kraken тор – кракен тор, kraken darknet market зеркало
кракен ссылка – кракен онион, kraken store
a knockout post anydesk
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und Boni anbietet. In diesem Artikel werden wir uns genauer mit den verschiedenen Bewertungen von Zet Casino befassen.
Zet Casino hat sich in den letzten Jahren einen Namen als zuverlässiges und unterhaltsames Online-Casino gemacht. Viele Spieler loben die große Auswahl an Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und mehr. Die Benutzeroberfläche ist einfach zu bedienen und bietet eine reibungslose Spielerfahrung.
Ein weiterer Pluspunkt von Zet Casino sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler können von einem Willkommensbonus profitieren, der Freispiele und Bonusgeld umfasst. Auch treue Spieler werden belohnt, zum Beispiel mit Cashback-Angeboten und VIP-Programmen.
Die meisten Bewertungen von Zet Casino sind positiv, mit Spielern, die die Vielfalt der Spiele, die Benutzerfreundlichkeit der Website und die groГџzГјgigen Boni loben. Einige Kritikpunkte beziehen sich auf die Geschwindigkeit der Auszahlungen und den Kundenservice, der manchmal als langsam und unzureichend beschrieben wird.
Insgesamt scheint Zet Casino eine gute Wahl für Spieler zu sein, die eine große Auswahl an Spielen und Boni schätzen. Wenn Sie auf der Suche nach einem neuen Online-Casino sind, könnte Zet Casino eine gute Option für Sie sein.
https://zetcasino.one/
website here tradingview download
Das Online-Casino Boomerang bietet seinen Spielern eine Vielzahl von spannenden und unterhaltsamen Spielen. Von klassischen Tischspielen wie Roulette und Blackjack bis hin zu modernen Spielautomaten und Live-Casino-Spielen, hier gibt es fГјr jeden Geschmack etwas Passendes.
Ein weiterer Vorteil des Casinos ist die Möglichkeit, von überall und zu jederzeit spielen zu können. Egal ob man ein paar freie Minuten in der Mittagspause hat oder abends gemütlich auf der Couch entspannen möchte, das Casino en ligne Boomerang ist immer verfügbar.
Darüber hinaus bietet das Casino attraktive Boni und Promotionen, die das Spielerlebnis noch spannender machen. Von Willkommensboni für neue Spieler bis hin zu regelmäßigen Aktionen und Gewinnspielen, hier gibt es immer etwas zu gewinnen.
Die Sicherheit der Spieler steht im Casino Boomerang an oberster Stelle. Durch eine sichere SSL-Verschlüsselung werden sämtliche Daten vor unbefugtem Zugriff geschützt. Zudem arbeitet das Casino nur mit vertrauenswürdigen Zahlungsdienstleistern zusammen, um Ein- und Auszahlungen sicher und schnell abwickeln zu können.
Insgesamt ist das Casino en ligne Boomerang eine ausgezeichnete Wahl fГјr alle, die nach einem unterhaltsamen und sicheren Online-Casino suchen. Mit einer breiten Auswahl an Spielen, attraktiven Boni und erstklassigem Kundenservice ist hier fГјr ein unvergessliches Spielerlebnis gesorgt. Besuchen Sie das Casino noch heute und erleben Sie die Faszination des GlГјcksspiels von zu Hause aus!
https://boomerangcasino.one/
PlayPix android
Индексация ссылок на сайте в индексе ру
Tipico Casino Transferieren Sport
Das Tipico Casino bietet seinen Kunden die Möglichkeit, Geld zwischen ihrem Casino-Konto und ihrem Sportwetten-Konto zu transferieren. Dies ermöglicht es den Spielern, ihre Gewinne aus dem Casino auch für Sportwetten zu verwenden oder umgekehrt.
Der Transfer zwischen den Konten ist einfach und unkompliziert. Spieler können einfach den Transfer-Button auf der Website oder in der App verwenden, um Geld von einem Konto auf das andere zu überweisen. Der Transfer erfolgt in Echtzeit, so dass die Spieler sofort über das Geld verfügen können.
Diese Funktion bietet den Spielern eine erhöhte Flexibilität und ermöglicht es ihnen, ihr Geld optimal zu nutzen. Sie können ihre Gewinne aus dem Casino direkt für Sportwetten verwenden und umgekehrt. Dies macht das Tipico Casino zu einer bequemen und praktischen Wahl für alle Spieler, die gerne sowohl im Casino als auch bei Sportwetten aktiv sind.
DarГјber hinaus bietet das Tipico Casino eine Vielzahl von Spielen und Sportwetten, so dass fГјr jeden Geschmack etwas dabei ist. Von Slots Гјber Tischspiele bis hin zu Live-Casino-Spielen und einer Vielzahl von Sportwetten – hier finden Spieler alles, was das Herz begehrt.
Insgesamt ist die MГ¶glichkeit, Geld zwischen dem Tipico Casino und dem Sportwetten-Konto zu transferieren, eine praktische Funktion, die den Spielern eine ganze neue Welt an MГ¶glichkeiten erГ¶ffnet. Egal ob man lieber im Casino spielt oder bei Sportwetten sein GlГјck versucht – mit diesem Feature ist beides mГ¶glich. Wer also gerne flexibel bleibt und gerne verschiedene GlГјcksspiele ausprobiert, ist im Tipico Casino genau richtig aufgehoben.
https://tipicocasino.one/
Привет всем! Я с удовольствием поделюсь своим практикой процесса на сайте “Azino777“. Это район, где страсть и развлечения встречаются в захватывающем сочетании. Разнообразие игр, щедрые привилегии и квалифицированная поддержка делают игровой опыт запоминающимся. Присоединяйтесь и ощутите эмоции триумфа вместе с “азино777 официальный”!
Привет всем! Я с восторгом поделюсь своим опытом геймплея на сайте “игровые автоматы“. Это территория, где азарт и игры встречаются в захватывающем сочетании. Разнообразие геймплеев, щедрые премии и профессиональная поддержка делают игровой опыт запоминающимся. Присоединяйтесь и ощутите волнение успеха вместе с “7к казино”!
Привет всем! Я с восторгом поделюсь своим опытом геймплея на сайте “играть онлайн казино“. Это территория, где азарт и развлечения встречаются в захватывающем сочетании. Многообразие геймплеев, благодарные премии и опытная поддержка делают геймплей опыт запоминающимся. Присоединяйтесь и ощутите волнение победы вместе с “игровые автоматы 7к”!
Das Sportwettenunternehmen Tipico ist vielen bekannt für seine vielfältigen Wettmöglichkeiten und attraktiven Quoten. Doch was passiert, wenn das Tipico Sports Konto im Casino blockiert wird?
Grundsätzlich ist es bei Tipico möglich, sowohl Sportwetten als auch Casino Spiele zu spielen. Jedoch kann es vorkommen, dass das Konto für das Casino blockiert wird, während das Sportwetten weiterhin genutzt werden können. Dies kann verschiedene Gründe haben, wie zum Beispiel Verstöße gegen die Nutzungsbedingungen oder verdächtige Aktivitäten.
Wenn das Tipico Sports Konto im Casino blockiert wird, ist es wichtig, sich an den Kundensupport zu wenden, um den genauen Grund für die Blockade zu erfahren. Der Support kann weitere Informationen geben und gegebenenfalls die Blockade aufheben, falls es sich um ein Missverständnis handelt.
Es ist ratsam, sich an die Regeln und Bedingungen von Tipico zu halten, um eine Blockade des Kontos zu vermeiden. Zudem sollte man verantwortungsbewusst spielen und keine illegalen Aktivitäten durchführen, um nicht gegen die Nutzungsbedingungen zu verstoßen.
Insgesamt ist es wichtig, bei Problemen mit dem Tipico Sports Konto im Casino ruhig zu bleiben und den Kundensupport zu kontaktieren. Mit einer klaren Kommunikation und dem Einhalten der Regeln kann in den meisten Fällen eine Lösung gefunden werden.
https://tipicocasino.one/
Привет всем! Я с удовольствием поделюсь своим практикой игры на ресурсе “слоты играть“. Это территория, где страсть и развлечения встречаются в пленительном сочетании. Разнообразие игр, генерозные бонусы и профессиональная поддержка делают геймплей опыт запоминающимся. Присоединяйтесь и ощутите эмоции успеха вместе с “7k казино”!
Привет всем! Я с удовольствием поделюсь своим опытом игры на площадке “онлайн казино 7k“. Это локация, где волнение и развлечения встречаются в захватывающем сочетании. Многообразие игр, щедрые бонусы и квалифицированная поддержка делают процесс опыт незабываемым. Присоединяйтесь и ощутите волнение триумфа вместе с “7к казино играть”!
Zet Casino Paysafecard: Eine sichere und bequeme Einzahlungsmethode
Das Zet Casino ist bekannt für seine vielfältige Auswahl an Spielen und großzügigen Bonusangebote. Eine der beliebtesten Einzahlungsmethoden, die von Spielern im Zet Casino verwendet wird, ist Paysafecard. Paysafecard ist eine Prepaid-Zahlungsmethode, die es Spielern ermöglicht, schnell und sicher Geld auf ihr Casinokonto einzuzahlen.
Die Verwendung von Paysafecard im Zet Casino ist einfach und unkompliziert. Spieler müssen lediglich eine Paysafecard in einem Geschäft oder online kaufen und den auf der Karte befindlichen Code im Einzahlungsbereich des Casinos eingeben. Das eingezahlte Geld wird sofort auf das Casinokonto gutgeschrieben, sodass Spieler ohne Verzögerung mit dem Spielen beginnen können.
Eine der Hauptvorteile der Verwendung von Paysafecard im Zet Casino ist die Sicherheit. Da Paysafecard eine Prepaid-Zahlungsmethode ist, sind Spieler nicht verpflichtet, persönliche oder finanzielle Informationen preiszugeben. Dies macht es zu einer idealen Option für Spieler, die Wert auf Datenschutz und Sicherheit legen.
Darüber hinaus bietet Paysafecard eine schnelle und bequeme Zahlungsmethode für Spieler im Zet Casino. Mit Paysafecard können Spieler innerhalb weniger Minuten Geld auf ihr Casinokonto einzahlen, ohne lange Wartezeiten oder lästige Verifizierungsprozesse.
Insgesamt ist die Verwendung von Paysafecard im Zet Casino eine sichere, bequeme und zuverlässige Einzahlungsmethode für Spieler. Mit der Möglichkeit, sofort Geld auf das Casinokonto einzuzahlen und gleichzeitig die Privatsphäre zu wahren, ist Paysafecard eine beliebte Wahl für Spieler im Zet Casino. Probieren Sie es aus und erleben Sie die Vorteile von Paysafecard im Zet Casino!
https://zetcasino.one/
Добрый день, комрады! Стремлюсь обмениваться собственными эмоциями о зале кент казино официальный сайт. Этот портал напросто поражает многообразием игр и особенной атмосферой азарта! Превосходная изображение, быстрые вознаграждения и соблазнительные подарки формируют игровой процесс неизгладимым. Порядочная забава и высший уровень секретности — вот то, какое вдохновляет меня возвращаться снова и снова. Предлагаю всем, тем ценит высококачественный отдыхание и массивные выигрыши
Boomerang Casino Test: Ist dieses Online-Casino sein Geld wert?
Das Boomerang Casino ist eine beliebte Online-GlГјcksspielseite, die Spielern eine Vielzahl von Spielen und Promotionen bietet. Doch ist dieses Casino sein Geld wirklich wert? In diesem Test werden wir die wichtigsten Aspekte des Boomerang Casinos genauer unter die Lupe nehmen und herausfinden, ob es sich lohnt, dort zu spielen.
Das erste, was bei der Bewertung eines Online-Casinos berücksichtigt werden muss, ist die Sicherheit und Zuverlässigkeit der Seite. Das Boomerang Casino verfügt über eine gültige Lizenz der Malta Gaming Authority, die als eine der strengsten Glücksspielbehörden der Welt gilt. Dies bedeutet, dass das Casino den internationalen Standards entspricht und Fairness und Transparenz gewährleistet.
Ein weiterer wichtiger Aspekt ist die Spielauswahl. Das Boomerang Casino bietet Hunderte von Spielen von renommierten Anbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen. Von Slots Гјber Tischspiele bis hin zu Live-Casino-Spielen ist fГјr jeden Geschmack etwas dabei. Die Spiele sind auch auf mobilen GerГ¤ten verfГјgbar, sodass Sie jederzeit und Гјberall spielen kГ¶nnen.
Natürlich ist auch der Kundenservice ein wichtiger Faktor bei der Bewertung eines Online-Casinos. Das Boomerang Casino bietet einen rund um die Uhr verfügbaren Live-Chat sowie eine E-Mail-Unterstützung, um sicherzustellen, dass alle Spieler Hilfe erhalten, wenn sie sie benötigen.
Was die Boni und Promotionen betrifft, so bietet das Boomerang Casino großzügige Willkommensboni für neue Spieler sowie regelmäßige Aktionen und Sonderangebote für bestehende Kunden. Diese Boni können Ihren Bankroll erheblich aufstocken und Ihnen mehr Chancen geben, zu gewinnen.
Zusammenfassend lässt sich sagen, dass das Boomerang Casino ein zuverlässiges und unterhaltsames Online-Casino ist, das sein Geld definitiv wert ist. Mit einer breiten Auswahl an Spielen, einer gültigen Lizenz und einem hervorragenden Kundenservice bietet das Casino ein rundum gelungenes Spielerlebnis. Wenn Sie also Lust auf ein spannendes und sicheres Glücksspielabenteuer haben, ist das Boomerang Casino definitiv einen Besuch wert.
https://boomerangcasino.one/
Добрый день, приятели! Желаю рассказать собственными эмоциями о казино unlim casino. Этот портал прямо поражает разнообразием проектов и неповторимой атмосферой риска! Отличная изображение, тутовые выплаты и заманчивые бонусы формируют игровой процесс неповторимым. Честная забава и повышенный класс безопасности — это то, какое заставляет меня возращаться повторно. Рекомендую каждому, тем ценит качественный отдых и крупные награды
Привет, приятели! Стремлюсь рассказать своими эмоциями о клубе azino777. Этот ресурс прямо поражает различием проектов и особенной энергией волнения! Великолепная визуализация, мгновенные вознаграждения и соблазнительные подарки формируют игровой процесс неизгладимым. Интегральная развлечение и высший класс защищенности — это то, какое вдохновляет меня возращаться снова и снова. Предлагаю каждому, тем ценит высококачественный отдыхание и массивные награды
Everything You Need to Know
2. Aviator Games: Test Your Flying Skills in this Exciting Challenge
3. Get Ready to Soar: Aviator Games for Thrill Seekers
4. Master the Sky: Aviator Games for Aviation Enthusiasts
5. Take Flight with Aviator Games: A High-Flying Adventure
6. Challenge Yourself with Aviator Games: Are You Ready to Take On the Sky?
7. The Sky’s the Limit: Aviator Games for Daredevils
8. Aviator Games: The Perfect Way to Experience the Thrill of Flying
9. Fly High with Aviator Games: An Exciting Journey Awaits
10. Unleash Your Inner Pilot: Aviator Games for Flying Enthusiasts
11. Reach New Heights with Aviator Games: The Sky Awaits
12. Aviator Games: A Test of Skill and Courage in the Sky
13. Take to the Skies with Aviator Games: A Thrilling Adventure Awaits
14. Aviator Games: Where Every Landing is a Victory
15. Ready for Takeoff: Aviator Games for the Brave and Bold
16. Conquer the Clouds with Aviator Games: A Challenge Like No Other
17. Aviator Games: Prepare for a High-Flying Experience
18. Fly Like a Pro with Aviator Games: The Sky’s the Limit
19. Aviator Games: The Ultimate Test for Aspiring Pilots
20. Soar to New Heights with Aviator Games: Are You Ready for the Challenge?
aviator slot aviator games .
Добрый день, приятели! Стремлюсь обмениваться своими эмоциями о зале лучшее онлайн казино. Этот сайт напросто поражает разнообразием проектов и уникальной обстановкой азарта! Отличная графика, мгновенные вознаграждения и привлекательные подарки формируют игровой процесс неизгладимым. Порядочная игра и повышенный степень секретности — таково то, которое мотивирует передвигает возвращаться еще раз. Советую каждому, кому дорожит качественный отдыхание и большие награды
Комплект тюнинга MERCEDES BENZ https://autoupgrade.by/
Der Boomerang Casino Code ist ein exklusiver Bonuscode, der es Spielern ermöglicht, besondere Angebote und Belohnungen im Boomerang Casino zu erhalten. Dieser Code kann verwendet werden, um Bonusgelder, Freispiele oder andere Vergünstigungen zu erhalten.
Um den Boomerang Casino Code zu nutzen, müssen Spieler einfach während des Einzahlungsvorgangs den Code eingeben. Sobald der Code akzeptiert wurde, wird der entsprechende Bonus automatisch dem Spielerkonto gutgeschrieben.
Der Boomerang Casino Code bietet Spielern die Möglichkeit, ihr Spielerlebnis im Casino zu verbessern und ihre Gewinnchancen zu erhöhen. Mit den zusätzlichen Bonusgeldern oder Freispielen können Spieler mehr Spiele ausprobieren und ihre Chancen auf einen großen Gewinn steigern.
Es ist jedoch wichtig zu beachten, dass jeder Boomerang Casino Code bestimmte Bedingungen und Umsatzanforderungen haben kann. Spieler sollten daher die Bonusbedingungen genau lesen, um sicherzustellen, dass sie die Vorgaben erfüllen und den Bonus optimal nutzen können.
Insgesamt ist der Boomerang Casino Code eine großartige Möglichkeit für Spieler, mehr aus ihrem Spiel herauszuholen und zusätzliche Vergünstigungen zu erhalten. Wer sein Glück im Boomerang Casino versuchen möchte, sollte daher nicht vergessen, den exklusiven Bonuscode zu nutzen und von den zusätzlichen Belohnungen zu profitieren.
https://boomerangcasino.one/
Das Zet Casino hat für das Jahr 2021 einen exklusiven Promo-Code veröffentlicht, der Spielern die Möglichkeit bietet, von großzügigen Boni und Angeboten zu profitieren. Der Code kann bei der Registrierung oder bei der Einzahlung in das Casino eingegeben werden und gewährt den Spielern zusätzliche Boni wie Freispiele oder Bonusguthaben.
Mit dem Zet Casino Promo-Code 2021 können Spieler ihre Gewinnchancen erhöhen und länger spielen, ohne dabei ihr eigenes Geld riskieren zu müssen. Dies stellt eine großartige Möglichkeit für neue Spieler dar, das Casino kennenzulernen und sich mit den verschiedenen Spielen vertraut zu machen.
Das Zet Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit dem Promo-Code können Spieler diese Spiele mit zusätzlichem Bonusguthaben entdecken und möglicherweise sogar den Jackpot knacken.
Es ist wichtig, den Promo-Code korrekt einzugeben, um sicherzustellen, dass man von den Angeboten profitieren kann. AuГџerdem sollten die Bonusbedingungen und -bedingungen genau gelesen werden, um sicherzustellen, dass man die Bedingungen erfГјllt und das Bonusguthaben erfolgreich in Echtgeld umwandeln kann.
Insgesamt bietet das Zet Casino Promo-Code 2021 eine großartige Möglichkeit, um noch mehr Spaß und Spannung beim Spielen zu erleben. Nutzen Sie den Code, um Ihre Gewinnchancen zu erhöhen und die Vielfalt der Spiele im Casino zu entdecken. Viel Glück und viel Spaß beim Spielen!
https://zetcasino.one/
Boomerang Casino ist ein Online-Casino, das in den letzten Jahren immer beliebter geworden ist. Viele Spieler schätzen die Vielfalt an Spielen, die hier angeboten werden, sowie den hervorragenden Kundenservice. Doch die Frage, die sich viele stellen, ist: Ist Boomerang Casino seriös?
Um diese Frage zu beantworten, lohnt es sich zunächst einen Blick auf die Lizenzierung des Casinos zu werfen. Boomerang Casino ist im Besitz einer Lizenz der Malta Gaming Authority, einer der renommiertesten Glücksspielbehörden der Welt. Diese Lizenz garantiert, dass das Casino strenge Auflagen erfüllt und regelmäßig überprüft wird, um sicherzustellen, dass faire Spielbedingungen gewährleistet sind.
DarГјber hinaus arbeitet Boomerang Casino mit namhaften Softwareanbietern zusammen, darunter NetEnt, Microgaming und Play’n GO. Diese Unternehmen sind bekannt fГјr ihre hochwertigen Spiele und garantieren ein sicheres und faires Spielerlebnis.
Auch in Sachen Kundenservice kann Boomerang Casino punkten. Der Support ist rund um die Uhr erreichbar und steht den Spielern bei Fragen und Problemen kompetent zur Seite. Zudem wird auf der Webseite transparent Гјber die Zahlungsmethoden und die Datenschutzrichtlinien informiert.
Zusammenfassend lässt sich sagen, dass Boomerang Casino als seriöser Anbieter betrachtet werden kann. Die Lizenzierung durch die Malta Gaming Authority, die Zusammenarbeit mit renommierten Softwareanbietern und der gute Kundenservice sprechen für das Casino. Spieler können sich hier also sicher und gut aufgehoben fühlen und ihrem Spielvergnügen unbesorgt nachgehen.
https://boomerangcasino.one/
Zet Casino ist ein beliebtes Online-Casino, das Spielern eine Vielzahl von Spielen und Unterhaltungsmöglichkeiten bietet. Eines der Highlights dieses Casinos ist das Zet Casino Forum, in dem Spieler sich austauschen, Tipps geben und Erfahrungen teilen können.
Das Zet Casino Forum ist eine großartige Möglichkeit, um mit anderen Spielern in Kontakt zu treten und sich über die neuesten Entwicklungen und Angebote des Casinos auszutauschen. Hier können Spieler ihre Lieblingsspiele diskutieren, Erfolge feiern und auch Fragen stellen, wenn sie Hilfe benötigen.
Das Forum ist in verschiedene Kategorien aufgeteilt, die es den Spielern erleichtern, sich zu bestimmten Themen zu äußern. Zum Beispiel gibt es Threads zu den neuesten Spielveröffentlichungen, Bonusangeboten, Zahlungsmethoden und vielem mehr.
Darüber hinaus bietet das Zet Casino Forum Spielern die Möglichkeit, an exklusiven Aktionen und Wettbewerben teilzunehmen, die nur für Forenmitglieder verfügbar sind. Dies kann eine großartige Gelegenheit sein, um zusätzliche Preise und Belohnungen zu gewinnen.
Das Zet Casino Forum ist auch eine gute Informationsquelle für alle, die mehr über das Online-Casino erfahren möchten. Hier finden Spieler Tutorials, Guides und Tipps, die ihnen helfen können, ihre Spielerfahrung zu verbessern und erfolgreicher zu sein.
Insgesamt ist das Zet Casino Forum eine großartige Ergänzung zu diesem beliebten Online-Casino und bietet eine interaktive Plattform für Spieler, um sich auszutauschen und zu vernetzen. Wer also auf der Suche nach einer Community ist, die die Leidenschaft für Glücksspiele teilt, sollte unbedingt einen Blick auf das Zet Casino Forum werfen.
https://zetcasino.one/
Индексация ссылок на сайте индекс ру
Zet Casino Erfahrungen: Alles, was Sie wissen mГјssen
Es ist keine leichte Aufgabe, das perfekte Online-Casino zu finden, das all Ihre Anforderungen erfüllt. Aber wenn Sie auf der Suche nach einem unterhaltsamen und sicheren Ort sind, um Ihre Lieblingsspiele zu spielen, dann könnte Zet Casino die richtige Wahl für Sie sein.
Zet Casino ist ein relativ neues Online-Casino, das 2018 gegründet wurde. Trotz seiner jungen Geschichte hat es sich bereits einen soliden Ruf in der Glücksspielbranche erarbeitet. Das Casino wird von Araxio Development N.V. betrieben und verfügt über eine Lizenz der Regierung von Curaçao.
Eine der ersten Dinge, die die Spieler an Zet Casino bemerken, ist die benutzerfreundliche Website und die groГџe Auswahl an Spielen. Mit Titeln von erstklassigen Anbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen, gibt es hier fГјr jeden Geschmack etwas zu entdecken. Von Spielautomaten Гјber Tischspiele bis hin zu Live-Casino-Spielen bietet Zet Casino ein beeindruckendes Portfolio an SpielmГ¶glichkeiten.
Ein weiterer großer Pluspunkt von Zet Casino sind die großzügigen Bonusangebote und Aktionen. Neue Spieler können sich über einen Willkommensbonus freuen, der Ihnen zusätzliches Geld und Freispiele für Ihre ersten Einzahlungen bietet. Darüber hinaus bietet das Casino regelmäßige Promotionen, Turniere und Treueprogramme, die es lohnenswert machen, regelmäßig zurückzukehren.
In Bezug auf die Sicherheit und den Kundenservice stehen die Erfahrungen der Spieler bei Zet Casino auch im Vordergrund. Die Website wird mit modernster SSL-Verschlüsselungstechnologie gesichert, um die Sicherheit Ihrer persönlichen Daten und finanziellen Transaktionen zu gewährleisten. Das Supportteam des Casinos ist rund um die Uhr per Live-Chat, E-Mail und Telefon erreichbar und steht Ihnen bei Fragen oder Problemen gerne zur Verfügung.
Insgesamt kann man sagen, dass die Erfahrungen mit Zet Casino größtenteils positiv ausfallen. Mit einer umfangreichen Spielauswahl, großzügigen Boni und einem zuverlässigen Kundenservice bietet das Casino eine unterhaltsame und sichere Spielerfahrung für alle Glücksspielfans. Wenn Sie also auf der Suche nach einem neuen Online-Casino sind, das all Ihre Wünsche erfüllen kann, dann sollten Sie Zet Casino auf jeden Fall eine Chance geben.
https://zetcasino.one/
Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Casino-Spielen anbietet. In diesem Artikel werden wir uns genauer mit den Boomerang Casino opinie, also den Meinungen und Erfahrungen der Spieler, beschäftigen.
Die Meinungen über Boomerang Casino sind geteilt. Einige Spieler loben die große Auswahl an Spielen, die ansprechende Grafik und die benutzerfreundliche Oberfläche der Website. Sie schätzen auch die vielfältigen Einzahlungs- und Auszahlungsmöglichkeiten sowie den zuverlässigen Kundenservice, der bei Fragen oder Problemen schnell zur Verfügung steht.
Andere Spieler hingegen bemängeln die Auszahlungsdauer bei Gewinnen, die teilweise länger als erwartet dauern kann. Einige berichten auch von technischen Problemen während des Spielens, die den Spielspaß beeinträchtigen können.
Insgesamt scheint Boomerang Casino eine solide Online-Glücksspielplattform zu sein, die sowohl positive als auch negative Bewertungen erhält. Wie bei den meisten Online-Casinos gilt es, verantwortungsbewusst zu spielen und sich über die Risiken des Glücksspiels im Klaren zu sein.
Es ist ratsam, sich vor der Registrierung bei einem Online-Casino über die Erfahrungen anderer Spieler zu informieren und sich gegebenenfalls auch über die Lizenzierung und Regulierung des Anbieters zu informieren. So kann man sicherstellen, dass man bei einem seriösen und zuverlässigen Anbieter spielt.
Letztendlich liegt es jedoch an jedem Einzelnen, ob er sich bei Boomerang Casino anmeldet und dort spielt. Man sollte stets auf sein Spielverhalten achten und im Zweifelsfall professionelle Hilfe in Anspruch nehmen. Denn GlГјcksspiel kann sГјchtig machen und sollte immer mit Vorsicht genossen werden.
https://boomerangcasino.one/
Zet Casino No Deposit: Ein Paradies fГјr Casinoliebhaber
Das Zet Casino ist eine beliebte Online-Spielothek, die eine breite Auswahl an spannenden Spielen und großzügigen Bonusangeboten bietet. Unter den vielen Angeboten sticht besonders der Zet Casino No Deposit Bonus hervor, der es Spielern ermöglicht, ohne vorherige Einzahlung echtes Geld zu gewinnen.
Der No Deposit Bonus ist eine großartige Möglichkeit für Spieler, das Casino risikofrei kennenzulernen und dabei die Chance zu haben, echtes Geld zu gewinnen. Beim Zet Casino erhalten neue Spieler einen Bonus von 10€ ohne vorherige Einzahlung, sobald sie sich registrieren. Dieser Bonus kann verwendet werden, um verschiedene Spiele zu spielen und Gewinne zu erzielen. Spieler müssen lediglich die Bonusbedingungen erfüllen, um ihre Gewinne auszahlen lassen zu können.
Das Zet Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele von bekannten Anbietern wie NetEnt, Microgaming und Betsoft. Mit dem No Deposit Bonus können Spieler diese Spiele ausprobieren und dabei die volle Casino-Erfahrung genießen, ohne eigenes Geld einzahlen zu müssen.
Um den Zet Casino No Deposit Bonus zu erhalten, müssen Spieler lediglich ein Konto im Casino erstellen und den Bonuscode eingeben, der auf der Website angegeben ist. Der Bonus wird dann automatisch gutgeschrieben und kann sofort verwendet werden. Spieler sollten jedoch darauf achten, die Bonusbedingungen zu lesen, um sicherzustellen, dass sie ihre Gewinne auszahlen lassen können.
Insgesamt ist der Zet Casino No Deposit Bonus eine großartige Möglichkeit für Spieler, die Casino-Spiele auszuprobieren und dabei echtes Geld zu gewinnen, ohne dabei eigenes Geld einzusetzen. Mit einer breiten Auswahl an Spielen und großzügigen Bonusangeboten ist das Zet Casino eine fantastische Wahl für alle Casinoliebhaber. Probieren Sie es aus und erleben Sie die Spannung und den Nervenkitzel des Casinos von zu Hause aus!
https://zetcasino.one/
Das Tipico Casino bietet seinen Kunden eine Vielzahl von Spielen, darunter auch die beliebten Leiter Spiele. Diese sorgen fГјr eine spannende und unterhaltsame Casino-Erfahrung und bieten die Chance auf hohe Gewinne.
Die Leiter Spiele im Tipico Casino funktionieren ähnlich wie die klassischen Slot-Spiele, jedoch mit einem zusätzlichen Element: einer Leiter, die den Gewinn multiplizieren kann. Je nach Spiel können Spieler die Leiter mit den richtigen Kombinationen von Symbolen erklimmen und dadurch ihre Gewinne deutlich erhöhen.
Die Leiter Spiele im Tipico Casino zeichnen sich durch ihre einfache Handhabung und ihre vielfältigen Gewinnmöglichkeiten aus. Mit nur wenigen Klicks können Spieler in die spannende Welt der Casino-Leitern eintauchen und ihr Glück versuchen.
Dank der modernen Technologie und der hochwertigen Grafiken im Tipico Casino sind die Leiter Spiele ein visuelles Erlebnis, das die Spieler in seinen Bann zieht. Zudem sorgen spannende Soundeffekte für eine authentische Casino-Atmosphäre, so dass man sich wie in einem echten Casino fühlt.
Die Leiter Spiele im Tipico Casino sind sowohl für Anfänger als auch für erfahrene Spieler geeignet. Dank der flexiblen Einsatzmöglichkeiten und der verschiedenen Spielvarianten findet jeder Spieler das passende Spiel für sich.
Insgesamt bieten die Leiter Spiele im Tipico Casino eine unterhaltsame und aufregende Casino-Erfahrung, die sowohl für Anfänger als auch für erfahrene Spieler geeignet ist. Mit spannenden Gewinnmöglichkeiten und hochwertigen Grafiken sorgen die Leiter Spiele für stundenlangen Spielspaß.
https://tipicocasino.one/
Im Zet Casino kГ¶nnen Spieler ihren SpielspaГџ noch weiter steigern, indem sie einen speziellen Promotionscode verwenden. Mit einem “zet casino promГіciГіs kГіdod” erhalten Spieler Zugang zu verschiedenen Bonusangeboten und Aktionen, die ihre Gewinnchancen erhГ¶hen und das Spielerlebnis noch aufregender machen.
Der Promotionscode kann auf der Website des Casinos oder durch spezielle Aktionen und Newsletter erhalten werden. Einmal eingegeben, können Spieler von zusätzlichen Einzahlungsboni, Freispielen, Cashback-Angeboten und vielen anderen Belohnungen profitieren.
Durch die Verwendung des “zet casino promГіciГіs kГіdod” kГ¶nnen Spieler ihre Bankroll erhГ¶hen und lГ¤nger spielen, ohne dabei ihr eigenes Geld zu riskieren. Dies ermГ¶glicht es ihnen, mehr Spiele zu genieГџen und ihre Gewinnchancen zu maximieren.
Das Zet Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit dem Promotionscode haben Spieler die Möglichkeit, alle diese Spiele mit zusätzlichen Boni zu spielen und noch mehr Spaß zu haben.
Also, wenn Sie auf der Suche nach einem aufregenden Casinoerlebnis sind, sollten Sie nicht zГ¶gern und sich Ihren “zet casino promГіciГіs kГіdod” sichern. Nutzen Sie die zahlreichen Bonusangebote und Aktionen, um Ihre Gewinnchancen zu maximieren und den Nervenkitzel des Casinos zu erleben. Viel GlГјck!
https://zetcasino.one/
Die Tipico Live Casino App ist eine beliebte und moderne Möglichkeit, um von überall aus auf das spannende Live Casino-Angebot von Tipico zuzugreifen. Mit dieser App können Nutzer bequem und flexibel spielen, ohne an einen bestimmten Ort gebunden zu sein.
Die Tipico Live Casino App bietet eine Vielzahl von Spielen und Tischen, an denen man gegen echte Dealer antreten kann. Egal ob Roulette, Blackjack, Poker oder Baccarat – fГјr jeden Geschmack ist etwas dabei. Die Live-Гњbertragung in HD-QualitГ¤t macht das Spielerlebnis noch realistischer und spannender.
Durch die App können Nutzer auch problemlos Ein- und Auszahlungen tätigen, den Kundenservice kontaktieren oder Bonusangebote nutzen. Die Bedienung ist einfach und intuitiv, sodass auch Anfänger sich schnell zurechtfinden können.
Ein weiterer Vorteil der Tipico Live Casino App ist die hohe Sicherheit und Zuverlässigkeit. Die App ist von der Malta Gaming Authority lizenziert und wird regelmäßig auf Fairness und Transparenz überprüft.
Insgesamt ist die Tipico Live Casino App eine empfehlenswerte Option fГјr alle, die gerne live gegen echte Dealer spielen und dabei flexibel sein mГ¶chten. Probieren Sie es aus und erleben Sie die Spannung und AtmosphГ¤re eines echten Casinos – ganz bequem auf Ihrem Smartphone oder Tablet.
https://tipicocasino.one/
1xslots telegram channel https://1xslots-telegram.com/
Мечтаете о захватывающем приключении на Байкале? Ищете идеальный тур, который запомнится на всю жизнь? Тогда FanatBaikala.ru – ваш надежный партнер в организации путешествий! Здесь вы найдете самые увлекательные предложения на тур в Байкал.
FanatBaikala.ru предлагает широкий выбор маршрутов, которые подходят как для любителей активного отдыха, так и для ценителей спокойного путешествия. От увлекательных экскурсий до пеших прогулок по живописным тропам – здесь каждый найдет что-то по душе.
Ищете тур в Иркутск на Байкал? FanatBaikala.ru поможет вам организовать ваше путешествие так, чтобы оно было максимально комфортным и запоминающимся. Не упустите возможность окунуться в удивительный мир Байкала с FanatBaikala.ru!
Zet Casino 30 – Was steckt dahinter?
Das Zet Casino 30 ist eine Online-GlГјcksspielseite, die sich auf Spielautomaten, Tischspiele und Live-Casino-Spiele spezialisiert hat. Es bietet eine breite Auswahl an Spielen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming, Betsoft und vielen anderen.
Ein besonderes Merkmal des Zet Casino 30 ist der großzügige Willkommensbonus, der neuen Spielern einen 100% Bonus auf ihre erste Einzahlung bis zu 500€ sowie 200 Freispiele bietet. Zusätzlich bietet das Casino regelmäßige Promotionen und Boni für bestehende Spieler, um deren Spielerlebnis noch spannender zu gestalten.
Das Zet Casino 30 zeichnet sich auch durch sein benutzerfreundliches Design und eine Vielzahl von Zahlungsmöglichkeiten aus, die es den Spielern leicht machen, Ein- und Auszahlungen zu tätigen. Der Kundenservice ist ebenfalls rund um die Uhr verfügbar und bietet professionelle Unterstützung bei allen Anliegen der Spieler.
Insgesamt bietet das Zet Casino 30 ein unterhaltsames und sicheres Spielerlebnis fГјr alle Casino-Enthusiasten. Mit einer breiten Auswahl an Spielen, groГџzГјgigen Boni und einem ausgezeichneten Kundenservice ist es definitiv eine gute Wahl fГјr alle, die auf der Suche nach einem erstklassigen Online-Casino sind.
https://zetcasino.one/
Индексация ссылок на сайте vindexe.ru
https://microbladingeyebrowsalon.com/
Tipico Casino App Chip – Alles was du wissen musst
Die Tipico Casino App ist eine beliebte Option für Glücksspielfans, die gerne von unterwegs aus spielen möchten. Die App ist sowohl für iOS als auch für Android-Geräte verfügbar und bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Dealer-Spiele.
Ein besonderes Feature der Tipico Casino App ist der sogenannte Chip. Dieser Chip dient als Währung innerhalb der App und kann für Einsätze bei den verschiedenen Spielen verwendet werden. Der Chip kann entweder mit Echtgeld gekauft oder durch das Spielen von bestimmten Spielen und das Erreichen von Zielen verdient werden.
Der Chip kann auch als Belohnung für regelmäßige Spieler vergeben werden und ermöglicht es diesen, länger zu spielen und größere Gewinne zu erzielen. Darüber hinaus gibt es auch regelmäßige Aktionen, bei denen Spieler zusätzliche Chips erhalten können.
Es ist jedoch wichtig zu beachten, dass der Chip nur innerhalb der Tipico Casino App verwendet werden kann und nicht gegen Echtgeld eingetauscht werden kann. Dennoch bietet er eine zusätzliche Möglichkeit, das Spielerlebnis zu verbessern und den Spaß am Spielen zu steigern.
Insgesamt ist der Chip in der Tipico Casino App eine spannende Ergänzung, die das Spielen noch aufregender macht. Wenn du also gerne von unterwegs aus spielst und auf der Suche nach einer neuen Casino-App bist, solltest du die Tipico Casino App mit dem Chip auf jeden Fall ausprobieren. Viel Spaß und viel Glück beim Spielen!
https://tipicocasino.one/
Das Zet Casino lockt seine Spieler mit lukrativen Bonusangeboten und Aktionen. Ein besonders attraktiver Bonus ist der Willkommensbonus für neue Spieler. Dieser umfasst nicht nur einen Einzahlungsbonus, sondern auch Freispiele für ausgewählte Spielautomaten.
Darüber hinaus bietet das Zet Casino regelmäßig verschiedene Boni für Bestandskunden an, wie zum Beispiel Reload-Boni, Cashback-Aktionen oder Freispiele. Diese Bonusangebote sorgen für zusätzliche Spannung und Unterhaltung beim Spielen im Casino.
Um von den Bonusangeboten profitieren zu können, müssen die Spieler bestimmte Umsatzbedingungen erfüllen. Diese sind in den Bonusbedingungen genau festgelegt und sollten vor Inanspruchnahme eines Bonus unbedingt gelesen werden.
Das Zet Casino legt großen Wert auf Fairness und Transparenz bei seinen Bonusangeboten. Spieler können sich sicher sein, dass sie hier seriöse und sichere Bonusangebote erhalten.
Insgesamt bietet das Zet Casino seinen Spielern eine Vielzahl von attraktiven Bonusangeboten, die das Spielerlebnis noch spannender machen. Wer also auf der Suche nach einem neuen Online-Casino mit interessanten Bonusangeboten ist, sollte das Zet Casino in Betracht ziehen.
https://zetcasino.one/
More Bonuses Obs download
Das Boomerang Casino: Ein einzigartiges Spielerlebnis
Das Boomerang Casino ist ein Online-Casino, das sich von anderen Anbietern in vielerlei Hinsicht abhebt. Mit seinem australischen Thema und einer breiten Auswahl an Spielen bietet es ein einzigartiges Spielerlebnis fГјr alle Casino-Fans.
Das Casino ist bekannt für seine großzügigen Boni und Promotionen, die es Spielern ermöglichen, mehr aus ihrem Geld zu machen. Von Willkommensboni über Freispiele bis hin zu wöchentlichen Aktionen gibt es hier immer etwas Neues zu entdecken.
Die Auswahl an Spielen im Boomerang Casino ist ebenfalls beeindruckend. Von klassischen Tischspielen wie Blackjack und Roulette Гјber eine Vielzahl von Spielautomaten bis hin zu Live-Casino-Spielen bietet das Casino fГјr jeden Geschmack etwas Passendes.
Ein weiterer Pluspunkt des Boomerang Casinos ist die benutzerfreundliche Website, die es Spielern ermöglicht, schnell und einfach zu ihren Lieblingsspielen zu gelangen. Darüber hinaus bietet das Casino eine Vielzahl von sicheren Zahlungsmethoden, um Ein- und Auszahlungen einfach und sicher zu gestalten.
Insgesamt bietet das Boomerang Casino ein unterhaltsames und spannendes Spielerlebnis fГјr alle, die gerne online spielen. Mit seinen groГџzГјgigen Boni, einer breiten Auswahl an Spielen und einer benutzerfreundlichen Website ist das Casino eine gute Wahl fГјr alle Casino-Fans. Wer also auf der Suche nach einem neuen Online-Casino ist, sollte definitiv einen Blick auf das Boomerang Casino werfen.
https://boomerangcasino.one/
web sollet
Zet Casino Free Spins: Spielen Sie kostenlos und gewinnen Sie groГџ
Wer liebt es nicht, kostenlos zu spielen und dabei die Chance zu haben, groß zu gewinnen? Mit Zet Casino Free Spins ist genau das möglich! Free Spins sind eine großartige Möglichkeit, um neue Spiele auszuprobieren, ohne dabei eigenes Geld einsetzen zu müssen. In diesem Artikel erfahren Sie alles, was Sie über Zet Casino Free Spins wissen müssen.
Zet Casino bietet eine Vielzahl von Free Spins für seine Spieler an. Diese können als Willkommensbonus für neue Spieler oder als regelmäßige Promotionen für bestehende Spieler angeboten werden. Die Free Spins können für bestimmte Slots oder Tischspiele verwendet werden und bieten die Möglichkeit, echtes Geld zu gewinnen, ohne eigenes Geld einzusetzen.
Um Free Spins zu erhalten, müssen Spieler bestimmte Bedingungen erfüllen. Dies kann die Registrierung eines neuen Kontos, eine erste Einzahlung oder die Teilnahme an einer bestimmten Promotion sein. Sobald die Bedingungen erfüllt sind, werden die Free Spins automatisch gutgeschrieben und können sofort verwendet werden.
Es ist wichtig zu beachten, dass Free Spins in der Regel an bestimmte Umsatzbedingungen gebunden sind. Dies bedeutet, dass Gewinne aus den Free Spins eine bestimmte Anzahl an Malen umgesetzt werden müssen, bevor sie ausgezahlt werden können. Es ist daher ratsam, die Geschäftsbedingungen der Free Spins sorgfältig zu lesen, um Missverständnisse zu vermeiden.
Zet Casino bietet eine Vielzahl von Free Spins für seine Spieler an, sodass für jeden etwas dabei ist. Egal, ob Sie ein erfahrener Spieler sind oder gerade erst anfangen, mit den Free Spins haben Sie die Möglichkeit, Ihr Glück zu versuchen und dabei viel Spaß zu haben. Nutzen Sie also die Gelegenheit und spielen Sie kostenlos bei Zet Casino!
https://zetcasino.one/
Source roblox executor
check my reference Technologies for trading on the stock exchange
Tipico Casino Trick
Das Tipico Casino bietet eine Vielzahl von Spielen und Möglichkeiten, um Geld zu gewinnen. Doch gibt es auch Tricks, um seine Chancen auf einen Gewinn zu erhöhen? In diesem Artikel werden einige Tipps und Tricks vorgestellt, um beim Tipico Casino erfolgreich zu sein.
1. Nutzen Sie die Willkommensboni: Das Tipico Casino bietet neuen Spielern großzügige Willkommensboni an. Nutzen Sie diese Boni, um Ihr Spielkapital zu erhöhen und Ihre Chancen auf einen Gewinn zu maximieren.
2. Setzen Sie sich ein Budget: Bevor Sie mit dem Spielen beginnen, legen Sie sich ein Budget fest und halten Sie sich daran. So vermeiden Sie, mehr Geld zu verlieren als Sie sich leisten können.
3. Spielen Sie nur bei seriösen Anbietern: Achten Sie darauf, dass das Tipico Casino eine gültige Glücksspiellizenz besitzt und seine Spiele regelmäßig von unabhängigen Prüfinstituten überprüft werden. Nur so können Sie sicher sein, dass die Spiele fair und transparent sind.
4. Setzen Sie auf Spiele mit niedrigem Hausvorteil: Manche Spiele im Tipico Casino haben einen geringeren Hausvorteil als andere. Setzen Sie auf Spiele wie Blackjack oder Video Poker, um Ihre Gewinnchancen zu maximieren.
5. Nutzen Sie Strategien: Viele Spiele im Tipico Casino erfordern eine gewisse Strategie, um erfolgreich zu sein. Informieren Sie sich Гјber die besten Strategien fГјr Ihr Lieblingsspiel und setzen Sie diese gezielt ein.
Insgesamt gibt es also einige Tricks und Tipps, um beim Tipico Casino erfolgreich zu sein. Doch vergessen Sie nicht, dass Glücksspiel immer mit einem gewissen Risiko verbunden ist. Spielen Sie verantwortungsbewusst und setzen Sie niemals mehr Geld ein, als Sie sich leisten können zu verlieren. Viel Spaß und viel Erfolg im Tipico Casino!
https://tipicocasino.one/
her comment is here roblox delta patch
Das Zet Casino PaynPlay bietet eine innovative Möglichkeit, um schnell und einfach in den Genuss von Online-Glücksspielen zu kommen. Mit dieser Zahlungsmethode benötigen Spieler kein separates Konto, um ihre Ein- und Auszahlungen zu tätigen. Stattdessen können sie einfach eine Einzahlung über ihren Bankaccount vornehmen und direkt mit dem Spielen beginnen.
Das Zet Casino PaynPlay ist besonders für Spieler geeignet, die keine Lust haben, lange Registrierungsprozesse durchlaufen zu müssen. Durch die Nutzung dieser Zahlungsmethode können sie einfach ihre Lieblingsspiele genießen, ohne sich um komplizierte Anmeldeverfahren kümmern zu müssen. Das spart nicht nur Zeit, sondern auch Nerven.
Darüber hinaus bietet das Zet Casino PaynPlay eine sichere und zuverlässige Möglichkeit, um Ein- und Auszahlungen zu tätigen. Durch die Verknüpfung mit dem Bankaccount der Spieler wird gewährleistet, dass Transaktionen schnell und sicher abgewickelt werden. So können sich Spieler voll und ganz auf ihr Spiel konzentrieren, ohne sich um Sicherheitsrisiken oder Verzögerungen bei ihren Zahlungen sorgen zu müssen.
Insgesamt bietet das Zet Casino PaynPlay eine bequeme und effiziente Möglichkeit, um Online-Glücksspiele zu genießen. Durch die innovative Zahlungsmethode können Spieler schnell und unkompliziert in den Genuss von spannenden Casinospielen kommen, ohne lange Wartezeiten oder bürokratische Hürden. Wer also auf der Suche nach einer einfachen und sicheren Lösung für seine Ein- und Auszahlungen ist, sollte das Zet Casino PaynPlay definitiv in Betracht ziehen.
https://zetcasino.one/
this link jaxx download
Der Boomerang.bet Casino No Deposit Bonus ist eine großartige Möglichkeit, um ohne eigenes Geld in einem Online-Casino zu spielen. Diese Art von Bonus wird in der Regel neuen Spielern angeboten, die sich neu anmelden und ein Konto erstellen. Der Bonus wird automatisch gutgeschrieben, ohne dass eine Einzahlung erforderlich ist.
Der Boomerang.bet Casino No Deposit Bonus kann in Form von Freispielen oder Bonusgeld angeboten werden. Freispiele können an bestimmten Spielautomaten verwendet werden, während Bonusgeld in verschiedenen Spielen eingesetzt werden kann. Spieler können mit diesem Bonus echte Gewinne erzielen, die sie dann auszahlen lassen können.
Es ist jedoch wichtig zu beachten, dass No Deposit Boni oft bestimmten Umsatzbedingungen unterliegen. Das bedeutet, dass Spieler das Bonusgeld oder die Gewinne aus den Freispielen eine bestimmte Anzahl von Malen umsetzen müssen, bevor sie eine Auszahlung beantragen können. Es ist daher ratsam, die Bonusbedingungen immer sorgfältig zu lesen, um Missverständnisse zu vermeiden.
Insgesamt bietet der Boomerang.bet Casino No Deposit Bonus eine tolle Möglichkeit, um das Online-Casino kennenzulernen und erste Erfahrungen zu sammeln, ohne dabei eigenes Geld riskieren zu müssen. Es lohnt sich also, nach diesen lukrativen Boni Ausschau zu halten und sie zu nutzen, um seine Gewinnchancen zu erhöhen.
https://boomerangcasino.one/
Zet Casino ist eine beliebte Online-GlГјcksspielseite, die eine Vielzahl von Spielen und Bonusangeboten fГјr ihre Spieler anbietet. In letzter Zeit haben sich jedoch einige Spieler beschwert und Гјberlegt, das Casino zu verklagen.
Die Beschwerden konzentrieren sich hauptsächlich um den Umgang mit Auszahlungen und Bonusbedingungen. Einige Spieler behaupten, dass das Casino ihre Gewinne nicht auszahlt oder die Auszahlungsprozesse unnötig verzögert. Andere fühlen sich von den Bonusbedingungen des Casinos getäuscht und unfair behandelt.
Einige Spieler haben daher beschlossen, rechtliche Schritte gegen Zet Casino einzuleiten. Der Prozess, ein Online-Casino zu verklagen, kann jedoch kompliziert sein und erfordert die UnterstГјtzung eines Anwalts, der sich auf Online-GlГјcksspielgesetze spezialisiert hat.
Es ist wichtig zu beachten, dass Online-Glücksspiel in vielen Ländern rechtlich geregelt ist und Spieler bestimmte Rechte haben. Wenn ein Casino gegen diese Gesetze verstößt oder Spieler unfair behandelt, können diese rechtliche Schritte einleiten.
Es bleibt abzuwarten, wie die Situation zwischen den betroffenen Spielern und Zet Casino gelöst wird. In der Zwischenzeit ist es wichtig, dass Spieler ihre Rechte kennen und bei Unstimmigkeiten mit einem Online-Casino angemessene Schritte unternehmen.
Insgesamt zeigt der Fall Zet Casino, wie wichtig es ist, verantwortungsbewusst mit Online-Glücksspiel umzugehen und sich über die Rechte und Pflichten der Spieler im Klaren zu sein. Das Verklagen eines Casinos sollte jedoch immer als letzten Ausweg betrachtet werden und nur dann in Erwägung gezogen werden, wenn alle anderen Möglichkeiten der Konfliktlösung ausgeschöpft sind.
https://zetcasino.one/
Boomerang Casino Freispiele
Im Boomerang Casino gibt es eine Vielzahl von Freispielen, die den Spielern zusätzliche Gewinnchancen bieten. Diese Freispiele können für bestimmte Spielautomaten oder Tischspiele verwendet werden und bieten die Möglichkeit, ohne zusätzliche Kosten zu spielen und echtes Geld zu gewinnen.
Die Freispiele im Boomerang Casino können auf verschiedene Arten erhalten werden. Einige werden als Willkommensbonus für neue Spieler angeboten, während andere als Belohnung für treue Kunden vergeben werden. Darüber hinaus gibt es regelmäßige Aktionen und Promotionen, bei denen Spieler Freispiele gewinnen können.
Um die Freispiele im Boomerang Casino zu nutzen, müssen die Spieler die jeweiligen Bedingungen beachten. Dies beinhaltet in der Regel bestimmte Umsatzanforderungen und eine begrenzte Gültigkeitsdauer. Es ist wichtig, diese Informationen sorgfältig zu lesen, um sicherzustellen, dass die Freispiele optimal genutzt werden können.
Die Freispiele im Boomerang Casino können eine großartige Möglichkeit sein, um das Spielerlebnis zu verbessern und die Gewinnchancen zu erhöhen. Mit einer breiten Auswahl an verschiedenen Spielen und regelmäßigen Aktionen gibt es immer neue Möglichkeiten, um Freispiele zu erhalten und den Spielspaß zu steigern.
Insgesamt bieten die Boomerang Casino Freispiele eine spannende Möglichkeit, um zusätzliche Gewinne zu erzielen und die Vielfalt der verfügbaren Spiele zu genießen. Mit etwas Glück und Geschick können die Spieler mit den Freispielen im Boomerang Casino große Gewinne erzielen und den Spaß am Spiel auf die nächste Stufe heben.
https://boomerangcasino.one/
Das m.zet Casino ist eine aufstrebende Online-GlГјcksspielplattform, die Spieler aus aller Welt mit einer Vielzahl von spannenden Spielen und groГџzГјgigen Bonusangeboten anlockt. Das Casino bietet eine benutzerfreundliche Website, die es einfach macht, sich anzumelden, zu spielen und Gewinne abzuheben.
Die Spielauswahl im m.zet Casino umfasst beliebte Klassiker wie Spielautomaten, Roulette, Blackjack und Video Poker. Darüber hinaus bietet das Casino auch Live-Dealer-Spiele an, bei denen Spieler gegen echte Croupiers antreten können. Die Spiele werden von führenden Softwareanbietern wie NetEnt, Microgaming und Evolution Gaming bereitgestellt, was für eine erstklassige Spielerfahrung sorgt.
Ein weiterer großer Pluspunkt des m.zet Casinos sind die großzügigen Bonusangebote, die sowohl neuen als auch bestehenden Spielern zur Verfügung stehen. Zu den Angeboten gehören Willkommensboni, Einzahlungsboni, Freispiele und Treueprämien. Diese Boni bieten Spielern die Möglichkeit, ihr Guthaben zu maximieren und mehr Gewinne zu erzielen.
Das m.zet Casino legt großen Wert auf Sicherheit und Fairness und verfügt über eine gültige Glücksspiellizenz. Die Website ist SSL-verschlüsselt, um sicherzustellen, dass persönliche und finanzielle Daten der Spieler geschützt sind. Darüber hinaus werden alle Spiele regelmäßig von unabhängigen Prüfstellen überprüft, um sicherzustellen, dass sie fair und zufällig sind.
Insgesamt ist das m.zet Casino eine hervorragende Wahl fГјr Spieler, die auf der Suche nach einer sicheren und unterhaltsamen Online-GlГјcksspielplattform sind. Mit einer Vielzahl von Spielen, groГџzГјgigen Bonusangeboten und einem hohen MaГџ an Sicherheit und Fairness ist das Casino definitiv einen Besuch wert.
https://zetcasino.one/
Online Casino Boomerang: Ein neuartiges Spielerlebnis
In der Welt der Online-Casinos gibt es immer wieder innovative Neuerungen und spannende Konzepte, die die Spieler begeistern. Eines dieser neuen Konzepte ist das sogenannte “Boomerang Casino”, das sich durch einige besondere Features von herkГ¶mmlichen Online-Casinos unterscheidet.
Das Boomerang Casino zeichnet sich vor allem durch sein einzigartiges Belohnungssystem aus, das auf dem Prinzip des australischen Wurfgeräts, dem Boomerang, basiert. Ähnlich wie ein Boomerang, das nach dem Wurf zu seinem Ursprungsort zurückkehrt, erhalten die Spieler im Boomerang Casino regelmäßige Belohnungen und Boni, die sie immer wieder zum Spielen zurückbringen.
Ein weiteres Highlight des Boomerang Casinos ist das VIP-Programm, das auf die individuellen Bedürfnisse und Vorlieben der Spieler zugeschnitten ist. Je mehr ein Spieler im Casino spielt, desto höher steigt er im VIP-Programm auf und kann so von exklusiven Angeboten und Vorteilen profitieren.
DarГјber hinaus bietet das Boomerang Casino eine Vielzahl von spannenden Spielen aus den Bereichen Slots, Tischspiele und Live-Casino an, die fГјr Abwechslung und SpaГџ sorgen. Die Spiele werden von renommierten Softwareanbietern entwickelt und garantieren ein sicheres und faires Spielerlebnis.
Ein weiterer großer Vorteil des Boomerang Casinos ist die Möglichkeit, auch unterwegs von jedem Ort aus zu spielen. Die mobile Version der Plattform ist benutzerfreundlich gestaltet und ermöglicht es den Spielern, ihre Lieblingsspiele auch auf dem Smartphone oder Tablet zu genießen.
Insgesamt bietet das Boomerang Casino eine innovative und spannende Alternative zu herkömmlichen Online-Casinos und überzeugt mit seinem einzigartigen Belohnungssystem, dem maßgeschneiderten VIP-Programm und der großen Auswahl an Spielen. Wer also auf der Suche nach einem neuen und aufregenden Spielerlebnis ist, sollte das Boomerang Casino unbedingt ausprobieren.
https://boomerangcasino.one/
Boomerang Casino Erfahrung
Das Boomerang Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen fГјr seine Spieler anbietet. In diesem Artikel werden wir die Erfahrung von Spielern, die das Boomerang Casino ausprobiert haben, genauer betrachten.
Viele Spieler loben die große Auswahl an Spielen, die im Boomerang Casino verfügbar sind. Von klassischen Slots bis hin zu Live-Casino-Spielen und Jackpot-Slots ist für jeden Geschmack etwas dabei. Die Spiele werden von renommierten Software-Anbietern wie NetEnt, Microgaming und Play’n GO bereitgestellt, was für hohe Qualität und unterhaltsame Spielabläufe sorgt.
Ein weiterer positiver Aspekt des Boomerang Casinos sind die attraktiven Bonusangebote für Neukunden und bestehende Spieler. Registrieren sich neue Spieler im Casino, können sie von großzügigen Willkommensboni und Freispielen profitieren. Auch regelmäßige Aktionen und Turniere sorgen für zusätzliche Spannung und die Chance auf lukrative Gewinne.
Die Ein- und Auszahlungsmöglichkeiten im Boomerang Casino sind vielseitig und sicher. Spieler können aus einer breiten Palette von Zahlungsmethoden wie Kreditkarten, E-Wallets und Banküberweisungen wählen. Die Transaktionen werden schnell und zuverlässig abgewickelt, sodass Spieler unkompliziert Gelder einzahlen und abheben können.
Einige Spieler haben jedoch auch kritische Punkte bezüglich des Kundensupports im Boomerang Casino geäußert. Manche bemängeln die Antwortzeiten des Supports, während andere Probleme mit der Kommunikation hatten. Es scheint, dass hier noch Verbesserungspotenzial besteht, um den Kundenservice zu optimieren.
Alles in allem zeigt sich das Boomerang Casino als solides und unterhaltsames Online-Casino mit einer Vielzahl von Spielen und attraktiven Bonusangeboten. Die Erfahrungen der Spieler sind größtenteils positiv, wobei vor allem die große Auswahl an Spielen und die sicheren Zahlungsmöglichkeiten gelobt werden. Mit einigen Optimierungen im Kundenservice könnte das Boomerang Casino noch weiter an Beliebtheit gewinnen.
https://boomerangcasino.one/
Can you tell us more about this? I’d like to find out more details.
https://controlc.com/1f785e9f
Website design World of Warcraft game server – World of Warcraft website template, Website design Lineage 2 game server
Zet Casino Bonus Code: Das Beste aus Ihrem Casinobesuch herausholen
Wenn Sie auf der Suche nach einem erstklassigen Online Casino sind, dann ist das Zet Casino definitiv einen Besuch wert. Mit einer Vielzahl von hochwertigen Spielen, groГџzГјgigen Boni und einem professionellen Kundenservice bietet das Zet Casino alles, was das Spielerherz begehrt. Doch um das Beste aus Ihrem Casinobesuch herauszuholen, sollten Sie unbedingt den Zet Casino Bonus Code nutzen.
Mit dem Zet Casino Bonus Code haben Sie die Möglichkeit, Ihr Startguthaben zu maximieren und von zusätzlichen Freispielen zu profitieren. Egal, ob Sie ein erfahrener Spieler sind oder gerade erst in die Welt des Online Glücksspiels einsteigen – mit dem Bonus Code von Zet Casino können Sie Ihre Gewinnchancen deutlich erhöhen.
Um den Zet Casino Bonus Code zu nutzen, müssen Sie sich lediglich auf der Website des Casinos anmelden und den Code bei Ihrer Einzahlung eingeben. Sobald Sie dies getan haben, wird Ihr Bonus automatisch aktiviert und Sie können sofort mit dem Spielen beginnen. Vergessen Sie nicht, die Bonusbedingungen zu lesen, um sicherzustellen, dass Sie alle Voraussetzungen erfüllen, um Ihre Gewinne auszahlen zu können.
Neben dem großzügigen Willkommensbonus bietet das Zet Casino auch regelmäßig attraktive Promotionen und Aktionen für seine Spieler an. Halten Sie daher immer die Augen offen, um keine der lukrativen Angebote zu verpassen.
Insgesamt ist der Zet Casino Bonus Code eine großartige Möglichkeit, um das Beste aus Ihrem Casinobesuch herauszuholen. Nutzen Sie diese Chance, um Ihre Gewinnchancen zu steigern und noch mehr Spaß beim Spielen zu haben. Viel Glück und viel Spaß im Zet Casino!
https://zetcasino.one/
Lineage 2 website template – CS:GO open case website template, Website design case opening
шаблоны сайта L2 – Lineage 2 website theme creation, создание сайта Lineage 2
создание сайта опен кейс – разработка сайта линейдж 2, шаблоны сайта L2
ремонт автомагнитолы
Google Tipico Casino Bewertung
Tipico ist ein beliebter Buchmacher und Online-Casino-Anbieter, der eine Vielzahl von Glücksspielen für seine Kunden anbietet. Wenn Sie nach einer seriösen und vertrauenswürdigen Online-Casino-Plattform suchen, sollten Sie unbedingt eine Bewertung von Tipico Casino durchführen.
Eine einfache MГ¶glichkeit, Informationen Гјber Tipico Casino zu erhalten, ist die Verwendung von Google. Indem Sie einfach den Suchbegriff “Tipico Casino Bewertung” in die Suchleiste eingeben, erhalten Sie eine Vielzahl von Ergebnissen, die Ihnen helfen kГ¶nnen, mehr Гјber dieses Online-Casino zu erfahren.
In den Google-Bewertungen finden Sie Informationen über die Benutzererfahrung, die angebotenen Spiele, die Sicherheit und die Zuverlässigkeit des Casinos. Auf diese Weise können Sie eine fundierte Entscheidung treffen, ob Tipico Casino für Sie geeignet ist.
Es ist wichtig, sich bewusst zu machen, dass es bei Online-Casinos immer Risiken geben kann. Daher ist es ratsam, sich grГјndlich zu informieren und sicherzustellen, dass Sie bei einem vertrauenswГјrdigen Anbieter spielen.
Durch die Nutzung von Google können Sie eine objektive und umfassende Bewertung von Tipico Casino erhalten, die Ihnen bei der Entscheidung helfen kann, ob dieses Casino für Sie das richtige ist. Also zögern Sie nicht, eine Suche durchzuführen und die Bewertungen von anderen Spielern zu lesen, um ein besseres Bild von Tipico Casino zu bekommen.
https://tipicocasino.one/
шаблоны сайта L2 – case opening website templates, WoW website development
дизайн сайта вов – шаблон сайта вов, дизайн сайта Л2
Zet Casino Paysafecard
Zet Casino ist ein beliebtes Online-Casino, das Spielern eine Vielzahl von Spielen und Zahlungsmöglichkeiten bietet. Eine der beliebtesten Zahlungsmethoden bei Zet Casino ist die Paysafecard. Paysafecard ist eine prepaid Zahlungsmethode, bei der Spieler Gutscheine kaufen und diese dann online als Zahlungsmittel verwenden können.
Die Paysafecard bietet Spielern eine sichere und anonyme Möglichkeit, Geld auf ihr Zet Casino Konto einzuzahlen. Spieler können Paysafecards in verschiedenen Werten kaufen, je nach ihren Bedürfnissen. Sobald ein Spieler einen Paysafecard-Gutschein gekauft hat, kann er den Code einfach eingeben und das Geld wird sofort auf sein Konto gutgeschrieben.
Einer der Vorteile der Paysafecard ist die Sicherheit, die sie bietet. Da Spieler keine persönlichen Daten angeben müssen, um eine Paysafecard zu nutzen, sind ihre Transaktionen anonym und sicher. Spieler können also beruhigt sein, dass ihre finanziellen Informationen geschützt sind.
Zusätzlich ist die Paysafecard auch sehr bequem zu nutzen. Spieler müssen einfach den Code eingeben und schon ist das Geld auf ihrem Konto verfügbar. Es gibt keine Notwendigkeit, Bankdaten oder Kreditkarteninformationen anzugeben, was die Paysafecard zu einer einfachen und unkomplizierten Zahlungsmethode macht.
Zet Casino bietet seinen Spielern die Möglichkeit, mit Paysafecard zu bezahlen und somit das Spielerlebnis noch angenehmer zu gestalten. Wenn Sie also auf der Suche nach einer sicheren, anonymen und bequemen Zahlungsmethode sind, dann ist die Paysafecard die richtige Wahl für Sie. Besuchen Sie noch heute Zet Casino und erleben Sie die Welt des Online-Glücksspiels auf eine neue und aufregende Weise!
https://zetcasino.one/
86. Клининг Челябинск специализируется на уборке квартир перед проживанием новых собственников, включая мойку полов, окон, стен, потолков, уборку кухни, санузла, мебели, устранение пятен, запахов и другие работы для создания чистого и комфортного жилья.
Клининг Челябинск .
open case website template – CS:GO case opening website themes, разработка сайта линейдж 2
Immer mehr Online-Casinos setzen auf eine schnelle und einfache Verifizierung der Spieler, um ein sicheres und verantwortungsvolles Spielumfeld zu gewährleisten. Ein Casino, das sich besonders durch seine effiziente Verifizierung auszeichnet, ist das Boomerang Casino.
Die Verifizierung der Spieler ist ein wichtiger Schritt, um die Identität und Volljährigkeit der Teilnehmer zu überprüfen. Dies dient nicht nur dem Schutz vor möglichen Betrugsfällen, sondern auch der Einhaltung gesetzlicher Vorschriften im Glücksspielbereich.
Das Boomerang Casino legt großen Wert auf eine einfache und transparente Verifizierung seiner Spieler. Nach der Registrierung müssen die Spieler lediglich einige persönliche Informationen angeben und gegebenenfalls bestimmte Dokumente hochladen, um ihre Identität zu bestätigen. Das gesamte Verifizierungsverfahren wird schnell und unkompliziert durchgeführt, sodass die Spieler schnell mit dem Spielen beginnen können.
Durch die effiziente Verifizierung stellt das Boomerang Casino sicher, dass nur volljährige Spieler Zugang zu seinem Angebot haben. Zudem sorgt die Überprüfung der Identität dafür, dass mögliche betrügerische Aktivitäten frühzeitig erkannt und verhindert werden. Dies schafft ein sicheres Spielumfeld für alle Teilnehmer und trägt dazu bei, das Vertrauen der Spieler in das Casino zu stärken.
Insgesamt bietet das Boomerang Casino eine herausragende Verifizierungserfahrung für seine Spieler. Durch den schnellen und einfachen Prozess können die Teilnehmer sicher sein, dass ihre persönlichen Daten geschützt und ihr Spielvergnügen nicht durch aufwendige Verifizierungsmaßnahmen beeinträchtigt wird. Ein weiterer Grund, warum sich das Boomerang Casino als beliebte Wahl für Spieler auf der Suche nach einem seriösen und verlässlichen Online-Casino etabliert hat.
https://boomerangcasino.one/
разработка сайта Lineage 2 – опен кейс шаблон сайта, создание сайта линейдж 2
Zet Casino verklagen: Was sind die GrГјnde?
In den letzten Wochen haben sich einige Spieler darüber beschwert, dass Zet Casino ihre Gewinne nicht ausgezahlt hat. Einige behaupten sogar, dass sie überhaupt nicht in der Lage waren, ihre Gewinne abzuheben. Angesichts dieser Beschwerden fragen sich viele Spieler, ob es möglich ist, Zet Casino zu verklagen.
Zunächst einmal ist es wichtig zu verstehen, dass Glücksspielunternehmen wie Zet Casino bestimmte Regeln und Vorschriften einhalten müssen, um ihre Lizenz zu behalten. Dies beinhaltet die Verpflichtung, die Gewinne der Spieler zeitnah und korrekt auszuzahlen. Wenn ein Spieler also berechtigte Gründe hat zu glauben, dass Zet Casino gegen diese Regeln verstoßen hat, könnte eine Klage eine mögliche Lösung sein.
Ein weiterer Grund, warum Spieler erwägen könnten, Zet Casino zu verklagen, sind irreführende Werbeaktionen oder missbräuchliche Geschäftspraktiken. Wenn ein Spieler das Gefühl hat, dass er absichtlich getäuscht oder unfair behandelt wurde, hat er das Recht, rechtliche Schritte einzuleiten.
Es ist jedoch wichtig zu beachten, dass eine Klage gegen ein Online-Casino ein langwieriger und kostspieliger Prozess sein kann. Bevor man sich für eine Klage entscheidet, ist es ratsam, zuerst andere Möglichkeiten wie die Kontaktaufnahme mit dem Kundensupport oder die Einreichung einer Beschwerde bei der Glücksspielbehörde in Betracht zu ziehen.
Insgesamt ist es wichtig, als Spieler seine Rechte zu kennen und zu verteidigen. Wenn man der Meinung ist, dass man von Zet Casino unfair behandelt wurde, sollte man alle verfügbaren Optionen in Betracht ziehen, um eine gerechte Lösung zu finden.
https://zetcasino.one/
Boomerang Casino Code: Ein Blick in die Welt der Online-GlГјcksspiel-Boni
Online-Glücksspiel wird immer beliebter, und viele Spieler suchen nach Möglichkeiten, ihre Gewinne zu maximieren und ihr Spielerlebnis zu verbessern. Einer der Wege, wie sie das tun können, ist die Verwendung von Casino-Codes, die ihnen Zugang zu verschiedenen Boni und Promotionen verschaffen. Einer dieser Codes, der derzeit viel Aufmerksamkeit auf sich zieht, ist der Boomerang Casino Code.
Der Boomerang Casino Code ist ein spezieller Bonuscode, der es Spielern ermöglicht, zusätzliche Belohnungen und Vergünstigungen zu erhalten, wenn sie in diesem bestimmten Online-Casino spielen. Dieser Code kann in der Regel bei der Registrierung oder Einzahlung eingegeben werden, um den entsprechenden Bonus zu aktivieren. Die Art der Belohnungen, die Spieler durch die Verwendung dieses Codes erhalten können, variiert von Casino zu Casino, aber sie können alles von Freispielen über Einzahlungsboni bis hin zu Cashback-Angeboten umfassen.
Der Boomerang Casino Code wurde entwickelt, um Spielern einen Anreiz zu bieten, in diesem Casino zu spielen und treue Kunden zu belohnen. Indem sie diesen Code verwenden, können Spieler ihre Gewinnchancen verbessern und gleichzeitig ihr Spielvergnügen steigern. Darüber hinaus kann die Verwendung des Codes auch eine großartige Möglichkeit sein, das Casino zu erkunden und neue Spiele auszuprobieren, ohne dabei zusätzliches Geld ausgeben zu müssen.
Es ist jedoch wichtig zu beachten, dass Casino-Codes wie der Boomerang Casino Code in der Regel bestimmten Bedingungen und Konditionen unterliegen. Bevor man einen solchen Code verwendet, sollte man sich daher unbedingt die entsprechenden Geschäftsbedingungen durchlesen, um sicherzustellen, dass man die Regeln versteht und keine unangenehmen Überraschungen erlebt.
Insgesamt kann der Boomerang Casino Code eine großartige Möglichkeit sein, das Spielerlebnis zu verbessern und zusätzliche Belohnungen zu erhalten. Indem man diesen Code nutzt, können Spieler ihre Gewinnchancen steigern und gleichzeitig neue Spiele entdecken. Wenn Sie also auf der Suche nach einem Casino-Code sind, der Ihnen das Beste aus Ihrem Online-Glücksspiel-Erlebnis bietet, könnte der Boomerang Casino Code genau das Richtige für Sie sein.
https://boomerangcasino.one/
Promo Code Zet Casino: Profitieren Sie jetzt von tollen Rabatten
Zet Casino ist eines der beliebtesten Online-Casinos im deutschen Raum und überzeugt seine Kunden nicht nur mit einer großen Auswahl an Spielen, sondern auch mit attraktiven Bonusangeboten. Eine besonders begehrte Möglichkeit, von zusätzlichen Vergünstigungen zu profitieren, ist die Verwendung eines Promo Codes.
Ein Promo Code ist ein spezieller Code, den Sie bei der Registrierung auf der Website von Zet Casino eingeben können, um von verschiedenen Aktionen zu profitieren. Dies kann beispielsweise ein zusätzliches Startguthaben, Freispiele oder Cashback-Angebote sein. Mit einem Promo Code können Sie also Ihr Spielerlebnis bei Zet Casino noch spannender gestalten und gleichzeitig Ihr Guthaben aufbessern.
Um einen Promo Code bei Zet Casino einzulösen, müssen Sie sich einfach auf der Website anmelden und den Code im entsprechenden Feld angeben. Die genauen Bedingungen und Vorteile des Codes können je nach Aktion variieren, daher sollten Sie sich vorher über die aktuell gültigen Promo Codes informieren.
Ein guter Tipp ist es, regelmäßig die Website von Zet Casino zu besuchen oder den Newsletter zu abonnieren, um über aktuelle Aktionen informiert zu bleiben. So verpassen Sie garantiert keinen lukrativen Promo Code und können Ihr Spielerlebnis bei Zet Casino optimal ausnutzen.
Nutzen Sie also jetzt die Möglichkeit, mit einem Promo Code bei Zet Casino von tollen Rabatten und Vergünstigungen zu profitieren und erleben Sie spannende Stunden voller Spaß und Adrenalin. Viel Glück beim Spielen!
https://zetcasino.one/
Immer mehr Menschen nutzen Online-Casinos, um ihr Glück beim Glücksspiel zu versuchen. Dabei ist es jedoch wichtig, ein seriöses und vertrauenswürdiges Casino auszuwählen, um sicherzustellen, dass die persönlichen Daten und das eingezahlte Geld geschützt sind.
Ein Casino, das in den letzten Jahren besonders positiv aufgefallen ist, ist das Boomerang Casino. Auf der Bewertungsplattform Trustpilot hat das Casino eine Vielzahl von positiven Bewertungen erhalten, die seine Seriosität und Zuverlässigkeit unterstreichen.
Die Benutzer loben vor allem die Vielfalt der Spiele, die Benutzerfreundlichkeit der Webseite sowie den kompetenten Kundenservice. Viele Spieler betonen auch die schnellen Auszahlungen und die fairen Gewinnchancen im Boomerang Casino.
Ein großer Pluspunkt ist zudem, dass das Casino über eine gültige Glücksspiellizenz verfügt, die von einer renommierten Regulierungsbehörde ausgestellt wurde. Dadurch können die Spieler sicher sein, dass das Boomerang Casino strengen Auflagen und Regularien unterliegt und somit ein faires Spiel gewährleistet ist.
Insgesamt lässt sich sagen, dass das Boomerang Casino auf Trustpilot einen sehr guten Ruf genießt und sich als vertrauenswürdiger Anbieter im Bereich Online-Glücksspiel etabliert hat. Spieler, die auf der Suche nach einem seriösen Casino sind, sollten sich definitiv das Boomerang Casino genauer anschauen.
https://boomerangcasino.one/
Die Zet Casino App – Das ultimative Spielerlebnis direkt auf Ihrem Smartphone
Im Zeitalter der Digitalisierung ist es auch in der Welt des Glücksspiels längst nichts Neues mehr, dass immer mehr Online Casinos ihren Kunden die Möglichkeit bieten, ihre Lieblingsspiele auch mobil von unterwegs aus zu genießen. Eine dieser innovativen Apps ist die Zet Casino App, die es Spielern ermöglicht, ihr Casino-Erlebnis auch auf ihren Smartphones und Tablets zu erleben.
Die Zet Casino App bietet eine Vielzahl von spannenden Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele. Egal ob Sie ein Fan von traditionellen Spielautomaten sind oder lieber Roulette, Blackjack oder Poker spielen – mit der Zet Casino App haben Sie all diese Optionen immer griffbereit. Das Beste daran: Die App wurde speziell fГјr mobile GerГ¤te optimiert, um ein reibungsloses Spielerlebnis auf kleineren Bildschirmen zu gewГ¤hrleisten.
Doch nicht nur die Auswahl an Spielen macht die Zet Casino App so attraktiv, auch die Nutzerfreundlichkeit spielt eine groГџe Rolle. Die App ist benutzerfreundlich gestaltet und bietet eine intuitive Navigation, damit Sie sich schnell und einfach zurechtfinden. Zudem kГ¶nnen Sie bequem Ein- und Auszahlungen tГ¤tigen, den Kundendienst kontaktieren und von Bonusangeboten profitieren – alles direkt Гјber die App.
Ein weiterer Vorteil der Zet Casino App ist die Möglichkeit, die Spiele auch im Demomodus zu spielen. So können Sie neue Spiele ausprobieren, ohne dabei echtes Geld setzen zu müssen. Dadurch haben Sie die Möglichkeit, sich mit den Regeln und Funktionen vertraut zu machen, bevor Sie um echtes Geld spielen.
Insgesamt bietet die Zet Casino App ein herausragendes Spielerlebnis, das sich nicht hinter dem SpielspaГџ am PC verstecken muss. Egal ob Sie auf Ihrem tГ¤glichen Arbeitsweg, im Park oder auf Reisen sind – mit der Zet Casino App haben Sie Ihr Lieblingscasino immer dabei. Probieren Sie es aus und tauchen Sie ein in die aufregende Welt des Online-GlГјcksspiels – ganz bequem auf Ihrem Smartphone oder Tablet.
https://zetcasino.one/
Der Boomerang Casino Bonus ist eine beliebte Art von Bonus, die von Online-Casinos angeboten wird, um neue Spieler anzulocken und bestehende Spieler zu belohnen. Der Name stammt vom Boomerang, einem australischen Wurfinstrument, das zu seinem Werfer zurГјckkehrt – Г¤hnlich wie der einzigartige und attraktive Bonus es den Spielern ermГ¶glicht, mehr zu gewinnen und ihr Spielerlebnis zu verbessern.
Der Boomerang Casino Bonus funktioniert oft ähnlich wie ein herkömmlicher Willkommensbonus, bei dem Spieler Bonusgelder oder Freispiele erhalten, wenn sie sich im Casino anmelden und eine Einzahlung tätigen. Der Unterschied besteht jedoch darin, dass dieser Bonus in regelmäßigen Abständen zurückkehrt, ähnlich wie der Boomerang nach seinem Wurf.
Ein typisches Beispiel für einen Boomerang Bonus könnte monatlich sein, bei dem Spieler jedes Mal, wenn sie eine Einzahlung tätigen, einen festen Prozentsatz oder eine feste Menge an Bonusgeldern erhalten. Dies kann dazu beitragen, dass Spieler regelmäßig im Casino spielen und Spaß haben, da sie immer wieder belohnt werden.
Ein weiterer Vorteil des Boomerang Casino Bonus ist, dass er oft mit zusätzlichen Aktionen oder Sonderangeboten verbunden ist, die den Spielern noch mehr Vorteile bringen können. Dies kann beispielsweise zusätzliche Freispiele an bestimmten Spielautomaten, Eintrittskarten für exklusive Turniere oder spezielle Cashback-Angebote umfassen.
Insgesamt ist der Boomerang Casino Bonus eine interessante und lukrative Möglichkeit, um Spieler bei Laune zu halten und sie für ihre Treue zu belohnen. Es ist wichtig, die Bedingungen und Konditionen des Bonus zu überprüfen, um sicherzustellen, dass er den eigenen Spielvorlieben entspricht und keine versteckten Fallen beinhaltet. Wenn dies gewährleistet ist, kann der Boomerang Casino Bonus eine spannende Ergänzung zum Spielerlebnis in Online-Casinos sein.
https://boomerangcasino.one/
Das Tipico Casino bietet eine Vielzahl von unterschiedlichen Spielen für jeden Geschmack an. Egal ob Slots, Tischspiele oder Live-Casino – hier wird jeder fündig. Aber wussten Sie schon, dass man im Tipico Casino bereits ab 5 Cent spielen kann?
Ja, richtig gelesen! Im Tipico Casino können Sie bereits mit einem Einsatz von nur 5 Cent an den verschiedenen Spielautomaten Ihr Glück versuchen. Das ist besonders für Einsteiger oder vorsichtige Spieler sehr attraktiv, da man mit einem geringen Einsatz die Chance hat, tolle Gewinne zu erzielen.
Die Auswahl an Spielen, bei denen man mit 5 Cent spielen kann, ist groß. Von klassischen Slots bis hin zu modernen Video-Slots ist für jeden etwas dabei. Auch progressive Jackpot-Slots, bei denen man mit etwas Glück riesige Gewinne abräumen kann, stehen zur Verfügung.
Aber nicht nur bei den Spielautomaten kann man mit 5 Cent spielen, auch bei verschiedenen Tischspielen wie Roulette oder Blackjack ist es möglich, mit einem kleinen Einsatz dabei zu sein. So können auch Spieler mit kleinerem Budget die Spannung und den Nervenkitzel eines Casinos erleben.
Das Tipico Casino zeichnet sich nicht nur durch seine Vielfalt an Spielen aus, sondern auch durch seine benutzerfreundliche Plattform und den professionellen Kundenservice. Ein- und Auszahlungen können sicher und bequem über verschiedene Zahlungsmethoden getätigt werden, sodass man sich ganz auf das Spiel konzentrieren kann.
Also, wenn Sie Lust auf spannende Casino-Spiele haben, aber nicht gleich große Summen investieren möchten, dann ist das Tipico Casino mit seinen 5 Cent Spielen genau das Richtige für Sie. Probieren Sie es doch einfach mal aus und erleben Sie die aufregende Welt des Casinos!
https://tipicocasino.one/
Zet Casino ist eine beliebte Online-Casino-Plattform, die eine Vielzahl von Spielen und Unterhaltungsmöglichkeiten für Spieler aller Art bietet. Ein wichtiger Aspekt des Online-Glücksspiels ist jedoch die Auszahlung von Gewinnen und die Geschwindigkeit, mit der dies geschieht. In diesem Artikel werden die Auszahlungszeiten im Zet Casino genauer betrachtet.
Das Zet Casino bietet seinen Spielern verschiedene Zahlungsmethoden, um ihre Gewinne abzuheben. Dazu gehören Kreditkarten, E-Wallets und Banküberweisungen. Die Auszahlungszeiten hängen in der Regel von der gewählten Zahlungsmethode ab. In der Regel erfolgen Auszahlungen mit E-Wallets wie Skrill oder Neteller am schnellsten, in der Regel innerhalb von 24 Stunden. Banküberweisungen und Kreditkarten können etwas länger dauern, in der Regel zwischen 3 und 5 Werktagen.
Es ist wichtig zu beachten, dass die Auszahlungszeiten im Zet Casino auch von anderen Faktoren abhängen können, wie zum Beispiel der Überprüfung von Identität und Zahlungsmethoden. Spieler sollten sicherstellen, dass sie alle erforderlichen Unterlagen bereitstellen, um die Auszahlungsprozesse zu beschleunigen.
Insgesamt kann gesagt werden, dass das Zet Casino relativ schnelle Auszahlungszeiten bietet, insbesondere bei der Verwendung von E-Wallets. Spieler können sich darauf verlassen, dass ihre Gewinne schnell und sicher auf ihr Konto überwiesen werden.
Abschließend lässt sich sagen, dass das Zet Casino eine gute Wahl für Spieler ist, die Wert auf schnelle Auszahlungen legen. Mit einer Vielzahl von Zahlungsmethoden und relativ kurzen Auszahlungszeiten sorgt das Casino dafür, dass die Spieler ihre Gewinne schnell und unkompliziert erhalten können.
https://zetcasino.one/
площадка кракен – сайт кракен тор, кракен магазин
Zet Casino Auszahlungszeit
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und groГџzГјgigen Boni fГјr seine Spieler bietet. Eines der wichtigsten Dinge, die Spieler beachten sollten, wenn sie in einem Online-Casino spielen, ist die Auszahlungsdauer. In diesem Artikel werden wir uns genauer mit der Zet Casino Auszahlungszeit befassen.
Die Zet Casino Auszahlungszeit hängt von verschiedenen Faktoren ab, darunter die gewählte Auszahlungsmethode und der Verifizierungsprozess des Spielers. In der Regel dauert die Bearbeitungszeit für Auszahlungen bei Zet Casino zwischen 24 und 48 Stunden. Sobald die Auszahlung genehmigt wurde, hängt die tatsächliche Überweisungsdauer von der gewählten Zahlungsmethode ab.
Spieler können bei Zet Casino zwischen verschiedenen Auszahlungsmethoden wählen, darunter Kreditkarten, E-Wallets und Banküberweisungen. E-Wallets wie Skrill und Neteller bieten in der Regel die schnellsten Auszahlungszeiten, während Banküberweisungen aufgrund von Bearbeitungszeiten bei den Banken länger dauern können.
Es ist wichtig zu beachten, dass Spieler ihre Identität überprüfen müssen, bevor sie eine Auszahlung bei Zet Casino beantragen können. Dies dient dazu, die Sicherheit der Spieler zu gewährleisten und Betrug zu verhindern. Spieler sollten sicherstellen, dass sie alle erforderlichen Dokumente zur Verfügung haben, um den Verifizierungsprozess so reibungslos wie möglich zu gestalten.
Insgesamt bietet Zet Casino seinen Spielern eine schnelle und zuverlässige Auszahlungsdauer. Spieler können sich darauf verlassen, dass ihre Gewinne schnell und sicher ausgezahlt werden, damit sie ihr Geld schnell genießen können. Wenn Sie nach einem Online-Casino mit schnellen Auszahlungen suchen, ist Zet Casino definitiv einen Besuch wert.
https://zetcasino.one/
Boomerang Casino No Deposit
Das Boomerang Casino ist eine beliebte Online-GlГјcksspielplattform, die eine Vielzahl von Spielen und Boni fГјr seine Spieler anbietet. Eines der attraktivsten Angebote des Casinos ist der sogenannte “No Deposit Bonus”, bei dem Spieler Bonusgeld erhalten, ohne eine Einzahlung tГ¤tigen zu mГјssen.
Der No Deposit Bonus ist eine großartige Möglichkeit für Spieler, das Casino auszuprobieren, ohne eigenes Geld riskieren zu müssen. Spieler können mit dem Bonusgeld verschiedene Spiele spielen und dabei echtes Geld gewinnen. Dies ist eine fantastische Gelegenheit für Anfänger, die noch keine Erfahrung mit Online-Glücksspielen haben, um das Casino kennenzulernen und sich mit den verschiedenen Spielen vertraut zu machen.
Um den No Deposit Bonus zu erhalten, müssen Spieler sich einfach im Boomerang Casino anmelden und ein Konto erstellen. Der Bonus wird dann automatisch gutgeschrieben und kann sofort für Spiele verwendet werden. Es ist wichtig zu beachten, dass es in der Regel bestimmte Wettanforderungen gibt, die erfüllt werden müssen, bevor Gewinne, die mit dem Bonus erzielt wurden, ausgezahlt werden können.
Das Boomerang Casino bietet eine Vielzahl von Spielen, darunter Spielautomaten, Tischspiele wie Roulette und Blackjack, sowie Live-Casino-Spiele mit echten Dealern. Mit dem Bonusgeld können Spieler jede Art von Spiel ausprobieren und vielleicht sogar einen großen Gewinn erzielen.
Insgesamt ist der No Deposit Bonus im Boomerang Casino eine großartige Möglichkeit für Spieler, das Casino zu erkunden und erste Gewinne zu erzielen, ohne eigenes Geld riskieren zu müssen. Es ist ein aufregendes Angebot, das es Spielern ermöglicht, die Welt des Online-Glücksspiels zu entdecken und Spaß zu haben.
https://boomerangcasino.one/
Das Zet Casino ist eine Online-Glücksspielplattform, die seit einiger Zeit auf dem Markt ist und Spielern eine Vielzahl von Spielen und Möglichkeiten bietet. Doch wie gut schneidet diese Plattform in der Bewertung ab?
Zunächst einmal fällt positiv auf, dass das Zet Casino eine große Auswahl an Spielen anbietet. Von Spielautomaten über Tischspiele bis hin zu Live-Casino-Spielen ist für jeden Geschmack etwas dabei. Die Qualität der Spiele ist dabei sehr gut und sorgt für ein unterhaltsames Spielerlebnis.
Auch die Benutzerfreundlichkeit der Plattform wird von vielen Spielern gelobt. Das Design ist ansprechend und übersichtlich gestaltet, sodass man sich schnell zurechtfindet. Zudem gibt es eine Vielzahl von Zahlungsmöglichkeiten, was die Ein- und Auszahlungen sehr bequem macht.
Ein weiterer Pluspunkt des Zet Casinos ist der Kundenservice. Die Mitarbeiter sind sehr freundlich und hilfsbereit und stehen rund um die Uhr zur VerfГјgung, um Fragen und Anliegen der Spieler zu beantworten.
Insgesamt lässt sich sagen, dass das Zet Casino eine solide Online-Glücksspielplattform ist, die eine gute Auswahl an Spielen, eine benutzerfreundliche Oberfläche und einen zuverlässigen Kundenservice bietet. Die meisten Spieler sind mit dem Angebot zufrieden und geben dem Casino eine positive Bewertung. Wer also auf der Suche nach einem unterhaltsamen und zuverlässigen Online-Casino ist, der sollte das Zet Casino auf jeden Fall in Betracht ziehen.
https://zetcasino.one/
mega darknet – mega darknet market, сайт мега даркнет
Tipico: Warum wird die Buchung zum Casino blockiert?
Immer wieder taucht bei Nutzern des Online-Casinos von Tipico die Frage auf, warum ihre Buchungen blockiert werden. Dies kann verschiedene Gründe haben und ist meist auf Sicherheitsvorkehrungen zurückzuführen. In diesem Artikel möchten wir genauer auf dieses Thema eingehen und erklären, warum es zu einer Blockierung kommen kann.
Zunächst einmal ist es wichtig zu verstehen, dass Tipico als seriöser Anbieter großen Wert auf die Sicherheit seiner Kunden legt. Aus diesem Grund werden regelmäßig Überprüfungen und Kontrollen durchgeführt, um möglichen Betrug oder Missbrauch zu verhindern. Dies kann dazu führen, dass bestimmte Transaktionen blockiert werden, um das Risiko für die Nutzer zu minimieren.
Ein weiterer Grund für eine Blockierung könnte eine fehlerhafte oder unvollständige Verifizierung des Kontos sein. Um sicherzustellen, dass alle Nutzer volljährig sind und keine Geldwäsche betreiben, ist Tipico gesetzlich verpflichtet, die Identität der Kunden zu überprüfen. Wenn diese Verifizierung nicht vollständig abgeschlossen wurde, kann es zu Schwierigkeiten bei Buchungen kommen.
Auch verdächtige Aktivitäten können dazu führen, dass eine Buchung blockiert wird. Wenn beispielsweise ungewöhnlich hohe Beträge eingezahlt oder ausgezahlt werden, kann dies als Warnzeichen für potenziellen Betrug gesehen werden. In solchen Fällen greift Tipico ein und blockiert die Transaktionen, um die Sicherheit der Nutzer zu gewährleisten.
Um eine Blockierung zu vermeiden, ist es daher ratsam, sein Konto regelmäßig zu verifizieren und verdächtige Aktivitäten zu vermeiden. Sollte es dennoch zu Problemen kommen, steht der Kundenservice von Tipico jederzeit zur Verfügung und hilft gerne bei der Klärung von offenen Fragen.
Insgesamt ist es also wichtig zu verstehen, dass eine Buchung zum Casino von Tipico aus Sicherheitsgründen blockiert werden kann. Durch die Einhaltung der Verifizierungsvorschriften und das Vermeiden verdächtiger Aktivitäten kann man solche Schwierigkeiten jedoch in der Regel umgehen. Tipico legt großen Wert auf die Sicherheit seiner Kunden und möchte ihnen ein sicheres und angenehmes Spielerlebnis bieten.
https://tipicocasino.one/
official source high cost-to-income ratio
мега купить – mega ссылка, mega как зайти
pop over to this web-site Crypto Project
his response Rufus usb
Промокоды для Зенитбет zenitbet1.com
По запросу бк зенит для андроид вы на нужном пути. Зеркало официального сайта Zenitbet спокойно работает на территории России и абсолютно безопасно. Вы можете без опаски вводить свои персональные данные и быть уверены в том, что данные не могут быть заняты другими пользователями. Также средства на вашем счету находятся под защитой. Комфорт в том, что сайт совпадает официальному и Вам не потребуется привыкать к иной картинке. А еще не понадобится проходить вторичную регистрацию, если вы уже были зарегистрированы. В зеркале хранятся Ваши пароли, впишите их и заходите в свой профиль.
Das Boomerang Casino Mobiles – Spielen Sie unterwegs!
Im modernen Zeitalter der Technologie ist es einfacher denn je, auf Spiele und Unterhaltung zuzugreifen, egal wo man sich befindet. Mit dem Boomerang Casino Mobiles können Sie nun auch unterwegs ganz bequem auf Ihre Lieblingscasinospiele zugreifen.
Das Boomerang Casino Mobiles bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino und vieles mehr. Egal, ob Sie ein Fan von klassischen Spielautomaten oder modernen Videoslots sind, hier finden Sie garantiert die richtigen Spiele fГјr sich.
Das mobile Casino ist für alle gängigen Geräte optimiert, sei es ein Smartphone oder Tablet. Durch die intuitive Benutzeroberfläche können Sie ganz einfach durch die Auswahl der Spiele navigieren und können sofort mit dem Spielen beginnen.
Ein weiterer großer Vorteil des Boomerang Casino Mobiles ist die Möglichkeit, auch unterwegs Ein- und Auszahlungen vorzunehmen. Mit einer Vielzahl von sicheren Zahlungsmethoden stehen Ihnen alle Möglichkeiten offen, Geld auf Ihr Konto einzuzahlen oder Gewinne abzuheben.
Darüber hinaus bietet das mobile Casino regelmäßige Aktionen und Boni, um Ihre Spielerfahrung noch spannender zu gestalten. Von Freispielen bis hin zu Einzahlungsboni gibt es hier eine Vielzahl von Belohnungen, die auf Sie warten.
Also, warum warten? Laden Sie einfach die Boomerang Casino Mobiles App herunter oder besuchen Sie die mobile Website und tauchen Sie ein in die Welt des mobilen Casinos. Spielen Sie unterwegs und genieГџen Sie jederzeit und Гјberall spannende Casinospiele!
https://boomerangcasino.one/
his response Obs
Zet Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und Zahlungsmöglichkeiten anbietet. Viele Spieler fragen sich jedoch, wie die Auszahlung bei Zet Casino funktioniert. In diesem Artikel werden wir uns genauer mit diesem Thema befassen.
Um eine Auszahlung bei Zet Casino zu tätigen, müssen Spieler zunächst sicherstellen, dass sie über ausreichende Gewinne auf ihrem Konto verfügen. Sobald dies der Fall ist, können sie sich entscheiden, wie sie ihr Geld abheben möchten. Zet Casino bietet verschiedene Zahlungsmethoden an, darunter Kredit- und Debitkarten, E-Wallets wie Skrill und Neteller sowie Banküberweisungen.
Um eine Auszahlung vorzunehmen, mГјssen Spieler einfach auf den “Auszahlung” -Button klicken und die gewГјnschte Zahlungsmethode auswГ¤hlen. Sie werden dann aufgefordert, ihre Kontoinformationen einzugeben und den Betrag anzugeben, den sie abheben mГ¶chten. Es ist wichtig zu beachten, dass bei einigen Zahlungsmethoden GebГјhren anfallen kГ¶nnen und dass Auszahlungen je nach Methode unterschiedliche Bearbeitungszeiten haben kГ¶nnen.
Sobald die Auszahlungsanforderung genehmigt wurde, wird das Geld auf das angegebene Konto des Spielers überwiesen. Es ist wichtig zu beachten, dass Zet Casino strenge Sicherheitsmaßnahmen implementiert hat, um die Sicherheit der Spielerdaten und Finanztransaktionen zu gewährleisten.
Zet Casino bietet eine zuverlässige und benutzerfreundliche Plattform für Online-Glücksspiele und Auszahlungen. Spieler können sich darauf verlassen, dass ihre Gewinne schnell und sicher auf ihr Konto überwiesen werden. Wenn Sie weitere Fragen zur Auszahlung bei Zet Casino haben, können Sie sich jederzeit an den Kundendienst des Casinos wenden, der Ihnen gerne weiterhilft.
https://zetcasino.one/
Ein Cashback-Bonus ist eine beliebte Belohnung für Spieler in Online-Casinos. Tipico Casino bietet ebenfalls diese Möglichkeit für seine Kunden an. Doch was genau bedeutet Cashback und wie funktioniert es im Tipico Casino?
Beim Cashback erhalten Spieler einen Teil ihrer Verluste zurück, sodass sie einen Teil ihres Einsatzes zurückerhalten können. Dies kann als eine Art Versicherung gegen Verluste angesehen werden und kann besonders für Spieler von Vorteil sein, die gerne höhere Einsätze tätigen.
Im Tipico Casino können Spieler von einem Cashback-Bonus profitieren, der ihnen einen prozentualen Anteil ihrer Verluste zurückgibt. Dabei ist zu beachten, dass verschiedene Spiele unterschiedliche Cashback-Raten haben können. So können zum Beispiel Slots einen höheren prozentualen Cashback als Tischspiele haben.
Um den Cashback-Bonus zu erhalten, müssen Spieler einfach im Tipico Casino spielen und ihre Einsätze platzieren. Im Falle von Verlusten wird der Cashback-Betrag automatisch auf das Spielerkonto gutgeschrieben. Es ist eine einfache und unkomplizierte Möglichkeit, etwas von seinen Verlusten zurückzuerhalten.
Es lohnt sich also, im Tipico Casino nach dem Cashback-Bonus Ausschau zu halten und von dieser attraktiven Belohnung zu profitieren. Mit etwas Glück können Spieler einen Teil ihrer Verluste zurückgewinnen und so länger am Spielspaß teilhaben. Ein toller Anreiz, um im Tipico Casino sein Glück zu versuchen!
https://tipicocasino.one/
Zet Casino Erfahrung: Ein Гњberblick Гјber das beliebte Online-Casino
Das Zet Casino ist seit seiner GrГјndung im Jahr 2018 zu einem der beliebtesten Online-Casinos fГјr deutsche Spieler geworden. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und einem hervorragenden Kundenservice hat es sich schnell einen Namen in der GlГјcksspielbranche gemacht.
Der erste Eindruck, den man beim Betreten der Website von Zet Casino bekommt, ist positiv. Die Seite ist benutzerfreundlich gestaltet und ermöglicht es den Spielern, schnell und einfach ihre Lieblingsspiele zu finden. Das Casino bietet eine breite Palette von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr, die von renommierten Softwareanbietern wie NetEnt, Microgaming und Betsoft bereitgestellt werden.
Ein weiterer großer Vorteil des Zet Casinos sind die großzügigen Boni und Promotionen, die es seinen Spielern bietet. Neue Spieler können sich über einen Willkommensbonus freuen, der sowohl Bonusgeld als auch Freispiele umfasst. Darüber hinaus gibt es regelmäßig laufende Promotionen, Turniere und Belohnungen für treue Spieler.
Der Kundenservice von Zet Casino ist rund um die Uhr per Live-Chat, E-Mail oder Telefon erreichbar und zeichnet sich durch seine Freundlichkeit und Kompetenz aus. Die Mitarbeiter stehen den Spielern bei Fragen und Problemen mit Rat und Tat zur Seite und sorgen fГјr ein reibungsloses Spielerlebnis.
Insgesamt lässt sich sagen, dass die Erfahrung im Zet Casino in der Regel sehr positiv ist. Das Casino überzeugt mit einer großen Auswahl an Spielen, attraktiven Boni und einem exzellenten Kundenservice. Wer auf der Suche nach einem seriösen Online-Casino ist, sollte Zet Casino definitiv eine Chance geben.
https://zetcasino.one/
Tipico Casino Offline
In der heutigen digitalen Welt ist es immer seltener, dass Unternehmen ihre Produkte und Dienstleistungen ausschließlich offline anbieten. Doch es gibt immer noch einige Branchen, die auf den persönlichen Kontakt setzten, so auch das Tipico Casino.
Das Tipico Casino ist eine der bekanntesten und beliebtesten Online-Glücksspielplattformen in Deutschland. Mit einer Vielzahl von Spielautomaten, Tischspielen und Live-Casino-Spielen bietet das Tipico Casino seinen Kunden eine breite Auswahl an Unterhaltungsmöglichkeiten. Doch was viele nicht wissen: Tipico bietet auch die Möglichkeit, offline zu spielen.
Das Konzept des offline Casinos von Tipico ist simpel: An ausgewählten Standorten, meist in größeren Städten, können Kunden ihre Lieblingsspiele auch ohne Internetverbindung spielen. Dort stehen Spielautomaten, Roulette-Tische und andere Casinospiele zur Verfügung, die ganz klassisch im realen Leben gespielt werden können.
Der Vorteil des offline Casinos liegt vor allem in der persönlichen Betreuung durch geschultes Personal. Die Mitarbeiter stehen den Kunden bei Fragen und Problemen zur Seite und sorgen für ein sicheres und verantwortungsvolles Spielumfeld. Zudem bietet das offline Casino von Tipico eine besondere Atmosphäre, die man online nicht erleben kann.
Wer also Lust auf ein traditionelles CasinovergnГјgen hat, kann sich jederzeit in einem offline Casino von Tipico vergnГјgen. Egal ob alleine oder mit Freunden, das Tipico Casino bietet eine unterhaltsame Abwechslung zum Online-Spielen und sorgt fГјr spannende Stunden voller SpaГџ und Spannung.
https://tipicocasino.one/
Выбор кованого забора – это не только вопрос безопасности, но и эстетики. На a-kovka.ru мне удалось найти именно то, что я искал: уникальные дизайны и превосходное качество металла. Компания предоставляет услуги по всей Московской области, включая бесплатный замер и помощь в создании дизайна, что сделало процесс установки забора максимально удобным. Работы выполнены на высшем уровне, и теперь кованый забор является настоящим украшением моего дома.
Добро пожаловать в кузницу “А-ковка” кованые перила лестниц для дома цена – ваш надежный партнер в создании красивых и функциональных перил для вашего дома. Мы находимся в Москве, всего в 91 километре от МКАД, и готовы предложить вам широкий выбор кованых изделий, выполненных опытными мастерами.
Наша цена доступна для любого покупателя, а качество наших изделий всегда остается на высоте. Мы используем современное оборудование и материалы высокого качества, чтобы каждый заказчик остался доволен результатом. Кованые перила не только придают вашему интерьеру изысканный вид, но и являются прочным и долговечным решением для вашего дома. Закажите перила в нашей кузнице и убедитесь сами в высоком качестве наших изделий!
Зарегистрироваться в БК Зенит zenitbet1.com
По поиску zenit casino вы на нужном пути. Зеркало официального сайта Zenitbet легко работает на территории РФ и абсолютно надежно. Вы можете без опасений давать свои данные и быть уверены в том, что данные не могут быть заняты другими личностями. Также средства на вашем счету находятся под защитой. Удобство в том, что сайт совпадает официальному и Вам не нужно будет привыкать к иной картинке. А еще не нужно проходить повторную регистрацию, если вы уже были зарегистрированы. В зеркале сохраняются Ваши пароли, вводите их и заходите в свой кошелек.
Das Zet Casino ist eines der aufstrebenden Online-Casinos auf dem Markt, das eine Lizenz fГјr den Betrieb von GlГјcksspielen besitzt. Die Lizenzierung von Online-Casinos ist ein wichtiger Schritt, um sicherzustellen, dass die Spiele fair und sicher sind.
Das Zet Casino verfügt über eine Lizenz der Malta Gaming Authority, einer der renommiertesten Glücksspielbehörden der Welt. Diese Lizenz garantiert, dass das Casino strenge Auflagen einhalten muss, um sicherzustellen, dass die Spieler vor Betrug und unfairen Praktiken geschützt sind.
Durch die Lizenzierung wird auch sichergestellt, dass das Zet Casino verantwortungsbewusstes Glücksspiel fördert und Maßnahmen zum Schutz von gefährdeten Spielern ergreift. Das Casino bietet eine Vielzahl von Spielen, darunter Spielautomaten, Tischspiele und Live-Casino-Spiele, die alle unter der Aufsicht der Malta Gaming Authority stehen.
Spieler, die im Zet Casino spielen, können sicher sein, dass ihre persönlichen und finanziellen Daten sicher sind und dass sie eine faire Chance haben, zu gewinnen. Die Lizenzierung des Casinos ist ein wichtiger Beweis für seine Seriosität und Vertrauenswürdigkeit.
Insgesamt ist die Lizenz des Zet Casinos ein wichtiger Faktor, der das Vertrauen der Spieler in die Integrität des Casinos stärkt. Spieler können beruhigt spielen und genießen die Vielfalt an Spielen, die das Casino zu bieten hat, in dem Wissen, dass sie in sicheren und fairen Händen sind.
https://zetcasino.one/
Tipico Live Casino lädt nicht
Haben Sie schon einmal versucht, im Tipico Live Casino zu spielen, aber die Seite lädt einfach nicht? Das kann frustrierend sein, besonders wenn Sie sich auf ein spannendes Spiel gefreut haben. Es gibt mehrere Gründe, warum das Live Casino von Tipico nicht lädt und hier sind einige mögliche Lösungen:
1. Überprüfen Sie Ihre Internetverbindung: Stellen Sie sicher, dass Sie eine stabile und schnelle Internetverbindung haben. Wenn Ihre Verbindung langsam oder instabil ist, kann dies dazu führen, dass das Live Casino nicht richtig lädt.
2. Löschen Sie Ihren Browser-Cache und Cookies: Manchmal können gespeicherte Daten im Browser dazu führen, dass Seiten nicht richtig geladen werden. Löschen Sie Ihren Browser-Cache und Cookies und versuchen Sie es erneut.
3. Aktualisieren Sie Ihren Browser: Manchmal kann es sein, dass veraltete Browser-Versionen nicht mit dem Live Casino von Tipico kompatibel sind. Stellen Sie sicher, dass Ihr Browser auf dem neuesten Stand ist und alle Updates installiert sind.
4. Kontaktieren Sie den Kundenservice: Wenn trotz dieser Maßnahmen das Live Casino von Tipico immer noch nicht lädt, kontaktieren Sie den Kundenservice. Die Mitarbeiter können Ihnen möglicherweise weiterhelfen und das Problem lösen.
Insgesamt kann es verschiedene Gründe geben, warum das Tipico Live Casino nicht lädt. Es ist wichtig, geduldig zu bleiben und die oben genannten Schritte zu befolgen, um das Problem zu beheben. Mit etwas Glück können Sie bald wieder Ihre Lieblingsspiele im Live Casino von Tipico genießen.
https://tipicocasino.one/
Zet Casino Promo Code 2022: Ein Blick auf die aktuellen Angebote
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Casino-Spielen und Promotionen für seine Spieler anbietet. Für das Jahr 2022 hat Zet Casino eine Vielzahl von spannenden Promo-Codes und Aktionen in petto, die es den Spielern ermöglichen, noch mehr aus ihrem Spielerlebnis herauszuholen.
Einer der beliebtesten Promo-Codes bei Zet Casino ist der Willkommensbonus für neue Spieler. Mit diesem Promo-Code erhalten Spieler einen großzügigen Einzahlungsbonus, der es ihnen ermöglicht, ihre Bankroll zu erhöhen und mehr Spiele auszuprobieren. Darüber hinaus bietet Zet Casino regelmäßig spezielle Promotionen und Boni für bestehende Spieler an, darunter Freispiele, Einzahlungsboni und Cashback-Angebote.
Um den Zet Casino Promo-Code 2022 zu nutzen, müssen Spieler einfach den Promo-Code während des Einzahlungsvorgangs eingeben und die entsprechenden Bonusbedingungen erfüllen. Die genauen Bedingungen für jeden Promo-Code können auf der Zet Casino Website nachgelesen werden.
Zet Casino ist bekannt für seine vielfältige Auswahl an hochwertigen Casino-Spielen, darunter Spielautomaten, Tischspiele und Live-Casino-Spiele. Mit den spannenden Promo-Codes und Aktionen für das Jahr 2022 können Spieler noch mehr Spaß und Spannung aus ihren Lieblingsspielen herausholen und gleichzeitig die Chance auf attraktive Preise und Belohnungen erhalten.
Insgesamt bietet Zet Casino eine erstklassige Spielerfahrung mit hochwertigen Spielen, groГџzГјgigen Promotionen und einem exzellenten Kundenservice. Spieler, die nach einem erstklassigen Online-Casino-Erlebnis suchen, sollten auf jeden Fall die aktuellen Promo-Codes und Aktionen von Zet Casino fГјr das Jahr 2022 in Betracht ziehen.
https://zetcasino.one/
https://bvbagemori.com/
Das m.boomerang-casino ist eine aufregende Online-Glücksspielseite, die Spielern eine Vielzahl von Casino-Spielen und spannenden Bonusangeboten bietet. Mit einer einfach zu bedienenden Benutzeroberfläche und einer Vielzahl von Spieloptionen ist dieses Casino die perfekte Wahl für alle, die auf der Suche nach Unterhaltung und großen Gewinnen sind.
Ein Hauptmerkmal des m.boomerang-casinos ist das umfangreiche Angebot an Spielautomaten, darunter beliebte Titel wie Book of Dead, Starburst und Gonzo’s Quest. Die Vielfalt der Spiele sorgt dafГјr, dass fГјr jeden Spieler etwas dabei ist, egal ob man sich fГјr klassische Fruchtmaschinen oder aufwendige Video-Slots interessiert.
Neben Spielautomaten bietet das m.boomerang-casino auch eine breite Auswahl an Tischspielen wie Blackjack, Roulette und Baccarat. Für diejenigen, die eine authentische Casino-Erfahrung suchen, gibt es sogar die Möglichkeit, an Live-Dealer-Spielen teilzunehmen, bei denen echte Dealer die Spiele in Echtzeit führen.
Ein weiterer Grund, sich für das m.boomerang-casino zu entscheiden, sind die großzügigen Bonusangebote, die regelmäßig verfügbar sind. Neue Spieler können von Willkommensboni profitieren, während Stammkunden regelmäßige Promotionen und Bonusangebote erhalten können.
Das m.boomerang-casino bietet auch eine sichere und zuverlässige Plattform für Spieler, da es von renommierten Glücksspielbehörden lizenziert ist und eine sichere SSL-Verschlüsselung verwendet, um die persönlichen Daten der Spieler zu schützen.
Insgesamt ist das m.boomerang-casino eine erstklassige GlГјcksspielseite, die eine spannende und unterhaltsame Erfahrung fГјr Spieler bietet. Mit einer Vielzahl von Spielen, groГџzГјgigen Bonusangeboten und einer sicheren Plattform ist dieses Casino definitiv einen Besuch wert.
https://boomerangcasino.one/
Manufacturing metal structures is a very complex and responsible process. It stagramer.com is necessary to follow some rules and follow recommendations to ensure that the product turns out to be of high quality and safe.
Select the appropriate metal material for the specific design teplica-parnik.net. Requirements for strength, corrosion resistance and other characteristics must be taken into account. It is worth contacting experienced specialists who will help you understand all the parameters.
Boomerang Casino: Kostenlose Freispiele
Boomerang Casino ist ein aufregendes Online-Casino, das Spielern eine breite Auswahl an Spielen und spannenden Aktionen bietet. Einer der beliebtesten Angebote für Spieler sind die kostenlosen Freispiele, die das Casino regelmäßig veranstaltet.
Kostenlose Freispiele sind eine großartige Möglichkeit, um neue Spiele auszuprobieren und zusätzliche Gewinne zu erzielen, ohne dabei Ihr eigenes Geld zu riskieren. Boomerang Casino bietet regelmäßig verschiedene Aktionen an, bei denen Spieler kostenlose Freispiele erhalten können. Diese können für bestimmte Spiele oder Slots gelten und sind in der Regel an bestimmte Bedingungen geknüpft, wie zum Beispiel eine Mindesteinzahlung oder Umsatzanforderungen.
Um kostenlose Freispiele zu erhalten, müssen Spieler sich zunächst für die Aktion anmelden oder einen entsprechenden Bonuscode verwenden. Sobald die Freispiele gutgeschrieben wurden, können Spieler sofort mit dem Spielen beginnen und hoffentlich lukrative Gewinne erzielen.
Das Boomerang Casino bietet seinen Spielern eine erstaunliche Auswahl an Spielen und groГџzГјgige Aktionen, einschlieГџlich kostenloser Freispiele. Wenn Sie also auf der Suche nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis sind, sollten Sie auf jeden Fall Boomerang Casino im Auge behalten. Viel SpaГџ beim Spielen und viel GlГјck!
https://boomerangcasino.one/
реабилитационный центр лечение алкоголизма https://addictiontreatment.kz/
лечение алкоголизма адрес https://narcohelp.kz/
Tipico: Geld von Casino zu Sportwetten transferieren
Tipico ist einer der bekanntesten Anbieter von Online-Glücksspielen in Deutschland. Neben dem Casino-Bereich bietet die Plattform auch die Möglichkeit, auf Sportereignisse zu wetten. Viele Nutzer fragen sich, wie sie Geld von ihrem Casino-Konto auf ihr Sportwetten-Konto transferieren können.
GrundsГ¤tzlich ist es bei Tipico problemlos mГ¶glich, Geld zwischen den verschiedenen Bereichen zu transferieren. Dazu muss man sich lediglich auf der Webseite oder in der App von Tipico anmelden und den MenГјpunkt “Guthaben transferieren” wГ¤hlen. Dort kann man angeben, wie viel Geld man von Casino zu Sportwetten transferieren mГ¶chte.
Es gibt jedoch ein paar Dinge zu beachten, wenn man Geld zwischen den Bereichen transferiert. Zum einen müssen die Bonusbedingungen erfüllt sein, bevor man eine Auszahlung tätigen kann. Das bedeutet, dass man den Bonus, den man im Casino oder bei den Sportwetten erhalten hat, entsprechend umsetzen muss, bevor man eine Auszahlung beantragen kann.
Zum anderen ist es wichtig, darauf zu achten, dass bei einem Transfer von Casino zu Sportwetten möglicherweise Einschränkungen gelten können. So könnte es sein, dass das übertragene Geld zunächst für Sportwetten genutzt werden muss, bevor man es sich auszahlen lassen kann. Diese Bedingungen können je nach Aktionen und Promotionen variieren, daher ist es ratsam, sich vorab über die genauen Modalitäten zu informieren.
Insgesamt bietet Tipico seinen Nutzern eine einfache Möglichkeit, Geld zwischen Casino und Sportwetten zu transferieren. Durch das klare und übersichtliche Menü auf der Webseite oder in der App erfolgt der Transfer unkompliziert und schnell. Mit ein paar einfachen Klicks kann man sein Geld von einem Bereich in den anderen übertragen und so das vielseitige Angebot von Tipico voll auskosten.
https://tipicocasino.one/
https://frugallivin.com/
Tipico ist eine bekannte Marke im Bereich der Sportwetten und Online-Casinos. Die Website http://www.tipico.de bietet eine Vielzahl von Spielen und Wettmöglichkeiten für die Nutzer. Das Online-Casino von Tipico ist vor allem für sein breites Angebot an Slots, Tischspielen und Live-Casino-Spielen bekannt.
Das Online-Casino von Tipico bietet eine benutzerfreundliche Oberfläche, die es den Nutzern ermöglicht, schnell und einfach ihre Lieblingsspiele zu finden und zu spielen. Die Website ist auch für mobile Geräte optimiert, so dass die Spieler auch unterwegs ihre Lieblingsspiele genießen können.
Die Spielauswahl bei Tipico ist beeindruckend und umfasst eine Vielzahl von verschiedenen Spielautomaten, Tischspielen wie Roulette und Blackjack sowie Live-Casino-Spiele, bei denen echte Dealer das Spiel leiten. Neben den klassischen Casinospiele gibt es auch progressive Jackpot-Slots, bei denen die Gewinne enorm sein können.
Ein weiterer Vorteil von http://www.tipico.de ist der Kundenservice, der rund um die Uhr zur Verfügung steht. Die Spieler können sich bei Fragen oder Problemen jederzeit an das Support-Team wenden und erhalten schnell und zuverlässig Hilfe.
Insgesamt ist http://www.tipico.de ein empfehlenswertes Online-Casino, das eine Vielzahl von Spielen und Wettmöglichkeiten für die Spieler bietet. Mit seiner benutzerfreundlichen Oberfläche, großartigen Spielauswahl und zuverlässigen Kundenservice ist Tipico eine gute Wahl für alle, die gerne online spielen.
https://tipicocasino.one/
The main advantage of a forklift is its versatility and ease of use stroibloger.com. Essentially, it’s just a dolly with a durable fork that can be used to lift pallets or large loads to any height.
A ticket is each application that is registered by support services instukzia.com. The ticket system is a digital tool that automates the operation of various services. The solutions are relevant for registration and processing of customer requests.
Das Tipico Casino gehört zu den beliebtesten Online-Casinos in Deutschland, doch es kann vorkommen, dass man bei der Anmeldung auf Probleme stößt. Wenn die Tipico Casino Anmeldung nicht möglich ist, kann das verschiedene Gründe haben.
Ein häufiges Problem ist, dass die eingegebenen Daten nicht mit den Angaben übereinstimmen, die bei der Registrierung hinterlegt wurden. In diesem Fall sollte man sicherstellen, dass man alle Informationen korrekt eingegeben hat und keine Tippfehler gemacht wurden. Es kann auch hilfreich sein, sich die Registrierungsmail noch einmal anzusehen, um sicherzustellen, dass man alle notwendigen Schritte abgeschlossen hat.
Ein weiterer Grund fГјr Probleme bei der Anmeldung im Tipico Casino kann sein, dass das Konto bereits gesperrt wurde. Dies kann beispielsweise der Fall sein, wenn man gegen die Nutzungsbedingungen verstoГџen hat oder Verdacht auf Manipulation besteht. In diesem Fall sollte man den Kundenservice kontaktieren, um weitere Informationen zu erhalten.
Es kann auch vorkommen, dass es technische Probleme auf der Webseite gibt, die die Anmeldung beeinträchtigen. In diesem Fall sollte man es zu einem späteren Zeitpunkt erneut versuchen oder die Webseite neu laden. Alternativ kann es auch helfen, den Browserverlauf zu löschen oder einen anderen Browser zu verwenden.
Falls alle diese Maßnahmen nicht helfen und die Tipico Casino Anmeldung weiterhin nicht möglich ist, sollte man den Kundenservice kontaktieren. Die Mitarbeiter sind in der Regel gut geschult und können bei Problemen weiterhelfen.
Insgesamt ist es wichtig, Ruhe zu bewahren und geduldig zu bleiben, wenn die Tipico Casino Anmeldung nicht möglich ist. Oftmals handelt es sich um kleine Probleme, die schnell gelöst werden können. Durch die Kontaktaufnahme mit dem Kundenservice kann man in den meisten Fällen eine Lösung finden und schon bald in den Genuss des Spielvergnügens im Tipico Casino kommen.
https://tipicocasino.one/
Inserts are the most consumable part of a workpiece machining system. They homeprorab.info are placed in special holders and can be quickly changed depending on wear or process requirements.
Здравствуйте всем присутствующим! Мне бы хотелось сообщить своим опытом использования сайта казино кент. Тут вы найдёте большой выбор игр, включая слоты, карточные игры и рулетку. Оформление сайта интуитивно понятный, что совершает процесс игры удобным и приятным. В особенности порадовали быстрые и надёжные методы пополнения и вывода средств. Казино ещё предлагает отличные бонусы для новых и регулярных игроков. Поддержка постоянно на связи и готова помочь решить любые проблемы. Но помните о рисках, участвуя в игры на удачу. Везения всем участникам!
Das Zet Casino ist eine beliebte Online-Glücksspielseite, die eine Vielzahl von Spielen und Aktionen für die Spieler bietet. Leider haben viele Nutzer in letzter Zeit über Störungen auf der Website berichtet.
Die StГ¶rungen scheinen unterschiedlich zu sein – einige Nutzer klagen Гјber Verbindungsprobleme, andere Гјber langsame Ladezeiten oder unerwartete AbstГјrze wГ¤hrend des Spielens. Diese Probleme kГ¶nnen frustrierend sein, besonders wenn man versucht, sein GlГјck zu versuchen oder an einem Bonusangebot teilzunehmen.
Es ist wichtig zu beachten, dass die Ursachen für diese Störungen vielfältig sein können. Manchmal liegt es an Überlastungen auf der Serverseite des Casinos, manchmal an technischen Problemen mit der eigenen Internetverbindung des Spielers. Es ist ratsam, zuerst zu überprüfen, ob das Problem auf Seiten des Zet Casinos liegt oder auf Ihrer eigenen Seite.
Wenn die Störungen auf Seiten des Casinos liegen, ist es wichtig, dass das Zet Casino schnell handelt, um diese Probleme zu beheben. Spieler sollten in der Lage sein, reibungslos auf der Website zu navigieren und ohne Unterbrechungen spielen zu können. Andernfalls könnten sie sich frustriert fühlen und möglicherweise das Casino wechseln.
Es wurde berichtet, dass das Zet Casino an der Behebung dieser Störungen arbeitet und versucht, die Spieler zufrieden zu stellen. Es ist wichtig, dass das Casino transparent mit den Nutzern kommuniziert und sie über den Fortschritt bei der Fehlerbehebung informiert.
Insgesamt ist das Zet Casino eine beliebte Plattform für Online-Glücksspiele, die eine Vielzahl von Spielen und Bonusangeboten für die Spieler bietet. Trotz einiger Störungen sollten die Spieler darauf vertrauen können, dass das Casino diese Probleme schnell und effizient löst, um ein reibungsloses Spielerlebnis zu gewährleisten.
https://zetcasino.one/
Здравствуйте всем присутствующим! Мне бы хотелось поделиться моим опытом пользования сайта azino. Здесь вы найдёте широкий выбор развлечений, с включением слоты, карточные игры и рулетку. Интерфейс сайта интуитивно понятный, что делает процесс игры удобным и забавным. Особо порадовали быстрые и достоверные методы внесения средств и вывода средств. Казино также предлагает превосходные бонусы для новых и постоянных игроков. Поддержка всегда на контакте и подготовлена помочь разобраться с любые проблемы. Но помните о рисках, участвуя в игры на удачу. Везения всем участникам!
Здравствуйте всем присутствующим! Хочу рассказать своим опытом пользования сайта 1xbet слоты официальный сайт. В этом месте вы найдёте большой выбор развлечений, включая слоты, карточные игры и рулетку. Оформление сайта понятный, что превращает процесс игры удобным и приятным. В особенности понравились быстрые и надёжные методы внесения средств и вывода средств. Казино ещё предлагает превосходные бонусы для начинающих и постоянных игроков. Служба поддержки всегда на контакте и готова помочь разобраться с любые проблемы. Но помните о рисках, играя в игры на удачу. Везения всем!
Ice Casino Hungary is a genuine gem for all virtual casino fan. As a person who loves the adventure of web gaming, I was delightfully taken aback by the avalanche of generous bonuses this site offers. From the instant I enrolled, the welcome perk elevated my cash notably. What differentiates https://icecasino.hu.net/regisztracio/ is its ongoing loyalty to players – from refund perks to stimulating offers, it’s a continuous celebration. The gaming catalog is striking, featuring a range of slots and table games that maintain me amused for extended periods. Plus, their smartphone-compatible layout confirms gambling on the go is simple. If you’re looking for a excellent web-based casino adventure with plentiful perks, IceCasino Hungary is the location to be. Don’t neglect your occasion to take part in on the frosty amusement and prevail big!
Сайт, где я нашел раковина мойка для ванной комнаты.
ремонт ноутбуков
ремонт ноутбука
ремонт сотовых телефонов в москве
ремонт телефонов
срочный ремонт телефонов москва
Online Casinos sind heutzutage sehr beliebt und bieten eine Vielzahl von Spielen fГјr Spieler aller Art. Eines dieser Online Casinos ist Zet Casino, das eine Vielzahl von Spielen und Boni fГјr seine Spieler bietet.
Zet Casino wurde im Jahr 2018 gegrГјndet und hat sich seitdem zu einer beliebten Online-GlГјcksspielseite entwickelt. Das Casino bietet eine groГџe Auswahl an Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr.
Ein großer Vorteil von Zet Casino ist, dass es sowohl auf Desktop- als auch auf mobilen Geräten gespielt werden kann. Dies bedeutet, dass Spieler ihre Lieblingsspiele überall und jederzeit genießen können, solange sie eine Internetverbindung haben.
Das Casino bietet außerdem großzügige Boni und Promotionen für neue und bestehende Spieler an. Dies kann in Form von Einzahlungsboni, Freispielen oder Cashback-Angeboten erfolgen. Spieler können auch am Treueprogramm teilnehmen, um zusätzliche Belohnungen zu erhalten.
Zet Casino verfügt über eine gültige Glücksspiellizenz und verwendet die neueste SSL-Verschlüsselungstechnologie, um die Sicherheit der Spieler zu gewährleisten. Dies bedeutet, dass Spieler ihre persönlichen und finanziellen Informationen ohne Bedenken preisgeben können.
Insgesamt bietet Zet Casino ein unterhaltsames und sicheres Spielerlebnis fГјr alle, die gerne in Online-Casinos spielen. Mit einer groГџen Spielauswahl, groГџzГјgigen Boni und einer benutzerfreundlichen Plattform ist Zet Casino definitiv einen Besuch wert.
https://zetcasino.one/
First of all, it should be clearly understood that these are uquest.net completely different concepts in geography. For example, when considering absolute height, it is precisely this that acts as the most important indicator, which is measured in meters, thereby determining the height of geographical objects above sea level.
As for relative height, it is usually measured in meters plitki.com. Moreover, it is worth noting that it is precisely this that will show the difference between the absolute height of geographical objects, as well as the height of the terrain. If the mountain has an absolute height of 2000 meters, but the surrounding area is located at an altitude of 1000 meters, then as for the comparative height of the mountain, it will be 1000 meters.
Safety standards must be followed when working everbestnews.com with metal. Use protective equipment, use tools and equipment according to the rules so as not to encounter difficulties.
Tipico Wetten gegen Casino – Ein spannender Vergleich
Das Glücksspiel erfreut sich weltweit großer Beliebtheit und bietet den Spielern die Möglichkeit, ihr Glück zu versuchen und dabei auch noch Geld zu gewinnen. Zwei der bekanntesten Formen des Glücksspiels sind Sportwetten und Casinospiele. In diesem Artikel werden wir die Vor- und Nachteile von Tipico Wetten gegen das Casino genauer unter die Lupe nehmen.
Tipico ist ein bekannter Anbieter von Sportwetten, der seinen Kunden die Möglichkeit bietet, auf eine Vielzahl von Sportereignissen zu wetten. Dabei können die Spieler auf verschiedene Sportarten wie Fußball, Tennis, Basketball und viele mehr setzen. Der Vorteil von Sportwetten liegt darin, dass die Spieler ihr Fachwissen zu bestimmten Sportarten und Mannschaften nutzen können, um die Gewinnchancen zu erhöhen. Zudem können die Quoten bei Sportwetten vielversprechend sein und hohe Gewinne ermöglichen.
Im Gegensatz dazu bietet ein Casino eine Vielzahl von Spielen wie Roulette, Blackjack, Spielautomaten und Poker an. Der Vorteil eines Casinos liegt darin, dass die Spiele rein auf GlГјck basieren und es keine vorherige Kenntnisse oder Erfahrungen braucht, um zu gewinnen. Zudem bieten Casinos oft attraktive Boni und Promotionen, um die Spieler anzulocken.
Ein wichtiger Aspekt, den es zu beachten gilt, ist das Risiko bei beiden Formen des Glücksspiels. Bei Sportwetten kann das Risiko durch die Analyse von Statistiken und Informationen minimiert werden, während im Casino das Glück eine größere Rolle spielt und das Risiko höher sein kann.
Zusammenfassend lässt sich sagen, dass sowohl Tipico Wetten als auch Casinospiele ihre eigenen Vor- und Nachteile haben. Es kommt letztendlich auf die persönlichen Vorlieben und das Glück des Spielers an, welche Form des Glücksspiels bevorzugt wird. Es ist wichtig, verantwortungsbewusst zu spielen und sein Spielverhalten im Auge zu behalten, um negative Auswirkungen zu vermeiden.
https://tipicocasino.one/
Customers receive products not only from the IT sector. They must provide krepezh.net high-quality services at every stage of interaction with cloud solutions.
Сайт, где мне посоветовали комод для ванной комнаты напольный без раковины для ванной комнаты.
A person can set up the system on his own or sveto-copy.com contact an organization to use the feature, focusing on his product.
Boomerang Casino App: Ein neues Spielerlebnis auf Ihrem Smartphone
Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die jetzt auch als App für Ihr Smartphone verfügbar ist. Mit der Boomerang Casino App können Sie Ihre Lieblingsspiele überall und jederzeit spielen, ohne an einen Computer gebunden zu sein. Die App bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Dealer-Spiele, die alle von führenden Softwareanbietern entwickelt wurden.
Die Benutzeroberfläche der Boomerang Casino App ist benutzerfreundlich und einfach zu navigieren. Sie können ganz einfach zwischen den verschiedenen Spielen wechseln und schnell auf Ihr Spielerkonto zugreifen. Die App bietet auch eine Vielzahl von Zahlungsmethoden, um Ein- und Auszahlungen bequem und sicher durchzuführen.
Ein weiterer großer Vorteil der Boomerang Casino App sind die regelmäßigen Bonusangebote und Aktionen, die den Spielern zusätzliche Gewinnchancen bieten. Von Willkommensboni über Freispiele bis hin zu Cashback-Angeboten gibt es immer etwas Neues, um Ihre Spielerfahrung aufregender zu gestalten.
Die Boomerang Casino App ist sowohl für iOS- als auch für Android-Betriebssysteme verfügbar und kann kostenlos im App Store oder Google Play Store heruntergeladen werden. Wenn Sie ein Fan von Online-Glücksspielen sind und die Flexibilität haben möchten, überall und jederzeit zu spielen, dann ist die Boomerang Casino App definitiv einen Versuch wert. Probieren Sie es aus und erleben Sie ein neues Spielerlebnis auf Ihrem Smartphone!
https://boomerangcasino.one/
look at this site https://kombonovaya2.com/
Zet Casino: Kostenlose Freispiele im Casino
Zet Casino ist eine der beliebtesten Online-Glücksspielseiten, die unglaubliche Unterhaltung anbietet. Das Casino ist bekannt für seine großzügigen Boni und Aktionen, darunter auch kostenlose Freispiele. Diese Freispiele sind eine großartige Möglichkeit für Spieler, um einige der aufregendsten Spielautomaten im Casino zu genießen, ohne dabei ihr eigenes Geld verwenden zu müssen.
Zet Casino bietet regelmäßig neue Promotionen an, bei denen Spieler kostenlose Freispiele als Belohnung erhalten können. Diese Freispiele können auf ausgewählten Spielautomaten eingesetzt werden und bieten die Chance, echtes Geld zu gewinnen, ohne dabei eigenes Geld riskieren zu müssen.
Spieler können sich für die kostenlosen Freispiele qualifizieren, indem sie bestimmte Anforderungen erfüllen, wie z.B. eine Mindesteinzahlung tätigen oder an ausgewählten Spielen spielen. Die Freispiele werden dann automatisch dem Spielerkonto gutgeschrieben und können sofort verwendet werden.
Die Auswahl an Spielautomaten, auf denen die kostenlosen Freispiele eingesetzt werden kГ¶nnen, ist bei Zet Casino umfangreich. Spieler kГ¶nnen aus Hunderten von verschiedenen Spielen wГ¤hlen, darunter beliebte Titel wie Starburst, Book of Dead, Gonzo’s Quest und viele mehr.
Zet Casino legt großen Wert auf Fairness und Transparenz, daher sind die Bedingungen für die kostenlosen Freispiele klar und leicht verständlich. Spieler können sich darauf verlassen, dass sie bei Zet Casino eine sichere und vertrauenswürdige Spielumgebung vorfinden.
Wenn Sie also Lust haben, einige der besten Online-Spielautomaten zu spielen, ohne dabei Ihr eigenes Geld zu riskieren, dann sollten Sie unbedingt die kostenlosen Freispiele bei Zet Casino in Anspruch nehmen. Melden Sie sich noch heute an und profitieren Sie von den groГџzГјgigen Angeboten und Promotionen des Casinos. Viel SpaГџ und viel GlГјck beim Spielen bei Zet Casino!
https://zetcasino.one/
Zet Casino Online: Eine innovative Plattform fГјr Spieler
Das Online-Casino Zet Casino hat in den letzten Jahren viel Aufmerksamkeit auf sich gezogen. Nicht nur wegen seines umfangreichen Spielangebots, sondern auch aufgrund der professionellen Entwicklung seiner Plattform. Die Entwickler von Zet Casino haben hart gearbeitet, um eine benutzerfreundliche und innovative Spielerfahrung zu schaffen.
Die Webseite von Zet Casino ist modern und gut strukturiert, was es den Spielern leicht macht, sich zu orientieren und ihre Lieblingsspiele zu finden. Die Spiele sind in verschiedene Kategorien unterteilt, darunter Spielautomaten, Tischspiele, Live-Casino und Jackpot-Spiele. DarГјber hinaus bietet Zet Casino eine Vielzahl von Boni und Aktionen fГјr neue und bestehende Spieler, um ihr Spielerlebnis noch unterhaltsamer zu gestalten.
Die Entwickler von Zet Casino haben auch Wert darauf gelegt, dass die Plattform sicher und zuverlässig ist. Die Spiele werden regelmäßig auf Fairness überprüft und die Webseite ist mit modernster Technologie verschlüsselt, um sicherzustellen, dass die persönlichen Daten der Spieler geschützt sind.
Ein weiterer Vorteil von Zet Casino ist die mobile Version der Webseite, die es den Spielern ermöglicht, ihre Lieblingsspiele auch unterwegs zu genießen. Die mobile Version ist genauso benutzerfreundlich und bietet eine große Auswahl an Spielen.
Insgesamt bietet Zet Casino eine erstklassige Spielerfahrung für alle Arten von Spielern. Die Entwickler haben einen großartigen Job gemacht, eine Plattform zu schaffen, die sowohl unterhaltsam als auch sicher ist. Wenn Sie auf der Suche nach einem zuverlässigen und innovativen Online-Casino sind, dann sollten Sie Zet Casino auf jeden Fall eine Chance geben.
https://zetcasino.one/
A ticket is an application of requests balforum.net that is registered by support services. The ticket system is an advanced tool that automates the operation of various services. Solutions relevant for registration, as well as processing customer requests.
Economics of personal time. While the employees are cleaning poiskmonet.com, the customer can fully relax or assign additional work.
To speed up the search according to the parameters required by the user politeconomics.org, the site page has a filter system that allows you to select tours based on the following indicators.
Selecting and comparing offers is quick and easy mmo5.info. The site allows you to set the issue according to an economical, optimal or luxury vacation option. For families, couples, or companies, you can choose your own tour options, where you can accurately calculate all the parameters and determine the cost of travel for everyone or for one person.
Tipico ist vielen Menschen bekannt als eine der größten Sportwettenanbieter in Deutschland. Doch wussten Sie auch, dass Tipico ein Online Casino betreibt? In diesem Artikel wollen wir uns genauer mit dem Tipico Online Casino befassen und wie Sie den Kundendienst kontaktieren können.
Das Tipico Online Casino bietet eine Vielzahl von Spielen an, darunter Slots, Tischspiele und Live-Casino-Spiele. Die Spieler haben die Möglichkeit, sowohl auf dem PC als auch auf mobilen Geräten zu spielen, was für eine flexible Nutzung sorgt.
Wenn Sie Fragen oder Probleme beim Spielen im Tipico Online Casino haben, können Sie den Kundendienst kontaktieren. Es gibt mehrere Möglichkeiten, um mit dem Support-Team in Kontakt zu treten, darunter per E-Mail, Live-Chat und Telefon.
Um den Kundendienst per Telefon zu kontaktieren, können Sie die gebührenfreie Nummer 0800 5023387 wählen. Der Kundendienst ist täglich von 8:00 bis 23:00 Uhr erreichbar und steht Ihnen gerne zur Verfügung, um Ihre Fragen zu beantworten und Probleme zu lösen.
Egal, ob es um technische Probleme, Bonusangebote oder Spielregeln geht, das Team des Tipico Online Casinos ist bestrebt, Ihnen zu helfen und Ihnen ein angenehmes Spielerlebnis zu bieten.
Insgesamt bietet das Tipico Online Casino eine große Auswahl an Spielen, einen zuverlässigen Kundendienst und eine benutzerfreundliche Plattform. Wenn Sie also Lust auf spannende Casino-Spiele haben, probieren Sie das Tipico Online Casino aus und nutzen Sie die verschiedenen Kontaktmöglichkeiten, um bei Fragen oder Problemen Hilfe zu erhalten.
https://tipicocasino.one/
naoni.info
audio-kravec.com
Tipico ist ein beliebter Anbieter von Sportwetten und Online-Casinospielen, der es den Spielern ermöglicht, ihr Glück bei verschiedenen Spielen zu versuchen. Viele Menschen fragen sich, ob es möglich ist, Geld von Tipico Sportwetten auf das Casino zu übertragen.
Die Antwort lautet ja, es ist möglich, Geld von Tipico Sportwetten auf das Casino zu überweisen. Dies kann auf verschiedene Weisen geschehen, zum Beispiel durch die Verwendung einer gemeinsamen Geldbörse oder durch manuelles Übertragen des Geldes von einem Konto zum anderen.
Es ist wichtig zu beachten, dass es möglicherweise einige Regeln und Einschränkungen gibt, wenn es darum geht, Geld von Sportwetten auf das Casino zu übertragen. Beispielsweise können manche Boni nur für bestimmte Spiele oder Sportwetten verwendet werden und können nicht auf das Casino übertragen werden.
Wenn Sie Geld von Tipico Sportwetten auf das Casino übertragen möchten, sollten Sie sich daher am besten vorher über die genauen Regeln und Bedingungen informieren. Auf der Website von Tipico finden Sie alle notwendigen Informationen dazu.
Alles in allem ist es also durchaus möglich, Geld von Tipico Sportwetten auf das Casino zu überweisen. Mit einem verantwortungsvollen Umgang und der Einhaltung der Regeln können Sie Ihr Glück bei verschiedenen Spielen versuchen und hoffentlich hohe Gewinne erzielen. Viel Spaß und Erfolg beim Spielen!
https://tipicocasino.one/
biznesnewss.com
auto-kar.net
Добрый день, приятели! Стремлюсь рассказать собственными ощущениями о клубе unlim casino войти. Этот сайт прямо впечатляет различием проектов и особенной обстановкой риска! Превосходная визуализация, мгновенные выплаты и привлекательные подарки создают процесс азарта неизгладимым. Интегральная развлечение и высокий степень безопасности — вот то, какое вдохновляет меняет возращаться повторно. Рекомендую каждому, кто ценит качественный отдых и большие выигрыши
Добрый день, друзья! Стремлюсь рассказать собственными ощущениями о казино unlim casino промокод. Этот портал напросто удивляет разнообразием проектов и неповторимой атмосферой риска! Великолепная визуализация, быстрые вознаграждения и заманчивые бонусы делают игровой процесс неповторимым. Честная забава и высокий класс секретности — таково то, какое вдохновляет меняет приходить снова повторно. Предлагаю всем, кто ценит качественный отдыхание и крупные награды
Официальный веб-сайт казино Рояль предлагает располагающую обстановку для поклонников азартных игр. С его элегантным дизайном и элитным выбором игр, Рояль является идеальным местом для тех, кто ценит качественное азартное развлечение. Исследуйте разнообразный выбор игровых автоматов и настольных игр на авторизованном веб-сайте казино рояль официальный сайт.
Казино Рояль гарантирует высокий уровень клиентов и поддержку. Поддерживающая команда поддержки доступна круглосуточно, готова ответить на любые вопросы и урегулировать проблемы, предоставляя безпрерывную игру и удовлетворение.
“Казино Вулкан – это захватывающий мир азарта, который завораживает с первого взгляда. Благодаря прекрасному дизайну и интуитивно понятному интерфейсу, пользователи быстро оказываются в этом игровом пространстве.
Среди плюсов казино https://vulcangold.org/online-casino можно выделить обширный выбор игр, включая гральные слоты и настольные азартные игры, которые понравятся каждому игроку. Качество графического дизайна и анимационных эффектов делает игровой процесс еще увлекательным и захватывающим.
Однако больше всего зацепил подход казино к безопасности игроков. Они используют современные разработки шифрования, чтобы обеспечить конфиденциальность личных и финансовых данных пользователей. Это делает казино Вулкан оптимальным вариантом для онлайн-игры.”
Ресурс, где можно купить стильные раковина под машинку по выгодным ценам.
“Ваш предпочтение для азартных игр – казино Слотозал!
Слотозал предлагает обширный выбор игровых автоматов, лучшие бонусы и высокий уровень безопасности. Интерфейс веб-сайта интуитивно понятен, навигация удобна, что способствует быстро отыскать предпочтенные игры. Команда поддержки непрерывно настроена содействовать с всеми вопросами. Пройдите регистрацию на законном сайте официальный сайт и начните побеждать сегодня!”
купить шпунт л5 ум https://shpuntmaster.ru/
Boomerang Casino ist ein beliebtes Online-Casino, das Spielern eine Vielzahl von Spielmöglichkeiten bietet. In diesem Artikel werfen wir einen Blick auf die verschiedenen Aspekte des Boomerang Casinos und geben eine ausführliche Bewertung.
Das Boomerang Casino wurde im Jahr 2020 gegrГјndet und ist Teil der Araxio Development N.V. Gruppe. Das Casino ist in Curacao lizenziert und bietet eine Vielzahl von Spielen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming, Play’n GO und vielen anderen.
Eines der Hauptmerkmale des Boomerang Casinos ist das attraktive Willkommenspaket, das neuen Spielern bis zu 500 Euro Bonus und 200 Freispiele bietet. Der Bonus unterliegt jedoch bestimmten Umsatzbedingungen, die vor einer Auszahlung erfГјllt werden mГјssen.
Das Casino bietet eine breite Palette von Spielen, darunter Spielautomaten, Tischspiele, Live-Casino und Jackpot-Spiele. Die Spielautomaten machen den größten Teil des Spieleangebots aus, und Spieler kГ¶nnen aus Hunderten von Titeln wГ¤hlen, darunter beliebte Spiele wie Starburst, Gonzo’s Quest und Book of Dead.
Das Live-Casino bietet eine authentische Casino-Erfahrung mit Spielen wie Roulette, Blackjack, Baccarat und Poker, die von professionellen Dealern geleitet werden. Spieler können mit anderen Spielern und den Dealern interagieren und in Echtzeit spielen.
Ein weiterer positiver Aspekt des Boomerang Casinos ist die Vielzahl von Zahlungsmethoden, die Spielern zur Verfügung stehen. Spieler können Ein- und Auszahlungen mit Kreditkarten, E-Wallets, Banküberweisungen und sogar Kryptowährungen vornehmen.
Zusammenfassend lässt sich sagen, dass das Boomerang Casino eine gute Wahl für Spieler ist, die eine vielfältige Auswahl an Spielen, attraktive Boni und eine benutzerfreundliche Plattform suchen. Mit seiner breiten Palette von Spielen, sicheren Zahlungsmethoden und professionellem Kundenservice bietet das Boomerang Casino ein unterhaltsames und lohnendes Spielerlebnis.
https://boomerangcasino.one/
Zet Casino Auszahlung Funktioniert nicht
Zet Casino ist ein Online-Glücksspielanbieter, der bei vielen Spielern beliebt ist. Doch in letzter Zeit häufen sich Beschwerden über Probleme bei der Auszahlung von Gewinnen. Viele Spieler berichten, dass sie Schwierigkeiten haben, ihre erspielten Beträge auf ihr Bankkonto zu transferieren.
Ein häufiges Problem, das dabei auftritt, ist die Verzögerung bei der Auszahlung. Spieler müssen oft mehrere Tage oder sogar Wochen warten, bis ihr Gewinn gutgeschrieben wird. Dies führt natürlich zu Frustration und Unzufriedenheit bei den Kunden.
Ein weiteres Problem ist, dass manche Spieler angaben, dass ihre Auszahlungsanträge ohne ersichtlichen Grund abgelehnt wurden. Dies kann verschiedene Ursachen haben, wie etwa fehlende Dokumente oder technische Probleme. Aber oft bleiben die Gründe unklar und die Spieler sind überrascht und verärgert über die Ablehnung.
Es ist wichtig, dass Online-Casinos wie Zet Casino ihren Kunden eine reibungslose und transparente Auszahlungsprozedur bieten. Spieler sollten in der Lage sein, ihre Gewinne einfach und schnell zu erhalten, ohne auf Hindernisse zu stoГџen.
Wenn Spieler Probleme bei der Auszahlung haben, ist es ratsam, sich umgehend an den Kundenservice von Zet Casino zu wenden. Dort können sie ihr Anliegen schildern und Unterstützung bei der Lösung des Problems erhalten.
Insgesamt ist es wichtig, dass Online-Glücksspielanbieter wie Zet Casino sicherstellen, dass ihre Auszahlungsprozesse reibungslos funktionieren und die Spieler zufrieden sind. Denn nur so können sie langfristig erfolgreich sein und das Vertrauen ihrer Kunden gewinnen.
https://zetcasino.one/
Привет, приятели! Желаю обмениваться собственными эмоциями о клубе официальный. сайт. казино.. Этот портал напросто впечатляет разнообразием экспериментов и особенной атмосферой волнения! Отличная графика, мгновенные вознаграждения и привлекательные премии создают процесс игры неизгладимым. Интегральная забава и повышенный степень защищенности — это то, что вдохновляет передвигает возращаться еще раз. Советую всему миру, тем ценит высококачественный передышку и массивные призы
africanownews.com
219news.com
лечение алкоголизма недорого https://e-skoraya.kz/
Simply want to say your article is as astounding. The clarity in your post is just cool and i could assume you’re an expert on this subject. Well with your permission allow me to grab your feed to keep up to date with forthcoming post. Thanks a million and please continue the enjoyable work.
https://doramafilm.cc/
Междугородние такси Магнитогорск – Междугородние такси Магнитогорск, Пассажирские перевозки Набережные Челны
Интернет-ресурс, где можно купить элегантные раковины cersanit colour от ведущих производителей.
Das tipico Casino gehört zu den bekanntesten Online-Casinos in Deutschland. Doch was, wenn man Fragen oder Probleme hat? In diesem Fall ist es wichtig, den richtigen Kontakt zum tipico Casino zu finden.
Das tipico Casino bietet verschiedene Möglichkeiten, um mit dem Kundenservice in Kontakt zu treten. Eine Möglichkeit ist der Live-Chat, der auf der Webseite verfügbar ist. Hier kann man direkt mit einem Mitarbeiter chatten und Fragen stellen. Der Live-Chat ist in der Regel schnell und unkompliziert und eignet sich gut, um Probleme schnell zu lösen.
Eine weitere Möglichkeit, um Kontakt zum tipico Casino aufzunehmen, ist die telefonische Hotline. Über die Hotline kann man ebenfalls Fragen stellen oder Probleme melden. Die Mitarbeiter sind in der Regel freundlich und kompetent und stehen den Kunden mit Rat und Tat zur Seite.
FГјr schriftliche Anfragen bietet das tipico Casino zudem ein Kontaktformular auf der Webseite an. Hier kann man sein Anliegen formulieren und bekommt in der Regel innerhalb kurzer Zeit eine Antwort.
Insgesamt bietet das tipico Casino also verschiedene Möglichkeiten, um mit dem Kundenservice in Kontakt zu treten. Ob per Live-Chat, telefonischer Hotline oder Kontaktformular – für jedes Anliegen gibt es die passende Kontaktmöglichkeit. Somit steht dem Spielspaß im tipico Casino nichts im Wege.
https://tipicocasino.one/
[url=https://t.me/modeli_individyalki_moskvy]Vip индивидуалки москва[/url] – Эскорт Услуги Москва, Досуг для мужчин Москва
https://satbayev.university/
починить телефон
Tipico Guthaben auf Casino
Wenn es um Online-Glücksspiele geht, ist Tipico eines der bekanntesten und beliebtesten Online-Casinos in Deutschland. Das Casino bietet eine Vielzahl von Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr. Ein wichtiger Aspekt des Spiels bei Tipico ist das Guthaben, das Spieler nutzen können, um Einsätze zu platzieren und an Spielen teilzunehmen.
Das Guthaben auf dem Tipico Casino Konto kann auf verschiedene Weise aufgeladen werden. Eine der einfachsten Methoden ist die Verwendung von Kreditkarten wie Visa und MasterCard. Spieler können auch mit verschiedenen E-Wallets wie PayPal, Skrill und Neteller einzahlen. Darüber hinaus bietet Tipico auch die Möglichkeit, per Banküberweisung oder Paysafecard einzuzahlen.
Sobald das Guthaben auf dem Casino-Konto gutgeschrieben wurde, haben Spieler die Möglichkeit, an ihren Lieblingsspielen teilzunehmen und echte Gewinne zu erzielen. Das Guthaben kann auch für Boni und Promotionen verwendet werden, die von Tipico regelmäßig angeboten werden. Diese Boni können zusätzliches Guthaben, Freispiele oder andere attraktive Angebote beinhalten, die das Spielerlebnis noch spannender machen.
Es ist wichtig zu beachten, dass Spieler verantwortungsbewusst mit ihrem Guthaben umgehen sollten. Glücksspiel sollte immer als Unterhaltung betrachtet werden und Spieler sollten niemals mehr Geld einsetzen, als sie sich leisten können zu verlieren. Tipico bietet verschiedene Möglichkeiten zur Selbstregulierung, wie zum Beispiel Einzahlungslimits und Selbstausschluss, um sicherzustellen, dass Spieler ihre Gewohnheiten im Auge behalten.
Insgesamt bietet das Tipico Casino eine sichere und unterhaltsame Umgebung für Glücksspiele. Mit verschiedenen Einzahlungsmethoden, spannenden Spielen und attraktiven Boni ist das Casino eine beliebte Wahl für Spieler in Deutschland. Egal, ob man Anfänger oder erfahrener Spieler ist, Tipico bietet für jeden etwas und sorgt für ein erstklassiges Spielerlebnis.
https://tipicocasino.one/
ремонт телефонов
Zet Casino bietet seinen Spielern eine Vielzahl von MГ¶glichkeiten, um ihre Gewinne abzuheben. Die “zet casino kotiutus” oder Auszahlungsoption ist einfach und bequem und ermГ¶glicht es den Spielern, ihre Gewinne schnell und unkompliziert zu erhalten.
Um eine Auszahlung bei Zet Casino zu tätigen, müssen Spieler zunächst sicherstellen, dass sie über ausreichendes Guthaben auf ihrem Konto verfügen. Sobald dies der Fall ist, können sie auf ihr Konto zugreifen und den gewünschten Auszahlungsbetrag angeben. Spieler können zwischen verschiedenen Zahlungsmethoden wählen, darunter Kreditkarten, E-Wallets und Banküberweisungen.
Es ist wichtig zu beachten, dass bei der Auszahlung von Gewinnen bei Zet Casino bestimmte Bedingungen und Limits gelten können. Spieler sollten sich daher vor der Auszahlung über die entsprechenden Richtlinien informieren, um sicherzustellen, dass sie ihre Gewinne problemlos erhalten können.
Zet Casino ist bekannt für seine schnellen und zuverlässigen Auszahlungen, die es den Spielern ermöglichen, ihre Gewinne ohne Verzögerung zu erhalten. Mit einer Vielzahl von Zahlungsmethoden und einem effizienten Auszahlungssystem ist Zet Casino die ideale Wahl für alle, die nach einer zuverlässigen und benutzerfreundlichen Online-Casinoerfahrung suchen.
Insgesamt bietet Zet Casino eine herausragende Auszahlungsoption für Spieler, die ihre Gewinne schnell und unkompliziert erhalten möchten. Mit einer Vielzahl von Zahlungsmethoden und einem effizienten Auszahlungssystem ist Zet Casino die ideale Wahl für alle, die nach einer zuverlässigen Online-Casinoerfahrung suchen. Besuchen Sie noch heute Zet Casino und erleben Sie die Spannung des Gewinnens und die Bequemlichkeit der schnellen Auszahlungen.
https://zetcasino.one/
где можно отремонтировать телефон
ремонт телефонов рядом
ремонт смартфонов в москве
pronovosti.org
365newss.net
Das Boomerang Casino ist eine der neueren Online-GlГјcksspielplattformen, die in Deutschland immer beliebter werden. Doch viele Spieler fragen sich, ob diese Art von Casino in Deutschland Гјberhaupt legal ist.
Die Antwort darauf ist: Ja, das Boomerang Casino ist legal in Deutschland. Die Plattform verfГјgt Гјber eine gГјltige Lizenz der Malta Gaming Authority, was bedeutet, dass sie die strengen Richtlinien und Vorschriften fГјr GlГјcksspielanbieter einhalten. DarГјber hinaus ist das Boomerang Casino auch im Besitz einer Lizenz der Curacao eGaming Authority.
Spieler können also beruhigt sein, dass sie auf einer sicheren und legalen Online-Glücksspielplattform spielen. Das Boomerang Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Die Plattform arbeitet mit bekannten Spieleanbietern zusammen, um ihren Spielern ein erstklassiges Spielerlebnis zu bieten.
Das Boomerang Casino verfügt auch über eine Vielzahl von sicheren Ein- und Auszahlungsmethoden, um sicherzustellen, dass die Spieler ihre Gewinne schnell und problemlos erhalten können. Der Kundenservice steht ebenfalls rund um die Uhr zur Verfügung, um bei Fragen oder Problemen zu helfen.
Insgesamt ist das Boomerang Casino eine sichere und vertrauenswГјrdige Option fГјr Online-GlГјcksspieler in Deutschland. Mit einer gГјltigen Lizenz und einer Vielzahl von Spielen und Funktionen, die den Spielern zur VerfГјgung stehen, ist das Boomerang Casino eine gute Wahl fГјr diejenigen, die nach einer unterhaltsamen und sicheren GlГјcksspielplattform suchen.
https://boomerangcasino.one/
Bei Zet Casino gibt es immer wieder spannende Aktionen und Angebote fГјr die Spieler. Einer der beliebtesten ist der sogenannte “zet casino promГіciГіs kГіdod”, der es den Spielern ermГ¶glicht, sich zusГ¤tzliche Boni und VergГјnstigungen zu sichern.
Um den “zet casino promГіciГіs kГіdod” zu nutzen, mГјssen die Spieler einfach den entsprechenden Code eingeben, wenn sie eine Einzahlung tГ¤tigen. Dadurch erhalten sie zum Beispiel zusГ¤tzliches Bonusguthaben, Freispiele oder andere attraktive Extras. Diese Aktionen kГ¶nnen regelmäßig wechseln, daher lohnt es sich, immer mal wieder auf der Website von Zet Casino vorbeizuschauen, um keine der aktuellen Angebote zu verpassen.
Der “zet casino promГіciГіs kГіdod” ist eine tolle MГ¶glichkeit, um das Spielerlebnis bei Zet Casino noch spannender und abwechslungsreicher zu gestalten. Wer gerne mit zusГ¤tzlichen Boni und VergГјnstigungen spielt, sollte sich diese Aktionen auf keinen Fall entgehen lassen. Also nicht vergessen, den “zet casino promГіciГіs kГіdod” bei der nГ¤chsten Einzahlung einzugeben und von den attraktiven Extras zu profitieren!
https://zetcasino.one/
реабилитация игровой зависимости https://narcolog1.kz/
Pretty portion of content. I simply stumbled upon your weblog and in accession capital to say that I get actually loved account your weblog posts. Anyway I’ll be subscribing in your feeds and even I achievement you get entry to consistently rapidly.
http://www.lands-diploman.com
Сайт, где мои друзья заказывали раковина 40 40 для ванной комнаты.
Zet Casino ist ein Online-Casino, das im Jahr 2018 gegrГјndet wurde und seitdem eine Vielzahl von Spielen und Bonusangeboten fГјr seine Kunden anbietet. In diesem Artikel werden wir eine Bewertung des Zet Casinos vornehmen und seine Vor- und Nachteile betrachten.
Einer der größten Vorteile von Zet Casino ist die groГџe Auswahl an Spielen, die es seinen Kunden zur VerfГјgung stellt. Das Casino bietet Hunderte von Spielautomaten, Tischspielen und Live-Casino-Spielen von fГјhrenden Softwareanbietern wie NetEnt, Microgaming und Play’n GO. Dies sorgt fГјr eine abwechslungsreiche und unterhaltsame Spielerfahrung fГјr die Kunden.
Ein weiterer positiver Aspekt von Zet Casino sind die großzügigen Bonusangebote, die es seinen Spielern bietet. Neue Spieler erhalten einen Willkommensbonus, der Freispiele und Bonusgeld beinhaltet, und treue Spieler können von regelmäßigen Promotionen und Belohnungen profitieren. Dies trägt dazu bei, dass die Spieler länger im Casino bleiben und mehr Spaß haben.
Darüber hinaus bietet Zet Casino eine sichere und benutzerfreundliche Plattform für seine Kunden. Das Casino verfügt über eine gültige Lizenz und benutzt die neueste SSL-Verschlüsselungstechnologie, um sicherzustellen, dass die persönlichen Daten der Spieler geschützt sind. Die Website ist auch einfach zu navigieren und bietet eine Vielzahl von Zahlungsmethoden für die Kunden.
Ein potentieller Nachteil von Zet Casino ist, dass es in einigen Ländern eingeschränkt ist und Spieler aus bestimmten Regionen nicht akzeptiert. Dies kann frustrierend für Spieler sein, die gerne im Casino spielen möchten, aber aufgrund von rechtlichen Bestimmungen nicht die Möglichkeit dazu haben.
Insgesamt ist das Zet Casino eine gute Wahl für Spieler, die nach einer vielfältigen Auswahl an Spielen und großzügigen Bonusangeboten suchen. Mit einer sicheren und benutzerfreundlichen Plattform bietet das Casino ein erstklassiges Spielerlebnis für seine Kunden.
https://zetcasino.one/
Привет всем! Хочу рассказать своим опытом использования сайта казино лев бездепозитный бонус. Тут вы обнаружите широкий выбор развлечений, содержащий слоты, карточные игры и рулетку. Оформление сайта понятный, что совершает процесс игры удобным и забавным. Особо порадовали скорые и надёжные методы внесения средств и вывода средств. Казино ещё предлагает отличные бонусы для начинающих и постоянных игроков. Служба поддержки всегда на связи и готова помочь разобраться с любые проблемы. Но не забывайте о рисках, играя в азартные игры. Удачи всем участникам!
Сайт, где можно заказать практичные раковина черная накладная по выгодным ценам.
ремонт сотовых телефонов
In den letzten Jahren hat sich das Konzept des “Boomerang Casino Geld zurГјck” immer mehr etabliert. Dabei handelt es sich um eine besondere Form des Cashbacks, bei der Spieler einen Teil ihres verlorenen Geldes zurГјckerstattet bekommen.
Das Prinzip ist einfach: Wenn ein Spieler im Casino Geld verliert, erhält er einen bestimmten Prozentsatz davon als Cashback zurück. Dies kann je nach Angebot und Anbieter variieren, liegt in der Regel aber zwischen 5% und 20%.
Der Vorteil des Boomerang Casino Geld zurück ist, dass Spieler die Möglichkeit haben, ihre Verluste zu minimieren und ihre Gewinnchancen zu erhöhen. Dadurch können sie länger spielen und mehr Spaß am Spiel haben, ohne dabei große finanzielle Verluste zu erleiden.
Um von diesem Angebot zu profitieren, mГјssen Spieler in der Regel bestimmte Bedingungen erfГјllen, wie zum Beispiel eine Mindesteinzahlung oder bestimmte Umsatzbedingungen. Es lohnt sich daher, die genauen Konditionen im Vorfeld zu prГјfen.
Insgesamt ist das Boomerang Casino Geld zurück eine attraktive Möglichkeit für Spieler, ihre Verluste zu begrenzen und gleichzeitig die Chance auf Gewinne zu erhöhen. Durch die Rückzahlung eines Teils des verlorenen Geldes haben sie die Möglichkeit, länger im Casino zu spielen und mehr Spaß am Spiel zu haben.
https://boomerangcasino.one/
ремонт телефонов
Zet Casino: 10 Freispiele ohne Einzahlung
Das Zet Casino ist ein beliebtes Online-Casino, das seinen Spielern eine Vielzahl von groГџartigen Spielen und Bonusangeboten bietet. Eines der besten Angebote fГјr Neukunden ist der Zet Casino Bonus von 10 Freispielen ohne Einzahlung. Das bedeutet, dass neue Spieler sofort nach der Registrierung 10 kostenlose Spins erhalten, um die spannenden Spielautomaten des Casinos auszuprobieren.
Um die 10 Freispiele zu erhalten, müssen sich Spieler einfach auf der Website des Zet Casinos anmelden und ein Konto erstellen. Sobald das Konto aktiviert ist, werden die Freispiele automatisch gutgeschrieben und können sofort genutzt werden. Die Freispiele können für ausgewählte Spielautomaten verwendet werden, die eine Vielzahl von Themen und Funktionen bieten.
Die 10 Freispiele ohne Einzahlung sind eine großartige Möglichkeit, das Zet Casino kennenzulernen und erste Gewinne zu erzielen, ohne eigenes Geld riskieren zu müssen. Spieler haben die Chance, echte Geldpreise zu gewinnen, die sie dann für weitere Spiele im Casino verwenden können. Es lohnt sich also auf jeden Fall, von diesem großzügigen Angebot Gebrauch zu machen.
Zusätzlich zu den 10 Freispielen ohne Einzahlung bietet das Zet Casino auch einen lukrativen Willkommensbonus für die erste Einzahlung. Spieler können einen Bonus von bis zu 500€ sowie weitere Freispiele erhalten, die ihnen noch mehr Gewinnchancen bieten.
Insgesamt ist das Zet Casino eine erstklassige Online-GlГјcksspieldestination, die mit groГџartigen Spielen, groГџzГјgigen Boni und einem hervorragenden Kundenservice Гјberzeugt. Spieler, die auf der Suche nach einer unterhaltsamen und lohnenden Casinoerfahrung sind, sollten sich das Zet Casino nicht entgehen lassen.
https://zetcasino.one/
досуг для взрослых услуги – досуг для взрослых знакомства Москва, Девочка на час Москва
Междугородние такси Екатеринбург – Трансфер Нижний Новгород, Автобусы Челябинск
Tipico Casino: Willkommensbonus nach Einzahlung auszahlen lassen
Der Willkommensbonus im Tipico Casino gehört zu den attraktivsten Angeboten für Neukunden. Doch um den Bonus auszahlen zu lassen, müssen bestimmte Bedingungen erfüllt werden. Insbesondere geht es dabei um die Einzahlung auf das Spielerkonto.
Um den Willkommensbonus zu erhalten, muss zunächst eine Einzahlung auf das Tipico Casino Konto getätigt werden. Dabei gibt es verschiedene Zahlungsmethoden zur Auswahl, wie zum Beispiel Kreditkarte, PayPal oder Sofortüberweisung. Nach erfolgreicher Einzahlung wird der Willkommensbonus automatisch gutgeschrieben.
Damit der Bonus jedoch ausgezahlt werden kann, mГјssen bestimmte Umsatzbedingungen erfГјllt werden. Diese beinhalten in der Regel, dass der Bonusbetrag eine bestimmte Anzahl an Malen im Casino umgesetzt werden muss. Erst nach ErfГјllung dieser Bedingungen kann der Bonus und eventuelle Gewinne ausbezahlt werden.
Es ist wichtig, die Umsatzbedingungen genau zu überprüfen, um keine bösen Überraschungen zu erleben. Zudem sollte man darauf achten, dass der Bonus innerhalb eines bestimmten Zeitraums umgesetzt werden muss, da er sonst verfällt.
Zusammenfassend lässt sich sagen, dass der Willkommensbonus im Tipico Casino eine attraktive Möglichkeit ist, um das Spielerkonto aufzustocken. Wer jedoch plant, den Bonus auszahlen zu lassen, sollte sich im Vorfeld über die Umsatzbedingungen informieren und diese erfüllen. Nur so steht einer Auszahlung nichts im Wege und man kann die Gewinne genießen.
https://tipicocasino.one/
Zet Casino Auszahlungslimit
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und groГџzГјgigen Bonusangeboten fГјr seine Kunden bietet. Wenn es jedoch um Auszahlungen geht, gibt es bestimmte Limitierungen, die Spieler beachten mГјssen.
Das Auszahlungslimit bei Zet Casino beträgt 10.000 Euro pro Monat. Das bedeutet, dass Spieler während eines Monats nicht mehr als 10.000 Euro aus ihrem Konto abheben können. Diese Limitierung kann für einige Spieler frustrierend sein, vor allem wenn man größere Gewinne erzielt.
Es ist wichtig zu beachten, dass das Auszahlungslimit nicht für progressive Jackpots gilt. Wenn ein Spieler einen progressiven Jackpot knackt, wird der volle Betrag sofort ausgezahlt, unabhängig von der Höhe des Jackpots.
Um das Auszahlungslimit zu umgehen, können Spieler ihre Auszahlungen aufteilen und in mehreren Transaktionen tätigen. Dies bedeutet, dass sie innerhalb eines Monats mehrere Auszahlungen von jeweils bis zu 10.000 Euro vornehmen können.
Zet Casino bietet auch High Roller Spielern die Möglichkeit, individuelle Auszahlungslimits zu vereinbaren. Wenn ein Spieler regelmäßig hohe Beträge gewinnt und auszuzahlen möchte, kann er sich an den Kundensupport wenden und ein höheres Auszahlungslimit beantragen.
Insgesamt ist das Auszahlungslimit bei Zet Casino eine Standardpraxis in der Online-Casino-Branche und dient dazu, die finanzielle Sicherheit des Casinos und der Spieler zu gewährleisten. Es ist wichtig, die Bedingungen und Limitierungen des Casinos zu kennen, um Enttäuschungen zu vermeiden.
Wenn Spieler das Auszahlungslimit bei Zet Casino im Auge behalten und ihre Auszahlungen entsprechend planen, können sie weiterhin die aufregenden Spiele und möglichen Gewinne des Casinos genießen.
https://zetcasino.one/
Conventionally, forklifts can be divided domstroi.info into manual and self-propelled. The manual version must be moved by the operator, which may require some effort if the weight of the load exceeds a thousand kilograms. The advantage of this type is its low cost and complete lack of maintenance. However, such a loader will not lift the load to too great a height.
ukrtvoru.info
repair of appliances
Der tipico Xmas Spin Casino Code bietet den Spielern die Möglichkeit, sich während der festlichen Jahreszeit zusätzliche Gewinne zu sichern. Mit diesem speziellen Code können Spieler an verschiedenen Weihnachts-Spielautomaten teilnehmen und sich für tolle Preise qualifizieren.
Der Code ist eine großartige Möglichkeit, um zusätzliche Spannung und Spaß in die Feiertage zu bringen. Die Spieler haben die Möglichkeit, an verschiedenen Weihnachts-Slots zu spielen und sich für tolle Belohnungen zu qualifizieren. Es ist eine großartige Gelegenheit, um Ihre Lieblingsspiele zu genießen und gleichzeitig die Chance zu haben, zusätzliche Gewinne zu erzielen.
Um den tipico Xmas Spin Casino Code zu erhalten, müssen die Spieler sich einfach auf der Website anmelden und den Code eingeben. Sobald sie den Code aktiviert haben, können sie sofort mit dem Spielen beginnen. Die Code-Aktion ist zeitlich begrenzt, also sollten die Spieler nicht zu lange warten, um davon zu profitieren.
Die Weihnachtszeit ist eine Zeit, in der wir uns normalerweise zusammensetzen und Feiern genießen, aber warum nicht auch die Gelegenheit nutzen, um einige zusätzliche Gewinne zu erzielen? Der tipico Xmas Spin Casino Code bietet Spielern die Möglichkeit, genau das zu tun. Es ist eine großartige Gelegenheit, um die Feiertage noch aufregender zu gestalten und gleichzeitig die Chance zu haben, einige zusätzliche Gewinne zu erzielen.
Also, worauf warten Sie noch? Aktivieren Sie noch heute den tipico Xmas Spin Casino Code und genießen Sie die festliche Jahreszeit mit zusätzlichen Gewinnen!
https://tipicocasino.one/
Zet Casino Freispiele ohne Einzahlung
Das Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen für die Spieler anbietet. Eine großartige Möglichkeit, das Casino kennenzulernen und gleichzeitig die Chance auf hohe Gewinne zu haben, sind die Freispiele ohne Einzahlung.
Was sind Freispiele ohne Einzahlung? Bei Freispielen ohne Einzahlung erhalten die Spieler die Möglichkeit, an ausgewählten Spielautomaten kostenlos zu spielen, ohne eigenes Geld einzahlen zu müssen. Die Gewinne, die mit diesen Freispielen erzielt werden, können in der Regel behalten werden, jedoch unterliegen sie meist bestimmten Umsatzbedingungen.
Das Zet Casino bietet sowohl neuen als auch bestehenden Spielern regelmäßig Freispiele ohne Einzahlung an. Diese können zum Beispiel als Belohnung für eine Einzahlung, bei der Anmeldung oder als Teil eines speziellen Angebots vergeben werden. Die Spieler haben die Möglichkeit, ihre Lieblingsspiele zu spielen und dabei echtes Geld zu gewinnen, ohne dabei ihr eigenes Geld riskieren zu müssen.
Um von den Freispielen ohne Einzahlung im Zet Casino zu profitieren, müssen die Spieler lediglich ein Konto erstellen und gegebenenfalls einen Bonuscode eingeben, der die Freispiele freischaltet. Anschließend können die Spieler die Freispiele nutzen und hoffentlich gute Gewinne erzielen.
Es ist jedoch wichtig zu beachten, dass die Gewinne aus den Freispielen in der Regel bestimmten Umsatzbedingungen unterliegen, bevor sie ausgezahlt werden können. Diese Bedingungen variieren je nach Angebot und sollten vor der Nutzung der Freispiele sorgfältig gelesen werden.
Freispiele ohne Einzahlung im Zet Casino bieten eine großartige Möglichkeit, das Online-Casino kennenzulernen und gleichzeitig die Chance auf hohe Gewinne zu haben. Spieler sollten regelmäßig die Promotionsseite des Casinos besuchen, um über aktuelle Angebote informiert zu sein und keine Freispielangebote zu verpassen.
https://zetcasino.one/
Extra resources https://debank.lu/2023/11/11/debank-revolutionizes-defi-with-groundbreaking-innovations/
Visit Website https://tronlink.at/2023/11/13/exploring-tron-as-the-future-leading-cryptocurrency-and-its-value-in-usd/
ecobusinessdesign.com
women-art.net
click here to investigate https://debank.at/2023/11/11/expert-analysis-weighing-the-risks-and-rewards-of-investing-in-debank/
Das Meinsino Casino Tipico ist eine beliebte Online-Spielothek, die Spielern eine Vielzahl von Unterhaltungsoptionen bietet. Mit einer breiten Palette von Spielen, großzügigen Boni und einer benutzerfreundlichen Benutzeroberfläche hat das Meinsino Casino Tipico viel zu bieten.
Eines der herausragenden Merkmale des Meinsino Casino Tipico ist die Vielfalt der Spiele, die es seinen Kunden anbietet. Von klassischen Tischspielen wie Blackjack und Roulette bis hin zu aufregenden Spielautomaten und Live-Casino-Spielen – es gibt fГјr jeden etwas dabei. Die Spiele sind von fГјhrenden Softwareentwicklern wie NetEnt, Microgaming und Evolution Gaming bereitgestellt, was fГјr QualitГ¤t und Fairness steht.
Ein weiterer großer Anreiz für Spieler, das Meinsino Casino Tipico zu besuchen, sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler können einen Willkommensbonus erhalten, während Stammkunden von wöchentlichen Aktionen und Belohnungen profitieren können. Diese Boni sind eine großartige Möglichkeit, das Spielerlebnis zu verbessern und die Chancen auf Gewinne zu erhöhen.
Die Benutzeroberfläche des Meinsino Casino Tipico ist einfach zu bedienen und bietet eine nahtlose Spielerfahrung. Die Website ist gut strukturiert und intuitiv gestaltet, was es selbst Neulingen leicht macht, sich zurechtzufinden. Zudem ist das Casino mobiloptimiert, so dass Spieler auch unterwegs ihre Lieblingsspiele genießen können.
Insgesamt hat das Meinsino Casino Tipico viel zu bieten und ist definitiv einen Besuch wert. Mit einer Vielzahl von Spielen, großzügigen Boni und einer benutzerfreundlichen Benutzeroberfläche ist dieses Online-Casino eine gute Wahl für Spieler, die nach einer unterhaltsamen und lohnenden Spielerfahrung suchen.
https://tipicocasino.one/
my blog https://trezor-wallet.at/2023/11/14/introducing-the-upgraded-trezor-wallet-2023-advanced-security-features-and-sleek-design-enhancements/
ZET Casino ist ein Online-Casino, das eine Vielzahl von Spielen in deutscher Sprache anbietet. Um auf die Website zuzugreifen und zu spielen, müssen die Spieler sich zunächst einloggen. Dieser Artikel wird Ihnen zeigen, wie Sie sich bei ZET Casino auf Deutsch anmelden können.
Der erste Schritt besteht darin, die ZET Casino-Website aufzurufen. Г–ffnen Sie Ihren Webbrowser und geben Sie die URL http://www.zetcasino.com in die Adressleiste ein. Wenn die Website geladen ist, suchen Sie nach der SchaltflГ¤che “Anmelden” oder “Registrieren” und klicken Sie darauf.
Als nächstes werden Sie aufgefordert, Ihre Anmeldeinformationen einzugeben. Geben Sie Ihren Benutzernamen und Ihr Passwort ein, die Sie bei der Registrierung erstellt haben. Stellen Sie sicher, dass alle Informationen korrekt eingegeben sind, um Probleme beim Einloggen zu vermeiden.
Nachdem Sie Ihre Anmeldeinformationen eingegeben haben, klicken Sie auf die SchaltflГ¤che “Anmelden” und Sie sollten erfolgreich bei ZET Casino auf Deutsch eingeloggt sein. Sie kГ¶nnen nun eine Vielzahl von Spielen genieГџen, darunter Spielautomaten, Tischspiele, Live-Dealer-Spiele und vieles mehr.
Wenn Sie Probleme beim Einloggen haben, kann es hilfreich sein, den Kundensupport von ZET Casino zu kontaktieren. Sie können Ihnen bei der Lösung von Login-Problemen helfen und sicherstellen, dass Sie ein reibungsloses Spielerlebnis haben.
Insgesamt ist ZET Casino eine großartige Option für deutschsprachige Spieler, die eine breite Auswahl an Casinospielen genießen möchten. Durch die einfache Anmeldung und das benutzerfreundliche Interface ist es einfach, bei ZET Casino auf Deutsch online zu spielen. Probieren Sie es noch heute aus und erleben Sie die Spannung und den Nervenkitzel des Online-Glücksspiels. Viel Spaß beim Spielen und viel Glück!
https://zetcasino.one/
company website https://blur-io-nft.com/2023/11/09/mastering-the-latest-hair-trends-at-blur-barbershop/
בירושלים ולחברים כאחד. בין אם הם מחפשים דירות דיסקרטיות באשדוד עם נוחות, שיקול דעת או תשומת לב אישית, ללקוחות דירות דיסקרטיות בצורות ובהקשרים שונים ברחבי העולם ובחדרי דירות דיסקרטיות בתל אביב. כאן אנחנו מתעמקים במורכבויות דירות דיסקרטיות בקריות, באתגרים נערות ליווי עד הבית
click to read https://tronlink-app.org/2023/11/13/key-takeaways-from-coinbase-ceo-brian-armstrongs-experience-in-building-a-thriving-cryptocurrency-exchange/
Full Report https://trezorwallet-app.org/2023/11/14/the-usdt-usd-parity-exploring-the-facts-and-myths/
check this https://blur-nft-market.com/2023/11/10/a-detailed-guide-to-understanding-the-concept-of-blur/
Tipico Casino Chips sind eine Währung, die in dem beliebten Online-Casino Tipico verwendet wird. Spieler können diese Chips verwenden, um verschiedene Spiele zu spielen und potenziell große Gewinne zu erzielen.
Die Chips können auf verschiedene Weise erworben werden. Zum einen können Spieler sie durch den Kauf von virtuellen Währungen erhalten, die dann in Chips umgetauscht werden können. Zum anderen werden Chips auch als Belohnung für bestimmte Aktionen vergeben, wie beispielsweise für das Spielen bestimmter Spiele oder für das Erreichen bestimmter Meilensteine.
Die Verwendung von Casino Chips bietet den Spielern viele Vorteile. Zum einen ermöglichen sie es den Spielern, ihre Einsätze zu verwalten und besser im Blick zu behalten, wie viel sie bereits ausgegeben haben. Zum anderen sorgen sie dafür, dass Transaktionen sicher und geschützt sind, da sie vollständig virtuell sind und keine persönlichen Finanzdaten preisgeben.
Darüber hinaus können Chips auch als Teil von Bonusprogrammen verwendet werden, die es den Spielern ermöglichen, zusätzliche Belohnungen zu erhalten. So können Spieler beispielsweise Freispiele oder Bonusgelder erhalten, die sie dann für weitere Spiele verwenden können.
Insgesamt sind Tipico Casino Chips eine praktische und sichere Möglichkeit, um in einem Online-Casino zu spielen. Sie bieten den Spielern eine einfache Möglichkeit, ihre Konten zu verwalten und sicherzustellen, dass ihre Transaktionen geschützt sind. Wer gerne Casino-Spiele spielt, sollte auf jeden Fall die Verwendung von Casino Chips in Betracht ziehen.
https://tipicocasino.one/
Zet Casino Störungen
Zet Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und großzügigen Boni für die Spieler anbietet. Die Plattform hat sich einen Ruf für ihre Zuverlässigkeit und Benutzerfreundlichkeit erworben, aber in letzter Zeit haben einige Spieler über Störungen beim Zugriff auf die Website berichtet.
Es ist nicht ungewöhnlich, dass Online-Casinos gelegentlich Störungen oder technische Probleme haben, die den Spielspaß beeinträchtigen können. Die Ursachen für diese Störungen können vielfältig sein, von Serverproblemen bis hin zu Verbindungsproblemen mit dem Internet.
Für Spieler, die von den Störungen betroffen sind, kann dies frustrierend sein. Sie könnten nicht in der Lage sein, ihre Lieblingsspiele zu spielen oder sich für geplante Turniere anzumelden. Darüber hinaus kann es auch zu Verlusten führen, wenn eine Störung während eines Spiels auftritt und der Einsatz verloren geht.
Zet Casino hat sich bisher bemüht, die Störungen schnell zu beheben und den Spielern eine reibungslose Spielerfahrung zu bieten. Sie haben auch ihren Kundenservice verbessert, um bei auftretenden Problemen schnell und effizient helfen zu können.
Spieler, die jedoch weiterhin Probleme mit Störungen bei Zet Casino haben, sollten nicht zögern, den Kundenservice zu kontaktieren und das Problem zu melden. Durch die Bereitstellung von detaillierten Informationen können die Techniker des Casinos das Problem schneller identifizieren und beheben.
Insgesamt ist Zet Casino eine ausgezeichnete Glücksspielplattform, die ihren Spielern eine unterhaltsame und spannende Erfahrung bietet. Es ist jedoch wichtig, dass das Kasino Probleme wie Störungen schnell und effizient löst, um das Vertrauen der Spieler zu wahren und sicherzustellen, dass sie weiterhin gerne auf der Plattform spielen.
https://zetcasino.one/
visit https://galxe-app.org/2023/11/19/revolutionizing-digital-credentialing-galxe-transforms-blockchain-landscape/
he said https://blur-nft-marketplace.org/2023/11/10/a-comprehensive-guide-for-designers-and-developers-on-harnessing-the-full-potential-of-the-blur-io-api/
check over here https://1inch-dex.com/2023/11/17/the-regulatory-challenges-and-opportunities-for-1inch-in-global-markets/
ומורכבות. בזמן ביקור במקום כמו דירות דיסקרטיות בבאר שבע גברים רבים מעריכים את ההזדמנות לעסוק בשיחות משמעותיות, לחלוק חוויות שבע מתעוררות לחיים. שירותים של דירות דיסקרטיות בירושלים נערות ליווי בתל אביב מציעות מגוון שירותים דירות דיסקרטיות באשדוד הזמנת נערת ליווי לביתך או בית מלון
aparthome.org
besttoday.org
Boomerang-Casinos sind eine relativ neue Form von Online-Casinos, die in der GlГјcksspielbranche immer beliebter werden. Der Name “Boomerang” bezieht sich auf die Tatsache, dass Spieler, die an diesen Casinos teilnehmen, immer wieder zurГјckkehren, um mehr zu spielen.
Das Besondere an Boomerang-Casinos ist, dass sie eine Vielzahl von attraktiven Boni und Belohnungen für ihre Spieler anbieten. Dies reicht von Willkommensboni und Freispielen bis hin zu regelmäßigen Aktionen und Treueprämien. Diese Boni dienen dazu, die Spieler zu motivieren, weiterzuspielen und ihnen ein besonderes Spielerlebnis zu bieten.
Ein weiteres Merkmal von Boomerang-Casinos ist ihre Benutzerfreundlichkeit und ihre Verfügbarkeit auf verschiedenen Geräten. Spieler können von überall und zu jeder Zeit auf ihre Lieblingsspiele zugreifen, sei es auf dem Computer, dem Smartphone oder dem Tablet. Diese Flexibilität macht es für die Spieler einfacher, ihre Lieblingsspiele zu genießen und gleichzeitig ihre Gewinnchancen zu maximieren.
Da Boomerang-Casinos noch relativ neu sind, gibt es eine Vielzahl von Anbietern, die um die Gunst der Spieler konkurrieren. Dies führt zu einem verstärkten Wettbewerb und einer Vielzahl von Angeboten, von denen die Spieler profitieren können. Es ist wichtig, jedoch darauf zu achten, dass man nur bei seriösen Anbietern spielt, um Betrug und unfaire Praktiken zu vermeiden.
Insgesamt sind Boomerang-Casinos eine aufregende Entwicklung in der Welt des Online-Glücksspiels und bieten Spielern die Möglichkeit, an unterhaltsamen und lohnenden Spielen teilzunehmen. Es ist jedoch wichtig, verantwortungsbewusst zu spielen und sich an die geltenden Gesetze und Vorschriften zu halten, um ein sicheres und faires Spielerlebnis zu gewährleisten.
https://boomerangcasino.one/
Zet Casino ist eine beliebte Online-GlГјcksspielseite, die eine Vielzahl von Casino-Spielen und Promotionen fГјr Spieler anbietet. Viele Menschen haben positive Erfahrungen mit Zet Casino gemacht, da sie eine benutzerfreundliche Plattform und eine Vielzahl von Spielen bieten.
Einer der Hauptgründe, warum Spieler Zet Casino lieben, ist die große Auswahl an Spielen, die sie zur Verfügung stellen. Von klassischen Tischspielen wie Roulette und Blackjack bis hin zu modernen Spielautomaten und Live-Dealer-Spielen, gibt es für jeden etwas zu spielen. Die Spiele werden von renommierten Softwareanbietern wie NetEnt, Microgaming und Betsoft bereitgestellt, was bedeutet, dass sie von höchster Qualität sind und ein reibungsloses Spielerlebnis bieten.
Außerdem bietet Zet Casino großzügige Promotionen und Boni für Spieler an. Neue Spieler können einen Willkommensbonus erhalten, der ihren ersten Einzahlungsbetrag erhöht und zusätzliche Freispiele für ausgewählte Spiele bietet. Darüber hinaus belohnt das Casino treue Spieler mit regelmäßigen Promotionen, Turnieren und Cashback-Angeboten.
Die Ein- und Auszahlungsmöglichkeiten bei Zet Casino sind vielfältig und sicher, was es den Spielern ermöglicht, schnell und problemlos Geld auf ihr Konto einzuzahlen und abzuheben. Der Kundensupport des Casinos ist ebenfalls rund um die Uhr verfügbar und bietet schnelle Lösungen für alle Anliegen der Spieler.
Insgesamt haben Spieler, die Zet Casino ausprobiert haben, positive Erfahrungen gemacht und schätzen die Vielfalt an Spielen, die großzügigen Boni und die zuverlässige Kundenbetreuung. Wenn Sie auf der Suche nach einem unterhaltsamen und sicheren Online-Casino-Erlebnis sind, könnte Zet Casino eine gute Option für Sie sein.
https://zetcasino.one/
stroihome.net
domfenshuy.net
Das Boomerang Casino ist ein neues und aufregendes Online-Casino, das seinen Spielern großzügige Bonusangebote ohne Einzahlung bietet. Mit den Boomerang Casino Bonuscodes ohne Einzahlung können die Spieler ohne Risiko echtes Geld gewinnen und dabei Spaß haben.
Die Bonusangebote ohne Einzahlung sind eine großartige Möglichkeit für neue Spieler, das Casino kennenzulernen und erste Gewinne zu erzielen, ohne ihr eigenes Geld riskieren zu müssen. Die Codes werden einfach bei der Registrierung oder im Kassenbereich des Casinos eingegeben und schon kann das kostenlose Spiel beginnen.
Die Boomerang Casino Bonuscodes ohne Einzahlung können verschiedene Vorteile wie Freispiele, kostenloses Bonusgeld oder sogar Cashback-Angebote beinhalten. So haben die Spieler die Möglichkeit, verschiedene Spiele im Casino auszuprobieren und ihre Lieblingsspiele zu finden, ohne dafür Geld ausgeben zu müssen.
Um von den Boomerang Casino Bonuscodes ohne Einzahlung zu profitieren, ist es wichtig, die jeweiligen Bedingungen und Umsatzanforderungen zu beachten. Diese können je nach Angebot variieren und müssen erfüllt werden, um Gewinne auszahlen zu können.
Insgesamt bietet das Boomerang Casino seinen Spielern eine großartige Möglichkeit, ohne Einzahlung echtes Geld zu gewinnen und dabei viel Spaß zu haben. Die Bonusangebote ohne Einzahlung sind eine gute Gelegenheit, das Casino kennenzulernen und vielleicht sogar den Jackpot zu knacken. Wer also auf der Suche nach einem unterhaltsamen und lukrativen Online-Casino ist, sollte das Boomerang Casino definitiv in Betracht ziehen.
https://boomerangcasino.one/
Im Zet Casino erwarten die Spieler großzügige Boni und lukrative Aktionen. Unter anderem können Neukunden von einem attraktiven Willkommensangebot profitieren, das bis zu 500 Euro Bonusguthaben sowie 200 Freispiele beinhaltet.
Besonders interessant sind hierbei die sogenannten Zet Casino 30 Freispiele, die den Spielern die Möglichkeit bieten, kostenlos erste Gewinne einzustreichen. Diese Freispiele können in ausgewählten Spielen eingesetzt werden und sorgen somit für zusätzlichen Spielspaß und Spannung.
Um von den Zet Casino 30 Freispielen zu profitieren, müssen Spieler lediglich ein Konto im Casino erstellen und eine Einzahlung tätigen. Anschließend stehen die Freispiele zur Verfügung und können sofort genutzt werden.
Die Freispiele sind eine tolle Gelegenheit, um neue Spiele auszuprobieren und erste Gewinne zu erzielen, ohne dabei eigenes Geld einsetzen zu müssen. Zudem bieten sie die Chance, das Casino und seine Spiele näher kennenzulernen, bevor man tiefer in die Welt des Glücksspiels eintaucht.
Alles in allem sind die Zet Casino 30 Freispiele eine attraktive Bonusaktion für alle Spieler, die sich auf der Suche nach einem spannenden und unterhaltsamen Casinoerlebnis befinden. Wer also sein Glück versuchen und dabei von lukrativen Freispielen profitieren möchte, sollte sich das Zet Casino genauer anschauen.
https://zetcasino.one/
בירושלים ויכולת מינית, תוך סטיגמה של מי שמסטה מהנורמות הללו. אתגר סטיגמה וקידום קבלת ביטויים מגוונים של מיניות הם חיוניים ליצירת יחסים, כולל שימוש בשירותי דירות דיסקרטיות בירושלים. תורות יהודיות מסורתיות מדגישות את קדושת הנישואין והמשפחה, תוך הכרה בחשיבות דירה דיסקרטית בחיפה והצפון – רחוק מלהיות משמעם
Die Tipico Casino App ist eine beliebte Option für all diejenigen, die gerne unterwegs in einem Online Casino spielen möchten. Mit dieser App haben Spieler die Möglichkeit, eine Vielzahl von Casino-Spielen wie Spielautomaten, Roulette, Blackjack und mehr auf ihren mobilen Geräten zu genießen.
Die App zeichnet sich durch ihr benutzerfreundliches Design und ihre hohe Qualität aus. Sie ist sowohl für Android- als auch für iOS-Geräte verfügbar und kann ganz einfach im jeweiligen App Store heruntergeladen werden.
Ein großer Vorteil der Tipico Casino App ist die große Auswahl an Spielen, die sie bietet. Spieler haben die Möglichkeit, aus Hunderten von verschiedenen Spielen zu wählen, so dass für jeden Geschmack etwas dabei ist. Darüber hinaus bietet die App auch regelmäßige Promotionen und Boni, die es Spielern ermöglichen, ihre Gewinne zu maximieren.
Ein weiterer Pluspunkt der Tipico Casino App ist die Möglichkeit, sowohl um Echtgeld als auch im Demo-Modus zu spielen. Auf diese Weise können Spieler die Spiele zunächst kostenlos ausprobieren, bevor sie echtes Geld einsetzen.
Zusammenfassend lässt sich sagen, dass die Tipico Casino App eine großartige Option für alle Casino-Liebhaber ist, die gerne mobil spielen möchten. Mit ihrer breiten Auswahl an Spielen, ihrem benutzerfreundlichen Design und ihren regelmäßigen Promotionen ist sie definitiv einen Download wert. Probieren Sie es noch heute aus und erleben Sie die Spannung eines Online Casinos ganz bequem von Ihrem Smartphone oder Tablet aus.
https://tipicocasino.one/
Частные интим объявления devkiru.com
Если Вы планировали найти индивидуалки сходненская в Москве, то быстрее переходите на вышеупомянутый сайт. Мы предлагаем купить самых недорогих проституток в столице. Но в этом вопросе, низкая цена не значит качество. Просто у девушек в данной группе не так много стажа, и принимают они в квартирах чуть далее от центра и не очень фешенебельных. Не нужно волноваться, что дешевая цена может испортить Ваш досуг, скорее — наоборот. Возможность классно провести свой отдых по хорошей стоимости-в двойном размере хорошо.
На сайте https://turk-kino.ru посмотрите интересное и запоминающееся турецкое кино вместе с другом. Есть такие именитые картины, как «Запах клубники», «Зимородок», «Великолепный век» и многое другое. Для того чтобы начать совместный просмотр, необходимо создать комнату. Сделать это получится в 3 шага, а инструкция прилагается. Перед вами многообещающие новинки, а также топ лучших фильмов за 2024 год. Во всех фильмах играют ваши любимые актеры, звучит приятная музыка. Есть подборка рекомендованных фильмов, которые выбирают многие.
На сайте http://magomagii.ru вы сможете получить всю необходимую информацию об обрядах, узнать про магические заклинания, увлекательные обряды, а также эзотерику. При этом вы сможете ознакомиться с полезными и любопытными материалами, а также пообщаться с единомышленниками, оценить посты и высказать свое мнение. Кроме того, можно будет попробовать провести обряды самостоятельно, чтобы получить необходимый результат. Ознакомьтесь со всеми рубриками сайта. Среди них: магия и отношения, магический словарь, магический календарь, заметки, магическая кулинария.
Zet Casino Bonus Code ohne Einzahlung
Zet Casino ist ein beliebtes Online-Casino, das seinen Spielern eine Vielzahl von Spielen und groГџzГјgigen Boni bietet. Einer der attraktivsten Boni, die von Zet Casino angeboten werden, ist der Bonus Code ohne Einzahlung.
Mit dem Bonus Code ohne Einzahlung können Spieler kostenlose Bonusgelder erhalten, ohne dass sie zuerst eine Einzahlung tätigen müssen. Dies ermöglicht es Spielern, das Casino und die angebotenen Spiele risikofrei zu testen, bevor sie sich entscheiden, echtes Geld einzuzahlen.
Um den Bonus Code ohne Einzahlung zu erhalten, müssen Spieler lediglich den entsprechenden Code bei der Registrierung eingeben. Nachdem der Code eingelöst wurde, wird das Bonusguthaben dem Spielerkonto gutgeschrieben und kann sofort zum Spielen verwendet werden.
Der Bonus Code ohne Einzahlung ist eine großartige Möglichkeit für Spieler, das Zet Casino kennenzulernen und gleichzeitig die Chance zu haben, echtes Geld zu gewinnen. Es lohnt sich daher, regelmäßig nach neuen Bonus Codes ohne Einzahlung Ausschau zu halten und diese zu nutzen, um das Beste aus Ihrem Spielerlebnis bei Zet Casino herauszuholen.
https://zetcasino.one/
На сайте https://nashi-teplicy.ru/ напишите сообщение для того, чтобы заказать производство теплиц из поликарбоната как в Москве, так и области. Разработка происходит по индивидуальным эскизам заказчика. В каталоге представлены как прямостенные, так и арочные, каплевидные теплицы, парники, навесы. Все они самых разных размеров, а потому сможете подобрать решение под свои предпочтения, требования. На продукцию установлены привлекательные расценки. Также есть и спецпредложения. Организуется доставка по всей России, СНГ.
Similar parts are created from hard alloys etalonsadforum.com such as tungsten carbide, titanium or tantalum with the addition of cobalt. After melting, such parts are pressed under high pressure to obtain the desired parameters.
Tipico Casino Bonus Code ohne Einzahlung 2020
Das Tipico Casino bietet seinen Kunden regelmäßig attraktive Bonusaktionen an, um das Spielerlebnis noch spannender zu gestalten. Einer der beliebtesten Bonusarten ist der Bonus ohne Einzahlung, bei dem Spieler eine bestimmte Geldsumme geschenkt bekommen, ohne dass sie dafür eine Einzahlung tätigen müssen. Auch im Jahr 2020 können sich Kunden des Tipico Casinos über solche lukrativen Angebote freuen.
Um an einen Bonus ohne Einzahlung zu gelangen, benötigt man in der Regel einen speziellen Bonuscode, den man während der Registrierung oder bei der Einzahlung eingeben muss. Mit diesem Code wird der Bonus aktiviert und man kann mit dem kostenlosen Geld direkt ins Casinovergnügen starten.
Ein solcher Bonus ohne Einzahlung kann verschiedene Formen annehmen. Es kann sich um einen festen Geldbetrag handeln, um Freispiele fГјr bestimmte Spielautomaten oder um einen Cashback-Bonus, bei dem man einen Teil seiner Verluste erstattet bekommt. Die genauen Bedingungen fГјr den Bonus sind in den jeweiligen Bonusbedingungen des Tipico Casinos nachzulesen.
Es ist jedoch wichtig zu beachten, dass ein Bonus ohne Einzahlung in der Regel an bestimmte Umsatzbedingungen geknГјpft ist, die erfГјllt werden mГјssen, bevor man sich Gewinne auszahlen lassen kann. Diese Bedingungen variieren je nach Angebot und sollten daher vor Annahme des Bonus genau gelesen werden.
Wer also auf der Suche nach einem spannenden Bonus ohne Einzahlung für das Tipico Casino ist, sollte regelmäßig die Promotionsseite des Casinos besuchen und sich über aktuelle Angebote informieren. Mit etwas Glück und Geschick kann man so ohne eigenes Geld einzusetzen attraktive Gewinne erzielen und das Spielvergnügen auf ein neues Level heben.
https://tipicocasino.one/
реонт техники
1newss.com
Wow that was odd. I just wrote an extremely long comment but after I clicked submit my comment didn’t appear. Grrrr… well I’m not writing all that over again. Anyhow, just wanted to say great blog!
Купить диплом Института экономики и антикризисного управления
Zet Casino Freispiele
Zet Casino ist ein beliebtes Online-Casino, das seinen Spielern eine Vielzahl von Spielen und Boni anbietet. Eine der beliebtesten Aktionen im Zet Casino sind die Freispiele, die den Spielern die Möglichkeit geben, kostenlose Runden an ausgewählten Spielautomaten zu spielen.
Um Freispiele im Zet Casino zu erhalten, müssen Spieler bestimmte Voraussetzungen erfüllen. Oftmals werden Freispiele als Teil eines Willkommensbonus oder als Belohnung für treue Spieler angeboten. Spieler können auch Freispiele durch Sonderaktionen oder Turniere gewinnen.
Die Anzahl der Freispiele, die Spieler erhalten, variiert je nach Aktion und Angebot. In der Regel können Spieler zwischen 10 und 100 Freispiele bekommen. Die Freispiele können nur an bestimmten Spielautomaten genutzt werden und haben einen festgelegten Wert pro Runde.
Freispiele sind eine großartige Möglichkeit, um neue Spielautomaten im Zet Casino auszuprobieren und echtes Geld zu gewinnen, ohne eigenes Geld riskieren zu müssen. Spieler können ihre Gewinne aus Freispielen in Form von Echtgeld behalten und für weitere Spiele verwenden.
Für alle Fans von Online-Casinospielen sind Freispiele im Zet Casino eine tolle Möglichkeit, um das Spielerlebnis zu verbessern und zusätzliche Gewinnchancen zu erhalten. Probiere es aus und sichere dir deine Freispiele im Zet Casino!
https://zetcasino.one/
What you typed made a great deal of sense. But, think about this, suppose you were to write a awesome headline? I ain’t suggesting your information isn’t good, but suppose you added a post title that grabbed people’s attention? I mean %BLOG_TITLE% is kinda plain. You ought to glance at Yahoo’s front page and note how they create article titles to get viewers to open the links. You might try adding a video or a related picture or two to get people excited about everything’ve written. In my opinion, it might bring your posts a little livelier.
Купить дипломы Вузов Архангельска
https://online-sms.org/
helpful hints https://metamask-wallet.at/2023/11/16/incorporating-avalanche-into-metamask-wallet-for-expanding-defi-opportunities/
read this https://orbiter-finance-bridge.com/2023/11/18/introduction-to-orbiter-finance-connecting-layer-2-solutions/
check my site https://galxe-web3.com/2023/10/08/stay-updated-on-galxe-campaigns-with-telegram-and-discord-bots/
Bonuses https://orbiter-finance.at/2023/11/19/orbiter-finance-leveraging-cosmos-for-a-decentralized-financial-infrastructure/
Красивые проститутки devkiru.com
Если Вы хотели заказать индивидуалки москвы с отзывами в Мск, то прямо сейчас переходите на наш сайт. Мы предлагаем посмотреть самых дешевых проституток в Москве. Но в этом вопросе, цена не означает плохое качество. Всего лишь у девочек в этой категории не так много опыта, и принимают они в квартирах чуть дальше от центра Москвы и не очень роскошных. Не нужно волноваться, что невысокая цена может подпортить Ваш отдых, правильнее — наоборот. Вероятность великолепно провести свой отдых по выигрышной цене-вдвойне хорошо.
Das Tipico Casino ist eines der beliebtesten Online-Casinos in Deutschland. Viele Spieler begeistern sich für die große Auswahl an Spielen und die benutzerfreundliche Oberfläche. Doch trotz aller positiven Aspekte gibt es immer wieder Berichte darüber, dass einige Spieler keine Gewinne erzielen.
Es ist wichtig zu erwähnen, dass Glücksspiel immer mit einem gewissen Risiko verbunden ist und Gewinne nie garantiert werden können. Dennoch häufen sich die Beschwerden von Spielern, die angaben, dass sie keine oder nur sehr geringe Gewinne im Tipico Casino erzielen konnten.
Ein Grund für die fehlenden Gewinne könnte möglicherweise die hohe Varianz der Casino-Spiele sein. Einige Spiele sind bekannt dafür, dass sie hohe Gewinne auszahlen können, jedoch nur selten. Das bedeutet, dass Spieler viele Runden spielen können, ohne einen nennenswerten Gewinn zu erzielen.
Ein anderer Grund könnte möglicherweise eine falsche Spielstrategie sein. Einige Spieler setzen zu viel Geld auf ein Spiel oder spielen übermäßig lange, was zu Verlusten führen kann. Es ist wichtig, verantwortungsbewusst zu spielen und sich an ein festgelegtes Budget zu halten.
Es gibt aber auch Spieler, die behaupten, dass das Tipico Casino nicht fair spielt und Gewinne zurückhält. Es ist jedoch wichtig zu betonen, dass Online-Casinos strengen Regulierungen unterliegen und regelmäßig von unabhängigen Behörden überprüft werden. Somit sind Manipulationen in seriösen Online-Casinos nahezu ausgeschlossen.
Letztendlich ist es wichtig, sich bewusst zu sein, dass Glücksspiel kein Weg ist, um sicher an Geld zu kommen. Es ist immer mit einem gewissen Risiko verbunden und Gewinne können nicht garantiert werden. Es ist ratsam, verantwortungsbewusst zu spielen und sich im Zweifelsfall an den Kundenservice des Tipico Casinos zu wenden, um mögliche Probleme zu klären.
https://tipicocasino.one/
try here https://metamask-wallet-web3.com/2023/11/16/exploring-the-advantages-and-uses-of-combining-polygon-and-metamask/
промокоды скидки айхерб
промокод айхерб вознаграждение
промокоды айхерб май
Das Zet Casino bietet auch im Jahr 2019 groГџzГјgige Bonusaktionen fГјr Neukunden an. Einer der beliebtesten Bonusangebote ist der sogenannte “No Deposit Bonus”, bei dem neue Spieler einen Bonus erhalten, ohne zuvor eine Einzahlung tГ¤tigen zu mГјssen. Um diesen Bonus zu beanspruchen, mГјssen Spieler lediglich einen speziellen Bonuscode eingeben, der auf der Webseite des Casinos verГ¶ffentlicht wird.
Der No Deposit Bonus beim Zet Casino kann in Form von Freispielen oder Bonusguthaben vergeben werden. Mit den Freispielen können Spieler bestimmte Spielautomaten kostenlos ausprobieren und dabei echte Gewinne erzielen. Das Bonusguthaben hingegen kann für verschiedene Spiele im Casino eingesetzt werden und erhöht somit die Gewinnchancen der Spieler.
Um den No Deposit Bonus zu erhalten, müssen Spieler in der Regel ein neues Konto beim Zet Casino registrieren und den entsprechenden Bonuscode eingeben. Nach erfolgreicher Registrierung wird der Bonus automatisch gutgeschrieben und kann sofort genutzt werden. Es ist jedoch wichtig zu beachten, dass die meisten No Deposit Boni bestimmten Umsatzbedingungen unterliegen, die erfüllt werden müssen, bevor eine Auszahlung der Gewinne möglich ist.
Insgesamt bietet das Zet Casino eine Vielzahl von attraktiven Bonusaktionen für neue und bestehende Spieler an. Der No Deposit Bonus ist eine großartige Möglichkeit, das Casino risikofrei kennenzulernen und dabei echte Gewinne zu erzielen. Spieler sollten jedoch darauf achten, die Bonusbedingungen genau zu lesen, um sicherzustellen, dass sie den Bonus optimal nutzen können.
https://zetcasino.one/
useful content https://1inch-app.org/2023/11/17/where-to-buy-1inch-tokens-for-the-best-prices/
Компания «Дока строй» успешно занимается ремонтом квартир с 2007 года. Здесь работают истинные специалисты с профильным образованием. Сотрудники прекрасно знают свою сферу и учитывают все нюансы. Гарантируем приемлемую стоимость и качественные услуги. Ищете стоимость ремонта? Doka-stroi.ru – сайт, где можете в любое удобное для вас время ознакомиться с выполненными проектами и многочисленными отзывами довольных клиентов. Мы всегда идем до конца, обращайтесь. Не забудьте порекомендовать нас своим друзьям.
In der Welt der Online-Glücksspiele ist es häufig möglich, Geld von einem Bereich wie Sportwetten auf einen anderen wie das Casino zu übertragen. Dies bietet Spielern eine größere Flexibilität und Auswahlmöglichkeiten, wenn es um ihre Einsätze und Gewinne geht.
Eine beliebte Plattform, die diese Übertragungsmöglichkeit bietet, ist Tipico. Obwohl bekannt für seine Sportwetten, hat Tipico auch ein umfangreiches Online-Casino-Angebot, das von Spielautomaten über Tischspiele bis hin zu Live-Dealer-Spielen reicht. Indem Sie Geld von Ihrem Sportwettenkonto auf Ihr Casino-Konto übertragen, können Sie nahtlos zwischen den beiden Bereichen wechseln und Ihre Lieblingsspiele genießen.
Um Geld von Sportwetten auf das Casino bei Tipico zu übertragen, müssen Sie einfach Ihr Konto aufrufen und den gewünschten Betrag angeben. Beachten Sie jedoch, dass möglicherweise bestimmte Umsatzbedingungen erfüllt werden müssen, bevor eine Übertragung möglich ist. Diese Bedingungen können von Fall zu Fall variieren, und es ist ratsam, die AGBs von Tipico zu überprüfen, um sicherzustellen, dass Sie alle Anforderungen erfüllen.
Die Übertragung von Geld zwischen verschiedenen Bereichen eines Online-Glücksspielanbieters kann Spielern nicht nur mehr Flexibilität bieten, sondern auch dazu beitragen, ihr Spielvergnügen zu maximieren. Indem Sie von Sportwetten auf das Casino wechseln, können Sie verschiedene Spiele ausprobieren und möglicherweise auch höhere Gewinne erzielen.
Insgesamt bietet die Möglichkeit, Geld von Sportwetten auf das Casino bei Tipico zu übertragen, den Spielern eine zusätzliche Möglichkeit, ihre Glücksspielerfahrung zu personalisieren und vielfältiger zu gestalten. Es lohnt sich, diese Option zu nutzen und das Beste aus beiden Welten zu genießen.
https://tipicocasino.one/
Проект Мир: Л был создан нами для того, чтобы вы научились отдавать любовь миру вокруг вас и ценить себя. Развивайтесь и самосовершенствуйтесь, смотрите вебинары, проходите обучение, посещайте мероприятия в разных уголках планеты. Ищете упражнения арт терапии? Mir-l.com – зарегистрировавшись тут абсолютно бесплатно, вы сразу получите доступ к интересным статьям, видеороликам, а также аудиозаписям по различным сферам. Если у вас возникли вопросы, пишите нам, укажите имя и e-mail на сайте. Исследуйте платформу Мир: Л прямо сейчас!
На сайте https://runobe.ru почитайте ранобэ онлайн и в отличном качестве. Все они на русском языке, а потому насладиться чтением сможет каждый. Все произведения имеют интересный сюжет, непредсказуемую развязку, а потому понравятся всем без исключения. Выбор японских романов обновляется ежедневно, чтобы вы смогли найти то, что действительно вам нравится. Вы можете ознакомиться сразу с несколькими, чтобы определиться с тем, какие из них вам нравятся больше. Для того чтобы подыскать определенный вариант, необходимо воспользоваться специальным поиском.
На сайте https://roossa.ru/ представлены лучшие книги популярного издательского дома «РООССА». Всем желающим доступна оперативная и бесплатная доставка при покупке от 2 500 рублей. В разделе представлены детские книги, для школьников, сказки для детей, раскраски, аудиосказки с книгой, стихотворения для детей, удивительные рассказы, говорящие игрушки, книги рецептов и многое другое, что позволит провести время с пользой для кругозора. Также имеются и подарочные книги, а также эксклюзивные издания.
Zet Casino, ein beliebtes Online-Casino, hat in den letzten Tagen mit einigen technischen Störungen zu kämpfen gehabt. Diese Störungen haben sich auf die Spielererfahrung ausgewirkt und zu Frustration bei den Nutzern geführt.
Die Ursachen für diese Störungen sind bisher noch nicht bekannt, jedoch hat das Zet Casino versichert, dass das Team hart daran arbeitet, das Problem so schnell wie möglich zu lösen. In der Zwischenzeit haben sie Maßnahmen ergriffen, um die Auswirkungen der Störungen zu minimieren.
Trotz dieser Störungen hat das Zet Casino weiterhin eine große Anzahl von Spielern, die das Online-Casino täglich besuchen. Die Vielzahl von Spielen und Promotionen, die das Casino anbietet, macht es zu einer beliebten Wahl für viele Spieler.
Es ist zu hoffen, dass das Zet Casino die technischen Probleme bald beheben kann, um seinen Ruf als vertrauenswürdige und unterhaltsame Glücksspielplattform aufrechtzuerhalten. Bis dahin bitten sie ihre Spieler um Geduld und Verständnis für die Unannehmlichkeiten, die diese Störungen verursacht haben.
Insgesamt ist das Zet Casino immer noch eine attraktive Option für Spieler, die auf der Suche nach einer breiten Auswahl an Spielen und aufregenden Promotionen sind. Mit der Hoffnung, dass die technischen Störungen bald behoben sind, können Spieler weiterhin ihr Glück im Zet Casino versuchen und hoffen, dass ihr Spiel ungestört bleibt.
https://zetcasino.one/
Онлайн журнал «В мире женщин» предоставляет актуальную и интересную информацию. Здесь вы найдете такие рубрики, как: красота, звезды, гороскопы, юмор, мода, здоровье, психология, стиль, отношения. Вы узнаете, как выглядит самый дорогой свадебный торт в мире, почему советские джинсы так и не стали модными, стоит ли ходить в тренажерный зал во время пандемии. https://vmirezhenshchin.ru – сайт, который сделан так, чтобы вам было комфортно им пользоваться. Мы размещаем качественные фотографии. У нас найдете много познавательной информации.
Tipico ist eine der bekanntesten und beliebtesten Online-Casino-Plattformen auf dem Markt. Mit einer breiten Palette an Spielen gibt es viele Möglichkeiten, sein Glück zu versuchen und hohe Gewinne zu erzielen.
Einige der besten Casino-Spiele bei Tipico sind definitiv die Spielautomaten. Mit einer Vielzahl von Themen und Bonusfunktionen bieten sie eine unterhaltsame und spannende Spielerfahrung. Zu den beliebtesten Spielautomaten bei Tipico gehГ¶ren Book of Dead, Starburst und Gonzo’s Quest.
Eine weitere beliebte Casino-Spielkategorie bei Tipico sind die Tischspiele. Hier kann man Klassiker wie Blackjack, Roulette und Baccarat spielen und sein Können gegen den Dealer unter Beweis stellen. Diese Spiele bieten die Möglichkeit, strategisch zu denken und die Gewinnchancen zu maximieren.
DarГјber hinaus bietet Tipico auch Live-Casino-Spiele an, bei denen echte Dealer das Spiel leiten und die Spieler in Echtzeit gegen andere Teilnehmer antreten. Das schafft eine authentische Casinoumgebung und sorgt fГјr ein besonderes Spielerlebnis.
Um die besten Casino-Spiele bei Tipico zu finden, ist es wichtig, die eigenen Vorlieben und Interessen zu berГјcksichtigen. Mit einer Vielzahl von Optionen und einer benutzerfreundlichen Plattform ist Tipico die ideale Wahl fГјr Casino-Liebhaber, die auf der Suche nach einem erstklassigen Spielerlebnis sind.
https://tipicocasino.one/
Вам нужна компетентная помощь автоюриста в Самаре? Анатолий Владимирович Мотин готов вам помочь. Адвокат по ДТП если берется за ведение дела, то доводит его до самого конца. Он не обещает то, чего выполнить не сможет. Специалист выезжает на ведение процессов по всей Самарской области. Ищете телефон автоюриста? Advokat-samara.ru – сайт, где указаны цены, вы можете ознакомиться с ними в любое удобное для вас время. Также тут предложены рекомендации адвоката по транспортным происшествиям. Вы узнаете, что делать водителю, пешеходу и пассажиру при ДТП.
На сайте https://dolgovnet82.ru вы сможете уточнить всю важную информацию, которая касается такой важной услуги, как банкротство физических лиц. Вас избавят от долгов, а также кредитов законным путем. За счет того, что обращение происходит к арбитражному управляющему напрямую, то вы сможете сэкономить приличную сумму денег. Процедура будет начата в день обращения, и при этом не нужно будет вносить платежи. Ваше имущество будет сохранено, как и покой близких. В этой компании действует привлекательная стоимость.
Ein Promo-Code ist eine fantastische Möglichkeit, um in Online-Casinos zusätzliche Vorteile zu erhalten. Der Zet Casino Promo-Code für 2023 verspricht spannende Bonusangebote und Belohnungen für alle Spieler.
Wenn Sie den Promo-Code für Zet Casino 2023 verwenden, können Sie von verschiedenen Boni profitieren, darunter Einzahlungsboni, Freispiele und Cashback-Angebote. Diese zusätzlichen Vorteile können Ihre Gewinnchancen erhöhen und Ihr Spielerlebnis noch aufregender machen.
Um den Promo-Code zu nutzen, müssen Sie einfach während der Registrierung oder Einzahlung den entsprechenden Code eingeben. Sobald der Code bestätigt wurde, werden die Bonusangebote automatisch Ihrem Konto gutgeschrieben.
Es ist wichtig zu beachten, dass Promo-Codes oft bestimmten Bedingungen und Umsatzanforderungen unterliegen. Bevor Sie einen Promo-Code nutzen, sollten Sie daher die entsprechenden Geschäftsbedingungen sorgfältig durchlesen, um sicherzustellen, dass Sie die Voraussetzungen erfüllen.
Mit dem Zet Casino Promo-Code für 2023 haben Sie die Möglichkeit, Ihr Glück auf die Probe zu stellen und großartige Preise zu gewinnen. Nutzen Sie diese aufregende Gelegenheit und tauchen Sie ein in die Welt des Online-Glücksspiels mit zusätzlichen Boni und Belohnungen. Viel Spaß und viel Erfolg beim Spielen!
https://zetcasino.one/
Das Boomerang Casino in Australien – ein Paradies fГјr Casino-Fans
Das Boomerang Casino in Australien ist ein beliebtes Ziel für Glücksspiel-Enthusiasten aus der ganzen Welt. Das Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Poker. Es gibt auch ein Live-Casino, in dem Spieler gegen echte Dealer antreten können.
Das Boomerang Casino zeichnet sich durch sein einzigartiges australisches Thema aus, das eine einladende und entspannte Atmosphäre schafft. Die Dekoration ist von der australischen Outback-Landschaft inspiriert, mit plüschigen roten Teppichen, Wandgemälden von Kängurus und Koalabären, und einem Ambiente, das an einen gemütlichen Lagerfeuerabend erinnert.
Das Casino bietet auch eine Vielzahl von Restaurants und Bars, in denen die Besucher kulinarische Köstlichkeiten und erfrischende Cocktails genießen können. Die Gäste können sich auch in einem der luxuriösen Hotelzimmer des Casinos entspannen und den Blick auf das umliegende Outback genießen.
Das Boomerang Casino ist nicht nur ein Ort zum Spielen, sondern auch eine echte Touristenattraktion. Viele Besucher kommen hierher, um das australische Glücksspiel-Erlebnis zu genießen und gleichzeitig die Schönheit des Landes zu erleben. Das Casino organisiert auch regelmäßig Veranstaltungen und Konzerte, um seine Gäste zu unterhalten.
Insgesamt ist das Boomerang Casino in Australien ein Paradies für Casino-Fans, die auf der Suche nach einem einzigartigen und unterhaltsamen Spielerlebnis sind. Mit seiner charmanten australischen Atmosphäre, einer Vielzahl von Spielen und Unterhaltungsmöglichkeiten, ist es definitiv einen Besuch wert.
https://boomerangcasino.one/
ireland-24.com
Select the appropriate metal material for the specific design. Strength requirements invest-building.com, corrosion resistance and other characteristics must be taken into account. It is worth contacting experienced specialists who will help you understand all the parameters.
На сайте http://magomagii.ru изучите интересную, увлекательную и содержательную информацию, которая связана с магией, эзотерикой. Вы научитесь правильно проводить обряды, пользоваться магией и будете радоваться полученным результатам. Маг размещает авторские статьи собственного сочинения. Он вкладывает в них свои умения, знания, душу. И точно знает, что данной темой заинтересуются. Здесь каждый сможет отыскать для себя что-то стоящее и интересное. На сайте можно и просто общаться, делиться впечатлениями.
Wenn Sie gerne online Casino-Spiele spielen, sollten Sie sich unbedingt beim Zet Casino anmelden. Dieses beliebte Casino bietet eine breite Auswahl an Spielen, groГџzГјgige Boni und eine benutzerfreundliche Plattform.
Um sich beim Zet Casino anzumelden, müssen Sie lediglich ein Konto erstellen und Ihre persönlichen Daten angeben. Danach können Sie sofort mit dem Spielen beginnen und die Vielzahl an angebotenen Spielen wie Slots, Tischspiele und Live-Casino-Spiele genießen.
Als neues Mitglied im Zet Casino können Sie von attraktiven Willkommensboni profitieren, die Ihnen zusätzliches Guthaben und Freispiele verschaffen. Darüber hinaus gibt es regelmäßig Promotionen und Sonderaktionen, mit denen Sie Ihre Gewinne maximieren können.
Das Zet Casino verfügt über eine sichere und zuverlässige Plattform, auf der Sie Ihre Lieblingsspiele ohne Sorgen genießen können. Die Ein- und Auszahlungen werden schnell und einfach abgewickelt, und der Kundenservice steht Ihnen rund um die Uhr zur Verfügung, um bei Fragen oder Problemen zu helfen.
Also worauf warten Sie noch? Melden Sie sich noch heute beim Zet Casino an und tauchen Sie ein in die aufregende Welt des Online-GlГјcksspiels. Viel SpaГџ und viel GlГјck!
https://zetcasino.one/
В нашем обществе, где диплом становится началом отличной карьеры в любой области, многие ищут максимально быстрый путь получения образования. Наличие официального документа об образовании переоценить невозможно. Ведь именно диплом открывает двери перед всеми, кто собирается начать трудовую деятельность или продолжить обучение в любом университете.
Мы предлагаем максимально быстро получить этот важный документ. Вы сможете приобрести диплом, и это будет удачным решением для человека, который не смог закончить образование, утратил документ или хочет исправить плохие оценки. Каждый диплом изготавливается аккуратно, с особым вниманием ко всем деталям. На выходе вы получите документ, полностью соответствующий оригиналу.
Плюсы подобного подхода заключаются не только в том, что можно быстро получить свой диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. Начиная от выбора требуемого образца документа до точного заполнения персональной информации и доставки по стране — все под абсолютным контролем наших специалистов.
Для тех, кто пытается найти максимально быстрый способ получить требуемый документ, наша компания готова предложить отличное решение. Заказать диплом – значит избежать продолжительного процесса обучения и сразу переходить к достижению своих целей, будь то поступление в ВУЗ или старт удачной карьеры.
http://homeforums.mybb.ru/viewtopic.php?id=3293
http://zoosurgut.mybb.ru/viewtopic.php?id=3015
https://realestatehungama.com/
Tipico Casino Free Spins
Das Tipico Casino bietet seinen Kunden eine Vielzahl von aufregenden Spielen und lukrativen Angeboten. Eine der begehrtesten Aktionen sind die Tipico Casino Free Spins, die es den Spielern ermöglichen, kostenlos an ausgewählten Spielautomaten zu spielen.
Diese Freispiele sind eine großartige Möglichkeit, neue Slots auszuprobieren, ohne dabei eigenes Geld riskieren zu müssen. Oftmals werden die Free Spins im Rahmen von speziellen Promotionen vergeben oder als Belohnung für treue Spieler. Manchmal sind sie auch Teil von Willkommensangeboten für neue Kunden.
Um die Tipico Casino Free Spins zu erhalten, mГјssen die Spieler bestimmte Bedingungen erfГјllen. Dies kann beispielsweise eine Mindesteinzahlung oder das Spielen einer bestimmten Anzahl von Runden sein. Die genauen Details der Aktionen werden in den jeweiligen Angeboten auf der Tipico Casino Website bekannt gegeben.
Es ist wichtig, die Teilnahmebedingungen für die Free Spins zu lesen und zu verstehen, um Missverständnisse zu vermeiden. Oftmals sind die Gewinne aus den Freispielen an Umsatzbedingungen gebunden, die erfüllt werden müssen, bevor eine Auszahlung möglich ist.
Alles in allem sind die Tipico Casino Free Spins eine tolle Möglichkeit, um das Casino und seine Spiele kostenlos kennenzulernen und dabei auch noch die Chance auf echte Gewinne zu haben. Es lohnt sich daher, regelmäßig die Promotionsseite des Tipico Casinos zu besuchen, um keine der spannenden Aktionen zu verpassen. Viel Spaß und gute Unterhaltung beim Spielen!
https://tipicocasino.one/
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha v.3, Hotmail (Microsoft), Google, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captchas.com (antigate), RuCaptcha, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
В современном мире, где диплом является началом удачной карьеры в любой области, многие пытаются найти максимально быстрый путь получения качественного образования. Факт наличия официального документа об образовании сложно переоценить. Ведь именно он открывает двери перед каждым человеком, который стремится начать профессиональную деятельность или продолжить обучение в ВУЗе.
В данном контексте наша компания предлагает максимально быстро получить этот важный документ. Вы сможете заказать диплом, что становится отличным решением для всех, кто не смог закончить обучение или утратил документ. Каждый диплом изготавливается с особой аккуратностью, вниманием ко всем деталям, чтобы на выходе получился 100% оригинальный документ.
Превосходство такого подхода заключается не только в том, что можно быстро получить свой диплом. Весь процесс организовывается комфортно, с нашей поддержкой. Начав от выбора подходящего образца до правильного заполнения личных данных и доставки по стране — все будет находиться под абсолютным контролем квалифицированных мастеров.
Всем, кто пытается найти оперативный способ получить требуемый документ, наша компания готова предложить отличное решение. Приобрести диплом – значит избежать продолжительного процесса обучения и сразу переходить к достижению личных целей: к поступлению в университет или к началу успешной карьеры.
http://zarabotok.userforum.ru/viewtopic.php?id=7798
http://stavklad.ru/viewtopic.php?f=9&t=4560
На сайте https://dostavka-shashlyk.ru закажите звонок для того, чтобы воспользоваться доставкой вкусного, ароматного, сочного шашлыка, который подарит невероятную радость. Вас обрадует оперативная доставка по городу Орел. Также здесь можно приобрести и куриные крылышки, шаурму, люля. Все блюда выполнены из свежих, отборных ингредиентов, за счет чего они тают во рту. Вы будете наслаждаться каждым кусочком. Воспользуйтесь бесплатной доставкой по Орлу, которая доступна вам при покупке от 1000 рублей.
На сайте https://moredoram.ru вы найдете дорамы, фильмы, сериалы высокого качества. Они понравятся всем любителям такого жанра и помогут расслабиться после трудового дня и просто получить приятные эмоции. Вы сможете воспользоваться функцией случайной дорамы, изучить список лучших из них. Все они в отличном качестве, с безупречным звуком, что позволит насладиться просмотром на любом устройстве, включая смартфон, ПК, планшет. Регулярно появляются многообещающие новинки, с которыми необходимо ознакомиться и вам.
Zet Casino Bonus ohne Einzahlung
Online-Casinos sind beliebter denn je und locken mit attraktiven Angeboten, um neue Spieler anzulocken. Einer der aktuellsten Trends in der Welt der Online-Casinos sind sogenannte “Bonus ohne Einzahlung” Angebote. Diese ermГ¶glichen es Spielern, ohne eigenes Geld zu riskieren, echte Gewinne zu erzielen.
Eines der Casinos, das solch ein Angebot anbietet, ist das Zet Casino. Der Zet Casino Bonus ohne Einzahlung ist eine großartige Möglichkeit, das Casino kennenzulernen, ohne gleich Geld einzahlen zu müssen. Neue Spieler können sich einfach registrieren und erhalten dann einen Bonus ohne Einzahlung in Form von Freispielen oder Bonusgeld, mit dem sie die verschiedenen Spiele des Casinos ausprobieren können.
Der Vorteil solcher Angebote liegt auf der Hand: Spieler können das Casino und dessen Spiele ganz ohne Risiko testen und sich so einen Eindruck davon verschaffen, ob sie sich in dem Casino wohlfühlen und gerne weiterspielen möchten. Zudem haben sie die Chance, echte Gewinne zu erzielen, ohne dabei eigenes Geld einzusetzen.
Allerdings gibt es auch einige Punkte zu beachten, wenn man einen Bonus ohne Einzahlung in Anspruch nimmt. Oftmals sind solche Boni an bestimmte Umsatzbedingungen geknüpft, die erfüllt werden müssen, bevor Gewinne auszahlbar sind. Zudem gelten häufig auch maximale Auszahlungslimits für Gewinne, die mit einem Bonus ohne Einzahlung erzielt wurden.
Insgesamt sind Bonus ohne Einzahlung Angebote eine großartige Möglichkeit, um neue Casinos kennenzulernen und erste Erfahrungen zu sammeln. Der Zet Casino Bonus ohne Einzahlung ist eine gute Gelegenheit, um das Casino zu testen und zu sehen, ob es den eigenen Vorlieben entspricht. Wer Glück hat, kann dabei sogar echte Gewinne erzielen und sein Spielerkonto aufbessern. Wer auf der Suche nach neuen Online-Casinos ist, sollte also definitiv einen Blick auf solche Angebote werfen und sie für sich nutzen.
https://zetcasino.one/
В нашем обществе, где диплом – это начало удачной карьеры в любой сфере, многие ищут максимально простой путь получения качественного образования. Необходимость наличия официального документа об образовании переоценить невозможно. Ведь диплом открывает двери перед любым человеком, желающим вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
В данном контексте наша компания предлагает быстро получить этот важный документ. Вы имеете возможность приобрести диплом старого или нового образца, что будет выгодным решением для всех, кто не смог завершить обучение, потерял документ или желает исправить плохие оценки. диплом изготавливается аккуратно, с особым вниманием ко всем нюансам. В итоге вы получите продукт, полностью соответствующий оригиналу.
Преимущество этого подхода заключается не только в том, что можно быстро получить диплом. Процесс организовывается комфортно, с нашей поддержкой. От выбора необходимого образца документа до консультации по заполнению персональных данных и доставки по стране — все находится под полным контролем квалифицированных специалистов.
В итоге, для всех, кто пытается найти быстрый способ получения необходимого документа, наша компания предлагает отличное решение. Приобрести диплом – это значит избежать долгого процесса обучения и сразу перейти к своим целям: к поступлению в университет или к началу трудовой карьеры.
http://kefirniygrib.7bb.ru/viewtopic.php?id=11824
http://passo.su/forums/index.php?showtopic=6427
Вызвать проститутку devkiru.com
По вопросу шлюхи москвы Вы на нужном пути. Наш надежный онлайн сайт предлагает превосходный отдых 18 плюс. Здесь есть: индивидуалки, массажистки, элитные красотки, БДСМ. А также Вы можете найти нужную девочку по параметрам: по станции метро, по возрасту, росту, цвету волос, карте. Всё для Вашего удобства.
סקס עם נערות ליווי בתל אביב בתעשיית המין. ניווט בשיקולים אתיים אלה דורש רגישות, אמפתיה ומחויבות לשמירה על זכויותיהם וכבודם של מהותי ממה שזה אומר להיות אנושי. סקס הוא חוויה דירות דיסקרטיות באשקלון חושית ועמוקה, המעסיקה את חושי המגע, הטעם, הריח, הראייה דירה סקס
Zet Casino: Kostenlose Freispiele
Zet Casino ist eine Online-Spielplattform, die Spielern ein aufregendes und unterhaltsames Spielerlebnis bietet. Neben einer Vielzahl von Casino-Spielen und Live-Casino-Optionen bietet Zet Casino auch eine groГџzГјgige Palette von Bonusangeboten, darunter kostenlose Freispiele, auch bekannt als “ilmaiskierrokset”.
Kostenlose Freispiele sind eine beliebte Form von Casino-Boni, die es Spielern ermöglichen, ausgewählte Spielautomaten kostenlos zu spielen, ohne ihr eigenes Geld einsetzen zu müssen. Bei Zet Casino können Spieler kostenlose Freispiele als Teil ihres Willkommensbonus erhalten oder durch laufende Promotionen und Aktionen im Casino.
Um kostenlose Freispiele zu erhalten, müssen Spieler oft eine Mindesteinzahlung vornehmen oder bestimmte Bonusbedingungen erfüllen. Diese Bedingungen können von Casino zu Casino variieren, daher ist es wichtig, die Geschäftsbedingungen sorgfältig zu lesen, um sicherzustellen, dass alle Anforderungen erfüllt sind.
Sobald Spieler ihre kostenlosen Freispiele erhalten haben, können sie diese verwenden, um ausgewählte Spielautomaten im Zet Casino zu spielen und möglicherweise echtes Geld zu gewinnen. Kostenlose Freispiele sind eine großartige Möglichkeit, neue Spiele auszuprobieren, ohne Risiko einzugehen, und können Spielern die Möglichkeit geben, ihre Gewinne zu steigern.
Insgesamt bieten kostenlose Freispiele bei Zet Casino den Spielern eine zusätzliche Chance auf Gewinne und erhöhen den Spaß und die Spannung des Spielens. Wenn Sie also auf der Suche nach einem aufregenden Casino-Erlebnis sind, das eine Vielzahl von Bonusangeboten und auch ilmaiskierrokset bietet, sollten Sie definitiv Zet Casino ausprobieren. Viel Glück beim Spielen! Prost!
https://zetcasino.one/
Ищете надежный и удобный способ приобрести необходимые детали для вашего автомобиля? Добро пожаловать в наш интернет-магазин автозапчастей http://partsshop03.ru! В нашем ассортименте вы найдете огромный выбор оригинальных запчастей для различных марок и моделей автомобилей. Мы предлагаем качественные детали по конкурентным ценам. Благодаря удобному сайту с подробными каталогами вы легко найдете нужные запчасти для вашего автомобиля. Покупайте с уверенностью в нашем интернет-магазине — мы знаем все о вашем автомобиле!
Das Boomerang Casino ist eine relativ neue Online-GlГјcksspielplattform, die in Deutschland immer beliebter wird. Viele Spieler fragen sich jedoch, ob das Spielen im Boomerang Casino legal ist.
Die Antwort darauf ist ja, das Boomerang Casino ist in Deutschland legal. Das Casino verfügt über eine Lizenz der Malta Gaming Authority, einer renommierten Glücksspielbehörde, die sicherstellt, dass das Casino strenge Richtlinien einhält und faire Spiele anbietet.
Spieler können also beruhigt sein, wenn sie im Boomerang Casino spielen. Sie können sicher sein, dass ihre persönlichen und finanziellen Daten geschützt sind und dass sie in einer sicheren und vertrauenswürdigen Umgebung spielen.
Das Boomerang Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele und Live-Casino-Spiele, die alle von führenden Softwareanbietern entwickelt wurden. Spieler können auch von lukrativen Boni und Aktionen profitieren, die regelmäßig angeboten werden.
Insgesamt ist das Boomerang Casino eine gute Wahl fГјr Spieler in Deutschland, die auf der Suche nach einer sicheren und unterhaltsamen GlГјcksspielplattform sind. Mit seiner Lizenz und seinem Ruf als vertrauenswГјrdiges Casino ist das Boomerang Casino definitiv eine gute Wahl fГјr deutsche Spieler.
https://boomerangcasino.one/
На сегодняшний день, когда диплом – это начало отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Необходимость наличия документа об образовании сложно переоценить. Ведь диплом открывает дверь перед любым человеком, желающим вступить в профессиональное сообщество или учиться в каком-либо университете.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы имеете возможность приобрести диплом, что становится удачным решением для человека, который не смог закончить образование, потерял документ или хочет исправить плохие оценки. диплом изготавливается аккуратно, с особым вниманием к мельчайшим деталям. В результате вы получите 100% оригинальный документ.
Преимущество данного подхода заключается не только в том, что можно максимально быстро получить свой диплом. Весь процесс организован удобно, с профессиональной поддержкой. От выбора требуемого образца до грамотного заполнения личных данных и доставки в любой регион страны — все под полным контролем квалифицированных специалистов.
Всем, кто хочет найти быстрый способ получения необходимого документа, наша услуга предлагает отличное решение. Приобрести диплом – это значит избежать долгого процесса обучения и сразу перейти к своим целям, будь то поступление в ВУЗ или старт трудовой карьеры.
https://feeder.topbb.ru/viewtopic.php?id=1824
http://deti.liveforums.ru/viewtopic.php?id=13910
לאינטימיות פיזית ועד לכוחן הטרנסצנדנטית של דירות דיסקרטיות בחיפה לאהבה רומנטית, יחסי הגומלין בין מין ותשוקה מקיפים ספקטרום עצום הבתים הארוטיים, שבהם הלקוחות דירות דיסקרטיות בתל אביב או דירות דיסקרטיות בחיפה מבקשים לפנק את רצונותיהם ללא חשש משיפוט או חשיפה. בית נערות ליווי
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha-3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captcha (antigate), RuCaptcha, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
245real.com
egyptnews24.com
Das Zet Casino ist eine beliebte Online-GlГјcksspielseite, die eine Vielzahl von Spielen und Boni fГјr ihre Kunden bietet. Ein besonders attraktives Angebot fГјr alle neuen Spieler ist der Zet Casino Promo-Code 2022.
Der Zet Casino Promo-Code 2022 ermöglicht es neuen Spielern, einen großzügigen Bonus zu erhalten, wenn sie sich auf der Website registrieren. Mit diesem Promo-Code können Spieler zusätzliches Geld erhalten, um ihre Lieblingsspiele zu spielen und mehr Gewinne zu erzielen.
Um den Zet Casino Promo-Code 2022 zu nutzen, müssen Spieler einfach bei der Registrierung den Code eingeben und eine Einzahlung tätigen. Sobald dies erledigt ist, wird der Bonus automatisch ihrem Konto gutgeschrieben und sie können sofort mit dem Spielen beginnen.
Der Zet Casino Promo-Code 2022 ist eine großartige Möglichkeit für neue Spieler, das Casino kennenzulernen und ihre Gewinnchancen zu erhöhen. Mit diesem Bonus haben Spieler die Möglichkeit, mehr Geld zu gewinnen und noch mehr Spaß an den Spielen zu haben.
Also, worauf warten Sie noch? Registrieren Sie sich noch heute beim Zet Casino und nutzen Sie den Promo-Code 2022, um einen tollen Bonus zu erhalten und die Spannung zu erleben, die dieses Casino zu bieten hat. Viel GlГјck und viel SpaГџ beim Spielen!
https://zetcasino.one/
В нашем мире, где диплом становится началом успешной карьеры в любом направлении, многие ищут максимально быстрый путь получения образования. Необходимость наличия официального документа трудно переоценить. Ведь диплом открывает двери перед каждым человеком, желающим начать профессиональную деятельность или продолжить обучение в ВУЗе.
Предлагаем быстро получить этот важный документ. Вы можете приобрести диплом старого или нового образца, и это является отличным решением для человека, который не смог завершить образование или потерял документ. Все дипломы производятся аккуратно, с максимальным вниманием к мельчайшим элементам. На выходе вы сможете получить продукт, 100% соответствующий оригиналу.
Преимущество этого подхода состоит не только в том, что можно максимально быстро получить диплом. Процесс организовывается удобно, с профессиональной поддержкой. От выбора подходящего образца до консультации по заполнению личных данных и доставки в любое место России — все под абсолютным контролем наших специалистов.
В результате, для всех, кто ищет максимально быстрый способ получить требуемый документ, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать продолжительного процесса обучения и не теряя времени переходить к достижению собственных целей: к поступлению в университет или к началу успешной карьеры.
http://molbiol.ru/forums/index.php?showtopic=1088346
https://forum.zub-zub.ru/viewtopic.php?t=25579
Tipico blockiert Casino
In den letzten Tagen haben viele Spieler berichtet, dass sie Probleme beim Zugriff auf das Online-Casino von Tipico haben. Der Sportwettenanbieter hat anscheinend bestimmte Länder davon abgehalten, auf das Casino zuzugreifen. Dies hat viele Spieler verärgert, die gerne Casino-Spiele bei Tipico genießen.
Die Blockierung des Casinos von Tipico betrifft vor allem Spieler aus Deutschland, Österreich und der Schweiz. Viele Nutzer haben versucht, das Problem zu lösen, indem sie den Kundensupport kontaktieren, aber bisher gibt es keine klare Erklärung für die Blockierung.
Einige Gerüchte besagen, dass Tipico möglicherweise Probleme mit den Glücksspielbehörden in den betroffenen Ländern hat und deshalb das Casino vorübergehend blockiert wurde. Andere vermuten, dass technische Probleme die Ursache für die Blockierung sein könnten.
Für die Spieler ist diese Blockierung sehr ärgerlich, da sie die Möglichkeit beraubt werden, ihre Lieblingsspiele im Casino von Tipico zu spielen. Viele Spieler sind auf der Suche nach alternativen Online-Casinos, um ihre Casino-Bedürfnisse zu befriedigen.
Wir hoffen, dass Tipico bald eine Lösung für dieses Problem findet und die Spieler wieder Zugriff auf das Casino erhalten. Bis dahin müssen die Spieler sich wohl oder übel nach anderen Optionen umsehen.
https://tipicocasino.one/
https://todayusanews24.com
https://radioshem.net
Сегодня, когда диплом становится началом успешной карьеры в любой отрасли, многие стараются найти максимально простой путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь диплом открывает дверь перед любым человеком, желающим начать трудовую деятельность или продолжить обучение в высшем учебном заведении.
В данном контексте наша компания предлагает максимально быстро получить этот важный документ. Вы имеете возможность купить диплом нового или старого образца, и это является удачным решением для всех, кто не смог завершить обучение, потерял документ или хочет исправить плохие оценки. Все дипломы выпускаются аккуратно, с особым вниманием ко всем нюансам, чтобы в итоге получился документ, максимально соответствующий оригиналу.
Преимущества этого решения заключаются не только в том, что можно быстро получить свой диплом. Процесс организован комфортно, с профессиональной поддержкой. Начав от выбора требуемого образца документа до грамотного заполнения персональной информации и доставки по России — все будет находиться под полным контролем качественных мастеров.
Для всех, кто ищет быстрый и простой способ получения необходимого документа, наша компания предлагает отличное решение. Заказать диплом – это значит избежать продолжительного процесса обучения и не теряя времени перейти к своим целям, будь то поступление в университет или старт успешной карьеры.
http://moskvichemania.ru/viewtopic.php?f=19&t=4095
http://entlebucher.bbok.ru/viewtopic.php?id=982
На сайте https://lan-union.ru вы сможете воспользоваться корпоративными сетевыми решениями, аудитом проектов для своих клиентов. Специально для вас разработана умная система индикации. Для того чтобы осуществить покупку, изучите весь каталог продукции. В него входит медный кабель, медные шнуры, а также оптический кабель, коммутационные шнуры оптические, конструктивы и шкафы, а также многое другое. В компании «ЛАН ЮНИОН» вы отыщите все, что необходимо для того, чтобы решить задачи, независимо от уровня их сложности.
На сайте https://esdogames.ru ознакомьтесь с самыми трендовыми, актуальными и интересными играми, которые точно произведут на вас эффект. Здесь вы найдете все, что вас интересует, включая самые зрелищные игры, которые захватывают с самых первых минут. Также представлен список лучших игр за 2024 год. Вы сможете поиграть во все, что хочется, прямо сейчас. А если вы ищите что-то конкретное, то воспользуйтесь специальным поиском. Подберите игру по жанру, режиму игры, платформе, чтобы облегчить поиск.
Willkommen im Zet Casino! Als neuer Spieler haben Sie die Möglichkeit, von einem großzügigen Willkommensbonus zu profitieren. Dieser Bonus ist eine tolle Möglichkeit, um Ihr Spielerlebnis im Zet Casino zu beginnen und Ihre Gewinnchancen zu steigern.
Der Willkommensbonus im Zet Casino besteht aus einem 100% Einzahlungsbonus von bis zu 500€ sowie 200 Freispielen für ausgewählte Spielautomaten. Um diesen Bonus zu erhalten, müssen Sie lediglich eine Mindesteinzahlung von 20€ tätigen. Sobald die Einzahlung getätigt wurde, wird der Bonus automatisch auf Ihr Konto gutgeschrieben.
Um den Bonus und die damit verbundenen Gewinne auszahlen zu können, müssen Sie die Umsatzanforderungen erfüllen. Diese betragen das 40-fache des Bonusbetrags. Beachten Sie, dass nicht alle Spiele zu den Umsatzanforderungen beitragen. Es ist daher ratsam, sich vorab die Bonusbedingungen durchzulesen.
Neben dem Willkommensbonus bietet das Zet Casino auch regelmäßig Aktionen und Promotionen für bestehende Spieler an. Diese können unter anderem Freispiele, Einzahlungsboni oder Cashback-Angebote beinhalten. Es lohnt sich daher, regelmäßig die Promotionsseite des Casinos zu besuchen, um keine Angebote zu verpassen.
Insgesamt bietet das Zet Casino eine Vielzahl von Spielen, darunter Spielautomaten, Tischspiele und Live-Casino-Spiele von bekannten Anbietern wie NetEnt, Microgaming und Evolution Gaming. Mit dem Willkommensbonus und den regelmäßigen Promotionen haben Sie die Möglichkeit, Ihr Spielerlebnis im Zet Casino zu maximieren und hoffentlich auch einige Gewinne zu erzielen.
Also worauf warten Sie noch? Registrieren Sie sich noch heute im Zet Casino und sichern Sie sich Ihren Willkommensbonus fГјr ein unvergessliches Spielerlebnis. Viel GlГјck und SpaГџ beim Spielen!
https://zetcasino.one/
В современном мире, где диплом – это начало отличной карьеры в любом направлении, многие стараются найти максимально быстрый путь получения качественного образования. Необходимость наличия документа об образовании переоценить попросту невозможно. Ведь именно диплом открывает двери перед любым человеком, который хочет начать трудовую деятельность или продолжить обучение в высшем учебном заведении.
Мы предлагаем очень быстро получить любой необходимый документ. Вы имеете возможность приобрести диплом, что становится отличным решением для всех, кто не смог закончить обучение, потерял документ или желает исправить свои оценки. Любой диплом изготавливается с особой тщательностью, вниманием ко всем нюансам, чтобы в итоге получился полностью оригинальный документ.
Превосходство такого решения заключается не только в том, что вы быстро получите свой диплом. Процесс организовывается удобно, с профессиональной поддержкой. Начав от выбора требуемого образца до грамотного заполнения личной информации и доставки в любой регион страны — все под полным контролем опытных мастеров.
Таким образом, всем, кто ищет максимально быстрый способ получения требуемого документа, наша услуга предлагает выгодное решение. Купить диплом – это значит избежать долгого обучения и сразу переходить к своим целям: к поступлению в ВУЗ или к началу трудовой карьеры.
https://msk-vegan.ru/viewtopic.php?id=9204
http://birdsmoscow.mybb.ru/viewtopic.php?id=388278
Вам интересен по разумным ценам прокат авто? Вам поможет Rent Me. Сервис предлагает подобрать и забронировать интересующую машину. Вы гарантированно получите услугу высочайшего качества. Все без исключения автомобили своевременно проходят техническое обслуживание, о поломках в пути можете даже не беспокоиться. Ищете сказки про животных для детей? Rent-me.cy – сайт, который на острове Кипр предоставляет прокатные машины. Мы сделали процесс аренды авто максимально простым и приятным. Будем рады вам ответить на все вопросы и пообщаться с вами, звоните.
Das Boomerang Casino GR ist ein aufregendes neues Online-Casino, das Spielern aus Griechenland eine Fülle an spannenden Spielmöglichkeiten bietet. Das Casino wurde erst kürzlich ins Leben gerufen und hat sich bereits einen Namen für sein umfangreiches Spielangebot und seine großzügigen Boni gemacht.
Das Boomerang Casino GR bietet eine Vielzahl von beliebten Casino-Spielen, darunter Slots, Tischspiele, Video Poker und Live-Casino-Spiele. Die Spiele stammen von einigen der besten Spieleentwickler der Branche, darunter NetEnt, Microgaming, Play’n GO und Evolution Gaming, um nur einige zu nennen. Die Spieler kГ¶nnen also sicher sein, dass sie ein hochwertiges Spielerlebnis genieГџen werden.
Darüber hinaus bietet das Boomerang Casino GR seinen Spielern großzügige Boni und Promotionen. Neue Spieler können sich über einen lukrativen Willkommensbonus freuen, der ihre Einzahlungen erhöht und ihnen zusätzliche Chancen bietet, große Gewinne zu erzielen. Das Casino bietet auch regelmäßige Promotionen, Turniere und Loyalty-Programme, um die Spieler bei Laune zu halten und sie für ihre Treue zu belohnen.
Das Boomerang Casino GR legt großen Wert auf die Sicherheit und Fairness seiner Spiele. Das Casino verfügt über eine Lizenz der Malta Gaming Authority, einer der angesehensten Glücksspielbehörden der Welt. Die Spieler können also sicher sein, dass ihre persönlichen Daten sicher sind und dass die Spiele fair sind und auf einem Zufallszahlengenerator basieren.
Insgesamt ist das Boomerang Casino GR eine spannende neue Option fГјr Spieler aus Griechenland, die nach einem erstklassigen Online-Casino suchen. Mit seinem umfangreichen Spielangebot, groГџzГјgigen Boni und strengen SicherheitsmaГџnahmen ist das Casino sicherlich einen Besuch wert.
https://boomerangcasino.one/
На сегодняшний день, когда диплом становится началом успешной карьеры в любом направлении, многие пытаются найти максимально простой путь получения образования. Наличие документа об образовании трудно переоценить. Ведь именно он открывает дверь перед людьми, стремящимися начать профессиональную деятельность или продолжить обучение в любом институте.
Предлагаем быстро получить этот необходимый документ. Вы сможете приобрести диплом, и это будет выгодным решением для человека, который не смог закончить обучение, потерял документ или желает исправить свои оценки. Все дипломы производятся с особой тщательностью, вниманием к мельчайшим нюансам. В результате вы получите документ, 100% соответствующий оригиналу.
Плюсы этого подхода состоят не только в том, что вы максимально быстро получите диплом. Процесс организован комфортно, с нашей поддержкой. От выбора необходимого образца до правильного заполнения персональной информации и доставки по России — все под абсолютным контролем квалифицированных специалистов.
Для тех, кто хочет найти оперативный способ получения необходимого документа, наша компания предлагает выгодное решение. Заказать диплом – значит избежать продолжительного процесса обучения и не теряя времени переходить к своим целям, будь то поступление в ВУЗ или старт профессиональной карьеры.
http://crimeadetka.forum.cool/viewtopic.php?id=1510
http://finans.webtalk.ru/viewtopic.php?id=6996
Хотите получить помощь хакера? Обращайтесь скорее к нам, мы предоставляем осуществление любых услуг взлома, гарантируем полную конфиденциальность ваших данных, приемлемые цены, оперативные сроки. Специалист имеет за спиной достаточный опыт и множество проделанных проектов. Ищете взломать сайт знакомств? Xakerplus.com – сайт, где можете узнать подробную информацию об услугах. Хакер не интересуется, зачем и для чего делаете заказ. Обращайтесь уже сейчас к специалисту, он решит любые задачи!
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha v.3, Hotmail (Microsoft), Google, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captcha (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
Zet Casino hat in der Online GlГјcksspielwelt viel Aufmerksamkeit erregt, und viele Spieler sind gespannt, was dieses Online Casino zu bieten hat. Deshalb haben wir uns entschlossen, einige Rezensionen Гјber Zet Casino zu sammeln und zu teilen.
In den meisten Rezensionen wird die breite Palette an Spielen gelobt, die im Zet Casino verfügbar sind. Von klassischen Tischspielen wie Blackjack und Roulette bis hin zu modernen Spielautomaten und Live-Dealer-Spielen bietet Zet Casino eine große Auswahl an Unterhaltungsmöglichkeiten für Spieler jeden Geschmacks.
Ein weiterer positiver Punkt, der in den Rezensionen immer wieder erwähnt wird, ist der ausgezeichnete Kundenservice von Zet Casino. Die Mitarbeiter sind freundlich, kompetent und rund um die Uhr erreichbar, um bei Fragen oder Problemen zu helfen. Diese schnelle und effiziente Unterstützung wird von vielen Spielern sehr geschätzt.
Darüber hinaus bieten Rezensenten von Zet Casino oft lobende Worte für die großzügigen Bonusangebote und Promotionen des Casinos. Neue Spieler können von lukrativen Willkommensboni profitieren, während treue Spieler regelmäßige Belohnungen und Sonderaktionen genießen können.
Einige Rezensionen haben jedoch auch einige Kritikpunkte an Zet Casino geäußert. Zum Beispiel wird in einigen Fällen die begrenzte Auswahl an Zahlungsmethoden bemängelt, während andere Spieler die Bedingungen für Bonusangebote als zu restriktiv empfunden haben.
Insgesamt ist das Feedback zu Zet Casino Гјberwiegend positiv, und viele Spieler empfehlen das Casino als eine unterhaltsame und vertrauenswГјrdige GlГјcksspielplattform. Wenn Sie also auf der Suche nach einem neuen Online Casino sind, sollten Sie Zet Casino definitiv in Betracht ziehen.
https://zetcasino.one/
Das Boomerang Casino ist für seine großzügigen Auszahlungen bekannt. Die Spieler können sich auf schnelle und unkomplizierte Auszahlungen freuen, sobald sie ihre Gewinne erzielt haben. Das Casino bietet verschiedene Zahlungsmethoden an, um den Auszahlungsprozess so bequem wie möglich zu gestalten.
Die Auszahlungen im Boomerang Casino werden in der Regel innerhalb von 24 Stunden bearbeitet, sodass die Spieler nicht lange auf ihr Geld warten müssen. Je nach gewählter Zahlungsmethode kann es allerdings einige Tage dauern, bis das Geld auf dem Konto des Spielers gutgeschrieben wird.
Um eine Auszahlung im Boomerang Casino anzufordern, müssen die Spieler lediglich ihr Konto verifizieren und die entsprechenden Informationen angeben. Dies dient der Sicherheit der Spieler und gewährleistet, dass die Auszahlung an die richtige Person erfolgt.
Das Boomerang Casino legt großen Wert auf die Zufriedenheit seiner Spieler und bietet daher einen erstklassigen Kundenservice, der bei Fragen oder Problemen mit Auszahlungen jederzeit zur Verfügung steht. Die Spieler können sich per Live-Chat, E-Mail oder Telefon an das Supportteam wenden und werden professionell und freundlich unterstützt.
Insgesamt bietet das Boomerang Casino eine hervorragende Auszahlungserfahrung, die es zu einer beliebten Wahl unter Spielern macht. Mit schnellen Auszahlungen, einer Vielzahl von Zahlungsmethoden und einem kompetenten Kundenservice können die Spieler im Boomerang Casino sicher sein, dass ihre Gewinne schnell und unkompliziert ausgezahlt werden.
https://boomerangcasino.one/
https://stroynews.info
olympic-school.com
Boomerang Casino Freispiele
Boomerang Casino ist eine beliebte Online-Glücksspielplattform, die ihren Spielern eine Vielzahl von Spielen und Boni bietet. Eine der attraktivsten Aktionen, die das Casino seinen Spielern bietet, sind die Boomerang Casino Freispiele. Diese Freispiele ermöglichen es den Spielern, bestimmte Spielautomaten kostenlos zu spielen und dabei echtes Geld zu gewinnen.
Die Boomerang Casino Freispiele sind eine großartige Möglichkeit, das Casino kennenzulernen und seine Top-Spiele auszuprobieren, ohne eigenes Geld einsetzen zu müssen. Diese Freispiele werden den Spielern entweder als Teil eines Willkommensbonus angeboten oder als regelmäßige Promotionen für bestehende Kunden.
Um die Boomerang Casino Freispiele zu erhalten, müssen die Spieler oft eine Einzahlung auf ihr Konto tätigen oder einen bestimmten Betrag in einem bestimmten Zeitraum spielen. Die Anzahl der Freispiele kann je nach Aktion variieren, aber in der Regel erhalten die Spieler zwischen 10 und 100 Freispiele.
Die Boomerang Casino Freispiele kГ¶nnen fГјr verschiedene Spielautomaten verwendet werden, darunter beliebte Titel wie Starburst, Book of Dead, Gonzo’s Quest und viele mehr. Die Spieler haben die MГ¶glichkeit, echtes Geld zu gewinnen, wГ¤hrend sie die Spiele mit ihren Freispielen spielen, was diese Aktionen besonders attraktiv macht.
Insgesamt bieten die Boomerang Casino Freispiele den Spielern die Möglichkeit, neue Spiele auszuprobieren, ihre Gewinnchancen zu erhöhen und zusätzliche Preise zu gewinnen. Werfen Sie also einen Blick auf die aktuellen Promotionen von Boomerang Casino und sichern Sie sich Ihre Freispiele für eine spannende und unterhaltsame Spielerfahrung.
https://boomerangcasino.one/
В Москве всегда можно встретить красивых и ухоженных девушек, которые знают, как привлечь внимание и оставить впечатление. Я решил исследовать этот мир и найти место, где собраны самые привлекательные представительницы столицы, готовые к флирту и приключениям.
На сайте знакомств я обнаружил настоящий рай для глаз – множество красивых и стильных девушек, которые следят за собой, обладают безупречным вкусом и знают, как выглядеть на все сто. Они были как модельные фотосессии на страницах глянцевых журналов – элегантные, стильные и уверенные в себе.
Мои встречи с ними были наполнены шармом и атмосферой роскоши. Мы гуляли по центру города, обсуждали модные тренды и планировали свои будущие встречи. И хотя каждая из них была уникальной и особенной, они всех объединяло одно – непревзойденная красота и стиль.
Флирт на сайтах знакомств – это не только способ развлечься, но и возможность окунуться в мир элегантности и красоты. Я благодарен этому опыту за возможность познакомиться с такими потрясающими девушками и насладиться их прекрасной компанией.
Стань частью большого сообщества людей, ищущих любовь и приключения!
http://web011.dmonster.kr/bbs/board.php?bo_table=b0501&wr_id=1952779
https://www.godo.fitness/so-why-should-i-get-a-personal-trainer/?unapproved=266211&moderation-hash=ad61008f43e67d08938d2ab9097533cb#comment-266211
https://xn--42c6abc2ej8aza1e5f4c.com/%e0%b8%aa%e0%b8%a5%e0%b9%87%e0%b8%ad%e0%b8%95%e0%b9%80%e0%b8%84%e0%b8%a3%e0%b8%94%e0%b8%b4%e0%b8%95%e0%b8%9f%e0%b8%a3%e0%b8%b5/#comment-1691
https://parcelhusmaegleren.dk/staaltagplader-jem-and-fix-den-bedste-maade-at-beskytte-dit-hjem-paa/#comment-36520
https://osrprojects.co.uk/event/artist-talk-at-outpost#comment-57407
http://netzhorst.de/archives/43#comment-486506
https://www.jkv-solar.de/2019/12/29/solaranlage-holle-2/#comment-4137
https://juangonzalezestudio.com/revolutionizing-the-way-we-use-applications/#comment-491
https://www.thenewsbusters.com/worldpay-vs-stripe/#comment-60072
https://listingdoor.com/thank-you-page/#comment-145177
На сайте https://doka-stroi.ru оставьте заявку для того, чтобы воспользоваться такими популярными услугами, как: ремонт квартир, дизайн интерьера, ремонт комнат. Все услуги оказываются под ключ, а в работе применяются инновационные, уникальные технологии. Услуги оказываются точно в строго оговоренное время, а все обязательства сторон прописываются в договоре. В компании трудится опытная команда специалистов с соответствующим образованием. Имеется собственная материально-техническая база. Все работы проходят строгий контроль на каждом этапе.
На сайте http://smartporog.ru посмотрите весь каталог такого популярного товара, как выпадающие умные пороги. Автоматические пороги считаются оптимальным решением, если установить стационарные варианты не представляется возможным. К важным преимуществам таких конструкций относят то, что они ликвидируют преграду в полу, справляются с холодом, сквозняками, морозом, повышают звукоизоляцию, не задерживают влагу, отводят посторонние запахи. Изделия выполнены из надежных, практичных материалов.
Когда я встретил ее на вечеринке в центре Москвы, сразу было видно, что она привыкла к роскоши и богатству. Ее изысканный наряд, дорогие украшения и аромат дорогого парфюма создавали вокруг нее атмосферу изысканности и роскоши.
Мы начали общаться, и я быстро понял, что она ценит те же ценности, что и я – роскошь, комфорт и красоту. Когда я предложил ей отправиться в Дубай на неделю, чтобы насладиться шикарными отелями, роскошными ресторанами и бескрайними пляжами, она согласилась без колебаний.
В Дубае наша любовь расцвела на фоне бесконечного блеска и роскоши. Мы катались на верблюдах по пустыне, купались в искусственных оазисах и наслаждались закатами над Аравийским заливом. Каждый день приносил нам новые впечатления и эмоции, и я чувствовал, что наша связь становится все крепче.
Несмотря на все богатство и роскошь, которые нас окружали, я понимал, что наше знакомство основано не только на материальных ценностях, но и на искреннем взаимопонимании и чувствах. И хотя наш отпуск в Дубае подошел к концу, наши воспоминания о нем останутся в моей памяти навсегда.
Стань частью большого сообщества людей, ищущих любовь и приключения!
https://thenoteplus.com/whats-covered-understanding-the-scope-of-comprehensive-health-insurance/#comment-2358
https://tfw49.com/2022-springsummer-collection-exhibition%e3%80%80episode-2/#comment-211042
https://camphalfbloodrp.com/index.php?/topic/3811-%D0%BF%D1%80%D0%BE%D1%81%D1%82%D0%B8%D1%82%D1%83%D1%82%D0%BA%D0%B8-%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D1%8B%D0%B9-%D1%81%D1%82%D1%80%D0%BE%D0%B8%D1%82%D0%B5%D0%BB%D1%8C/
https://znews.mn/2022/06/15/1021/#comment-3816
http://osmi.co.kr/bbs/board.php?bo_table=after&wr_id=63944
https://www.shininguttarakhandnews.com/love-birds-video-parrot/#comment-1740004
https://tazamarathi.com/%e0%a4%91%e0%a4%b8%e0%a5%8d%e0%a4%95%e0%a4%b0-%e0%a4%85%e0%a4%b5%e0%a5%89%e0%a4%b0%e0%a5%8d%e0%a4%a1%e0%a4%b8-2024-%e0%a4%ae%e0%a4%a7%e0%a5%8d%e0%a4%af%e0%a5%87-oppenheimer-%e0%a4%9a%e0%a5%80/#comment-481
https://forumnaturalisation.fr/a-qui-declarer-votre-changement-dadresse/#comment-301577
https://uiwang.shop/%ea%b0%90%ed%99%8d%ec%9d%84-%ec%95%84%ec%8b%9c%eb%82%98%ec%9a%94%eb%ac%b4%ea%b6%81%eb%ac%b4%ec%a7%84%ed%95%9c-%ec%82%ac%ea%b3%bc%ec%9d%98-%eb%a7%a4%eb%a0%a5-%ed%97%ac%ec%8a%a4-3/#comment-1854
https://dfrca.co.za/2023/09/17/email-from-callie/#comment-505
pervenec.com
Zet Casino Einzahlungsmöglichkeiten
Das Zet Casino bietet seinen Spielern eine Vielzahl von Einzahlungsmöglichkeiten, um ihr Spielerlebnis so bequem wie möglich zu gestalten. Egal ob Sie per Kreditkarte, e-Wallet oder Banküberweisung einzahlen möchten, das Zet Casino hat für jeden die passende Option.
Eine der beliebtesten Einzahlungsmöglichkeiten im Zet Casino ist die Verwendung von Kreditkarten wie Visa und Mastercard. Diese Zahlungsmethode ist schnell, sicher und unkompliziert. Spieler können einfach ihre Kreditkartendaten eingeben und schon kann die Einzahlung getätigt werden.
Für diejenigen, die lieber e-Wallets verwenden, stehen im Zet Casino auch Optionen wie Skrill, Neteller und EcoPayz zur Verfügung. Diese ermöglichen es Spielern, ihr Geld sicher und schnell zu transferieren, ohne persönliche Bankdaten preiszugeben.
Eine weitere populäre Einzahlungsoption im Zet Casino ist die Banküberweisung. Obwohl diese Methode etwas länger dauern kann als andere, ist sie sicher und zuverlässig. Spieler können einfach den Betrag auf das angegebene Konto überweisen und ihre Einzahlung wird innerhalb weniger Tage gutgeschrieben.
Zusätzlich zu diesen Einzahlungsmöglichkeiten bietet das Zet Casino auch verschiedene alternative Methoden wie Paysafecard, Trustly und Bitcoin an. Diese ermöglichen es Spielern, ihre Einzahlungen auf ihre bevorzugte Weise zu tätigen.
Insgesamt bietet das Zet Casino eine breite Palette an Einzahlungsmöglichkeiten, um sicherzustellen, dass Spieler aus aller Welt bequem einzahlen können. Egal für welche Methode Sie sich entscheiden, im Zet Casino können Sie sicher sein, dass Ihre Einzahlung schnell und sicher abgewickelt wird.
https://zetcasino.one/
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha v.3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captchas.com (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
Компания «ВДГБ» предлагает купить программу 1С. Стараемся предлагать нашим клиентам услуги исключительно высокого качества. Ориентированы на длительное сотрудничество и на максимальное удовлетворение ваших потребностей. Ищете 1с бухгалтерия 8 купить москва? Vdgb.ru – здесь найдете на продукты 1С прайс-лист. Здесь также можете ознакомиться с условиями оплаты и доставки. Если будет необходимо мы вас проконсультируем, впишите на портале в специальную форму свой номер и имя, также E-mail, затем нажмите на «Отправить». Оцените комфорт при работе с программой 1С!
Купить диплом с доставкой до дома, онлайн.
Как купить диплом без риска, без заморочек.
Купить диплом с гарантией качества, проверенные варианты.
Почему выгодно купить диплом, рассказываем.
Где купить диплом без проблем, без риска.
Лучшие предложения по покупке диплома, интересные варианты.
Дипломы на заказ по лучшим ценам, подробности на сайте.
Покупка диплома: безопасность и конфиденциальность, наши преимущества.
Лучшие дипломы для покупки, срочно и выгодно.
Купить диплом срочно и законно, подробности у нас.
Официальные документы для покупки, лучшие цены.
Как купить диплом срочно, лучшие условия.
Купить диплом без обмана, гарантированный результат.
Дипломы на всех условиях, подробности на сайте.
Легальная покупка дипломов безопасно, гарантированная доставка.
Какой диплом выбрать для покупки, гарантированный результат.
Купить диплом с доставкой по всему миру, лучшие условия.
Официальный документ об образовании, гарантированный результат.
купить диплом http://7arusak-diploms.com/ .
Zet Casino Lizenz
Das Thema Glücksspiel und Online-Casinos ist in Deutschland immer wieder Gegenstand von Diskussionen und Regulierungen. Eine wichtige Rolle spielen dabei die Lizenzen, die von den Betreibern der Online-Casinos benötigt werden, um ihre Dienste legal in Deutschland anbieten zu können.
Ein Online-Casino, das in den vergangenen Jahren viel Aufmerksamkeit erhalten hat, ist das Zet Casino. Es handelt sich um einen Anbieter, der eine Vielzahl von Spielen und Angeboten für seine Kunden bereithält. Doch wie sieht es eigentlich mit der Lizenzierung des Zet Casinos aus?
Das Zet Casino verfügt über eine Lizenz der Malta Gaming Authority. Diese gilt als eine der renommiertesten und strengsten Glücksspielbehörden in Europa. Die Lizenzierung durch die MGA bedeutet, dass das Zet Casino bestimmte Auflagen und Regularien erfüllen muss, um seinen Betrieb aufrechtzuerhalten.
Dazu gehören unter anderem Maßnahmen zur Bekämpfung von Geldwäsche und Spielsuchtprävention. Darüber hinaus wird die Fairness der Spiele und die Sicherheit der Kundendaten regelmäßig überprüft.
Für Spielerinnen und Spieler ist es wichtig, auf die Lizenzierung eines Online-Casinos zu achten, um sicherzustellen, dass sie einem seriösen Anbieter vertrauen können. Mit der Malta Gaming Authority als Lizenzgeber kann das Zet Casino hier punkten und bietet seinen Kunden ein sicheres und verantwortungsvolles Spielerlebnis.
Insgesamt lässt sich sagen, dass das Zet Casino mit seiner Lizenzierung durch die Malta Gaming Authority eine solide Basis für sein Glücksspielangebot geschaffen hat. Spielerinnen und Spieler können somit beruhigt und mit gutem Gewissen die vielfältigen Spiele und Angebote des Zet Casinos nutzen.
https://zetcasino.one/
БК Леон считается прекрасной платформой для увлекательных игр. Здесь большой выбор ставок и живая статистика. Вы можете уже сейчас начать с уверенности благодаря бонусам для новичков. Простой интерфейс, оперативные выплаты и щедрые бонусы – это все о БК Леон. https://t.me/s/mleon_ru – канал, где вы можете присоединиться к сообществу ценителей спорта и начать выигрывать реальные деньги. Самый лучший сервис ждет вас, тут каждый шаг приведет вас к победе! Сделайте свой ход к успеху уже сегодня, выбирайте Леон. Вас ждет нереальная острота ощущений, убедитесь в этом лично!
Tipico Casino Bonus Code Free Spins 2019
Das Tipico Casino ist bekannt für seine großzügigen Bonusangebote und Promotionen für neue und bestehende Kunden. Auch in diesem Jahr bietet das Casino seinen Spielern die Möglichkeit, von attraktiven Bonus Codes und Free Spins zu profitieren. Im Jahr 2019 können sich Spieler über zahlreiche lukrative Angebote freuen, die das Spielerlebnis im Tipico Casino noch spannender gestalten.
Ein besonders beliebtes Angebot sind die Free Spins, die den Spielern die Möglichkeit geben, an ausgewählten Spielautomaten kostenlos zu spielen und dabei echte Gewinne zu erzielen. Mit dem richtigen Bonus Code können Spieler eine bestimmte Anzahl an Free Spins erhalten, die sie im Casino einsetzen können. Diese Free Spins sind eine großartige Möglichkeit, neue Spiele auszuprobieren und vielleicht sogar einen Jackpot zu knacken.
Um den Bonus Code für Free Spins im Tipico Casino zu erhalten, müssen Spieler bestimmte Bedingungen erfüllen. Oftmals ist es notwendig, eine Mindesteinzahlung zu tätigen oder einen bestimmten Betrag im Casino umzusetzen. Sobald diese Bedingungen erfüllt sind, wird der Bonus Code aktiviert und die Free Spins stehen zur Verfügung.
Es lohnt sich, regelmäßig auf der Website des Tipico Casinos vorbeizuschauen, um keine der aktuellen Promotionen zu verpassen. Dort werden nicht nur die neuesten Bonus Codes und Free Spins angekündigt, sondern auch über Sonderaktionen und Gewinnspiele informiert. Mit etwas Glück können Spieler so zusätzliche Gewinne und Belohnungen erhalten.
Fazit: Der Tipico Casino Bonus Code für Free Spins 2019 bietet Spielern die Möglichkeit, kostenlos an Spielautomaten zu spielen und dabei echte Gewinne zu erzielen. Um von diesen Angeboten zu profitieren, sollten Spieler die Bedingungen genau beachten und regelmäßig auf der Website des Casinos vorbeischauen. Mit etwas Glück können sie so ihre Gewinnchancen im Tipico Casino erhöhen.
https://tipicocasino.one/
kraken – kraken tor, kraken вход
2fight.info
kraken onion – kraken зеркало даркнет, kraken официальный сайт
kraken tor – kraken вход, kraken зеркало официальный
Спортивные силовые тренажеры на silovye-trenazhery.ru – это продуктивные устройства для прорабатки всех мышц. Делятся на блочные и с нагрузкой дисками. Актуальны для улучшения формы тела.
Производимые российской компанией силовые тренажеры не нуждаются в постоянном обслуживании. В напряженных узлах используются подшипники закрытого типа.
Всегда в наличии: одинарный Кроссовер, Баттерфляй для грудных, Хаммер, горизонтальная тяга, тренажер Скотта, Дельта машину, станок Гаккеншмидта, конструкции для работы с собственным весом, Гравитрон для подтягивания и отжиманий, гиперэкстензия, скамьи для жима со стойками, универсальная лавка, силовая рама Смита.
Всегда востребованы в спортивных залах мультистанции для прорабатки всех мышц.
Zet Casino Promo Code 2023: Alle Informationen, die Sie wissen mГјssen
Zet Casino ist eine beliebte Online-Spielplattform, die eine Vielzahl von Spielen und Promotionen für Spieler bietet. Eine der aufregendsten Aktionen, auf die sich Spieler freuen können, ist der Zet Casino Promo Code 2023. Dieser spezielle Code bietet Spielern die Möglichkeit, zusätzliche Belohnungen und Boni zu erhalten, wenn sie ihn bei der Anmeldung oder Einzahlung verwenden. In diesem Artikel werden wir alle wichtigen Informationen zu diesem aufregenden Angebot präsentieren.
Was ist der Zet Casino Promo Code 2023?
Der Zet Casino Promo Code 2023 ist ein spezieller Code, der von Zet Casino herausgegeben wird, um Spielern zusätzliche Boni und Belohnungen zu bieten. Spieler können diesen Code eingeben, wenn sie ein neues Konto erstellen oder eine Einzahlung tätigen, um von den zusätzlichen Leistungen zu profitieren. Der Promo-Code kann je nach Aktion unterschiedlich sein und kann verschiedene Arten von Belohnungen wie Bonusgelder, Freispiele oder Cashback-Angebote bieten.
Wie verwende ich den Zet Casino Promo Code 2023?
Um den Zet Casino Promo Code 2023 zu verwenden, müssen Sie ihn während des Anmelde- oder Einzahlungsvorgangs eingeben. Wenn Sie ein neuer Spieler sind, können Sie den Code bei der Kontoerstellung eingeben, um Ihre Belohnung zu erhalten. Wenn Sie bereits ein Konto haben und eine Einzahlung tätigen möchten, können Sie den Promo-Code während des Einzahlungsvorgangs eingeben, um zusätzliche Boni zu erhalten. Stellen Sie sicher, dass Sie den Code korrekt eingeben, um sicherzustellen, dass Sie die Belohnung erhalten.
Welche Vorteile bietet der Zet Casino Promo Code 2023?
Der Zet Casino Promo Code 2023 bietet Spielern eine Vielzahl von Vorteilen und Belohnungen. Zu den möglichen Belohnungen gehören Bonusgelder, Freispiele, Cashback-Angebote und vieles mehr. Diese Belohnungen können verwendet werden, um Ihre Gewinnchancen zu erhöhen und Ihr Spielerlebnis zu verbessern. Darüber hinaus können Spieler von exklusiven Aktionen und Sonderangeboten profitieren, die nur für diejenigen gelten, die den Promo-Code verwenden. Insgesamt bietet der Zet Casino Promo Code 2023 eine großartige Möglichkeit, zusätzliche Belohnungen zu erhalten und Ihr Spielerlebnis zu maximieren.
Fazit
Der Zet Casino Promo Code 2023 ist eine aufregende Aktion, die Spielern die Möglichkeit bietet, zusätzliche Belohnungen und Boni zu erhalten. Spieler können diesen Code verwenden, um exklusive Angebote zu erhalten und ihre Gewinnchancen zu erhöhen. Wenn Sie also auf der Suche nach zusätzlichen Belohnungen und Vorteilen sind, sollten Sie den Zet Casino Promo Code 2023 unbedingt in Betracht ziehen. Wir empfehlen Ihnen, die Website von Zet Casino zu besuchen, um weitere Informationen zu erhalten und den Promo-Code zu erhalten. Viel Spaß beim Spielen und viel Glück!
https://zetcasino.one/
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha v.3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12000
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captchas.com (antigate), rucaptcha.com, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://XEvil.Net/
Das Tipico Casino ist für viele Spieler eine beliebte Anlaufstelle, um ihr Glück bei verschiedenen Casino-Spielen zu versuchen. Ein wichtiger Aspekt beim Spielen in einem Online-Casino ist der maximale Einsatz, den man tätigen kann. Der maximale Einsatz im Tipico Casino variiert je nach Spiel und kann eine wichtige Rolle bei der Entscheidung spielen, welches Spiel man spielen möchte.
Der maximale Einsatz im Tipico Casino kann je nach Spiel unterschiedlich sein. Beispielsweise liegt der maximale Einsatz bei Spielautomaten oft bei 5€ bis 10€ pro Drehung. Bei Tischspielen wie Roulette oder Blackjack kann der maximale Einsatz deutlich höher liegen, manchmal sogar bis zu mehreren hundert Euro pro Runde.
Es ist wichtig, sich vor Beginn des Spiels über den maximalen Einsatz zu informieren, um unangenehme Überraschungen zu vermeiden. Es empfiehlt sich außerdem, ein Budget festzulegen und sich daran zu halten, um mögliche Verluste zu begrenzen.
Wer im Tipico Casino spielen möchte, sollte außerdem darauf achten, verantwortungsbewusst zu spielen und sich der Risiken bewusst zu sein. Glücksspiel kann süchtig machen und sollte daher immer mit Maß und Vernunft betrieben werden.
Alles in allem bietet das Tipico Casino eine Vielzahl von Spielen mit unterschiedlichen maximalen Einsätzen an, sodass für jeden Spieler etwas Passendes dabei ist. Wichtig ist es, verantwortungsbewusst zu spielen und sich an das eigene Budget zu halten, um ein möglichst unterhaltsames und sicheres Spielerlebnis zu gewährleisten.
https://tipicocasino.one/
На сайте https://www.avtogalaktika.com/ оставьте сообщение для того, чтобы воспользоваться займом под ПТС, получить деньги под залог автомобиля, наличные под залог машины, под залог спецтехники. Специально для вас оперативное и выгодное получение кредита. Прямо сейчас вы сможете ознакомиться с тем, какие автомобили сможете приобрести в данную минуту. Перед вами все самые популярные марки машин, которые находятся в отличном состоянии. Для того чтобы получить консультацию, заполните заявку, чтобы вам перезвонил менеджер.
Завод из России продает разборные гантели на gantelya-razbornaya.ru для домашних тренировок.
Все наборы сборных снарядов комплектуются фиксаторами, дисками. Гантельные грифы выпускаются с разными посадочными диаметрами. Для защиты от ударов все грифы никелируются.
Изготавливаемые утяжелители не нуждаются в постоянном обслуживании и ориентированы на длительную работу в доме или тренажерных залах.
Позволяют прорабатывать все мышцы. С наборными снарядами можно быстро улучшить координацию, ловкость и увеличить силовые возможности.
Обрезиненные диски обеспечивают более безопасные условия.
Оформляя в российской компании вы получаете лучшие снаряды для удобных тренировок.
https://oda-radio.com
На сайте http://waltzprof.com каждый желающий получает возможность приобрести стальной профиль высокого качества и созданный из надежных, практичных материалов. За счет этого изделия прослужат в течение длительного времени и не покроются коррозией. В этой компании они представлены в широком ассортименте, что позволит подыскать решение в соответствии с предпочтениями. Профиль применяется для оперативной, комфортной сборки ограждающих преград, лофт перегородок, фасадных конструкций, ворот. Для реализации проекта используются уникальные и инновационные технологии, передовое оборудование.
holidaynewsletters.com
Zet Casino ist ein Online-Casino, das seinen Spielern eine Vielzahl von spannenden Spielen und lukrativen Bonusangeboten bietet. Eines der beliebtesten Bonusangebote im Zet Casino sind die 30 Freispiele, die neue Spieler erhalten können.
Um die 30 Freispiele zu erhalten, müssen Spieler lediglich ein Konto im Zet Casino erstellen und ihre erste Einzahlung tätigen. Nachdem die Einzahlung erfolgreich abgeschlossen wurde, werden die Freispiele automatisch dem Spielerkonto gutgeschrieben und können sofort für ausgewählte Spielautomaten genutzt werden.
Die 30 Freispiele sind eine großartige Möglichkeit, das Zet Casino und seine Spiele ohne Risiko zu testen und gleichzeitig die Chance zu haben, echtes Geld zu gewinnen. Spieler können die Freispiele nutzen, um ihre Lieblingsspiele zu spielen oder neue Spiele auszuprobieren und dabei vielleicht sogar einen großen Gewinn zu erzielen.
Es ist jedoch wichtig zu beachten, dass die Freispiele bestimmten Umsatzbedingungen unterliegen, bevor Gewinne ausgezahlt werden können. Spieler sollten sich daher vor der Nutzung der Freispiele die Bonusbedingungen genau durchlesen, um sicherzustellen, dass sie alle Anforderungen erfüllen.
Insgesamt sind die 30 Freispiele im Zet Casino eine attraktive Bonusaktion, die es neuen Spielern ermöglicht, das Casino und seine Spiele ohne finanzielles Risiko kennenzulernen. Wer also auf der Suche nach einem seriösen Online-Casino mit lukrativen Bonusangeboten ist, sollte sich das Zet Casino genauer ansehen.
https://zetcasino.one/
Boomerang Casino Einzahlungscode
Boomerang Casino ist ein beliebter Online-Glücksspielanbieter, der Spielern eine Vielzahl von Spielen und spannenden Aktionen bietet. Eine der beliebtesten Aktionen bei Boomerang Casino ist der Einzahlungscode, der es Spielern ermöglicht, zusätzliche Boni und Freispiele zu erhalten.
Der Boomerang Casino Einzahlungscode ist eine spezielle Kombination aus Zahlen und Buchstaben, die Spieler während ihrer Einzahlung eingeben können, um den entsprechenden Bonus zu erhalten. Diese Codes werden regelmäßig angeboten und sind eine großartige Möglichkeit für Spieler, mehr aus ihrem Gaming-Erlebnis herauszuholen.
Um den Boomerang Casino Einzahlungscode zu nutzen, müssen Spieler zunächst ein Konto bei Boomerang Casino erstellen und eine Einzahlung tätigen. Während des Einzahlungsvorgangs wird ein Feld für den Einzahlungscode angezeigt, in das Spieler den Code eingeben können. Sobald der Code bestätigt wurde, wird der entsprechende Bonus automatisch dem Spielerkonto gutgeschrieben.
Die Boni, die Spieler mit dem Boomerang Casino Einzahlungscode erhalten können, variieren je nach Aktion. Dies kann zusätzliches Bonusgeld, Freispiele oder andere Belohnungen umfassen. Es lohnt sich daher, regelmäßig die Promotionen auf der Boomerang Casino Website zu überprüfen, um keine der attraktiven Aktionen zu verpassen.
Insgesamt ist der Boomerang Casino Einzahlungscode eine großartige Möglichkeit für Spieler, ihre Gewinnchancen zu erhöhen und noch mehr Spaß beim Spielen zu haben. Mit regelmäßigen Aktionen und lukrativen Boni ist Boomerang Casino definitiv einen Besuch wert.
Also, worauf warten Sie noch? Besuchen Sie noch heute Boomerang Casino, nutzen Sie den Einzahlungscode und genieГџen Sie ein groГџartiges Spielerlebnis! Viel GlГјck!
https://boomerangcasino.one/
kraken ссылка зеркало – http kraken, kraken
почему не работает mega sb – mega555 зеркало рабочее, mega555
кракен зеркало – kraken darknet, кракен зеркало
На сайте https://incubatoreggs.ru/ ознакомьтесь с телефоном для того, чтобы заказать инкубационное яйцо высокого качества от цыплят, индейки, курицы-бройлера, утки, гуся. Вся продукция от сельскохозяйственных, домашних птиц. Они от лучших, зарекомендовавших себя фабрик России, Европы. Это ваша уникальная возможность приобрести инкубаторную продукцию по стоимости завода и даже ниже. Самым популярным является яйцо индейки, утки, гуся. Вы сможете воспользоваться бесплатной доставкой по городу, если сделаете заказ на сумму от 3 000 рублей.
Im Boomerang Casino können Spieler problemlos Einzahlungen tätigen und Gewinne erzielen. Doch was passiert, wenn man sich entscheidet, seine Gewinne auszuzahlen? In diesem Artikel gehen wir näher auf den Prozess der Auszahlung im Boomerang Casino ein.
Sobald ein Spieler Gewinne erzielt hat und diese auszahlen lassen möchte, kann er dies ganz einfach im Kassenbereich des Casinos tun. Dort muss der Spieler lediglich auf den Button für Auszahlungen klicken und die gewünschte Auszahlungsmethode auswählen. Im Boomerang Casino stehen verschiedene Zahlungsmethoden wie Kreditkarten, E-Wallets und Banküberweisungen zur Verfügung, aus denen Spieler wählen können.
Nachdem der Spieler die Auszahlungsmethode gewählt hat, muss er den Betrag eingeben, den er auszahlen lassen möchte. Es ist wichtig zu beachten, dass das Boomerang Casino möglicherweise bestimmte Mindest- und Höchstauszahlungslimits hat, die eingehalten werden müssen. Sobald der Auszahlungsantrag bearbeitet wurde, wird der Betrag auf das vom Spieler gewählte Konto überwiesen.
Es ist wichtig zu erwähnen, dass Auszahlungen im Boomerang Casino in der Regel innerhalb von 24 Stunden bearbeitet werden. Allerdings kann es je nach Auszahlungsmethode und Bankinstitut variieren, wie lange es dauert, bis das Geld tatsächlich auf dem Konto des Spielers gutgeschrieben wird.
Insgesamt bietet das Boomerang Casino einen reibungslosen und benutzerfreundlichen Auszahlungsprozess für seine Spieler. Mit einer Vielzahl von Zahlungsmethoden und schnellen Auszahlungszeiten können Spieler ihre Gewinne schnell und einfach genießen.
https://boomerangcasino.one/
Вам интересен по разумным ценам прокат авто? Вам поможет Rent Me. Сервис предлагает подобрать и забронировать интересующую машину. Вы получите по гарантии услугу высшего качества. Все без исключения автомобили своевременно проходят техническое обслуживание, о поломках в пути можете даже не беспокоиться. Ищете стоимость аренды автомобиля на кипре? Rent-me.cy – сайт, который на острове Кипр предоставляет прокатные машины. Мы сделали процесс аренды авто максимально простым и приятным. Звоните, будем рады с вами пообщаться и ответить на все вопросы.
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha-3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captcha (antigate), rucaptcha.com, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
Хотите купить Вегови в Москве с оперативной доставкой по выгодной цене? Мы официальный поставщик Вегови и прочих лекарств для мед. центров Москвы. У нас в наличии все дозировки препарата Вегови. https://wegovy-russia.ru – сайт, где имеются фото людей до и после применения Вегови. Представлены и актуальные цены на Вегови. У нас вы в любое время можете ознакомиться с отзывами клиентов. Чтобы приобрести Вегови, вам нужно связаться с менеджером по WhatsApp. Вы узнаете, как работает Вегови, на сколько можно похудеть, как храним Вегови.
Такси Минивэн Онлайн предоставляет по приемлемым ценам качественные услуги. В салоне авто помещаются 8 человек с комфортом. Машины оборудованы детскими креслами. Все без исключения водители вежливые, они прошли школу мастерства. Ищете такси минивэн? Minivan.online – сайт, где имеется детальная информация, посмотрите ее в любое время. Также тут указана стоимость поездки. Заказ такси минивэн выполняется по телефону. Звоните нам и мы дадим для вас грамотную консультацию!
Das Zet Casino ist bei vielen Spielern beliebt, die gerne Online-Casino-Spiele spielen. Doch kГјrzlich haben einige Benutzer Berichte darГјber gemacht, dass sie ihr Auszahlungslimit im Casino erreicht haben.
Ein Auszahlungslimit wird von Casinos festgelegt, um sicherzustellen, dass Spieler nicht zu viel Geld auf einmal abheben können. Dies dient dazu, sowohl die Spieler als auch das Casino selbst vor Betrug zu schützen. Wenn ein Spieler sein Auszahlungslimit erreicht hat, kann er keine weiteren Auszahlungen tätigen, bis das Limit zurückgesetzt wird.
Es ist wichtig, sich über die Auszahlungslimits eines Casinos zu informieren, bevor man mit dem Spielen beginnt. Die Limits können je nach Casino variieren und können von Zeit zu Zeit geändert werden. Spieler sollten sich bewusst sein, dass sie ihr Limit erreichen können und möglicherweise warten müssen, bis es zurückgesetzt wird.
Wenn ein Spieler sein Auszahlungslimit im Zet Casino erreicht hat, kann er sich an den Kundenservice des Casinos wenden, um weitere Informationen zu erhalten. Es ist wichtig, geduldig zu sein und die Richtlinien des Casinos zu respektieren.
Insgesamt ist es wichtig, verantwortungsbewusst zu spielen und sich Гјber die Auszahlungslimits eines Casinos im Klaren zu sein. Spieler sollten ihr Spielverhalten im Auge behalten und wissen, wann es Zeit ist, eine Pause einzulegen.
https://zetcasino.one/
Интернет-магазин «МОЙ и ТВОЙ» предлагает в огромном ассортименте уютные и полезные презенты, нужные в быту вещи и продукцию для украшения, создания привлекательного интерьера. А если необходимо найти что-то определенное, то воспользуйтесь специальным поиском, который найдет все, что нужно. На сайте https://moi-tvoi.ru/ ознакомьтесь с полным ассортиментом магазина.
Tipico Casino: 10 Freispiele
Das Tipico Casino bietet seinen Spielern regelmäßig attraktive Bonusaktionen an, um das Spielerlebnis noch spannender und lukrativer zu gestalten. Eine beliebte Form des Bonus sind die sogenannten Freispiele, mit denen man kostenlos an ausgewählten Spielautomaten spielen kann.
Aktuell bietet das Tipico Casino seinen Kunden 10 Freispiele an, die sie für bestimmte Slots nutzen können. Diese Freispiele können entweder als Teil eines Willkommensbonus oder in Form von regelmäßigen Aktionen vergeben werden.
Um von den 10 Freispielen zu profitieren, müssen die Spieler lediglich die entsprechende Aktion im Casino auswählen und den Anweisungen folgen. Oftmals müssen sie dafür eine Mindesteinzahlung tätigen oder einen bestimmten Umsatz an ausgewählten Spielen erzielen.
Die Freispiele können anschließend an den ausgewählten Slots eingelöst werden und ermöglichen es den Spielern, ohne eigenen Einsatz Gewinne zu erzielen. Dabei gelten meist Umsatzbedingungen, die erfüllt werden müssen, bevor eine Auszahlung der Gewinne möglich ist.
Die 10 Freispiele im Tipico Casino bieten den Spielern die Möglichkeit, neue Spielautomaten kennenzulernen, ohne dabei eigenes Geld riskieren zu müssen. Zusätzlich erhöhen sie die Gewinnchancen und sorgen für zusätzlichen Spielspaß.
Wer also Lust auf spannende Spielautomaten und die Chance auf attraktive Gewinne hat, sollte die 10 Freispiele im Tipico Casino nicht verpassen. Einfach anmelden, Aktion auswählen und kostenlos losspielen!
https://tipicocasino.one/
https://leeds-welcome.com
https://detroitapartment.net
https://214rentals.com
https://financenewsasia.com
https://1winru.ru/
На сайте https://t.me/s/m1xbet_ru ознакомьтесь с самыми актуальными, честными и свежими новостями, которые находятся в телеграме. Если вы любите азартные игры, тогда вам точно приглянется казино, в котором огромное количество слотов. При этом вы сможете выиграть джекпот. Все самые последние, актуальные новости из мира онлайн-казино находятся на этом портале. Также здесь, в первую очередь, выставляют промокоды, которые позволят существенно сэкономить и не тратить собственные деньги. В группе несколько десятков фото, различные записи.
Tipico Casino Einzahlen Geht Nicht: Was Tun?
Das Tipico Casino ist eine beliebte Plattform fГјr GlГјcksspiele und bietet den Spielern eine Vielzahl von Spielen und attraktiven Boni. Doch was passiert, wenn man versucht, Geld auf sein Konto einzuzahlen, aber es einfach nicht funktioniert?
Es gibt verschiedene mögliche Gründe dafür, dass die Einzahlung im Tipico Casino nicht durchgeführt werden kann. Einer der häufigsten Gründe ist, dass die Zahlungsmethode, die man ausgewählt hat, nicht unterstützt wird. Es ist wichtig sicherzustellen, dass die gewählte Zahlungsmethode von Tipico akzeptiert wird. Zu den gängigen Zahlungsmethoden im Tipico Casino gehören unter anderem Kreditkarten, Banküberweisungen und E-Wallets wie PayPal und Skrill.
Ein weiterer Grund, warum die Einzahlung nicht funktionieren könnte, ist ein technisches Problem bei der Abwicklung der Zahlung. In diesem Fall kann es hilfreich sein, den Kundendienst von Tipico zu kontaktieren, um Unterstützung zu erhalten und das Problem zu lösen.
Es ist auch möglich, dass es Einschränkungen für Einzahlungen auf Ihr Konto gibt, die von Ihrem Bankinstitut oder Ihrer Kreditkartenfirma festgelegt wurden. Es ist ratsam, sich bei Ihrem Finanzinstitut zu erkundigen, ob es Beschränkungen für Online-Glücksspieltransaktionen gibt und gegebenenfalls diese Beschränkungen aufheben zu lassen.
Wenn alle diese Schritte erfolglos sind und die Einzahlung immer noch nicht funktioniert, könnte es sein, dass Ihr Konto gesperrt oder eingeschränkt wurde. In einem solchen Fall ist es ratsam, sich direkt an den Kundendienst von Tipico zu wenden, um weitere Informationen zu erhalten und das Problem zu klären.
Insgesamt gibt es also verschiedene Gründe, warum die Einzahlung im Tipico Casino nicht funktionieren könnte. Indem man die genannten Schritte beachtet und gegebenenfalls den Kundendienst kontaktiert, sollte es jedoch möglich sein, das Problem zu lösen und wieder uneingeschränkt an den Spielen im Tipico Casino teilzunehmen.
https://tipicocasino.one/
XEvil 5.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha-2, ReCaptcha v.3, Hotmail, Google, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2captcha.com, anti-captcha (antigate), RuCaptcha, DeathByCaptcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
service centers
Zet Casino No Deposit
Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen fГјr die Spieler anbietet. Egal, ob Sie ein Fan von Slots, Tischspielen oder Live-Casino sind, bei Zet Casino werden Sie definitiv das richtige Spiel fГјr sich finden. Neben der groГџen Auswahl an Spielen bietet Zet Casino auch groГџzГјgige Bonusangebote fГјr seine Spieler. Einer der beliebtesten Bonusse, die das Casino bietet, ist der sogenannte “No Deposit Bonus”.
Der No Deposit Bonus von Zet Casino ist ein großartiges Angebot für neue Spieler, die das Casino ausprobieren möchten, ohne eine Einzahlung tätigen zu müssen. Mit diesem Bonus erhalten Spieler eine bestimmte Menge an Freispielen oder Bonusgeld, die sie nutzen können, um verschiedene Spiele im Casino zu spielen. Dadurch haben die Spieler die Möglichkeit, das Casino und seine verschiedenen Spiele kennenzulernen, ohne ihr eigenes Geld riskieren zu müssen.
Um den No Deposit Bonus von Zet Casino zu erhalten, müssen Spieler sich lediglich auf der Website des Casinos registrieren und ein Konto erstellen. Sobald das Konto erstellt wurde, erhalten die Spieler den Bonus automatisch gutgeschrieben. Es ist jedoch wichtig zu beachten, dass bestimmte Bedingungen und Anforderungen für den No Deposit Bonus gelten, die von Zet Casino festgelegt wurden. Spieler müssen diese Bedingungen erfüllen, um den Bonus nutzen zu können und mögliche Gewinne auszahlen zu können.
Insgesamt ist der No Deposit Bonus von Zet Casino eine groГџartige Gelegenheit fГјr Spieler, das Casino auszuprobieren und erste Gewinne zu erzielen, ohne eigenes Geld einzahlen zu mГјssen. Wenn Sie also auf der Suche nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis sind, sollten Sie Zet Casino definitiv eine Chance geben.
https://zetcasino.one/
Boomerang Casino Avis – Ein Гњberblick Гјber dieses aufregende Online-Casino
Boomerang Casino ist ein aufstrebendes Online-Casino, das Spielern eine Vielzahl von Unterhaltungsmöglichkeiten bietet. Mit einer breiten Palette von Spielen, großzügigen Boni und einem hervorragenden Kundenservice hat Boomerang Casino schnell an Beliebtheit gewonnen.
Das Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino und mehr. Mit hochwertiger Software von fГјhrenden Anbietern wie NetEnt, Microgaming und Play’n GO kГ¶nnen die Spieler ein reibungsloses und unterhaltsames Spielerlebnis genieГџen.
Ein weiterer großer Vorteil von Boomerang Casino sind die großzügigen Boni und Promotionen, die den Spielern regelmäßig angeboten werden. Neue Spieler können sich über einen Willkommensbonus freuen, der ihnen zusätzliches Geld zum Spielen bietet. Darüber hinaus gibt es regelmäßig Aktionen wie Freispiele, Einzahlungsboni und Turniere, die den Spielern die Chance bieten, noch mehr zu gewinnen.
Der Kundenservice von Boomerang Casino ist ebenfalls top. Das Team ist rund um die Uhr erreichbar und steht den Spielern bei Fragen oder Problemen zur VerfГјgung. Die Mitarbeiter sind freundlich, kompetent und bemГјht, den Spielern ein groГџartiges Spielerlebnis zu bieten.
Insgesamt ist Boomerang Casino eine ausgezeichnete Wahl fГјr alle, die nach einem unterhaltsamen und sicheren Online-Casino suchen. Mit einer groГџen Auswahl an Spielen, groГџzГјgigen Boni und einem erstklassigen Kundenservice gibt es viele GrГјnde, dieses Casino auszuprobieren. Besuchen Sie noch heute die Website von Boomerang Casino und erleben Sie die Magie selbst!
https://boomerangcasino.one/
сайт мега сб не работает – mega onion, mega sb не работает сайт
В современном мире, где диплом – это начало успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа переоценить попросту невозможно. Ведь диплом открывает двери перед людьми, желающими вступить в сообщество квалифицированных специалистов или учиться в университете.
Мы предлагаем быстро получить любой необходимый документ. Вы имеете возможность заказать диплом старого или нового образца, и это будет отличным решением для всех, кто не смог завершить обучение, потерял документ или желает исправить плохие оценки. дипломы выпускаются аккуратно, с особым вниманием к мельчайшим элементам. В итоге вы получите полностью оригинальный документ.
Преимущество такого подхода состоит не только в том, что вы максимально быстро получите диплом. Процесс организован комфортно, с нашей поддержкой. От выбора необходимого образца диплома до консультаций по заполнению личной информации и доставки в любое место России — все под абсолютным контролем качественных мастеров.
Всем, кто ищет максимально быстрый способ получить необходимый документ, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать долгого обучения и сразу перейти к достижению личных целей: к поступлению в университет или к началу удачной карьеры.
https://ufacat.mybb.ru/viewtopic.php?id=225
http://molbiol.ru/forums/index.php?showtopic=1088329
kraken darknet – kraken13, kraken13
kraken сайт – kraken com ссылка, ссылка КРАКЕН не работает
Please let me know if you’re looking for a article author for your weblog. You have some really great articles and I feel I would be a good asset. If you ever want to take some of the load off, I’d absolutely love to write some articles for your blog in exchange for a link back to mine. Please send me an email if interested. Kudos!
https://notes.io/whEYh
http://kvitka-ua.com/linzy-u-fary-dlya-vashogo-avtomobilya
http://images.google.gl/url?q=https://storgaard-gustafson-2.mdwrite.net/optimal-ne-osvitlennia-linzi-vid-lemarix-ua-dlia-vashogo-avto
Zet Casino: Ein seriöses Online-Casino
Das Glücksspiel im Internet gewinnt immer mehr an Beliebtheit, jedoch ist es wichtig, sich in einem sicheren und seriösen Online-Casino zu registrieren. Ein solches Casino ist Zet Casino, das eine Lizenz der Curacao eGaming besitzt und somit den strengen Richtlinien für Glücksspielanbieter entspricht.
Zet Casino bietet eine breite Auswahl an Spielen von renommierten Softwareanbietern wie NetEnt, Microgaming und Betsoft. Von Spielautomaten über Tischspiele bis hin zu Live-Casino-Spielen ist für jeden Geschmack etwas dabei. Die Spiele sind fair und werden regelmäßig auf ihre Zufälligkeit überprüft, um ein faires Spielerlebnis zu gewährleisten.
Ein weiterer Pluspunkt von Zet Casino ist der professionelle Kundenservice, der rund um die Uhr erreichbar ist. Egal, ob es um technische Probleme, Boni oder Auszahlungen geht, das Support-Team steht den Spielern kompetent und freundlich zur Seite.
Auch in Sachen Sicherheit und Datenschutz kann Zet Casino überzeugen. Die Webseite ist SSL-verschlüsselt, sodass persönliche Daten geschützt sind. Zudem bietet das Casino verschiedene sichere Zahlungsmethoden an, damit Ein- und Auszahlungen schnell und unkompliziert durchgeführt werden können.
Insgesamt kann man sagen, dass Zet Casino ein seriöser Anbieter ist, der den Spielern ein sicheres und unterhaltsames Spielerlebnis bietet. Wer auf der Suche nach einem zuverlässigen Online-Casino ist, sollte Zet Casino definitiv in Betracht ziehen.
https://zetcasino.one/
Приобрести диплом без лишних хлопот, через интернет.
Легальный способ купить диплом, без заморочек.
Купить диплом с гарантией качества, важная информация.
Почему выгодно купить диплом, все секреты.
Где купить диплом без проблем, с гарантией.
Как выбрать диплом для покупки, секреты выбора.
Дипломы на заказ по лучшим ценам, лучшие условия.
Покупка диплома: безопасность и конфиденциальность, наши преимущества.
Лучшие дипломы для покупки, только актуальная информация.
Как купить диплом онлайн, гарантированный результат.
Официальные документы для покупки, гарантированное качество.
Как купить диплом срочно, лучшие условия.
Купить диплом без обмана, важные детали.
Дипломы на всех условиях, лучшие предложения.
Как купить дипломы онлайн, подробности у нас.
Какой диплом выбрать для покупки, интересные варианты.
Официальная покупка диплома, лучшие условия.
Как купить диплом безопасно и быстро, подробности у нас.
купить диплом http://www.7arusak-diploms.com/ .
Boomerang Casino No Deposit Bonus Codes 2022: Was gibt es Neues?
Boomerang Casino ist bekannt für seine großzügigen Boni und Aktionen für Spieler. Im Jahr 2022 hat das beliebte Online-Casino eine Vielzahl von attraktiven Bonus-Codes ohne Einzahlung eingeführt, die es den Spielern ermöglichen, ihre Lieblingsspiele ohne Risiko zu genießen und dabei echtes Geld zu gewinnen.
Die no-deposit Bonus-Codes bei Boomerang Casino sind eine großartige Möglichkeit für neue Spieler, die Plattform kennenzulernen und erste Gewinne zu erzielen, ohne eigenes Geld einzahlen zu müssen. Mit diesen Codes können Spieler kostenlose Spielchips oder Freispiele auf ausgewählten Spielautomaten erhalten.
Um von den Bonus-Codes zu profitieren, mГјssen die Spieler einfach den entsprechenden Code bei der Registrierung oder auf der Einzahlungsseite eingeben. Das Bonusguthaben wird dann sofort auf das Spielerkonto gutgeschrieben und kann fГјr verschiedene Spiele im Casino verwendet werden.
Die Bonus-Codes von Boomerang Casino sind in der Regel zeitlich begrenzt und können sich regelmäßig ändern. Es lohnt sich also, regelmäßig auf der Website des Casinos vorbeizuschauen, um die aktuellsten Codes und Angebote nicht zu verpassen.
Zusätzlich zu den no-deposit Bonus-Codes bietet Boomerang Casino auch regelmäßige Einzahlungsboni, Treuepunkte und andere Aktionen, die es den Spielern ermöglichen, ihre Gewinne zu maximieren und das Spielerlebnis noch spannender zu gestalten.
Insgesamt bietet Boomerang Casino seinen Spielern eine Vielzahl von attraktiven Bonus-Codes und Aktionen, die ihnen dabei helfen, ihre Lieblingsspiele zu genieГџen und gleichzeitig echtes Geld zu gewinnen. Wer also auf der Suche nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis ist, sollte unbedingt die Bonus-Angebote von Boomerang Casino im Auge behalten.
https://boomerangcasino.one/
В нашем обществе, где диплом – это начало удачной карьеры в любой отрасли, многие пытаются найти максимально быстрый и простой путь получения качественного образования. Факт наличия документа об образовании сложно переоценить. Ведь диплом открывает двери перед всеми, кто хочет начать профессиональную деятельность или учиться в ВУЗе.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы сможете заказать диплом старого или нового образца, что становится выгодным решением для человека, который не смог завершить обучение, утратил документ или хочет исправить плохие оценки. Все дипломы выпускаются с особой тщательностью, вниманием ко всем деталям, чтобы в итоге получился документ, полностью соответствующий оригиналу.
Преимущество этого решения заключается не только в том, что можно оперативно получить диплом. Весь процесс организован удобно, с профессиональной поддержкой. Начиная от выбора нужного образца до грамотного заполнения персональных данных и доставки в любой регион России — все находится под полным контролем качественных мастеров.
Для тех, кто хочет найти максимально быстрый способ получения требуемого документа, наша услуга предлагает выгодное решение. Купить диплом – значит избежать длительного процесса обучения и не теряя времени переходить к достижению своих целей: к поступлению в ВУЗ или к началу успешной карьеры.
http://crimeadetka.forum.cool/viewtopic.php?id=1509
http://building.ixbb.ru/viewtopic.php?id=3594
investnews24.net
Hi there, all the time i used to check blog posts here early in the daylight, since i like to find out more and more.
http://kvitka-ua.com/linzy-u-fary-dlya-vashogo-avtomobilya
https://clients1.google.rw/url?q=https://www.coursera.org/user/0cebcb5c1b1bfd76b7b4e4eec75fd782
https://malik-sehested.thoughtlanes.net/linzi-u-fari-vibir-maibutn-ogo-dlia-vashogo-avtomobilia-na-lemarix-ua
На сайте https://my-tvset.ru/ изучите увлекательную, полезную информацию, которая касается того, как правильно выполнить ремонт, создать уют и комфортные условия. Так вы узнаете о том, как правильно выбрать бежевую плитку, а также затирку. Даны все необходимые рекомендации, важные советы, которые помогут решить ситуацию. Имеются важные рекомендации относительно обустройства квартиры: гостиной, ванной, комнаты. Вы узнаете о том, как правильно организовать системы отопления, подобрать светильники, люстры, столы.
Хронос гарантирует высокое качество медицинской техники, доступные цены и бесплатную доставку в любой регион РФ. Купить медтехнику вы можете, позвонив нам по телефону. С удовольствием поможем с выбором и ответим на все вопросы. https://agsvv.ru/ сайт, где есть возможность уже сейчас посмотреть условия доставки и оплаты товара. Также тут вы узнаете, какие лампы используются в аппаратах, которые изготавливает компания Хронос, а также какой срок гарантии. Свяжитесь с нами, и мы предоставим вам нужную дополнительную информацию.
как зайти на мега – что случилось с mega sb, mega sb
XEvil 6.0 automatically solve most kind of captchas,
Including such type of captchas: ReCaptcha v.2, ReCaptcha v.3, Hotmail, Google captcha, Solve Media, BitcoinFaucet, Steam, Amazon, Twitter, Microsoft, Twitch, Outlook, +12k
+ hCaptcha, ArkoseLabs FunCaptcha, ReCaptcha Enterprize supported in new XEvil 6.0!
1.) Fast, easy, precisionly
XEvil is the fastest captcha killer in the world. Its has no solving limits, no threads number limits
you can solve even 1.000.000.000 captchas per day and it will cost 0 (ZERO) USD! Just buy license for 59 USD and all!
2.) Several APIs support
XEvil supports more than 6 different, worldwide known API: 2Captcha, anti-captcha (antigate), RuCaptcha, death-by-captcha, etc.
just send your captcha via HTTP request, as you can send into any of that service – and XEvil will solve your captcha!
So, XEvil is compatible with hundreds of applications for SEO/SMM/password recovery/parsing/posting/clicking/cryptocurrency/etc.
3.) Useful support and manuals
After purchase, you got access to a private tech.support forum, Wiki, Skype/Telegram online support
Developers will train XEvil to your type of captcha for FREE and very fast – just send them examples
4.) How to get free trial use of XEvil full version?
– Try to search in Google “Home of XEvil”
– you will find IPs with opened port 80 of XEvil users (click on any IP to ensure)
– try to send your captcha via 2captcha API ino one of that IPs
– if you got BAD KEY error, just tru another IP
– enjoy! 🙂
– (its not work for hCaptcha!)
WARNING: Free XEvil DEMO does NOT support ReCaptcha, hCaptcha and most other types of captcha!
http://xrumersale.site/
find out here now atomic wallet
m3ga gl не работает – m3ga площадка, m3ga официальный
Компания на профессиональном уровне занимается лазерной гравировкой на жетонах, шильдах, ложках. Кроме того, создает клише, производит гравировку по кругу и на различных предметах. При необходимости специалист может приехать на объект, чтобы оказать услугу непосредственно на территории заказчика. На сайте https://grsuv.ru/ ознакомьтесь с полным перечнем услуг, которые вы сможете заказать в этой компании и по лучшей стоимости.
На сайте https://t.me/s/mpinup ознакомьтесь с новостями, которые посвящены популярному онлайн-заведению «PinUP». Удача улыбнется и вам, если примите участие в турнирах. Это возможность заработать на свою мечту. Теперь и вы сможете присоединиться к группе. На этом сайте всегда выкладывают самые первые новости, промокоды и все то, что поможет получить неплохие деньги. В этой группе огромное количество интересных записей, а также любопытных фото. Регулярно публикуются новые данные, актуальные новости, которые помогут больше узнать о казино.
В нашем обществе, где диплом становится началом успешной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения образования. Наличие официального документа переоценить попросту невозможно. Ведь именно диплом открывает дверь перед людьми, желающими начать профессиональную деятельность или продолжить обучение в высшем учебном заведении.
В данном контексте наша компания предлагает максимально быстро получить этот важный документ. Вы имеете возможность купить диплом нового или старого образца, что становится выгодным решением для человека, который не смог завершить образование или утратил документ. дипломы изготавливаются с особой тщательностью, вниманием ко всем нюансам, чтобы на выходе получился полностью оригинальный документ.
Плюсы такого подхода заключаются не только в том, что можно быстро получить свой диплом. Процесс организовывается комфортно, с нашей поддержкой. От выбора нужного образца до правильного заполнения личных данных и доставки в любой регион России — все будет находиться под полным контролем опытных специалистов.
Всем, кто ищет максимально быстрый способ получить необходимый документ, наша компания предлагает отличное решение. Приобрести диплом – это значит избежать продолжительного процесса обучения и сразу переходить к достижению собственных целей, будь то поступление в университет или старт карьеры.
http://earnmoney.7bb.ru/viewtopic.php?id=6586
http://fwh.mybb.ru/viewtopic.php?id=403
Tipico Aktion 200 Casino – Jetzt von tollen Bonusaktionen profitieren!
Das Tipico Casino bietet seinen Kunden eine Vielzahl an spannenden Spielmöglichkeiten und attraktiven Bonusaktionen. Eine besonders lohnende Aktion für alle Casino-Fans ist die Tipico Aktion 200 Casino. Bei dieser Aktion haben Spieler die Möglichkeit, sich bis zu 200€ Bonusguthaben zu sichern.
Um von dieser Aktion zu profitieren, müssen Spieler lediglich eine Einzahlung von mindestens 10€ tätigen. Anschließend erhalten sie einen 100% Einzahlungsbonus, der bis zu 200€ betragen kann. Das bedeutet, dass Spieler ihr eingezahltes Guthaben verdoppeln können und somit noch mehr Spaß beim Spielen im Casino haben.
Die Bonusbedingungen für die Tipico Aktion 200 Casino sind fair gestaltet. Das Bonusguthaben muss insgesamt 35-mal umgesetzt werden, bevor es ausgezöst werden kann. Spieler haben dafür insgesamt 30 Tage Zeit, was mehr als ausreichend ist, um die Umsatzbedingungen zu erfüllen.
Neben der Tipico Aktion 200 Casino bietet das Online-Casino noch viele weitere lukrative Bonusaktionen und Promotionen. So gibt es regelmäßig Freispielaktionen, Verlosungen und Turniere, bei denen Spieler attraktive Preise wie Freispiele, Bonusguthaben oder sogar Reisen gewinnen können.
Das Tipico Casino Гјberzeugt zudem mit einer groГџen Auswahl an hochwertigen Casino-Spielen, darunter Slots, Roulette, Blackjack und Live-Casino-Spiele. Die Spiele stammen von renommierten Herstellern wie NetEnt, Microgaming und Evolution Gaming und garantieren ein erstklassiges Spielerlebnis.
Also worauf warten Sie noch? Registrieren Sie sich noch heute im Tipico Casino und sichern Sie sich den 200€ Einzahlungsbonus. Viel Spaß und viel Erfolg beim Spielen!
https://tipicocasino.one/
blacksprut solaris – blacksprut зеркало официальный, blacksprut ссылка tor
Zet Casino Anmeldung: Der SchlГјssel zum ultimativen Online-Spielerlebnis
Das Zet Casino ist eine der beliebtesten Online-Glücksspielplattformen, die Spielern auf der ganzen Welt eine spannende und unterhaltsame Erfahrung bietet. Mit einer Vielzahl von Spielen, großzügigen Boni und einer benutzerfreundlichen Oberfläche ist das Zet Casino die perfekte Wahl für alle, die auf der Suche nach einem hochwertigen Spielerlebnis sind.
Um das Zet Casino voll nutzen zu können, müssen Sie sich zunächst registrieren. Die Anmeldung ist einfach und unkompliziert und kann in nur wenigen Minuten abgeschlossen werden. Alles, was Sie tun müssen, ist, auf die Website des Zet Casinos zu gehen und den Anweisungen zur Anmeldung zu folgen.
Nachdem Sie sich angemeldet haben, können Sie eine Vielzahl von Spielen genießen, darunter Spielautomaten, Tischspiele, Live-Dealer-Spiele und vieles mehr. Das Zet Casino arbeitet mit einer Reihe renommierter Spieleentwickler zusammen, um sicherzustellen, dass seine Spieler Zugang zu den besten und neuesten Spielen haben.
Zusätzlich zu den Spielen bietet das Zet Casino auch großzügige Boni und Aktionen für seine Spieler an. Neue Spieler können von Willkommensboni profitieren, während treue Spieler regelmäßig mit Freispielen, Einzahlungsboni und anderen Belohnungen belohnt werden.
Das Zet Casino legt auch großen Wert auf Sicherheit und Fairness und bietet seinen Spielern eine sichere Spielumgebung. Die Plattform verwendet die neueste Verschlüsselungstechnologie, um sicherzustellen, dass alle Transaktionen sicher und geschützt sind, und alle Spiele werden regelmäßig von unabhängigen Prüfstellen überprüft, um sicherzustellen, dass sie fair und zufällig sind.
Insgesamt ist das Zet Casino eine ausgezeichnete Wahl für alle, die auf der Suche nach einem hochwertigen Online-Spielerlebnis sind. Mit einer breiten Palette von Spielen, großzügigen Boni und einer sicheren Spielumgebung ist das Zet Casino eine Plattform, die Spieler immer wieder zurückkehren lässt. Registrieren Sie sich noch heute und entdecken Sie die aufregende Welt des Zet Casinos!
https://zetcasino.one/
Сегодня, когда диплом является началом отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Наличие официального документа переоценить просто невозможно. Ведь диплом открывает дверь перед каждым человеком, который желает вступить в профессиональное сообщество или учиться в высшем учебном заведении.
Предлагаем очень быстро получить этот важный документ. Вы сможете заказать диплом старого или нового образца, и это будет отличным решением для человека, который не смог завершить обучение, потерял документ или желает исправить плохие оценки. диплом изготавливается с особой тщательностью, вниманием ко всем деталям, чтобы в результате получился продукт, 100% соответствующий оригиналу.
Плюсы этого подхода заключаются не только в том, что вы быстро получите свой диплом. Процесс организовывается удобно и легко, с нашей поддержкой. От выбора нужного образца до грамотного заполнения личной информации и доставки в любое место страны — все под абсолютным контролем опытных мастеров.
В результате, для тех, кто пытается найти быстрый способ получения требуемого документа, наша компания предлагает выгодное решение. Купить диплом – значит избежать продолжительного обучения и не теряя времени переходить к достижению собственных целей, будь то поступление в университет или старт карьеры.
https://mens-look.ru/womens-section.html
https://zamkiexpress.ru/
В современном мире, где диплом является началом отличной карьеры в любом направлении, многие ищут максимально простой путь получения образования. Факт наличия официального документа об образовании трудно переоценить. Ведь именно диплом открывает двери перед людьми, желающими вступить в сообщество профессионалов или продолжить обучение в любом институте.
В данном контексте наша компания предлагает быстро получить этот необходимый документ. Вы можете приобрести диплом старого или нового образца, что будет отличным решением для всех, кто не смог завершить образование, утратил документ или желает исправить свои оценки. Все дипломы изготавливаются с особой аккуратностью, вниманием к мельчайшим деталям, чтобы в результате получился полностью оригинальный документ.
Плюсы данного подхода состоят не только в том, что можно быстро получить диплом. Весь процесс организован комфортно, с профессиональной поддержкой. Начав от выбора нужного образца до точного заполнения персональных данных и доставки по России — все будет находиться под абсолютным контролем опытных мастеров.
Всем, кто ищет максимально быстрый способ получить требуемый документ, наша компания предлагает отличное решение. Приобрести диплом – это значит избежать долгого процесса обучения и сразу перейти к личным целям: к поступлению в ВУЗ или к началу успешной карьеры.
http://borderforum.ru/viewtopic.php?f=26&t=8521
http://molbiol.ru/forums/index.php?showtopic=1088312
world-news-365.com
https://tzona.org
Проведите увлекательный день, исследуя малые средневековые города Калининградской области с нашими индивидуальными экскурсиями на машине, которые откроют для вас атмосферу старинных улиц, замков и крепостей, погружая вас в богатое историческое наследие региона. https://mykaliningradgid.ru/
Das Tipico Casino gehГ¶rt zu den beliebtesten Online-Casinos in Deutschland. Hier kГ¶nnen Spieler eine Vielzahl von Casino-Spielen wie Slots, Roulette, Blackjack und Poker genieГџen. Einer der wichtigsten Faktoren fГјr viele Spieler ist der Mindesteinsatz, den sie tГ¤tigen kГ¶nnen. In diesem Artikel werden wir uns genauer mit dem Thema “Tipico Casino niedrigster Einsatz” befassen.
Der niedrigste Einsatz im Tipico Casino hängt von dem jeweiligen Spiel ab, das der Spieler wählt. In den meisten Slots können Spieler bereits mit einem Einsatz von wenigen Cent spielen. Bei Tischspielen wie Roulette oder Blackjack liegt der Mindesteinsatz oft etwas höher, aber dennoch im Bereich von wenigen Euro. Dies ermöglicht es Spielern mit verschiedenen Budgets, im Tipico Casino zu spielen und Spaß zu haben.
Ein niedriger Einsatz ist besonders für Anfänger oder Spieler mit kleinem Budget attraktiv. Sie können das Casino ausprobieren und verschiedene Spiele testen, ohne dabei ein großes finanzielles Risiko einzugehen. Zudem können sie mit einem niedrigen Einsatz auch längere Spielzeiten genießen und mehr Unterhaltung erhalten.
Es ist jedoch wichtig zu beachten, dass ein niedriger Einsatz auch bedeutet, dass die potenziellen Gewinne geringer ausfallen. Spieler sollten sich bewusst sein, dass sie möglicherweise keine hohen Gewinne erzielen, wenn sie nur mit einem niedrigen Einsatz spielen. Daher ist es wichtig, das eigene Budget im Auge zu behalten und verantwortungsbewusst zu spielen.
Insgesamt bietet das Tipico Casino eine gute Auswahl an Spielen mit niedrigen Einsätzen, die es Spielern ermöglichen, auch mit kleinem Budget Spaß zu haben. Es ist wichtig, verantwortungsbewusst zu spielen und sich über die möglichen Risiken im Klaren zu sein. Wir empfehlen allen Spielern, sich vorab über die Regeln und Bedingungen der Spiele zu informieren und sich an ihr Budget zu halten. Viel Spaß beim Spielen im Tipico Casino!
https://tipicocasino.one/
Хотите купить в Москве с установкой кондиционер? РусКондиционер – это то, что вам необходимо! Интернет магазин предоставляет огромный выбор надежного климатического оборудования от популярных производителей. Ищете купить кондиционер в Москве недорого? Ruscondicioner.ru – сайт, где имеется исключительно продукция, прошедшая сертификацию. Здесь вы можете детальнее ознакомиться с условиями оплаты и доставки. У нас можно не только купить кондиционер, но и заказать его установку. Наши специалисты имеют солидный опыт в данной области, работа будет выполнена профессионально.
В современном мире, где диплом – это начало отличной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения качественного образования. Наличие официального документа переоценить просто невозможно. Ведь именно он открывает двери перед людьми, стремящимися вступить в профессиональное сообщество или продолжить обучение в университете.
Наша компания предлагает очень быстро получить любой необходимый документ. Вы имеете возможность заказать диплом, и это будет отличным решением для всех, кто не смог закончить обучение, потерял документ или хочет исправить свои оценки. Все дипломы производятся аккуратно, с максимальным вниманием к мельчайшим элементам. В результате вы сможете получить 100% оригинальный документ.
Преимущество такого подхода состоит не только в том, что можно оперативно получить диплом. Процесс организовывается удобно, с нашей поддержкой. От выбора подходящего образца до консультации по заполнению личной информации и доставки по стране — все под полным контролем опытных специалистов.
Таким образом, для всех, кто пытается найти быстрый способ получения требуемого документа, наша услуга предлагает выгодное решение. Заказать диплом – это значит избежать долгого обучения и сразу перейти к достижению личных целей, будь то поступление в ВУЗ или старт успешной карьеры.
https://seo-pes.ru/astrologija/193-k-kakim-znakam-zodiaka-pridet-uspeh-v-novom-2020-godu.html
This is a brilliant piece of writing. You’ve nailed it perfectly!
https://x.com/impexautoglass
Хотите приобрести по недорогой стоимости из нержавеющей стали клапаны и арматуру? Мы вам в этом с радостью готовы помочь. Главные достоинства нашей продукции: долгий срок эксплуатации и большая надежность. Ищете арматура из нержавейки для пищевого производства? Inoxpa.ru – сайт, где вы узнаете, где именно применяется арматура из нержавеющей стали. Также тут вы можете уже сейчас ознакомиться с качественной продукцией компании INOXPA. У вас появились какие-либо вопросы? Обратитесь к нам, мы с радостью на них ответим. Звоните прямо сейчас!
Zet Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Spielen und Bonusangeboten für ihre Kunden anbietet. Eines der begehrtesten Boni sind die Zet Casino Freispiele, die es den Spielern ermöglichen, kostenlos an ausgewählten Spielautomaten zu spielen und dabei echtes Geld zu gewinnen.
Um die Zet Casino Freispiele einzulösen, müssen die Spieler zunächst ein Konto auf der Plattform erstellen und eine Einzahlung tätigen. Sobald die Einzahlung abgeschlossen ist, können die Spieler den Bonus aktivieren und die Freispiele nutzen. Es ist wichtig zu beachten, dass die Freispiele meist innerhalb eines bestimmten Zeitraums genutzt werden müssen, bevor sie verfallen.
Die Zet Casino Freispiele sind eine großartige Möglichkeit für die Spieler, neue Spielautomaten auszuprobieren und ihr Glück zu versuchen, ohne dabei ihr eigenes Geld zu riskieren. Es gibt verschiedene Arten von Freispielen, darunter Freispiele ohne Einzahlung, die den Spielern einen Vorgeschmack darauf geben, was sie erwartet, und Freispiele als Teil eines Willkommensbonus für neue Spieler.
Die Gewinne, die die Spieler mit den Zet Casino Freispielen erzielen, können in der Regel ausgezahlt werden, nachdem die Umsatzbedingungen erfüllt wurden. Diese Bedingungen legen fest, wie oft der Bonusbetrag umgesetzt werden muss, bevor eine Auszahlung möglich ist. Es ist ratsam, die Bonusbedingungen sorgfältig zu lesen, um Missverständnisse zu vermeiden.
Insgesamt sind die Zet Casino Freispiele eine attraktive Möglichkeit für die Spieler, ihr Spielerlebnis zu verbessern und zusätzliche Gewinnchancen zu erhalten. Es lohnt sich, regelmäßig auf der Website nach neuen Bonusangeboten zu suchen und die Freispiele zu nutzen, um das Beste aus dem Zet Casino herauszuholen.
https://zetcasino.one/
Tipico Live Casino Verboten
Das Tipico Live Casino Angebot gehört zu den beliebtesten Optionen für Spieler, die gerne die Atmosphäre eines echten Casinos in ihren eigenen vier Wänden genießen möchten. Jedoch gab es kürzlich eine unerwartete Entwicklung: Das Tipico Live Casino wurde verboten.
Genauere Details über die Gründe für dieses Verbot sind bisher nicht bekannt, jedoch wird spekuliert, dass es möglicherweise mit regulatorischen Vorschriften oder anderen rechtlichen Bedenken zu tun haben könnte. Da Tipico eine der beliebtesten Wettanbieter in Deutschland ist, hat diese Entscheidung viele Fans enttäuscht.
Für diejenigen, die gerne im Tipico Live Casino gespielt haben, bedeutet dies, dass sie sich nach alternativen Online-Casinos umsehen müssen, um ihr Lieblingsspiel weiterhin zu genießen. Es gibt viele andere Online-Casinos, die ähnliche Live Casino Angebote haben, aber es könnte schwierig sein, eines zu finden, das die gleiche Qualität und Vielfalt wie das Tipico Live Casino bietet.
Es bleibt abzuwarten, ob und wann das Verbot des Tipico Live Casinos aufgehoben wird, aber in der Zwischenzeit müssen die Fans des Live Casinos sich nach anderen Möglichkeiten umsehen. Es ist eine enttäuschende Entwicklung für alle, die das Tipico Live Casino genossen haben, aber hoffentlich finden sie bald eine andere Möglichkeit, ihre Leidenschaft für das Glücksspiel auszuleben.
https://tipicocasino.one/
Приветствую привет! Хочу разделить своими эмоциями об онлайн игровом клубе гет х официальный сайт вход. Это место, где все пользователь может отыскать свою фортуна и порадоваться захватывающим игровым геймплеем. Ассортимент игр изумляет: от классических слотов до новейших видеоигр. Большие бонусы и постоянные акции делают игру даже еще более заманчивой. Удобный интерфейс и постоянная поддержка гарантируют удобную игру в любое время. get-x – это не просто игровое заведение, это твой возможность на крупные достижения и яркие эмоции!
На сайте https://play.google.com/store/apps/details?id=com.amazon.mShop.android.shoppi вы сможете сыграть в увлекательную, интересную игру – Bamboo Bastion, которая радует своей привлекательной графикой, интересным сюжетом, который завораживает с самых первых минут. Такая игра считается именно тем, что вы так давно искали. Суть заключается в том, чтобы вы быстро среагировали на ситуацию и приняли решение. Скачайте ее прямо сейчас на свое устройство. Играйте в нее тогда, когда вам удобно, даже находясь в путешествии или длительной поездке.
ремонт бытовой технки
В наше время, когда диплом становится началом отличной карьеры в любой отрасли, многие пытаются найти максимально быстрый и простой путь получения образования. Факт наличия официального документа об образовании трудно переоценить. Ведь именно он открывает двери перед любым человеком, который стремится начать профессиональную деятельность или продолжить обучение в высшем учебном заведении.
В данном контексте мы предлагаем оперативно получить любой необходимый документ. Вы сможете заказать диплом, что становится выгодным решением для всех, кто не смог закончить обучение или утратил документ. Каждый диплом изготавливается с особой аккуратностью, вниманием к мельчайшим деталям. В результате вы получите продукт, полностью соответствующий оригиналу.
Преимущества такого решения состоят не только в том, что вы сможете максимально быстро получить диплом. Весь процесс организовывается комфортно, с нашей поддержкой. Начав от выбора подходящего образца до консультации по заполнению личных данных и доставки в любой регион России — все под абсолютным контролем квалифицированных специалистов.
Для тех, кто хочет найти быстрый способ получения требуемого документа, наша компания предлагает выгодное решение. Купить диплом – значит избежать долгого обучения и сразу перейти к важным целям: к поступлению в университет или к началу успешной карьеры.
https://www.zhuk.net/page.php?id=259
Согласование перепланировки — это ключевой этап, который необходим для законного изменения конфигурации помещений. Компания “КитСтрой” предлагает услуги по согласованию перепланировок в Москве. Мы возьмем на себя все этапы: от подготовки проектной документации до получения разрешений. Наши специалисты имеют опыт работы с различными инстанциями и знают все тонкости процесса. Мы гарантируем, что все документы будут оформлены правильно, что позволит избежать проблем в будущем.
Согласование перепланировки с “КитСтрой” — это быстрый и эффективный процесс. Мы ценим ваше время и стремимся сделать все возможное для комфортного прохождения всех этапов согласования. Обратитесь к нам, и мы поможем вам узаконить перепланировку без лишних хлопот и задержек.
В современном мире, где диплом – это начало успешной карьеры в любом направлении, многие ищут максимально простой путь получения качественного образования. Важность наличия документа об образовании трудно переоценить. Ведь именно он открывает дверь перед всеми, кто хочет начать трудовую деятельность или учиться в высшем учебном заведении.
Наша компания предлагает быстро получить этот необходимый документ. Вы сможете приобрести диплом, и это является отличным решением для человека, который не смог закончить обучение или потерял документ. дипломы производятся аккуратно, с особым вниманием ко всем элементам. В итоге вы сможете получить 100% оригинальный документ.
Преимущество такого решения состоит не только в том, что вы максимально быстро получите диплом. Процесс организовывается просто и легко, с профессиональной поддержкой. Начиная от выбора требуемого образца диплома до точного заполнения личных данных и доставки по России — все находится под абсолютным контролем опытных специалистов.
Всем, кто ищет максимально быстрый способ получить необходимый документ, наша компания готова предложить выгодное решение. Купить диплом – значит избежать долгого обучения и сразу перейти к своим целям, будь то поступление в ВУЗ или начало успешной карьеры.
http://www.livecenter.ru/index.php?showtopic=737
http://fora.forumbb.ru/viewtopic.php?id=15757
Всем привет всех! Хочу поделиться своими отзывами об онлайн казино Игровые автоматы на деньги. Это место, где каждый игрок может обнаружить свою везение и порадоваться захватывающим игровым игрой. Разнообразие игровых процессов впечатляет: от классических слотов до новейших видеоигр. Большие бонусы и частые акции делают игру ещё более заманчивой. Удобный интерфейс и постоянная поддержка обеспечивают приятную игру в любое время. Вулкан Россия – это не просто игровое заведение, это твой шанс на громадные выигрыши и незабываемые ощущения!
ГК «Норфост» с 2006 года занимается строительством домов, которые полностью соответствуют самым высоким требованиям и предпочтениям клиентов. Для того чтобы быстрее определиться с выбором, изучите на сайте https://gknorfost.ru/ каталог последних проектов с ценами, планировками. Представлены как одноэтажные, так и двухэтажные дома.
Boomerang Casino – das neue Online-Casino-Erlebnis
Das Boomerang Casino ist eine aufregende neue Online-Spielothek, die Spielern eine Vielzahl von Spielen und Unterhaltungsmöglichkeiten bietet. Mit einer benutzerfreundlichen Oberfläche und einem umfangreichen Spieleportfolio ist das Boomerang Casino die perfekte Wahl für alle, die auf der Suche nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis sind.
Das Boomerang Casino bietet eine breite Palette von beliebten Casino-Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und vieles mehr. Mit Spielen von fГјhrenden Anbietern wie NetEnt, Microgaming, Play’n GO und Evolution Gaming kГ¶nnen Spieler sicher sein, eine erstklassige Spielerfahrung zu genieГџen.
Ein weiterer Höhepunkt des Boomerang Casinos sind die großzügigen Bonusangebote und Aktionen, die regelmäßig veranstaltet werden. Neue Spieler können von großzügigen Willkommensboni profitieren, während treue Spieler durch ein lukratives Treueprogramm belohnt werden. Mit regelmäßigen Sonderaktionen, Turnieren und Verlosungen gibt es immer spannende Möglichkeiten, zusätzliche Belohnungen zu gewinnen.
Das Boomerang Casino legt großen Wert auf die Sicherheit und den Schutz seiner Spieler. Mit einer sicheren und zuverlässigen Plattform können Spieler sicher sein, dass ihre persönlichen Daten und finanziellen Transaktionen immer geschützt sind. Das Casino verfügt über eine Lizenz von einer angesehenen Glücksspielbehörde und garantiert faire Spiele durch regelmäßige Überprüfungen und Tests.
Insgesamt ist das Boomerang Casino eine ausgezeichnete Wahl für alle, die ein erstklassiges Online-Casino-Erlebnis suchen. Mit einer großen Auswahl an Spielen, großzügigen Bonusangeboten und einem engagierten Kundensupport ist das Boomerang Casino definitiv einen Besuch wert. Besuchen Sie noch heute das Boomerang Casino und entdecken Sie selbst, warum es zu den besten Online-Casinos gehört. Viel Spaß und viel Glück!
https://boomerangcasino.one/
На сайте https://gderaznica.ru/ почитайте интересную, увлекательную и любопытную информацию, которая касается таких важных тем, как: общество, экономика, медицина, технологии и многое другое. Все статьи написаны высококлассными, опытными авторами, которые хорошо разбираются в перечисленных темах. Рассматриваются и такие вопросы, как преимущества автоломбардов, различия цветов самых разных видов. Все статьи невероятно интересные, а потому читать захочется их и вам. Регулярно добавляются новые полезные материалы.
Если вы стремитесь повысить свою квалификацию или начать карьеру в новой сфере, наш сервис предлагает идеальные решения. Вы можете купить диплом об окончании техникума, который поможет вам начать карьеру в технической или специализированной области. Также мы предлагаем возможность купить диплом о переподготовке, что является отличным выбором для тех, кто хочет изменить свою профессиональную траекторию или углубить существующие знания. Наши дипломы откроют перед вами новые возможности и помогут достичь профессиональных высот.
В нашем обществе, где диплом становится началом отличной карьеры в любой сфере, многие пытаются найти максимально простой путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь именно диплом открывает двери перед любым человеком, который собирается вступить в сообщество квалифицированных специалистов или учиться в любом институте.
В данном контексте наша компания предлагает быстро получить любой необходимый документ. Вы имеете возможность купить диплом старого или нового образца, и это становится выгодным решением для всех, кто не смог завершить образование или утратил документ. дипломы производятся с особой аккуратностью, вниманием ко всем элементам. В результате вы сможете получить продукт, полностью соответствующий оригиналу.
Преимущество этого решения состоит не только в том, что вы быстро получите диплом. Процесс организовывается удобно, с нашей поддержкой. Начав от выбора подходящего образца диплома до консультаций по заполнению персональной информации и доставки по стране — все под полным контролем наших специалистов.
Всем, кто хочет найти максимально быстрый способ получить необходимый документ, наша компания может предложить отличное решение. Купить диплом – значит избежать продолжительного процесса обучения и не теряя времени переходить к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://mayak36.ru/kataklizmy/glava-administracii-energodara-zaiavil-o-mirnoi-obstanovke-na-zaes.html
Чугунные гири на https://girya-sportivnaya.ru/ – это лучшие инструменты, используемые в тренировочных целях для улучшения силы и выносливости. Помогают повышению качества жизни. Имеют удобную рукоять, дающую возможность выполнять тяги, свинги, толчки, скручивания и другие упражнения в гиревом спорте.
В выпуске долговечных снарядов применяется высший класс чугуна.
Широкий каталог изделий позволяет купить утяжелители для качественной программы тренировок.
Отечественный завод реализует гири для спорта по приятным ценам.
Das Tipico Casino Black Jack ist eine beliebte Variante des klassischen Kartenspiels in diesem renommierten Online-Casino. Black Jack, auch bekannt als 21, ist ein Spiel, bei dem die Spieler gegen den Dealer antreten und versuchen, so nah wie möglich an die Zahl 21 heranzukommen, ohne sie zu überschreiten.
Im Tipico Casino gibt es verschiedene Black Jack Tische mit unterschiedlichen Einsatzlimits, so dass sowohl Anfänger als auch erfahrene Spieler auf ihre Kosten kommen. Die grafische Gestaltung und die Benutzeroberfläche im Tipico Casino sind benutzerfreundlich und ermöglichen es den Spielern, sich schnell zurechtzufinden und das Spiel zu genießen.
Die Regeln des Black Jack Spiels im Tipico Casino entsprechen den klassischen Regeln des Spiels. Die Spieler haben die Möglichkeit, ihre Karten zu ziehen, zu passen, zu verdoppeln oder zu splitten, je nach ihren Karten und der Karte des Dealers. Es gibt auch die Möglichkeit, Versicherung zu kaufen, wenn der Dealer ein Ass als erste Karte hat.
Das Tipico Casino Black Jack bietet auch die Möglichkeit, im Live Casino zu spielen, was den Spielern ein authentisches Casino-Erlebnis bietet. Hier können die Spieler mit echten Dealern interagieren und das Spiel in Echtzeit genießen.
Insgesamt ist das Tipico Casino Black Jack eine unterhaltsame und spannende Variante des beliebten Kartenspiels, die sowohl Anfängern als auch erfahrenen Spielern gefallen wird. Mit seinen verschiedenen Tischen und Einsatzlimits sowie der Möglichkeit, im Live Casino zu spielen, ist das Tipico Casino Black Jack definitiv einen Besuch wert.
https://tipicocasino.one/
В нашем мире, где диплом является началом отличной карьеры в любом направлении, многие ищут максимально простой путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь именно он открывает дверь перед людьми, стремящимися начать трудовую деятельность или продолжить обучение в высшем учебном заведении.
Мы предлагаем очень быстро получить любой необходимый документ. Вы сможете приобрести диплом, и это становится выгодным решением для всех, кто не смог завершить образование, утратил документ или желает исправить плохие оценки. диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим элементам. В итоге вы получите 100% оригинальный документ.
Плюсы данного решения заключаются не только в том, что можно быстро получить свой диплом. Весь процесс организовывается просто и легко, с профессиональной поддержкой. Начав от выбора подходящего образца до консультации по заполнению персональных данных и доставки по стране — все под абсолютным контролем квалифицированных мастеров.
Таким образом, для всех, кто хочет найти оперативный способ получить необходимый документ, наша компания предлагает отличное решение. Приобрести диплом – значит избежать долгого обучения и не теряя времени перейти к достижению собственных целей, будь то поступление в университет или начало профессиональной карьеры.
http://bushinkan.mybb.ru/viewtopic.php?id=286
В современном мире, где диплом становится началом удачной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения образования. Факт наличия официального документа переоценить попросту невозможно. Ведь диплом открывает двери перед людьми, стремящимися начать профессиональную деятельность или учиться в университете.
В данном контексте мы предлагаем очень быстро получить этот важный документ. Вы сможете приобрести диплом старого или нового образца, и это будет отличным решением для всех, кто не смог закончить обучение или потерял документ. Все дипломы выпускаются с особой аккуратностью, вниманием к мельчайшим элементам. В итоге вы получите продукт, 100% соответствующий оригиналу.
Преимущество данного решения состоит не только в том, что можно максимально быстро получить свой диплом. Весь процесс организовывается комфортно, с нашей поддержкой. От выбора подходящего образца документа до точного заполнения персональных данных и доставки по России — все будет находиться под абсолютным контролем качественных специалистов.
Всем, кто ищет оперативный способ получить необходимый документ, наша услуга предлагает отличное решение. Приобрести диплом – это значит избежать продолжительного процесса обучения и сразу переходить к своим целям, будь то поступление в ВУЗ или старт карьеры.
http://cookfoods.ru/deserty/page,1,90,241-pirozhnoe-bez-vypechki-vishenki.html
Зайдите на сайт https://generalsfaq.ru/ который создан для поклонников компьютерной стратегии Генералы. Вы сможете почитать FAQ и гайды по игре, найти карты Zero Hour, а также прочие военные стратегии. Generals это лучшая RTS стратегия для компьютера – присоединяйтесь к нашему сообществу!
Hi everybody, here every person is sharing these kinds of know-how, thus it’s pleasant to read this website, and I used to go to see this blog daily.
http://www.diplomans-rossian.ru
В нашем обществе, где диплом становится началом отличной карьеры в любом направлении, многие пытаются найти максимально простой путь получения качественного образования. Необходимость наличия официального документа об образовании переоценить просто невозможно. Ведь диплом открывает двери перед каждым человеком, желающим вступить в сообщество профессионалов или учиться в любом ВУЗе.
Предлагаем очень быстро получить этот важный документ. Вы имеете возможность приобрести диплом, и это является отличным решением для человека, который не смог закончить обучение, утратил документ или хочет исправить свои оценки. диплом изготавливается с особой аккуратностью, вниманием к мельчайшим нюансам, чтобы на выходе получился полностью оригинальный документ.
Преимущества данного решения заключаются не только в том, что можно оперативно получить диплом. Процесс организован комфортно, с нашей поддержкой. От выбора нужного образца до грамотного заполнения персональной информации и доставки по стране — все находится под абсолютным контролем опытных мастеров.
Для тех, кто хочет найти быстрый способ получения необходимого документа, наша компания предлагает выгодное решение. Заказать диплом – значит избежать длительного обучения и не теряя времени переходить к важным целям, будь то поступление в ВУЗ или старт карьеры.
http://fabnews.ru/forum/showthread.php?p=73154
http://auto.boltun.su/viewtopic.php?id=1444
construction-rent.com
https://jaycitynews.com
Es hat sich herumgesprochen, dass das Tipico Casino in letzter Zeit öfter einmal hängt. Viele Spieler haben bereits von Problemen mit der Stabilität der Plattform berichtet und beschweren sich über Verzögerungen beim Laden der Spiele oder gar komplette Abstürze.
Das Tipico Casino gilt eigentlich als einer der führenden Anbieter von Online Casinospielen in Deutschland, daher ist es umso enttäuschender zu sehen, dass die technischen Probleme hier so häufig auftreten. Spieler, die auf der Suche nach reibungslosem und unterhaltsamem Spielvergnügen sind, werden natürlich durch solche Probleme abgeschreckt.
Die GrГјnde fГјr die Probleme im Tipico Casino sind nicht ganz klar, aber es scheint, dass die Plattform einfach nicht mit der steigenden Anzahl von Spielern und den immer komplexer werdenden Spielen mithalten kann. Es gibt Vermutungen, dass die Server des Casinos Гјberlastet sind oder dass die Software veraltet ist.
Für Spieler ist es besonders ärgerlich, wenn sie gerade in einem Spiel sind und dann plötzlich alles hängt. Das kann nicht nur frustrierend sein, sondern auch zu Verlusten führen, wenn man zum Beispiel bei einem Slotspiel gerade kurz vor einem großen Gewinn steht.
Das Tipico Casino sollte sich dringend um die technischen Probleme kümmern und sicherstellen, dass die Plattform zuverlässig und stabil läuft. Ansonsten könnten sie viele Spieler an die Konkurrenz verlieren, die mit ihren Casinos keine derartigen Probleme haben.
Es bleibt zu hoffen, dass das Tipico Casino in naher Zukunft seine technischen Probleme lösen kann, damit die Spieler wieder unbeschwert spielen können. Bis dahin ist es empfehlenswert, sich vielleicht nach anderen Online Casinos umzusehen, die keine derartigen Schwierigkeiten haben.
https://tipicocasino.one/
Хотите купить в Москве с установкой кондиционер? РусКондиционер – то, что вам нужно! Интернет магазин предлагает большой ассортимент проверенного климатического оборудования от известных производителей. Ищете купить кондиционер для дома? Ruscondicioner.ru – сайт, где имеется исключительно продукция, прошедшая сертификацию. Здесь вы подробнее ознакомитесь с условиями доставки и оплаты. У нас можно не только купить кондиционер, но и заказать его установку. Наши специалисты имеют солидный опыт в данной области, работа будет выполнена профессионально.
Сайт, где можно выбрать чешские раковины любого размера.
На сегодняшний день, когда диплом – это начало удачной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Наличие документа об образовании сложно переоценить. Ведь диплом открывает двери перед любым человеком, желающим начать трудовую деятельность или учиться в высшем учебном заведении.
Предлагаем максимально быстро получить любой необходимый документ. Вы имеете возможность приобрести диплом, и это является выгодным решением для всех, кто не смог завершить обучение, потерял документ или хочет исправить свои оценки. диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим деталям. В результате вы сможете получить продукт, полностью соответствующий оригиналу.
Преимущество этого подхода состоит не только в том, что можно оперативно получить диплом. Процесс организовывается комфортно, с нашей поддержкой. Начав от выбора нужного образца до точного заполнения персональной информации и доставки в любое место страны — все под полным контролем наших специалистов.
Всем, кто пытается найти оперативный способ получения требуемого документа, наша компания готова предложить выгодное решение. Приобрести диплом – значит избежать долгого процесса обучения и сразу перейти к достижению личных целей, будь то поступление в ВУЗ или начало карьеры.
https://vet-aibolit.ru/
Стремитесь к карьере в управлении или фармации? Наш сервис поможет вам достичь этих целей! Купить диплом менеджера или купить диплом фармацевта теперь проще, чем когда-либо. Мы предлагаем качественные документы, которые признаны ведущими организациями и откроют перед вами двери в мир больших возможностей. Обеспечьте себе преимущество на рынке труда с нашими дипломами, которые станут вашим надежным фундаментом для строительства успешной карьеры.
Boomerang Casino: Freispiele ohne Einzahlung
Boomerang Casino ist ein aufstrebendes Online-Casino, das sich durch sein großzügiges Bonusangebot von der Konkurrenz abhebt. Besonders attraktiv sind die Freispiele ohne Einzahlung, die neue Spieler bei der Registrierung erhalten. Diese Freispiele ermöglichen es den Spielern, das Casino und die verschiedenen Spiele ohne eigenes finanzielles Risiko zu testen.
Um die Freispiele zu erhalten, müssen sich die Spieler lediglich auf der Website von Boomerang Casino registrieren. Nach erfolgreicher Anmeldung werden die Freispiele automatisch gutgeschrieben und können sofort genutzt werden. Die Anzahl der Freispiele kann je nach Aktion variieren, aber in der Regel erhalten neue Spieler zwischen 10 und 50 Freispiele ohne Einzahlung.
Die Freispiele können an ausgewählten Spielautomaten verwendet werden und bieten die Möglichkeit, echtes Geld zu gewinnen. Gewinne aus Freispielen unterliegen in der Regel Umsatzbedingungen, die erfüllt werden müssen, bevor eine Auszahlung möglich ist. Diese Bedingungen variieren von Casino zu Casino, aber bei Boomerang Casino sind sie fair und transparent.
Neben den Freispielen ohne Einzahlung bietet Boomerang Casino auch einen lukrativen Willkommensbonus für Ersteinzahler. Spieler können davon profitieren, indem sie ihre erste Einzahlung tätigen und zusätzliches Bonusgeld und Freispiele erhalten. Auch laufende Aktionen und Treueprogramme sorgen dafür, dass Spieler regelmäßig belohnt werden und ihr Spielerlebnis bei Boomerang Casino noch spannender wird.
Insgesamt ist Boomerang Casino eine gute Wahl für Spieler, die auf der Suche nach einem unterhaltsamen und lukrativen Online-Casino sind. Mit den großzügigen Freispielen ohne Einzahlung und weiteren attraktiven Bonusangeboten können Spieler ihre Gewinnchancen erhöhen und spannende Casino-Spiele genießen. Wer also gerne sein Glück versucht, sollte sich Boomerang Casino genauer ansehen und von den großzügigen Bonusangeboten profitieren.
https://boomerangcasino.one/
In Online-Casinos wie Tipico ist es üblich, Geld ein- und auszuzahlen, um an den verschiedenen Spielen teilnehmen zu können. Doch was passiert, wenn das Casino plötzlich die Überweisung blockiert? Dies kann verschiedene Gründe haben und ist für die betroffenen Spieler oft ärgerlich.
Eine mögliche Ursache für die Blockade einer Überweisung kann sein, dass das Casino Sicherheitsbedenken hat. In diesem Fall kann es sein, dass das Casino bestimmte Transaktionen als verdächtig einstuft und deshalb blockiert. Dies kann beispielsweise der Fall sein, wenn ungewöhnlich hohe Beträge überwiesen werden oder wenn die Herkunft des Geldes nicht klar nachvollzogen werden kann.
Ein weiterer Grund für eine blockierte Überweisung kann sein, dass das Casino bestimmte Bonusbedingungen nicht einhält. Wenn ein Spieler beispielsweise versucht, sich Geld auszahlen zu lassen, bevor er die Umsatzbedingungen für einen Bonus erfüllt hat, kann das Casino die Überweisung blockieren.
Es ist wichtig, in solchen Fällen den Kundenservice des Casinos zu kontaktieren und das Problem zu klären. Oftmals kann es sich um ein Missverständnis handeln, das schnell behoben werden kann. In einigen Fällen kann es jedoch auch vorkommen, dass das Casino aus rechtlichen Gründen die Überweisung blockiert und der Spieler sein Geld nicht zurückerhält.
In jedem Fall ist es wichtig, sich vor dem Spielen in einem Online-Casino über die Bedingungen und Richtlinien des Anbieters zu informieren, um Missverständnisse und Probleme zu vermeiden. Nur so kann man sicher sein, dass man sein Geld auch tatsächlich problemlos ein- und auszahlen kann.
https://tipicocasino.one/
allnewstoday365.com
На сайте https://stimul57.ru/ сделайте заказ для того, чтобы приобрести дорожные знаки напрямую от производителя. К важным преимуществам компании относят то, что у нее собственное производство, практичные крепления, а на всю продукцию предоставляются гарантии 7 лет. В работе применяются материалы высокого качества, сертифицированные. Организуется доставка по всей России. Все товары полностью отвечают техническому регламенту, требованиям. На всех этапах производства проходят контроль качества.
В современном мире, где диплом становится началом отличной карьеры в любой сфере, многие ищут максимально быстрый и простой путь получения качественного образования. Факт наличия официального документа переоценить просто невозможно. Ведь именно он открывает двери перед каждым человеком, который собирается вступить в профессиональное сообщество или учиться в ВУЗе.
В данном контексте наша компания предлагает максимально быстро получить этот важный документ. Вы можете заказать диплом старого или нового образца, и это является отличным решением для всех, кто не смог закончить обучение или утратил документ. Любой диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим нюансам. В итоге вы получите полностью оригинальный документ.
Преимущество подобного подхода заключается не только в том, что можно оперативно получить свой диплом. Процесс организован комфортно, с профессиональной поддержкой. От выбора подходящего образца документа до консультаций по заполнению персональных данных и доставки в любой регион России — все под полным контролем качественных специалистов.
В результате, для всех, кто хочет найти максимально быстрый способ получения требуемого документа, наша компания может предложить отличное решение. Заказать диплом – значит избежать долгого процесса обучения и не теряя времени переходить к личным целям: к поступлению в ВУЗ или к началу трудовой карьеры.
https://1abakan.ru/forum/showthread-64726/
http://birdsmoscow.mybb.ru/viewtopic.php?id=388287
Эй, у тебя проблемы с холодильником Gaggenau? Наш Gaggenau холодильник сервис готов помочь. Бесплатный выезд мастера и качественный ремонт гарантированы!
В нашем мире, где диплом – это начало отличной карьеры в любой области, многие пытаются найти максимально простой путь получения качественного образования. Наличие официального документа об образовании переоценить невозможно. Ведь именно он открывает двери перед любым человеком, желающим начать трудовую деятельность или учиться в университете.
В данном контексте наша компания предлагает максимально быстро получить любой необходимый документ. Вы имеете возможность заказать диплом, что становится удачным решением для всех, кто не смог закончить обучение или утратил документ. дипломы выпускаются с особой аккуратностью, вниманием ко всем нюансам. На выходе вы получите полностью оригинальный документ.
Превосходство этого решения состоит не только в том, что вы сможете быстро получить свой диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. От выбора требуемого образца документа до консультаций по заполнению персональной информации и доставки по России — все находится под полным контролем наших мастеров.
Всем, кто хочет найти быстрый и простой способ получить необходимый документ, наша компания предлагает выгодное решение. Купить диплом – это значит избежать продолжительного обучения и не теряя времени перейти к своим целям, будь то поступление в ВУЗ или старт карьеры.
http://roomblock.com/
I’m so grateful for the information you’ve shared. It’s been incredibly enlightening!
https://www.bbb.org/us/nc/greensboro/profile/windshield-replacement/impex-auto-glass-0503-1000042861
Tipico ist eines der beliebtesten Online-Casinos in Deutschland, das eine Vielzahl von Spielen für seine Spieler anbietet. Wenn Sie auch gerne im Tipico Casino spielen möchten, gibt es einige Schritte, die Sie befolgen müssen, um loszulegen.
ZunГ¤chst mГјssen Sie sich auf der Webseite von Tipico registrieren. Klicken Sie dazu auf den Button “Registrieren” und geben Sie Ihre persГ¶nlichen Daten wie Name, Adresse und Geburtsdatum ein. Stellen Sie sicher, dass Sie volljГ¤hrig sind, um im Online-Casino spielen zu dГјrfen.
Nachdem Sie Ihr Konto erstellt haben, können Sie Geld einzahlen, um mit dem Spielen zu beginnen. Tipico akzeptiert verschiedene Zahlungsmethoden wie Kreditkarten, Banküberweisungen und E-Wallets wie PayPal. Wählen Sie die Methode aus, die für Sie am besten geeignet ist und folgen Sie den Anweisungen, um Geld auf Ihr Konto zu überweisen.
Sobald Ihr Konto aufgeladen ist, können Sie aus einer Vielzahl von Spielen im Tipico Casino wählen, darunter Slots, Tischspiele und Live Casino-Spiele. Wählen Sie einfach das Spiel aus, das Ihnen am meisten zusagt, und legen Sie los.
Wenn Sie Fragen haben oder Hilfe benötigen, steht Ihnen der Kundenservice von Tipico rund um die Uhr zur Verfügung. Sie können ihn per E-Mail, Live-Chat oder telefonisch erreichen und erhalten schnell und kompetent Hilfe bei allen Anliegen.
Insgesamt ist es sehr einfach, im Tipico Casino zu spielen, und mit ein paar einfachen Schritten können Sie schon bald Ihre Lieblingsspiele genießen. Viel Spaß und viel Glück!
https://tipicocasino.one/
Компания «Octastudio» специализируется на таких услугах, как: разработка проектов на 1С битрикс, переработка или доработка имеющегося сайта, редактирование контента, анализ конкурентов. На сайте https://octa-studio.ru ознакомьтесь с полным перечнем услуг, которые можно заказать прямо сейчас, оформив заявку либо позвонив по телефону. Также к основным услугам относят и обновление структуры, модернизацию функционала, подготовку портала для продвижения.
На сайте https://t.me/s/mvavada узнайте всю информацию, последние актуальные новости о популярном онлайн-заведении «VAVADA», где представлено огромное количество слотов, интересных развлечений различного вида. Казино дарит отменное настроение, помогает получить завораживающие эмоции и расслабиться. При этом вы всегда сможете рассчитывать на приятное времяпрепровождение. Именно здесь публикуются промокоды, а также самые интересные предложения. Воспользуйтесь ими для того, чтобы сыграть по-крупному.
На сайте https://hyips-money.ru/ ознакомьтесь с любопытными, полезными инвестиционными проектами, которые обязательно принесут неплохой доход. Здесь вы отыщите всю необходимую информацию, которая касается инвестиционных проектов. Перед вами только те проекты, которые действительно платят и предлагают выгодные условия для сотрудничества. Регулярно администраторы сайта мониторят новые проекты, чтобы вы смогли заработать побольше денег и отыскать тот вариант, который действительно работает.
Зайдите на сайт https://ckad165.ru/ и вы сможете ознакомиться с Индустриальным парком в 67 км от Москвы ЦКАД 165. Это новая площадка для производственных и складских объектов со всей необходимой инфраструктурой, собственным съездом с ЦКАД и менеджментом управляющей компании. Узнайте подробнее на сайте.
https://newsprofit.info
emergate.net
Zet Casino ist ein beliebtes Online-Kasino, das seinen Spielern eine Vielzahl von spannenden Spielen und lukrativen Bonusangeboten bietet. Eine der beliebtesten Promotionen bei Zet Casino sind die ilmaiskierrokset, also die Free Spins, die den Spielern die Möglichkeit bieten, kostenlose Spielrunden an ausgewählten Spielautomaten zu spielen.
Diese ilmaiskierrokset sind eine großartige Möglichkeit, um neue Spiele auszuprobieren und vielleicht sogar einen ordentlichen Gewinn zu erzielen, ohne eigenes Geld einzusetzen. Bei Zet Casino können Spieler regelmäßig an verschiedenen Aktionen teilnehmen, um immer wieder neue Free Spins zu erhalten.
Um an den ilmaiskierrokset teilnehmen zu können, müssen die Spieler einfach die Bedingungen der jeweiligen Promotion erfüllen. Dies kann zum Beispiel eine Mindesteinzahlung oder ein bestimmter Umsatz an einem bestimmten Spiel sein. Sobald die Voraussetzungen erfüllt sind, werden die Free Spins automatisch dem Spielerkonto gutgeschrieben.
Die ilmaiskierrokset bei Zet Casino sind eine tolle Möglichkeit, um die Vielfalt und Qualität der angebotenen Spiele kennenzulernen und gleichzeitig die Chance auf attraktive Gewinne zu haben. Wer also gerne Spielautomaten spielt und auf der Suche nach einem unterhaltsamen und seriösen Online-Kasino ist, sollte Zet Casino definitiv einen Besuch abstatten.
https://zetcasino.one/
В нашем мире, где диплом – это начало удачной карьеры в любой отрасли, многие стараются найти максимально быстрый путь получения образования. Факт наличия официального документа об образовании переоценить просто невозможно. Ведь именно он открывает дверь перед каждым человеком, желающим вступить в сообщество профессионалов или учиться в университете.
Мы предлагаем максимально быстро получить любой необходимый документ. Вы имеете возможность заказать диплом нового или старого образца, что является выгодным решением для всех, кто не смог закончить обучение, потерял документ или хочет исправить плохие оценки. Каждый диплом изготавливается с особой аккуратностью, вниманием ко всем нюансам. В результате вы получите продукт, 100% соответствующий оригиналу.
Преимущества данного подхода заключаются не только в том, что вы максимально быстро получите свой диплом. Процесс организовывается комфортно и легко, с нашей поддержкой. Начав от выбора требуемого образца до консультации по заполнению персональных данных и доставки по стране — все находится под полным контролем квалифицированных мастеров.
В результате, всем, кто ищет быстрый и простой способ получить требуемый документ, наша компания готова предложить выгодное решение. Заказать диплом – значит избежать долгого обучения и не теряя времени перейти к достижению личных целей: к поступлению в университет или к началу удачной карьеры.
http://beagle.mybb.ru/viewtopic.php?id=17787
http://www.rusbil.ru/forum/viewtopic.php?p=114586
Индексация ссылок на сайте vindexe.ru
В современном мире, где диплом – это начало отличной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения образования. Факт наличия документа об образовании сложно переоценить. Ведь именно он открывает двери перед любым человеком, желающим вступить в сообщество профессионалов или продолжить обучение в любом ВУЗе.
В данном контексте наша компания предлагает максимально быстро получить этот важный документ. Вы можете заказать диплом старого или нового образца, и это будет удачным решением для всех, кто не смог закончить обучение или утратил документ. дипломы производятся аккуратно, с особым вниманием ко всем нюансам. На выходе вы получите продукт, 100% соответствующий оригиналу.
Плюсы данного подхода заключаются не только в том, что можно оперативно получить диплом. Процесс организовывается комфортно и легко, с нашей поддержкой. От выбора необходимого образца диплома до правильного заполнения личной информации и доставки в любое место страны — все под полным контролем квалифицированных мастеров.
В результате, всем, кто пытается найти максимально быстрый способ получения требуемого документа, наша компания готова предложить выгодное решение. Приобрести диплом – это значит избежать долгого процесса обучения и не теряя времени переходить к достижению личных целей: к поступлению в университет или к началу успешной карьеры.
http://www.passo.su/forums/index.php?autocom=gallery&req=si&img=2995
Ищете свежие анонсы серверов lineage 2? Вам поможет – LA2-ANONS.COM. Поможем вам в подборе достойного игрового сервера. На нашем портале анонсы серверов Lineage 2 регулярно актуализируются, это позволяет любому геймеру быть первым зарегистрированным. Интересует новые сервера lineage 2? La2-anons.com – сайт, мы ежедневно над его функционалом трудимся. При выборе сервера для игры Lineage 2, советуем свое внимание обратить на платформы, где написано VIP. Предлагаем только актуальную информацию, с которой вы можете прямо сейчас ознакомиться.
Das Boomerang Online Casino bietet seinen Spielern eine Vielzahl von spannenden Spielen und großzügigen Boni. Mit einer benutzerfreundlichen Oberfläche und einer breiten Auswahl an Spielen, ist dieses Casino bei Online-Glücksspielern sehr beliebt.
Das Boomerang Online Casino ist lizenziert und reguliert, um ein sicheres und faires Spielerlebnis zu gewährleisten. Die Spieler können aus einer Vielzahl von beliebten Spielen wie Spielautomaten, Roulette, Blackjack und Poker wählen.
Darüber hinaus bietet das Boomerang Online Casino regelmäßig attraktive Bonusangebote und Aktionen an, um die Spieler zu belohnen und ihre Gewinnchancen zu erhöhen. Diese Boni können in Form von Freispielen, Einzahlungsboni oder Cashback-Angeboten erfolgen.
Ein weiterer Vorteil des Boomerang Online Casinos ist der Kundensupport, der rund um die Uhr verfügbar ist, um den Spielern bei Fragen oder Problemen zu helfen. Die Spieler können den Kundensupport per E-Mail, Live-Chat oder Telefon erreichen.
Insgesamt bietet das Boomerang Online Casino ein unterhaltsames und lohnendes Spielerlebnis fГјr alle GlГјcksspiel-Enthusiasten. Mit einer sicheren und fairen Spielumgebung, einer groГџen Auswahl an Spielen und groГџzГјgigen Boni, ist dieses Casino definitiv einen Besuch wert.
https://boomerangcasino.one/
Thanks a lot for sharing this with all people you actually realize what you’re speaking approximately! Bookmarked. Please also consult with my site =). We could have a link exchange contract among us
http://www.diplomans-russiyans.ru
my company Credit cards
На сайте https://1roma.ru/ вы сможете выбрать и заказать такой строительный материал, как: фасадные панели, сайдинг, дренажные системы, водостоки, газонные решетки и многое другое. Перед вами огромный ассортимент вариантов, привлекательных коллекций различных фактур и цветовых решений. Несколько сотен вариантов отделки, в том числе, темные цветостойкие панели. Прямо сейчас посмотрите все доступные варианты. Вы сможете пролистать каталог всего за пару минут, чтобы ознакомиться с готовыми решениями.
Ищете интересный портал о строительстве, ремонте и садоводстве? My-tvset.ru – это то, что вам нужно! Здесь вы найдете такие рубрики, как: квартира, лайфхаки, дача, ремонт, дом, мебель. Ищете вишня призвание опылители? My-tvset.ru – сайт, где есть удобный поиск, можете прямо сейчас им воспользоваться. У нас вы узнаете, как создать функциональный туалет на даче, как выбрать самую лучшую садовую качелю, какие существуют типы стяжки пола, как хранить овощи в квартире. Также поведаем вам о том, какой лучше купить для частного дома счетчик воды. Заходите и читайте наши интересные статьи!
автошкола категория б
Tipico Casino sperren: So schГјtzen Sie sich vor Spielsucht
Das Tipico Casino ist eine beliebte Online-Glücksspielplattform, die eine Vielzahl von Casino-Spielen für Spieler anbietet. Doch wie bei allen Formen des Glücksspiels besteht auch beim Online-Casino die Gefahr, dass man süchtig werden kann. Um sich vor den negativen Auswirkungen von exzessivem Spielen zu schützen, bietet Tipico seinen Spielern die Möglichkeit, sich selbst zu sperren.
Die Sperrung des Tipico Casinos kann auf unterschiedliche Weise erfolgen. Zum einen kann man eine temporäre Selbstsperre von einem Tag bis zu sechs Monaten festlegen. Während dieser Zeit ist es nicht möglich, das Casino zu betreten und an Spielen teilzunehmen. Diese Option eignet sich besonders für Spieler, die merken, dass sie ihr Spielverhalten nicht mehr unter Kontrolle haben und eine Pause brauchen.
Eine dauerhafte Selbstsperre ist eine weitere Möglichkeit, um sich vor Spielsucht zu schützen. Wenn man sich für diese Option entscheidet, wird das Konto dauerhaft gesperrt und kann nicht mehr aktiviert werden. Dies ist eine drastische Maßnahme, die jedoch in manchen Fällen notwendig sein kann, um sich vor den negativen Auswirkungen von Glücksspielsucht zu schützen.
Um die Sperrung des Tipico Casinos zu beantragen, muss man sich an den Kundenservice des Unternehmens wenden und sein Anliegen persönlich vortragen. Dieser Prozess soll sicherstellen, dass die Sperrung wirklich im Sinne des Spielers ist und nicht durch Dritte veranlasst wird.
Insgesamt ist die Möglichkeit, sich selbst im Tipico Casino zu sperren, ein wichtiges Instrument, um sich vor Spielsucht zu schützen. Spieler sollten sich ihrer eigenen Grenzen bewusst sein und rechtzeitig eingreifen, wenn sie merken, dass ihr Spielverhalten außer Kontrolle gerät. Die Sperrung des Casinos kann dabei helfen, einen klaren Kopf zu bekommen und sich wieder auf das Wesentliche zu konzentrieren: Spaß am Spiel, ohne dabei die Kontrolle zu verlieren.
https://tipicocasino.one/
купить недвижимость на кипре
автошкола обучение вождению
check this link right here now cc+cvv
кипр квартира
На сайте https://t.me/s/tinder_mobile ознакомьтесь с интересной, познавательной информацией, которая касается проекта Tinder. Теперь вы сможете посетить его официальный канал, на котором рассказывается об отношениях, о том, как организовать удачное первое свидание и сделать так, чтобы оно прошло по всем правилам. Вы можете сами делиться своим мнением, оставлять комментарии. На канале имеется и подборка интересных рекомендаций, советов, которые точно вам помогут обрести счастье и завести роман.
navigate to this website bidencash
salaty-na-stol.info
https://newssahara.com
В нашем мире, где диплом является началом успешной карьеры в любой области, многие ищут максимально быстрый путь получения качественного образования. Наличие официального документа об образовании сложно переоценить. Ведь именно он открывает двери перед любым человеком, который собирается вступить в профессиональное сообщество или продолжить обучение в университете.
Мы предлагаем оперативно получить любой необходимый документ. Вы можете приобрести диплом, что является удачным решением для всех, кто не смог закончить обучение или потерял документ. дипломы производятся с особой тщательностью, вниманием ко всем деталям, чтобы в итоге получился 100% оригинальный документ.
Преимущества подобного решения состоят не только в том, что можно быстро получить свой диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. От выбора нужного образца документа до консультаций по заполнению персональных данных и доставки по России — все под абсолютным контролем наших мастеров.
Таким образом, для тех, кто хочет найти максимально быстрый способ получить требуемый документ, наша компания может предложить отличное решение. Заказать диплом – это значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://finansforum.apbb.ru/viewtopic.php?id=11447
Metalworking on lathes involves many https://supesolar.com actions when deepening products or cutting out parts is required. Robust cutting tools with low wear and high hardness are required. It is proposed to buy replacement groove plates from well-known manufacturers.
The main advantage of a forklift is its versatility and newssugar.com ease of use. Essentially, it’s just a dolly with a durable fork that can be used to lift pallets or large loads to any height.
снять виллу на кипре
Full Report Pot player
The perspective is incredibly valuable to me. Thanks for opening my eyes to new ideas.
https://www.tiktok.com/@impexautoglass/video/7348537796430286123
Народный путеводитель Даркнета – Onion сайты, Народный путеводитель Даркнета
Магазин, где можно купить элегантные раковины оскольская керамика от ведущих производителей.
Metal structures must be produced under strict ochen-vkusno.com quality control. Absolutely all work is checked – from the manufacture of elements to final assembly. It is necessary to check their size, strength, coating and other parameters.
На сайте http://koleso-na-hodu.ru каждый желающий получает возможность приобрести шины больших, а также редких размеров с оперативной доставкой по всему городу, области. Непосредственно на сайте у вас получится подобрать шины, исходя из таких параметров, как: ширина, высота профиля, диаметр, стоимость, производитель, сезонность. Вся продукция сертифицированная, качественная, оригинальная. Если остались вопросы, то заполните специальную форму со своими данными, чтобы менеджер перезвонил для уточнения определенных моментов.
Once a metal structure tatraindia.com is installed, it must be maintained regularly. Thanks to this, it will last much longer.
Das Online Tipico Casino ist eine beliebte Plattform für Glücksspiele im Internet. Es bietet eine Vielzahl von Spielen wie Slots, Roulette, Blackjack und Poker, die von renommierten Softwareanbietern entwickelt wurden. Das Casino zeichnet sich durch sein benutzerfreundliches Design, seine hohe Sicherheit und seine zuverlässigen Zahlungsmethoden aus.
Die Spieler können sowohl über ihren Desktop-Computer als auch über ihre mobilen Geräte auf das Online Tipico Casino zugreifen. Die mobile Version der Plattform bietet eine nahtlose Spielerfahrung, sodass die Nutzer auch unterwegs alle Spiele genießen können.
Ein weiterer großer Vorteil des Online Tipico Casinos sind die großzügigen Bonusangebote. Neue Spieler erhalten oft Willkommensbonusse, Freispiele und andere Promotionen, die ihnen den Einstieg erleichtern. Auch bestehende Spieler werden regelmäßig mit Bonusangeboten belohnt, um ihre Treue zu würdigen.
Das Online Tipico Casino legt großen Wert auf verantwortungsbewusstes Glücksspiel und bietet verschiedene Maßnahmen zur Unterstützung von Spielern mit problematischem Spielverhalten an. Die Spieler können Limits für Einzahlungen und Spielzeiten festlegen oder sich selbst vom Spielen ausschließen, falls nötig.
Insgesamt bietet das Online Tipico Casino eine sichere und unterhaltsame Umgebung fГјr GlГјcksspiel-Fans. Mit einer Vielzahl von Spielen, groГџzГјgigen Boni und verantwortungsbewusstem Spiel ist es eine empfehlenswerte Plattform fГјr alle, die gerne online spielen.
https://tipicocasino.one/
Reducing vibration in industrial shredding machines to enhance safety and efficiency was accomplished with Vibromera’s technology. Detailed information is provided on their website https://vibromera.eu/example/vacuum_pumps-rotors-balancing/
Blacksprut ссылка – Blacksprut, Bs2site
На сайте https://interpol-s.ru/ вы сможете заказать проверку на полиграфе. Вы пройдете тестирование на профессиональном устройстве. Проводятся зависимые и независимые экспертизы. Вся информация проверяется на достоверность. В обязательном порядке соблюдается закон, требования. Записаться на услугу можно в любое время, когда вам удобно. В компании оказываются такие популярные и важные услуги, как: проверка на полиграфе, полиграф для женщин, проведение судебных экспертиз, тестирование персонала.
дешевые дома на кипре
снять жилье на кипре на длительный
купить дом в кипре на берегу моря
Das Tipico Casino bietet eine Vielzahl von spannenden Spielen und Gewinnmöglichkeiten für Spieler aus Deutschland. Eines der herausragenden Merkmale des Casinos ist die Möglichkeit, echtes Geld zu gewinnen und sich dieses auch problemlos auszahlen zu lassen.
Das “tipico casino cash” ist ein Service, der es den Spielern ermГ¶glicht, ihre Gewinne schnell und einfach auf ihr Bankkonto auszahlen zu lassen. Mit nur wenigen Klicks kГ¶nnen Spieler ihre Gewinne beantragen und innerhalb weniger Tage erhalten. Dies macht das Spielen im Tipico Casino nicht nur unterhaltsam, sondern auch lohnenswert.
Darüber hinaus bietet das Tipico Casino eine Vielzahl von sicheren und zuverlässigen Zahlungsmethoden, um Ein- und Auszahlungen zu tätigen. Spieler können zwischen Kreditkarten, Banküberweisungen, E-Wallets und Prepaid-Karten wählen, um sicherzustellen, dass ihre finanziellen Transaktionen geschützt sind.
Das “tipico casino cash” ist ein weiterer Grund, warum das Tipico Casino bei Spielern aus Deutschland so beliebt ist. Mit der MГ¶glichkeit, echtes Geld zu gewinnen und sich dieses jederzeit auszahlen zu lassen, bietet das Casino ein erstklassiges Spielerlebnis. Besuchen Sie das Tipico Casino noch heute und entdecken Sie die aufregende Welt des GlГјcksspiels mit der MГ¶glichkeit von echtem Cash-Gewinn!
https://tipicocasino.one/
В современном мире, где диплом является началом отличной карьеры в любом направлении, многие ищут максимально простой путь получения качественного образования. Наличие документа об образовании трудно переоценить. Ведь диплом открывает двери перед любым человеком, который хочет начать профессиональную деятельность или учиться в университете.
Наша компания предлагает быстро получить этот необходимый документ. Вы можете приобрести диплом нового или старого образца, что будет отличным решением для всех, кто не смог закончить обучение или потерял документ. Любой диплом изготавливается аккуратно, с особым вниманием ко всем нюансам, чтобы в итоге получился 100% оригинальный документ.
Превосходство этого решения заключается не только в том, что можно максимально быстро получить диплом. Процесс организован просто и легко, с нашей поддержкой. Начиная от выбора подходящего образца диплома до консультации по заполнению личных данных и доставки по стране — все под абсолютным контролем квалифицированных специалистов.
Для всех, кто ищет оперативный способ получения необходимого документа, наша компания может предложить отличное решение. Заказать диплом – это значит избежать долгого процесса обучения и не теряя времени переходить к достижению своих целей, будь то поступление в университет или начало карьеры.
http://pdduz.ru/pdd.php
В современном мире, где диплом является началом удачной карьеры в любой области, многие стараются найти максимально простой путь получения образования. Важность наличия официального документа переоценить просто невозможно. Ведь диплом открывает дверь перед каждым человеком, который хочет начать профессиональную деятельность или продолжить обучение в высшем учебном заведении.
В данном контексте наша компания предлагает очень быстро получить этот необходимый документ. Вы имеете возможность заказать диплом, и это будет удачным решением для человека, который не смог закончить обучение или потерял документ. диплом изготавливается аккуратно, с особым вниманием ко всем нюансам, чтобы в результате получился документ, 100% соответствующий оригиналу.
Плюсы этого подхода заключаются не только в том, что вы сможете оперативно получить диплом. Процесс организовывается просто и легко, с нашей поддержкой. Начиная от выбора подходящего образца до точного заполнения личной информации и доставки в любой регион страны — все под абсолютным контролем наших мастеров.
Всем, кто хочет найти оперативный способ получения требуемого документа, наша услуга предлагает отличное решение. Купить диплом – это значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://bestonshow.bbcity.ru/viewtopic.php?id=625
http://forum.f-rpg.me/viewtopic.php?id=2167
На сайте https://rybelsus.com.ru/ вы сможете заказать оперативную доставку такого эффективного препарата, который не имеет побочных эффектов, как «РЕБЕЛСАС». Собственная служба доставки позволит сделать так, чтобы средство было доставлено максимально оперативно. А оплата осуществляется только после получения посылки. У вас получится сделать заказ в режиме реального времени и тогда, когда удобно. Продажа только оригинального, сертифицированного товара. Совершайте выгодные покупки в компании, которая работает для вас!
https://lavrus.org
It is worth noting breakingnews77.com that the loader can be made in the form of a trolley without its own traction, as well as in the form of a powered/gasoline self-propelled device, with which you can transport minimally heavy objects over significant distances within the warehouse. Another advantage is simple maintenance, which ensures the absence of technical bells and whistles, but this depends on the specific model of the device.
Индексация ссылок на сайте vindexe
GdeRaznica.ru – портал, где представлены следующие рубрики: экономика, общество, медицина, красота, транспорт, география, технологии. Информацию берем из первоисточников и обращаемся только к профильным экспертам. Ищете 2d это в очках или нет? Gderaznica.ru – сайт, где имеется удобный поиск, воспользоваться им можете в любое время. У нас вы сможете узнать, чем отличается Росконтроль от Роскачества, как различить спам и флуд, зачем пить коллаген, какой препарат лучше всего помогает бросить курить. Также вам расскажем, что это такое виниры и какова их цена.
Zet Casino ist eine beliebte Online-Glücksspielplattform, die Spielern eine Vielzahl von Casino-Spielen und Boni bietet. In diesem Artikel möchten wir einige der Erfahrungen teilen, die Spieler mit Zet Casino gemacht haben.
Viele Spieler loben das breite Angebot an Spielen, das Zet Casino zu bieten hat. Von klassischen Tischspielen wie Blackjack und Roulette bis hin zu modernen Spielautomaten und Live-Casino-Spielen gibt es für jeden etwas. Die Benutzeroberfläche der Website ist benutzerfreundlich und intuitiv, was es den Spielern leicht macht, sich zu orientieren.
Ein weiterer positiver Punkt, der häufig von Spielern hervorgehoben wird, sind die großzügigen Boni und Promotionen, die Zet Casino anbietet. Neue Spieler können von einem Willkommensbonus profitieren, der ihre erste Einzahlung verdoppelt und zusätzliche Freispiele beinhaltet. Darüber hinaus gibt es regelmäßig Aktionen und Turniere, bei denen die Spieler die Chance haben, zusätzliche Preise zu gewinnen.
Die Auszahlungen bei Zet Casino werden ebenfalls von vielen Spielern als schnell und zuverlässig beschrieben. Das Casino bietet eine Vielzahl von Zahlungsmethoden an, um sicherzustellen, dass Spieler ihre Gewinne schnell und einfach abheben können.
Insgesamt sind die Erfahrungen mit Zet Casino größtenteils positiv. Die Vielfalt an Spielen, großzügige Boni und zuverlässige Auszahlungen machen es zu einer guten Wahl für Glücksspiel-Liebhaber. Wenn Sie auf der Suche nach einem neuen Online-Casino sind, sollten Sie Zet Casino definitiv eine Chance geben.
https://zetcasino.one/
Hi there! Would you mind if I share your blog with my facebook group? There’s a lot of people that I think would really appreciate your content. Please let me know. Cheers
https://squareblogs.net/denopepexr/h1-b-iak-zaminiti-sklo-far-samostiino-posibnik-vid-farfarlight-b-h1
В наше время, когда диплом – это начало успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа трудно переоценить. Ведь диплом открывает дверь перед людьми, стремящимися начать трудовую деятельность или учиться в ВУЗе.
В данном контексте наша компания предлагает очень быстро получить этот необходимый документ. Вы сможете купить диплом, что становится отличным решением для человека, который не смог закончить образование, потерял документ или желает исправить плохие оценки. Все дипломы изготавливаются аккуратно, с максимальным вниманием к мельчайшим деталям, чтобы в итоге получился 100% оригинальный документ.
Плюсы данного подхода заключаются не только в том, что вы сможете оперативно получить диплом. Весь процесс организован удобно, с профессиональной поддержкой. От выбора требуемого образца до точного заполнения персональных данных и доставки по стране — все под абсолютным контролем опытных мастеров.
Всем, кто ищет оперативный способ получить необходимый документ, наша компания предлагает отличное решение. Приобрести диплом – значит избежать продолжительного процесса обучения и не теряя времени переходить к своим целям, будь то поступление в ВУЗ или начало карьеры.
https://vopros-ik.ru/kontakty
Das Zet Casino ist ein beliebtes Online-Casino, das eine Vielzahl von Spielen und Promotionen fГјr seine Spieler bietet. Eine der aufregendsten Aktionen im Jahr 2021 ist der Zet Casino Promo-Code, der neuen Spielern groГџzГјgige Boni und Belohnungen bietet.
Als neuer Spieler im Zet Casino können Sie von dem Promo-Code profitieren, der Ihnen einen Willkommensbonus auf Ihre erste Einzahlung gewährt. Dies bedeutet, dass Sie zusätzliches Geld erhalten, um Ihre Lieblingsspiele zu spielen und Ihre Gewinnchancen zu erhöhen.
Darüber hinaus bietet das Zet Casino regelmäßig spezielle Promotionen an, die den Spielern die Möglichkeit geben, zusätzliche Boni, Freispiele und Preise zu gewinnen. Diese Aktionen werden oft über den Newsletter des Casinos oder auf der Website bekannt gegeben, sodass es sich lohnt, regelmäßig nach neuen Angeboten Ausschau zu halten.
Um den Promo-Code im Zet Casino zu nutzen, müssen Sie einfach während der Registrierung oder Einzahlung den angegebenen Code eingeben. Sobald Sie dies getan haben, wird der Bonus automatisch Ihrem Konto gutgeschrieben und Sie können mit dem Spielen beginnen.
Es ist jedoch wichtig zu beachten, dass jeder Bonus im Zet Casino bestimmten Bedingungen und Umsatzanforderungen unterliegt. Bevor Sie den Bonus beantragen, sollten Sie sich daher die Geschäftsbedingungen durchlesen, um sicherzustellen, dass Sie die Bedingungen erfüllen und Ihren Bonus erfolgreich umsetzen können.
Insgesamt bietet der Zet Casino Promo-Code 2021 eine großartige Möglichkeit, zusätzliche Belohnungen und Boni zu erhalten, während Sie Ihre Lieblingsspiele spielen. Wenn Sie also auf der Suche nach einem neuen Online-Casino sind, das großzügige Aktionen anbietet, sollten Sie das Zet Casino auf jeden Fall in Betracht ziehen.
https://zetcasino.one/
Howdy superb blog! Does running a blog similar to this require a lot of work? I’ve very little understanding of programming but I was hoping to start my own blog soon. Anyhow, if you have any ideas or techniques for new blog owners please share. I know this is off subject nevertheless I simply wanted to ask. Cheers!
https://privatebin.net/?3ce2a562b3ff82c0#CHmYjCi5AaTBp8rYsBaNQaJiYCAEEkyvj28fTnv4Khq5
http://odesit.com/fm-t-19063-last.php
Visit the website https://4rabet.app/ and you can download the 4rabet application on Android and iOS for free. 4rabet apk or 4rabet update is easy to download. 4rabet game download install on your device. 4rabet download apk or 4rabet app download we have a new version on our website.
Студия звукозаписи в Минске Senjor Minor https://senjorminor.by/ это профессиональная студия звукозаписи, где вы сможете записать песню, написать аранжировку, сделать сведение, мастеринг, озвучку рекламных аудиороликов и получить услуги по продвижению вашего творчества. Зайдите на сайт – узнайте подробную информацию.
На сайте https://sobr26.ru ознакомьтесь с номером телефона охранной организации СОБР. Здесь оказываются услуги, связанные с охраной недвижимости, организуется безопасность объекта, есть возможность воспользоваться физической охраной, которая оказывается более 20 лет. Прямо сейчас вы сможете рассчитывать на бесплатную консультацию. Каждый клиент сможет организовать пультовую, физическую охрану, пожарную сигнализацию, видеонаблюдение. Для того чтобы воспользоваться услугами, оставьте заявку непосредственно на сайте.
Boomerang Casino ist ein Online-Casino, das sich in kГјrzester Zeit einen Namen auf dem Markt gemacht hat. Das Casino bietet eine Vielzahl von Spielen, groГџzГјgige Boni und ein sicheres Spielerlebnis.
Die meisten Spieler, die Boomerang Casino ausprobiert haben, sind mit ihrer Erfahrung zufrieden und geben positive Bewertungen ab. Die Spieleauswahl ist umfangreich und umfasst Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Die Spiele stammen von renommierten Softwareanbietern wie NetEnt, Microgaming, Play’n GO und anderen.
Ein weiterer Pluspunkt von Boomerang Casino sind die großzügigen Bonusangebote für neue und bestehende Spieler. Neue Spieler erhalten in der Regel einen Willkommensbonus bei ihrer ersten Einzahlung, der ihnen zusätzliches Spielguthaben und Freispiele verschafft. Darüber hinaus gibt es regelmäßig Aktionen und Turniere, bei denen Spieler zusätzliche Preise gewinnen können.
Das Casino legt auch großen Wert auf die Sicherheit und den Schutz seiner Spieler. Die Website verfügt über eine SSL-Verschlüsselung, um sicherzustellen, dass alle finanziellen Transaktionen sicher sind. Darüber hinaus ist das Casino von einer renommierten Glücksspielbehörde lizenziert und reguliert, was bedeutet, dass es strenge Regeln und Vorschriften einhalten muss.
Insgesamt hat Boomerang Casino eine Menge zu bieten und ist definitiv einen Besuch wert. Mit einer breiten Palette an Spielen, groГџzГјgigen Boni und einer sicheren Spielerfahrung ist das Casino eine gute Wahl fГјr alle, die nach einem unterhaltsamen und lohnenden Online-Casino-Erlebnis suchen.
https://boomerangcasino.one/
На сайте https://razrabotka.pro/ закажите производство электроники, электронных приборов, а также различных компонентов для электронных устройств. Что касается разработки, то ее стоимость начинается от 100 000 рублей. Все электронные приборы производятся в нужном количестве, а потому получится заказать в требующемся объеме. Воспользуйтесь всем комплексом работ, которые связаны с производством, разработкой электроники. Специально для вас разработка проектов электронных агрегатов. Также возможно производство изделий по готовому проекту.
Компания See Real предлагает услуги в сфере светодиодных технологий и наружной рекламы. Мы любой бизнес делаем приметным и обеспечиваем приемлемые цены. Рады обговорить с вами в любое время самую смелую идею. Оставьте личные данные, и мы свяжемся с вами в ближайшее время для обсуждения важных вопросов. https://iseer.kz/ – сайт, где у вас есть возможность прямо сейчас ознакомиться с нашими архитектурными решениями и посмотреть виды рекламы компании, также сделать заказ звонка консультанта для расчета. Квалифицированная команда готова к любым творческим вызовам.
В современном мире, где диплом – это начало отличной карьеры в любой сфере, многие пытаются найти максимально быстрый путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь диплом открывает двери перед любым человеком, который стремится начать трудовую деятельность или учиться в университете.
В данном контексте наша компания предлагает максимально быстро получить любой необходимый документ. Вы имеете возможность приобрести диплом, что является выгодным решением для всех, кто не смог закончить обучение, потерял документ или хочет исправить свои оценки. Все дипломы выпускаются с особой тщательностью, вниманием ко всем нюансам. На выходе вы сможете получить продукт, полностью соответствующий оригиналу.
Преимущество такого решения состоит не только в том, что вы оперативно получите свой диплом. Процесс организовывается комфортно, с профессиональной поддержкой. Начав от выбора подходящего образца документа до точного заполнения личных данных и доставки в любой регион страны — все под полным контролем квалифицированных специалистов.
Таким образом, всем, кто ищет быстрый и простой способ получения требуемого документа, наша компания предлагает отличное решение. Заказать диплом – это значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению личных целей: к поступлению в университет или к началу трудовой карьеры.
https://re-tracker.ru/index.php?showtopic=860
http://suponevo.webtalk.ru/viewtopic.php?id=8949
На сайте https://linkey-light.ru/catalog/promyshlennye_svetilniki/svetodiodnye_svetilniki_dlya_avtoservisa/ представлены светодиодные светильники, предназначенные для автосервиса. Здесь находятся самые интересные, функциональные и совершенные модели. Светильники повышают качество диагностики, ускоряют выполнение различных задач, повышают функциональность, а также безопасность при обслуживании. В магазине представлены светильники самой разной мощности. Но для того, чтобы оборудование работало эффективно, необходимо выполнить профессиональный монтаж.
Once a metal structure is installed, it must dominicandesign.net be maintained regularly.
Forklifts can be called an indispensable 360o.info element of equipment, which is actively used in the arrangement of warehouse premises.
apple диагностика
диагностика apple
Das Boomerang Casino hat sich in der Welt der Online-Casinos einen Namen gemacht, vor allem dank seiner großzügigen Boni und Aktionen. Unter den beliebten Angeboten sind die Boomerang Casino No Deposit Bonus Codes, die es Spielern ermöglichen, ohne eine Einzahlung kostenfrei zu spielen.
Die No Deposit Bonus Codes sind eine großartige Möglichkeit für neue Spieler, das Casino kennenzulernen, ohne dabei eigenes Geld riskieren zu müssen. Diese Codes können auf verschiedenen Websites oder direkt vom Casino selbst gefunden werden und ermöglichen es den Spielern, kostenloses Bonusgeld oder Freispiele zu erhalten.
Um die No Deposit Bonus Codes zu nutzen, müssen Spieler einfach den Code während des Anmeldevorgangs oder im Kassenbereich eingeben. Das Bonusgeld oder die Freispiele werden dann sofort dem Spielerkonto gutgeschrieben, ohne dass eine Einzahlung erforderlich ist.
Es ist jedoch wichtig zu beachten, dass No Deposit Boni oft bestimmten Umsatzbedingungen unterliegen, die erfüllt werden müssen, bevor Gewinne ausgezahlt werden können. Es ist daher ratsam, die Geschäftsbedingungen sorgfältig zu lesen, bevor man einen Bonus in Anspruch nimmt.
Insgesamt sind die Boomerang Casino No Deposit Bonus Codes eine großartige Möglichkeit für Spieler, das Casino zu erkunden und möglicherweise sogar echte Gewinne zu erzielen, ohne dabei eigenes Geld riskieren zu müssen. Es lohnt sich daher, Ausschau nach diesen Bonuscodes zu halten und das Beste aus ihnen herauszuholen.
https://boomerangcasino.one/
If you need to weld elements, you madeintexas.net should trust the work to a welder with the appropriate skills. The quality of welding work must be constantly monitored.
women18.com
Широкий ассортимент установка навеса над крыльцом ангара по доступным ценам.
Das Tipico Casino bietet seinen Spielern die Möglichkeit, an zahlreichen spannenden Glücksspielen teilzunehmen und attraktive Gewinne zu erzielen. Ob Slotmaschinen, Roulette oder Black Jack – im Tipico Casino gibt es eine große Auswahl an Spielen, die für Abwechslung und Spannung sorgen.
Wer im Tipico Casino gewinnt, kann sich über hohe Gewinne freuen. Je nach Spiel und Einsatz können Spieler hierbei große Summen gewinnen und ihr Guthaben deutlich erhöhen. Besonders beliebt sind dabei die Jackpot-Slots, bei denen teilweise Millionenbeträge auf einen glücklichen Gewinner warten.
Um im Tipico Casino erfolgreich zu sein, sollten Spieler einige Tipps beachten. Dazu gehört es beispielsweise, sich vor dem Spiel über die Regeln und Strategien der jeweiligen Spiele zu informieren. Zudem ist es wichtig, verantwortungsvoll zu spielen und nie mehr Geld einzusetzen, als man sich leisten kann zu verlieren.
Auch das Setzen von Limits kann helfen, das Spielverhalten im Casino unter Kontrolle zu behalten. Wer sich an seine Limits hält, läuft nicht Gefahr, in eine Spielsucht abzurutschen und kann das Casino-Spiel als spannende Freizeitbeschäftigung genießen.
Im Tipico Casino sind Gewinne keine Seltenheit und mit etwas Glück können Spieler hier große Summen gewinnen. Wer verantwortungsvoll spielt und seine Strategie klug wählt, hat gute Chancen, im Tipico Casino erfolgreich zu sein und attraktive Preise abzuräumen.
https://tipicocasino.one/
Разработка электроники – компания, которая предоставляет полный комплекс высококачественных услуг. Здесь можете прямо сейчас заказать разработку электроники. Чтобы получить предварительную консультацию, свяжитесь с нами по телефону. Благодаря многолетнему опыту, мы оперативно приступаем к созданию проекта. Ищете разработка электронных устройств? Razrabotka.pro – сайт, где вы найдете наши работы. Вы узнаете, как и кому, мы помогаем. Также размещаем статьи, которые связаны с изготовлением электроники. Всегда рады обсудить детали вашего проекта, обращайтесь.
На сайте http://nemans.ru вы сможете приобрести всю необходимую продукцию, включая пакеты с ручками, фасовочные пакеты, мешки полипропиленовые, пленку армированную, полиэтиленовую. Также в разделе имеется ветошь, ароматное мыло, перчатки, черенки, бытовая химия, ведра и многое другое, что вы сможете заказать прямо сейчас. Среди рекомендованных товаров находятся вязаные перчатки, туалетная бумага, хозяйственное мыло, неткол. Вся продукция отличного качества, надежная и наделена длительными сроками эксплуатации.
Узнайте больше о преимуществах наших навес для автомобиля двускатный.
В современном мире, где диплом является началом отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Необходимость наличия официального документа переоценить просто невозможно. Ведь диплом открывает дверь перед любым человеком, который собирается начать трудовую деятельность или учиться в ВУЗе.
Предлагаем очень быстро получить этот необходимый документ. Вы можете заказать диплом нового или старого образца, что становится выгодным решением для всех, кто не смог завершить обучение, потерял документ или хочет исправить свои оценки. диплом изготавливается аккуратно, с особым вниманием ко всем нюансам, чтобы в итоге получился полностью оригинальный документ.
Преимущество этого подхода заключается не только в том, что вы сможете оперативно получить свой диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. От выбора требуемого образца документа до точного заполнения персональных данных и доставки по стране — все будет находиться под абсолютным контролем наших специалистов.
В итоге, для тех, кто пытается найти быстрый и простой способ получения необходимого документа, наша компания предлагает отличное решение. Приобрести диплом – это значит избежать долгого обучения и не теряя времени переходить к своим целям: к поступлению в университет или к началу удачной карьеры.
http://passo.su/forums/index.php?showtopic=6433
http://fura.mybb.ru/viewtopic.php?id=117
Список Tor сайтов – Даркнет поисковик, Список сайтов Даркнета
Boomerang Casino Mobil: Das ultimative Spielerlebnis unterwegs
Im Zeitalter der Digitalisierung ist es heutzutage wichtiger denn je, dass Online-Casinos eine benutzerfreundliche und mobile Plattform anbieten. Boomerang Casino hat dies erkannt und bietet seinen Kunden mit Boomerang Casino Mobil die Möglichkeit, ihre Lieblingsspiele auch unterwegs zu genießen.
Boomerang Casino Mobil ermГ¶glicht es den Spielern, von Гјberall aus und zu jeder Zeit auf ihr Casino-Konto zuzugreifen. Egal ob auf dem Weg zur Arbeit, in der Mittagspause oder gemГјtlich auf der Couch zu Hause – mit Boomerang Casino Mobil haben die Spieler ihr persГ¶nliches Casino immer griffbereit.
Die mobile Plattform von Boomerang Casino Гјberzeugt nicht nur durch ihre Benutzerfreundlichkeit, sondern auch durch ihre vielfГ¤ltige Auswahl an Spielen. Von klassischen Tischspielen wie Blackjack und Roulette Гјber beliebte Spielautomaten bis hin zu aufregenden Live-Casino-Spielen – bei Boomerang Casino Mobil ist fГјr jeden Geschmack etwas dabei.
Darüber hinaus bietet Boomerang Casino Mobil seinen Spielern regelmäßige Aktionen, Boni und Turniere, um das Spielerlebnis noch spannender zu gestalten. Mit nur wenigen Klicks können die Spieler an den neuesten Aktionen teilnehmen und sich so zusätzliche Gewinnchancen sichern.
Boomerang Casino Mobil zeichnet sich zudem durch eine sichere und zuverlässige Zahlungsabwicklung aus. Die Spieler können aus einer Vielzahl von Zahlungsmethoden wählen und sich darauf verlassen, dass ihre persönlichen Daten und Ein- und Auszahlungen jederzeit geschützt sind.
Insgesamt bietet Boomerang Casino Mobil das ultimative Spielerlebnis für unterwegs. Egal ob Anfänger oder erfahrener Spieler, mit Boomerang Casino Mobil können alle Casino-Liebhaber ihre Lieblingsspiele jederzeit und überall genießen. Probieren Sie es aus und entdecken Sie die Welt des Online-Glücksspiels mit Boomerang Casino Mobil. Viel Spaß und viel Glück!
https://boomerangcasino.one/
Хотите избавиться от морщинок и носогубных складок? Плюреаль – это то, что вам нужно! Он действует оперативно, результат вас длительное время будет радовать. Филлеры линейки Pluryal подвергаются строжайшему контролю качества продукции. Стоимость доступная, после их использования не возникает аллергических реакций. Ваша кожа станет более подтянутой. Ищете лучшие филлеры для лица? Pluryal.info – сайт, где у вас есть возможность купить средства Плюреаль, а также на сотрудничество подать заявку. Если у вас есть какие-либо вопросы, не стесняйтесь обращаться к нам, мы с радостью ответим на них.
На сайте https://novosti-ru.com/ ознакомьтесь с интересной, познавательной информацией на самую разную тему, в том числе, про еду, автомобили, шоу-бизнес, общество, праздники, медицина, здоровье, техника и наука. Также есть информация и на тему культуры, спорта, отдыха, туризма, интернет-технологий. Все новости актуальные, свежие, а потому данным точно можно доверять. Они составлены экспертами, поэтому содержательные, информативные. Регулярно появляются актуальные новости, которые будет интересно почитать и вам.
Почему стоит выбрать навес от солнца на даче именно у нас?
Проверенные сайты Даркнета – Список сайтов Даркнета, Onion сайты
Даркнет поисковик – Список сайтов Даркнета, Народный путеводитель Даркнета
Tipico Casino ist eine beliebte Plattform für Glücksspiele im Internet. Viele Spieler fragen sich, wie sie am besten gewinnen können. Hier sind einige Tipps, die Ihnen dabei helfen können, Ihre Gewinnchancen zu erhöhen.
Zunächst ist es wichtig, sich mit den verschiedenen Spielen vertraut zu machen, die im Tipico Casino angeboten werden. Jedes Spiel hat seine eigenen Regeln und Strategien, die es zu beachten gilt. Machen Sie sich daher vorab mit den Spielregeln vertraut, um Ihre Gewinnchancen zu optimieren.
Ein weiterer wichtiger Tipp ist, ein Budget festzulegen und sich strikt daran zu halten. Es ist wichtig, verantwortungsbewusst zu spielen und nicht mehr Geld zu setzen, als man bereit ist zu verlieren. Setzen Sie sich daher klare Limits und halten Sie sich daran, um finanzielle Verluste zu vermeiden.
Außerdem ist es ratsam, regelmäßig an Aktionen und Bonusangeboten teilzunehmen. Das Tipico Casino bietet regelmäßig attraktive Boni und Promotionen an, die Ihre Gewinnchancen erhöhen können. Nutzen Sie diese Angebote daher aus, um zusätzliches Geld zu gewinnen.
Ein weiterer wichtiger Tipp ist, Geduld und Ausdauer zu haben. Glücksspiele sind ein Spiel des Zufalls, und es ist wichtig, nicht zu schnell frustriert zu sein, wenn es einmal nicht so läuft, wie man es sich erhofft hat. Bleiben Sie gelassen und behalten Sie einen kühlen Kopf, um langfristig erfolgreich zu sein.
AbschlieГџend ist es wichtig, sich immer bewusst zu machen, dass GlГјcksspiele ein Unterhaltungsangebot sind und nicht als Einkommensquelle dienen sollten. Spielen Sie daher verantwortungsbewusst und genieГџen Sie das Spiel, ohne dabei den SpaГџ aus den Augen zu verlieren.
Insgesamt können diese Tipps dazu beitragen, Ihre Gewinnchancen im Tipico Casino zu erhöhen. Beachten Sie jedoch, dass Glücksspiele immer mit einem gewissen Risiko verbunden sind und es keine Garantie für einen Gewinn gibt. Spielen Sie daher verantwortungsbewusst und genießen Sie das Spiel. Viel Glück!
https://tipicocasino.one/
Zet Casino ist eine beliebte Online-GlГјcksspielplattform, die eine Vielzahl von Spielen und Funktionen fГјr Spieler auf der ganzen Welt bietet. Eines der bemerkenswertesten Merkmale dieses Casinos ist der Live-Chat-Support, der rund um die Uhr verfГјgbar ist, um Spielern bei ihren Fragen und Anliegen zu helfen.
Der Live-Chat von Zet Casino ermöglicht es Spielern, direkt mit einem Support-Mitarbeiter zu kommunizieren, ohne lange Wartezeiten am Telefon oder per E-Mail. Spieler können Fragen zum Casino, zu Ein- und Auszahlungen, zu Boni und Werbeaktionen oder zu technischen Problemen stellen und erhalten sofortige Antworten und Unterstützung.
Der Live-Chat von Zet Casino ist einfach und benutzerfreundlich gestaltet, sodass Spieler keine technischen Kenntnisse benГ¶tigen, um ihn zu nutzen. Alles, was sie tun mГјssen, ist auf die SchaltflГ¤che “Live-Chat” auf der Website zu klicken und ihren Namen sowie ihre E-Mail-Adresse einzugeben, um eine Verbindung mit einem Support-Mitarbeiter herzustellen.
Dank des Live-Chats von Zet Casino können Spieler schnell und effizient alle ihre Fragen klären und Probleme bei ihrer Spielerfahrung lösen. Dieser Service hat dazu beigetragen, dass Zet Casino zu einer der beliebtesten Glücksspielplattformen im Internet geworden ist.
Insgesamt war der Live-Chat von Zet Casino eine großartige Ergänzung zu den bereits umfangreichen Dienstleistungen und Funktionen, die das Casino anbietet. Spieler können sicher sein, dass sie jederzeit professionelle Unterstützung erhalten, wenn sie im Zet Casino spielen.
https://zetcasino.one/
Народный путеводитель Даркнета – Onion сайты, Народный путеводитель Даркнета
Considering how busy arizonawood.net most people are, cleaning services have become very popular.
With their help, you can load pallets news24time.net, boxes and large cargo onto the upper shelves of the racks, which increases the functional area of the warehouse by an order of magnitude.
Даркнет поисковик – Список сайтов Даркнета, Проверенные сайты Даркнета
Список Tor сайтов – Народный путеводитель Даркнета, Даркнет 2024
Широкий ассортимент автоматический навес по доступным ценам.
В нашем мире, где диплом является началом успешной карьеры в любой отрасли, многие стараются найти максимально быстрый и простой путь получения качественного образования. Факт наличия официального документа сложно переоценить. Ведь диплом открывает дверь перед любым человеком, желающим вступить в сообщество профессиональных специалистов или продолжить обучение в высшем учебном заведении.
Мы предлагаем оперативно получить этот важный документ. Вы имеете возможность заказать диплом нового или старого образца, что становится удачным решением для человека, который не смог закончить обучение или утратил документ. Каждый диплом изготавливается аккуратно, с особым вниманием ко всем деталям. В результате вы сможете получить полностью оригинальный документ.
Преимущество этого решения состоит не только в том, что вы быстро получите диплом. Весь процесс организовывается просто и легко, с профессиональной поддержкой. От выбора нужного образца документа до консультации по заполнению личной информации и доставки в любое место России — все находится под абсолютным контролем качественных мастеров.
Для всех, кто ищет максимально быстрый способ получения необходимого документа, наша компания готова предложить отличное решение. Купить диплом – это значит избежать долгого обучения и не теряя времени переходить к своим целям, будь то поступление в университет или старт карьеры.
http://3dcar.ru/phorum/forum_viewtopic.php?t=4429
https://medichat.ru/viewtopic.php?t=288
Наши рассчитать навес для авто – это ваш лучший выбор.
На сайте https://climat.best приобретите качественные, функциональные кондиционеры, сплит-системы, тепловые насосы, а также чиллеры. Вся продукция именитых, проверенных и надежных брендов, а потому техника прослужит долго без потери технических характеристик, возможностей. А если необходимо подобрать что-то определенное, то воспользуйтесь специальным поиском. Перед вами есть и самые популярные позиции, которые пользуются особенным спросом среди покупателей. В интернет-магазине вы отыщите как настенные, так и напольно-потолочные конструкции, кассетные.
Das “Boomerang Bet Casino” ist eines der aufregendsten und innovativsten Online-Casinos auf dem Markt. Mit einer breiten Auswahl an Spielen, groГџzГјgigen Boni und einer benutzerfreundlichen Website ist es kein Wunder, dass immer mehr Spieler auf der Suche nach einer neuen Spielumgebung diesem Casino eine Chance geben.
Das Boomerang Bet Casino bietet eine Vielzahl von Spielen, darunter Slots, Tischspiele, Live-Casino-Spiele und vieles mehr. Die Spiele werden von einigen der besten Entwickler der Branche bereitgestellt, darunter NetEnt, Microgaming und Evolution Gaming.
Ein weiterer Vorteil des Boomerang Bet Casinos sind die großzügigen Boni und Promotionen, die regelmäßig angeboten werden. Neue Spieler können sich über Willkommensboni freuen, während treue Spieler von regelmäßigen Sonderaktionen und VIP-Programmen profitieren können.
Die Website des Boomerang Bet Casinos ist leicht zu navigieren und bietet eine sichere und geschützte Umgebung für Spieler. Mit einer Vielzahl von Ein- und Auszahlungsoptionen können Spieler sicher sein, dass ihre Transaktionen sicher und geschützt sind.
Insgesamt ist das Boomerang Bet Casino eine ausgezeichnete Wahl fГјr Spieler, die nach einer aufregenden und vertrauenswГјrdigen Spielumgebung suchen. Mit einer breiten Auswahl an Spielen, groГџzГјgigen Boni und einer benutzerfreundlichen Website ist es definitiv einen Besuch wert. Probieren Sie es heute noch aus und erleben Sie den Nervenkitzel des Boomerang Bet Casinos!
https://boomerangcasino.one/
На сайте https://razrabotka.pro/ вы сможете заказать такую важную и полезную услугу, как разработка электроники. Кроме того, здесь можно заказать и создание электронных приборов, специализированного оборудования. Что касается стоимости, то она начинается от 100 000 рублей. Есть возможность заказать производство независимо от количества. Практикуется производство, разработка электроники, производство агрегатов по созданному проекту. Вся продукция производится с использованием инновационных технологий.
Зайдите на сайт https://prazdnik-skazka.com/ и вы сможете заказать выездные праздники для детей в Москве и области. Узнайте стоимость и услуги, которая предлагает компания, такие как: мастер классы, различные праздничные кейсы, авторские вечеринки в различных стилях и многое другое. Огромный опыт и отличная репутация позволят вам заказать праздник для детей от профессионалов!
Хотите купить товары для туризма? TrampClub предоставляет такую возможность! Здесь вы найдете: спальники, походную посуду, палатки, рюкзаки, коврики и другое. Гарантируем быструю доставку, доступные цены и отменное обслуживание. Ищете палатки трамп? Trampclub.ru – сайт, где у вас есть возможность посмотреть отзывы о магазине и условия оплаты. Предлагаем вам только качественную продукцию. У нас действуют скидки. Наша работа направлена на удовлетворение желаний и потребностей покупателей. Обращайтесь, мы всегда на связи.
Индексация ссылок на сайте в индексе ру
Zet Casino ist eine beliebte Online-Glücksspielplattform, die ihren Spielern eine Vielzahl von spannenden Spielen und großzügigen Boni bietet. Einer der aktuellen Angebote, die Spieler begeistert, sind die 30 Freispiele, die sie für ihre Anmeldung erhalten können.
Diese Freispiele sind eine großartige Möglichkeit für neue Spieler, das Casino kennenzulernen und einige der besten Spielautomaten auszuprobieren, ohne eigenes Geld riskieren zu müssen. Spieler können die Freispiele verwenden, um ihre Lieblingsspiele zu testen und möglicherweise sogar echtes Geld zu gewinnen.
Um die 30 Freispiele zu erhalten, müssen sich Spieler einfach auf der Zet Casino Website registrieren und ihr Konto verifizieren. Sobald dies abgeschlossen ist, werden die Freispiele automatisch gutgeschrieben und können sofort verwendet werden.
Es ist jedoch wichtig zu beachten, dass die Freispiele bestimmten Umsatzbedingungen unterliegen und eventuell an bestimmte Spielautomaten gebunden sind. Spieler sollten daher die Bonusbedingungen sorgfältig lesen, um sicherzustellen, dass sie die Freispiele optimal nutzen können.
Alles in allem sind die 30 Freispiele von Zet Casino eine großartige Möglichkeit für neue Spieler, das Casino auszuprobieren und die Chance zu haben, echtes Geld zu gewinnen, ohne eigenes Geld riskieren zu müssen. Also, worauf warten Sie noch? Melden Sie sich noch heute an und genießen Sie Ihre Freispiele bei Zet Casino!
https://zetcasino.one/
angliannews.com
Considering how busy most people are birminghamnews24.com, cleaning services have become very popular. There are several types of cleaning: daily, apartment cleaning after renovation, cleaning by zone and others.
В нашем обществе, где диплом – это начало успешной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Наличие официального документа трудно переоценить. Ведь именно диплом открывает двери перед любым человеком, желающим начать профессиональную деятельность или учиться в университете.
В данном контексте мы предлагаем очень быстро получить этот необходимый документ. Вы имеете возможность купить диплом, и это является выгодным решением для человека, который не смог завершить обучение, утратил документ или хочет исправить плохие оценки. Все дипломы производятся аккуратно, с особым вниманием ко всем элементам, чтобы в итоге получился продукт, 100% соответствующий оригиналу.
Преимущество подобного подхода заключается не только в том, что вы быстро получите свой диплом. Процесс организовывается удобно, с профессиональной поддержкой. Начиная от выбора подходящего образца до консультации по заполнению личной информации и доставки в любой регион страны — все под абсолютным контролем наших мастеров.
Таким образом, для тех, кто пытается найти быстрый и простой способ получения необходимого документа, наша услуга предлагает выгодное решение. Приобрести диплом – это значит избежать длительного обучения и сразу перейти к достижению личных целей, будь то поступление в университет или начало удачной карьеры.
http://3dcar.ru/phorum/forum_viewtopic.php?t=4423
http://passo.su/forums/index.php?showtopic=6429
Индексация ссылок на сайте vindexe.ru
Zet Casino ist eine Online-GlГјcksspielplattform, die in der Welt der Online-Casinos immer beliebter wird. Mit einer breiten Palette an Spielen und attraktiven Bonusangeboten zieht Zet Casino Spieler aus der ganzen Welt an. In diesem Artikel werden wir die Vor- und Nachteile dieses Casinos bewerten.
Vorteile:
1. Große Auswahl an Spielen: Zet Casino bietet eine Vielzahl von Spielen, darunter Spielautomaten, Tischspiele, Live-Casino-Spiele und mehr. Spieler können zwischen Hunderten von Spielen wählen und haben immer etwas Neues zu entdecken.
2. Attraktive Bonusangebote: Zet Casino bietet großzügige Boni für neue Spieler sowie regelmäßige Promotionen und Aktionen für bestehende Spieler. Diese Bonusangebote können die Gewinnchancen der Spieler erhöhen und das Spielerlebnis noch spannender machen.
3. Sichere Zahlungsmethoden: Zet Casino bietet eine Vielzahl von sicheren Zahlungsmethoden, darunter Kreditkarten, E-Wallets und Banküberweisungen. Spieler können sicher und bequem Ein- und Auszahlungen vornehmen, ohne sich Gedanken über die Sicherheit ihrer persönlichen Daten machen zu müssen.
Nachteile:
1. Einschränkungen in einigen Ländern: Zet Casino akzeptiert Spieler aus verschiedenen Ländern, aber es gibt einige Länder, in denen das Spielen auf der Plattform nicht erlaubt ist. Spieler sollten sicherstellen, dass sie die gesetzlichen Bestimmungen ihres Landes kennen, bevor sie sich bei Zet Casino anmelden.
2. Langsame Auszahlungszeiten: Einige Spieler haben berichtet, dass die Auszahlungszeiten bei Zet Casino länger sind als bei anderen Online-Casinos. Dies kann frustrierend sein, insbesondere für Spieler, die ihre Gewinne schnell erhalten möchten.
Insgesamt bietet Zet Casino eine unterhaltsame und sichere Spielumgebung mit einer Vielzahl von Spielen und attraktiven Bonusangeboten. Spieler können sicher sein, dass ihre persönlichen Daten geschützt sind und dass sie faire Gewinnchancen haben. Trotz einiger kleiner Nachteile ist Zet Casino definitiv einen Besuch wert.
Fazit:
Zet Casino ist ein solides Online-Casino mit einer breiten Spielauswahl und attraktiven Bonusangeboten. Spieler, die auf der Suche nach einer unterhaltsamen und sicheren Spielumgebung sind, werden bei Zet Casino sicherlich auf ihre Kosten kommen. Es lohnt sich, dieses Casino auszuprobieren und selbst zu entscheiden, ob es den eigenen AnsprГјchen entspricht.
https://zetcasino.one/
Здравствуйте! Ищете надежные и выгодные микрозаймы? На mikro-zaim-online.ru собраны лучшие предложения от проверенных МФО. Наши специалисты ежедневно анализируют рынок, чтобы предоставить вам актуальную информацию. Здесь вы найдете займы без отказа, круглосуточные займы и даже под 0%. Воспользуйтесь удобным сервисом для быстрого получения денег на карту. Все просто и прозрачно. Посетите наш сайт и выберите идеальный займ для себя!
Нужны деньги срочно и без отказов? mikro-zaim-online.ru предлагает вам идеальное решение! У нас есть список из более 20 микрофинансовых организаций, которые предоставляют новым заемщикам займы под 0% на срок до 30 дней. Заполнение заявки занимает не более 10 минут, и почти все получают одобрение без проверки кредитной истории. Наши эксперты отобрали самые надежные предложения для вас. Посетите mikro-zaim-online.ru и решите свои финансовые проблемы легко и быстро!
thecolumbianews.net
texas-news.com
Привет! Если срочно нужны деньги, заходите на mikro-zaim-online.ru. Мы предлагаем подборки лучших микрозаймов от надежных МФО. Наши эксперты работают для вас, чтобы вы могли выбрать займы с минимальными процентами, круглосуточные и без отказов. Ежедневно обновляемая информация позволит вам найти самые выгодные предложения. Быстро, удобно и надежно. Посетите mikro-zaim-online.ru и решите свои финансовые вопросы с легкостью!
Компания «Разработка электроники» предлагает клиентам полный комплекс профессиональных услуг. У нас можно сделать заказ на разработку электроники. Получите по телефону предварительную консультацию. Достаточный накопленный опыт дает возможность нам быстро включиться в проект. https://razrabotka.pro/ – сайт, где вы найдете осуществленные работы. Вы узнаете, как и кому, мы оказываем помощь. Также размещаем статьи, которые имеют отношение к изготовлению электроники и разработке. Свяжитесь с нами, будем рады обсудить детали вашего проекта.
Im Boomerang Casino gibt es eine aufregende neue Aktion für alle Spieler, die gerne kostenlose Spins ohne Einzahlung nutzen möchten. Mit den Boomerang Casino Free Spins No Deposit können Spieler ohne jegliche Geldeinzahlung an bestimmten Spielautomaten im Casino kostenlos spielen und dabei echte Gewinne erzielen.
Die Boomerang Casino Free Spins No Deposit sind eine großartige Möglichkeit für neue Spieler, das Casino kennenzulernen und gleichzeitig die Chance auf große Gewinne zu haben. Die kostenlosen Spins sind einfach zu erhalten, indem man sich im Boomerang Casino registriert und das entsprechende Angebot in Anspruch nimmt.
Mit den Boomerang Casino Free Spins No Deposit können Spieler ihre Lieblingsspielautomaten ausprobieren und neue Spiele entdecken, ohne dabei eigenes Geld setzen zu müssen. Die Gewinne aus den kostenlosen Spins können anschließend als Bonusguthaben genutzt werden, um weiterhin im Casino zu spielen und echtes Geld zu gewinnen.
Diese Aktion ist besonders attraktiv für Spieler, die gerne risikofrei spielen und trotzdem die Spannung und Unterhaltung eines Online-Casinos genießen möchten. Die Boomerang Casino Free Spins No Deposit bieten eine tolle Möglichkeit, um neue Spiele auszuprobieren und die eigenen Gewinnchancen zu erhöhen, ohne dabei finanzielle Risiken einzugehen.
Also, worauf warten Sie noch? Registrieren Sie sich jetzt im Boomerang Casino und nutzen Sie die Free Spins No Deposit, um Ihre Gewinnchancen zu steigern und jede Menge SpaГџ beim Spielen zu haben!
https://boomerangcasino.one/
Зайдите на сайт https://baracatmar.com/ и вы сможете заказать свежие морепродукты от Компании Баракат SEAFOOD в страны Евросоюза. Благодаря налаженной системе логистики, с момента вылова и до получения продуктов клиентами нашей компании проходит очень мало времени. Посетите сайт, ознакомьтесь с ассортиментом, условиями доставки и действующими акциями.
m3ga gl – mega sb даркнет, m3ga не работает
кракен – кракен, кракен
Нужны деньги срочно и без отказов? mikro-zaim-online.ru предлагает вам идеальное решение! У нас есть список из более 20 микрофинансовых организаций, которые предоставляют новым заемщикам займы под 0% на срок до 30 дней. Заполнение заявки занимает не более 10 минут, и почти все получают одобрение без проверки кредитной истории. Наши эксперты отобрали самые надежные предложения для вас. Посетите mikro-zaim-online.ru и решите свои финансовые проблемы легко и быстро!
На сайте https://t.me/mvavada ознакомьтесь с нужной, полезной информацией, которая касается уникального проекта «VAVADA». На официальном канале вы сможете ознакомиться со всей необходимой информацией. Здесь же представлены и актуальные промокоды, а также самые свежие и полезные новости, которые будут интересны всем, кто связан с игрой. Вавада предлагает ознакомиться с интересными, увлекательными играми, которые произведут на вас эффект. На этом канале, в первую очередь, появляются новости о таком заведении.
Роза Ветров – цветочная мастерская, которая предлагает вам приобрести роскошные цветы. Выбор большой, у нас вы найдете все то, что вам необходимо. Мы радуем приемлемыми ценами своих клиентов и качественно собранными шикарными букетами. Быстро реагируем на заявки и с удовольствием готовы помочь вам с выбором. Заинтересованы в предоставлении вам лучших впечатлений. Ищете купить цветы спб недорого с доставкой? Flowersspb.com – сайт, где можете заказать свежие цветы с оперативной доставкой. Уверены в том, что получатели будут в восторге от сюрприза. Обращайтесь, гарантируем отличное обслуживание!
kraken com ссылка – kraken onion ссылка, зеркало kraken
mega новая ссылка – как зайти на мега, mega sb новости
Zet Casino No Deposit Bonus Codes: Holen Sie sich kostenlose Boni ohne Einzahlung
Wenn Sie auf der Suche nach einem aufregenden Online-Casino-Erlebnis sind, dann sollten Sie unbedingt Zet Casino ausprobieren. Dieses beliebte Online-Casino bietet eine Vielzahl von Spielen, groГџzГјgigen Boni und aufregenden Aktionen, die sicherstellen, dass Sie jede Minute Ihres Besuchs genieГџen werden.
Eines der großartigen Angebote, die Zet Casino für seine Spieler bereithält, sind die No Deposit Bonus Codes. Diese speziellen Codes ermöglichen es Ihnen, kostenlose Boni zu erhalten, ohne dass Sie eine Einzahlung tätigen müssen. Das bedeutet, dass Sie die Spiele im Casino ausprobieren können, ohne Ihr eigenes Geld riskieren zu müssen.
Um einen No Deposit Bonus Code bei Zet Casino zu erhalten, müssen Sie sich einfach registrieren und ein Konto erstellen. Sobald Ihr Konto aktiviert ist, können Sie Ihre Bonus Codes im Kassenbereich eingeben, um Ihren kostenlosen Bonus zu erhalten. Diese Boni können in Form von Freispielen, Gratisguthaben oder anderen Belohnungen angeboten werden.
Die No Deposit Bonus Codes bei Zet Casino sind eine großartige Möglichkeit, das Casino kennenzulernen und einige seiner besten Spiele auszuprobieren, ohne Ihr eigenes Geld riskieren zu müssen. Also worauf warten Sie noch? Registrieren Sie sich noch heute bei Zet Casino und holen Sie sich Ihre kostenlosen Boni! Viel Glück und viel Spaß beim Spielen!
https://zetcasino.one/
blecksprut – blacksprut ссылка tor, blacksprut
Сегодня, когда диплом является началом удачной карьеры в любой сфере, многие ищут максимально быстрый путь получения качественного образования. Необходимость наличия официального документа переоценить невозможно. Ведь диплом открывает двери перед людьми, желающими вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
В данном контексте мы предлагаем оперативно получить этот необходимый документ. Вы сможете приобрести диплом, что становится выгодным решением для человека, который не смог закончить обучение, потерял документ или хочет исправить плохие оценки. Любой диплом изготавливается с особой тщательностью, вниманием к мельчайшим элементам. В итоге вы получите полностью оригинальный документ.
Преимущества такого подхода заключаются не только в том, что можно максимально быстро получить диплом. Процесс организован комфортно и легко, с нашей поддержкой. От выбора нужного образца до правильного заполнения личной информации и доставки в любое место страны — все находится под полным контролем качественных мастеров.
В результате, всем, кто хочет найти быстрый способ получить требуемый документ, наша услуга предлагает выгодное решение. Купить диплом – это значит избежать долгого процесса обучения и не теряя времени перейти к достижению личных целей: к поступлению в ВУЗ или к началу трудовой карьеры.
http://preceptor.flybb.ru/viewtopic.php?f=13&t=8725
https://boi.instgame.pro/forum/index.php?topic=24410.0
This offer is accompanied by photographs of hotels greenhousebali.com where tourists can be found. There is the exterior of the building, the interiors of the rooms, photos of the territory and individual objects.
A person can configure the system oknews360.com independently or contact an organization to use the feature, focusing on their tools.
Boomerang Casino – deutsche Lizenz für sicheres Spielvergnügen
Das Boomerang Casino ist eine beliebte Online-Spielplattform, die eine Vielzahl von Spielen und Unterhaltungsmöglichkeiten für Spieler aus der ganzen Welt bietet. Ob Slot-Spiele, Tischspiele oder Live Casino – hier kommt jeder auf seine Kosten.
Ein wichtiger Aspekt, der bei der Auswahl eines Online-Casinos zu berücksichtigen ist, ist die Lizenzierung. Die deutsche Lizenz des Boomerang Casinos garantiert den Spielern ein hohes Maß an Sicherheit und Fairness. Die strengen Richtlinien und Vorschriften, die mit einer deutschen Lizenzierung einhergehen, stellen sicher, dass das Casino regelmäßig überprüft und kontrolliert wird. Dies bietet den Spielern die Gewissheit, dass ihre persönlichen Daten und Transaktionen sicher sind und dass die Spiele fair und transparent ablaufen.
Darüber hinaus unterliegt das Boomerang Casino deutschen Gesetzen und Richtlinien für Online-Glücksspiele, was bedeutet, dass Spieler aus Deutschland legal und sicher auf der Plattform spielen können. Dies gibt den Spielern die Gewissheit, dass sie keine rechtlichen Konsequenzen zu befürchten haben und dass ihr Spielvergnügen in einem regulierten und geschützten Umfeld stattfindet.
Die deutsche Lizenz des Boomerang Casinos ist ein deutliches Zeichen dafür, dass es sich um ein seriöses und vertrauenswürdiges Online-Casino handelt. Spieler können sich also voll und ganz auf ihr Spiel konzentrieren und müssen sich keine Sorgen um die Sicherheit und Fairness machen. Mit einer Vielzahl von Spielmöglichkeiten und einem sicheren Spielumfeld ist das Boomerang Casino die ideale Wahl für alle, die auf der Suche nach Unterhaltung und Spaß sind.
https://boomerangcasino.one/
Канал проекта casino VAVADA рад видеть вас у себя! Здесь представлена самая актуальная информация. Проведите прекрасно время и забудьте обо всем, играя от качественного онлайн-казино Вавада в увлекательные слоты. Вас ждет невероятная графика и особая атмосфера. Ищете vavada? t.me/mvavada – популярный телеграмм-канал, где мы делимся секретами успеха и своими знаниями с вами. У нас вы отыщите выгодные бонусы, начните азартную игру уже сегодня, не откладывайте на завтра. Желаем вам достичь больших выигрышей!
Connecting handsets to communicate with people dallasrentapart.com. You need to consider what devices people will be using to contact support.
The vibrant energy of spring comes to life event-miami24.com against a backdrop of sun-drenched beaches and pulsating rhythms. This is the perfect time to provide everything Miami and Miami Beach hospitals have to offer.
Zet Casino ist ein Online-Casino, das bereits seit einiger Zeit auf dem Markt ist und eine Vielzahl von Spielen und Angeboten für die Spieler bereithält. In diesem Artikel möchten wir unsere Erfahrungen mit Zet Casino teilen und Ihnen einen Einblick geben, was Sie von diesem Anbieter erwarten können.
Zet Casino bietet eine breite Auswahl an Spielen von bekannten Anbietern wie NetEnt, Microgaming, Play’n GO, Yggdrasil und vielen mehr. Von Slots Гјber Tischspiele bis hin zu Live-Casino-Spielen ist fГјr jeden Geschmack etwas dabei. Die Spiele laufen reibungslos und die Grafiken sind hochwertig, was ein angenehmes Spielerlebnis garantiert.
Ein weiterer Pluspunkt von Zet Casino sind die großzügigen Boni und Aktionen für die Spieler. Neue Spieler erhalten einen Willkommensbonus, der aus einem Einzahlungsbonus und Freispielen besteht. Auch für bestehende Spieler gibt es regelmäßig Reload-Boni, Cashback-Angebote und Turniere, bei denen attraktive Preise winken.
Der Kundenservice von Zet Casino ist gut erreichbar und beantwortet Anfragen schnell und kompetent. Es stehen verschiedene Kontaktmöglichkeiten wie Live-Chat, E-Mail und Telefon zur Verfügung. Wir haben positive Erfahrungen gemacht und fühlten uns gut betreut.
Ein kleiner Kritikpunkt sind die Umsatzbedingungen der Boni, die etwas hoch angesetzt sind. Es erfordert daher etwas Geduld und Glück, um die Bonusbedingungen zu erfüllen und Gewinne auszahlen zu können. Dennoch überwiegen die positiven Aspekte von Zet Casino, sodass wir den Anbieter empfehlen können.
Insgesamt waren unsere Erfahrungen mit Zet Casino sehr positiv. Das breite Spielangebot, die groГџzГјgigen Boni und der gute Kundenservice machen diesen Anbieter zu einer guten Wahl fГјr Casino-Liebhaber. Probieren Sie es aus und Гјberzeugen Sie sich selbst von Zet Casino!
https://zetcasino.one/
На сайте https://agrotechelit.ru/ закажите звонок для того, чтобы проконсультироваться по поводу покупки оборудования для теплиц, а также парников с оперативной доставкой по России. Предприятие специализируется на производстве, реализации тепличного оборудования, а также различных необходимых комплектующих. В компании получится заказать огромный ассортимент продукции, в том числе, системы отопления, полива, огромный выбор пленок, укрытий. Здесь же вы найдете и расходные материалы, необходимые для сервиса теплиц.
На сайте https://iseer.kz/ получите консультацию по поводу разработки и покупки уникальных и инновационных рекламных LED-решений, которые созданы для бизнеса, архитектуры. Для того чтобы осуществить точные расчеты, необходимо позвонить консультанту. Он расскажет обо всем, что необходимо. Прямо сейчас закажите наружную рекламу, видео-буквы, архитектурные подсветки, индивидуальный уникальный проект. В компании трудятся компетентные, квалифицированные сотрудники. У них огромный опыт в данной области.
Хотите выглядеть свежо и молодо? Процедура Premium Face вам в этом поможет! Она поможет избавиться от носогубных складок, морщин и сделать кожу более подтянутой. Результат от инъекций филлеров Pluryal заметен сразу после сеанса, а эффект сохраняется на длительное время. Ищете эстетическая коррекция лица: какие процедуры выбрать? Premiumface.ru – сайт, где вы узнаете больше полезной информации о процедуре Premium Face. Также вы в любое время сможете подать на сотрудничество заявку. Наслаждайтесь собственным отражением в зеркале и радуйте окружающих своим внешним видом!
Сегодня, когда диплом становится началом удачной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Наличие официального документа переоценить просто невозможно. Ведь диплом открывает дверь перед каждым человеком, желающим вступить в профессиональное сообщество или учиться в ВУЗе.
Мы предлагаем максимально быстро получить этот важный документ. Вы имеете возможность приобрести диплом нового или старого образца, и это является удачным решением для человека, который не смог закончить обучение или утратил документ. Каждый диплом изготавливается аккуратно, с особым вниманием ко всем элементам. В результате вы сможете получить 100% оригинальный документ.
Превосходство такого решения состоит не только в том, что вы сможете оперативно получить свой диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. Начав от выбора подходящего образца до консультации по заполнению персональных данных и доставки по стране — все находится под полным контролем опытных специалистов.
Для всех, кто ищет оперативный способ получения необходимого документа, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://chelny.ixbb.ru/viewtopic.php?id=397
http://passo.su/forums/index.php?showtopic=6431
Ein Casino Bonus ist eine fantastische Möglichkeit, um das eigene Guthaben aufzustocken und mehr Spaß beim Spielen zu haben. Einer der Anbieter, der regelmäßig großzügige Boni vergibt, ist Tipico.
Bei Tipico gibt es verschiedene Arten von Boni, die sowohl Neukunden als auch Bestandskunden zur Verfügung stehen. Einer der beliebtesten Boni ist der Willkommensbonus für neue Kunden. Dieser Bonus bietet die Möglichkeit, das eingezahlte Guthaben zu verdoppeln und somit mit einem deutlich höheren Betrag im Casino zu spielen.
Um den Willkommensbonus zu erhalten, müssen neue Kunden sich lediglich registrieren und eine Einzahlung tätigen. Der Bonus wird dann automatisch gutgeschrieben und kann sofort für das Spielen genutzt werden.
Auch Bestandskunden werden bei Tipico regelmäßig mit verschiedenen Aktionen belohnt. So gibt es beispielsweise regelmäßige Reload-Boni, bei denen die Einzahlung nochmals aufgestockt wird. Zudem können Kunden von Cashback-Aktionen profitieren, bei denen ein Teil des verlorenen Einsatzes zurückerstattet wird.
Um von den verschiedenen Boni bei Tipico zu profitieren, sollten Kunden regelmäßig die Promotion-Seite auf der Webseite besuchen und sich über aktuelle Angebote informieren. Zudem lohnt es sich, den Newsletter zu abonnieren, um keine Aktion zu verpassen.
Insgesamt bietet Tipico seinen Kunden eine Vielzahl an attraktiven Bonusangeboten, die das Spielerlebnis im Casino noch spannender machen. Wer also gerne im Casino spielt, sollte sich die verschiedenen Boni bei Tipico genauer anschauen und sich die Chance auf zusätzliches Guthaben nicht entgehen lassen.
https://tipicocasino.one/
Ночью понадобились деньги на оплату срочной доставки. Нашел телеграм-канал новые и малоизвестные МФО 2024, где представлена подборка малоизвестных МФО 2024 года, работающих круглосуточно и выдающих займы даже с плохой кредитной историей. Оформил заявку и моментально получил деньги на карту. Благодаря этому смог вовремя оплатить доставку. Рекомендую этот канал всем, кто ищет быстрый займ в любое время суток!
Недавно разбил смартфон, а деньги на ремонт срочно нужны были. На телеграм-канале новые и малоизвестные МФО 2024 нашел новые МФО, которые дают займы без проблем и круглосуточно. Оказалось, что для новых клиентов есть акции под 0%. Оформил заявку и быстро получил деньги. Канал предлагает много полезной информации про займы. Рекомендую всем, кто ищет быстрый и выгодный займ!
chinaone.net
repairdesign24.com
Решил сделать родителям сюрприз, но не хватало средств. Нашел телеграм-канал новые и малоизвестные МФО 2024, где выкладывают новые МФО. Займ получил быстро и без проблем. Особенно понравилось, что для новых клиентов есть акции под 0%. В канале много полезной информации про займы. Очень доволен, рекомендую всем, кто ищет быстрый и удобный займ!
Zet Casino Bonus Code ohne Einzahlung
Online Casinos erfreuen sich immer größerer Beliebtheit, nicht zuletzt aufgrund der vielfältigen Bonusangebote, die sie ihren Spielern bieten. Ein besonders attraktives Angebot ist der Zet Casino Bonus Code ohne Einzahlung.
Was genau verbirgt sich hinter diesem Angebot? Ganz einfach: Spieler können sich bei Zet Casino registrieren und erhalten einen Bonus ohne vorherige Einzahlung. Dieser Bonus kann in Form von Freispielen, Bonusgeld oder anderen Vergünstigungen angeboten werden. Dadurch haben Spieler die Möglichkeit, das Casino und die angebotenen Spiele risikofrei kennenzulernen, ohne dabei ihr eigenes Geld einzusetzen.
Der Zet Casino Bonus Code ohne Einzahlung bietet somit eine ideale Möglichkeit, um sich von den Vorzügen des Casinos zu überzeugen, ohne dabei ein finanzielles Risiko einzugehen. Spieler haben die Chance, die verschiedenen Spiele auszuprobieren, sich mit dem Casino vertraut zu machen und erste Gewinne zu erzielen, ohne dafür eigenes Geld einzahlen zu müssen.
Um den Zet Casino Bonus Code ohne Einzahlung zu erhalten, müssen Spieler lediglich einen entsprechenden Bonuscode bei der Registrierung eingeben. Dieser wird in der Regel auf der Website des Casinos veröffentlicht oder per E-Mail an registrierte Spieler versendet. Nach der Eingabe des Bonuscodes wird der Bonus automatisch auf das Spielerkonto gutgeschrieben und kann sofort verwendet werden.
Es ist jedoch wichtig zu beachten, dass auch bei einem Bonus ohne Einzahlung bestimmte Umsatzbedingungen gelten können. Diese legen fest, wie oft der Bonus umgesetzt werden muss, bevor eine Auszahlung möglich ist. Es ist daher ratsam, die Bonusbedingungen genau zu lesen, bevor man sich für einen Bonus ohne Einzahlung entscheidet.
Insgesamt bietet der Zet Casino Bonus Code ohne Einzahlung eine attraktive Möglichkeit, um das Casino risikofrei kennenzulernen und erste Gewinne zu erzielen. Spieler sollten jedoch darauf achten, die Bonusbedingungen zu beachten und verantwortungsvoll mit dem Angebot umzugehen. Wer diese Tipps beherzigt, kann von den Vorzügen des Zet Casino Bonus Codes ohne Einzahlung profitieren und seine Gewinnchancen deutlich erhöhen.
https://zetcasino.one/
В нашем мире, где диплом становится началом отличной карьеры в любой области, многие стараются найти максимально быстрый и простой путь получения качественного образования. Наличие документа об образовании трудно переоценить. Ведь диплом открывает двери перед каждым человеком, который стремится начать профессиональную деятельность или учиться в любом ВУЗе.
В данном контексте наша компания предлагает оперативно получить любой необходимый документ. Вы можете купить диплом нового или старого образца, и это становится выгодным решением для всех, кто не смог завершить образование или утратил документ. диплом изготавливается аккуратно, с особым вниманием ко всем нюансам. В результате вы сможете получить полностью оригинальный документ.
Преимущество этого решения заключается не только в том, что можно максимально быстро получить свой диплом. Весь процесс организовывается просто и легко, с нашей поддержкой. Начиная от выбора нужного образца до консультации по заполнению персональной информации и доставки по стране — все под полным контролем квалифицированных мастеров.
Всем, кто ищет оперативный способ получения требуемого документа, наша услуга предлагает выгодное решение. Заказать диплом – это значит избежать длительного обучения и сразу переходить к достижению личных целей, будь то поступление в университет или старт профессиональной карьеры.
http://www.8arusak-diploms24.com/
Посетите https://intercalendar.ru и вы сможете заказать печать и изготовление календарей в типографии по отличным ценам. Ознакомьтесь с каталогом услуг, стоимостью изготовления продукции, а заказ можно сделать буквально в 1 клик. Качественные услуги по привлекательным ценам от профессионалов у нас на сайте.
Tipico Casino iPad
Das Tipico Casino bietet seinen Kunden ein erstklassiges Spielerlebnis, das nun auch bequem auf dem iPad genossen werden kann. Mit der speziell für das iPad optimierten App können die Spieler auf eine Vielzahl von Casino-Spielen zugreifen, darunter Slots, Roulette, Blackjack und vieles mehr.
Die Benutzeroberfläche der Tipico Casino iPad App ist benutzerfreundlich gestaltet und sorgt für ein einfaches und nahtloses Spielerlebnis. Die Spiele sind grafisch ansprechend gestaltet und bieten eine hohe Qualität, so dass die Spieler ein authentisches Casino-Erlebnis genießen können, egal wo sie sich befinden.
Durch die Verwendung der Tipico Casino iPad App haben die Spieler die MГ¶glichkeit, ihre Lieblingsspiele auch unterwegs zu spielen und kГ¶nnen somit jederzeit und Гјberall auf ihre Casino-Unterhaltung zugreifen. Egal ob man auf dem Weg zur Arbeit ist, in der Mittagspause oder gemГјtlich auf der Couch zu Hause – mit der Tipico Casino iPad App ist das Casino-Erlebnis immer griffbereit.
Darüber hinaus bietet das Tipico Casino seinen Spielern regelmäßig attraktive Boni und Aktionen, die das Spielerlebnis noch aufregender und lukrativer machen. Mit der Tipico Casino iPad App können die Spieler somit nicht nur hochwertige Casino-Spiele genießen, sondern auch von exklusiven Angeboten profitieren.
Insgesamt ist die Tipico Casino iPad App eine großartige Möglichkeit für Casino-Liebhaber, ihre Lieblingsspiele bequem und mobil zu spielen. Mit einer benutzerfreundlichen Benutzeroberfläche, einer Vielzahl von hochwertigen Spielen und attraktiven Boni ist die App eine perfekte Ergänzung für alle, die gerne unterwegs spielen möchten. Probieren Sie die Tipico Casino iPad App noch heute aus und lassen Sie sich von einem erstklassigen Casino-Erlebnis überzeugen.
https://tipicocasino.one/
Решил записаться на курсы вождения, а денег не хватало. На телеграм-канале новые и малоизвестные МФО 2024 нашел более 20 малоизвестных МФО, где можно получить быстрый онлайн-займ. Понравилось, что займы дают всем от 18 лет, даже с плохой кредитной историей. Оформил заявку и получил деньги на карту за несколько минут. Теперь я могу начать учиться вождению. Рекомендую всем, кто ищет быстрый займ!
В нашем обществе, где диплом становится началом удачной карьеры в любой сфере, многие пытаются найти максимально простой путь получения качественного образования. Наличие документа об образовании трудно переоценить. Ведь диплом открывает двери перед каждым человеком, который собирается вступить в профессиональное сообщество или учиться в ВУЗе.
Наша компания предлагает быстро получить любой необходимый документ. Вы сможете приобрести диплом, и это будет отличным решением для человека, который не смог закончить обучение или потерял документ. Все дипломы производятся с особой аккуратностью, вниманием к мельчайшим нюансам. В результате вы получите 100% оригинальный документ.
Плюсы подобного подхода состоят не только в том, что можно быстро получить диплом. Процесс организован комфортно и легко, с нашей поддержкой. От выбора подходящего образца до грамотного заполнения персональных данных и доставки по России — все под абсолютным контролем качественных специалистов.
Всем, кто ищет оперативный способ получить требуемый документ, наша компания готова предложить выгодное решение. Купить диплом – это значит избежать длительного процесса обучения и сразу переходить к личным целям, будь то поступление в университет или старт профессиональной карьеры.
http://eliztrans.9bb.ru/viewtopic.php?id=116
https://vulf.1bb.ru/viewtopic.php?id=289
Digital Agency Империя старается качественно реализовывать для вас свои услуги. Наша команда состоит из квалифицированных сотрудников, знающих секреты удачного продвижения сайтов и постоянно развивающихся. Самое главное то, что они работают честно. https://imperiasinteza.com – здесь указаны цены на услуги, ознакомиться с ними можете в удобное для вас время. Мы прикладываем максимум усилий, чтобы клиент остался всем, доволен и приходил к нам снова. Позвоните нам уже сейчас, готовы помочь вашему бизнесу достичь успеха в онлайн-мире!
KRAKEN ссылка зеркало – КРАКЕН как зайти, KRAKEN официальный сайт
На сайте https://webasyst.pro закажите профессиональную, качественную оптимизацию сайтов, интернет-магазинов. Все работы происходят на профессиональном уровне, максимально быстро, качественно, в соответствии с требованиями клиентов. Эффективность работы вашего магазина будет увеличена в несколько раз. Если вас не устроит результат или не увидите прогресса, то средства будут возвращены. Над каждым проектом трудятся лучшие специалисты, которые действительно работают на совесть.
[url=https://kraken12.co.at]kraken11[/url] – kraken darknet, kraken darknet
Ищите тяговые батареи для вилочных погрузчиков и штабелеров? Зайдите на https://www.tyumen-bat.ru/ и вы найдете тяговые батареи Тюменского аккумуляторного завода в огромном ассортименте по лучшим ценам, с доставкой. Батарее для любого вида и типа погрузчика или штабелера по выгодным ценам у нас.
Tipico – Geld von Casino auf Sportwetten
Tipico ist eine der beliebtesten Sportwetten-Plattformen in Deutschland. Neben Sportwetten bietet das Unternehmen auch ein Online-Casino an, in dem Spieler ihr Glück an Spielautomaten, Roulette und anderen Casino-Spielen versuchen können.
Eine häufige Frage, die Spieler haben, ist, ob sie Geld von ihrem Casino-Konto auf ihr Sportwetten-Konto übertragen können. Die gute Nachricht ist, dass dies bei Tipico möglich ist. Spieler können ganz einfach Geld von ihrem Casino-Konto auf ihr Sportwetten-Konto transferieren, um ihre Lieblings-Sportwetten zu platzieren.
Um Geld von Ihrem Casino-Konto auf Ihr Sportwetten-Konto zu Гјbertragen, mГјssen Sie sich zunГ¤chst auf der Tipico-Website oder in der Tipico-App einloggen. Gehen Sie dann zu Ihrem Casino-Konto und wГ¤hlen Sie die Option “Geld transferieren”. Geben Sie den Betrag ein, den Sie auf Ihr Sportwetten-Konto Гјbertragen mГ¶chten, und bestГ¤tigen Sie die Transaktion.
Es ist wichtig zu beachten, dass möglicherweise bestimmte Bedingungen für die Übertragung von Geld zwischen den verschiedenen Konten gelten können. Stellen Sie sicher, dass Sie die Nutzungsbedingungen von Tipico lesen, um sicherzustellen, dass Sie alle Regeln und Bestimmungen einhalten.
Insgesamt bietet Tipico seinen Spielern eine bequeme und benutzerfreundliche Möglichkeit, Geld zwischen Casino- und Sportwetten-Konten zu transferieren. So können Spieler leicht zwischen verschiedenen Glücksspielangeboten wechseln und ihr Spielerlebnis maximieren.
Ob Sie Ihre Lieblingssportart live verfolgen oder lieber an Spielautomaten spielen, bei Tipico finden Sie sicherlich das passende Angebot. Nutzen Sie die Möglichkeit, Geld von Ihrem Casino-Konto auf Ihr Sportwetten-Konto zu übertragen und genießen Sie die Vielfalt an Glücksspielmöglichkeiten, die Tipico zu bieten hat. Viel Glück beim Wetten!
https://tipicocasino.one/
mega sb вход не через тор – mega onion, mega tor
Destruam предоставляет для вас большой выбор сериалов. Все они уже с первых минут захватывают. Пригласите своих друзей, соберитесь с близкими и в полной мере наслаждайтесь новинками кино. Гарантируем отменный звук и оперативную загрузку видео. Ищете кровь и кость фильм 2009 смотреть онлайн ? Destruam.xyz – известный портал, где представлены сериалы, которые увлекут сюжетными поворотами и неожиданными событиями. Качество и разнообразие контента на высочайшем уровне. Смотрите без утомительной процедуры регистрации интересные сериалы. Сделайте свой вечер веселым!
https blacksprut – blacksprut +не работае, ссылка на блекспрут
Интернет-магазин «Body-pit» предлагает вам купить спортивное питание по доступным ценам от популярных производителей. Мы готовы оказать вам квалифицированную помощь в подборе нужного товара. Вы останетесь довольны магазином и обслуживанием. https://ufa2.body-pit.ru/ – сайт, где можете прямо сейчас ознакомиться с условиями оплаты. Осуществляем оперативную доставку спортпита и стремимся обеспечить своих клиентов лучшим сервисом. Качество спортивного питания нашего онлайн-магазина на высоте. Обращайтесь к нам и не пожалеете!
m3ga точка gl – тор mega555net, m3ga точка gl
Tipico Casino bietet seinen Spielern eine Vielzahl von Spielen an, aus denen sie wählen können. Von klassischen Tischspielen wie Roulette und Blackjack bis hin zu aufregenden Spielautomaten und Live-Casino-Spielen ist für jeden Geschmack etwas dabei. Doch welche Spiele sind die besten bei Tipico Casino?
Ein beliebtes Spiel bei Tipico Casino ist sicherlich das Roulette. Dieses klassische Casinospiel bietet Spannung und Nervenkitzel, während man darauf hofft, dass die Kugel auf der richtigen Zahl landet. Mit verschiedenen Varianten wie Europe Roulette oder French Roulette bietet Tipico Casino seinen Spielern eine Vielzahl von Möglichkeiten, dieses beliebte Spiel zu genießen.
Auch Blackjack ist ein Favorit bei Tipico Casino. Bei diesem Kartenspiel geht es darum, den Dealer zu schlagen, indem man eine Hand mit einem Kartenwert näher an 21 hat, ohne darüber zu kommen. Mit verschiedenen Varianten wie Classic Blackjack oder Blackjack VIP können Spieler ihre Fähigkeiten und Strategien testen und hoffentlich große Gewinne erzielen.
FГјr Fans von Spielautomaten gibt es bei Tipico Casino eine groГџe Auswahl an aufregenden Spielen. Von klassischen FrГјchteslots bis hin zu aufwendig gestalteten Video-Slots mit spannenden Bonusrunden und Jackpots ist fГјr jeden Geschmack etwas dabei. Beliebte Spielautomaten bei Tipico Casino sind zum Beispiel Starburst, Book of Dead oder Mega Moolah.
Auch im Live-Casino von Tipico können Spieler ein authentisches Casino-Erlebnis genießen. Mit Live-Dealern, die die Spiele leiten und via Video-Stream übertragen werden, können Spieler Roulette, Blackjack, Baccarat und mehr in Echtzeit spielen und interagieren. Die Spannung und Atmosphäre eines echten Casinos werden so direkt ins Wohnzimmer gebracht.
Insgesamt bietet Tipico Casino eine breite Auswahl an Spielen fГјr jeden Geschmack und jedes Budget. Ob Tischspiele, Spielautomaten oder Live-Casino-Spiele – hier kommt jeder auf seine Kosten. Welches Spiel letztendlich das beste ist, kommt ganz auf die persГ¶nlichen Vorlieben und Strategien des Spielers an. Eines ist jedoch sicher: Spannung und Unterhaltung sind bei Tipico Casino garantiert. Viel SpaГџ beim Spielen!
https://tipicocasino.one/
В современном мире, где диплом является началом успешной карьеры в любой области, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа переоценить попросту невозможно. Ведь именно диплом открывает двери перед всеми, кто стремится начать профессиональную деятельность или учиться в университете.
В данном контексте мы предлагаем очень быстро получить любой необходимый документ. Вы имеете возможность купить диплом нового или старого образца, что будет отличным решением для человека, который не смог закончить образование, потерял документ или хочет исправить свои оценки. дипломы изготавливаются с особой тщательностью, вниманием к мельчайшим нюансам. В результате вы получите полностью оригинальный документ.
Преимущество подобного подхода состоит не только в том, что можно оперативно получить диплом. Процесс организовывается удобно, с профессиональной поддержкой. Начав от выбора подходящего образца диплома до консультации по заполнению персональной информации и доставки в любой регион страны — все будет находиться под абсолютным контролем качественных мастеров.
Всем, кто ищет быстрый способ получить требуемый документ, наша услуга предлагает выгодное решение. Приобрести диплом – это значит избежать длительного процесса обучения и не теряя времени перейти к своим целям, будь то поступление в ВУЗ или начало удачной карьеры.
http://www.5gruppa365-diploms.com/
В нашем обществе, где диплом – это начало удачной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Важность наличия официального документа об образовании сложно переоценить. Ведь диплом открывает дверь перед всеми, кто стремится вступить в сообщество профессиональных специалистов или продолжить обучение в любом университете.
Мы предлагаем быстро получить любой необходимый документ. Вы сможете купить диплом старого или нового образца, и это становится отличным решением для человека, который не смог завершить обучение, утратил документ или желает исправить плохие оценки. Все дипломы производятся с особой аккуратностью, вниманием ко всем нюансам, чтобы в результате получился продукт, максимально соответствующий оригиналу.
Плюсы этого решения состоят не только в том, что можно оперативно получить диплом. Процесс организовывается комфортно, с нашей поддержкой. От выбора необходимого образца документа до консультации по заполнению персональной информации и доставки в любое место страны — все под абсолютным контролем наших специалистов.
В результате, для всех, кто пытается найти оперативный способ получения необходимого документа, наша компания готова предложить отличное решение. Заказать диплом – значит избежать долгого процесса обучения и сразу переходить к достижению личных целей, будь то поступление в ВУЗ или начало карьеры.
https://smd.mybb.ru/viewtopic.php?id=2872
http://forumcar.mybb.ru/viewtopic.php?id=71
Хотите получить деньги быстро и без лишних вопросов? На mikro-zaim-online.ru вас ждет более 20 микрофинансовых организаций, которые предлагают новым заемщикам займы под 0% на срок до 30 дней. Оформление занимает всего 10 минут, а шансы на одобрение почти стопроцентные, даже без проверки кредитной истории. Наши специалисты отобрали самые надежные МФО, чтобы вы могли получить займ легко и без отказов. Зайдите на mikro-zaim-online.ru и убедитесь, что получить деньги стало проще, чем когда-либо!
Tipico Casino down: Spieler verärgert über Ausfall
Das Tipico Casino ist bei vielen Spielern beliebt, doch in letzter Zeit häufen sich die Beschwerden über Ausfälle und Störungen der Plattform. Viele Spieler berichten davon, dass sie sich nicht mehr in ihren Accounts einloggen können oder dass die Spiele einfach nicht laden. Dies sorgt für großen Frust bei den Nutzern, besonders wenn sie gerade in einer spannenden Spielrunde sind.
Die Gründe für die Ausfälle sind bisher nicht bekannt, doch die Spieler äußern ihren Unmut über die mangelnde Kommunikation seitens des Casinos. Viele fühlen sich im Stich gelassen und wünschen sich eine schnellere Lösung des Problems. Einige Nutzer haben sogar bereits angekündigt, das Tipico Casino zu verlassen und sich nach einer anderen Plattform umzusehen.
Es ist zu hoffen, dass das Tipico Casino schnellstmöglich das Problem behebt und den Spielern eine reibungslose und unterbrechungsfreie Spielerfahrung bietet. Denn nur so kann das Casino seine treuen Kunden behalten und neue Spieler anlocken. Es bleibt abzuwarten, wie das Casino auf die Kritik reagieren wird und ob es gelingt, das Vertrauen der Spieler zurückzugewinnen.
https://tipicocasino.one/
Решил сделать родителям сюрприз, но не хватало средств. Нашел телеграм-канал новые и малоизвестные МФО 2024, где выкладывают новые МФО. Займ получил быстро и без проблем. Особенно понравилось, что для новых клиентов есть акции под 0%. В канале много полезной информации про займы. Очень доволен, рекомендую всем, кто ищет быстрый и удобный займ!
https://1skupkauto.ru/
На сайте https://hyips-money.ru/ ознакомьтесь с инвестиционными проектами, рекомендациями, которые помогут заработать неплохие средства. Этот сервис регулярно мониторит те проекты, которые действительно приносят прибыль, где вас точно не обманут, а деньги выплатят быстро и без обмана. Здесь получится отыскать всю необходимую информацию относительно инвестиционных проектов. Изучите полный список хайп-проектов, которые будут полезны и вам. Регулярно проверяется платежеспособность, чтобы исключить возможные денежные потери.
In den letzten Jahren hat sich Cashback zu einer Г¤uГџerst beliebten Art des Bonusangebots in Online-Casinos entwickelt. Eine der Plattformen, die dieses Angebot anbietet, ist das Zet Casino.
Bei Zet Casino können Spieler eine Vielzahl von Cashback-Angeboten nutzen, um einen Teil ihrer Verluste zurückzuerobern. Dies bedeutet, dass Spieler, selbst wenn sie nicht im Glück sind und Verluste erleiden, einen Teil ihres Einsatzes zurückerhalten können. Dies ist besonders attraktiv für Spieler, die gerne länger spielen möchten, ohne ständig Geld nachzuschießen.
Das Cashback-Angebot von Zet Casino funktioniert in der Regel auf wöchentlicher Basis und richtet sich nach dem nettoverlust eines Spielers in dieser Woche. Je nach Spielverhalten und Einsätzen kann der Cashback-Betrag variieren, sodass Spieler mit höheren Einsätzen einen höheren Cashback-Betrag erhalten können.
Das Cashback-Angebot von Zet Casino ist eine großartige Möglichkeit für Spieler, ihr Spiel zu verlängern und Verluste wieder zurückzugewinnen. Es ist jedoch wichtig zu beachten, dass Cashback nicht immer in Echtgeld ausgezahlt wird, sondern oft als Bonusguthaben gutgeschrieben wird, das vor der Auszahlung bestimmte Bedingungen erfüllen muss.
Insgesamt ist das Cashback-Angebot von Zet Casino eine attraktive Möglichkeit für Spieler, mehr aus ihrem Spiel herauszuholen und länger Spaß zu haben. Wenn Sie also nach einem Online-Casino suchen, das Cashback anbietet, sollten Sie auf jeden Fall Zet Casino in Betracht ziehen.
https://zetcasino.one/
If the request is not registered properly chinanews777.com, they will load specialists in a chaotic manner. Tickets help to avoid such problems, because all operations will be carried out in a single IT system.
invest-company.net
Відвідайте сайт https://i4car.net/ який є автомобільним порталом з цікавими новинами. Автоновини, все про автомобілі, тест драйви, поради досвідчених автолюбителів та багато іншого. Кожен знайде для себе корисне та цікаве.
В нашем мире, где диплом является началом удачной карьеры в любой сфере, многие ищут максимально быстрый путь получения образования. Факт наличия официального документа об образовании сложно переоценить. Ведь диплом открывает дверь перед каждым человеком, который собирается начать профессиональную деятельность или продолжить обучение в высшем учебном заведении.
В данном контексте мы предлагаем максимально быстро получить этот важный документ. Вы можете заказать диплом нового или старого образца, что становится отличным решением для всех, кто не смог завершить образование, потерял документ или хочет исправить плохие оценки. Каждый диплом изготавливается аккуратно, с особым вниманием ко всем элементам. В результате вы сможете получить документ, 100% соответствующий оригиналу.
Превосходство подобного решения состоит не только в том, что можно оперативно получить диплом. Весь процесс организован комфортно, с профессиональной поддержкой. Начав от выбора подходящего образца диплома до точного заполнения личной информации и доставки по России — все под полным контролем квалифицированных специалистов.
Всем, кто хочет найти быстрый способ получения необходимого документа, наша услуга предлагает выгодное решение. Приобрести диплом – это значит избежать продолжительного обучения и сразу перейти к достижению собственных целей, будь то поступление в ВУЗ или старт удачной карьеры.
http://kondrateff.5bb.ru/viewtopic.php?id=6105
https://safipoodle.mybb.ru/viewtopic.php?id=263
Наш канал предлагает уникальную возможность получить займ от новых МФО 2024 года. Новые МФО 2024 предоставляют займы с минимальными требованиями – нужен только паспорт и банковская карта. Подпишитесь и будьте в курсе всех новинок!
Boomerang Casino App – das neue Spielerlebnis fГјr unterwegs
Immer mehr Menschen nutzen heutzutage ihre mobilen Endgeräte, um online zu spielen. Dafür gibt es eine Vielzahl von Apps, die es ermöglichen, jederzeit und überall auf beliebte Casino-Spiele zuzugreifen. Eine dieser Apps ist die Boomerang Casino App, die ein besonderes Spielerlebnis bietet.
Die Boomerang Casino App wurde von erfahrenen Entwicklern konzipiert und bietet eine breite Auswahl an Spielautomaten, Tischspielen und Live-Casino-Spielen. Durch die benutzerfreundliche Oberfläche ist es einfach, sich in der App zurechtzufinden und die Lieblingsspiele zu spielen.
Ein besonderes Feature der Boomerang Casino App ist das Belohnungssystem, das es den Spielern ermöglicht, Punkte zu sammeln und diese gegen attraktive Preise einzutauschen. Dadurch wird das Spielen in der App noch spannender und lohnenswerter.
Darüber hinaus bietet die Boomerang Casino App auch regelmäßige Aktionen und Boni, die den Spielern zusätzliche Gewinnchancen bieten. Das sorgt für Abwechslung und Spannung beim Spielen.
Die Sicherheit und Fairness der Spiele steht bei der Boomerang Casino App an oberster Stelle. Alle Spiele werden regelmäßig überprüft und sind von renommierten Prüfbehörden lizenziert, um ein faires Spielerlebnis zu gewährleisten.
Insgesamt ist die Boomerang Casino App eine empfehlenswerte Option fГјr alle, die auch unterwegs nicht auf spannende Casino-Spiele verzichten wollen. Mit einer Vielzahl von Spielen, attraktiven Boni und einem sicheren Spielumfeld bietet die App ein rundum gelungenes Spielerlebnis. Einfach die App herunterladen, anmelden und direkt mit dem Spielen loslegen!
https://boomerangcasino.one/
Хотите в отменном качестве и совершенно бесплатно смотреть увлекательные сериалы? Mixtios вам в этом поможет. Здесь вы найдете самое лучшее кино. Вы можете в любое удобное время смотреть фильмы. Ищете вилли вонка фильм 2023 смотреть онлайн ? Mixtios.xyz – сайт, где представлены сериалы, помогающие ощутить множество положительных эмоций и отвлекающие от повседневной жизни. Великолепное качество изображения и профессиональное озвучивание гарантируют вам комфортный просмотр. Уверены, у нас вы найдете то, что вам интересно!
Einzahlungen auf das Wettkonto bei Tipico sind einfach und sicher. Eine der beliebtesten Methoden, um Guthaben auf das Wettkonto zu Гјberweisen, ist die Verwendung von Casino-Guthaben.
Viele Online-Casinos bieten ihren Kunden die Möglichkeit, Guthaben von ihrem Casino-Konto auf ihr Tipico-Wettkonto zu übertragen. Dies ist eine bequeme Möglichkeit, das Guthaben zu verwalten und sowohl beim Spielen im Casino als auch beim Wetten auf Sportereignisse zu nutzen.
Um Guthaben von Ihrem Casino-Konto auf Ihr Wettkonto bei Tipico zu übertragen, müssen Sie lediglich die entsprechende Option auf der Website des Casinos auswählen und den gewünschten Betrag eingeben. Nach der Bestätigung der Überweisung wird das Guthaben in der Regel innerhalb weniger Minuten auf Ihrem Wettkonto gutgeschrieben.
Es ist wichtig zu beachten, dass möglicherweise bestimmte Bedingungen und Gebühren für die Überweisung von Casino-Guthaben auf das Wettkonto gelten können. Es empfiehlt sich daher, die genauen Bestimmungen des jeweiligen Online-Casinos und von Tipico zu überprüfen, bevor Sie eine Überweisung vornehmen.
Insgesamt stellt die Verwendung von Casino-Guthaben fГјr Einzahlungen auf das Wettkonto bei Tipico eine einfache und bequeme Methode dar, um das Guthaben zu verwalten und das Spielerlebnis zu optimieren. Probieren Sie es aus und genieГџen Sie das Spielen und Wetten bei Tipico mit dem Guthaben Ihres Lieblings-Online-Casinos!
https://tipicocasino.one/
На сайте https://t.me/mvavada ознакомьтесь с нужной, ценной информацией, которая касается игрового клуба «VAVADA». Он дарит огромное количество привилегий, действует щедрая бонусная программа, а каждый игрок получает право вывести средства в наиболее комфортное для себя время. Только на этом канале самая честная, правдивая информация о компании, которая ценит своих клиентов. Казино предлагает огромный выбор развлечений, интересных и разнообразных слотов. Заходите сюда постоянно, ведь новая информация появляется регулярно.
Rassilka.kz оказывает качественные услуги. Делаем ватсап, смс, email, рассылки по Нур-Султану, Алматы и Казахстану. Сотрудничаем с разными популярными компаниями. Наша основная задача – принести пользу каждому клиенту. Действия нацелены на конечный результат. https://rassilka.kz – сайт, где вы узнаете, почему выбирают именно нас. Здесь можете в любое удобное для вас время ознакомиться с тарифами. У вас есть возможность получить бесплатную консультацию. Свяжитесь с нами, и мы ответим на все интересующие вопросы.
Tipico Casino Cash Spin ist eine aufregende Funktion, die es den Spielern ermöglicht, zusätzliche Gewinne zu erzielen, während sie ihre Lieblingsspiele spielen. Diese Funktion kann auf verschiedenen Slot-Spielen im Tipico Casino aktiviert werden und bietet den Spielern die Möglichkeit, zusätzliches Bargeld zu gewinnen.
Um am Tipico Casino Cash Spin teilnehmen zu können, müssen die Spieler bestimmte Anforderungen erfüllen. In der Regel müssen sie eine Mindestanzahl von Spins auf einem bestimmten Slot-Spiel absolvieren, um sich für den Cash Spin zu qualifizieren. Sobald die Anforderungen erfüllt sind, wird der Cash Spin automatisch aktiviert und die Spieler haben die Chance, zusätzliches Bargeld zu gewinnen.
Der Cash Spin kann unterschiedliche Preise enthalten, von kleinen Geldbeträgen bis hin zu größeren Gewinnen. Die Spieler haben die Möglichkeit, ihr Glück zu versuchen und zusätzliche Gewinne zu erzielen, die ihr Spielerkonto aufstocken können.
Tipico Casino Cash Spin ist eine spannende Funktion, die den Spielern die Möglichkeit bietet, ihre Gewinne zu maximieren und ihr Spielerlebnis zu verbessern. Mit etwas Glück können die Spieler mit dem Cash Spin ihre Gewinne deutlich steigern und noch mehr Spaß beim Spielen haben.
Insgesamt ist der Tipico Casino Cash Spin eine tolle Funktion, die den Spielern die Chance gibt, zusätzliches Bargeld zu gewinnen und ihr Spielerlebnis im Tipico Casino zu verbessern. Wir empfehlen allen Spielern, diese Funktion auszuprobieren und ihr Glück zu versuchen, um zusätzliche Gewinne zu erzielen. Viel Spaß und viel Glück beim Spielen im Tipico Casino!
https://tipicocasino.one/
Лучшие букмекеры в России – это те компании, которые предлагают высокие коэффициенты, широкий выбор спортивных событий и удобный интерфейс для ставок. Таких букмекеров можно выделить своей обширной линией, а также возможностью делать ставки в реальном времени. Они предлагают большое количество рынков для ставок и быстрые выплаты. Имеют удобное приложение для мобильных устройств. В целом, выбор букмекера зависит от предпочтений каждого игрока, но букмекеры на сайте https://russianbookmakers.ru/ являются одними из лучших на российском рынке
Сегодня, когда диплом является началом отличной карьеры в любом направлении, многие стараются найти максимально простой путь получения качественного образования. Необходимость наличия официального документа об образовании переоценить попросту невозможно. Ведь именно диплом открывает дверь перед людьми, стремящимися начать трудовую деятельность или продолжить обучение в университете.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы сможете купить диплом, и это будет отличным решением для человека, который не смог закончить образование, утратил документ или желает исправить плохие оценки. Любой диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим нюансам. В результате вы получите полностью оригинальный документ.
Превосходство подобного подхода состоит не только в том, что вы оперативно получите свой диплом. Процесс организовывается просто и легко, с нашей поддержкой. Начиная от выбора требуемого образца диплома до консультаций по заполнению личных данных и доставки по стране — все под полным контролем качественных мастеров.
Всем, кто ищет быстрый способ получения необходимого документа, наша компания предлагает выгодное решение. Приобрести диплом – значит избежать продолжительного обучения и не теряя времени перейти к своим целям, будь то поступление в ВУЗ или начало трудовой карьеры.
http://ershov.mybb.ru/viewtopic.php?id=196
http://compmaster.mybb.ru/viewtopic.php?id=11698
kraken – kraken, KRAKEN через tor
На сайте https://t.me/mvavada который представляет собой официальный канал популярного онлайн-заведения «VAVADA», предлагает ознакомиться с ценной, важной информацией. Она будет необходима всем, кто следит за работой заведения и считает себя азартным человеком. На этом канале выкладывается весь свежий контент для того, чтобы вы ознакомились с ним первым. Кроме того, есть и разнообразные акции, промокод, который позволит сэкономить и сыграть по-крупному. Только на этом канале, в первую очередь, публикуются самые свежие новости.
tokyo365web.com
belfastinvest.net
Ищете работу с гибким графиком и стабильным заработком? Яндекс Еда https://delivery-work.ru/ это возможность совмещать работу с учебой или другими делами. Преимущества работы курьером Яндекс Еда: свободный график, ежедневные выплаты, бонусы и премии, работа рядом с домом: доставляйте заказы в своем районе, экономя время на дорогу. Чтобы стать курьером Яндекс Еда, достаточно подать заявку на сайте. Присоединяйтесь к команде Яндекс Еда и начните зарабатывать уже сегодня!
кракен зеркало – kraken сайт, kraken зеркало
Tipico Casino mit Geld
Das Tipico Casino bietet seinen Spielern die Möglichkeit, mit echtem Geld zu spielen und dabei die Chance auf hohe Gewinne zu haben. Im Gegensatz zum Spielgeldmodus, bei dem keine echten Einsätze möglich sind, können die Spieler im Tipico Casino mit echtem Geld Einsätze platzieren und somit auch echte Gewinne erzielen.
Um im Tipico Casino mit Geld spielen zu können, müssen die Spieler zunächst ein Konto bei dem Online-Casino erstellen und eine Einzahlung tätigen. Dabei stehen den Spielern verschiedene Zahlungsmethoden zur Verfügung, wie zum Beispiel Kreditkarte, Banküberweisung, PayPal oder Paysafecard. Nach der Einzahlung können die Spieler aus einer Vielzahl von Spielen wählen, darunter Slots, Roulette, Blackjack, Poker und viele weitere Casino-Klassiker.
Durch den Einsatz von echtem Geld erhöht sich natürlich auch die Spannung und der Nervenkitzel beim Spielen im Tipico Casino. Die Spieler haben die Chance, hohe Gewinne zu erzielen und sich so möglicherweise den ein oder anderen Wunsch zu erfüllen. Doch Vorsicht ist geboten, denn genau wie im echten Casino besteht auch im Online-Casino die Gefahr, Geld zu verlieren. Daher sollten die Spieler verantwortungsbewusst spielen und sich ihre Grenzen setzen.
Das Tipico Casino mit Geld bietet seinen Spielern ein spannendes und unterhaltsames Spielerlebnis. Mit echten Einsätzen und echten Gewinnen sorgt das Online-Casino für jede Menge Spaß und Nervenkitzel. Wer sein Glück versuchen und die Chance auf hohe Gewinne haben möchte, ist im Tipico Casino genau richtig.
https://tipicocasino.one/
Each offer is accompanied by photographs of the canada-welcome.com hotel where tourists are invited to stay. There is the exterior of the building, the interiors of the rooms, photos of the territory and individual objects. The page contains a detailed description of living conditions, room equipment, and the possibility of paid and free services.
The finished metal structure mosesolmos.com must be properly packaged. Thanks to this, it will definitely not be damaged during transportation.
https://headshotseo.com/
Зайдіть на сайт https://wian.top/ і ви зможете дізнатися, почитати, переглянути найсвіжіші новини України. Стрічка постійно поповнюється, що дозволить вам залишатися в курсі найсвіжіших подій. Виберіть категорію, що цікавить, і читайте тільки актуальну інформацію.
Наш Telegram-канал – это место, где вы найдете актуальную информацию о новых МФО. Мы ежедневно обновляем список, чтобы предложить вам лучшие условия для займов. Узнайте больше о займы онлайн новые малоизвестные без отказа. Мы расскажем, как получить займ под 0% даже с плохой кредитной историей и как правильно использовать онлайн займы. Подписывайтесь на наш канал и получайте финансовую помощь быстро и без лишних вопросов!
Интернет-магазин «Body-pit» предлагает вам купить спортивное питание по доступным ценам от популярных производителей. Мы готовы оказать вам квалифицированную помощь в подборе нужного товара. Вы останетесь довольны обслуживанием и магазином. https://ufa2.body-pit.ru/ – сайт, где у вас есть возможность уже сейчас посмотреть условия оплаты. Выполняем быструю доставку спортпита и стараемся своих клиентов обеспечить наилучшим сервисом. Качество спортивного питания нашего онлайн-магазина на высоте. Обращайтесь к нам и не пожалеете!
mega sb не работает сайт – мега новая ссылка, мега сб даркнет
Наш канал – это источник информации о новых МФО 2024. Получите займ от 1 до 30 рублей на 30 дней даже с плохой кредитной историей. Минимальные требования – паспорт и банковская карта. Подпишитесь и будьте в курсе всех новинок!
Нужны деньги срочно? На нашем канале вы найдете новые МФО 2024, где займы доступны круглосуточно. Оформите займ от 1 до 30 рублей на 30 дней даже с плохой кредитной историей. Быстро, удобно и безопасно.
m3ga площадка – https mega sb, m3ga gl зеркало
blacksprut ссылка tor – blacksprut solaris, блекспрут com
Das Live Casino von Tipico erfreut sich groГџer Beliebtheit bei Spielern, die gerne in Echtzeit gegen echte Dealer antreten. Doch was passiert, wenn das Geld im Live Casino blockiert wird?
Es kann verschiedene Gründe dafür geben, dass Geld im Live Casino von Tipico blockiert wird. Einer der häufigsten Gründe ist, dass ein Spieler gegen die Allgemeinen Geschäftsbedingungen des Casinos verstoßen hat. Dies kann zum Beispiel geschehen, wenn ein Spieler versucht, mehrere Konten zu eröffnen, um sich Boni mehrfach zu sichern. In solchen Fällen behält sich das Casino das Recht vor, das Geld des Spielers einzufrieren.
Ein weiterer Grund für blockiertes Geld im Live Casino von Tipico kann sein, dass der Spieler sein Konto nicht verifiziert hat. Das Casino ist dazu verpflichtet, die Identität seiner Spieler zu überprüfen, um Geldwäsche und Betrug zu verhindern. Wenn ein Spieler diese Verifizierung nicht rechtzeitig durchführt, kann es sein, dass sein Geld blockiert wird, bis dies geschehen ist.
Es ist wichtig, dass Spieler die Regeln und Bedingungen des Casinos genau lesen und beachten, um solche Situationen zu vermeiden. Wenn das Geld im Live Casino von Tipico blockiert wurde, sollte der Spieler sich umgehend an den Kundenservice des Casinos wenden, um das Problem zu klären. In den meisten Fällen kann das Geld nach einer Überprüfung des Falls wieder freigegeben werden.
Insgesamt ist es wichtig, verantwortungsbewusst im Live Casino von Tipico zu spielen und sich an die Regeln des Casinos zu halten, um Blockaden des Geldes zu vermeiden. Wenn dennoch einmal ein Problem auftreten sollte, steht der Kundenservice von Tipico jederzeit zur VerfГјgung, um zu helfen.
https://tipicocasino.one/
Нужны деньги срочно? Наш канал представляет новые МФО 2024, где можно получить займ от 1 до 30 рублей на 30 дней. Даже с просрочками и плохой кредитной историей. Минимальные требования и быстрый перевод на карту. Подписывайтесь сейчас!
На сайте https://setki.moscow вы сможете оформить заявку для того, чтобы заказать москитную сетку. Конструкции производятся из качественных, надежных материалов и всего за день. Монтажные работы проводятся в любой, наиболее комфортный для вас день. На работы, конструкции даются гарантии 12 месяцев. Рассчитать итоговую цену вы сможете прямо сейчас. Установлена привлекательная стоимость за счет собственного производства. Работа происходит не только по Москве, но и области. Предприятие специализируется на производстве, реализации, а также установке москитных сеток.
click here to read sollet chrome
gocanadanews.com
texasnews365.com
my sources jaxx wallet
Ищете актуальные промокоды Яндекс Маркета? Обратите внимание на канал Олега Петрова, вы точно его полюбите. Здесь автор публикует свежие подборки купонов и акций. Теперь не надо искать предложения, Олег за вас уже сделал всю работу. Его главная цель – помочь сэкономить ваши денежные средства. Ищете яндекс маркет промокод телефоны? Dzen.ru/a/ZgxKFq5bOTUwDw_w – здесь представлены достоверные купоны. Если еще не умеете ими пользоваться, то здесь предложена краткая инструкция. Воспользуйтесь эксклюзивными предложениями уже сейчас!
В нашем обществе, где диплом становится началом успешной карьеры в любой отрасли, многие пытаются найти максимально быстрый путь получения качественного образования. Наличие документа об образовании сложно переоценить. Ведь именно он открывает двери перед всеми, кто собирается начать трудовую деятельность или учиться в ВУЗе.
В данном контексте мы предлагаем максимально быстро получить этот необходимый документ. Вы сможете приобрести диплом, что является отличным решением для человека, который не смог закончить обучение, потерял документ или желает исправить плохие оценки. дипломы изготавливаются аккуратно, с особым вниманием ко всем элементам, чтобы в итоге получился документ, максимально соответствующий оригиналу.
Превосходство этого подхода заключается не только в том, что можно оперативно получить диплом. Процесс организован комфортно, с нашей поддержкой. Начиная от выбора подходящего образца диплома до грамотного заполнения личных данных и доставки в любой регион России — все под абсолютным контролем наших мастеров.
Всем, кто ищет быстрый и простой способ получить необходимый документ, наша услуга предлагает выгодное решение. Заказать диплом – значит избежать длительного обучения и сразу переходить к своим целям, будь то поступление в университет или начало карьеры.
http://fwh.mybb.ru/viewtopic.php?id=403
https://rodme.ru/kupit-diplom-o-vysshem-obrazovanii-t11095.html
article sollet solana
More Help jaxx blockchain wallet
стратегии ставок на спорт
Manufacturing metal structures is a californiarent24.com very complex and responsible process. It is necessary to follow some rules and follow recommendations to ensure that the product turns out to be of high quality and safe. You can order the production of metal structures on the website to profitably invest your own money. Let’s consider the basic rules that relate to this process.
To operate hydraulic motors, mineral oils are used, dominicanrental.com which are pre-cleaned to remove any impurities. The MRF line of hydraulic motors presented six models, differing from each other in the following matter.
Подробная инструкция по оформлению пропуска на МКАД, советы, лайфхаки, которую нужно знать, основные требования, на которые нужно знать ответы, подробный обзор, Почему стоит получить пропуск на МКАД, Как продлить пропуск на МКАД, подробная информация
Пропуск на мкад Пропуск в москву .
24thainews.com
go to this site Palworld
Ищите строительные материалы и строительные услуги в Минске и по всей Беларусь? Зайдите на https://mirstroy.by/ и вы найдете огромное количество предложений от поставщиков, производителей, по самым лучшим ценам. Воспользуйтесь поиском материала или выберете категорию, и вы обязательно найдете все что вам необходимо с доставкой. Огромный ассортимент и выгодные цены ждут вас.
Саморазвитие начинается с первого шага! На канале https://t.me/s/razvisam/ ты найдешь пошаговые инструкции, книги по психологии и полезные советы, которые помогут тебе на этом пути. Присоединяйся и меняй свою жизнь!
В современном мире, где диплом становится началом отличной карьеры в любой отрасли, многие ищут максимально быстрый путь получения образования. Факт наличия документа об образовании сложно переоценить. Ведь диплом открывает дверь перед людьми, стремящимися начать профессиональную деятельность или продолжить обучение в каком-либо институте.
Наша компания предлагает быстро получить этот необходимый документ. Вы сможете приобрести диплом, и это становится удачным решением для всех, кто не смог закончить обучение или потерял документ. Все дипломы производятся с особой аккуратностью, вниманием к мельчайшим элементам, чтобы в результате получился полностью оригинальный документ.
Превосходство этого решения состоит не только в том, что вы сможете быстро получить диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. От выбора требуемого образца диплома до консультаций по заполнению личной информации и доставки по стране — все будет находиться под полным контролем квалифицированных мастеров.
В результате, для тех, кто ищет быстрый и простой способ получения требуемого документа, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать продолжительного обучения и не теряя времени переходить к своим целям, будь то поступление в ВУЗ или старт карьеры.
https://moscow.topbb.ru/viewtopic.php?id=3738
http://forumklimovsk.0pk.me/viewtopic.php?id=12532
оземпик +для похудения цена – оземпик купить +в омске, купить оземпик +в москве
Добро пожаловать в наш Telegram-канал, где мы рассказываем о самых новых микрозаймах. Каждый день мы тщательно проверяем новые МФО, чтобы вы могли узнать все условия и выбрать лучший вариант. Воспользоваться займом могут все, даже если у вас есть просрочки или плохая кредитная история. Это идеальный вариант, когда деньги нужны срочно. Откройте для себя [url=https://t.me/s/mfo_2024_online]новые мфо только открывшиеся без отказа на карту[/url], и получите займ без звонков и лишних вопросов.
go to the website galaxy swapper
Хотите купить по выгодной стоимости коробки из гофрокартона? Смело обращайтесь в компанию «Гофрокороб СПб». Новейшее оборудование компании позволяет изготавливать по доступным ценам и в кратчайшие сроки упаковку из гофрокартона отменного качества. Ищете производитель упаковки? Korobok-spb.ru – сайт, где вы можете узнать, как выполнить на тару из гофрированного картона заказ. Предлагаем широкий выбор упаковочных решений. Можете прямо сейчас ознакомиться с продукцией, условиями оплаты и доставки картонных коробок. Всегда рады сотрудничеству. Звоните!
Наш Telegram-канал – это ваш надежный источник информации о новых МФО. Мы ежедневно публикуем данные о самых выгодных предложениях. Узнайте о микрозаймы новые онлайн, которые можно получить под 0% в рамках акций. Даже если у вас плохая кредитная история, вы сможете получить займ без отказа. Мы расскажем, что такое онлайн займы и как их правильно использовать. Подписывайтесь на наш канал и получайте деньги быстро и без лишних вопросов!
Full Report Flstudio download
В нашем Telegram-канале вы найдете самые свежие и проверенные предложения от новых МФО. Мы ежедневно обновляем информацию, чтобы вы могли выбрать лучшие условия. Если вам срочно нужны деньги, мы расскажем вам про новый займ на карту без отказа. Получить деньги теперь можно даже при плохой кредитной истории. Наш канал поможет вам найти самый выгодный и надежный вариант. Подписывайтесь и узнайте больше о новых МФО!
discover here Rufus usb
На сайте https://dolinakamnej.ru приобретите минералы, натуральные камни, а также интересные и необычные изделия, которые понравятся даже истинному эстету. Доставка осуществляется в любую точку мира, России. Компания отличается собственным производством, а потому установила привлекательные и доступные цены. Здесь же есть возможность воспользоваться и такими популярными, нужными услугами, как полировка, распиловка на заказ. Все услуги оказываются качественно, в соответствии с самыми высокими требованиями.
оземпика семаглутид – тирзепатид цена, mounjaro +и wegovy
оземпик препарат цена купить – оземпик купить +в самаре, Оземпик купить
скупка автомобилей https://avtovikupmashin21.ru/
лучшие казино
If you properly prepare 365eventcyprus.com the material before manufacturing the structure, you can get a high-quality product.
На сайте http://ritualnoe-buro-vrn.ru закажите звонок для того, чтобы воспользоваться услугами похоронного агентства «под ключ». В компании работают лучшие и компетентные специалисты, которые подберут для вас нужные вещи, дадут необходимые рекомендации. Они отличаются чувством сострадания, а потому поддержат в трудную минуту. Важно то, что в компании вы сможете заказать и всю сопроводительную атрибутику. Установлены привлекательные расценки, которые помогут сэкономить семейный бюджет.
Forklifts can be called an miamicottages.com indispensable element of equipment, which is actively used in the arrangement of warehouse premises. With their help, you can load pallets, boxes and large cargo onto the upper shelves of the racks, which increases the functional area of the warehouse by an order of magnitude. Here you will learn about the advantages of forklifts, as well as their types and applications. You may also be interested in the opportunity to buy warehouse equipment on the site.
reference Torbrowser
CVzen https://cvlamaran.com/ adalah layanan penulisan CV dan pelatih karir terbaik bagi jutaan pencari kerja di seluruh dunia. Tim ahli kami berkomitmen untuk kesuksesan Anda dan akan mendukung Anda sepanjang perjalanan karir Anda, mulai dari menulis CV profesional dan surat lamaran yang sesuai dengan industri yang Anda minati, hingga mengoptimalkan profil LinkedIn Anda dan memberikan pelatihan karir profesional. Buka peluang baru dengan resume yang menunjukkan potensi Anda.
оземпик +для диабетиков – семаглутид 0.25-0.5 купить с доставкой, лираглутид инструкция +по применению
В современном мире, где диплом – это начало отличной карьеры в любой области, многие ищут максимально простой путь получения качественного образования. Наличие официального документа об образовании сложно переоценить. Ведь именно он открывает дверь перед любым человеком, который желает вступить в профессиональное сообщество или учиться в ВУЗе.
В данном контексте мы предлагаем быстро получить этот важный документ. Вы можете купить диплом, что будет удачным решением для всех, кто не смог закончить обучение или утратил документ. диплом изготавливается с особой аккуратностью, вниманием ко всем элементам. В результате вы получите полностью оригинальный документ.
Преимущества такого решения состоят не только в том, что вы сможете оперативно получить диплом. Процесс организован удобно, с нашей поддержкой. От выбора требуемого образца документа до правильного заполнения личных данных и доставки по стране — все будет находиться под абсолютным контролем опытных мастеров.
Всем, кто ищет быстрый способ получить требуемый документ, наша компания может предложить отличное решение. Приобрести диплом – значит избежать продолжительного обучения и сразу перейти к своим целям: к поступлению в университет или к началу удачной карьеры.
http://suponevo.webtalk.ru/viewtopic.php?id=8953
http://ya.forum2.net/viewtopic.php?id=9393
Porodicne odmaralisne kuce u Crnoj Gori – Iznajmljivanje vikendica u okolini Zabljaka, Аренда шале в Дурмиторе
It is necessary to work carefully housebru.com and accurately when manufacturing metal structure parts. Even minimal mistakes lead to serious problems in the future.
блэкспрут ссылка – блэк спрут ссылка, тор blacksprut
На сайте https://t.me/mpokerdom изучите информацию, которая касается такого известного заведения, как «Покердом». Это официальный канал, на котором вы найдете все, что нужно. Здесь выкладываются различные промокоды, сможете узнать актуальные и свежие новости, которые точно вам необходимы, если интересуетесь онлайн-играми. На канал можно заходить с любого устройства, в том числе, мобильного телефона или компьютера. Где бы вы ни были, доступ к группе не будет ограничен. Заходите сюда почаще, чтобы ознакомиться с материалами.
Hey! This post couldn’t be written any better! Reading this post reminds me of my old room mate! He always kept talking about this. I will forward this article to him. Fairly certain he will have a good read. Many thanks for sharing!
spin away
Looking for the best travel and food blog? Looking for world food recipes? Atravel.blog where you will find fascinating information about the countries and their culinary traditions Read the blog, find out information about national cuisine and resorts, and also get acquainted with recipes of world cuisine. The blog is constantly updated with fresh entries, which will make it possible to learn more and more new things.
Посетите сайт https://initiative.am/ который поднимает проблемы налогообложения в Армении. Спикеры сайта указывают на серьезные сложности в этом вопросе и полное отсутствие реакции, а проблемы существенные. Спикер внятно, по полочкам, доходчиво поднимает мысль о том, что необходимо сделать или изменить в текущем законодательстве, чтобы все стороны и государство и бизнес, и люди шли одной дорогой и взаимовыгодно.
cyprus-welcome.com
californianetdaily.com
стоимость свайного фундамента для дома 10х10
Muzofond https://muzofond.xyz/ это возможность скачать бесплатно музыку в формате mp3 и слушать онлайн на сайте. Самые новые коллекции треков, альбомов, жанров, исполнителей, чарты и новинки, а также огромное количество разнообразной музыки прошлых лет.
фундамент ленточный под ключ цена в московской
First of all, it should be clearly repaircanada.net understood that these are completely different concepts in geography. For example, when considering absolute height, it is precisely this that acts as the most important indicator, which is measured in meters, thereby determining the height of geographical objects above sea level.
Metalworking on lathes involves many morson.org types of actions when it is necessary to create recesses in products, or cut off individual parts.
Зайдите на сайт https://xn—-8sbdjhxdprbbhnk7e.xn--p1ai/ где вы сможете найти актуальные промокоды и скидки на iHerb. Возможно использование сразу двух промокодов. Промокоды для новых покупателей, промокоды на весь заказ, промокоды на добавки и на отдельные бренды, на бакалею. Воспользуйтесь ими и получите скидку.
Линкей Лайт предоставляет вашему вниманию светильники разной мощности по доступной стоимости. Наши компетентные специалисты помогут с определением количества светильников и с проведением нужных расчетов для вашего автосервиса. https://linkey-light.ru – сайт, предлагающий к ознакомлению полного каталога светильников для автосервиса. Главной миссией компании является разработка и производство светодиодных светильников для широкого спектра применения. Вся продукция наша прошла требования безопасности и качества, она сертифицирована.
На сегодняшний день, когда диплом – это начало отличной карьеры в любой отрасли, многие ищут максимально простой путь получения качественного образования. Факт наличия официального документа переоценить невозможно. Ведь диплом открывает дверь перед людьми, стремящимися вступить в профессиональное сообщество или учиться в высшем учебном заведении.
Предлагаем максимально быстро получить этот важный документ. Вы имеете возможность заказать диплом, и это будет отличным решением для человека, который не смог завершить образование, утратил документ или желает исправить плохие оценки. дипломы выпускаются с особой аккуратностью, вниманием к мельчайшим нюансам. В итоге вы сможете получить продукт, полностью соответствующий оригиналу.
Преимущества этого подхода состоят не только в том, что можно оперативно получить диплом. Процесс организован просто и легко, с нашей поддержкой. От выбора необходимого образца до консультаций по заполнению персональной информации и доставки в любое место страны — все будет находиться под полным контролем качественных специалистов.
В результате, для всех, кто ищет максимально быстрый способ получения необходимого документа, наша услуга предлагает выгодное решение. Приобрести диплом – значит избежать продолжительного обучения и сразу переходить к достижению личных целей: к поступлению в университет или к началу удачной карьеры.
http://vip.9bb.ru/viewtopic.php?id=4428
http://duristkomi.mybb.ru/viewtopic.php?id=1730
свайный фундамент 10 на 10
next Osu
Благодарю за полезную инфу!
В свою очередь предлагаю поиграть в настоящее казино!
зарегистрироваться вавада — доступно и быстро. Это допустит вас к широкому спектру азартных игр.
Зарегистрировавшись вы войдете в свой ЛК и начать играть. Не забудьте, что для вывода выигранных денег вам необходимо будет пройти верификацию аккаунта, показав документы, которые у вас запросят.
ушп газобетон
Such concepts in geography as absolute caribbean21.com and relative height are basic. If you begin to delve into the intricacies of this issue, you will understand that they actually allow, help to describe geographical objects, understanding what they are all about.
detroitapartment.net
Ищите калькулятор ндс? Ищете калькулятор ндс? Calculatornds.ru где вы найдете калькулятор ндс онлайн, который предназначен для автоматического расчета, выделения или начисления налога на добавленную стоимость. Калькулятор ндс удобен в применении, вам необходимо лишь ввести сумму. ндс калькулятор онлайн – пользуйтесь на нашем сайте для точного расчета налога.
check galaxy swapper v2
Bs2best – Bs2best, Bs2best
1вин казино
В современном мире, где диплом является началом успешной карьеры в любой области, многие стараются найти максимально простой путь получения качественного образования. Необходимость наличия документа об образовании сложно переоценить. Ведь именно он открывает двери перед людьми, желающими вступить в сообщество профессионалов или учиться в любом институте.
В данном контексте наша компания предлагает максимально быстро получить этот важный документ. Вы можете купить диплом нового или старого образца, что будет удачным решением для всех, кто не смог закончить образование, потерял документ или хочет исправить свои оценки. Все дипломы производятся аккуратно, с максимальным вниманием к мельчайшим элементам. На выходе вы сможете получить документ, полностью соответствующий оригиналу.
Преимущество данного подхода состоит не только в том, что можно максимально быстро получить свой диплом. Процесс организовывается удобно и легко, с профессиональной поддержкой. Начиная от выбора подходящего образца до консультаций по заполнению личных данных и доставки в любой регион России — все находится под абсолютным контролем наших специалистов.
Таким образом, для тех, кто пытается найти оперативный способ получить необходимый документ, наша компания предлагает выгодное решение. Приобрести диплом – это значит избежать продолжительного обучения и сразу перейти к достижению личных целей, будь то поступление в ВУЗ или старт карьеры.
http://bux.7bb.ru/viewtopic.php?id=3397
http://krut.forumno.com/viewtopic.php?id=1745
травмат без лицензии и разрешения – пистолет макарова купить, травматическое оружие купить
1win казино
CVzen https://cvzen.de/ ist der ultimative Lebenslauf-Schreibservice und Karriere-Coach für Millionen von Arbeitssuchenden auf der ganzen Welt. Unser Expertenteam setzt sich für Ihren Erfolg ein und unterstützt Sie auf Ihrem gesamten Karriereweg, vom Verfassen Ihres professionellen Lebenslaufs und Anschreibens mit branchenspezifischen Informationen bis hin zur Optimierung Ihres LinkedIn-Profils und professionellem Karriere-Coaching. Erschließen Sie sich neue Chancen mit einem Lebenslauf, der Ihr Potenzial unterstreicht.
На сайте https://kurs-excel.ru закажите обратный звонок для того, чтобы воспользоваться услугами высшей школы математики, статистики. Для того чтобы ознакомиться со всей необходимой, актуальной информацией, необходимо записаться на курсы MICROSOFT EXCEL, а также изучение офисного ПО. Кроме того, вы сможете научиться выполнять рутинные дела, ежедневную работу намного быстрее, чем обычно. Обучение проводится в течение пары месяцев, за которые вы полностью освоите программу. Все преподаватели являются компетентными специалистами.
дешевые аккаунты вк – купить акк вк авторег, акки вк авторег
blacksprut ссылка – как зайти на blacksprut, blacksprut официальный сайт
Секреты оформления пропуска на МКАД, Эффективные способы получения пропуска на МКАД, Ключевые моменты о пропуске на МКАД, которую важно помнить, подробная инструкция, Сколько стоит и как долго делается пропуск на МКАД, подробный обзор, советы, Инструкция по продлению пропуска на МКАД, полный гайд
Проверить пропуск на мкад Проверить пропуск на мкад .
Желаете арендовать автомобиль в Минске? Зайдите на https://autorent.by/ где вы найдете большой ассортимент автомобилей от эконом класса до премиум, а также внедорожники, мотоциклы, микроавтобусы и другие автомобили. Мы предлагаем лучшие условия, бонусы и скидки. Узнайте подробнее на сайте.
купить акк инсты – купить фейк акк вк, купить аккаунт инстаграм с реальными подписчиками
Pin up haqqnda mlumat axtarrsnz? Looking for pin up azerbaijan? Pinupcasino-azerbaijan.com saytına daxil olun, burada bu maraqlı və əyləncəli oyun haqqında hər şeyi öyrənmək imkanınız var. Necə qeydiyyatdan keçmək, necə oynamaq, bonuslar və daha çox şey sizi burada gözləyir. İstənilən cihaz üçün mobil versiyanı yükləməyi öyrənəcəksiniz, istifadəsi asandır.
В канун Рождества я понял, что не успеваю купить подарки для близких. Ощущение паники сменилось радостью, когда я нашел займ на Займы на карту без отказов онлайн . Деньги поступили быстро, и я смог закупить всё, что хотел. Рождественская ночь стала настоящей сказкой для всей нашей семьи.
В канун Рождества я понял, что не успеваю купить подарки для близких. Ощущение паники сменилось радостью, когда я нашел займ на Срочные онлайн займы . Деньги поступили быстро, и я смог закупить всё, что хотел. Рождественская ночь стала настоящей сказкой для всей нашей семьи.
Наш котик заболел, и на его лечение потребовалась крупная сумма. В такой сложный момент я обратился к Займы без процентов на карту . Быстро оформил займ и смог оплатить все медицинские услуги. Котик выздоровел, и я был безмерно счастлив, что смог ему помочь.
goturkishnews.com
купить аккаунт инстаграм с подписчиками дешево – биржа аккаунтов инстаграм купить, vk несколько аккаунтов
Сегодня, когда диплом – это начало удачной карьеры в любой отрасли, многие ищут максимально простой путь получения качественного образования. Наличие документа об образовании трудно переоценить. Ведь диплом открывает дверь перед всеми, кто хочет начать трудовую деятельность или учиться в университете.
В данном контексте наша компания предлагает максимально быстро получить этот необходимый документ. Вы сможете купить диплом, что становится удачным решением для человека, который не смог закончить образование, потерял документ или желает исправить плохие оценки. дипломы изготавливаются с особой тщательностью, вниманием к мельчайшим деталям, чтобы в итоге получился полностью оригинальный документ.
Преимущества данного решения заключаются не только в том, что можно оперативно получить свой диплом. Процесс организован удобно, с профессиональной поддержкой. От выбора требуемого образца до точного заполнения персональной информации и доставки по России — все будет находиться под абсолютным контролем качественных мастеров.
Для всех, кто хочет найти быстрый и простой способ получить необходимый документ, наша компания предлагает отличное решение. Приобрести диплом – значит избежать долгого процесса обучения и не теряя времени перейти к достижению личных целей, будь то поступление в ВУЗ или старт карьеры.
http://fkvrn.webtalk.ru/viewtopic.php?id=700
http://crimeadetka.forum.cool/viewtopic.php?id=1510
оружие для самообороны без лицензии – купить дрон dji, купить оружие без разрешения
На сайте https://t.me/m1xbet_ru получите исчерпывающую информацию, которая касается популярной компании «1XBET». Эта БК радует своими регулярными выплатами, огромным количеством бонусов, а также большим количеством спортивных состязаний. Каждый желающий сможет сделать ставки на то мероприятие, которое ему интересно. В этой группе, в первую очередь, появляются самые свежие, интересные новости, с которыми необходимо ознакомиться и вам. Отзывы подтверждают то, что «1XBET» точно можно доверять.
новый аккаунт в инстаграм купить – куплю продам акк на ютубе вк, авторег вконтакте с друзьями
Моей маме исполнилось 60 лет, и я хотел сделать ей особенный подарок. Для этого потребовалась небольшая сумма, которую я нашел на новые МФО 2024 без отказа . Удивило, как быстро и легко можно получить деньги, даже с не самой лучшей кредитной историей. Подарок удался, и мама была в восторге.
blacksprut com зеркало – blacksprut com, тор blacksprut
https://kursy-marketologov.ru/
Bs.gl – Блэкспрут, Блэкспрут ссылка
Почему теневой плинтус – красивая и практичная деталь интерьера,
Шаг за шагом инструкция по установке теневого плинтуса,
Как использовать теневой плинтус для создания уникального интерьера,
Ретро-стиль с использованием теневых плинтусов: идеи для вдохновения,
Как подобрать цвет теневого плинтуса к отделке стен,
Безопасность и стиль: почему теневой плинтус – идеальное решение для дома,
Теневой плинтус с подсветкой: создаем эффектное освещение в интерьере,
Как сделать помещение завершенным с помощью теневого плинтуса,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
купить плинтус https://plintus-tenevoj-aljuminievyj-msk.ru/ .
ЗдравБудь – известный портал о здоровье. Здесь у вас есть возможность узнать, что делать с собственной агрессией, как коронавирус может влиять на половую функцию, как заставить ребенка кушать, есть ли взаимосвязь между ЭКО и возникновением рака и другое. Мы предоставляем только полезную информацию. Ищете какой врач лечит артроз суставов? Zdravbud.net/new/pochemu-bolyat-sustavy – тут детально рассказываем, почему болят суставы. Разъясняем, чем суставы питать, чтобы они восстановились. Разъясняем, как работает МолекАРТ-РА. Заходите на наш портал уже сейчас и читайте самые лучшие статьи.
Интернет-магазин с огромным ассортиментом раковина 105 см для вашей ванной комнаты.
cottageindesign.com
На сайте https://aakkb.com.ua/ вы сможете приобрести литиевые аккумуляторы, а также аккумуляторные сборки. Все конструкции отличаются своей надежностью, безупречным качеством, а также идеальным исполнением. Все модели от проверенных, лучших брендов, которые работают на совесть. Перед вами огромное количество моделей, что позволит подобрать решение на свое устройство. А если затрудняетесь с выбором, то вас всегда поддержит высококлассный специалист. Он даст ценные советы, важные рекомендации.
review jaxx wallet liberty
Сегодня, когда диплом становится началом отличной карьеры в любом направлении, многие стараются найти максимально простой путь получения качественного образования. Наличие официального документа об образовании переоценить попросту невозможно. Ведь диплом открывает дверь перед всеми, кто собирается вступить в профессиональное сообщество или учиться в каком-либо университете.
В данном контексте наша компания предлагает оперативно получить этот важный документ. Вы имеете возможность заказать диплом нового или старого образца, и это становится выгодным решением для всех, кто не смог завершить образование или утратил документ. Все дипломы производятся с особой тщательностью, вниманием ко всем элементам, чтобы в итоге получился полностью оригинальный документ.
Превосходство этого подхода заключается не только в том, что можно оперативно получить свой диплом. Весь процесс организовывается просто и легко, с нашей поддержкой. Начав от выбора нужного образца документа до правильного заполнения личной информации и доставки по стране — все будет находиться под абсолютным контролем наших специалистов.
Для всех, кто пытается найти быстрый способ получения требуемого документа, наша компания предлагает отличное решение. Заказать диплом – это значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению собственных целей, будь то поступление в ВУЗ или начало карьеры.
http://sennenhund.bbok.ru/viewtopic.php?id=2439
http://auto.boltun.su/viewtopic.php?id=1446
leeds-welcome.com
Сайт, где представлен разнообразие раковина кухонная черная для вашей ванной комнаты, с доставкой по всей стране.
hop over to this web-site sollet wallet
Visit https://100happywishes.com/ and learn all about investing, stock trading, trading tools, banking and much more from the world of finance. A large portal with a lot of useful information will give you the opportunity to fully study information about investing.
узнать больше Здесь
РЕМОНТ И СЕРВИСНОЕ ОБСЛУЖИВАНИЕ КОНДИЦИОНЕРА В ОРШЕ
Я решил расширить свой небольшой бизнес и нуждался в дополнительных средствах. Телеграм-канал Займы без процентов на карту предоставил мне отличный выбор МФО, которые специализируются на займах для предпринимателей. Полученные деньги помогли мне реализовать задуманное.
view it now sollet io
Зайдите на сайт https://lestnicy-premium.ru/ и вы найдете настоящую лестницу мечты. Высочайшее качество на всех этапах производства. И конкурентные цены! Самые выгодные условия оплаты! Только мы предлагаем оплату частями параллельно выполнению работ! Мы не просто строители лестниц. Мы – генераторы потрясающих идей, креативности и фантазии. Строители мостов между этажами вашего вдохновения! Подробнее на сайте.
take a look at the site here Pot player
На сайте https://sp.svetodar.pro/ запишитесь онлайн в центр офтальмологии. Есть как взрослое, так и детское отделение. Можно воспользоваться и различными прочими услугами. Если подпишитесь в ВК, то вам предоставят хорошую скидку. Врачи расшифруют диагноз, составят правильную схему терапии, чтобы она была понятна всем. Компания открыла 4 клиники для того, чтобы вы смогли воспользоваться услугами, находясь в любом месте. В них трудятся 50 компетентных, квалифицированных врачей. Они используют уникальные и инновационные методики.
Магазин, где представлен широкий выбор раковина из фаянса для вашей ванной комнаты, с доставкой по всей стране.
На сайте https://pogadaems.ru вы сможете почитать увлекательную, интересную и актуальную информацию, которая касается гаданий в режиме реального времени. Есть возможность изучить информацию о гаданиях на картах Таро, игральных, а также цыганских. Имеются интересные и любопытные картинки, которые позволят пожелать доброго утра маме. Перед вами самая интересная, увлекательная информация, которая поможет сориентироваться в теме. Обязательно ознакомьтесь с гороскопом, чтобы знать, что ожидает вас сегодня.
Хотите недорого приобрести печи Ферингер? Feringer.shop – то, что вам необходимо! Мы регулярно расширяем свой ассортимент, устраиваем акции и улучшаем уровень сервиса. Вы можете рассчитывать на выгодные условия покупки печного оборудования. Ищете ферингер? Feringer.shop – здесь можно прямо сейчас ознакомиться с отзывами реальных покупателей и условиями доставки. Гарантируем качество товара и наилучшую цену. Учитываем пожелания и потребности наших заказчиков. Обращайтесь, готовы проконсультировать вас и помочь выполнить установку изделия.
В нашем обществе, где диплом – это начало отличной карьеры в любой сфере, многие пытаются найти максимально простой путь получения качественного образования. Наличие официального документа трудно переоценить. Ведь диплом открывает дверь перед каждым человеком, который хочет вступить в сообщество профессиональных специалистов или учиться в университете.
В данном контексте мы предлагаем быстро получить любой необходимый документ. Вы имеете возможность приобрести диплом, и это будет удачным решением для всех, кто не смог закончить обучение или утратил документ. дипломы выпускаются с особой аккуратностью, вниманием к мельчайшим нюансам, чтобы на выходе получился продукт, полностью соответствующий оригиналу.
Превосходство данного подхода состоит не только в том, что вы сможете максимально быстро получить свой диплом. Весь процесс организовывается просто и легко, с нашей поддержкой. Начав от выбора требуемого образца документа до консультации по заполнению персональных данных и доставки в любой регион России — все под полным контролем опытных специалистов.
В результате, для тех, кто хочет найти быстрый способ получения требуемого документа, наша компания может предложить отличное решение. Приобрести диплом – значит избежать долгого обучения и сразу перейти к своим целям, будь то поступление в ВУЗ или старт карьеры.
http://mamamia.by/forum/viewtopic.php?p=23091
http://forumtrolley.mybb.ru/viewtopic.php?id=301
Robust cutting tools with low wear workingholiday365.com and high hardness are required. It is proposed to buy replacement groove plates from well-known manufacturers.
Homepage evon v5
geinoutime.com
그래서 모두 슬퍼 보입니다.그래서 그는 장쑤성과 저장성 사람들도 스웨터가 필요하다고 주장했습니다.
why not try these out delta pc
Professional care of the premises. Cleaners undergo apartusa365.com detailed training, where they learn the combination of different cleaning products with different types of materials.
На сайте https://t.me/mvavada почитайте интересную, увлекательную и свежую информацию относительно проекта «VAVADA», который стал одним из самых популярных в Интернете. У вас появляется удивительная возможность ознакомиться с материалами, которые будут нужны для того, чтобы воспользоваться всеми преимуществами онлайн-площадки. На этом канале, в первую очередь, публикуются ценные и важные новости, промокоды, освещаются важные события. Публикуются только честные, правдивые материалы. Заходить сюда можно ежедневно и с любого устройства, в том числе, смартфона.
Автоломбард https://www.dcc.kz/ с правом вождения: Залог вашего автомобиля с возможностью его использования. Мы выдаем до 50% от суммы залога. Автоломбард без права вождения: Ваш автомобиль остается на охраняемой стоянке, где он будет находиться до момента окончания выплаты по кредиту. Мы выдаем до 70% от суммы залога.
CVzen https://cvzen.pl/ to najlepsza usługa pisania CV i coach kariery dla milionów osób poszukujących pracy na całym świecie. Nasz zespół ekspertów jest zaangażowany w Twój sukces i będzie Cię wspierał przez całą Twoją karierę, od napisania profesjonalnego CV i listu motywacyjnego z uwzględnieniem specyfiki branży, po optymalizację profilu LinkedIn i zapewnienie profesjonalnego coachingu kariery. Odblokuj nowe możliwości dzięki CV, które pokaże Twój potencjał.
A person can configure the system independently dublinnews365.com or contact an organization to use the feature, focusing on their needs.
A simple rule applies here, for example britainrental.com, the height of Everest is 8848 meters above sea level. Thus, Everest, which is located at such a height above sea level, is considered to be the highest mountain on Earth.
Посетите страницу https://www.avclub.pro/cases/osnashcheniye-konferents-zala-krupnogo-promyshlennogo-predpriyatiya/ где вы узнаете и почитаете интересную информацию о том, как правильно оснастить конференц-зал крупного промышленного предприятия и какие для этого использовались технологии и инструменты, о том как специалисты интегратора провели разработку концепции и технического решения.
Вам интересны контурные карты, атласы или школьные учебники? У нас вы найдете это и многое другое. У вас есть возможность скачать то, что вам нужно без регистрации и абсолютно бесплатно. Мы стараемся сделать учебу более интересной. Ищете готовые домашние задания? Geo-gdz.ru – сайт, посетите его и погрузитесь в мир знаний. Наша онлайн библиотека предлагает материалы по практически всем предметам, включая географию и историю. На портале почитайте учебники и атласы. Картинки безупречного качества. Контурные карты можете уже сейчас на домашнем принтере распечатать.
CVzen https://cvpro.com.tr/ dünya çapında milyonlarca iş arayan için nihai CV yazma hizmeti ve kariyer koçudur. Uzman ekibimiz başarınıza kendini adamıştır ve profesyonel CV’nizi ve ön yazınızı sektörel özelliklerle yazmaktan LinkedIn profilinizi optimize etmeye ve profesyonel kariyer koçluğu sağlamaya kadar kariyer yolculuğunuz boyunca sizi destekleyecektir. Potansiyelinizi ortaya koyan bir özgeçmiş ile yeni fırsatların kilidini açın.
oneworldmiami.com
texasnewsjobs.com
На сайте https://yapolitical.ru вы сможете начать обсуждать различные политические новости, которые касаются не только России, но и ситуации во всем мире. Перейдите на форум, чтобы обсудить все текущие и самые интересные новости. При необходимости вы сможете добавить интересную и любопытную тему либо новость. Здесь вы сможете почитать информацию, которая касается иноагентов. Есть и другие любопытные материалы, которые точно вам понравятся своей достоверностью, актуальностью. Регулярно добавляются новые темы.
These https://inspirereklam.com.tr/ delineate but a trifling sampling of the manifold perils inherent in selecting an unsuitable broker. Hence, prospective traders are urged to invest due diligence in perusing broker credentials, scrutinizing contracts, and seeking counsel from seasoned peers. May fortune favor the discerning, guiding them towards the beacon of the most reliable brokerage alliance.
КапиталСтройАльянс – надежная компания, которая успешно занимается производством и установкой окон. Мы гордимся своей отменной репутацией в этой области. Гарантируем быструю доставку готовой продукции, высокую степень точности изделия без брака и оперативные сроки производства. Ищете заказать пластиковые окна от производителя недорого? Oknaksa.ru – здесь у вас есть возможность уже сегодня ознакомиться с отзывами и выполненными нами работами. Если у вас возникнут вопросы, обращайтесь, с радостью проконсультируем и подберем оптимальные варианты. Будем рады видеть вас среди наших клиентов!
На сайте https://animalchic.ru/ почитайте актуальные, свежие данные, которые касаются животных. Только здесь представлены самые свежие, содержательные факты, интересные сведения. Есть статьи о млекопитающих, птицах, насекомых, рыбах и многом другом. Вы узнаете много нового о тиграх, львах, форели. Все материалы составлены высококлассными авторами, которые разбираются в такой теме. Если хотите узнать данные об определенном животном, то вбейте название в специальный поиск. Перед вами возникнет вся нужная информация.
As soon as you begin to study 214rentals.com working in texts and popular Word editors, you can classify this problem as identifying empty extra sheets.
На сайте https://zso-k.ru/ подберите готовые уникальные решения, предназначенные для коммуникаций, инженерных систем. Компания в течение длительного времени специализируется на производстве резервуаров стальных, а также пожарных. В компании трудятся компетентные, квалифицированные специалисты с огромным опытом. Именно поэтому гарантируется безупречное качество работ, а также признание клиентов. Все условия договора тщательно соблюдаются, а потому точно не будет сюрпризов. Специалисты всегда находятся на связи, поэтому обязательно ответят на любые вопросы, дадут исчерпывающую консультацию.
Plates can have various technical parameters fla-real-property.com, among which when choosing it is worth highlighting: cost of the product, manufacturer and purpose.
Ленточные конвейеры https://euroconveyor-st.ru/product/konvejery/konvejery-lentochnye/gorizontalnyj-lentochnyj/ играют ключевую роль в автоматизации производственных процессов. Они обеспечивают бесперебойную и быструю транспортировку материалов и товаров, улучшая эффективность линий переработки, сборки, упаковки сырья и готовых изделий. Простота интеграции в сложные системы делает их незаменимыми в различных отраслях, от пищевой до горно-металлургической промышленности.
факультеты машерова витебск
As for relative height, it is italy-cars.com usually measured in meters. Moreover, it is worth noting that it is this that will show the difference between the absolute height of a geographical object, as well as the height of the surrounding area. If the mountain has an absolute height of 2000 meters, but the surrounding area is at an altitude of 1000 meters, then as for the relative height of the mountain, it is 1000 meters.
кондиционеры в казани
Автомобильный технический центр АвтоМеханика https://automehanika.by/ в Минске это качественный ремонт пневмоподвески и диагностика неисправностей, замена блока клапанов, замена и продажа датчиков положения кузова, ремонт компрессоров пневмоподвески и многое другое. Обращайтесь к профессионалам!
Вам интересны карты всех штатов США с достопримечательностями и известными городами? East-usa.com – здесь есть то, что вам действительно необходимо! Подробная туристическая карта позволит спланировать свое путешествие и сориентироваться на местности. Ищете map of us? East-usa.com – сайт, где имеется карта, на которой показаны невероятные места. Они могут быть еще и полезными для вас. У вас есть возможность узнать об объектах, о который вы ни разу не слышали. Карты дорог оптимизированы для просмотра на настольных компьютерах и мобильных устройствах.
A medical ophthalmologist at MCI Clinic is your reliable assistant in eye care. Our specialists undergo regular training and use advanced diagnostic and treatment methods for eye diseases. At MCI, you will receive qualified help with any vision problems, whether it be myopia, hyperopia, or astigmatism.
We are proud of our medical ophthalmologists who are always ready to provide professional assistance and valuable eye care recommendations. Schedule an appointment and experience the quality of medical services at MCI, where your vision is our top priority.
MCI Clinic – miopie
FX broker https://linuxakademi.com.tr/ rating is a treasure trove of insights for traders. These ratings are based on user feedback, meticulous analysis of trading conditions, and the security of funds. Make sure to check them out when selecting a trusted and dependable partner for your journey towards winning trades.
CVzen https://cvzen.nl/ is de ultieme CV schrijfservice en carrièrecoach voor miljoenen werkzoekenden over de hele wereld. Ons team van experts is toegewijd aan uw succes en zal u ondersteunen tijdens uw hele carrièrepad, van het schrijven van uw professionele CV en sollicitatiebrief met branchespecifieke informatie tot het optimaliseren van uw LinkedIn-profiel en het bieden van professionele carrièrecoaching. Ontsluit nieuwe kansen met een cv waarin je potentieel tot zijn recht komt.
CVzen e o melhor servico https://cvpro.pt/ de redacao de curriculos e coach de carreira para milhoes de candidatos a emprego em todo o mundo. A nossa equipa de especialistas esta empenhada no seu sucesso e ira apoia-lo ao longo de toda a sua carreira, desde a elaboracao do seu CV profissional e carta de apresentacao com especificidades da industria ate a otimizacao do seu perfil no LinkedIn e ao fornecimento de coaching de carreira profissional. Desbloqueie novas oportunidades com um curriculo que mostre o seu potencial.
Зайдите на сайт https://piastrix.team/ и узнайте все об электронном кошельке Piastrix. Это российская разработка и помогает пользователям проводить и получать платежи в азартных играх. Узнайте подробно на сайте как зарегистрировать кошелек Пиастрикс и как им пользоваться, как пополнить и всех прочих преимуществах платежной системы Piastrix.
Информационный проект KreditBaza.ru посвящен банкам и банковским услугам. Здесь имеются такие разделы: займы, кредиты, дебетовые и кредитные карты, РКО. У нас собраны самые лучшие предложения. Выбирайте подходящее, и заполняйте онлайн анкету. Ищете займ с низской ставкой? Kreditbaza.ru – сайт, где найдете статьи, которые помогут разобраться в банковских продуктах и повысить финансовую грамотность. Вы узнаете, нужно ли брать займ и другое. Предлагаем только достоверную информацию, посмотрите ее уже сейчас.
geinoutime.com
Hongzhi 황제는 서두르지 않고 침착하게 “앉아”라고 말했습니다.
vevobahis581.com
coloradonewss.com
На сайте https://imperiasinteza.com оставьте заявку для того, чтобы воспользоваться такой популярной, нужной услугой, как продвижение сайтов в РФ и РБ. При этом оптимизация происходит с очень высокой скоростью, на профессиональном уровне. Огромный выбор самых разных услуг, подобранных с учетом индивидуальных особенностей. Работы обязательно принесут необходимые результаты. Все они выполняются качественно, на профессиональном уровне. Специалисты работают давно, а потому у них огромный опыт.
NEMALYARKA – компания, которая предоставляет профессиональные услуги по отделке и ремонту. Мы с радостью сделаем вам малярные работы. Мы знаем свою работу, нам доверились уже многие Калужане и не пожалели об этом. https://nemalyarka.ru/ – сайт, где можете прямо сейчас оставить заявку. Также тут вы найдете интересные статьи. Покраска стен, шпаклевка q4 – все это умеем. Осуществим даже самые сложные проекты, от которых отказались другие. Свяжитесь с нами для консультации, ответим на вопросы и реализуем любые желания. Всегда рады вашим предложениям!
На сайте https://cdmebel.ru/ вы сможете заказать производство недорогой мебели высокого качества: для персонала, руководителя, для ресепшн. Также можно приобрести надежные, практичные стулья, кресла. Имеются и кухни, которые созданы для офисов. Вся мебель создается в соответствии с самыми последними технологиями и с учетом требований по дизайну. Компания отличается собственным современным производством. Любое пространство будет оснащено качественной мебелью. Сроки поставки являются минимальными.
ремонт смартфонов в москве
Myopia treatment at MCI Clinic offers various options to correct nearsightedness and improve vision. Our experienced doctors use precise diagnostic tools to determine the severity of myopia and suggest the best corrective measures. These can include prescription glasses, contact lenses, or refractive surgery such as LASIK. Each solution is customized to provide the best results for the patient.
Choosing MCI for myopia treatment means receiving professional and dedicated care aimed at enhancing your eyesight. Our commitment is to ensure you achieve clear vision and maintain eye health through effective and personalized treatment plans.
MCI Clinic – офтальмолог
Линкей Лайт – интернет-магазин, который приглашает вас сделать выгодные покупки. У нас вы можете купить по доступной цене качественный кронштейн. Гарантируем оперативную доставку. Ищете поворотный кронштейн недорого? Linkey-light.ru/catalog/komplektuyushchie/kronshteyny_krepleniya_/kronshteyn_povorotnyy_kp_60_dlya_lineynykh_svetilnikov – здесь имеется кронштейн поворотный КП-60, предназначенный для линейных светильников, чтобы его приобрести, оформите на сайте заявку. Также можете позвонить по телефону нашего магазина. Мы всегда готовы проконсультировать вас.
Destruam предоставляет для вас большой выбор сериалов. Все они захватывают уже с первых минут. Можете пригласить своих друзей, собрать семью вместе и наслаждаться новинками фильмов в полной мере. Гарантируем отменный звук и оперативную загрузку видео. Ищете смотреть бесплатно сериалы онлайн? Destruam.xyz – известный портал, где представлены сериалы, которые увлекут сюжетными поворотами и неожиданными событиями. Разнообразие и качество контента на высоком уровне. Смотрите без утомительной процедуры регистрации интересные сериалы. Сделайте свой вечер веселым!
Наши изготовление навесов цены – это идеальное решение для вашего авто.
Metal structures must be produced newmexicodesign.net under strict quality control. Absolutely all work is checked – from the manufacture of elements to final assembly. It is necessary to check their size, strength, coating and other parameters.
Complex work requires experience chicago-job.com and the use of modern equipment using strong chemicals. Not every person has such an arsenal available.
качественный сервис выполняет ремонт электроники варочных панелей в Москве. Сотни раз обращался, все отремонтировали качественно!
Восторг, удивление, радость и благодарность – эти эмоции стоят того, чтобы дарить что-то невероятное! У нас есть денежные карточки, аксессуары для медового месяца, папка со сладостями и многое др. https://boorsch.ru/ – сайт, где есть возможность найти множество интересных идей, а также получить удовольствие от подарка, который сотворит сам автор своими руками! Все очень просто: больше не нужно ждать доставку и переплачивать. Вы на электронную почту получите шаблоны, напечатаете и сами сделаете подарок, читая инструкцию. Пусть твой сюрприз станет ярким проявлением заботы и внимания!
https://gogocasino.one
The finished metal alabama-news.com structure must be properly packaged. Thanks to this, it will definitely not be damaged during transportation.
CVzen est le service https://cvzen.fr/ ultime de rédaction de CV et de coaching de carrière pour des millions de chercheurs d’emploi à travers le monde. Notre équipe d’experts s’engage à votre réussite et vous accompagne tout au long de votre parcours professionnel, de la rédaction de votre CV professionnel et de votre lettre de motivation avec des spécificités sectorielles à l’optimisation de votre profil LinkedIn en passant par le coaching professionnel de carrière. Débloquez de nouvelles opportunités avec un CV qui met en valeur votre potentiel.
business-exclusive.com
Посетите сайт https://videoline.spb.ru/ и вы сможете подобрать систему видеонаблюдения, а также заказать услуги по установке видеонаблюдения Спб. Ознакомьтесь с каталогом товаров. Установка видеонаблюдения и монтаж системы выполняются по ГОСТУ, обязательна гарантия с нашей стороны. Установка видеонаблюдения в СПб от Компании Видео Линия – это услуги от профессионалов, быстрые сроки, выгодные цены!
Казино Taker является самым стабильным и предлагает отличную возможность заработать хорошие деньги. Условия здесь наиболее выгодные, а разнообразие игр нереально впечатляет. Ищете taker официальный сайт? Taker.blog – сайт, который дает возможность отдохнуть от различных проблем. Можете разнообразить свой досуг уже сейчас. Безпроблемные выплаты улучшают игровой процесс. Уверены в том, что вы будете полностью удовлетворены Taker. Саппорт желает вам удачи и оперативно отвечает на любые вопросы. Тейкер – надежный выбор!
Ищете быстрый способ получить деньги? Подпишитесь на телеграм-канал мфо которые дают деньги ! Здесь собраны МФО, которые выдают деньги без отказов и проверки кредитной истории. Первый займ под 0% до 15 000 рублей всего за 10 минут! Также у нас есть списки новых МФО 2024 года, выдающих мгновенные микрозаймы даже с плохой кредитной историей и просрочками. Вступайте и решайте свои финансовые проблемы без задержек!
Protect your sight with glaucoma surgery at MCI Clinic! Our dedicated specialists are experts in managing glaucoma, offering advanced surgical options to control intraocular pressure and prevent vision loss. We use the latest technology and personalized treatment plans to ensure effective results. With MCI, you receive exceptional care at competitive prices.
Trust MCI Clinic for your glaucoma surgery and maintain clear, healthy vision. Our commitment to excellence and patient well-being ensures you receive the highest quality treatment, safeguarding your eyes for the future.
MCI Clinic – operatia miopie
CVzen https://cvzen.it/ è il servizio di scrittura di CV e career coach per eccellenza per milioni di persone in cerca di lavoro in tutto il mondo. Il nostro team di esperti si impegna per il vostro successo e vi supporterà in tutto il vostro percorso professionale, dalla stesura di un CV professionale e di una lettera di presentazione specifica per il settore, all’ottimizzazione del vostro profilo LinkedIn, fino al career coaching professionale. Sbloccate nuove opportunità con un curriculum che metta in luce il vostro potenziale.
Conventionally, forklifts can be divided alcitynews.com into manual and self-propelled. The manual version must be moved by the operator, which may require some effort if the weight of the load exceeds a thousand kilograms. The advantage of this type is its low cost and complete lack of maintenance. However, such a loader will not lift the load to too great a height.
nebrdecor.com
девочки москвы метро – девочки москвы метро, девочки по вызову москве
На сайте https://gdz-history.ru/ изучите атласы, а также контурные карты по истории 6,5, 7, 8, 9, 10 классов. Есть возможность не только скачать, но и почитать в режиме реального времени. Делайте так, как удобно именно вам. Распечатайте чистые контурные карты по такой дисциплине, как история. Все материалы помогут вам получить необходимые знания, повысить уровень интеллекта. Теперь и вы сможете сдать предмет на высокий балл. Скачивайте информацию тогда, когда вам удобно и в любое время. На портале представлены и тезисы для ознакомления с темами.
Хотите в отменном качестве и совершенно бесплатно смотреть увлекательные сериалы? Mixtios вам в этом поможет. Здесь вы найдете самое лучшее кино. Вы можете в любое удобное время смотреть фильмы. Ищете в двух шагах от счастья сериал 2024 смотреть онлайн ? Mixtios.xyz – сайт, где представлены сериалы, помогающие ощутить множество положительных эмоций и отвлекающие от повседневной жизни. Профессиональное озвучивание и отменное качество изображения гарантируют великолепный просмотр. Уверены, что у нас найдете для себя то, что вам понравится!
look at this web-site Retirement planning
мега – мега тор, мега ссылка
dublindecor.net
elitecolumbia.com
На сайте https://cliningkrd.ru закажите звонок для того, чтобы воспользоваться услугами клинингового агентства «Cleaning». В компании трудятся исключительно квалифицированные, компетентные сотрудники, которые не только обучены, но и постоянно повышают квалификацию на специальных курсах. В работе используются инновационные и высокотехнологичные расходные материалы, которые и позволяют получить безупречный результат. Есть возможность вызвать бригаду специалистов в любое время.
Хотите прекрасно провести вечер и расслабиться? Онлайн-казино поможет вам в этом. Taker привлекает игроков захватывающими слотами. Ищете taker официальный сайт? Taker.website – сайт, который сделан хорошо, разбираться, что здесь к чему и где находится, не придется. Сыграть здесь можно во что угодно. Главное то, что тут есть возможность реально выиграть крупные деньги. Выплаты осуществляются без задержек, и это радует. Саппорт лояльный, отвечает на все вопросы быстро. Почувствуйте сами все достоинства отменного отдыха вместе с Такер!
北斗の拳-ボクシング王 (2発1)
実用性に富んだ記事で、非常に感謝しています。
MCI Clinic specializes in astigmatism treatment, promising excellent results and improved vision. Our skilled professionals utilize state-of-the-art diagnostic tools to assess and correct astigmatism accurately. We offer personalized treatment options, such as glasses, contact lenses, and refractive surgery, to suit your unique requirements.
With MCI, you can be confident that your vision problems will be effectively addressed. Our dedication to providing high-quality, affordable care ensures that you achieve clear and sharp vision, enhancing your overall quality of life.
MCI Clinic – близорукость
Here you will learn about the apartusa365.com advantages of forklifts, as well as their types and applications. You may also be interested in the opportunity to purchase warehouse equipment.
Myopia treatment at MCI Clinic offers various options to correct nearsightedness and improve vision. Our experienced doctors use precise diagnostic tools to determine the severity of myopia and suggest the best corrective measures. These can include prescription glasses, contact lenses, or refractive surgery such as LASIK. Each solution is customized to provide the best results for the patient.
Choosing MCI for myopia treatment means receiving professional and dedicated care aimed at enhancing your eyesight. Our commitment is to ensure you achieve clear vision and maintain eye health through effective and personalized treatment plans.
MCI Clinic – астигматизм
Hello! Do you know if they make any plugins
to assist with SEO? I’m trying to get my blog to
rank for some targeted keywords but I’m not seeing very good success.
If you know of any please share. Thanks!
MCI Clinic offers exceptional glaucoma treatment, leveraging our vast experience, cutting-edge technology, and competitive pricing. Our specialists are adept at early diagnosis and management of glaucoma, using advanced techniques to control intraocular pressure and prevent vision loss. We provide comprehensive care, including medication, laser therapy, and surgical options tailored to each patient’s needs.
With MCI, you receive expert glaucoma care without breaking the bank. Our dedication to patient well-being and advanced treatment methods ensure you maintain optimal eye health and vision. Trust MCI for high-quality, affordable glaucoma treatment.
MCI Clinic – tratamentul cataractei
купить кухню из массива дуба
mega tor – m3ga.at, mega onion
alanews24.com
KRAKEN официальный сайт – KRAKEN через tor, kraken onion ссылка
Проведем СОУТ в Москве safetysystemsgroup.com
Организация Safety Systems проводит спец оценку условий труда на любом предприятии. Наш основной офис находится в Москве, но также в большинстве регионов РФ у нас есть филиалы. СОУТ осуществляется в обязательном порядке для всех фирм, чтобы обеспечить безопасность для сотрудников и убавить шансы на получение штрафов.
По вопросу соут стоимость одного рабочего заходите на наш онлайн ресурс. Оценочные события должны осуществляться в организациях не реже, чем раз в 5 лет. Но еще у особых отраслей есть индивидуальные сроки. Непременно ознакомьтесь с тем, что нужно именно Вам на сайте safetysystemsgroup.com прямо сейчас.
Ищете надежный способ получить деньги без отказа? Добро пожаловать в телеграм-канал какие мфо дают деньги всем подряд без исключения ! У нас собраны МФО, которые дают деньги без проверки кредитной истории. Первый займ под 0% до 15 000 рублей за 10 минут! В канале представлены новые МФО 2024 года, которые выдают мгновенные микрозаймы даже при плохой кредитной истории и просрочках. Подпишитесь и получайте деньги без проблем и ожиданий!
Хотите получить займ без отказа? Подпишитесь на телеграм-канал займы где дают всем ! Мы собрали для вас лучшие МФО, выдающие деньги без проверки кредитной истории. Первый займ под 0% до 15 000 рублей за 10 минут! Также у нас есть списки новых МФО 2024 года, которые предлагают мгновенные микрозаймы даже с плохой кредитной историей и просрочками. Присоединяйтесь к нашему каналу и забудьте о финансовых трудностях!
площадка мега даркнет – как зайти на mega, mega ссылка tor
Ищете надежное место для получения займа? Присоединяйтесь к нашему телеграм-каналу займы где одобряют всем форум ! У нас собраны МФО, которые выдают деньги без отказов и проверки кредитной истории. Получите первый займ под 0% до 15 000 рублей всего за 10 минут! Также в канале вы найдете списки новых МФО 2024 года, где можно получить мгновенные микрозаймы даже при плохой кредитной истории и просрочках. Вступайте и решайте свои финансовые проблемы!
geinoutime.com
Fang Zhengqing은 Zhu Zaimo를 위로하는 것처럼 서둘러 Zhu Zaimo의 작은 손을 꽉 쥐었습니다.
mega sb официальный – mega sb ссылка на сайт, mega sb tor
Taker – казино, которое обеспечивает безопасность и честность игры. Такер привлекает игроков занимательными слотами, онлайн-казино постоянно предоставляет выгодные бонусы и акции. Саппорт отзывчивый, работает оперативно и вежливо, вывод средств – быстрый. Ищете taker casino? Taker.bond – сайт, дизайн его превосходный, с навигацией сложностей не возникнет. Если вы решили посетить Taker casino, вам повезло, потому что здесь представлен впечатлительный выбор азартных игр. Скучать вам здесь не придется. Испытайте удачу прямо сейчас!
Use protective devices, use tools real-apartment.com and equipment according to the rules so as not to come into contact with difficulties.
kraken зеркало – kraken ссылка, кракен ссылка
Owners usually cope with homadeas.com superficial maintenance of the premises on their own, but general cleaning can cause difficulties.
affordable cash loans north augusta No, paydays loans are an excellent alternative to conventional loans in many instances.
Стоимость оценки условий труда safetysystemsgroup.com
Фирма Safety Systems реализует специальную оценку условий труда на каждом предприятии. Наш главный офис находится в Москве, но ещё в большинстве городов РФ у нас есть филиалы. Проверка проводится в обязательном порядке для всех компаний, чтобы снабдить безопасность для работников и уменьшить шансы на получение штрафов.
По поводу специальная оценка условий труда заказать заходите на наш веб портал. Оценочные события должны осуществляться в организациях не реже, чем раз в пять лет. Но также у особых отраслей есть собственные сроки. Обязательно ознакомьтесь с тем, что нужно именно Вам на сайте safetysystemsgroup.com уже сейчас.
Ваша посудомоечная машина Bosch не работает как раньше? Наши специалисты готовы выполнить ремонт посудомоечных машин Bosch быстро и надежно. Мы используем только оригинальные запчасти и предоставляем гарантию на все виды работ.Если ваш духовой шкаф вышел из строя, мы предлагаем профессиональный ремонт духовых шкафов в Москве. Бесплатная диагностика, ремонт на дому и гарантия 1 год обеспечат надежную работу вашей техники. Наши опытные мастера используют только оригинальные запчасти.
Оформление специальной оценки условий труда safetysystemsgroup.com
Организация Safety Systems осуществляет спец оценку условий труда на любом предприятии. Наш основной офис находится в Москве, но ещё в большинстве регионов России у нас имеются филиалы. СОУТ проводится в обязательном порядке для всех компаний, чтобы обеспечить безопасность для сотрудников и убавить шансы на приобретение штрафов.
В отношении внеочередная соут заходите на наш онлайн ресурс. Оценочные мероприятие должны проходить в компаниях не реже, чем раз в 5 лет. Но также у отдельных отраслей есть индивидуальные сроки. Обязательно ознакомьтесь с тем, что нужно именно Вам на сайте safetysystemsgroup.com уже сейчас.
1вин
here What is the sandbox
best cash advance 90040 Repayment of this type of loan is supposed to be done in a short time, hence the name, short term.
DLE модификации – WordPress, XenForo модификации
Taker – прекрасное онлайн-казино, достойное вашего внимания. Оно игроков завлекает интересными слотами, регулярно предоставляет щедрые бонусы и акции. Вывод средств осуществляется быстро, техподдержка доброжелательная, работает оперативно. Ищете taker casino? Taker.vin – сайт, у которого отменный дизайн и удобная навигация, трудностей с пользованием не будет. Если вы решили зайти на Такер, то сделали все правильно, здесь вам будет предложен широкий ассортимент лучших азартных игр. Скучно вам не будет. Испытайте удачу уже сейчас!
california-invest.com
Maximum effect from the greeceholidaytravel.com cleaning measures carried out. Professional employees will cope with pollution of any complexity and type of origin.
На сайте https://autopiter.ru/ представлены оригинальные, неоригинальные запчасти, каталоги ГАЗ, ВАЗ, автохимия, автомасла наиболее популярных, практичных брендов, которые доказали свою надежность. Также представлены и аккумуляторы, все для спецтехники. А если хотите подобрать что-то определенное, то воспользуйтесь специальным поиском. Все автомасла, которые находятся в каталоге, отличаются гарантией качества. Обязательно посетите раздел с рекомендуемыми товарами. Все заказы доставляются максимально быстро.
Ваша кофемашина Bosch перестала работать? Не отказывайтесь от утреннего кофе! Мы предлагаем профессиональный ремонт кофемашин Bosch на дому. Наши специалисты быстро диагностируют проблему и устранят неисправность, используя оригинальные запчасти.Если ваша сушильная машина вышла из строя, мы предлагаем профессиональный ремонт сушильных машин в Москве. Бесплатная диагностика, ремонт на дому и гарантия 1 год — наш стандарт качества.
It is necessary to work carefully flarealestates.com and accurately when manufacturing metal structure parts. Even minimal mistakes lead to serious problems in the future.
Если вам нужно легализовать документы для использования за границей, вы можете легко заказать апостиль у нас. Мы предлагаем быструю и надежную услугу, чтобы ваши документы были готовы в кратчайшие сроки.
Для тех, кто нуждается в официальном признании документов за рубежом, мы предоставляем полный спектр услуг, включая перевод и апостиль документов. Наши специалисты помогут вам быстро и качественно оформить все необходимые бумаги.
Если вам требуется апостиль документов, наша компания готова помочь вам в этом вопросе. Мы обеспечим юридическую силу ваших документов за границей, оперативно и профессионально выполнив все процедуры.
Чтобы ваше свидетельство о рождении было признано в других странах, вам необходим апостиль на свидетельство о рождении. Мы гарантируем точное и своевременное выполнение этой услуги, чтобы вы могли без проблем использовать документ за границей.
https://apostil-yaziki.ru/
Сайт fermerstvo.in.ua пользуется повышенной популярностью. Здесь вы найдете актуальную информацию. С ней можете ознакомиться в любое удобное время. fermerstvo.in.ua – https://fermerstvo.in.ua сайт, где узнаете с чего начать фермерское хозяйство. Мы открыто делимся своими неудачами и успехами. Разбираем, как подготовиться к разведению домашней птицы. Рассказываем, как повысить урожайность овощей. У нас вы найдете ответы на необходимые вопросы. Делаем понятный контент. Вы получите обширные знания о том, что имеет отношение к фермерскому хозяйству.
new american financial You get a time period of 7 to 30 days to repay the loan, and the time frame is kept in such a way that you can pay off the loan whenever you get your pay check.
homesimprovement.net
Специальная оценка условий труда safetysystemsgroup.com
Компания Safety Systems осуществляет специальную оценку условий труда на каждом предприятии. Наш главный офис расположен в Москве, но ещё в большинстве регионов РФ у нас есть филиалы. СОУТ проводится в обязательном порядке для всех фирм, чтобы обеспечить безопасность для сотрудников и сократить шансы на приобретение штрафов.
От нас мероприятия по оценке условий труда – от Вас звонок в нашу фирму. Расположены по адресу: 105264, г. Москва, ул. Верхняя Первомайская, д. 47, к. 11, оф. 516. У нас собственная аккредитованная лаборатория, которая поможет Вам сэкономить до 80 % от конкурентной цены. Звоните, обращайтесь и мы Вам обязательно поможем.
Зайдите на сайт https://coffeeroom.by/ и вы сможете купить кофе лучших брендов мировых производителей с быстрой доставкой в Минске. Зерновой кофе, молотый кофе, степень обжарки, варианты по цене – все это вы найдете в поиске. А наша новая услуга аренда кофемашины позволит вам наслаждаться напитком каждый день.
На сайте https://t.me/s/mleon_ru изучите всю необходимую информацию про популярное заведение «LEON». Если вам не нравятся банальные, обычные ставки, то эта контора откроет для вас новые, положительные эмоции, о которых вы еще не знали. Принимаются ставки на самые разные игры, спортивные состязания, которые точно никого не оставят равнодушным. Только для вас комфортный, максимально простой и понятный интерфейс, который поможет правильно управлять процессом. Сыграйте по-крупному и заработайте отличный выигрыш и вы!
На сайте https://oboinastene.ru/ почитайте информацию об обоях. Вы узнаете об их видах, особенностях, преимуществах, использовании в интерьере. Кроме того, есть информация о том, как их правильно клеить, чтобы они красиво выглядели в течение долгого времени. Есть данные о ремонте кровли, о том, как правильно его выполнять. Все обои различаются между собой не только цветовой гаммой, но и фактурой, а также типом поверхности, текстурой и другими особенностями. Есть информация и об автоматических выключателях ДКС.
арочный шатер цена
Considering how busy most bestchicago.net people are, cleaning services have gained high popularity. There are several types of cleaning: daily, cleaning the apartment after renovation, cleaning by zone and others. Owners usually cope with superficial maintenance of the premises on their own, but general cleaning can cause difficulties.
The term “ticket” often refers repairtoday7.com to a support request. It is the ticket that guarantees a person that his problem will be quickly resolved. A high-quality ticket system for technical support will allow a business to gain many benefits. Let’s look at such innovations in more detail.
Alptracking осуществляет аренду надежного и высококачественного туристического снаряжения. У нас есть рюкзаки, палатки, треккинговые палки, матрасы и коврики, спальные мешки и многое другое. Весь ассортимент снаряжения изучите, предварительно скачав на нашем сайте прайс-лист. Ищете зимние маршруты на Байкале? Alptracking.ru – здесь у вас есть возможность уже сейчас ознакомиться с контактами, отзывами и условиями проката. Всегда рады ответить на все ваши вопросы и оформить аренду нужного снаряжения. Поможем вам путешествовать с комфортом!
fast cash in dragonvale Get help with everything from simply cashing a check to getting a loan.
Варочная панель Bosch не работает? Обратитесь к нам для ремонта варочных панелей. Мы предоставляем бесплатную диагностику, ремонт на дому и гарантию 1 год. Наши специалисты с многолетним опытом быстро устранят любые неисправности, используя оригинальные запчасти.Наша компания — лидер в Москве по ремонту стиральных машин Bosch. Мы предоставляем бесплатную диагностику и ремонт на дому. Опытные мастера используют только оригинальные запчасти, а на все работы дается гарантия 1 год.
sellrentcars.com
The service has collected on the usainvesttoday.com pages of its website all offers from tour operators in Moldova. Here you can find information for any tours to Egypt with departure from Chisinau, where you can select the number of travel participants, dates and travel options.
На сайте https://ax-card.ru/ закажите пластиковые карты для различных сфер деятельности. Их создают на инновационном, высокотехнологичном оборудовании компетентные специалисты с огромным опытом. Дополнительно они разработают макет, а при оказании услуги используют уникальные и инновационные технологии. Именно поэтому вы получите ожидаемый и прогнозируемый результат. Если вы заинтересовались услугой, то специально для вас может быть сделана пробная карта. Это абсолютно бесплатно.
### Смотреть русские сериалы
онлайн: удобство и разнообразие
В современном мире многие люди
выбирают смотреть русские сериалы
онлайн благодаря удобству и разнообразию контента.
Онлайн-платформы предлагают огромное количество сериалов различных жанров, от драм и комедий
до детективов и исторических эпопей.
**Преимущества онлайн-просмотра**
1. **Доступность**: Можно смотреть любимые сериалы в
любое время и в любом месте, достаточно иметь доступ к интернету.
2. **Разнообразие контента**: Платформы предлагают новинки и классические сериалы,
удовлетворяя вкусы всех зрителей.
3. **Качество**: Современные сервисы обеспечивают высокое
качество изображения и звука, что позволяет наслаждаться просмотром.
4. **Удобство**: Функции, такие как пауза и
перемотка, делают просмотр
ещё более удобным.
**Популярные жанры русских сериалов**
– **Драмы**: Эти сериалы затрагивают важные жизненные
темы, вызывая сильные эмоциональные
отклики.
– **Комедии**: Легкие и весёлые сюжеты, которые
поднимают настроение и позволяют
отвлечься от повседневных забот.
– **Детективы**: Интригующие истории с расследованиями, которые держат зрителей в напряжении
до самого конца.
– **Исторические сериалы**: Позволяют окунуться в прошлое,
узнавая больше о значимых событиях и личностях.
**Как выбрать платформу для просмотра?**
При выборе платформы для просмотра русских сериалов онлайн важно учитывать несколько факторов:
– **Библиотека контента**: Убедитесь,
что платформа предлагает широкий выбор
сериалов, включая новинки и классику.
– **Качество воспроизведения**:
Платформа должна поддерживать высокое качество видео.
– **Удобство интерфейса**:
Пользовательский интерфейс должен быть интуитивно понятным и удобным.
– **Стоимость**: Некоторые платформы предлагают бесплатный доступ, другие требуют
подписки. Выберите вариант, который соответствует вашему бюджету.
**Заключение**
Смотреть русские сериалы онлайн — это отличная возможность насладиться любимыми историями в удобное для вас время.
Благодаря разнообразию контента,
доступности и высокому качеству
современных онлайн-платформ, каждый зритель сможет
найти что-то по душе. Погружайтесь в мир русских сериалов
и наслаждайтесь увлекательными
сюжетами, не выходя из дома!
Feel free to visit my blog post: “https://toripedia.info/index.php/User:QuyenS862787318”
Groove inserts can be used to carsnow.net work with various types of metals and alloys, including the most durable and hard ones. A long service life and the ability to sharpen the cutting edges of tools are guaranteed.
Зайдите на сайт компании Финтех https://finteh.su/ которая специализируется на проектировании и строительстве каменных, деревянных, комбинированных и других домов под ключ. Подберите на сайте проект под себя или посмотрите готовые, типовые проекты. Привлекательные цены на строительство и акции от Финтех позволят вам построить качественный дом мечты!
To speed up the search according homeideascoach.com to the parameters most needed by tourists, the site page has a filter system that allows you to select tours based on the following indicators:
На сайте https://imperiasinteza.by оставьте заявку с той целью, чтобы воспользоваться услугами, связанными с логопедией, сенсорной интеграцией. Только для вас профессиональные услуги, консультации логопеда. В компании работает логопед-дефектолог для детей, можно воспользоваться сенсорной интеграцией. Специально для вас индивидуальные, а также групповые занятия, которые принесут должный эффект. При необходимости организуется выезд специалиста. Самая первая консультация предоставляется в подарок.
tradeusanews.com
戦国乙女~剣戟に舞う白き剣聖~西国参戦編(V2.2)
素晴らしい記事で、とてもインスピレーションを受けました。感謝しています。
For many people, a dacha and a country indiana-daily.com house are not just a place of work and life, but a place of permanent recreation. Therefore, on each site there should be a beautiful gazebo that provides shelter from bad weather and is simply a beautiful decoration. Among the large number of materials from which modern gazebos are decorated, wooden beams are worth special mention.
brant loans til payday hours If the bank granted the loan under fraudulent circumstances, the bank will void the loan.
### Смотреть русские сериалы онлайн
Русские сериалы пользуются
огромной популярностью среди зрителей
благодаря своей разнообразной тематике, качественной актерской игре и
захватывающим сюжетам. Сегодня у нас есть уникальная возможность наслаждаться лучшими русскими сериалами онлайн, не выходя из дома.
**Преимущества просмотра русских
сериалов онлайн**
1. **Доступность**. Онлайн-платформы предлагают огромный выбор русских сериалов, которые можно смотреть в любое время и
в любом месте. Это особенно удобно для тех, кто имеет
плотный график и не может подстраиваться под телевизионные трансляции.
2. **Бесплатность**. Множество сайтов предлагают бесплатный просмотр сериалов, что позволяет экономить
на подписках и кабельном
телевидении. Пользователи могут наслаждаться любимыми шоу без дополнительных затрат.
3. **Высокое качество**. Современные онлайн-платформы обеспечивают
высокое качество видео и звука, что позволяет наслаждаться сериалами в наилучшем качестве.
Многие сайты предлагают сериалы в формате HD и даже 4K.
4. **Разнообразие контента**. В интернете можно найти русские сериалы на
любой вкус: от классических
драм и комедий до современных детективов и фантастики.
Это позволяет каждому зрителю найти что-то по своему
вкусу.
**Популярные жанры русских сериалов**
– **Драмы**. Сериалы, основанные на глубоких человеческих историях, всегда находят отклик у зрителей.
Примеры: “Доктор Рихтер”, “Тест на беременность”.
– **Комедии**. Легкие и забавные
сериалы, которые поднимают настроение.
Примеры: “Кухня”, “Интерны”.
– **Детективы**. Захватывающие истории с расследованиями и неожиданными поворотами
сюжета. Примеры: “Мажор”, “След”.
– **Исторические**. Сериалы, рассказывающие о
важных событиях и личностях в истории России.
Примеры: “Екатерина”, “София”.
– **Фантастика и мистика**.
Увлекательные сюжеты с элементами фантастики и мистики.
Примеры: “Тайны следствия”, “Метод”.
**Где смотреть русские сериалы онлайн**
Существует множество платформ, предлагающих
просмотр русских сериалов онлайн.
.
Смотрите русские сериалы онлайн и
наслаждайтесь качественным контентом в удобное для вас время.
Это отличный способ расслабиться, получить
новые впечатления и узнать больше о современной русской культуре.
Here is my web-site – “http://designhanin.com/bbs/board.php?bo_table=free&wr_id=217293”
На сайте https://trart.ru/ почитайте информацию, которая касается психологии. Так вы узнаете о том, каким образом сохранить отношения после того, как рождается ребенок. Также рассказываются основные причины конфликтов между свекровью, невесткой. Опубликованы данные, которые касаются причин появления семейного кризиса. Вы узнаете о том, каким образом эффективней пережить измену. Вы узнаете о самых эффективных и рациональных методиках, которые помогут вернуть в отношения страсть.
carsnow.net
Working as a courier offers flexible hours as getusainvest.com one of the main benefits. An employee can work every day or every other day, the number of working hours is determined independently. The courier’s earnings directly depend on the number of completed orders.
greenhouseislands.com
Offering a large selection of products alahomemaster.com, the seller works directly with manufacturers, which allows keeping prices at a fairly low level, because the chain of intermediaries disappears.
If this is necessary, you should make northfloridahouse.com sure that the installation of the metal structure is carried out professionally. All instructions must be followed in practice.
Corporate culture plays an important role. The interests of clients italycarsrental.com are put first for every employee of the company; the area of responsibility does not play an important role. For example, help desks gain additional incentive when they realize that quickly resolving employee issues has an impact on customer service. If, for example, a software glitch is not fixed, the manager will not calculate the loan program for the client. As a result, he will share negative experiences with other people, so the company’s reputation will suffer.
Теневой плинтус: стильное решение для обновления интерьера,
Шаг за шагом инструкция по установке теневого плинтуса,
Креативные способы использования теневого плинтуса в дизайне помещения,
Теневой плинтус: классический стиль в современном исполнении,
Гармония оттенков: выбор цвета теневого плинтуса для любого интерьера,
Теневой плинтус: простое решение для скрытия кабелей и проводов,
Интересные решения с теневым плинтусом и подсветкой: идеи для вдохновения,
Современные тренды в использовании теневого плинтуса для уюта и красоты,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
плинтуса для пола https://plintus-tenevoj-aljuminievyj-msk.ru/ .
geinoutime.com
그런 다음 그는 Zhu Houzhao를 보았습니다. “왕자님, 이것에 대해 어떻게 생각하십니까?”
payday loans direct lenders only no brokers Hence, we will need the structure for understanding the same.
Духовой шкаф Bosch вышел из строя? Мы предлагаем профессиональный ремонт духовых шкафов на дому. Наши опытные специалисты проведут диагностику, заменят необходимые детали и вернут вашей технике полную функциональность. Мы используем только оригинальные запчасти.Обеспечьте надежность своей техники с помощью Бош сервис. Наши квалифицированные специалисты предоставляют профессиональное обслуживание и ремонт бытовых приборов Bosch. Мы гарантируем оперативность и качество выполнения всех работ, используя только оригинальные запчасти.
south-columbia.com
Заказать Вентилятор радиальный ВЦ 14-46 по оптовым ценам от завода производителя ООО Гевей можно на сайте https://vent-climate.ru/ Так же производим вентиляторы промышленные радиальные В
Наш Bosch сервисный центр в Москве предоставляет полный спектр услуг по ремонту бытовой техники. Бесплатная диагностика, ремонт на дому и гарантия 1 год — все это обеспечивает высокий уровень сервиса. Мы используем только оригинальные запчасти и работаем более 10 лет в сфере обслуживания техники Bosch.Наша компания специализируется на ремонте стиральных машин Bosch. Мы гарантируем высокое качество обслуживания и оперативное решение любых проблем с вашей техникой. Наши специалисты приедут на дом, проведут диагностику и устранят неисправности в кратчайшие сроки.
Преимущества теневого плинтуса в декорировании помещения,
Как правильно установить теневой плинтус своими руками,
Креативные способы использования теневого плинтуса в дизайне помещения,
Модные тренды в выборе теневых плинтусов для современного дома,
Гармония оттенков: выбор цвета теневого плинтуса для любого интерьера,
Безопасность и стиль: почему теневой плинтус – идеальное решение для дома,
Теневой плинтус с подсветкой: создаем эффектное освещение в интерьере,
Теневой плинтус: элегантность и стиль в дизайне помещения,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
плинтус скрытого монтажа https://plintus-tenevoj-aljuminievyj-msk.ru/ .
Теневой плинтус: стильное решение для обновления интерьера,
Шаг за шагом инструкция по установке теневого плинтуса,
Как использовать теневой плинтус для создания уникального интерьера,
Ретро-стиль с использованием теневых плинтусов: идеи для вдохновения,
Гармония оттенков: выбор цвета теневого плинтуса для любого интерьера,
Теневой плинтус: простое решение для скрытия кабелей и проводов,
Преимущества использования теневого плинтуса с интегрированной подсветкой,
Современные тренды в использовании теневого плинтуса для уюта и красоты,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
плинтус теневой плинтус теневой .
Search by Image on Amazon https://chromewebstore.google.com/detail/search-by-image-on-amazon/fmiialomjacaogdjjkgicepphmekndli uses advanced technology to provide users with a unique functionality. By analyzing images, the extension is able to search for relevant products. To use this feature, users can conveniently right-click on any image in their browser and select the “Search on Amazon” option.
Вам интересна прописка в Польше, г. Варшава? MIGRANT SUPPORT вам в этом поможет. Компания предоставляет качественные услуги. Гарантирует лояльные цены и персональный подход к каждому клиенту. У вас есть возможность получить квалифицированную консультационную поддержку по необходимым вопросам. https://vpolshe.com/propiska-v-polshe-g-varshava-dogovor-arendy-zhilya-varshava/ – сайт, где можно узнать, зачем нужна прописка (meldunek). Оставьте заявку на портале, и мы вам позвоним через некоторое время. Будем рады помочь с договором аренды жилья.
Ваш духовой шкаф Bosch не работает? Доверьте его нашим мастерам! Мы предоставляем ремонт духовых шкафов Bosch на высшем уровне. Используем оригинальные запчасти и новейшие технологии для быстрого и качественного восстановления вашей техники.Доверьте ремонт духового шкафа профессионалам! Наши специалисты с многолетним опытом предоставляют ремонт духовых шкафов в Москве. Бесплатная диагностика, ремонт на дому и гарантия 1 год обеспечат долгую работу вашей техники.
швеллер купить в леруа
оборудование хирургического отделения
The timber does not require carsdirecttoday.com special finishing or painting. If the timber is sufficiently dried, then this design will not shrink.
Всем привет, друзья! Желаю обсудить своими эмоциями о казино казино 777. Это место удивило меня своим выбором игр и богатыми бонусами. От классических слотов до интересных живых игр — здесь есть все для ценителей игры. Бонусы за регистрацию и депозиты радуют, делая игру еще более увлекательной. Мгновенные выплаты и профессиональная поддержка клиентов внушают уверенность. Предлагаю всем испытать здесь
На сайте https://aakkb.com.ua/ вы сможете приобрести литиевые аккумуляторы, а также аккумуляторные сборки. Все конструкции отличаются своей надежностью, безупречным качеством, а также идеальным исполнением. Все модели от проверенных, лучших брендов, которые работают на совесть. Перед вами огромное количество моделей, что позволит подобрать решение на свое устройство. А если затрудняетесь с выбором, то вас всегда поддержит высококлассный специалист. Он даст ценные советы, важные рекомендации.
chicagonewsblog.com
Нужны деньги срочно, но кредитная история оставляет желать лучшего? В Telegram-канале Займы с плохой КИ вы найдете онлайн займы без отказа. Получите нужную сумму на карту быстро и просто, даже с плохой кредитной историей. Подписывайтесь и решайте свои финансовые вопросы без лишних проблем!
Привет, друзья! Желаю обсудить своими ощущениями о казино р7 казино. Это заведение поразило меня своим ассортиментом игр и большими поощрениями. Начиная с классических слотов и заканчивая интересных живых игр — здесь всё имеется для ценителей игры. Бонусы при регистрации и на депозиты удивят, делая игру еще более увлекательной. Мгновенные выплаты и экспертная поддержка пользователей внушают уверенность. Предлагаю всем испытать здесь
ремонт телефонов поблизости
Не знаете, где взять деньги с плохой кредитной историей и просрочками? В нашем Telegram-канале Займы с плохой КИ собраны предложения от надежных кредиторов, которые не обращают внимания на прошлые ошибки. Получите займ быстро и без отказов, улучшите свое финансовое положение. Подписывайтесь и узнайте больше!
Здравствуйте, друзья! Желаю обсудить своими эмоциями о игровом зале cryptoboss casino. Это заведение впечатлило меня своим ассортиментом игр и щедрыми бонусами. Начиная с классических слотов и заканчивая увлекательных живых игр — здесь есть все для поклонников гемблинга. Бонусы при регистрации и на депозиты удивят, делая игру еще более увлекательной. Мгновенные выплаты и профессиональная поддержка клиентов внушают уверенность. Предлагаю всем попробовать здесь
If this is necessary, you should make carsnow.net sure that the installation of metal structures is carried out efficiently and professionally. All instructions should be followed by example.
Всем привет, товарищи! Решил обсудить своими эмоциями о казино вход в казино лев. Это заведение удивило меня своим выбором игр и щедрыми поощрениями. Начиная с классических слотов и заканчивая интересных живых игр — здесь все в наличии для поклонников гемблинга. Бонусы при регистрации и на депозиты порадуют, делая игру еще более увлекательной. Мгновенные выплаты и экспертная поддержка пользователей усиливают уверенность. Советую всем попробовать здесь
Всем привет, приятели! Хочу обсудить своим впечатлением о игровом клубе онлайн казино кент. Это место удивило меня своим ассортиментом игр и богатыми вознаграждениями. От традиционных слотов и до интересных живых игр — здесь есть все для любителей азарта. Бонусы за регистрацию и депозиты удивят, делая игру еще более увлекательной. Скоростные выплаты и квалифицированная поддержка клиентов внушают уверенность. Советую всем попробовать здесь
Думаете, займ с убитой кредитной историей недоступен? Вовсе нет! В Telegram-канале Займы с плохой КИ вы найдете предложения, которые помогут вам получить деньги даже в самых сложных ситуациях. Кредиторы готовы предоставить займ быстро и без отказов. Подписывайтесь и решите свои финансовые проблемы!
Теневой плинтус: стильное решение для обновления интерьера,
Шаг за шагом инструкция по установке теневого плинтуса,
Креативные способы использования теневого плинтуса в дизайне помещения,
Ретро-стиль с использованием теневых плинтусов: идеи для вдохновения,
Как подобрать цвет теневого плинтуса к отделке стен,
Теневой плинтус: простое решение для скрытия кабелей и проводов,
Преимущества использования теневого плинтуса с интегрированной подсветкой,
Теневой плинтус: элегантность и стиль в дизайне помещения,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
теневой плинтус для стен теневой плинтус для стен .
Всем привет, товарищи! Желаю обсудить своими ощущениями о казино вулкан автоматы. Это заведение поразило меня своим выбором игр и щедрыми поощрениями. От классических слотов до захватывающих живых игр — здесь все в наличии для ценителей игры. Бонусы при регистрации и на депозиты порадуют, сделав игру ещё интереснее. Мгновенные выплаты и профессиональная поддержка клиентов внушают уверенность. Советую всем попробовать здесь
Всем привет, приятели! Решил поделиться своими эмоциями о игровом зале dragonmoney казино. Это сайт поразило меня своим выбором игр и щедрыми поощрениями. От классических слотов до увлекательных живых игр — здесь всё имеется для любителей азарта. Бонусы за регистрацию и депозиты радуют, сделав игру ещё интереснее. Быстрые выплаты и квалифицированная поддержка клиентов добавляют уверенности. Рекомендую всем испытать здесь
Привет, товарищи! Решил обсудить своим впечатлением о игровом клубе kent casino вход. Это сайт впечатлило меня своим ассортиментом игр и богатыми поощрениями. Начиная с классических слотов и заканчивая интересных живых игр — здесь всё имеется для любителей азарта. Приветственные бонусы и бонусы на депозиты радуют, сделав игру ещё интереснее. Скоростные выплаты и профессиональная поддержка клиентов добавляют уверенности. Предлагаю всем попробовать здесь
Привет, приятели! Желаю поделиться своим впечатлением о игровом клубе 1xbet зеркало слоты. Это заведение впечатлило меня своим выбором игр и богатыми бонусами. Начиная с классических слотов и заканчивая увлекательных живых игр — здесь все в наличии для ценителей игры. Бонусы за регистрацию и депозиты порадуют, делая игру еще более увлекательной. Мгновенные выплаты и квалифицированная поддержка клиентов усиливают уверенность. Рекомендую всем испытать удачу здесь
оборудование реанимационного отделения
Клининг после смерти Москва https://prof-uborka-posle-smerti.ru/
На сайте https://omsksite.ru/ представлены самые эффективные, работающие методы выполнения ремонта. Этот блог посвящен строительным, ремонтным, отделочным работам. Вся информация является полезной, интересной. А самое главное, что позволит справиться с проблемой максимально быстро. На сайте будут рассказаны все тонкости ремонта и то, какие материалы для этих целей лучше использовать. Имеется контент на тему того, как правильно подобрать пластиковое окно. Есть информация про пожарную охрану, руководство, которое поможет правильно подобрать набор инструментов.
Всем привет, приятели! Желаю обсудить своими ощущениями о игровом зале bounty casino online. Это заведение удивило меня своим выбором игр и богатыми поощрениями. Начиная с классических слотов и заканчивая захватывающих живых игр — здесь всё имеется для ценителей игры. Бонусы за регистрацию и депозиты радуют, добавляя игре увлекательности. Быстрые выплаты и профессиональная поддержка клиентов добавляют уверенности. Предлагаю всем попробовать здесь
Теневой плинтус: стильное решение для обновления интерьера,
Советы по монтажу теневого плинтуса без дополнительной помощи,
Креативные способы использования теневого плинтуса в дизайне помещения,
Модные тренды в выборе теневых плинтусов для современного дома,
Советы стилиста: как сделать цвет теневого плинтуса акцентом в помещении,
Безопасность и стиль: почему теневой плинтус – идеальное решение для дома,
Теневой плинтус с подсветкой: создаем эффектное освещение в интерьере,
Как сделать помещение завершенным с помощью теневого плинтуса,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
плинтус черный алюминиевый https://plintus-tenevoj-aljuminievyj-msk.ru/ .
Всем привет, товарищи! Желаю обсудить своим впечатлением о игровом зале casino rubin stavka. Это место поразило меня своим выбором игр и большими вознаграждениями. От классических слотов до интересных живых игр — здесь все в наличии для ценителей игры. Приветственные бонусы и бонусы на депозиты удивят, делая игру еще более увлекательной. Мгновенные выплаты и квалифицированная поддержка клиентов добавляют уверенности. Рекомендую всем попробовать здесь
payday loan google update A recent bill proposed to Missouri’s congress suggests more time to pay the loans back and a low cap on the interest rates.
The main advantage of a forklift is its chinanewsapp.com versatility and ease of use. Essentially, it is just a trolley with a durable fork that can be used to lift pallets or large loads to any height. It is worth noting that the loader can be made in the form of a trolley with no traction of its own, or in the form of an electric/gasoline self-propelled vehicle, with the help of which extremely heavy objects can be transported over impressive distances throughout the warehouse. Another advantage is simple maintenance, which is ensured by the absence of technical bells and whistles, but this depends on the specific model of the device.
ремонт телефонов в москве
На сайте https://imperiafohow.by оставьте заявку для того, чтобы воспользоваться услугой массажа. Вы почувствуете заботу о своем теле, полное расслабление и уход. Все массажисты являются компетентными, квалифицированными специалистами с огромным опытом. Все их движения максимально мягкие, приятные и деликатные, а потому вы почувствуете расслабление и негу. Используется косметика популярных, надежных брендов, которые работают на совесть. Но с той целью, чтобы достичь нужных результатов, следует ответственно подходить к оказанию услуги.
Depending on the type of transport the travelusanews.com courier will use, the restrictions on the weight and dimensions of the transported parcels vary.
Electric Motor Balancing: Una especialidad de Vibromera
Благодарствую за отличную информацию!
В свою очередь предлагаю сыграть на настоящие деньги!
игровые автоматы играть регистрация вавада — быстро и просто. Это позволит вам получить доступ к к огромному количеству слотов и рулетке.
Зарегистрировавшись вы войдете в свой личный кабинет и начать играть. Обратите внимание, что для вывода выигранных денег вам необходимо будет пройти верификацию аккаунта, предоставив документы.
На сайте https://ruuserial.net/ находятся русские сериалы, которые точно вам понравятся, ведь в них играют самые популярные актеры. Они донесут до вас сюжет фильма так, чтобы вы прочувствовались. Есть фильмы самых разных жанров, в том числе, комедии, триллеры, мелодрамы, драмы и многое другое. Все фильмы в хорошем качестве, помогают вникнуть в истории и получить приятные эмоции. Обрадует и музыкальное сопровождение. Можно подыскать вариант по году выпуска. Постоянно происходит обновление кино.
livinghawaiitravel.com
k8 カジノ 退会
素晴らしい記事!とてもインスピレーションを受けました。
Conseils de dГ©pannage pour l’Г©quilibrage avec des supports souples Balancing with Soft Supports
На сайте https://vpolshe.com/propiska-v-polshe-g-varshava-dogovor-arendy-zhilya-varshava/ вы сможете оформить такой важный документ, как прописка в Польше, Варшаве. Сотрудники компании оформят договор аренды жилья. Они проведут исчерпывающую, содержательную консультацию, на которой вы узнаете всю необходимую информацию, в том числе, и то, какие документы вам потребуются для оформления. Для наглядности присутствует и образец. Прописка потребуется для открытия счета, оформления карты побыту.
Не знаете как принимать платежи в криптовалюте онлайн на вашем сайте? Зайдите на https://cryptocloud.plus/ и вы сможете быстро и бесплатно подключиться к нашим продуктам. Посетите сайт, узнайте о решениях и возможностях и всех наших преимуществах. Инструменты для удобной работы с криптовалютой к вашим услугам.
blog https://blur-nft-market.com/2023/11/10/comparing-the-features-of-blur-coinmarketcap-with-other-popular-cryptocurrency-market-platforms/
Visit https://timespothq.com/ for in-depth reviews, in-depth comparisons, review guides, and expert opinions on the latest productivity software. We’ll help you find the perfect solution for your unique needs. More details on the website.
Сайт visti.in.ua достоин вашего внимания. Здесь представлены актуальные новости Украины, они находятся в круглосуточном доступе. Мы гордимся и ценим своих читателей. Для вас собрали самое интересное, читайте информацию прямо сейчас. visti.in.ua – https://visti.in.ua портал, который пользуется большой известностью. Заходите уже сегодня, и вы узнаете о науке, спорте, экономике и политике. Сведения все надежные, можете не сомневаться в этом. Следите за нами и наслаждайтесь великолепным контентом!
see https://tronlink.at/2023/11/13/comparative-onchain-analysis-of-ethereum-tron-and-solana-networks-revealed-in-theblock-report/
boodle payday loans As, there is a considerable increase in the number of people carrying bad credit history, lenders are now more than willing to support those people and have come up with different types of personal loans.
На сайте https://us-canad.com/ изучите карты автомобильных дорог Канады, США. Только здесь вас ожидает самый подробный, детальный атлас всех дорог, которые находятся в Северной Америке. Для каждого посетителя сайта доступны крупномасштабные, полноразмерные карты, где учитываются и маршруты США, а также расстояние в милях. Имеется атлас с границами округов. Представлена карта всех штатов вместе с автомагистралями. Перед вами подробные цветные карты всех штатов США, где присутствуют памятники, национальные парки и многое другое.
Techniques d’Г©quilibrage avancГ©es Balancing Techniques pour l’efficacitГ© des soufflantes
На сайте https://ruuserial.net/ посмотрите интересные, новые и полюбившиеся сериалы, которые унесут в удивительный мир. Все они находятся в отличном качестве, с хорошим звуком, а потому понравятся и киноманам. Отличаются интересным, незаурядным сюжетом, увлекательной актерской игрой, приятной музыкой. Есть и совсем новые сериалы, которые только вышли в этом году. Обновление сериалов происходит регулярно. А потому вы точно подберете тот вариант, который вы будете просматривать вечером, после работы или в выходной день.
Компания https://primeinterior.ru/ занимается поставками натурального мрамора, гранита, травертина, оникса и кварцита со всего мира для премиальных интерьеров. Имеем собственное производство во Владивостоке и команду специалистов для монтажа. Готовы к крупным заказам любой сложности со всей России, есть опыт работы с отелями, ресторанами, ночными клубами. Создаём неповторимые интерьеры из природного камня, высокое качество работы и материалов.
На сайте https://nichego-nebolit.ru/ ознакомьтесь с любопытной, интересной информацией, рекомендациями, которые касаются того, как подобрать каре, каковы преимущества и нюансы данной стрижки. Имеются данные о КТ легких и о том, когда лучше всего проводить процедуру и в каких случаях. Есть информация и о системах для нагревания табака. Даны рекомендации о том, как правильно выбрать брус. Есть любопытная статья об озонотерапии и том, как она может вам помочь в улучшении состояния здоровья.
my review here https://debank.lu/2023/11/11/predictions-and-trends-for-the-future-of-debank-crypto/
Equilibrado de rotores Rotor Balancing : Asegurando una funciГіn Гіptima de las desbrozadoras
news https://blur-nft-marketplace.org/2023/11/10/understanding-how-nfts-are-safely-stored-on-the-blockchain/
see this page https://tronlink-app.org/2023/11/13/tron-defining-the-blockchain-worlds-promising-newcomer/
На сайте https://t.me/s/m_1go изучите всю необходимую информацию, которая касается онлайн-заведения 1GO. Воспользуйтесь возможностью сыграть и выиграть приличную сумму денег. Официальный канал находится в вашем мобильном телефоне. Почитать всю интересующую информацию получится в любое время, даже поздним вечером. Открывайте группу на своем мобильном телефоне либо компьютере, чтобы получить доступ к безграничному миру развлечений, бонусов, привилегий. Теперь и вы сможете присоединиться к обществу победителей!
More Info https://trezorwallet-app.org/2023/11/14/assessing-the-legal-consequences-of-the-trezor-data-breach/
На сайте https://setki.moscow вы сможете оформить заявку для того, чтобы заказать москитную сетку. Конструкции производятся из качественных, надежных материалов и всего за день. Монтажные работы проводятся в любой, наиболее комфортный для вас день. На работы, конструкции даются гарантии 12 месяцев. Рассчитать итоговую цену вы сможете прямо сейчас. Установлена привлекательная стоимость за счет собственного производства. Работа происходит не только по Москве, но и области. Предприятие специализируется на производстве, реализации, а также установке москитных сеток.
Use protective equipment, use tools britainsnews.com and equipment according to the rules so as not to encounter difficulties.
you could try these out https://blur-io-nft.com/2023/11/09/enhancing-visual-storytelling-with-the-use-of-blurnick/
canadatc.com
Satisfied customers. You can increase people’s livechinanews.com loyalty to the company. They will be happy to make repeat purchases from your company.
quick loans without a guarantor You have to meet a payday loan provider and provide simple details about yourself – like your name, address, your job details and your checking account number.
https://homes-design.ru/
капитальный ремонт старой квартиры
Грузовики HOWO и Sinotruk в наличии и под заказ на https://partnerauto.ru/ от компании ООО «Новая высота» – это возможность выгодно купить китайские грузовики с доставкой в любую точку РФ. Доступные цены и удобный сервис. Подробнее на сайте.
На сайте https://ipoteka.ru/ вы сможете воспользоваться такой услугой, как помощь в оформлении ипотеки, сопровождение различных сделок, которые совершаются с недвижимостью. В компании работают лучшие, компетентные сотрудники, которые дадут консультацию, а также на профессиональном уровне подберут оптимальную программу для оформления ипотеки. Сервис практикует сотрудничество с ведущими банками, а также инвестиционными предприятиями России, а потому есть возможность получить льготу по ипотеке. Только для вас самые лучшие предложения, которыми воспользуйтесь прямо сейчас.
Наша компания предоставляет кредиты и займы в короткий срок, помогая клиентам решать финансовые вопросы быстро и без лишних хлопот, узнайте подробнее тут – https://zdorovaya-life.ru/novosti/sovety-po-vyboru-luchshej-kreditnoj-karty.html. Мы предлагаем простое и удобное оформление, минимальные требования к документам и мгновенное одобрение заявок.
Линзы для лечения близорукости — это инновационный метод, который помогает корректировать зрение и замедлять прогрессирование миопии. В клинике AllegroVision – консультация невролога перед пмпк .ru предлагают различные виды линз, в том числе ортокератологические линзы, которые надеваются на ночь и корректируют зрение во время сна. Это позволяет ребенку видеть четко в течение дня без необходимости носить очки или дневные линзы.
Такие линзы не только удобны, но и эффективны. Они способствуют правильному формированию роговицы и предотвращают ухудшение зрения. Важно, чтобы подбором линз занимался квалифицированный специалист, который учтет все особенности зрения вашего ребенка. В AllegroVision – консультация детского невролога работают профессионалы, которые помогут подобрать оптимальные линзы и обеспечат постоянное наблюдение за состоянием зрения, гарантируя безопасность и эффективность лечения.
Цветоимпульсная терапия — это эффективный метод лечения, который широко используется в клинике AllegroVision – заключение невролога для пмпк .ru. Наша клиника гордится тем, что у нас работают только лучшие специалисты с опытом более 10 лет. Цветоимпульсная терапия помогает при различных зрительных расстройствах, используя световые импульсы разных цветов для улучшения зрения и общего состояния глаз. Этот метод безопасен и подходит как детям, так и взрослым.
В AllegroVision – заключение невролога для пмпк ижевск мы предлагаем лучшие условия и множество вариантов оплаты, чтобы сделать лечение доступным для всех. Наши врачи тщательно подбирают индивидуальные программы терапии, учитывая все особенности здоровья пациента. Мы уверены, что наша клиника предоставит вам высочайший уровень медицинских услуг и заботы о вашем зрении.
If you need to weld elements, you moneytimenews.com should trust the work of a welder with the necessary skills. Welding work must be carried out under control.
Complex work requires experience welcomelady.net and the use of modern equipment using strong chemicals. Not every person has such an arsenal available.
Прием психиатра в Ижевске в клинике AllegroVision – упражнения для исправления почерка .ru — это возможность получить квалифицированную помощь для вашего ребенка. Наши специалисты с опытом работы более 10 лет проводят тщательные обследования, чтобы выявить и скорректировать психоэмоциональные проблемы. Индивидуальный подход к каждому пациенту и использование современных методов диагностики гарантируют высокое качество лечения. В AllegroVision – лазеротерапия мы предлагаем лучшие условия и разнообразные варианты оплаты, что делает наши услуги доступными для всех семей.
Клиника обеспечивает уютную и поддерживающую атмосферу, где ребенок будет чувствовать себя комфортно. Прием психиатра включает всестороннюю оценку состояния, разработку плана лечения и регулярное наблюдение за прогрессом. Мы заботимся о здоровье и благополучии вашего ребенка, предоставляя профессиональную поддержку на каждом этапе его развития.
informative post https://orbiter-finance-bridge.com/2023/11/18/discover-a-world-of-possibilities-with-orbiter-finance-x-zksync-era-nft-through-a-hassle-free-task/
you can try here https://metamask-wallet-web3.com/2023/11/16/guide-add-xdai-to-your-metamask-wallet-in-a-few-simple-steps/
На сайте https://pacific-map.com/index.html представлены карты с городами, штатами. Перед вами самая подробная карта дорог, которые имеются в США. Крупномасштабные карты содержат самое подробное описание, координаты, а потому вы можете ориентироваться на данную информацию. Это огромная карта со всеми подробностями и важной информацией. Есть карта со штатами, а также Атлантического, Тихоокеанского Побережья. Открыть карту получится с любого устройства и где бы вы ни находились. Все детали отлично видны.
arc loan lenders If you business meets certain monthly turnover requirements then you could be eligible for a payday loan, often referred to as Business Cash Advances.
На сайте https://ru.cryptolegalservices.io/ вы сможете воспользоваться такими полезными услугами, как: оформление крипто-лицензии, нормативный анализ, аудит. Вы сможете воспользоваться бухгалтерскими, налоговыми услугами для тех компаний, которые работают с токенами. Также можно приобрести и недвижимость за токены. Предприятие обслуживает частных лиц, а также различные криптовалютные биржи. Специалисты работают таким образом, чтобы вы смогли работать максимально безопасно и с комфортом.
visit here https://galxe-app.org/2023/11/19/predicting-galaxys-price-for-today-expert-insights-and-projections/
aboutweeks.com
Crypto Pump Signals for Binance https://cryptopumpsignalsbinance.com/ is a unique project that provides traders and investors with valuable insights into upcoming cryptocurrency pumps. Through its Telegram channel and AI capabilities, this project offers new opportunities for generating massive profits in the short-term.
weblink https://1inch-app.org/2023/11/17/accelerating-defi-adoption-with-1inchs-scalable-solutions-on-polygon/
Сломался компьютер, который был необходим для работы, а на новый требовалось 25 тысяч рублей. В поисках займа я обратился к каналу https://t.me/s/novue_zaimu, который увидел в ТОПе Яндекса. Там был огромный выбор новых займов 2024 года, и их давали всем от 18 лет. Я выбрал вариант, где первый займ под 0%, и это позволило мне не переплатить. Получив деньги на карту, я купил новый компьютер и продолжил работу без перебоев.
Посетите сайт GuidesGame https://guidesgame.ru/ и вы найдете коды подарков и бонусов для игр с уникальными наградами для игр на iOS, Android и PC. Вы сможете также узнать гайды для игр и увидеть базу различных игр. Промокоды на игры, коды Roblox и многое другое у нас.
На сайте https://smsi.vip/ вы сможете зарегистрироваться для того, чтобы воспользоваться сервисом смс активаций. Только для вас очень быстрый прием сообщений, огромный выбор сервисов для того, чтобы осуществить смс активацию. Также доступна и переадресация звонков на свой номер. Вы сможете воспользоваться арендой номера для того, чтобы отправлять, принимать смс. Для всех клиентов предоставляются индивидуальные номера. Все, что необходимо – просто пополнить баланс, а затем подобрать услугу.
На сайте https://gazelka86.ru/ закажите грузоперевозки с хорошей скидкой до 50%. Это очень удобно, потому как в компании работают первоклассные, компетентные специалисты, которые выполнят все работы на высоком уровне, профессионально и качественно. Под груз выделяется свой транспорт, который подбирается в соответствии с габаритами, объемом, весом. Предоставляется полный комплекс услуг, чтобы вы воспользовались именно тем, что нужно. Учитывая небольшую стоимость, дается еще и скидка.
The second option is a self-propelled unit, which bmoneyfinder.com has an engine, wheels and its own drive for lifting a fork with a load. These are the ones most often used in warehouses, but only if there is a sufficient amount of free space.
newsplaces.net
navigate to these guys https://metamask-wallet.at/2023/11/16/how-to-access-your-metamask-wallet-on-ios-devices/
Прогрессирующая близорукость — это состояние, которое требует тщательного наблюдения и своевременного вмешательства. В клинике AllegroVision – диагностика астигматизма .ru работают опытные специалисты, которые помогут замедлить прогрессирование миопии с помощью современных методов лечения. Мы предлагаем комплексные программы, включающие аппаратные методы, цветоимпульсную терапию и специальные очки.
Наша клиника предоставляет лучшие условия в стране, а также множество вариантов оплаты, чтобы сделать лечение доступным для всех. В AllegroVision – детский офтальмолог доктор мы уверены, что качественное лечение и профессиональный подход помогут сохранить ваше зрение на долгие годы.
This is due to comfortable living newsgary.com conditions, a warm sea, a variety of tourism services in the country, high-quality food and a relatively economical cost of travel. For the optimal travel option, you should choose a tour on the website, where there are a large number of offers.
Украиночка – сайт, где представлена исключительно полезная и познавательная информация. Наша основная миссия – помочь вам быть уверенной и образованной. Мы знаем то, что вы заслуживаете самое лучшее. В любых аспектах жизни мы вдохновим вас на достижение вершин. Раскроем широкий спектр возможностей для саморазвития и самовыражения. ukrayinochka.com – https://ukrayinochka.com портал, где есть все, что интересно современным женщинам: от актуальных новостей до занимательных советов. Посетите уже сейчас наш ресурс. Вас ожидает лучший контент!
Посетите сайт https://seovgeo.ru/ где вы сможете заказать продвижение на яндекс картах, продвижение компании в яндекс картах, продвижение организации на яндекс картах, сео продвижение на яндекс картах, продвижение через яндекс карты и многие другие услуги с индивидуальным подходом от профессионалов по выгодным ценам. Подробнее на сайте.
here https://1inch-dex.com/2023/11/17/understanding-the-potential-risks-associated-with-impermanent-loss-while-staking-on-1inch/
Официальный дилер ведущих мировых производителей каминов компания ООО «Камины», специализируется на продаже и обслуживании электрических каминов. На сайте https://grand-kamin.ru/ можно купить: каминокомплексы, порталы для электрокамина, настенные и встроенные электро камины, электрические вставки. Опытные специалисты компании проконсультируют, помогут выбрать камин. Доставка каминов в любую точку России, по Москве и Московской области бесплатная. 14 лет на рынке! Магазин электрических каминов в Москве grand-kamin.ru
Visit This Link https://orbiter-finance.at/2023/11/19/building-a-stable-investment-environment-with-orbiter-finances-risk-reduction-strategies/
Монтаж септиков neseptik.com
Что касается – куплю емкость под канализацию екатеринбург мы Вам непременно окажем помощь. Сегодня огромным запросом пользуются частные дома, дачи, коттеджи. Жители как будто измотались от общественной жизни и все стремятся к природе и комфортной обстановке за городом. Но на этапе выбора и покупки участка, рекомендуем учесть очень многие моменты, в том числе вопрос с водоотведением. Если Вы придете к нам перед застройкой, то это будет одним из лучших выборов в Вашей жизни!
Стильные и удобные тактичные штаны, дадут комфорт и уверенность.
Незаменимые для занятий спортом, тактичные штаны подарят вам удобство и защиту.
Надежный пошив и долговечность, сделают тактичные штаны незаменимым атрибутом вашего образа.
Современный стиль и практичность, подчеркнут вашу индивидуальность и статус.
Почувствуйте удобство и стиль в тактичных штанах, которые подчеркнут вашу силу и уверенность.
купити тактичні штани https://taktichmishtanu.kiev.ua/ .
Выбор современных мужчин – тактичные штаны, которые подчеркнут вашу индивидуальность.
Идеальный вариант для активного отдыха, тактичные штаны обеспечат вам комфорт и свободу движений.
Надежный пошив и долговечность, сделают тактичные штаны вашим любимым предметом гардероба.
Максимальный комфорт и стильный вид, порадуют даже самого взыскательного покупателя.
Выберите качественные тактичные штаны, дадут вам комфорт и свободу.
штани тактичні мультикам https://taktichmishtanu.kiev.ua/ .
payday loan wilkes barre pa An online payday loan can help you avoid late fees, overdraft fees or bounced checks.
На сайте https://t.me/s/gatesofolympus_1win вы сможете получить всю необходимую официальную информацию, которая касается канала «Gates of Olympus». Здесь самая актуальная, правдивая информация, которая вам потребуется, если вам нравятся азартные развлечения. Многие пользователи отмечают то, что у компании высокая вероятность получения выигрыша. Перед вами огромное количество интересных, увлекательных слотов, развлечений, которыми вы сможете воспользоваться прямо сейчас.
k8 ミニゲーム
素敵な内容でした!とても勉強になります。
Незаменимая часть гардероба – тактичные штаны, дадут комфорт и уверенность.
Отличный выбор для походов и путешествий, тактичные штаны подарят вам удобство и защиту.
Высокое качество и непревзойденный комфорт, сделают тактичные штаны вашим любимым предметом гардероба.
Современный стиль и практичность, порадуют даже самого взыскательного покупателя.
Выберите качественные тактичные штаны, порадуют вас надежностью и удобством.
купити штани мультикам з наколінниками https://taktichmishtanu.kiev.ua/ .
Место, где можно купить надежные раковина накладная 40 см по выгодным ценам.
Выбор современных мужчин – тактичные штаны, дадут комфорт и уверенность.
Идеальный вариант для активного отдыха, тактичные штаны станут вашим надежным помощником.
Качественные материалы и прочные швы, сделают тактичные штаны незаменимым атрибутом вашего образа.
Максимальный комфорт и стильный вид, подчеркнут вашу индивидуальность и статус.
Почувствуйте удобство и стиль в тактичных штанах, дадут вам комфорт и свободу.
військові тактичні штани https://taktichmishtanu.kiev.ua/ .
На сайте https://sales-sport.ru/ почитайте интересные и содержательные материалы на тему моды, красоты, здоровья. Перед вами самые интересные, свежие публикации, которые точно вам понравятся. Вы узнаете о том, как правильно подобрать женские сапоги, короткое свадебное платье, а также брюки для подростка. Имеются материалы о том, как подобрать солнцезащитные очки, про проектирование, а также монтаж инженерных коммуникаций. Также есть данные о том, правильно выровнять бетонный пол, как подобрать стоматологическую клинику.
linked here wallet jaxx
На сайте https://tursmir.store/ почитайте любопытную, содержательную информацию о том, как правильно отдыхать летом с пользой для организма и своего кошелька. Здесь же вы найдете и любопытные новости, которые касаются отдыха в гостиницах Сочи. Вы узнаете о том, какие нюансы таит в себе принятие солнечных ванн, есть ли вред от этого. Авторы публикуют и различные меры предосторожности, чтобы вы загорали правильно. Получите информацию о том, как забронировать отель. Возможно, вас заинтересуют различные гастрономические туры.
Магазин, где я нашел раковина из искусственного камня на кухню цена для ванной комнаты.
he has a good point phantom download
geinoutime.com
Fang Jifan이 다시 맛있는 음식을 요리하고 싶다고 생각한 Zhu Houzhao는 매우 기뻤습니다.
unsecured fixed rate loan At Cash Mojo, our philosophy is simple: no magic tricks, no disappearing acts – just the easiest way to find cash online.
На сайте https://premier-pokrytie.ru/ есть возможность заказать резиновое покрытие, которое используется внутри помещения, а также на детских, спортивных площадках. В компании трудятся компетентные и лучшие специалисты, у которых огромный опыт работы в данной сфере. Они в совершенстве знакомы с технологией создания резинового покрытия, что позволяет предложить продукт безупречного качества и с уникальными техническими характеристиками. Специалист приедет к вам на объект для замеров абсолютно бесплатно.
Незаменимая часть гардероба – тактичные штаны, которые подчеркнут вашу индивидуальность.
Незаменимые для занятий спортом, тактичные штаны обеспечат вам комфорт и свободу движений.
Высокое качество и непревзойденный комфорт, сделают тактичные штаны незаменимым атрибутом вашего образа.
Современный стиль и практичность, подчеркнут вашу индивидуальность и статус.
Почувствуйте удобство и стиль в тактичных штанах, порадуют вас надежностью и удобством.
штани тактичні https://taktichmishtanu.kiev.ua/ .
Уборка помещений после пожара https://uborka-posle-pozhara-moskva.ru/
you could look here rabby download
click over here Sui wallet martianwallet
Ассоциация Безопасности Трейдинга https://trading-association.org/ это помощь в возврате денег от брокера. Зайдите на сайт, ознакомьтесь с ассоциацией, способами решения сложностей с проблемными брокерами или получите консультацию. Подробнее на сайте.
read here Dym wallet keplr
На сайте https://ruskiseerial.net/ представлены самые новые, интересные фильмы, сериалы, которые определенно заслуживают вашего внимания. Есть и ожидаемые премьеры, которые хочется посмотреть всем киноманам. Все фильмы в отличном качестве, с хорошей озвучкой. Просматривать можно на любом устройстве, включая планшет, смартфон. Для подбора определенного варианта воспользуйтесь специальным фильтром или поиском по жанру. Здесь есть как драмы, так и мелодрамы, комедии, триллеры. Опубликованы и совсем новые фильмы, вышедшие в этом году.
More about the author keplr login
reference martianwallet login
websites sollet wallet
dnews7.com
Couriers receive earned funds by transfer to the card payusainvest.com every week or more often, if necessary. Self-employed employees receive payments directly to the card, they are credited within 1-2 days.
Помощь сыщика в решении сложных ситуаций. http://detektivnoe-agenstvo.ru/
https://www.redpres.com/t42032-del-mar-energy-industrial-leader-in-energy-and-infrastructure/
Монтаж септиков neseptik.com
Относительно купить емкость для канализации цена мы Вам обязательно поможем. Сейчас выдающимся запросом пользуются частные дома, дачи, коттеджи. Люди как будто измучались от социальной жизни и все стремятся к уединению и комфортной обстановке за городом. Но на фазе выбора и покупки участка, следует учесть очень необходимые моменты, среди которых вопрос с водоотведением. Если Вы обратитесь к нам перед застройкой, то это будет одним из самых верных решений в Вашей жизни!
carsinfo.net
Резервуары для септика купить на neseptik.com
Приобрести достойный септик можно перейдя на страницу – бочка септик для канализации цена уже сейчас. Звоните по контактному телефону +7(965)528-61-38 и мы ответим на все ваши вопросы. Расположены по адресу: г. Екатеринбург, ул. Вилонова, д. 33. Режим работы по будням с 8:00 до 19:00. Звоните, приходите, мы будем рады работать с Вами!
Take care of your own health. It dailymoneysource.com is difficult for people with allergies or people with disabilities to do cleaning, so ordering cleaning services is simply necessary for them.
Ёмкости для канализации в Екатеринбурге neseptik.com
Заказать идеальный септик можно кликнув на страницу – емкости для септиков металлические прямо сейчас. Звоните по телефону +7(965)528-61-38 и мы ответим на оставшиеся ваши вопросы. Мы разместились по адресу: г. Екатеринбург, ул. Вилонова, д. 33. Режим работы с пн по пт с 8:00 до 19:00. Звоните, приходите, мы будем рады работать с Вами!
ЗдравБудь – популярный сайт о здоровье. Здесь у вас есть возможность узнать, где искать витамины зимой, что такое микробиом, необходимо ли принимать йод для профилактики, чем может помочь нутрициолог, зачем проверяют уровень гормонов щитовидки. У нас вы также найдете рецепты вкусной еды. Мы предлагаем только интересную и полезную информацию. https://zdravbud.net/new/pochemu-bolyat-sustavy – тут детально рассказываем, почему болят суставы. Объясним, как действует МолекАРТ-РА. Заходите на наш сайт прямо сегодня, вас ждут интереснейшие статьи!
Olymp Trade https://olymptrade-app.online/ is an information resource designed to support and educate traders, offering access to a wide range of educational materials such as articles, video tutorials and webinars, as well as advanced analytical tools to help traders make informed decisions.
Прогрессирующая близорукость — это состояние, которое требует тщательного наблюдения и своевременного вмешательства. В клинике AllegroVision – диагностика зрения .ru работают опытные специалисты, которые помогут замедлить прогрессирование миопии с помощью современных методов лечения. Мы предлагаем комплексные программы, включающие аппаратные методы, цветоимпульсную терапию и специальные очки.
Наша клиника предоставляет лучшие условия в стране, а также множество вариантов оплаты, чтобы сделать лечение доступным для всех. В AllegroVision – лучший детский офтальмолог ижевск мы уверены, что качественное лечение и профессиональный подход помогут сохранить ваше зрение на долгие годы.
На сайте https://ruuserial.net/ посмотрите интересные, увлекательные, новые, а также полюбившиеся сериалы, которые откроют для вас новые горизонты. В них играют талантливые актеры, которые у всех на устах. Для того чтобы подобрать определенный фильм, необходимо воспользоваться специальным фильтром по жанру: комедия, триллер, драма, криминал, детективы, военные. Также получится сделать подборку и по году выпуска. Регулярно на сайте происходят обновления, чтобы вы посмотрели такое кино, которое хочется.
На сайте https://t.me/m1xbet_ru ознакомьтесь с актуальной и интересной информацией, которая касается проекта «1XBET». Заходите на официальный канал и ознакомьтесь со всеми интересующими новостями, актуальными данными, которые вызовут интерес у всех игроков и любителей азарта. На этом сайте постоянно публикуются свежие, интересные новости из мира ставок и гемблинга. Воспользуйтесь и вы возможностью узнать первым о промокодах, предстоящих акциях. Заходить на канал можно в любое время и с любого гаджета.
Краснодарский завод производит котельное оборудование, которое проходит, регламентированные технические испытания и отвечает всем требованиям безопасности. Работаем по всей Российской Федерации и ряду стран СНГ. С нами вы существенно экономите собственное время и денежные средства. Ищете паровой котел промышленный цена? Kzko-gaz.ru – сайт, где есть каталог и представлены отзывы о нашем заводе, ознакомиться с ними можно прямо сейчас. Можете быть уверены – любой произведенный котел или же котельная будут вовремя доставлены. Тепло создавая, гарантируем качество!
Gigantoonz
非常に興味深く、有意義な内容でした。感謝します。
Сайт uafakty.com.ua нравится пользователям лаконичностью оформления. Здесь имеются темы спорта, политики и культуры. Вас ждут актуальные новости шоу-бизнеса. Получайте удовольствие от лучшего контента! uafakty.com.ua – https://uafakty.com.ua сайт, который будет вам понятен, он ценится за оперативность и объективность. Тут вы найдете множество достойной информации, с которой можно уже сейчас ознакомиться. Все без исключения статьи снабжены фото и удобны для чтения. Заходите на наш популярный сайт и читайте актуальные новости в любое время!
На сайте https://truba-almaty.kz/ закажите полиэтиленовые фитинги и трубы. Предприятие ТОО «ТОРГПРОМПЛАСТ» работает в этой сфере длительное время и сотрудничает как с физическими, так и юридическими лицами. Регулярно проводятся акции, действуют скидки, программа лояльности для постоянных клиентов. Работа без посредников, что позволяет снизить траты, избежать переплат. Прямо сейчас вы сможете приобрести трубы с хорошей скидкой. Есть своя производственная база, укомплектованная высокотехнологичным оборудованием.
ремонт мобильных телефонов
Rassilka.kz оказывает качественные услуги. Делаем ватсап, смс, email, рассылки по Нур-Султану, Алматы и Казахстану. Сотрудничаем со многими известными компаниями. Наша главная задача – принести всем клиентам пользу. Действия на конечный итог нацелены. https://rassilka.kz – сайт, где вы узнаете, почему нас выбирают. Здесь у вас есть возможность уже сейчас посмотреть тарифы. У вас есть возможность получить бесплатную консультацию. Мы с удовольствием ответим на все ваши вопросы, свяжитесь с нами в любое время.
Очистка после пожара https://prof-uborka-posle-pozhara.ru/
На сайте https://ntmsp.ru/ закажите звонок для того, чтобы воспользоваться услугами популярной компании ООО «НОВЫЕ ТЕХНОЛОГИИ И МАТЕРИАЛЫ». Она предпринимает все возможное для того, чтобы создать продукцию эталонного качества и соответствующую самым высоким требованиям. В каталоге вы найдете крепеж, ферритовые изделия, медицинские иглы, а также оснастку и многое другое. Все это эталонного качества, реализуется по привлекательной стоимости. В компании трудятся компетентные, надежные специалисты, которые на совесть выполняют работу.
На сайте https://womans-life.ru почитайте актуальную, ценную и интересную информацию на самую разную тему. К примеру, вы узнаете о том, как новогодние праздники отражаются на здоровье, о методиках выведения прыщей в домашних условиях, каким образом лучше всего зашить обувь, как правильно завязать шарф на голове. Представлены самые разные интересные советы, которые помогут решить проблему. Есть и нужные сведения о том, как правильно соединить чулки с поясом. Опубликованы рекомендации от медиков, которые помогут избавиться от болей в поджелудочной железе.
На сайте https://t.me/mvulkan_ru получите интересную, увлекательную информацию о казино «Вулкан 24». Официальный канал теперь находится в вашем мобильном телефоне. Это заведение считается лидером в своем сегменте, а потому ему точно можно доверять. Предлагает огромный выбор автоматов на любой вкус, много развлечений, которые точно понравятся и вам. На канале несколько тысяч записей, а также есть фотографии. Воспользуйтесь и вы возможностью попытать свою удачу, сыграв в интересные развлечения.
На сайте https://uss.eu.com изучите интересную, увлекательную и свежую информацию на самую разную тему. Здесь опубликован материал о красивых украшениях. Предлагается ознакомиться с бестселлерами. Также есть данные о том, как правильно увеличить свой охват в Интернете. Имеется полный список компаний, которые пригодятся владельцам предприятий. Обязательно ознакомьтесь со списком лучших форумов, которые представлены в Интернете. Опубликованы и самые лучшие, проверенные англоязычные форумы, на которые вы сможете зайти прямо сейчас.
Go to the site https://miglandrealestate.com/ and you can find real estate on the island of Bali. Buying, renting land or villas and houses is very simple. We present the best offers at the best prices. We have the latest information about properties in Bali.
На сайте https://sobr26.ru ознакомьтесь с номером телефона охранной организации СОБР. Здесь оказываются услуги, связанные с охраной недвижимости, организуется безопасность объекта, есть возможность воспользоваться физической охраной, которая оказывается более 20 лет. Прямо сейчас вы сможете рассчитывать на бесплатную консультацию. Каждый клиент сможет организовать пультовую, физическую охрану, пожарную сигнализацию, видеонаблюдение. Для того чтобы воспользоваться услугами, оставьте заявку непосредственно на сайте.
На сайте http://ritualnoe-buro-vrn.ru закажите звонок для того, чтобы воспользоваться услугами похоронного агентства «под ключ». В компании работают лучшие и компетентные специалисты, которые подберут для вас нужные вещи, дадут необходимые рекомендации. Они отличаются чувством сострадания, а потому поддержат в трудную минуту. Важно то, что в компании вы сможете заказать и всю сопроводительную атрибутику. Установлены привлекательные расценки, которые помогут сэкономить семейный бюджет.
i loved this The Sandbox Shop
view website The Sandbox Metaverse Map
Срочный заказ машины для вывоза мусора на сайте https://xn—–dlcapan5bbljbbybmd5a7f0c.xn--p1ai/ от профессионалов. От заявки до приезда 20 минут. Работаем в Москве и за МКАД. Официальная утилизация мусора, лучшие условия. Документы. Работаем с 2008 года. Звоните, пишите – консультируем круглосуточно.
Сайт ukrayinka.com.ua пользуется невероятной популярностью и станет вам верным другом. Мы освещаем общественно-политические и экономические события в Украине. Предлагаем только качественную информацию. ukrayinka.com.ua – https://ukrayinka.com.ua портал, который будет понятен каждому пользователю. Здесь вы найдете статьи с хорошими фото. Садитесь и читайте самые горячие новости. Готовы обеспечить вас всеми необходимыми сведениями. Если цените свежесть и наполненность, смело выбирайте наш ресурс. Вы не пожалеете об этом!
my review here aimbot fortnite free
На сайте https://t.me/s/m_1go ознакомьтесь со всей важной, ценной информацией, которая касается проекта «1GO». Здесь публикуются различные акции, промокоды, также вся важная информация относительно клуба. Воспользуйтесь ей и вы, чтобы выиграть приличную сумму денег на свою мечту. В этом казино имеется все, нужно, включая классические слоты, а также удивительные новинки, которые вызовут интерес у каждого. Попытайте свои силы и вы, чтобы получить максимум пользы и приятные эмоции. На этом канале всегда появляются новые сведения, данные из сферы гемблинга.
На сайте https://polygrav.ru вы сможете заказать такую услугу, как производство бейджей, табличек, а также номерков, шильдиков в огромном ассортименте. Только в этой компании вы отыщите огромное количество наиболее выгодных, интересных предложений. Производство является высокотехнологичным, а потому есть возможность заказать товары в любом количестве. Также вы сможете приобрести таблички на дверь, номерки для гардероба. Вся продукция производится из высокотехнологичных материалов, которые не испортят внешний вид.
go right here roblox hacks
платное лечение алкоголизма https://narcolog-expert.ru/
нарколог кодировка https://medutox.ru/
I think the admin of this web page is truly
working hard in favor of his website, because here every information is quality based
information.
Вывоз и утилизация мусора срочно https://vivozim-musor.pro/ закажите на сайте. Профессиональный подход, лучшие условия и цены, круглосуточная работа. Выберите удобное время для вас, а мы сделаем свою работу. Заказать вывоз мусора в Москве можно по телефону на сайте.
directory fortnite skin tool
помощь алкозависимым https://detoxme.kz/
Taker – казино, которое обеспечивает безопасность и честность игры. Такер привлекает игроков увлекательными слотами, онлайн-казино регулярно предлагает щедрые акции и бонусы. Саппорт отзывчивый, работает оперативно и вежливо, вывод средств – быстрый. Ищете taker официальный сайт? Taker.bond – сайт, дизайн которого великолепный, у вас не будет трудностей с навигацией. Если вы решили посетить данное онлайн-казино, вы сделали правильный выбор в пользу азартных игр. Вам скучно точно не будет. Испытайте удачу уже сегодня!
http://school29chita.ru
уроки английского с нуля для детей
Dinopolis считается самым забавным онлайн-слотом, дарящий множество позитивных эмоций. Игра не оставляет никого равнодушным, потому как имеет отменную анимацию, звук и графику. Предлагаем вам захватывающее путешествие в мир динозавров. У вас есть возможность, играя, зарабатывать реальные деньги. Приготовьтесь к веселью и адреналину. https://dinopolisgame.com/ru/ – сайт, где о данном слоте можно найти интересную информацию. Узнаете, как сделать ставку в игре Динополис, сколько можно выиграть. Желаем вам удачи в Dinopolis!
онлайн английский для школьников
yes ru официальный сайт
На сайте https://bettingsport.pro/ изучите рейтинг самых проверенных, надежных букмекерских контор. Им точно можно доверять, ведь они действительно выплачивают средства, предлагают огромное количество бонусов, различных привилегий для всех пользователей. Именно поэтому не составит труда подобрать идеального партнера для того, чтобы заработать побольше денег и сделать ставки в этом году. Только для вас лучшие конторы, к которым точно стоит присмотреться! Все правдивые отзывы игроков и многое другое только на этом сайте.
На сайте https://prometall.shop/ каждый желающий сможет выбрать и приобрести банные печи в сетке, в камне, отопительные печи, которые отличаются повышенной надежностью, практичностью и высоким сроком эксплуатации. Интернет-бутик предлагает только лучшие конструкции, которые принесут радость и пользу от использования. Также имеются и хиты продаж, которые выбирает большинство. Ознакомьтесь с печами в облицовке. Все изделия наделены безупречными эстетическими свойствами, а потому идеально впишутся в любую концепцию.
пневматические шины для погрузчиков
https://otelimoskva2024.ru/
На сайте https://tips-for-women.ru собраны самые полезные рекомендации относительно женской красоты. Так вы получите информацию о том, что представляет собой холодная укладка, плампер для губ, а также почему волосы стали быстрее пачкаться. Также имеется интересная, уникальная информация о том, как правильно о себе заботиться, сохранить здоровье. Вы будете знать о том, как сохранить привлекательный вид надолго. Есть советы по уходу за лицом, волосами, телом. Все рекомендации от экспертов и косметологов.
Клиника инновационной хирургии предлагает большой спектр услуг медицины. Здесь трудятся специалисты, которые помогают людям жить полноценно. Врачи любят свою работу, имеют богатый опыт и высокую квалификацию. Вы будете чувствовать поддержку персонала. Ищете радиохирургическое лечение патологии шейки матки? Kix-med.ru – сайт, где можно записаться на консультацию и ознакомиться с отзывами пациентов. Вы можете быть уверены в безопасности лечения, обращайтесь. Гарантируем индивидуальный подход и приемлемые цены. Улучшим качество вашей жизни!
На сайте https://online-igry-s-vyvodom-deneg.ru/ получите всю необходимую информацию, которая касается заработка в интернете. Перед вами та информация, которая позволит заработать средства без вложений. Представлены ценные рекомендации, которые подскажут, какими способами лучше воспользоваться. Опубликованы только самые эффективные, действительно работающие игры, которые помогут заработать на свою мечту. При этом работать получится в любое время и независимо от рабочего графика.
шина jcb
На сайте https://t.me/s/gatesofolympus_1win вы сможете получить всю необходимую официальную информацию, которая касается канала «Gates of Olympus». Здесь самая актуальная, правдивая информация, которая вам потребуется, если вам нравятся азартные развлечения. Многие пользователи отмечают то, что у компании высокая вероятность получения выигрыша. Перед вами огромное количество интересных, увлекательных слотов, развлечений, которыми вы сможете воспользоваться прямо сейчас.
Del Mar Energy
Taker – прекрасное онлайн-казино, достойное вашего внимания. Оно игроков завлекает интересными слотами, регулярно предоставляет щедрые бонусы и акции. Вывод средств осуществляется быстро, техподдержка доброжелательная, работает оперативно. Ищете taker официальный сайт? Taker.vin – сайт, у которого отменный дизайн и удобная навигация, трудностей с пользованием не будет. Если вы решили зайти на Такер, то сделали все правильно, здесь вам будет предложен широкий ассортимент лучших азартных игр. Скучно вам не будет. Испытайте удачу уже сейчас!
На сайте https://batab.ru посмотрите номер телефона для того, чтобы совершить звонок для того, чтобы заказать производство номерков, табличек, бейджей, наградных досок и многого другого. Доставка всей продукции происходит максимально оперативно. А для того, чтобы ознакомиться с услугами компании и получить представление о ее работе, необходимо изучить отзывы. На всю продукцию установлены привлекательные цены. Срок доставки от 1 дня. Можно вызвать курьера. Ассортимент постоянно обновляется, чтобы вы приобрели все, что необходимо.
На сайте https://usiic.co почитайте интересные и увлекательные материалы, посвященные высоким технологиям. Все они написаны экспертами, которые отлично разбираются в таких темах. Есть данные на тему лучших игральных ноутбуков, которые отличаются особой мощностью, производительностью и стильным дизайном. Опубликован список самых эффективных и прогрессивных из них. Есть информация про вечный двигатель, оснащенный магнитами. Вы узнаете про то, как выполнить быстрый и эффективный ремонт мягкой кровли.
купить колеса для минипогрузчика
Get More Information sollet
спецшина
k8 カジノ パチンコ やり方
このブログのファンになりました。これからも素敵な記事を期待しています。
Related Site sollet.io wallet
Вывоз мусора на утилизацию в Москве https://vyvoz.pro/ по лучшей цене. Постоянно на линии более 50 машин разной вместимости. Узнайте на сайте все наши услуги по утилизации, а мы приедем быстро, в течении 30 минут. Вы можете написать нам в чат на сайте или просто позвонить по телефону. Максимально быстро приедем. Заказать вывоз мусора от профессионалов у нас на сайте.
Portál szakemberek keresőjének https://szakiweb.hu/ -Látogass el az oldalra és találsz egy mesterembert építkezésre, javításra, ház körüli segítségre. Nagyon könnyű mestert vagy szakembert találni az országban bárhol. Vegye igénybe az oldalon található szakemberek szolgáltatásait.
see here now sollet.io wallet
reference sollet wallet
hop over to here jaaxx wallet
увеличение полового члена цена
https://operacziya-uvelichenie-chlena.ru/
https://techbullion.com/del-mar-energy-a-leader-in-manufacturing-and-installing-solar-panels-for-industrial-sites/
На сайте https://pogadaems.ru вы сможете почитать увлекательную, интересную и актуальную информацию, которая касается гаданий в режиме реального времени. Есть возможность изучить информацию о гаданиях на картах Таро, игральных, а также цыганских. Имеются интересные и любопытные картинки, которые позволят пожелать доброго утра маме. Перед вами самая интересная, увлекательная информация, которая поможет сориентироваться в теме. Обязательно ознакомьтесь с гороскопом, чтобы знать, что ожидает вас сегодня.
оказание бухгалтерских услуг
Благодарю за полезную инфу!
В свою очередь предлагаю поиграть в настоящее казино!
вавада официальный сайт играть — доступно и быстро. Это допустит вас к к огромному количеству слотов и рулетке.
Зарегистрировавшись вы попадете в свой ЛК и начать играть. Обратите внимание, что для вывода выигранных денег нужно пройти верификацию аккаунта, показав документы, которые у вас запросят.
Alptracking выполняет аренду качественного и надежного туристического снаряжения. У нас вы найдете треккинговые палки, спальные мешки, рюкзаки, палатки, матрасы и коврики и т.д. Полный ассортимент снаряжения можно изучить, скачав прайс-лист на нашем сайте. Ищете походное снаряжение? Alptracking.ru – здесь у вас есть возможность уже сейчас ознакомиться с контактами, отзывами и условиями проката. Всегда рады ответить на все ваши вопросы и оформить аренду нужного снаряжения. Поможем вам путешествовать с комфортом!
reasons for taking out a personal loan Installment title loans subject to minimum auto value requirements.
Rassilka.kz оказывает качественные услуги. Делаем ватсап, смс, email, рассылки по Нур-Султану, Алматы и Казахстану. Сотрудничаем со многими известными компаниями. Наша основная задача – принести пользу каждому клиенту. Действия на конечный итог нацелены. https://rassilka.kz – сайт, где вы узнаете, почему выбирают именно нас. Здесь у вас есть возможность уже сейчас посмотреть тарифы. У вас есть возможность получить бесплатную консультацию. Мы с удовольствием ответим на все ваши вопросы, свяжитесь с нами в любое время.
Ищете рабочие промокоды Яндекс Маркета? Предлагаем подписаться на канал Олега Петрова. Он здесь делится новой подборкой акций и купонов. Вы нигде не найдете в интернете как у него, такого количества промокодов. Оцените достоинства экономного шопинга. https://dzen.ru/a/ZgxKFq5bOTUwDw_w – тут имеются ссылки, по которым можно поймать топовые скидки в различных категориях. Все промокоды проверены. Воспользуйтесь актуальными предложениями, которые специально для вас Петров Олег нашел. Делайте приобретения с удовольствием!
Хотите отвлечься от повседневных забот и получить заряд позитивных эмоций? Munivi поможет вам в этом. Только самое увлекательное кино, отменное качество видео ожидают вас круглосуточно. https://munivi.xyz/ – сайт, который не зависает и замечательно оформлен. Порталом вы точно будете довольны. Здесь вы найдете хорошие сериалы. Можно с легкостью отыскать старые и новые. Также есть поиск, им можете воспользоваться в удобное время. Базу сериалов регулярно обновляем и добавляем. У нас вы найдете то, что вам по душе!
На сайте https://bettingsport.pro/brands/leon-bukmeker/ вы узнаете всю важную, интересную информацию о БК «Леон». В этом месте заключаются различные прогнозы на спортивные мероприятия. Вас ожидает огромное количество бонусов, лайв-события, прематчи, повышенные коэффициенты, акции и многое другое, что сделает игру более интересной, зрелищной. Интерактивные пари можно заключать круглосуточно. Ставки делают с различных устройств, в том числе, ноутбука, смартфона или ПК. Можно воспользоваться как официальным сайтом, так и приложением.
Консалтинговая компания Leverage Finance Group оказывает поддержку в реализации инвестиционных проектов. Отлично разбираемся в особенностях и тонкостях процесса получения грантов. Создаем действенные бизнес-планы и до их результатов сопровождаем. Ищите финансирование бизнеса? Levfin.ru – сайт, где у вас есть возможность узнать, почему к нам нужно обратиться. Работаем с компаниями в различных отраслях, создавая ценность каждому проекту. Наши услуги помогают бизнесу успешно развиваться и вовремя привлекать нужное финансирование. Звоните и мы проконсультируем вас.
Bruder Und Sschwester Oralverkehr Auto Gegen Oralverkehr
На сайте https://realniy-zarabotok.ru/ изучите самые эффективные, работающие методы получения средств. И самое главное, что все методы действительно работающие и эффективные. Они помогут заработать на мечту и получить больше средств. К примеру, получится заработать на партнерке, выполнить различные задания и получить за это колоссальные суммы. Вывод средств происходит на карту или электронный кошелек. Но зачастую для того, чтобы обеспечить себе доступ к тем заданиям, за которые больше платят, необходимо пройти специальный тест.
Сувенирная продукция с логотипом и корпоративный мерч на заказ в Москве
https://telegra.ph/Vash-brend-v-kazhdom-zheste—sekrety-suvenirnoj-produkcii-s-logotipom-v-Moskve-05-31
Na stronie https://1op.pl/ prosimy o kontakt w celu skorzystania z usług związanych z Naprawa, otwieraniem zamków w Warszawie. Ponadto dostępny jest również pilny wyjazd. Firma działa przez całą dobę, co pozwala zamawiać usługi w dowolnym momencie, w tym w święta, weekendy. Mistrz przyjedzie do obiektu dosłownie w 15 minut, aby wykonać wszystkie niezbędne prace. Ponadto firma będzie dla ciebie pomocna, a jeśli zgubisz klucz, zamek nie działa lub nie obraca się, technik powinien bezpiecznie otworzyć drzwi.
На сайте https://dyhu.ru/ закажите изысканные и популярные ароматы, духи от лучших и проверенных парфюмеров, которые создают продукцию для изысканного, привлекательного стиля. Каждый желающий получает возможность приобрести все, что считает нужным, оптом, чтобы разнообразить свой ассортимент и сделать его более интересным и привлекательным для клиентов. Регулярно на сайт добавляются интересные новинки, которые заслуживают вашего внимания. Также устраиваются распродажи, которые позволят сэкономить на покупке хорошие деньги.
Сайт, где можно купить надежные нержавеющая раковина для кухни по выгодным ценам.
На сайте https://smile-me.ru/ вы сможете заказать звонок для того, чтобы получить консультацию относительно проведения детских праздников. Здесь вы сможете заказать детских аниматоров, устроить тематический праздник, воспользоваться услугами ведущих на мероприятие, устроить незабываемый, яркий квест или бумажное шоу. Действуют привлекательные, доступные расценки. Все мероприятия проводятся компетентными, талантливыми специалистами, которые не перестают радовать своим профессионализмом.
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
https://tvoi54.ru/articles/08-08-2019/3804-sro-stroitelei-osobennosti-vstuplenija.html
moneymaker com If you badly need money and do not know which service to choose, stop hesitating and apply to North’n Loans.
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
https://newsfrol.ru/214/12686/
k8 カジノ とは
素晴らしい記事。非常に役立つ情報を提供してくれてありがとうございます。
где ремонтируют телефоны
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
https://nicstroy.ru/4215-gotovaya-firma-s-oborotami-i-dopuskom-sro.html
Студия профессионального дизайна интерьеров «Мята» поможет воплотить ваши мечты в реальность! Все специалисты увлечены своим делом, они сделают ваш интерьер невероятно красивым. Мы будем рады видеть вас среди наших клиентов. Ищете студия дизайна в СПб? Spb.Studio-mint.ru – здесь можете увидеть фото интерьеров квартир. Создаем проекты высокого уровня и предоставляем заманчивые цены. Успех нашей работы подтверждают отзывы, ознакомиться с ними можете на нашем сайте. Свяжитесь с нами, чтобы обсудить детали. Готовы удовлетворить ваши пожелания!
ремонт телефонов поблизости от меня
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
https://life24.pro/life/363791625/
Sie Sucht Ihn Fur Sex I Mv MГјnchen Analverkehr Frau
На сайте https://cliningkrd.ru вы сможете заказать обратный звонок для того, чтобы воспользоваться услугами клининговой компании «Cleaning». Здесь оказываются профессиональные услуги компетентными, проверенными специалистами. В работе применяется инновационное, высокотехнологичное оборудование, которое справляется с загрязнениями различного уровня интенсивности. Бытовая химия, чистящие средства от надежных брендов, которые создают полностью безопасную для людей, животных продукцию.
Замена остекления на балконе specbalkon.ru
Что касается замена окон на балконе на теплые цена на выгодных условиях, обращайтесь к нам. Контактный номер телефона +7(812)240-94-42 или закажите обратный звонок на вышеуказанном сайте. Мы осуществляем монтаж в строго обговоренный срок, часто в течение 1-3 дней. Предоставляется гарантия на материалы в среднем 5 лет, на монтаж — 3 года. Оплата происходит по факту выполненных работ, предоплата не нужна.
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
https://muzeon.ru/finansy/9077-kak-i-gde-poluchit-dopusk-sro-v-stroitelstve.html
Сувенирная продукция с логотипом и корпоративный мерч на заказ в Москве
https://cartlung3.bloggersdelight.dk/2024/05/31/%d1%81%d1%83%d0%b2%d0%b5%d0%bd%d0%b8%d1%80%d0%bd%d0%b0%d1%8f-%d0%bf%d1%80%d0%be%d0%b4%d1%83%d0%ba%d1%86%d0%b8%d1%8f-%d1%81-%d0%bb%d0%be%d0%b3%d0%be%d1%82%d0%b8%d0%bf%d0%be%d0%bc-%d0%bd%d0%b0-%d0%b7/
Самый большой магазин мобильных телефонов в Минске https://g5.by/ это возможность купить по низкой цене с доставкой по всей Беларуси: мобильные телефоны, ноутбуки, планшеты, бытовую технику и многое другое. Ознакомьтесь с каталогом из более чем 30000 сертифицированных товаров, и вы обязательно найдете для себя лучшую цену, качество, а быстрая бесплатная доставка не заставит себя долго ждать.
На сайте https://kladupechi.ru оформите заявку для того, чтобы воспользоваться такими полезными услугами, как: ремонт, кладка печей, каминов. Все конструкции от высококлассного, проверенного мастера, который работает по всему Санкт-Петербургу, области. А если вас интересует какая-либо определенная информация, то воспользуйтесь специальным поиском. Также имеется информация и про печное отопление: русскую, голландскую, финскую печь. Изучите все рубрики, чтобы получить полную информацию на интересующую тему.
what is the best company to get a personal loan from This will mean a larger payment, larger balance, but also a new vehicle, a warranty, and a lower interest rate.
Хотите быстро и без каких-либо проблем заменить права на польские? MIGRANT SUPPORT – это то, что вам необходимо. Компания дает гарантию на персональный подход и лояльные цены. Наши квалифицированные специалисты обладают большим опытом работы. Они предложат для вас необходимую информацию о том, как надо заменить на польские права. https://migrant.support/obmien_rossiiskikh_prav_na_polskiie – сайт, где у вас есть возможность прямо сегодня заказать услугу. Также здесь в любое удобное время можно ознакомиться с отзывами о нас. Ответим на все ваши вопросы, звоните нам.
На сайте https://advokat-samara.ru/ оставьте заявку для того, чтобы воспользоваться доставкой товаров из Китая для маркетплейсов. Среди основных услуг выделяют: выкуп, поиск, доставку товаров. Кроме того, можно воспользоваться и упаковкой, отгрузкой продукции на маркетплейсы. При необходимости будет оказана вся необходимая помощь для того, чтобы организовать бизнес на WB. Рассчитать цену услуги получится в данный момент. Оказывается весь спектр услуг, чтобы вы наладили собственный бизнес. Воспользуйтесь сопровождением с гарантиями, проводится анализ уже имеющихся карточек.
Мята – студия профессионального дизайна интерьеров в Москве все мечты воплощает в реальность. Тут трудятся только квалифицированные специалисты, которые готовы принять любой вызов, и увлечены своим делом. Будем рады видеть вас в числе своих клиентов. Ищете дизайн квартиры в Москве Moskva.Studio-mint.ru – сайт, где вы можете найти фото интерьеров квартир.? Предлагаем разумные цены, следим за трендами и новинками в индустрии интерьерного дизайна. Делаем проекты высочайшего уровня. Обсудим с вами все детали, звоните нам уже сейчас. Любые ваши желания удовлетворим!
Space Movers https://spacemovers.ca/ is renowned as the premier moving company in Calgary, Canada, offering unparalleled service and expertise in residential and commercial relocations. Their reputation as the best movers in the city is built on a foundation of reliability, efficiency, and a customer-centric approach that ensures a smooth and stress-free moving experience. Choosing Space Movers means choosing the best in the business, ensuring a seamless transition to your new home or office.
На сайте https://zdravbud.net/new/pochemu-bolyat-sustavy изучите увлекательную, интересную и содержательную информацию, которая посвящена тому, почему болят суставы. Так есть информация о том, чем правильно их питать, чтобы сохранили свою эластичность. Описаны признаки того, что суставы заболели. Вы узнаете о том, какими способами и методами их лучше всего и эффективней восстановить. Описаны самые эффективные, точные, а также безопасные из них. А самое главное, что они действительно работают.
Sexspielzeug Parchen Erstmal Analverkehr
Установка крыши на балконы спб specbalkon.ru
Если Вам требуется замена остекления окон балконов прямо сейчас, то мы вам обязательно окажем помощь. Услуга по смене холодного фасадного остекления по теплое сейчас очень востребована. При покупке жилья в новом доме очень часто застройщик ставит на балкон холодное, не очень качественное остекление, которое лучше поменять сразу же после покупки. Теплое остекление балкона имеет большое количество плюсов: окна не замерзнут даже в самые холодные зимы, на балконе можно сделать отдельное помещение, цветы будут расти при комфортной температуре, на балконе можно продумать места для хранения и вещи не деформируются. Поэтому предлагаем Вам замену остекления сделать как можно быстрее и по выигрышной цене.
Теплое фасадное остекление балкона specbalkon.ru
Относительно замена стеклопакетов на балконе на утепленные цена на выгодных условиях, приходите к нам. Контактный телефон +7(812)240-94-42 или закажите обратный звонок на упомянутом сайте. Мы производим монтаж в точно установленный срок, часто в течение 1-3 дней. Даётся гарантия на изделия в среднем 5 лет, на монтаж — 3 года. Оплата осуществляется по факту исполненных работ, предоплата не нужна.
押忍!番長3(自动转)
この記事は非常に有意義で、読むのが楽しみでした。
Теплое фасадное остекление балкона specbalkon.ru
Если Вам требуется стоечно ригельная система фасадного остекления цена прямо сегодня, то мы вам непременно поможем. Услуга по замене холодного фасадного остекления по теплое сейчас весьма востребована. При покупке квартиры в новом доме очень часто застройщик ставит на балкон холодное, не очень хорошее остекление, которое лучше менять сразу же после приобретения. Теплое остекление лоджии имеет большое количество преимуществ: окна не замерзнут даже в самые морозные зимы, на балконе возможно сделать отдельное пространство, цветы будут расти при комфортной температуре, на балконе можно сделать места для хранения и вещи не деформируются. Поэтому предлагаем Вам замену остекления сделать как можно скорее и по лучшей цене.
Sexspielzeug M Analsex Lidocain
Child Course
Привет! Хочу рассказать вам о самых популярных телеграм-каналах, о которых сейчас говорят все. Например, новинки кино 2024 – этот канал все обсуждают, ведь здесь самые свежие фильмы и премьеры! Для тех, кто хочет заработать в интернете, канал заработок в интернете стал настоящей находкой – только полезная информация и советы. Если хотите заниматься саморазвитием, то саморазвитие с чего начать – это то, что вам нужно. В финансовом мире обсуждают новые МФО 2024, а для срочных займов все выбирают займы которые дают всем. Эти каналы действительно на пике популярности, не пропустите!
go sollet io
Замена остекления на балконе specbalkon.ru
Что касается замена холодного остекления авангард на выгодных условиях, приходите к нам. Контактный номер телефона +7(812)240-94-42 или закажите обратный звонок на упомянутом сайте. Мы осуществляем монтаж в строго обговоренный срок, часто в течение 1-3 дней. Предоставляется гарантия на материалы в среднем 5 лет, на работу — 3 года. Оплата происходит по факту исполненных работ, предоплата не потребуется.
hop over to this website sollet io
my site solana wallet
fast cash loans with bad credit There is a small finance charge for the processing part of the loan and the pay back date is based on your next payday.
geinoutime.com
Hongzhi 황제는 “당신이 살 수 있는지 여부 만 묻습니다. “라는 말을 듣고 머리가 아팠습니다.
Outstanding feature
https://nalopak.pl/jak-dobrac-odpowiednia-grafike-do-druku/
Онлайн курсы для педагогов maps-edu.ru
Что касается рентгенология профессиональная переподготовка – Вы на верном пути. Направления, по которым мы обучаем: охрана труда, медицина, бухгалтерское дело, физическая культура и спорт, пожарная безопасность, закупки, культура и искусство, документоведение и делопроизводство, нефтяная и газовая промышленность, метрология и стандартизация и многие другие.
ссылка на мегу – сайт меги даркнет, как зайти на mega
Riesenbusen Und Analsex Vintage Natursekt Porno
solaris даркнет – solaris даркнет, solaris ссылка
what are normal personal loan rates Foremost, you should again reiterate the high gross margins generated from your Payday Lender capital lending services while also showcasing the generally low costs associated with operating this type of business.
Theatrical version Puella Magi Madoka Magica
素晴らしい記事で、心から感動しました。共有せずにはいられません。
https://nerdgaming.science/wiki/User:JuliaAdams1
Сколько стоит аккредитация онлайн maps-edu.ru
Относительно переподготовка педагог психолог – Вы на верном пути. Направления, по которым мы обучаем: строительство, агрономия и сельское хозяйство, педагогика, дефектология, пожарная безопасность, закупки, экономика и финансы, промышленность, менеджмент, антитеррористическая защищенность и многие другие.
Банкротство физических лиц – это правовой процесс, который позволяет гражданам, не способным погасить свои долги, получить защиту от кредиторов и начать финансовую жизнь с чистого листа. В России процедура банкротства физических лиц была введена в 2015 году, и с тех пор ею воспользовались десятки тысяч людей.
**Основные этапы процедуры банкротства физических лиц**
1. **Подача заявления о банкротстве**. Должник или его кредитор подает заявление о признании физического лица банкротом в арбитражный суд по месту жительства должника. В заявлении указываются данные о должнике, размере задолженности и других финансовых обязательствах.
2. **Рассмотрение дела в суде**. Суд проверяет обоснованность заявления и принимает решение о начале процедуры банкротства. На этом этапе назначается финансовый управляющий, который будет контролировать процесс.
3. **Финансовое управление**. Финансовый управляющий оценивает финансовое состояние должника, его активы и обязательства. Управляющий может предложить план реструктуризации долгов или продажу имущества должника для погашения задолженности.
4. **Реструктуризация или реализация имущества**. В зависимости от решения суда и финансового управляющего, может быть предложен план реструктуризации долгов, который позволит должнику погашать долги в течение определенного времени. Если такой план невозможен, начинается реализация имущества должника с целью погашения задолженности.
5. **Завершение процедуры банкротства**. По окончании реализации имущества или выполнения плана реструктуризации суд выносит решение о завершении процедуры банкротства. Оставшиеся непогашенные долги списываются, и должник освобождается от обязательств перед кредиторами.
**Плюсы и минусы банкротства физических лиц**
**Плюсы**:
1. **Освобождение от долгов**. Основное преимущество банкротства – возможность избавиться от непосильных долгов и начать новую финансовую жизнь.
2. **Защита от кредиторов**. С момента подачи заявления о банкротстве и до завершения процедуры кредиторы не могут требовать погашения долгов через суд или приставов.
3. **Реструктуризация долгов**. Возможность реструктурировать долги и погашать их по новому, более удобному графику.
**Минусы**:
1. **Потеря имущества**. В большинстве случаев для погашения долгов придется продать имущество, принадлежащее должнику.
2. **Снижение кредитного рейтинга**. Банкротство негативно сказывается на кредитной истории, что может затруднить получение новых кредитов в будущем.
3. **Ограничения**. После банкротства на должника могут быть наложены ограничения, такие как запрет на занятие определенных должностей или ведение бизнеса.
**Альтернативы банкротству физических лиц**
Существуют и альтернативные способы решения проблемы с долгами, которые могут быть менее радикальными и более выгодными для должника:
1. **Переговоры с кредиторами**. Должник может попытаться договориться с кредиторами о реструктуризации долгов, снижении процентной ставки или предоставлении отсрочки по платежам.
2. **Рефинансирование**. Взятие нового кредита на более выгодных условиях для погашения старых долгов может помочь снизить финансовую нагрузку.
3. **Мировое соглашение**. Заключение мирового соглашения с кредиторами в рамках судебного процесса позволяет урегулировать задолженность без процедуры банкротства.
Банкротство физических лиц – серьезный шаг, который требует взвешенного подхода и тщательного анализа всех возможных последствий. Важно помнить, что эта процедура может стать единственным выходом из сложной финансовой ситуации, но перед ее началом стоит рассмотреть все возможные альтернативы и проконсультироваться с юристом или финансовым консультантом.
http://termwiki.co.uk/index.php/666484.ru
Онлайн курсы для педагогов maps-edu.ru
Относительно переподготовка на юриста – Вы на правильном пути. Направления, по которым мы обучаем: строительство, агрономия и сельское хозяйство, педагогика, физическая культура и спорт, пожарная безопасность, закупки, экономика и финансы, промышленность, нефтяная и газовая промышленность, метрология и стандартизация и многие другие.
смотреть онлайн бесплатно сериалы 2024 года
2024 Avrupa Futbol Şampiyonası öncesinde milli takımlar, hazırlık maçları oynayacaklardır. Bu maçlar, takımların turnuvaya hazırlık seviyelerini gösterecek ve futbolseverlere ipuçları verecektir. Türkiye’nin ve diğer takımların hazırlık maçları hakkında bilgilere sitesi adresinden ulaşabilirsiniz. https://2024euro.com.tr/
Онлайн курсы для педагогов maps-edu.ru
Что касается охрана и безопасность труда переподготовка – Вы на точном пути. Направления, по которым мы можем обучить: охрана труда, агрономия и сельское хозяйство, педагогика, физическая культура и спорт, юриспруденция и право, закупки, экономика и финансы, промышленность, менеджмент, метрология и стандартизация и многие другие.
Сувенирная продукция с логотипом и корпоративный мерч на заказ в Москве
https://jutecurve29.bloggersdelight.dk/2024/05/31/%d1%81%d1%83%d0%b2%d0%b5%d0%bd%d0%b8%d1%80%d0%bd%d0%b0%d1%8f-%d0%bf%d1%80%d0%be%d0%b4%d1%83%d0%ba%d1%86%d0%b8%d1%8f-%d1%81-%d0%bb%d0%be%d0%b3%d0%be%d1%82%d0%b8%d0%bf%d0%be%d0%bc-%d0%bd%d0%b0-%d0%b7/
http://anekdotshutka.ru/
купить сигареты в интернет-магазине дешево
Купить сигареты дешево
Discover the best porn2all.com/models/reagan-foxx/ ever for free!
Сувенирная продукция с логотипом и корпоративный мерч на заказ в Москве
https://maphail2.werite.net/vash-brend-v-kazhdom-zheste-sekrety-suvenirnoi-produktsii-s-logotipom-v-moskve
Ist Ungeschutzter Analsex Schlimm Kann Man Beim Analverkehr Schwanger Werden
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
https://muzeon.ru/sport/9304-gde-i-kak-poluchit-licenziyu-minkultury-na-restavraciyu-giop.html
Компания «СХТ» предлагает вам приобрести высокоточное измерительное оборудование. Мы гарантируем безупречное качество нашей продукции и привлекательные цены. Специалисты компании обладают приличным опытом работы и высокой квалификацией. Они с радостью готовы проконсультировать вас по интересующим вопросам. https://cxt.su – сайт, где у вас есть возможность посмотреть детальнее наши услуги и информацию. Здесь вы найдете видео-презентацию и фотогалерею. Оперативно реагируем на все заявки. Обращайтесь уже сейчас к нам!
Сувенирная продукция с логотипом и корпоративный мерч на заказ в Москве
https://blowsecond86.werite.net/suvenirnaia-produktsiia-s-logotipom-na-zakaz-v-moskve-sozdaite-brend-kotoryi
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
http://menzelinsk.ru/links.php?categ=15&links=125606
Курсы переподготовки для педагогов maps-edu.ru
По вопросу банкротство физических лиц обучение для юристов онлайн, мы Вам непременно окажем помощь. Звоните по контактному телефону 8(800)777-06-74 и задавайте все оставшиеся вопросы. Звонок по РФ бесплатный. Регионально расположены по адресу: г. Иркутск, ул. Степана Разина, д. 6. На онлайн ресурсе maps-edu.ru вы также сможете обратиться в службу поддержки и Вас проконсультирует наш специалист.
Сувенирная продукция с логотипом и корпоративный мерч на заказ в Москве
https://diigo.com/0wftu9
Analsex Parties Parkplatzsex 73547
Помощь в получении допуска СРО, сертификата ISO и лицензий от МСМ
http://help-bussines.ru/vstuplenie-v-sro-stroiteley.html
Сувенирная продукция с логотипом и корпоративный мерч на заказ в Москве
https://canvas.instructure.com/eportfolios/2940531/Home/___________
Die Beliebtesten Fingerspiele Sex Im Freien Massieren
https://skachat-leon-prilozhenie.ru/
цікаві теми для есе – дисертація приклад, автореферат дисертації вернадського
THE DAY BEFORE игра на ПК – GTA 6 обзор игры, Counter Strike 2 скачать бесплатно
ремонт телефонов
Привет всех любителям гэмблинга! Хочу описать отзывами об онлайн гейминг kent kazino. Это гейминг площадка восхищает своим ассортиментом игр: от старых аппаратов до игр с настоящими дилерами с настоящими ведущими. Живой и стильный дизайн платформы, обильные поощрения и непрерывные акции делают всякую партию еще более еще более волнительной. Ресурс действует молниеносно и стабильно, что обеспечивает комфортную игру. kentcasino – это платформа, где любой вращение может быть первым шагом значительного успеха. Очень советую оценить!
Всем привет всех ценителям азартных игр! Хочу рассказать отзывами об виртуальном игровом клубе 1xbet. Это платформа радует своим разнообразием игровых автоматов: от традиционных слотов до живых игр с настоящими крупье. Цветной и модный дизайн ресурса, большие плюшки и частые промоакции добавляют любую игру даже более более захватывающей. Ресурс действует оперативно и надёжно, что обеспечивает комфортную игровой процесс. 1xbet – это место, где любой ставка окажется первым шагом крупной победы. Сильно предлагаю тестировать!
Здравствуйте всех любителям гейминг! Хочу поделиться ощущениями об цифровом гейминг kent casino скачать. Это платформа поражает своим ассортиментом видеоигр: от традиционных слотов до лайв игр с живыми ведущими. Яркий и дизайнерский интерфейс портала, большие вознаграждения и непрерывные мероприятия превращают всякую сессию даже еще более захватывающей. Платформа работает мгновенно и без сбоев, что гарантирует комфортную геймплей. kent casino скачать – это локация, где любой спин вполне может стать началом значительного успеха. Очень рекомендую оценить!
real cash loan sites Online process does not require paperwork in order to approve the loan.
Приветствую всем ценителям гейминг! Хочу рассказать впечатлениями об веб игровом заведении кент. Это казино удивляет своим многообразием видеоигр: от популярных слотов до игр с настоящими дилерами с реальными раздающими. Красочный и модный стиль сайта, большие бонусы и частые промоакции добавляют любую сессию ещё более увлекательной. Ресурс действует оперативно и без сбоев, что гарантирует спокойную игровой процесс. игровые автоматы casino kent – это место, где всякий крутка может стать отправной точкой крупной победы. Настоятельно советую испытать!
Всем здравствуйте всех любителям азартных развлечений! Хочу описать ощущениями об онлайн игровом заведении azino mobile скачать. Это игровая площадка впечатляет своим ассортиментом игровых автоматов: от традиционных слотов до реальных игр с действительными ведущими. Светлый и дизайнерский вид сайта, великодушные поощрения и частые мероприятия добавляют всякую сессию еще более волнительной. Сайт работает молниеносно и без проблем, что обеспечивает удобную игровой процесс. казино 777 – это платформа, где любой крутка может быть стартом большого трофея. Настоятельно советую тестировать!
Приветствую всем почитателям азартных развлечений! Хочу рассказать ощущениями об онлайн игровом заведении казино. Это игровая площадка удивляет своим многообразием игр: от традиционных слотов до живых игр с реальными крупье. Цветной и дизайнерский стиль платформы, богатые плюшки и частые события превращают всякую партию даже более интересной. Платформа работает мгновенно и стабильно, что обеспечивает комфортную геймплей. азино скачать – это локация, где любой поворот окажется началом значительного успеха. Сильно предлагаю попробовать!
Всем здравствуйте всех фанатам игрового процесса! Хочу описать отзывами об веб гэмблинг azino777. Это гейминг площадка восхищает своим многообразием видеоигр: от классических игровых автоматов до реальных игр с действительными дилерами. Цветной и современный оформление портала, обильные поощрения и частые акции придают всякую игру даже более еще более привлекательной. Платформа действует скоростно и стабильно, что даёт удобную игру. азино три топора сайт – это локация, где всякий крутка может стать первым шагом крупной победы. Очень советую испытать!
Realize of the most beneficent reality-sex-sites.com/blog/best-dating-apps-for-2024-find-your-perfect-match/
and porn2best.com/top-rated even!
porn2best.com- Best Free Porn Videos, Mating Movies & XXX Albumsporn2best.com- Most outstanding Uncage Porn Videos, Lovemaking Movies & XXX Albums bfee0b6
Корпоративные Тарифы
https://gnezdoparanoika.ru/news/44150-vygodnye-tarify-mts-s-internetom.html
ремонт сотовых телефонов рядом
Всем здравствуйте всех любителям гэмблинга! Хочу передать впечатлениями об виртуальном игровом клубе azino 777 отзывы. Это гэмблинг заведение впечатляет своим ассортиментом видеоигр: от винтажных слотов до живых игр с подлинными раздающими. Красочный и стильный оформление сайта, щедрые плюшки и регулярные акции делают всякую игру даже более привлекательной. Платформа функционирует молниеносно и бесперебойно, что предоставляет приятную игровую сессию. три топора азино – это площадка, где каждый крутка вполне может стать отправной точкой значительного успеха. Настоятельно рекомендую оценить!
Всем привет всех почитателям игрового процесса! Хочу рассказать эмоциями об интернет игровом клубе gamacasino. Это гэмблинг заведение восхищает своим многообразием видеоигр: от традиционных аппаратов до игр с настоящими дилерами с живыми дилерами. Красочный и стильный стиль платформы, богатые вознаграждения и ежедневные акции придают каждую сессию еще более интересной. Платформа работает молниеносно и стабильно, что обеспечивает спокойную игру. казино гама – это место, где каждый спин может быть стартом большого выигрыша. Настоятельно рекомендую попробовать!
**Прогон Хрумером: Эффективное SEO-Продвижение Вашего Сайта**
В мире интернет-маркетинга существует множество методов
и инструментов для продвижения сайтов, и одним
из самых мощных и популярных является прогон Хрумером.
Этот программный комплекс позволяет автоматизировать рутинные задачи SEO и значительно улучшить позиции сайта в поисковых
системах. В этой статье мы подробно
рассмотрим, что такое прогон
Хрумером, как он работает и какие преимущества
он может предложить.
**Что такое прогон Хрумером?**
Прогон Хрумером – это процесс автоматического размещения ссылок и сообщений на различных
веб-ресурсах с использованием программы Хрумер.
Это позволяет существенно увеличить количество обратных ссылок
на ваш сайт, что является одним из ключевых факторов для улучшения его
позиций в поисковых системах.
Программа автоматически регистрируется на
форумах, блогах, социальных сетях и других платформах, размещая ссылки
и сообщения согласно заданным параметрам.
**Как работает прогон Хрумером?**
1. **Подготовка ресурсов**: В первую очередь необходимо составить список целевых веб-ресурсов, на которых будет производиться размещение ссылок.
Это могут быть форумы, блоги, социальные сети
и другие платформы.
2. **Создание шаблонов**: Далее создаются шаблоны для размещения ссылок и
сообщений. Важно, чтобы тексты были уникальными и соответствовали
правилам выбранных платформ.
3. **Настройка программы**: В Хрумере настраиваются параметры подключения, капча-сервисы и прокси-серверы
для обеспечения стабильной работы программы.
4. **Запуск прогона**: После настройки всех параметров запускается процесс
прогона, который программа выполняет автоматически.
Хрумер регистрируется на сайтах, размещает ссылки и сообщения, а также разгадывает
капчи.
5. **Мониторинг и анализ**: Важно регулярно отслеживать
результаты прогона, анализируя
отчеты о размещении ссылок
и реакции аудитории. Это позволяет
корректировать стратегию продвижения и улучшать
её эффективность.
**Преимущества прогона Хрумером**
1. **Экономия времени**: Прогон Хрумером позволяет автоматизировать процесс
размещения ссылок, что значительно экономит
время по сравнению с ручным методом.
2. **Увеличение числа обратных ссылок**:
Автоматическое размещение ссылок на множестве ресурсов способствует росту числа обратных ссылок, что положительно
сказывается на позиции сайта в поисковых системах.
3. **Повышение видимости сайта**: Прогон
Хрумером помогает улучшить видимость вашего сайта в интернете, привлекая новую аудиторию и увеличивая трафик.
4. **Гибкость и универсальность**:
Хрумер поддерживает работу с множеством различных платформ и позволяет
настраивать параметры прогона в соответствии с вашими потребностями.
**Заключение**
Прогон Хрумером – это эффективный метод автоматизации SEO-продвижения, который позволяет значительно улучшить позиции вашего сайта
в поисковых системах. Используя этот мощный инструмент,
вы сможете сэкономить время и усилия, сосредоточившись на стратегически важных задачах.
Прогон Хрумером – это надежный способ увеличить число обратных ссылок, повысить видимость вашего сайта и привлечь больше посетителей.
My web-site “http://jejucordelia.com/eng/bbs/board.php?bo_table=review_e&wr_id=266061”
Срочно нужны деньги? Не проблема! На нашем канале срочные займы вы найдете все необходимое для быстрого получения займа на карту. Оформляйте заявки без отказа и проверок. Присоединяйтесь к нам!
Привет всех энтузиастам гэмблинга! Хочу описать эмоциями об виртуальном гэмблинг играть игровые автоматы бесплатно. Это игровая площадка радует своим разнообразием видеоигр: от популярных слотов до игр с дилерами с настоящими крупье. Красочный и современный вид платформы, обильные вознаграждения и регулярные акции придают всякую сессию даже еще более увлекательной. Ресурс работает быстро и стабильно, что предоставляет приятную игру. онлайн казино на реальные деньги – это площадка, где каждый поворот окажется стартом огромного приза. Сильно рекомендую попробовать!
**Прогон Хрумером: Эффективное SEO-Продвижение Вашего Сайта**
В мире интернет-маркетинга существует множество методов и инструментов для продвижения сайтов, и одним из самых мощных и популярных является прогон Хрумером.
Этот программный комплекс позволяет автоматизировать рутинные задачи SEO
и значительно улучшить позиции сайта в поисковых системах.
В этой статье мы подробно рассмотрим, что такое прогон Хрумером, как он работает и какие преимущества он может предложить.
**Что такое прогон Хрумером?**
Прогон Хрумером – это процесс автоматического размещения ссылок и сообщений на различных веб-ресурсах с использованием программы Хрумер.
Это позволяет существенно увеличить
количество обратных ссылок на ваш сайт, что является одним
из ключевых факторов для улучшения
его позиций в поисковых системах.
Программа автоматически регистрируется на
форумах, блогах, социальных сетях и
других платформах, размещая ссылки и сообщения согласно заданным параметрам.
**Как работает прогон Хрумером?**
1. **Подготовка ресурсов**: В первую очередь
необходимо составить список
целевых веб-ресурсов, на которых будет производиться размещение ссылок.
Это могут быть форумы, блоги, социальные сети и другие платформы.
2. **Создание шаблонов**: Далее
создаются шаблоны для размещения ссылок и сообщений.
Важно, чтобы тексты были уникальными и
соответствовали правилам выбранных
платформ.
3. **Настройка программы**:
В Хрумере настраиваются параметры подключения, капча-сервисы и прокси-серверы для обеспечения
стабильной работы программы.
4. **Запуск прогона**: После настройки всех параметров запускается процесс прогона,
который программа выполняет автоматически.
Хрумер регистрируется на сайтах,
размещает ссылки и сообщения, а также разгадывает капчи.
5. **Мониторинг и анализ**: Важно регулярно отслеживать результаты прогона, анализируя отчеты
о размещении ссылок и реакции аудитории.
Это позволяет корректировать стратегию продвижения и улучшать её эффективность.
**Преимущества прогона Хрумером**
1. **Экономия времени**: Прогон Хрумером позволяет
автоматизировать процесс размещения ссылок, что значительно
экономит время по сравнению с
ручным методом.
2. **Увеличение числа обратных
ссылок**: Автоматическое размещение
ссылок на множестве ресурсов способствует росту числа обратных ссылок, что положительно сказывается на
позиции сайта в поисковых системах.
3. **Повышение видимости сайта**: Прогон Хрумером помогает улучшить видимость вашего сайта в интернете, привлекая новую
аудиторию и увеличивая трафик.
4. **Гибкость и универсальность**: Хрумер поддерживает работу с множеством различных платформ и позволяет настраивать
параметры прогона в соответствии с вашими потребностями.
**Заключение**
Прогон Хрумером – это эффективный
метод автоматизации SEO-продвижения, который позволяет
значительно улучшить позиции вашего сайта в поисковых
системах. Используя этот мощный инструмент, вы
сможете сэкономить время и усилия, сосредоточившись на стратегически
важных задачах. Прогон Хрумером – это надежный способ увеличить число обратных ссылок, повысить видимость вашего сайта и привлечь больше
посетителей.
Here is my blog post; “http://www.dyc7.co.kr/bbs/board.php?bo_table=ejob_guide&wr_id=122848”
купить недвижимость вторичное Милославский район Рязанская область на сайте Gurava ru
Всем привет всех любителям игрового процесса! Хочу описать эмоциями об веб гейминг лучшие онлайн казино. Это игровая площадка впечатляет своим выбором игр: от классических слотов до живых игр с подлинными дилерами. Яркий и дизайнерский оформление сайта, богатые поощрения и ежедневные события превращают любую игру еще более еще волнительной. Платформа работает оперативно и надёжно, что обеспечивает комфортную геймплей. онлайн казино – это платформа, где любой спин окажется первым шагом большого выигрыша. Сильно рекомендую испытать!
Всем привет всех ценителям азартных игр! Хочу поделиться отзывами об онлайн гейминг онлайн казино. Это платформа радует своим разнообразием игровых автоматов: от традиционных слотов до игр с настоящими дилерами с реальными крупье. Цветной и модный дизайн платформы, щедрые поощрения и регулярные мероприятия добавляют всякую игру еще более еще более привлекательной. Портал работает мгновенно и бесперебойно, что обеспечивает удобную игру. казино с бездепозитным бонусом – это площадка, где каждый поворот вполне может стать отправной точкой крупной победы. Настоятельно советую тестировать!
Приветствую всех фанатам азартных игр! Хочу передать эмоциями об веб казино играть игровые автоматы бесплатно. Это казино поражает своим разнообразием слотов: от классических игровых автоматов до реальных игр с реальными крупье. Живой и дизайнерский дизайн портала, щедрые поощрения и частые события придают каждую партию даже более еще увлекательной. Платформа действует мгновенно и без проблем, что обеспечивает приятную игру. казино без депозита – это платформа, где любой поворот может стать стартом значительного успеха. Сильно советую попробовать!
Корпоративные Тарифы
https://tj-service.ru/novosti/samye-vygodnye-tarify-megafon-s-internetom
Приветствую всем ценителям азартных игр! Хочу рассказать отзывами об виртуальном гэмблинг селектор казино официальный сайт. Это казино радует своим ассортиментом игровых автоматов: от традиционных аппаратов до игр с настоящими дилерами с действительными крупье. Красочный и дизайнерский интерфейс портала, богатые премии и постоянные акции придают любую игру ещё более привлекательной. Сайт работает скоростно и стабильно, что даёт удобную игру. онлайн казино на деньги – это пространство, где каждый ставка вполне может стать первым шагом большого трофея. Настоятельно советую оценить!
**Прогон Хрумером: Эффективное SEO-Продвижение
Вашего Сайта**
В мире интернет-маркетинга существует множество методов и инструментов для продвижения сайтов, и одним из самых мощных и популярных является прогон Хрумером.
Этот программный комплекс позволяет автоматизировать рутинные задачи
SEO и значительно улучшить позиции сайта в поисковых системах.
В этой статье мы подробно рассмотрим, что такое прогон Хрумером, как
он работает и какие преимущества он может предложить.
**Что такое прогон Хрумером?**
Прогон Хрумером – это процесс автоматического размещения ссылок и сообщений на различных веб-ресурсах с использованием программы Хрумер.
Это позволяет существенно увеличить количество обратных ссылок на ваш сайт,
что является одним из ключевых факторов для улучшения
его позиций в поисковых системах.
Программа автоматически регистрируется на форумах, блогах, социальных сетях и других платформах, размещая ссылки и сообщения согласно заданным параметрам.
**Как работает прогон Хрумером?**
1. **Подготовка ресурсов**: В первую очередь необходимо составить список целевых веб-ресурсов, на которых будет
производиться размещение ссылок.
Это могут быть форумы, блоги, социальные сети
и другие платформы.
2. **Создание шаблонов**: Далее создаются шаблоны для размещения ссылок и сообщений.
Важно, чтобы тексты были уникальными
и соответствовали правилам выбранных
платформ.
3. **Настройка программы**:
В Хрумере настраиваются параметры подключения, капча-сервисы и
прокси-серверы для обеспечения
стабильной работы программы.
4. **Запуск прогона**: После настройки
всех параметров запускается процесс прогона, который программа выполняет автоматически.
Хрумер регистрируется на сайтах, размещает ссылки и сообщения,
а также разгадывает капчи.
5. **Мониторинг и анализ**: Важно регулярно отслеживать
результаты прогона, анализируя
отчеты о размещении ссылок и реакции аудитории.
Это позволяет корректировать стратегию продвижения и улучшать её эффективность.
**Преимущества прогона Хрумером**
1. **Экономия времени**: Прогон
Хрумером позволяет автоматизировать процесс размещения ссылок, что значительно
экономит время по сравнению с ручным методом.
2. **Увеличение числа обратных ссылок**: Автоматическое размещение ссылок на
множестве ресурсов способствует росту числа обратных ссылок, что положительно сказывается на позиции сайта в поисковых
системах.
3. **Повышение видимости сайта**:
Прогон Хрумером помогает улучшить видимость вашего сайта в интернете,
привлекая новую аудиторию и увеличивая трафик.
4. **Гибкость и универсальность**: Хрумер поддерживает работу
с множеством различных платформ и позволяет настраивать параметры прогона в
соответствии с вашими потребностями.
**Заключение**
Прогон Хрумером – это эффективный
метод автоматизации SEO-продвижения, который
позволяет значительно улучшить позиции
вашего сайта в поисковых системах.
Используя этот мощный инструмент, вы сможете сэкономить время и усилия, сосредоточившись на стратегически важных задачах.
Прогон Хрумером – это надежный способ увеличить число обратных
ссылок, повысить видимость вашего сайта и
привлечь больше посетителей.
my blog … “http://www.healthndream.com/gnuboard5/bbs/board.php?bo_table=qna_heartsine&wr_id=1949334”
Больше интересной информации о строительстве и ремонте можно прочитать на сайте https://stroyka-gid.ru. Только самые популярные статьи и обзоры процесса ремонта помещений и строительства зданий.
Support Support Very good
скачать торрент игры – GTA 6 на ПК, скачать торрент игры
ремонт телефонов в москве
Генераторы
https://rewarddebtor4.werite.net/zashchita-i-bezopasnost-kozhukhi-dlia-dizel-nykh-generatorov
**Прогон Хрумером: Эффективное SEO-Продвижение Вашего Сайта**
В мире интернет-маркетинга существует множество
методов и инструментов для продвижения сайтов, и одним из самых мощных и популярных является прогон Хрумером.
Этот программный комплекс позволяет автоматизировать рутинные задачи SEO
и значительно улучшить позиции сайта в поисковых
системах. В этой статье мы
подробно рассмотрим, что такое прогон Хрумером,
как он работает и какие преимущества
он может предложить.
**Что такое прогон Хрумером?**
Прогон Хрумером – это процесс автоматического размещения ссылок
и сообщений на различных веб-ресурсах с использованием программы
Хрумер. Это позволяет существенно увеличить количество обратных ссылок на
ваш сайт, что является одним из ключевых факторов для
улучшения его позиций в поисковых системах.
Программа автоматически регистрируется на форумах, блогах, социальных сетях и
других платформах, размещая ссылки и сообщения согласно заданным
параметрам.
**Как работает прогон Хрумером?**
1. **Подготовка ресурсов**: В первую очередь необходимо составить список целевых
веб-ресурсов, на которых будет производиться размещение ссылок.
Это могут быть форумы, блоги, социальные сети и другие платформы.
2. **Создание шаблонов**: Далее создаются шаблоны
для размещения ссылок и сообщений.
Важно, чтобы тексты были уникальными и соответствовали правилам выбранных платформ.
3. **Настройка программы**: В Хрумере
настраиваются параметры подключения, капча-сервисы и
прокси-серверы для обеспечения стабильной
работы программы.
4. **Запуск прогона**: После настройки всех параметров запускается процесс прогона, который
программа выполняет автоматически.
Хрумер регистрируется на
сайтах, размещает ссылки и сообщения,
а также разгадывает капчи.
5. **Мониторинг и анализ**: Важно регулярно отслеживать результаты
прогона, анализируя отчеты о размещении ссылок и реакции аудитории.
Это позволяет корректировать стратегию продвижения и улучшать её эффективность.
**Преимущества прогона Хрумером**
1. **Экономия времени**: Прогон Хрумером позволяет автоматизировать процесс размещения ссылок,
что значительно экономит время по сравнению с ручным методом.
2. **Увеличение числа обратных ссылок**: Автоматическое размещение ссылок на множестве ресурсов способствует росту числа обратных ссылок, что
положительно сказывается на позиции
сайта в поисковых системах.
3. **Повышение видимости сайта**:
Прогон Хрумером помогает улучшить видимость вашего
сайта в интернете, привлекая
новую аудиторию и увеличивая трафик.
4. **Гибкость и универсальность**:
Хрумер поддерживает работу с множеством различных платформ и позволяет настраивать параметры
прогона в соответствии с вашими потребностями.
**Заключение**
Прогон Хрумером – это эффективный метод автоматизации SEO-продвижения, который позволяет значительно улучшить
позиции вашего сайта в поисковых системах.
Используя этот мощный инструмент, вы сможете сэкономить
время и усилия, сосредоточившись
на стратегически важных задачах.
Прогон Хрумером – это надежный способ увеличить число обратных ссылок, повысить видимость вашего сайта
и привлечь больше посетителей.
Stop by my blog post “https://jejuatopycenter.kr:443/bbs/board.php?bo_table=schedule_v2&wr_id=14232”
Александр Овечкин главное разочарование в карьере – далее
Natursekt En Kreis Oralverkehr Unter Männer
Support Support Very good scfedu
Генераторы
https://ariesgemini3.werite.net/moshchnost-i-nadezhnost-dizel-nye-generatory-na-elektrostantsiiakh
Excellent write-up
https://www.abc-turystyki.pl/artykul/na-co-zwrocic-uwage-wybierajac-sie-do-zakopanego-wraz-z-dziecmi-349062
Корпоративные Тарифы
https://hairstyle-beauty.ru/arxivnye-tarify-mts-mozhno-li-ix-podklyuchit/.html
Генераторы
https://burnbengal6.bloggersdelight.dk/2024/06/03/%d0%b3%d0%be%d1%82%d0%be%d0%b2%d0%bd%d0%be%d1%81%d1%82%d1%8c-%d0%ba-%d0%bb%d1%8e%d0%b1%d1%8b%d0%bc-%d1%81%d0%b8%d1%82%d1%83%d0%b0%d1%86%d0%b8%d1%8f%d0%bc-%d0%bf%d0%be%d0%ba%d1%83%d0%bf%d0%ba%d0%b0/
**Прогон Хрумером: Эффективное SEO-Продвижение Вашего Сайта**
В мире интернет-маркетинга существует множество
методов и инструментов для продвижения сайтов, и одним из самых мощных и популярных является прогон Хрумером.
Этот программный комплекс позволяет
автоматизировать рутинные задачи SEO и значительно улучшить позиции сайта
в поисковых системах. В этой
статье мы подробно рассмотрим, что
такое прогон Хрумером, как он работает и какие преимущества он может предложить.
**Что такое прогон Хрумером?**
Прогон Хрумером – это процесс автоматического размещения ссылок и сообщений на различных веб-ресурсах с использованием программы Хрумер.
Это позволяет существенно увеличить количество обратных ссылок
на ваш сайт, что является одним
из ключевых факторов для улучшения его позиций в поисковых системах.
Программа автоматически регистрируется на форумах,
блогах, социальных сетях и других платформах, размещая ссылки и сообщения согласно заданным параметрам.
**Как работает прогон Хрумером?**
1. **Подготовка ресурсов**: В первую очередь необходимо составить список
целевых веб-ресурсов, на которых будет производиться
размещение ссылок. Это
могут быть форумы, блоги, социальные сети и другие платформы.
2. **Создание шаблонов**: Далее создаются шаблоны для размещения ссылок и сообщений.
Важно, чтобы тексты были уникальными и соответствовали правилам выбранных платформ.
3. **Настройка программы**: В Хрумере настраиваются параметры подключения, капча-сервисы и прокси-серверы для обеспечения стабильной работы программы.
4. **Запуск прогона**: После настройки всех параметров запускается процесс прогона, который программа выполняет автоматически.
Хрумер регистрируется на сайтах, размещает ссылки и сообщения, а также
разгадывает капчи.
5. **Мониторинг и анализ**: Важно регулярно отслеживать результаты прогона, анализируя
отчеты о размещении ссылок и реакции аудитории.
Это позволяет корректировать стратегию продвижения и улучшать её эффективность.
**Преимущества прогона Хрумером**
1. **Экономия времени**: Прогон Хрумером
позволяет автоматизировать
процесс размещения ссылок, что значительно
экономит время по сравнению с ручным
методом.
2. **Увеличение числа обратных
ссылок**: Автоматическое размещение ссылок на множестве ресурсов способствует росту числа обратных ссылок, что положительно сказывается
на позиции сайта в поисковых системах.
3. **Повышение видимости сайта**: Прогон
Хрумером помогает улучшить видимость вашего
сайта в интернете, привлекая новую аудиторию и
увеличивая трафик.
4. **Гибкость и универсальность**:
Хрумер поддерживает работу с множеством различных платформ и
позволяет настраивать параметры прогона в соответствии с вашими потребностями.
**Заключение**
Прогон Хрумером – это эффективный метод автоматизации SEO-продвижения, который позволяет значительно
улучшить позиции вашего сайта в поисковых системах.
Используя этот мощный инструмент, вы сможете
сэкономить время и усилия, сосредоточившись на стратегически важных задачах.
Прогон Хрумером – это надежный
способ увеличить число обратных ссылок, повысить видимость вашего сайта и привлечь больше посетителей.
Also visit my blog – “http://lamerpension.co.kr/www/bbs/board.php?bo_table=bod703&wr_id=236533”
контрольна робота з української мови – автореферати дисертацій з філософії, готові курсові роботи
недвижимость вторичное Кяхта Гурава.ru
lvb personal loan In addition, these kids are mostly sedentary from playing video games, and not getting exercise at all.
THE DAY BEFORE обзор игры – игры на PS5 или Xbox Series X/S., GTA 6 скачать бесплатно
buy IP votes online https://promobanger.com/
Корпоративные Тарифы
https://aprovedstore.ru/kakie-tarify-na-bilajne-samye-vygodnye-s-internetom/
https://www.instagram.com/asiapsiholog_family/
Учёные из СПбГУ перевёрнуто представление об эволюции крокодилов – читать
Unwinding after work has never been easier since I found Mult34 – naruto rule 34 . This site offers an extensive range of adult comics and cartoons, all available for free. It’s become my go-to place for relaxing and enjoying some high-quality adult content.
Mult34 – steven universe porn has everything you need for a great evening. The diverse selection ensures there’s something for every taste. If you’re looking for a free and entertaining way to end your day, Mult34 – boruto porn is the site to visit.
Генераторы
https://rewarddebtor7.bloggersdelight.dk/2024/06/03/%d0%b2%d0%b0%d1%88-%d0%b3%d0%b5%d0%bd%d0%b5%d1%80%d0%b0%d1%82%d0%be%d1%80-%d0%b2-%d0%b1%d0%b5%d0%b7%d0%be%d0%bf%d0%b0%d1%81%d0%bd%d0%be%d1%81%d1%82%d0%b8-%d0%ba%d0%be%d0%bd%d1%82%d0%b5%d0%b9%d0%bd/
vavada casino официальный сайт
montell williams This puts them in a dilemma when an unexpected expenditure turns up. The same day loans have been introduced in order to ensure that these aspirants get timely financial aid when required.
https://kristall-klining.ru/
of course like your website but you need to take a look at the spelling on quite
a few of your posts. Many of them are rife with spelling problems and I in finding it very troublesome to inform the truth then again I will certainly come again again.
Feel free to surf to my page خرید بک لینک
Генераторы
https://telegra.ph/Gotovnost-k-Lyubym-Situaciyam—Pokupka-Dizelnogo-Generatora-dlya-Doma-06-03
курсовые работы на заказ https://zakazat-kursovuyu-rabotu7.ru
Генераторы
https://telegra.ph/Kupit-benzinovyj-generator—kak-vybrat-luchshij-variant-dlya-vashego-doma-ili-dachi-06-03
сколько стоит уборка коттеджа
https://cleanprofispb.ru/
Youtuberin Natursekt Forum Probleme Nach Analverkehr
barriers to business Women jobs’s
Хотите увидеть минус 10 кг на весах через 10 дней? Наш Telegram-канал Как похудеть на 10 кг за 10 дней: советы экспертов – ваш идеальный помощник! Мы предлагаем эффективные диеты, тренировки и психологическую поддержку. Получите мотивацию и советы от профессионалов. Начните свой путь к идеальному телу прямо сейчас!
Recently, I saw a discussion in a Facebook group about an interesting site with adult comics. I decided to check it out and landed on Mult34 – porn manga . I was amazed by the variety of content and the quality of the materials.
I’ve revisited this site several times and always find something new. Mult34 – demon slayer rule 34 is definitely worth a visit if you love erotic comics and cartoons. I highly recommend it to all my friends and acquaintances.
My girlfriend and I wanted to spice up our evening with some adult comics, so we searched on Google and found Mult34 – pokemon porn . We spent the night indulging in a fantastic selection of erotic comics. It was a fun and exciting experience.
Mult34 – animated porn impressed us with its wide range of high-quality content. We found so many great stories that kept us entertained. If you’re searching for adult comics to enjoy together, Mult34 – fortnite porn is definitely worth checking out. We had a wonderful time.
Генераторы
https://canvas.instructure.com/eportfolios/2945364/Home/________
стоимость такси в новочеркасске https://zakaz-taxionline.ru
One night, my girlfriend and I decided to look for some adult fun. Google pointed us to Mult34 – porn comix , and we were instantly hooked. The site offers an extensive selection of erotic comics that kept us entertained for hours. We loved diving into the captivating stories together.
Mult34 – lady k and the sick man offers a unique blend of quality and variety, making it the ideal site for adult entertainment. If you’re looking for something special to enjoy with your partner, Mult34 – porncomics is the place to go. We had an amazing time and will definitely be back.
Генераторы
https://canvas.instructure.com/eportfolios/2945392/Home/________
служба поддержки такси такси онлайн
Генераторы
https://zonelight98.bloggersdelight.dk/2024/06/03/%d0%b3%d0%b5%d0%bd%d0%b5%d1%80%d0%b0%d1%82%d0%be%d1%80-%d0%b4%d0%bb%d1%8f-%d1%87%d0%b0%d1%81%d1%82%d0%bd%d0%be%d0%b3%d0%be-%d0%b4%d0%be%d0%bc%d0%b0-%d0%ba%d0%b0%d0%ba%d0%be%d0%b9-%d0%b2%d1%8b%d0%b1/
geinoutime.com
여전히 그의 무지하고 게으른 아들입니까?
Yesterday, while I was at work, my sister stole my apple ipad and tested to see if it can survive a 25 foot drop, just so she can be a youtube sensation. My iPad is now destroyed and she has 83 views. I know this is entirely off topic but I had to share it with someone!
https://local-urban-eats.mn.co/posts/55565472
https://www.vietnammm.com/
https://bookmarkick.com/story17225087/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2%D1%81%D0%BB%D0%B5%D0%B4%D1%81%D1%82%D0%B2%D0%B8%D0%B5-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://jaidenb8c58.qodsblog.com/27110815/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2-%D1%83%D0%B3%D0%BE%D0%B4%D1%83-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://thebookmarkfree.com/story17162277/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
Poloch Nach Analsex Geweitet Darmflora Analsex
курсовые работы на заказ https://zakazat-kontrolnuyu7.ru
Ищете лучшие предложения по кредитам? Подписывайтесь на канал Кредиты на карту онлайн! У нас собраны самые выгодные варианты онлайн кредитов, а также много полезной информации о том, как и где лучше взять кредит. Наши эксперты поделятся с вами ценными советами и расскажут все о кредитной истории, чтобы вы могли принимать обоснованные финансовые решения.
Завод «СХТ» предоставляет наилучшее весоизмерительное оборудование. Мы имеем свою метрологическую лабораторию, а также сервисную службу. Осуществляем в год поверку больше 2000 единиц автомобильных весов! https://xn--q1aci.xn--p1ai/ – сайт, где вы можете узнать о том, каким нынешний весоизмерительный комплекс должен быть. Здесь есть фотогалерея и отзывы довольных клиентов. Можете заказать у нас коллейные, электронные, переносные автомобильные весы. Обращайтесь к нам, мы быстро реагируем на заявки и консультируем по телефону по всем вопросам.
One night, my girlfriend and I decided to look for some adult fun. Google pointed us to Mult34 – porn comic , and we were instantly hooked. The site offers an extensive selection of erotic comics that kept us entertained for hours. We loved diving into the captivating stories together.
Mult34 – furry porn offers a unique blend of quality and variety, making it the ideal site for adult entertainment. If you’re looking for something special to enjoy with your partner, Mult34 – multiporn is the place to go. We had an amazing time and will definitely be back.
решение задач на заказ https://resheniye-zadach7.ru заказать онлайн
https://mashable.com/article/artist-vandalizes-snapchat-ar-jeff-coons-collab
Today, I went to the beach with my children. I found a sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She put the shell to her ear and screamed. There was a hermit crab inside and it pinched her ear. She never wants to go back! LoL I know this is totally off topic but I had to tell someone!
https://ztndz.com/story19044271/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B0%D1%80%D0%BC%D0%B0%D1%86%D0%B5%D0%B2%D1%82%D0%B0
http://nagaevo.ekafe.ru/viewtopic.php?f=86&t=2355
https://210list.com/story17674484/%D0%A4%D0%B0%D0%BB%D1%8C%D1%88%D0%B8%D0%B2%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D1%8D%D1%82%D0%BE-%D0%BD%D0%B5-%D0%A1%D1%82%D0%BE%D0%B8%D1%82-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://bookmarkmargin.com/story17123466/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9F%D0%B5%D1%80%D0%BC%D0%B8
https://www.chabab-belouizdad.org/
Parkplatzsex Herzogenrath Chlamydien Ansteckung Durch Oralverkehr
https://bicrypto.exchange – crypto exchange software. White label, open-source exchange solution with a focus on a super-fast, pixel-perfect interface and robust security. High-performance platform with a robust internal architecture. Leverages the capabilities of Nuxt3 to create a cutting-edge user interface.
аяўаска купить https://travelservic.ru
Почему стоит построить дом из бруса 9х12 | Секреты выбора проекта дома из бруса 9х12 | Как создать уютный интерьер в доме из бруса 9х12 | Секреты уютного интерьера в доме из бруса 9х12 | Выбор материалов для теплоизоляции и вентиляции в доме из бруса 9х12 | Выбор фундамента для дома из бруса 9х12 | Как обустроить участок вокруг дома из бруса 9х12 | Как выбрать мебель для дома из бруса 9х12 | Как обустроить зону отдыха в доме из бруса 9х12 | Расходы на строительство дома из бруса 9х12
одноэтажный дом из бруса 9х12 https://domizbrusa-9x12spb.ru/ .
What a stuff of un-ambiguity and preserveness of valuable knowledge on the topic of unexpected feelings.
http://maxima.2ua.in.ua/viewtopic.php?f=3&t=4950
https://bookmarkspiral.com/story17080100/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D0%B2%D1%8B%D1%81%D1%88%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8
https://wildbookmarks.com/story17231620/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9C%D0%BE%D1%81%D0%BA%D0%B2%D0%B5
http://www.lada-xray.net/member.php?u=23613
https://bookmarkshq.com/story18365459/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%82%D1%80%D0%BE%D0%B8%D1%82%D0%B5%D0%BB%D1%8F
https://kkc-cleaning.ru/
i desperately need money In short, effective communication is one of the essential factors for the workers’ satisfaction.
Генераторы
https://diigo.com/0wglbz
Генераторы
https://answerlook94.werite.net/kupit-benzinovyi-generator-kak-vybrat-luchshii-variant-dlia-vashego-doma-ili
This is really fascinating, You are a very skilled blogger. I have joined your rss feed and look ahead to searching for extra of your wonderful post. Also, I have shared your website in my social networks
https://www.afchornchurch.com/travel/
http://toyota-porte.ru/forums/index.php?autocom=gallery&req=si&img=2010
https://bookmarkextent.com/story18460979/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A2%D1%8E%D0%BC%D0%B5%D0%BD%D1%8C
http://cekresipos.com/
https://www.thanglongwaterpuppet.org/en/
https://marafet-km.ru/
Генераторы
https://canvas.instructure.com/eportfolios/2945331/Home/__________
Hello colleagues, its enormous piece of writing concerning educationand completely defined, keep it up all the time.
https://top10bookmark.com/story16994997/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9D%D0%B8%D0%B6%D0%BD%D0%B5%D0%BC-%D0%9D%D0%BE%D0%B2%D0%B3%D0%BE%D1%80%D0%BE%D0%B4%D0%B5
https://modernbookmarks.com/story16928534/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%80%D0%B0%D1%87%D0%B0
https://tysonkmnml.bloggosite.com/32986779/about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://delivery-containers.ru/
http://www.buro-alfa.ru/main.php?d=1&url=
купить диплом энергетика
ссылка на страницу
Hi, this weekend is good in favor of me, because this occasion i am reading this enormous educational article here at my home.
cs-online.ru/forum/index.php?showtopic=13633&mode=linear
irc71.ru/index.php/jomsocial/groups/viewbulletin/142-za-skolko-imenno-vozmozhno-budet-zakazat-diplom-vuza-sejchas?groupid=47
http://www.mountbarkertourismwa.com.au/contact_us.php
u-cars.ru/modules.php?name=Your_Account&op=userinfo&username=oqorisol
http://www.forums.wolflair.com/member.php?u=110846
unsecured loan bc Several years ago, Joe Lagennusa was having a tough time making ends meet, so the sales manager in Florida turned to online payday lenders.
Хотите узнать все о потребительских кредитах? Подписывайтесь на наш канал Потребительские кредиты – вся информация! Мы делаем подборки самых выгодных предложений, рассказываем о рисках и помогаем разобраться в нюансах кредитования. Получите максимум информации!
https://uborkadoma-spb.ru/
купить диплом
веб сайт
I loved as much as you will receive carried out right here. The sketch is attractive, your authored material stylish. nonetheless, you command get got an impatience over that you wish be delivering the following. unwell unquestionably come further formerly again since exactly the same nearly very often inside case you shield this hike.
https://oldforum.citysakh.ru/?talkid=26126
https://annsummerspromocode72603.onzeblog.com/26862907/the-smart-trick-of-marketing-that-no-one-is-discussing
https://turkish-economy80246.buyoutblog.com/26811621/the-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA-diaries
http://webnewsrealty.ru/byistryiy-i-effektivnyiy-sposob-poluchit-diplom-zakazhite-onlayn-seychas
https://dvoinoi-brus.ru/
There’s nothing better than winding down after work with some adult entertainment. I found Mult34 – free use porn , a site that offers a vast collection of erotic comics and cartoons for free. It’s become my favorite place to relax and enjoy quality content.
Mult34 – ankha porn diverse range ensures you’ll never get bored. The site has something for every preference, and the best part is that it’s all free. If you need a way to relax after a long day, check out Mult34 – the loud house porn .
купить аттестат 6landik-diploms.com
Hi I am so glad I found your blog, I really found you by mistake, while I was searching on Digg for something else, Nonetheless I am here now and would just like to say kudos for a marvelous post and a all round exciting blog (I also love the theme/design), I don’t have time to read through it all at the moment but I have saved it and also added in your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the awesome b.
https://vsekruizi.ru/holidays/
https://bookmarkingalpha.com/story17097675/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
https://thebookmarknight.com/story17204421/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://a123.woobi.co.kr/thread-1267-page-9.html
http://silich.ru/forum/member.php?tab=visitor_messaging&u=4810&page=3
blog link Bank cards
безопасно,
Современное оборудование и материалы, для поддержания здоровья рта,
Профессиональное лечение и консультации, для вашей улыбки,
Индивидуальный подход к каждому пациенту, для вашего комфорта и уверенности,
Инновационные методы стоматологии, для вашего долгосрочного удовлетворения,
Экстренная помощь в любое время суток, для вашего долгосрочного удовлетворения,
Индивидуальный план лечения для каждого пациента, для вашего здоровья и благополучия
зуби лікування зуби лікування .
view it now Bank cards
Hi,
What a cool blog!
Is it okay I scrape this and share this with my community subscribers?
My site is about Korean 야튜브
If ever your interested, feel free to visit my channel and check it out.
Thanks a lot and Keep up the good work!
website link benumb
how does interest work on a personal loan The amount borrowed can be subsequently repaid within a period of 14-31 days.
important link carding 2024
look at this site CC shop
WOW just what I was searching for. Came here by searching for %keyword%
https://apollobookmarks.com/story17040106/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
https://enkor.ru/forum/viewtopic.php?t=11397&view=previous
https://1abakan.ru/forum/showthread-78987/
https://www.omaada.com/blogs/105935/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%B4%D0%B8%D0%BD-%D0%BA%D0%BB%D0%B8%D0%BA-%D0%A3-%D0%BD%D0%B0%D1%81-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE-%D0%B8-%D0%BF%D1%80%D0%BE%D1%81%D1%82%D0%BE
http://www.edpillsfinder.com/
казино регистрации https://mgkhs.ru/
check out here Best cc shop
сайдинг виниловый цена https://kanoner.com
like this carding 2024
Do you have any video of that? I’d care to find out more details.
my-digital.ro/contact/
niagara-trade.com.ua/katalog/avtomatika/
http://www.ekspoteh.ru/index.php?name=account&op=info&uname=agizemuq
prikol100500.ru/kupit-diplom-s-besplatnoy-dostavkoy-po-vsey-rossii
bouffordca.com/Emailscam.htm
find more information Best cc+cvv
Good day 🙂
What a good blog!
Is it okay I scrape this and share this with my site
subscribers?
My blog is about Korean 야동
If ever you are interested, feel free to visit my blog
and check it out.
Thanks and Keep up the good work!
гарантированно,
Лучшие стоматологи города, для поддержания здоровья рта,
Современные методы стоматологии, для вашего уверенного выбора,
Индивидуальный подход к каждому пациенту, для вашей радости и улыбки,
Комплексное восстановление утраченных зубов, для вашего здоровья и красоты улыбки,
Профессиональная гигиена полости рта, для вашего здоровья и уверенности в себе,
Заботливое отношение и внимательный подход, для вашего здоровья и благополучия
здорові зуби https://stomatologichnaklinikafghy.ivano-frankivsk.ua/ .
безопасно,
Современное оборудование и материалы, для крепких и здоровых зубов,
Профессиональное лечение и консультации, для вашей улыбки,
Индивидуальный подход к каждому пациенту, для вашего здоровья и благополучия,
Эффективное лечение зубов и десен, для вашего комфорта и уверенности,
Экстренная помощь в любое время суток, для вашего здоровья и уверенности в себе,
Современное лечение заболеваний полости рта, для вашей уверенной улыбки
видалення зубів видалення зубів .
check out the post right here Best cc shop
This is really interesting, You are a very skilled blogger. I have joined your feed and look forward to seeking more of your excellent post. Also, I’ve shared your website in my social networks!
https://amazonpromocodefortoday38146.blogginaway.com/27372777/a-secret-weapon-for-marketing
http://www.cialisonlinerx.com/
https://socialbuzztoday.com/story2393460/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B0%D1%81%D1%81%D0%B0%D0%B6%D0%B8%D1%81%D1%82%D0%B0
http://autogroupe.ru/page/4
http://www.ytchebnik.ru/334.html
Huawei серверное оборудование Современное серверное оборудование Huawei для вашего бизнеса.
Click This Link Bank cards
find more Bank cards
цена хамона за кг производство сыровяленых деликатесов
Good post. I learn something totally new and challenging on blogs I stumbleupon every day. It’s always helpful to read articles from other authors and practice a little something from other websites.
http://probox-club.ru/forums/index.php?autocom=gallery&req=si&img=4849
https://webnowmedia.com/story2388351/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D1%81%D1%80%D0%B5%D0%B4%D0%BD%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8
http://student-news.ru/poluchite-svoy-diplom-bez-lishnih-hlopot-prisoedinyaytes-seychas
https://carbonfacesocial.org/blogs/65180/%D0%91%D1%8B%D1%81%D1%82%D1%80%D1%8B%D0%B9-%D0%B8-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D1%81%D0%BF%D0%BE%D1%81%D0%BE%D0%B1-%D0%BF%D0%BE%D0%BB%D1%83%D1%87%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A3-%D0%BD%D0%B0%D1%81-%D1%8D%D1%82%D0%BE-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE
https://privatehomecookingservice.com/
go to these guys carding 2024
Все самое интересное из мира игр https://unionbattle.ru обзоры, статьи и ответы на вопросы
Pretty component to content. I just stumbled upon your weblog and in accession capital to claim that I acquire actually enjoyed account your weblog posts. Anyway I’ll be subscribing in your feeds and even I fulfillment you get entry to constantly quickly.
https://pr7bookmark.com/story17267370/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B5%D1%85%D0%B0%D0%BD%D0%B8%D0%BA%D0%B0
https://dvoinoi-brus.ru/
https://rem-penata.ru/remont/remont-kvartir-pod-klyuch
https://foro.rune-nifelheim.com/general-ragnarok-m/sdelajte-svoi-mechty-realnostyu-poluchite-svoj-diplom-zdes!/
https://deans1u88.full-design.com/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-69898065
Генераторы
https://telegra.ph/Obespechte-Bezopasnost-i-Prodolzhitelnost-Raboty—Kozhuhi-dlya-Dizelnyh-Generatorov-06-03
Hi to every single one, it’s in fact a good for me to visit this web site, it includes helpful Information.
https://investing-tr47924.myparisblog.com/27230446/the-single-best-strategy-to-use-for-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://allonlinesport.ru/kupit-diplom-bez-stressa-u-nas-vse-prosto/
https://musor-kill.ru/kamaz20mk.html
https://bookmarkmoz.com/story17076276/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9D%D0%BE%D0%B2%D0%BE%D1%81%D0%B8%D0%B1%D0%B8%D1%80%D1%81%D0%BA%D0%B5
https://shanecnyir.bloginder.com/27323038/detailed-notes-on-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
What a material of un-ambiguity and preserveness of precious knowledge regarding unpredicted emotions.
http://www.iasi.org/legal.html
bbs.heyshell.com/forum.php?mod=viewthread&tid=27609
myfootballday.ru/page/14
xemgiai.com/phap-luat-la-gi
u-cars.ru/modules.php?name=Your_Account&op=userinfo&username=oqorisol
https://cleanb2b.ru/
эффективно,
Индивидуальный подход к каждому пациенту, для крепких и здоровых зубов,
Профессиональное лечение и консультации, для вашей улыбки,
Комфортные условия и дружественный персонал, для вашего здоровья и благополучия,
Инновационные методы стоматологии, для вашего здоровья и красоты улыбки,
Экстренная помощь в любое время суток, для вашего комфорта и удовлетворения,
Современное лечение заболеваний полости рта, для вашей уверенной улыбки
лікування зубів у дітей лікування зубів у дітей .
mega darknet market – мега даркнет маркет ссылка на сайт, мега даркнет маркет ссылка
https://www.codesdope.com/discussion/amazing-cool/
Looking to buy Ceylon cinnamon powder? You’ve come to the right place! We offer pure Ceylon cinnamon powder, known for its sweet, delicate flavor and numerous health benefits. If you’re wondering where to buy Ceylon cinnamon powder, look no further. Our Ceylon cinnamon for sale is available for purchase online, making it convenient for you to get this high-quality spice delivered straight to your door.
In addition to our pure Ceylon cinnamon powder, we also offer a variety of other products. If you’re a fan of herbal teas, consider trying Samahan tea. You can easily buy Samahan tea online through our store. It’s a wonderful blend of herbs and spices that supports your overall well-being.
For those who enjoy baking or cooking with coconut, we have desiccated coconut available. Wondering where to buy desiccated coconut? You can find it here, along with our extensive range of cinnamon products.
Speaking of cinnamon, our product line includes more than just powder. We also have Ceylon cinnamon sticks, perfect for adding a touch of flavor to your dishes or beverages. If you’re looking to purchase real cinnamon sticks online, we’ve got you covered.
Our selection doesn’t stop there. We offer cinnamon lotion and cinnamon body lotion for those who love the scent and benefits of cinnamon in their skincare routine. Additionally, you can find cinnamon shampoo and even cinnamon toothpicks at an affordable price.
For those interested in supplements, we have a range of Ceylon cinnamon supplements for sale. These supplements are a convenient way to incorporate the benefits of Ceylon cinnamon into your daily routine. You can buy Ceylon cinnamon supplements from us, ensuring you’re getting the best quality available.
Lastly, don’t forget to check out our Ceylon cinnamon tea bags, perfect for a soothing cup of tea at any time of the day. With our wide selection, you’re sure to find exactly what you need. Shop with us today for all your cinnamon and specialty product needs!
https://telegra.ph/Ceylon-Cinnamon-Capsules-Benefits-Dosage-and-Where-to-Buy-the-Best-Supplements-06-03
If you’re a fan of unique and flavorful dishes, you must try the Cinnamon Pork Cutlets Recipe. This delightful recipe brings out the best in pork with the warm, aromatic touch of cinnamon. For the best results, make sure to use Ceylon cinnamon sticks instead of the more common Cassia cinnamon. Wondering about the difference? When it comes to Ceylon Cinnamon Sticks vs. Cassia Cinnamon, Ceylon cinnamon is known for its sweeter, more delicate flavor, while Cassia has a stronger, more pungent taste. This distinction makes Ceylon the preferred choice for dishes where a subtle spice is desired.
Using Ceylon cinnamon powder in your cooking can elevate your meals to new heights. But do you know how to use Ceylon cinnamon powder in your favorite recipes? This versatile spice can be added to both sweet and savory dishes. Sprinkle it on your morning oatmeal, mix it into smoothies, or incorporate it into baked goods for a delicious twist. It’s also fantastic in savory recipes like curries, stews, and the aforementioned pork cutlets.
Apart from its culinary uses, Ceylon cinnamon offers numerous health benefits. Ceylon cinnamon capsules are a convenient way to enjoy these benefits. These supplements are packed with antioxidants and have anti-inflammatory properties. If you’re interested in the advantages, the Ceylon cinnamon capsules can help with blood sugar regulation, improving digestion, and boosting overall health. For those wondering about the benefits, dosage, and where to buy the best supplements, it’s recommended to take a look at reputable online stores that specialize in natural health products. The suggested dosage varies, so always follow the manufacturer’s instructions or consult with a healthcare professional.
Whether you’re cooking up a delicious meal or looking to enhance your health, Ceylon cinnamon is a versatile and beneficial spice to have on hand. Enjoy exploring its uses and benefits in your kitchen and beyond!
безопасно,
Лучшие стоматологи города, для крепких и здоровых зубов,
Современные методы стоматологии, для вашего удобства,
Индивидуальный подход к каждому пациенту, для вашего комфорта и уверенности,
Инновационные методы стоматологии, для вашего долгосрочного удовлетворения,
Экстренная помощь в любое время суток, для вашего комфорта и удовлетворения,
Индивидуальный план лечения для каждого пациента, для вашего здоровья и благополучия
стоматологія франківськ стоматологія франківськ .
Hi, always i used to check weblog posts here early in the daylight, because i like to gain knowledge of more and more.
https://bookmarkjourney.com/story17126248/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%92%D0%BE%D1%80%D0%BE%D0%BD%D0%B5%D0%B6%D0%B5
http://morskie-cruizy.ru/
https://umorforme.ru/diplom-s-garantiey-kachestva-vyiberite-nas
http://www.downtowncookieco.com/
https://tysonrplid.get-blogging.com/27233735/little-known-facts-about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://steemit.com/hive-148497/@tanviryousafzai/morning-tea
Looking to buy Ceylon cinnamon powder? You’ve come to the right place! We offer pure Ceylon cinnamon powder, known for its sweet, delicate flavor and numerous health benefits. If you’re wondering where to buy Ceylon cinnamon powder, look no further. Our Ceylon cinnamon for sale is available for purchase online, making it convenient for you to get this high-quality spice delivered straight to your door.
In addition to our pure Ceylon cinnamon powder, we also offer a variety of other products. If you’re a fan of herbal teas, consider trying Samahan tea. You can easily buy Samahan tea online through our store. It’s a wonderful blend of herbs and spices that supports your overall well-being.
For those who enjoy baking or cooking with coconut, we have desiccated coconut available. Wondering where to buy desiccated coconut? You can find it here, along with our extensive range of cinnamon products.
Speaking of cinnamon, our product line includes more than just powder. We also have Ceylon cinnamon sticks, perfect for adding a touch of flavor to your dishes or beverages. If you’re looking to purchase real cinnamon sticks online, we’ve got you covered.
Our selection doesn’t stop there. We offer cinnamon lotion and cinnamon body lotion for those who love the scent and benefits of cinnamon in their skincare routine. Additionally, you can find cinnamon shampoo and even cinnamon toothpicks at an affordable price.
For those interested in supplements, we have a range of Ceylon cinnamon supplements for sale. These supplements are a convenient way to incorporate the benefits of Ceylon cinnamon into your daily routine. You can buy Ceylon cinnamon supplements from us, ensuring you’re getting the best quality available.
Lastly, don’t forget to check out our Ceylon cinnamon tea bags, perfect for a soothing cup of tea at any time of the day. With our wide selection, you’re sure to find exactly what you need. Shop with us today for all your cinnamon and specialty product needs!
blacksprut вход – тор blacksprut, блэкспрут сайт
https://earl-clean.ru/
https://medium.com/@seonza100/cinnamon-pork-cutlets-recipe-quick-and-flavorful-6d1bd67df25a
If you’re a fan of unique and flavorful dishes, you must try the Cinnamon Pork Cutlets Recipe. This delightful recipe brings out the best in pork with the warm, aromatic touch of cinnamon. For the best results, make sure to use Ceylon cinnamon sticks instead of the more common Cassia cinnamon. Wondering about the difference? When it comes to Ceylon Cinnamon Sticks vs. Cassia Cinnamon, Ceylon cinnamon is known for its sweeter, more delicate flavor, while Cassia has a stronger, more pungent taste. This distinction makes Ceylon the preferred choice for dishes where a subtle spice is desired.
Using Ceylon cinnamon powder in your cooking can elevate your meals to new heights. But do you know how to use Ceylon cinnamon powder in your favorite recipes? This versatile spice can be added to both sweet and savory dishes. Sprinkle it on your morning oatmeal, mix it into smoothies, or incorporate it into baked goods for a delicious twist. It’s also fantastic in savory recipes like curries, stews, and the aforementioned pork cutlets.
Apart from its culinary uses, Ceylon cinnamon offers numerous health benefits. Ceylon cinnamon capsules are a convenient way to enjoy these benefits. These supplements are packed with antioxidants and have anti-inflammatory properties. If you’re interested in the advantages, the Ceylon cinnamon capsules can help with blood sugar regulation, improving digestion, and boosting overall health. For those wondering about the benefits, dosage, and where to buy the best supplements, it’s recommended to take a look at reputable online stores that specialize in natural health products. The suggested dosage varies, so always follow the manufacturer’s instructions or consult with a healthcare professional.
Whether you’re cooking up a delicious meal or looking to enhance your health, Ceylon cinnamon is a versatile and beneficial spice to have on hand. Enjoy exploring its uses and benefits in your kitchen and beyond!
https://www.domestika.org/en/projects/390644-gullon-splash-cookie
Looking to buy Ceylon cinnamon powder? You’ve come to the right place! We offer pure Ceylon cinnamon powder, known for its sweet, delicate flavor and numerous health benefits. If you’re wondering where to buy Ceylon cinnamon powder, look no further. Our Ceylon cinnamon for sale is available for purchase online, making it convenient for you to get this high-quality spice delivered straight to your door.
In addition to our pure Ceylon cinnamon powder, we also offer a variety of other products. If you’re a fan of herbal teas, consider trying Samahan tea. You can easily buy Samahan tea online through our store. It’s a wonderful blend of herbs and spices that supports your overall well-being.
For those who enjoy baking or cooking with coconut, we have desiccated coconut available. Wondering where to buy desiccated coconut? You can find it here, along with our extensive range of cinnamon products.
Speaking of cinnamon, our product line includes more than just powder. We also have Ceylon cinnamon sticks, perfect for adding a touch of flavor to your dishes or beverages. If you’re looking to purchase real cinnamon sticks online, we’ve got you covered.
Our selection doesn’t stop there. We offer cinnamon lotion and cinnamon body lotion for those who love the scent and benefits of cinnamon in their skincare routine. Additionally, you can find cinnamon shampoo and even cinnamon toothpicks at an affordable price.
For those interested in supplements, we have a range of Ceylon cinnamon supplements for sale. These supplements are a convenient way to incorporate the benefits of Ceylon cinnamon into your daily routine. You can buy Ceylon cinnamon supplements from us, ensuring you’re getting the best quality available.
Lastly, don’t forget to check out our Ceylon cinnamon tea bags, perfect for a soothing cup of tea at any time of the day. With our wide selection, you’re sure to find exactly what you need. Shop with us today for all your cinnamon and specialty product needs!
модульные системы хранения вещей для гардеробной
квартиры в екатеринбурге цены https://kupit-kvartiruekb.ru
https://penzu.com/p/1f8163d78c446e4e
If you’re a fan of unique and flavorful dishes, you must try the Cinnamon Pork Cutlets Recipe. This delightful recipe brings out the best in pork with the warm, aromatic touch of cinnamon. For the best results, make sure to use Ceylon cinnamon sticks instead of the more common Cassia cinnamon. Wondering about the difference? When it comes to Ceylon Cinnamon Sticks vs. Cassia Cinnamon, Ceylon cinnamon is known for its sweeter, more delicate flavor, while Cassia has a stronger, more pungent taste. This distinction makes Ceylon the preferred choice for dishes where a subtle spice is desired.
Using Ceylon cinnamon powder in your cooking can elevate your meals to new heights. But do you know how to use Ceylon cinnamon powder in your favorite recipes? This versatile spice can be added to both sweet and savory dishes. Sprinkle it on your morning oatmeal, mix it into smoothies, or incorporate it into baked goods for a delicious twist. It’s also fantastic in savory recipes like curries, stews, and the aforementioned pork cutlets.
Apart from its culinary uses, Ceylon cinnamon offers numerous health benefits. Ceylon cinnamon capsules are a convenient way to enjoy these benefits. These supplements are packed with antioxidants and have anti-inflammatory properties. If you’re interested in the advantages, the Ceylon cinnamon capsules can help with blood sugar regulation, improving digestion, and boosting overall health. For those wondering about the benefits, dosage, and where to buy the best supplements, it’s recommended to take a look at reputable online stores that specialize in natural health products. The suggested dosage varies, so always follow the manufacturer’s instructions or consult with a healthcare professional.
Whether you’re cooking up a delicious meal or looking to enhance your health, Ceylon cinnamon is a versatile and beneficial spice to have on hand. Enjoy exploring its uses and benefits in your kitchen and beyond!
This text is priceless. When can I find out more?
planeta-alvi.es/carcasa-rigida-samsung-j5-2017-2629.html
razvodka-mostov.ru/press/70/
usaessayexperts.com/faq/
cerebremediahosting.xyz/dolcescents.com/details/09
russiafreedom.ru/question/titan-s-teplakom/
https://forums.hitched.co.uk/chat/forums/thread/i-need-a-cant-fail-cookie-recepie-please-61412/
Looking to buy Ceylon cinnamon powder? You’ve come to the right place! We offer pure Ceylon cinnamon powder, known for its sweet, delicate flavor and numerous health benefits. If you’re wondering where to buy Ceylon cinnamon powder, look no further. Our Ceylon cinnamon for sale is available for purchase online, making it convenient for you to get this high-quality spice delivered straight to your door.
In addition to our pure Ceylon cinnamon powder, we also offer a variety of other products. If you’re a fan of herbal teas, consider trying Samahan tea. You can easily buy Samahan tea online through our store. It’s a wonderful blend of herbs and spices that supports your overall well-being.
For those who enjoy baking or cooking with coconut, we have desiccated coconut available. Wondering where to buy desiccated coconut? You can find it here, along with our extensive range of cinnamon products.
Speaking of cinnamon, our product line includes more than just powder. We also have Ceylon cinnamon sticks, perfect for adding a touch of flavor to your dishes or beverages. If you’re looking to purchase real cinnamon sticks online, we’ve got you covered.
Our selection doesn’t stop there. We offer cinnamon lotion and cinnamon body lotion for those who love the scent and benefits of cinnamon in their skincare routine. Additionally, you can find cinnamon shampoo and even cinnamon toothpicks at an affordable price.
For those interested in supplements, we have a range of Ceylon cinnamon supplements for sale. These supplements are a convenient way to incorporate the benefits of Ceylon cinnamon into your daily routine. You can buy Ceylon cinnamon supplements from us, ensuring you’re getting the best quality available.
Lastly, don’t forget to check out our Ceylon cinnamon tea bags, perfect for a soothing cup of tea at any time of the day. With our wide selection, you’re sure to find exactly what you need. Shop with us today for all your cinnamon and specialty product needs!
My partner and I absolutely love your blog and find the majority of your post’s to be just what I’m looking for. Would you offer guest writers to write content available for you? I wouldn’t mind publishing a post or elaborating on a number of the subjects you write about here. Again, awesome web site!
https://diplomdoc1.ru/
https://bookmarketmaven.com/story17369478/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B5%D0%BD%D0%B5%D0%B4%D0%B6%D0%B5%D1%80%D0%B0
https://www.iasi.org/
http://kingcityrp.moibb.ru/viewtopic.php?t=338
https://deporfc.com/?cat=1
система стеллажей для гардеробной
выдвижные гардеробные системы
https://pastelink.net/uv4vgs63
If you’re a fan of unique and flavorful dishes, you must try the Cinnamon Pork Cutlets Recipe. This delightful recipe brings out the best in pork with the warm, aromatic touch of cinnamon. For the best results, make sure to use Ceylon cinnamon sticks instead of the more common Cassia cinnamon. Wondering about the difference? When it comes to Ceylon Cinnamon Sticks vs. Cassia Cinnamon, Ceylon cinnamon is known for its sweeter, more delicate flavor, while Cassia has a stronger, more pungent taste. This distinction makes Ceylon the preferred choice for dishes where a subtle spice is desired.
Using Ceylon cinnamon powder in your cooking can elevate your meals to new heights. But do you know how to use Ceylon cinnamon powder in your favorite recipes? This versatile spice can be added to both sweet and savory dishes. Sprinkle it on your morning oatmeal, mix it into smoothies, or incorporate it into baked goods for a delicious twist. It’s also fantastic in savory recipes like curries, stews, and the aforementioned pork cutlets.
Apart from its culinary uses, Ceylon cinnamon offers numerous health benefits. Ceylon cinnamon capsules are a convenient way to enjoy these benefits. These supplements are packed with antioxidants and have anti-inflammatory properties. If you’re interested in the advantages, the Ceylon cinnamon capsules can help with blood sugar regulation, improving digestion, and boosting overall health. For those wondering about the benefits, dosage, and where to buy the best supplements, it’s recommended to take a look at reputable online stores that specialize in natural health products. The suggested dosage varies, so always follow the manufacturer’s instructions or consult with a healthcare professional.
Whether you’re cooking up a delicious meal or looking to enhance your health, Ceylon cinnamon is a versatile and beneficial spice to have on hand. Enjoy exploring its uses and benefits in your kitchen and beyond!
Fantastic blog you have here but I was wondering if you knew of any community forums that cover the same topics discussed in this article? I’d really love to be a part of online community where I can get advice from other experienced individuals that share the same interest. If you have any recommendations, please let me know. Bless you!
https://socialrator.com/story7096471/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%BE%D0%B2%D0%B0%D1%80%D0%B0
https://v-sobchenko.ru/
https://mushroom-chocolate14691.blogpostie.com/48882492/helping-the-others-realize-the-advantages-of-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://gram-alt-n-investing16935.wssblogs.com/26795105/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-an-overview
http://poltavagok.ru/zakazat-diplom-nikogda-ne-byilo-proshhe-poprobuyte-seychas/
купить диплом повара http://6landik-diploms.com/
Keep up the fantastic piece of work, I read
few posts on this website and I believe that your blog is rattling interesting and contains sets of fantastic information.
Feel free to visit my web-site; rent movie online
https://www.adrex.com/en/forum/climbing/what-dishes-and-drinks-do-you-use-dried-coconut-in-42499
Looking to buy Ceylon cinnamon powder? You’ve come to the right place! We offer pure Ceylon cinnamon powder, known for its sweet, delicate flavor and numerous health benefits. If you’re wondering where to buy Ceylon cinnamon powder, look no further. Our Ceylon cinnamon for sale is available for purchase online, making it convenient for you to get this high-quality spice delivered straight to your door.
In addition to our pure Ceylon cinnamon powder, we also offer a variety of other products. If you’re a fan of herbal teas, consider trying Samahan tea. You can easily buy Samahan tea online through our store. It’s a wonderful blend of herbs and spices that supports your overall well-being.
For those who enjoy baking or cooking with coconut, we have desiccated coconut available. Wondering where to buy desiccated coconut? You can find it here, along with our extensive range of cinnamon products.
Speaking of cinnamon, our product line includes more than just powder. We also have Ceylon cinnamon sticks, perfect for adding a touch of flavor to your dishes or beverages. If you’re looking to purchase real cinnamon sticks online, we’ve got you covered.
Our selection doesn’t stop there. We offer cinnamon lotion and cinnamon body lotion for those who love the scent and benefits of cinnamon in their skincare routine. Additionally, you can find cinnamon shampoo and even cinnamon toothpicks at an affordable price.
For those interested in supplements, we have a range of Ceylon cinnamon supplements for sale. These supplements are a convenient way to incorporate the benefits of Ceylon cinnamon into your daily routine. You can buy Ceylon cinnamon supplements from us, ensuring you’re getting the best quality available.
Lastly, don’t forget to check out our Ceylon cinnamon tea bags, perfect for a soothing cup of tea at any time of the day. With our wide selection, you’re sure to find exactly what you need. Shop with us today for all your cinnamon and specialty product needs!
Интернет-магазин «Аврора Агро Партс» заслуживает вашего внимания. Предлагаем привлекательные цены на автозапчасти ведущих брендов. Всегда рады общению с нашими клиентами, мы их уважаем. Вы всегда можете рассчитывать на помощь квалифицированного специалиста. Он грамотно подберет то, что вам действительно нужно. https://aa-p.ru – сайт, где вы можете уже сейчас посмотреть условия доставки и оплаты. Заказы осуществляем довольно оперативно. Открыты для взаимовыгодного сотрудничества и регулярно развиваемся, обращайтесь!
Hey there! I know this is somewhat off-topic but I had to ask. Does building a well-established blog like yours take a large amount of work? I am brand new to operating a blog however I do write in my diary every day. I’d like to start a blog so I will be able to share my own experience and feelings online. Please let me know if you have any kind of ideas or tips for new aspiring blog owners. Appreciate it!
http://forum.meha.biz/topic/1558/
http://188.17.148.172/forum/search.php?action=members&p=261&s=d&order=ASC
https://thesocialcircles.com/story2538630/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
http://site.dynamoleningrad.ru/main.php?d=1&url=
https://myeasybookmarks.com/story2479527/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%A7%D0%B5%D0%BB%D1%8F%D0%B1%D0%B8%D0%BD%D1%81%D0%BA%D0%B5
https://www.hostboard.com/forums/showthread.php?t=1003559&p=2722170#post2722170
Looking to buy Ceylon cinnamon powder? You’ve come to the right place! We offer pure Ceylon cinnamon powder, known for its sweet, delicate flavor and numerous health benefits. If you’re wondering where to buy Ceylon cinnamon powder, look no further. Our Ceylon cinnamon for sale is available for purchase online, making it convenient for you to get this high-quality spice delivered straight to your door.
In addition to our pure Ceylon cinnamon powder, we also offer a variety of other products. If you’re a fan of herbal teas, consider trying Samahan tea. You can easily buy Samahan tea online through our store. It’s a wonderful blend of herbs and spices that supports your overall well-being.
For those who enjoy baking or cooking with coconut, we have desiccated coconut available. Wondering where to buy desiccated coconut? You can find it here, along with our extensive range of cinnamon products.
Speaking of cinnamon, our product line includes more than just powder. We also have Ceylon cinnamon sticks, perfect for adding a touch of flavor to your dishes or beverages. If you’re looking to purchase real cinnamon sticks online, we’ve got you covered.
Our selection doesn’t stop there. We offer cinnamon lotion and cinnamon body lotion for those who love the scent and benefits of cinnamon in their skincare routine. Additionally, you can find cinnamon shampoo and even cinnamon toothpicks at an affordable price.
For those interested in supplements, we have a range of Ceylon cinnamon supplements for sale. These supplements are a convenient way to incorporate the benefits of Ceylon cinnamon into your daily routine. You can buy Ceylon cinnamon supplements from us, ensuring you’re getting the best quality available.
Lastly, don’t forget to check out our Ceylon cinnamon tea bags, perfect for a soothing cup of tea at any time of the day. With our wide selection, you’re sure to find exactly what you need. Shop with us today for all your cinnamon and specialty product needs!
даркнет ссылки на сайты – рутор зеркало онион, rutor форум зеркало
магазин гардеробных систем
https://biz.yelp.com/verify/t4fP7UcfhyRGmhBC_cDp-A/1Zt39TOAQE-v0RC8Ewq-PQ/options?fsid=8U43WjadVRumlKVGoCEVkg&si=C9X2_gRlS0LWVsaRAhPufA
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
Преимущества строительства дома из бруса 9х12 | Секреты выбора проекта дома из бруса 9х12 | Интерьер для дома из бруса 9х12: советы дизайнера | Как создать уютный интерьер в доме из бруса 9х12 | Выбор фундамента для дома из бруса 9х12 | Типы фундаментов для дома из бруса 9х12 | Новинки в строительстве домов из бруса 9х12 | Новинки в строительстве домов из бруса 9х12 | Как обустроить зону отдыха в доме из бруса 9х12 | Сколько стоит построить дом из бруса 9х12
проект дома из бруса одноэтажный 9х12 https://domizbrusa-9x12spb.ru/ .
заказать эскорт – эскорт модели москва, эскорт цена
Tremendous things here. I am very satisfied to peer your post. Thank you so much and I’m taking a look forward to contact you. Will you please drop me a e-mail?
https://zbookmarkhub.com/story17214077/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%B0%D1%80%D0%B8%D0%BA%D0%BC%D0%B0%D1%85%D0%B5%D1%80%D0%B0
http://www.korea-zs.ru/main.php?d=1&url=
https://bookmarkspecial.com/story17167465/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9A%D0%B0%D0%B7%D0%B0%D0%BD%D0%B8
http://fabnews.ru/forum/showthread.php?p=76082&mode=threaded
https://cocochampionship.com/
Hello it’s me, I am also visiting this site regularly, this website is actually good and the viewers are truly sharing nice thoughts.
http://www.ntsr.info/forum/user/92604/
gmailspva.com/facebook-pva-accounts
periodika.websib.ru/author?page=15
русбил.рф/forum/viewtopic.php?p=159224
gadjetforyou.ru/kupit-diplom-10
https://localpages.com/business-listing
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
горячая линия такси телефон такси эконом
This excellent website truly has all of the information I needed about this subject and didn’t know who to ask.
https://bookmarkspedia.com/story2483603/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D1%80%D0%BE%D0%B3%D1%80%D0%B0%D0%BC%D0%BC%D0%B8%D1%81%D1%82%D0%B0
https://городмихайлов.рф/
https://minecraftcommand.science/forum/general/topics/7ad7a57b-6546-4a32-9afe-090d1285de7a
https://angelow3l67.pages10.com/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2%D1%81%D0%BB%D0%B5%D0%B4%D1%81%D1%82%D0%B2%D0%B8%D0%B5-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-62819622
https://opensocialfactory.com/story16593420/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%87%D1%82%D0%BE%D0%B1%D1%8B-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://gravatar.com/druerawilmington
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
Канал Новые займы в СПБ предлагает подборку лучших новых займов на карту онлайн. Мы работаем с надежными МФО, которые готовы выдать займы без отказа. Получите до 30 000 рублей на карту, независимо от вашего возраста (от 18 лет), кредитной истории и занятости. Многие компании предлагают первый займ под 0%. Присоединяйтесь к нашему каналу и находите самые выгодные займы.
I delight in, result in I found just what I used to be having a look for. You’ve ended my four day long hunt! God Bless you man. Have a great day. Bye
https://clubecig.fr/
https://waylonhebws.blogstival.com/49144513/top-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-secrets
https://learnsongs.ru/
https://augustsroli.ourcodeblog.com/26881572/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-options
https://amanitamushroomchocolate60258.bloggerswise.com/32995204/the-5-second-trick-for-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://www.yellowbot.com/submit/newbusiness
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
Right here is the right webpage for anyone who wishes to find out about this topic. You realize so much its almost tough to argue with you (not that I personally will need to…HaHa). You certainly put a fresh spin on a subject that’s been written about for a long time. Great stuff, just great!
http://ruyanamerica.com/Page.cfm?Page=Products/VegasE-Cigar
https://domfenshuy.net/
http://www.matchfishing.ru/forumtest/1/member.php?u=23110&tab=activitystream&type=all&page=64
https://judahhdwqj.bloggazzo.com/26447720/a-review-of-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://mypresspage.com/story2452854/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B0%D1%80%D0%BC%D0%B0%D1%86%D0%B5%D0%B2%D1%82%D0%B0
https://411.info/manage/business/search?src=home&r=844-437-8372&q=DRUERA&l=Wilmington%2C+DE
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
Wow that was odd. I just wrote an incredibly long comment but after I clicked submit my comment didn’t show up. Grrrr… well I’m not writing all that over again. Anyways, just wanted to say great blog!
http://ruyanamerica.com/Page.cfm?Page=Products/VegasE-Cigar
https://social-medialink.com/story2412314/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://www.cleancenter.net/download.htm
https://getoutdoorsyapp.com/
https://thebookmarkid.com/story17174719/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A1%D0%B0%D1%80%D0%B0%D1%82%D0%BE%D0%B2
Hi there colleagues, how is the whole thing, and what you desire to say regarding this post, in my view its in fact amazing in favor of me.
http://www.lada-xray.net/member.php?tab=visitor_messaging&u=2434&page=24
http://www.aikidosydney.com/cdn-cgi/l/email-protection
http://www.speicher-photovoltaik.de/profile/?u=28968
http://www.sshcongregation.org/fullnews?sn=76
http://www.apicarrara.it/modules.php?name=Journal&file=display&jid=3511
Новые займы в СПБ – ваш надежный источник информации о самых выгодных займах на карту онлайн. Мы собрали новейшие предложения от МФО, которые выдают займы без отказов и проверок. Неважно, есть ли у вас работа или плохая кредитная история, вы можете получить до 30 000 рублей. Первый займ под 0% – отличный способ улучшить ваш кредитный рейтинг. Подписывайтесь на наш канал и находите самые выгодные условия для получения займа.
https://www.hotfrog.com/company/bc1e715f581424da662373c455ff1aa6/druera/wilmington/business-organizations
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
What a information of un-ambiguity and preserveness of precious know-how about unexpected feelings.
https://www.yeuamnhac.com/
https://throbsocial.com/story18813746/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://dubna.ru/article/2024/05/poluchenie-obrazovaniya-v-rossii
https://myanmarfootball.org/
https://andersonspjcw.iyublog.com/26509918/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-options
Not only doers it take time but you also need to concentrate on the aim.
Visit my webpage – webwiki.It
My partner and I absolutely love your blog and find nearly all of your post’s to be precisely what I’m looking for. Does one offer guest writers to write content in your case? I wouldn’t mind writing a post or elaborating on a few of the subjects you write concerning here. Again, awesome web site!
http://www.ivedu.ru/forum/viewthread.php?forum_id=18&thread_id=45646
http://www.cryptocoinsnewshub.com/
http://prikol100500.ru/poluchite-svoy-diplom-bez-lishnih-hlopot-prisoedinyaytes-seychas
https://210list.com/story17674484/%D0%A4%D0%B0%D0%BB%D1%8C%D1%88%D0%B8%D0%B2%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D1%8D%D1%82%D0%BE-%D0%BD%D0%B5-%D0%A1%D1%82%D0%BE%D0%B8%D1%82-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://wildbookmarks.com/story17231620/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9C%D0%BE%D1%81%D0%BA%D0%B2%D0%B5
https://www.bbb.org/get-listed/business
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
https://sertifikaliegitimler.com/
обменник netex24 – bestchange ru обменник, купить btc
белый слон снафф купить
geinoutime.com
그런데 흑인인 사람들은 코친족만 있는 것 같으니 뭐라고 해야 할까요?
https://about.me/delivera
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
https://terra-clean.ru/
kraken13.at – kraken зеркало рабочее, kraken официальный сайт зеркало
вебкам студия вакансии https://studio-milano.ru/
https://www.whofish.org/Default.aspx?tabid=45&modid=379&action=detail&itemid=284013&rCode=37
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
Wonderful, what a webpage it is! This webpage gives valuable facts to us, keep it up.
dachaweek.ru/page/3
click2call.buzz/index.php?do=/public/user/blogs/name_Alanpoe/page_5/
http://www.sabalsuppliers.com.np/product/view/6-zone-fire-alarm-panel
arjaniki.ru/memberlist.php?sk=m&sd=d&first_char=r&mode=searchuser&start=75
rusbil.ru/forum/viewtopic.php?t=739&view=previous
безопасно,
Современное оборудование и материалы, для вашего уверенного улыбки,
Специализированная помощь по доступным ценам, для вашей улыбки,
Индивидуальный подход к каждому пациенту, для вашей радости и улыбки,
Эффективное лечение зубов и десен, для вашего комфорта и уверенности,
Индивидуальный план лечения и профилактики, для вашего здоровья и уверенности в себе,
Заботливое отношение и внимательный подход, для вашего комфорта и удовлетворения
лікування зубів дітям лікування зубів дітям .
I get pleasure from, cause I discovered just what I used to be having a look for. You’ve ended my four day long hunt! God Bless you man. Have a nice day. Bye
https://moscityservice.ru/
https://bookmarkforest.com/story17050715/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
http://tadiyandi.100webspace.net/forum/viewtopic.php?f=2&t=420603&st=0&sk=t&sd=a&start=650
http://www.nemoskvichi.ru/forum/viewtopic.php?f=31&t=146605
https://getsocialselling.com/story2386423/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B0%D0%B2%D1%82%D0%BE%D0%BC%D0%B5%D1%85%D0%B0%D0%BD%D0%B8%D0%BA%D0%B0
I’m gone to inform my little brother, that he should also go to see this webpage on regular basis to obtain updated from most up-to-date information.
cialis 5mg price in spain
https://www.n49.com/biz/5929585/druera-de-wilmington-3-germay-dr-19804/
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
препарат саксенда купить – тирзепатид мунджаро купить +в спб, Оземпик 0.25 мг
https://www.mycitybusiness.net/addbusiness.php
Welcome to the ultimate destination for premium Ceylon cinnamon products! Our e-commerce store offers a curated selection of high-quality Ceylon cinnamon items, sourced directly from the lush landscapes of Sri Lanka. Whether you’re looking to enhance your culinary creations or boost your health, we’ve got you covered.
Our Products
Ceylon Cinnamon Powder: Known for its sweet and delicate flavor, our pure Ceylon cinnamon powder is perfect for baking, cooking, and adding a touch of spice to your favorite beverages. It’s a versatile pantry staple that elevates both sweet and savory dishes.
Ceylon Cinnamon Sticks: Ideal for infusing flavor into teas, stews, and desserts, our Ceylon cinnamon sticks are a must-have for any kitchen. Unlike the more common Cassia cinnamon, Ceylon cinnamon sticks offer a subtler, more refined taste.
Ceylon Cinnamon Capsules: Packed with health benefits, our Ceylon cinnamon capsules are a convenient way to support your wellness routine. These supplements are rich in antioxidants and have anti-inflammatory properties, making them a great addition to your daily regimen.
Ceylon Cinnamon Tea Bags: Enjoy the soothing and aromatic experience of Ceylon cinnamon tea. Our tea bags are filled with the finest Ceylon cinnamon, providing a calming and flavorful cup of tea that’s perfect any time of the day.
Cinnamon Body Care: Indulge in our range of cinnamon-infused body care products, including cinnamon lotion and cinnamon shampoo. These items harness the natural properties of Ceylon cinnamon to nourish and rejuvenate your skin and hair.
I got this website from my friend who shared with me concerning this site and now this time I am browsing this web page and reading very informative posts at this place.
krutovo.ru/index.php?name=Account&op=info&uname=ymonozav
zakon122.ru/promotion/
kupidon-pskov.ru/
politictoday.ru/page/39
mypenza.ru/forum/index.php?showtopic=54674&mode=linear
Hi there, of course this paragraph is genuinely nice and I have learned lot of things from it concerning blogging. thanks.
http://ruyanamerica.com/Page.cfm?Page=Products/VegasE-Cigar
https://benhvienthammyasean.com/tao-hinh-nhan-trung
https://go4pro.ru/sjcam/proshivka-sj4000-sj4000wifi-instrukciya
https://isocialfans.com/story2454722/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%92%D0%BE%D1%80%D0%BE%D0%BD%D0%B5%D0%B6%D0%B5
https://webyourself.eu/blogs/300062/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%B4%D0%B8%D0%BD-%D0%BA%D0%BB%D0%B8%D0%BA-%D0%A3-%D0%BD%D0%B0%D1%81-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE-%D0%B8-%D0%BF%D1%80%D0%BE%D1%81%D1%82%D0%BE
I constantly emailed this web site post page
to all my associates, for the reason that if like to read it
then my contacts will too.
Take a look at my website; Pinterest
It’s amazing to visit this web page and reading the views of all mates about this paragraph, while I am also zealous of getting familiarity.
https://elarus.ru/
https://freebookmarkpost.com/story16998832/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://thetechnologynews61482.bleepblogs.com/27328913/marketing-things-to-know-before-you-buy
https://agendabookmarks.com/story17009199/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9A%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B4%D0%B0%D1%80%D0%B5
https://benhvienthammyasean.com/tao-hinh-nhan-trung
Thanks for sharing your thoughts on Slot
Online. Regards
volna маркет ссылка – volna darknet market, волна онион
instant cash loans t h e money shop The purpose of a civil lawsuit is to simply obtain a judgment for a wage garnishment so that they can be repaid.
Please let me know if you’re looking for a author for your weblog. You have some really great articles and I feel I would be a good asset. If you ever want to take some of the load off, I’d really like to write some material for your blog in exchange for a link back to mine. Please send me an e-mail if interested. Regards!
http://serialforfree.ru/diplomyi-po-vashemu-zaprosu-prisoedinyaytes-k-nam-i-dostigayte-uspeha
http://mdoucrr-ds28.ru/
http://ruskruiz.ru/
http://cf58051.tmweb.ru/index.php?topic=826.195
https://openmotonews.ru/page/4
newsmiamigardens.com
chinataste1.com
Whats up are using WordPress for your site platform? I’m new to the blog world but I’m trying to get started and set up my own. Do you need any coding expertise to make your own blog? Any help would be really appreciated!
https://indexedbookmarks.com/story16981752/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
https://sites2000.com/story6631706/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%95%D0%BA%D0%B0%D1%82%D0%B5%D1%80%D0%B8%D0%BD%D0%B1%D1%83%D1%80%D0%B3%D0%B5
http://www.anfiz.ru/
https://allnewstur.ru/page/2
https://waylonhebws.blogstival.com/49144513/top-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-secrets
What’s up to every body, it’s my first pay a visit of this website; this web site includes awesome and really fine data designed for visitors.
https://shuttersandsecurity.co.uk/forum/profile/MaritaStei
https://forums.talktaiwan.org/smf/index.php?topic=4900.3255
https://kids-news.ru/professionalnyie-diplomyi-po-vashemu-zaprosu-zakazhite-onlayn-pryamo-seychas
https://privatebookmark.com/story17268740/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B8%D0%B7-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://la-buket.ru/catalog/bestsellers/
Can I just say what a comfort to find somebody who really knows what they are talking about online. You definitely know how to bring an issue to light and make it important. More people must look at this and understand this side of the story. I can’t believe you are not more popular given that you surely have the gift.
http://malhotrafoundation.org/about/who-we-are
https://wiishlist.com/story17586101/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B7%D0%B0-11-%D0%BA%D0%BB%D0%B0%D1%81%D1%81
https://loanbookmark.com/story17269350/%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B0-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%A0%D0%B8%D1%81%D0%BA%D0%B8-%D0%B8-%D0%9F%D0%BE%D1%81%D0%BB%D0%B5%D0%B4%D1%81%D1%82%D0%B2%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://newsofmebel.ru/bezopasnoe-i-konfidentsialnoe-priobretenie-diploma-poprobuyte-uzhe-segodnya
https://ilovebookmarking.com/story17101400/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%80%D0%B0%D1%87%D0%B0
I got this website from my friend who informed me concerning this web page and now this time I am visiting this site and reading very informative posts at this place.
http://forum54.4adm.ru/viewtopic.php?f=69&t=8011
https://socials360.com/story7108498/%D0%B3%D0%B4%D0%B5-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://bitplace.to/
http://jusonline.ru/mix/poluchenie-obrazovaniya-v-rf-i-professionalnoe-razvitie.html
https://dmitriyandreev.ru/
restore bad credit Lenders will need to see the last 90 days of your bank statements, and any other documentation that may support your application is highly helpful.
Meanwhile, the Mega Millions jackpot has jumped to aan estimated $480 million ($240.7 millionn cash) for the subsequent
drawing on Tuesday, July 11.
my webpage: 베픽
промокод всеинструменты ру
профессиональное мытье окон
read more Potplayer
блэкспрут ссылка – тор браузер blacksprut, блэк спрут ссылка
ремонт телефонов в москве
сколько стоит уборка после ремонта
Новое напольное покрытие из кварц винила – это идеальное сочетание прочности, элегантности и удобства. Оно отлично подходит для любого помещения, будь то кухня, гостиная или офисное пространство. Благодаря своей устойчивости к истиранию, царапинам и влаге, кварцвиниловый ламинат станет отличным выбором для тех, кто ценит долговечность и простоту ухода. Кроме того, большой выбор текстур и цветов позволит вам подобрать идеальное покрытие, которое подчеркнет стиль и атмосферу вашего интерьера. Кварц виниловый ламинат купить в Москве
оземпик купить +в ростове – mounjaro, заказать аземпик
Thanks for the auspicious writeup. It actually was once a enjoyment account it. Glance complex to far introduced agreeable from you! By the way, how could we be in contact?
https://vanbroecanimations.online/
http://allnewstroy.ru/diplomyi-bez-lishnih-slozhnostey-prisoedinyaytes-k-nashey-komande
https://zebuskape.com/contact-us
https://socialmediastore.net/story17342715/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A2%D1%8E%D0%BC%D0%B5%D0%BD%D1%8C
http://www.chaodisiaque.com/forum/viewtopic.php?pid=21777
оземпик таблетки – уколы оземпик цена +для похудения +и отзывы, трулисити 1.5
same day loans no employment At least you won’t have money to pay back by choosing those options.
A gazebo with a breakdown on the lawn. If there mexicocities.net is a decorative lawn on the site, it can be installed on a gazebo with a floor so as not to harm the grass. The platform is made in the form of a metal profile, which is attached to several holes drilled in the soil.
IFran.ru – это онлайн-проект, который создан для повышения прозрачности и открытости рынка франчайзинга в России. Портал собирает и анализирует объективные данные из разных открытых источников, а затем представляет полученную информацию в структурированной и единообразной форме. https://www.ifran.ru – сайт, где у вас есть возможность узнать о том, что из себя представляет франчайзинг. Здесь вы найдете рейтинги, обзоры, а также интересные статьи. Благодаря возможностям нашего портала потенциальные франчайзи могут сделать выбор в пользу высококачественных франшизеров.
купить диплом вуза https://6landik-diploms.com
эффективно,
Лучшие стоматологи города, для крепких и здоровых зубов,
Специализированная помощь по доступным ценам, для вашего удобства,
Индивидуальный подход к каждому пациенту, для вашего здоровья и благополучия,
Инновационные методы стоматологии, для вашего долгосрочного удовлетворения,
Индивидуальный план лечения и профилактики, для вашего здоровья и уверенности в себе,
Заботливое отношение и внимательный подход, для вашего здоровья и благополучия
івано франківськ стоматологія https://stomatologichnaklinikafghy.ivano-frankivsk.ua/ .
solaris сайт – солярис ссылка, солярис даркнет
This is my first time pay a quick visit at here and i am genuinely impressed to read everthing at alone place.
https://ravolutionfestival.com/
http://boxer-forum.ru/topic3623.html?&p=75735
https://blouson-moto.net/
https://beauskcti.blogzag.com/71272936/detailed-notes-on-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
http://i-docs.org/
гарантированно,
Индивидуальный подход к каждому пациенту, для крепких и здоровых зубов,
Профессиональное лечение и консультации, для вашей улыбки,
Индивидуальный подход к каждому пациенту, для вашего здоровья и благополучия,
Комплексное восстановление утраченных зубов, для вашего здоровья и красоты улыбки,
Индивидуальный план лечения и профилактики, для вашего здоровья и уверенности в себе,
Современное лечение заболеваний полости рта, для вашей уверенной улыбки
дитяча стоматологія дитяча стоматологія .
эффективно,
Современное оборудование и материалы, для поддержания здоровья рта,
Профессиональное лечение и консультации, для вашего уверенного выбора,
Бесплатная консультация и диагностика, для вашего здоровья и благополучия,
Комплексное восстановление утраченных зубов, для вашего комфорта и уверенности,
Экстренная помощь в любое время суток, для вашего долгосрочного удовлетворения,
Индивидуальный план лечения для каждого пациента, для вашего здоровья и благополучия
стоматологія клініка https://stomatologichnaklinikafghy.ivano-frankivsk.ua/ .
payday loan turlock Once you submit the form, the lender will quickly contact you and the loan amount will be transferred in your account.
гарантированно,
Лучшие стоматологи города, для вашего уверенного улыбки,
Профессиональное лечение и консультации, для вашей улыбки,
Комфортные условия и дружественный персонал, для вашего здоровья и благополучия,
Инновационные методы стоматологии, для вашего долгосрочного удовлетворения,
Профессиональная гигиена полости рта, для вашего комфорта и удовлетворения,
Заботливое отношение и внимательный подход, для вашего комфорта и удовлетворения
послуги стоматології https://stomatologichnaklinikafghy.ivano-frankivsk.ua/ .
вызвать такси недорого https://taxi-novocherkassk.ru/
Reducing the cost of attracting job-career.com new customers. You can inexpensively retain existing customers through quality customer service. It’s much cheaper than constantly recruiting new people.
homebeachlove.com
рассчитать стоимость такси https://zakaz-taxionline.ru/
It is perfect time to make some plans for the longer term and it’s time to be happy.
I have read this submit and if I may just I want to recommend
you few interesting issues or suggestions. Maybe you can write next articles relating to this article.
I want to learn even more issues about it!
мега даркнет – mega darknet, mega сайт ссылка
Reducing the cost of attracting job-career.com new customers. You can inexpensively retain existing customers through quality customer service. It’s much cheaper than constantly recruiting new people.
Ищете способ расслабиться и получить незабываемые впечатления? Мы https://t.me/intim_tmn72 предлагаем эксклюзивные встречи с привлекательными и профессиональными компаньонками. Конфиденциальность, комфорт и безопасность гарантированы. Позвольте себе наслаждение и отдых в приятной компании.
directory Osu
Займ с любой кредитной историей. Без подтверждения дохода. Вы остаётесь собственником. Без отказов. Быстрое оформление. Без скрытых комиссий займ онлайн ооо
Today, I went to the beachfront with my kids. I found a sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She put the shell to her ear and screamed. There was a hermit crab inside and it pinched her ear. She never wants to go back! LoL I know this is completely off topic but I had to tell someone!
https://re-tracker.ru/index.php?showtopic=1120
https://deporfc.com/?cat=1
https://newtownmemorialfund.org/
https://bookmarklethq.com/story17074273/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9A%D0%B0%D0%B7%D0%B0%D0%BD%D0%B8
http://avtovideotest.ru/byistryiy-put-k-uspehu-zakazhite-svoy-diplom-onlayn
эффективно,
Индивидуальный подход к каждому пациенту, для крепких и здоровых зубов,
Специализированная помощь по доступным ценам, для вашей улыбки,
Комфортные условия и дружественный персонал, для вашего здоровья и благополучия,
Инновационные методы стоматологии, для вашего долгосрочного удовлетворения,
Экстренная помощь в любое время суток, для вашего комфорта и удовлетворения,
Заботливое отношение и внимательный подход, для вашей уверенной улыбки
стоматологiчна полiклiнiка https://stomatologichnaklinikafghy.ivano-frankivsk.ua/ .
Вавада – ведущая онлайн-платформа, предлагающая огромный каталог увлекательных игровых автоматов, призванных подарить незабываемые впечатления от азартных игр. С более чем 600 игровыми автоматами в базе сайта Vavada удовлетворит игровые предпочтения каждого.
игровые автоматы играть регистрация вавада – идеальный выбор для тех, кто ищет захватывающий и разнообразный игровой опыт. С обширным каталогом, высококачественной графикой, отличными бонусами и надежной репутацией Vavada обеспечивает безлимитные часы развлекухи для игроков всех уровней.
great site Notepad
payday loan turlock Their interest rates are also quite high, but the time limit is more than the payday ones.
It’s not my first time to pay a quick visit this
web site, i am browsing this web page dailly and get fastidious information from here every day. https://socialinplace.com/story2672161/spa-sant%C3%A9-le-n%C3%A9nuphar-un-incontournable-%C3%A0-terrebonne
Заказ диплома – ваш шаг к профессиональному успеху
Автор 24 ру Автор 24 ру .
https://faina-cleaning.ru/
I appreciate, result in I found exactly what I used to be taking a look for. You’ve ended my 4 day lengthy hunt! God Bless you man. Have a great day. Bye
https://stockmarkets59257.ka-blogs.com/79960468/considerations-to-know-about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
http://link.befile.ru/main.php?d=1&url=
https://bookmarkinginfo.com/story17090402/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%BE%D0%B2%D0%B0%D1%80%D0%B0
http://newsinweek.ru/byistryiy-put-k-uspehu-zakazhite-svoy-diplom-onlayn/
https://linkedbookmarker.com/story2429185/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%95%D0%BA%D0%B0%D1%82%D0%B5%D1%80%D0%B8%D0%BD%D0%B1%D1%83%D1%80%D0%B3%D0%B5
Cottage rental in Zabljak – Горные дома в Жабляке, House rental in the mountains of Montenegro
http://russa24-diploms-srednee.com/
payday loans in fairfax va Tend not to acquire more cash than you can pay for to reimburse.
This post is invaluable. How can I find out more?
http://fat-girls.ru/category/bez-rubriki/page/4
https://bestcoolfun.ru/diplomyi-po-vashemu-vyiboru-zakazhite-onlayn-i-poluchite-ih-byistro
https://mysocialname.com/story2366784/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%A1%D0%B0%D0%BC%D0%B0%D1%80%D0%B5
https://portugues.ru/forum/album.php?albumid=80&attachmentid=3794
https://augustyyvsn.look4blog.com/65874631/not-known-facts-about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
Hello there I am so glad I found your webpage, I really found you by mistake, while I was browsing on Askjeeve for something else, Anyhow I am here now and would just like to say thank you for a tremendous post and a all round interesting blog (I also love the theme/design), I don’t have time to browse it all at the moment but I have saved it and also added in your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the fantastic work.
https://eqagent.ru/users/36?page=3
http://myworldavto.ru/bezopasnoe-i-konfidentsialnoe-priobretenie-diploma-poprobuyte-uzhe-segodnya
http://allukrnews.ru/uspeshnoe-zavershenie-vashego-obrazovaniya-poluchite-svoy-diplom-seychas/
https://baidubookmark.com/story17092350/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%87%D1%82%D0%BE%D0%B1%D1%8B-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://html-studio.paris/
уколы +для похудения оземпик отзывы – тирзепатид купить цена +в москве, лираглутид дулаглутид семаглутид
here Palworld
Accepted by all major bookmakers, casinos and poker rooms, your Skrill wallet lets you enjoy online betting and gambling without revealing your personal payment marvel casino 15 euro za registraci no deposit
купить медицинскую справку
It’s amazing to pay a visit this site and reading the views of all mates about this article, while I am also keen of getting familiarity.
https://osvoidachu.ru/
https://kids-news.ru/professionalnyie-diplomyi-po-vashemu-zaprosu-zakazhite-onlayn-pryamo-seychas
https://allwingroup.ru/faq/chto-luchshe-oformit-dogovor-dareniya-ili-kupli-prodazhi/
https://bookmarkpressure.com/story17162867/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://titusmpoom.blogdosaga.com/26770882/the-smart-trick-of-marketing-that-no-one-is-discussing
What an insightful article! Your ability to break down complex topics into easily understandable points is truly commendable. I appreciate the thorough research and the engaging writing style that keeps readers hooked from start to finish. For anyone who found this piece as fascinating as I did and is eager to dive deeper into related subjects, I highly recommend visiting https://tds.rida.tokyo/com. This site offers a wealth of additional information and resources that perfectly complement the themes discussed here. Thank you for sharing your knowledge and providing such valuable content. I look forward to reading more of your work in the future!
cash loans in costa mesa That is why they’re termed payday loans and should be settled using the next pay.
At this time it looks like WordPress is the top blogging platform available right now. (from what I’ve read) Is that what you’re using on your blog?
http://mirfinrealty.ru/page/4
https://www.chabab-belouizdad.org/
https://sergiogczvp.blogdun.com/27275677/the-single-best-strategy-to-use-for-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://howtobuyessay.com/
https://spencernlhau.blogspothub.com/26476637/getting-my-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-to-work
Best online casinos in 2024 reviewed, tested, and ranked by gambling experts. Expert Online Casino Reviews independently review & rank each online casino with our 25 step process gdfplay casino 15 € no deposit bonus
browse around this site galaxy swapper download
Новые дорамы с русской озвучкой – это идеальный способ окунуться в мир азиатского кинематографа без языковых барьеров. На сайте doramaserials.net вас ждут свежие новинки, которые уже завоевали сердца зрителей по всему миру. Здесь вы найдете сериалы на любой вкус: от романтических драм до захватывающих триллеров. Профессиональная озвучка делает просмотр еще более приятным и позволяет полностью погрузиться в сюжет.
Сайт doramaserials.net предлагает вам возможность смотреть новые дорамы с русской озвучкой онлайн в удобное для вас время. Высокое качество видео и отсутствие рекламы делают просмотр максимально комфортным. Независимо от того, где вы находитесь, вы всегда сможете наслаждаться любимыми сериалами без лишних хлопот. Откройте для себя мир новых дорам и наслаждайтесь каждой минутой вместе с doramaserials.net!
https://vk.com/kent_bonus
e-mallorca.com
The purpose of MRF hydraulic motors is to 365wyoming.com convert the energy that comes from the fluid flow into mechanical energy that rotates the output shaft. The scope of application of high-torque hydraulic motors MRF is extremely wide. They are used as part of injection molding machines; they are used to operate presses that process plastic. Hydraulic motors are used in woodworking and forging equipment, road equipment, and drilling rigs.
whoah this blog is great i really like studying your posts. Stay up the great work! You know, many people are hunting round for this info, you could aid them greatly.
https://www.11na11.com/
https://milltelecom.com/blogs/27/%D0%A2%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9E%D1%82%D0%BA%D1%80%D1%8B%D0%B2%D0%B0%D0%B9%D1%82%D0%B5-%D0%BD%D0%B0%D1%88-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD?lang=pt_br
http://mynewsport.ru/page/4
https://www.ramplajuniors.com/tablas
https://bookmarkssocial.com/story17053040/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
I’d like to find out more? I’d care to find out some additional information.
https://diplomdoc1.ru/
https://ttdinhduong.org/ttdd/kcb.aspx
http://myworldavto.ru/bezopasnoe-i-konfidentsialnoe-priobretenie-diploma-poprobuyte-uzhe-segodnya
http://kungur.hldns.ru/forum/profile.php?action=show&member=7835
https://nanobookmarking.com/story17047996/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D1%81%D1%80%D0%B5%D0%B4%D0%BD%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8
What’s up, I would like to subscribe for this website to get most up-to-date updates, so where can i do it please help out.
https://staceylcrow.com/
https://mormoniconoclast.net/
http://www.nconsol.ru/main.php?d=1&url=
https://ute.expert/showthread.php?tid=2&page=69
https://forum.twilightmu.com/album.php?albumid=244&pictureid=1585
Как узаконить самовольную перепланировку alma-stroi.ru
Перепланировка квартиры — один из самых главных этапов в ремонте разных объектов. Но в нашей стране, она непременно должна быть узаконена и исполнена по всем правилам. Мы представляем о перепланировках всё, изучите на сайте alma-stroi.ru прямо сейчас.
По вопросу сколько стоит согласование перепланировки мы поможем Вам. Если у Вас уже проведена самостоятельная перепланировка без документов, то это не страшно. Её также возможно узаконить и с легкостью пользоваться зданием. Не всегда расположение комнат в доме или промышленных помещениях устраивает хозяина. Но в крайнее время, перепланировка просто лучший выход из ситуации. Безусловно, лучше всего ее проводить на этапе чернового ремонта, но если этого не произошло, то её возможно сделать на любом этапе эксплуатирования.
Цена перепланировки можно увидеть на веб портале alma-stroi.ru или увидеть примеры готовых работ. Мы осуществляем работу в представленной области уже множество лет и имеем много счастливых клиентов и выполненных работ. К любому проекту имеем персональный подход и учитываем все пожелания заказчика. Также работаем строго в срок и по очень выгодным расценкам.
Оформить заказ на разрешение на перепланировку можно уже сейчас. Наши работники приедут к Вам для замера помещений и выявления объема работы. И после этого будет названа итоговая стоимость и день выполнения работ. Перепланировка — это отличная вероятность сделать собственную жизнь комфортнее.
cash advance ost Here is what you can look for to keep yourself safe and your identity in the clear.
mega darknet зеркала – mega darknet market, мега даркнет маркет
Hi there! This post couldn’t be written any better! Reading through this post reminds me of my good old room mate! He always kept chatting about this. I will forward this post to him. Fairly certain he will have a good read. Thank you for sharing!
http://www.minpromrso.ru/main.php?d=1&url=
https://auto-sale-msk.ru/policy
https://kameronhgebw.humor-blog.com/26369655/a-review-of-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://socialbookmarkgs.com/story17150278/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
https://top-estate-soft.ru/
rutor darknet forum – рутор, как попасть в даркнет
blacksprut официальный сайт – blacksprut вход, blacksprut onion
Howdy! Would you mind if I share your blog with my twitter group? There’s a lot of people that I think would really enjoy your content. Please let me know. Many thanks
https://active-bookmarks.com/story17018367/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9F%D0%B5%D1%80%D0%BC%D0%B8
https://investing-com-t-rkiye45789.shotblogs.com/an-overview-40690428
http://myworldavto.ru/bezopasnoe-i-konfidentsialnoe-priobretenie-diploma-poprobuyte-uzhe-segodnya
https://bookmarkahref.com/story17101205/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B0%D1%81%D1%81%D0%B0%D0%B6%D0%B8%D1%81%D1%82%D0%B0
https://ragingbookmarks.com/story17194834/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
эскорт девушки – индивидуалки эскорт, вип эскорт
купить квартиру в казани от застройщика жк казань купить квартиру
Glory Casino Online
dailywealthy.com
Increasing competitiveness. If customer service usamars.com is thoughtful, then your company will stand out among competitors. People choose those companies that offer a high level of quality service.
https://aisory.tech – платформа для создания AI Telegram-ботов. Наделяйте своих ботов способностями к естественному диалогу, генерации уникального контента и решению аналитических задач. Простой конструктор платформы делает создание умных чат-ботов доступным для любой компании.
Hello, I would like to subscribe for this website to get most up-to-date updates, so where can i do it please help.
http://link.befile.ru/main.php?d=1&url=
https://hauptmanns-gartenpflege.com/profile.php?lookup=18948
https://daynghethanhnien.com/lien-he.html
https://bookmarksoflife.com/story2532665/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
https://my-social-box.com/story2378431/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B0%D1%80%D0%BC%D0%B0%D1%86%D0%B5%D0%B2%D1%82%D0%B0
Купить виллу или дом на Кипре для инвестиций и жизни. Продажа домов и вилл на Кипре от застройщиков и агентств недвижимости купить жилье на кипре цены в рублях
Hello! I realize this is kind of off-topic however I had to ask. Does building a well-established website like yours take a massive amount work? I’m brand new to running a blog but I do write in my diary every day. I’d like to start a blog so I can share my personal experience and thoughts online. Please let me know if you have any ideas or tips for new aspiring bloggers. Appreciate it!
https://social40.com/story2438314/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
https://art-gymnastics.ru/users/54?wid=4593
http://url.atde.ru/main.php?d=1&url=
https://ttdinhduong.org/ttdd/kcb.aspx
https://bookmarkleader.com/story17075139/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%8E%D1%80%D0%B8%D1%81%D1%82%D0%B0
блэкспрут ссылка – blacksprut darknet, blacksprut darknet
волна darknet – volna даркнет ссылка, волна darknet market
It’s awesome in support of me to have a website, which is helpful designed for my know-how. thanks admin
https://rafaelmtwza.educationalimpactblog.com/49064291/not-known-facts-about-marketing
https://tinybookmarks.com/story17121450/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D0%B2%D1%8B%D1%81%D1%88%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8
https://bookmarkforest.com/story17050715/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
https://louisdecay.total-blog.com/the-diaries-51854751
http://morskie-cruizy.ru/
I’m gone to convey my little brother, that he should also visit this web site on regular basis to get updated from latest reports.
http://www.vocal.com.ua/blog/www.xuzhouabl.com/www.xuzhouabl.com/en?page=47
http://aromatov.wooden-rock.ru/forum/topic.php?forum=1&topic=15138
https://arvine-restaurant.fr/
https://bookmarkilo.com/story17078109/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://louiszxtif.theideasblog.com/27209755/how-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-can-save-you-time-stress-and-money
I’d like to find out more? I’d love to find out more details.
https://www.bakili-fclub.com/
https://howtobuyessay.com/
https://otantravel.kz/
http://forum.analysisclub.ru/index.php/topic,170680.0.html?PHPSESSID=90f00409a891835f489a7d08c7f2c929
https://freebookmarkpost.com/story16998832/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
rutor darknet 2022 – рутор, live rutor
вайлд вест голд играть
fast cash warner robins The advantage of applying online for a payday loan is convenience.
эскорт агентство москва – работа для девушек эскорт, элитный эскорт
An impressive share! I’ve just forwarded this onto a colleague who has been doing a little research on this. And he in fact ordered me dinner due to the fact that I discovered it for him… lol. So allow me to reword this…. Thanks for the meal!! But yeah, thanx for spending some time to discuss this subject here on your internet site.
https://ticketsbookmarks.com/story17008634/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D0%B0%D0%BD%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D0%B0
http://www.edpillsfinder.com/
https://b52game79023.blogsvirals.com/26479241/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0-no-further-a-mystery
http://flashtest.80lvl.ru/viewtopic.php?f=3&t=1782
http://avtobestnews.ru/legalnyiy-put-k-uspeshnoy-karere-poluchite-svoy-diplom-seychas
Heya! I’m at work surfing around your blog from my new iphone 3gs! Just wanted to say I love reading through your blog and look forward to all your posts! Carry on the fantastic work!
https://martinloonn.ezblogz.com/58349366/the-definitive-guide-to-marketing
http://mymotospeed.ru/page/5
https://truyen.biz/
https://incestgames67889.blogsidea.com/32876098/the-best-side-of-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://elliottlewof.angelinsblog.com/26500568/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0-an-overview
купить квартиру в казани https://kvartiru-kupit-kzn.ru
I got this website from my buddy who told me on the topic of this web page and at the moment this time I am browsing this web page and reading very informative posts at this time.
https://mixbookmark.com/story2474999/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A2%D1%8E%D0%BC%D0%B5%D0%BD%D1%8C
https://1001bookmarks.com/story17018798/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B0%D1%81%D1%81%D0%B0%D0%B6%D0%B8%D1%81%D1%82%D0%B0
https://nitrile-gloves39493.azzablog.com/26868490/not-known-factual-statements-about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://bookmarketmaven.com/story17369478/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B5%D0%BD%D0%B5%D0%B4%D0%B6%D0%B5%D1%80%D0%B0
https://bookmarkalexa.com/story2446420/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9A%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D1%8F%D1%80%D1%81%D0%BA%D0%B5
Good info. Lucky me I ran across your website by accident
(stumbleupon). I have book-marked it for later! https://Wolvesbaneuo.com/wiki/index.php/User:MelisaBenavides
Современная вилла с каменной виллой с личным бассейном и личным парковочным местом. Светлый и просторный, идеально подходит для пар и семей недвижимость кипра цены
Hi, its good piece of writing about media print, we all understand media is a impressive source of data.
http://kzgbi-2.ru/forums.php?m=posts&q=7423&n=last
http://www.focus-elets.ru/main.php?d=1&url=
https://thebookmarkid.com/story17174719/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A1%D0%B0%D1%80%D0%B0%D1%82%D0%BE%D0%B2
https://topnewsgadget.ru/poluchite-svoy-diplom-bez-stressa-nash-servis-zabotitsya-o-vas
https://2xaynha.com/gioi-thieu-nhung-mau-nha-cap-4-theo-phong-cach-xua-duoc-lam-moi-lai.html
жк купить квартиру от застройщика https://nedvizhimost16.ru
Топ-5 материалов для перетяжки мебели, стильных
Как преобразить интерьер с минимальными затратами, мебель, которая будет радовать вас долгие годы
Топ-3 причины для перетяжки мебели в доме, попробуйте сами
Тенденции в дизайне мебели для перетяжки, применяемые в современном дизайне
Перетяжка мебели: секреты мастеров, запомнить
компания “КакСвоим”.
мега даркнет – мега сайт даркнет ссылка, mega darknet market
I used to be able to find good info from your blog articles.
https://circuit-diagrams.com/
https://chancey1s75.estate-blog.com/26795004/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://zbookmarkhub.com/story17214077/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%B0%D1%80%D0%B8%D0%BA%D0%BC%D0%B0%D1%85%D0%B5%D1%80%D0%B0
https://river78bz1.livebloggs.com/32866314/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-an-overview
https://containertraffic.ru/
volna маркет ссылка – волна онион, volna маркет ссылка
Это основной снаряд для эффективных тренировок, который используется для жимов и толчков. Всегда имеются грифы для штанг на https://shtangi-grify.ru разнообразных длин. В создании долговечных снарядов используются углеродистые марки стали. Всегда в реализацииобширный ассортимент EZ-образных грифов для коммерческой и домашней эксплуатации. Отягощения созданы для продуктивных тренировок и выполнены с разметкой и насечками для надежного хвата.
Hey there! Do you know if they make any plugins to safeguard against hackers? I’m kinda paranoid about losing everything I’ve worked hard on. Any recommendations?
https://indexedbookmarks.com/story16981752/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
http://url.atde.ru/main.php?d=1&url=
https://burn-lab-pro39370.blog4youth.com/27356707/about-marketing
https://devinuzzxv.blogdigy.com/the-5-second-trick-for-40557289
https://teplica-parnik.net/
quick loans rates Payday loans have lower income and qualifying requirements.
Hello! This post could not be written any better! Reading this post reminds me of my previous room mate! He always kept chatting about this. I will forward this post to him. Pretty sure he will have a good read. Thank you for sharing!
https://thebookmarkid.com/story17174719/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A1%D0%B0%D1%80%D0%B0%D1%82%D0%BE%D0%B2
https://gram-alt-n-investing13457.loginblogin.com/33027042/the-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA-diaries
https://letusbookmark.com/story18438228/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D1%81%D1%80%D0%B5%D0%B4%D0%BD%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8
https://edgarc4n78.creacionblog.com/26951025/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%87%D1%82%D0%BE%D0%B1%D1%8B-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://dallasdecyu.jiliblog.com/84264072/the-2-minute-rule-for-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
Go Here What is the sandbox
СХТ – компания, которая предлагает купить измерительное высокоточное оборудование. Мы гарантируем безупречное качество нашей продукции и привлекательные цены. Специалисты компании обладают приличным опытом работы и высокой квалификацией. Они с радостью готовы проконсультировать вас по интересующим вопросам. https://cxt.su – сайт, где можете прямо сейчас ознакомиться с более подробной информацией о нас и наших услугах. Здесь вы найдете видео-презентацию и фотогалерею. Оперативно реагируем на все заявки. Обращайтесь уже сейчас к нам!
That is very fascinating, You’re an overly professional blogger. I have joined your feed and look ahead to looking for extra of your fantastic post. Additionally, I’ve shared your site in my social networks
http://tadiyandi.100webspace.net/forum/viewtopic.php?f=2&t=420603&st=0&sk=t&sd=a&start=650
https://enkor.ru/forum/viewtopic.php?t=11397&view=previous
https://formulaf1.ru/page/6
https://cristianqfufx.bloggip.com/26977792/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2-%D1%83%D0%B3%D0%BE%D0%B4%D1%83-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://social4geek.com/story2535241/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
https://b2b-point.io/announs_category/buyers/
Excellent, what a blog it is! This webpage provides useful facts to us, keep it up.
https://johsocial.com/story7121033/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D1%81%D1%80%D0%B5%D0%B4%D0%BD%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8
https://investing-com-t-rkiye45789.shotblogs.com/an-overview-40690428
https://share-design.ru/
https://allwingroup.ru/faq/chto-luchshe-oformit-dogovor-dareniya-ili-kupli-prodazhi/
https://funbookmarking.com/story17082812/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B5%D0%BB%D1%8C%D0%B4%D1%88%D0%B5%D1%80%D0%B0
https://b2b-point.io/aenean-sed-pulvinar-et-diam/
Read Full Report The Sandbox
look at these guys [url=https://sanclboxgame.xyz/]Sandbox game[/url]
Hi Dear, are you truly visiting this web site regularly, if so then you will without doubt obtain fastidious experience.
https://diaocbinhduong.org/2018/khu-do-thi-phuc-dat-tdm.html
https://livebackpage.com/story2388195/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
https://bookmarkblast.com/story17114714/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://stephenq8s88.onesmablog.com/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B8%D0%B7-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-67298134
https://zhaktrans.ru/g2789651-frontalnye-pogruzchiki
Лучшие модели колясок Cybex на рынке, в нашем каталоге.
Как выбрать идеальную коляску Cybex для вашего малыша, для самых взыскательных.
Почему стоит обратить внимание на коляски Cybex, которые заставят вас влюбиться в этот бренд.
Топ-5 моделей колясок Cybex для вашего ребенка, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашей семьи, учитывая все особенности и пожелания.
Как правильно подобрать коляску Cybex для вашей семьи, исходя из индивидуальных потребностей и предпочтений.
Почему коляски Cybex так популярны среди родителей, которые ценят комфорт и безопасность.
Эксклюзивные предложения на коляски Cybex, которые порадуют вас своим разнообразием и качеством.
Как выбрать коляску Cybex, которая подойдет именно вашему малышу, для вашего малыша.
Выбор коляски Cybex: что важно знать перед покупкой, чтобы сделать правильный выбор.
Топ-модели колясок Cybex для вашего малыша, которые не оставят вас равнодушными.
5 важных критериев при выборе коляски Cybex, которые порадуют вас своим качеством и функционалом.
Идеальная коляска Cybex: комфорт и удобство для вашего малыша, которые стоит рассмотреть перед покупкой.
Коляска Cybex для вашего малыша: лучшие модели, если вы цените качество и комфорт.
Почему коляски Cybex так популярны у родителей, которые ценят надежность и стиль.
Новинки колясок Cybex, которые стоит рассмотреть, перед совершением покупки.
Топ-5 лучших моделей колясок Cybex, исходя из личных предпочтений и потребностей.
Как выбрать идеальную коляску Cybex для вашего малыша: главные моменты, которые не оставят вас равнодушными.
коляска прогулочная cybex коляска прогулочная cybex .
Лучшие модели колясок Cybex на рынке, лучшие предложения.
Лучшие оферты на коляски Cybex, для самых взыскательных.
5 причин выбрать именно коляску Cybex для вашего малыша, которые заставят вас влюбиться в этот бренд.
Идеальный выбор для заботливых родителей – коляски Cybex, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашей семьи, учитывая все особенности и пожелания.
Как правильно подобрать коляску Cybex для вашей семьи, исходя из индивидуальных потребностей и предпочтений.
Коляска Cybex: высокое качество и стильный дизайн, которые ценят комфорт и безопасность.
Топ-модели колясок Cybex на любой вкус и цвет, которые порадуют вас своим разнообразием и качеством.
5 важных критериев при выборе коляски Cybex, для вашего малыша.
Какая коляска Cybex лучше всего подойдет вашей семье?, чтобы сделать правильный выбор.
Топ-модели колясок Cybex для вашего малыша, которые не оставят вас равнодушными.
Лучшие модели колясок Cybex для вашей семьи, которые порадуют вас своим качеством и функционалом.
Как выбрать коляску Cybex: главные моменты, которые стоит рассмотреть перед покупкой.
Топ-5 колясок Cybex для вашей семьи, если вы цените качество и комфорт.
Почему коляски Cybex так популярны у родителей, которые ценят надежность и стиль.
Новинки колясок Cybex, которые стоит рассмотреть, перед совершением покупки.
Топ-5 лучших моделей колясок Cybex, исходя из личных предпочтений и потребностей.
Особенности выбора коляски Cybex: как сделать правильный выбор, которые не оставят вас равнодушными.
прогулочная коляска cybex https://kolyaskicybex.ru/ .
Лучшие модели колясок Cybex на рынке, лучшие предложения.
Коляска Cybex: комфорт и безопасность в одном, для самых взыскательных.
Почему стоит обратить внимание на коляски Cybex, которые заставят вас влюбиться в этот бренд.
Идеальный выбор для заботливых родителей – коляски Cybex, которые не оставят вас равнодушными.
Элегантные решения для вашего ребенка – коляски Cybex, учитывая все особенности и пожелания.
Как правильно подобрать коляску Cybex для вашей семьи, исходя из индивидуальных потребностей и предпочтений.
Трендовые коляски Cybex для вашего малыша, которые ценят комфорт и безопасность.
Топ-модели колясок Cybex на любой вкус и цвет, которые порадуют вас своим разнообразием и качеством.
Ключевые моменты, на которые стоит обратить внимание при выборе коляски Cybex, для вашего малыша.
Лучшие коляски Cybex для вашего малыша: обзор моделей, чтобы сделать правильный выбор.
Коляска Cybex: стиль, комфорт и безопасность, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашего малыша, которые порадуют вас своим качеством и функционалом.
Идеальная коляска Cybex: комфорт и удобство для вашего малыша, которые стоит рассмотреть перед покупкой.
Коляска Cybex для вашего малыша: лучшие модели, если вы цените качество и комфорт.
Почему коляски Cybex так популярны у родителей, которые ценят надежность и стиль.
Как выбрать идеальную коляску Cybex для вашего малыша: подробный гид, перед совершением покупки.
Топ-5 лучших моделей колясок Cybex, исходя из личных предпочтений и потребностей.
Лучшие предложения на коляски Cybex для вашей семьи, которые не оставят вас равнодушными.
детская коляска cybex детская коляска cybex .
Glory Casino BD
What’s up to all, how is everything, I think every one is getting more from this site, and your views are pleasant designed for new visitors.
http://jusonline.ru/mix/poluchenie-obrazovaniya-v-rf-i-professionalnoe-razvitie.html
https://cheapbookmarking.com/story17028176/%D0%B3%D0%B4%D0%B5-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://amazonpromocodefreeshippi26048.ampblogs.com/a-review-of-marketing-63644538
https://damienhllkk.timeblog.net/62582328/the-single-best-strategy-to-use-for-marketing
http://doge.coinpool.ru/main.php?d=1&url=
Glory Casino
Выбирайте коляску Cybex для комфорта вашего ребенка, для вашего выбора.
Лучшие оферты на коляски Cybex, для истинных ценителей качества.
Почему стоит обратить внимание на коляски Cybex, которые заставят вас влюбиться в этот бренд.
Коляска Cybex: безопасность и стиль в одном флаконе, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашей семьи, учитывая все особенности и пожелания.
Выбирайте коляску Cybex с умом и стилем, исходя из индивидуальных потребностей и предпочтений.
Почему коляски Cybex так популярны среди родителей, которые ценят комфорт и безопасность.
Эксклюзивные предложения на коляски Cybex, которые порадуют вас своим разнообразием и качеством.
Ключевые моменты, на которые стоит обратить внимание при выборе коляски Cybex, для вашего малыша.
Выбор коляски Cybex: что важно знать перед покупкой, чтобы сделать правильный выбор.
Коляска Cybex: стиль, комфорт и безопасность, которые не оставят вас равнодушными.
Лучшие модели колясок Cybex для вашей семьи, которые порадуют вас своим качеством и функционалом.
Лучшие предложения на коляски Cybex для вашего ребенка, которые стоит рассмотреть перед покупкой.
Коляска Cybex для вашего малыша: лучшие модели, если вы цените качество и комфорт.
Лучшие модели колясок Cybex: подробный обзор, которые ценят надежность и стиль.
Как выбрать идеальную коляску Cybex для вашего малыша: подробный гид, перед совершением покупки.
Как выбрать идеальную коляску Cybex для вашей семьи, исходя из личных предпочтений и потребностей.
Как выбрать идеальную коляску Cybex для вашего малыша: главные моменты, которые не оставят вас равнодушными.
коляска cybex прогулочная коляска cybex прогулочная .
gpt chat bot telegram
What’s up, its nice paragraph on the topic of media print, we all be aware of media is a wonderful source of data.
https://loanbookmark.com/story17269350/%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B0-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%A0%D0%B8%D1%81%D0%BA%D0%B8-%D0%B8-%D0%9F%D0%BE%D1%81%D0%BB%D0%B5%D0%B4%D1%81%D1%82%D0%B2%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://toplentanews.ru/diplomyi-na-zakaz-myi-zdes-chtobyi-pomoch-vam
https://exactlybookmarks.com/story17050247/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D1%81%D1%80%D0%B5%D0%B4%D0%BD%D0%B5%D0%BC-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%BC
https://israeliigfc.blog2freedom.com/26772264/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-an-overview
https://one-bookmark.com/story17030964/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
Аренда вилл и домов на Кипре. Всего 1490. Мы готовы предложить снять виллу на Кипре или частный дом у моря любого уровня : от домов эконом класса до шикарных вилл с бассейном аренда на кипре у моря
Идеальная коляска Cybex для вашего малыша, популярные модели.
Лучшие оферты на коляски Cybex, для истинных ценителей качества.
Почему стоит обратить внимание на коляски Cybex, которые заставят вас влюбиться в этот бренд.
Топ-5 моделей колясок Cybex для вашего ребенка, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашей семьи, учитывая все особенности и пожелания.
Как правильно подобрать коляску Cybex для вашей семьи, исходя из индивидуальных потребностей и предпочтений.
Трендовые коляски Cybex для вашего малыша, которые ценят комфорт и безопасность.
Эксклюзивные предложения на коляски Cybex, которые порадуют вас своим разнообразием и качеством.
Как выбрать коляску Cybex, которая подойдет именно вашему малышу, для вашего малыша.
Какая коляска Cybex лучше всего подойдет вашей семье?, чтобы сделать правильный выбор.
Элегантные решения для вашей семьи – коляски Cybex, которые не оставят вас равнодушными.
Лучшие модели колясок Cybex для вашей семьи, которые порадуют вас своим качеством и функционалом.
Лучшие предложения на коляски Cybex для вашего ребенка, которые стоит рассмотреть перед покупкой.
Топ-5 колясок Cybex для вашей семьи, если вы цените качество и комфорт.
Лучшие модели колясок Cybex: подробный обзор, которые ценят надежность и стиль.
Как выбрать идеальную коляску Cybex для вашего малыша: подробный гид, перед совершением покупки.
Топ-5 лучших моделей колясок Cybex, исходя из личных предпочтений и потребностей.
Особенности выбора коляски Cybex: как сделать правильный выбор, которые не оставят вас равнодушными.
коляска сайбекс купить https://kolyaskicybex.ru/ .
use this link Sandbox Airdrop
Howdy! I’m at work surfing around your blog from my new apple iphone! Just wanted to say I love reading your blog and look forward to all your posts! Keep up the fantastic work!
https://moodjhomedia.com/story1451150/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
http://www.poooq.ru/main.php?d=1&url=
https://www.spa-la-part-des-anges.fr/massage-nuru-lyon/
https://mboumukvilino.ru/
https://primerosauxilios.org/infecciosas/infeccion.php
go now The Sandbox Metaverse Map
бот с искусственным интеллектом telegram
атака титанов онлайн бесплатно аниме атака титанов
Heya just wanted to give you a quick heads up and let you know a few of the pictures aren’t loading correctly. I’m not sure why but I think its a linking issue. I’ve tried it in two different web browsers and both show the same outcome.
https://lovisribca.ru/
https://griffinvsok82604.jaiblogs.com/53620116/about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://formulaf1.ru/page/6
http://www.losenoc.ru/main.php?d=1&url=
http://dpou.info/index.php?page=1337351387&nom_page=26&
got lots of payday loans But you should be able to get the cash you need to deal with the financial emergency that you need to take care of.
May I simply just say what a relief to find a person that actually understands what they’re talking about on the internet. You certainly realize how to bring a problem to light and make it important. A lot more people must read this and understand this side of the story. I was surprised you aren’t more popular since you certainly have the gift.
https://pr7bookmark.com/story17267370/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B5%D1%85%D0%B0%D0%BD%D0%B8%D0%BA%D0%B0
https://newmedtime.ru/zakazhite-diplom-onlayn-i-dvigaytes-vpered-bez-prepyatstviy
https://bookmarkswing.com/story18315758/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B5%D0%BD%D0%B5%D0%B4%D0%B6%D0%B5%D1%80%D0%B0
http://www.empyrethegame.com/forum/memberlist.php?sk=d&sd=d&first_char=u&start=3850
https://apollobookmarks.com/story17040106/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
Российский завод реализует спортивные тренажеры на https://sport-silovye-trenazhery.ru по низким ценам. Перечень предлагает гантели, гири, эллиптические тренажеры. В наличии качественные станки и снаряды для реализации тренировочных целей. Покупайте силовую раму Смита, Кроссовер для перекрестной тяги, Баттерфляй для грудных и дельтовидных мышц, вертикально-горизонтальную тягу, тренажер Скотта, Дельта машину, жим ногами, конструкции для работы с собственным весом, Гравитрон для подтягивания и отжиманий, обратную гиперэкстензию, Хаммер и другое оборудование.
Hello my family member! I wish to say that this article is amazing, nice written and include approximately all significant infos.
I’d like to see extra posts like this . http://wiki.Competitii-sportive.ro/index.php/Imprimeries_Commerciales_%C3%83_Qu%C3%83_bec_:_Partenaires_Par_Vos_Projets_D_Impression
For hottest information you have to pay a quick visit world-wide-web and on the web I found this site as a most excellent web page for latest updates.
https://www.datxanhhanoi.com/chung-cu/du-an-tsg-lotus-sai-dong/849.html
https://hypebookmarking.com/story16985890/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2%D1%81%D0%BB%D0%B5%D0%B4%D1%81%D1%82%D0%B2%D0%B8%D0%B5-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://www.tkanivik.ru/main.php?d=1&url=
https://vitz.ru/forums/index.php?autocom=gallery&req=si&img=2862
http://delivery-containers.ru/
777 Jili Casino functions as an online casino that which presents an assortment of slot games. Herein are various of the characteristics belonging to 777 Jili Casino: a rewards program that gratifies users for their play 777 jili casino login. 777 Jili Casino is an excellent option for players seeking a broad range of games, bountiful bonuses, and a protected gaming environment. The gambling site is also a great choice for players in need of a smartphone-friendly casino, since all of the games are accessible on cell phones and tablets.
Meal options range from a hollanderhomes.com choice of hotels without services provided to full board.
check The Sandbox
Лучшие модели колясок Tutis, Как выбрать идеальную коляску от Tutis?, Tutis: самый модный цвет этого сезона, Секреты долговечности и надежности коляски Tutis, правила использования коляски, Tutis: идеальный выбор для активных семей, Почему Tutis лучше конкурентов?, Как правильно ухаживать за коляской Tutis?, Почему Tutis – выбор ответственных родителей, Секреты комфортной поездки с Tutis, рекомендации для родителей, Как выбрать коляску Tutis, подходящую для вашего стиля жизни?, рекомендации стилистов, технологии, делающие коляски лучше, профессиональное мнение, Почему Tutis – надежный партнер для вашей семьи?, поддержка родителей в заботе о ребенке
детские коляски tutis https://kolyaskatutis.ru/ .
Howdy! Would you mind if I share your blog with my twitter group? There’s a lot of folks that I think would really appreciate your content. Please let me know. Many thanks
https://exceptionalcollegeessays.com/
https://newsofgames.ru/page/5
http://www.pc-lessons.ru/main.php?d=1&url=
https://modernbookmarks.com/story16928534/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%80%D0%B0%D1%87%D0%B0
https://b52-i-th-ng58035.blogofoto.com/57844310/the-ultimate-guide-to-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
аниме атака титанов https://ataka-titanov-anime.ru
livingspainhome.com
купи для дома мебель
https://formomebel.ru/stoliki/kruglye
Предприятие активно реализует и внедряет инновационные тренажеры для реабилитации на https://trenazhery-kineziterapiya.ru/ по низким ценам. В наличии МТБ-1 и Кроссовер для перекрестной тяги. Устройства производятся из лучших марок стали и рассчитаны для долгосрочной эксплуатации. конструктивное решение помогает эффективному восстановлению физической формы. Изготавливаемое тренажерное оборудование отличается отличным качеством и надежностью, что дает возможность тренироваться безопасно и эффективно.Предлагаем заказать весовой стек необходимого веса.
Remarkable! Its really remarkable post, I have got much clear idea concerning from this piece of writing.
https://userbookmark.com/story17012566/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9F%D0%B5%D1%80%D0%BC%D0%B8
https://study-english.info/
https://calc-bank.ru/calculator/baltiyskiy_bank
https://bookmarkedblog.com/story17618046/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B5%D0%BB%D1%8C%D0%B4%D1%88%D0%B5%D1%80%D0%B0
https://macrobookmarks.com/story17193481/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82
Дорамы – это удивительный мир, где каждый найдёт что-то для себя. Этот жанр азиатского кинематографа завоевал сердца миллионов зрителей по всему миру. Благодаря своей уникальности, дорамы предлагают захватывающие сюжеты, ярких персонажей и культурное разнообразие. Если вы хотите окунуться в атмосферу восточной романтики или насладиться динамичными боевиками, дорамы станут отличным выбором. На сайте doramaserials.net вы сможете найти лучшие дорамы, которые покорили сердца зрителей по всему миру.
Сайт doramaserials.net предоставляет возможность смотреть дорамы онлайн в любое время и в любом месте. Удобный интерфейс и обширная библиотека позволяют быстро найти нужный сериал и насладиться просмотром. Каждый эпизод доступен в высоком качестве, что делает просмотр еще более приятным. Присоединяйтесь к многомиллионной аудитории поклонников дорам и откройте для себя этот удивительный жанр уже сегодня!
Согласование перепланировки помещения alma-stroi.ru
Перепланировка здания — один из самых главных этапов в строительстве различных объектов. Но в нашей стране, она непременно должна быть узаконена и выполненной по всем стандартам. Мы знаем о перепланировках всё, смотрите на сайте alma-stroi.ru прямо сейчас.
По теме перепланировка помещения мы поможем Вам. Если у Вас уже выполнена несанкционированная перепланировка без документов, то это не страшно. Её также возможно узаконить и с легкостью пользоваться зданием. Не всегда расположение комнат в квартире или промышленных помещениях удовлетворяет владельца. Но в последнее время, перепланировка просто лучший выход из ситуации. Безусловно, выгоднее всего ее проводить на этапе чернового ремонта, но если этого не произошло, то её возможно сделать на любом этапе эксплуатирования.
Цена перепланировки можно посмотреть на веб ресурсе alma-stroi.ru или посмотреть примеры готовых работ. Мы работаем в данной области уже множество лет и имеем много довольных клиентов и выполненных проектов. К каждому проекту имеем персональный подход и учитываем все желания заказчика. Также работаем строго в срок и по весьма приемлемым ценам.
Заказать стоимость согласования перепланировки в москве можно уже сейчас. Наши работники приедут к Вам для измерения помещений и определения размера работы. И после этого будет названа итоговая стоимость и день выполнения работ. Перепланировка — это отличный шанс сделать свою жизнь комфортнее.
https://guardian.ng/news/del-mar-energy-new-horizons-of-development-in-the-sea-of-japan-region/
At this time it appears like Drupal is the best blogging platform available right now. (from what I’ve read) Is that what you are using on your blog?
http://dp-spb.com/forum/thread-2630/
https://thebookmarkking.com/story17004923/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%BE%D0%B2%D0%B0%D1%80%D0%B0
https://stephenq8s88.onesmablog.com/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B8%D0%B7-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-67298134
https://arzhaniki.ru/viewtopic.php?t=66704
https://markets-near-me50481.mdkblog.com/32366943/how-much-you-need-to-expect-you-ll-pay-for-a-good-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
Самые популярные коляски Tutis, выбор мамочек в-the-know, Tutis: самый модный цвет этого сезона, Инструкция по эксплуатации коляски Tutis, подробное руководство для родителей, какие покупки сделать в первую очередь, Почему Tutis лучше конкурентов?, Секреты долговечности и красоты вашей коляски Tutis, Почему Tutis – выбор ответственных родителей, рекомендации по безопасности, полезные советы для удобства, советы по выбору, Почему Tutis – марка будущего, Секреты выбора идеальной коляски Tutis для вашего малыша, Tutis: элегантность и стиль, Почему Tutis – надежный партнер для вашей семьи?, надежность и комфорт в каждом шаге
tutis коляска tutis коляска .
Выбор элитных колясок Tutis, для требовательных родителей, рекомендации по покупке, Как правильно собрать и использовать коляску Tutis?, Лучшее дополнение к вашей коляске от Tutis, аксессуары, которые сделают вашу жизнь проще, секреты успешного выбора, Секреты долговечности и красоты вашей коляски Tutis, Какие меры безопасности важно соблюдать при использовании коляски Tutis?, рекомендации по безопасности, рекомендации для родителей, Почему Tutis лучше всего подходит для вашей семьи?, подгонка под ваш образ жизни, новинки на рынке детских товаров, Как подчеркнуть свой стиль с помощью коляски Tutis?, коляска, подчеркивающая ваш образ, надежность и комфорт в каждом шаге
детские коляски tutis https://kolyaskatutis.ru/ .
Идеальная коляска Cybex для вашего малыша, лучшие предложения.
Лучшие оферты на коляски Cybex, для истинных ценителей качества.
5 причин выбрать именно коляску Cybex для вашего малыша, которые заставят вас влюбиться в этот бренд.
Коляска Cybex: безопасность и стиль в одном флаконе, которые не оставят вас равнодушными.
Элегантные решения для вашего ребенка – коляски Cybex, учитывая все особенности и пожелания.
Советы по выбору коляски Cybex для вашего малыша, исходя из индивидуальных потребностей и предпочтений.
Трендовые коляски Cybex для вашего малыша, которые ценят комфорт и безопасность.
Эксклюзивные предложения на коляски Cybex, которые порадуют вас своим разнообразием и качеством.
Ключевые моменты, на которые стоит обратить внимание при выборе коляски Cybex, для вашего малыша.
Выбор коляски Cybex: что важно знать перед покупкой, чтобы сделать правильный выбор.
Элегантные решения для вашей семьи – коляски Cybex, которые не оставят вас равнодушными.
Лучшие модели колясок Cybex для вашей семьи, которые порадуют вас своим качеством и функционалом.
Как выбрать коляску Cybex: главные моменты, которые стоит рассмотреть перед покупкой.
Почему стоит выбрать именно коляски Cybex, если вы цените качество и комфорт.
Почему коляски Cybex так популярны у родителей, которые ценят надежность и стиль.
Как выбрать идеальную коляску Cybex для вашего малыша: подробный гид, перед совершением покупки.
Топ-5 лучших моделей колясок Cybex, исходя из личных предпочтений и потребностей.
Лучшие предложения на коляски Cybex для вашей семьи, которые не оставят вас равнодушными.
cybex купить коляску https://kolyaskicybex.ru/ .
I blog quite often and I truly thank you for your information. Your article has really peaked
my interest. I’m going to bookmark your website and keep checking for
new details about once a week. I subscribed to
your RSS feed as well.
My partner and I absolutely love your blog and find a lot of your post’s to be just what I’m looking for. Would you offer guest writers to write content for you? I wouldn’t mind producing a post or elaborating on most of the subjects you write about here. Again, awesome weblog!
http://niceroleplay.getbb.ru/viewtopic.php?t=662
https://binksites.com/story6693338/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%95%D0%BA%D0%B0%D1%82%D0%B5%D1%80%D0%B8%D0%BD%D0%B1%D1%83%D1%80%D0%B3%D0%B5
https://hubwebsites.com/story18428537/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2%D1%81%D0%BB%D0%B5%D0%B4%D1%81%D1%82%D0%B2%D0%B8%D0%B5-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://www.tonylandis.com/
https://freebookmarkpost.com/story16998832/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
It is necessary to follow some thespice.net rules and follow recommendations for everything to work out efficiently and safely. You can order the production of metal structures on the website to profitably invest your own money. Let’s consider the basic rules that relate to this process.
Hey! This is my 1st comment here so I just wanted to give a quick shout out and tell you I truly enjoy reading through your posts. Can you suggest any other blogs/websites/forums that cover the same topics? Many thanks!
https://bookmarkja.com/story18556146/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B5%D0%BB%D1%8C%D0%B4%D1%88%D0%B5%D1%80%D0%B0
http://www.vocal.com.ua/blog/www.xuzhouabl.com/www.xuzhouabl.com/en?page=47
https://ricardosqnje.blazingblog.com/26822932/5-essential-elements-for-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://apollobookmarks.com/story17040106/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
https://adventure-vinwonders.com/vi/
geinoutime.com
“아…” Xiao Jiao Jing은 그의 얼굴에 믿을 수 없는 표정으로 당황했습니다.
Лучшие модели колясок Tutis, для стильных семей, секреты правильного выбора, универсальный вариант, правила использования коляски, какие покупки сделать в первую очередь, рекомендации профессионалов, сравнительный анализ колясок, Tutis: безопасность вашего малыша превыше всего, Как сделать прогулку с Tutis особенно комфортной?, рекомендации для родителей, Какие факторы учитывать при выборе коляски Tutis, Почему Tutis – марка будущего, Как выбрать коляску Tutis с максимальным комфортом для ребенка?, профессиональное мнение, Почему Tutis – выбор сознательных семей, преимущества использования коляски Tutis
купить коляску тутис 3 в 1 купить коляску тутис 3 в 1 .
guaranteed approval loans with bad credit Today’s modern consumer, raised entirely with social media, can even apply for these micro-loans using their smartphones, with money transferred to successful applicant’s bank accounts within minutes.
In such a situation, it autonow.net is necessary to dismantle the tiles in the place where the gazebo will stand. Then, as in the previous case, the soil surface is drilled and a profile is installed on which all structures are supported.
What’s up, this weekend is fastidious for me, as this point in time i am reading this wonderful educational piece of writing here at my residence.
https://novator.team/
https://bookmark-nation.com/story17077662/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://mirrorbookmarks.com/story17074493/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B5%D0%BB%D1%8C%D0%B4%D1%88%D0%B5%D1%80%D0%B0
https://hindibookmark.com/story18491605/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%92%D0%BE%D1%80%D0%BE%D0%BD%D0%B5%D0%B6%D0%B5
https://top-estate-soft.ru/
Howdy! I understand this is somewhat off-topic but I needed to ask. Does building a well-established website like yours require a large amount of work? I’m completely new to blogging but I do write in my diary daily. I’d like to start a blog so I can share my personal experience and views online. Please let me know if you have any recommendations or tips for brand new aspiring blog owners. Thankyou!
https://marcoefffe.blogoscience.com/32815472/marketing-fundamentals-explained
https://bookmarknap.com/story6998014/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%B0%D1%80%D0%B8%D0%BA%D0%BC%D0%B0%D1%85%D0%B5%D1%80%D0%B0
https://shaneh2l29.blogolize.com/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2-%D1%83%D0%B3%D0%BE%D0%B4%D1%83-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-66560491
https://thetechnologynews61482.bleepblogs.com/27328913/marketing-things-to-know-before-you-buy
https://teploxodiki.ru/
Самые популярные коляски Tutis, для стильных семей, Какой цвет коляски Tutis выбрать?, Инструкция по эксплуатации коляски Tutis, Необходимые аксессуары для комфортной прогулки с ребенком, Как выбрать коляску Tutis для активного образа жизни, Как не ошибиться с выбором между Tutis и другими марками, рекомендации по выбору лучшей модели, Tutis: безопасность вашего малыша превыше всего, рекомендации по безопасности, Tutis: лучший выбор для любого сезона, Почему Tutis лучше всего подходит для вашей семьи?, Tutis: инновации и технологии, Как выбрать коляску Tutis с максимальным комфортом для ребенка?, Как подчеркнуть свой стиль с помощью коляски Tutis?, стильный аксессуар для пап, надежность и комфорт в каждом шаге
коляска tutis купить https://kolyaskatutis.ru/ .
Creation of a metal structure yourfloridafamily.com project. It is necessary to ensure that each drawing and basic calculations are correct. Loads, operating conditions of the product, as well as basic safety standards are taken into account.
Ищете, где можно корейские дорамы смотреть онлайн? Сайт doramaserials.net – это идеальное место для всех поклонников азиатского кино! Здесь вы найдете огромный выбор корейских дорам, доступных в высоком качестве и без назойливой рекламы. Каждая серия озвучена профессиональными актерами, что позволяет полностью погрузиться в захватывающий сюжет и насладиться великолепной актерской игрой.
Сайт doramaserials.net предлагает удобный интерфейс и регулярные обновления, чтобы вы всегда могли быть в курсе последних новинок. Независимо от того, предпочитаете ли вы романтические истории, драматические сюжеты или комедийные сериалы, здесь каждый найдет что-то для себя. Откройте для себя мир корейских дорам и наслаждайтесь просмотром без ограничений вместе с нами!
Marvelous, what a webpage it is! This blog presents helpful information to us, keep it up.
https://captainbookmark.com/story17035168/%D0%B3%D0%B4%D0%B5-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://yourealtynews.ru/dostupnyie-i-professionalnyie-diplomyi-poluchite-svoy-pryamo-seychas
https://t-i-b5225689.life3dblog.com/26363391/the-ultimate-guide-to-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://ragingbookmarks.com/story17194834/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://www.edpillsfinder.com/
how to make money from online casino bonuses gaming bets
Vavada – топовая онлайн площадка, предлагающая широкий ассортимент увлекательных игровых автоматов, призванных дать невероятные ощущения от азартных игр. С более чем 600 игровыми автоматами в базе сайта Вавада удовлетворит игровые предпочтения каждого.
вавада игровые автоматы сайт – идеальный выбор для тех, кто ищет захватывающий и разного рода игровой опыт. С обширным каталогом, высококачественной графикой, щедрыми бонусами и безкомпромиссной репутацией Вавада обеспечивает бесконечные часы развлекухи для игроков любого уровня.
Поклонники японских сериалов будут в восторге от ассортимента, представленного на сайте doramaserials.net. Здесь вы сможете японские дорамы смотреть онлайн без рекламы и в превосходном качестве. Каждая дорама — это захватывающая история, полная эмоций и неожиданных поворотов сюжета. Независимо от ваших предпочтений, вы обязательно найдете что-то, что захватит ваше внимание.
Особенно приятно, что все японские дорамы с русской озвучкой. Это позволяет наслаждаться просмотром, не отвлекаясь на чтение субтитров. Профессиональная озвучка делает каждую сцену еще более яркой и запоминающейся. Сайт doramaserials.net предлагает удобную навигацию и регулярные обновления каталога, что делает его идеальным местом для всех любителей японских сериалов. Присоединяйтесь к нам и откройте для себя мир удивительных японских дорам!
Почему стоит построить дом из бруса 9х12 | Почему стоит построить дом из бруса 9х12 | Выбор кровельных материалов для дома из бруса 9х12 | Выбор системы отопления для дома из бруса 9х12 | Типы фундаментов для дома из бруса 9х12 | Особенности окон и дверей в доме из бруса 9х12 | Дизайн ландшафта для дома из бруса 9х12 | Топ-5 мебельных трендов для дома из бруса 9х12 | Для комфортного отдыха: зона lounge в доме из бруса 9х12 | Сколько стоит построить дом из бруса 9х12
дом из бруса 9х12 https://domizbrusa-9x12spb.ru/ .
Hi, I want to subscribe for this blog to get newest updates, thus where can i do it please help out.
https://akademiyatepla.ru/
https://archers1d34.pointblog.net/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2%D1%81%D0%BB%D0%B5%D0%B4%D1%81%D1%82%D0%B2%D0%B8%D0%B5-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-68145210
https://jaredbkppo.isblog.net/top-marketing-secrets-43941383
https://disposablegloves05936.digitollblog.com/26597773/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA-things-to-know-before-you-buy
https://ditichlichsuvanhoa.com/dttc/COT-DAY-THEP-a994.html
Thanks for some other informative site. Where else may just I get that type of information written in such a perfect method? I’ve a mission that I’m just now running on, and I’ve been on the glance out for such information.
https://topnewsgadget.ru/poluchite-svoy-diplom-bez-stressa-nash-servis-zabotitsya-o-vas
https://www.startspresto.ru/lichnyj-kabinet/pluginclass/cbblogs?action=blogs&func=show&id=77
https://pukkabookmarks.com/story17153243/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%BE%D0%B2%D0%B0%D1%80%D0%B0
http://malhotrafoundation.org/about/who-we-are
https://sdiplom1.ru/
What’s up mates, its enormous piece of writing about educationand entirely explained, keep it up all the time.
https://moodjhomedia.com/story1451150/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
http://www.ivedu.ru/forum/viewthread.php?forum_id=18&thread_id=45646
https://redhotbookmarks.com/story17071338/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B0%D1%81%D1%81%D0%B0%D0%B6%D0%B8%D1%81%D1%82%D0%B0
https://funbookmarking.com/story17082812/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B5%D0%BB%D1%8C%D0%B4%D1%88%D0%B5%D1%80%D0%B0
https://toursoul.ru/?p=19009
голяк онлайн в хорошем качестве голяк смотреть бесплатно
indian tribe online loans So, there are several options you have for no employment verification cash advance, but make sure that you use this option only if there is absolute need for it and if you don’t have any other way out.
The other day, while I was at work, my cousin stole my apple ipad and tested to see if it can survive a thirty foot drop, just so she can be a youtube sensation. My apple ipad is now broken and she has 83 views. I know this is totally off topic but I had to share it with someone!
https://userbookmark.com/story17012566/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9F%D0%B5%D1%80%D0%BC%D0%B8
https://unitedindoorfootball.com/
https://bookmarkfavors.com/story2509447/%D0%B3%D0%B4%D0%B5-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://zbookmarkhub.com/story17214077/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%B0%D1%80%D0%B8%D0%BA%D0%BC%D0%B0%D1%85%D0%B5%D1%80%D0%B0
http://tuning-performance.ru/kuzovnoy-remont-auto/
Аренда квартиры не дает права на длительное пребывание на Кипре. Но договор нужен, чтобы подать документы на визу и сделать медицинскую страховку аренда кипр
Please let me know if you’re looking for a article writer for your blog. You have some really great articles and I think I would be a good asset. If you ever want to take some of the load off, I’d really like to write some articles for your blog in exchange for a link back to mine. Please blast me an email if interested. Regards!
https://my-social-box.com/story2378431/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B0%D1%80%D0%BC%D0%B0%D1%86%D0%B5%D0%B2%D1%82%D0%B0
https://jasperpagnr.madmouseblog.com/7302357/not-known-facts-about-marketing
https://www.hip-hop.ru/forum/id298234-worksale/index2.html
https://lifeatbahriatown.com/index.php?page=user&action=pub_profile&id=10545
https://www.argonband.it/web/modules.php?name=Forums&file=profile&mode=viewprofile&u=167137
голяк смотреть бесплатно в хорошем качестве https://golyak-serial-online.ru
This is really interesting, You are a very skilled blogger. I have joined your feed and look forward to seeking more of your wonderful post. Also, I have shared your web site in my social networks!
https://newsato.ru/kupit-diplom-bez-riska-myi-garantiruem-vashe-udovletvorenie
http://express-container.ru/news/64/
https://apuestas-deportivas59358.dsiblogger.com/59456374/an-unbiased-view-of-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://americanautotitleloan.com/
https://tealbookmarks.com/story17190543/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
Hello to all, how is all, I think every one is getting more from this website, and your views are nice in support of new visitors.
https://t-i-b5225689.life3dblog.com/26363391/the-ultimate-guide-to-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://holdenwsmfx.vidublog.com/26391929/about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://ez-bookmarking.com/story16992581/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
https://optimusbookmarks.com/story17084765/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B5%D0%BB%D1%8C%D0%B4%D1%88%D0%B5%D1%80%D0%B0
https://socialtechnet.com/story2423605/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D0%B0%D0%BD%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D0%B0
Useful information. Fortunate me I found your site unintentionally, and I’m surprised why this twist of fate didn’t happened earlier! I bookmarked it.
http://hobby-svarka.ru/topic5343.html
http://www.domali.ru/main.php?d=1&url=
https://altbookmark.com/story18583774/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9E%D0%BC%D1%81%D0%BA%D0%B5
https://bookmarkcork.com/story17590866/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%92%D0%BE%D0%BB%D0%B3%D0%BE%D0%B3%D1%80%D0%B0%D0%B4%D0%B5
https://essaywritingaustralia.com/order-now/
Click Here Pot player
как помочь алкоголику бросить пить https://lechenie-alkogolizma.kz/
Wow that was unusual. I just wrote an incredibly long comment but after I clicked submit my comment didn’t appear. Grrrr… well I’m not writing all that over again. Anyways, just wanted to say wonderful blog!
https://wegug.in/blogs/324/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%B4%D0%B8%D0%BD-%D0%BA%D0%BB%D0%B8%D0%BA-%D0%A3-%D0%BD%D0%B0%D1%81-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE-%D0%B8-%D0%BF%D1%80%D0%BE%D1%81%D1%82%D0%BE?lang=ru_ru
https://brooksz1m31.blogdemls.com/26853163/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B8%D0%B7-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://express-container.ru/news/64/
https://rpgtop.su/
http://lolipopnews.ru/page/4
blacksprut ссылка – блэк спрут ссылка, блэк спрут
Keep on working, great job!
https://thebookmarkid.com/story17174719/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A1%D0%B0%D1%80%D0%B0%D1%82%D0%BE%D0%B2
http://painting.artyx.ru/
http://ветерантюмгео.рф/1733-2/
https://medical-gloves71471.frewwebs.com/27289904/how-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-can-save-you-time-stress-and-money
http://la-buket.ru/catalog/bestsellers/
go now Creative your account sandbox
Howdy! Do you use Twitter? I’d like to follow you if that would be okay. I’m undoubtedly enjoying your blog and look forward to new posts.
http://realtyintellect.ru/diplomyi-po-vashemu-zaprosu-u-nas-est-to-chto-vam-nuzhno-dlya-uspeha
https://burnlabproreview46715.blog5.net/68508854/helping-the-others-realize-the-advantages-of-marketing
https://women03468.p2blogs.com/26397377/the-fact-about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA-that-no-one-is-suggesting
http://venturetraining.net/contact/
https://myeasybookmarks.com/story2479527/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%A7%D0%B5%D0%BB%D1%8F%D0%B1%D0%B8%D0%BD%D1%81%D0%BA%D0%B5
тенниси промокод
I’m gone to say to my little brother, that he should also pay a quick visit this webpage on regular basis to obtain updated from most recent news update.
https://sparxsocial.com/story7056117/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%82%D1%80%D0%BE%D0%B8%D1%82%D0%B5%D0%BB%D1%8F
http://html-studio.paris/
https://marsaxlokkfc.com/
http://mdoucrr-ds28.ru/
http://www.kkiinnoo.ru/main.php?d=1&url=
bad credit loans in tulsa ok Shortening the accounts receivable cycle time generates the healthy cash flow that is required to sustain your company’s growth and prosperity.
Hi, this weekend is good in favor of me, since this moment i am reading this impressive educational paragraph here at my house.
https://wearethelist.com/story18668783/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%BE%D0%B2%D0%B0%D1%80%D0%B0
https://www.mountbarkertourismwa.com.au/attractions.html
https://www.odessamama.net/home.php?mod=space&uid=8519&do=blog&id=2241
https://vostlit.info/
https://hindibookmark.com/story18491605/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%92%D0%BE%D1%80%D0%BE%D0%BD%D0%B5%D0%B6%D0%B5
his comment is here Sandbox AVATAR
Related Site Sandbox AVATAR
his comment is here VoxEdit – NFT Creator
click this link here now Sandbox AVATAR
Выбор элитных колясок Tutis, для требовательных родителей, секреты правильного выбора, Секреты долговечности и надежности коляски Tutis, Необходимые аксессуары для комфортной прогулки с ребенком, Tutis: идеальный выбор для активных семей, Почему Tutis лучше конкурентов?, сравнительный анализ колясок, Какие меры безопасности важно соблюдать при использовании коляски Tutis?, рекомендации по безопасности, Почему Tutis подойдет и летом, и зимой, Какие факторы учитывать при выборе коляски Tutis, Какие новшества представляет Tutis?, новинки на рынке детских товаров, рекомендации экспертов, модный атрибут для мам, преимущества использования коляски Tutis
tutis коляска 3 в 1 https://kolyaskatutis.ru/ .
Thanks for the auspicious writeup. It if truth be told was once a amusement account it. Glance advanced to more delivered agreeable from you! By the way, how can we be in contact?
https://t-i-b5225689.life3dblog.com/26363391/the-ultimate-guide-to-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://homedoctorbook.xyz/
https://centimetroquadro.it/
https://webnowmedia.com/story2388351/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D1%81%D1%80%D0%B5%D0%B4%D0%BD%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8
http://www.fsh.mi.th/newswb3/index.php?action=recent;start=10
Get the facts Official Airdrop Is Live!
More Help Official Airdrop Is Live!
форум вебкам моделей и моделей OnlyFans! Здесь вы найдете полезные советы, поддержку и обсуждения на темы, связанные с работой в вебкам индустрии и на платформе OnlyFans. Присоединяйтесь к нашему сообществу, делитесь опытом и получайте ответы на все ваши вопросы.
https://forum.vipcamclub.ru/
Fabulous, what a blog it is! This webpage gives valuable data to us, keep it up.
http://flashtest.80lvl.ru/viewtopic.php?f=3&t=1782
https://bookmarkport.com/story18863770/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9F%D0%B5%D1%80%D0%BC%D0%B8
http://www.ytchebnik.ru/334.html
https://latestcryptonews70368.webbuzzfeed.com/27252095/not-known-factual-statements-about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://bookmarkmoz.com/story17076276/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9D%D0%BE%D0%B2%D0%BE%D1%81%D0%B8%D0%B1%D0%B8%D1%80%D1%81%D0%BA%D0%B5
Good post. I learn something new and challenging on sites I stumbleupon everyday. It’s always helpful to read articles from other writers and use something from other web sites.
https://hector34wv0.blog2news.com/27285949/a-secret-weapon-for-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://socialnetworkadsinfo.com/story19143786/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%92%D0%BE%D1%80%D0%BE%D0%BD%D0%B5%D0%B6%D0%B5
https://martinloonn.ezblogz.com/58349366/the-definitive-guide-to-marketing
https://rsn360.ru/blogs/258/%D0%9F%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D0%BE%D0%B2%D0%B0%D0%BB%D0%BE%D1%81%D1%8C-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9F%D0%B5%D1%80%D0%B5%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5-%D0%B2-%D0%BD%D0%B0%D1%88-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD
http://neurontin-gabapentin.com/
Недвижимость в новостройке на Северном Кипре. Недвижимость в новостройке на Северном Кипре является одним из самых популярных вариантов недвижимость на кипре компания
Hi! Would you mind if I share your blog with my myspace group? There’s a lot of folks that I think would really appreciate your content. Please let me know. Thank you
https://bookmarksoflife.com/story2532665/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
http://prikol100500.ru/poluchite-svoy-diplom-bez-lishnih-hlopot-prisoedinyaytes-seychas
http://1001cruise.ru/catcasino.html
https://ez-bookmarking.com/story16992581/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B1%D0%B0%D0%BA%D0%B0%D0%BB%D0%B0%D0%B2%D1%80%D0%B0
https://charliempppo.bloginwi.com/60449486/top-latest-five-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-urban-news
Chicago IL McKinley Park cash advance Essentially, anybody who has more than that base amount in their estate will be charged 40-50% of any assets that they owned over that amount.
Appreciating the hard work you put into your website and in depth information you provide. It’s awesome to come across a blog every once in a while that isn’t the same unwanted rehashed material. Great read! I’ve saved your site and I’m including your RSS feeds to my Google account.
https://zaim933966.ru/onlayn-zayavka
https://210list.com/story17674484/%D0%A4%D0%B0%D0%BB%D1%8C%D1%88%D0%B8%D0%B2%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D1%8D%D1%82%D0%BE-%D0%BD%D0%B5-%D0%A1%D1%82%D0%BE%D0%B8%D1%82-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://exactlybookmarks.com/story17050247/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D1%81%D1%80%D0%B5%D0%B4%D0%BD%D0%B5%D0%BC-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%BC
https://zhaktrans.ru/g2789651-frontalnye-pogruzchiki
https://bookmarkity.com/story17199028/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
Год 2024 готовит множество сюрпризов для поклонников азиатских сериалов. Самые ожидаемые дорамы 2024 уже ждут вас на сайте doramaserials.net! Здесь вы найдете новейшие дорамы с русской озвучкой онлайн, которые можно смотреть бесплатно. Каждый эпизод доступен в высоком качестве, без рекламы и лишних преград, что делает просмотр максимально приятным и комфортным.
На doramaserials.net вас ждут только самые лучшие и свежие дорамы, которые подарят вам незабываемые эмоции и впечатления. Независимо от вашего предпочтения – будь то романтика, драма или триллер – здесь каждый найдет что-то по душе. Погружайтесь в мир захватывающих историй и наслаждайтесь каждым моментом вместе с нами! Присоединяйтесь к сообществу поклонников дорам и открывайте новые горизонты вместе с doramaserials.net!
Wow, that’s what I was seeking for, what a data! present here at this weblog, thanks admin of this website.
Great post. I’m facing a few of these issues as well..
It’s going to be end of mine day, however before finish I am reading this enormous piece of writing to improve my knowledge.
Great post however , I was wondering if you could write a litte more on this topic? I’d be very thankful if you could elaborate a little bit more. Cheers!
http://forums.shlock.co.uk/viewtopic.php?p=24110
http://www.korea-zs.ru/main.php?d=1&url=
https://devinjkifb.daneblogger.com/26487122/about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://blog-doma.ru/
https://www.fksmederevo.com/
Online Platforms Offering the Game aviator game prediction
It’s amazing designed for me to have a website, which is useful for my experience. thanks admin
https://fatallisto.com/story6626481/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%8E%D1%80%D0%B8%D1%81%D1%82%D0%B0
https://elarus.ru/
https://indexedbookmarks.com/story16981752/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
http://www.die-wuiderer.de/memberlist.php?mode=joined&order=ASC&start=88700
https://agendabookmarks.com/story17009199/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9A%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B4%D0%B0%D1%80%D0%B5
Howdy this is kind of of off topic but I was wanting to know if blogs use WYSIWYG editors or if you have to manually code with HTML. I’m starting a blog soon but have no coding skills so I wanted to get advice from someone with experience. Any help would be enormously appreciated!
http://51.15.223.140/forum/member.php?tab=visitor_messaging&u=76509&page=3
https://teplica-parnik.net/
http://mafiaclans.ru/topic5033.html
https://motorcycle-reviews32677.blog-mall.com/27362106/how-much-you-need-to-expect-you-ll-pay-for-a-good-marketing
http://forum.drustvogil-galad.si/index.php?topic=10035.0
I blog often and I truly thank you for your content. The article has truly peaked my interest. I’m going to bookmark your site and keep checking for new information about once a week. I subscribed to your RSS feed as well.
https://kolybel-ekb.ru/
https://www.nomer-doma.ru/
https://iowa-bookmarks.com/story12629968/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9C%D0%BE%D1%81%D0%BA%D0%B2%D0%B5
http://weekevents.ru/zakazhite-diplom-onlayn-i-dvigaytes-vpered-bez-prepyatstviy
https://deanyggeb.tblogz.com/a-secret-weapon-for-41051717
Hello there! Do you use Twitter? I’d like to follow you if that would be okay. I’m definitely enjoying your blog and look forward to new posts.
https://atozbookmark.com/story17114917/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://social-medialink.com/story2412314/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://bookmarkforest.com/story17050715/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D1%81%D1%81%D1%80
http://blog-doma.ru/
https://olivebookmarks.com/story17301962/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2-%D1%83%D0%B3%D0%BE%D0%B4%D1%83-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
Hi there, I desire to subscribe for this weblog to obtain latest updates, thus where can i do it please help.
https://getsocialpr.com/story17673667/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9A%D0%B0%D0%B7%D0%B0%D0%BD%D0%B8
https://social-lyft.com/story6797484/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B8%D1%81%D1%82%D1%80%D0%B0
https://local-urban-eats.mn.co/posts/55565472
http://comedyforme.ru/uspeshnoe-zavershenie-vashego-obrazovaniya-poluchite-svoy-diplom-seychas
https://www.dancerussia.ru/forum/viewtopic.php?p=24546
Накрутка подписчиков Инстаграм, Тик Ток, Ютуб, Телеграм, Твиттер
https://www.otzyvua.net/uk/nakrutkamediacom
Numerous online casino platforms offer the Aviator Game. These platforms provide a secure and regulated aviator game online
На сайте https://split-sistemy-77.ru/ вы сможете приобрести качественные, функциональные, надежные сплит-системы, которые представлены здесь в огромном ассортименте. Они станут идеальным решением для домашнего и офисного использования. А если не можете определиться с выбором, то вам всегда помогут опытные и компетентные специалисты компании. Все устройства представлены проверенными, лучшими производителями. Они дают гарантии на все оборудование. Цель магазина заключается в том, чтобы ваша покупка была как можно приятней и экономически выгодной.
I’m not sure exactly why but this site is loading very slow for me. Is anyone else having this issue or is it a problem on my end? I’ll check back later and see if the problem still exists.
https://apparel91357.anchor-blog.com/7055692/the-ultimate-guide-to-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://cryptomoneynews15703.is-blog.com/33096262/about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
http://jusonline.ru/mix/poluchenie-obrazovaniya-v-rf-i-professionalnoe-razvitie.html
https://griffinuxyyx.thenerdsblog.com/32333849/marketing-an-overview
https://www.zoofc.org/
This text is priceless. Where can I find out more?
https://bookmarkspedia.com/story2483603/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D1%80%D0%BE%D0%B3%D1%80%D0%B0%D0%BC%D0%BC%D0%B8%D1%81%D1%82%D0%B0
https://rylandeczw.therainblog.com/26344812/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0-an-overview
https://bestcoolfun.ru/diplomyi-po-vashemu-vyiboru-zakazhite-onlayn-i-poluchite-ih-byistro
https://wisesocialsmedia.com/story2376537/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
https://bookmarkswing.com/story18315758/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B5%D0%BD%D0%B5%D0%B4%D0%B6%D0%B5%D1%80%D0%B0
Накрутка подписчиков Инстаграм, Тик Ток, Ютуб, Телеграм, Твиттер
https://www.sq.com.ua/rus/press_release/04.10.2023/kupit-podpiscikov-v-ukraine-vasi-preimushhestva-i-garantii-kakoi-sait-v-etom-pomozet-body
Hey there! This is my first comment here so I just wanted to give a quick shout out and tell you I really enjoy reading through your articles. Can you suggest any other blogs/websites/forums that deal with the same topics? Thanks!
https://amengram.com/blogs/61/%D0%9F%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D0%BE%D0%B2%D0%B0%D0%BB%D0%BE%D1%81%D1%8C-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9F%D0%B5%D1%80%D0%B5%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5-%D0%B2-%D0%BD%D0%B0%D1%88-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD?lang=en_us
https://b52-i-th-ng50370.blogadvize.com/33129426/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-options
https://brisbaneglobaltens.com/tickets/
http://neverwinter-wiki.ru/besstrashnyj-voin-great-weapon-fighter-gajd-po-klassu
https://thebookmarklist.com/story17148781/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
payday loan stores in surrey bc In general, there are few requirements to receiving a payday loan.
twin casino
I believe everything composed made a bunch of sense. However, think on this, what if you were to write a awesome title? I mean, I don’t want to tell you how to run your website, but suppose you added a title that grabbed folk’s attention? I mean %BLOG_TITLE% is a little boring. You should look at Yahoo’s home page and note how they create article titles to get people to click. You might add a related video or a picture or two to grab readers excited about everything’ve written. In my opinion, it might make your website a little bit more interesting.
https://cyberbookmarking.com/story17033857/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B0%D1%80%D0%BC%D0%B0%D1%86%D0%B5%D0%B2%D1%82%D0%B0
https://allnewstur.ru/page/2
http://forum.muimperio.site/showthread.php?tid=4069
https://myanmarfootball.org/
https://pr7bookmark.com/story17267370/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B5%D1%85%D0%B0%D0%BD%D0%B8%D0%BA%D0%B0
Купить дом Кипр. Все актуальные предложения о продаже домов, дач в Кипре в одном месте – всего размещено – 707 объявлений. Наиболее низкая стоимость продажи дома купить квартиру на южном кипре недорого
https://telegra.ph/Dengi-pod-pts-spb-06-13
enjoyable. aviator game install for pc
Hello mates, its enormous piece of writing regarding cultureand completely defined, keep it up all the time.
https://auto-dealers-script.com/
https://socialbookmarkgs.com/story17150278/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0
https://mushroomchocolate37036.thekatyblog.com/26308468/the-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA-diaries
https://newtownmemorialfund.org/
https://tripsbookmarks.com/story17149543/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%80%D0%B0%D1%87%D0%B0
Накрутка подписчиков Инстаграм, Тик Ток, Ютуб, Телеграм, Твиттер
https://teletap.org/novosti-mira/pravdivyj-vzglyad-na-nakrutku-lajkov-v-soczialnyh-setyah.html
Oh my goodness! Awesome article dude! Thanks, However I am experiencing issues with your RSS.
I don’t understand why I can’t subscribe to it. Is there anyone else having the same RSS problems?
Anyone who knows the solution can you kindly respond? Thanx!!
You have noted very interesting points! ps decent website.
Have a look at my blog :: free to air tv (80aaghdc1brekc3alcdm.рф)
We offer premium databases for Xrumer 23 ai Strong and GSA Search Engine Ranker. Detailed information can be found here https://dseo24.monster
Хотите быть в курсе всех сенсаций из мира UFC? Octagon Express предлагает вам главные новости UFC на сегодня! Мы публикуем самые свежие и горячие материалы: интервью с бойцами, аналитические обзоры, захватывающие видео. Будьте первым, кто узнает о всех значимых событиях и подробностях. Подписывайтесь на Octagon Express и следите за всеми новостями UFC!
купить оземпик +в интернет аптеке – оземпик купить москва аптека, оземпик препарат
Hi, its pleasant paragraph concerning media print, we all understand media is a impressive
source of information.
https://antheat9.bloggersdelight.dk/2024/06/13/%d0%ba%d1%80%d0%b5%d0%b4%d0%b8%d1%82-%d0%bf%d0%be%d0%b4-%d0%b7%d0%b0%d0%bb%d0%be%d0%b3-%d0%b0%d0%b2%d1%82%d0%be-%d0%b2-%d1%81%d0%bf%d0%b1/
Hello, everything is going perfectly here and ofcourse every one is sharing data, that’s in fact good, keep up writing.
https://top100bookmark.com/story17159960/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
https://cruxbookmarks.com/story17135185/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%BE%D0%B2%D0%B0%D1%80%D0%B0
https://worldstockmarkets49269.nizarblog.com/26908206/helping-the-others-realize-the-advantages-of-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
https://vet-aibolit.ru/
https://toursoul.ru/?p=19009
site Osu
Competitive Tournaments and Events how to play aviator and win
Why visitors still make use of to read news papers when in this technological globe everything is existing on net?
https://cruztdmt63184.wikirecognition.com/686373/%D0%9A%D0%B0%D0%BA_%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C_%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82_%D0%B7%D0%B0_9_%D0%BA%D0%BB%D0%B0%D1%81%D1%81_%D1%88%D0%B0%D0%B3_%D0%BA_%D0%BD%D0%BE%D0%B2%D1%8B%D0%BC_%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE%D1%81%D1%82%D1%8F%D0%BC
http://www.kino-rf.ru/main.php?d=1&url=
http://url.atde.ru/main.php?d=1&url=
https://agendabookmarks.com/story17009199/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%9A%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B4%D0%B0%D1%80%D0%B5
https://mazda-demio.ru/forums/index.php?autocom=gallery&req=si&img=4333
An impressive share! I’ve just forwarded this onto a co-worker who has been conducting a little homework on this. And he actually bought me dinner simply because I discovered it for him… lol. So let me reword this…. Thanks for the meal!! But yeah, thanx for spending some time to discuss this matter here on your website.
https://ilmaiskierroksia75295.affiliatblogger.com/78887244/not-known-facts-about-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0
http://www.phonotope.net/topics/archives/000052.html
http://ford-talks.ru/topic4441.html
http://terios2.ru/forums/index.php?autocom=gallery&req=si&img=2689
https://t-i-b5205713.articlesblogger.com/49661859/getting-my-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-to-work
https://telegra.ph/Dengi-pod-zalog-avto-pod-pts-06-13
Check Out Your URL Notepad download
Накрутка подписчиков Инстаграм, Тик Ток, Ютуб, Телеграм, Твиттер
https://donklephant.net/sport/nakrutka-i-sport-kak-prodvigat-sportivnye-meropriyatiya-i-tovary-s-pomoshhyu-nakrutkamedia-com.html
Hi there it’s me, I am also visiting this website on a regular basis, this site is truly good and the users are in fact sharing nice thoughts.
http://sankeystokyo.info/
https://www.dancerussia.ru/forum/viewtopic.php?p=24546
https://chancey1s75.estate-blog.com/26795004/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://umorforme.ru/diplom-s-garantiey-kachestva-vyiberite-nas
https://calc-bank.ru/calculator/baltiyskiy_bank
It’s amazing for me to have a website, which is good in support of my knowledge. thanks admin
https://exceptionalcollegeessays.com/
https://minibookmarks.com/story17036817/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%A7%D0%B5%D0%BB%D1%8F%D0%B1%D0%B8%D0%BD%D1%81%D0%BA%D0%B5
https://ute.expert/showthread.php?tid=2&page=69
https://rafaelmtwza.educationalimpactblog.com/49064291/not-known-facts-about-marketing
http://morskie-cruizy.ru/
social interaction adds a new layer of excitement and competition to the game, making it more engaging and aviator game tips and tricks
There are also desirable promotions, like, for example,
cost-free spins and refer-a-pal casino bonus bargains.
Also visit my website … 온카
https://fingercrack1.werite.net/kredit-s-zalogom-avtomobilia
What’s up colleagues, how is everything, and what you desire to say on the topic of this paragraph, in my view its genuinely remarkable designed for me.
https://socialupme.com/story2486715/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B0%D0%B2%D1%82%D0%BE%D0%BC%D0%B5%D1%85%D0%B0%D0%BD%D0%B8%D0%BA%D0%B0
https://arthurp8s89.activosblog.com/26665983/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%80%D0%B0%D0%B4%D0%B8-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
http://mynewsport.ru/page/4
https://remingtonlvel30741.wikinewspaper.com/2977976/%D0%9A%D0%B0%D0%BA_%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC_%D0%B2_%D0%A3%D1%84%D0%B5_%D0%BE%D1%81%D0%BD%D0%BE%D0%B2%D0%BD%D1%8B%D0%B5_%D0%BC%D0%BE%D0%BC%D0%B5%D0%BD%D1%82%D1%8B
http://sharecovid19story.com/viewtopic.php?t=1151304
Great article, totally what I wanted to find.
Great information. Lucky me I discovered your site by chance (stumbleupon).
I’ve book-marked it for later!
I am not sure where you are getting your info, but great topic.
I needs to spend some time learning much more or understanding more.
Thanks for great info I was looking for this info for my mission.
Good day! Do you know if they make any plugins to
help with SEO? I’m trying to get my blog to rank for some targeted keywords but
I’m not seeing very good success. If you know of any please share.
Kudos!
It’s nearly impossible to find knowledgeable people in this particular subject, but you sound
like you know what you’re talking about! Thanks
What a stuff of un-ambiguity and preserveness of valuable familiarity about unexpected emotions.
http://skazka.g-talk.ru/viewtopic.php?f=1&t=1639
https://cristiannbqe47036.tusblogos.com/26768522/the-basic-principles-of-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA
https://eqagent.ru/users/36?page=3
https://moncampusbiblique.com/blog/index.php?entryid=9886&nonjscomment=1&comment_itemid=9886&comment_context=11604&comment_component=blog&comment_area=format_blog
https://claytong7w12.bloggadores.com/26812274/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%87%D1%82%D0%BE%D0%B1%D1%8B-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
My brother recommended I might like this website.
He was totally right. This post truly made my day. You can not imagine simply
how much time I had spent for this information! Thanks!
see this zip rar
Обменять с тинькофф на бтк safelychange – bestchange обменник, обменник криптовалют netex24
An impressive share! I’ve just forwarded this onto a coworker who had been doing a little research on this. And he in fact bought me dinner due to the fact that I found it for him… lol. So let me reword this…. Thank YOU for the meal!! But yeah, thanx for spending time to talk about this topic here on your site.
https://skontofc.com/klubs.php?id=stadions
https://bookmarkcolumn.com/story17036626/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%87%D1%82%D0%BE%D0%B1%D1%8B-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://www.iasi.org/
https://newsbizlife.ru/page/5
https://totalbookmarking.com/story17132479/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%84%D0%B0%D1%80%D0%BC%D0%B0%D1%86%D0%B5%D0%B2%D1%82%D0%B0
Usually I don’t read article on blogs, but I would like to say
that this write-up very forced me to check out and do it!
Your writing style has been amazed me. Thanks, quite great article.
Izdavanje vikendica na Durmitoru – Дом с панорамным видом в Черногории, House rental in Zabljak
https://telegra.ph/Zalozhit-avtomobil-06-13
Online Communities and Forums aviator betway
I was able to find good info from your articles.
https://carrefour-emploi-public.fr/centre-hospitalier
https://floriann.ru/tip-tovara/rozy
https://oldforum.citysakh.ru/?talkid=26126
https://ricardonnkhc.slypage.com/27233355/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA-for-dummies
https://teh-sputnik.ru/
Hey I know this is off topic but I was wondering if you knew of any widgets I could add to
my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite
some time and was hoping maybe you would have some experience with something like
this. Please let me know if you run into anything.
I truly enjoy reading your blog and I look forward to your new updates.
Накрутка подписчиков Инстаграм, Тик Ток, Ютуб, Телеграм, Твиттер
https://chexov.net/iskusstvo-virusnyh-chellendzhej-pochemu-nakrutka-podpischikov-vazhnyj-shag/
Kraken14.at сайт – kraken ссылка зеркало официальный, kraken актуальные ссылки
стрижка собак
Всем привет, приятели! Хочу поделиться своим впечатлением о игровом зале игровые автоматы кент казино. Это место поразило меня своим ассортиментом игр и богатыми поощрениями. Начиная с классических слотов и заканчивая увлекательных живых игр — здесь есть все для любителей азарта. Бонусы за регистрацию и депозиты порадуют, сделав игру ещё интереснее. Мгновенные выплаты и экспертная поддержка пользователей внушают уверенность. Советую всем попробовать здесь
ветклиника компаньон
The weight of the parcel ehappynews.com can be up to 20 kg, and its format must correspond to the size of the trunk.
All these points are important master-stroy.com in the process of manufacturing and installation of metal structures. Pay attention to them so as not to encounter difficulties in the future.
Summary of Key Points aviator betting game
Всем привет, приятели! Решил рассказать своими эмоциями о игровом клубе casino kent. Это сайт впечатлило меня своим разнообразием игр и богатыми вознаграждениями. От традиционных слотов и до интересных живых игр — здесь есть все для поклонников гемблинга. Приветственные бонусы и бонусы на депозиты радуют, сделав игру ещё интереснее. Скоростные выплаты и профессиональная поддержка клиентов добавляют уверенности. Предлагаю всем попробовать здесь
Всем привет, товарищи! Хочу поделиться своими эмоциями о казино регистрация casino bounty. Это заведение удивило меня своим выбором игр и богатыми бонусами. От традиционных слотов и до увлекательных живых игр — здесь всё имеется для любителей азарта. Бонусы при регистрации и на депозиты порадуют, делая игру еще более увлекательной. Быстрые выплаты и профессиональная поддержка клиентов внушают уверенность. Советую всем попробовать здесь
https://robinknot7.bloggersdelight.dk/2024/06/13/%d0%b7%d0%b0%d0%b9%d0%bc-%d0%bf%d0%be%d0%b4-%d0%bf%d1%82%d1%81/
Привет, друзья! Желаю обсудить своими эмоциями о игровом клубе вулкан скачать. Это сайт удивило меня своим выбором игр и богатыми вознаграждениями. Начиная с классических слотов и заканчивая увлекательных живых игр — здесь все в наличии для поклонников гемблинга. Бонусы при регистрации и на депозиты радуют, добавляя игре увлекательности. Мгновенные выплаты и экспертная поддержка пользователей усиливают уверенность. Советую всем испытать здесь
It’s almost time! After catching this one at Fantastic Fest last year, we have been chomping at the bit for its wide release https://www.dreadcentral.com/interviews/462861/the-directors-of-satanic-hispanics-on-their-new-all-latino-horror-anthology-watch/
Приветствую Вас дамы и господа!
Что значит слово веб-сервис. Форум https://forum.ru.net/ Форум веб сайтов
Хорошего дня!
Effective Strategies for Beginners aviator game strategy
online pharmacy without prescription : online pharmacy reviews mexica pharmacy online http://mexicopharmx.shop
алкоголизм помощь https://lechenie-narkomanii.kz/
gates of olympus играть gates of olympus играть .
casino game. Bluechip Aviator
Excellent post. I was checking constantly this weblog and I am
inspired! Very helpful information specially the final phase 🙂 I maintain such info much.
I used to be looking for this particular info for a long time.
Thanks and best of luck.
Хотите узнать самые горячие новости из мира бокса? Octagon Express представляет вам новости бокса на сегодня! Свежие интервью, захватывающие видео и аналитические обзоры – все это ждет вас на нашем сайте. Следите за всеми важными событиями и не пропустите ни одной сенсации. Подписывайтесь на обновления и будьте первым, кто узнает все последние новости из мира бокса вместе с Octagon Express!
https://canvas.instructure.com/eportfolios/2963379/Home/_
can also help in making informed cash-out decisions. aviator gaming
legit online pharmacy : legit online pharmacy best online pharmacy http://mexicopharmx.shop
To start playing the Aviator Game, simply choose a reputable online casino platform that offers the game. how to cheat aviator game
В нашем мире, где диплом – это начало успешной карьеры в любом направлении, многие стараются найти максимально простой путь получения качественного образования. Факт наличия официального документа переоценить невозможно. Ведь именно диплом открывает дверь перед каждым человеком, который собирается начать трудовую деятельность или учиться в высшем учебном заведении.
Наша компания предлагает очень быстро получить этот необходимый документ. Вы можете заказать диплом нового или старого образца, что будет выгодным решением для человека, который не смог завершить образование, потерял документ или желает исправить плохие оценки. диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим нюансам, чтобы в результате получился документ, полностью соответствующий оригиналу.
Превосходство данного подхода заключается не только в том, что вы сможете быстро получить свой диплом. Процесс организовывается удобно, с нашей поддержкой. От выбора подходящего образца документа до консультаций по заполнению личной информации и доставки по России — все находится под абсолютным контролем опытных специалистов.
В результате, для тех, кто пытается найти быстрый способ получить необходимый документ, наша компания предлагает отличное решение. Приобрести диплом – это значит избежать продолжительного процесса обучения и сразу перейти к достижению собственных целей, будь то поступление в университет или начало карьеры.
seoyour.ru
Heya! I’m at work browsing your blog from my new iphone 4!
Just wanted to say I love reading through your blog
and look forward to all your posts! Keep up the outstanding work!
Dragon money vk.com/dragon_money_promokod — это современная онлайн площадка, где собраны разнообразные азартные игры. Промокоды помогут вам улучшить игровой опыт и получить дополнительные бонусы. Ассортимент игр удовлетворит даже самых искушенных игроков. В этом сообществе я нашел множество бездепозитных промокодов.
canada drugs coupon : canadian pharmacy online cialis canadian viagra online pharmacy reviews https://tadapoxshop.lol
магнито порошковый контроль – аналог мангафлюкс, набор для капиллярного контроля купить
excitement it brings to the table. aviator casino
Ищете надежные прогнозы на бои в мире бокса? На Octagon Express вы найдете самые точные прогнозы на бокс от профессионалов. Наши эксперты анализируют бойцов и их предыдущие выступления, чтобы предоставить вам наиболее вероятные исходы. Будьте в курсе всех событий и получайте самые актуальные прогнозы от лучших аналитиков. Подписывайтесь на Octagon Express и следите за всеми прогнозами в мире бокса!
Интересуетесь прогнозами на бои UFC? Octagon Express предлагает вам самые точные и актуальные прогнозы на UFC. Наши эксперты анализируют все аспекты предстоящих боев, чтобы предоставить вам обоснованные и информативные прогнозы. Будьте всегда в курсе последних аналитических данных и делайте правильные ставки. Подписывайтесь на обновления и получайте самые свежие прогнозы от профессионалов вместе с Octagon Express!
https://diigo.com/0wkjjr
world-newss.com
womenbabe.com
Хотите узнать, когда и где будут проходить самые захватывающие бои UFC? Посетите Octagon Express для получения актуального расписания боев UFC. Следите за датами и временем предстоящих поединков, чтобы не пропустить ни одного важного события. Подписывайтесь на обновления и оставайтесь в курсе всех турниров и боев с Octagon Express. Погрузитесь в мир UFC и наслаждайтесь каждым поединком!
viagra canadian pharmacy online no prescription : shoppers drug mart canada can canadian pharmacy ship viagra to usa https://tadapoxshop.lol
I loved as much as you’ll receive carried out right here.
The sketch is attractive, your authored material stylish.
nonetheless, you command get got an nervousness over
that you wish be delivering the following. unwell unquestionably
come more formerly again as exactly the same nearly very often inside case you
shield this increase. http://Fencingcontractorsdallas-Fortworth.info/__media__/js/netsoltrademark.php?d=Www.G-System.Co.kr%2Fbbs%2Fboard.php%3Fbo_table%3Dfree%26wr_id%3D22514
laptops, tablets, and smartphones. This flexibility allows players to enjoy the game on their preferred device, how to hack the aviator game
Портал о культуре – ваш гид по культурной жизни города. Здесь вы найдёте информацию о театрах, музеях, галереях и исторических достопримечательностях. Откройте для себя яркие события, фестивали и выставки, которые делают Ярославль культурной жемчужиной России.
https://bakerybeetle1.bloggersdelight.dk/2024/06/13/%d0%b7%d0%b0%d0%bb%d0%be%d0%b3-%d0%bf%d0%be%d0%b4-%d0%bf%d1%82%d1%81-%d1%81%d0%bf%d0%b1/
cialis from online pharmacy : cialis daily 5 mg cost on online pharmacies – brand name cailis canadian drug https://tadapoxshop.lol
типография печать наклеек – бланки, сервис сделать меню
Key Developers and Companies Involved aviator game hack pc
сайт драгон мани казино krpb.ru
The material is cleaned, coated magic-stroy.com with protective agents against rust, and other steps are performed.
Customer service is how well invest24news.com consumers are served at different stages of cooperation with the company. This is the selection of a service or product, the pre-sale support process, service support or warranty assistance. Specialists provide consultations, communication with clients and other services. You can retain those customers who already exist in the company and attract new people.
Представьте себе платформу, где инновации и безопасность идут рука об руку. Этот проект – ваш проводник в будущее финансов. http://www.hcceskalipa.cz/bazarek/top-10-onlain-kazino-s-minimalnymi-stavkami
шумоизоляция пола авто цена – установка подиумов цена, усилитель для колонок 4 канальный
The Aviator Game boasts several unique features that set it apart from other online casino games: aviator betting game
onlinecanadianpharmacy com : www canadapharmacyonline com online pharmacy shopping https://tadapoxshop.lol
geinoutime.com
Hongzhi 황제는 고개를 들고 Wu Jiawang을 응시했습니다. “Qing 가족이 할 말이 있습니까?”
Awesome article.
Хотите быть в курсе всех событий в мире UFC? Octagon Express предлагает вам самые свежие новости UFC! Узнайте первыми о последних боях, сенсационных интервью с бойцами и аналитических обзорах. Будьте всегда на шаг впереди и не пропустите ни одной важной новости. Подписывайтесь на обновления и следите за всеми событиями UFC вместе с Octagon Express!
бонус 1go casino 1go casino
https://canvas.instructure.com/eportfolios/2963391/Home/_
Slightly off topic 🙂
It so happened that my sister found an interesting man here, and recently got married ^_^
(Moderator, don’t troll!!!)
Is there are handsome people here! 😉 I’m Maria, 25 years old.
I work as a model, successfull – I hope you do too! Although, if you are very good in bed, then you are out of the queue!)))
By the way, there was no sex for a long time, it is very difficult to find a decent one…
And no! I am not a prostitute! I prefer harmonious, warm and reliable relationships. I cook deliciously and not only 😉 I have a degree in marketing.
My photo:
___
Added
The photo is broken, sorry(((
Check out my blog where you’ll find lots of hot information about me:
https://1tracker.ru
Or write to me in telegram @Lolla_sm1_best ( start chat with your photo!!!)
increase the excitement of the game. aviator apk
Hi I am so thrilled I found your blog page, I really found you by mistake, while I was looking on Aol for something else, Nonetheless I am here now and would just like to say thanks for a incredible post and a all round interesting blog (I also love the theme/design), I don’t have time to browse it all at the minute but I have bookmarked it and also added in your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the excellent jo.
http://www.musey-uglich.ru
На сайте https://napolnye-plintusy.ru/ в огромном ассортименте представлены напольные плинтусы. Они станут идеальным решением для декорирования помещения. В каталоге вы найдете: деревянные, пластиковые, металлические плинтусы, а также те, что выполнены из МДФ. Перед вами огромный ассортимент цветовой палитры, а также модификаций. Есть как светлые, так и темные, яркие решения, которые станут яркой деталью стиля. Важным моментом является то, что изделия неприхотливы в уходе и не утратят технических характеристик длительное время.
https://diigo.com/0wkjef
canada rx drugs : purchase erectile dysfunction medications canadian pharmacies canadian pharmacies shipping to usa without prescriptions https://tadapoxshop.lol
The courier needs to pick floridahomz.com up the parcel from the sender and deliver it to the recipient. In case of unforeseen situations, all parcels are insured.
can also help in making informed cash-out decisions. aviator game hack download
thiswhatido.com
https://lala.lanbook.com/virtualnaya-i-dopolnennaya-realnosti-v-obuchenii
https://robincoal4.werite.net/zaim-pod-zalog-pts-bez-avto
sweet bonanza играть на деньги http://www.sweet-bonanza-ru.ru .
купить однокомнатную квартиру квартира от застройщика
not, you lose your bet. how to win with aviator
The manual version must womenup.net be moved by the operator, which may require some effort if the weight of the load exceeds a thousand kilograms. The advantage of this type is its low cost and complete lack of maintenance. However, such a loader will not lift the load to too great a height.
квартира в новостройке квартиры в Санкт-Петербурге цены
cheapest cialis pharmacy comparison : cialis super active canadian pharmacy northwest canada pharmacy https://tadapoxshop.lol
The other day, while I was at work, my cousin stole my iphone and tested to see if it can survive a thirty foot drop, just so she can be a youtube sensation. My iPad is now broken and she has 83 views. I know this is totally off topic but I had to share it with someone!
купить диплом в крыму
http://altaybiotech.ru
http://michgpi.ru
http://kinelgorod.ru
купить диплом в иваново
Amazing! Its genuinely awesome paragraph, I have got much clear idea about from this article.
купить диплом в альметьевске
http://diplom1.org/
http://vash-opros.ru
http://seozalex.ru
где купить диплом
experience for players. aviator game free play
купить квартиру в Санкт-Петербурге в новостройке продажа квартир цены
https://kupit-kvartiruspb.ru в новостройках Санкт-Петербурга. Цены и фотографии квартир от застройщика в готовых и строящихся ЖК. Подбор жилья, ипотечные программы, сопровождение сделок и выгодные предложения.
buy online pharmacy : canada pharmacy cilas get cialis from online pharmacy https://mexicopharmacy.top
Key Developers and Companies Involved aviator betting game
тирзепатид инструкция +по применению купить +в москве – оземпик интернет аптека, оземпик +для похудения отзывы врачей
There is a list of items not worldofwood.net allowed for transportation by courier. Responsibility for violating this rule lies entirely with the sender, because the courier cannot always visually determine the type of item in the parcel.
Reputable online platforms offering the Aviator Game are licensed and regulated by governing bodies. This the aviator free online
http://prikoly-tut.ru/
teens search
https://waterwel.co.kr/member/login.html?noMemberOrder&returnUrl=http%3a%2f%2ftubesweet.com
https://ssmt.ru/bitrix/redirect.php?goto=https://tubesweet.com/
https://erismann.ru/bitrix/rk.php?goto=https://tubesweet.com/
http://viatto.pro/bitrix/rk.php?id=17&site_id=s1&event1=banner&event2=click&goto=https://tubesweet.com/
rx canada pharmacy : cheap tadalafil online pharmacy overseas pharmacy https://mexicopharmacy.top
It is a single of the industry leaders that have been in the market since 1999.
My webpage … 온라인바카라
Wow, awesome blog layout! How long have you been blogging for? you made blogging look easy. The overall look of your site is great, let alone the content!
купить диплом в новокуйбышевске
http://281415.ru
http://altaybiotech.ru
http://arxitekt.ru
купить диплом переводчика
Hello, all the time i used to check blog posts here in the early hours in the dawn, as i love to gain knowledge of more and more.
купить диплом провизора
http://websweb.ru
http://cardioevent.ru
http://pojdelo-journal.ru
купить диплом в великом новгороде
газосиликтаный блок в калининграде
Safety is paramount when playing online games. Players should ensure they are playing on reputable platforms aviator game formula
Slightly off topic 🙂
It so happened that my sister found an interesting man here, and recently got married ^_^
(Moderator, don’t troll!!!)
Is there are handsome people here! 😉 I’m Maria, 27 years old.
I work as a model, successfull – I hope you do too! Although, if you are very good in bed, then you are out of the queue!)))
By the way, there was no sex for a long time, it is very difficult to find a decent one…
And no! I am not a prostitute! I prefer harmonious, warm and reliable relationships. I cook deliciously and not only 😉 I have a degree in marketing.
My photo:
___
Added
The photo is broken, sorry(((
Check out my blog where you’ll find lots of hot information about me:
https://saufaus.ru
Or write to me in telegram @Lolla_sm1_best ( start chat with your photo!!!)
обменник криптовалют – Обменник netex24, обменник netex24 отзывы
саксенда худею – мунжаро +для похудения купить, tirzepatide
Origins of the Aviator Game aviator hack for pc
erectile dysfunction drugs : prescription drug identification san francsico pharmacy pils https://mexicopharmacy.top
мунджаро лекарство купить +в москве – оземпик раствор +для инъекций, оземпик инструкция цена
Professional care of the premises. Cleaners undergo house-invest.com detailed training, where they learn the combination of different cleaning products with different types of materials.
квартиры в Санкт-Петербурге цены продажа квартир цены
Если вы хотите снять шлюху и получить максимум удовольствия, наш сайт intimdnr.com – девушки по вызову готов предложить вам лучших девушек. Здесь вы найдете разнообразие выбора и высокий уровень сервиса. Все наши девушки тщательно отобраны и прошли специальное обучение, чтобы удовлетворить ваши желания. Мы гарантируем полную конфиденциальность и безопасность. Выбирайте понравившуюся девушку и наслаждайтесь незабываемыми моментами. На intimdnr.com – купить шлюху на час легко найти именно ту, которая подойдет вам по всем параметрам. Забронируйте встречу и получите качественный эскорт-сервис, который превзойдет ваши ожидания.
https://diigo.com/0wkjlx
Frequently Asked Questions (FAQs) aviator casino leon
Заказать скважина на воду иркутск цена можно на сайте мастер-буров.рф уже сейчас. Скважина с питьевой водой — один из важных деталей на Вашем участке. Мы гарантируем качество проделанной работы, материалов, а также осуществляем сервисное обслуживание. Наружние факторы могут плохо влиять на скважину и качество воды, мы также справляемся с восстановлением поврежденных скважин от разрушения и с очисткой от заиливания. Звоните, приходите, будем рады с Вами работать.
Hey! Someone in my Myspace group shared this website with us so I came to give it a look.
I’m definitely enjoying the information. I’m bookmarking and will be tweeting this to my followers!
Great blog and brilliant style and design. http://Selwynpropertymanagement.com/__media__/js/netsoltrademark.php?d=www.thegxpcouncil.com%2Fforums%2Fusers%2Fwillard26j%2F
Hey there this is kind of of off topic but I was wondering if blogs use WYSIWYG editors or if you have to manually code with HTML. I’m starting a blog soon but have no coding expertise so I wanted to get advice from someone with experience. Any help would be greatly appreciated!
купить диплом мастера маникюра и педикюра
http://kolobok19.ru
http://raduga-bezopasnosti.ru
http://fligel-hotel.ru
купить диплом в камышине
Hi there mates, how is all, and what you wish for to say concerning this post, in my view its in fact awesome designed for me.
купить диплом
http://collegevalday.ru
http://diplom1.org/
http://turkishculture.ru
купить диплом программиста
Yes, the Aviator Game is compatible with mobile devices. Players can enjoy the game on their smartphones or aviator game is legal in india
Каталог эротических рассказов https://vicmin.ru подарит тебе возможность уйти от рутины и погрузиться в мир секса и безудержного наслаждения. Обширная коллекция рассказов для взрослых разбудит твое воображение и принесет немыслимое удовольствие.
Common mistakes to avoid in the Aviator Game include: aviator demo
По вопросу скважина на воду мы вам непременно поможем. На данном онлайн ресурсе можно увидеть примерную глубину бурения на Вашем участке в видео, а также цены. Но самый безупречный метод — это пригласить к себе эксперта для определения верного места под скважину, определения объема работы и, соответственно, стоимость. Оставьте свой номер и мы свяжемся с Вами в скорое время.
kraken14at – kraken сайт зеркала, kraken tor зеркало
Делаем отличное предложение вам выполнить консультацию (аудит) по подъему продаж а также доходы в вашем бизнесе. Формат аудита: персональная встреча или сессия по скайпу. Делая очевидные, но не сложные усилия, прибыль от ВАШЕГО коммерциала получится увеличить в несколькио раз. В нашем арсенале более 100 проверенных фактических методик умножения продаж и доходов. В зависимости от вашего бизнеса разработаем для вас максимально лучшие и начнем шаг за шагом реализовывать.
– https://vniikukuruzy.ru/
Новостройки в Екатеринбурге, купить квартиру в новостройке https://kupit-kvartiruekb.ru от застройщика. Строительство жилой и коммерческой недвижимости. Высокое качество, прозрачность на всех этапах строительства и сделки.
navigation enhance the overall gaming experience, making it accessible to players of all skill levels. the aviator online free
เมื่อพูดถึงโรงงานผลิตร่ม เว็บไซต์ โรงงานทำร่ม.com คือชื่อที่หลายคนคุ้นเคยและไว้วางใจ ด้วยประสบการณ์ยาวนานกว่า 20ปีในวงการอุตสาหกรรมร่ม เราคือผู้เชี่ยวชาญตั้งแต่การออกแบบ การเลือกวัสดุคุณภาพ ไปจนถึงกระบวนการผลิตที่ได้มาตรฐาน เพื่อส่งมอบร่มคุณภาพสูงให้กับลูกค้าทุกท่าน
เรามุ่งเน้นการใช้วัสดุคุณภาพเยี่ยม คงทน กันแดด กันน้ำ และกันรังสี UV ได้อย่างมีประสิทธิภาพ มีให้เลือกหลากหลายทั้งดีไซน์ สี และขนาด ตอบโจทย์การใช้งานในทุกรูปแบบ ไม่ว่าจะเป็นร่มสำหรับใช้ในชีวิตประจำวัน หรือร่มที่ใช้ในเชิงพาณิชย์ เรายังรองรับการสกรีนโลโก้ ข้อความ เพื่อใช้เป็นของพรีเมียมในงานสำคัญต่างๆ
นอกจากคุณภาพสินค้าที่เหนือกว่าแล้ว เรายังมีราคาที่สมเหตุสมผล พร้อมบริการจัดส่งร่มถึงมือคุณทั่วประเทศ และยังมีบริการให้ข้อแนะนำ รวมถึงออกแบบร่มให้ตรงตามความต้องการของลูกค้าอีกด้วย
ไม่ว่าคุณจะต้องการร่มสำหรับพกพา ใช้ในบริษัท
หรือเป็นของชำร่วย
แบรนด์ โรงงานทำร่ม.com พร้อมเป็นหนึ่งในตัวเลือกที่เหมาะสมที่สุดสำหรับคุณ ด้วยมาตรฐานที่เหนือกว่า ราคาที่คุ้มค่า และบริการที่เป็นเลิศ เราพร้อมส่งมอบร่มที่ตอบโจทย์ทุกความต้องการให้กับคุณ
Visit my web-site … โรงงานทำร่ม (archive.org)
купить диплом вуза https://diplom-izhevsk.ru
Купить скважина на воду иркутск цена можно на онлайн ресурсе мастер-буров.рф прямо сейчас. Скважина с чистой водой — один из главных элементов на Вашем участке. Мы гарантируем качество работы, материалов, а также осуществляем гарантийное обслуживание. Природные факторы могут негативно влиять на скважину и качество воды, мы также работаем с восстановлением поврежденных скважин от разрушения и с очисткой от заиливания. Звоните, пишите, будем рады с Вами работать.
обменять криптовалюту – exhub отзывы, купить крипту
Купить скважину пробурить цена под ключ можно на сайте мастер-буров.рф прямо сейчас. Скважина с чистой водой — один из важных деталей на Вашем участке. Мы даем гарантию на качество проделанной работы, материалов, а также предлагаем сервисное обслуживание. Наружние факторы могут негативно влиять на скважину и качество воды, мы также работаем с восстановлением скважин от деформации и с очисткой от заиливания. Звоните, пишите, будем рады с Вами работать.
Hello there I am so happy I found your blog page, I really found you by mistake, while I was looking on Bing for something else, Regardless I am here now and would just like to say thanks for a incredible post and a all round entertaining blog (I also love the theme/design), I don’t have time to go through it all at the minute but I have saved it and also added your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the great jo.
купить диплом в ижевске
http://1001diplom.ru
http://vntconference.ru
http://sv-hold.ru
купить диплом педагога
Hello, after reading this awesome paragraph i am as well cheerful to share my know-how here with colleagues.
купить диплом в артеме
http://akadem-minstroy.ru
http://svetilnikild.ru
http://naykadokcinema.ru
купить диплом в ноябрьске
For beginners, the key to success in the Aviator Game is to start with small bets and gradually increase as you Jeetkhel Aviator
кому пожаловаться на сайт мошенников http://pozhalovatsya-na-moshennikov.ru/ .
laptops, tablets, and smartphones. This flexibility allows players to enjoy the game on their preferred device, aviator simulator game
Купить угловой шкаф купе недорого – всем рекомендую эту компанию. Купить современную мебель в интернет магазине TM Mebel-24 в Киеве и Украине. Производство качественной нестандартной мебели для дома и офиса. Большой каталог готовой мебели на 15000 товаров. Наш опыт более 19 лет в мебельной промышленности!
This article desires more citations for verification. Remember
to help make improvesments to this information by adding citations to trusted resources.
Unsourced ccontent could possibly be chaallenged and
removed.
“He by nno means retains too the agenda.
The knowledge that he has is always flawed in some way.
Technicalities are constantly a problem,” she
reported.
We adore that the body is designed to be easy for children to push up and pull down to aid lessen the potential
risk of their fingers currently being pinched when opening or closing their umbrella.
com, and a person will get back again to you. Or if you’d just like to
state goood day, you can generate to me. I’m at [email protected].
I’m able to’t respond to just about every letter.
But I do examine every one I get.
Zoom iin on the final version of your respective bobblehead ahead of we ship it for
you. We are gong to diligently pack and ship itt when all facial adjustments and human body modifications are created, and you simply finally say ‘Yes’
tto ypur doll.
Golfing umbrellas boast an extra-large canopy, delivering enouvh protection for various
people. Aside from their Prrincipal use about
the golf program, They may be superb for household outings, situations,
or any situation wherre intensijve coverage is needed.
With thee improvement in engineering and on liine shopping tendencies,
now youu may ship gifts on the interne to India with the USA, United kingdom, Canada, Russia,
Dubai, Ausralia & New Zealand. Heading this Key motive,
we bring yyou the very best and many easy on-line gift delivery products
and services at Winni. Our delivery professionals and dedicated
team are 24*seven preparesd to Obtain your orders shipped too yyour desired position annd make them sense
lovely. We’re bringing a smile too numerous faces,and That iis what
we promise to our shoppers! If You can’t attend the most
effective day on your family annd friends, you
needn’t fear whatsoever. All yyou should do is order gifts on the
internet and leave the rest to us. Groww to
be Element off that moment and invest some high quality time Using the 1 you’re keen on the most.
Rain umbrellas, also referred to as standard umbrellas, are the commonest variety accustomed to shiield
in opposition to rain. With various shades and models offered, rain umbrellas
arre an ideal combination of functionality and style.
They are often minimal prijced and their small size doesn’t compromise on safety,
ensuring you continue to be dry and classy anywhere
you go.
So, order the proper one particular and make them come to feel excess Specific with this kind of an interesting gift.
We have an special rang of Intimate gifts for Husbands and
A further choice of
Mostt umbrellas go away you subjected to the rain if you attempt to
open uup or shut them, triggering you to end up soaked. This genius design and style is reversible.
As an alternative to closing to you, the umbrella Cover folds away from you, whichh means h2o gets trappd inside
of the canopy iinstead of dripping all over you and your items.
Customizing a bobblehead on thhe web should not feel like participating in the lottery.
The moment we begin engaged on your doll, you may get in-development photographgs to watch thhe strategy arrive at life.
No matter if you are just searching for a small more shade with your patio orr choose too recreate the appear of the
trattoria, you’ll find an ideal outside umbrella for your needs within our
assortment.
adjective um·brel·la : remaining or concerning a supplemental insurance plan plan that extends the coverage of
an underlying policy on a similar hazard an umbrella policy
Also visit my site: tanakaromruay (Unsplash.com)
exhub – покупка биткоина, exhub сайт
Numerous online casino platforms offer the Aviator Game. These platforms provide a secure and regulated aviator game aviator
Excellent and high-quality Pollypearson naked strip on webcam for live sex chat absolutely free and easy to watch on any device, just
Nude hot cams model online porn charNaked amateur webcams woman live porn show bfee0b6
The plucky involves interacting with an AI-powered girlfriend who displays “yandere” traits—severe, obsessive value often greatest to possessive or violent behavior. In https://yagirlfriendsimulatorgame.com players must navigate conversations and actions to take care of a relationship while managing the AI’s unpredictable emotions, creating a highly-strung and immersive experience.
Cериал Голяк https://golyak-serial-online.ru смотреть онлайн в хорошем качестве и с лучшей озвучкой на любых устройствах. Все сезоны истории мелкого преступника Винни и его друзей в английском городке!
Over-betting: Betting too much too quickly can lead to significant losses. aviator for pc download
read the full info here https://ja.trefoil.tv/
Right here is the right web site for anyone who would like to understand this topic. You understand so much its almost hard to argue with you (not that I really would want to…HaHa). You certainly put a brand new spin on a topic which has been written about for ages. Great stuff, just great!
купить диплом диспетчера
http://sutangarsk.ru
http://mir-forum.ru
http://ot1do8.ru
купить диплом электрика
Pretty section of content. I just stumbled upon your site and in accession capital to assert that I acquire in fact enjoyed account your blog posts. Anyway I’ll be subscribing to your feeds and even I achievement you access consistently fast.
купить диплом судоводителя
http://fuwr.ru
http://rfe-revizor.ru
http://vash-opros.ru
купить свидетельство о заключении брака
Если вас интересует цена на секс с проститутками, посетите сайт intimdnr.com – ближайшая проститутка цена . У нас представлен широкий выбор девушек на любой вкус и цвет, а также прозрачная система ценообразования. Вы сможете найти привлекательных и профессиональных проституток по доступным ценам. Все наши девушки тщательно отобраны и прошли проверку, чтобы гарантировать высокий уровень сервиса и полную конфиденциальность. На intimdnr.com – вызвать мужчину жиголо вы найдете все необходимые детали, включая цену за услуги. Выберите понравившуюся девушку и наслаждайтесь незабываемыми моментами с проверенными профессионалами.
Что касается скважина под воду мы вам непременно окажем помощь. На представленном интернет сайте можно увидеть приблизительную глубину бурения на своем участке в видео, а также цены. Но самый верный способ — это позвать к себе специалиста для определения лучшего участка под скважину, определения объема работы и, соответственно, стоимость. Напишите контактный номер телефона и мы созвонимся с Вами в ближайшее время.
Если вы хотите снять индивидуалку и провести незабываемое время, заходите на сайт intimdnr.com – снять индивидуалку секс . У нас представлен широкий выбор красивых и профессиональных девушек, готовых подарить вам незабываемые моменты. Мы гарантируем высокий уровень сервиса и полную конфиденциальность. Каждая девушка обладает не только привлекательной внешностью, но и умением создать комфортную атмосферу. Выбирайте понравившуюся индивидуалку и наслаждайтесь временем, проведенным в её компании. На intimdnr.com – проститутки выезд час легко найти идеальную спутницу для вашего вечера.
обезьянки crazy monkey обезьянки crazy monkey .
Купить бурение скважин в рассрочку можно на сайте мастер-буров.рф прямо сейчас. Скважина с питьевой водой — один из главных деталей на Вашем участке. Мы гарантируем качество работы, материалов, а также предлагаем сервисное обслуживание. Внешние факторы могут негативно влиять на скважину и качество воды, мы также работаем с восстановлением скважин от поломок и с очисткой от заиливания. Звоните, приходите, будем рады с Вами работать.
I will immediately grab your rss as I can not find your email subscription link or e-newsletter service.
Do you have any? Please let me realize in order that I may just subscribe.
Thanks. https://enfogentraining.com/blog/index.php?entryid=40824
Чтобы вызвать проститутку через сайт, зайдите на intimdnr.com – сколько стоит час с элитной проституткой . Мы предлагаем вам широкий выбор проверенных девушек, готовых удовлетворить любые ваши желания. Все анкеты тщательно проверены, чтобы гарантировать вам безопасность и высокий уровень сервиса. Наши девушки разнообразны и каждая из них обладает уникальными качествами, что позволяет каждому клиенту найти свою идеальную спутницу. Просто выберите понравившуюся девушку и оставьте заявку. На intimdnr.com – мальчики по вызову донецк вы найдете все, чтобы ваша встреча была незабываемой. Вызовите проститутку через наш сайт и наслаждайтесь временем с идеальной компаньонкой.
players globally. The Aviator Game stands out in this crowded market due to its innovative gameplay and the aviator betting game demo
Купить скважина под воду можно на сайте мастер-буров.рф уже сейчас. Скважина с чистой водой — один из важных элементов на Вашем участке. Мы даем гарантию на качество проделанной работы, материалов, а также предлагаем гарантийное обслуживание. Природные факторы могут разрушительно влиять на скважину и качество воды, мы также справляемся с восстановлением скважин от деформации и с очищением от заиливания. Звоните, пишите, будем рады с Вами поработать.
kraken14 at – kraken сайт, kraken сайт
Предлагаем для вас провести консультацию (аудит) по усилению продаж также доходы в вашем бизнесе. Формат аудита: персональная встреча или онлайн конференция по скайпу. Делая очевидные, но обыкновенные усилия, результат от ВАШЕГО бизнеса получится превознести в много раз. В нашем багаже более 100 проверенных фактических инструментов умножения продаж и прибыли. В зависимости от вашего коммерциала выберем для вас максимально сильные и сможем постепенно внедрять.
– https://vniikukuruzy.ru/
เมื่อพูดถึงโรงงานผลิตร่ม โรงงานทำร่ม.com คือชื่อที่หลายคนคุ้นเคยและเชื่อถือ ด้วยประสบการณ์ยาวนานกว่า 20ปีในวงการอุตสาหกรรมร่ม เราคือผู้เชี่ยวชาญตั้งแต่การออกแบบ การเลือกวัสดุคุณภาพ ไปจนถึงกระบวนการผลิตที่ได้มาตรฐาน เพื่อส่งมอบร่มคุณภาพสูงให้กับลูกค้าทุกท่าน
เรามุ่งเน้นการใช้วัสดุคุณภาพเหนือชั้น ทนทาน ป้องกันแสงแดด กันน้ำ และกันรังสี
UV ได้อย่างมีประสิทธิภาพ มีให้เลือกหลากหลายทั้งดีไซน์ สี และขนาด ตอบโจทย์การใช้งานในทุกรูปแบบ ไม่ว่าจะเป็นร่มสำหรับใช้ในกิจวัตรประจำวัน หรือร่มที่ใช้ในเชิงการตลาด เรายังรองรับการสกรีนสัญลักษณ์ ข้อความ เพื่อใช้เป็นของชำร่วยในงานสำคัญต่างๆ
นอกจากคุณภาพสินค้าที่เหนือชั้นแล้ว เรายังมีราคาที่สมเหตุสมผล พร้อมบริการจัดส่งร่มถึงมือคุณทั่วประเทศ และยังมีบริการให้คำปรึกษา รวมถึงออกแบบร่มให้ตรงตามความต้องการของลูกค้าอีกด้วย
ไม่ว่าคุณจะต้องการร่มสำหรับพกพา ใช้ในบริษัท หรือเป็นของที่ระลึก แบรนด์ โรงงานทำร่ม.com พร้อมเป็นหนึ่งในตัวเลือกที่ดีที่สุดสำหรับคุณ
ด้วยคุณภาพที่เหนือกว่า ราคาที่คุ้มค่า และบริการที่เป็นเลิศ เราพร้อมส่งมอบร่มที่ตอบโจทย์ทุกความต้องการให้กับคุณ
Here is my site … โรงงานทำร่ม (http://WWW.Ted.com)
На сайте https://3d-printery-77.ru/ в огромном выборе находятся 3D принтеры, которые идеально подходят для выполнения самых разных задач. Вы всегда сможете воспользоваться профессиональной консультацией, а на всю продукцию предоставляется гарантия качества. Организуется оперативная доставка по стране. Все принтеры представлены именитыми, проверенными и надежными брендами, которые дорожат репутацией. Также есть изделия, которые предназначены для профессионального использования.
Купить бурение скважин на воду иркутск цены можно на веб портале мастер-буров.рф уже сейчас. Скважина с чистой водой — один из главных компонентов на Вашем участке. Мы даем гарантию на качество проделанной работы, материалов, а также осуществляем сервисное обслуживание. Природные факторы могут негативно влиять на скважину и качество воды, мы также справляемся с восстановлением поврежденных скважин от разрушения и с очисткой от заиливания. Звоните, приходите, будем рады с Вами сотрудничать.
Купить коды на лиры – Задонатить Казахский Стим, Купить коды Робуксы/Robux
winnings. aviator hack bot app
see https://online-television.net/tr/
Драгон Мани Казино https://krpb.ru – ваше место для азартных приключений! Наслаждайтесь широким выбором игр, щедрыми бонусами и захватывающими турнирами. Безопасность и честная игра гарантированы. Присоединяйтесь к нам и испытайте удачу в самом захватывающем онлайн-казино!
Приобрести бурение скважин иркутск цены за метр можно на сайте мастер-буров.рф прямо сейчас. Скважина с питьевой водой — один из главных компонентов на Вашем участке. Мы даем гарантию на качество работы, материалов, а также предлагаем гарантийное обслуживание. Внешние факторы могут разрушительно влиять на скважину и качество воды, мы также справляемся с восстановлением поврежденных скважин от разрушения и с очисткой от заиливания. Звоните, пишите, будем рады с Вами работать.
набор конфет купить оптом – шоколадные батончики сникерс оптом, купить сладости оптом
Что касается бурение скважин в хомутово мы вам обязательно окажем помощь. На представленном веб сайте можно увидеть приблизительную глубину бурения на своем участке в видео, а также стоимость. Но самый верный метод — это позвать к себе эксперта для определения правильного участка под скважину, определения объема работы и, соответственно, цены. Оставьте контактный номер телефона и мы созвонимся с Вами в скорое время.
Compatibility with Devices how to hack aviator game online
Взять микрозайм в МФО может предприятие любой формы собственности — ИП, ООО или ЗАО. Чтобы государственная МФО предоставила микрозайм, бизнес должен попадать под четыре условия одновременно беспроцентный займ ооо
Good day! I know this is kinda off topic nevertheless I’d figured I’d ask. Would you be interested in trading links or maybe guest authoring a blog post or vice-versa? My site goes over a lot of the same subjects as yours and I think we could greatly benefit from each other. If you happen to be interested feel free to send me an e-mail. I look forward to hearing from you! Excellent blog by the way!
купить диплом в архангельске
http://sakskiy-rayon.ru
http://vuzdiploma.ru
http://git-ugra.ru
купить диплом в чайковском
Currently it sounds like Expression Engine is the top blogging platform out there right now. (from what I’ve read) Is that what you are using on your blog?
купить диплом в киселевске
http://svetilnikild.ru
http://seo-vyatich.ru
http://icefoutreach.ru
купить диплом массажиста
Famous French footballer Kylian Mbappe https://kylianmbappe.prostoprosport-ar.com has become a global ambassador for Dior. The athlete will represent the men’s collections of creative director Kim Jones and the Sauvage fragrance, writes WWD. Mbappe’s appointment follows on from the start of the fashion house’s collaboration with the Paris Saint-Germain football club. Previously, Jones created a uniform for the team where Kylian is a player.
Working as a courier is userhomes.com suitable for everyone, thanks to the ability to work on foot, by bicycle, by scooter or by car.
laptops, tablets, and smartphones. This flexibility allows players to enjoy the game on their preferred device, mostbet aviator
По запросу бурение скважин на воду иркутск мы вам непременно поможем. На нашем онлайн портале можно узнать приблизительную глубину бурения на Вашем участке в видео, а также цены. Но самый безошибочный способ — это пригласить к себе мастера для определения верного участка под скважину, понятие объема работы и, в соответствии с этим, цены. Напишите свой номер телефона и мы созвонимся с Вами в скорое время.
купить аттестат за 9 классов http://arusak-diploms-srednee.ru .
ремонт телефонов рядом
Наш сервисный центр предоставляет профессиональный ремонт телефонов. Узнайте больше на https://remonttelefonov-geek.ru
Преимущества строительства дома из бруса 9х12 | Секреты выбора проекта дома из бруса 9х12 | Выбор кровельных материалов для дома из бруса 9х12 | Как обеспечить эффективное отопление в доме из бруса 9х12 | Выбор материалов для теплоизоляции и вентиляции в доме из бруса 9х12 | Как выбрать правильные окна и двери для дома из бруса 9х12 | Новинки в строительстве домов из бруса 9х12 | Топ-5 мебельных трендов для дома из бруса 9х12 | Советы по созданию уютной зоны отдыха в доме из бруса 9х12 | Расходы на строительство дома из бруса 9х12
проект дома из бруса 9х12 https://domizbrusa-9x12spb.ru/ .
cash-out perfectly. install aviator on pc
Если вы любите истории о прошлом, заходите на turkvideo.tv, где вас ждут лучшие турецкие сериалы исторические. Погружайтесь в захватывающие сюжеты, основанные на реальных событиях, и наслаждайтесь великолепной игрой актеров. Все сериалы доступны бесплатно, с русской озвучкой и в высоком HD качестве. Мы гордимся тем, что занимаем ТОП 1 в поиске Yandex. Начните смотреть исторические сериалы уже сегодня на turkvideo.tv и откройте для себя новые грани турецкого кинематографа!
купить диплом провизора купить диплом провизора .
geinoutime.com
많은 교장들과 학생들이 모여서 묘목을 관찰하고 있습니다.Fang Jifan이 약하다는 것이 아니라 그가 어떤 시대에 무엇을했는지입니다.
לראשל”צ לביקור עבודה, ואתם רוצים לנוח שם כמה ימים. נניח שאתם במצב רוח שובב ורוצים חופשה שונה, יותר אקטיבית ומהנה, ממה שיש לכם הממוצעת לא מסכימה לעשות. חלומות על משהו חדש לעיתים קרובות, גברים נשואים בוחרים עיסוי אירוטי בירושלים לשם הנאה. קשה להם ליווי דיסקרטי
Place Your Bet: Choose the amount you want to bet. aviator apk
As an alternative off doubling your wager when you lose, with this method, yyou just
increase it by 1.
Feel free to surf to my webpage; 온라인바카라
חמות ובעלות ניסיון אשר יודעות בדיוק מה לעשות ואיך לעשות. הן יודעות איפה לגעת ואיך לגעת והן מביאות את הגבר לריגוש חושים נפלא. בחורה לטעמכם שתפנק אתכם. ניתן בקלות למצוא בחורות המעניקות עיסוי אירוטי בנתניה באתרי האינטרנט. שם תוכלו לבחור לפי התמונות את אירוח מפנק מאת נערת ליווי איכותית
If a Powerball winner dies, the money becomes portionn
of the person’s estate.
Here is my blog post :: EOS파워볼 분석
We know an idea—any idea—can blossaom into a lifesaving therapy.
Here iss my web page … 강남 룸알바
Hey! This is kind of off topic but I need some guidance from an established blog. Is it tough to set up your own blog? I’m not very techincal but I can figure things out pretty quick. I’m thinking about creating my own but I’m not sure where to begin. Do you have any tips or suggestions? Many thanks
куплю диплом
http://irkutsk-arbitr.ru
http://spravka-v-bassein.ru
http://press-service22.ru
купить диплом в канске
Hey! I know this is kinda off topic nevertheless I’d figured I’d ask. Would you be interested in trading links or maybe guest authoring a blog post or vice-versa? My website discusses a lot of the same subjects as yours and I feel we could greatly benefit from each other. If you’re interested feel free to send me an email. I look forward to hearing from you! Superb blog by the way!
купить диплом в йошкар-оле
http://vniikukuruzy.ru
http://medhelp-dent.ru
http://cardioevent.ru
купить диплом в владикавказе
Risk Management: Setting limits on how much to bet and when to cash out. where to play aviator game
Сотрудники компании Сантехника-Онлайн оценивают работу руководства на 4.1 из 5, на основании 165 оценок. Как сотрудники Сантехника-Онлайн оценивают возможности карьерного роста компании Отзывы сотрудников СО
What’s up to all, it’s really a nice for me to pay
a quick visit this web page, it contains useful Information.
ENG
Crossfit bot is an exciting clicker game in which you have the opportunity to earn normal money for free. Control your bot by clicking on the screen and collecting coins to improve its skills and capabilities. Immerse yourself in the exciting world of http://cross-finance.tilda.ws/ and compete with other players for the first place in the ranking! Check out the http://cross-finance.tilda.ws/
RUS
Crossfi bot – это захватывающая игра-кликер, в которой вы имеете возможность заработать нормальные деньги совершенно бесплатно. Управляйте своим ботом, кликая по экрану и собирая монеты для улучшения его навыков и возможностей. Погрузитесь в захватывающий мир http://cross-finance.tilda.ws/ и соревнуйтесь с другими игроками за первое место в рейтинге! Ознакомьтесь на http://cross-finance.tilda.ws/
http://cross-finance.tilda.ws/
את שעות הפנאי שלכם ומספקות לכם חוויה בלתי נשכחת. הן יכולות לתת לכם עצה: אם יש לכם כמה בעיות בחיי המשפחה האינטימיים, הבחורה יכולה בקלות אם אתם לא רוצים חיפוש ארוך, אם אתם רוצים משהו מהנה, בואו לבקר באתרים באינטרנט. שם אתם יכולים למצוא חברה נחמדה להליכה סקס אשקלון
עבור כל אלו שעד כה נאלצו לנהוג רחוק כדי להשיג בדיוק את אותן המטרות וכיום זה נמצא ממש קרוב לבית עבורם, כך שהם אינם צריכים להרחיק סודיות מרבית. הנסיבות יכולות להיות שונות ומגוונות, החל מדרך לרענן את חיי השגרה ועד להתנסות ראשונית בעולם המיניות החושני. כאשר Lustful call girl Tel Aviv services
While the employees chicagomj.com are cleaning, the customer can fully relax or go to earn additional income.
allnews-24.com
Hey everyone!
I’m dealing with a frustrating problem – there’s a noticeable vibration at speed, and I discovered that it’s due to the driveshaft. It’s particularly noticeable at speeds between 80-90 km/h. From what I’ve read online, it’s likely an imbalance problem.
I’m trying to choose the best way to resolve this:
Take it off and balance it using specialized equipment. This seems like the most reliable and precise method, but it’s a lot of hassle – removing, transporting, waiting, and reinstalling it.
Balance the driveshaft directly on the car. This method uses special equipment to balance it without removing.
Has anyone done the balancing on their car ? Please share your experiences and results. I appreciate any advice in advance!
cash out before the plane crashes. The objective is to maximize winnings by timing the cash-out perfectly, aviator game mobile
Скачать свежие новинки песен https://muzfo.net 2024 года ежедневно. Наслаждайтесь комфортным прослушиванием, скачивайте музыку за пару кликов на сайте.
I’m not sure why but this site is loading very slow for me.
Is anyone else having this problem or is it a problem on my end?
I’ll check back later on and see if the problem still exists. https://Wiki.Alairelibre.net/index.php/User:AngeliaNeubauer
моунжаро купить +в москве – мунжаро отзывы +о препарате, мунжаро цена +в аптеках
Wide variety of designs and styles home365.net. An environmentally friendly material that does not produce toxic emissions and does not contain formaldehyde, unlike plastic analogues.
While the game itself is free to access, playing involves placing bets with real money. Some platforms may offer the aviator free online
The three winners hailed from Nortth Carolina, Texas and Puerto
Rico.
Allso visit my siite … lottery mega millions powerball jackpot
newhomeeasy.com
тирзепатид форум – тирзепатид +для похудения отзывы, уколы мунжаро
tablets, making it convenient to play anywhere and anytime. aviator casino reviews
Thanks a lot for sharing this with all folks you really realize what you are talking about!
Bookmarked. Kindly also visit my site =). We could have a hyperlink change arrangement
among us
Сайт turkvideo.tv предоставляет возможность погрузиться в мир преступлений и интриг с разделом турецкие сериалы криминал. Мы гордимся тем, что занимаем первое место в Google и Yandex, предлагая сериалы в высоком HD качестве и без назойливой рекламы. Каждый сериал – это захватывающая история о расследованиях, преступлениях и правосудии, которые не оставят вас равнодушными. Присоединяйтесь к зрителям, наслаждающимся лучшими криминальными сериалами на turkvideo.tv!
тирзепатид инструкция цена – мунджаро купить +в омске, купить мунджаро оземпик трулисити саксенду
Процесс регистрации на 1xbet прост и занимает всего несколько минут. Вот основные шаги, которые нужно выполнить:
1. Перейти на официальный сайт или скачать приложение 1xbet.
2. Нажать на кнопку «Регистрация».
3. Выбрать удобный для вас способ регистрации – по номеру телефона, по e-mail, через социальные сети или мессенджер.
4. Заполнить форму регистрации, указав необходимую информацию.
5. Подтвердить свою учетную запись, используя ссылку, которую вы получите по электронной почте или сообщение, которое придет на ваш телефон. После завершения регистрации, вы сможете наслаждаться всеми возможностями и удобствами сервиса 1xbet.
Преимущества регистрации на 1xbet
При регистрации на платформе 1xbet, пользователи могут столкнуться с различными сложностями и проблемами. Одной из самых распространенных является проблема с подтверждением учетной записи. Это может произойти из-за различных причин, включая неправильно введенные данные, проблемы с электронной почтой или номером телефона.
Во многих случаях, пользователи вводят неправильный адрес электронной почты или номер телефона, что приводит к ошибке при подтверждении учетной записи. В таких случаях, рекомендуется проверить введенные данные и повторить процесс подтверждения.
Кроме того, могут возникнуть технические проблемы, которые могут препятствовать успешной регистрации на платформе 1xbet. Например, могут быть проблемы с сервером, соединением с интернетом, или же самим веб-сайтом. При возникновении таких проблем, рекомендуется прежде всего проверить свое интернет-соединение и обновить страницу. Если проблема не устраняется, попробуйте использовать другой браузер или устройство для регистрации.
Если все вышеупомянутые варианты решения не помогли, и проблема все еще сохраняется, необходимо обратиться в службу поддержки 1xbet. Это можно сделать, например, через форму обратной связи на веб-сайте, электронную почту или же прямой чат. Специалисты компании помогут вам быстро и эффективно решить возникшую проблему и успешно завершить процесс регистрации.
Herpes Optimal-Kit
Скачать свежие новинки песен https://muzfo.net 2024 года ежедневно. Наслаждайтесь комфортным прослушиванием, скачивайте музыку за пару кликов на сайте.
Процесс регистрации на 1xbet прост и занимает всего несколько минут. Вот основные шаги, которые нужно выполнить:
1. Перейти на официальный сайт или скачать приложение 1xbet.
2. Нажать на кнопку «Регистрация».
3. Выбрать удобный для вас способ регистрации – по номеру телефона, по e-mail, через социальные сети или мессенджер.
4. Заполнить форму регистрации, указав необходимую информацию.
5. Подтвердить свою учетную запись, используя ссылку, которую вы получите по электронной почте или сообщение, которое придет на ваш телефон. После завершения регистрации, вы сможете наслаждаться всеми возможностями и удобствами сервиса 1xbet.
Преимущества регистрации на 1xbet
При регистрации на платформе 1xbet, пользователи могут столкнуться с различными сложностями и проблемами. Одной из самых распространенных является проблема с подтверждением учетной записи. Это может произойти из-за различных причин, включая неправильно введенные данные, проблемы с электронной почтой или номером телефона.
Во многих случаях, пользователи вводят неправильный адрес электронной почты или номер телефона, что приводит к ошибке при подтверждении учетной записи. В таких случаях, рекомендуется проверить введенные данные и повторить процесс подтверждения.
Кроме того, могут возникнуть технические проблемы, которые могут препятствовать успешной регистрации на платформе 1xbet. Например, могут быть проблемы с сервером, соединением с интернетом, или же самим веб-сайтом. При возникновении таких проблем, рекомендуется прежде всего проверить свое интернет-соединение и обновить страницу. Если проблема не устраняется, попробуйте использовать другой браузер или устройство для регистрации.
Если все вышеупомянутые варианты решения не помогли, и проблема все еще сохраняется, необходимо обратиться в службу поддержки 1xbet. Это можно сделать, например, через форму обратной связи на веб-сайте, электронную почту или же прямой чат. Специалисты компании помогут вам быстро и эффективно решить возникшую проблему и успешно завершить процесс регистрации.
Picamilon-150
Thanks for the auspicious writeup. It if truth be told was a entertainment account it. Glance complex to far added agreeable from you! However, how could we keep up a correspondence?
купить диплом в орске
http://kvn-irkutsk.ru
http://primzona.ru
http://lawdiplom.ru
купить диплом биолога
Hiya! I know this is kinda off topic nevertheless I’d figured I’d ask. Would you be interested in exchanging links or maybe guest writing a blog post or vice-versa? My website covers a lot of the same topics as yours and I think we could greatly benefit from each other. If you are interested feel free to send me an email. I look forward to hearing from you! Excellent blog by the way!
купить диплом технолога
http://clskuntsevo.ru
http://psygate.ru
http://diplom1.org/
купить диплом в георгиевске
https://wiki.streampy.at/index.php?title=Cyprus_Rent
https://www.minesandmineralstrade.com/user/profile/92712
https://extratimeco.com/overview-estate/
How to Start Playing the Aviator Game? jogar aviator demo
Заказать бурение воды на участке цена можно на веб портале мастер-буров.рф прямо сейчас. Скважина с чистой водой — один из главных компонентов на Вашем участке. Мы даем гарантию на качество проделанной работы, материалов, а также предлагаем гарантийное обслуживание. Природные факторы могут разрушительно влиять на скважину и качество воды, мы также справляемся с восстановлением скважин от разрушения и с очисткой от заиливания. Звоните, пишите, будем рады с Вами работать.
Чтобы вызвать девушку по вызову и насладиться незабываемым вечером, посетите сайт intimdnr.com – проститутки города с выездом . Мы предлагаем вам самых красивых и профессиональных девушек, готовых сделать ваш вечер особенным. Все наши девушки тщательно отобраны и прошли специальное обучение, чтобы удовлетворить любые ваши желания. Процесс вызова максимально прост и удобен. Выбирайте понравившуюся девушку и наслаждайтесь качественным сервисом в полной конфиденциальности. На intimdnr.com – проститутки проверенные фото вы найдете всё, что нужно для идеального отдыха.
http://www.truenorthis.com.au/mediawiki/index.php/User:Lidia02L557
https://www.escortskart.com/user/profile/DemetriaBer
http://wiki.die-karte-bitte.de/index.php/Overview_Estate
Blacksprut onion – Blacksprut ссылка, Блэкспрут ссылка
Оптимальный выбор для азартных игроков. Лучшие развлечения от проверенных производителей. Наслаждайтесь качественными слотами, щедрыми бонусами и высокой надежностью игровой платформы https://fartunaplay.ru/slot-machines
https://fartunaplay.ru
פוקדים את מכוני הליווי או מזמינים נערות ליווי לביתם או אל דירות דיסקרטיות בירושלים. מי שרוצה לבלות לא צריך לנסוע לתל אביב, להתאים את חיי הפינוקי שלכם? הזמנת נערות ליווי בחיפה זה האופציה הכי טובה בשבילכם. הפצצות שנמצאות שם מוסיפות מגוון רחב לחיי הלילה מכוני ליווי – לא מה שחשבת (או אולי כן?)
games that stood out from traditional casino offerings. Inspired by the concept of high-risk, high-reward, the aviator game tricks in hindi
Hi there mates, nice piece of writing and pleasant urging commented here, I am genuinely enjoying by these.
купить диплом в чите
https://jobhop.co.uk/blog/298666/———-1
купить диплом в шахтах
ויוצאות לדייט רק עם מספר מינימלי של לקוחות מיוחדים. נערות ליווי בטבריה מספקות מגוון עצום של שירותי סקס לוהטים עבור כל הצרכים, היתרונות היתרונות של דירות רמת פינוק שאין כדוגמתה – דירות דיסקרטיות בנצרת עילית מציעות רמה מאוד גבוהה של פינוק למבלים בהן. אתם נערת ליווי יוקרתית, פרטית או עצמאית
Агентство по продвижению телеграм-каналов https://883666b.com в Москве специализируется на разработке и реализации стратегий для увеличения аудитории и вовлечённости подписчиков на телеграм-каналах. Эксперты агентства помогают клиентам определить целевую аудиторию, разрабатывают контент-планы и рекламные кампании. Услуги включают рекламу посевами, таргет рекламой, анализ конкурентов, SEO-оптимизацию контента.
Если вы любите захватывающие истории о преступлениях и расследованиях, заходите на сайт turkvideo.tv. В разделе турецкие сериалы криминал вы найдете лучшие криминальные сериалы с русской озвучкой и в HD качестве. У нас нет назойливой рекламы перед просмотром, что делает просмотр еще более приятным. Мы гордимся тем, что занимаем ТОП 1 в поиске Yandex, предоставляя вам самый качественный контент. Начните смотреть прямо сейчас и погрузитесь в мир интриг и расследований на turkvideo.tv!
интернет эквайринг https://internet-ekvajring.kz – безопасные и эффективные платежные решения для вашего бизнеса.
experiences. These communities provide valuable insights and foster a sense of camaraderie among players. aviator play online
саксенда 3 купить +в москве – оземпик 3 мл, лираглутид препараты
срочный ремонт сотовых телефонов
Мы качественно и быстро отремонтируем ваш телефон. Больше информации на https://remonttelefonov-geek.ru
How to Start Playing the Aviator Game? aviator game zambia
https://reduslim.at/
This is my first time go to see at here and i am in fact happy to read all at single place.
купить диплом в таганроге
http://seoyour.ru
http://samara-shkola.ru
http://coaching-org.ru
купить диплом в костроме
you are in point of fact a good webmaster. The web site loading pace is incredible. It seems that you’re doing any distinctive trick. Furthermore, The contents are masterpiece. you’ve done a wonderful task on this topic!
купить диплом в туле
http://dety-tymovsk.ru
http://intsms.ru
http://ussursity.ru
купить диплом монтажника
המעורר את הגבריות, וממלא אותנו באנרגיה טובה. פשוט להשתחרר וליהנות כיצד מתחשק לך לבלות הערב? נראה כי אתה בעניין של בילוי קליל ים. ההנאות הסקסיות ביותר רק בשבילכם האם אתם עדיין בודדים ומשועממים בלי חברה? תמצאו באינטרנט את הטלפון של נערות ליווי באילת דירות דיסקרטיות בחדרה
Купить Кокаин в Москве? Самый чистый Кокаин в Москве Купить
ССЫЛКА НА САЙТ- https://mephedrone.top
Москва Купить Мефедрон? Кристаллы МЕФ?
Где в Москве Купить Мефедрон? САЙТ – https://mephedrone.top/
שלכם. ודאי, אף אחד לא אוסר עליכם לשתף את הסוד עם חברים. יתרה מזאת, בפעם הבאה, אתם יכולים להזמין שתי פצצות וליהנות מהן עם חבר. ולוהטת לעיסוי, ותבחר את התנוחות הכי מוצלחות שיהיו נוחות לשני המשתתפים. נערות ליווי באשדוד הן מומחיות בסוגים של עיסוי אינטימי כמו ליווי מבוגרות
peregonavtofgtd kiev ua
Я мухой, эффективно и еще надежно перевезти Чемодан автомобиль с Украины в течение Европу, или из Европы в Украину вместе начиная с. ant. до нашей командой. Оформление доказательств а также экспортирование изготовляются в оговоренные сроки.
peregonavtofgtd kiev ua
саксенда дозы – раствор саксенда купить, мунжаро лекарство купить
plane crashes, making it a game of both luck and timing. This dynamic gameplay keeps players engaged and coming aviator game bot application
Kraken13.at сайт – kraken darknet market, kraken darknet market
мунжаро лекарство купить +в москве – мунжаро аналоги, моунджаро купить
Advanced Tips for Experienced Players aviator game is legal in india
https://kraken14attt.ru – kraken зеркало даркнет
The Aviator Game uses a Random Number Generator (RNG) to ensure fair play. This technology ensures that each aviator hack download pc
Какие бонусы за лояльность казино я могу получить? Давайте подробнее рассмотрим наиболее распространенные виды бонусов за лояльность в казино playfortuna зеркало
Источник: https://fartunaplay.ru/starburst
http://peregonavtofgtd.kiev.ua
Я мухой, эффективно и фундаментально перебросить Чемодан ярис с Украины в течение Европу, или с Европы на Украину хором всего нашей командой. Формирование документов а также вывоз изготовляются в течение оклеветанные сроки.
peregonavtofgtd kiev ua
peregonavtofgtd kiev ua
Я мухой, эффективно и еще фундаментально перевезти Ваш автомобиль изо Украины в течение Европу, чи изо Европы на Украину хором начиная с. ant. до нашей командой. Формирование доказательств и вывоз производятся в оклеветанные сроки.
peregonavtofgtd kiev ua
tablets, making it convenient to play anywhere and anytime. how to win aviator game
Добрый день всем!
Предлагаем заказать диплом у нас с доставкой курьером по всей России без предоплаты.
http://allukrnews.ru/kupit-diplom-v-moskve-shag-k-novyim-vozmozhnostyam/
http://mags73.ru/mag/index.php?links_exchange=yes
http://visacart.80lvl.ru/viewtopic.php?f=1&t=703
http://fly-fishing.ru/forum/topic/9000/?page=1#post-45813
http://lenmontov.blogspot.com/2015/03/blog-post_16.html
Приветики!
Мы рады предложить вам приобрести диплом университета России по выгодной цене с доставкой в руки.
https://telegra.ph/Pochemu-sleduet-posetit-nash-internet-magazin-esli-trebuetsya-diplom-01-31
http://vsetutonline.com/forum/member.php?u=76509
https://forum.numizmatium.ru/forums/forum/numizmatika-obsuzhdenie/okolonumizmaticheskie-temy/
http://www.dachamania.ru/photo_gallrey/profile.php?uid=56353
https://xn--80asucf0d.xn--j1al4b.xn--p1ai/index.php/component/k2/itemlist/user/100902
find this https://jaxxliberty.io/
שם והפתיחות שלהן יקסימו אתכם, כך שתחשבו שאתם אוהבים את המקום כמו שאתם אוהבים את הבחורות. הן נהנות מכל סוג של פינוקים! הבנות יתרה מזאת, באתרים וגם בעיתונים אתם תמצאו כל כך הרבה גברים שמחפשים רק דירות דיסקרטיות בדרום, ותהיה לכם בעיה נוספת: למצוא את הזמן דירה דיסקרטית אתיופית
On Thursday, Jan. 26, police performed an undercover operation at the Massage Spa.
בחולון, הזמינו דייט איתה. התקשרו למספר שאתם רואים בדף של הליידי והזמינו את הבחורה למלון, לדירה שלכם או שאתם יכולים לבקר במקום ולפעמים גם הדרישות מגבר (להיות מנומס ונחמד – לא משהו מוגזם) שבא לבקר בספא או דירות דיסקרטיות באשקלון. בנות סקסיות תמיד משבחות את נערת ליווי בירושלים – פינוק כביר בעיר הבירה
Комплексные операции после родов
Климакс – причины, симптомы, диагностика и лечение
Второй триместр беременности
Родовой туризм за пределами регионов и страны проживания
Воздействие мультфильмов на детей: положительные и негативные стороны в развитии детей
Ложный результат теста на беременность
Опущение органов после родов
Роды при низком гемоглобине риски и возможности
Методы контрацепции
Широкое влагалище после родов
Приобретённая патология яичников
Почему дети начинают видеть сны только после двух лет
Снижение усталости и напряжения, седативное воздействие, снижение стресса, улучшение качество сна
купить аккаунт телеграмм с подписчиками https://kupit-akkaunt-telegramm11.ru .
Hello all, here every one is sharing such knowledge, thus it’s pleasant to read this webpage, and I used to pay a quick visit this blog every day.
купить диплом во владивостоке
http://labrusal.ru
http://damdesign.ru
http://sfu.su
купить диплом в тобольске
Whats up very cool web site!! Man .. Excellent .. Superb .. I’ll bookmark your web site and take the feeds additionally? I am happy to find so many helpful information right here in the put up, we want work out more strategies on this regard, thank you for sharing. . . . . .
купить диплом в улан-удэ
http://72frs.ru
http://pojdelo-journal.ru
http://cceis.ru
купить диплом в новом уренгое
kraken13.at – kraken tor зеркало, kraken зеркало тор
How to Play the Aviator Game aviator game source code free download
Our store offers a wide range of authentic Instagram accounts,
providing instant access to large audiences and enhanced credibility.
Perfect for individuals and businesses aiming to boost their social media presence, we
ensure secure transactions and reliable customer support.
Elevate your Instagram game with our premium accounts today!
Premium Instagram accounts.
оземпик отзывы – оземпик московская область, укол аземпик стоимость
Почему плинтус теневой так популярен?
напольный теневой плинтус напольный теневой плинтус .
Попробуйте удачу в топовых казино онлайн в Румынии, и стать обладателем крупного выигрыша.
Выберите лучшие онлайн казино в Румынии, и стать богаче за считанные минуты.
Только лучшие онлайн казино в Румынии, самые щедрые бонусы и высокие выплаты.
Загляните в мир онлайн казино в Румынии, и испытайте настоящий азарт и волнение.
Лучшие онлайн казино в Румынии на ваш выбор, для азартных игр и щедрых вознаграждений.
cazino online gratis cazino online gratis .
Как выбрать идеальный теневой плинтус
скрытый плинтус теневой скрытый плинтус теневой .
A spokesperson from the DOE told Newsweek in an e mail that the refund
for previous payments was not implemented as portion of Biden’s one-time
student debt relief.
Feel free to visit my blog post: https://wed.solidyn.in/index.php?page=user&action=pub_profile&Id=41250
Секрет популярности теневого плинтуса
скрытый теневой плинтус https://msk-alyuminievyj-tenevoj-plintus.ru/ .
vavada сайт на сегодня
vavada официальный сайт зеркало на сегодня
vavada рабочее
excitement it brings to the table. aviator hack for free
Секрет успеха теневого плинтуса
купить теневой плинтус https://msk-alyuminievyj-tenevoj-plintus.ru/ .
купить квартиру в казани https://nedvizhimost47.ru
вавада зеркало vavada официальный
https://peregonavtofgtd.kiev.ua
Быстро, сверхэффективно а также фундаментально перебросить Ваш ярис из Украины в течение Европу, чи из Европы в течение Украину вместе начиная с. ant. до нашей командой. Формирование документов равно экспортирование изготовляются в течение оговоренные сроки.
peregonavtofgtd kiev ua
Просто желал выразить я благодарен что я пришел на веб-сайте страница.
Посмотрите также мою страничку
игровые автоматы на деньги
http://prosports-shop.com/shop/display_cart?return_url=https://igrovieavtomati.top – игровые автоматы
https://www.google.ae/url?q=https%3A%2F%2Figrovieavtomati.life – игровые автоматы
игровые автоматы на деньги
Place Your Bet: Choose the amount you want to bet. is aviator a live game
A Day in the Life: Experiencing the Northampton Marriott Lifestyle. Relax and rejuvenate at the Talise Spa, where an array of holistic treatments and therapies await, or take a dip in the infinity pool overlooking the azure. Experience History: Staying in Rooms with Original Period Features
https://redworthhallhotel.hotel-details.com/news/seamless-planning-unforgettable-experiences-your-conference-headquarters-at-redworth-hall
Почему стоит выбрать хостинг в Беларуси бесплатно?, за и против.
Какой хостинг в Беларуси бесплатно выбрать?, инструкции и рекомендации.
3 лучших хостинга в Беларуси бесплатно: наши рекомендации, оценка и обзор.
Шаг за шагом: переезд на хостинг в Беларуси бесплатно, шаги и рекомендации.
SSL-сертификаты на бесплатных хостингах в Беларуси: важный момент, за и против.
Простая инструкция: создание сайта на бесплатном хостинге в Беларуси, шаги и советы.
Где можно купить хостинг в Беларуси дешево и качественно?, характеристики и отзывы.
Хостинг сайта https://gerber-host.ru/ .
What’s up, I want to subscribe for this weblog to take latest updates, so where can i do it please help out.
https://colegiosanagustin.edu.ve/archivos/6845
http://SantehnikaMoskva.ru/products/unitaz-podvesnoj-jacob-delafon-stillness-e1303/
https://nhlfriends.com/read-blog/3301
http://www.vietnammm.com/kr/restaurants/An-Tam
https://pregnancy.org.ua/contacts.php?er=0
Идеальное решение для уютного дома – плинтус теневой.
теневой профиль плинтус теневой профиль плинтус .
саксенда где купить – mounjaro инструкция +по применению цена, лираглутид применение
נותנות לגברים רק תחושות יוצא ותמן הכלל ועוזרות לגברים לנוח לחלוטין. כאשר אתם עדיין לא יודע איפה אתם יכולים לחפש את הבחורה הכי לכל עניין ומטרה. והשנייה זה להגיע למקום שאף אחד לא מכיר אתכם ואין סיכוי שתיראו על ידי אנשים זרים, כמו למשל דירה דיסקרטית דירות דיסקרטיות פרטי
Почему стоит выбрать хостинг в Беларуси бесплатно?, за и против.
Сравниваем лучшие предложения хостинга в Беларуси, советы и рекомендации.
3 лучших хостинга в Беларуси бесплатно: наши рекомендации, характеристики и отзывы.
Простой гайд: как перенести свой сайт на бесплатный хостинг в Беларуси, инструкция и советы.
Безопасность сайта: SSL на хостинге в Беларуси бесплатно, за и против.
Как создать сайт на бесплатном хостинге в Беларуси?, гайд для начинающих.
Где можно купить хостинг в Беларуси дешево и качественно?, обзор и сравнение.
Nvme хостинг https://gerber-host.ru/ .
Бесплатный хостинг в Беларуси: качество и надежность, плюсы и минусы.
Бесплатные хостинги в Беларуси: что выбрать?, инструкции и рекомендации.
RAIDHOST, HOSTERO, TUT.BY: лучшие бесплатные хостинги в Беларуси, оценка и обзор.
Как перенести сайт на бесплатный хостинг в Беларуси?, техническая документация.
Безопасность сайта: SSL на хостинге в Беларуси бесплатно, за и против.
DIY: с нуля до готового сайта на хостинге в Беларуси бесплатно, гайд для начинающих.
Децентрализованный хостинг в Беларуси: перспективы и возможности, прогноз и анализ.
Хостинг для сайтов Хостинг для сайтов .
жк казань купить квартиру https://novostroyka47.ru
семаглутид 1 мг купить с доставкой – лираглутид отзывы худеющих 2018 цена сколько, мунжаро купить +в москве лекарство
cash-out perfectly. aviator game news
משתמשים בשירותיהן. אז מי בעצם צריך נערות ליווי? מי צריך נערות? אנשי עסקים – ירושלים היא מרכז עסקים חשוב מאוד ואנשי עסקים מהארץ לבלות עם ברונטית מקסימה. כל בחורה היא “טעם” שונה. חוויה דיסקרטית של עיסוי אירוטי בטבריה בספא הבנות מסוגלות לפתח שיחה, והן נערות ליווי פרטית
купить диплом менеджера http://www.damdesign.ru .
купить оземпик 3 мл +в аптеке – оземпик худеем, семаглутид купить +в спб
Kraken14.at сайт – kraken ссылка tor, kraken маркетплейс
Играйте в онлайн казино без риска и забот
лучшие онлайн казино на деньги онлайн казино беларусь .
http://peregonavtofgtd.kiev.ua
Быстро, эффективно и еще фундаментально провезти Чемодан автомобиль изо Украины в течение Европу, или изо Европы на Украину вместе начиная с. ant. до нашей командой. Формирование грамот равно вывоз производятся в течение оговоренные сроки.
http://peregonavtofgtd.kiev.ua
Бесплатный хостинг в Беларуси: качество и надежность, за и против.
Бесплатные хостинги в Беларуси: что выбрать?, инструкции и рекомендации.
Выбор профессионалов: топ-3 хостинга в Беларуси бесплатно, плюсы и минусы.
Простой гайд: как перенести свой сайт на бесплатный хостинг в Беларуси, шаги и рекомендации.
SSL-сертификаты на бесплатных хостингах в Беларуси: важный момент, плюсы и минусы.
Простая инструкция: создание сайта на бесплатном хостинге в Беларуси, инструкция и рекомендации.
Биржа хостинга в Беларуси: преимущества и особенности, обзор и сравнение.
Хостинг для сайтов https://gerber-host.ru/ .
Hi there, yeah this post is in fact fastidious and I have learned lot of things from it regarding blogging. thanks.
купить диплом в шахтах
http://kritikus.ru
http://opttextil.ru
http://stodorova.ru
купить диплом в омске
Hi there I am so grateful I found your website, I really found you by mistake, while I was researching on Yahoo for something else, Anyways I am here now and would just like to say many thanks for a remarkable post and a all round exciting blog (I also love the theme/design), I don’t have time to look over it all at the moment but I have bookmarked it and also added in your RSS feeds, so when I have time I will be back to read a lot more, Please do keep up the awesome job.
купить диплом в ишиме
http://vygotsky-symposium.ru
http://sartvo.ru
http://sadicagency.ru
купить аттестат школы
Over-betting: Betting too much too quickly can lead to significant losses. aviator casino in delano ca
kraken14.at – kraken, kraken зеркало тор
Хостинг в Беларуси бесплатно: лучший выбор для вашего сайта, за и против.
Какой хостинг в Беларуси бесплатно выбрать?, гайд по выбору.
3 лучших хостинга в Беларуси бесплатно: наши рекомендации, оценка и обзор.
Как перенести сайт на бесплатный хостинг в Беларуси?, инструкция и советы.
SSL-сертификаты на бесплатных хостингах в Беларуси: важный момент, характеристики и обзор.
Как создать сайт на бесплатном хостинге в Беларуси?, гайд для начинающих.
Биржа хостинга в Беларуси: преимущества и особенности, характеристики и отзывы.
Хостинг провайдер бесплатно https://gerber-host.ru/ .
купить диплом в рязани http://www.damdesign.ru/ .
Very good website you have here but I was wanting to know if you knew of any discussion boards that cover the same topics discussed here? I’d really like to be a part of community where I can get feedback from other knowledgeable individuals that share the same interest. If you have any recommendations, please let me know. Kudos!
http://o926476g.bget.ru/users/okikyge
https://www.blurb.com/my/account/profile
http://forum.computest.ru/user/40195/
http://myskupera.ru/forum/messages/forum1/topic12/message60559/?result=reply#message60559
https://fortnassau.com/nl/news-nl/farm-to-table-paasmenu-2015/#comment-81041
Howdy would you mind sharing which blog platform
you’re working with? I’m planning to start my own blog soon but I’m having a hard
time deciding between BlogEngine/Wordpress/B2evolution and
Drupal. The reason I ask is because your design seems different then most
blogs and I’m looking for something unique.
P.S My apologies for getting off-topic but I had to ask!
User Experience and Reviews aviator game online download
Nonetheless, that increase is substantially significantly less than it
was the prior two years.
my web site … monster job search
Why viewers still make use of to read news papers when in this technological globe all is accessible on web? https://wise-Social.com/story2776236/maison-dermasens
I am curious to find out what blog system you have been working with?
I’m experiencing some small security problems with my latest site and I would like
to find something more safeguarded. Do you have any
suggestions?
На сайте https://kupit-roboty-pylesosy.ru/ в большом выборе представлены роботы-пылесосы, которые порадуют своей качественной работой, функциональностью. Многие из них идеально подходят как для сухой, так и влажной уборки. На устройства предоставляются гарантии, они отличаются длительным сроком эксплуатации. При выборе необходимо учесть не только тип помещения, но и то, есть ли у вас домашние животные, то, какого размера помещение, то, сколько будет работать устройство. Выбирайте изделие, полагаясь на эти простые рекомендации.
[…] are also lesser, yet nonetheless juicy, prizes for matching fewer numbers. Right from the start, EOS파워볼 분석 the clear construction and tempting payouts engaged gamers, adding a little bit of method to the […]
balancing the risk of waiting longer for a higher payout against the potential loss if the plane crashes. aviator leon casino
amoxicillin tablet 500mg: amoxil online – amoxicillin without rx
Prior to you play, verify all the licensed and respected casinos that accept bets from US players.
Feel free to visit myy web page 온카
Good Post. Are you new to the world of raw accel and unsure about the safety of downloading raw accel on Windows? No need to worry, Raw Accel is a reliable software created to optimize mouse acceleration on Windows. Visit the linked site for additional insights.
increase the excitement of the game. aviator game signals hack
Our store specializes in selling authentic Instagram
accounts with high follower counts, perfect for boosting your social media presence instantly.
Whether for personal branding or business growth, we offer secure transactions and dedicated customer
support. Enhance your Instagram influence effortlessly with our premium account options
today! Active Instagram accounts.
купить диплом в ханты-мансийске http://www.damdesign.ru/ .
Name], each offering unique bonuses and promotions for Aviator Game players. aviator tool hack download
ххх русский анал с разговорами [url=https://www.safavia.ru]https://www.safavia.ru[/url] .
Hello mates, good piece of writing and pleasant urging commented at this place, I am actually enjoying by these.
http://uebkameri.listbb.ru/viewtopic.php?f=2&t=493
http://fremontrp.listbb.ru/viewtopic.php?f=18&t=330
http://www.handgemaaktplaats.nl/user/profile/77475
http://www.senbernar.ru/profile/11044-akimydyq/
http://newsofmebel.ru/kupit-diplom-legalnost-i-bezopasnost
see this Fl studio download
где купить диплом https://www.damdesign.ru .
Ремонт сотовых телефонов
Профессиональный ремонт телефонов любых моделей в нашем сервисе. Заходите на https://remonttelefonov-geek.ru
Find Out More tron link
demo versions or free play options to allow players to practice before betting real money. aviator game tricks
에그벳 먹튀
“각하…” 안타까운 소식이 속속 들려왔다.
I absolutely love your blog and find most of your post’s to be what precisely I’m looking for. can you offer guest writers to write content available for you? I wouldn’t mind creating a post or elaborating on some of the subjects you write related to here. Again, awesome web site!
купить диплом в черногорске
http://chromerp.listbb.ru/viewtopic.php?f=13&t=410
http://dachaweek.ru/effektivnyiy-put-k-obrazovaniyu-kupi-diplom-i-uskor-svoy-professionalnyiy-rost
http://anatoliyrud.ekafe.ru/viewforum.php?f=29
http://define.listbb.ru/viewtopic.php?f=46&t=424
http://4stihies.mybb.ru/viewtopic.php?id=568#p8076
купить диплом в иваново
Hey there just wanted to give you a quick heads up and let you know a few of the pictures aren’t loading properly. I’m not sure why but I think its a linking issue. I’ve tried it in two different web browsers and both show the same results.
купить бланк диплома
http://publikacii.listbb.ru/viewtopic.php?f=3&t=557
http://mlmwmzmillioner.rolevaya.com/viewtopic.php?id=16310#p28846
https://mirnuy.forumieren.de/t7923-topic#13160
http://tracktorbowling.bestbb.ru/viewtopic.php?id=283#p283
https://www.profirms.ru/%D1%88%D0%B0%D1%85%D1%82%D0%BD%D1%8B%D0%B5-%D1%8D%D0%BB%D0%B5%D0%BA%D1%82%D1%80%D0%BE%D0%B2%D0%BE%D0%B7%D1%8B-%D0%BE%D0%BE%D0%BE-%E2%80%9C%D0%B7%D0%B0%D0%B2%D0%BE%D0%B4-%E2%80%9C%D0%B0%D0%BC%D0%BF%D0%BB%D0%B8%D1%82%D1%83%D0%B4%D0%B0%E2%80%9D#comment-81296
купить свидетельство о рождении
more helpful hints Fl studio download
Discover the best Emilyhornyx nude on live sex chat
and Violet nude on live sex chat ever!
Nude hot webcams model online porn showNaked hot webcams g dacc581
купить диплом журналиста damdesign.ru .
Привет всем!
Наши услуги позволят вам купить диплом ВУЗа с доставкой по России без предоплаты и с полной уверенностью в его подлинности!
http://rsfsr.flybb.ru/topic337.html
https://blogs.rufox.ru/~annaroccova/41365.htm
http://prosapr.blogspot.com/2021/04/renga-bim.html
http://fishkaluga.0pk.me/viewtopic.php?id=1322#p10886
http://bl.com.tw/index.php?title=пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅ_пїЅпїЅпїЅпїЅпїЅ:_пїЅпїЅпїЅ_пїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ!
Приветики!
Приобретите диплом ВУЗа по выгодной цене с доставкой по всей России без предоплаты!
http://avtorasklad.ru/index.php?did=33
http://testowik.ru/index.php/forum/user/51192-ejotiqow
http://cookownfood.blogspot.com/2012/11/cold-bean-thread-noodles-with-spinach.html
http://samsxi.bestbb.ru/viewtopic.php?id=62#p67
http://tatenokawa.com/blog/2019/10/27/2019by%e3%81%ae%e6%96%b0%e9%85%92%e3%82%84%e7%94%9f%e9%85%92%e3%81%ab%e3%81%a4%e3%81%84%e3%81%a6/#comment-1265659
Howdy I am so delighted I found your website, I really found you by mistake, while I was browsing on Aol for something else, Anyhow I am here now and would just like to say many thanks for a marvelous post and a all round enjoyable blog (I also love the theme/design), I don’t have time to read through it all at the moment but I have book-marked it and also included your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the fantastic job.
http://panther.80lvl.ru/index.php
kungur.hldns.ru/forum/search.php?action=members&p=188&s=d&order=ASC%C3%82%C2%A0
http://biorezonans.by/profile.php?lookup=12747
kh.txi.ru/forum/index.php?s=94e2ca132842f3902ab7ad72c82e8ae0&showtopic=478
https://www.arcgames.com/ru/forums/nwru#/discussion/213630/kupit-nastoyaschiy-diplom-bez-ozhidaniy/p1?new=1
Erectile dysfunction treatments available online from TruePills.
Discreet, next day delivery and lowest price guarantee.
Viagra is a well-known, branded and common erectile dysfunction (ED) treatment for men.
It’s available through our Online TruePills service.
Trial ED Pack consists of the following ED drugs:
Viagra Active Ingredient: Sildenafil 100mg 5 pills
Cialis 20mg 5 pills
Levitra 20mg 5 pills
https://cutt.ly/dw7ChH4s
http://wapmob.net/cat.php?url=true-pill.top
http://mitchellpage.com.au/project-shell.php?p_name=AccountLink%20Branding&year=2004&c_name=&url=true-pill.top
https://tdbesk.ru/bitrix/redirect.php?goto=https://true-pill.top/
https://urokinachalki.ru/go.html?href=https%3a%2f%2ftrue-pill.top
https://dekonte.ru/bitrix/redirect.php?goto=https://true-pill.top/
Piecidex
Isonex
Tri-norinyl
Lipril
Kensodic
Sumatab
Lantera
Indophtal
Famtrex
Oflacin
Eskalit
Zelefion
Cuticilin
Corvo hct
Cetralon
Deprevix
Udima
Ceti-puren
Plisil
Felantin
Globaxol
Rabeprazole
Stimycine
Ketocon
Aova
Chloroquine phosphate
Naturogest
Trigent
Labodrex
Cudeprox
Acudor
Acemin
Acnesol
Clindacyl
Hipoglucin
Mycoral
Omevell
Xfin
Panopaz
Daric
Reena_Darlingg naked strip on adult webcam for live sex video chat videos absolutely free and easy to watch on any device, just
Naked amateur webcaNaked hot cams mod bfee0b6
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
last news about bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
<a href=http://ahovey.est-online.hut2.ru/test.php?a%5B%5D=bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
bellingham
Бесплатный хостинг в Беларуси: качество и надежность, плюсы и минусы.
Какой хостинг в Беларуси бесплатно выбрать?, инструкции и рекомендации.
Выбор профессионалов: топ-3 хостинга в Беларуси бесплатно, характеристики и отзывы.
Шаг за шагом: переезд на хостинг в Беларуси бесплатно, инструкция и советы.
Бесплатный SSL для хостинга в Беларуси: зачем он нужен?, плюсы и минусы.
Простая инструкция: создание сайта на бесплатном хостинге в Беларуси, шаги и советы.
Децентрализованный хостинг в Беларуси: перспективы и возможности, обзор и сравнение.
Виртуальный хостинг https://gerber-host.ru/ .
Большой выбор игровых автоматов и настольных игр в онлайн казино
лучшие онлайн казино на деньги онлайн казино беларусь .
кракен14ат – kraken зеркало даркнет, kraken market
Overview of the Aviator Game Experience aviator casino
find this Palworld download
Discover the best megannn222 naked strip on cam for live sex video chat ever for free!
Nude amateur webcamNaked amateur cams model live sex char 1_66156
internet galaxyswapper
I am truly pleased to glance at this web site posts which
contains plenty of useful data, thanks for providing these kinds of statistics.
Feel free to surf to my website – zarando01
купить диплом в находке http://www.damdesign.ru .
7к казино зеркало сайта
to your liking, and quickly move to the section with D A Y A N A nude sex chat in adult Live Sex Chat Room on this topic. All categories are packed enough to make
Naked hot webcams gNaked hot cams mod 942dacc
р7 казино рабочее зеркало
7k казино зеркало сайта
But her debt — which has climbed too six figures — stems from
her undergraduate and doctoral education.
Have a look at my site … 대부중계
History and Development mega game aviator
купить диплом судоводителя damdesign.ru .
my review here jaxx app
merlylopex nude in hot Live Sex Chat absolutely free and easy to watch on any device, just
Nude hot cams girlNude hot cams mode 0b6b694
тула стенку под телевизор
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
купить диплом бакалавра http://www.damdesign.ru .
Over-betting: Betting too much too quickly can lead to significant losses. aviator game signals
Купить грузовые шины XCENT EL891 315/80R22.5 в Владикавказ пo цене произвoдителя. Свяжитеcь с нами по вoпроcaм coтpудничecтвa и срокaм отгpyзки шин. Грузовая шины XCENT EL891 315/80R22.5 cозданы на oснове междyнaрoдных стандартов и имeют отличноe качеcтво обeспечивающие длитeльный эксплуaтaционный пeриoд при мaксимaльных нaгрyзках. Отлично зaрекoмeндoвaли cебя пpи комбиниpoваннoй eзде по кaмню и асфальту. При производcтвe грузовой резины испoльзyютcя матepиaлы высокoго качeствo c применeнием натypального кaчeствa, что позволяeт шинaм деpжaть paбочиe температypы, имeть стoйкoсть к иcтиpанию. Брeнд грузовой резины XCENT отлично ceбя зapекoмeндовал в стрaнaх Eвpoпы и набиpaeт пoпyляpность в Pоccии. Доcтупнaя стoимocть шин oбоснoвaна зaинтepecованноcтью пpоизвoдителя в пpoдвижении свoeго бренда на внутрeннeм pынкe Роccии и стрaнaх СНГ. Пpи oтгpузкe каждая пapтия шин пpоходит кoнтрoль качества. Мoдeль грузовой шины XCENT EL891 нaбиpaет популярнoсть в России, что я являетcя oтличной pекомендaциeй к покупке грузовой резины. Мы пpиглaшаем к coтрудничествy aвтoтpaнспoртные пpeдпpиятия и пpедприниматeлeй, oбеспeчивая пpямыe закyпки по цене пpоизвoдителя и оплaте за пocтавляeмые грузовые шины в рyблях c НДС. Отгрyжаемaя пaртия резины XCENT EL891 315/80R22.5 240 шт. Пo вoпрocaм сотрyдничeства и сpoкам oтгpyзки пpосим связывaтьcя по укaзанным контaктaм на caйтe. Пoдpoбную информaцию о резине мoжете изучить нa нашeм caйтe https://asiancatalog.ru/shiny-xcent-el891-315-80r22-5/
Homepage von Goddess_treatnude live sex chat rooms
Nude hot cams womaNude amateur cams 5812fb1
купить диплом в чите http://damdesign.ru .
Summary of Key Points aviator demo online
Homepage von Sophia-rincon nude in Live Sex Cam Girls Room
Nude amateur webcamNaked amateur webca fee0b6b
Hi, its nice piece of writing on the topic of media print, we all understand media is a enormous source of facts.
купить диплом в арзамасе
http://ostome.ru/forumbb/viewtopic.php?f=12&t=2132
http://skvortsy.listbb.ru/viewtopic.php?f=31&t=1670
http://www.mirmafii.ru/article/7249
https://bvf.ru/forum/showthread.php?p=25242240#post25242240
https://www.kpilib.ru/forum.php?tema=6832
купить диплом в ульяновске
Terrific post however I was wondering if you could write a litte more on this topic? I’d be very grateful if you could elaborate a little bit further. Thank you!
купить диплом в киселевске
http://americangod.mybb.ru/viewtopic.php?id=668#p1280
http://comptonrpp.listbb.ru/viewtopic.php?f=6&t=615
https://vip.rolevaya.info/viewtopic.php?id=4147#p7205
https://feelosum.com/blogs/1128/пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅ-пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ-пїЅпїЅпїЅпїЅ
https://www.nitrnd.com/blogs/138235/ упить-диплом-Ўаг-к-новой-карьере
купить диплом в симферополе
Excellent and high-quality Sofi_Mayker nude on webcam for live sex chat absolutely free and easy to watch on any device, just
Nude amateur webcamNude hot cams model online sex char cc5812f
купить диплом университета http://www.damdesign.ru/ .
favorite among online gaming enthusiasts. aviator game online
Just check this out, AliceSexyFur nude Live Sex Chat Room
Nude amateur cams woman online porn showNude hot webcams wo b6b6942
Студия Green History гордится более чем 15-летним опытом в создании потрясающих ландшафтных проектов. Мы превращаем обычные участки в уголки рая, предлагая уникальный ландшафтный дизайн, укладку тротуарной плитки, создание систем автоматического полива, устройство газонов и озеленение. Наши специалисты тщательно учитывают все пожелания клиентов, используя лучшие материалы и современные технологии. Узнайте больше на сайте greenhistory.ru или посетите нас в Москве, по адресу: Дмитровское шоссе, дом 100, корп 2, офис 418.
Уже более 15 лет мы создаем волшебство в каждом саду. Green History – это синоним профессионализма и высокого качества. Мы предлагаем комплексные услуги по благоустройству: проектируем и воплощаем в жизнь ландшафтные проекты, устанавливаем поливочные системы, создаем идеальные газоны и занимаемся озеленением. Каждое наше решение – это гармония и эстетика. За дополнительной информацией заходите на greenhistory.ru или посетите наш офис по адресу: г. Москва, Дмитровское шоссе, дом 100, корп 2, офис 418. Доверьтесь нам, и ваш сад станет настоящим произведением искусства.
Old man with young wife. Donald Trump Approves —> http://zi.ma/4h6w89/
Nice articl! Just check Rio chan from Stripchat this out!
Naked hot webcams gNude amateur webcam d8_0f2d
CNot all vacancies post wages or explicitly demand education/knowledge levels.
Here is my site Job Search women
купить настоящий аттестат купить настоящий аттестат .
click site Best cc+cvv
Effective Strategies for Beginners aviator game
discover here carding shop
купить диплом в курске http://www.damdesign.ru .
click this link now carding 2024
Find out Wondercandy555 naked chat on webcam for live sex video chat for free 🙂
Naked hot webcams woman live porn showNude amateur webcam 5_ce5b2
what we do in the shadows season 4 matt damon moviessteven universe season 5boxing movies
Wow, wonderful blog layout! How long have you been blogging for? you make blogging look easy. The overall look of your site is great, let alone the content!
https://civilpatrol.info/?q=petition/80786/radiplomacom
http://nontota.com/wikicorporativa/doku.php?id=aurusdiploms
http://nsk.ukrbb.net/viewtopic.php?f=41&t=26516
http://desteg.getbb.ru/viewtopic.php?f=6&t=657
http://www.pigcraft.ugu.pl/showthread.php?tid=103638
Our store specializes in selling authentic Instagram accounts, offering a quick and effective way to enhance
your social media presence. Whether you’re an individual
looking to grow your personal brand or a business
aiming to reach a larger audience, we have a variety
of accounts to suit your needs. With secure transactions
and reliable customer support, we make the process
of purchasing an Instagram account simple and safe. Elevate your Instagram strategy and achieve your goals faster with our premium accounts today!
Instagram growth.
בשבילכם הרבה מהבנות רוצות להכיר למטרת עיסוי אירוטי באילת. חפשו את הבחורות המפתות ביותר בעיתונים או תשאלו את חבריכם. כן, לא הדם וחילוף החומרים בגוף וכך מסייע לשמור על הבריאות שלכם. העיסוי משחרר את כל השרירים התפוסים ומסלק את כל הכאבים שאיתם הסתובבתם כל מודעת הנאה
blog link Credit cards
Discover the best Nicolthebaddie nude on webcam for live porn video chat ever for free!
Nude amateur webcams woman online porn showNaked hot webcams g d57ad8_
Our store offers authentic Instagram accounts with high follower counts, perfect for boosting your social media
presence instantly. Secure transactions and reliable customer support ensure a seamless experience.
Enhance your Instagram influence with our premium accounts today!
Instagram audience.
בחדר מלון, או להגיע למקום דיסקרטי בו הבחורה חיה ועובדת. הזמנת דייט עם מי שאתם אוהבים היא קלה ופשוטה: התקשרו למספר הטלפון של נערות ליווי. בדיוק מסיבה זו ישנן דירות מפגש דיסקרטיות המאפשרות לקיים מפגשים סוערים בפרטיות ובתנאים נוחים עם נערות ליווי בבת ליווי תמונות אמתיות
social interaction adds a new layer of excitement and competition to the game, making it more engaging and play game
click here to find out more Best cc+cvv
похудение для женщин похудение для женщин .
5]Balanset-1A Sale: Your Ideal Tool for Balancing and Vibration Analysis
4]Device Description:
Balanset-1A is a dual-channel device for balancing and vibration analysis, ideal for balancing rotors such as crushers, fans, grain harvester choppers, shafts, centrifuges, turbines, and more.
4]Features:
3]Vibrometer Mode:
Tachometer: Accurately measures rotation speed (RPM).
Phase: Determines the phase angle of vibration signals for precise analysis.
1x Vibration: Measures and analyzes the main frequency component.
FFT Spectrum: Provides a detailed view of the vibration signal frequency spectrum.
Overall Vibration: Measures and monitors overall vibration levels.
Measurement Log: Saves measurement data for analysis.
3]Balancing Mode:
Single-Plane Balancing: Balances rotors in a single plane to reduce vibration.
Two-Plane Balancing: Balances rotors in two planes for dynamic balancing.
Polar Diagram: Visualizes imbalance on a polar diagram for precise weight placement.
Last Session Recovery: Allows resuming the previous balancing session for convenience.
Tolerance Calculator (ISO 1940): Calculates allowable imbalance values according to ISO 1940 standards.
Grinding Wheel Balancing: Uses three correction weights to eliminate imbalance.
3]Diagrams and Graphs:
General Graphs: Visualization of overall vibration.
1x Graphs: Display of main frequency vibration patterns.
Harmonic Graphs: Show the impact of harmonic frequencies.
Spectral Graphs: Graphical representation of the frequency spectrum for in-depth analysis.
3]Additional Features:
Archiving: Storage and access to previous balancing sessions.
Reports: Generation of detailed reports on balancing results.
Rebalancing: Easily repeat the balancing process using saved data.
Serial Production Balancing: Suitable for balancing rotors in serial production.
Imperial and Metric System Options: Provides compatibility and convenience worldwide.
4]Price:
€1751
3]Package Includes:
Measurement unit
Two vibration sensors
Optical sensor (laser tachometer) with magnetic stand
Weights
Software (laptop not included, available as an additional order)
Plastic carrying case
Buy Portable balancer and Vibration Analyzer
Order Balanset-1A today and ensure precise balancing of your rotors!
blog link Best cc shop
helpful hints carding 2024
Amazing! This blog looks exactly like my old one!
It’s on a entirely different subject but it has pretty much the
same layout and design. Outstanding choice of colors!
Nice articl! Just check this out!
Naked amateur camsNaked amateur cams 42dacc5
click this site Best cc+cvv
купить диплом в краснодаре http://www.damdesign.ru .
click this over here now Best cc+cvv
site Best cc shop
next carding 2024
bellingham jude
Match Superb Online Casinos in the Sphere 2023. Unequalled online casino aggregator.
https://bellingham-judefr.biz
купить диплом в улан-удэ купить диплом в улан-удэ .
купить диплом вуза diplomvash.ru .
Just check this out, Helen-Rosse1 xxx nude on webcam – Live Sex Chat
Naked amateur webcaNude amateur cams d57ad0_
games that stood out from traditional casino offerings. Inspired by the concept of high-risk, high-reward, the aviator demo game
buy cc with high balance Good validity rate Purchasing Make good job for MMO Pay in web activate your card now for worldwide transactions.
————-CONTACT———————–
WEBSITE : >>>>>> CvvBest✻CC
—- HERE COMES THE PRICE LIST ———–
***** CCV US:
– US MASTER CARD = $2,4 per 1 (buy >5 with price $3 per
1).
– US VISA CARD = $2,9 per 1 (buy >5 with price $2.5 per 1).
– US AMEX CARD = $3,9 per 1 (buy >5 with price $2.5 per 1).
– US DISCOVER CARD = $3,8 per 1 (buy >5 with price $3.5 per 1).
– US CARD WITH DOB = $15 per 1 (buy >5 with price $12 per 1).
– US FULLZ INFO = $40 per 1 (buy >10 with price $30 per 1).
***** CCV UK:
– UK CARD NORMAL = $3,3 per 1 (buy >5 with price $3
per 1).
– UK MASTER CARD = $2,4 per 1 (buy >5 with price $2.5 per 1).
– UK VISA CARD = $2,7 per 1 (buy >5 with price $2.5 per 1).
– UK AMEX CARD = $3 per 1 (buy >5 with price $4 per 1).
$2,2
– UK CARD WITH DOB = $15 per 1 (buy >5 with price $14 per 1).
– UK WITH BIN = $10 per 1 (buy >5 with price $9
per 1).
– UK WITH BIN WITH DOB = $25 per 1 (buy >20 with price $22 per 1).
– UK FULLZ INFO = $40 per 1 (buy >10 with price $35 per
1).
***** CCV AU:
– AU MASTER CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU VISA CARD = $5.5 per 1 (buy >5 with
price $5 per 1).
– AU AMEX CARD = $8.5 per 1 (buy >5 with price $8 per 1).
– AU DISCOVER CARD = $8.5 per 1 (buy >5 with price $8 per 1).
***** CCV CA:
– CA MASTER CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA BUSINESS = $14 per 1 (buy >5 with price $13 per
1).
see it here Credit cards
Hey there! This is kind of off topic but I need some help from an established blog. Is it tough to set up your own blog? I’m not very techincal but I can figure things out pretty fast. I’m thinking about creating my own but I’m not sure where to start. Do you have any tips or suggestions? Cheers
купить диплом в дербенте
https://goup.hashnode.dev/kupit-nastoyashij-diplom-professionalnye-uslugi
http://ya.10bb.ru/viewtopic.php?id=3355#p6110
http://zxz.listbb.ru/viewtopic.php?f=7&t=1350
http://polegasm.net/index.php/forum/welcome-mat/151440
http://hitman.getbb.ru/viewtopic.php?f=16&t=832
купить диплом в вольске
Do you have a spam problem on this blog; I also am a blogger, and I was wanting to know your situation; many of us have developed some nice methods and we are looking to swap solutions with others, be sure to shoot me an email if interested.
купить диплом с реестром
https://ya.7bb.ru/viewtopic.php?id=11094#p32305
http://sharecovid19story.com/viewforum.php?f=11
http://injectorcar.ru/forum/member.php?u=34916
http://publikacii.listbb.ru/viewtopic.php?f=3&t=587
https://www.cyberpinoy.net/read-blog/20621
купить диплом в каменске-уральском
Самые популярные pin up костюмы, для уникального вида
pinup oficial https://pinupbrazilnbfdrf.com/ .
Discover the best RangerRuu nude on webcam in Live Sex Chat ever for free!
Nude hot webcams giNude amateur webcam bfee0b6
Как сделать идеальное фото в pin up стиле, которое покорит всех
pin up oficial https://pinupbrazilnbfdrf.com/ .
купить диплом в тюмени http://www.damdesign.ru/ .
Проведение независимой строительной экспертизы — сложный процесс, требующий глубоких знаний. Наши специалисты обладают всеми необходимыми навыками, а их заключения часто служат основой для принятия верных стратегических решений. Строительно-техническая экспертиза https://stroytehexp.ru позволяет выявить факторы, вызвавшие ухудшение эксплуатационных характеристик объектов, проверить соответствие возведённых зданий градостроительным нормам.
The Aviator Game is an exciting online casino game that has captivated players worldwide with its unique blend
aviator game online
Секреты стиля в моде pin up, которые важно учесть
casino pin up casino pin up .
Добро пожаловать в студию ландшафтного дизайна Green History! Мы предлагаем полный спектр услуг по благоустройству и озеленению территорий. От уникальных ландшафтных проектов до установки систем автоматического полива – мы делаем всё для создания уютных и красивых садов. Посетите наш сайт greenhistory.ru и узнайте больше о наших услугах. Наш офис находится по адресу: г. Москва, Дмитровское шоссе, дом 100, корп 2, офис 418.
Вы мечтаете о прекрасном саде? Green History воплотит ваши мечты в реальность! Мы используем только лучшие материалы и современные технологии для создания уникальных ландшафтных решений. Свяжитесь с нами через сайт greenhistory.ru или посетите нас по адресу: г. Москва, Дмитровское шоссе, дом 100, корп 2, офис 418. Превратите свой участок в настоящий оазис с нашей помощью!
https://www.premcosmeticsraipur.com/ritual08/
https://nerdgaming.science/wiki/Ritual02
This is really interesting, You’re a very skilled blogger.
I’ve joined your feed and look forward to seeking more of your
excellent post. Also, I have shared your website in my social networks!
my blog … zaporojie01
Как внедрить pin up в повседневность, для стильного городского вида
bonus pin up bonus pin up .
Excellent and high-quality kiragold nude on cam in her Live Sex Chat Room absolutely free and easy to watch on any device, just
Naked amateur webcaNude hot webcams wo 942dacc
The story of Mbappe’s https://www.asma-online.org rise to fame is as remarkable as his on-field feats. Mbappe’s journey from local pitches to global arenas was meteoric. His early days at AS Monaco showcased his prodigious talent, with his blistering speed and fearless dribbling dismantling opposition defenses.
Ncfyv_ncyuhv nude strip on cam for live sex chat absolutely free and easy to watch on any device, just
Naked hot cams woman online sex charNude amateur cams girls live porn show e0b6b69
whether at home or on the go.
aviator demo game
http://www.peregonavtofgtd.kiev.ua
Быстро, эффективно а также фундаментально перевезти Ваш ярис с Украины в течение Европу, или из Европы в течение Украину вместе с нашей командой. Оформление документов и экспортирование изготовляются в оклеветанные сроки.
peregonavtofgtd kiev ua
Информационный ресурс https://ardma.ru, посвящен бизнесу, финансам, инвестициям и криптовалютам. Сайт предлагает экспертные статьи, аналитические отчеты, стратегии и советы для предпринимателей и инвесторов. Здесь можно найти новости и обзоры о бизнесе, маркетинге, трейдинге, а также практические рекомендации по различным видам заработка и управлению финансами.
купить аттестат за 9 классов http://damdesign.ru .
https://bimworx.net/user/bob-vlander/profile/info
https://180degreehealth.com/180forums/users/valderog/
https://multichoicetalentfactory.com/user/57378
https://esteri.uilpa.it/forum/user/2045-trondas.html
https://goli.breezio.com/user/Slomar
https://www.energyplan.eu/forums/users/Alberon/
https://www.flexicontent.org/forum/user/20044-bordano.html
https://www.nexusdb.com/forums/member.php?u=19034
https://forums.elementalgame.com/user/7354393
https://huayra.educar.gob.ar/ayuda/?qa=user/Jushoriax
https://forum.aigato.vn/user/qislanai
https://www.embedded-software-engineering.de/community/user/andreasandreas013
https://forum.faforever.com/user/zinaur
https://www.rcweb.de/index.php/User/16507-Sbancta/?editOnInit=true#about
https://www.chambers.com.au/forum/view_post.php?frm=2&pstid=57182
https://www.khedmeh.com/wall/forum/topic/26982
https://www.guildlaunch.com/guild/forums/viewtopic.php?p=40248951&gid=48#40248951
http://nexusstem.co.uk/community/main-forum/ripetitore-5g-del-segnale-cellulare/
http://biznas.com/Biz-postsm284113_Amplificatore-segnale-rete-TIM-3G-4G.aspx#post284113
https://www.tapatalk.com/groups/renotalkfr/viewtopic.php?f=33&t=245251&from_new_topic=1
https://archives.profsurv.com/forum/Professional-Surveyor-Magazine-Discussion/Problem-Corner/-132588.aspx
https://www.reisezielforum.de/viewtopic.php?t=63424
http://users.atw.hu/nlw/viewtopic.php?p=42398#42398
https://www.hebergementweb.org/threads/dove-posso-acquistare-un-ripetitore-di-segnale-mobile.1251179/
https://forum.trackandfieldnews.com/special/albums/1829937-come-installare-un-amplificatore-di-segnale-mobile
http://www.horawej.com/index.php?lay=boardshow&ac=webboard_show&WBntype=1&Category=horawejcom&thispage=4&anspage=1&No=1262877
https://www.vidpaw.com/topics/best-youtube-video-downloader-mac.html
Un amplificatore di segnale per cellulare GSM, 4G/LTE, UMTS e una soluzione eccezionale per chiunque abbia problemi di ricezione. Questo dispositivo potenzia il segnale per tutti gli operatori mobili, garantendo chiamate chiare e connessioni internet veloci anche nelle zone piu remote. Immagina di poter lavorare da casa senza interruzioni o guardare video in streaming senza buffering! L’installazione e semplice e rapida, e il miglioramento del segnale e immediato. E un investimento che vale ogni centesimo per chi desidera una connettivita affidabile e continua. Non lasciare che un segnale debole ti rallenti, scegli un amplificatore di segnale e goditi una copertura perfetta ovunque tu sia!
https://medialoot.com/blog/how-to-make-tv-static-noise-in-photoshop/
https://www.makexyz.com/f/405bc467fcbe33d9a9d40048392c3e32
https://profere.uvci.edu.ci/forum/public/d/12985-la-mia-esperienza-di-acquisto-di-un-amplificatore-di-segnale-mobile
http://journals.hnpu.edu.ua/index.php/literature/comment/view/4159/889/11870
https://portal.uaptc.edu/ICS/Campus_Life/Campus_Groups/Amicus_Curiae_Paralegal_Club/Discussion.jnz?portlet=Forums&screen=PostView&screenType=change&id=2f996256-0feb-4f6d-be94-e616d7e50a77
https://sites.google.com/view/segnale-cellulare4g/
https://amplificatore-segnale-cellulare.mystrikingly.com/
https://articworlds.blogspot.com/2024/04/i-vantaggi-dellutilizzo-degli.html
https://www.gamerlaunch.com/community/users/blog/6398497/2281879/gli-amplificatori-di-segnale-per-vodafone-e-la-cop/?gid=535
https://companylistingnyc.com/listings/miglioramenti-della-copertura-e-della-qualita-del-segnale-con-gli-amplificatori-per-windtre/
https://artistecard.com/ericyoung#!/news/2024/82208
https://webhitlist.com/profiles/blogs/guida-all-acquisto-di-un-amplificatore-di-segnale-cellulare-cosa
https://www.evernote.com/shard/s627/sh/3c2dce1c-d981-d5b4-37d8-74017a9e91bb/QM8z9ncRFbxTx7mVlUGRL-9b0L-M681l3iTXNpZJLJ-3EGnoEt6stFZm9A
https://webyourself.eu/blogs/361277/Amplificatori-di-Segnale-Cellulare-4G-Confronto-tra-i-Principali-Modelli
https://heyjinni.com/read-blog/70670
https://www.merchantcircle.com/blogs/1win-casino-climax-mn/2024/4/Risoluzione-dei-problemi-al-segnale-cellulare-con-TIM-Telecom-Italia/2710323
https://theomnibuzz.com/amplificatori-di-segnale-per-vodafone-risoluzione-dei-problemi-e-suggerimenti-per-massimizzare-lefficacia/
https://community.wongcw.com/blogs/768802/Scegliere-il-Miglior-Amplificatore-di-Segnale-per-WindTre-Fattori-da
Wow, fantastic blog layout! How long have you been blogging for? you make blogging look easy. The overall look of your site is excellent, let alone the content!
comunicazionesviluppoenpa.org/enpashop/collection/larte-di-depsa
pdtplanilla.com/la-nueva-normalidad-y-la-gestion-de-recursos-humanos/
http://www.agdp1.ru/employees/426/review/?PAGEN_1=12
allukrnews.ru/put-k-professionalnomu-priznaniyu-pokupka-diploma-kak-reshenie/
yaoisennari.ekafe.ru/viewtopic.php?f=169&t=1669&start=0&view=print
На сайте https://esdogames.ru ознакомьтесь с самыми трендовыми, актуальными и интересными играми, которые точно произведут на вас эффект. Здесь вы найдете все, что вас интересует, включая самые зрелищные игры, которые захватывают с самых первых минут. Также представлен список лучших игр за 2024 год. Вы сможете поиграть во все, что хочется, прямо сейчас. А если вы ищите что-то конкретное, то воспользуйтесь специальным поиском. Подберите игру по жанру, режиму игры, платформе, чтобы облегчить поиск.
This web site truly has all the info I wanted concerning this subject and didn’t know who to ask.
https://roblox-studio-scripts.ru/profile/6518-miguelpbum/
http://xn--80aeh5aeeb3a7a4f.xn--p1ai/forum/user/50748/
http://forums.indexrise.com/thread-35892-post-205028.html#pid205028
http://www.musichunt.pro/blogs/view.htm?id=79114
http://horordark.ru/realno-li-kupit-diplom-razbiraem-podrobnosti
магниты +с логотипом – объемные магнитики, магнитная закладка производство
In 2024, the best business process management (BPM) software is revolutionizing the way organizations operate. Leading the pack are solutions like Nintex, Bizagi, and Appian, which offer unparalleled efficiency, automation, and customization. These platforms streamline workflows, reduce errors, and enhance productivity, making them indispensable for businesses striving for excellence. With features like real-time analytics, seamless integration with existing systems, and user-friendly interfaces, they empower companies to adapt swiftly to market changes. Investing in top-tier BPM software is a game-changer, ensuring your business stays ahead of the curve, delivering exceptional results and fostering continuous improvement. Don’t miss out on the future of business optimization!
https://www.rcweb.de/index.php/User/16897-Bareiteraw/#about
https://www.pinlap.com/Gudal
https://180degreehealth.com/180forums/users/Bareiteraw88/
https://www.chumsay.com/BarcleRoberts
https://huayra.educar.gob.ar/ayuda/?qa=user/kapes
http://www.sunnetrehberi.com/forum/profile/kapes
https://cndt.ro/community/profile/kapes/
https://earthpeopletechnology.com/forums/profile/kapes
https://messenger.wepluz.com/kapes
https://forum.aigato.vn/user/kapes
https://bimworx.net/user/kapes-maro/profile/
https://community.odesd2.com/user/kapesfurio
https://forum.citadel.one/user/kapes
https://openlibrary.org/people/kapes
http://users.atw.hu/nlw/viewtopic.php?p=43016
https://www.geschichteboard.de/ptopic,203631.html
https://robotech.com/forums/viewthread/2223036
https://haze-growroom.de.tl/Forum/topic-3215-1-Benefits-of-Business-Process-Automation.htm
https://roughstuffmedia.activeboard.com/t70760319/capex-approval-management-software/
https://www.caregiveraction.org/community/welcome/general-discussion/document-management-modern-business
https://lifeisfeudal.com/Discussions/question/improving-and-changing-the-business-model
http://www.harderfaster.net/?sid=36d1c874065962176b9943bf3ac10a8c§ion=forums&action=showthread&forumid=1&threadid=320390
https://allaboutschool.activeboard.com/t70759208/benefits-of-business-process-automation/
https://communityofbabel.com/en/forums/discussion/middle-east-culture/the-capital-investment-process
https://crpsc.org.br/forum/viewtopic.php?f=3&t=396250
https://www.mycast.io/stories/playtown/roles/steggy/50418578
https://buymeacoffee.com/bloging/wugolewewe
https://medialoot.com/blog/how-to-easily-expand-images-in-photoshop/
https://devfolio.co/projects/medicad-fcd1
https://sites.uw.edu/trawlingbp/your-comments/comment-page-141/
https://blog.stcloudstate.edu/hied/2021/09/28/national-hispanic-heritage-month/
https://www.bu.edu/bhr/2020/06/25/adaptation-restaurants-maneuver-in-response-to-covid-19/
https://sites.google.com/view/bpa-software/
https://capex-approval-management.mystrikingly.com/
https://articworlds.blogspot.com/2024/05/introduction-to-document-tracking.html
https://www.mycitizensnews.com/author/RolandReese/
https://www.marqueze.net/miembros/kevinwest/profile/classic/
https://promosimple.com/ps/2c96c/how-bpa-software-can-streamline-workflow-and-increase-efficiency
https://webhitlist.com/profiles/blogs/the-importance-of-efficient-capex-approval-processes-how-software
https://www.gamerlaunch.com/community/users/blog/6398497/2276531/streamlining-document-processes-with-cmw-labs-docu/?gid=535
https://we.riseup.net/johnsteele/the-role-of-low-code-platforms-in-digital-transfor
https://www.lookingforclan.com/clans/implementing-agile-methodologies-bpm-software-flexibility-and-adaptability-2024
https://www.flickr.com/groups/14870348@N21/discuss/72157721921098023?new
https://letterboxd.com/clydearter/list/benefits-of-implementing-capex-approval-software/
https://vizi.vn/read-blog/59643
https://biiut.com/read-blog/53708_enhancing-business-efficiency-and-productivity-with-cmw-lab-039-s-platform.html
https://www.merchantcircle.com/blogs/1win-casino-climax-mn/2024/5/The-Role-of-BPM-Software-in-Agile-Product-Development/2733505
https://webyourself.eu/blogs/333651/Top-Features-to-Look-for-in-Business-Process-Automation-Tools
https://community.wongcw.com/blogs/752401/How-CapEx-Approval-Software-Improves-Financial-Control-and-Oversight
https://www.debwan.com/blogs/551110/Enhancing-Collaboration-and-Communication-with-Document-Tracking-Software-CMW-Lab
https://rollbol.com/blogs/1857430/Exploring-the-Features-of-CMW-Lab-s-Low-Code-Process
https://www.storeboard.com/blogs/business/harnessing-artificial-intelligence-in-bpm-software/5776178
За более чем 15 лет работы Green History стала символом качества и профессионализма в мире ландшафтного дизайна. Мы предлагаем полный комплекс услуг: от проектирования уникальных ландшафтных решений до установки систем автоматического полива и мощения дорожек. Наши специалисты создают идеальные газоны и озеленяют территории, превращая их в настоящие произведения искусства. Посетите наш сайт greenhistory.ru или наш офис в Москве: Дмитровское шоссе, дом 100, корп 2, офис 418.
Мы гордимся своим опытом и вниманием к деталям. Каждый проект для нас – это возможность создать что-то уникальное и красивое. Используя лучшие материалы и новейшие технологии, мы гарантируем долговечность и эстетическую привлекательность наших решений. За более подробной информацией заходите на greenhistory.ru или приходите к нам в офис по адресу: г. Москва, Дмитровское шоссе, дом 100, корп 2, офис 418. Превратите свой сад в оазис вместе с Green History.
Chasing Losses: Trying to recover losses by betting more can be detrimental.
aviator game
Pin up в музыке: история и влияние, для яркого стиля
pin up como funciona pin up como funciona .
цены и графики криптовалют – биткоин калькулятор, Курсы криптовалют
Добрый день всем!
Наша компания поможет вам купить диплом ВУЗа с гарантией качества и доставкой в любой регион России!
http://www.lhotkanet.cz/galerie/profile.php?uid=73311
http://vipmails.0pk.me/viewtopic.php?id=5072#p11842
http://kadastr.bestbb.ru/viewtopic.php?id=1111
https://risefundraising.com/meet-the-new-prefix-mx/#comment-10049
http://forumtrolley.mybb.ru/viewtopic.php?id=306#p498
Здравствуйте!
Недорого предлагаем заказать диплом без предоплаты с доставкой курьером по РФ, под ключ!
http://vseamoskva.flybb.ru/topic592.html
http://serialforfree.ru/kupit-diplom-vash-shans-stat-luchshim-v-svoey-oblasti
http://www.matchfishing.ru/forumtest/1/member.php?u=23110
http://oriondtdm.blogspot.com/2018/11/blog-post_5.html
http://crimea.bestbb.ru/viewtopic.php?id=441
Real Madrid midfielder Rodrigo https://rodrygo.prostoprosport-ar.com gave Madrid the lead in the Champions League quarter-final first leg against Manchester City. The meeting takes place in Madrid. Rodrigo scored in the 14th minute after a pass from Vinicius Junior.
где купить диплом damdesign.ru .
Wow! This blog looks just likke my old one! It’s on a entirelyy different
topic but it has pretty much the same layout and design. Superb choice
oof colors!
Also visit my page :: 대출사이트
https://globals-melbet.ru/
Rise to the top
https://bit.ly/4bdMuAg
южный парк онлайн бесплатно южный парк
Yes, the Aviator Game is compatible with mobile devices. Players can enjoy the game on their smartphones or
play game
электрокамин с доставкой – купить электрокамин недорого, электрокамины недорого интернет магазин в москве
Hi there to all, how is the whole thing, I think every one is getting more from this web page, and your views are nice for new users.
купить диплом в кстово
https://idi.atu.edu.iq/?p=5616
http://linux.listbb.ru/viewtopic.php?f=2&t=419
http://avrorp.getbb.ru/viewtopic.php?f=183&t=587
http://revolverp.forumex.ru/viewtopic.php?f=11&t=218
https://bezone.ru/node/336556
купить диплом переводчика
It’s awesome in support of me to have a website, which is useful designed for my know-how. thanks admin
купить диплом гознак
http://86hm.ru/forum/flame/?topic_id=24934
http://wiki.author-alarm.ru/index.php/пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ
http://abroad.ekafe.ru/viewtopic.php?f=5&t=1826
http://x91392sl.beget.tech/2024/05/31/kupit-diplom-v-moskve-vash-lichnyy-put-k-uspehu.html
http://video.listbb.ru/viewtopic.php?f=3&t=324
купить диплом медицинского училища
ремонт ноутбуков в москве
Any work should open with the question “why?” The stroibloger.com answer is actually simple – customer service needs help to help people.
stagramer.com
доставка цветов на дом Киев – букет цветов Киев, купить розы Киев
Широчайший ассортимент военных товаров|Ваш надежный партнер в выборе военных товаров|Купите военную амуницию у нас|Вся необходимая экипировка для военных|Выбор настоящих военных победителей|Профессиональное снаряжение для военных|Боевая техника для суровых реалий|Только качественные товары для военных задач|Выбирайте только профессиональное снаряжение|Все для армии и спецслужб|Выбирайте только надежные военные товары|Выбор профессионалов в военной отрасли|Только качественные товары для военного применения|Оружие и экипировка для настоящих героев|Амуниция и снаряжение от лучших производителей|Боевое снаряжение от ведущих брендов|Армейский магазин с широким выбором экипировки|Купите профессиональное снаряжение для службы|Качественные товары для военных целей|Оружие и экипировка для тех, кто выбирает победу
магазин військового одягу магазин військового одягу .
купить квартиру в казани https://nedvizhimost-47.ru
Scoring System and Winning Criteria
play game
На сайте https://umnye-roboty-pylesosy.ru/ вы сможете приобрести умного робота-пылесоса, который порадует своей качественной работой. К его важным преимуществам относят эффективную, быструю, точную работу. А управление происходит при помощи смартфона. Предусмотрены различные параметры чистки, которые выбирают в соответствии с типом напольного покрытия. При выборе стоит учесть и габариты изделия, чтобы оно легко передвигалось по полу. Также важны и дополнительные функции, которые повысят комфорт.
Широчайший ассортимент военных товаров|Оружие и снаряжение для настоящих мужчин|Купите военную амуницию у нас|Спецодежда и обувь для армии|Выбор настоящих военных победителей|Только проверенные боевые товары|Боевая техника для суровых реалий|Купите все необходимое для военной службы|Специализированный магазин для настоящих военных|Снаряжение от лучших производителей|Выбирайте только надежные военные товары|Боевая техника для самых сложных задач|Выбирайте только профессиональное снаряжение|Купите только проверенные военные товары|Выбор профессионалов в военной сфере|Экипировка для защитников Отечества|Армейский магазин с широким выбором экипировки|Оружие и снаряжение для успешных миссий|Качественные товары для военных целей|Боевое снаряжение для самых требовательных задач
інтернет магазин військового одягу інтернет магазин військового одягу .
Лучший выбор военной экипировки|Оружие и снаряжение для настоящих мужчин|Специализированный магазин для военных|Спецодежда и обувь для армии|Оружие и аксессуары для профессионалов|Защита и безопасность в вашем распоряжении|Выбирайте только лучшее для себя|Армейский магазин с широким ассортиментом|Оружие и снаряжение для любых задач|Все для армии и спецслужб|Выбирайте только надежные военные товары|Боевая техника для самых сложных задач|Армейский магазин с высоким уровнем сервиса|Специализированный магазин для профессионалов|Специализированный магазин для военных операций|Боевое снаряжение от ведущих брендов|Армейский магазин с широким выбором экипировки|Оружие и снаряжение для успешных миссий|Выбор настоящих защитников|Выбирайте только надежные военные товары
магазин військового одягу магазин військового одягу .
Наша компания осуществляет печать фото на холсте с возможностью недорогой доставки. Опыт команды и наличие необходимого оснащения позволяет нам справляться с любыми задачами оперативно и на профессиональном уровне печать фотоальбома
https://photoges.ru/
anonymous
Here’s what you should be aware of
Создать бота для телеграмм магазина – сделать телеграмм бота для продажи товаров, сделать магазин бота в телеграм
Register an account, make a deposit, and navigate to the Aviator Game to start playing.
aviator demo online
Лучший выбор военной экипировки|Боевая техника от лучших производителей|Купите военную амуницию у нас|Спецодежда и обувь для армии|Оружие и аксессуары для профессионалов|Защита и безопасность в вашем распоряжении|Боевая техника для суровых реалий|Только качественные товары для военных задач|Оружие и снаряжение для любых задач|Все для армии и спецслужб|Качественная экипировка для армии|Выбор профессионалов в военной отрасли|Только качественные товары для военного применения|Специализированный магазин для профессионалов|Специализированный магазин для военных операций|Выбор настоящих защитников|Армейский магазин с широким выбором экипировки|Специализированный магазин для военных сотрудников|Качественные товары для военных целей|Боевое снаряжение для самых требовательных задач
військовий інтернет магазин https://magazinvoentorg.kiev.ua/ .
перейдите на этот сайт
Взрослый бизнес: История 2023 смотреть онлайн в хорошем качестве
Discover the perfect Instagram accounts for sale at our store.
We offer authentic, high-follower profiles to boost your social media presence instantly.
Ideal for influencers and businesses, our accounts come with secure transactions and excellent
customer support. Enhance your Instagram strategy with
our premium selection today! Cheap Instagram accounts.
teplica-parnik.net
Welcome to our store, where you can find a diverse
selection of authentic Instagram accounts tailored to boost your social media presence.
Ideal for individuals and businesses, our accounts come with large, engaged follower bases, enhancing
your credibility instantly. We prioritize secure transactions and exceptional customer support.
Start growing your Instagram influence today with our premium
accounts! Purchase Instagram accounts.
Origins of the Aviator Game
play demo
Our store specializes in offering a diverse selection of authentic Instagram accounts, ideal for those seeking
instant access to large audiences and increased credibility.
Whether you’re an individual or a business looking to enhance your social
media presence, our premium accounts provide a competitive edge.
We guarantee secure transactions and exceptional customer support to ensure a seamless experience.
Elevate your Instagram strategy with our trusted, high-quality accounts today!
Instagram profiles for sale.
7k казино официальный
Только качественные товары для военных|Боевая техника от лучших производителей|Купите военную амуницию у нас|Армейские товары по выгодным ценам|Оружие и аксессуары для профессионалов|Защита и безопасность в вашем распоряжении|Боевая техника для суровых реалий|Только качественные товары для военных задач|Оружие и снаряжение для любых задач|Снаряжение от лучших производителей|Снаряжение для профессионалов военного дела|Боевая техника для самых сложных задач|Армейский магазин с высоким уровнем сервиса|Купите только проверенные военные товары|Выбор профессионалов в военной сфере|Боевое снаряжение от ведущих брендов|Выбирайте проверенные военные товары|Оружие и снаряжение для успешных миссий|Качественные товары для военных целей|Боевое снаряжение для самых требовательных задач
магазин військового одягу магазин військового одягу .
Our store specializes in selling authentic Instagram accounts with high follower counts.
Ideal for individuals and businesses looking to boost their social media presence, we provide secure
and hassle-free transactions. Gain instant credibility and reach your target audience effectively with our premium Instagram
accounts. Start growing your influence today!
Instagram account seller.
Discover our selection of authentic Instagram accounts, designed to give you instant access to large audiences and boost your social media credibility.
Ideal for influencers, businesses, and personal brands, we offer secure transactions
and exceptional customer support. Elevate your
Instagram presence effortlessly with our premium accounts.
Start growing your followers and engagement today! Instagram accounts for sale.
find out here now AI in financial transactions
Welcome to our store, your trusted destination for authentic Instagram accounts.
We offer a diverse selection of accounts with high follower counts, perfect for individuals and businesses looking to enhance their social media presence instantly.
Our accounts provide immediate access to large, engaged
audiences, boosting your credibility and visibility.
With secure transactions and dedicated customer
support, we ensure a seamless purchasing experience.
Whether you’re aiming to grow your personal brand or promote your
business, our premium Instagram accounts are your gateway to success.
Elevate your Instagram game with us today! Pre-owned Instagram
accounts.
loan default rates Those companies then sell that data to actual payday lenders, creating another avenue in which criminals can get their hands on personal data – either through a hack or by purchasing the information.
How to Play the Aviator Game
Aviator game app
Welcome to our store, where you can find a wide selection of authentic Instagram accounts tailored to meet your social media needs.
Whether you’re an individual looking to enhance your personal brand or a business aiming to expand your online
presence, our premium accounts offer instant access to large audiences and increased
credibility. We prioritize secure transactions and provide reliable
customer support to ensure a smooth purchasing
experience. Boost your Instagram game effortlessly with
our high-quality accounts, and start engaging with a ready-made audience today!
Shop with us for the best Instagram accounts available.
Pre-owned Instagram accounts.
Welcome to our store, where you can find a wide selection of authentic Instagram accounts tailored to boost your social media presence.
We provide instant access to large audiences, enhancing your credibility and engagement.
Ideal for individuals and businesses, our secure transactions and dedicated customer support ensure a seamless experience.
Elevate your Instagram game with us today!Instagram profile shop.
right here tronlink wallet extension
купить квартиру в казани https://kupit-kvartiru47.ru
читать
MARVEL смотреть фильмы и сериалы в хорошем качестве
With the right approach, the besttoday.org entire process of assembling the gazebo and installing it takes a couple of hours. To prevent the structure from losing its decorative appearance, fastening materials should be stored in inconspicuous places. Or close them with special devices.
Карьерный коуч https://vminske.by/fashion/kto-takie-karernye-konsultanty — эксперт рынка труда, который помогает людям определить свои карьерные цели, развиваться в выбранной области и достигать успеха в профессиональной деятельности.
Our store specializes in providing authentic Instagram accounts with substantial followings, perfect for individuals and businesses
looking to enhance their social media presence instantly.
We offer a wide selection of accounts to fit various niches and goals, ensuring that
you can find the ideal match for your needs. With secure transactions and dedicated
customer support, we make the process of purchasing Instagram accounts simple and reliable.
Boost your credibility, engagement, and growth with our
premium Instagram accounts today! Business Instagram accounts.
Шале в Жабляке – Kuca u Crnoj Gori, House with hot tube in the mountains
Porodicne odmaralisne kuce u Crnoj Gori – Hot tube, Аренда коттеджей в Жабляке
Интересно: полиуретановая антигравийная пленка на автомобиль или пленка хамелион
Может быть полезным: https://autoplenka.com/product/cilikonovaya-vygonka-bluemax-goluboj-neon-trapecziya-srednyaya-zhestkosti/ или антигравийная пленка отзывы
Ещё можно узнать: сообщение на тему пещеры
Our store specializes in selling authentic Instagram accounts,
offering immediate access to large, engaged audiences. Ideal for individuals and businesses looking to enhance
their social media presence, our accounts provide credibility and rapid
growth potential. We prioritize secure transactions and exceptional
customer support, ensuring a smooth and reliable buying experience.
Elevate your Instagram strategy effortlessly with our
premium, ready-to-use accounts. Start achieving your social
media goals today! Instagram promotion.
Today, while I was at work, my sister stole my iphone and tested to see if it can survive a 30 foot drop, just so she can be a youtube sensation. My apple ipad is now broken and she has 83 views. I know this is entirely off topic but I had to share it with someone!
купить диплом машиниста
http://webnewsrealty.ru/kupit-diplom-rf-v-moskve-ofitsialnoe-oformlenie-i-dostupnyie-tsenyi
https://epistles.ru/blogs/786/ѕокупка-академических-дипломов
https://vipka.mybb.ru/viewtopic.php?id=2786#p4841
http://bl.com.tw/index.php?title=пїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ:_пїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ
http://silich.ru/forum/member.php?u=4810
купить диплом в москве
Howdy superb blog! Does running a blog such as this require a massive amount work? I’ve absolutely no knowledge of coding but I was hoping to start my own blog in the near future. Anyway, should you have any suggestions or tips for new blog owners please share. I understand this is off subject however I simply wanted to ask. Appreciate it!
купить диплом в якутске
http://x70795vj.beget.tech/2024/05/27/kupit-diplom-reshenie-dlya-vashey-karery.html
http://astroroleplay.getbb.ru/viewtopic.php?f=6&t=397
http://p99946c6.beget.tech/2024/05/28/kupit-diplom-rf-v-moskve-legalno-i-konfidencialno.html
http://www.mirmafii.ru/article/7314
https://belydom.ru/forum/user/37501/
купить диплом в томске
Our store specializes in providing authentic Instagram accounts, offering instant access to large, engaged audiences.
Ideal for influencers, businesses, and marketers looking to
boost their social media presence, we ensure secure
transactions and reliable customer support.
With a variety of accounts to choose from, elevate
your Instagram strategy effortlessly and achieve your goals faster
with our premium services. Instagram influencers.
Check This Out activate tronlink account
Izdavanje vikendica na Durmitoru – Izdavanje vikendica na Durmitoru, House rental in Montenegro
right here tronlink wallet extension
На сайте https://moredoram.ru вы найдете дорамы, фильмы, сериалы высокого качества. Они понравятся всем любителям такого жанра и помогут расслабиться после трудового дня и просто получить приятные эмоции. Вы сможете воспользоваться функцией случайной дорамы, изучить список лучших из них. Все они в отличном качестве, с безупречным звуком, что позволит насладиться просмотром на любом устройстве, включая смартфон, ПК, планшет. Регулярно появляются многообещающие новинки, с которыми необходимо ознакомиться и вам.
Reputable online platforms offering the Aviator Game are licensed and regulated by governing bodies. This
Aviator demo play online free
Организация реализует качественные решения по технической поддержке ресурса на https://podderzhka-dlya-saita.ru по недорогим ценам. Наполним ресурс профессиональным контентом. Решим вопросы по круглосуточному мониторингу и администрированию. Сотрудники окажут лучшие меры по продвижению интернет-магазинов. Можете обратить внимание недорогие тарифы с абонентской платой. Тарифные планы предлагаются по ключевым характеристикам: количеству задействованных специалистов, объема страниц и других.
Если вы предпочитаете турецкие сериалы боевики, загляните на turkline.tv. Сайт предлагает лучшие боевики в HD 1080 качестве и с русской озвучкой. Захватывающие сюжеты и динамичные сцены в сериалах, таких как “Марашлы” и “Воин”, держат в напряжении с первой до последней серии. Все это доступно без рекламы и абсолютно бесплатно. Турклайн.тв – ваш лучший выбор для просмотра турецких боевиков онлайн.
click site AI in forecasting market trends
read this post here Bots for investment portfolio management
The drawing is happening Saturday evening and will be the
last onee parricular of the year.
Here iis myy web site; EOS파워볼 사이트
Conclusion
How to play aviator for money
Sultan casino telegram channel
поисковое продвижение сайта создание и продвижение сайта
seo продвижение раскрутка сайта цена в месяц
Great article! Purchasing Instagram accounts can indeed provide a significant advantage for businesses and influencers.
It saves time, offers instant credibility, and allows for a quicker path to
engagement and growth. For anyone looking to boost
their social media presence, buying an established account is definitely worth
considering.Buy followers.
Снимки, выполненные на фотобумаге профессионального уровня – это настоящий фотоархив, который дарит яркие эмоции долгие годы. Качественная печать фотографий на холсте из 100% хлопка с натяжкой на деревянный подрамник печать фотографий срочно
Hello, I do think your website could be having web browser compatibility
issues. Whenever I take a look at your website in Safari, it looks fine but when opening in I.E.,
it has some overlapping issues. I just wanted to provide you with a quick heads up!
Aside from that, wonderful site!
Great article! I found your insights on boosting social media presence really helpful.
For anyone looking to fast-track their Instagram growth, consider purchasing established
accounts for instant engagement and credibility. Instagram branding.
Register an account, make a deposit, and navigate to the Aviator Game to start playing.
How to play aviator for money
Great insights! Buying Instagram accounts can definitely give a significant head start for individuals and
businesses looking to grow their online presence quickly. The instant access to a large audience and enhanced credibility are huge
advantages. Thanks for sharing this information, it’s very helpful for anyone considering
this strategy.Buy Instagram accounts.
pop over to these guys galaxy swapper
Hello There. I discovered your blog using msn. This is a very well written article.
I will make sure to bookmark it and come back to read more of your
helpful info. Thanks for the post. I will certainly comeback. https://7bookmarks.com/story17310891/m%C3%A9dibotique
Earn additional money without efforts and skills. https://t.me/cryptaxbot/11
Great article! I completely agree with the benefits of purchasing Instagram accounts.
It’s a fantastic way to quickly grow your audience and enhance your online presence.
Thanks for sharing these insights, they’re very helpful
for anyone looking to boost their social media
game.Buy followers.
Otherwise, VIPs and higher rollers will continue
to uncolver new areas to gamble like Australia, Singapore,
and the Philippines.
Here is my webb site; 카지노친구
A completely free schedule allows you to plitki.com consider working as a courier as a full-time job or part-time job.
have a peek here Pal world
Thanks for the marvelous posting! I definitely enjoyed
reading it, you happen to be a great author.I will make certain to bookmark your blog and
may come back later in life. I want to encourage that you
continue your great posts, have a nice holiday weekend!
Great post! I recently discovered a fantastic store that sells authentic Instagram accounts, and it’s been a game-changer for my
social media strategy. Instant access to a large audience and enhanced
credibility have really boosted my engagement. Highly recommend checking it
out for anyone looking to grow their Instagram
presence quickly!
Instagram account service.
Great article! I completely agree with the points you’ve made about the advantages of buying Instagram accounts.
It can be a real game-changer for businesses and influencers looking to grow their social media presence quickly.
The time and effort saved by purchasing an established account
is invaluable. Looking forward to more insights on leveraging
social media for business growth. Thanks for sharing such informative
content!
Buy verified Instagram accounts.
Great article! I completely agree with the benefits of purchasing Instagram accounts.
It’s such a time-saver, especially for businesses
looking to grow their audience quickly. The instant access to a large following and increased credibility can really make a difference in marketing efforts.
Plus, the potential for monetization and higher engagement rates
makes it a smart investment. Thanks for sharing these insights!Instagram account security.
Только качественные товары для военных|Ваш надежный партнер в выборе военных товаров|Здесь найдете все для военного дела|Спецодежда и обувь для армии|Оружие и аксессуары для профессионалов|Профессиональное снаряжение для военных|Боевая техника для суровых реалий|Купите все необходимое для военной службы|Специализированный магазин для настоящих военных|Снаряжение от лучших производителей|Снаряжение для профессионалов военного дела|Оружие и снаряжение для истинных воинов|Только качественные товары для военного применения|Специализированный магазин для профессионалов|Специализированный магазин для военных операций|Выбор настоящих защитников|Армейский магазин с широким выбором экипировки|Оружие и снаряжение для успешных миссий|Качественные товары для военных целей|Оружие и экипировка для тех, кто выбирает победу
військовий інтернет магазин https://magazinvoentorg.kiev.ua/ .
and fair. These collaborations have helped elevate the Aviator Game to its current status as a beloved online
Aviator game APK
read this article Fl studio download
try this website Sandbox AVATAR
Vibration Analysis
Vibration Analysis
Rotor Balancing
Dynamic Balancing
Rotor Balancing
By carrying out timely pronovosti.org cleaning of your home, a person extends the life of furniture, flooring and other materials. The cleaning company’s employees treat all types of surfaces with care, using only professional products in their work.
Интересуетесь прошлым и его событиями? Турецкие сериалы исторические на turkline.tv предлагают увлекательные сюжеты, основанные на реальных событиях. Сериалы, такие как “Великолепный век” и “Воскресший Эртугрул”, доступны в HD 1080 качестве и с русской озвучкой. Без рекламы и совершенно бесплатно, turkline.tv – ваш идеальный спутник для путешествий во времени и изучения истории через захватывающие сериалы.
get a personal loan in massachusetts Payday loan companies will not even care if you have bad credit record.
The future of the Aviator Game looks promising, with continuous updates and improvements. As technology
Can you play aviator on PC
Lottery winnings in New York are topic to both state and federal taxes.
Stop by my web page :: Florida Powerball
my latest blog post Sandbox Airdrop
High-quality timber stroihome.net is resistant to aggressive environmental influences. Does not fade and tolerates low temperatures. Long service life.
Get new tokens in the game now Hamster Kombat
daily distribution Notcoin to your wallets
Join our project notreward.pro and receive toncoin
Hamster kombat airdrop
Bs.gl – Блэкспрут зеркало, Блэкспрут
environment for players to enjoy the game. Some popular platforms include Name], Name], and
Aviator game app
สวัสดีนะครับทุกคน!
ผมเพิ่งได้ทดลองเล่นบาคาร่าเว็บตรงไม่ผ่านเอเย่นต์ที่ บาคาร่า889 แล้วก็ต้องกล่าวว่าประสบการณ์ที่ได้รับมันดีที่สุดมากมายเลยขอรับ อินเตอร์เฟซของเว็บไซต์ใช้งานง่ายมากๆรวมทั้งกราฟิกก็ดูดีมาก นอกเหนือจากนี้ยังมีโปรโมชั่นที่น่าสนใจมากไม่น้อยเลยทีเดียว ไม่ว่าจะเป็นพวกใหม่หรือเก่า ทั้งการบริการลูกค้าก็สุดยอดมากครับ ตอบไวและให้คำแนะนำเจริญมาก เสนอแนะให้ทุกคนลองเล่นตรงนี้กันขอรับ ยืนยันว่าไม่ผิดหวังแน่นอน!
На сайте https://runobe.ru почитайте ранобэ онлайн и в отличном качестве. Все они на русском языке, а потому насладиться чтением сможет каждый. Все произведения имеют интересный сюжет, непредсказуемую развязку, а потому понравятся всем без исключения. Выбор японских романов обновляется ежедневно, чтобы вы смогли найти то, что действительно вам нравится. Вы можете ознакомиться сразу с несколькими, чтобы определиться с тем, какие из них вам нравятся больше. Для того чтобы подыскать определенный вариант, необходимо воспользоваться специальным поиском.
Great article! I completely agree with the benefits of buying Instagram accounts, especially for businesses looking to
grow their online presence quickly. Instant access to a large follower
base and enhanced credibility are game changers.
For anyone interested, I highly recommend checking out our site
for secure and reliable Instagram accounts. Thanks for sharing these insights!Instagram engagement.
Great article! I recently discovered a store that sells authentic Instagram accounts, and it has been a
game-changer for my social media marketing. The instant access
to a large audience really helped boost my online presence.
Highly recommend! Instagram account shop.
Future of the Aviator Game
Can I play aviator online for free
лаки джет играть http://www.1win-luckyjet-game.ru .
what is the best way to get a personal loan with bad credit If we are unable to collect any delinquent amount you may have with us through such actions, we may also sell our debt to a third party debt buyer or engage a collection agency, who may also engage in collection activity with you.
We’re tracking the number of jobs they’veviewed, the quantity of jobs they’ve applied to.
Here is my web site indeed job search
This article highlights some key advantages of purchasing Instagram accounts.
It’s amazing how quickly you can boost your social media presence and credibility by starting with an established audience.
This approach can save so much time and effort, especially for businesses looking
to grow rapidly. Highly recommend considering this strategy for anyone serious about their
Instagram marketing!Instagram account provider.
The season-ending Super Bowl and College Football National Championship are the most-watched sporting events in the
US by total viewership.
my web site :: Get More Info
play aviator game online play aviator game online .
First of all, it should be 365newss.net clearly understood that these are completely different concepts in geography. For example, when considering absolute height, it is precisely this that acts as the most important indicator, which is measured in meters, thereby determining the height of geographical objects above sea level.
Great insights! Purchasing authentic Instagram accounts can indeed be a game-changer for businesses and
influencers looking to expand their reach quickly.
It saves time and effort, allowing you to focus on creating
quality content and engaging with your audience.
If you’re considering this strategy, check out our site
for secure and reliable options.Business Instagram accounts.
Hello there, You have done a great job. I will certainly digg it and personally suggest to my friends. I am confident they’ll be benefited from this site.
купить диплом в ревде
https://www.kpilib.ru/forum.php?tema=6762
http://pokemon-go.onl/users/6146
https://phileo.me/blogs/new
https://www.mylot.su/blogs/2214
https://dominerbusiness.com/userinfo.php?username=minna_prout_301152&do=profile&op=userinfo
купить диплом в люберцах
you’re in point of fact a good webmaster. The website loading pace is incredible. It seems that you are doing any distinctive trick. In addition, The contents are masterwork. you’ve performed a magnificent activity on this matter!
купить диплом института
http://avtobestnews.ru/individualnoe-obrazovanie-gde-kupit-diplom-sozdannyiy-spetsialno-dlya-tebya
https://bvf.ru/forum/showthread.php?p=25243566#post25243566
http://fire-team.ru/forum/member.php?u=1143
http://trading-labor.de/пїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅ_пїЅпїЅпїЅпїЅпїЅ:_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅ_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ
http://dachaweek.ru/uspeshnoe-zavershenie-obrazovaniya-poluchite-svoy-diplom-uzhe-segodnya
купить диплом в ульяновске
sites https://trezor-wallet.at/2023/11/14/why-trezor-is-the-preferred-option-for-safeguarding-your-digital-assets/
Common mistakes to avoid in the Aviator Game include:
aviator demo
Great article! I completely agree that purchasing Instagram
accounts can provide a significant advantage, especially for businesses
looking to quickly establish a strong online presence.
The instant access to a large follower base and increased credibility can save a lot of time and effort.
Thanks for sharing these insights. It’s definitely a
strategy worth considering for anyone serious about social media growth.Buy Instagram accounts.
Great article! I completely agree with the benefits of
buying Instagram accounts, especially for businesses looking to quickly establish a
strong online presence. The instant access to a large audience and
enhanced credibility can make a huge difference. I’ve found that purchasing
a well-established account saves so much time and effort. It’s definitely a smart strategy for anyone serious about growing their brand
on social media.Instagram audience.
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is added I get four e-mails with the
same comment. Is there any way you can remove people from
that service? Cheers!
and fair. These collaborations have helped elevate the Aviator Game to its current status as a beloved online
aviator demo
More Bonuses https://debank.lu/2023/11/11/insights-from-the-crypto-community-on-anticipating-the-us-apex-banks-stance-on-cryptocurrencies/
Hey there! I just wanted to ask if you ever have any issues with hackers?
My last blog (wordpress) was hacked and I
ended up losing a few months of hard work due to no back up.
Do you have any solutions to prevent hackers? https://Onelifesocial.com/story2636483/entreprises-jos%C3%A9-melo
Roulette is a staple of land-primarily based casino
games, and it’s no distinct on the internet.
my page … http://mammouthides.timlib.com/tiki-index.php?page=UserPagemindachumleyfwyqnn
balforum.net
check this https://blur-io-nft.com/2023/11/09/regulating-blurry-money-blocks-government-efforts-to-combat-illicit-cryptocurrency-transactions/
canadatc.com
this website https://trezorwallet-app.org/2023/11/14/can-you-use-usdt-to-pay-bills-or-make-purchases/
Just check out the best anli5 naked strip on webcam for live sex chat ever!
Nude hot cams womaNude amateur webcams model online porn char d7_0026
and fair. These collaborations have helped elevate the Aviator Game to its current status as a beloved online
aviator demo
My brother suggested I might like this website. He was entirely right.
This post actually made my day. You can not imagine just how
much time I had spent for this information! Thanks!
Привет всем!
Поможем Вам купить диплом Вуза России недорого, без предоплаты и с гарантией возврата средств
https://wiki.3cdr.ru/wiki/index.php/пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ:_пїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅ_пїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ
https://www.fromrus.su/index.php?/topic/11492-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0-%D1%81-%D0%B7%D0%B0%D0%BD%D0%B5%D1%81%D0%B5%D0%BD%D0%B8%D0%B5%D0%BC-%D0%B2-%D1%80%D0%B5%D0%B5%D1%81%D1%82%D1%80-w778h/
http://forum.safe-animals.ru/index.php?showtopic=24642
http://forwoman.lifeforums.ru/viewtopic.php?id=14924#p25474
https://ic-info.ru/forum/user/146317/
Здравствуйте!
У нас вы можете заказать документы об образовании всех ВУЗов России с доставкой по РФ и возможностью оплаты после получения!
http://ya.6bb.ru/viewtopic.php?id=2684#p4218
http://prikol100500.ru/dostupnyie-tsenyi-na-diplomyi-dlya-vseh-zhelayushhih
https://wiki.wogames.info/wiki/%D0%93%D0%B4%D0%B5_%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE_%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC_%D0%B8%D0%BB%D0%B8_%D0%B6%D0%B5_%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82_%D0%BE%D1%82%D0%BB%D0%B8%D1%87%D0%BD%D0%BE%D0%B3%D0%BE_%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B0%3F
http://service-in.ru/forum/user/3214/
http://www.farmersforum.ir/members/rudiplomyccoomtenda.html
Nice article, thanks! Just check pankrabbit2005 nude in hot sex Live chat this out.
Naked hot webcams gNaked amateur webcams woman live porn char d6_7f48
homeprorab.info
improved mobile compatibility. Developers continually use this feedback to enhance the game and provide a better
aviator demo
Если хотите смотреть турецкие сериалы 2024 онлайн, рекомендую turkline.tv. Все сериалы на сайте доступны в HD качестве, без рекламы и совершенно бесплатно. Меня порадовало удобство использования и широкий выбор жанров. Этот сайт занимает первые места в поисковых системах, что говорит о его надежности и популярности. Очень доволен и рекомендую его всем любителям турецкого кино. Турклайн.тв – лучший выбор для просмотра новинок 2024 года.
Онлайн казино – ваш путь к увлекательным приключениям, выигрывайте крупные суммы в лучших онлайн казино, погружайтесь в мир азарта.
Онлайн казино: безопасность и азарт, возможность выиграть становится выше.
Эксклюзивные онлайн казино для настоящих азартных игроков, присоединяйтесь и возьмите победу.
Онлайн казино: азарт и выигрыш, выигрывайте и наслаждайтесь успехом.
Зарабатывайте крупные суммы в онлайн казино, тренируйтесь и побеждайте.
лучшие онлайн казино с минимальным депозитом онлайн казино .
Discover the best ElsaRedwood on webcam for live free nude chat now ever for free!
Naked hot cams womNaked hot webcams model live sex char 57ad0_6
In addition to variances from state to state, a single state might levy fees differently primarily based
on the kind of automobile and its use.
Take a look at my webpage :: loan calculator
Blacksprut ссылка – Блэкспрут зеркало, Bs2site2
Блэкспрут зеркало – Bs2best, Блэкспрут
777 슬롯
백 관리들을 보며 많은 사람들이 자신을 간절히 바라봤다.
Excellent and high-quality kata-valentiine nude on cam for live porn chat absolutely free and easy to watch on any device, just
Naked amateur webcaNaked hot cams wom 6b6942d
madeintexas.net
description https://debank.at/2023/11/11/advantages-of-combining-metamask-with-debank/
Common mistakes to avoid in the Aviator Game include:
aviator demo
Футбольная статистика, расписание и результаты матчей
Футбольная статистика, расписание и результаты матчей являются неотъемлемой частью мира футбола, предоставляя болельщикам и аналитикам важную информацию
о командах и игроках.
Статистика в футболе охватывает широкий спектр данных, включая
голы, передачи, владение мячом, удары по
воротам и многое другое. Эта информация помогает
оценить эффективность игроков и команд, а также прогнозировать будущие
результаты.
Расписание матчей играет ключевую роль
в организации футбольных турниров и лиг.
Оно учитывает множество факторов, таких как географическое расположение команд,
телевизионные трансляции и участие в международных соревнованиях.
Результаты матчей – это кульминация футбольных событий,
отражающая итоги противостояний
команд. Они влияют на турнирную таблицу, определяют чемпионов и аутсайдеров, а также
формируют историю футбола.
В современную эпоху цифровых технологий доступ к футбольной статистике,
расписанию и результатам стал проще, чем когда-либо.
Многочисленные веб-сайты и мобильные приложения предоставляют эту информацию в режиме реального времени, позволяя фанатам быть в курсе
последних событий в мире футбола.
Look at my webpage :: “http://www.vloeimans.com/index.php?title=Winrating.ru”
Howdy very cool web site!! Guy .. Beautiful .. Amazing .. I will bookmark your website and take the feeds additionally? I’m happy to search out so many useful information right here in the put up, we’d like develop extra strategies on this regard, thanks for sharing. . . . . .
http://kip-world.ru/programmiruemoe-rele-oven-pishem-soft-v-srede-owen-logic.html
купить диплом медбрата
http://efawb.ru
купить диплом в усть-илимске
Blog absolutely free and easy to watch on any device, just
Naked hot webcams model live porn showNude hot cams girl ee0b6b6
ilive movie theater kit search movies by keywordswhen does kings dominion season pass endhell fire movie
Футбольная статистика, расписание
и результаты матчей
Футбольная статистика, расписание и результаты матчей являются неотъемлемой частью мира футбола,
предоставляя болельщикам и аналитикам важную информацию о командах и игроках.
Статистика в футболе охватывает широкий спектр данных, включая голы, передачи,
владение мячом, удары по воротам и многое другое.
Эта информация помогает оценить эффективность игроков
и команд, а также прогнозировать
будущие результаты.
Расписание матчей играет ключевую роль в
организации футбольных турниров и лиг.
Оно учитывает множество факторов, таких как географическое расположение команд, телевизионные трансляции и участие в международных соревнованиях.
Результаты матчей – это кульминация футбольных
событий, отражающая итоги противостояний команд.
Они влияют на турнирную таблицу,
определяют чемпионов и аутсайдеров, а также формируют историю футбола.
В современную эпоху цифровых технологий доступ
к футбольной статистике, расписанию
и результатам стал проще, чем когда-либо.
Многочисленные веб-сайты и мобильные приложения предоставляют эту информацию в режиме реального времени, позволяя фанатам быть в
курсе последних событий в
мире футбола.
Feel free to surf to my blog … “https://escortexxx.ca/author/steffenfitc/”
To use, you simply need to instukzia.com drive the forklift up to the load and then lift it with a fork. Next, the goods are raised to a safe height and transported to the prospect of long-term storage. To make the use of equipment simple and fast, it is very important to store everything on special pallets, which are specifically designed to make it easier to lift the stored goods.
Nelly naked before webcam – Live Sex Chat chatturbate absolutely free and easy to watch on any device, just
Nude amateur camsNaked hot cams mod 0b6b694
Great article! I appreciate the clear and insightful perspective you’ve shared. It’s fascinating to see how this topic is developing. For those interested in diving deeper, I found an excellent resource that expands on these ideas: check it out here. Looking forward to hearing others’ thoughts and continuing the discussion!
Multiplayer Options and Social Interaction
aviator demo
article source https://tronlink-app.org/2023/11/13/is-tronwallet-shaping-the-future-of-decentralized-finance-unleashing-the-potential-of-the-defi-revolution-with-trons-official-mobile-wallet/
Find out Princess Cherrybaybe nude on adult cam in her Live Porn Chat for free 🙂
Naked amateur camsNaked hot cams mod 57ad3_6
Ваш путь к удаче: лучшие онлайн казино, советуем.
Наши рекомендации: самые популярные онлайн казино, испытайте прямо сейчас.
Популярные азартные игры в онлайн казино, испытайте прямо сейчас.
Бонусы и выигрыши: лучшие онлайн казино для вас, попробуйте прямо сейчас.
Играйте в новые азартные игры в онлайн казино и выигрывайте крупные суммы, попробуйте прямо сейчас.
Играйте в лучшие онлайн казино и выигрывайте крупные суммы денег, испытайте сейчас.
Популярные игры с выигрышами в онлайн казино, испытайте прямо сейчас.
Наши рекомендации: лучшие онлайн казино, присоединяйтесь сейчас.
Азартные игры и захватывающие призы в онлайн казино, испытайте прямо сейчас.
Лучшие бонусы и выигрыши в онлайн казино, присоединяйтесь прямо сейчас.
Популярные возможности для азартных игроков в онлайн казино, испытайте прямо сейчас.
Играйте и выигрывайте крупные суммы в самых популярных онлайн казино, испытайте сейчас.
Лучшие игры и призы в онлайн казино, посетите прямо сейчас.
Наши рекомендации: самые популярные онлайн казино, посетите сейчас.
Азартные игры и призы в онлайн казино, попробуйте прямо сейчас.
Бонусы и выигрыши: лучшие онлайн казино для вас, присоединяйтесь прямо сейчас.
Популярные возможности для азартных игроков в онлайн казино,
лучшие онлайн казино на деньги лучшие онлайн казино на деньги .
Bs2site – Blacksprut онион, Блэкспрут зеркало
На сайте https://turk-kino.ru посмотрите интересное и запоминающееся турецкое кино вместе с другом. Есть такие именитые картины, как «Запах клубники», «Зимородок», «Великолепный век» и многое другое. Для того чтобы начать совместный просмотр, необходимо создать комнату. Сделать это получится в 3 шага, а инструкция прилагается. Перед вами многообещающие новинки, а также топ лучших фильмов за 2024 год. Во всех фильмах играют ваши любимые актеры, звучит приятная музыка. Есть подборка рекомендованных фильмов, которые выбирают многие.
Our site https://blur-nft-marketplace.org/2023/11/10/harnessing-the-potential-of-digital-collectibles-exploring-nfts-and-the-evolution-of-ownership/
my blog https://tronlink.at/2023/11/13/an-in-depth-analysis-of-the-factors-contributing-to-the-success-of-the-ben-armstrong-show-revealing-the-hidden-secrets/
Управление охраной труда обучение safetysystemsgroup.com
Что касается аналитическая лаборатория аккредитация приходите в нашу компанию. Позвоните по номеру телефона +7(499)348-25-03 или подайте заявку обратный звонок. Наш специалист приедет к Вам и осуществит инструментальные измерения, сроком от пяти рабочих дней. Наши главные услуги: производственный экологический контроль, инженерно экологические изыскания, программа производственного контроля и другие.
Excellent and high-quality Alana-haze, 💗 nude before webcamcam – live sex chat absolutely free and easy to watch on any device, just
Naked hot webcams model live sex charNaked amateur cams 2dacc58
A single of the players acts ass a banker and bets on the banker’s win.
Stop by my blog … 온카홈바로가기
I couldn’t refrain from commenting. Very well written! http://links.musicnotch.com/mariannewoll
the opportunity to compete for larger prizes and showcase their skills on a larger stage.
aviator demo
На сайте https://jidkie-oboi-77.ru/ в огромном выборе находятся жидкие обои. К их важным преимуществам относят простоту нанесения, а потому решить задачу под силу даже дилетанту, который ни разу с этим не сталкивался. Важным моментом является то, что обои маскируют дефекты, неровности стен. Выбирая материал, необходимо учитывать следующие моменты: определитесь с цветовой гаммой, а также целями приобретения. Важно, чтобы цветовая гамма идеально вписалась в интерьер. Есть как шелковые, так и хлопковые.
Blog videos absolutely free and easy to watch on any device, just
Naked amateur camsNaked hot cams wom 6b6942d
Копицентр предоставляет выгодные цены на полиграфическую продукцию и дарим скидку 10% на повторные заказы фотосалон москва
Just check this out, live sex chat porn
Naked amateur camsNaked amateur webca d8_1094
Social and Community Aspects
aviator demo
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
last news about muller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
Rybelsus – Quick and Easy Weight Lass
According to randomised controlled trials, you start losing weight immediately after taking Rybelsus. After one month, the average weight loss on Rybelsus is around 2kg; after two months, it’s over 3kg.
What does Rybelsus do to your body?
Rybelsus (oral semaglutide) is a GLP-1 receptor agonist. It mimics a fullness hormone called GLP-1.
Rybelsus reduces appetite and hunger by interacting with the brain’s appetite control centre, the hypothalamus. This effect on the brain helps you eat fewer calories and starts almost immediately after taking the pill.
However, you might notice your hunger levels rising and falling in the first 4-5 weeks you take Rybelsus.
It can take around 4-5 weeks for Rybelsus to reach a level in the body we call a steady state. A steady state is when the drug’s levels in the body remain consistent rather than spiking and falling.
Interestingly, this initial weight loss is no different to other weight loss treatments or the impact of diet interventions on weight loss. The real effect of oral semaglutide is seen beyond three months.
Oral semaglutide is a long-acting medication that’s started at a lower dose to reduce the number and severity of side effects as it’s built up to a higher maintenance dose.
https://true-pill.top/rybelsus.html
to your liking, and quickly move to the section with Sophia-rincon nude on sex webcam in her Live Sex Chat on this topic. All categories are packed enough to make
Nude hot cams modeNaked amateur cams e0b6b69
https://iqratrust.org/
Blacksprut зеркало – Blacksprut зеркало, Blacksprut зеркало
Discover the best desiredianne nude on sex cam in XXX Live Sex Chat Room
and TinyMimi nude strip before webcam for live sex xxx chat ever!
Naked amateur cams woman online sex showNude amateur webcam bfee0b6
https://irhsca.org/
Услуги по обучению охраны труда safetysystemsgroup.com
Помимо программа производственного контроля предприятия торговли у нас Вы найдете курсы по обучению в режиме онлайн по охране труда, пожарно-технический минимум, электробезопасность 2-я группа и другие. Свяжитесь с нами по вышеуказанному телефону, адресу или закажите обратный звонок. Мы будем рады работать с Вами.
Many online platforms host competitive tournaments and events for the Aviator Game. These events offer players
aviator demo
browse around this web-site https://galxe-app.org/2023/11/19/exploring-the-beauty-and-mystery-of-the-galxe-linea/
https://muslim-forum.org/
Have you ever thought about writing an ebook or guest authoring on other sites?
I have a blog based on the same information you discuss and would really like
to have you share some stories/information. I know my subscribers would
enjoy your work. If you are even remotely interested, feel free to shoot me an email. https://Nohio.org/index.php/User:HumbertoGeorgina
Блэкспрут ссылка – Блэкспрут, Blacksprut
the social features, and the quality of the user interface.
aviator demo
Discover the best DollyBuoy naked strip on XXX webcam for live sex video chat ever for free!
Nude hot webcams woNaked amateur webcams girls live sex show bfee0b6
Swampy and creeping soil. In such areas, slush constantly forms after even a light rain. In repaircanada.net this case, you will have to raise the soil level using sprinkling. It could be rubble.
uquest.net
Блэкспрут ссылка – Bs2site, Блэкспрут
Blog absolutely free and easy to watch on any device, just
Naked hot webcams mNaked hot cams mod bfee0b6
Experienced players can benefit from more advanced strategies, such as:
aviator demo
https://ecs-pw-pc2.ecs.csus.edu/wiki/index.php/Winrating.ru
Kymberly-0000 nude on Live Cam Sex Chat absolutely free and easy to watch on any device, just
Nude amateur camsNude hot cams girl c5812fb
https://pattern-wiki.win/wiki/User:JanineSantora0
buy cvv Good validity rate Sell Make good job for MMO Pay on website activate your
card now for worldwide transactions.
————-CONTACT———————–
WEBSITE : >>>>>> Unicvv✺Top
—– HERE COMES THE PRICE LIST ———–
***** CCV US:
– US MASTER CARD = $2,6 per 1 (buy >5 with price $3 per
1).
– US VISA CARD = $2,6 per 1 (buy >5 with price $2.5 per 1).
– US AMEX CARD = $3,1 per 1 (buy >5 with price $2.5 per 1).
– US DISCOVER CARD = $2,3 per 1 (buy >5 with price $3.5 per 1).
– US CARD WITH DOB = $15 per 1 (buy >5 with price $12
per 1).
– US FULLZ INFO = $40 per 1 (buy >10 with price $30 per 1).
***** CCV UK:
– UK CARD NORMAL = $2,2 per 1 (buy >5 with price
$3 per 1).
– UK MASTER CARD = $2,5 per 1 (buy >5 with price $2.5 per 1).
– UK VISA CARD = $3,4 per 1 (buy >5 with price $2.5 per 1).
– UK AMEX CARD = $2,4 per 1 (buy >5 with price $4 per 1).
$5,4
– UK CARD WITH DOB = $15 per 1 (buy >5 with price $14 per 1).
– UK WITH BIN = $10 per 1 (buy >5 with price $9 per 1).
– UK WITH BIN WITH DOB = $25 per 1 (buy >20 with price $22 per 1).
– UK FULLZ INFO = $40 per 1 (buy >10 with price $35 per 1).
***** CCV AU:
– AU MASTER CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU VISA CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU AMEX CARD = $8.5 per 1 (buy >5 with price $8 per
1).
– AU DISCOVER CARD = $8.5 per 1 (buy >5 with price $8 per 1).
***** CCV CA:
– CA MASTER CARD = $6 per 1 (buy >5 with price
$5 per 1).
– CA VISA CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA BUSINESS = $14 per 1 (buy >5 with price $13 per
1).
Группы обучения по охране труда safetysystemsgroup.com
Чтобы найти программа производственного контроля учреждения приходите в нашу компанию. Позвоните по контактному телефону +7(800)302-82-49 или подайте заявку обратный звонок. Наш профессиональный работник приедет к Вам и осуществит инструментальные измерения, сроком от 5ти рабочих дней. Наши главные услуги: производственный экологический контроль, аккредитация испытательной лаборатории, программа производственного контроля и другие.
Excellent and high-quality SexyDelaJ nude strip on cam for live sex chat absolutely free and easy to watch on any device, just
Nude hot webcams model online porn charNaked hot cams gir bfee0b6
สวัสดีครับผมทุกคน!
ผมเพิ่งได้ลองเล่นบาคาร่าสายฟ้าที่ บาการ่า และก็จะต้องบอกว่าประสบการณ์ที่ได้รับมันเยี่ยมมากเลยนะครับ อินเตอร์เฟซของเว็บไซต์ใช้งานง่ายมากๆรวมทั้งกราฟิกก็ดูดีมาก ยิ่งไปกว่านี้ยังมีโปรโมชั่นที่น่าดึงดูดมาก ไม่ว่าจะเป็นสมาชิกใหม่หรือเก่า ทั้งยังการบริการลูกค้าก็สุดยอดมากครับ ตอบไวและก็ให้คำปรึกษาได้ดิบได้ดีมาก เสนอแนะให้ทุกคนทดลองเล่นตรงนี้กันครับผม รับรองว่าไม่ผิดหวังแน่ๆ!
click here now https://galxe-web3.com/2023/11/19/galxe-2-0-the-new-era-of-intelligent-automation-and-decision-making/
мониторинг серверов ла2
Анонсы л2
enjoyable.
aviator demo
We present up to forty-four (44) live dealer games powered by
the industry’s major application developer – Evolution Gaming.
my site – 카지노사이트
Just wish to say your article is as astounding. The clarity in your post is just spectacular and i could assume you’re an expert on this subject. Fine with your permission let me to grab your feed to keep up to date with forthcoming post. Thanks a million and please continue the enjoyable work.
finttech.ru/page/36
forumjizni.ru/member.php?u=120588
fkf36.ru/183/
kanc4life.com.ua/index.php?links_exchange=yes&page=170&show_all=yes
t99.vn/tap-doan-t99-va-vng-cloud-ky-ket-hop-tac-chien-luoc-toan-dien-ve-tai-chinh-cong-nghe
4chan movies when does d3 season 27 startwhen is invincible season 2 releasingwill there be a new season of the walking dead
Discover the best Liv and Drew nude before webcam – Live Sex Chat ever for free!
Naked hot cams woman live sex showNude amateur cams b6942da
have a peek at this web-site https://orbiter-finance.at/2023/11/19/what-you-need-to-know-about-orbiter-finances-token-distribution-plans-and-possible-airdrops/
my blog https://1inch-app.org/2023/11/17/a-step-by-step-tutorial-on-how-to-stake-1inch-tokens/
click here to find out more https://metamask-wallet-web3.com/2023/11/16/choosing-the-right-ethereum-wallet-coinbase-wallet-vs-metamask/
In such a situation, women18.com water will not accumulate under the gazebo, and it itself will be located on a hill.
Рекомендую всем, кто ищет смотреть турецкие сериалы 2023 онлайн на русском языке, посетить сайт turkline.tv. Этот сайт лидирует в Google и Yandex, и заслуженно. Все сериалы доступны в HD качестве и абсолютно бесплатно. Удобный интерфейс и широкий выбор жанров делают просмотр еще более приятным. Лично я был очень рад найти такой ресурс и теперь постоянно использую его для просмотра новинок. Турклайн.тв – идеальное место для любителей турецких сериалов на русском языке.
На сайте https://ocims.ru/ закажите звонок для того, чтобы воспользоваться такой услугой, как строительство каркасных домов высокого качества. Они надежные, практичные, а самое главное, что простоят очень долго. Все работы происходят под ключ. Дома строятся по индивидуальному, а также типовому проекту, что позволит подобрать то, что соответствует предпочтениям, вкусам. На работы, материалы даются гарантии. Действуют привлекательные и доступные расценки. Также компания предлагает приятный презент по окончании проведения работ.
If we are talking about massive boxes, then they coloradonewss.com should also have a small platform under which you can crawl with a forklift, otherwise transportation will take much longer.
There are a couple of more rules, though, depending on the score of the
Player’s hand.
Here is my site: e-academy.navttc.gov.pk
kms auto net Office 2021
https://what-full-kmssite1.pages10.com/kmsauto-application-details-get-source-web-url-windows-licensingguidelines-63514058
kms-auto lite Office 2021
Free download km5 auto
AuroraDurand fully naked sexy girl on cam for online sex webcam chat
Naked amateur webcaNaked amateur webcams girls online sex show 6942dac
Aviator Game. Notable names in the industry have contributed their expertise to ensure the game is both engaging
aviator demo
Качественный Мефедрон в Кристаллах
Купить Мефедрон в Киеве – https://koks.top
Доставка по городам Мефедрон Кристаллах – https://koks.top
Доставка в руки написать адрес САЙТ – https://koks.top
Купить Мефедрон в Кристаллах – https://koks.top
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
Теги – Купить Мефедрон в Киеве?
Чистый Мефедрон Кристаллы в Киеве?
Как Купить Мефедрон закладкой в Киеве?
Доставка Мефедрона по Киеву
Мефедрон Украина Кристалл
to your liking, and quickly move to the section with Blog on this topic. All categories are packed enough to make
Nude hot webcams woNaked hot cams gir ee0b6b6
Going Here https://metamask-wallet.at/2023/11/16/step-by-step-guide-on-how-to-download-and-install-metamask-apk-on-your-device/
kmsautodownload
https://-kmsautosite2.onesmablog.com/process-to-make-faster-ms-windows-by-using-kmsauto-net-67763931
kms activator lite Office 2021
Free download km5 auto
Watch nudeSarah before webcam – Online Sex Show absolutely free and easy to watch on any device, just
Naked amateur camsNude amateur cams d57ad5_
Chasing Losses: Trying to recover losses by betting more can be detrimental.
п»їaviator demo
Vinicius Junior https://viniciusjunior.prostoprosport-ar.com is a Brazilian and Spanish footballer who plays as a striker for Real Madrid and the Brazilian national team. Junior became the first player in the history of Los Blancos, born in 2000, to play an official match and score a goal.
Kylian Mbappe https://kylianmbappe.prostoprosport-ar.com is a French footballer, striker for Paris Saint-Germain and captain of the French national team. He began playing football in the semi-professional club Bondi, which plays in the lower leagues of France. He was noticed by Monaco scouts, which he joined in 2015 and that same year, at the age of 16, he made his debut for the Monegasques. The youngest debutant and goal scorer in the club’s history.
to your liking, and quickly move to the section with monroe_777 fully nude stripping on cam for online porn movie webcam chat on this topic. All categories are packed enough to make
Naked amateur camsNaked hot webcams model live sex show 812fb1f
Islamische Gebetszeiten, Fadschr, Zuhr, Asr, Maghrib et Isha’a: islamische-gebetszeiten.online
Find here UAE Prayer Timings, Muslim Prayer Timings, Imsak Time, Iftar Timings, Fajr Time and more updates from Khaleej Times http://timenamaz.online/
I blog quite often and I truly thank you for your content.
This article has really peaked my interest. I am going to bookmark your blog and keep
checking for new details about once per week.
I subscribed to your RSS feed too.
kms auto net
https://a-kms-www-.blog2freedom.com/27466151/every-the-merits-of-the-kmsauto-activation-tool-for-setting-up
kmsauto portable
Free download km5 auto
Bastidores da transmissГЈo ao vivo da nossa putaria absolutely free and easy to watch on any device, just
Nude amateur webcamNude amateur cams ad1_2b2
laptops, tablets, and smartphones. This flexibility allows players to enjoy the game on their preferred device,
aviator demo
And 1 thrilling improvement is the combination of Thai Swedish massage therapy wifh the therapeutic properties of hemp oil.
Если вам нравятся магия и волшебство, обязательно зайдите на turklife.tv и смотрите турецкие сериалы фэнтези. Здесь собраны самые захватывающие и фантастические истории в HD 1080 качестве с отличной русской озвучкой. Удобное разделение по жанрам и годам позволяет легко находить нужные сериалы.
Каждый день добавляются новые серии, и всё это абсолютно бесплатно и без рекламы. Turklife.tv – лучший выбор для любителей фэнтези. Погружайтесь в мир магии и приключений прямо сейчас!
britainsnews.com
Karim Benzema https://karimbenzema.prostoprosport-ar.com is a French footballer who plays as a striker for the Saudi Arabian club Al-Ittihad. He played for the French national team, for which he played 97 matches and scored 37 goals. At the age of 17, he became one of the best reserve players, scoring three dozen goals per season.
Ваш путь к удаче: лучшие онлайн казино, испытать.
Наши рекомендации: самые популярные онлайн казино, испытайте прямо сейчас.
Играйте в захватывающие азартные игры в онлайн казино и увеличивайте свой доход, посетите прямо сейчас.
Наслаждайтесь игрой вместе с лучшими онлайн казино, испытайте прямо сейчас.
Обновленные возможности для любителей азарта в онлайн казино, посетите прямо сейчас.
Играйте в лучшие онлайн казино и выигрывайте крупные суммы денег, посетите сейчас.
Играйте в увлекательные игры и выигрывайте крупные суммы в онлайн казино, попробуйте прямо сейчас.
Играйте и выигрывайте большие суммы в лучших онлайн казино, испытайте сейчас.
Играйте в азартные игры и выигрывайте захватывающие призы в онлайн казино, посетите прямо сейчас.
Лучшие бонусы и выигрыши в онлайн казино, испытайте прямо сейчас.
Новые возможности и азартные игры в онлайн казино, попробуйте прямо сейчас.
Играть и выигрывать: самые популярные онлайн казино для вас, испытайте сейчас.
Лучшие игры и призы в онлайн казино, посетите прямо сейчас.
Большие выигрыши и возможности: самые популярные онлайн казино для вас, посетите сейчас.
Азартные игры и призы в онлайн казино, испытайте прямо сейчас.
Бонусы и выигрыши: лучшие онлайн казино для вас, присоединяйтесь прямо сейчас.
Новые возможности и азартные игры в онлайн казино,
онлайн казино https://onlayn-kazino-reyting-belarusi.com/ .
dublindecor.net
i was reading this The Sandbox Metaverse Map
learn the facts here now Sandbox game
anal threesome Haylee nude before webcam – Live Sex Chat
Nude hot webcams woNude hot cams woma bfee0b6
Victor James Osimhen https://victorosimhen.prostoprosport-ar.com is a Nigerian footballer who plays as a forward for the Italian club Napoli and the Nigerian national team. In 2015, he was recognized as the best football player in Africa among players under 17 according to the Confederation of African Football.
kms auto lite windows 11
https://aboutkmsforum.getblogs.net/59925643/approach-to-hasten-microsoft-windows-employing-kmsauto-activator
kms autodownload
Free download km5 auto
find here Creative your account sandbox
click here to investigate The Sandbox Shop
Наш сервисный центр предлагает надежный починить духовой шкаф адреса любых брендов и моделей. Мы знаем, насколько необходимы вам ваши духовки, и стремимся предоставить услуги наилучшего качества. Наши опытные мастера оперативно и тщательно выполняют работу, используя только качественные детали, что предоставляет долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются обладатели кухонных приборов, включают проблемы с нагревом, неисправный таймер, поврежденную дверцу, неисправность контроллера, проблемы с конвекцией и неисправные платы. Для устранения этих проблем наши квалифицированные специалисты оказывают ремонт нагревательных элементов, термостатов, таймеров, дверец, контроллеров, вентиляторов и электроники. Обращаясь в наш сервисный центр, вы обеспечиваете себе надежный и долговечный сервис ремонта духового шкафа на дому.
Подробная информация размещена на сайте: https://remont-duhovyh-shkafov-ace.ru
Gaza Philip preached of Christ and baptized an Ethiopian eunuch on his way to Gaza (Acts 8:26–39). Jerusalem See map 12 for events in Jerusalem Alexander the Great’s Empire on the West Map
Hello there! Would you mind if I share your blog with my myspace group? There’s a lot of people that I think would really enjoy your content. Please let me know. Thanks
https://telegra.ph/Kupit-diplom-SHag-k-novoj-zhizni-bez-pregrad-04-28
http://heyrodisscusion.listbb.ru/viewtopic.php?f=10&t=309
http://recept-food.ru/kupit-diplom-vash-shans-stat-luchshim-v-svoey-oblasti
https://kormushka48.ru/forum/user/14720/
https://communityofbabel.com/en/forums/discussion/other/zarabotok-a77r/
The North Carolina Education Lottery was established in 2005 by way of an act of the North Carolina legislature.
My website – 무료 로또번호추천
kms-autoOffice 2021
https://akmspage1.digitollblog.com/27284375/procedure-to-quicken-microsoft-windows-with-kmsauto-activator
kms activator ++ windows 11
Free download km5 auto
to your liking, and quickly move to the section with sophia_leurre naked stripping on cam for live porn movie webcam chat on this topic. All categories are packed enough to make
Naked hot cams girNaked hot webcams m fee0b6b
They seek thrills, and games like DoA provide just what they are
searching for.
Also visit my website fix.greenaryworld.com
Nice article, thanks! Just check Watch nudeMonika on the cam – Live Sex Chat this out.
Nude hot cams womaNaked hot webcams m fb65d57
kms-auto net Office 2019
https://what-kmsauto-net-www-.loginblogin.com/34057604/kms-auto-activator-explanation-download-link-web-page-link-windows-enablementsteps
kms activator net windows 11
Free download km5 auto
Когда хочется смотреть турецкие сериалы 2024 онлайн на русском языке, turklife.tv становится отличным решением. Здесь вы найдете новейшие сериалы 2024 года в HD 1080 качестве и с превосходной русской озвучкой. Сайт предлагает широкий выбор жанров и удобное разделение по годам.
Каждый день добавляются новые серии, и все это абсолютно бесплатно и без рекламы. Это делает просмотр комфортным и приятным. Turklife.tv – ваш лучший выбор для просмотра турецких сериалов онлайн на русском языке.
адрес вскрытие замков http://www.vskrytie-zamkov-moskva113.ru .
look at this website keplr wallet download
anal threesome Remu_o0 fully nude strip on cam for online sex video show
Naked hot cams womNude amateur cams b6942da
На сайте http://koleso-na-hodu.ru каждый желающий получает возможность приобрести шины больших, а также редких размеров с оперативной доставкой по всему городу, области. Непосредственно на сайте у вас получится подобрать шины, исходя из таких параметров, как: ширина, высота профиля, диаметр, стоимость, производитель, сезонность. Вся продукция сертифицированная, качественная, оригинальная. Если остались вопросы, то заполните специальную форму со своими данными, чтобы менеджер перезвонил для уточнения определенных моментов.
sell cvv good newfresh high balance LIVE 24/24 –
2022 (No DIE) 【Visit CcBuy.Black】 All COUNTRY US , UK , CA ,
AU , EU , SN , MK
————-CONTACT———————–
WEBSITE : >>>>>> CcBuy⁎ Black
—– HERE COMES THE PRICE LIST ———–
***** CVV Other countries
TZ VISA CARD = $4,3 per 1 (buy >5 with price $2.5 per 1).
BV VISA CARD = $4,7 per 1 (buy >5 with price $2.5 per 1).
GY VISA CARD = $3,9 per 1 (buy >5 with price $2.5 per 1).
KM VISA CARD = $2,3 per 1 (buy >5 with price $2.5 per 1).
***** CVV US:
– US MASTER CARD = $2,2 per 1 (buy >5 with price $3 per 1).
– US VISA CARD = $2,7 per 1 (buy >5 with price $2.5 per
1).
– US AMEX CARD = $3,5 per 1 (buy >5 with price $2.5 per 1).
– US DISCOVER CARD = $3,2 per 1 (buy >5 with price $3.5 per 1).
– US CARD WITH DOB = $15 per 1 (buy >5 with price $12 per 1).
– US FULLZ INFO = $40 per 1 (buy >10 with price $30 per 1).
***** CCV UK:
– UK CARD NORMAL = $2,8 per 1 (buy >5 with price $3 per
1).
– UK MASTER CARD = $2,1 per 1 (buy >5 with price $2.5 per 1).
– UK VISA CARD = $2,8 per 1 (buy >5 with
price $2.5 per 1).
– UK AMEX CARD = $3,8 per 1 (buy >5 with price $4 per 1).
$4,9
– UK CARD WITH DOB = $15 per 1 (buy >5 with price $14 per 1).
– UK WITH BIN = $10 per 1 (buy >5 with price $9 per 1).
– UK WITH BIN WITH DOB = $25 per 1 (buy >20 with price $22 per 1).
– UK FULLZ INFO = $40 per 1 (buy >10 with price $35 per 1).
***** CCV AU:
– AU MASTER CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU VISA CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU AMEX CARD = $8.5 per 1 (buy >5 with price $8 per 1).
– AU DISCOVER CARD = $8.5 per 1 (buy >5 with price $8 per 1).
***** CCV CA:
– CA MASTER CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA BUSINESS = $14 per 1 (buy >5 with price $13 per 1).
Discover the best Zoe69-smith fully naked on cam – online porn webcam chat ever for free!
Naked hot webcams wNude amateur cams 942dacc
Netflix’s Best Movies for June 2024: Rotten Tomatoes Picks zach galifianakis comedy moviesmovie undertowmovie all the pretty horses
kms activatorOffice 2019
https://thekmsauto-net-web-.blogunteer.com/27015036/directions-to-improve-the-speed-of-windows-by-way-of-kmsauto-net
kms activator lite windows 10
Free download km5 auto
Glory Casino
Анонсы л2
great site Celestia wallet keplr
Glory Casino
to your liking, and quickly move to the section with Watch nudeMs Paradise before webcam – Live Porn Webcam chat on this topic. All categories are packed enough to make
Naked hot cams womNude hot cams girl ee0b6b6
Наша мастерская предлагает высококачественный сервисный центр по ремонту видеокарт в москве различных марок и моделей. Мы осознаем, насколько необходимы вам ваши графические карты, и готовы предложить сервис наилучшего качества. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что гарантирует долговечность и надежность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются владельцы видеокарт, включают проблемы с вентиляцией, выход из строя памяти, неработающие разъемы, сбои контроллера и ошибки драйверов. Для устранения этих поломок наши опытные мастера оказывают ремонт системы охлаждения, памяти, разъемов, контроллеров и ПО. Обратившись к нам, вы обеспечиваете себе качественный и надежный ремонт видеокарт.
Подробная информация доступна на сайте: https://remont-videokart-biz.ru
explanation phantom wallet login
https://salah-time.online/
live sex cams xxx
Toni Kroos https://tonikroos.prostoprosport-ar.com is a German footballer who plays as a central midfielder for Real Madrid and the German national team. World champion 2014. The first German player in history to win the UEFA Champions League six times.
To put these kinds off delivers to the test, our team utilizes the refer-a-pal hyperlinks.
Feel free to visit my site 공식홈페이지
Effective Tactics and Cheats for Thunder War
to Master the Combat Zone
Understanding the Essentials of Battle Thunder Hacks for Beginners
Thunder War, a popular internet multi-player experience, delivers
an engaging journey in aerial, terrain, and sea conflict.
For numerous users, dominating the title entails not just expertise but also
awareness of specific hacks that can boost play.
In this post, we’ll delve into some productive approaches
and hacks for Thunder War that can give you an lead over your
enemies cheats war thunder.
Why Applying Cheats in Thunder War Can Alter Your Play
Employing cheats in War Thunder can greatly transform your play adventure.
These exploits can deliver edges such as unlimited ammo,
augmented perception, or even immortality. However, it’s vital to comprehend
the moral implications and the possible risks, including profile bans.
Therefore, always utilize hacks sensibly and within the restrictions defined by the title designers.
Top Practices for Safe and Successful Combat Thunder Cheats Use
To risk-freely and successfully utilize exploits in Combat Thunder,
adhere to these recommended practices:
1. Examine and Confirm: Always verify the author of the exploit to avoid harmful programs.
2. Apply Carefully: Apply tricks in a way that minimizes the
hazard of discovery.
3. Remain Updated: Cheats often need upgrades to operate with the newest game
updates.
Premier Cheats in Battle Thunder and Ways to Implement Them Productively
Here are some of the most sought-after tricks for War Thunder:
– Auto-aims: Improve your firing exactness.
– See-through Walls: View inside barriers.
– ESP Cheats: Obtain intelligence about opponent positions.
To employ these hacks, you typically require to get designated apps.
Always ensure your protection programs is active to avoid
any risk dangers.
Perils and Benefits of Employing Hacks in War Thunder Play
Utilizing exploits in Thunder War can offer significant
rewards, such as enhanced performance and faster leveling.
However, the risks involve likely bans and the loss of your user.
It’s vital to evaluate these hazards against the rewards
and determine if using cheats coincides with your lasting gameplay
aims.
Ways in Which Exploits in War Thunder Affect Player Behavior and Fair Game
Exploits can interrupt the balance of just gameplay in Combat Thunder, causing frustration among other players.
While hacks might offer brief edges, they can impair the title’s player
base and total fun. Weigh the consequence on other users and the platform’s fairness before applying cheats.
Options to Exploits: Legitimate Ways to Improve in Combat Thunder
Instead of counting on cheats, consider these legal techniques
to enhance your expertise in Battle Thunder:
1. Practice Routinely: Frequent practice can enhance your experience.
2. Sign up with a Guild: Gaming with knowledgeable gamers can offer useful advice.
3. Study Tutorials: Learn from expert users through internet tutorials.
Developing Knowledgeable Conclusions About Cheats in Thunder War
While exploits in Battle Thunder can offer some gamers a superior position, it’s crucial to weigh the ethical and practical consequences.
Grasping the dangers, employing tricks carefully, and examining authorized approaches to
augment your experience can culminate to a more fulfilling and equitable gameplay experience.
Always value the welfare of the gaming user base and your pleasure of the platform.
free live porm
live cam guys
lice porn
Excellent and high-quality Zoee fully naked strip before cam for live sex webcam chat absolutely free and easy to watch on any device, just
Nude amateur camsNude hot webcams mo 7ad7_0e
smartblip home gadgets https://smartblip.com best price
kms-auto net windows 11
https://about-kms-www-.timeblog.net/63557831/instrument-kmsauto-software-for-activation-the-os-and-the-office-collection
kmsauto portable Office 2021
Free download km5 auto
Naomie-sky naked on webcam – live porn webcam chat absolutely free and easy to watch on any device, just
Nude hot cams modeNaked amateur cams 42dacc5
Robert Lewandowski https://robertlewandowski.prostoprosport-ar.com is a Polish footballer, forward for the Spanish club Barcelona and captain of the Polish national team. Considered one of the best strikers in the world. Knight of the Commander’s Cross of the Order of the Renaissance of Poland.
hairy cam dudes
live nude cams
На turklife.tv вы найдете всё, чтобы турецкий сериал смотреть онлайн на русском было удобно и приятно. Новинки 2024 года, отличное HD 1080 качество, профессиональная русская озвучка – всё это доступно на одном сайте. Множество жанров, ежедневные обновления и никакой рекламы в плеере.
На turklife.tv каждый день появляются новые серии, и всё это бесплатно! Заходите и наслаждайтесь лучшими турецкими сериалами без ограничений и регистрации.
shemele live
nude webcam couples
Промокоды в up-x позволят вам получить больше бонусов и выигрышей. Заходите на up-x промокоды и начните свою игру с преимуществом.
Just check out the best nude before webcam – Live Sex Chat ever!
Nude hot webcams woNude hot cams mode 6942dac
This is very attention-grabbing, You are an excessively professional blogger. I’ve joined your rss feed and look ahead to in search of more of your magnificent post. Additionally, I’ve shared your site in my social networks
http://zoa.su/prigotovit-edu-dlya-kota-samostoyatelno
купить диплом во владивостоке
http://uk-ahml.ru
купить диплом в вологде
Hey there! This post could not be written any better! Reading this post reminds me of my good old room mate! He always kept chatting about this. I will forward this post to him. Fairly certain he will have a good read. Thanks for sharing!
http://www.moglobi.ru/lenta-41.html
купить диплом в туймазы
http://superdiplomnik.ru
купить диплом в братске
live trans porn
Learn More martianwallet download
go to the website Cosmos wallet
couples live nude
сериал все сезоны волчонок бесплатно https://volchonok-tv.ru
click this link now martianwallet extension
says:Just check this out, sofi__lours nude strip on cam for live sex video chat for free!
Nude amateur webcamNude hot cams mode d57ad0_
read the full info here rabby login
Недавно у меня сломался автомобиль, а он мне необходим для работы. Денег на ремонт не было, и кредитная история оставляла желать лучшего. Друг посоветовал мне Телеграм канал малоизвестные мфо без отказа на карту . Он сказал, что там можно найти малоизвестные займы, которые дают деньги всем по паспорту от 18 лет. Также на канале есть поддержка, которая помогает выбрать лучший вариант и правильно подать заявку. Оформив займ за 10 минут, я получил 30 тысяч и отремонтировал автомобиль. Теперь я снова на ходу! Всем советую подписаться на этот канал.
to your liking, and quickly move to the section with Watch nudeNelly Live webcam – Sex Chat on this topic. All categories are packed enough to make
Naked hot webcams mNaked hot cams woman online porn show c5812fb
free live nude
nude live sex
Mohamed Salah https://mohamedsalah.prostoprosport-ar.com is an Egyptian footballer who plays as a forward for the English club Liverpool and the Egyptian national team. Considered one of the best football players in the world. Three-time winner of the English Premier League Golden Boot: in 2018 (alone), 2019 (along with Sadio Mane and Pierre-Emerick Aubameyang) and 2022 (along with Son Heung-min).
Excellent and high-quality SexyDelaJ naked strip on cam for live sex video chat absolutely free and easy to watch on any device, just
Nude hot cams model online sex showNude hot cams woma 2dacc58
Когда хочется смотреть турецкие сериалы 2024 онлайн на русском языке, turklife.tv становится отличным решением. Здесь вы найдете новейшие сериалы 2024 года в HD 1080 качестве и с превосходной русской озвучкой. Сайт предлагает широкий выбор жанров и удобное разделение по годам.
Каждый день добавляются новые серии, и все это абсолютно бесплатно и без рекламы. Это делает просмотр комфортным и приятным. Turklife.tv – ваш лучший выбор для просмотра турецких сериалов онлайн на русском языке.
Шаги к получению лицензии на недвижимость|Ключевая информация о лицензии на недвижимость|Как начать карьеру в недвижимости с лицензией|Успешные стратегии получения лицензии на недвижимость|Эффективные способы получения лицензии на недвижимость|Полезные советы по получению лицензии на недвижимость|Простой путь к получению лицензии на недвижимость|Шаг за шагом к лицензии на недвижимость|Эффективные стратегии получения лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Процесс получения лицензии на недвижимость: как это работает|Секреты скорого получения лицензии на недвижимость|Легкий путь к получению лицензии на недвижимость|Лицензия на недвижимость: ключ к успешной карьере|Профессиональные советы по получению лицензии на недвижимость|Как получить лицензию на недвижимость без стресса|Секреты получения лицензии на недвижимость от экспертов|Как быстро и легко получить лицензию на недвижимость|Ключевые моменты получения лицензии на недвижимость|Легко получите лицензию на недвижимость с этими советами|Получите лицензию на недвижимость и станьте профессиональным агентом|Основные шаги к профессиональной лицензии на недвижимость|Получение лицензии на недвижимость для начинающих: советы от экспертов|Простой путь к получению лицензии на недвижимость|Три шага к профессиональной лицензии на недвижимость|Лицензия на недвижимость: важные аспекты для успешного получения
How do I get my real estate license in Massachusetts How do I get my real estate license in Massachusetts .
dalycitynewspaper.com
to your liking, and quickly move to the section with DAFNE-HOT fully nude on cam – online sex chat on this topic. All categories are packed enough to make
Naked amateur cams girls online porn charNaked hot webcams m 812fb1f
Excellent and high-quality Blog absolutely free and easy to watch on any device, just
Nude hot webcams moNude hot webcams model live sex show d7_f11d
El uso regular de Yenki Derm puede reducir la apariencia de arrugas. Yenki Derm ayuda a mejorar la hidrataciГіn de la piel.
Hey I know this is off topic but I was wondering if you knew
of any widgets I could add to my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite some
time and was hoping maybe you would have some
experience with something like this. Please let me know if you run into
anything. I truly enjoy reading your blog and I look forward to your new updates. https://365.expresso.blog/question/les-avantages-des-remorques-fermees-pour-le-transport-de-votre-motoneige-2/
seo продвижение сайтов в москве агентство seo продвижение сайтов в москве агентство .
Just check out the best Ms Butterworths fully nude on cwebam – online porn show ever!
Naked hot webcams gNude hot cams model live porn char c5812fb
Секреты успешного получения лицензии на недвижимость|Ключевая информация о лицензии на недвижимость|Станьте лицензированным агентом по недвижимости|Советы по получению лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Получите профессиональную лицензию на недвижимость|Лицензия на недвижимость: важные аспекты|Как стать агентом с лицензией на недвижимость|Как получить лицензию на недвижимость: советы экспертов|Лицензия на недвижимость для начинающих: советы и рекомендации|Секреты профессиональной лицензии на недвижимость|Секреты скорого получения лицензии на недвижимость|Легкий путь к получению лицензии на недвижимость|Топ советы по получению лицензии на недвижимость|Как получить лицензию на недвижимость легко и быстро|Разберитесь в процессе получения лицензии на недвижимость: полное руководство|Получение лицензии на недвижимость: лучшие практики и советы|Как быстро и легко получить лицензию на недвижимость|Профессиональные советы по получению лицензии на недвижимость|Секреты успешного получения лицензии на недвижимость: что вам нужно знать|Как стать агентом по недвижимости с лицензией|Как получить лицензию на недвижимость быстро и легко|Получение лицензии на недвижимость для начинающих: советы от экспертов|Процесс получения лицензии на недвижимость: ключевые моменты|Эффективные советы по успешному получению лицензии на недвижимость|Лицензия на недвижимость: важные аспекты для успешного получения
How to get a real estate license in Arizona How to get a real estate license in Arizona .
Секреты успешного получения лицензии на недвижимость|Ключевая информация о лицензии на недвижимость|Подробное руководство по получению лицензии на недвижимость|Секреты быстрого получения лицензии на недвижимость|Эффективные способы получения лицензии на недвижимость|Полезные советы по получению лицензии на недвижимость|Лицензия на недвижимость: важные аспекты|Как стать агентом с лицензией на недвижимость|Как получить лицензию на недвижимость: советы экспертов|Успешное получение лицензии на недвижимость: шаг за шагом|Основные моменты получения лицензии на недвижимость|Секреты скорого получения лицензии на недвижимость|Получите лицензию на недвижимость и станьте профессионалом|Топ советы по получению лицензии на недвижимость|Советы по получению лицензии на недвижимость от профессионалов|Как получить лицензию на недвижимость без стресса|Шаги к успешной лицензии на недвижимость|Как быстро и легко получить лицензию на недвижимость|Ключевые моменты получения лицензии на недвижимость|Легко получите лицензию на недвижимость с этими советами|Получите лицензию на недвижимость и станьте профессиональным агентом|Секреты успешного получения лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Процесс получения лицензии на недвижимость: ключевые моменты|Эффективные советы по успешному получению лицензии на недвижимость|Сек
How to get a real estate license in California How to get a real estate license in California .
проститутки тюмени
use this link Cosmos wallet
Discover the best Blog ever for free!
Naked amateur webcams model live porn showNaked amateur cams b6b6942
мастерская по ремонту стиральных машин
определить местоположение по номеру
Lionel Andres Messi Cuccittini https://lionelmessi.prostoprosport-ar.com is an Argentine footballer, forward and captain of the MLS club Inter Miami, captain of the Argentina national team. World champion, South American champion, Finalissima winner, Olympic champion. Considered one of the best football players of all time.
сайт https://filmos.net/serials/
Cristiano Ronaldo https://cristiano-ronaldo.prostoprosport-ar.com is a Portuguese footballer, forward, captain of the Saudi Arabian club An-Nasr and the Portuguese national team. European Champion. Considered one of the best football players of all time. The best scorer in the history of football according to the IFFIS and fourth according to the RSSSF
Ncfyv_ncyuhv nude strip on cam for live sex chat
Naked amateur webcaNaked amateur webcams model live porn char 5d57ad4
определение местоположения по номеру телефона онлайн бесплатно
геолокация телефона по номеру онлайн бесплатно на карте в реальном времени
Some casinos even let you deposit and withdraw
utilizing cryptocurrencies, sujch as Bitcoin, Ethereum, Litecoin, and Ripple.
Also visit my web blog – 온카
vavada официальный вход
온라인 슬롯 사이트 추천
Zhu Houzhao는 Huang Jinzhou라는 단어를 들었을 때 눈이 빛났습니다.
Homepage von Melissa_crazy nude strip on webcam for StripChat live chat
Naked amateur camsNaked amateur webca 0b6b694
ремонт стиральных машин миле
Как получить лицензию на недвижимость|Легко и быстро получите лицензию на недвижимость|Как начать карьеру в недвижимости с лицензией|Советы по получению лицензии на недвижимость|Эффективные способы получения лицензии на недвижимость|Полезные советы по получению лицензии на недвижимость|Лицензия на недвижимость: важные аспекты|Как стать агентом с лицензией на недвижимость|Эффективные стратегии получения лицензии на недвижимость|Успешное получение лицензии на недвижимость: шаг за шагом|Процесс получения лицензии на недвижимость: как это работает|Секреты скорого получения лицензии на недвижимость|Легкий путь к получению лицензии на недвижимость|Топ советы по получению лицензии на недвижимость|Как получить лицензию на недвижимость легко и быстро|Эффективные стратегии для успешного получения лицензии на недвижимость|Секреты получения лицензии на недвижимость от экспертов|Инструкция по получению лицензии на недвижимость|Ключевые моменты получения лицензии на недвижимость|Легко получите лицензию на недвижимость с этими советами|Получите лицензию на недвижимость и станьте профессиональным агентом|Основные шаги к профессиональной лицензии на недвижимость|Получение лицензии на недвижимость для начинающих: советы от экспертов|Секреты быстрого получения лицензии на недвижимость|Эффективные советы по успешному получению лицензии на недвижимость|Лицензия на недвижимость: важные аспекты для успешного получения
How to get a realtor license in Colorado https://realestatelicensehefrsgl.com/states/colorado-real-estate-license/ .
movies dripping springs percy jackson 3 movie 2021watch 8mm filmwing on a prayer movie
kraken14 at – kraken зеркало, kraken клирнет зеркало
Официальный городской информационный портал – новости Ижевска и Удмуртии, криминал, дорожно-транспортные происшествия (ДТП), чрезвычайные происшествия(ЧП) https://vk.com/mdps18
Блэкспрут ссылка – Bs2site2, Blacksprut зеркало
Секреты успешного получения лицензии на недвижимость|Ключевая информация о лицензии на недвижимость|Станьте лицензированным агентом по недвижимости|Советы по получению лицензии на недвижимость|Разберитесь в процессе получения лицензии на недвижимость|Следуйте этим шагам для получения лицензии на недвижимость|Лицензия на недвижимость: важные аспекты|Как стать агентом с лицензией на недвижимость|Как получить лицензию на недвижимость: советы экспертов|Инструкция по получению лицензии на недвижимость|Процесс получения лицензии на недвижимость: как это работает|Секреты скорого получения лицензии на недвижимость|Получите лицензию на недвижимость и станьте профессионалом|Лицензия на недвижимость: ключ к успешной карьере|Профессиональные советы по получению лицензии на недвижимость|Эффективные стратегии для успешного получения лицензии на недвижимость|Секреты получения лицензии на недвижимость от экспертов|Как быстро и легко получить лицензию на недвижимость|Лицензия на недвижимость: ключ к успеху в индустрии недвижимости|Легко получите лицензию на недвижимость с этими советами|Простой путь к получению лицензии на недвижимость|Основные шаги к профессиональной лицензии на недвижимость|Шаги к успешной лицензии на недвижимость|Процесс получения лицензии на недвижимость: ключевые моменты|Эффективные советы по успешному получению лицензии на недвижимость|Лицензия на недвижимость: важные аспекты для успешного получения
How to get real estate license in Nevada https://realestatelicensehefrsgl.com/states/nevada-island-real-estate-license/ .
Zoe69-smith fully nude on cam – online porn webcam chat videos absolutely free and easy to watch on any device, just
Naked amateur webcams model online sex showNaked hot cams wom acc5812
Thanks for every other magnificent post. The place else may anyone get that type of information in such an ideal approach of writing? I have a presentation subsequent week, and I’m at the look for such info.
http://24news-24.ru/chem-tak-polezen-diplom-ob-okonchanii-vuza/
купить диплом в череповце
http://baikal-sez.ru
купить диплом в туймазы
Thanks , I have recently been searching for info approximately this subject for a while and yours is the greatest I have discovered till now. However, what in regards to the bottom line? Are you positive in regards to the supply?
http://mypechen.com/alfa-normiks/
купить диплом архитектора
http://diplom-msk.ru
купить диплом о среднем специальном
Excellent and high-quality Liliana nude sexy before webcam Sex Chat absolutely free and easy to watch on any device, just
Nude hot cams girls live sex showNude hot webcams gi 942dacc
отремонтировать телефон
мастер по ремонту стиральных машин бош
https://kraken14attt.ru/ – как зайти на kraken
my response jaxx app
Discover the best Ms Paradise nude before adult cam – Live Sex Chat ever for free!
Nude amateur camsNaked amateur cams 942dacc
carding shopping sites newfresh balance min 650$ LIVE
24/24 – 2024 (No DIE) 【Visit CvvDumps.US】 All COUNTRY US , UK , CA , AU , EU ,
CL , MO
————-CONTACT———————–
WEBSITE : >>>>>> CvvDumps✦ US
—– HERE COMES THE PRICE LIST ———–
***** CVV Other countries
JM VISA CARD = $4,1 per 1 (buy >5 with price $2.5 per 1).
MK VISA CARD = $2,6 per 1 (buy >5 with price $2.5 per 1).
SE VISA CARD = $4,2 per 1 (buy >5 with price $2.5 per 1).
ZA VISA CARD = $2,8 per 1 (buy >5 with price
$2.5 per 1).
***** CVV US:
– US MASTER CARD = $2,4 per 1 (buy >5 with price $3 per 1).
– US VISA CARD = $2,4 per 1 (buy >5 with price $2.5 per 1).
– US AMEX CARD = $2,7 per 1 (buy >5 with price $2.5 per 1).
– US DISCOVER CARD = $2,8 per 1 (buy >5 with price $3.5 per 1).
– US CARD WITH DOB = $15 per 1 (buy >5 with price $12 per 1).
– US FULLZ INFO = $40 per 1 (buy >10 with price $30
per 1).
***** CCV UK:
– UK CARD NORMAL = $2,9 per 1 (buy >5 with price $3 per 1).
– UK MASTER CARD = $3 per 1 (buy >5 with price $2.5 per 1).
– UK VISA CARD = $2,5 per 1 (buy >5 with price $2.5 per 1).
– UK AMEX CARD = $4,2 per 1 (buy >5 with price $4 per 1).
$5,1
– UK CARD WITH DOB = $15 per 1 (buy >5 with price $14 per 1).
– UK WITH BIN = $10 per 1 (buy >5 with price $9 per 1).
– UK WITH BIN WITH DOB = $25 per 1 (buy >20 with price $22 per 1).
– UK FULLZ INFO = $40 per 1 (buy >10 with price $35 per 1).
***** CCV AU:
– AU MASTER CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU VISA CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU AMEX CARD = $8.5 per 1 (buy >5 with price $8 per 1).
– AU DISCOVER CARD = $8.5 per 1 (buy >5 with price $8 per 1).
***** CCV CA:
– CA MASTER CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA BUSINESS = $14 per 1 (buy >5 with price $13 per 1).
kraken14.at – kraken darknet ссылка, kraken darknet
Вакцинация во время беременности, Аменорея с высоким уровнем ФСГ, Влияет ли стресс у мужчин на вероятность зачатия, Вагинальные кровотечения между менструациями, Мягкие роды
Усиление эффекта ванны с натуральными добавками
купить крипту – купить eth, exhub
Anderson Sousa Conceicao better known as Talisca https://talisca.prostoprosport-ar.com is a Brazilian footballer who plays as a midfielder for the An-Nasr club. A graduate of the youth team from Bahia, where he arrived in 2009 ten years ago.
Yassine Bounou https://yassine-bounou.prostoprosport-ar.com also known as Bono, is a Moroccan footballer who plays as a goalkeeper for the Saudi Arabian club Al-Hilal and the Moroccan national team. On November 10, 2022, he was included in the official application of the Moroccan national team to participate in the matches of the 2022 World Cup in Qatar
вавада казино официальный сайт вход
вавада зеркало рабочее
вавада рабочее зеркало
vavada casino официальный сайт
More hints localcryptos alternative
Blacksprut – Bs2site2, Bs2webes
Harry Edward Kane https://harry-kane.prostoprosport-ar.com is an English footballer, forward for the German club Bayern and captain of the England national team. Considered one of the best football players in the world. He is Tottenham Hotspur’s and England’s all-time leading goalscorer, as well as the second most goalscorer in the Premier League. Member of the Order of the British Empire.
Neymar da Silva Santos Junior https://neymar.prostoprosport-ar.com is a Brazilian footballer who plays as a striker, winger and attacking midfielder for the Saudi Arabian club Al-Hilal and the Brazilian national team. Considered one of the best players in the world. The best scorer in the history of the Brazilian national team.
https://telegra.ph/futbol-statistika-sbornyh-06-26-2
срочный ремонт телефонов москва
Искал автошколу в своем районе у м. Аэропорт или Сокол, там одна улица проходит. Считаю, что сделал неплохой выбор волжская автошкола
Онлайн казино с мгновенными выплатами и безопасной игрой
лучшие онлайн казино на деньги онлайн казино беларусь .
https://telegra.ph/smotret-futbolnuyu-statistiku-06-26-2
ремонт телефонов
article injector roblox
Достижение положительного результата в освоении управления легковым автомобилем и получении водительских прав гарантирует автошкола с репутацией автошкола текстильщики
see it here fortnite aimbot download
Ла2
Erling Breut Haaland https://erling-haaland.prostoprosport-ar.com is a Norwegian footballer who plays as a forward for the English club Manchester City and the Norwegian national team. English Premier League record holder for goals per season.
cs2 cheat – cs2 injector, cs2 cheats free
где ремонтируют телефоны
Преимущества строительства дома из бруса 9х12 | Преимущества строительства дома из бруса 9х12 | Выбор кровельных материалов для дома из бруса 9х12 | Секреты уютного интерьера в доме из бруса 9х12 | Типы фундаментов для дома из бруса 9х12 | Как выбрать правильные окна и двери для дома из бруса 9х12 | Дизайн ландшафта для дома из бруса 9х12 | Новинки в строительстве домов из бруса 9х12 | Советы по созданию уютной зоны отдыха в доме из бруса 9х12 | Расходы на строительство дома из бруса 9х12
дома из бруса 9х12 https://domizbrusa-9x12spb.ru/ .
Шаги к получению лицензии на недвижимость|Ключевая информация о лицензии на недвижимость|Подробное руководство по получению лицензии на недвижимость|Секреты быстрого получения лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Следуйте этим шагам для получения лицензии на недвижимость|Секреты успешного получения лицензии на недвижимость|Шаг за шагом к лицензии на недвижимость|Три шага к успешной лицензии на недвижимость|Успешное получение лицензии на недвижимость: шаг за шагом|Процесс получения лицензии на недвижимость: как это работает|Как получить лицензию на недвижимость и стать успешным агентом|Легкий путь к получению лицензии на недвижимость|Топ советы по получению лицензии на недвижимость|Профессиональные советы по получению лицензии на недвижимость|Как получить лицензию на недвижимость без стресса|Шаги к успешной лицензии на недвижимость|Как быстро и легко получить лицензию на недвижимость|Лицензия на недвижимость: ключ к успеху в индустрии недвижимости|Секреты успешного получения лицензии на недвижимость: что вам нужно знать|Простой путь к получению лицензии на недвижимость|Как получить лицензию на недвижимость быстро и легко|Шаги к успешной лицензии на недвижимость|Секреты быстрого получения лицензии на недвижимость|Эффективные советы по успешному получению лицензии на недвижимость|Сек
How to Get a Real Estate License in Texas How to Get a Real Estate License in Texas .
bookmarked!!, I like your website!
Ali al-Buleahi https://ali-al-bulaihi.prostoprosport-ar.com Saudi footballer, defender of the club ” Al-Hilal” and the Saudi Arabian national team. On May 15, 2018, Ali al-Buleakhi made his debut for the Saudi Arabian national team in a friendly game against the Greek team, coming on as a substitute midway through the second half.
Попробуйте свою удачу в лучших онлайн казино, советуем.
Веселье и азарт: самые популярные онлайн казино, попробуйте прямо сейчас.
Популярные азартные игры в онлайн казино, испытайте прямо сейчас.
Бонусы и выигрыши: лучшие онлайн казино для вас, попробуйте прямо сейчас.
Обновленные возможности для любителей азарта в онлайн казино, испытайте прямо сейчас.
Играйте в лучшие онлайн казино и выигрывайте крупные суммы денег, испытайте сейчас.
Играйте в увлекательные игры и выигрывайте крупные суммы в онлайн казино, посетите прямо сейчас.
Большие выигрыши и возможности: лучшие онлайн казино, попробуйте сейчас.
Популярные игры и призы в онлайн казино, попробуйте прямо сейчас.
Бонусы и выигрыши: самые популярные онлайн казино для вас, присоединяйтесь прямо сейчас.
Популярные возможности для азартных игроков в онлайн казино, посетите прямо сейчас.
Играйте и выигрывайте крупные суммы в самых популярных онлайн казино, присоединяйтесь сейчас.
Лучшие игры и призы в онлайн казино, попробуйте прямо сейчас.
Наши рекомендации: самые популярные онлайн казино, посетите сейчас.
Популярные игры и призы в онлайн казино, попробуйте прямо сейчас.
Лучшие бонусы и выигрыши в онлайн казино, присоединяйтесь прямо сейчас.
Новые возможности и азартные игры в онлайн казино,
лучшие онлайн казино с минимальным депозитом https://onlayn-kazino-reyting-belarusi.com/ .
Самые интересные и познавательные статьи про проституток: https://sexcloud.ru/
Здесь вы найдете интересное общение о любви и сексе: https://sexcloud.ru/
skinchanger – skinchanger cs2 free, skinchanger
Hi, for all time i used to check webpage posts here early in the daylight, for the reason that i enjoy to find out more and more.
http://adobe-photoshop.ru/load/14/
купить диплом в ишимбае
http://vash-opros.ru
купить диплом строителя
Because the admin of this website is working, no hesitation very rapidly it will be well-known, due to its quality contents.
http://izimil.ru/2022/02/
купить диплом программиста
http://wmtext.ru
купить диплом охранника
Luka Modric https://lukamodric.prostoprosport-ar.com is a Croatian footballer, central midfielder and captain of the Spanish club Real Madrid, captain of the Croatian national team. Recognized as one of the best midfielders of our time. Knight of the Order of Prince Branimir. Record holder of the Croatian national team for the number of matches played.
wikipedia reference skin swapper
ремонт телефонов в москве
beef movie cast where to stream smile moviegrand theft auto movie 2021nell newman movies
Borrowers who’ve been misled by colleges have lengthy had the ideal to
request biden student loan forgiveness forgiveness.
Играйте в лучшие онлайн казино в Румынии, для шанса на крупные выплаты.
Выберите лучшие онлайн казино в Румынии, чтобы испытать удачу и заработать миллионы.
Выбор казино онлайн для румынских геймеров, где вас ждут невероятные бонусы и акции.
Загляните в мир онлайн казино в Румынии, для увлекательных игровых приключений.
Выберите самое надежное онлайн казино в Румынии, для возможности выиграть крупные суммы денег.
cazino online bani reali cazino online bani reali .
gaggenau ремонт холодильника
https://e-porn.net free xxx tube videos webcams dating,
онлайн камеры, знакомства
ремонт телефонов
Playing the Aviator Game involves a few simple steps:
tigrinho demo gratis
http://kvadrociklov-prokat.ru/
look at this website how to mod fortnite
buy real tiktok followers best place to buy tiktok followers
next fortnite cheats free
ремонт смартфонов в москве
buy tiktok followers uk https://www.templates.com/blog/how-to-get-more-followers-on-tiktok-expert-tips/
Захватывающий мир онлайн казино, ставьте на удачу и выигрывайте в известных онлайн казино, наслаждайтесь азартом.
Онлайн казино: безопасность и азарт, вероятность выиграть увеличивается.
Играйте в лучших онлайн казино, переходите и побеждайте.
Онлайн казино: азарт и выигрыш, выигрывайте и наслаждайтесь.
Зарабатывайте крупные суммы в онлайн казино, тренируйтесь и побеждайте.
лучшие онлайн казино на деньги лучшие онлайн казино на деньги .
ремонт сотовых телефонов рядом
http://atvbizon.ru/
social interaction adds a new layer of excitement and competition to the game, making it more engaging and
tigrinho
You also need to develop a password to access your account.
My web blog … Florida Lottery
где ремонт телефонов
There is such a wiude range of sports that are well-known across South Africa.
my web-site … Check here
Наши – гарантия надежности и долговечности.
кракен14.ат – как зайти на kraken kraken onion site, kraken ссылка зеркало
Unique Features of the Aviator Game
tigrinho demo gratis
https://besuchszweck.org/
Hello.
Looking for the best online casinos? Check out our pro-curated list of real money casino sites ranked by game variety, fairness, bonus ease, and more -https://tinyurl.com/ypp4smrx
https://lavirgule.news/
look at this site jaxx wallet
demo versions or free play options to allow players to practice before betting real money.
tigrinho demo
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в альметьевске, купить диплом в бердске, купить диплом в нижневартовске, купить диплом в северодвинске, купить диплом в братске, потом про дипломы вузов, подробнее здесь http://arts.gpaeburgas.org/profile.php?uid=10271
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успешной учебы!
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом электрика, купить диплом физика, купить диплом массажиста, купить диплом в клинцах, купить диплом в находке, получил базовую информацию.
Остановился в итоге на материале купить диплом товароведа, https://inspektor.blox.ua/2024/06/%d0%ba%d1%83%d0%bf%d0%b8%d1%82%d1%8c-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc-%d0%b2-%d0%be%d0%b1%d0%bd%d0%b8%d0%bd%d1%81%d0%ba%d0%b5.html
https://devpost.com/diplomrussian
http://jagplay.ekafe.ru/viewtopic.php?f=22&t=4037
http://arsenal.spybb.ru/viewtopic.php?id=634#p691
http://mydnepr.pp.ua/forum/topic.php?forum=7&topic=911
Успехов в учебе!
his response jaxx liberty download
https://kraken14attt.ru – kraken официальный сайт ссылка
Thanks for the auspicious writeup. It actually
was a leisure account it. Look advanced to far added agreeable from you!
By the way, how could we keep up a correspondence? http://[email protected]/message/index.php
Зачем выбирать дом из бруса 9х12 | Как выбрать идеальный проект для дома из бруса 9х12 | Особенности кровли дома из бруса 9х12 | Выбор системы отопления для дома из бруса 9х12 | Типы фундаментов для дома из бруса 9х12 | Выбор фундамента для дома из бруса 9х12 | Как обустроить участок вокруг дома из бруса 9х12 | Современные технологии строительства дома из бруса 9х12 | Для комфортного отдыха: зона lounge в доме из бруса 9х12 | Сколько стоит построить дом из бруса 9х12
одноэтажный дом из бруса 9х12 https://domizbrusa-9x12spb.ru/ .
https://interventionist.us/
линии средств для интимной гигиены IntiLINE каталог
kraken14.at – kraken официальный, kraken ссылка для тору
The best film magazin https://orbismagazine.com, film industry trade publications in 2024 to keep you informed with the latest video production, filmmaking, photographynews. We create beautiful and magnetic projects.
exhub официальный сайт – exhub обменник, bestchange обменник
plane crashes, making it a game of both luck and timing. This dynamic gameplay keeps players engaged and coming
tigrinho demo gratis
Если любите турецкие сериалы 2023 на русском языке, то вам точно понравится сайт turkhit.tv. Здесь есть сериалы разных годов и жанров, все в HD качестве и с полноценным русским переводом. Вы можете наслаждаться просмотром бесплатно и без всплывающей рекламы.
Каждый день добавляются новые серии, так что вы всегда будете в курсе последних событий в мире турецких сериалов. Заходите на turkhit.tv и наслаждайтесь лучшими сериалами 2023 года без ограничений и без лишних хлопот.
Мой старый компьютер стал сильно тормозить, а я давно мечтал собрать новый, мощный. Денег на это не хватало, и кредитная история была не самой лучшей. В поисках решения я наткнулся на Телеграм канал займ на карту мфо в Яндексе на первом месте. Это сразу внушило доверие. На канале я нашел список малоизвестных займов, которые давали деньги всем по паспорту от 18 лет, с выгодными ставками от 0 до 0.8 процента в день. За 10 минут я оформил займ и получил 30 тысяч. Теперь у меня мощный компьютер, и я могу работать и играть без проблем. Всем советую подписаться на этот канал!
discover this info here localbitcoins review
They acquire numbers on their tickets and, if they match
the numbers you picked, you get the prize at that right moment.
Have a look at my webpage; https://Empiressmp.gay/wikis/MCRP/index.php/User:VernonIngamells
mounjaro tirzepatide купить – мунджаро тирзепатид, mounjaro москва
Nice article, thanks! Just check SkyelarSommer nude strip on cam for live sex video chat this out.
Naked amateur camsNude hot webcams mo d7_0ebd
установка компонентной акустики в передние – динамик прайд 20, штатная акустика веста
All profits generated from Powerball ticket sales in Florida are given to the Educational
Enhancement Trust Fund (EETF) to advantage education all through the state.
Feel free to surf to mmy website – 네임드
What’s up i am kavin, its my first time to commenting anyplace, when i read this paragraph i thought i could also make comment due to this sensible post.
http://yogictv.ru/dzhalandhara-bandha/
купить диплом в минусинске
http://git-ugra.ru
купить диплом в дзержинске
Hmm is anyone else having problems with the images on this blog loading? I’m trying to find out if its a problem on my end or if it’s the blog. Any feed-back would be greatly appreciated.
http://animesocial.su/blogs/1138/Как-купить-аттестат-или-диплом-у-нас-в-онлайн-магазине
купить диплом повара
http://diploms-help.ru
купить дипломы о высшем цены
Анализ почвы или анализ питьевой воды
анализ микроклимата рабочего места
https://gklab.ru/korrektirovka-inventarizaczii-vybrosov/
Ещё можно узнать: евро значок валюты
анализ отходов производства
https://livecamsporno.com/
ТК АзияТорг: Надежный Партнер в Мире Сетевого и Телекоммуникационного Оборудования
В современном бизнесе успех определяется скоростью и качеством коммуникаций.
ТК АзияТорг, с более чем пятилетним опытом, представляет собой ведущего поставщика сетевого и телекоммуникационного оборудования, а также серверов для бизнеса.
Наши клиенты и партнеры доверяют нам благодаря нашему безупречному
обслуживанию и высококачественной
продукции.
## Почему ТК АзияТорг?
### Широкий Ассортимент Оборудования
Мы предлагаем широкий спектр сетевого и телекоммуникационного оборудования, а также серверов,
которые идеально подходят для любых бизнес-задач.
Наша продукция отвечает
самым высоким стандартам качества и надежности, что обеспечивает бесперебойную работу ваших систем.
### Профессиональное Сотрудничество
Более пяти лет успешного сотрудничества с клиентами и поставщиками доказывают нашу репутацию надежного партнера.
Мы всегда стремимся к долгосрочным и взаимовыгодным отношениям, предлагая индивидуальный подход и
гибкие условия сотрудничества.
### Филиал в Гуанчжоу
Наличие собственного филиала в
Гуанчжоу позволяет нам быть ближе к нашим
азиатским партнерам и поставщикам,
что обеспечивает оперативные поставки и конкурентные цены.
Это стратегическое расположение также
дает нам возможность быстро реагировать на изменения рынка и потребности клиентов.
### Комплексные Финансово-Логистические Услуги
Мы предлагаем финансово-логистические услуги “под ключ”, которые включают в себя все этапы — от
закупки оборудования до его доставки и установки.
Наши эксперты берут на себя все заботы, связанные с транспортировкой и таможенным
оформлением, что позволяет вам
сосредоточиться на развитии бизнеса.
## Доверие и Качество
ТК АзияТорг стремится предоставлять только лучшее оборудование и услуги, чтобы
помочь вашему бизнесу достигать новых высот.
Мы гордимся нашей репутацией и всегда нацелены на
совершенствование всех аспектов нашей деятельности.
Доверяйте нам, и вы получите надежного партнера, который всегда готов поддержать ваш бизнес и
помочь ему расти.
Свяжитесь с нами сегодня и узнайте, как ТК АзияТорг может помочь вашему
бизнесу стать еще успешнее!
My homepage: “http://kjpump.hdib.gethompy.com/bbs/board.php?bo_table=free&wr_id=130516”
Playing the Aviator Game online offers several benefits:
tigrinho demo gratis
ТК АзияТорг: Надежный Партнер в Мире Сетевого и Телекоммуникационного Оборудования
В современном бизнесе успех определяется скоростью и качеством коммуникаций.
ТК АзияТорг, с более чем пятилетним опытом, представляет собой ведущего поставщика сетевого и телекоммуникационного оборудования, а также серверов для бизнеса.
Наши клиенты и партнеры доверяют
нам благодаря нашему безупречному обслуживанию и высококачественной
продукции.
## Почему ТК АзияТорг?
### Широкий Ассортимент Оборудования
Мы предлагаем широкий спектр
сетевого и телекоммуникационного оборудования, а также серверов, которые идеально подходят для любых бизнес-задач.
Наша продукция отвечает самым
высоким стандартам качества и надежности, что обеспечивает бесперебойную работу ваших систем.
### Профессиональное Сотрудничество
Более пяти лет успешного сотрудничества с клиентами и поставщиками доказывают нашу репутацию надежного партнера.
Мы всегда стремимся к долгосрочным и взаимовыгодным отношениям, предлагая
индивидуальный подход и гибкие условия
сотрудничества.
### Филиал в Гуанчжоу
Наличие собственного филиала в Гуанчжоу позволяет нам быть ближе к нашим азиатским партнерам и поставщикам, что
обеспечивает оперативные поставки
и конкурентные цены. Это стратегическое расположение также
дает нам возможность быстро реагировать на
изменения рынка и потребности клиентов.
### Комплексные Финансово-Логистические Услуги
Мы предлагаем финансово-логистические
услуги “под ключ”, которые включают
в себя все этапы — от закупки оборудования до его доставки и установки.
Наши эксперты берут на себя все заботы, связанные с транспортировкой и таможенным оформлением, что позволяет вам сосредоточиться на развитии бизнеса.
## Доверие и Качество
ТК АзияТорг стремится предоставлять только лучшее оборудование и услуги, чтобы помочь вашему бизнесу достигать
новых высот. Мы гордимся нашей репутацией и всегда нацелены на совершенствование всех
аспектов нашей деятельности.
Доверяйте нам, и вы получите надежного партнера, который всегда готов поддержать
ваш бизнес и помочь ему расти.
Свяжитесь с нами сегодня и узнайте, как ТК АзияТорг может помочь
вашему бизнесу стать еще успешнее!
Also visit my web site :: “https://usdwiki.com/index.php/Server”
http://ek-x.ru/
Does your site have a contact page? I’m having trouble locating it but, I’d like to shoot you an e-mail.
I’ve got some ideas for your blog you might be interested in hearing.
Either way, great blog and I look forward to seeing it improve over time.
Yesterday, while I was at work, my sister stole my iphone and tested
to see if it can survive a twenty five foot drop, just so she can be a
youtube sensation. My iPad is now destroyed and she has 83
views. I know this is completely off topic but I had to
share it with someone!
Ваш надежный партнер в строительстве
Наша строительная компания предлагает высококачественные услуги по постройке фундаментов и стен для различных сооружений. Мы предоставляем услуги под ключ, обеспечивая применение качественных материалов и соблюдение всех строительных норм. В стоимость входит поэтапная оплата, и мы предоставляем гарантию на все виды работ.
Список наших услуг:
Фундамент под ключ: https://mosvip-stroy.ru
Фундаментная плита: https://mosvip-stroy.ru/fundamentnaya_plita
Шведская утепленная плита: https://mosvip-stroy.ru/ushp
Ленточное основание: https://mosvip-stroy.ru/lentochnyj_fundament
Свайное основание: https://mosvip-stroy.ru/svajnyj_fundament
Монтаж стен: https://mosvip-stroy.ru/vozvedenie-sten
Столбчатое основание: https://mosvip-stroy.ru/stolbchatyj_fundament
Блочная основа: https://mosvip-stroy.ru/blochnyj_fundament
Свайно-ростверковая система: https://mosvip-stroy.ru/svajno-rostverkovyj_fundament
Player Reviews and Testimonials
tigrinho demo
https://xploredomains.com/2024-06-01?page=51
Just check this out, -Sexy_Barbie- naked strip on cam for live sex video chat
Naked hot cams girNaked amateur webca 812fb1f
ТК АзияТорг: Надежный Партнер в Мире Сетевого и Телекоммуникационного Оборудования
В современном бизнесе успех определяется скоростью и качеством коммуникаций.
ТК АзияТорг, с более чем пятилетним опытом, представляет собой ведущего
поставщика сетевого и телекоммуникационного оборудования, а также серверов для бизнеса.
Наши клиенты и партнеры доверяют нам благодаря нашему безупречному обслуживанию и высококачественной продукции.
## Почему ТК АзияТорг?
### Широкий Ассортимент Оборудования
Мы предлагаем широкий спектр сетевого
и телекоммуникационного оборудования, а также серверов,
которые идеально подходят для любых бизнес-задач.
Наша продукция отвечает самым высоким стандартам качества и надежности, что обеспечивает бесперебойную работу ваших систем.
### Профессиональное Сотрудничество
Более пяти лет успешного сотрудничества с клиентами и поставщиками доказывают нашу репутацию надежного партнера.
Мы всегда стремимся к долгосрочным и взаимовыгодным отношениям, предлагая индивидуальный подход и гибкие условия сотрудничества.
### Филиал в Гуанчжоу
Наличие собственного филиала
в Гуанчжоу позволяет нам быть ближе к нашим азиатским партнерам и поставщикам, что обеспечивает
оперативные поставки и конкурентные цены.
Это стратегическое расположение также дает нам возможность быстро реагировать на изменения рынка и потребности клиентов.
### Комплексные Финансово-Логистические
Услуги
Мы предлагаем финансово-логистические услуги “под ключ”,
которые включают в себя все этапы — от закупки оборудования до его доставки и установки.
Наши эксперты берут на себя все заботы, связанные с
транспортировкой и таможенным оформлением, что позволяет вам сосредоточиться
на развитии бизнеса.
## Доверие и Качество
ТК АзияТорг стремится предоставлять только лучшее оборудование и услуги, чтобы помочь вашему бизнесу достигать новых высот.
Мы гордимся нашей репутацией и всегда нацелены на совершенствование всех аспектов нашей деятельности.
Доверяйте нам, и вы получите надежного партнера, который всегда готов поддержать ваш бизнес и помочь ему расти.
Свяжитесь с нами сегодня и узнайте, как ТК АзияТорг
может помочь вашему бизнесу стать
еще успешнее!
Take a look at my web blog – “https://angryowners.site/index.php/User:WendyLeverett7”
NGolo Kante https://ngolokante.prostoprosport-ar.com is a French footballer who plays as a defensive midfielder for the Saudi Arabian club Al-Ittihad and the French national team. His debut for the first team took place on May 18, 2012 in a match against Monaco (1:2). In the 2012/13 season, Kante became the main player for Boulogne, which played in Ligue 3.
Наши специалисты помогут вам выбрать лучшие .
csgo cheats – cs2 hacks free download, wallhack cs2
SavageKitty naked on webcam – live sex show absolutely free and easy to watch on any device, just
Nude amateur camsNude hot webcams woman online sex show fee0b6b
На сайте https://dekorativnye-shtukaturki-77.ru/ в огромном многообразии находится декоративная штукатурка. Она необходима для того, чтобы разнообразить интерьер и сделать его более стильным и ярким. Для того чтобы принять окончательное решение, необходимо ознакомиться с каталогом. Штукатурка дает возможность создать удивительные узоры, интересные рисунки, которые станут яркой деталью. Этот материал отличается экологической чистотой, он полностью безопасен для здоровья людей, животных.
scooby doo movies the movie heat 1995characters on all american season 3movie montage songs
cs2 skin changer inknowncheats – skin change cs2, free cs2 skinchanger
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом инженера механика, купить диплом массажиста, купить диплом в керчи, купить диплом механика, купить диплом в бугульме, потом попал на http://odessaforum.getbb.ru/viewtopic.php?f=5&t=19963 и там решили все мои учебные заботы!
Удачи!
рќ™єрќљ’рќљ›рќљЉвќ¦вњЇајєвЅвј 𝐨𝐧𝐥𝐲𝐟𝐚𝐧𝐬/𝐜𝐡𝐢𝐥𝐥𝐰𝐢рќђрќђЎрќђ¤рќђўрќђ«рќђљ fully naked strip before cam for online porn chat absolutely free and easy to watch on any device, just
Naked amateur camsNude amateur webcam ee0b6b6
Place Your Bet: Choose the amount you want to bet.
fortune tiger
Купить Кокаин в Киеве? Цена на Кокаин САЙТ – https://koks.top/
.
.
Доставка В руки Кокаин в Киеве – https://koks.top/
Закладки с гарантией в Киеве – https://koks.top/
Чистый Кокаин в Киеве САЙТ – https://koks.top/
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
Теги – Купить Кокаин в Киеве?
Кокаин в Киеве Доставка в руки?
Закладки Кокаин в Киеве?
Где Купить Кокаин в Киеве?
Лучший Кокаин в Киеве заказать Кокаин круглосуточно?
Кокаин Украина
https://www.intensivecare.org.tr/ttb/1129/teged-%E2%80%9Culusal-tip-e%C4%9Fitimi-sempozyumu-2017%E2%80%9D
https://technofizi.net/sitelike/satilikbahis.net
Excellent and high-quality Saritahoneyy nude on cam – online porn webcam chat absolutely free and easy to watch on any device, just
Naked hot webcams mNude amateur webcam 57ad2_c
Ruben Diogo da Silva Neves https://ruben-neves.prostoprosport-ar.com is a Portuguese footballer who plays as a midfielder for the Saudi Arabian club Al-Hilal and the Portuguese national team. Currently, Ruben Neves plays for the Al-Hilal club wearing number 8. His contract with the Saudi club is valid until the end of June 2026.
wohnungen montenegro
hotels zum verkaufen
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом о среднем образовании, купить диплом в костроме, можно ли купить диплом, купить диплом в кемерово, купить аттестат за 9 класс. Постепенно углубляясь, нашел отличный ресурс здесь: http://www.hcceskalipa.cz/bazarek/radiplomacom-0, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
says:Just check this out, Ariel Moore fully nude on cam – live porn webcam chat for free!
Naked amateur camsNaked hot webcams girls online porn char cc5812f
While the game itself is free to access, playing involves placing bets with real money. Some platforms may offer
tigrinho
griezmann antoine
play in diablo game here
griezmann-antoine-fr.biz
Discover the best sophia_leurre fully naked stripping on cam for live sex video webcam chat ever for free!
Naked hot webcams model live porn showNaked amateur cams b1fb65d
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в ижевске, купить диплом архитектора, купить диплом врача, купить диплом в таганроге, купить диплом в новочебоксарске. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://fanfiction.borda.ru/?1-10-0-00007449-000-0-0-1714289886 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успехов в учебе!
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в азове, купить диплом во владивостоке, купить диплом технический, купить диплом магистра, купить диплом в южно-сахалинске и получил базовые знания. В итоге остановился на материале: https://www.fototage-karlsruhe.de/blog/2024/06/02/%d1%84%d0%be%d1%80%d0%bc%d0%b0-%d0%bf%d0%be%d0%b8%d1%81%d0%ba%d0%b0-%d0%bd%d1%83%d0%b6%d0%bd%d0%be%d0%b3%d0%be-%d1%81%d1%81%d1%83%d0%b7%d0%b0/
Успехов в учебе!
https://www.livevideochat.xyz/
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом нового образца, купить диплом строителя, купить аттестат школы, купить диплом охранника, купить диплом в рязани, затем наткнулся на http://mockwanasvyazi.getbb.ru/viewtopic.php?f=12&t=519
https://www.southjerseyonline.net/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=84
https://bmw-donbass.ru/gallery/image/540-%D0%B1%D0%BE%D0%BB%D1%8C%D1%88%D0%BE%D0%B9-%D0%B0%D1%81%D1%81%D0%BE%D1%80%D1%82%D0%B8%D0%BC%D0%B5%D0%BD%D1%82-%D1%83%D0%BD%D0%B8%D0%B2%D0%B5%D1%80%D1%81%D0%B8%D1%82%D0%B5%D1%82%D1%81%D0%BA%D0%B8%D1%85-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2-%D0%BF%D0%BE-%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D1%8B%D0%BC-%D1%86%D0%B5%D0%BD%D0%B0%D0%BC/
http://mus-ecole.maxbb.ru/topic1799.html
http://probnikzvi.bestbb.ru/viewtopic.php?id=277
, где все мои учебные вопросы были решены!
Успешной учебы!
cash-out perfectly.
jogo do tigrinho
Hi there, just became aware of your blog through Google, and
found that it’s really informative. I am gonna watch out for brussels.
I’ll be grateful if you continue this in future.
Numerous people will be benefited from your writing.
Cheers! https://newy.Lordfilm-S.club/user/DanieleBlamey/
to your liking, and quickly move to the section with Monika_youthful naked strip on cam for live porn movie show on this topic. All categories are packed enough to make
Nude hot webcams moNaked hot cams mod 6942dac
Kobe Bean Bryant https://kobebryant.prostoprosport-ar.com is an American basketball player who played in the National Basketball Association for twenty seasons for one team, the Los Angeles Lakers. He played as an attacking defender. He was selected in the first round, 13th overall, by the Charlotte Hornets in the 1996 NBA Draft. He won Olympic gold twice as a member of the US national team.
A player in Michigan had a excellent commence to the new year, winning the $842.4 million Powerball
jackpot on Monday night.
Feel free to surf to my web blog; 이번주 로또번호 추천
Make thousands of bucks. Financial robot will help you to do it! https://t.me/cryptaxbot/14
The major goals of Swdish massage are to unwind the muscle tissues and strengthen blood and lymph circulation.
My web page … 출장 마사지
Excellent and high-quality Lola naked strip before cam for live sex webcam chat absolutely free and easy to watch on any device, just
Nude hot cams modeNaked amateur webca 1fb65d5
Thanks for every other great post. Where else may anybody
get that type of information in such an ideal manner of writing?
I’ve a presentation next week, and I’m at the look for such
info. http://Forum.Altaycoins.com/profile.php?id=552054
https://lebelligerant.com/
https://pornkingcams.com/
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить аттестат за 11 класс, куплю диплом высшего образования, купить диплом в курске, купить диплом в великих луках, купить диплом фитнес инструктора. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://wiki.mdomtv.net/index.php?title=??????_??????_??_?_??????:_????????_?_???????? и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
https://polskikompas.com/
Register an account, make a deposit, and navigate to the Aviator Game to start playing.
tigrinho demo
рќ™єрќљ’рќљ›рќљЉвќ¦вњЇајєвЅвј 𝐨𝐧𝐥𝐲𝐟𝐚𝐧𝐬/𝐜𝐡𝐢𝐥𝐥𝐰𝐢рќђрќђЎрќђ¤рќђўрќђ«рќђљ fully nude strip before cam for live porn chat absolutely free and easy to watch on any device, just
Naked amateur camsNude hot cams woma 0b6b694
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом в сарове, купить диплом в якутске, купить диплом логопеда, купить диплом в ейске, #купить диплом в гуково, а затем переключился на дипломы вузов. Подробности здесь: https://olivebookmarks.com/story17442381/%D0%BD%D0%B5%D0%B4%D0%B0%D0%B2%D0%BD%D0%BE-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%BE%D0%BB%D1%83%D1%87%D0%B8%D0%BB%D0%B0
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Хорошей учебы!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом техника, купить диплом в йошкар-оле, купить диплом в тобольске, купить аттестаты за 9, #купить диплом геодезиста, а затем переключился на дипломы вузов. Подробности здесь: http://bl.com.tw/index.php?title=???_????????_??????_?_??????_???_??????_?_???????_?_???????
http://pyha.ru/forum/topic/11355.1#msg213780
http://dachaweek.ru/kupit-diplom-bezopasno-i-legalno
http://ya.10bb.ru/viewtopic.php?id=2449#p4517
http://jamsun.net/doku.php?id=??????_??????_?_??????_?_??????_???????????
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Удачи!
It is not my first time to pay a quick visit this web site,
i am visiting this web page dailly and obtain fastidious information from here all the time. https://rajmudraofficial.com/question/designer-de-cuisine-sur-la-rive-sud-creez-votre-espace-culinaire-ideal-10/
to your liking, and quickly move to the section with Carolina naked webcam – online sex webcam chat on this topic. All categories are packed enough to make
Naked hot cams modNude hot webcams mo 65d57ad
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить дипломы о высшем, купить диплом о среднем образовании, купить диплом дизайнера, купить диплом в иваново, купить аттестаты за 11 и получил базовые знания. В итоге остановился на материале: http://vsetutonline.com/forum/member.php?u=76509
Успехов в учебе!
The user interface of the Aviator Game is designed to be intuitive and user-friendly. The clean design and easy
п»їtigrinho demo
Hi, everything is going nicely here and ofcourse every one is sharing data,
that’s truly excellent, keep up writing.
Открытки https://t.me/cards_and_congratulations и Поздравления с открытками
Купити ліхтарики https://bailong-police.com.ua оптом та в роздріб, каталог та прайс-лист, характеристики, відгуки, акції та знижки. Купити ліхтарик онлайн з доставкою. Відмінний вибір ліхтарів: налобні, ручні, тактичні, ультрафіолетові, кемпінгові, карманні за вигідними цінами.
Discover the best Young_hot_mom naked strip on cam for online porn video webcam chat ever for free!
Nude amateur webcams girls online sex charNaked amateur webca ee0b6b6
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в георгиевске, купить аттестаты за 11, купить свидетельство о браке, купить диплом менеджера по туризму, купить диплом в курске, потом попал на https://arwenvogel.blox.ua/2024/06/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D1%8D%D1%81%D0%B8-%D0%B8%D0%BB%D0%B8-%D0%BB%D1%8E%D0%B1%D0%BE%D0%B3%D0%BE-%D0%B2%D1%83%D0%B7%D0%B0-%D1%80%D0%BE%D1%81.html и там решили все мои учебные заботы!
Успехов в учебе!
WOW just what I was looking for. Came here by searching for
Wall Repair Omaha
my blog post … Casey
[…] full consideration and participation. Movies are not mere tales; they are events you reside via, lottery mega millions powerball jackpot creating memories that far surpass the standard viewing […]
of players who enjoy the excitement of this high-flying adventure and see if you have what it takes to time your
tigrinho
Продажа подземных канализационных ёмкостей https://neseptik.com по выгодным ценам. Ёмкости для канализации подземные объёмом до 200 м3. Металлические накопительные емкости для канализации заказать и купить в Екатеринбурге.
кипр недвижимость квартиры
виллы на кипре у моря
элитная недвижимость кипр
You’ve made some decent points there. I looked on the net
for more information about the issue and found most individuals will
go along with your views on this site. https://Hispanet.biz/q2a/index.php?qa=365465&qa_1=jonc-en-or-homme
The most stunning transsexual shows on Stripchat. Popular trans chat rooms on free live sex cams. Watch, flirt, and have fun with trans cam models trans cam to cam
Lola nude before webcam – Live Sex Chat
Nude hot cams girlNude amateur webcam ee0b6b6
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в каменске-уральском, купить диплом россия, купить диплом в дзержинске, купить диплом фитнес инструктора, купить диплом в пятигорске. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://lubercy.ixbb.ru/viewtopic.php?id=6050#p13846
http://foto.rzia.ru/profile.php?uid=65061
http://sfpdsa.listbb.ru/viewtopic.php?f=2&t=105
http://music.bestbb.ru/viewtopic.php?id=268
http://moskat.flybb.ru/topic3266.html
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успехов в учебе!
Lebron Ramone James https://lebronjames.prostoprosport-ar.com American basketball player who plays the positions of small and power forward. He plays for the NBA team Los Angeles Lakers. Experts recognize him as one of the best basketball players in history, and a number of experts put James in first place. One of the highest paid athletes in the world.
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в иваново, купить диплом учителя физической культуры, купить диплом в усть-илимске, купить аттестаты за 9, купить диплом мастера маникюра и педикюра, потом попал на http://medicineshocknews.ru/nastoyashhie-diplomyi-po-nizkoy-tsene и там решили все мои учебные заботы!
Удачи!
Features and Benefits
tigrinho demo
Find out alessandraossa naked on Live Adult Webcams Girls for free 🙂
Naked hot webcams wNaked amateur cams bfee0b6
квартиры кипр
슬롯 머신 무료
Dowager 황후의 생일을 축하하기 전에 Longquan Temple에 가고 싶습니까?
Привет, приятели! Желаю рассказать своими эмоциями о казино GGbet online casino. Это заведение поразило меня своим ассортиментом игр и щедрыми вознаграждениями. От классических слотов до увлекательных живых игр — здесь всё имеется для ценителей игры. Бонусы за регистрацию и депозиты порадуют, делая игру еще более увлекательной. Скоростные выплаты и профессиональная поддержка клиентов внушают уверенность. Предлагаю всем испытать здесь
We know how to make our future rich and do you? https://t.me/cryptaxbot/14
Привет, приятели! Решил рассказать своим впечатлением о игровом зале играть в казино 7K. Это заведение впечатлило меня своим разнообразием игр и большими поощрениями. От традиционных слотов и до интересных живых игр — здесь все в наличии для поклонников гемблинга. Приветственные бонусы и бонусы на депозиты удивят, добавляя игре увлекательности. Мгновенные выплаты и экспертная поддержка пользователей усиливают уверенность. Предлагаю всем попробовать здесь
Netflix’s Best Movies to Watch in June 2024, Rated by Rotten Tomatoes season 4 love is warwhat season is south park world of warcraftseason 4 the borgias
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом в ярославле, купить диплом в междуреченске, купить дипломы о высшем, купить диплом в грозном, #купить диплом в ангарске, а затем переключился на дипломы вузов. Подробности здесь: http://armatryrp.forumex.ru/viewtopic.php?f=11&t=47
http://www.volgogradsky.ru/forum/viewtopic.php?p=534651
https://dogovor.top/wiki/%D0%93%D0%B4%D0%B5_%D0%BB%D1%83%D1%87%D1%88%D0%B5_%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%3F_%D0%A1%D0%BE%D0%B2%D0%B5%D1%82%D1%8B_%D1%8D%D0%BA%D1%81%D0%BF%D0%B5%D1%80%D1%82%D0%BE%D0%B2
https://opaseke.com/users/1243
https://phobia.lt/index.php?/gallery/image/12-%D0%BF%D0%BB%D0%B0%D0%BD%D0%B8%D1%80%D1%83%D0%B5%D1%82%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D0%B8%D1%82%D0%B5%D1%81%D1%8C-%D0%B2-%D0%BD%D0%B0%D1%88-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD/
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успехов в учебе!
Luis Fernando Diaz Marulanda https://luis-diaz.prostoprosport-ar.com Colombian footballer, winger for Liverpool and the Colombian national team . Diaz is a graduate of the Barranquilla club. On April 26, 2016, in a match against Deportivo Pereira, he made his Primera B debut. On January 30, 2022, he signed a contract with the English Liverpool for five years, the transfer amount was 40 million euros.
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом с реестром, купить диплом дизайнера, купить диплом в донском, купить диплом в чебоксарах, купить диплом в барнауле, потом про дипломы вузов, подробнее здесь https://forum.bedwantsinfo.nl/member.php?action=profile&uid=82764
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успешной учебы!
Добро пожаловать на GPSPhone.ru! Определение местоположения по номеру телефона онлайн! ??
?? Не можете найти свой телефон? Бесплатно отследите его по номеру через спутник прямо сейчас! ??
??? Узнайте местоположение по номеру телефона онлайн на карте России с помощью геолокации! ???
?? Наш сервис позволяет найти телефон по номеру через спутник бесплатно без регистрации! ??
?? Отследите местоположение человека в реальном времени онлайн без регистрации! ??
?? Поиск по номеру телефона и определение местоположения стали проще! Попробуйте прямо сейчас на GPSPhone.ru! ??
Найдите телефон по номеру и узнайте местоположение онлайн с нашим удобным и бесплатным сервисом! ??
Геолокация по номеру телефона
Overview of the Aviator Game Experience
aviator game online
Maria Sharapova https://maria-sharapova.prostoprosport-ar.com Russian tennis player. The former first racket of the world, winner of five Grand Slam singles tournaments from 2004 to 2014, one of ten women in history who has the so-called “career slam”.
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в киселевске, купить диплом в костроме, купить диплом в владивостоке, купить диплом инженера механика, купить диплом вуза. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://blogs.uoregon.edu/aundreasaad930/love-at-fist-sight/#comment-16771 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
Погружайтесь в мир турецких драм на сайте turkhit.tv! Турецкие сериалы драмы – это захватывающие истории, которые трогают за душу. Мы предлагаем самые свежие новинки и проверенные временем хиты, всё в великолепном HD качестве и с профессиональной русской озвучкой.
Каждый день вас ждут новые серии, без назойливой рекламы, что позволяет полностью насладиться просмотром. Удобный интерфейс и огромный выбор жанров делают turkhit.tv идеальным местом для любителей драматических сериалов. Присоединяйтесь и погружайтесь в драматические истории вместе с нами!
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в копейске, купить диплом в энгельсе, старые дипломы купить, купить диплом тренера, купить диплом в междуреченске, потом про дипломы вузов, подробнее здесь http://desteg.getbb.ru/viewtopic.php?f=6&t=631
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успешной учебы!
Just check out the best rei1926 fully naked stripping on cam for online sex movie show ever!
Nude hot webcams woNude amateur webcam ad1_8b2
Glory casino
https://kvixi.com/blogs/782/%D0%A3%D0%BD%D0%B8%D0%BA%D0%B0%D0%BB%D1%8C%D0%BD%D1%8B%D0%B9-%D0%9E%D0%BF%D1%8B%D1%82-%D0%A0%D0%BE%D1%81%D0%BA%D0%BE%D1%88%D0%B8-%D0%B2-%D0%9E%D1%82%D0%B5%D0%BB%D0%B5-Glory – Glory casino
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в волгограде, купить аттестат школы, купить диплом тренера, купить диплом в нижневартовске, купить диплом бакалавра, потом про дипломы вузов, подробнее здесь http://o97765bq.beget.tech/2023/06/29/realizuyte-svoi-uchebnye-ambicii-kupite-diplom-i-dostignite-novyh-vysot.html
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успешной учебы!
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом врача, купить диплом в тольятти, купить диплом в ревде, купить диплом сварщика, купить диплом в шадринске, а потом наткнулся на http://militarymuster.ca/forum/search.php
http://mastergrad.getbb.ru/viewtopic.php?f=12&t=1047
https://stareishina.com/gallery/image/3538-1premialnie-diplomansycom/
https://bib.az/read-blog/14824
https://wiki.3cdr.ru/wiki/index.php/%D0%97%D0%B0%D1%87%D0%B5%D0%BC_%D0%B2_%D0%BD%D0%B0%D1%88%D0%B5_%D0%B2%D1%80%D0%B5%D0%BC%D1%8F_%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D1%8E%D1%82_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B_%D0%B2_%D1%81%D0%B5%D1%82%D0%B8%3F
, где все мои учебные проблемы были решены!
Хорошей учебы!
Many online platforms host competitive tournaments and events for the Aviator Game. These events offer players
aviator game demo
Психоаналитик Андрей Суляев помогает справиться со сложными, запутанными и давно накопившимися проблемами. Его основная работа, которую он ведет официально, является частная психологическая практика. Консультации осуществляются онлайн, из любой точки мира и в очном формате. https://sulyaev.ru – здесь представлена актуальная стоимость услуги, ознакомиться с ней можете прямо сейчас. Материалы сайта дадут возможность вам лучше в области психологии сориентироваться. Суляев Андрей готов к дополнительным вопросам и с радостью ответит на них. Задавайте их уже сейчас!
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить речной диплом, купить диплом в новоуральске, купить диплом кандидата наук, купить диплом учителя физической культуры, купить диплом в калининграде, потом про дипломы вузов, подробнее здесь http://forexsnews.ru/uskorennyiy-put-k-obrazovaniyu-kupite-diplom-i-sekonomte-vremya-i-usiliya
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Удачи!
to your liking, and quickly move to the section with рџ’¦, Sexy Keonaрџ’¦ naked on sex cam for live porn chat on this topic. All categories are packed enough to make
Naked amateur webcaNude hot cams mode 12fb1fb
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в рязани, купить диплом в березниках, купить диплом кандидата наук, купить диплом в бугульме, купить диплом в донском, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://wiki.3cdr.ru/wiki/index.php/??????_?????????_??????_??_?_??????:_???????????_??????????
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Удачи!
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-ar.com Belgian footballer, midfielder of the Manchester club City” and the Belgian national team. A graduate of the football clubs “Ghent” and “Genk”. In 2008 he began his adult career, making his debut with Genk.
Нужен качественный ремонт стиральной машины в Москве? Наш сервисный центр предлагает оперативные и профессиональные услуги по ремонт стиральной машины г москва. Присоединяйтесь к нашей группе в Telegram и узнайте больше: https://t.me/s/remont_stiralnyh_mashin_moskve
Mohammed Khalil Ibrahim Al-Owais https://mohammed-alowais.prostoprosport-ar.com is a Saudi professional footballer who plays as a goalkeeper for the national team Saudi Arabia and Al-Hilal. He is known for his quick reflexes and alertness at the gate.
Hi there all, here every person is sharing such know-how, thus it’s nice to read this website, and I used to visit this website everyday. https://bookmarkspy.com/story18694187/sigmaac
Discover the best sexo en la cama ever for free!
Naked hot webcams wNude amateur cams fb65d57
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом геодезиста, купить диплом логопеда, купить диплом в зеленодольске, купить диплом программиста, купить диплом в белгороде, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://www.ivedu.ru/forum/index.php
https://belconsole.ru/club/user/10623/blog/1976/
https://lucylink.com/read-blog/7
https://upuge.com/read-blog/16542_we-buy-a-diploma-on-the-internet-expert-tips.html
http://power.ekafe.ru/viewtopic.php?f=2&t=1661
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успешной учебы!
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в кисловодске, купить аттестат за 11 класс, купить диплом в ессентуках, купить диплом в волгодонске, купить диплом в муроме, затем наткнулся на https://njt.ru/forum/user/165397/
https://wip.at.ua/forum/6-14140-1
https://berkerus.ru/blog/radio-berker-touch-dostupno-k-zakazu
https://www.bookmarks4all.win/unlocking-prospective-the-power-of-a-diploma
https://rodme.ru/kupit-diplom-o-vysshem-obrazovanii-po-nizkoy-cene-t11533.html
, где все мои учебные вопросы были решены!
Удачи!
Reputable online platforms offering the Aviator Game are licensed and regulated by governing bodies. This
aviator game demo
Higher rollers mihht wager thousands per hand, when other players wager just a couple off bucks.
my site – 온카
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом в иваново, купить аттестат за 11 класс, купить диплом в кемерово, купить диплом сварщика, купить диплом в кызыле, а потом наткнулся на http://anamaliya.ru/otzyvy/bolshoy-katalog-diplomov-raznyh-vuzov-v-populyarnom-internet-magazine, где все мои учебные проблемы были решены!
Удачи!
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом монтажника, купить диплом косметолога, купить диплом в алуште, купить диплом в керчи, купить диплом в химках, получил базовую информацию.
Остановился в итоге на материале купить диплом в ханты-мансийске, https://tissu-cube.biz/2024/06/08/Где-найти-диплом-Рѕ-высшем-образовании-для-РїРѕРєСѓРїРєРё
Удачи!
https://fuckingcouple.com
Find out live sex chat 1 on 1 for free 🙂
Naked amateur webcaNaked amateur webcams woman live sex show ad7_208
Quincy Anton Promes https://quincy-promes.prostoprosport-br.com Dutch footballer, attacking midfielder and forward for Spartak Moscow . He played for the Dutch national team. He won his first major award in 2017, when Spartak became the champion of Russia.
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в смоленске, купить диплом преподавателя, купить диплом в ревде, купить диплом в шахтах, купить диплом инженера. Постепенно углубляясь, нашел отличный ресурс здесь: https://datasphere.ru/club/user/12/blog/3179/
https://volnodumie.bbmy.ru/viewtopic.php?id=12084#p24547
https://www.nhps1914.com/wiki/%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83_%D0%BB%D1%83%D1%87%D1%88%D0%B5_%D0%BF%D0%BE%D1%81%D0%B5%D1%82%D0%B8%D1%82%D1%8C_%D0%BD%D0%B0%D1%88_%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD,_%D0%B5%D1%81%D0%BB%D0%B8_%D0%BF%D0%BE%D0%BD%D0%B0%D0%B4%D0%BE%D0%B1%D0%B8%D0%BB%D1%81%D1%8F_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%3F
https://rsn360.ru/blogs/138/%D0%A1%D0%BA%D0%BE%D0%BB%D1%8C%D0%BA%D0%BE-%D0%BF%D1%80%D0%B8%D0%BC%D0%B5%D1%80%D0%BD%D0%BE-%D1%81%D0%B5%D0%B3%D0%BE%D0%B4%D0%BD%D1%8F-%D1%81%D1%82%D0%BE%D0%B8%D1%82-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://rsn360.ru/blogs/131/%D0%95%D1%81%D0%BB%D0%B8-%D0%BD%D1%83%D0%B6%D0%B5%D0%BD-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%81%D0%BC%D0%BE%D0%B6%D0%B5%D0%BC-%D0%BF%D0%BE%D0%B4%D1%81%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D1%85%D0%BE%D1%80%D0%BE%D1%88%D0%B8%D0%B9-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
In specific circumstances, the player or the banker or bboth can have a third card.
mywebpage Wiki.Salimar.It
sex cams live absolutely free and easy to watch on any device, just
Naked amateur webcams model online sex charNaked amateur webca b6b6942
Дизайн студия «Kontrast» долгие годы помогает своим заказчикам воплощать мечты о доме и квартире в реальность. Проектируем неповторимый дизайн интерьера. Любую элитную недвижимость способны сделать уютной и изысканной. Используем новейшие разработки в дизайне. Вы будете довольны результатом. Ищете дизайн квартиры заказать|дизайн загородного дома заказать? Kontrastdesign.ru – сайт, где есть наши лучшие работы, а также предложены цены, посмотреть которые вы можете уже сегодня. Позвоните нам, мы проконсультируем абсолютно бесплатно и обсудим ваш будущий проект. Будем рады видеть вас у нас!
Экспертиза ремонта в квартире https://remnovostroi.ru проводится для оценки качества выполненных работ, соответствия требованиям безопасности и стандартам строительства. Специалисты проверяют используемые материалы, исполнение работ, конструктивные особенности, безопасность, внешний вид и эстетику ремонта. По результатам экспертизы составляется экспертное заключение с оценкой качества и рекомендациями по устранению недостатков.
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в нижнем тагиле, купить свидетельство о разводе, купить диплом в чебоксарах, купить диплом о среднем, купить диплом в ленинск-кузнецком, потом про дипломы вузов, подробнее здесь https://blogs.bgsu.edu/sbally/2009/04/21/annotated-bib/comment-page-2574/#comment-173849
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Удачи!
become more comfortable with the gameplay. Observing patterns and understanding the timing of the plane’s ascent
aviator game online
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в новоуральске, купить диплом в северске, купить диплом магистра, купить диплом в нижнекамске, куплю диплом высшего образования, потом про дипломы вузов, подробнее здесь http://turservisnews.ru/originalyi-diplomov-i-attestatov
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успехов в учебе!
https://e-porn.net free xxx videos, web cams, dating for sex, adult
movies, hot babes, porno
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в камышине, купить диплом в брянске, купить диплом техникума, купить диплом средне техническое, купить диплом образцы, потом про дипломы вузов, подробнее здесь http://bouwbedrijfleiderdorp.nl/2015/10/30/hallo-wereld/#comment-17357
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Удачи!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом института, купить диплом провизора, купить диплом бухгалтера, купить диплом в ленинск-кузнецком, купить диплом железнодорожника. Постепенно углубляясь, нашел отличный ресурс здесь: http://sch8671995v.bestbb.ru/viewtopic.php?id=240
http://stroyk.bestbb.ru/viewtopic.php?id=322
http://wiki.roximo.ru/index.php/%D0%97%D0%B0%D1%87%D0%B5%D0%BC_%D0%B2_%D0%BD%D0%B0%D1%88%D0%B5_%D0%B2%D1%80%D0%B5%D0%BC%D1%8F_%D0%BC%D0%BD%D0%BE%D0%B3%D0%B8%D0%B5_%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D1%8E%D1%82_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B_%D0%B2_%D1%81%D0%B5%D1%82%D0%B8_%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%3F
https://ai.cheap/read-blog/12471
http://antonovschool.ru/forum/messages/forum1/topic317/message326/?result=new
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
https://semlava.com/
Variety: Access to a wide range of betting options and gameplay modes.
aviator game demo
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить аттестат за 11 класс, купить диплом колледжа, купить аттестат за 11 класс, купить диплом повара-кондитера, купить дипломы о высшем цены, затем наткнулся на http://shurikrggus.spybb.ru/viewtopic.php?id=1897#p2914, где все мои учебные вопросы были решены!
Хорошей учебы!
оборудование для актового зала оборудование для актового зала .
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом электрика, купить диплом в находке, купить аттестат, купить диплом колледжа, купить диплом о среднем специальном. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://tennis67.ru/club/user/74067/forum/1218/ и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом высшее, купить диплом в энгельсе, купить диплом в севастополе, купить диплом кандидата наук, купить диплом геодезиста. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://komfort.rusff.me/viewtopic.php?id=11448#p35613 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: куплю диплом с занесением, купить диплом в ставрополе, купить диплом мастера маникюра и педикюра, купить диплом, купить диплом в дербенте. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://alex-neil.ru/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=116
http://justvoip.listbb.ru/viewtopic.php?f=2&t=377
https://edmontonoilersclub.com/read-blog/305
http://znanee.flybb.ru/topic516.html
http://bukmeker.bbok.ru/viewtopic.php?id=25177
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Student loan Calculator refinancing lets you combine numerous loans into one
particular, thereby simplifying repayment.
improvements have not only made the game more appealing but also more accessible to a wider audience.
aviator game demo
This crypto casino delivers up to a 10 BTC welcome package,
which it achieves by supplying a 520% matched deposit bonus.
Also visit my web page; lottery
Сова гг – Сова гг обменник, Sova gg обменник
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом автомеханика, купить диплом в невинномысске, купить диплом в клинцах, купить диплом в хасавюрте, купить диплом стоматолога. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://business.bbok.ru/viewtopic.php?id=17550#p19848 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом о высшем образовании, купить диплом в бугульме, купить диплом в кинешме, купить диплом в липецке, купить диплом о высшем образовании и получил базовые знания. В итоге остановился на материале: http://notes1c8.blogspot.com/2014/04/otbor-v-tablice-znachenij-s.html
Успешной учебы!
you can try here trader joe
smartblip home gadgets https://smartblip.com best price, free shipping,
hot offer!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом в дербенте, купить диплом в химках, купить диплом геодезиста, купить диплом в новосибирске, #купить диплом бурильщика, а затем переключился на дипломы вузов. Подробности здесь: http://kontorka.flybb.ru/topic1955.html
https://yourcia.mybb.ru/viewtopic.php?id=8801
http://sealedraid.flybb.ru/topic255.html
http://worksale.wikidot.com/kupit-diplom:bystro-i-legko
http://linux.listbb.ru/viewtopic.php?f=2&t=417
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успехов в учебе!
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в керчи, купить диплом в туле, купить диплом в нижневартовске, купить диплом в ачинске, купить диплом в новоалтайске, постепенно вникая в суть дела нашел отличный материал здесь http://burgasdent.listbb.ru/viewtopic.php?f=3&t=319 и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Успешной учебы!
Go Here coinmarketcap
ремонт телефонов в москве
mountain lake payday loan It was last minute… I had to get money in the bank or my life insurance would lapse.
you’ll have hard on all night —> http://zi.ma/skwzq3/
Cash Out: Decide when to cash out to secure your winnings. If you cash out before the plane crashes, you win. If
aviator demo game
Generous rewards and fair terms and situations contribute to greater ratings in this category.
My web page – 온카홈페이지
muhammad ali apk
best boxer in the world Muhammad Ali
muhammad ali apk
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в новосибирске, купить диплом ссср, купить диплом в грозном, купить диплом в керчи , купить диплом в перми и получил базовые знания. В итоге остановился на материале: https://kaiztech.net/IPB/index.php?/gallery/image/401-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D0%BE%D0%BF%D0%B8%D1%8E-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5/
Хорошей учебы!
Larry Joe Bird https://larry-bird.prostoprosport-br.com American basketball player who spent his entire professional career in the NBA ” Boston Celtics.” Olympic champion (1992), champion of the 1977 Universiade, 3-time NBA champion (1981, 1984, 1986), three times recognized as MVP of the season in the NBA (1984, 1985, 1986), 10 times included in the symbolic teams of the season (1980-88 – first team, 1990 – second team).
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом ссср, купить диплом в глазове, купить диплом в москве, купить диплом в новотроицке, купить диплом в саратове. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://k96586v0.beget.tech/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=95
http://naturetour.ru/club/user/19/blog/1034/
https://sparktv.net/read-blog/20873
https://vip.9bb.ru/viewtopic.php?id=5432#p9077
http://nachosking.com/read-blog/137
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
Roberto Firmino Barbosa de Oliveira https://roberto-firmino.prostoprosport-br.com Brazilian footballer, attacking midfielder, forward for the Saudi club “Al-Ahli”. Firmino is a graduate of the Brazilian club KRB, from where he moved to Figueirense in 2007. In June 2015 he moved to Liverpool for 41 million euros.
ремонт телефонов в москве
http://mamalovesherbargains.com
блэкспрут 2fa – блэкспрут 2fa, blacksprut onion
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в саратове, купить диплом химика, купить диплом кандидата наук, купить диплом в асбесте , купить диплом в ухте и получил базовые знания. В итоге остановился на материале: https://e-nautia.com/worksale/blog?a=17549
Успехов в учебе!
Hi, its nice piece of writing about media print, we all be aware
of media is a great source of facts. https://wed.solidyn.in/index.php?page=user&action=pub_profile&id=72955
Bonuses: Online casinos often offer bonuses and promotions, enhancing the gaming experience.
aviator game
?? Добро пожаловать в мир геолокации по номеру телефона! ??
https://youtu.be/eylZkYUEN6M
?? Узнайте, как легко и точно определить местоположение по номеру с нашим инновационным сервисом! ??
??? Откройте для себя возможности геолокации через спутники и узнайте, где находится ваш телефон в реальном времени! ??
?? Не упустите шанс узнать местоположение по номеру телефона прямо сейчас! ??
?? Попробуйте наш сервис и откройте новые горизонты в определении местоположения по номеру телефона! ??
Найдите телефон по номеру и узнайте местоположение онлайн с нашим удобным и бесплатным сервисом! ??
Геолокация по номеру телефона
ремонт ноутбуков смартфонов
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом экономиста, купить диплом в салавате, купить дипломы о высшем образовании цена, купить диплом в кстово, купить диплом лаборанта и получил базовые знания. В итоге остановился на материале: https://krugozorov.ru/forum/user/7821/
Удачи!
https://strip-cams.com/
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом цена, купить диплом инженера электрика, купить диплом в дзержинске, купить диплом в кисловодске, купить новый диплом, постепенно вникая в суть дела нашел отличный материал здесь http://bazhenova.greatforum.ru/viewtopic.php?f=17&t=3860
http://ultimatum.bestbb.ru/viewtopic.php?id=242
https://wiki.odessanews.biz/index.php/%D0%A8%D0%B8%D1%80%D0%BE%D0%BA%D0%B8%D0%B9_%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2_%D1%80%D0%B0%D0%B7%D0%BD%D1%8B%D1%85_%D0%92%D0%A3%D0%97%D0%BE%D0%B2_%D0%B2_%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC_%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
http://p99946c6.beget.tech/2024/05/13/diplom-na-zakaz-vash-personalnyy-uspeh.html
https://nwkqnvz5.ixbb.ru/viewtopic.php?id=33#p33
и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Успешной учебы!
Топ-5 материалов для перетяжки мебели, современных
Как преобразить интерьер с минимальными затратами, перетянутую мебель мечтали ваши друзья
Сделай свой дом уютным с помощью перетяжки мебели, закажите услугу профессионалов
Какой стиль выбрать для перетяжки мебели, подчеркнут вашу индивидуальность
Перетяжка мебели: секреты мастеров, запомнить
“КакСвоим”.
Компания «БытовкиСтарт» успешно работает уже более 5 лет. Мы выполняем быструю доставку и удерживаем лучшие цены на рынке. Продукция вся есть в наличии. Бытовки изготовлены исключительно из прочных и надежных материалов. Уверены в качестве наших товаров. https://bytovkistart.ru – сайт, где можете прямо сейчас оставить заявку на профессиональную консультацию. Все менеджеры вежливые, они готовы помочь с выбором необходимого вам варианта. При возникновении вопросов, сразу же обращайтесь к нам!
ремонт телефонов в москве
https://qureshileathers.com/ppk/
Семейные турецкие сериалы – это всегда тепло и уют! Турецкие сериалы семейные на turkhit.tv предлагают трогательные и вдохновляющие истории для всех возрастов. HD качество и отличная русская озвучка делают просмотр еще приятнее.
Каждый день добавляются новые серии, и вы всегда будете в курсе последних событий. На turkhit.tv нет назойливой рекламы, так что вы можете полностью погрузиться в атмосферу семейных ценностей и любви.
https://humanlove.stream/wiki/PPK
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить аттестаты за 11, купить диплом отзывы, купить аттестат школы, купить диплом в невинномысске, купить диплом в кызыле, затем наткнулся на http://reflections.listbb.ru/viewtopic.php?f=45&t=668, где все мои учебные вопросы были решены!
Удачи!
The Aviator Game boasts several unique features that set it apart from other online casino games:
aviator game online
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом технолога, купить диплом химика, купить диплом в коврове, купить диплом в альметьевске , купить диплом о среднем и получил базовые знания. В итоге остановился на материале: http://newsbizlife.ru/kupit-diplom-v-moskve-4
Удачи!
Ranking secpnd right after three years is Clinton, with almost 8%, followed by Trump with four.four%.
Feel free to visit my blog; 이지알바
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в георгиевске, куплю диплом цена, купить диплом в шадринске, купить диплом нового образца, купить диплом в пензе. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://n.bestbb.ru/viewtopic.php?id=113
https://ballinthe6.ca/blogs/13157/?иплом-без-усилий-¬озможности-онлайн-покупки
http://o91707v5.beget.tech/2024/01/29/ogromnyy-katalog-diplomov-ot-znamenitogo-magazina.html
http://www.lada-xray.net/member.php?u=2434
https://www.cyclopede.com/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=88
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успехов в учебе!
Khvicha Kvaratskhelia https://khvicha-kvaratskhelia.prostoprosport-br.com Georgian footballer, winger for Napoli and captain of the Georgian national team. A graduate of Dynamo Tbilisi. He made his debut for the adult team on September 29, 2017 in the Georgian championship match against Kolkheti-1913. In total, in the 2017 season he played 4 matches and scored 1 goal in the championship.
ремонт телефонов в москве
Damian Emiliano Martinez https://emiliano-martinez.prostoprosport-br.com Argentine footballer, goalkeeper of the Aston Villa club and national team Argentina. Champion and best goalkeeper of the 2022 World Cup.
Использование промокодов в Cat casino открывает новые возможности для игроков. Они позволяют получать бонусы и наслаждаться игровым процессом с дополнительными привилегиями
срочный ремонт телефонов
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом ссср, купить диплом в ижевске, купить диплом в самаре, купить диплом в тюмени , купить диплом в хабаровске и получил базовые знания. В итоге остановился на материале: https://gunneryfjmn.humor-blog.com/27098638/??????-?????????-????????
Хорошей учебы!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом с внесением в реестр, купить диплом в уфе, купить диплом в саратове, купить диплом в новочебоксарске, #купить диплом с внесением в реестр, а затем переключился на дипломы вузов. Подробности здесь: http://jrockhabarovsk.bestbb.ru/viewtopic.php?id=151
http://school37slr.bestbb.ru/viewtopic.php?id=531
http://mosday.getbb.ru/viewtopic.php?f=12&t=899
https://wiki.shayvam.com/index.php?title=%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B_%D0%BE%D1%82%D0%B5%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D1%85_%D0%92%D0%A3%D0%97%D0%BE%D0%B2_-_%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B9_%D0%B2_%D1%80%D0%B5%D0%B6%D0%B8%D0%BC%D0%B5_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD!
http://autoprajs.ru/14765.html
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успехов в учебе!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в омске, купить диплом медицинского училища, купить свидетельство о рождении, купить свидетельство о браке, купить диплом в магадане. Постепенно углубляясь, нашел отличный ресурс здесь: http://mosros.flybb.ru/topic226.html, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успехов в учебе!
Watch the Plane Ascend: The plane takes off and starts climbing.
play aviator game
На сайте https://elektricheskie-kaminy.ru/ представлены электрические камины в огромном ассортименте. Эти конструкции подарят вашему дому незабываемый уют, комфорт. И самое важное, что они прослужат очень долго. Магазин предпринимает все возможное для того, чтобы процесс покупки был очень простым и понятным. Камины не выбрасывают в атмосферу вредные вещества. А для того, чтобы они начали обогревать, не потребуются дрова, а только розетка. Отсутствует открытый огонь, а потому возможность пожара сведена к минимуму.
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в северодвинске, купить диплом в балашихе, купить диплом в ессентуках, купить диплом в ревде, купить диплом в рязани, потом попал на http://foro.lagrihost.com/safelink.php?url=http://rudiploma.com/???????-??-?????????/??????-??????-???????????-?????? и там решили все мои учебные заботы!
Успешной учебы!
Jack Peter Grealish https://jackgrealish.prostoprosport-br.com English footballer, midfielder of the Manchester City club and the England national team. A graduate of the English club Aston Villa from Birmingham. In the 2012/13 season he won the NextGen Series international tournament, playing for the Aston Villa under-19 team
This is the right web site for anyone who wishes to understand
this topic. You understand a whole lot its almost tough to argue
with you (not that I really will need to…HaHa). You definitely put a brand new spin on a topic
which has been written about for many years.
Wonderful stuff, just great! https://Dublinohiousa.gov/
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом инженера электрика, купить диплом в минусинске, купить диплом в рязани, купить диплом физика, купить диплом в нижневартовске, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://rashin.4adm.ru/viewtopic.php?f=27&t=1944
http://wiki.astrakhan.pro/index.php/%D0%98%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD_%D1%81_%D0%BE%D0%B3%D1%80%D0%BE%D0%BC%D0%BD%D1%8B%D0%BC_%D0%B2%D1%8B%D0%B1%D0%BE%D1%80%D0%BE%D0%BC_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2_%D0%B8_%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%BE%D0%B2
http://damien.bestbb.ru/viewtopic.php?id=264
http://publikacii.listbb.ru/viewtopic.php?f=3&t=563
http://panther.80lvl.ru/viewtopic.php?f=19&t=374
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Удачи!
Kyle Andrew Walker https://kylewalker.prostoprosport-br.com English footballer, captain of the Manchester City club and the England national team. In the 2013/14 season, he was on loan at the Notts County club, playing in League One (3rd division of England). Played 37 games and scored 5 goals in the championship.
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом в серове, купить диплом швеи, купить диплом тренера, купить диплом в армавире, купить атестат об окончании школы, получил базовую информацию.
Остановился в итоге на материале купить диплом в прокопьевске, http://formfinance.ru/kupit-diplom-vash-klyuch-k-novyim-vozmozhnostyam-i-perspektivam-v-karere
Хорошей учебы!
Glory Casino
The Aviator Game boasts several unique features that set it apart from other online casino games:
aviator game online
Glory Casino
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом в норильске, купить аттестат за 9 класс, купить диплом в кузнецке, купить диплом техникума, купить диплом в благовещенске, а потом наткнулся на https://huarenjiaohui.com/index.php?/gallery/image/85-%D0%B3%D0%B4%D0%B5-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B8%D0%BB%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%BE%D1%82%D0%BB%D0%B8%D1%87%D0%BD%D0%BE%D0%B3%D0%BE-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B0/, где все мои учебные проблемы были решены!
Успешной учебы!
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом в кирово-чепецке, купить диплом прораба, купить диплом в нижним тагиле, купить диплом в курске, купить диплом в люберцах, получил базовую информацию.
Остановился в итоге на материале купить бланк диплома, http://iluzeia.flybb.ru/topic118.html
http://u90517ol.beget.tech/2023/10/30/kak-sdelat-kachestvennyy-diplom.html
http://slliver.getbb.ru/viewtopic.php?f=62&t=762
http://minimoo.eu/index.php/en/forum/welcome-mat/660312
http://wtf.bestbb.ru/viewtopic.php?id=101
Успешной учебы!
спрут как попасть на сайт – блек спрут онион, блэкспрут ссылка
Когда я искал турецкие сериалы 2024 онлайн, наткнулся на turklife.tv. Сайт поразил меня разнообразием жанров и удобным разделением сериалов по годам. Все новинки 2024 года здесь доступны бесплатно, без регистрации и рекламы, и в отличном HD качестве с русской озвучкой.
Люблю смотреть турецкие сериалы за их увлекательные сюжеты и харизматичных героев. Теперь я всегда в курсе новинок благодаря turklife.tv – это лучшее место для просмотра любимых сериалов!
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом фитнес инструктора, купить диплом в новокуйбышевске, купить дипломы о высшем цены, купить диплом биолога, купить диплом массажиста, постепенно вникая в суть дела нашел отличный материал здесь https://www.vodozone.ru/forum/user/47313/ и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Успехов в учебе!
На сайте turkhit.tv вы найдете обширный выбор турецкие сериалы на русском языке. Здесь представлено множество жанров: драмы, комедии, боевики и фэнтези. Каждый сериал доступен с качественной русской озвучкой, что делает просмотр приятным и удобным.
Платформа регулярно обновляется новыми сериями и популярными хитами, такими как “Основание Осман” и “Кровавые цветы”. Регистрация и оплата не требуются, что позволяет наслаждаться любимыми сериалами без лишних хлопот. Заходите на turkhit.tv и погружайтесь в мир захватывающих историй.
Convenience: Play from the comfort of your home or on the go.
play aviator game
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом эколога, купить речной диплом, купить аттестат за 9 класс, купить диплом в серове, где купить диплом среднем, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://tissu-cube.biz/2024/06/08/Где-найти-диплом-Рѕ-высшем-образовании-для-РїРѕРєСѓРїРєРё
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успешной учебы!
Laure Boulleau https://laure-boulleau.prostoprosport-fr.com French football player, defender. She started playing football in the Riom team, in 2000 she moved to Isere, and in 2002 to Issigneux. All these teams represented the Auvergne region. In 2003, Bullo joined the Clairefontaine academy and played for the academy team for the first time.
Наша мастерская предлагает профессиональный сервис ремонта духовых шкафов в москве любых брендов и моделей. Мы знаем, насколько необходимы вам ваши духовки, и стремимся предоставить услуги наилучшего качества. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что обеспечивает надежность и долговечность проведенных ремонтов.
Наиболее частые неисправности, с которыми сталкиваются обладатели кухонных приборов, включают неисправности термостата, поломку таймера, треснувшую дверцу, сбои контроллера, неисправности вентилятора и повреждения электроники. Для устранения этих поломок наши квалифицированные специалисты проводят ремонт нагревательных элементов, термостатов, таймеров, дверец, контроллеров, вентиляторов и электроники. Обращаясь в наш сервисный центр, вы получаете качественный и надежный официальный ремонт духовых шкафов адреса.
Подробная информация представлена на нашем сайте: https://remont-duhovyh-shkafov-ace.ru
Son Heung Min https://sonheung-min.prostoprosport-br.com South Korean footballer, striker and captain of the English Premier League club Tottenham Hotspur and the Republic of Korea national team. In 2022 he won the Premier League Golden Boot. Became the first Asian footballer in history to score 100 goals in the Premier League
Вас интересуют последние новости Санкт-Петербурга и Ленинградской области? Nowosti.spb.ru – это то, что вам действительно нужно! Здесь вы найдете такие категории: культура, экономика, политика, ЖКХ, спорт, медицина, общество. Мы выделяем важное и предоставляем читателям в понятном виде. За каждой фотографией и заголовком располагается сюжет. Ищете что произошло сегодня в петербурге? Nowosti.spb.ru – здесь вы найдете много полезной информации. Портал наш выбирают те, кто ценит свежесть и наполненность. Читайте у нас самые горячие новости. Всегда рады вам!
Discover the best http://www.18closeup.net
and sex live chat free ever!
Nude amateur camsNaked hot webcams w 57ad7_f
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в комсомольске-на-амуре, купить диплом в вологде, купить диплом в новом уренгое, купить диплом цена, купить диплом в верхней пышме, потом попал на https://laporteproperty.com/en/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=78
http://panther.80lvl.ru/viewtopic.php?f=15&t=350
https://prof-komplekt.com/club/user/1035/blog/9952/
http://edinstvoarmenia.bestbb.ru/viewtopic.php?id=249
https://forum.shvedun.ru/ucp.php?mode=login
и там решили все мои учебные заботы!
Успешной учебы!
ремонт айфон ремонт айфон .
[b]Здравствуйте[/b]!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом в усолье-сибирском, купить диплом в кирово-чепецке, купить диплом в невинномысске, купить диплом автомеханика, купить диплом ссср, получил базовую информацию.
Остановился в итоге на материале купить диплом строителя, https://kamen.6bb.ru/viewtopic.php?id=2147#p7323
Удачи!
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в пятигорске, купить диплом в туапсе, купить диплом в сарове, купить диплом о среднем специальном, купить диплом матроса, потом про дипломы вузов, подробнее здесь http://hpc.bestbb.ru/viewtopic.php?id=408#p414
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успехов в учебе!
Наша мастерская предлагает высококачественный починить видеокарту рядом различных марок и моделей. Мы осознаем, насколько значимы для вас ваши графические карты, и обеспечиваем ремонт первоклассного уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что предоставляет надежность и долговечность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются обладатели графических адаптеров, включают перегрев, поломку памяти, проблемы с коннекторами, сбои контроллера и неисправности ПО. Для устранения этих поломок наши профессиональные техники выполняют ремонт системы охлаждения, памяти, разъемов, контроллеров и ПО. Обращаясь в наш сервисный центр, вы гарантируете себе качественный и надежный официальный ремонт видеокарт с гарантией.
Подробная информация размещена на сайте: https://remont-videokart-biz.ru
Excellent and high-quality babesladies.com absolutely free and easy to watch on any device, just
Nude amateur webcamNude amateur cams bfee0b6
While the game itself is free to access, playing involves placing bets with real money. Some platforms may offer
aviator game online
find more info https://mangoandmoreshop.com
view publisher site https://onlinecasinohomes.com
Excellent and high-quality online sex cam absolutely free and easy to watch on any device, just
Nude amateur webcamNude amateur webcams model online sex show 812fb1f
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом энергетика, купить диплом в златоусте, купить диплом воспитателя, купить диплом в оренбурге, #купить диплом старого образца, а затем переключился на дипломы вузов. Подробности здесь: https://sports-pharmacology31986.ezblogz.com/59157497/???????-????????-??????
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успехов в учебе!
Наш сервисный центр предлагает профессиональный вызвать мастера по ремонту электросамоката адреса различных марок и моделей. Мы знаем, насколько важны для вас ваши электроскутеры, и обеспечиваем ремонт высочайшего уровня. Наши опытные мастера оперативно и тщательно выполняют работу, используя только качественные детали, что обеспечивает долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются владельцы электросамокатов, включают проблемы с батареей, неисправности двигателя, поломку контроллера, неисправные тормоза и повреждения корпуса. Для устранения этих проблем наши профессиональные техники проводят ремонт батарей, двигателей, контроллеров, тормозных систем и механических компонентов. Обратившись к нам, вы гарантируете себе надежный и долговечный мастерская по ремонту электросамоката на выезде.
Подробная информация размещена на сайте: https://remont-elektrosamokatov-fun.ru
[b]Привет всем[/b])
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: где купить диплом о среднем образование, купить диплом в южно-сахалинске, купить свидетельство о браке, купить диплом в новоуральске, купить диплом в асбесте, а потом наткнулся на http://jagplay.ekafe.ru/viewtopic.php?f=22&t=4060, где все мои учебные проблемы были решены!
Удачи!
Thefe had been also 67 tickets that won $50,000 prizes and 20 tickets that won $200,
000 prizes.
My site: powerball results
Effective Strategies for Beginners
aviator game demo
Discover the best cuteyoungpussy.pro ever for free!
Naked hot webcams gNude amateur cams d3_308a
Jude Victor William Bellingham https://jude-bellingham.prostoprosport-fr.com English footballer, midfielder of the Spanish club Real Madrid and the England national team. In April 2024, he won the Breakthrough of the Year award from the Laureus World Sports Awards. He became the first football player to receive it.
Наши специалисты предлагает надежный сервисный центр по ремонту электровелосипедов в москве всех типов и брендов. Мы знаем, насколько важны для вас ваши электрические велосипеды, и обеспечиваем ремонт высочайшего уровня. Наши опытные мастера оперативно и тщательно выполняют работу, используя только качественные детали, что гарантирует долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются обладатели электробайков, включают проблемы с батареей, неисправности двигателя, сбои контроллера, проблемы с тормозами и механические повреждения. Для устранения этих поломок наши профессиональные техники проводят ремонт батарей, двигателей, контроллеров, тормозных систем и механических компонентов. Обращаясь в наш сервисный центр, вы обеспечиваете себе надежный и долговечный ремонт электровелосипедов рядом.
Подробная информация размещена на сайте: https://remont-elektrovelosipedov-gem.ru
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом повара-кондитера, купить диплом с внесением в реестр, купить диплом института, купить диплом университета, купить диплом в тобольске и получил базовые знания. В итоге остановился на материале: http://newmedtime.ru/diplom-za-dengi-nadezhnyie-postavshhiki-i-proverennyie-metodyi
Хорошей учебы!
FinandCrypto.com provides relevant and useful information on the topic of cryptocurrencies, finance, technology. Talking about blockchain in simple words. You can view the content at any time convenient for you. https://finandcrypto.com – a well-known site that is valued primarily for its simplicity and clear interface. Exchange rates are presented here. There is also a convenient search here, we recommend using it. Our main task is to help you accept financial and investment solutions. With us you will be aware of the latest news!
Homepage von free sex cam chat
Naked hot webcams wNude amateur cams acc5812
Antoine Griezmann https://antoine-griezmann.prostoprosport-fr.com French footballer, striker and midfielder for Atletico Madrid. Player and vice-captain of the French national team, as part of the national team – world champion 2018. Silver medalist at the 2016 European Championship and 2022 World Championship.
demo versions or free play options to allow players to practice before betting real money.
play aviator game
In January 2010, Harry Kane https://harry-kane.prostoprosport-fr.com received an invitation to the England U-team for the first time 17 for the youth tournament in Portugal. At the same time, the striker, due to severe illness, did not go to the triumphant 2010 European Championship for boys under 17 for the British.
Наш сервисный центр предлагает высококачественный ремонт электронной книги адреса любых брендов и моделей. Мы понимаем, насколько необходимы вам ваши eBook-ридеры, и обеспечиваем ремонт высочайшего уровня. Наши опытные мастера работают быстро и аккуратно, используя только оригинальные запчасти, что обеспечивает долговечность и надежность наших услуг.
Наиболее частые неисправности, с которыми сталкиваются обладатели цифровых книг, включают неисправный дисплей, выход из строя батареи, ошибки ПО, неработающие разъемы и проблемы с контроллером. Для устранения этих поломок наши квалифицированные специалисты выполняют ремонт экранов, батарей, ПО, разъемов и контроллеров. Обратившись к нам, вы обеспечиваете себе надежный и долговечный мастер по ремонту электронных книг рядом.
Подробная информация размещена на сайте: https://remont-elektronnyh-knig-hit.ru
Nice article, thanks! Just check chat sex cam live this out.
Nude amateur camsNude amateur cams 2fb1fb6
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в вольске, купить диплом в нижним тагиле, купить диплом о среднем, купить диплом в ачинске, купить диплом о среднем образовании, затем наткнулся на http://myfootballday.ru/byistryiy-dostup-k-professionalnyim-vozmozhnostyam-kupit-diplom-i-nachat-kareru, где все мои учебные вопросы были решены!
Удачи!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в рязани, купить диплом прораба, где купить диплом образование, купить диплом в мурманске, купить диплом в смоленске. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://www.vidagrafia.com/read-blog/173433 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом логопеда, купить диплом в ростове, купить диплом в донском, купить диплом в тюмени, #купить диплом института, а затем переключился на дипломы вузов. Подробности здесь: http://www.amalgama-forum.com/album.php?albumid=93&attachmentid=1858&commentid=1248
http://x91392sl.beget.tech/2024/03/14/glavnye-prichiny-iz-za-chego-mnogie-pokupayut-diplomy-v-seti-internet.html
http://zdshi-tula.ru/forum/?PAGE_NAME=message&FID=1&TID=70&MID=3861&result=new
https://sovetushka.forum2x2.ru/t28190-topic
http://pdlspd.listbb.ru/viewtopic.php?f=3&t=359
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успешной учебы!
Discover the best live sex cam chat ever for free!
Naked hot webcams mNaked hot cams model online porn char d57ad3_
cash advance on unemployment Is blogging the future of the world?
Playing the Aviator Game online offers several benefits:
aviator demo game
Karim Mostafa Benzema https://karim-benzema.prostoprosport-fr.com French footballer, striker for the Saudi club Al-Ittihad . He played for the French national team, for which he played 97 matches and scored 37 goals.
Achraf Hakimi Mou https://achraf-hakimi.prostoprosport-fr.com Moroccan footballer, defender of the French club Paris Saint-Germain “and the Moroccan national team. He played for Real Madrid, Borussia Dortmund and Inter Milan.
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом менеджера, купить диплом в кстово, купить диплом в ханты-мансийске, купить диплом инженера по охране труда, #купить диплом строителя, а затем переключился на дипломы вузов. Подробности здесь: http://drochan.listbb.ru/viewtopic.php?f=4&t=343
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успехов в учебе!
anal threesome black sex cam
Nude amateur camsNaked hot webcams m 942dacc
this website https://vuoksenkalastuspuisto.com
official statement https://haasfoundation.org
Наша мастерская предлагает профессиональный отремонтировать гироскутер с гарантией различных марок и моделей. Мы понимаем, насколько значимы для вас ваши электроскутеры, и обеспечиваем ремонт высочайшего уровня. Наши опытные мастера работают быстро и аккуратно, используя только качественные детали, что обеспечивает долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются обладатели самобалансирующихся скутеров, включают неисправную батарею, неработающий двигатель, неисправный контроллер, проблемы с гиросенсорами и поломки корпуса. Для устранения этих проблем наши профессиональные техники проводят ремонт батарей, двигателей, контроллеров, гиросенсоров и механических компонентов. Доверив ремонт нам, вы получаете долговечный и надежный мастерская по ремонту гироскутеров рядом.
Подробная информация доступна на сайте: https://remont-giroskuterov-key.ru
i thought about this https://iniciocafe.com
Are There Any Costs Involved?
aviator game online
click site https://bounyayin.com
Перетяжка мягкой мебели
https://bmx.by/forum/messages/forum5/topic2818/message4694/?result=new .
Недавно стал играть в старда казино и оказался впечатлен. Большой выбор слотов и настольных игр обеспечивает подобрать приключения на всякий вкус. Особенно впечатлили выгодные предложения и регулярные акционные предложения. Схема вывода выигрышей понятный и скорый, а клиентская поддержка всегда может поддержать с каким угодно вопросом. Комфортный и простой для восприятия пользовательский интерфейс делает геймплей приятной и увлекательной. Советую попробовать казино старда всем поклонникам высококлассного геймплея и игровых приключений.
Совсем недавно стал играть в легзо и остался удовлетворен. Огромный набор игровых автоматов и картежных игр дает возможность подобрать игры на какой угодно предпочтения. Конкретно обрадовали привлекательные предложения и частые бонусы. Процесс вывода выигрышей понятный и незамедлительный, а служба поддержки всегда готова поддержать с всяким проблемами. Интуитивно понятный и простой для восприятия интерфейс превращает развлечение приятной и интересной. Рекомендую поиграть legzo казино всем любителям высококлассного гемблинга и азартных игр.
Наши специалисты предлагает высококачественный сервисный центр по ремонту гироскутеров рядом любых брендов и моделей. Мы знаем, насколько важны для вас ваши электроскутеры, и стремимся предоставить услуги первоклассного уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что предоставляет долговечность и надежность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются обладатели самобалансирующихся скутеров, включают проблемы с батареей, проблемы с мотором, неисправный контроллер, проблемы с гиросенсорами и повреждения рамы. Для устранения этих поломок наши опытные мастера оказывают ремонт батарей, двигателей, контроллеров, гиросенсоров и механических компонентов. Доверив ремонт нам, вы гарантируете себе долговечный и надежный мастер по ремонту гироскутеров на выезде.
Подробная информация размещена на сайте: https://remont-giroskuterov-key.ru
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом слесаря, купить диплом в калуге, купить диплом специалиста, купить диплом в шадринске, купить диплом в ишиме, потом попал на http://forum-abkhazia.ru/member-u_9263.html и там решили все мои учебные заботы!
Успехов в учебе!
Discover the best live cam sex
and indian hidden cam sex ever!
Nude amateur camsNaked amateur cams 12fb1fb
helpful resources https://98toto0228.com
Совсем недавно начал играть в гет-х и остался удовлетворен. Огромный набор игр и игр за столом дает возможность найти приключения на какой угодно предпочтения. Особенно порадовали щедрые бонусы и регулярные акции. Процедура снятия средств простой и быстрый, а клиентская поддержка всегда старается поддержать с всяким обращением. Интуитивно понятный и дружелюбный интерфейс обеспечивает развлечение приятной и интересной. Настоятельно рекомендую оценить в игровые автоматы всем любителям надежного азартных игр и игрового азарта.
Sweet Bonanza https://sweet-bonanza.prostoprosport-fr.com is an exciting slot from Pragmatic Play that has quickly gained popularity among players thanks to its unique gameplay, colorful graphics and the opportunity to win big prizes. In this article, we’ll take a closer look at all aspects of this game, from mechanics and bonus features to strategies for successful play and answers to frequently asked questions.
Недавно стал играть в Водка бет вход и оказался удовлетворен. Широкий ассортимент слотов и картежных игр дает возможность обнаружить игры на какой угодно вкус. В частности порадовали привлекательные бонусы и постоянные мероприятия. Процедура вывода выигрышей легкий и быстрый, а техподдержка всегда рада помогать с любым вопросом. Простой в использовании и дружелюбный интерфейс сайта обеспечивает геймплей комфортной и приятной. Настоятельно рекомендую испытать в водка козино всем поклонникам надежного гемблинга и игрового азарта.
Philip Walter Foden https://phil-foden.prostoprosport-fr.com better known as Phil Foden English footballer, midfielder of the Premier club -League Manchester City and the England national team. On December 19, 2023, he made his debut at the Club World Championship in a match against the Japanese club Urawa Red Diamonds, starting in the starting lineup and being replaced by Julian Alvarez in the 65th minute.
Совсем недавно начал играть в сайт drip casino и остался рад. Широкий каталог аппаратов и картежных игр позволяет обнаружить развлечения на всякий вкусовые предпочтения. Конкретно понравились привлекательные бонусы и регулярные акции. Механизм вывода выигрышей простой и молниеносный, а поддержка клиентов всегда готова помочь с всяким обращением. Комфортный и простой для восприятия пользовательский интерфейс делает геймплей комфортной и увлекательной. Настоятельно рекомендую испытать в drip casino игровые автоматы всем ценителям надежного азартных игр и игрового азарта.
Social Elements: Options for multiplayer gameplay and chat features enhance the social experience.
aviator game online
Bernardo Silva https://bernardo-silva.prostoprosport-fr.com Portuguese footballer, midfielder. Born on August 10, 1994 in Lisbon. Silva is considered one of the best attacking midfielders in the world. The football player is famous for his endurance and performance. The athlete’s diminutive size is more than compensated for by his creativity, dexterity and foresight.
find out https://granbyma.net
Cat Casino предлагает уникальные промокоды для своих игроков. Введите код и получите дополнительные бонусы при пополнении счета.
В последнее время попробовал играть в 1xslots официальный сайт и оказался удовлетворен. Обширный выбор игровых автоматов и настольных развлечений гарантирует найти приключения на любой вкус. В частности впечатлили выгодные акции и регулярные акции. Схема вывода денег непроблемный и быстрый, а техподдержка всегда рада поддержать с любым вопросом. Комфортный и простой для восприятия интерфейс сайта обеспечивает развлечение удобной и увлекательной. Предлагаю поиграть в онлайн казино 1xslots всем любителям стабильного игровых развлечений и игрового азарта.
live indian sex chat absolutely free and easy to watch on any device, just
Naked amateur camsNaked hot webcams model online sex show 7ad3_02
next https://mangoandmoreshop.com
Незадолго до этого начал играть играть в в up-x и оказался удовлетворен. Обширный выбор игровых автоматов и игр за столом позволяет подобрать развлечения на какой угодно предпочтения. Особенно обрадовали щедрые бонусные программы и частые акционные предложения. Схема вывода денег легкий и быстрый, а служба поддержки всегда может поддержать с любым проблемами. Комфортный и понятный пользовательский интерфейс гарантирует геймплей удобной и интересной. Рекомендую испытать в up x зеркало всем любителям качественного геймплея и игровых приключений.
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про дешево купить диплом, купить диплом в воткинске, куплю диплом, купить диплом геодезиста, где купить атестат об окончании школы, постепенно вникая в суть дела нашел отличный материал здесь http://vsetutonline.com/forum/member.php?u=76509 и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Удачи!
Наш сервисный центр предлагает надежный вызвать мастера по ремонту холодильника различных марок и моделей. Мы знаем, насколько значимы для вас ваши рефрижераторы, и стремимся предоставить услуги наилучшего качества. Наши опытные мастера проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что предоставляет надежность и долговечность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются владельцы холодильников, включают проблемы с охлаждением, неработающий термостат, неисправности программного обеспечения, проблемы с подключением и механические повреждения. Для устранения этих проблем наши опытные мастера выполняют ремонт компрессоров, термостатов, ПО, разъемов и механических компонентов. Обратившись к нам, вы получаете надежный и долговечный ремонт холодильника.
Подробная информация доступна на сайте: https://remont-holodilnikov-lux.ru
Kylian Mbappe Lotten https://kylian-mbappe.prostoprosport-fr.com Footballeur francais, attaquant du Paris Saint-Germain et capitaine de l’equipe de France. Le 1er juillet 2024, il deviendra joueur du club espagnol du Real Madrid.
https://www.livevideochat.xyz/
inthecrackfan.pro videos absolutely free and easy to watch on any device, just
Nude amateur webcams model live sex charNude hot cams model live porn char 5812fb1
games that stood out from traditional casino offerings. Inspired by the concept of high-risk, high-reward, the
play aviator game
Discover More https://iniciocafe.com
Наш сервисный центр предлагает надежный центр ремонта бесперебойников на выезде различных марок и моделей. Мы знаем, насколько значимы для вас ваши ИБП, и стремимся предоставить услуги высочайшего уровня. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что обеспечивает надежность и долговечность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются владельцы ИБП, включают неисправную батарею, неисправности инвертора, поломку контроллера, проблемы с подключением и программные сбои. Для устранения этих проблем наши опытные мастера выполняют ремонт батарей, инверторов, контроллеров, разъемов и ПО. Обращаясь в наш сервисный центр, вы обеспечиваете себе надежный и долговечный вызвать мастера по ремонту бесперебойника на дому.
Подробная информация доступна на сайте: https://remont-ibp-max.ru
web https://allslotwallet.org
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в балаково, купить диплом института, купить аттестат за 9 класс, купить диплом в великих луках, купить диплом в вологде, потом про дипломы вузов, подробнее здесь http://x91392sl.beget.tech/2023/06/19/vash-put-k-uspehu-poluchite-diplom-ot-priznannogo-uchebnogo-zavedeniya.html
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Удачи!
Excellent and high-quality live one on one sex chat absolutely free and easy to watch on any device, just
Naked hot webcams model live porn charNude hot cams model live porn show fb65d57
Jogo do Tigre https://jogo-do-tigre.prostoprosport-br.com is a simple and fun game that tests your reflexes and coordination. In this game you need to put your finger on the screen, pull out the stick and go through each peg. However, you must ensure that the stick is the right length, neither too long nor too short.
1win casino
1вин казино зеркало рабочее
Наша мастерская предлагает профессиональный мастерская по ремонту игровой приставки в москве различных марок и моделей. Мы знаем, насколько важны для вас ваши консоли, и готовы предложить сервис первоклассного уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что обеспечивает длительную работу проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются владельцы игровых приставок, включают поломку HDD, неисправные порты, неисправности контроллеров, программные сбои и неисправности системы охлаждения. Для устранения этих проблем наши профессиональные техники проводят ремонт жестких дисков, разъемов, контроллеров, ПО и систем охлаждения. Обратившись к нам, вы гарантируете себе качественный и надежный центр ремонта игровой приставки в москве.
Подробная информация доступна на сайте: https://remont-igrovyh-konsoley-mob.ru
Mohamed Salah Hamed Mehrez Ghali https://mohamed-salah.prostoprosport-fr.com Footballeur egyptien, attaquant du club anglais de Liverpool et l’equipe nationale egyptienne. Considere comme l’un des meilleurs footballeurs du monde
In addition to the Gastonia spas, Weei and Huang are alleged to
personal spas in Indian Trail, Charlotte, Greensboro, and Columbia and Rock Hill, South Carolina.
My website Swedish massage therapy
environment for players to enjoy the game. Some popular platforms include Name], Name], and
aviator game
Если хотите новые турецкие сериалы, заходите на turkhit.tv! Здесь вас ждут самые свежие новинки, которые уже успели завоевать сердца зрителей. Все сериалы представлены в HD качестве и с качественной русской озвучкой.
На сайте каждый день появляются новые серии, так что вы всегда будете в курсе последних событий. Платформа удобна в использовании и не содержит навязчивой рекламы. Заходите на turkhit.tv и наслаждайтесь лучшими новинками турецких сериалов.
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в кирове, купить диплом в ижевске, купить диплом в абакане, купить диплом в верхней пышме, купить аттестат за 9 класс, потом попал на http://school45.bestbb.ru/viewtopic.php?id=222 и там решили все мои учебные заботы!
Успешной учебы!
Nice articl! Just check live cam sex chat this out!
Nude hot cams womaNaked amateur webca bfee0b6
On-line applications are stored at NEOGOV, a secure third-party web-site.
Also visit my webpage :: part Time jobs
Наш сервисный центр предлагает высококачественный мастерская по ремонту аймака на выезде всех типов и брендов. Мы знаем, насколько необходимы вам ваши компьютеры Apple, и стремимся предоставить услуги первоклассного уровня. Наши опытные мастера проводят ремонтные работы с высокой скоростью и точностью, используя только качественные детали, что гарантирует надежность и долговечность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются пользователи моноблоков iMac, включают проблемы с жестким диском, неисправности дисплея, неработающие разъемы, неисправности программного обеспечения и неисправности системы охлаждения. Для устранения этих проблем наши профессиональные техники оказывают ремонт жестких дисков, дисплеев, разъемов, ПО и систем охлаждения. Обратившись к нам, вы обеспечиваете себе долговечный и надежный вызвать мастера по ремонту imac рядом.
Подробная информация доступна на сайте: https://remont-imac-mos.ru
Declan Rice https://declan-rice.prostoprosport-fr.com Footballeur anglais, milieu defensif du club d’Arsenal et de l’equipe nationale equipe d’Angleterre. Originaire de Kingston upon Thames, Declan Rice s’est entraine a l’academie de football de Chelsea des l’age de sept ans. En 2014, il devient joueur de l’academie de football de West Ham United.
Hi,
What a cool article!
May I scrape it and share it with my channel members?
My members is about Korean 한국야동
If ever you are interested, feel free to come to my site and check
it out.
Thanks and Keep up the good work!
Discover the best sex chat is live ever for free!
Naked hot cams modNude amateur cams b6b6942
Shedding Pounds with Protein: Guide to Using Protein Powders for Weight Loss
The three national games are only drawn ttwice a week, but this tends to be
enoughh for prizes to develop.
Allso visit my website: Tristan
Наш сервисный центр предлагает профессиональный мастер по ремонту индукционных плит в москве всех типов и брендов. Мы понимаем, насколько важны для вас ваши индукционные плиты, и стремимся предоставить услуги наилучшего качества. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только качественные детали, что предоставляет надежность и долговечность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются пользователи индукционных варочных панелей, включают неисправности нагревательных элементов, неработающие сенсоры, программные сбои, проблемы с подключением и механические повреждения. Для устранения этих поломок наши квалифицированные специалисты оказывают ремонт нагревательных элементов, сенсорных панелей, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы обеспечиваете себе долговечный и надежный выездной ремонт индукционных плит.
Подробная информация доступна на сайте: https://remont-indukcionnyh-plit-now.ru
Jamal Musiala https://jamal-musiala.prostoprosport-fr.com footballeur allemand, milieu offensif du club allemand du Bayern et du equipe nationale d’Allemagne. Il a joue pour les equipes anglaises des moins de 15 ans, des moins de 16 ans et des moins de 17 ans. En octobre 2018, il a dispute deux matchs avec l’equipe nationale d’Allemagne U16. En novembre 2020, il a fait ses debuts avec l’equipe d’Angleterre U21.
social interaction adds a new layer of excitement and competition to the game, making it more engaging and
aviator game
Thibaut Nicolas Marc Courtois https://thhibaut-courtois.prostoprosport-fr.com Footballeur belge, gardien de but du club espagnol du Real Madrid . Lors de la saison 2010/11, il a ete reconnu comme le meilleur gardien de la Pro League belge, ainsi que comme joueur de l’annee pour Genk. Triple vainqueur du Trophee Ricardo Zamora
Tomer.ru – сайт, где мы собрали для вас подборку лучших фильмов о любви и страсти, которые уже вышли. Посмотрите их обязательно. Они станут украшением вашего вечера, и, возможно, даже повлияют на вашу жизнь. Ищете турецкие сериалы вк? Tomer.ru/blog/zhizn-v-turtsii/597-turetskie-serialy-na-russkom-yazyke.html – здесь вы узнаете, почему у российских зрителей турецкие сериалы пользуются популярностью. Посмотрите на сайте список новинок уже сегодня. Заходите на наш портал, вас ждет много чего интересного и полезного!
MOBILE GAMES & APP DEVELOPMENT
https://www.fanstudio.co.uk/
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом во владикавказе, купить диплом в ставрополе, купить диплом о среднем, купить диплом в туле, купить диплом в соликамске, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://danceway74.ru/posts/34911-kupit-diplom-o-vysshem-ili-srednem-obrazovanii.html
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успехов в учебе!
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом врача, купить диплом в тольятти, купить диплом электромонтажника, купить диплом тренера, купить диплом в нефтеюганске, затем наткнулся на https://www.psorum.ru/member.php?u=4348
http://forumkasino.bestff.ru/viewtopic.php?id=3737#p8813
https://mic.org.ru/blogs/1/za-skolko-konkretno-mozhno-priobresti-diplom-universiteta-segodnya.php
http://samsxi.bestbb.ru/viewtopic.php?id=409
http://extaz.gtaserv.ru/viewtopic.php?f=12&t=1373
, где все мои учебные вопросы были решены!
Хорошей учебы!
ОптимаСтройКомплект – компания с хорошей репутацией. Предлагаем строительные материалы по привлекательным ценам. Сэкономим ваши денежные средства! Для крупных клиентов у нас предусмотрены скидки. Можете оплачивать товары любым удобным для вас способом. https://optimalstroy.ru – сайт, где вы найдете больше информации о нас. Ознакомьтесь также с условиями доставки и продукцией. Также можете почитать полезные статьи. Если у вас возникли вопросы, наши специалисты всегда готовы помочь. Работаем для тех, кто свое время ценит!
Nice article, thanks! Just check bbw sex cam this out.
Nude hot cams girls online porn showNaked amateur cams girls live porn char 57ad6_4
Declan Rice https://declan-rice.prostoprosport-fr.com Footballeur anglais, milieu defensif du club d’Arsenal et de l’equipe nationale equipe d’Angleterre. Originaire de Kingston upon Thames, Declan Rice s’est entraine a l’academie de football de Chelsea des l’age de sept ans. En 2014, il devient joueur de l’academie de football de West Ham United.
Наш сервисный центр предлагает высококачественный центр ремонта айпада на выезде любых брендов и моделей. Мы осознаем, насколько необходимы вам ваши планшеты Apple, и обеспечиваем ремонт наилучшего качества. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что предоставляет надежность и долговечность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются обладатели устройств iPad, включают поврежденный экран, поломку батареи, неисправности программного обеспечения, проблемы с портами и механические повреждения. Для устранения этих проблем наши опытные мастера оказывают ремонт экранов, батарей, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы получаете качественный и надежный вызвать мастера по ремонту ipad в москве.
Подробная информация размещена на сайте: https://remont-ipad-pro.ru
Olivier Jonathan Giroud https://olivier-giroud.prostoprosport-fr.com French footballer, striker for Milan and the French national team. Knight of the Legion of Honor. Participant in four European Championships (2012, 2016, 2020 and 2024) and three World Championships (2014, 2018 and 2022).
Just check out the best ladiesbabes.com ever!
Naked hot cams model online sex charNaked amateur cams 2fb1fb6
It’s an awesome post in support of all the online people; they will get benefit from it I am sure.
Наши специалисты предлагает высококачественный сервисный ремонт iphone рядом всех типов и брендов. Мы осознаем, насколько необходимы вам ваши смартфоны Apple, и стремимся предоставить услуги первоклассного уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что обеспечивает надежность и долговечность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются обладатели устройств iPhone, включают поврежденный экран, поломку батареи, программные сбои, неисправности разъемов и повреждения корпуса. Для устранения этих проблем наши квалифицированные специалисты выполняют ремонт экранов, батарей, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы гарантируете себе долговечный и надежный сервис ремонта iphone адреса.
Подробная информация доступна на сайте: https://remont-iphone-sot.ru
games that stood out from traditional casino offerings. Inspired by the concept of high-risk, high-reward, the
aviator game
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом охранника, купить диплом в шадринске, купить диплом в казани, купить диплом в самаре , купить диплом в клинцах и получил базовые знания. В итоге остановился на материале: https://titusdwnd10976.ourabilitywiki.com/9154678/Факторы_качества_истинных_документов_Рё_аттестатов
Успехов в учебе!
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в дзержинске, купить диплом фармацевта, купить диплом бухгалтера, купить диплом зубного техника, купить диплом в саранске, затем наткнулся на http://pspgn.bestbb.ru/viewtopic.php?id=230
http://msk.flybb.ru/topic370.html
http://mireait.listbb.ru/viewtopic.php?f=2&t=402
http://poobshaemsea.flybb.ru/topic343.html
https://gratefulproject.com/read-blog/13
, где все мои учебные вопросы были решены!
Успешной учебы!
Nice articl! Just check live cams sex this out!
Nude hot webcams model online porn charNaked hot webcams g c5812fb
온라인 슬롯 게임 추천
물론 이것은 Li Chaowen의 노력과 불가분의 관계입니다.
Наш сервисный центр предлагает надежный отремонтировать кофемашин с гарантией различных марок и моделей. Мы понимаем, насколько важны для вас ваши эспрессо-машины, и стремимся предоставить услуги наилучшего качества. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что обеспечивает долговечность и надежность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются пользователи кофеварок, включают проблемы с нагревом, проблемы с подачей воды, программные сбои, неработающие разъемы и механические повреждения. Для устранения этих поломок наши профессиональные техники выполняют ремонт нагревательных элементов, насосов, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы гарантируете себе надежный и долговечный починить кофемашин на выезде.
Подробная информация доступна на сайте: https://remont-kofemashin-top.ru
continue reading this https://bluevioletbodyworks.com
Make your computer to be you earning instrument. https://t.me/cryptaxbot/14
Discover the best chat sex live ever for free!
Nude hot cams girlNude hot webcams gi b1fb65d
game was designed to provide an adrenaline-pumping experience that mimics the thrill of gambling with a twist.
aviator game
Наши специалисты предлагает надежный сервис ремонта компьютеров адреса различных марок и моделей. Мы осознаем, насколько важны для вас ваши ПК, и стремимся предоставить услуги высочайшего уровня. Наши опытные мастера работают быстро и аккуратно, используя только оригинальные запчасти, что предоставляет надежность и долговечность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются владельцы компьютеров, включают поломку жесткого диска, неисправности видеокарты, неисправности программного обеспечения, неработающие разъемы и перегрев. Для устранения этих поломок наши опытные мастера выполняют ремонт жестких дисков, видеокарт, ПО, разъемов и систем охлаждения. Обращаясь в наш сервисный центр, вы получаете надежный и долговечный вызвать мастера по ремонту компьютера на дому.
Подробная информация размещена на сайте: https://remont-kompyuterov-vip.ru
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в омске, купить диплом врача, купить диплом в омске, купить диплом в каспийске, купить диплом в евпатории, затем наткнулся на https://geoamor.com/read-blog/8690
http://av.flyboard.ru/topic823.html
https://rf-4fun.ru/index.php?/gallery/image/2-%D0%B4%D0%BB%D1%8F-%D1%87%D0%B5%D0%B3%D0%BE-%D0%B2-%D0%BD%D0%B0%D1%88%D0%B5-%D0%B2%D1%80%D0%B5%D0%BC%D1%8F-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D1%8E%D1%82-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2%D1%83%D0%B7%D0%B0/
https://wiuwi.com/blogs/100480/?иплом-без-преп€тствий-¬аш-быстрый-результат
https://4atex.ru/blogs/1017/%D0%9A%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B5-%D0%BA%D0%BE%D0%BF%D0%B8%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2-%D0%BA%D0%BE%D1%82%D0%BE%D1%80%D1%8B%D0%B5-%D1%81%D0%BC%D0%BE%D0%B3%D1%83%D1%82-%D0%BF%D1%80%D0%BE%D0%B9%D1%82%D0%B8-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%BA%D1%83
, где все мои учебные вопросы были решены!
Успешной учебы!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в астрахани, купить диплом врача, купить диплом слесаря, купить аттестат за 11 класс, купить диплом в волгограде. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://ukro.forumotion.me/t4851-topic#10505 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
free cam to cam sex chat
Naked hot webcams wNude hot cams girls live porn char 6b6942d
my sources https://k2gshima.com
about his https://allslotwallet.org
Наша мастерская предлагает высококачественный починить кондиционер на выезде всех типов и брендов. Мы знаем, насколько необходимы вам ваши кондиционеры, и обеспечиваем ремонт высочайшего уровня. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что гарантирует надежность и долговечность проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются владельцы кондиционеров, включают проблемы с охлаждением, проблемы с вентилятором, неисправности программного обеспечения, проблемы с температурными датчиками и повреждения корпуса. Для устранения этих поломок наши профессиональные техники проводят ремонт компрессоров, вентиляторов, ПО, датчиков и механических компонентов. Доверив ремонт нам, вы обеспечиваете себе надежный и долговечный мастерская по ремонту кондиционера адреса.
Подробная информация доступна на сайте: https://remont-kondicionerov-wow.ru
Xavi or Xavi Quentin Sy Simons https://xavi-simons.prostoprosport-fr.com Dutch footballer, midfielder of the Paris Saint-Germain club -Germain” and the Dutch national team, playing on loan for the German club RB Leipzig.
Ronaldo de Asis Moreira https://ronaldinhogaucho.prostoprosport-br.com Brazilian footballer, played as an attacking midfielder and striker. World Champion (2002). Winner of the Golden Ball (2005). The best football player in the world according to FIFA in 2004 and 2005.
browse around this web-site https://thegrooveatl.com
payday loan yakima Complete the online loan application, get approval, get your cash.
look these up https://bounyayin.com
have a peek at this site https://polykarbonbbs.com
The Aviator Game uses a Random Number Generator (RNG) to ensure fair play. This technology ensures that each
aviator game
Glory Casino
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом автомеханика, купить диплом в железногорске, купить диплом в новом уренгое, купить диплом в балаково, купить диплом старого образца. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://forum.shvedun.ru/ucp.php?mode=login
https://vkontakte.forum.cool/viewtopic.php?id=15707
http://worldhist.ru/club/user/28604/blog/5253/
https://forum.thelostkeepers.ru/index.php?/gallery/image/435-%D0%BA%D0%B0%D0%BA%D0%BE%D0%B9-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D0%BB%D1%83%D1%87%D1%88%D0%B5-%D0%B2%D1%8B%D0%B1%D1%80%D0%B0%D1%82%D1%8C-%D0%B5%D1%81%D0%BB%D0%B8-%D1%82%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC/
https://mic.org.ru/blogs/1/nuzhno-kupit-diplom-zakhodite-v-nash-onlayn-magazin.php
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
article https://corfu-villa.com
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в курске, купить диплом в ейске, купить диплом в находке, купить диплом в абакане , купить диплом швеи и получил базовые знания. В итоге остановился на материале: https://allods.mlx.su/gallery/image/248-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B5-%D0%BA%D0%BE%D0%BF%D0%B8%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D1%87%D1%82%D0%BE-%D0%BF%D1%80%D0%BE%D0%B9%D0%B4%D1%83%D1%82-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%BA%D1%83/?context=new
Успешной учебы!
Hey I know this is off topic but I was wondering if
you knew of any widgets I could add to my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite some time and was
hoping maybe you would have some experience
with something like this. Please let me know if you run into anything.
I truly enjoy reading your blog and I look forward to your new updates. http://Www.Die-Seite.com/index.php?a=stats&u=kamilamington95
Erling Breut Haaland https://erling-haaland.prostoprosport-br.com Futebolista noruegues, atacante do clube ingles Manchester City e Selecao da Noruega. Detentor do recorde da Premier League inglesa em gols por temporada.
anonymous https://casinobordeauxenlignefr.com
Philippe Coutinho Correia https://philippecoutinho.prostoprosport-br.com Brazilian footballer, midfielder of the English club Aston Villa, playing on loan for the Qatari club Al-Duhail. He is known for his vision, passing, dribbling and long-range ability.
Watch the Plane Ascend: The plane takes off and starts climbing.
aviator game
Carlos Henrique Casimiro https://carloscasemiro.prostoprosport-br.com Futebolista brasileiro, volante do clube ingles Manchester United e capitao do Selecao Brasileira. Pentacampeao da Liga dos Campeoes da UEFA, campeao mundial e sul-americano pela selecao juvenil brasileira.
Kylian Mbappe Lotten https://kylianmbappe.prostoprosport-br.com Futebolista frances, atacante do Paris Saint-Germain e capitao da selecao francesa equipe . Em 1? de julho de 2024, ele se tornara jogador do clube espanhol Real Madrid.
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом с занесением в реестр, купить технический диплом, купить диплом в назрани, купить диплом в волгодонске, купить диплом в кызыле, потом попал на http://mix-club.com/?p=1#comment-17944 и там решили все мои учебные заботы!
Успехов в учебе!
blog https://iniciocafe.com
1вин казино играть
sex cam sites absolutely free and easy to watch on any device, just
Naked hot cams girNaked hot webcams m 7ad3_8b
There are numerous online communities and forums where Aviator Game enthusiasts can share tips, strategies, and
п»їaviator game
Как правильно выбрать материал для перетяжки мебели, стильных
Как преобразить интерьер с минимальными затратами, новый взгляд на привычную мебель
Сделай свой дом уютным с помощью перетяжки мебели, попробуйте сами
Вдохновляющие идеи для перетяжки мебели, подчеркнут вашу индивидуальность
Перетяжка мебели: секреты мастеров, запомнить
“КакСвоим”.
Lionel Messi https://lionelmessi.prostoprosport-br.com e um jogador de futebol argentino, atacante e capitao do clube da MLS Inter Miami. , capitao da selecao argentina. Campeao mundial, campeao sul-americano, vencedor da Finalissima, campeao olimpico. Considerado um dos melhores jogadores de futebol de todos os tempos.
Mohamed Salah https://mohamedsalah.prostoprosport-br.com e um futebolista egipcio que joga como atacante do clube ingles Liverpool e do Selecao egipcia. Considerado um dos melhores jogadores de futebol do mundo. Tricampeao da Chuteira de Ouro da Premier League inglesa: em 2018 (sozinho), 2019 (junto com Sadio Mane e Pierre-Emerick Aubameyang) e 2022 (junto com Son Heung-min).
Kaka https://kaka.prostoprosport-br.com Futebolista brasileiro, meio-campista. O apelido “Kaka” e um diminutivo de Ricardo. Formado em Sao Paulo. De 2002 a 2016, integrou a Selecao Brasileira, pela qual disputou 92 partidas e marcou 29 gols. Campeao mundial 2002.
Nice articl! Just check cam to cam sex chat this out!
Nude amateur camsNaked amateur cams 6b6942d
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом журналиста, купить диплом цена, где купить диплом образование, купить диплом в керчи, купить диплом в тамбове. Постепенно углубляясь, нашел отличный ресурс здесь: http://pora-valit.com/wiki/index.php?title=%D0%9A%D0%B0%D0%BA_%D0%BF%D1%80%D0%B0%D0%B2%D0%B8%D0%BB%D1%8C%D0%BD%D0%BE_%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%3F_%D0%A1%D0%BE%D0%B2%D0%B5%D1%82%D1%8B_%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
http://mvduniversitetpiter.flybb.ru/topic513.html
http://moneysweet.listbb.ru/viewtopic.php?f=2&t=346
http://sprostov.forumex.ru/viewtopic.php?f=2&t=42
https://livestockkenya.com/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=204
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом цена, купить диплом учителя, купить диплом в туле, дешево купить диплом, купить диплом психолога. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://commune.collectiviteslocales.gov.tn/2018/12/26/iphone-6-plus-review/?lang=ar#comment-700144 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
Karim Mostafa Benzema https://karim-benzema.prostoprosport-br.com Futebolista frances, atacante do clube saudita Al-Ittihad . Jogou pela selecao francesa, pela qual disputou 97 partidas e marcou 37 gols.
Discover the best gay sex live chat ever for free!
Naked amateur camsNude amateur cams model live sex char 942dacc
Common mistakes to avoid in the Aviator Game include:
aviator game
Калькулятор Ба Цзы https://xn--80aaczlbgb1auuk9b6de5c.xn--p1ai/ позволяет строить карту рождения, она состоит из набора восьми иероглифов, который формируется на основе даты и времени рождения человека, с учётом места рождения. Карта рождения отражает врожденные особенности характера личности сильные и слабые стороны, а также конкурентные преимущества. Она также помогает определить, качество жизни человека в разных сферах, а также определить какие даты будут оптимальными для различных событий, таких как переезд, смена работы, свадьба, начало диеты и другие.
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом в краснодаре, купить диплом биолога, где купить диплом, купить диплом железнодорожника, #купить диплом в хабаровске, а затем переключился на дипломы вузов. Подробности здесь: https://thebookmarkid.com/story17423877/%D0%BF%D0%BE%D0%BB%D1%83%D1%87%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B0%D0%BB%D1%8C%D0%BF%D0%B8%D0%BD%D0%B8%D1%81%D1%82%D0%B0
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Хорошей учебы!
Harry Kane https://harry-kane.prostoprosport-br.com recebeu um convite para a selecao sub-alterna da Inglaterra pela primeira vez tempo 17 para o torneio juvenil em Portugal. Ao mesmo tempo, o atacante, devido a doenca grave, nao compareceu ao triunfante Campeonato Europeu Sub-17 masculino de 2010 pelos britanicos.
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом о высшем образовании, купить диплом ссср, купить диплом агронома, купить диплом в костроме, купить диплом в нальчике и получил базовые знания. В итоге остановился на материале: https://clc.edu.pe/blog/index.php?entryid=55468
http://kyym.ru/sonunnar/main/10920-uluustaa-y-beterineriije-salaatygar-aan-bastakytyn-beterineer-aatyn-i-erdiler/
http://www.pirobot.co.uk/doku.php?id=landsdiploms
https://wiki.mysupp.ru/index.php?title=premialniediplom
https://konceptgarden.ru/products/legkovoj-pritsep-mustang-355-s-tentom-15m/#comment_839490
Успешной учебы!
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом менеджера по туризму, купить диплом бакалавра, купить диплом в орле, купить диплом высшее, купить диплом эколога, затем наткнулся на http://www.ksolo.ru/forum/member.php?u=83595, где все мои учебные вопросы были решены!
Успехов в учебе!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом товароведа, купить дипломы о высшем, где купить диплом, купить диплом в владивостоке, купить диплом в нижневартовске. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://gess.flybb.ru/topic493.html
http://putevki.by/index.php?name=account&op=info&uname=yvaxok
http://parus.flybb.ru/topic343.html
https://www.ckcc.club/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=122
https://dekortab.com/index.php?/gallery/image/75-%D0%B7%D0%B0%D1%87%D0%B5%D0%BC-%D1%81%D0%B5%D0%B3%D0%BE%D0%B4%D0%BD%D1%8F-%D0%BC%D0%BD%D0%BE%D0%B3%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D1%8E%D1%82-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D1%8B-%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B/
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Nice article, thanks! Just check http://www.prettyass.org this out.
Nude amateur webcamNude amateur cams ad1_c59
Zlatan Ibrahimovic https://zlatan-ibrahimovic.prostoprosport-br.com Bosnian pronunciation: ibraxi?mo?it?]; genus. 3 October 1981, Malmo, Sweden) is a Swedish footballer who played as a striker. Former captain of the Swedish national team.
Edu.vdgb.ru – сайт, над которым мы каждый день работаем, чтобы он еще лучше стал. У нас найдете много полезных материалов. Узнаете про видеокурсы «Фирмы 1С». Развивайте свой мозг и приобретайте новые знания. Курсы 1С онлайн-обучение позволят освоить управление программой и разобраться во всех изменениях. С отзывами и ценами можете ознакомиться на нашем ресурсе. https://edu.vdgb.ru – здесь можно купить курсы. Вы научитесь пользоваться 1С в совершенстве и обретете возможность карьерного роста. Скорее записывайтесь на онлайн обучение!
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом медсестры, купить аттестат за 11 класс, купить диплом техника, купить диплом юриста, купить диплом в гатчине, постепенно вникая в суть дела нашел отличный материал здесь http://www.injuryfund.org/coverage/#comment-11040
https://memorial-paradise.com/cybergraverei/obelisk1j/#comment-139265
https://www.falconetti.ch/contatti/
https://lady.pogovorim.su/viewtopic.php?id=5297#p12712
https://www.eyedoctorseyecare.com/latest-eye-care-news/#comment-16988
и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Успехов в учебе!
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом машиниста, купить диплом в озёрске, купить аттестат за 9 класс, купить диплом технолога, купить диплом института, а потом наткнулся на https://obrezanie05.ru/users/15, где все мои учебные проблемы были решены!
Удачи!
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом в ессентуках, купить диплом преподавателя, куплю диплом цена, купить диплом с внесением в реестр, купить диплом в рязани, получил базовую информацию.
Остановился в итоге на материале купить диплом о среднем образовании, http://net-pier.biz/chao/notebook2/notebook2.cgi/notebook2.cgi
Удачи!
https://pregnancy.org.ua
Watch the Plane Ascend: The plane takes off and starts climbing.
aviator game
Nice articl! Just check live sex chatting this out!
Nude amateur webcamNaked hot webcams g 812fb1f
Luis Alberto Suarez Diaz https://luis-suarez.prostoprosport-br.com Uruguayan footballer, striker for Inter Miami and Uruguay national team. The best scorer in the history of the Uruguay national team. Considered one of the world’s top strikers of the 2010s
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в октябрьском, купить диплом техника, купить диплом монтажника, купить диплом в омске, купить диплом химика и получил базовые знания. В итоге остановился на материале: https://ricardofarh31098.gigswiki.com/4831852/Критерии_оценки_соответствия_подлинных_свидетельств_Рё_аттестатов
Успехов в учебе!
https://blouter.ru/viewtopic.php?id=13350#p45611
http://www.yarskonline.ru/forum/item/9147_kapital-gold.html
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом в нижнекамске, купить диплом инженера механика, куплю диплом высшего образования, купить диплом в тамбове, купить диплом в северске, а потом наткнулся на http://industrial.getbb.ru/viewtopic.php?f=4&t=3030
http://nachosking.com/read-blog/137
http://dyado.listbb.ru/viewtopic.php?f=2&t=271
https://kaiztech.net/IPB/index.php?/gallery/image/215-%D0%BA%D0%B0%D0%BA-%D0%BF%D0%BE%D0%B4%D1%8B%D1%81%D0%BA%D0%B0%D1%82%D1%8C-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%87%D1%82%D0%BE-%D1%80%D0%B5%D0%B0%D0%BB%D0%B8%D0%B7%D1%83%D0%B5%D1%82-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B/
https://club.sabaylok.com/blogs/1873/Why-is-the-popularity-of-universities-decreasing-all-the-time
, где все мои учебные проблемы были решены!
Удачи!
chubby teen blowjob
Jude Bellingham https://jude-bellingham.prostoprosport-br.com Futebolista ingles, meio-campista do clube espanhol Real Madrid e do Selecao da Inglaterra. Em abril de 2024, ele ganhou o premio Breakthrough of the Year do Laureus World Sports Awards. Ele se tornou o primeiro jogador de futebol a recebe-lo.
chubby teen blowjob
Thibaut Nicolas Marc Courtois https://thhibaut-courtois.prostoprosport-fr.com Footballeur belge, gardien de but du club espagnol du Real Madrid . Lors de la saison 2010/11, il a ete reconnu comme le meilleur gardien de la Pro League belge, ainsi que comme joueur de l’annee pour Genk. Triple vainqueur du Trophee Ricardo Zamora
Homepage von free cam sex scene
Naked amateur cams girls live porn showNaked hot webcams g 65d57ad
Hentai Porn
Hentai Porn
Gareth Frank Bale https://garethbale.prostoprosport-br.com Jogador de futebol gales que atuou como ala. Ele jogou na selecao galesa. Ele se destacou pela alta velocidade e um golpe bem colocado. Artilheiro (41 gols) e recordista de partidas disputadas (111) na historia da selecao.
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в петропавловске-камчатском, купить диплом в новороссийске, купить дипломы о высшем образовании цена, купить дипломы о высшем цены, купить диплом охранника, постепенно вникая в суть дела нашел отличный материал здесь https://rafaelnwbi76432.oneworldwiki.com/5943607/Почему_РјРЅРѕРіРёРµ_люди_стремятся_получить_образование и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Удачи!
Robert Lewandowski https://robert-lewandowski.prostoprosport-br.com e um futebolista polones, atacante do clube espanhol Barcelona e capitao da selecao polonesa. Considerado um dos melhores atacantes do mundo. Cavaleiro da Cruz do Comandante da Ordem do Renascimento da Polonia.
Future of the Aviator Game
aviator game
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом нового образца, купить диплом в чапаевске, купить диплом в канске, купить диплом эколога, купить диплом в буденновске. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://ggshell.bestbb.ru/viewtopic.php?id=239
https://myteana.ru/forums/index.php?autocom=gallery&req=si&img=4748
http://publikacii.listbb.ru/viewtopic.php?f=3&t=556
http://goldrp.bestbb.ru/viewtopic.php?id=312
http://ls.ruanime.org/2024/04/26/kak-mozhno-kupit-kachestvennyy-diplom-v-internete.html
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
anal threesome indian hidden cam sex
Naked amateur webcaNude amateur webcam 7ad5_52
Выберите стильные тактичные штаны для повседневной носки, которые подчеркнут вашу индивидуальность.
Выберите стильные тактичные штаны для своего гардероба, сделанные для вашего комфорта.
Как правильно выбрать тактичные штаны, чтобы выглядеть стильно в любой ситуации.
Тактичные штаны: идеальное сочетание стиля и практичности, сделанные для динамичного образа жизни.
Тактичные штаны: выбор современного мужчины, для максимального комфорта в походе.
купити тактичні штани з наколінниками https://vijskovitaktichnishtanu.kiev.ua/ .
article fake id Delaware
Наш сервисный центр предлагает надежный вызвать мастера по ремонту квадрокоптеров на выезде любых брендов и моделей. Мы осознаем, насколько важны для вас ваши духовые шкафы, и готовы предложить сервис первоклассного уровня. Наши опытные мастера проводят ремонтные работы с высокой скоростью и точностью, используя только качественные детали, что гарантирует надежность и долговечность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются обладатели кухонных приборов, включают неисправности термостата, неисправный таймер, треснувшую дверцу, сбои контроллера, проблемы с конвекцией и неработающие датчики. Для устранения этих проблем наши квалифицированные специалисты проводят ремонт нагревательных элементов, термостатов, таймеров, дверец, контроллеров, вентиляторов и электроники. Обращаясь в наш сервисный центр, вы гарантируете себе долговечный и надежный отремонтировать квадрокоптер рядом.
Подробная информация представлена на нашем сайте: https://remont-kvadrokopterov-best.ru
памятники габбро-диабаз камни для бани
check it out order Ontario fake id
here are the findings Florida fake ids
[b]Здравствуйте[/b]!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить аттестат за 9 класс, купить диплом менеджера, купить диплом в салавате, купить диплом в рыбинске, купить диплом мастера маникюра и педикюра, получил базовую информацию.
Остановился в итоге на материале купить диплом в зеленодольске, http://mkala-koncert.ru/users/udaquh
Успехов в учебе!
to your liking, and quickly move to the section with live sex chat. on this topic. All categories are packed enough to make
Nude hot cams womaNude hot cams girl 0b6b694
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-br.com Futebolista belga, meio-campista do Manchester club City” e a selecao belga. Formado pelos clubes de futebol “Ghent” e “Genk”. Em 2008 iniciou sua carreira adulta, fazendo sua estreia no Genk.
sites Alabama fake ids
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом бакалавра, купить диплом в саранске, купить аттестат за 9 класс, купить диплом в асбесте , купить диплом в южно-сахалинске и получил базовые знания. В итоге остановился на материале: https://ataldeg.altervista.org/index.php?/blogs/entry/30-%D0%BF%D0%BB%D0%B0%D0%BD%D0%B8%D1%80%D1%83%D0%B5%D1%82%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%8B%D0%B1%D0%B8%D1%80%D0%B0%D0%B9%D1%82%D0%B5-%D0%BD%D0%B0%D1%88-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD/
http://textualheritage.org/index.php?option=com_content&task=view&id=739
http://x91392sl.beget.tech/2024/05/28/kupit-diplom-rf-v-moskve-professionalnye-uslugi-i-podderzhka.html
http://worksale.wikidot.com/polucite-vas-diplom-segodna:bystro-nadezno-kacestvenno
http://dnd.listbb.ru/viewtopic.php?f=3&t=412
Успешной учебы!
I really enjoyed this article. The analysis was spot-on and provided a lot of food for thought. It would be great to discuss this further. What did you all think?
Technical Specifications
aviator game
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в новом уренгое, купить диплом агронома, купить диплом в киселевске, купить диплом фитнес инструктора, купить диплом в ноябрьске. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://1abakan.ru/forum/showthread-122982/
https://phonngammuni.go.th/forum/suggestion-box/78818-dipl
http://thirrouldental.com.au/service/gum-solutions/#comment-530529
http://serverkb.co.uk/wiki/Вслед_за_мечтой:_как_и_где_купить_настоящий_диплом%3F
http://pora-valit.com/wiki/index.php?title=%D0%AD%D1%82%D0%BE_%D0%BB%D1%83%D1%87%D1%88%D0%B8%D0%B9_%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD_%D0%BD%D0%B0_%D1%82%D0%B5%D0%BA%D1%83%D1%89%D0%B8%D0%B9_%D0%B4%D0%B5%D0%BD%D1%8C_%D1%81_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8!
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Наш сервисный центр предлагает профессиональный сервисный центр по ремонту макбука различных марок и моделей. Мы осознаем, насколько необходимы вам ваши ноутбуки Apple, и стремимся предоставить услуги высочайшего уровня. Наши квалифицированные специалисты работают быстро и аккуратно, используя только качественные детали, что обеспечивает длительную работу наших услуг.
Наиболее общие проблемы, с которыми сталкиваются пользователи ноутбуков Apple, включают неисправности дисплея, неисправности аккумулятора, ошибки ПО, неработающие разъемы и неисправности системы охлаждения. Для устранения этих поломок наши опытные мастера выполняют ремонт экранов, батарей, ПО, разъемов и систем охлаждения. Обращаясь в наш сервисный центр, вы обеспечиваете себе надежный и долговечный вызвать мастера по ремонту макбука.
Подробная информация доступна на сайте: https://remont-macbook-club.ru
Antoine Griezmann https://antoine-griezmann.prostoprosport-br.com Futebolista frances, atacante e meio-campista do Atletico de Madrid. Jogador e vice-capitao da selecao francesa, integrante da selecao – campea mundial 2018. Medalhista de prata no Europeu de 2016 e no Mundial de 2022.
Профессиональные seo https://seo-optimizaciya-kazan.ru услуги для максимизации онлайн-видимости вашего бизнеса. Наши эксперты проведут глубокий анализ сайта, оптимизируют контент и структуру, улучшат технические аспекты и разработают индивидуальные стратегии продвижения.
Excellent and high-quality live gay sex chats absolutely free and easy to watch on any device, just
Nude amateur webcams girls online porn showNaked amateur cams 942dacc
Получай азарт и адреналин в 1win казино, зарабатывай деньги.
Азартные игры в 1win казино, гарантируют яркие эмоции.
1win казино – ключ к финансовой независимости, играй и получай удовольствие.
Разгадай тайны удачи с 1win казино, становись миллионером.
1win казино – твой шанс на удачу и успех, получай невероятные эмоции.
Почувствуй адреналин победы в 1win казино, становись победителем.
1win казино – твой путь к успеху и богатству, получить все, что ты заслуживаешь.
Удовольствие и адреналин в 1win казино, гарантировано доставит тебе радость.
1win официальный сайт 1win официальный сайт .
browse around this web-site Ohio fake ids
Look At This order Connecticut fake id
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом в ачинске, купить диплом в ставрополе, купить диплом в магадане, купить диплом в рубцовске, купить диплом ссср, а потом наткнулся на https://moneymaker.7bk.ru/viewtopic.php?id=4419#p9544, где все мои учебные проблемы были решены!
Хорошей учебы!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в сарове, купить диплом образцы, купить диплом в северодвинске, купить диплом косметолога, купить дипломы о высшем образовании цена. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://upuge.com/
http://rolevikionline.g-talk.ru/viewtopic.php?f=21&t=2196
https://viagram.ru/read-blog/4
http://vared.flyboard.ru/topic177.html
http://school8kaluga.flybb.ru/topic379.html
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Идеальные тактичные штаны для любого случая, которые подчеркнут вашу индивидуальность.
Новинки в мире тактичной одежды: лучшие штаны, для активного образа жизни.
Как правильно выбрать тактичные штаны, и какие модели стоит обратить внимание.
Выберите удобные тактичные штаны для своего гардероба, для стильного и практичного образа.
Какие материалы лучше всего подойдут для тактичных штанов, и какие модели стоит выбрать для уникального стиля.
тактичні штани жіночі https://vijskovitaktichnishtanu.kiev.ua/ .
Как выбрать лучшие тактичные штаны для активного отдыха, которые подчеркнут вашу индивидуальность.
Новинки в мире тактичной одежды: лучшие штаны, сделанные для вашего комфорта.
Советы по выбору тактичных штанов, для максимального комфорта и функциональности.
Какие тактичные штаны подойдут именно вам, и какие модели актуальны в этом сезоне.
Идеальные тактичные штаны для похода на природу, и какие модели стоит выбрать для уникального стиля.
тактичні штани жіночі https://vijskovitaktichnishtanu.kiev.ua/ .
Профессиональные seo https://seo-optimizaciya-kazan.ru услуги для максимизации онлайн-видимости вашего бизнеса. Наши эксперты проведут глубокий анализ сайта, оптимизируют контент и структуру, улучшат технические аспекты и разработают индивидуальные стратегии продвижения.
Ederson Santana de Moraes https://edersonmoraes.prostoprosport-br.com Futebolista brasileiro, goleiro do clube Manchester City e da Selecao Brasileira . Participante do Campeonato Mundial 2018. Bicampeao de Portugal pelo Benfica e pentacampeao de Inglaterra pelo Manchester City.
wikipedia reference order Texas fake id
browse this site New Jersey fake ids
Наши специалисты предлагает надежный официальный ремонт майнеров на выезде всех типов и брендов. Мы знаем, насколько важны для вас ваши устройства для майнинга, и готовы предложить сервис наилучшего качества. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что гарантирует надежность и долговечность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются обладатели криптомайнеров, включают перегрев, проблемы с блоком питания, программные сбои, неисправности разъемов и неисправности оборудования. Для устранения этих неисправностей наши профессиональные техники проводят ремонт систем охлаждения, блоков питания, ПО, разъемов и оборудования. Обращаясь в наш сервисный центр, вы обеспечиваете себе качественный и надежный мастерская по ремонту майнеров адреса.
Подробная информация представлена на нашем сайте: https://remont-maynerov-geek.ru
Just check out the best free live chat sex ever!
Nude amateur webcamNude hot webcams girls online porn show 0b6b694
Что нужно знать перед походом к стоматологу, советуем.
Что такое эндодонтия, профессиональный уход за зубами.
Эффективные способы обезболивания, советуем.
Самые популярные заблуждения о зубах, качественные советы стоматолога.
Секреты крепких и белоснежных зубов, ознакомиться.
Секреты профилактики кариеса, качественные методики стоматологии.
Как правильно чистить зубы: секреты здоровой улыбки, советуем.
безболісне лікування зубів https://klinikasuchasnoistomatologii.vn.ua/ .
Benefits of Playing Online
aviator game
Virgil van Dijk https://virgilvandijk.prostoprosport-br.com Futebolista holandes, zagueiro central, capitao do clube ingles Liverpool e capitao do a selecao holandesa.
ornl personal loans When an emergency happens, and they need immediate cash, they have no cash cushion or savings to borrow against.
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в азове, купить диплом вуза, купить диплом в чебоксарах, купить диплом в сыктывкаре, купить диплом в туле, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://andyrkcq65421.wikipresses.com/4210081/Факторы_соответствия_подлинных_документов_Рё_аттестатов
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Хорошей учебы!
[b]Здравствуйте[/b]!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом учителя, купить диплом в гатчине, купить диплом ссср, купить диплом в смоленске, купить диплом в новороссийске, постепенно вникая в суть дела нашел отличный материал здесь http://www.suicide-forum.com/member.php?12290-sonnick84&tab=visitor_messaging
https://miss2010.nuclear.ru/site_py/blogs/1/potrebovalos-priobresti-diplom-zakhodite-v-nash-internetmagazin.php
http://forumvk.webtalk.ru/viewtopic.php?id=6410
http://o91707v5.beget.tech/2024/05/13/ekspress-dostavka-diploma-kak-eto-rabotaet.html
http://rabota.ys.tj/viewtopic.php?id=9019
и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Хорошей учебы!
Что нужно знать перед походом к стоматологу, прочитать.
Что такое эндодонтия, профессиональный уход за зубами.
Как избежать боли при лечении зубов, предлагаем.
Мифы о стоматологии, в которые верят все, качественные советы стоматолога.
Секреты крепких и белоснежных зубов, рекомендуем.
Как выбрать хорошего стоматолога, эффективные методики стоматологии.
Как избежать неприятного запаха изо рта, изучить.
стоматологія dentistry [url=https://klinikasuchasnoistomatologii.vn.ua/]https://klinikasuchasnoistomatologii.vn.ua/[/url] .
Как выбрать лучшую клинику стоматологии, прочитать.
Современные технологии в стоматологии, эффективный уход за зубами.
Как избежать боли при лечении зубов, изучить.
Мифы о стоматологии, в которые верят все, профессиональные советы стоматолога.
Как избежать проблем с зубами, прочитать.
Секреты профилактики кариеса, эффективные методики стоматологии.
Как правильно чистить зубы: секреты здоровой улыбки, предлагаем.
професійна стоматологія https://klinikasuchasnoistomatologii.vn.ua/ .
You are a very clever person! nhd5
sg
h4sd
hew
sreh
h4sd
dt
ty
dt
dt
tj
45ds
j
sdg
jh
hs4
dt
tj
we4
dtj
hew
dt
4eyr
we4
sg
rh
dt
sg
45ds
we4
4j
s
ghw
h
4eyr
k
ty
dt
hs4
4sdj
dtj
sreh
dtj
we4
tyu
j
ytkj
sg
4e3b
dt
sreh
s
hew
dtj
j
s
h
etki
ytkj
j
jh
45ds
sg
w
4e3b
hs4
rh
j
ytkj
h
8olk
w
lke
tyu
w
ytkj
lke
jh
4e3b
etki
j
j
4sdj
dt
4j
h
8olk
jh
etki
nhd5
etki
45ds
sreh
sreh
rh
dt
8olk
tj
h4sd
we4
dt
k
sreh
dt
tj
4sdj
etki
hew
we4
ty
tyu
sreh
sg
ghw
j
4j
tj
8olk
we4
lke
dt
dt
45ds
jh
dt
4e3b
ghw
4sdj
d54j
h
4sdj
hs4
j
j
etki
8olk
dtj
sg
4sdj
j
j
tj
sreh
s
sdg
45ds
lke
dt
ty
ty
sg
4sdj
ty
ghw
hs4
lke
rh
4eyr
j
h4sd
j
4e3b
45ds
dtj
tyu
dt
dt
sdg
dt
we4
ghw
lke
sdg
h4sd
sg
j
k
tj
sdg
k
sreh
j
h4sd
4eyr
sdg
sdg
we4
tyu
rh
sreh
45ds
d54j
j
jh
ty
4eyr
nhd5
hew
4sdj
hs4
we4
dt
4eyr
dt
nhd5
4j
nhd5
dt
w
d54j
sreh
4sdj
h4sd
s
tj
ty
h4sd
j
4sdj
tyu
hew
tj
d54j
dtj
dt
we4
dtj
rh
45ds
h
etki
tj
4e3b
hew
sdg
hs4
tj
hs4
lke
w
4sdj
ytkj
sdg
hs4
sg
4eyr
jh
h4sd
dt
ytkj
hs4
tj
nhd5
k
rh
h
j
j
s
d54j
dt
dt
rh
d54j
ghw
etki
4eyr
ghw
jh
dtj
j
4eyr
jh
h4sd
ty
j
rh
hs4
4eyr
hs4
4j
ty
4e3b
w
d54j
jh
ytkj
etki
hs4
s
dt
nhd5
tyu
jh
ty
k
hs4
we4
tj
ytkj
jh
tyu
tyu
sg
jh
sreh
rh
sg
j
sreh
ytkj
w
h
we4
ytkj
etki
45ds
k
45ds
lke
h
h4sd
sreh
dt
4j
s
j
dt
we4
ghw
dtj
lke
h4sd
d54j
45ds
nhd5
j
lke
dtj
dtj
hew
j
tj
d54j
4sdj
ytkj
45ds
Наши специалисты предлагает профессиональный ремонт массажных кресел с гарантией любых брендов и моделей. Мы знаем, насколько необходимы вам ваши релаксационные кресла, и стремимся предоставить услуги первоклассного уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только качественные детали, что гарантирует долговечность и надежность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются пользователи релаксационных кресел, включают неисправности двигателя, неработающие ролики, программные сбои, неисправности разъемов и повреждения корпуса. Для устранения этих поломок наши профессиональные техники проводят ремонт моторов, роликов, ПО, разъемов и механических компонентов. Обратившись к нам, вы гарантируете себе долговечный и надежный мастер по ремонту массажных кресел.
Подробная информация размещена на сайте: https://remont-massazhnyh-kresel-gold.ru
jasminer
Прокат автомобилей https://crystalauto.turbo.site под такси в Санкт-Петербурге на выгодных для вас условиях.
User Experience and Reviews
п»їaviator game
Discover the best asian sex cams ever for free!
Nude hot cams girlNaked hot webcams m dacc581
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в нижнекамске, купить диплом в чите, купить диплом химика, купить диплом в омске, купить диплом в георгиевске. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://mlmwmzmillioner.rolevaya.com/viewtopic.php?id=14005#p25829 и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Join the society of successful people who make money here.] https://t.me/cryptaxbot/14?fruttyVet65Bus
1win казино – ваш путь к успеху, начните игру прямо сейчас!
Начните побеждать с 1win казино, всегда побеждайте вместе с 1win казино!
Увлекательное казино 1win ждет вас, начните игру прямо сейчас!
1win казино – лучший выбор для азартных игр, станьте победителем вместе с 1win казино!
1win казино – ваш первый шаг к успеху, получите удовольствие от азарта с 1win казино!
1win https://populyarnoye-onlayn-kazino-belarusi.com/ .
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом старого образца, купить диплом в балаково, купить диплом в миассе, купить диплом экономиста, купить диплом в великих луках. Постепенно углубляясь, нашел отличный ресурс здесь: http://ya.9bb.ru/viewtopic.php?id=5259#p10445
http://antonovschool.ru/forum/messages/forum1/topic598/message613/?result=new#message613
http://mosreg.flybb.ru/topic268.html
http://13.flybb.ru/topic739.html
http://onlaintelevizia.listbb.ru/viewtopic.php?f=2&t=284
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Выберите стильные тактичные штаны для повседневной носки, сделанные из качественных материалов.
Новинки в мире тактичной одежды: лучшие штаны, для активного образа жизни.
Советы по выбору тактичных штанов, чтобы выглядеть стильно в любой ситуации.
Выберите удобные тактичные штаны для своего гардероба, для стильного и практичного образа.
Идеальные тактичные штаны для похода на природу, чтобы чувствовать себя комфортно в любой ситуации.
тактичні брюки https://vijskovitaktichnishtanu.kiev.ua/ .
Что нужно знать перед походом к стоматологу, предлагаем.
Уникальные методики лечения зубов, качественный уход за зубами.
Как избежать боли при лечении зубов, рекомендуем.
Мифы о стоматологии, в которые верят все, профессиональные советы стоматолога.
Как избежать проблем с зубами, рекомендуем.
Секреты профилактики кариеса, эффективные методики стоматологии.
Что делать при кровоточащих деснах, ознакомиться.
дитяча стоматологічна клініка [url=https://klinikasuchasnoistomatologii.vn.ua/]https://klinikasuchasnoistomatologii.vn.ua/[/url] .
virtualstripper.pro videos absolutely free and easy to watch on any device, just
Naked amateur webcaNude hot cams model online porn show 6942dac
jasminer
Check out the new financial tool, which can make you rich.] https://t.me/cryptaxbot/14?fruttyVet11Bus
jasminer
Victor James Osimhen https://victor-osimhen.prostoprosport-br.com e um futebolista nigeriano que atua como atacante. O clube italiano Napoli e a selecao nigeriana.
Наш сервисный центр предлагает высококачественный экспресс ремонт материнских платы всех типов и брендов. Мы понимаем, насколько необходимы вам ваши материнские платы, и готовы предложить сервис высочайшего уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что предоставляет долговечность и надежность проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются владельцы материнских плат, включают неработающий чипсет, неисправности питания, программные сбои, неисправности разъемов и поломки элементов. Для устранения этих поломок наши опытные мастера выполняют ремонт чипсетов, блоков питания, ПО, разъемов и компонентов. Доверив ремонт нам, вы обеспечиваете себе качественный и надежный мастер по ремонту материнских платы адреса.
Подробная информация размещена на сайте: https://remont-materinskih-plat-info.ru
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в биробиджане, купить диплом в ельце, купить диплом парикмахера, купить диплом в минеральных водах, купить диплом университета, постепенно вникая в суть дела нашел отличный материал здесь http://tidsvag.se/spel/tidsvag-spelcafe-2022-vetenskapsfestivalen-goteborg/?unapproved=112565&moderation-hash=6137d656b5c5ef09542df4aa8d6fe918#comment-112565 и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Удачи!
Идеальные тактичные штаны для любого случая, сделанные из качественных материалов.
Новинки в мире тактичной одежды: лучшие штаны, которые подчеркнут вашу уверенность и стиль.
Как правильно выбрать тактичные штаны, и какие модели стоит обратить внимание.
Тактичные штаны: идеальное сочетание стиля и практичности, для стильного и практичного образа.
Какие материалы лучше всего подойдут для тактичных штанов, и какие модели стоит выбрать для уникального стиля.
тактичні зимові штани чоловічі https://vijskovitaktichnishtanu.kiev.ua/ .
ฉันจำเป็นต้องกล่าวว่า บทความนี้ให้ข้อมูลที่มีประโยชน์มากมายเกี่ยวกับ คาสิโนออนไลน์
ฟรี! ฉันเองเป็นอีกคนหนึ่งที่ชอบด้านการเล่นเกมและเดิมพันออนไลน์ เพราะมันสบายรวมทั้งสามารถเล่นได้ทุกหนทุกแห่ง ทั้งยังยังมีเกมให้เลือกหลากหลาย ตั้งแต่เกมสสล็อต รูเล็ต คืออะไร ไปจนถึงโป๊กเกอร์ บล็อกนี้ช่วยทำให้ฉันเข้าใจถึงการเลือกเว็บคาสิโนออนไลน์ บาคาร่า เสือมังกรที่น่าไว้ใจ แล้วก็การดูแลเรื่องความปลอดภัยสำหรับเพื่อการเล่นมากเพิ่มขึ้น ขอบคุณในการแบ่งปันข้อมูลดีๆอย่างงี้ค่ะ!
Can I Play the Aviator Game on Mobile?
aviator game
jasminer
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом железнодорожника, купить диплом в смоленске, купить диплом в новочебоксарске, купить диплом архитектора, купить диплом в зеленодольске. Постепенно углубляясь, нашел отличный ресурс здесь: http://frank-shkola.ru/forum/messages/forum1/topic245/message248/?result=new
http://paning.flybb.ru/topic778.html
https://forum.thelostkeepers.ru/index.php?/gallery/image/347-%D0%B3%D0%BB%D0%B0%D0%B2%D0%BD%D1%8B%D0%B5-%D0%BF%D1%80%D0%B8%D1%87%D0%B8%D0%BD%D1%8B-%D0%B8%D0%B7-%D0%B7%D0%B0-%D1%87%D0%B5%D0%B3%D0%BE-%D0%BC%D0%BD%D0%BE%D0%B3%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D1%8E%D1%82-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B/
http://toby.bestbb.ru/viewtopic.php?id=305
http://peaceofficial.5nx.ru/viewtopic.php?f=111&t=730
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
jasminer
jasminer
live sex chat video
Nude hot cams woman live sex showNude amateur cams b65d57a
jasminer
jasminer
jasminer
jasminer
Как выбрать лучшую клинику стоматологии, советуем.
Современные технологии в стоматологии, профессиональный уход за зубами.
Как избежать боли при лечении зубов, предлагаем.
Самые популярные заблуждения о зубах, эффективные советы стоматолога.
Секреты крепких и белоснежных зубов, ознакомиться.
Лечение зубов без боли: реальность или миф?, качественные методики стоматологии.
Как избежать неприятного запаха изо рта, ознакомиться.
стоматологія кабінет https://klinikasuchasnoistomatologii.vn.ua/ .
jasminer
конференционный зал http://oborudovanie-konferenc-zalov11.ru .
video chat live sex
Nude hot cams modeNaked hot webcams girls live sex show d5_9999
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом тренера, где купить диплом образование, купить диплом в ростове-на-дону, купить диплом фармацевта, купить диплом товароведа. Постепенно углубляясь, нашел отличный ресурс здесь: https://lada-clubs.ru/gallery/image/633-pochemu-seychas-mnogie-lyudi-zakazyvayut-diplomy-i-attestaty/
http://ekb.bestbb.ru/viewtopic.php?id=564
http://next.bestbb.ru/viewtopic.php?id=268
https://rcdrift.ru/forum/member.php?u=21074
http://most.maxbb.ru/topic494.html
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
jasminer
jasminer
Повышайте свои шансы на победу в 1win казино
1win скачать https://xn—-7sbb2afcierdfbl.xn--90ais/ .
winnings.
aviator game
Столешницы, барные стойки, подоконники и другие изделия из искусственного камня от производителя мебели из камня “Акрилиум” https://worldgonesour.ru/novosti/36670-kak-vybrat-stoleshnicu-iz-iskusstvennogo-kamnya-7-poleznyh-sovetov.html
jasminer
jasminer
sex video chat live videos absolutely free and easy to watch on any device, just
Naked hot webcams gNude hot webcams wo fee0b6b
jasminer
jasminer
Male nurses had a long
Review my blog … Latosha
Romelu Menama Lukaku Bolingoli https://romelulukaku.prostoprosport-br.com Futebolista belga, atacante do clube ingles Chelsea e da selecao belga . Por emprestimo, ele joga pelo clube italiano Roma.
jasminer
There is on thhe web gambling in NY for casino players,
but as points stand this is only with social casinos.
Feel free to visit my homepage – 토토모아
Roberto Carlos da Silva Rocha https://roberto-carlos.prostoprosport-br.com Brazilian footballer, left back. He was also capable of playing as both a central defender and a defensive midfielder. World champion 2002, silver medalist at the 1998 World Championships.
jasminer
Nice articl! Just check indian sex cam this out!
Naked hot webcams wNaked amateur webcams girls live sex show 5812fb1
Выберите стильные тактичные штаны для повседневной носки, сделанные из качественных материалов.
Новинки в мире тактичной одежды: лучшие штаны, которые подчеркнут вашу уверенность и стиль.
Как правильно выбрать тактичные штаны, и какие модели стоит обратить внимание.
Выберите удобные тактичные штаны для своего гардероба, и какие модели актуальны в этом сезоне.
Идеальные тактичные штаны для похода на природу, и какие модели стоит выбрать для уникального стиля.
купити тактичні штани https://vijskovitaktichnishtanu.kiev.ua/ .
Strategies and Tips
aviator game
jasminer
jasminer
Идеальные тактичные штаны для любого случая, которые подчеркнут вашу индивидуальность.
Новинки в мире тактичной одежды: лучшие штаны, сделанные для вашего комфорта.
Советы по выбору тактичных штанов, чтобы выглядеть стильно в любой ситуации.
Выберите удобные тактичные штаны для своего гардероба, сделанные для динамичного образа жизни.
Идеальные тактичные штаны для похода на природу, для максимального комфорта в походе.
тактичні штани https://vijskovitaktichnishtanu.kiev.ua/ .
jasminer
Neymar da Silva Santos Junior https://neymar.prostoprosport-br.com e um futebolista brasileiro que atua como atacante, ponta e atacante. meio-campista do clube saudita Al-Hilal e da selecao brasileira. Considerado um dos melhores jogadores do mundo. O maior artilheiro da historia da Selecao Brasileira.
Thomas Mueller https://thomasmueller.prostoprosport-br.com is a German football player who plays for the German Bayern Munich. Can play in different positions – striker, attacking midfielder. The most titled German footballer in history
Идеальные тактичные штаны для любого случая, которые подчеркнут вашу индивидуальность.
Тактичные штаны: модные тренды этого сезона, сделанные для вашего комфорта.
Советы по выбору тактичных штанов, и какие модели стоит обратить внимание.
Выберите удобные тактичные штаны для своего гардероба, для стильного и практичного образа.
Какие материалы лучше всего подойдут для тактичных штанов, и какие модели стоит выбрать для уникального стиля.
військові тактичні штани військові тактичні штани .
sex live chats absolutely free and easy to watch on any device, just
Nude hot cams modeNaked hot webcams w e0b6b69
Kylian Mbappe is a French professional footballer who plays as a forward for Paris Saint-Germain and the French national team. Renowned for his speed, dribbling, and finishing, Mbappe has won numerous titles, including multiple Ligue 1 championships and the FIFA World Cup in 2018. Find out more about him here – https://kylianmbappe.paris-saint-germain-ar.com/
Выберите стильные тактичные штаны для повседневной носки, для идеального комфорта и функциональности.
Тактичные штаны: модные тренды этого сезона, сделанные для вашего комфорта.
Советы по выбору тактичных штанов, и какие модели стоит обратить внимание.
Какие тактичные штаны подойдут именно вам, и какие модели актуальны в этом сезоне.
Какие материалы лучше всего подойдут для тактичных штанов, и какие модели стоит выбрать для уникального стиля.
тактичні штани чоловічі тактичні штани чоловічі .
back for more.
aviator game
Nice article, thanks! Just check sex toys live cam chat this out.
Naked amateur webcaNaked amateur cams 65d57ad
Jude Victor William Bellingham https://jude-bellingham.prostoprosport-cz.org anglicky fotbalista, zaloznik spanelskeho klubu Real Madrid a anglicky narodni tym. V dubnu 2024 ziskal cenu za prulom roku z Laureus World Sports Awards. Stal se prvnim fotbalistou, ktery ji obdrzel.
Edson Arantes do Nascimento https://pele.prostoprosport-br.com Brazilian footballer, forward (attacking midfielder. Played for Santos clubs) and New York Cosmos. Played 92 matches and scored 77 goals for the Brazilian national team.
says:Just check this out, amateurgang.com for free!
Nude hot cams woman live sex charNaked amateur cams 942dacc
Играйте в бесплатные игровые автоматы онлайн без регистрации и смс на нашем сайте, наслаждайтесь крупными выигрышами и увлекательными играми!
Попробуй свою удачу в 1win казино, становись богаче.
Азартные игры в 1win казино, гарантируют яркие эмоции.
1win казино – место, где рождаются победы, выигрывай и радуйся.
Играй и побеждай вместе с 1win казино, становись миллионером.
1win казино – место, где рождаются победы, воплоти свои мечты в реальность.
Почувствуй адреналин победы в 1win казино, забирай свой джекпот.
1win казино – твой путь к успеху и богатству, в котором ты можешь стать лучшим.
Богатство и успех с 1win казино, сталкивайся с удачей и побеждай.
1win https://luchshiye-onlayn-kazino-rb.com/ .
Erling Breut Haaland https://erling-haaland.prostoprosport-cz.org je norsky fotbalista, ktery hraje jako utocnik za Anglicky klub Manchester City a norska reprezentace. Rekordman anglicke Premier League v poctu golu za sezonu.
Kylian Mbappe Lotten https://kylian-mbappe.prostoprosport-cz.org Francouzsky fotbalista, utocnik Paris Saint-Germain a kapitan tymu francouzskeho tymu. 1. cervence 2024 se stane hracem spanelskeho klubu Real Madrid.
Идеальные тактичные штаны для любого случая, для идеального комфорта и функциональности.
Тактичные штаны: модные тренды этого сезона, сделанные для вашего комфорта.
Советы по выбору тактичных штанов, и какие модели стоит обратить внимание.
Тактичные штаны: идеальное сочетание стиля и практичности, сделанные для динамичного образа жизни.
Идеальные тактичные штаны для похода на природу, и какие модели стоит выбрать для уникального стиля.
чоловічі тактичні штани чоловічі тактичні штани .
free live sex chat cams
Naked hot cams modNude hot webcams mo 65d57ad
I like the valuable info you provide in your articles.
I’ll bookmark your blog and check again here frequently.
I’m quite sure I will learn many new stuff right here! Best of luck for the next!
Наш сервисный центр предлагает профессиональный вызвать мастера по ремонту мфу на выезде всех типов и брендов. Мы осознаем, насколько значимы для вас ваши МФУ, и стремимся предоставить услуги наилучшего качества. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что предоставляет надежность и долговечность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются обладатели многофункциональных принтеров, включают неисправности печатающей головки, неработающий сканер, неисправности программного обеспечения, неисправности разъемов и механические повреждения. Для устранения этих неисправностей наши профессиональные техники оказывают ремонт печатающих головок, сканеров, ПО, разъемов и механических компонентов. Обратившись к нам, вы обеспечиваете себе надежный и долговечный сервисный центр по ремонту мфу рядом.
Подробная информация размещена на сайте: https://remont-mfu-lite.ru
amateur-teen-nude.net videos absolutely free and easy to watch on any device, just
Naked amateur webcaNaked hot webcams model online sex show fb65d57
Harry Kane https://harry-kane.prostoprosport-cz.org dostal pozvanku do anglickeho tymu nezletilych jako prvni cas 17. na turnaj mladeze v Portugalsku. Utocnik se zaroven kvuli vazne nemoci neobjevil na triumfalnim mistrovstvi Evropy muzu do 17 let 2010 pro Brity.
Mohamed Salah https://mohamed-salah.prostoprosport-cz.org je egyptsky fotbalista, ktery hraje jako utocnik za anglictinu. klub Liverpool a egyptsky narodni tym. Povazovan za jednoho z nejlepsich fotbalistu na svete.
Недавно я узнал о классном музыкальном фестивале, который пройдет в соседнем городе. Очень хотелось поехать, но денег на поездку не хватало, а кредитная история у меня была не лучшей. В Яндексе на первом месте нашел Телеграм канал займы мфо новые . Это сразу вызвало доверие. На канале был список малоизвестных займов, которые давали деньги всем по паспорту от 18 лет. Ставки от 0 до 0.8 процента в день – просто супер! Оформив займ за 10 минут, я получил 30 тысяч и смог отправиться на фестиваль. Провел там незабываемое время. Всем советую подписаться на этот канал!
Financial robot is your success formula is found. Learn more about it. https://t.me/cryptaxbot/17?fruttyVet98Bus
Наш сервисный центр предлагает надежный вызвать мастера по ремонту монитора на дому любых брендов и моделей. Мы осознаем, насколько важны для вас ваши экраны, и готовы предложить сервис наилучшего качества. Наши опытные мастера проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что обеспечивает долговечность и надежность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются пользователи дисплеев, включают неисправности подсветки, неисправности матрицы, неисправности программного обеспечения, проблемы с портами и механические повреждения. Для устранения этих неисправностей наши опытные мастера оказывают ремонт подсветки, матриц, ПО, разъемов и механических компонентов. Обратившись к нам, вы получаете качественный и надежный мастер по ремонту монитора рядом.
Подробная информация размещена на сайте: https://remont-monitorov-plus.ru
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-cz.org Belgicky fotbalista, zaloznik Manchesteru klub City” a belgicky narodni tym. Absolvent fotbalovych klubu „Ghent” a „Genk”. V roce 2008 zahajil svou karieru dospelych, debutoval v Genku.
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
Just check this out, one on one sex cams
Nude hot cams womaNaked hot webcams m b1fb65d
Секреты ухода за зубами, предлагаем.
Уникальные методики лечения зубов, качественный уход за зубами.
Эффективные способы обезболивания, изучить.
Мифы о стоматологии, в которые верят все, качественные советы стоматолога.
Как избежать проблем с зубами, советуем.
Лечение зубов без боли: реальность или миф?, качественные методики стоматологии.
Как правильно чистить зубы: секреты здоровой улыбки, предлагаем.
професійна стоматологія професійна стоматологія .
Vinicius Jose Paixan de Oliveira Junior vinicius-junior.prostoprosport-cz.org bezne znamy jako Vinicius Junior je brazilsky a spanelsky fotbalista , utocnik klubu Real Madrid a brazilsky reprezentant.
cash advance bunbury Customers with credit difficulties should seek credit counseling.
На сайте http://koleso-na-hodu.ru каждый желающий получает возможность приобрести шины больших, а также редких размеров с оперативной доставкой по всему городу, области. Непосредственно на сайте у вас получится подобрать шины, исходя из таких параметров, как: ширина, высота профиля, диаметр, стоимость, производитель, сезонность. Вся продукция сертифицированная, качественная, оригинальная. Если остались вопросы, то заполните специальную форму со своими данными, чтобы менеджер перезвонил для уточнения определенных моментов.
На сайте https://best-vendor.ru/product/kabel-avbbshv/ приобретите кабель АВБбШв силовой и с жилой из алюминия, а также изоляцией, шлангом из ПВХ. Вся продукция выполнена из современных материалов, а потому точно не покроется коррозией. В этой компании у вас получится приобрести кабель максимально оперативно и с комфортом. При этом на все конструкции даются гарантии. Установлены привлекательные и честные расценки. Имеются все необходимые микроразмеры, что позволит подобрать вариант в зависимости от предпочтений.
Наша мастерская предлагает надежный мастер по ремонту моноблока адреса всех типов и брендов. Мы понимаем, насколько значимы для вас ваши моноблоки, и обеспечиваем ремонт наилучшего качества. Наши опытные мастера работают быстро и аккуратно, используя только оригинальные запчасти, что гарантирует надежность и долговечность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются пользователи все-в-одном ПК, включают проблемы с жестким диском, проблемы с экраном, ошибки ПО, неисправности разъемов и неисправности системы охлаждения. Для устранения этих неисправностей наши опытные мастера выполняют ремонт жестких дисков, дисплеев, ПО, разъемов и систем охлаждения. Обращаясь в наш сервисный центр, вы получаете долговечный и надежный вызвать мастера по ремонту моноблока на дому.
Подробная информация доступна на сайте: https://remont-monoblokov-rial.ru
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в перми, купить диплом в азове, купить диплом в бийске, купить диплом в астрахани, купить диплом в нижневартовске, постепенно вникая в суть дела нашел отличный материал здесь http://mega-zaim96.ru/forum/user/34558/
http://sergei-cheremushkin.blogspot.com/2010/03/blog-post.html
https://myarabis.ru/blog/mbui-dramaticheskij-teatr-g-tynda/#comment_74705
http://lenmontov.blogspot.com/2015/03/blog-post_16.html
http://fatcow.com/blog/?p=344#comment-3680335
и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Успехов в учебе!
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в муроме, купить диплом в нижнекамске, купить диплом агронома, купить диплом сварщика, где купить диплом о среднем образование, потом попал на https://krushwatch.ru/products/anne-klein-3775-svrt/#comment_3438 и там решили все мои учебные заботы!
Успешной учебы!
says:Just check this out, live free sex cams for free!
Naked hot webcams gNaked amateur webcams girls live sex char 1fb65d5
Lionel Messi https://lionel-messi.prostoprosport-cz.org je argentinsky fotbalista, utocnik a kapitan klubu MLS Inter Miami. , kapitan argentinske reprezentace. Mistr sveta, vitez Jizni Ameriky, vitez finale, olympijsky vitez. Povazovan za jednoho z nejlepsich fotbalistu vsech dob.
Bernardo Silva https://bernardo-silva.prostoprosport-cz.org Portugalsky fotbalista, zaloznik. Narozen 10. srpna 1994 v Lisabonu. Silva je povazovan za jednoho z nejlepsich utocnych zalozniku na svete. Fotbalista je povestny svou vytrvalosti a vykonem.
Antoine Griezmann https://antoine-griezmann.prostoprosport-cz.org Francouzsky fotbalista, utocnik a zaloznik za Atletico de Madrid. Hrac a vicekapitan francouzskeho narodniho tymu, clen tymu – mistr sveta 2018 Stribrny medailista z mistrovstvi Evropy 2016 a mistrovstvi sveta 2022.
Как выбрать материал для перетяжки мебели: советы и рекомендации, которые помогут вам сделать правильный выбор.
Горячие тенденции в мире перетяжки мебели: эксклюзивные идеи для дома, которые поразят ваших гостей.
Перетяжка мебели своими руками: идеи для творческого подхода, которые придадут вашему дому неповторимый шарм.
Зачем стоит обратить внимание на перетяжку мебели: основные преимущества и выгоды, которые вы оцените с первого взгляда.
Как выбрать подходящего мастера для перетяжки мебели: советы и рекомендации, для успешного завершения вашего проекта.
Как создать современный интерьер с помощью перетяжки мебели: минималистический подход, для оформления вашего дома в едином стиле.
Секреты перетяжки мебели в скандинавском стиле: как создать атмосферу комфорта, для оформления вашего интерьера в скандинавском духе.
Почему перетяжка мебели является отличным способом экономии: выгодно и стильно, для экономии бюджета и создания стильного дизайна.
Какие расцветки выбрать для перетяжки мебели в провансальском стиле: нежные и пастельные оттенки, которые принесут в ваш дом атмосферу тепла и ностальгии.
Как создать интерьер высокого класса с помощью перетяжки мебели: роскошный подход, для оформления вашего интерьера в стиле элегантности.
Профессиональные секреты перетяжки мебели: как сделать работу максимально эффективной, для успешной реализации вашего проекта и получения отличного результата.
перетяжка мебели в минске перетяжка мебели в минске .
Robert Lewandowski https://robert-lewandowski.prostoprosport-cz.org je polsky fotbalista, utocnik spanelskeho klubu Barcelona a kapitan polskeho narodniho tymu. Povazovan za jednoho z nejlepsich utocniku na svete. Rytir krize velitele polskeho renesancniho radu.
Наши специалисты предлагает высококачественный отремонтировать моноколесо рядом всех типов и брендов. Мы осознаем, насколько необходимы вам ваши моноколеса, и стремимся предоставить услуги первоклассного уровня. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что гарантирует долговечность и надежность проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются владельцы моноколес, включают проблемы с батареей, неисправности двигателя, сбои контроллера, проблемы с гиросенсорами и поломки корпуса. Для устранения этих поломок наши опытные мастера выполняют ремонт батарей, двигателей, контроллеров, гиросенсоров и механических компонентов. Обратившись к нам, вы гарантируете себе качественный и надежный ремонт моноколеса рядом.
Подробная информация размещена на сайте: https://remont-monokoles-serv.ru
Nice article, thanks! Just check live free sex chat this out.
Nude amateur camsNude amateur webcam cc5812f
Discover the best black sex cam
and communitysexy.net ever!
Nude hot webcams woNude amateur webcam 7ad7_37
Наш сервисный центр предлагает профессиональный центр ремонта морозильных камер с гарантией любых брендов и моделей. Мы знаем, насколько необходимы вам ваши морозильники, и стремимся предоставить услуги первоклассного уровня. Наши квалифицированные специалисты работают быстро и аккуратно, используя только качественные детали, что предоставляет надежность и долговечность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются пользователи морозильников, включают неисправности компрессора, проблемы с температурным датчиком, программные сбои, проблемы с подключением и поломки корпуса. Для устранения этих проблем наши опытные мастера выполняют ремонт компрессоров, термостатов, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы обеспечиваете себе долговечный и надежный сервисный ремонт морозильной камеры на выезде.
Подробная информация доступна на сайте: https://remont-morozilnyh-kamer-spec.ru
jasminer
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом о среднем образовании, купить диплом физика, купить диплом в кирове, купить диплом в нефтекамске, купить диплом в саранске, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://greenbaxna.com/profile/dpplommccoomamect/
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Удачи!
https://crazyamateurporn.com absolutely free and easy to watch on any device, just
Naked amateur webcaNude amateur webcam bfee0b6
You’re the best, I just ran across your weblog and wanted to say that I’ve truly enjoyed browsing your blog posts. I have subscribed to your feed and I hope you write again very soon!
고소득알바
jasminer
jasminer
Наши специалисты предлагает надежный вызвать мастера по ремонту ноутбука адреса любых брендов и моделей. Мы знаем, насколько важны для вас ваши переносные компьютеры, и готовы предложить сервис наилучшего качества. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что обеспечивает длительную работу проведенных ремонтов.
Наиболее частые неисправности, с которыми сталкиваются владельцы ноутбуков, включают поломку жесткого диска, неисправности экрана, неисправности программного обеспечения, проблемы с портами и проблемы с охлаждением. Для устранения этих неисправностей наши квалифицированные специалисты оказывают ремонт жестких дисков, экранов, ПО, разъемов и систем охлаждения. Обращаясь в наш сервисный центр, вы обеспечиваете себе качественный и надежный центр ремонта ноутбуков в москве.
Подробная информация доступна на сайте: https://remont-noutbukov-first.ru
jasminer
Regulated sports books use encryption of sensitive information (this suggests
the url begins with https, not http).
Feel free to surf to my web page; craigrice.Com
Just check this out, indian sex cam
Nude hot webcams woman online porn showNude hot cams girl ad4_1ab
see this website forgot tronlink password
Индивидуалки Тюмень
Mountain cabins in Montenegro – Iznajmljivanje koliba na Durmitoru, Iznajmljivanje vikendica sa dakuzijem
The arguments in this article were very well-presented. I appreciate the depth of analysis. It would be interesting to hear how others interpret these points. What do you think?
jasminer
jasminer
Наш сервисный центр предлагает надежный сервисный центр по ремонту объективов в москве различных марок и моделей. Мы знаем, насколько важны для вас ваши фотообъективы, и обеспечиваем ремонт высочайшего уровня. Наши профессиональные техники работают быстро и аккуратно, используя только сертифицированные компоненты, что обеспечивает долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются пользователи линз, включают неисправности фокуса, залипшую диафрагму, повреждения корпуса, неисправности автофокуса и загрязнения линз. Для устранения этих проблем наши опытные мастера оказывают ремонт фокусировки, диафрагмы, автофокуса, очистку линз и восстановление корпуса. Обратившись к нам, вы обеспечиваете себе качественный и надежный центр ремонта объективов с гарантией.
Подробная информация доступна на сайте: https://remont-obektivov-magic.ru
Nice article, thanks! Just check https://elitdmodels.com this out.
Nude amateur camsNude amateur cams c5812fb
Hello it’s me, I am also visiting this web site on a regular basis,
this website is actually fastidious and the people are actually sharing good thoughts.
Take a look at my webpage rijbewijs kopen betrouwbaar
Pablo Martin Paez Gavira https://gavi.prostoprosport-cz.org Spanelsky fotbalista, zaloznik barcelonskeho klubu a spanelske reprezentace. Povazovan za jednoho z nejtalentovanejsich hracu sve generace. Ucastnik mistrovstvi sveta 2022. Vitez Ligy narodu UEFA 2022/23
Luka Modric https://luka-modric.prostoprosport-cz.org je chorvatsky fotbalista, stredni zaloznik a kapitan spanelskeho tymu. klub Real Madrid, kapitan chorvatskeho narodniho tymu. Uznavan jako jeden z nejlepsich zalozniku nasi doby. Rytir Radu prince Branimira. Rekordman chorvatske reprezentace v poctu odehranych zapasu.
Son Heung Min https://son-heung-min.prostoprosport-cz.org Jihokorejsky fotbalista, utocnik a kapitan anglickeho klubu Premier League Tottenham Hotspur a narodniho tymu Korejske republiky. V roce 2022 vyhral Zlatou kopacku Premier League.
Cristiano Ronaldo https://cristiano-ronaldo.prostoprosport-cz.org je portugalsky fotbalista, utocnik, kapitan Saudske Arabie klubu An-Nasr a portugalskeho narodniho tymu. Mistr Evropy. Povazovan za jednoho z nejlepsich fotbalistu vsech dob. Nejlepsi strelec v historii fotbalu podle IFFIS a ctvrty podle RSSSF
hello!,I really like your writing very so much! share we communicate more
about your post on AOL? I need a specialist on this area to unravel my
problem. Maybe that is you! Taking a look ahead to peer you.
My website – movie pit sofa
jasminer
jasminer
company website Flstudio download
More about the author galaxy swapper download
Just check this out, cam sex live
Nude hot webcams giNude amateur cams woman live sex show 12fb1fb
jasminer
Fantastic post but I was wondering if you could write a
litte more on this topic? I’d be very grateful if you could elaborate a little bit
further. Many thanks!
Feel free to visit my web-site … energy healing courses
Наш сервисный центр предлагает надежный сервисный ремонт парогенераторов на выезде различных марок и моделей. Мы знаем, насколько важны для вас ваши устройства для генерации пара, и готовы предложить сервис наилучшего качества. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что обеспечивает надежность и долговечность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются владельцы парогенераторов, включают неисправности нагревательных элементов, неработающий насос, ошибки ПО, неисправности разъемов и механические повреждения. Для устранения этих проблем наши квалифицированные специалисты выполняют ремонт нагревательных элементов, насосов, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы обеспечиваете себе качественный и надежный официальный ремонт парогенератора рядом.
Подробная информация доступна на сайте: https://remont-parogeneratorov-piece.ru
Thanks for sharing your thoughts about best energy healing classes healing courses online.
Regards
jasminer
Web Site Pal world download
jasminer
cam sex videos absolutely free and easy to watch on any device, just
Nude hot cams girlNaked amateur webca c5812fb
Pedro Gonzalez Lopez https://pedri.prostoprosport-cz.org lepe znamy jako Pedri, je spanelsky fotbalista, ktery hraje jako utocny zaloznik. za Barcelonu a spanelskou reprezentaci. Bronzovy medailista z mistrovstvi Evropy 2020 a zaroven nejlepsi mlady hrac tohoto turnaje.
Normally I do not read article on blogs, but I wish to say
that this write-up very forced me to check out and do it!
Your writing taste has been surprised me. Thanks, very great post.
Feel free to surf to my blog: Kids Books
Alison Ramses Becker https://alisson-becker.prostoprosport-cz.org Brazilsky fotbalista nemeckeho puvodu, brankar klubu Liverpool a brazilsky narodni tym. Je povazovan za jednoho z nejlepsich brankaru sve generace a je znamy svymi vynikajicimi zakroky, presnosti prihravek a schopnosti jeden na jednoho.
Karim Benzema https://karim-benzema.prostoprosport-cz.org je francouzsky fotbalista, ktery hraje jako utocnik za Saudskou Arabii. Arabsky klub Al-Ittihad. Hral za francouzsky narodni tym, za ktery odehral 97 zapasu a vstrelil 37 branek. V 17 letech se stal jednim z nejlepsich hracu rezervy, nastrilel tri desitky golu za sezonu.
Rodrigo Silva de Goiz https://rodrygo.prostoprosport-cz.org Brazilsky fotbalista, utocnik Realu Madrid a brazilskeho narodniho tymu. V breznu 2017 byl Rodrigo povolan do narodniho tymu Brazilie U17 na zapasy Montague Tournament.
I read this piece of writing completely about the difference
of most up-to-date and earlier technologies, it’s amazing article.
Take a look at my blog post – Computer Safety Kids
Наши специалисты предлагает профессиональный мастерская по ремонту планшетов в москве любых брендов и моделей. Мы осознаем, насколько значимы для вас ваши устройства планшетного типа, и обеспечиваем ремонт наилучшего качества. Наши квалифицированные специалисты работают быстро и аккуратно, используя только качественные детали, что гарантирует длительную работу выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются владельцы планшетов, включают неисправности дисплея, неисправности аккумулятора, программные сбои, проблемы с портами и поломки корпуса. Для устранения этих проблем наши профессиональные техники проводят ремонт экранов, батарей, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы обеспечиваете себе надежный и долговечный отремонтировать планшет адреса.
Подробная информация размещена на сайте: https://remont-planshetov-profi.ru
says:Just check this out, http://www.freeshemalesource.com for free!
Naked hot webcams model live porn charNaked amateur webca 7ad5_2a
Thibaut Nicolas Marc Courtois https://thibaut-courtois.prostoprosport-cz.org Belgicky fotbalista, brankar spanelskeho klubu Real Madrid . V sezone 2010/11 byl uznan jako nejlepsi brankar v belgicke Pro League a take hrac roku pro Genk. Trojnasobny vitez Ricardo Zamora Trophy
Nice article, thanks! Just check web cam sex this out.
Naked hot webcams gNaked hot cams model online sex show 7ad8_91
Virgil van Dijk https://virgil-van-dijk.prostoprosport-cz.org Nizozemsky fotbalista, stredni obrance, kapitan anglickeho klubu Liverpool a kapitan nizozemskeho narodniho tymu.
Bruno Guimaraes Rodriguez Moura https://bruno-guimaraes.prostoprosport-cz.org Brazilsky fotbalista, defenzivni zaloznik Newcastlu United a Brazilsky narodni tym. Vitez olympijskych her 2020 v Tokiu.
Toni Kroos https://toni-kroos.prostoprosport-cz.org je nemecky fotbalista, ktery hraje jako stredni zaloznik za Real Madrid a nemecky narodni tym. Mistr sveta 2014. Prvni nemecky hrac v historii, ktery sestkrat vyhral Ligu mistru UEFA.
blacksprut даркнет – blacksprut даркнет, блек спрут оригинальная ссылка
Наш сервисный центр предлагает профессиональный центр ремонта плоттера рядом любых брендов и моделей. Мы осознаем, насколько важны для вас ваши графопостроители, и стремимся предоставить услуги наилучшего качества. Наши квалифицированные специалисты работают быстро и аккуратно, используя только оригинальные запчасти, что обеспечивает долговечность и надежность выполненных работ.s
Наиболее общие проблемы, с которыми сталкиваются владельцы плоттеров, включают неработающий картридж, проблемы с подачей бумаги, неисправности программного обеспечения, неработающие разъемы и механические повреждения. Для устранения этих проблем наши квалифицированные специалисты проводят ремонт печатающих головок, механизмов подачи бумаги, ПО, разъемов и механических компонентов. Обратившись к нам, вы получаете долговечный и надежный мастер по ремонту плоттеров адреса.
Подробная информация размещена на сайте: https://remont-plotterov-style.ru
This is my first time visit at here and i am actually pleassant to read everthing at
alone place.
When someone writes an piece of writing he/she maintains the image of a user
in his/her brain that how a user can be
aware of it. Therefore that’s why this piece of writing is outstdanding.
Thanks! https://wolvesbaneuo.com/wiki/index.php/Comment_Un_Optom%C3%83_triste_Effectue_Un_Examen_De_La_Vue
Discover the best indian live sex chat
and sex cam live ever!
Naked amateur webcams woman live sex showNaked amateur webcams girls online sex char c5812fb
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом в камышине, купить диплом специалиста, купить диплом в каспийске, купить диплом техникума, #купить диплом хореографа, а затем переключился на дипломы вузов. Подробности здесь: https://jeepgarage.ru/forum/topic.php?forum=24&topic=703
http://www.forum.7x.ru/member.php?u=16498
http://c90226sl.beget.tech/2024/06/17/diplomy-s-polnoj-garantiej/
http://gti-club.ru/forum/member.php?u=23001
http://masterflower.listbb.ru/viewtopic.php?f=6&t=294
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успешной учебы!
На сайте https://best-vendor.ru/product/kabel-vbbshv/ приобретите кабель ВБбШв с медной жилой, изоляцией, а также защитным шлангом, который произведен из ПВХ. Используется для того, чтобы перераспределить энергию в электрических установках. Прямо сейчас вы сможете приобрести все необходимое оптом и в любом количестве, по доступной стоимости. Предоставляются гарантии качества. Совершите приобретение прямо сейчас. В наличии огромное количество различных размеров. На кабель действуют предложения круглогодично.
2fa blacksprut – блек спрут онион, блек спрут оригинальная ссылка
파워 슬롯
이것은 모두가 관심을 갖고 왕 부시를 간절히 바라 보는 것입니다.
видеостена купить москва видеостена купить москва .
Привет!
Для многих людей, купить диплом ВУЗа – это необходимость, возможность получить выгодную работу. Впрочем для кого-то – это желание не терять время на учебу в ВУЗе. Что бы ни толкнуло вас на такой шаг, мы готовы помочь вам. Максимально быстро, качественно и недорого сделаем диплом нового или старого образца на государственных бланках со всеми требуемыми подписями и печатями.
Наши специалисты предлагают быстро и выгодно приобрести диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Данный документ пройдет лубую проверку, даже при помощи специфических приборов. Решите свои задачи быстро и просто с нашей компанией.
Превосходства наших дипломов:
• используются только настоящие бланки “Гознак”;
• оригинальные подписи должностных лиц;
• настоящие печати университета;
• специальные водяные знаки, нити и иные степени защиты;
• идеальное качество оформления – ошибки полностью исключены;
• любая проверка оригинальности документа.
Где приобрести диплом специалиста?
http://forum.bestgamer.ru/newthread.php?do=postthread&f=88
Удачи!
Добрый день!
Для определенных людей, купить диплом ВУЗа – это острая необходимость, уникальный шанс получить достойную работу. Однако для кого-то – это желание не терять огромное количество времени на учебу в ВУЗе. Что бы ни толкнуло вас на такое решение, наша фирма готова помочь. Оперативно, профессионально и недорого изготовим документ любого ВУЗа и любого года выпуска на государственных бланках со всеми необходимыми печатями.
Заказать документ о получении высшего образования можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы СССР. Даем 100% гарантию, что в случае проверки документа работодателями, никаких подозрений не возникнет.
Превосходства наших дипломов:
• используются только фирменные бланки “Гознака”;
• подлинные подписи должностных лиц;
• мокрые печати ВУЗа;
• специальные водяные знаки, нити и прочие степени защиты;
• идеальное заполнение и оформление – ошибок не будет;
• любая проверка документа.
Наша компания предлагает максимально быстро купить диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями. Документ способен пройти лубую проверку, даже при использовании профессионального оборудования. Решите свои задачи максимально быстро с нашей компанией.
Где купить диплом специалиста?
http://pornodrochka.club/index.php?subaction=userinfo&user=olowypu
https://medbereg.ru/communication/forum/user/1707/
http://www.superstitionism.com/forum/profile.php?id=1393264
http://mockwa.com/forum/thread-151192/
http://www.detskiy-mir.net/index.php?subaction=userinfo&user=ebyvizedy
Удачи!
Toni Kroos https://toni-kroos.prostoprosport-cz.org je nemecky fotbalista, ktery hraje jako stredni zaloznik za Real Madrid a nemecky narodni tym. Mistr sveta 2014. Prvni nemecky hrac v historii, ktery sestkrat vyhral Ligu mistru UEFA.
Darwin Gabriel Nunez Ribeiro https://darwin-nunez.prostoprosport-cz.org Uruguaysky fotbalista, utocnik anglickeho klubu Liverpool a Uruguaysky narodni tym. Bronzovy medailista mistrovstvi Jizni Ameriky mezi mladeznickymi tymy.
Romelu Menama Lukaku Bolingoli https://romelu-lukaku.prostoprosport-cz.org Belgicky fotbalista, utocnik anglickeho klubu Chelsea a Belgican vyber. Na hostovani hraje za italsky klub Roma.
Наша мастерская предлагает высококачественный вызвать мастера по ремонту приборов ночного видения на дому любых брендов и моделей. Мы понимаем, насколько необходимы вам ваши ПНВ, и обеспечиваем ремонт высочайшего уровня. Наши опытные мастера работают быстро и аккуратно, используя только сертифицированные компоненты, что гарантирует надежность и долговечность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются пользователи устройств ночного видения, включают проблемы с изображением, поврежденные линзы, программные сбои, неработающие разъемы и поломки компонентов. Для устранения этих поломок наши профессиональные техники оказывают ремонт сенсоров, оптики, ПО, разъемов и механических компонентов. Обратившись к нам, вы гарантируете себе надежный и долговечный отремонтировать пнв с гарантией.
Подробная информация доступна на сайте: https://remont-pnv-ultra.ru
Just check this out, free sex web cam
Nude hot webcams woman online porn charNude amateur cams 7ad0_ea
https://blacksprut-sait.top/ – blacksprut onion, блэкспрут сайт
Don’t Let Local Expenses Slow You Down. Get a 24 Hour Loan Available Now in (Zip Code Area)! Take away the uncertainty with detailed answers above that might help you sway from one decision to the other!
jasminer
блек спрут оригинальная ссылка – спрут как попасть на сайт, 2fa blacksprut
Excellent and high-quality indian professor hidden cam sex scandal absolutely free and easy to watch on any device, just
Naked hot webcams gNaked hot cams gir d4_a9d1
Наши специалисты предлагает высококачественный сервисный центр по ремонту посудомоечной машины на выезде всех типов и брендов. Мы понимаем, насколько важны для вас ваши посудомоечные машины, и готовы предложить сервис первоклассного уровня. Наши опытные мастера работают быстро и аккуратно, используя только оригинальные запчасти, что обеспечивает надежность и долговечность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются пользователи посудомоек, включают проблемы с температурными датчиками, неработающие насосы, программные сбои, неработающие разъемы и механические повреждения. Для устранения этих неисправностей наши квалифицированные специалисты оказывают ремонт нагревательных элементов, насосов, ПО, разъемов и механических компонентов. Обратившись к нам, вы гарантируете себе надежный и долговечный центр ремонта посудомоечных машин на выезде.
Подробная информация доступна на сайте: https://remont-posudomoechnyh-mashin-expert.ru
On line casino gambling is also now legal in Rhode Island,
but the market is not set to launch till April 2024.
Look into my web page :: Eco-friendly
Наша мастерская предлагает профессиональный мастерская по ремонту принтера в москве любых брендов и моделей. Мы понимаем, насколько важны для вас ваши устройства для печати, и обеспечиваем ремонт наилучшего качества. Наши квалифицированные специалисты работают быстро и аккуратно, используя только сертифицированные компоненты, что гарантирует надежность и долговечность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются пользователи печатающих устройств, включают неисправности печатающей головки, неисправности механизма подачи, ошибки ПО, неработающие разъемы и поломки компонентов. Для устранения этих поломок наши опытные мастера проводят ремонт печатающих головок, механизмов подачи бумаги, ПО, разъемов и механических компонентов. Обратившись к нам, вы гарантируете себе качественный и надежный ремонт принтера с гарантией.
Подробная информация доступна на сайте: https://remont-printerov-master.ru
free live sex chat cams absolutely free and easy to watch on any device, just
Naked hot cams modNude amateur webcam d6_3641
старые проститутки москвы https://prostitutki-213.ru
buy tiktok followers and likes https://tiktok-followers-buy.com
buy 1000 followers on tiktok tiktok followers buy
Наши специалисты предлагает профессиональный мастерская по ремонту проектора адреса различных марок и моделей. Мы осознаем, насколько важны для вас ваши видеопроекторы, и готовы предложить сервис первоклассного уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что обеспечивает долговечность и надежность проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются обладатели видеопроекторов, включают проблемы с лампой, перегрев, неисправности программного обеспечения, неисправности разъемов и поломки компонентов. Для устранения этих проблем наши квалифицированные специалисты оказывают ремонт ламп, вентиляторов, ПО, разъемов и механических компонентов. Обратившись к нам, вы получаете качественный и надежный отремонтировать проектор с гарантией.
Подробная информация размещена на сайте: https://remont-proektorov-online.ru
отчаянные домохозяйки 1 онлайн https://domohozyayki-serial.ru
igirls.space absolutely free and easy to watch on any device, just
Nude hot cams girls online sex charNude hot cams girl cc5812f
Safety Council resolutions that have imposed punishing sanctions on the North for its past banned weapons tests.
My page: Buy
Наша мастерская предлагает надежный ремонт роботов пылесосов на выезде всех типов и брендов. Мы понимаем, насколько значимы для вас ваши автоматические пылесосы, и обеспечиваем ремонт наилучшего качества. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что предоставляет долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются пользователи роботизированных уборщиков, включают поломку аккумулятора, неработающий двигатель, неисправности программного обеспечения, неработающие датчики и повреждения корпуса. Для устранения этих проблем наши опытные мастера проводят ремонт батарей, двигателей, ПО, сенсоров и механических компонентов. Обратившись к нам, вы обеспечиваете себе качественный и надежный отремонтировать робот пылесос с гарантией.
Подробная информация размещена на сайте: https://remont-robotov-pylesosov-servis.ru
Сервера ла2
anal threesome https://incrack.pro
Naked hot webcams mNude hot cams mode b6b6942
Сервера л2
kms activatorwindows 10
https://about-free-forum.suomiblog.com/kms-auto-activator-explanation-download-link-hyperlink-windowsprocess-43217587
free download id9qf0915
Kms auto activator 42dacc5
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в улан-удэ, купить диплом в новочебоксарске, купить диплом в новокузнецке, купить диплом в красноярске , купить сертификат специалиста и получил базовые знания. В итоге остановился на материале: http://army.clanfm.ru/viewtopic.php?f=2&t=38201
Хорошей учебы!
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом кандидата наук, купить диплом в новочеркасске, купить диплом в иркутске, купить диплом в рыбинске, купить диплом для иностранцев, а потом наткнулся на https://lamaria.gov.co/beatriz-eugenia-campillo-velez
https://www.ocf.berkeley.edu/~paultkim/whos-watching-what-you-are-reading
http://www.altasugar.it/new/index.php?option=com_kunena&view=topic&catid=3&id=71645&Itemid=151
http://truongvietducthainguyen.edu.vn/index.php?language=vi&nv=statistics&nvvithemever=t&nv_redirect=aHR0cHM6Ly9hZGlzZ3J1bnRsZWRyZXB1YmxpY2FuLmNvbQ
https://sovavtoprom.ru/wiki/index.php/??????_??????:_???_????????????????_????_??????????_?????!
, где все мои учебные проблемы были решены!
Хорошей учебы!
вход Rio Bet Casino Rio Bet
Привет!
Для определенных людей, приобрести диплом о высшем образовании – это острая необходимость, возможность получить выгодную работу. Но для кого-то – это желание не терять время на учебу в универе. С какой бы целью вам это не потребовалось, наша фирма готова помочь. Оперативно, качественно и недорого сделаем документ любого ВУЗа и года выпуска на подлинных бланках со всеми необходимыми печатями.
Приобрести документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов России. Вы получите диплом по любым специальностям, включая документы образца СССР. Гарантируем, что при проверке документов работодателями, подозрений не возникнет.
Преимущества наших дипломов:
• используются лишь качественные бланки “Гознак”;
• все подписи должностных лиц;
• все печати учебного заведения;
• водяные знаки, нити и прочие степени защиты;
• идеальное заполнение и оформление – ошибки исключены;
• любые проверки оригинальности документа.
Наша компания предлагает быстро и выгодно купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Диплом пройдет любые проверки, даже с применением специально предназначенного оборудования. Достигайте своих целей максимально быстро с нашими дипломами.
Где заказать диплом по необходимой специальности?
https://chrstms.ru/club/user/11503/blog/9571/
Успешной учебы!
Привет, друзья!
Для определенных людей, купить диплом о высшем образовании – это необходимость, шанс получить достойную работу. Но для кого-то – это очевидное желание не терять время на учебу в ВУЗе. Что бы ни толкнуло вас на такой шаг, наша компания готова помочь вам. Быстро, качественно и недорого изготовим документ нового или старого образца на государственных бланках со всеми требуемыми печатями.
Приобрести документ о получении высшего образования вы сможете в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что в случае проверки документа работодателями, подозрений не появится.
Преимущества наших документов:
• используем настоящие бланки “Гознака”;
• все подписи руководства;
• мокрые печати ВУЗа;
• специальные водяные знаки, нити и другие степени защиты;
• безупречное заполнение и оформление – ошибки исключены;
• любые проверки документов.
Наши специалисты предлагают быстро и выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями официальных лиц. Диплом способен пройти лубую проверку, даже при использовании профессиональных приборов. Достигайте своих целей быстро и просто с нашим сервисом.
Где купить диплом специалиста?
https://inopl.com/blogs/572/%D0%A2%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9F%D0%B5%D1%80%D0%B5%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5-%D0%B2-%D0%BD%D0%B0%D1%88-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD
https://bmw-donbass.ru/gallery/image/642-%D0%B2%D1%8B%D1%81%D0%BE%D0%BA%D0%BE%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B5-%D0%BA%D0%BE%D0%BF%D0%B8%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2-%D1%87%D1%82%D0%BE-%D1%81%D0%BC%D0%BE%D0%B3%D1%83%D1%82-%D0%BF%D1%80%D0%BE%D0%B9%D1%82%D0%B8-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%BA%D1%83/
https://forum.thelostkeepers.ru/index.php?/gallery/image/406-%D0%B7%D0%B0%D1%87%D0%B5%D0%BC-%D0%B2-%D0%BD%D0%B0%D1%88%D0%B5-%D0%B2%D1%80%D0%B5%D0%BC%D1%8F-%D0%BC%D0%BD%D0%BE%D0%B3%D0%B8%D0%B5-%D0%BB%D1%8E%D0%B4%D0%B8-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D1%8E%D1%82-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5/
https://fileua.forum.cool/viewtopic.php?id=6397
http://www.suicide-forum.com/member.php?12290-sonnick84&tab=visitor_messaging
Успехов в учебе!
драгон мани казино официальный сайт драгон мани казино
Большой выбор игровых автоматов, рабочее зеркало сайта https://fartunaplay.ru играть на реальные деньги онлайн
Наши специалисты предлагает профессиональный вызвать мастера по ремонту серверов в москве всех типов и брендов. Мы понимаем, насколько важны для вас ваши серверные устройства, и стремимся предоставить услуги высочайшего уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что гарантирует долговечность и надежность проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются пользователи серверных систем, включают неисправности HDD, неисправности блока питания, неисправности программного обеспечения, неработающие сетевые интерфейсы и поломки компонентов. Для устранения этих проблем наши квалифицированные специалисты оказывают ремонт жестких дисков, блоков питания, ПО, сетевых интерфейсов и компонентов. Обратившись к нам, вы получаете качественный и надежный официальный ремонт сервера на дому.
Подробная информация доступна на сайте: https://remont-serverov-express.ru
Привет!
Для многих людей, купить диплом о высшем образовании – это острая необходимость, уникальный шанс получить достойную работу. Но для кого-то – это очевидное желание не терять множество времени на учебу в универе. Что бы ни толкнуло вас на это решение, мы готовы помочь. Максимально быстро, профессионально и по разумной цене сделаем документ нового или старого образца на подлинных бланках с реальными печатями.
Наши специалисты предлагают выгодно заказать диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями должностных лиц. Документ пройдет любые проверки, даже при использовании специального оборудования. Достигайте свои цели быстро и просто с нашей компанией.
Основные преимущества наших документов:
• используются только настоящие бланки “Гознак”;
• подлинные подписи должностных лиц;
• мокрые печати учебного заведения;
• водяные знаки, нити и иные степени защиты;
• безупречное качество оформления – ошибки полностью исключены;
• любые проверки документа.
Где приобрести диплом по нужной специальности?
http://www.lada-xray.net/member.php?u=2434
Успехов в учебе!
Привет, друзья!
Для многих людей, купить диплом ВУЗа – это острая потребность, удачный шанс получить хорошую работу. Но для кого-то – это очевидное желание не терять время на учебу в институте. Что бы ни толкнуло вас на это решение, наша компания готова помочь вам. Быстро, профессионально и недорого изготовим диплом любого ВУЗа и года выпуска на настоящих бланках с реальными печатями.
Купить документ ВУЗа можно у нас. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любой специальности, включая документы СССР. Гарантируем, что при проверке документа работодателями, никаких подозрений не возникнет.
Плюсы наших дипломов:
• используем настоящие бланки “Гознака”;
• все подписи руководства;
• все печати учебного заведения;
• водяные знаки, нити и другие степени защиты;
• безупречное качество оформления – ошибки исключены;
• любая проверка документов.
Наши специалисты предлагают выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями должностных лиц. Наш документ пройдет лубую проверку, даже при помощи специально предназначенного оборудования. Решите свои задачи быстро и просто с нашим сервисом.
Где купить диплом по необходимой специальности?
http://tatarstan.iastr.ru/index.php?subaction=userinfo&user=ufufal
http://www.icmms.co.kr/bbs/board.php?bo_table=free&wr_id=398395
http://samsoberi.ru/index.php?subaction=userinfo&user=yhuqysif
http://elka54.ru/forum/?PAGE_NAME=profile_view&UID=108146
http://www.dachamania.ru/photo_gallrey/profile.php?uid=57191
Удачи!
Discover the best camaras de sexo en vivo ever for free!
Naked amateur webcaNude amateur webcams model online porn show b6b6942
Качественная и недорогая купить мебель в детскую комнату лучшие цены, доставка и сборка.
Georgia has strict anti-gambling laws, butt these 18 and older
can bet although on cruise ships off the coast.
my page: High-Performance
Find out random sex cam for free 🙂
Nude amateur webcams model online porn showNaked amateur webcams woman online sex char fb1fb65
Наш сервисный центр предлагает надежный сервисный ремонт сетевых хранилищ в москве любых брендов и моделей. Мы знаем, насколько значимы для вас ваши NAS-системы, и обеспечиваем ремонт высочайшего уровня. Наши профессиональные техники работают быстро и аккуратно, используя только оригинальные запчасти, что обеспечивает длительную работу выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются обладатели серверов хранения данных, включают неисправности HDD, неработающий блок питания, неисправности программного обеспечения, неработающие сетевые интерфейсы и неисправности компонентов. Для устранения этих неисправностей наши профессиональные техники оказывают ремонт жестких дисков, блоков питания, ПО, сетевых интерфейсов и компонентов. Обращаясь в наш сервисный центр, вы обеспечиваете себе качественный и надежный ремонт сетевого хранилища в москве.
Подробная информация представлена на нашем сайте: https://remont-setevyh-hranilishh-service.ru
I do agree with all of the concepts you have introduced for your post.
They are very convincing and can certainly work.
Nonetheless, the posts are too quick for starters.
May you please extend them a bit from next time? Thank you for the post. https://Welnesbiolabs.com/detaillant-en-ligne-de-meubles-et-equipement-a-montreal/
dummy visa card number newfresh high balance LIVE 24/24 – 2023 (No DIE) 【Visit CvvDumps.US】 All COUNTRY US , UK ,
CA , AU , EU , PK , MD
————-CONTACT———————–
WEBSITE : >>>>>> CvvDumps✺ US
—– HERE COMES THE PRICE LIST ———–
***** CVV Other countries
DO VISA CARD = $4 per 1 (buy >5 with price $2.5 per 1).
BT VISA CARD = $3,8 per 1 (buy >5 with price $2.5 per 1).
EC VISA CARD = $3,2 per 1 (buy >5 with price $2.5 per 1).
BD VISA CARD = $2,7 per 1 (buy >5 with price $2.5 per 1).
***** CVV US:
– US MASTER CARD = $3 per 1 (buy >5 with price $3 per 1).
– US VISA CARD = $2,4 per 1 (buy >5 with price $2.5 per 1).
– US AMEX CARD = $2,5 per 1 (buy >5 with price $2.5 per 1).
– US DISCOVER CARD = $3,9 per 1 (buy >5 with price $3.5 per 1).
– US CARD WITH DOB = $15 per 1 (buy >5 with price $12 per 1).
– US FULLZ INFO = $40 per 1 (buy >10 with price $30 per 1).
***** CCV UK:
– UK CARD NORMAL = $3 per 1 (buy >5 with price $3 per 1).
– UK MASTER CARD = $2,4 per 1 (buy >5 with price $2.5 per 1).
– UK VISA CARD = $3,3 per 1 (buy >5 with price $2.5 per 1).
– UK AMEX CARD = $2,8 per 1 (buy >5 with price $4 per 1).
$6
– UK CARD WITH DOB = $15 per 1 (buy >5 with price $14 per 1).
– UK WITH BIN = $10 per 1 (buy >5 with price $9 per 1).
– UK WITH BIN WITH DOB = $25 per 1 (buy >20 with price $22 per 1).
– UK FULLZ INFO = $40 per 1 (buy >10 with price $35 per
1).
***** CCV AU:
– AU MASTER CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU VISA CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU AMEX CARD = $8.5 per 1 (buy >5 with price $8 per 1).
– AU DISCOVER CARD = $8.5 per 1 (buy >5 with price $8 per 1).
***** CCV CA:
– CA MASTER CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA BUSINESS = $14 per 1 (buy >5 with price $13 per 1).
If you win more than $10,000 in a state lottery game, you can opt for to stay
anonymous.
Also visit my blog post: 게임몬 파워볼
Hi there to every , because I am truly eager of reading this webpage’s post
to be updated daily. It includes nice information.
Pin Up casino https://pin-up.salexy.kz official website, Pin Up slot machines play for money online, Pin Up mirror working for today.
Slot machines on the official website and mirrors of the Pin Up online casino https://pin-up.tr-kazakhstan.kz are available for free mode, and after registering at Pin Up Casino Ru you can play for money.
jasminer
Just check this out, live sex live cam
Nude amateur webcams woman live sex charNude hot webcams gi bfee0b6
Pin up entry to the official website. Play online casino Pin Up https://pin-up.prostoprosport.ru for real money. Register on the Pin Up Casino website and claim bonuses!
Sports in Azerbaijan https://idman-xeberleri.com.az development and popular sports Azerbaijan is a country with rich sports traditions and outstanding achievements on the international stage.
Наш сервисный центр предлагает высококачественный ремонт сигвеев адреса различных марок и моделей. Мы осознаем, насколько необходимы вам ваши сигвеи, и готовы предложить сервис наилучшего качества. Наши квалифицированные специалисты работают быстро и аккуратно, используя только сертифицированные компоненты, что обеспечивает долговечность и надежность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются владельцы сигвеев, включают проблемы с батареей, неработающий двигатель, неисправный контроллер, неисправности сенсоров и механические повреждения. Для устранения этих поломок наши опытные мастера оказывают ремонт батарей, двигателей, контроллеров, гиросенсоров и механических компонентов. Доверив ремонт нам, вы получаете долговечный и надежный качественный ремонт сигвеев.
Подробная информация доступна на сайте: https://remont-sigveev-expertise.ru
Здравствуйте!
Для многих людей, купить диплом о высшем образовании – это острая потребность, возможность получить достойную работу. Но для кого-то – это понятное желание не терять время на учебу в ВУЗе. С какой бы целью вам это не потребовалось, наша фирма готова помочь. Оперативно, качественно и по доступной цене сделаем документ нового или старого образца на настоящих бланках со всеми подписями и печатями.
Наша компания предлагает быстро и выгодно приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Данный диплом пройдет лубую проверку, даже при помощи специфических приборов. Достигайте цели быстро и просто с нашим сервисом.
О преимуществах наших дипломов:
• используем только качественные бланки “Гознака”;
• необходимые подписи руководства;
• все печати ВУЗа;
• специальные водяные знаки, нити и иные степени защиты;
• безупречное качество оформления – ошибок не бывает;
• любые проверки документов.
Дипломы и аттестаты об окончании ВУЗов и ССУЗов России:
– Повышают статус своего владельца;
– Открывают большие возможности на рынке труда;
– Повышают рейтинг в глазах окружающих;
– Повышают персональную уверенность и самооценку.
Где приобрести диплом по актуальной специальности?
https://erama.info/plyusy-i-minusy-pokupki-diploma-o-vysshem-obrazovanii_320724.html
Успехов в учебе!
cam to cam sex chat
Nude hot webcams woNude hot cams girl fb1fb65
jasminer
Как Купить Метамфетамин в Киеве? Киев Купить Метамфетамин? САЙТ – https://koks.top
.
.
Доставка в Руки Метамфетамина в Киеве? САЙТ – https://koks.top
Закладки в Киеве Метамфетамин Купить? САЙТ – https://koks.top
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
Теги – Купить в Киеве Метамфетамин?
Цена на Метамфетамин в Киеве?
Сколько стоит грамм Метамфетамина в Киеве?
Кристаллы Метамфетамина Купить в Киеве?
Украина Метамфетамин Кристаллы Доставка Купить
Excellent and high-quality free live sex chat absolutely free and easy to watch on any device, just
Naked hot webcams wNude amateur webcams girls online sex show 4_0b724
Наш сервисный центр предлагает надежный мастер по ремонту стиральной машины рядом всех типов и брендов. Мы знаем, насколько необходимы вам ваши устройства для стирки, и стремимся предоставить услуги высочайшего уровня. Наши квалифицированные специалисты работают быстро и аккуратно, используя только оригинальные запчасти, что гарантирует длительную работу проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются обладатели устройств для стирки, включают проблемы с барабаном, неисправности нагревательного элемента, программные сбои, неисправности насоса и повреждения корпуса. Для устранения этих неисправностей наши профессиональные техники оказывают ремонт барабанов, нагревательных элементов, ПО, насосов и механических компонентов. Доверив ремонт нам, вы обеспечиваете себе надежный и долговечный ремонт стиральных машин в москве.
Подробная информация размещена на сайте: https://remont-stiralnyh-mashin-ace.ru
Добрый день!
Для многих людей, заказать диплом университета – это острая необходимость, шанс получить достойную работу. Но для кого-то – это понятное желание не терять множество времени на учебу в институте. С какой бы целью вам это не понадобилось, мы готовы помочь. Быстро, профессионально и по доступной цене сделаем документ любого года выпуска на подлинных бланках со всеми печатями.
Заказать документ университета можно в нашей компании в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР. Даем 100% гарантию, что при проверке документов работодателем, каких-либо подозрений не появится.
Преимущества наших дипломов:
• используются настоящие бланки “Гознака”;
• все подписи должностных лиц;
• все печати учебного заведения;
• водяные знаки, нити и иные степени защиты;
• безупречное качество оформления – ошибок не будет;
• любые проверки оригинальности документа.
Наши специалисты предлагают быстро заказать диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Данный документ способен пройти любые проверки, даже при помощи специально предназначенного оборудования. Решайте свои задачи быстро с нашей компанией.
Где заказать диплом специалиста?
https://nsk-asl.ru/forum/messages/forum1/topic169/message179/?result=new#message179
Удачи!
Добрый день!
Для некоторых людей, купить диплом о высшем образовании – это необходимость, шанс получить отличную работу. Но для кого-то – это желание не терять множество времени на учебу в ВУЗе. С какой бы целью вам это не потребовалось, мы готовы помочь вам. Максимально быстро, профессионально и по доступной цене сделаем документ любого ВУЗа и года выпуска на подлинных бланках со всеми необходимыми печатями.
Приобрести документ ВУЗа можно в нашей компании. Мы оказываем услуги по производству и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы старого образца. Даем гарантию, что при проверке документа работодателем, подозрений не появится.
О преимуществах наших дипломов:
• используем лишь настоящие бланки “Гознака”;
• подлинные подписи должностных лиц;
• настоящие печати ВУЗа;
• водяные знаки, нити и иные степени защиты;
• идеальное качество оформления – ошибки исключены;
• любые проверки документа.
Наши специалисты предлагают максимально быстро приобрести диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями должностных лиц. Наш документ пройдет лубую проверку, даже с использованием специального оборудования. Достигайте цели быстро с нашим сервисом.
Где заказать диплом по нужной специальности?
https://xn--80ajjabicd1cty1a4fvb.xn--p1ai/blogs/1/trebuetsya-zakazat-diplom-otkryvayte-nash-magazin.php
https://vipka.mybb.ru/viewtopic.php?id=2678#p4659
http://wayworld.listbb.ru/viewtopic.php?f=2&t=24259
http://www.autopasjonaci.pl/forum/viewtopic.php?f=24&t=255509
https://lastdemo.primepix.ru/club/user/88/blog/6998/
Успехов в учебе!
Алтайский центр природного камня предоставляет прекрасную возможность купить глыбы с лишайником и мхом по самым привлекательным ценам. Сэкономим ваши деньги! Мы осуществляем доставку. Гарантируем великолепное обслуживание. Вы можете в этом удостовериться лично. Чтобы узнать сроки поставки и получить фото камня, пожалуйста, отправьте в WhatsApp запрос. Ищете купить скальные глыбы со мхом? Altdikam.ru – сайт, постоянно работаем над его улучшением. Здесь все ясно и наглядно. Если у вас возникли какие-то вопросы, свяжитесь с нами по телефону. С удовольствием вам поможем!
Just check this out, asian sex cams
Nude hot cams womaNaked amateur cams dacc581
kms auto lite Office 2019
https://aboutkms-web-.activablog.com/27338904/instrument-kms-auto-for-authorizing-the-system-software-and-the-office-software-package-deal
free download id9qf0915
Kms auto activator 57ad8_8
blacksprut даркнет – блек спрут онион, блек спрут оригинальная ссылка
Appreciate the recommendation. Let me try it out.
Feel free to surf to my page: کازینو آنلاین با پول واقعی
jasminer
World of Games https://onlayn-oyunlar.com.az provides the latest news about online games, game reviews, gameplay and ideas, game tactics and tips. The most popular and spectacular
The main sports news of Azerbaijan https://idman.com.az. Your premier source for the latest news, exclusive interviews, in-depth analysis and live coverage of everything happening in sports in Azerbaijan.
На сайте https://best-vendor.ru/product-tag/kanat-gost/ приобретите стальные канаты, которые потребуются для самых разных целей. Продукция выполнена по ГОСТу, что подтверждает эталонное высокое качество. Действует оперативная доставка. Есть возможность заказать продукцию в самом разном объеме и количестве. Канаты различаются техническими характеристиками. Для того чтобы заказать товары, необходимо просто позвонить менеджеру по телефону. У него получится уточнить всю необходимую информацию.
UFC in Azerbaijan https://ufc.com.az news, schedule of fights and tournaments 2024, rating of UFC fighters, interviews, photos and videos. Live broadcasts and broadcasts of tournaments, statistics.
NHL (National Hockey League) News https://nhl.com.az the latest and greatest NHL news for today. Sports news – latest NHL news, standings, match results, online broadcasts.
Hi to every one, the contents present at this web site are actually remarkable for people experience,
well, keep up the nice work fellows.
Here is my web blog: SkinOrigins skincare products
I have been surfing online greater than three hours as of late, yet
I by no means discovered any fascinating article like yours.
It is beautiful price sufficient for me. Personally,
if all site owners and bloggers made excellent content as you probably did, the net will probably be a lot more helpful than ever before.
Check out my blog post: Skintag removal
Mobile video production
http://aeroviewimage.com/
Great delivery. Sound arguments. Keep up the great effort.
Check out my web blog سایت انفجار
https://bs4shop.top/ – блэкспрут ссылка, блэкспрут 2fa
Thanks for every other great post. Where else may just anyone get that type of information in such an ideal approach
of writing? I have a presentation subsequent week, and I’m on the search
for such information.
Feel free to visit my web site; 카지노솔루션
Привет!
Наша компания предлагает выгодно и быстро приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Диплом пройдет лубую проверку, даже при помощи специфических приборов. Решайте свои задачи максимально быстро с нашей компанией.
Где купить диплом специалиста?
http://justvoip.listbb.ru/posting.php?mode=post&f=2&sid=152e88aabd372eda7b64efe2e31c0d83
Хорошей учебы!
The fastest way to make your wallet thick is found.] https://t.me/cryptaxbot/17?fruttyVet36Bus
I’d like to find out more? I’d care to find out more details.
Stop by my web blog – https://sewazoom.com/online-slots-and-entertainment-past-just-winning-money/
Добрый день!
Для определенных людей, купить диплом о высшем образовании – это острая необходимость, шанс получить достойную работу. Но для кого-то – это осмысленное желание не терять огромное количество времени на учебу в ВУЗе. С какой бы целью вам это не потребовалось, наша компания готова помочь вам. Оперативно, профессионально и по разумной стоимости изготовим диплом любого года выпуска на государственных бланках со всеми печатями.
Наши специалисты предлагают быстро приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Документ пройдет любые проверки, даже при использовании специальных приборов. Решите свои задачи быстро и просто с нашим сервисом.
Преимущества наших документов:
• используем настоящие бланки “Гознака”;
• необходимые подписи руководства;
• мокрые печати университета;
• специальные водяные знаки, нити и прочие степени защиты;
• безупречное заполнение и оформление – ошибок не бывает;
• любая проверка документа.
Дипломы об окончании ВУЗов и ССУЗов Российской Федерации:
– Способны повысить статус владельца;
– Открывают массу возможностей в социуме;
– Повышают рейтинг в глазах окружающих;
– Повышают личную самооценку.
Где приобрести диплом специалиста?
http://newsofgames.ru/kupit-diplom-ili-attestat-lyubogo-uchebnogo-zavedeniya-rf
Успехов в учебе!
Common mistakes to avoid in the Aviator Game include:
aviator game
Hello to every one, the contents existing at this web site are really amazing for people
knowledge, well, keep up the nice work fellows.
Stop by my webpage … หนังโป๊
to your liking, and quickly move to the section with https://pussytubehd.com on this topic. All categories are packed enough to make
Naked hot webcams girls live porn charNaked hot webcams girls live sex show 65d57ad
Hi! This is kind of off topic but I need some help from an established blog.
Is it tough to set up your own blog? I’m not very techincal but I can figure things
out pretty quick. I’m thinking about creating my own but I’m not sure
where to begin. Do you have any points or suggestions?
Thank you
Feel free to visit my site :: SkinOrigins
This is a topic that is close to my heart…
Best wishes! Exactly where are your contact details though?
Also visit my blog: hiding followers on tiktok
Cool blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple tweeks would really make my blog shine.
Please let me know where you got your design. Cheers
Also visit my web site: 카지노솔루션
This study is confirming decades of anecdotal stories our instructors shared in college.
My blog: 충남 스웨디시
It’s difficult to find well-informed people about this topic,
but how can you hide followers on tiktok seem like you know what you’re talking about!
Thanks
Can’t Sleep Because of Money Worries? Get Relief with a Fast Online Payday Loan. Payday lenders have had seen booming success worldwide, and credit that success to offering a service that was not formerly available.
Активируйте бонусы Vavada казино и наслаждайтесь бонусами на депозиты. Увеличьте шансы на выигрыш с дополнительными средствами. Играйте и выигрывайте больше!
Nice articl! Just check free sex cam chat this out!
Nude amateur webcamNaked amateur cams dacc581
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в нижнем тагиле, купить диплом вуза, купить диплом бухгалтера, купить диплом зубного техника, купить диплом математика. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://clicky.buzz/index.php?do=/public/blog/view/id_119666/title_/
http://whatsauto.ru/profile.php?u=ykiwe
http://plastic-solutions.ru/stykovoj-svarochnyj-apparat/widos-hrg-10/
https://stoliistulya.ru/products/stol-serii-sptm-1207-1208/#comment_272
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
http://rvolchansk.ru/user/bejaminjunioro424/
эскорт услуги от индивидуалок москвы https://prostitutki-213.ru. Вызвать проститутку на любой вкус по низким ценам. Каталог шлюх Москвы
kmsauto portable download
https://thekmsauto2.myparisblog.com/28454325/kms-auto-activator-summary-source-link-hyperlink-windows-activationmethod
free download id9qf0915
Kms auto activator fb65d57
winnings.
aviator game
https://multi-air.ru/
блек спрут онион – блек спрут оригинальная ссылка, спрут как попасть на сайт
Discover the best gay sex cam ever for free!
Naked amateur cams model live sex charNude amateur cams 12fb1fb
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в клинцах, купить диплом слесаря, купить диплом в симферополе, купить диплом логопеда, купить аттестат за 11 класс, потом попал на http://lisagerrard99.blogspot.com/2015/10/blog-post_23.html и там решили все мои учебные заботы!
Успешной учебы!
https://blacksprut-sait.top/ – блек спрут онион, блэкспрут ссылка тор
Наш сервисный центр предлагает профессиональный экспресс ремонт смартфона всех типов и брендов. Мы знаем, насколько важны для вас ваши мобильные устройства, и обеспечиваем ремонт первоклассного уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что обеспечивает надежность и долговечность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются обладатели мобильных устройств, включают неисправности дисплея, неисправности аккумулятора, программные сбои, неработающие разъемы и поломки корпуса. Для устранения этих проблем наши опытные мастера оказывают ремонт экранов, батарей, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы гарантируете себе долговечный и надежный сервис ремонта смартфона на выезде.
Подробная информация размещена на сайте: https://remont-telefonov-biz.ru
Just check out the best sex video chat live ever!
Nude hot webcams moNude amateur webcam 42dacc5
Добрый день!
Мы предлагаем выгодно приобрести диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Документ способен пройти любые проверки, даже с использованием профессиональных приборов. Решайте свои задачи быстро и просто с нашей компанией.
Где приобрести диплом специалиста?
http://reflections.listbb.ru/viewtopic.php?f=45&t=699
Хорошей учебы!
На сайте https://linii-okraski.ru/ вы сможете заказать линии окраски рулонного металла. Только в этой компании все изделия созданы с использованием революционных технологий и представляют собой уникальную и инновационную разработку, которая обязательно поможет вашему бизнесу. Линии Окраски отличаются отсутствием аналогов, являются особым изобретением. На технику предоставляются гарантии – 24 месяца. При необходимости воспользуйтесь профессиональной технической поддержкой, которая работает в круглосуточном режиме.
jasminer
Наш сервисный центр предлагает надежный мастер по ремонту телевизоров на дому всех типов и брендов. Мы знаем, насколько значимы для вас ваши TV, и готовы предложить сервис высочайшего уровня. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только качественные детали, что гарантирует надежность и долговечность наших услуг.
Наиболее частые неисправности, с которыми сталкиваются пользователи TV, включают проблемы с экраном, неисправности подсветки, неисправности программного обеспечения, неисправности разъемов и поломки компонентов. Для устранения этих поломок наши опытные мастера оказывают ремонт дисплеев, подсветки, ПО, разъемов и механических компонентов. Обратившись к нам, вы гарантируете себе качественный и надежный мастер по ремонту телевизоров на выезде.
Подробная информация размещена на сайте: https://remont-televizorov-fun.ru
jasminer
The Aviator Game is a thrilling online casino game that combines chance and strategy. With its unique gameplay,
aviator game
На сайте https://ipoteka-1.ru представлена вся самая актуальная, полезная информация, касающаяся ипотеки на вторичку, новостройку. Представлен материал о созаемщиках, о том, что лучше: арендовать жилье либо взять ипотеку. Есть данные о расходах на ипотеку и каким образом их понизить. Вы узнаете все о займах в режиме реального времени, как получить ипотеку, чтобы вам не отказали. Все статьи написаны экспертами, поэтому в них только точная и надежная информация. Вы получите ответ на вопрос, как быть, если нечем платить за ипотеку.
Добрый день!
Мы готовы предложить дипломы психологов, юристов, экономистов и других профессий по приятным ценам. Цена зависит от конкретной специальности, года выпуска и университета. Стараемся поддерживать для клиентов адекватную ценовую политику.
Где приобрести диплом специалиста?
1001cruise.ru/carnival-cruises/114-news/762-liner-royal-princess-will-be-released-in-the-first-flight.html
Хорошей учебы!
Здравствуйте!
Заказать документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России. Вы сможете получить диплом по любой специальности, любого года выпуска, включая документы образца СССР. Даем гарантию, что в случае проверки документов работодателем, подозрений не появится.
Где купить диплом специалиста?
http://sportandpolitics.ukrbb.net/viewtopic.php?f=24&t=11454
Успехов в учебе!
https://bs4shop.top/ – блэкспрут даркнет, блэкспрут сайт
Здравствуйте!
Эксперты с высшим образованием всегда ценились на рынке труда. Диплом ВУЗа необходим для того, чтобы доказать свое мастерство. Он позволяет понять работодателю, что сотрудник обладает всеми необходимыми знаниями чтобы качественно выполнить поставленную задачу. Но что делать, в случае если знания присутствуют, а подтверждающего документа у опытного специалиста нет? Покупка диплома поможет решить эту проблему. Приобретение диплома любого ВУЗа РФ в нашей компании является надежным процессом, поскольку документ заносится в реестр. Печать выполняется на специальных бланках, установленных государством.
Где заказать диплом специалиста?
http://fotomaniya.getbb.ru/ucp.php?mode=login&sid=4b341bf6d3854737cda582d2d05b9d41
Успехов в учебе!
Discover the best sex chat live free ever for free!
Nude amateur camsNaked amateur cams model live porn show 5d57ad4
blacksprut даркнет – блэкспрут ссылка тор, блэкспрут 2fa
Наши специалисты предлагает высококачественный сервис ремонта тепловизора рядом всех типов и брендов. Мы осознаем, насколько важны для вас ваши устройства теплового видения, и стремимся предоставить услуги наилучшего качества. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что обеспечивает долговечность и надежность проведенных ремонтов.
Наиболее частые неисправности, с которыми сталкиваются владельцы тепловизоров, включают проблемы с изображением, поврежденные линзы, программные сбои, проблемы с портами и поломки компонентов. Для устранения этих поломок наши профессиональные техники выполняют ремонт матриц, оптики, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы получаете долговечный и надежный мастерская по ремонту тепловизоров рядом.
Подробная информация размещена на сайте: https://remont-teplovizorov-gem.ru
Wonderful, what a website it is! This website gives useful
information to us, keep it up. https://Socialicus.com/story2793466/ideesrange
kms-auto ++
https://thekms-auto2.blogpayz.com/28038539/the-complete-the-pluses-of-the-kmsauto-lite-for-licensing
free download id9qf0915
Kms auto activator 942dacc
If you want to make confident that you are browsing just mobile-friendly games, use the ‘Mobile Devices Supported’
filter inn the Casino Guru free of charge games section.
My blog; Convenient
Добрый день!
Заказать диплом ВУЗа.
Цена значительно меньше нежели довелось бы заплатить за обучение в ВУЗе
Где заказать диплом специалиста?
http://bank-garantiya.ru/index.php?subaction=userinfo&user=ocejexer
Успешной учебы!
Привет!
Приобрести диплом университета.
Получаемый диплом с приложением 100% отвечает условиям и стандартам Министерства образования и науки, неотличим от оригинала. Не следует откладывать свои мечты на долгие годы, реализуйте их с нашей компанией – отправьте заявку на диплом прямо сейчас!
Где заказать диплом по нужной специальности?
http://buhtarma.ru/users/ebekixo
http://vecmir.ru/index.php/vecmirlife/58301-iweqy/profile
http://doktorpishet.ru/index.php?subaction=userinfo&user=ivemite
http://www.91hongyi.com/member/index.php?uid=aryqora
http://g95183sh.bget.ru/users/ywexibiwa
Успехов в учебе!
anal threesome #1 cam sex
Nude hot webcams model online sex showNaked amateur webca 2dacc58
Interactive Interface: Players can interact with the game in real-time, making decisions that impact their
aviator game
Наши специалисты предлагает профессиональный мастерская по ремонту варочных панелей в москве любых брендов и моделей. Мы понимаем, насколько важны для вас ваши варочные панели, и обеспечиваем ремонт первоклассного уровня. Наши опытные мастера работают быстро и аккуратно, используя только оригинальные запчасти, что гарантирует длительную работу проведенных ремонтов.
Наиболее частые неисправности, с которыми сталкиваются обладатели кухонных поверхностей, включают неисправности нагревательных элементов, неработающие сенсоры, программные сбои, неработающие разъемы и механические повреждения. Для устранения этих неисправностей наши опытные мастера выполняют ремонт нагревательных элементов, сенсоров, ПО, разъемов и механических компонентов. Обратившись к нам, вы получаете качественный и надежный сервисный ремонт варочных панелей с гарантией.
Подробная информация представлена на нашем сайте: https://remont-varochnyh-paneley-hit.ru
Discover the best free cam sex scene ever for free!
Nude amateur webcamNude amateur cams 6b6942d
Наш сервисный центр предлагает профессиональный центр ремонта видеокамеры на выезде любых брендов и моделей. Мы понимаем, насколько необходимы вам ваши видеорегистраторы, и обеспечиваем ремонт высочайшего уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что предоставляет долговечность и надежность проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются владельцы видеокамер, включают проблемы с записью, поврежденный объектив, неисправности программного обеспечения, неработающие разъемы и механические повреждения. Для устранения этих поломок наши квалифицированные специалисты выполняют ремонт записи, объективов, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы гарантируете себе качественный и надежный центр ремонта видеокамеры с гарантией.
Подробная информация размещена на сайте: https://remont-videokamer-ink.ru
1win игра с самолетом
aviator 1win live
the anticipation building as the plane climbs higher. The key is to cash out at the right moment before the
aviator game
chat live sex videos absolutely free and easy to watch on any device, just
Nude amateur cams woman online porn charNaked hot cams wom e0b6b69
http://www.nuursciencepedia.com/index.php/Saransk
https://kolejowelk207.pl:443/index.php/Dosaaf
Financial robot is the best companion of rich people. https://t.me/cryptaxbot/17?fruttyVet38Bus
Bet365 Ohio is 1 of the most competitive sportsbook operators in the whole Ohio betting landscape.
Here is my web site :: 안전놀이터
современные спортивные площадки ploshadka-sport.ru .
Just check this out, live sex chat and video
Nude amateur camsNaked hot webcams w e0b6b69
kmsauto lite download
https://thekmsauto-net-web-.weblogco.com/27956182/method-to-improve-the-speed-of-microsoft-windows-using-kmsauto-software
free download id9qf0915
Kms auto activator 4_11c86
навес металлический для машин
https://cps-mediawiki.cs.rptu.de/index.php/Saransk
https://gayageum.org/bbs/board.php?bo_table=free&wr_id=285130
Сайт 1x slots
Официальный сайт казино 1xslots играет ведущую роль в вопросе доверия и защищенности. На официальном сайте клиенты могут найти всю нужную информацию о казино. Мобильная версия сайта обеспечивает клиентам доступ ко всем функциями казино на мобильных устройствах, что крайне удобно. К тому же, на официальном портале можно получить мобильное приложение для игры.
1xslots зеркало на сегодня
В области онлайн-азартных игр значимость альтернативных сайтов трудно переоценить. Зеркало 1хслотс способствует игрокам обходить блокировки и получать неограниченно доступ ко всем слотам и игровым автоматам. Зеркало даёт стабильный доступ, позволяет посетителям наслаждаться игровым процессом.
Преимущества альтернативных сайтов:
1. Обход ограничений;
2. Бесперебойный доступ.
регистрация в 1xslots casino
Процесс регистрации на сайте 1хслотс легок и ясен. Пользователям важно пройти регистрацию, чтобы зарегистрировать профиль. Регистрация занимает всего несколько минут, после регистрации можно войти в личный кабинет. Вход в личный кабинет позволяет клиентам управлять финансами, делать депозиты и снимать деньги.
Этапы регистрации:
1. Заполнить регистрационную анкету;
2. Подтверждение информации;
3. Вход в личный кабинет 1xslots casino;
Казино и игры
Казино 1xslots предлагает большое количество игр, включая игровые автоматы. Играть онлайн в казино можно всегда, наслаждаясь игрой в различные автоматы. Мобильные приложения позволяют играть в дороге, что особенно важно для тех, кто ценит удобство и доступность. Финансовые операции проводятся быстро и безопасно, что делает игру более комфортной и безопасной.
Промоакции и бонусы
Одним из привлекательных аспектов игры в 1xslots являются промоакции и бонусные предложения. Специальные коды дают дополнительные деньги для ставок, а бонусы делают игру интереснее. Промокоды и бонусы увеличивают вероятность выигрыша.
Преимущества использования промокодов и бонусов:
– Бонусные деньги для игры
– Бесплатные игры на автоматах
– Большие шансы на выигрыш
Бонус при регистрации для первых четырех депозитов. В сумме приветственный пакет включает до 1500 евро и 150 фриспинов. А промокод «ESDINERO» поможет еще больше расширить пакет.
Установка мобильного приложения 1 x slots
Для удобства клиентов 1xslots предлагает скачать приложение. Мобильная версия приложения дает возможность играть везде и всегда, предоставляя доступ ко всем функциям казино. Установка приложения требует несколько минут, но дает возможность насладиться игрой в любое удобное время.
Выводы
Использование официального сайта и зеркал 1xslots разнообразие игр, промоакции и бонусы, делают 1xslots удобным и безопасным. Игроки могут наслаждаться своими любимыми играми всегда и везде, уверенные в надежности и защищенности доступа к 1xslots.
The basic rule of the Aviator Game is straightforward: place a bet, watch the plane take off, and decide when to
aviator game
If bettors want to location bets on additional obscure markets like rugby or table tennis, bet365
provides that, also.
My site … 토토친구
Discover the best live one on one sex chat ever for free!
Nude hot webcams giNaked amateur cams girls live sex show 2dacc58
На сайте https://lordfilm-hd.cfd/ вы сможете ознакомиться со всеми интересными, увлекательными и головокружительными фильмами, которые точно произведут на вас эффект. Все фильмы выполнены в отличном высоком качестве и с хорошим звуком. Есть и ожидаемые премьеры, выхода которых ожидали давно. У фильмов оригинальный, непредсказуемый сюжет. В кино играют лучшие актеры. Вас обрадуют спецэффекты, приятная музыка и любопытное повествование. Из всего многообразия вы точно найдете то, что посмотреть сегодня.
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в новоуральске, купить диплом историка, купить диплом штукатура, купить диплом агронома, купить свидетельство о заключении брака, затем наткнулся на https://my.djtechtools.com/users/1392942
https://re-port.ru/users/51713/
http://fabnews.ru/forum/showthread.php?p=71942#post71942
https://www.pling.com/u/diplomrussian/
https://www.becco.com.au/home-reduced-menu/becco_logo_small-2/#comment-113215
, где все мои учебные вопросы были решены!
Успешной учебы!
https://sdsle.sk/forum/profile/timothyspriggs6/
http://www.tampabaybusiness.directory/dir/index.php?title=Dosaaf
Ищите строительство дома в Сочи и Краснодарском крае под ключ? Зайдите на сайт https://alternativa-sochi.ru/ где вы сможете ознакомиться с проектами домов и портфолио Компании Альтернатива и заказать строительство под ключ – качественные, быстровозводимые, энергоэффективные каркасные дома от фундамента до чистовой отделки. Гарантия, поэтапная оплата, помощь с ипотекой. Подробнее на сайте.
jasminer
Player Reviews and Testimonials
aviator game
본즈 카지노에서는 간편한 로그인 절차가 제공됩니다. Bons Casino에 가입하고 본즈 보너스 코드를 입력하여 다양한 혜택을 누리세요. 슬롯 게임도 다양하게 즐길 수 있으며, bons 보너스로 더욱 재미있게 게임을 즐길 수 있습니다. Bons Casino는 항상 새로운 보너스를 제공합니다. 본즈와 함께 흥미로운 시간을 보내세요. VIP 프로그램도 있어 더 많은 혜택을 누릴 수 있습니다. bons casino
Problems selecting up players in transition and with half-court rotations has been evident.
Also visit my website: Get more info
Homepage von online live sex chat
Naked amateur webcaNaked amateur webca 6b6942d
На сайте https://lan-union.ru предлагается к покупке сетевое и кабельное оборудование. В каталоге компании вы найдете подробное описание, также характеристики продукции и товаров производителя. На сайте вы можете увидеть сертификаты на продукцию, и детальнее ознакомиться с сервисом. Из преимуществ компании, можно отметить быструю логистику, высочайшее качество оборудования и расширенную гарантию. Для того чтобы быть в курсе акций и новостей компании, подпишитесь на рассылку.
блэкспрут 2fa – блек спрут оригинальная ссылка, 2fa blacksprut
kms activator net Office 2019
https://akmssite2.articlesblogger.com/50658502/kmsauto-net-summary-get-source-web-url-windows-authorizationguidelines
free download id9qf0915
Kms auto activator 942dacc
jasminer
jasminer
Discover the best Chloe! nude before webcam – Live Sex Chat ever for free!
Naked amateur cams girls live porn charNude amateur cams d2_7f48
Playing the Aviator Game is a thrilling experience. Players place their bets and watch the plane take off, with
aviator game
This indicates that by depositing 5 BTC, the player’s opening
balance will commence at 10 BTC.
Look into my web site :: http://www.die-seite.com
https://bs4shop.top – blacksprut onion, блэкспрут сайт
Nice articl! Just check cam for sex this out!
Naked hot cams womNude amateur webcam 1fb65d5
jasminer
Привет!
Для определенных людей, купить диплом о высшем образовании – это острая потребность, шанс получить хорошую работу. Но для кого-то – это очевидное желание не терять массу времени на учебу в университете. С какой бы целью вам это не понадобилось, наша фирма готова помочь вам. Максимально быстро, профессионально и по разумной стоимости изготовим диплом нового или старого образца на подлинных бланках со всеми требуемыми печатями.
Наша компания предлагает быстро и выгодно приобрести диплом, который выполнен на оригинальном бланке и заверен печатями, штампами, подписями. Документ способен пройти лубую проверку, даже с использованием специально предназначенного оборудования. Решите свои задачи максимально быстро с нашей компанией.
Основные преимущества наших документов:
• используем только настоящие бланки “Гознак”;
• подлинные подписи руководства;
• мокрые печати учебного заведения;
• специальные водяные знаки, нити и иные степени защиты;
• идеальное заполнение и оформление – ошибок не бывает;
• любая проверка оригинальности документа.
Дипломы и аттестаты об окончании ВУЗов и ССУЗов Российской Федерации:
– Повышают статус владельца;
– Открывают большие возможности на рынке труда;
– Повышают уважение в глазах окружающих;
– Повышают самооценку.
Где купить диплом по нужной специальности?
https://gigspeeddev.biz/2024/06/08/Купить-диплом-о-высшем-образовании-на-заказ
Хорошей учебы!
Здравствуйте!
Для многих людей, заказать диплом ВУЗа – это острая потребность, удачный шанс получить достойную работу. Однако для кого-то – это желание не терять время на учебу в университете. Что бы ни толкнуло вас на такой шаг, наша фирма готова помочь. Оперативно, профессионально и по доступной цене изготовим документ любого года выпуска на государственных бланках с реальными подписями и печатями.
Купить документ о получении высшего образования вы имеете возможность в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы СССР. Гарантируем, что в случае проверки документов работодателем, подозрений не появится.
Преимущества наших дипломов:
• используем только настоящие бланки “Гознака”;
• все подписи руководства;
• мокрые печати учебного заведения;
• специальные водяные знаки, нити и другие степени защиты;
• идеальное заполнение и оформление – ошибок не бывает;
• любая проверка документов.
Мы предлагаем выгодно заказать диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Диплом пройдет любые проверки, даже при помощи профессиональных приборов. Достигайте цели быстро с нашей компанией.
Где приобрести диплом специалиста?
http://sheriffstation.bestbb.ru/viewtopic.php?id=283
http://onelife.forumex.ru/viewtopic.php?f=3&t=52
http://www.fiammeblu.it/profile.php?uid=27490
http://frank-shkola.ru/forum/topic/add/forum1/#postform
http://www.vocal.com.ua/node/61538
Удачи!
Education Secretary Miguel Cardona announced a sweeping plan for student debt
relief in August.
Feel free to visit my webpage :: 당일대출
jasminer
jasminer
blacksprut даркнет – 2fa blacksprut, блэкспрут 2fa
best personal loans texas Generally, the applicant is informed about the status of the application within 6 hours of applying for the loan.
Common feedback from players includes requests for more in-game bonuses, additional multiplayer options, and
aviator game
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me?
kms activatorwindows 11
https://aboutfree-forum.bloguetechno.com/kmsauto-lite-overview-download-path-url-windows-enablementinstructions-63485644
free download id9qf0915
Kms auto activator 942dacc
Добрый день!
Для некоторых людей, заказать диплом ВУЗа – это острая необходимость, шанс получить отличную работу. Однако для кого-то – это желание не терять массу времени на учебу в ВУЗе. С какой бы целью вам это не понадобилось, наша фирма готова помочь. Быстро, профессионально и выгодно сделаем диплом любого ВУЗа и года выпуска на государственных бланках со всеми печатями.
Заказать документ университета можно в нашей компании в столице. Мы предлагаем документы об окончании любых университетов России. Вы получите диплом по любой специальности, включая документы Советского Союза. Гарантируем, что в случае проверки документов работодателями, каких-либо подозрений не появится.
О преимуществах наших дипломов:
• используем настоящие бланки “Гознак”;
• необходимые подписи должностных лиц;
• мокрые печати университета;
• водяные знаки, нити и прочие степени защиты;
• безупречное качество оформления – ошибок не будет;
• любая проверка документов.
Наши специалисты предлагают максимально быстро приобрести диплом, который выполняется на оригинальном бланке и заверен печатями, штампами, подписями должностных лиц. Документ пройдет лубую проверку, даже с применением профессионального оборудования. Достигайте цели максимально быстро с нашими дипломами.
Где купить диплом специалиста?
http://truck-legion.ru/index.php?subaction=userinfo&user=egalycys
http://vashtehnadzor.ru/index.php?subaction=userinfo&user=enyzeliw
https://www.brodyaga.org/club/user/110627/blog/6166/
http://mos-it.ru/index.php?subaction=userinfo&user=aqydi
http://kamaz-ukraine.com/index.php?subaction=userinfo&user=eruheqewu
Хорошей учебы!
Откройте тайны берців зсу, Какую роль играют берці зсу в обрядах?, познакомьтесь с, Легенды и предания о берцах зсу, Берці зсу: символ верности и чести, тайны, поищите, Берці зсу: духовное наследие Украины, Берці зсу: подвиги и традиции, в душу, дізнайтесь, дізнайтеся
літні берці зсу купити літні берці зсу купити .
Привет, друзья!
Для некоторых людей, купить диплом о высшем образовании – это острая необходимость, возможность получить достойную работу. Однако для кого-то – это желание не терять время на учебу в институте. Что бы ни толкнуло вас на такой шаг, наша компания готова помочь. Оперативно, профессионально и выгодно изготовим документ нового или старого образца на подлинных бланках с реальными подписями и печатями.
Наши специалисты предлагают быстро и выгодно приобрести диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями должностных лиц. Наш документ способен пройти лубую проверку, даже при помощи специально предназначенного оборудования. Решите свои задачи быстро и просто с нашими дипломами.
Превосходства наших дипломов:
• используются настоящие бланки “Гознака”;
• все подписи руководства;
• настоящие печати университета;
• водяные знаки, нити и другие степени защиты;
• безупречное заполнение и оформление – ошибки исключены;
• любая проверка документа.
Где заказать диплом по нужной специальности?
http://catalogue.bbok.ru/viewtopic.php?id=2927#p24749
Хорошей учебы!
Привет!
Для многих людей, приобрести диплом о высшем образовании – это необходимость, уникальный шанс получить достойную работу. Однако для кого-то – это желание не терять множество времени на учебу в университете. С какой бы целью вам это не понадобилось, наша фирма готова помочь. Быстро, профессионально и недорого сделаем диплом нового или старого образца на настоящих бланках с реальными печатями.
Приобрести документ о получении высшего образования вы имеете возможность у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Гарантируем, что при проверке документов работодателями, каких-либо подозрений не возникнет.
Превосходства наших дипломов:
• используются настоящие бланки “Гознак”;
• подлинные подписи руководства;
• все печати учебного заведения;
• водяные знаки, нити и другие степени защиты;
• идеальное качество оформления – ошибок не будет;
• любая проверка оригинальности документа.
Наши специалисты предлагают максимально быстро заказать диплом, который выполнен на оригинальном бланке и заверен печатями, штампами, подписями должностных лиц. Диплом пройдет лубую проверку, даже при помощи специального оборудования. Достигайте своих целей быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
https://wiki.odessanews.biz/index.php/%d0%9e%d0%bd%d0%bb%d0%b0%d0%b9%d0%bd_%d0%bc%d0%b0%d0%b3%d0%b0%d0%b7%d0%b8%d0%bd,_%d1%80%d0%b5%d0%b0%d0%bb%d0%b8%d0%b7%d1%83%d1%8e%d1%89%d0%b8%d0%b9_%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc%d1%8b_%d1%83%d1%87%d0%b5%d0%b1%d0%bd%d1%8b%d1%85_%d0%b7%d0%b0%d0%b2%d0%b5%d0%b4%d0%b5%d0%bd%d0%b8%d0%b9_%d0%bd%d0%b0_%d0%93%d0%9e%d0%97%d0%9d%d0%90%d0%9a%d0%b5
Успехов в учебе!
Nice articl! Just check Caroline-ellin live chat nude before webcam – Live Chaturbate this out!
Nude amateur webcamNude hot webcams mo e0b6b69
блек спрут оригинальная ссылка – блэкспрут 2fa, блэкспрут ссылка тор
сервис ремонта смартфонов
Откройте тайны берців зсу, историю, обычаи, погрузитесь в, раскройте, Берці зсу: путь к мудрости, смысл, энергией, культурой, Почуйте, як б’ють від Берця зсу, анатомію, значення
берці зсу 2021 берці зсу 2021 .
game is random and unbiased, providing a fair chance for all players to win.
aviator game
Погрузитесь в мир берців зсу, Почему берці зсу так важны для культуры?, познакомьтесь с, значении, раскройте, мистику, Берці зсу: талисман силы, энергией, Берці зсу: подвиги и традиции, Як живеться в берцах зсу, дізнайтесь, вивчіть
нові берці зсу 2021 https://bercitaktichnizsu.vn.ua/ .
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: где купить диплом образование, купить диплом в таганроге, купить диплом в пятигорске, купить диплом в троицке, купить диплом химика. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://slbook-kaluga.ru/index.php/forum/user/245029-obexuz и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в сочи, купить диплом в нижнекамске, купить диплом в ростове, купить диплом в крыму, купить диплом парикмахера и получил базовые знания. В итоге остановился на материале: https://www.hashtap.com/@artur.sh/ваш-диплом-надежность-и-качество-eagWLen8qqwx
http://myturtime.ru/nastoyashhie-diplomyi-bez-problem
https://stil.5bb.ru/viewtopic.php?id=4360#p10431
http://s-s-o.ru/forum.php?PAGE_NAME=profile_view&UID=52338
http://rorp.4admins.ru/viewforum.php?f=33
Хорошей учебы!
Las Atlantis has a healthful selection of slots and online casino games.
Visit my blog post :: 온카
Nice articl! Just check stefannichka fully nude stripping on cam for live porn movie show this out!
Naked hot webcams gNaked hot webcams m b6b6942
Погрузитесь в мир берців зсу, значение, освойте, погрузитесь в, Берці зсу: традиции древних времен, Берці зсу: путь к мудрости, найдите, Берці зсу: духовное наследие Украины, традициями, в мир, З чого починаються берці зсу, зрозумійте
берці зсу літні https://bercitaktichnizsu.vn.ua/ .
блэкспрут darknet – блэкспрут ссылка, блэкспрут даркнет
anal threesome Julia Davis, рџЌ‘ naked on sex cam for live porn chat
Nude amateur cams girls live sex showNaked amateur cams b65d57a
Sweet blog! I found it while searching on Yahoo News.
Do you have any tips on how to get listed in Yahoo News? I’ve been trying for a while but I never seem to
get there! Cheers
Here is my webpage – Artificial Intelligence
game was designed to provide an adrenaline-pumping experience that mimics the thrill of gambling with a twist.
aviator game
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом в кургане, купить диплом в люберцах, купить диплом цена, купить диплом техникума, купить диплом в зеленодольске, а потом наткнулся на https://khavu.com/shop/sampler/sampler/#comment-3127, где все мои учебные проблемы были решены!
Успехов в учебе!
Привет!
Наша компания предлагает выгодно купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Наш документ способен пройти лубую проверку, даже при помощи специального оборудования. Достигайте цели быстро и просто с нашими дипломами.
Где заказать диплом специалиста?
http://mastrerkon.ru/forum/ucp.php?mode=login&sid=3a4d0dee16ba3c9517ba059edbe170f7
Успехов в учебе!
Добрый день!
Для многих людей, приобрести диплом ВУЗа – это острая необходимость, шанс получить достойную работу. Но для кого-то – это желание не терять время на учебу в институте. Что бы ни толкнуло вас на это решение, наша компания готова помочь вам. Быстро, качественно и по разумной цене изготовим диплом нового или старого образца на подлинных бланках с реальными печатями.
Наша компания предлагает быстро и выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Наш документ способен пройти лубую проверку, даже с использованием специального оборудования. Достигайте цели быстро и просто с нашим сервисом.
Плюсы наших дипломов:
• используем лишь настоящие бланки “Гознака”;
• оригинальные подписи должностных лиц;
• настоящие печати учебного заведения;
• специальные водяные знаки, нити и другие степени защиты;
• безупречное качество оформления – ошибок не бывает;
• любая проверка оригинальности документа.
Документы об окончании ВУЗов и ССУЗов Российской Федерации:
– Автоматически повышают статус своих владельцев;
– Открывают множество возможностей на рынке труда;
– Повышают уважение в глазах окружающих;
– Повышают самооценку.
Где приобрести диплом по нужной специальности?
http://bl.com.tw/index.php?title=???????_??_?????????_?????:_????????_?????_???????????_?_??????_????????????????_???????????
Успехов в учебе!
Здравствуйте!
Для определенных людей, приобрести диплом о высшем образовании – это необходимость, удачный шанс получить хорошую работу. Но для кого-то – это очевидное желание не терять время на учебу в ВУЗе. С какой бы целью вам это не потребовалось, мы готовы помочь. Максимально быстро, качественно и недорого изготовим диплом любого года выпуска на подлинных бланках со всеми подписями и печатями.
Приобрести документ университета можно в нашей компании. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца. Даем 100% гарантию, что при проверке документов работодателем, никаких подозрений не возникнет.
Основные преимущества наших дипломов:
• используются только настоящие бланки “Гознак”;
• оригинальные подписи должностных лиц;
• все печати ВУЗа;
• водяные знаки, нити и прочие степени защиты;
• безупречное заполнение и оформление – ошибок не будет;
• любые проверки документов.
Наша компания предлагает выгодно и быстро заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Диплом способен пройти любые проверки, даже при использовании специфических приборов. Достигайте свои цели быстро с нашей компанией.
Где заказать диплом специалиста?
http://www.club-kia.com/forum/thread30745.html
http://forum.anime.org.ua/bbs/showthread.php?p=128403
http://mirstalkera.4admins.ru/viewtopic.php?f=50&t=1840
https://akademiyavodopad.ru/forum/messages/forum7/topic333/message641/?result=new#message641
https://www.rugladyseminars.com/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=288
Успехов в учебе!
Just check this out, live sex chats
Nude amateur camsNaked hot cams wom 0b6b694
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом экономиста, где купить атестат об окончании школы, купить диплом в крыму, можно ли купить диплом, купить диплом в железногорске, потом попал на https://tdtaler.ru/catalog/armirovannye-rezinovye-shlangi/shlang-iz-epdm-dlya-nasyshchennogo-para-sodivap-230-c/
http://topforbaby.ru/product/adameks-koljaska-transf-galaxy-ljulka-imit/reviews/
https://stroigarant13.ru/blog/napolnaya-styazhka-osnovnye-vidy/#comment_150302
https://mecool.com.ru/mecool-mxv-4k/#comment_2059/
http://www.avatars.cc/member.php?action=showprofile&user_id=34845
и там решили все мои учебные заботы!
Успехов в учебе!
Many online platforms host competitive tournaments and events for the Aviator Game. These events offer players
aviator game
Excellent and high-quality https://sexytube.pro absolutely free and easy to watch on any device, just
Nude hot cams womaNaked amateur webca 942dacc
Internet uzerinden casino oyunlar? oynamak isteyenler icin pin-up online, eglenceli ve guvenilir bir platform sunuyor. Genis oyun secenekleri, comert bonuslar ve h?zl? odeme islemleriyle uyelerine kaliteli bir oyun deneyimi yasat?yor.
pin up 7/24 giris en onemli ozelliklerinden biri, 1000’den fazla oyun secenegi sunmas?d?r. Slot makineleri, canl? casino oyunlar? pin-up giris spor bahisleri, poker ve daha pek cok oyun alternatifi bulunuyor. Microgaming, NetEnt, Pragmatic Play pin up giris gibi sektorun onde gelen oyun saglay?c?lar?n?n en populer oyunlar?n? <a href="https://groups.google.com/g/pin-up-online-trkiye-gncel-giri-724/c/s-iSz1wgKa8"pin up guncel giris oynamak mumkun.
Sitede pin up casino online yeni uyelere ozel hos geldin bonusu pin up slot ve mevcut uyeler icin duzenli pin-up oyunu olarak sunulan promosyonlar pin up turkiye bulunuyor. Bu bonuslar sayesinde daha fazla oyun oynama ve kazanma sans? elde ediliyor. Ayr?ca VIP program? <a href="https://groups.google.com/g/pin-up-online-trkiye-gncel-giri-724/c/s-iSz1wgKa8"pin-up casino ile en sad?k ve aktif uyeler ozel avantajlardan yararlanabiliyor.
pin-up online casino, uyelerinin guvenligini ve gizliligini pin up giris turkiye on planda tutuyor. SSL pin up sifreleme teknolojisi pin up casino ile kisisel ve pin up giris finansal veriler korunuyor. Lisansl? ve denetlenen bir site oldugu icin uyeler yasal ve adil bir ortamda oyun oynayabiliyorlar. Musteri hizmetleri ekibi 7/24 destek sagl?yor.
Siteye uye olmak ve para pin-up yat?r?p cekmek oldukca kolay. Kredi kart? pin-up casino giris banka transferi, e-cuzdan gibi pin up casino guncel giris farkl? odeme yontemleri pin up bet destekleniyor. Islemler h?zl? ve pin up casino giris sorunsuz bir sekilde gerceklestiriliyor.
Sonuc olarak, Pin Up Casino s?k tasar?m?, zengin icerigi, avantajl? bonuslar? ve guvenilir altyap?s?yla online casino tutkunlar?na hitap ediyor. Eglenceli ve kaliteli bir oyun deneyimi yasamak isteyenlerin mutlaka denemesi gereken bir platform.
Узнайте всю правду о берцах зсу, историю, Почему берці зсу считаются священными?, разберитесь в, красоту, Берці зсу: символ силы, Берці зсу: талисман силы, Украинские берці зсу: традиции и современность, освойте, Спробуйте на власній шкірі бути Берцем зсу, погляньте, силу
військові берці зсу https://bercitaktichnizsu.vn.ua/ .
Здравствуйте!
Для некоторых людей, приобрести диплом о высшем образовании – это необходимость, возможность получить хорошую работу. Впрочем для кого-то – это желание не терять множество времени на учебу в ВУЗе. Что бы ни толкнуло вас на такое решение, мы готовы помочь вам. Быстро, качественно и по доступной цене сделаем документ нового или старого образца на подлинных бланках с реальными печатями.
Купить документ о получении высшего образования вы имеете возможность в нашей компании в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых университетов РФ. Вы сможете получить диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что в случае проверки документа работодателем, подозрений не появится.
Основные преимущества наших документов:
• используем настоящие бланки “Гознак”;
• все подписи руководства;
• настоящие печати учебного заведения;
• водяные знаки, нити и другие степени защиты;
• идеальное качество оформления – ошибки полностью исключены;
• любые проверки оригинальности документа.
Наши специалисты предлагают выгодно приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ пройдет лубую проверку, даже при помощи профессиональных приборов. Достигайте своих целей максимально быстро с нашим сервисом.
Где приобрести диплом по нужной специальности?
http://crtdu-kras.ru/communication/forum/user/241307/
http://cobaki.ru/users.php?m=details&id=90788
http://cooleda.com/index.php?subaction=userinfo&user=akurudyn
http://geolan-ksl.ru/forum/user/85838/
https://boosty.to/zukunft2/posts/cc9b2ee9-289d-4320-94e0-1fde4e3749a4
Удачи!
Привет!
Для многих людей, заказать диплом о высшем образовании – это необходимость, удачный шанс получить достойную работу. Но для кого-то – это понятное желание не терять массу времени на учебу в институте. С какой бы целью вам это не потребовалось, мы готовы помочь. Быстро, качественно и по разумной цене изготовим документ любого года выпуска на государственных бланках со всеми подписями и печатями.
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Документ пройдет лубую проверку, даже при использовании специальных приборов. Достигайте цели быстро и просто с нашими дипломами.
О преимуществах наших дипломов:
• используем настоящие бланки “Гознак”;
• подлинные подписи руководства;
• настоящие печати университета;
• водяные знаки, нити и прочие степени защиты;
• идеальное заполнение и оформление – ошибок не будет;
• любая проверка оригинальности документа.
Где купить диплом по нужной специальности?
https://zarabotok.forumrpg.ru/viewtopic.php?id=67691#p147669
Успехов в учебе!
Добрый день!
Для многих людей, заказать диплом о высшем образовании – это острая необходимость, уникальный шанс получить выгодную работу. Но для кого-то – это понятное желание не терять время на учебу в институте. Что бы ни толкнуло вас на такое решение, мы готовы помочь вам. Быстро, профессионально и по разумной цене сделаем документ нового или старого образца на подлинных бланках с реальными подписями и печатями.
Купить документ университета можно у нас. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы старого образца. Гарантируем, что в случае проверки документов работодателями, подозрений не появится.
Преимущества наших дипломов:
• используем лишь настоящие бланки “Гознака”;
• необходимые подписи руководства;
• настоящие печати ВУЗа;
• водяные знаки, нити и иные степени защиты;
• идеальное заполнение и оформление – ошибок не бывает;
• любые проверки документов.
Наши специалисты предлагают выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Данный диплом пройдет любые проверки, даже с применением специального оборудования. Решайте свои задачи быстро и просто с нашими дипломами.
Где купить диплом специалиста?
http://bahchisaray.org.ua/index.php?showtopic=27820
Хорошей учебы!
ремонт стиральных машин ремонт стиральных машин .
https://blacksprut-sait.top – спрут как попасть на сайт, спрут как попасть на сайт
Just check out the best free cam sex ever!
Naked amateur webcaNude amateur cams d6_520e
You can nevertheless use the app though to make deposits and
withdrawals, check lines, sweat bets, and much More info.
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в ачинске, купить диплом в архангельске, купить диплом мастера маникюра и педикюра, купить диплом в великом новгороде, купить диплом повара-кондитера, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://dolgoprudni.rusff.me/viewtopic.php?id=1827#p4320
http://skazka.g-talk.ru/viewtopic.php?f=1&t=1306
https://youhelp.artbb.me/viewtopic.php?id=712#p1448
https://www.vikisport.ru/index.php?links_exchange=yes
https://lubercy.ixbb.ru/viewtopic.php?id=6118#p13972
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Хорошей учебы!
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в пятигорске, купить диплом в димитровграде, где купить диплом, купить диплом в георгиевске, купить диплом в люберцах, постепенно вникая в суть дела нашел отличный материал здесь http://nvkb.ru/forum/index.php/user/101059/ и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Хорошей учебы!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом в спб, купить диплом в белово, купить диплом журналиста, купить диплом в казани, #купить диплом университета, а затем переключился на дипломы вузов. Подробности здесь: https://kinopuk.ru/viewtopic.php?id=9020#p56546
http://www.chaodisiaque.com/forum/viewtopic.php?pid=21984#p21984
https://rodme.ru/kupit-diplomy-s-garantiey-podlinnosti-t12559.html
https://buyandsellhair.com/dashboard/
https://www.orderviewdocs.online/doku.php?id=??????_??????_???????_?????????_????????
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успешной учебы!
Ищете лучшие промокоды для Vavada казино? Используйте актуальные предложения, чтобы получить бонусы на депозиты и фриспины, делая вашу игру еще более увлекательной.
The Aviator Game is a thrilling online casino game that combines chance and strategy. With its unique gameplay,
aviator game
We also cover everything that you will
Here is my web blog :: base28.Fitnell.Com
obviously like your web site but you have to take a look at the
spelling on several of your posts. Many of them are rife with spelling
issues and I to find it very troublesome to tell the reality however I’ll surely come back again. http://Christinarosecarr.com/__media__/js/netsoltrademark.php?d=365.expresso.blog%2Fquestion%2Fkarin-herzog-cosmetiques-une-revolution-dans-le-monde-des-soins-dune-peau-2%2F
Использование промокодов Drip казино – это шанс получить дополнительные средства для игры. Бонусы и фриспины сделают процесс игры более увлекательным и прибыльным.
Привет, друзья!
Наши специалисты предлагают выгодно купить диплом, который выполняется на оригинальной бумаге и заверен печатями, штампами, подписями. Документ пройдет любые проверки, даже с применением профессиональных приборов. Достигайте цели быстро и просто с нашей компанией.
Где купить диплом по нужной специальности?
https://blogs.rufox.ru/~worksale/47159.htm
Успешной учебы!
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом в новокузнецке, купить диплом в кургане, купить диплом механика, купить диплом электрика, купить диплом фельдшера, а потом наткнулся на http://igrimachklas.blogspot.com/2017/04/blog-post_10.html, где все мои учебные проблемы были решены!
Хорошей учебы!
social interaction adds a new layer of excitement and competition to the game, making it more engaging and
aviator game
To start playing the Aviator Game, simply choose a reputable online casino platform that offers the game.
aviator game
Once thhe wager reaches a preset maximum bet value 10000, we
reset the gambler with a minimum bet.
Also visit my homepagte Casino79.in
Shoppers may take component in a variety of live poker tournaments there.
my web site :: 카지노친구
No need to stay awake all night long to earn money. Launch the robot.] https://t.me/cryptaxbot/17?fruttyVet96Bus
Узнайте больше о преимуществах наших двухскатный навес.
Еще мы предлагаем:
консольные навесы
навесы для авто
навес на дачу
навес из поликарбоната для автомобиля
навесы для автомобилей из поликарбоната
Больше информации на нашем сайте https://naves-sale.ru
프라그마틱 슬롯 무료
“…” 홍지황제는 갑자기 무언가를 깨달았다.
Each and every game you play at a casino has a statistical probability against you winning—every
single time.
Here is my web site; Totalfreewebcams.chaturbate.com
На сайте https://iz-nerzhaveyki.ru/ вы можете приобрести из нержавеющей стали подводки, фитинги, фланцы, краны и другое. Здесь вы подробнее узнаете про шаровые краны, рукав высокого давления и гибкую подводку. Каталог на сайте позволит подобрать то, что вас интересует. Вся продукция качественная, она представлена на портале с фото и техническими характеристиками. Если у вас возникли вопросы по продукции, обратитесь к нам по телефону на сайте, либо на электронную почту.
Since its inception, the Aviator Game has undergone numerous updates and enhancements. Technological
aviator game
You’re Not Alone: Payday Loans Can Help Thousands Get Through Tough Times. It’s important to remember that nothing in this world is free, so if you want to take advantage of a payday loan you will have to pay for it. Payday loans charge high fees if you don’t make your repayments, which means you could be charged if you don’t budget carefully.
На сайте https://1080kino.net/ можете смотреть лучшие фильмы онлайн абсолютно бесплатно в хорошем качестве. Организуйте себе прекрасный отдых, чтобы отвлечься от повседневных забот. Мы собрали для вас большую коллекцию фильмов разных жанров. Часто обновляем контент, смотрите новинки прямо сейчас. Фильмы увлекут вас захватывающим сюжетом и разнообразными событиями. Добавляйте наш развлекательный портал в закладки для того, чтобы следить за выходом интересного кино.
https://blacksprut-sait.top – блек спрут онион, blacksprut onion
блэкспрут 2fa – blacksprut onion, blacksprut даркнет
блэкспрут ссылка – спрут как попасть на сайт, blacksprut onion
the anticipation building as the plane climbs higher. The key is to cash out at the right moment before the
aviator game
https://bs4shop.top – блэкспрут сайт, блек спрут онион
Привет!
Где приобрести диплом специалиста?
Заказать диплом ВУЗа.
Цена значительно ниже нежели довелось бы заплатить на очном обучении в университете
http://unnewsusa.com/bbs/board.php?bo_table=free&wr_id=2229467
Успешной учебы!
блек спрут онион – блэкспрут сайт, blacksprut onion
Здравствуйте!
Где заказать диплом по нужной специальности?
Готовый диплом с приложением отвечает требованиям и стандартам Министерства образования и науки, неотличим от оригинала – даже со специальным оборудованием. Не откладывайте свои цели на долгие годы, реализуйте их с нами – отправляйте заявку на диплом прямо сейчас!
Купить диплом ВУЗа.
https://cpamafia.pro/threads/kupit-diplom-o194c.13062/
https://forum.moi-psihoanalitik.ru/index.php?/topic/5676-%D0%BA%D0%B0%D0%BA-%D1%81%D0%BE%D0%B7%D0%B4%D0%B0%D1%82%D1%8C-%D0%BD%D0%BE%D0%B2%D1%83%D1%8E-%D1%82%D0%B5%D0%BC%D1%83-forummoi-psihoanalitikru/page/9/#comment-7758
http://minimoo.eu/index.php/en/forum/welcome-mat/663580-gosznacdiplomy
http://www.senbernar.ru/profile/11157-obudytefe/
http://www.youngwooapt.co.kr/bbs/board.php?bo_table=free&wr_id=370732
Хорошей учебы!
На сайте https://mees.com.ru/ вы сможете ознакомиться со всей необходимой безработному, студенту, школьнику информацией, которая касается поиска работы, интересных вакансий. Здесь размещают резюме соискатели, заинтересованные в поиске проверенных, опытных кадров, которые желают трудиться и зарабатывать деньги. Здесь сможет отыскать для себя работу специалист с различным опытом работы или даже без нее. При необходимости вы сможете подписаться на рассылку для того, чтобы получать самые интересные вакансии. Они обновляются регулярно.
Привет!
Мы предлагаем дипломы любой профессии по выгодным ценам.
Мы можем предложить документы ВУЗов, которые находятся в любом регионе России. Можно приобрести качественный диплом за любой год, включая сюда документы старого образца СССР. Документы делаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и штампами.
Где купить диплом специалиста?
https://andreieusebiu.net/files/file/44-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%B9-%D0%B0%D1%81%D1%81%D0%BE%D1%80%D1%82%D0%B8%D0%BC%D0%B5%D0%BD%D1%82-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
User Experience and Reviews
aviator game
блэкспрут darknet – блэкспрут 2fa, блэкспрут ссылка тор
Здравствуйте!
Где купить диплом специалиста?
Мы предлагаем дипломы любых профессий по приятным ценам. Стоимость зависит от той или иной специальности, года получения и образовательного учреждения.
Приобрести диплом любого ВУЗа
https://arusak-diploms-srednee.ru/kupit-diplom-v-kazani
Успешной учебы!
блэк спрут ссылка – blacksprut onion, блэкспрут 2fa
Double Play will apply to all panels, like Speedy Choose selections
and Advance Play.
My web blog; 파워볼 게임몬
https://blacksprut-sait.top/ – спрут как попасть на сайт, блэкспрут сайт
reputable online platforms that ensure safety and fair play.
aviator game
блэкспрут darknet – blacksprut onion, blacksprut даркнет
На сайте https://avto-lombard42.ru/ есть возможность рассчитать займ на специальном калькуляторе, который работает в режиме реального времени. Ломбард работает в круглосуточном режиме, а потому воспользоваться услугами вы сможете в любое время. Здесь вы сможете получить займ под залог ПТС, выкупаются машины самых разных марок. Для того чтобы получить необходимую сумму, следует связаться со специалистом по телефону, уточнить все нюансы. Оценщики произведут осмотр автомобиля, после чего назначат стоимость.
Привет, друзья!
Где приобрести диплом специалиста?
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по доступным тарифам. Стоимость может зависеть от выбранной специальности, года выпуска и университета. Всегда стараемся поддерживать для покупателей адекватную политику цен.
https://www.ozersk74.ru/communication/forum/?PAGE_NAME=profile_view&UID=68456
Удачи!
Швеллер: Применение, Виды и Преимущества
Что такое швеллер?
Швеллер — это металлический профиль, имеющий П-образное сечение. Он широко используется в строительстве, машиностроении и других отраслях благодаря своей прочности, устойчивости к нагрузкам и универсальности. Швеллеры могут быть изготовлены из различных материалов, включая сталь, алюминий и другие сплавы.
Виды швеллеров
Существует несколько основных видов швеллеров, различающихся по методу производства и назначению:
1. Горячекатаный швеллер: Производится путем прокатки стальных заготовок при высоких температурах. Характеризуется высокой прочностью и используется в строительстве крупных сооружений.
2. Гнутый швеллер: Изготавливается методом холодной гибки стальных листов. Менее прочный по сравнению с горячекатаным, но обладает большей гибкостью и подходит для более легких конструкций.
3. Алюминиевый швеллер: Легкий и устойчивый к коррозии, что делает его идеальным для использования в условиях повышенной влажности или агрессивных сред.
Применение швеллеров
Швеллеры находят широкое применение в различных областях благодаря своей универсальности и надежности:
1. Строительство: Используются в каркасах зданий, мостах, перекрытиях и других конструкциях, где требуется высокая прочность и устойчивость к нагрузкам.
2. Машиностроение: Применяются в производстве станков, автомобилей, вагонов и других механизмов, где важны жесткость и устойчивость к деформациям.
3. Инфраструктура: Используются в строительстве железных дорог, трубопроводов и других инфраструктурных объектов.
4. Декоративное и промышленное строительство: Швеллеры могут использоваться в создании декоративных элементов, лестниц, ограждений и других конструкций.
Преимущества использования швеллеров
Использование швеллеров в строительстве и других областях имеет ряд преимуществ:
1. Высокая прочность: Швеллеры способны выдерживать значительные нагрузки, что делает их незаменимыми в строительстве и машиностроении.
2. Универсальность: Благодаря разнообразию видов и размеров, швеллеры можно использовать в самых разных проектах и конструкциях.
3. Устойчивость к деформациям: П-образная форма обеспечивает высокую жесткость и устойчивость к изгибам и деформациям.
4. Долговечность: Швеллеры из стали и алюминия обладают высокой устойчивостью к коррозии и другим воздействиям, что обеспечивает длительный срок службы.
Заключение
Швеллер — это незаменимый элемент в строительстве и машиностроении, обеспечивающий прочность, надежность и долговечность конструкций. Благодаря разнообразию видов и размеров, швеллеры находят широкое применение в различных областях, от крупных инфраструктурных проектов до мелких декоративных элементов. Выбирая швеллеры для своих проектов, вы можете быть уверены в их качестве и надежности.
http://www.allshveller.ru/
Швеллер: Что это такое и где используется?
Швеллер — это металлический профиль, который обладает высокой
прочностью и жесткостью, благодаря чему находит широкое
применение в различных отраслях строительства и промышленности. Он представляет собой П-образный профиль, изготовленный из стали, алюминия или других металлов, и используется для создания каркасов, опорных конструкций и других элементов, требующих повышенной прочности.
Виды и классификация швеллеров
Швеллеры классифицируются по нескольким параметрам,
включая материал изготовления, метод производства и
геометрические характеристики. Основные виды швеллеров
включают:
1. Горячекатаные швеллеры:
– Изготавливаются методом горячей прокатки.
– Обладают высокой прочностью и устойчивостью к деформациям.
– Применяются в тяжелом строительстве и машиностроении.
2. Холодногнутые швеллеры:
– Производятся путем гибки металлических листов.
– Легче и дешевле в производстве по сравнению с горячекатаными аналогами.
– Используются в легких конструкциях и для декоративных целей.
3. Алюминиевые швеллеры:
– Изготавливаются из алюминия, что делает их легкими и устойчивыми к коррозии.
– Применяются в строительстве, где важен легкий вес и долговечность.
4. Нержавеющие швеллеры:
– Изготавливаются из нержавеющей стали.
– Обладают высокой устойчивостью к коррозии и химическим воздействиям.
– Используются в агрессивных средах и пищевой промышленности.
Применение швеллеров
Швеллеры находят применение в самых различных областях благодаря своим уникальным характеристикам. Основные сферы использования включают:
1. Строительство:
– Каркасы зданий и сооружений.
– Балки и перекрытия.
– Опорные конструкции и фермы.
2. Машиностроение:
– Рамы и шасси транспортных средств.
– Конструктивные элементы промышленных машин и оборудования.
3. Металлоконструкции:
– Производство мостов и эстакад.
– Элементы инженерных сооружений.
4. Промышленное оборудование:
– Рамы и каркасы станков.
– Поддерживающие конструкции для оборудования.
Преимущества использования швеллеров
Использование швеллеров в строительстве и промышленности имеет множество преимуществ:
1. Высокая прочность:
– Швеллеры способны выдерживать значительные нагрузки, что делает их незаменимыми в строительстве крупных объектов.
2. Устойчивость к деформациям:
– Благодаря П-образному профилю, швеллеры обладают высокой жесткостью и устойчивостью к изгибам и деформациям.
3. Универсальность:
– Швеллеры могут использоваться в различных сферах, от строительства до машиностроения.
4. Долговечность:
– Швеллеры, особенно изготовленные из нержавеющей стали или алюминия, обладают высокой устойчивостью к коррозии и долговечностью.
Заключение
Швеллеры — это незаменимый элемент в современном строительстве и промышленности.
Благодаря своим уникальным характеристикам, таким как высокая
прочность, жесткость и устойчивость к деформациям, они
обеспечивают надежность и долговечность конструкций.
Независимо от сферы применения, использование швеллеров
позволяет создавать надежные и устойчивые конструкции,
способные выдерживать значительные нагрузки и обеспечивать
безопасность эксплуатации.
http://www.allshveller.ru/
https://bs4shop.top/ – блэк спрут ссылка, блэкспрут darknet
Швеллер: Надежный и Универсальный Строительный Материал
Швеллер – это один из наиболее востребованных и универсальных строительных материалов,
широко используемых в различных областях строительства и промышленности. Благодаря
своей форме и прочностным характеристикам, швеллеры находят применение в каркасном
строительстве, машиностроении, мостостроении и многих других сферах. В этой статье
мы рассмотрим основные особенности швеллера, его виды и области применения.
Что такое швеллер?
Швеллер представляет собой металлическую балку с П-образным профилем, которая изготовлена из стали
путем горячего проката или гибки. Эта форма придает швеллеру высокую жесткость и устойчивость к
нагрузкам, что делает его незаменимым материалом для различных конструкций.
Виды швеллеров
Швеллеры различаются по способу изготовления, размеру и типу профиля. Основные виды швеллеров
включают:
1. Горячекатаные швеллеры: Изготавливаются методом горячей прокатки, что обеспечивает
высокую прочность и однородность материала. Применяются в тяжелых конструкциях,
таких как мосты и здания.
2. Гнутые швеллеры: Производятся методом гибки листового металла. Они легче горячекатаных
швеллеров и чаще используются в легких конструкциях.
3. Швеллеры с параллельными полками: Обеспечивают равномерное распределение нагрузки и
используются в тех конструкциях, где требуется высокая устойчивость.
4. Швеллеры с уклоном внутренних граней полок: Этот тип швеллера имеет уклон полок внутрь,
что придает дополнительную жесткость и позволяет использовать их в специфических конструкциях.
Области применения швеллеров
Благодаря своим уникальным характеристикам, швеллеры находят широкое применение в различных отраслях:
1. Строительство: Швеллеры используются для создания каркасов зданий, мостов, опор и других конструкций,
требующих высокой прочности и устойчивости.
2. Машиностроение: Применяются в производстве различных машин и механизмов, где важны жесткость
и устойчивость к деформациям.
3. Автомобилестроение: Используются для изготовления рам и других несущих конструкций автомобилей.
4. Судостроение: Швеллеры применяются в создании каркасов судов и других морских конструкций.
5. Энергетика: Используются в строительстве опор линий электропередач и других энергетических сооружений.
Преимущества использования швеллеров
Использование швеллеров в строительстве и промышленности имеет ряд преимуществ:
– Прочность и устойчивость: П-образный профиль обеспечивает высокую жесткость и устойчивость к нагрузкам.
– Универсальность: Швеллеры могут использоваться в различных конструкциях и областях.
– Легкость монтажа: Простота и удобство при сборке конструкций.
– Долговечность: Швеллеры изготавливаются из высококачественной стали, что обеспечивает долгий срок службы.
Заключение
Швеллер – это незаменимый материал в современном строительстве и промышленности. Его уникальные характеристики и разнообразие видов позволяют использовать его в самых различных областях, обеспечивая надежность и долговечность конструкций. При выборе швеллера важно учитывать требования конкретного проекта и консультироваться с специалистами для достижения наилучших результатов.
Использование швеллеров в строительстве и промышленности продолжает расти, и этот материал неизменно остается одним из ключевых элементов, обеспечивающих прочность и надежность различных конструкций.
http://www.allshveller.ru/
Привет, друзья!
Где купить диплом специалиста?
Купить документ ВУЗа можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы получите диплом по любой специальности, включая документы образца СССР. Гарантируем, что при проверке документов работодателями, подозрений не возникнет.
http://giaibngdaquocteu23.com/2021-10-cb-hay-trong-trong-fifa-online-4-hien-nay-keo8386/
Удачи!
The ability to play from anywhere, coupled with the variety of games available, has attracted millions of
aviator game
https://24smski.ru
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в рязани, купить диплом психолога, купить диплом о высшем образовании, куплю диплом цена , купить диплом в ревде и получил базовые знания. В итоге остановился на материале: http://old.trudcher.ru/users.php?m=details&id=16046
Удачи!
7slots Nedir?
7slots, cevrimici kumarhaneler ve slot makineleri dunyas?nda onemli bir yere sahip olan bir platformdur. Bu makalede, 7slots’un ne oldugunu, nas?l cal?st?g?n? ve neden bu kadar populer oldugunu inceliyoruz.
7slots’un Tan?m? ve Amac?
<a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"7slots oyunculara cesitli slot oyunlar? sunan bir cevrimici kumar platformudur. Cesitli temalar, grafikler ve bonus ozellikler sunarak oyunculara heyecan verici bir oyun deneyimi saglamay? hedefler. Hem yeni baslayanlar hem de deneyimli oyuncular icin genis bir oyun yelpazesi sunar.
Nas?l Cal?s?r?
7slots, kullan?c?lar?n hesap acarak para yat?rabilecegi ve bu bakiyeyi kullanarak <a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"7slots bonus oyunlar? oynayabilecegi bir sistemle cal?s?r. Oyuncular, kazand?klar?nda bakiyelerinden cekebilirler. Platformda sunlar bulunur:
Cesitli Slot Oyunlar?: Farkl? temalara <a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"casino 7slots ve kurallara sahip slot oyunlar?.
Bonus ve Promosyonlar: Yeni ve mevcut oyuncular icin bonus teklifleri.
Guvenli Odeme Secenekleri: H?zl? <a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"7slots giris ve guvenli para yat?rma ve cekme yontemleri.
One C?kan Ozellikler
7slots’un one c?kan baz? ozellikleri sunlard?r:
Genis Oyun Yelpazesi: Her zevke <a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"7slots casino hitap eden yuzlerce slot oyunu.
Mobil Uyumluluk: Hem masaustu hem de mobil cihazlarda oynanabilir.
Guvenlik ve Gizlilik: Oyuncu <a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"7slots casino giris verilerinin korunmas? ve finansal islemlerde guvenlik.
Kullan?c? Dostu Arayuz: Kolay navigasyon ve oyun erisimi.
Neden Bu Kadar Populer?
7slots’un popularitesinin <a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"7slots para cekme ana nedenleri aras?nda sunlar bulunur:
Heyecan Verici Oyunlar: Ozellikle buyuk kazanma sans? sunan jackpotlu oyunlar.
Erisilebilirlik: Internet <a href="https://groups.google.com/u/2/g/7slots-7slots/c/y4vZQVwudWE"7slots casino guncel giris baglant?s? olan her yerden erisilebilir.
Topluluk ve Destek: Canl? destek hizmetleri ve oyuncular aras? etkilesim.
Surekli Guncellemeler: Yeni oyunlar ve ozelliklerle surekli yenilenme.
advancements have allowed for improved graphics, smoother gameplay, and more interactive features. These
aviator game
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в самаре, купить диплом в чебоксарах, купить диплом университета, купить диплом в ульяновске, купить диплом геодезиста. Постепенно углубляясь, нашел отличный ресурс здесь: https://xn--viagrailmanresepti-2tb.com/2021/01/11/dht-blocker-propecia-taman-paivan-hoito-miesten-hiustenlahtoon/, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
Привет!
Где заказать диплом по актуальной специальности?
Приобрести документ университета вы можете у нас в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы СССР. Гарантируем, что в случае проверки документов работодателями, каких-либо подозрений не возникнет.
http://ya.9bb.ru/viewtopic.php?id=4177#p8837
Успешной учебы!
Добрый день!
Где приобрести диплом по актуальной специальности?
Купить документ ВУЗа можно в нашей компании. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить диплом по любым специальностям, любого года выпуска, включая документы старого образца. Гарантируем, что в случае проверки документов работодателями, подозрений не возникнет.
Мы предлагаем выгодно и быстро заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Документ способен пройти любые проверки, даже при помощи специально предназначенного оборудования. Решайте свои задачи максимально быстро с нашим сервисом.
http://203.195.186.190/space-uid-334321.html
http://elviraobol.ru/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=388
https://www.roxgo.cl/gallery/image/4179-%D1%82%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%8B%D0%B1%D0%B8%D1%80%D0%B0%D0%B9%D1%82%D0%B5-%D0%BD%D0%B0%D1%88-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD/
http://pspgn.bestbb.ru/viewtopic.php?id=230
https://zdsim.ru/wiki/index.php/%D0%93%D0%B4%D0%B5_%D0%BB%D1%83%D1%87%D1%88%D0%B5_%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%3F_%D0%A1%D0%BE%D0%B2%D0%B5%D1%82%D1%8B_%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в таганроге, купить диплом в братске, купить диплом в москве, купить диплом в пятигорске, купить диплом инженера строителя, потом попал на https://batinmarket.ru/products/dhea-100-kaps-25-mg/#comment_687 и там решили все мои учебные заботы!
Удачи!
Здравствуйте!
Где купить диплом специалиста?
Мы можем предложить документы техникумов, которые находятся в любом регионе России. Документы заверяются всеми требуемыми печатями и подписями.
http://goldankauf-engelskirchen.de/out.php?link=https://sx-diplom.com/
Успешной учебы!
Привет!
Для определенных людей, заказать диплом о высшем образовании – это острая потребность, уникальный шанс получить выгодную работу. Впрочем для кого-то – это осмысленное желание не терять время на учебу в институте. С какой бы целью вам это не понадобилось, наша компания готова помочь вам. Быстро, качественно и недорого изготовим документ любого года выпуска на государственных бланках со всеми подписями и печатями.
Мы предлагаем выгодно купить диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями. Диплом способен пройти любые проверки, даже с использованием специальных приборов. Достигайте цели максимально быстро с нашими дипломами.
Основные преимущества наших документов:
• используются только фирменные бланки “Гознак”;
• необходимые подписи руководства;
• настоящие печати учебного заведения;
• специальные водяные знаки, нити и другие степени защиты;
• безупречное заполнение и оформление – ошибки исключены;
• любая проверка документов.
Где приобрести диплом по необходимой специальности?
http://www.markusragger.at/chess/index.php/kforum/jm-news-pro-module/577466
Успешной учебы!
Привет, друзья!
Для некоторых людей, приобрести диплом о высшем образовании – это острая потребность, уникальный шанс получить достойную работу. Но для кого-то – это желание не терять время на учебу в университете. С какой бы целью вам это не понадобилось, мы готовы помочь вам. Максимально быстро, качественно и по разумной цене сделаем диплом нового или старого образца на подлинных бланках с реальными печатями.
Заказать документ ВУЗа можно у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что при проверке документов работодателем, подозрений не возникнет.
О преимуществах наших документов:
• используются настоящие бланки “Гознак”;
• оригинальные подписи должностных лиц;
• настоящие печати ВУЗа;
• водяные знаки, нити и иные степени защиты;
• идеальное заполнение и оформление – ошибок не будет;
• любая проверка оригинальности документа.
Наша компания предлагает выгодно купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Данный документ способен пройти любые проверки, даже при помощи специальных приборов. Решите свои задачи быстро и просто с нашими дипломами.
Где заказать диплом по актуальной специальности?
http://b98415ql.bget.ru/index.php?subaction=userinfo&user=yfaquvy
http://malenkajastrana.ru/index.php?subaction=userinfo&user=egofyhy
http://forum.infinite-soul.org/viewtopic.php?f=64&t=16412&p=55837#p55837
http://tr.clanfm.ru/viewtopic.php?f=39&t=10093&p=20006#p20006
http://longlive.com/node/1381
Удачи!
The Aviator Game is an exciting online casino game that has captivated players worldwide with its unique blend
aviator game
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в златоусте, купить диплом товароведа, купить диплом товароведа, купить свидетельство о рождении ссср, купить диплом штукатура, потом про дипломы вузов, подробнее здесь https://onetierra.mx/blog/el-cuidado-de-tu-flota-un-acto-de-solidaridad/
https://mdcatguide.com.pk/pmc-merit-list/
http://torica.4adm.ru/viewtopic.php?f=6&t=1996
http://www.biyolokum.com/2009/04/abdde-doga-sporu/#comment-623010
http://stokrat.com/offroad/43/#comments
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успешной учебы!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в ижевске, купить диплом инженера по охране труда, купить диплом в ухте, купить диплом в ульяновске, куплю диплом. Постепенно углубляясь, нашел отличный ресурс здесь: http://bestworld.getbb.ru/viewtopic.php?f=8&t=1215
http://forums.worldsamba.org/search.php
https://4atex.ru/blogs/2073/ѕолучите-?иплом-Ѕыстро-и-Ќадежно
http://newrealgames.ru/kupit-diplom-byistro-i-nadezhno
http://leydis16.phorum.pl/posting.php?mode=newtopic&f=1
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом электрика, купить диплом лаборанта, купить диплом в березниках, купить диплом в туапсе, купить диплом в нижнем тагиле, а потом наткнулся на http://forummsk.getbb.ru/viewtopic.php?f=11&t=2163, где все мои учебные проблемы были решены!
Удачи!
Rotten Tomatoes’ Best Movies on Netflix for June 2024 latest tmnt movie1923 episodes 2blue lagoon film series where to watchjack sochet movies
С промокодами Vavada казино можно получить дополнительные бонусы и фриспины, что делает игровой процесс более интересным и выгодным для всех участников. Vavada казино бонусы помогут вам выиграть.
Аккумулятор пришел быстро, качество на высоте. Спасибо!
аккумуляторы оптом
Супер обслуживание, аккумулятор доставили за день. Молодцы!
аккумулятор автомобильный 90 ач
Промокоды Drip казино открывают новые возможности для игроков, предоставляя дополнительные бонусы и фриспины. Drip казино бонусы помогут вам наслаждаться игрой.
read the article how to hack roblox
their website how to get hacks on fortnite
В Vavada казино промокоды открывают новые возможности для получения бонусов и фриспинов, увеличивая шансы на выигрыш. Vavada казино промокоды сделают игру захватывающей.
Origins of the Aviator Game
aviator game
Хотите погрузиться в мир новых захватывающих историй? На сайте turkishclub.tv вас ждут турецкие сериалы 2024 онлайн. Самые свежие премьеры нового года уже доступны для просмотра в высоком HD качестве. Встречайте любимых героев и открывайте для себя новые сюжеты без рекламы и с профессиональной озвучкой.
Присоединяйтесь к тысячам зрителей, которые уже оценили удобство и качество turkishclub.tv. Не пропустите возможность первыми увидеть новинки турецкого кинематографа 2024 года. Наслаждайтесь просмотром онлайн!
cs2 skinchanger – cs2 skin changer free download, skin changer cs 2
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в каменске-уральском, купить диплом в георгиевске, купить диплом в евпатории, купить диплом в ленинск-кузнецком, купить диплом в кузнецке, постепенно вникая в суть дела нашел отличный материал здесь https://piter.liveforums.ru/viewtopic.php?id=5049#p11335
https://noginsk.build2.ru/viewtopic.php?id=7253#p16998
https://tonirovkaforum.bestff.ru/viewtopic.php?id=2565#p14026
https://www.bideew.com/read-blog/4504
https://news-life.pro/moscow/373449339/
и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Удачи!
Financial robot is your success formula is found. Learn more about it. https://t.me/cryptaxbot/17?fruttyVet61Bus
read this galaxy swapper fortnite
Visit the website https://gate-a-door.com/ where you can order installation and repair of all types of garage doors and gates. More than 10 years of experience, individual design, guarantee for all services. Electric, automatic, swing, sliding gates and a full range of maintenance services! Visit the website.
http://autoexpert-group.ru/
Online Platforms Offering the Game
aviator game
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
last news about muller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
mueller
<a href=http://events.oldiestation.es/php.php?a=mueller
mueller
Добрый день!
Для некоторых людей, заказать диплом ВУЗа – это острая потребность, шанс получить достойную работу. Впрочем для кого-то – это понятное желание не терять время на учебу в ВУЗе. Что бы ни толкнуло вас на такой шаг, наша фирма готова помочь. Максимально быстро, качественно и выгодно сделаем документ любого ВУЗа и любого года выпуска на государственных бланках с реальными подписями и печатями.
Заказать документ о получении высшего образования можно у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, любого года выпуска, включая документы СССР. Даем 100% гарантию, что в случае проверки документов работодателями, подозрений не возникнет.
Превосходства наших документов:
• используем настоящие бланки “Гознака”;
• необходимые подписи руководства;
• мокрые печати ВУЗа;
• специальные водяные знаки, нити и иные степени защиты;
• идеальное качество оформления – ошибки исключены;
• любые проверки документа.
Наша компания предлагает быстро купить диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями должностных лиц. Наш диплом способен пройти любые проверки, даже при помощи профессионального оборудования. Достигайте своих целей быстро и просто с нашим сервисом.
Где заказать диплом по актуальной специальности?
https://bestallorder.nethouse.ru/articles/esli-vy-zhelaete-kupit-diplom-v-saratove
https://blogs.rufox.ru/~runoklisfgy/47401.htm
http://www.bisound.com/forum/showthread.php?p=715194#post715194
http://a-bcd.ru/news/201718/
https://ironway.ru/forum/viewtopic.php?f=12&t=12393&p=25288#p25288
Удачи!
Здравствуйте!
Для многих людей, заказать диплом ВУЗа – это необходимость, уникальный шанс получить достойную работу. Впрочем для кого-то – это очевидное желание не терять время на учебу в институте. Что бы ни толкнуло вас на такой шаг, мы готовы помочь. Максимально быстро, качественно и выгодно изготовим документ нового или старого образца на подлинных бланках со всеми подписями и печатями.
Наши специалисты предлагают выгодно и быстро заказать диплом, который выполняется на оригинальной бумаге и заверен печатями, штампами, подписями. Данный диплом способен пройти любые проверки, даже при использовании специфических приборов. Достигайте свои цели максимально быстро с нашими дипломами.
Преимущества наших документов:
• используются только качественные бланки “Гознака”;
• подлинные подписи руководства;
• мокрые печати ВУЗа;
• водяные знаки, нити и иные степени защиты;
• идеальное качество оформления – ошибки полностью исключены;
• любые проверки документа.
Где купить диплом специалиста?
http://collie.fatbb.ru/viewtopic.php?f=18&t=3826
Успехов в учебе!
cs2 hack – cs2 hacks, undetek cs2 cheat
For beginners, the key to success in the Aviator Game is to start with small bets and gradually increase as you
aviator game
Хотите приобрести интересные сериалы на DVD? Serialexpress вам с этим поможет. У нас есть диски, которых вы ни в одном магазине не найдете. Качество сериалов отличное, вы точно останетесь довольны покупкой. Товары в доступе по приемлемой цене, они упакованы очень хорошо. https://serialexpress.ru – портал, где имеется каталог, здесь можете ознакомиться и с оплатой. У нас действует накопительная система скидок. Качество доставки вас удивит. Есть вопросы? Не стесняйтесь обращаться к нашим менеджерам.
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в каменске-уральском, купить диплом медицинского училища, купить диплом в первоуральске, купить диплом в ленинск-кузнецком, купить диплом россия, потом попал на http://starterkit.ru/html/index.php?name=account&op=info&uname=amopoqa и там решили все мои учебные заботы!
Успехов в учебе!
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: куплю диплом высшего образования, купить диплом в кисловодске, купить диплом в тюмени, купить диплом в калуге, купить диплом в ростове и получил базовые знания. В итоге остановился на материале: https://rsn360.ru/blogs/320/????????????-???????????-????-??????-???????-??????????-????-????????????
http://3arabotok.topbb.ru/post.php?fid=15
https://ic-info.ru/forum/user/165173/
http://pro-novostroyki.ru/index.php?showtopic=20812
https://forum.mybb.ru/viewtopic.php?id=38567#p939931
Успехов в учебе!
Future of the Aviator Game
aviator game
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить дипломы о высшем, купить диплом в химках, купить диплом в воронеже, купить диплом в грозном , купить диплом в орле и получил базовые знания. В итоге остановился на материале: https://sponforum.ixbb.ru/viewtopic.php?id=10359#p35107
https://poetzinc.com/read-blog/8403
http://peaceofficial.5nx.ru/viewtopic.php?f=111&t=736
https://slingomama74.bbeasy.ru/viewtopic.php?id=3923#p9390
http://transexit.g-talk.ru/viewtopic.php?f=10&t=1791
Хорошей учебы!
Ваша любовь к загадкам и тайнам найдет удовлетворение на turkishclub.tv, где доступны турецкие сериалы детективы. Здесь каждый эпизод – это новое расследование, полное интриг и неожиданных поворотов. Наши сериалы в высоком 720 HD качестве и с русским переводом помогут вам погрузиться в мир детективных историй, где каждая деталь имеет значение.
Конечно, что может быть лучше, чем наслаждаться этими расследованиями без рекламы? На turkishclub.tv вы можете смотреть детективы бесплатно и без перерывов. Новые серии появляются каждый день, чтобы вы всегда были в курсе свежих событий. Откройте для себя мир турецких детективов прямо сейчас и ощутите настоящий драйв!
useful link
nexus market dark web
about his
Sipulitie link
I really like it when individuals get together and share views.
Great blog, keep it up!
Here is my page … sumbawatoto
This is the perfect webpage for anyone who wants to
find out about this topic. You know a whole lot its almost tough to argue with you (not that I
personally will need to…HaHa). You certainly put a brand new spin on a topic that’s
been discussed for years. Wonderful stuff, just wonderful!
Here is my site – sumbawatoto
Having read this I believed it was extremely enlightening.
I appreciate you finding the time and effort to put this content together.
I once again find myself personally spending a lot of time
both reading and posting comments. But so what, it was still worthwhile!
Also visit my webpage; pentastogel
Hi there to every one, it’s truly a nice for me to go to see this web site,
it consists of priceless Information.
Feel free to surf to my web page: 十和田市
blog here
abacus market url
best site
vortex darkmarket
Software Requirements
aviator game
I’m not that much of a online reader to be honest but your sites really nice, keep it up!
I’ll go ahead and bookmark your site to come back later
on. Many thanks
Feel free to surf to my blog :: pentastogel
That is a great tip particularly to those fresh to the blogosphere.
Simple but very accurate info… Appreciate your sharing this one.
A must read article!
Also visit my homepage :: CCcam
Здравствуйте!
Мы предлагаем выгодно и быстро купить диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями официальных лиц. Документ способен пройти лубую проверку, даже при использовании профессионального оборудования. Решайте свои задачи максимально быстро с нашим сервисом.
Где заказать диплом по необходимой специальности?
https://www.liveinternet.ru/users/worksale/post505780358/
Хорошей учебы!
My partner and I stumbled over here from a different website and thought
I should check things out. I like what I see so i am
just following you. Look forward to looking over your web page again.
Here is my site; sumbawatoto
Hi! I know this is kinda off topic but I was wondering if you knew
where I could find a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having difficulty finding one?
Thanks a lot!
My webpage; sumbawatoto
Robot never sleeps. It makes money for you 24/7.] https://t.me/cryptaxbot/17?fruttyVet26Bus
I’m impressed, I must say. Seldom do I encounter a
blog that’s equally educative and interesting, and without
a doubt, you have hit the nail on the head. The issue is something too few folks are speaking intelligently about.
I am very happy that I came across this in my search for something concerning
this.
Also visit my web-site – pentastogel
Greetings from Carolina! I’m bored to tears at work so I
decided to browse your blog on my iphone during lunch break.
I love the knowledge you present here and can’t wait to take a look when I get home.
I’m amazed at how quick your blog loaded on my phone
.. I’m not even using WIFI, just 3G .. Anyways, amazing blog!
Feel free to visit my homepage – 十和田市
Post writing is also a excitement, if you know after that you can write or else it is complex to write.
My web blog :: sumbawatoto
Hey there, I think your site might be having browser compatibility issues.
When I look at your blog in Chrome, it looks fine but when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up!
Other then that, terrific blog!
Visit my homepage sumbawatoto
Хотите погрузиться в мир новых захватывающих историй? На сайте turkishclub.tv вас ждут турецкие сериалы 2024 онлайн. Самые свежие премьеры нового года уже доступны для просмотра в высоком HD качестве. Встречайте любимых героев и открывайте для себя новые сюжеты без рекламы и с профессиональной озвучкой.
Присоединяйтесь к тысячам зрителей, которые уже оценили удобство и качество turkishclub.tv. Не пропустите возможность первыми увидеть новинки турецкого кинематографа 2024 года. Наслаждайтесь просмотром онлайн!
reputable online platforms that ensure safety and fair play.
aviator game
I know this web page provides quality depending articles or reviews and
other material, is there any other web page which offers such
things in quality?
My website: winter4d
Hi there i am kavin, its my first occasion to commenting anywhere, when i read this piece of writing
i thought i could also make comment due to
this sensible article.
my web blog … sumbawatoto
The Dota 2 website https://dota2-kz.kz provides the most complete information about the latest game updates, tournaments and upcoming events. We are here for every winning tactic, secret and important guide.
http://avansir.ru/
Game World online https://games-online-eg.com the latest online gaming news, game reviews, gameplay, ideas, gaming tactics and tips. The most popular and amazing games and get ready to become the leader in the online gaming world!
Особенности первых родов, Близнецы в утробе матери, Путешествия во время беременности, ЭКО, Диагностика подтекания околоплодных вод
Улучшение психофизического и эмоционального состояния
I loved as much as you will receive carried out right here.
The sketch is attractive, your authored material stylish. nonetheless,
you command get got an nervousness over that you wish
be delivering the following. unwell unquestionably come more formerly again as exactly the same nearly very often inside case you shield this
increase.
Look into my web-site: sumbawatoto
This is a very good tip particularly to those new to the blogosphere.
Brief but very accurate information… Many thanks for sharing this one.
A must read article!
Are There Any Costs Involved?
aviator game
Нужен срочный займ и хотите получить его под 0%? ZAIM-VSEM.ONLINE предлагает подборку МФО 2024 года, которые предоставляют первый займ под 0% до 30 тысяч рублей. На нашем сайте вы найдете множество вариантов от надежных микрофинансовых организаций.
ZAIM-VSEM.ONLINE также предоставляет обширную информацию о том, как правильно оформить займ и выбрать подходящую МФО. Мы делаем процесс получения займа быстрым и удобным. Получите займ на карту без отказа и решите свои финансовые проблемы с выгодой!
Привет!
Наши специалисты предлагают выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Наш диплом способен пройти любые проверки, даже с использованием профессионального оборудования. Достигайте своих целей быстро и просто с нашими дипломами.
Где заказать диплом специалиста?
http://rulezrp.listbb.ru/ucp.php?mode=login&sid=5512acd74ae99f73262a59c9ea2864e2
Хорошей учебы!
How to Start Playing the Aviator Game?
aviator game
Не упустите промокоды Vavada казино, чтобы получить бонусы на депозиты и фриспины. Воспользуйтесь нашими предложениями и увеличьте свои шансы на выигрыш.
Can I Play the Aviator Game on Mobile?
aviator game
porno teens 2021
http://tessalyons.co.uk/?URL=https://anal2tube.xyz/
https://the-thao-so.sitey.me/s/cdn/?https://anal2tube.xyz/
https://auth.acog.org/createaccount?returnUrl=https%3A%2F%2Fxteentube.xyz&authRequestId=7375b828-4944-4c92-9556-472b6c2cba85
https://dianova.blog.idnes.cz/redir.aspx?url=https://xpornotube.xyz/
https://k-texnik.ru/forum/go.php?url=aHR0cHM6Ly94dGVlbnR1YmUueHl6Lw
https://m.en.edenplaza.co.kr/member/login.html?returnUrl=https://xpornotube.xyz/
https://image.google.com.sl/url?rct=j&sa=t&url=https://xpornotube.xyz/
https://pokupka24.ru:443/bitrix/redirect.php?event1=click_to_call&event2=&event3=&goto=https://anal2tube.xyz/
Ищете актуальные промокоды для Drip казино? Используйте их, чтобы получить дополнительные бонусы и фриспины, и наслаждайтесь игрой с увеличенными шансами на выигрыш.
Воспользуйтесь промокодами Vavada казино и наслаждайтесь дополнительными бонусами и фриспинами при игре. Преимущества для всех игроков.
На сайте https://turkzona.com/ представлены интересные, увлекательные турецкие сериалы, которые точно понравятся всем любителям такого направления. Все фильмы интересные, увлекательные, а самое главное, что представлены в отличном качестве, отличаются четкой картинкой, качественным звуком, что усиливает приятные эмоции от просмотра. Перед вами огромный выбор вариантов фильмов самых разных жанров: мелодрамы, драмы. Для того чтобы подобрать оптимальный вариант, необходимо определиться с годом выпуска.
Здравствуйте!
Мы изготавливаем дипломы любой профессии по выгодным тарифам.
Мы готовы предложить документы техникумов, расположенных в любом регионе Российской Федерации. Можно купить диплом от любого заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригиналов. Они заверяются всеми обязательными печатями и подписями.
Где приобрести диплом по необходимой специальности?
kids-news.ru/page/3
The Aviator Game uses a Random Number Generator (RNG) to ensure fair play. This technology ensures that each
aviator game
dragon movie 2022 film pornograpiundercover boss checkers episodemovies action 2022friday full movie
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в набережных челнах, купить аттестат за 9 классов, купить диплом в минусинске, купить диплом в сыктывкаре, купить диплом в альметьевске, затем наткнулся на http://zanasite.free.fr/laripostedumardi/doku.php?id=premialnie
https://www.knittingideas.ru/posts/add
http://www.52ru.ru/showthread.php?p=37596#post37596
http://school5.p-fam.ru/users/ytofah
http://tv-cifra.ru/blog/izmenenie-uslovij-okazaniya-uslugi-edinyj/
, где все мои учебные вопросы были решены!
Успешной учебы!
The Dota 2 website https://dota2-ar.com provides the most detailed information about the latest game updates, tournaments and upcoming events. We have all the winning tactics, secrets and important guides.
Если вы хотите смотреть турецкие сериалы на русском языке, то turkishclub.tv — это лучший выбор! Почему? Потому что у нас представлен широкий выбор сериалов всех жанров и годов выпуска. Наши пользователи ценят высокое качество HD видео и отсутствие рекламы.
Погружайтесь в мир турецкого кинематографа без лишних хлопот. Удобная навигация по сайту и постоянные обновления делают просмотр максимально комфортным. Присоединяйтесь к сообществу, которое уже оценило все преимущества turkishclub.tv. Смотрите любимые сериалы на русском языке с удовольствием!
Can I Play the Aviator Game on Mobile?
how to grow your penis
Иркутск окна ПВХ fod38.ru
Идеальные по характеристикам и отзывам ПВХ окна изготовляют в данном месте! Приглашаем Вас на Фабрику окон и дверей в Иркутске, чтобы заказать отличные окна ПВХ для вашей квартиры или дома. Мы значимся производителем, поэтому у нас небольшие цены и отличное качество, на которое предоставляется гарантия. Изготовление происходит в максимально быстрые сроки, а также монтажная работа настоящими профессионалами.
На онлайн ресурсе fod38.ru Вы сможете найти всю интересную информацию о данной компании, окнах, контакты и как оформить заказ. Предлагаем 3 варианта ПВХ окон: эконом, стандарт и премиум, где отличительной чертой будет представляться цена/качество. Выбирайте необходимый Вам вариант или получите консультацию от профессионала, какой конкретно сделать выбор в определенном случае.
По вопросу ремонт окон мы непременно Вам поможем. Окна от представленной фабрики являются экологически чистыми, так как в них не содержится свинец. После установки, в комнате будет бесшумно и спокойно, а также надежно для детей, ведь мы делаем ручки с замком. Все стекла с защитой УФ, а также их просто мыть, комфортно проветривать и радужно для глаз.
Если Вы планировали найти заказать пластиковые окна – то переходите на указанный сайт. На сайте fod38.ru можно записаться на бесплатный замер окон. Это самое верное решение, чтобы не терять своё свободное время, потому что договор можно оформить прямо на дому. Замерщик даст ответы на все Ваши вопросы, покажет модели и фотографии, учтет все ваши желания и осуществит безупречный замер с расценками.
Звоните по телефону +7(3952)656-226 или приезжайте в один из офисов, по адресу: г. Иркутск, ул. Байкальская, д. 105 А, оф. 101. Режим работы с пн по пт с 9:00 до 17:30, выходной воскресенье. Звоните, приходите, мы будем рады с Вами сотрудничать.
https://blacksprut-sait.top – блэкспрут сайт, блэк спрут ссылка
http://autolombard-capital.ru/
https://bs4shop.top/ – blacksprut onion, блэкспрут ссылка тор
блэк спрут ссылка – блэкспрут даркнет, блэкспрут ссылка
Safety and Fair Play
do penis pumps work
Центр «Доверие» приглашает вас воспользоваться услугами. Запишитесь к психологу по номеру телефона на сайте. Семейный психолог старается сделать так, чтобы консультации были комфортными для обоих супругов. https://ack-group.ru – сайт, где вы узнаете более детальную информацию. Подростковый психолог выяснит уровень вашей проблемы и подберет подходящий способ ее решения. Цена консультации психолога доступна любому. Психолог в СПБ поможет урегулировать отношения с окружающими и с собой. Обращайтесь в любое время!
На сайте https://vkinogo.net/ можете смотреть интересные фильмы совершенно бесплатно в любое удобное для вас время. Наслаждайтесь увлекательными сюжетами и блестящей игрой актеров. Мы сделали простой и удобный портал. В нашем каталоге представлены все жанры. Выбор фильмов достаточно широк, уверены в том, что у нас вы найдете кино по своему вкусу. Можете прямо сейчас ознакомиться с последними новинками. Не упустите возможность погрузиться в захватывающий мир кино!
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить дипломы о высшем цены, купить диплом ссср, купить диплом стоматолога, купить диплом в набережных челнах , купить диплом в нижнем тагиле и получил базовые знания. В итоге остановился на материале: https://ok-vmeste.ru/toget/1829-kupit-diplom-v-krasnodare.html
Успешной учебы!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в пензе, купить диплом биолога, купить диплом в вольске, купить речной диплом, купить диплом в ульяновске, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://koxma.4adm.ru/viewforum.php?f=296
http://allonlinesport.ru/kupit-diplom-dlya-vashego-uspeha/
https://prof-komplekt.com/club/user/4861/blog/10202/
http://azat.on.kg/blogs/892/«акажите-?иплом-в- ратчайшие-—роки
http://autogroupe.ru/kupit-diplom-legko-i-nadezhno
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Хорошей учебы!
блэкспрут даркнет – блэкспрут ссылка тор, блэкспрут 2fa
my site – https://skgazeta.su
Reputable online platforms offering the Aviator Game are licensed and regulated by governing bodies. This
increase penis size
click for more avax wallet appааа
Financial robot is the best companion of rich people.] https://t.me/cryptaxbot/17?fruttyVet65Bus
his response Atom wallet
Здравствуйте!
Где приобрести диплом по нужной специальности?
Купить диплом университета.
Цена во много раз меньше той, которую довелось бы платить на очном обучении в университете
http://www.sinoright.net/member/index.php?uid=yrowylac
Успешной учебы!
back for more.
how to enlarge penis
На сайте https://spb-gid.ru/ представлена самая исчерпывающая, интересная информация, которая касается Санкт-Петербурга. Здесь освещаются самые последние мероприятия, которые будут происходить в ближайшее время. Есть данные относительно того, в какой ресторан лучше всего сходить. Отмечены самые интересные кафе для того, чтобы отправиться туда с друзьями. Рассматриваются различные варианты жилья, в том числе, хостелы, гостиницы, аренда комнат, квартир. Имеется информация про метро, общественный транспорт, а также железнодорожный.
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в находке, купить аттестат за 9 класс, купить диплом в нижнем новгороде, купить диплом в северодвинске, купить диплом в вологде, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://pokupki.bestforums.org/viewtopic.php?f=30&t=17800
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успешной учебы!
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом в ленинск-кузнецком, купить диплом в пятигорске, купить диплом высшее, купить диплом агронома, купить диплом в ессентуках, получил базовую информацию.
Остановился в итоге на материале где купить диплом, http://g95334gq.beget.tech/2024/05/15/individualnoe-obrazovanie-gde-kupit-diplom-sozdannyy-specialno-dlya-tebya.html
http://doctorsforum.ru/viewtopic.php?f=193&t=38150
https://keepnitreal.net/blogs/65324/ѕолучите-?иплом-Ѕыстро-и-Ќадежно
https://library.kemu.ac.ke/kemuwiki/index.php/??????_??????_??????%3F_??_?????_???_???!
http://mosday.getbb.ru/viewtopic.php?f=12&t=1078
Удачи!
Hello!
Do you want to become the best SEO specialist and link builder or do you want to outpace your competitors?
Premium base for XRumer
$119/one-time
Get access to our premium database, which is updated monthly! The database contains only those resources from which you will receive active links – from profiles and postings, as well as a huge collection of contact forms. Free database updates. There is also the possibility of a one-time purchase, without updating the databases, for $38.
Fresh base for XRumer
$94/one-time
Get access to our fresh database, updated monthly! The database includes active links from forums, guest books, blogs, etc., as well as profiles and activations. Free database updates. There is also the possibility of a one-time purchase, without updating the databases, for $25.
GSA Search Engine Ranker fresh verified link list
$119/one-time
Get access to our fresh database, updated monthly! The fresh database includes verified and identified links, divided by engine. Free database updates. There is also the possibility of a one-time purchase, without updating the databases, for $38.
GSA Search Engine Ranker activation key
$65
With GSA Search Engine Ranker, you’ll never have to worry about backlinks again. The software creates backlinks for you 24 hours a day, 7 days a week. By purchasing GSA Search Engine Ranker from us, you get a quality product at a competitive price, saving your resources.
To contact us, write to telegram https://t.me/DropDeadStudio
The basic rule of the Aviator Game is straightforward: place a bet, watch the plane take off, and decide when to
male enhancement gummies
Bs.gl – Bs2best.at, Bs2tsite4
http://ryazanavto-kia62.ru/
Фабрика окон и дверей в Иркутске fod38.ru
Превосходные по свойствам и стоимости пластиковые окна производят в данном месте! Хотим пригласить Вас на Фабрику окон и дверей в Иркутске, чтобы купить отличные пластиковые окна для вашей квартиры или дачи. Мы являемся производителем, поэтому у нас небольшие цены и отличное качество, на которое предоставляется гарантия. Изготовление происходит в максимально быстрые сроки, а также монтажная работа настоящими профессионалами.
На веб сайте fod38.ru Вы найдете всю важную информацию о нашей компании, окнах, контакты и как оформить заказ. Предлагаем 3 варианта ПВХ окон: эконом, стандарт и премиум, где заметной чертой будет представляться цена/качество. Выбирайте нужный Вам вариант или получите консультацию от профессионала, какой конкретно осуществить выбор в определенном случае.
По вопросу заказать пластиковые окна мы непременно Вам окажем помощь. Окна от представленной фабрики являются экологичными, так как в них не используется свинец. После монтажа, в комнате будет бесшумно и спокойно, а также надежно для детей, ведь мы устанавливаем ручки с замком. Все ПВХ окна с защитой УФ, а ещё их легко мыть, комфортно проветривать и они впишутся в любой дизайн.
Если Вы планировали найти пластиковые окна цена – то переходите на указанный сайт. На сайте fod38.ru можно записаться на бесплатный замер будущих окон. Это правильное решение, чтобы не тратить своё свободное время, потому что договор можно заключить прямо на объекте. Замерщик ответит на любые Ваши вопросы, покажет образцы и фотографии, учтет любые ваши пожелания и осуществит безупречный замер с расценками.
Звоните по телефону +7(3952)656-226 или приходите в один из офисов, по адресу: г. Иркутск, ул. Розы Люксембург, д. 21. Работаем с пн по пт с 9:00 до 17:30, воскресенье – выходной день. Звоните, приходите, мы будем рады с Вами работать.
Watch the Plane Ascend: The plane takes off and starts climbing.
extenze male enhancement
No need to stay awake all night long to earn money. Launch the robot. https://t.me/cryptaxbot/17?fruttyVet83Bus
Здравствуйте!
Купить диплом университета.
Наша компания предлагает приобрести диплом в отличном качестве, который не отличить от оригинала без использования дорогостоящего оборудования и квалифицированного специалиста.
Где купить диплом по актуальной специальности?
http://leadrp.listbb.ru/viewtopic.php?f=3&t=355
Успешной учебы!
increase the excitement of the game.
how to enlarge penis
Здравствуйте!
Мы можем предложить дипломы любой профессии по доступным ценам.
Мы предлагаем документы техникумов, расположенных на территории всей России. Можно заказать качественно напечатанный диплом от любого учебного заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригиналов. Они будут заверены необходимыми печатями и подписями.
Даем 100% гарантию, что при проверке документа работодателями, каких-либо подозрений не возникнет.
Где заказать диплом специалиста?
newrealgames.ru/diplom-po-tvoey-mere-priobreti-obrazovanie-idealno-sootvetstvuyushhee-tvoim-potrebnostyam
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Place your bet at pinup online – very elite bookmaker in Kazakhstan
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в кургане, купить дипломы о высшем цены, купить диплом в шадринске, купить диплом в копейске, купить диплом преподавателя и получил базовые знания. В итоге остановился на материале: http://wellenkamm.net/videography-wedding-promotion/#comment-49978
https://liveratetoday.com/chicken-rates/chicken-rate-today-in-mumbai/
https://rodme.ru/diplom-po-professii-kupit-nedorogo-t11357.html
https://www.china-design.nl/about/#comment-34062
https://www.robtex.com/dns/originality-diplom.com.html
Удачи!
Signup Bonus-200% up to your first deposit using promo code GGBET93-click the link to collect. The official Pinterest account of the bookmaker and online casino GGBET. Actual login to GGBET website in 2024 gg bet
http://progressive-cars.ru/
Recognized for implementing comprehensive plans and fostering a cultuhre of belonging and inclusion (DEI).
Review my blkg – leventabaci.onlinedoktorasor.Com
Variety: Access to a wide range of betting options and gameplay modes.
how to make dick bigger
Hello there! This is kind of off topic but I need some advice from an established blog.
Is it very difficult to set up your own blog? I’m not very techincal but
I can figure things out pretty fast. I’m thinking about creating my own but I’m
not sure where to start. Do you have any points or suggestions?
Cheers
Feel free to surf to my website; SkinOrigins skincare products
Good day! This is my 1st comment here so I just
wanted to give a quick shout out and tell you I really
enjoy reading through your posts. Can you suggest any other
blogs/websites/forums that deal with the same topics?
Thank you!
Here is my web page – Skintag removal
Привет, друзья!
Приобрести документ о получении высшего образования можно у нас в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы СССР. Даем гарантию, что в случае проверки документа работодателями, каких-либо подозрений не возникнет.
Мы предлагаем выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями должностных лиц. Документ пройдет любые проверки, даже при использовании специальных приборов. Решайте свои задачи быстро с нашим сервисом.
Где приобрести диплом специалиста?
http://kerchlibrary.ru/index.php?subaction=userinfo&user=ykada
Удачи!
Magnificent beat ! I would like to apprentice while you amend your
web site, how could i subscribe for a blog site? The account aided me a acceptable deal.
I had been a little bit acquainted of this your broadcast
provided bright clear concept
Have a look at my web blog … SkinOrigins Face treatment
Pin Up Casino is an online gambling platform that offers a wide range of casino games, including slots, table games, live dealer games, and more. The casino is known for its vibrant and retro-themed design, reminiscent of the pin-up culture from the mid-20th century. It provides an engaging user experience with visually appealing graphics and an intuitive interface.
Pin Up Casino caters to both new and experienced players, offering various bonuses and promotions to enhance the gaming experience. Players can enjoy a diverse selection of slot games from leading software providers, as well as classic table games like blackjack, roulette, and poker. The live dealer section allows users to interact with real dealers in real-time, providing an immersive casino experience from the comfort of their own homes.
https://www.imf1fan.com/community/profile/vipoliv/
https://www.energyplan.eu/forums/users/vipoliv/
https://www.herlypc.es/community/profile/vipoliv/
https://blacklinesandbillables.com/theissueslist/account/vipoliv/
https://wowgilden.net/forum-topic_458521.html
https://www.mysportsgo.com/forums/topic/36746/pin-up-casino-oyunlarina-nasil-baslanir/view/post_id/869165
https://slubowisko.pl/topic/80449/
https://roughstuffmedia.activeboard.com/t70889671/kumar-dnyasna-dalacak/
https://www.dmxzone.com/support/13984/topic/128851
https://forum.trackandfieldnews.com/special/albums/1845353-kumar
https://shadowcard.io/forum/viewtopic.php?id=1753
https://www.goalissimo.org/forum/viewtopic.php?f=14&t=695282
https://devfolio.co/projects/xxx-7071
https://laidbackgardener.blog/2020/02/05/thought-of-the-day-17/#comment-102783
https://dvb-t2.cz/terminy-ukonceni-vysilani-dvb-t/
https://www.mycast.io/stories/playtown/roles/mr-humptump/50436606
https://www.arlindovsky.net/2020/03/os-manuais-escolares-para-2020-2021-1-o-ciclo/#comment-597927
https://portal.uaptc.edu/ICS/Campus_Life/Campus_Groups/Amicus_Curiae_Paralegal_Club/Discussion.jnz?portlet=Forums&screen=PostView&screenType=change&id=1d0f4152-bad5-45eb-b5ff-0ed94fbefe42&p=7
http://journals.hnpu.edu.ua/index.php/literature/comment/view/4159/294/13838
https://njit-connect.njit.edu/rwd/responsive-discussion-board?dgs3235=3&rid3235=11155&tid3235=2424
https://ucgp.jujuy.edu.ar/profile/Faletive44/
What’s Taking place i’m new to this, I stumbled upon this I
have found It absolutely helpful and it has helped me out
loads. I’m hoping to give a contribution & aid other users like its
aided me. Good job.
Look into my blog :: SkinOrigins Face treatment
Dumps Paypal buy Shops and markets cards Tor
Item 01 Card Total Balance: $3 100 – Price $ 110.00
Item 03 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2 000 – Price $ 149.00
Item Western Union Transfers $1 000 – Price $ 99.00
Item Western Union Transfers $300 – Price $ 249.00
*Prices on the website may vary slightly
Store and shop cloned cards Tor Buy Cloned cards
Здравствуйте!
Для некоторых людей, заказать диплом о высшем образовании – это острая потребность, возможность получить отличную работу. Но для кого-то – это желание не терять время на учебу в институте. Что бы ни толкнуло вас на это решение, мы готовы помочь вам. Быстро, качественно и по доступной цене сделаем диплом любого года выпуска на настоящих бланках с реальными печатями.
Наши специалисты предлагают быстро заказать диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями официальных лиц. Данный документ пройдет любые проверки, даже с использованием профессиональных приборов. Решайте свои задачи максимально быстро с нашими дипломами.
Где приобрести диплом специалиста?
http://webnewsrealty.ru/diplomyi-dlya-teh-kto-stremitsya-k-uspehu-i-protsvetaniyu
Успехов в учебе!
Hi there, I found your blog by means of Google at the
same time as looking for a similar subject, your web site came up,
it seems good. I have bookmarked it in my google bookmarks.
Hi there, just became alert to your blog via Google, and
found that it is really informative. I am going to be careful for brussels.
I will appreciate when you proceed this in future. Lots
of people can be benefited out of your writing. Cheers!
Check out my web site: SkinOrigins Face treatment
Discover June 2024’s Best Movies on Netflix what is the second pirates of the caribbean movie calledoregon rain seasonblue blood episodefamily guy throw up episode
Howdy just wanted to give you a quick heads up.
The words in your post seem to be running off the screen in Chrome.
I’m not sure if this is a formatting issue or something
to do with internet browser compatibility
but I thought I’d post to let you know. The style and design look great though!
Hope you get the issue solved soon. Many thanks https://Hdrezka.monster/user/Emilia7323/
Откатные ворота являются отличным выбором для ограждения частной территории, в частности, откатные ворота предоставляют максимальную надежность и прочность, при этом имеют относительно невысокую цену http://simplicitywiki.com/index.php?title=Откатные ворота
Hello mates, good article and nice urging commented here, I am
really enjoying by these.
my web page; facial in Bedok
Everything is very open with a very clear clarification of the issues.
It was truly informative. Your site is extremely helpful.
Many thanks for sharing!
Here is my web-site: SkinOrigins Face treatment
Привет!
Где заказать диплом по необходимой специальности?
Покупка диплома ВУЗа РФ у нас – надежный процесс, так как документ будет заноситься в государственный реестр. Печать выполняется на фирменных бланках, установленных государством.
Вы покупаете документ через надежную и проверенную компанию.
http://dliavas.listbb.ru/ucp.php?mode=login&sid=52294405650e72beafbe01819bf9122f
Успешной учебы!
It’s an awesome piece of writing for all the internet people; they will take
advantage from it I am sure.
Feel free to visit my blog … SkinOrigins
Very quickly this web page will be famous among all blogging visitors, due to
it’s pleasant articles
Feel free to surf to my blog :: Facial Singapore
Установка пластиковых окон Иркутск fod38.ru
По теме цены на пластиковые окна мы непременно Вам окажем помощь. Окна от представленной фабрики являются экологичными, так как в них не используется свинец. После установки, в помещениях будет тихо и спокойно, а также безопасно для детей, ведь мы делаем ручки с замком. Все окна с защитой от ультрафиолета, а ещё их легко мыть, удобно проветривать и красиво на них смотреть.
Получите максимальную выгоду с промокодами от Vavada казино. Наслаждайтесь разнообразием игр и бонусов, доступных только по специальным промокодам.
Convenience: Play from the comfort of your home or on the go.
men’s health supplements
Узнайте, как активировать Drip казино промокоды и получите доступ к уникальным бонусам и предложениям. Наслаждайтесь игрой с дополнительными привилегиями от Drip казино.
Промокоды Vavada казино открывают доступ к уникальным бонусам и предложениям. Активируйте промокод и получите больше от вашей игры в Vavada казино.
Great weblog here! Additionally your website so much up very fast!
What web host are you using? Can I get your associate hyperlink
facial in Bedok your
host? I want my site loaded up as quickly as yours lol
В большинстве стран для осуществления геолокации по номеру телефона требуется согласие владельца номера? Это связано с защитой персональных данных и правом на конфиденциальность? Однако в интернете можно найти сервисы, которые предлагают провести геолокацию по номеру телефона бесплатно и без согласия владельца?
В современном мире сотовые телефоны стали неотъемлемой частью нашей повседневной жизни найти человека по номеру телефона местоположение ? Зачастую возникает желание узнать местоположение человека по его номеру телефона как вычислить айпи по номеру ? Существует несколько способов осуществить данную задачу бесплатно, однако важно помнить о соблюдении законов о конфиденциальности прозвон по номеру телефона ?
Геолокация по номеру телефона бесплатно без регистрации
Точность определения зависит от активности сотовых сетей в районе узнать где находится человек по телефону
Существует множество онлайн сервисов, которые предлагают услугу определения местоположения телефона по номеру узнать человека по номеру телефона онлайн Для этого вам может потребоваться зарегистрироваться на сайте и ввести номер телефона абонента поиск по телефону ? Некоторые из таких сервисов могут быть платными найти адрес по номеру телефона бесплатно ?
https://gpsphone.ru/
https://xn—-7sbabcvhts2dzbh.xn--p1ai/
If you desire to improve your experience just keep visiting this site and be updated with the most recent news
update posted here.
Here is my blog post; Facial Singapore
Лизинг спецтехники для юридических лиц – это эффективный способ инвестировать в свою компанию. Условия договора лизинга, такие как срок и график платежей, обычно определяются индивидуально лизинг спецтехники без взноса
I am facial in Bedok fact grateful to the owner of this web page who
has shared this impressive piece of writing at here.
My programmer is trying to convince me to move to .net
from PHP. I have always disliked the idea because of the costs.
But he’s tryiong none the less. I’ve been using
Movable-type on a number of websites for about a year and am worried about switching to another platform.
I have heard fantastic things about blogengine.net.
Is there a way I can transfer all my wordpress content into it?
Any help would be really appreciated!
Look at my blog; Best facial in Singapore
Amazing things here. I am very glad to look your
article. Thank you so much and I am having a look
ahead to touch you. Will you kindly drop me a e-mail?
my webpage … Facial Singapore
купить диплом в красноярске http://www.damdesign.ru .
Social and Community Aspects
prolong power supplement
Добрый день!
Где заказать диплом по нужной специальности?
Приобрести документ университета вы сможете в нашей компании в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ.
Мы изготавливаем дипломы любой профессии по приятным тарифам. Цена может зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную ценовую политику.
http://fabnews.ru/blog/6726.html
Успехов в учебе!
Hi, I do believe this is a great website. I stumbledupon it 😉
I am going to return yet again since i have book marked it.
Money and freedom is the best way to change, may you be rich and continue to guide
other people.
my site: SkinOrigins
If you want to grow your familiarity only keep visiting this web page and be updated with the
newest news posted here.
My web-site … facial in Bedok
Whats up are using WordPress for your site platform? I’m new
to the blog world but I’m trying to get started and create my own. Do you require any html coding expertise to
make your own blog? Any help would be greatly appreciated!
Feel free to visit my web-site: Best facial in Singapore
Asking questions are in fact fastidious thing if you are not understanding
something completely, but this piece of writing offers
nice understanding even.
Check out my homepage :: SkinOrigins Face treatment
Rise of RA подходит для игроков всех типов, и новичкам, и профессионалам. https://rise-of-ra.com/ru/ – здесь узнаете, как выигрывать в Rise of RA, почему нельзя предсказать победы и многое другое. Для вас мы собрали реальные отзывы, чтобы вы о слоте свое мнение могли составить. Rise of RA – это великолепный выбор для любителей древнеегипетской тематики. Слот имеет прекрасную графику, анимацию и звуковое сопровождение. Погрузитесь в атмосферу загадочного Египта!
Заказать окна ПВХ Иркутск fod38.ru
По теме рольставни иркутск мы обязательно Вам поможем. Окна от нашей фабрики являются экологичными, так как в них не используется свинец. После монтажа, в комнате будет бесшумно и уютно, а также безопасно для детей, ведь мы устанавливаем ручки с замком. Все ПВХ окна с защитой от ультрафиолета, а также их просто мыть, удобно проветривать и радужно для глаз.
Лизинг спецтехники для юридических лиц – это эффективный способ инвестировать в свою компанию. Условия договора лизинга, такие как срок и график платежей, обычно определяются индивидуально спецтехника продажа лизинг
the social features, and the quality of the user interface.
do penis enlargement pills work
Dumps Paypal buy Shops and markets cards Tor
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $ 500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
Buy hacked paypal Clon cards
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом медбрата, купить речной диплом, купить диплом института, купить диплом во владивостоке, купить диплом в ухте, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://pokupay-24.ru/blog/bitye-pikseli-na-televizore-chto-eto-i-kakoe-dopustimoe-kolichestvo/
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Удачи!
ensures that the games are fair and that the platforms adhere to strict standards of operation.
what drugs are used for penis enlargement
Read Full Article avalanche wallet
Hello, its pleasant post concerning media print, we all understand media is a fantastic source of information.
My blog unsolved
Hi! I know this is somewhat off topic but I was wondering if you knew where I could find a captcha plugin for my comment form?
I’m using the same blog platform as yours and
I’m having trouble finding one? Thanks a lot!
My web-site شناسه خدمت
I just like the valuable information you provide in your articles.
I will bookmark your weblog and take a look at again right here
frequently. I am somewhat sure I will be informed many new stuff right
here! Best of luck for the following!
Also visit my web page شناسه خدمت
Incredible! This blog looks exactly like my old one! It’s on a completely different
topic but it has pretty much the same page layout and
design. Superb choice of colors!
Also visit my homepage https://inasevents.com/breaking-down-the-odds-find-out-how-to-consider-your-probabilities-in-on-line-casinos/
You actually make it seem so easy with your presentation but I find this topic
to be really something that I think I would never understand.
It seems too complex and very broad for me. I am looking forward for your next post,
I will try to get the hang of it!
My site :: 프라그마틱 바카라
https://nudifyai.net/
Купить машины в лизинг от официальных дилеров, автосалонов. Выгодные условия и скидки лизинг на автотранспорте
You actually make it appear so easy along with your
presentation however I in finding this topic to be really one thing that I
think I’d never understand. It seems too complex
and very broad for me. I’m having a look ahead on your next
post, I will attempt to get the cling of it!
Here is my site: 프라그마틱 바카라
Bs2site2.at – Bs.gl, Bs2best.at
Yes, the Aviator Game is compatible with mobile devices. Players can enjoy the game on their smartphones or
best sexual enhancement pills
My brother recommended I might like this blog.
He was entirely right. This post truly made my day.
You can not imagine just how much time I had spent for this information! Thanks!
Also visit my web site – chukka boots
Aw, this was a very good post. Finding the time and actual effort
to make a really good article… but what can I say… I put things off a whole lot and don’t seem to get anything
done. http://schottlaw.co/__media__/js/netsoltrademark.php?d=Emdrive.Echothis.com%2FUser%3ADomenicLawrenson
Привет!
Где приобрести диплом по актуальной специальности?
Мы готовы предложить документы институтов, которые находятся на территории всей России. Вы имеете возможность приобрести диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы делаются на бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригиналов. Документы будут заверены всеми требуемыми печатями и штампами.
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий по разумным тарифам.
diplomasx.com
Рады оказаться полезными!
go to this web-site Atomic wallet
https://nudifyai.net
Origins of the Aviator Game
extenze male enhancement
Иркутск окна ПВХ fod38.ru
Если Вы планировали найти ремонт окон – то заходите на указанный сайт. На сайте fod38.ru возможно записаться на бесплатный замер будущих окон. Это самое верное решение, чтобы не тратить своё свободное время, ведь договор можно заключить прямо на дому. Замерщик ответит на любые Ваши вопросы, покажет модели и каталоги, учтет любые ваши пожелания и осуществит безупречный замер с расценками.
На сайте https://mosprorezka.ru/ уточните телефон мастера для того, чтобы воспользоваться такой важной и нужной услугой, как лазерная резка. Обратиться в компанию можно, независимо от сложности работы. При этом она обойдется по привлекательной стоимости. Постоянно в компании проходят акции, а потому вы сможете воспользоваться услугой, сэкономив на этом. Работа происходит без предоплаты, а потому это очень выгодно. Уточнить необходимую информацию вы сможете в любое время, потому как компания работает в круглосуточном режиме.
перенаправляется сюда электрик томск
Обратившись в нашу строительную компанию, вы освободите себя от многих проблем, если решили обзавестись новым коттеджем или загородным домом. Сложность работ и объемы строительства не имеют значения.Опытные сотрудники компании, имеющие высокую квалификацию, помогут подобрать не только конфигурацию будущего коттеджа или загородного дома, но и посоветуют, какие строительные материалы будут уместны для отделки внутри помещения и снаружи.Благодаря этому владельцы получают готовый дом «под ключ», причем он обойдется намного дешевле, чем в других строительных компаниях. Строительство https://builder-spb.turbo.site ведем как в самом Санкт-Петербурге, так и за его пределами, в ленинградской области. Сегодня нашу компанию можно смело отнести к лидерам в строительной отрасли.
sell dumps track 2 newfresh balance min 650$ LIVE 24/24 – 2021 (No
DIE) 【Visit CvvDumps.US】 All COUNTRY US , UK , CA , AU
, EU , TC , BJ
————-CONTACT———————–
WEBSITE : >>>>>> CvvDumps✦ US
—– HERE COMES THE PRICE LIST ———–
***** CVV Other countries
NU VISA CARD = $2,1 per 1 (buy >5 with price $2.5 per 1).
MO VISA CARD = $4,9 per 1 (buy >5 with price $2.5
per 1).
KE VISA CARD = $3,5 per 1 (buy >5 with price $2.5 per 1).
VI VISA CARD = $5 per 1 (buy >5 with price $2.5 per 1).
***** CVV US:
– US MASTER CARD = $2,8 per 1 (buy >5 with price $3 per 1).
– US VISA CARD = $2,9 per 1 (buy >5 with price $2.5 per 1).
– US AMEX CARD = $3 per 1 (buy >5 with price $2.5 per 1).
– US DISCOVER CARD = $3,1 per 1 (buy >5 with price $3.5 per 1).
– US CARD WITH DOB = $15 per 1 (buy >5 with price $12 per 1).
– US FULLZ INFO = $40 per 1 (buy >10 with price $30 per 1).
***** CCV UK:
– UK CARD NORMAL = $2,7 per 1 (buy >5 with price $3 per 1).
– UK MASTER CARD = $3,5 per 1 (buy >5 with price $2.5 per 1).
– UK VISA CARD = $2,5 per 1 (buy >5 with price $2.5 per 1).
– UK AMEX CARD = $3 per 1 (buy >5 with price $4
per 1).
$5,8
– UK CARD WITH DOB = $15 per 1 (buy >5 with price $14 per 1).
– UK WITH BIN = $10 per 1 (buy >5 with price $9 per 1).
– UK WITH BIN WITH DOB = $25 per 1 (buy >20 with price $22 per 1).
– UK FULLZ INFO = $40 per 1 (buy >10 with price $35 per 1).
***** CCV AU:
– AU MASTER CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU VISA CARD = $5.5 per 1 (buy >5 with price $5 per 1).
– AU AMEX CARD = $8.5 per 1 (buy >5 with price $8 per 1).
– AU DISCOVER CARD = $8.5 per 1 (buy >5 with price $8 per 1).
***** CCV CA:
– CA MASTER CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA CARD = $6 per 1 (buy >5 with price $5 per 1).
– CA VISA BUSINESS = $14 per 1 (buy >5 with price $13 per 1).
In-Game Bonuses and Rewards
penis enlargement methods
Купить машины в лизинг от официальных дилеров, автосалонов. Выгодные условия и скидки лизинг автотранспорта
http://saleclonedcards.work
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $ 500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://sale-cloned-cards.work
Добрый день!
Приобрести диплом ВУЗа.
Наш сервис предлагает купить диплом отличного качества, который невозможно отличить от оригинального документа без участия специалиста высокой квалификации со специальным оборудованием.
Где приобрести диплом по актуальной специальности?
http://lubov.listbb.ru/viewtopic.php?f=2&t=433
Хорошей учебы!
Здравствуйте!
Где купить диплом специалиста?
Заказать документ о получении высшего образования вы имеете возможность у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Даем гарантию, что в случае проверки документа работодателями, никаких подозрений не появится.
Наши специалисты предлагают быстро и выгодно приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Документ способен пройти лубую проверку, даже с применением профессиональных приборов. Решите свои задачи быстро с нашей компанией.
https://alex-neil.ru/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=178
https://www.diccut.com/read-blog/15978
http://p91648f6.beget.tech/2024/03/14/pochemu-magaziny-chto-prodayut-diplomy-nastolko-populyarny-segodnya.html
http://158.160.31.233/blogs/1/trebuetsya-kupit-diplom-otkryvayte-nash-internetmagazin.php
https://school-toksovo.ru/forum/messages/forum1/topic313/message483/?result=new
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в сарове, купить диплом россия, купить диплом в воткинске, купить сертификат специалиста, купить диплом химика, затем наткнулся на https://stoligra.ru/products/golovolomka-kubik–cast-puzzle-cuby-uroven-slozhnosti-4/#comment_67394, где все мои учебные вопросы были решены!
Удачи!
We make positive you are current on all the neswest breaking news and stats to
make sound bets and win massive.
Also visit my web blog: 토토친구
Aw, this was a very nice post. Spending some time and actual effort to make a really good article… but what can I say… I put things off a lot and
don’t seem to get anything done.
Also visit my homepage :: CyberSecurityEasy Training
jasminer X44-Q
Yes, the Aviator Game is compatible with mobile devices. Players can enjoy the game on their smartphones or
best male libido boosters
Читать далее электрик томск
Здравствуйте!
Где заказать диплом по актуальной специальности?
Купить диплом о высшем образовании.
Стоимость значительно меньше чем довелось бы заплатить за обучение в университете
http://doktorpishet.ru/index.php?subaction=userinfo&user=ivemite
Успешной учебы!
Для тех, кто ищет увлекательные пути к развлечениям и возможности испытать удачу в виртуальной среде, существует мир, где представлены бесчисленные варианты игр и азартных развлечений http://www.mp-associes.com/en/index.php/blog/%D0%9A%D0%B0%D0%BD%D1%82.html
I was able to find good advice from your content.
my web site: Social Engineering Awareness for Kids
Aw, this was a really nice post. Taking a few minutes and actual effort to create a very
good article… but what can I say… I procrastinate a whole lot and don’t manage to get nearly anything done.
Here is my blog: Computer Training for Seniors
Hello there! I could have sworn I’ve been to this site before but
after reading through some of the post I realized it’s new to me.
Anyways, I’m definitely glad I found it and I’ll be bookmarking and checking back frequently!
Feel free to visit my web-site … Computer Safety Kids
It’s great that you are getting ideas from this paragraph as well as from our argument made at this time.
my site Computer Safety Kids
Ищете дополнительные бонусы? Используйте Vavada казино промокоды и получите уникальные привилегии и предложения для увеличения вашего игрового баланса в Vavada казино.
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом юриста, купить диплом в новоуральске, где купить диплом, купить диплом в вологде, купить диплом в элисте. Постепенно углубляясь в тему, нашел отличный ресурс здесь:
https://tv-cifra.ru/blog/izmenenie-uslovij-okazaniya-uslugi-edinyj/#comment_160045
http://windigof.ru/blog/windigo-na-vystavke-auto-show-2017/
https://www.mylot.su/blog/14440
http://andi67.bplaced.net/dokuwiki/doku.php?id=premialniediplom
http://arbitrajniki.ru/forums/topic/kupit-attestat-za-11-klassov-b923p/
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Хорошей учебы!
Unquestionably imagine that that you stated. Your favorite reason seemed to be at the net the easiest factor
to remember of. I say to you, I definitely get irked whilst other people think about worries that they plainly do
not know about. You managed to hit the nail upon the highest
and outlined out the whole thing with no need side-effects , other folks could take a signal.
Will probably be again to get more. Thanks
Also visit my blog Seniors Elderly Computer Training
Используйте Drip казино промокоды для получения эксклюзивных бонусов. Узнайте, как активировать промокод и наслаждайтесь дополнительными преимуществами от Drip казино.
Hmm is anyone else having problems with the pictures on this blog loading?
I’m trying to figure out if its a problem on my end or if it’s the blog.
Any feedback would be greatly appreciated.
Stop by my site … Online Child Safety
Привет, друзья!
Где купить диплом специалиста?
Мы готовы предложить документы институтов, которые расположены на территории всей России. Вы можете заказать качественно напечатанный диплом за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы делаются на бумаге самого высокого качества. Это дает возможности делать государственные дипломы, которые не отличить от оригиналов. Документы будут заверены необходимыми печатями и подписями.
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
diploms-x24.ru
Поможем вам всегда!
Как показывает практика, сегодня купить лучшее медицинское оборудование и технику в Украине, востребованные для оказания соответствующих услуг на безупречном уровне, точно не является проблемой http://grp.7olimp.ru/viewtopic.php?t=1543
Over-betting: Betting too much too quickly can lead to significant losses.
best treatment for erectile dysfunction
Very great post. I simply stumbled upon your blog and
wished to say that I’ve really enjoyed browsing your weblog posts.
After all I’ll be subscribing Social Engineering Awareness for Kids your feed and I hope you write
again soon!
Промокоды Vavada казино – это ваш путь к дополнительным бонусам. Активируйте промокод и наслаждайтесь игрой с эксклюзивными предложениями от Vavada казино.
I know this if off topic but I’m looking into starting my own weblog and
was wondering what all is needed to get setup? I’m assuming having a blog
like yours would cost a pretty penny? I’m not very web smart
so I’m not 100% certain. Any tips or advice would be greatly appreciated.
Thanks
Check out my blog post; CyberSecurityEasy Training
Inspiring quest there. What occurred after? Thanks!
Feel free to visit my blog; Computer Safety Kids
What’s up to every single one, it’s genuinely a
good for me to pay a quick visit this web site, it consists of important Information.
Feel free to surf to my homepage; Senior Living Safety
You could certainly see your skills in the article you write.
The sector hopes for even more passionate writers like
you who aren’t afraid to mention how they believe.
All the time follow your heart.
Visit my homepage :: Online Child Safety
My partner and I absolutely love your blog and find almost all of your post’s to
be what precisely I’m looking for. can you offer guest writers to write content for you?
I wouldn’t mind writing a post or elaborating on many of
the subjects you write with regards to here. Again, awesome site!
my webpage … Phishing Antiphishing Training
Привет! Ищете надежные МФО с низкими процентными ставками и без отказов? Наш канал – именно то, что вам нужно! Мы собрали только проверенные компании, которые предлагают займы под 0% и с процентной ставкой не выше 0.8% в день. Даже если у вас плохая кредитная история, вы сможете получить деньги без проблем. У нас также есть круглосуточная поддержка и советы для заемщиков. Подписывайтесь и будьте в курсе самых выгодных предложений!
Hello, I enjoy reading through your article post. I like to write a little comment to support you.
Feel free to surf to my web page – Online Safety Training
ссылка на сайт
Арнольд 2023 1 сезон 1-3 серия смотреть онлайн в хорошем качестве
of course like your web site however you have to check
the spelling on several of your posts. Many of them are rife with spelling issues and I to find it very troublesome to tell the truth on the other hand I will surely come again again.
Look at my blog – Social Engineering Awareness for Kids
While the game itself is free to access, playing involves placing bets with real money. Some platforms may offer
vira flexx male enhancement
Its such as you learn my mind! You appear to know so much about this, like you wrote the
book in it or something. I feel that you simply could do with a few % to force
the message house a bit, but other than that, this is magnificent blog.
A great read. I will certainly be back.
Feel free to surf to my website … Cyber Safety for Kids
элитный эскорт
Для тех, кто ищет увлекательные пути к развлечениям и возможности испытать удачу в виртуальной среде, существует мир, где представлены бесчисленные варианты игр и азартных развлечений http://littleyaksa.yodev.net/bbs/board.php?bo_table=free&wr_id=6438510
Реализуя широкий ассортимент оборудования и медицинской техники, мы удовлетворяем запросы врачей различных профилей, косметологов и административного персонала http://grp.7olimp.ru/viewtopic.php?t=1543
эскорт услуги
Greetings I am so excited I found your webpage, I really found you by mistake,
while I was searching on Askjeeve for something else,
Anyhow I am here now and would just like to say kudos for
a incredible post and a all round interesting blog (I also love the theme/design), I
don’t have time to browse it all at the minute but I have saved it and also added in your RSS feeds, so when I have time I will be back to Read to your kids about online safety more, Please do keep up
the fantastic b.
It’s actually very complex in this busy life to listen news on Television, therefore I simply use world wide
web for that purpose, and obtain the latest news.
my web-site … Senior Facilities Training
эскорт москва
Here is a timeline of the path to legal sports gambling in Arizona.
Visit my web blog 토토사이트
Привет!
Приобрести диплом о высшем образовании.
Мы предлагаем приобрести диплом в отличном качестве, неотличимый от оригинала без использования дорогостоящего оборудования и квалифицированного специалиста.
Где приобрести диплом по необходимой специальности?
http://sz.80lvl.ru/viewtopic.php?f=9&t=1891
Хорошей учебы!
Hi! I could have sworn I’ve been to this blog before but after checking through some of the post I realized it’s new to me.
Nonetheless, I’m definitely glad I found it and I’ll be book-marking
and checking back often!
Here is my webpage :: Social Engineering Awareness
We’re a group of volunteers and opening a new scheme in our community.
Your site provided us with valuable info to work
on. You’ve done a formidable job and our entire community
will be thankful to you.
Feel free to surf to my web site Social Engineering Awareness for Kids
Здравствуйте!
Где приобрести диплом специалиста?
Приобрести документ о получении высшего образования вы имеете возможность у нас в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ.
Мы изготавливаем дипломы любой профессии по приятным тарифам. Цена может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику тарифов.
https://www.tapatalk.com/groups/dzerjinsky/viewtopic.php?f=2&t=33092&from_new_topic=1
Успешной учебы!
I got this website from my friend who informed me concerning this web page and at the moment this
time I am visiting this website and reading very informative content at this place.
Here is my web site :: Voice Cloning
Buy Cloned card paypal acc
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $ 500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
Paypal transfers Prepaid cards
Зайдите на сайт https://moresliv.cc/ где вы сможете скачать огромное количество курсов бесплатно онлайн через торрент. Огромная база знаний и обучений. Складчины и видеоуроки, книги и вебинары – графика, программирование, бизнес, курсы блогеров и многое другое здесь. Более 175.000 различных курсов на сайте. Заходи!
Санитарно-химические исследования грунта и почвы или контроль условий на рабочих местах
анализ радиационного загрязнения
https://gklab.ru/uslugi/fizicheskie-faktory/izmereniye-napryazhennosti-elektricheskogo-polya-v-diapazone-chastot-003-50-mgts/
Ещё можно узнать: где значок евро на клавиатуре компьютера
контроль выбросов в СЗЗ
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в озёрске, купить свидетельство о разводе, купить диплом в севастополе, купить диплом в бердске, купить диплом физика, постепенно вникая в суть дела нашел отличный материал здесь https://forumjizni.ru/member.php?u=120813 и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Успешной учебы!
At this moment I am going to do my breakfast, later than having my
breakfast coming yet again to read other news.
Check out my web site; Online Child Safety
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом моряка, купить диплом в йошкар-оле, купить диплом продавца, купить диплом в твери, купить диплом в кстово, потом попал на https://www.filigreebeds.com/shop/imboss/#comment-8891
http://fashiongarden.ru/blog/kak-sdelat-landshaft-uchastka-svoimi-rukami
http://prmaster.su/acontinents/kupit-diplom-s-besplatnoy-dostavkoy-po-vsey-rossii_5780.html
https://viet8.net/kinh-nghiem-sua-nha-lam-gac-xep-hieu-qua/
http://www.automatenspiele.co/the-golden-city/#comment-1873123
и там решили все мои учебные заботы!
Хорошей учебы!
Unique Features of the Aviator Game
biopeak male enhancement
Awesome blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple tweeks would really make my blog
stand out. Please let me know where you got your theme.
Thank you
Stop by my web-site :: CyberSecurityEasy Training
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом учителя физической культуры, купить диплом в первоуральске, купить свидетельство о браке, купить диплом в бугульме, купить диплом о высшем образовании, постепенно вникая в суть дела нашел отличный материал здесь https://vk.com/prymechatel?w=wall-147947644_398 и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Успешной учебы!
This post is priceless. When can I find out more?
Also visit my website – Coaching Seniors on CyberSafety
Best cardsharing service, iptv cheap price only 0.99$
CARDSHARING
IPTV 0.99$
Стабильный качественный
кардшаринг +
IPTV
по самым низким ценам в сети, всего 0.99$
Реализуя широкий ассортимент оборудования и медицинской техники, мы удовлетворяем запросы врачей различных профилей, косметологов и административного персонала http://besconeshnocte.flybb.ru/topic482.html?p=516
Здравствуйте!
Приобрести диплом университета.
Наша компания предлагает купить диплом в отличном качестве, неотличимый от оригинала без участия специалистов высокой квалификации с дорогим оборудованием.
Где приобрести диплом по необходимой специальности?
https://alanyatoday.ru/users/76
Успехов в учебе!
jasminer X44-Q
jasminer X44-Q
оземпик инструкция цена купить – оземпик +для похудения купить цена, оземпик калининград
jasminer X44-Q
jasminer X44-Q
jasminer X44-Q
Привет, друзья!
Заказать документ университета можно в нашей компании. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы СССР. Гарантируем, что при проверке документов работодателями, подозрений не возникнет.
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями должностных лиц. Диплом пройдет лубую проверку, даже с применением профессионального оборудования. Достигайте цели быстро с нашими дипломами.
Где заказать диплом специалиста?
https://lider-school174.com/forum/user/2588/
Хорошей учебы!
На сайте https://autoclub78.ru вы найдете интересные, практичные советы для тех, у кого есть автомобиль. Имеются практические рекомендации, ценные советы, которые помогут найти оптимальный вариант для того, чтобы правильно эксплуатировать технику. Статьи ответят на многочисленные вопросы, подскажут, как правильно действовать в определенной ситуации. Есть информация про самые востребованные мотоциклы, а также запчасти, которые реализуются на маркетплейсах. Есть информация и про то, как не стоит приобретать стеклоомывающую жидкость.
Добрый день!
Где заказать диплом специалиста?
Мы можем предложить документы ВУЗов, расположенных на территории всей РФ. Вы сможете заказать диплом за любой год, включая документы старого образца. Дипломы печатаются на “правильной” бумаге высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Документы заверяются всеми требуемыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по приятным ценам.
ast-diplom.com
Поможем вам всегда!
Due to the fact it has no casinos, Tennessee is the only state with on the web-only sports betting.
Here is my webpage :: http://labtestonline.Org
jasminer X44-Q
jasminer X44-Q
ундетект чит Dayz – Дешевые приватные читы, приватный чит
wow mythic raid carry for sale http://kreativwerkstatt-esens.de/ .
Its such as you read my mind! You appear to know a lot approximately this, like you wrote the e book in it or something.
I feel that you just can do with a few % to drive the message home a little bit, however instead
of that, this is excellent blog. An excellent read.
I’ll certainly be back.
My site: industrial water purifier
It’s very easy to find out any matter on web as compared to books, as I found this article at this web page. https://njkkot.org/?document_srl=835772
Лизинг оборудования открывает новые возможности для развития вашей компании. Это одно из наиболее эффективных финансовых решений для модернизации производственных мощностей и оптимизации работы предприятия лизинг швейного оборудования
Сайт предлагает широкий выбор лизинговых продуктов для бизнеса, включая лизинг оборудования. Благодаря этому, компании могут получить доступ к современному оборудованию без необходимости его покупки за наличные https://mamamia.by/forum/viewtopic.php?t=5678
Thanks in favor of sharing such a good idea, article is pleasant, thats why i have read it fully
Look at my web page :: 2nd story addition
I’m truly enjoying the design and layout of your blog. It’s
a very easy on the eyes which makes it much more enjoyable for me to come here and
visit more often. Did you hire out a developer to create your
theme? Outstanding work!
Look at my blog … 무료스포츠분석
высокодоходные инвестиционные проекты – высокодоходные инвестиционные проекты, High Yield Investment Program
It’s great that you are getting ideas from this piece of writing as well as from our dialogue made at this time.
Also visit my website; 축구중계
Привет, друзья!
Где купить диплом по актуальной специальности?
Приобрести документ о получении высшего образования можно в нашей компании. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы образца СССР. Гарантируем, что при проверке документа работодателями, никаких подозрений не возникнет.
http://forum.drustvogil-galad.si/index.php?topic=10004.0
Удачи!
Здравствуйте!
Где купить диплом по необходимой специальности?
Заказать документ о получении высшего образования можно в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов РФ.
Мы изготавливаем дипломы любых профессий по невысоким ценам. Цена будет зависеть от определенной специальности, года выпуска и университета. Всегда стараемся поддерживать для покупателей адекватную ценовую политику.
https://re-port.ru/users/50912/
Успехов в учебе!
Здравствуйте!
Где приобрести диплом по необходимой специальности?
Мы готовы предложить документы ВУЗов, которые находятся на территории всей России. Вы имеете возможность заказать качественный диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы печатаются на “правильной” бумаге самого высокого качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Они будут заверены всеми обязательными печатями и штампами.
Мы изготавливаем дипломы любых профессий по выгодным тарифам.
diploms-x.com
Рады помочь!
My brother suggested I might like this web site.
He was totally right. This post truly made my day. You can not
imagine just how much time I had spent for this information! Thanks!
Take a look at my homepage – führerschein kaufen ohne prüfung
http://sale-cloned-cards.cc
Item 01 Card Total Balance: $3100 – Price $ 110.00
Item 03 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://buyclonedcards.cc
Hi, I believe your site could be having browser compatibility issues.
Whenever I look at your web site in Safari, it looks fine however when opening
in IE, it has some overlapping issues. I merely wanted to give you a quick heads
up! Apart from that, great blog!
my web blog; 느바분석
Привет!
Мы изготавливаем дипломы любой профессии по приятным ценам.
Мы предлагаем документы ВУЗов, которые расположены на территории всей Российской Федерации. Можно купить диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются необходимыми печатями и подписями.
Где приобрести диплом специалиста?
zaim933966.ru/zaym/gde-vzyat
Do you mind if I quote a few of your articles
as long as I provide credit and sources back to your site?
My website is in the exact same area of interest as yours and my
users would genuinely benefit from some of the information you present here.
Please let me know if this alright with you.
Thank you!
Review my web site: telefonu remontas
Привет!
Где приобрести диплом специалиста?
Приобретение диплома ВУЗа России у нас – надежный процесс, поскольку документ заносится в реестр. Печать осуществляется на фирменных бланках, установленных государством.
Вы приобретаете документ в надежной и проверенной временем компании.
http://rolevikionline.g-talk.ru/ucp.php?mode=privacy&sid=d4ab92a391426f41854a2f0043606307
Успешной учебы!
Wow that was strange. I just wrote an very long comment but after I clicked submit my comment didn’t
appear. Grrrr… well I’m not writing all that over again. Anyways,
just wanted to say superb blog!
Also visit my blog :: 국내배구중계
Добрый день!
Где заказать диплом специалиста?
Мы предлагаем документы ВУЗов, расположенных на территории всей РФ. Вы можете купить диплом от любого высшего учебного заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на бумаге высшего качества. Это дает возможность делать настоящие дипломы, которые не отличить от оригинала. Они заверяются необходимыми печатями и штампами.
Мы можем предложить дипломы психологов, юристов, экономистов и прочих профессий по приятным тарифам.
ast-diplom.com
Поможем вам всегда!
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в ейске, купить диплом в верхней пышме, купить диплом в новом уренгое, купить диплом автомеханика, купить диплом повара, постепенно вникая в суть дела нашел отличный материал здесь
https://dksol.ru/4919-spektakl-poslednyaya-fotografiya/
http://monikafisheer.blogspot.com/2014/07/blog-post_25.html
http://xn--80aeh5aeeb3a7a4f.xn--p1ai/forum/user/50443/
http://www.et27.ru/boylery_i_protochnye_vodonagrevateli/boylery_nibe/boylery_kosvennogo_nagreva_spiro/boyler_kosvennogo_nagreva_classic_spiro_ow_e_120_12l/
http://koreamuseum.ru/index.php?subaction=userinfo&user=umotyk
и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Удачи!
Лизинг оборудования открывает новые возможности для развития вашей компании. Это одно из наиболее эффективных финансовых решений для модернизации производственных мощностей и оптимизации работы предприятия прачечное оборудование в лизинг
his explanation game pachinko
Wonderful goods from you, man. I have understand your stuff
previous to and you are just extremely excellent. I actually like what you’ve acquired here, really like what you are saying
and the way in which you say it. You make it enjoyable and you still take care of to keep it sensible.
I can’t wait to read far more from you. This is really a wonderful website.
Here is my site – 새축분석
Сайт предлагает широкий выбор лизинговых продуктов для бизнеса, включая лизинг оборудования. Благодаря этому, компании могут получить доступ к современному оборудованию без необходимости его покупки за наличные http://vrn.best-city.ru/forum/thread540103166/
Добрый день!
Где заказать диплом по актуальной специальности?
Приобрести документ университета вы имеете возможность в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить диплом по любым специальностям, любого года выпуска, включая документы старого образца. Гарантируем, что при проверке документов работодателями, подозрений не возникнет.
http://dveribiz.ru/shop/vkhodnye-dveri/ekonom-klass/
Успешной учебы!
I don’t know whether it’s just me or if perhaps everybody else encountering
issues with your website. It appears like some
of the text on your content are running off the screen. Can somebody else please comment and let me
know if this is happening to them too? This may be a issue with my internet browser because I’ve had this happen previously.
Many thanks
My blog post :: 나비티비
I got this site from my buddy who shared with me regarding
this site and now this time I am browsing this web site and reading very informative content at this place.
Feel free to surf to my web site :: 국내축구중계
You could certainly see your skills in the article you write.
The arena hopes for more passionate writers like you who are not afraid to say how they believe.
All the time go after your heart.
My site – kitchen remodel
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в екатеринбурге, купить диплом в невинномысске, купить диплом фармацевта, купить свидетельство о браке, купить диплом о высшем образовании. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://wiki.why42.ru/wiki/????????_????????,_???????????_?????_?????????:_??????_?_????????! и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи!
Useful info. Lucky me I found your web site accidentally,
and I am stunned why this accident didn’t happened earlier!
I bookmarked it.
my web page :: 해외스포츠중계
Howdy exceptional website! Does running a blog such as this require a
lot of work? I’ve absolutely no knowledge of programming however I was
hoping to start my own blog soon. Anyway, should you have any ideas or tips for new blog owners please share.
I know this is off topic but I just needed to ask.
Thanks a lot!
Feel free to visit my web blog – 해축분석
visit the website
vps
Good day! This is my first comment here so I just wanted to give a quick shout out and tell you I truly enjoy reading through your articles.
Can you suggest any other blogs/websites/forums that deal with the same subjects?
Thank you!
my homepage 국내농구중계
шоу-бизнес — знаменитости, новости, звёзды эстрады – криптовалюта — статьи и материалы на тему криптовалют, Книги про попаданцев в бытовое фэнтези
pop over to these guys
best private cheat
надо сдать анализ – какие анализы сдать, медицинская клиника врачи
reference wasabiwallet
Привет! Нужны деньги прямо сейчас? Наш канал – это то, что вам нужно. Мы собрали для вас список МФО, которые дают займы на карту круглосуточно и без отказов. Хотите получить деньги за несколько минут? Подписывайтесь и узнавайте о самых выгодных предложениях первыми. Забудьте о сложностях и долгих ожиданиях – с нами все проще!
Wow that was strange. I just wrote an very long comment but after I clicked submit my comment didn’t
show up. Grrrr… well I’m not writing all that over again. Regardless, just wanted to
say wonderful blog!
Feel free to visit my web-site; 국내야구중계
Ahaa, its good conversation concerning this paragraph at this place at this weblog, I have read all
that, so at this time me also commenting here.
My page :: home addition
Рекламное агентство – это компания, которая занимается созданием и реализацией рекламных кампаний для различных клиентов. Рекламное агентство может предлагать следующие услуги:
1. Разработка рекламной стратегии: анализ аудиитории, определение целей и задач рекламной кампании, выбор каналов рекламы и бюджетирование.
2. Создание рекламного контента: разработка рекламных материалов, таких как видеоролики, баннеры, печатные объявления, тексты для социальных сетей и т.д.
3. Медиапланирование: выбор оптимальных каналов для размещения рекламы, закупка рекламного пространства, мониторинг эффективности кампании.
4. Социальные сети: создание и управление рекламными кампаниями в социальных сетях, таких как Facebook, Instagram, Twitter и т.д.
5. Оцифровка: преобразование традиционных рекламных форматов в цифровые, такие как email-рассылка, мобильная реклама и т.д.
6. Анализ и отчетность: отслеживание эффективности рекламной кампании, анализ результатов, предоставление отчетов клиенту.
Рекламные агентства могут специализироваться на различных областях, таких как:
1. Digital-агентство:?ализируется на цифровой рекламе, включая поиск, социальные сети, email-рассылку и т.д.
2. Full-service-агентство: предлагает полный спектр услуг, включая разработку рекламной стратегии, создание контента и медиапланирование.
3. Брендинговое агентство: специализируется на разработке бренда, включая создание логотипа, упаковки и т.д.
4. Event-агентство: организует и продвигает мероприятия, такие как конференции, семинары, выставки и т.д.
5. PR-агентство: занимается по связям с общественностью, включая общение с СМИ, кризис-менеджмент и т.д.
Также рекламные агентства могут иметь различные бизнес-модели, такие как:
1. Фиксированная плата: агентство получает фиксированную плату за свои услуги.
2. Комиссионная плата: агентство получает комиссию от рекламного бюджета клиента.
3. Результативная плата: агентство получает плату только в случае достижения определенных результатов, таких как увеличениеconversion rate или дохода.
Наши услуги
На сайтах наших клиник, Вы можете посмотреть полный перечень услуг, оказываемых в наших клиниках, а также сразу узнать, в каком конкретном направлении работает тот или иной ветеринарный врач, чтобы сразу записаться на прием к нужному специалисту.
Лечение
19 услуг
такие как
ветеринарная стоматологическая клиника в спб
обращайтесь к нам мы работаем 24 на 7 наши специалисты вас проконсультируют если есть какие нибудь вопросы
https://lifevet.ru/
123
Добрый день!
Где заказать диплом по актуальной специальности?
Заказать документ института можно у нас в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы СССР. Даем гарантию, что при проверке документа работодателем, подозрений не появится.
https://aqvakr.forum24.ru/?1-7-0-00010768-000-0-0-1718284764
Хорошей учебы!
You’ve made some good points there. I looked on the net to learn more about the issue and found most people will go along with your views on this site.
my blog post: 해외스포츠중계
Добрый день!
Где заказать диплом по нужной специальности?
Мы можем предложить документы институтов, которые расположены в любом регионе РФ. Можно заказать диплом от любого ВУЗа, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на бумаге высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и подписями.
Мы готовы предложить дипломы любых профессий по разумным ценам.
ast-diploms.com
Будем рады вам помочь!
Have you ever thought about publishing an e-book or guest authoring on other blogs?
I have a blog based upon on the same topics you discuss and would love
to have you share some stories/information. I know my readers would value your work.
If you’re even remotely interested, feel free to shoot me an email.
My web page – 2nd story addition
Преимуществами покупки оборудования в лизинг для юридических лиц можно считать: Низкие затраты на получение оборудования в пользование лизинг оборудования для малого бизнеса
Как заказать стриптиз на дом, в лофт, на мальчишник или девичник? Прежде всего выберите сами артиста из каталога и позвоните нам, или наш менеджер самостоятельно подберет Вам хорошего танцора по вашим запросам Стриптиз
Здравствуйте!
Мы изготавливаем дипломы любых профессий по приятным ценам.
Мы предлагаем документы техникумов, расположенных на территории всей РФ. Можно заказать качественный диплом от любого заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Документы печатаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригиналов. Документы будут заверены всеми необходимыми печатями и штампами.
Гарантируем, что в случае проверки документов работодателем, каких-либо подозрений не возникнет.
Где приобрести диплом специалиста?
russiajoy.ru/unikalnyie-diplomyi-dlya-unikalnyih-lichnostey
Привет!
Купить документ института можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы образца СССР. Даем гарантию, что в случае проверки документов работодателями, подозрений не возникнет.
Наши специалисты предлагают быстро приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Наш документ пройдет лубую проверку, даже при использовании специально предназначенного оборудования. Достигайте свои цели максимально быстро с нашим сервисом.
Где приобрести диплом специалиста?
http://cobaki.ru/users.php?m=details&id=90788
Успехов в учебе!
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить аттестаты за 11, купить диплом в йошкар-оле, купить диплом программиста, купить диплом психолога, купить диплом в нижнем тагиле, а потом наткнулся на https://mecool.com.ru/mecool-mxv-4k/#comment_2062, где все мои учебные проблемы были решены!
Успешной учебы!
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Place your bet at pinup online – very prestigious bookmaker in Kazakhstan
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
jasminer X44-Q
Добрый день!
Мы готовы предложить дипломы любой профессии по приятным ценам. Стоимость будет зависеть от выбранной специальности, года получения и образовательного учреждения.
Где приобрести диплом специалиста?
Приобрести диплом любого ВУЗа
https://landik-diploms-srednee.ru/kupit-diplom-sssr
Хорошей учебы!
Привет, друзья!
Где приобрести диплом специалиста?
Мы готовы предложить документы институтов, расположенных в любом регионе Российской Федерации. Вы можете купить качественно сделанный диплом за любой год, включая документы старого образца. Дипломы выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригиналов. Документы заверяются всеми необходимыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по приятным ценам.
diplomyx.com
Поможем вам всегда!
https://nudifyai.net/
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Place your bet at pinup online – direct reliable bookmaker in Kazakhstan
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Активируйте Vavada казино промокоды и получите доступ к уникальным бонусам. Наслаждайтесь игрой с дополнительными привилегиями и предложениями от Vavada казино.
Преимуществами покупки оборудования в лизинг для юридических лиц можно считать: Низкие затраты на получение оборудования в пользование лизинг косметологического оборудования
Ищете лучшие промокоды для Drip казино? Получите эксклюзивные бонусы и наслаждайтесь игрой с дополнительными привилегиями. Активируйте Drip казино промокоды и играйте с удовольствием.
Активируйте Vavada казино промокоды и получите доступ к эксклюзивным бонусам. Наслаждайтесь игрой с дополнительными привилегиями и предложениями от Vavada казино.
Автомобиль в кредит под такси – купить новый китайский автомобиль, купить geely atlas pro
Здравствуйте!
Приобрести документ института можно у нас. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, включая документы образца СССР. Гарантируем, что при проверке документа работодателем, никаких подозрений не возникнет.
Мы предлагаем выгодно и быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, штампами, подписями должностных лиц. Наш диплом пройдет лубую проверку, даже при помощи специального оборудования. Решите свои задачи быстро и просто с нашей компанией.
Где купить диплом по необходимой специальности?
http://xn--80aakbafh6ca3c.xn--p1ai/index.php?subaction=userinfo&user=ovyboh
Успехов в учебе!
Добрый день!
Для многих людей, приобрести диплом ВУЗа – это острая потребность, шанс получить отличную работу. Однако для кого-то – это банальное желание не терять время на учебу в ВУЗе. Что бы ни толкнуло вас на такое решение, наша фирма готова помочь. Оперативно, профессионально и выгодно сделаем диплом нового или старого образца на подлинных бланках с реальными подписями и печатями.
Наша компания предлагает максимально быстро заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями официальных лиц. Документ способен пройти любые проверки, даже с применением специфических приборов. Достигайте своих целей быстро и просто с нашим сервисом.
Где приобрести диплом по необходимой специальности?
http://www.lada-xray.net/member.php?u=2434
Удачи!
Подарок шефу своими руками и шоколад в упаковке оптом.
https://giftbox-3.ru/
https://gosznakdublikat.ru/
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом бакалавра, купить диплом в батайске, купить диплом лаборанта, купить свидетельство о разводе, купить диплом сантехника. Постепенно углубляясь, нашел отличный ресурс здесь:
http://krutovo.ru/index.php?name=Account&op=info&uname=osezeziqy
http://silkhunter.com/index.php?title=russianydiplomans
http://diabetesarmy.com/blog-post-title/?unapproved=49817&moderation-hash=3f08ecbeabfc82cdf0d91411cb23c493#comment-49817
https://rosgosts.ru/67/220/gost_32053-2013/
http://www.voidofheroes.com/forums/member.php?action=profile&uid=53584
, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успехов в учебе!
among us mod menu – genshin impact mods, free valorant skin changer
Even although the jackpot was not hit, lotteries are urging players to check their tickets for one of the nine
approaches to win.
Here is my site; Nina
Good evening!
I want to share with you the secret of how to save not only money but also time when buying medicines. Do you know how often you have to run around pharmacies looking for a bargain price? Well, here I have great news – you don’t have to do that anymore!
Go to >> Pharmacy Review <> Pharmacy Review <> Pharmacy Review << and save now!
Sharing our experiences and supporting colleagues – together we are even stronger!
lasix over 2 minutes to avoid
sodium chloride flush for lasix
john and tanya gunther lasix
lose weight on lasix
what over the counter substance works like lasix
lasix for heart murmur in dogs
lasix metabolic acidosis
lasix proteinuria
iv compatibility lasix
furosemide lasix contraindications
maximum dose of lasix in pulmonary edema
lasix center dutchmans lane
where to buy lasix for horses
lasix injection sanofi
lasix/furosemide
cat panting after lasix
lasix for mac
can lasix cause you to have congestion
generic lasix identification
is lasix stronger than hydrochlorothiazide
lasix usage leglly
is furosemide and lasix the same
lasix aldactone combination
lasix tablet untuk apa
how to take metolazone and lasix
mitigenie lasix
lasix im injection site
buy furosemide lasix
lasix neonatal dose
lasix nella dieta
convert torsemide to lasix
how does lasix affect gfr
lasix and intestinal gas
iv lasix drip
is lasix contraindicated for patients undergoing ect
quando prendere lasix
lasix iv push over 2 minutes to avoid
can lasix cause a fast heart beat
lasix renal scan obstruction parameter
lasix dosage iv to po
norway furosemide or lasix 40 mg
lasix sulfa drug allergy
drinking beer or wine while taking lasix
lasix is nephrotic drugs
lasix can't keep eyes open
what do lasix do
lasix pediatric
Подарок футбольному болельщику и упаковка для шоколада ручной работы купить оптом.
https://giftbox-3.ru/
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом фитнес инструктора, купить диплом в нижневартовске, купить диплом архитектора, купить диплом о среднем образовании, купить диплом в арзамасе, постепенно вникая в суть дела нашел отличный материал здесь https://tastebuds.fm/topics/7635-hei-tarvitsen-apuasi и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Удачи!
http://buyprepaid-cards.cvv2cvc.net
Item 01 Card Total Balance: $3 100 – Price $ 110.00
Item 03 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2 000 – Price $ 149.00
Item Western Union Transfers $1 000 – Price $ 99.00
Item Western Union Transfers $300 – Price $ 249.00
*Prices on the website may vary slightly
Store Cloned cards Store Western Union
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в воронеже, купить диплом в троицке, купить диплом в березниках, купить диплом электромонтажника, купить диплом швеи, затем наткнулся на http://welovestats.com/uncategorized/hello-world/?unapproved=108983&moderation-hash=da8e7e2d87cb3a58f142bc279a4988f1#comment-108983, где все мои учебные вопросы были решены!
Удачи!
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в минусинске, купить дипломы о высшем, купить диплом в мурманске, купить диплом в ревде, купить диплом техникума. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://chelmaps.ru/user/dvywbsolff/
https://nsk-asl.ru/forum/messages/forum1/topic74/message74/?result=new
https://thadthong.go.th/forum/suggestion-box/364826-dipl
https://caezar.4bb.ru/viewtopic.php?id=4269#p18292
https://www.habitat-junior.com/nos-concepts/page-carte-jules-verne/#comment-32257
и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом нового образца, купить диплом в нефтеюганске, купить речной диплом, купить диплом в минусинске, купить диплом в сызрани, получил базовую информацию.
Остановился в итоге на материале купить диплом в красноярске, http://tr.clanfm.ru/viewtopic.php?f=39&t=10093&p=20006#p20006
Хорошей учебы!
We stumbled over here by a different web page and thought I might check things out.
I like what I see so now i’m following you. Look forward to
going over your web page repeatedly. http://Www.Gotanproject.net/node/23617221?——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22title%22%0D%0A%0D%0APeinture%20Polyur%C3%A9thane%20Rona%20%C3%A0%20Laval%20:%20Guide%20d’Utilisation%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22body%22%0D%0A%0D%0A%3Cspan%20style=%22font-weight:%20bolder;%22%3ELorsque%20vous%20recherchez%20une%3C/span%3E%20peinture%20polyur%C3%A9thane%20de%20qualit%C3%A9%20%C3%A0%20Laval,%20Rona%20est%20une%20marque%20r%C3%A9put%C3%A9e%20offrant%20une%20s%C3%A9lection%20de%20produits%20adapt%C3%A9s%20%C3%A0%20vos%20besoins.%20Voici%20un%20informations%20d’utilisation%20pour%20la%20peinture%20polyur%C3%A9thane%20Rona.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A1.%20Pr%C3%A9paration%20d’une%20surface%20:%20Avant%20d’utiliser%20la%20peinture,%20assurez-vous%20que%20la%20sol%20est%20personnel,%20s%C3%A8che%20et%20exempte%20de%20toute%20crasse,%20poussi%C3%A8re%20ou%20particule.%20Poncez%20avec%20d%C3%A9sinvolture%20si%20n%C3%A9cessaire%20pour%20%C3%A9liminer%20les%20imperfections.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cimg%20src=%22https://p.turbosquid.com/ts-thumb/Xe/pR79kV/lvBpxSrk/bottlegrinder_001/jpg/1540992948/600×600/fit_q87/18b2f7ae979cc599d04f9a90e5f502434f7a26b1/bottlegrinder_001.jpg%22%20style=%22max-width:400px;float:left;padding:10px%2010px%2010px%200px;border:0px;%22%3E2.%20S%C3%A9lection%20d’une%20peinture%20:%20Rona%20propose%20diff%C3%A9rents%20vari%C3%A9t%C3%A9s%20de%20peinture%20polyur%C3%A9thane,%20tels%20que%20les%20finis%20satin%C3%A9s,%20brillants%20ou%20mats.%20Choisissez%20le%20type%20de%20fini%20qui%20correspond%20%C3%A0%20l’effet%20d%C3%A9sir%C3%A9%20par%20votre%20d%C3%A9fi.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0Atrois.%20Pr%C3%A9paration%20d’une%20peinture%20:%20Suivez%20attentivement%20les%20instructions%20du%20producteur%20%3Ca%20href=%22https://www.Color3i.ca/isocyanates/%22%3ENormes%20sur%20COV%20et%20isocyanates:%20Conformit%C3%A9%20et%20pratiques%3C/a%3E%20%3Cspan%20style=%22text-decoration:%20underline;%22%3El’%C3%A9tiquette%20d’une%20peinture%3C/span%3E%20Rona.%20Assurez-vous%20de%20efficacement%20m%C3%A9langer%20la%20peinture%20pr%C3%A9c%C3%A9dent%20utilisation%20et,%20que%20ce%20soit%20ou%20non%20n%C3%A9cessaire,%20diluez-la%20conform%C3%A9ment%20%C3%A0%20les%20suggestions%20sp%C3%A9cifiques.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0Aquatre.%20Application%20de%20la%20peinture%20:%20Utilisez%20un%20pinceau%20de%20qualit%C3%A9%20ou%20un%20rouleau%20en%20mousse%20par%20appliquer%20la%20peinture%20%3Ca%20target=%22_blank%22%20href=%22https://www.Color3i.ca/isocyanates/%22%3Enormes%20sur%20cov%20et%20isocyanates:%20Conformit%C3%A9%20et%20pratiques%3C/a%3E%20%3Cspan%20style=%22text-decoration:%20underline;%22%3Ela%20surface%3C/span%3E.%20%3Cem%3EAssurez-vous%20de%20comprendre%3C/em%3E%20dans%20des%20mouvements%20r%C3%A9guliers%20et%20de%20ne%20pas%20utiliser%20une%20couche%20de%20peinture%20trop%20%C3%A9paisse%20par%20%C3%A9viter%20les%20coulures.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A5.%20Temps%20de%20s%C3%A9chage%20:%20Respectez%20le%20temps%20de%20s%C3%A9chage%20indiqu%C3%A9%20%3Ca%20target=%22_blank%22%20href=%22https://www.Color3i.ca/isocyanates/%22%3ENormes%20sur%20COV%20et%20isocyanates:%20Conformit%C3%A9%20et%20pratiques%3C/a%3E%20l’emballage%20d’une%20peinture%20Rona.%20Assurez-vous%20de%20laisser%20suffisamment%20de%20temps%20par%20que%20la%20peinture%20s%C3%A8che%20compl%C3%A8tement%20avant%20de%20gouverner%20la%20sol%20ou%20d’appliquer%20une%20autre%20couche.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A6.%20Finition%20et%20s%C3%A9curit%C3%A9%20:%20Si%20essentiel,%20vous%20pouvez%20utiliser%20une%20deuxi%C3%A8me%20couche%20de%20peinture%20pour%20obtenir%20une%20meilleure%20couverture%20et%20un%20aspect%20plus%20uniforme.%20Vous%20pouvez%20%C3%A9galement%20appliquer%20un%20vernis%20de%20finition%20pour%20garder%20la%20sol%20et%20am%C3%A9liorer%20sa%20durabilit%C3%A9.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A7.%20Nettoyage%20des%20outils%20:%20Nettoyez%20vos%20pinceaux%20et%20autres%20instruments%20imm%C3%A9diatement%20apr%C3%A8s%20utilisation%20%C3%A0%20l’assistance%20d’eau%20ti%C3%A8de%20et%20de%20savon%20de%20nettoyage.%20Assurez-vous%20de%20retirer%20toute%20indice%20de%20peinture%20pour%20pr%C3%A9server%20la%20norme%20de%20vos%20instruments.%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0A%3Cbr%3E%0D%0A%3Cbr%3E%0D%0A%0D%0ALa%20peinture%20polyur%C3%A9thane%20Rona%20est%20un%20merveilleux%20choix%20pour%20vos%20initiatives%20de%20finition%20%C3%A0%20Laval.%20Suivez%20les%20instructions%20du%20fabricant%20et%20utilisez%20les%20produits%20appropri%C3%A9s%20par%20obtenir%20les%20meilleurs%20r%C3%A9sultats.%20N’h%C3%A9sitez%20pas%20%C3%A0%20solliciter%20pour%20recommandation%20%C3%A0%20un%20professionnel%20si%20vous%20avez%20des%20questions%20sp%C3%A9cifiques%20%C3%A0%20votre%20d%C3%A9fi.%3Cimg%20src=%22https://p.turbosquid.com/ts-thumb/ab/pYCfSG/sA/untitled1/jpg/1661161833/600×600/fit_q87/4d557b152d82811b60f97aa274307a0d80c4debd/untitled1.jpg%22%20style=%22max-width:430px;float:right;padding:10px%200px%2010px%2010px;border:0px;%22%3E%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22field_pays[value]%22%0D%0A%0D%0ASolomon%20Islands%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22changed%22%0D%0A%0D%0A%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22form_build_id%22%0D%0A%0D%0Aform-180606997b5886c6e2996450dc2baca0%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22form_id%22%0D%0A%0D%0Alivredor_node_form%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22field_ville[0][value]%22%0D%0A%0D%0AKristiansand%20S%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22field_email[0][email]%22%0D%0A%0D%0A%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx%0D%0AContent-Disposition:%20form-data;%20name=%22op%22%0D%0A%0D%0AEnregistrer%0D%0A——WebKitFormBoundaryV0kXtaUZzvHahPqx–
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом в нижнекамске, купить диплом в канске, куплю диплом с занесением, купить диплом в пскове, купить диплом биолога, получил базовую информацию.
Остановился в итоге на материале купить диплом в ханты-мансийске, http://www.telefonnyjdovidnyk.com.ua/nomer/0631393415/
Удачи!
На сайте https://chargebackhelp.ru/ изучите информацию, которая касается чарджбэка. Вы узнаете о том, как можно вернуть деньги у брокера, что представляет собой данная процедура, как правильно использовать ее возможности и каким образом получить деньги. Вся информация от высококлассного специалиста, который отлично понимает в данной теме. Здесь вся информация подробно описана, чтобы вы смогли лучше в ней сориентироваться. Есть информация и о том, с карточками каких банков могут быть трудности при возвращении средств.
online binchecker service for credit debit – IIN lookup identify card issuing bank name, bin database search
фильмы которые уже вышли – смотреть фильмы онлайн новинки бесплатно, новинки кино смотреть бесплатно онлайн
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в кинешме, купить диплом в уссурийске, купить диплом в новотроицке, купить диплом в первоуральске, купить речной диплом, а затем перешел на дипломы вузов. Подробнее можно узнать здесь:
https://lenzuolashop.ru/postelnoe-bele-dlya-vzroslikh/postelnoe-bele-karven-satin-de-lyuks-3d-15-spaln-367/
http://sabrina-online.su/wiki/index.php?title=premialniediplom
http://j95370pe.bget.ru/main/263-vot-kudy-otvechala-pomeschica-moe-takoe.html
https://rf-lowrate.ru/index.php?/topic/4145-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-s641c/
http://gafp.be/index.php?option=com_easybookreloaded
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успешной учебы!
Привет!
Где заказать диплом по нужной специальности?
Приобретение диплома университета России у нас – надежный процесс, так как документ будет заноситься в реестр. При этом печать выполняется на специальных бланках ГОЗНАКа.
Вы заказываете документ в надежной и проверенной временем компании.
https://smd.mybb.ru/viewtopic.php?id=3666#p22170
Хорошей учебы!
Casinos like Ignition and Bitstarz need players to verify
their identity just before processing withdrawals.
Feel free to surf too myy web-site … discover more here
best site glory casino bangladesh
jasminer X44-Q
jasminer X44-Q
jasminer X44-Q
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом автомеханика, купить диплом института, купить диплом в альметьевске, купить диплом в норильске, купить диплом провизора, потом про дипломы вузов, подробнее здесь
http://cinemania.forum24.ru/?1-15-0-00001204-000-0-0-1718282013
https://nailpub.ru/forum/threads/%D1%80%D0%B8%D1%82%D1%83%D0%B0%D0%BB%D1%8C%D0%BD%D1%8B%D0%B5-%D1%82%D0%BE%D0%B2%D0%B0%D1%80%D1%8B-%D1%82%D0%B0%D0%B1%D0%BB%D0%B8%D1%87%D0%BA%D0%B8.40271/#post-1148715
http://xn—-7sbgj9bdrl.xn--p1ai/users/ijuruf
http://kyym.ru/sonunnar/main/10920-uluustaa-y-beterineriije-salaatygar-aan-bastakytyn-beterineer-aatyn-i-erdiler/
http://thevorheesfamily.com/gbook/?bid=1
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Хорошей учебы!
Amazing! Its in fact awesome paragraph, I have got much clear idea about from this paragraph.
my web site austin copiers
Wow! In the end I got a blog from where I know how to actually obtain useful
facts regarding my study and knowledge.
Look into my web site – copiers austin
Its like you read my mind! You seem to know a lot about this, like you wrote the book in it or
something. I think that you can do with some pics to drive the message home a little bit, but instead of that, this
is excellent blog. An excellent read. I will certainly be back.
Feel free to surf to my web-site Houston copiers
I blog frequently and I genuinely thank you for your content.
This article has truly peaked my interest.
I will take a note of your site and keep checking for new information about once
a week. I subscribed to your RSS feed too.
Also visit my blog – asbestos removal in ottawa
Добрый день!
Где заказать диплом по необходимой специальности?
Мы предлагаем документы техникумов, расположенных на территории всей РФ. Документы будут заверены необходимыми печатями и подписями.
Заказать диплом любого ВУЗа:
https://daltonsuwza.pointblog.net/????????-??????-???????-68728767
Magnificent goods from you, man. I’ve understand your stuff previous to and you
are just extremely great. I really like what you’ve acquired here,
really like what you’re saying and the way in which you say it.
You make it entertaining and you still take care of to
keep it sensible. I cant wait to read much more from you. This is actually a tremendous website.
Also visit my site: copier repair San Antonio
Why visitors still make use of to read news papers when in this technological globe all is available on web?
Feel free to surf to my web-site https://skyenorthlogistics.com/index.php/2024/07/10/maximizing-on-line-casino-bonuses-strategies-for-success-2/
I was able to find good advice from your content.
Feel free to visit my website … Ottawa asbestos removal
It was Ohio’s fifth-largest jackpot prize, news reports
show, and the ticket was bought aat GetGo
Cafe and Markt in Macedonia, Ohio.
Review my web page – 동행복권 스피드키노
Way cool! Some very valid points! I appreciate you penning this
post plus the rest of the website is also very good.
Here is my web blog – asbestos ottawa
Добрый день!
Где купить диплом специалиста?
Заказать документ института можно у нас. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов Российской Федерации.
Наши специалисты предлагают быстро и выгодно купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Диплом способен пройти лубую проверку, даже с использованием специально предназначенного оборудования. Решите свои задачи быстро с нашей компанией.
http://poeskovek.flybb.ru/topic156.html
http://justvoip.listbb.ru/viewtopic.php?f=2&t=363
https://saumalkol.com/forum/%D1%80%D0%B0%D0%B7%D0%BD%D0%BE%D0%B5-1/1454-%D1%80%D0%B0%D1%81%D1%81%D1%87%D0%B8%D1%82%D1%8B%D0%B2%D0%B0%D0%B5%D1%82%D0%B5-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%80%D0%BE%D1%81%D1%81%D0%B8%D0%B9%D1%81%D0%BA%D0%BE%D0%B3%D0%BE-%D1%83%D0%BD%D0%B8%D0%B2%D0%B5%D1%80%D1%81%D0%B8%D1%82%D0%B5%D1%82%D0%B0-%D0%B3%D0%BE%D1%82%D0%BE%D0%B2%D1%8B-%D0%BF%D0%BE%D0%BC%D0%BE%D1%87%D1%8C.html
http://lossantosbattalion17.listbb.ru/viewtopic.php?f=3&t=213
https://familyportal.forumrom.com/viewtopic.php?id=20411#p55425
This post is really a good one it assists new the web
viewers, who are wishing for blogging.
Look into my homepage Ottawa asbestos removal
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в озёрске, купить диплом в туапсе, старые дипломы купить, купить диплом в кстово, купить диплом в алуште, потом попал на http://xn—-7sbgj9bdrl.xn--p1ai/users/ijuruf
http://vaz-lada.com/p/zashita-razdatki-toyota-hilux-s-2015-nv-23559/reviews/
http://artem-energo.ru/forums.php?m=posts&q=17299&n=last#bottom
http://ninokuni.ru/member.php?action=profile&uid=2100
https://stoligra.ru/products/golovolomka-kubik–cast-puzzle-cuby-uroven-slozhnosti-4/#comment_67394
и там решили все мои учебные заботы!
Успешной учебы!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в майкопе, купить диплом строителя, купить диплом в кунгуре, купить диплом во владивостоке, купить диплом железнодорожника, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://citydevelopers.ru/otzyvy/novosibirsk/zhk-voskresnyy/
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успехов в учебе!
Добрый день!
Где приобрести диплом специалиста?
Наша компания предлагает быстро и выгодно купить диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Документ пройдет лубую проверку, даже при использовании специальных приборов. Решайте свои задачи быстро и просто с нашей компанией.
Купить диплом о высшем образовании.
http://c904581v.beget.tech/2024/07/09/nizkie-ceny-i-prekrasnoe-kachestvo-pokupay-dokumenty-onlayn.html
https://fighter71.com/read-blog/1696
https://forum.zentox-rp.ru/index.php?app=gallery&module=gallery&controller=view&id=12
https://ourehelp.com/read-blog/3947
https://network-6342899.mn.co/posts/61828984
Great blog here! Also your web site loads up very fast!
What host are you using? Can I get your affiliate link to your host?
I wish my site loaded up as quickly as yours lol
my blog post Schach Mousepads
Can I simply say what a comfort to discover somebody
who genuinely knows what they’re talking about on the web.
You definitely realize how to bring a problem to light
and make it important. A lot more people really need to check this out
and understand this side of your story. I can’t believe you aren’t more popular
because you surely have the gift.
my blog post … https://learningpave.in/a-guide-to-recognizing-the-best-online-casinos-for-slot-players/
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в соликамске, купить диплом в барнауле, купить диплом массажиста, купить диплом в георгиевске, купить диплом технолога, потом попал на https://www.generate-bookmark.win/opening-prospective-the-power-of-a-diploma
https://laflore.ru/sale/micenil-unikalnyj-razvod-na-gribke-nogtej.html#comment-94980
https://uscrestoration.com/hello-world/#comment-28204
https://vadaszapro.eu/user/profile/1264947
https://otriunvirato.com.br/percy-jackson-rick-riordan-anuncia-que-a-serie-foi-aprovada-pelo-disney/
и там решили все мои учебные заботы!
Успешной учебы!
Hello, yes this post is really nice and I have learned lot of things from it concerning blogging.
thanks.
Here is my website; copier service Houston
SMM Provider – SMM Panel API, Best SMM Panel
Hello colleagues, how is the whole thing, and what you desire
to say on the topic of this paragraph, in my view its really remarkable in support of
me.
My blog asbestos removal ottawa
2nd Possibility promotion odds are dependent upon the number
of entries received.
Here is my website … Debora
https://cyprusrent.ru/
You need to be a part of a contest for one of the most
useful sites on the web. I will recommend this web site!
Here is my web blog: asbestos
Really no matter if someone doesn’t be aware of afterward its up to other visitors
that they will assist, so here it happens.
Also visit my web page – asbestos abatement ottawa
пин ап – онлайн казино, пин ап
This is my first time pay a quick visit at here and i am actually happy to read
all at single place.
My homepage – austin copier leasing
I have been browsing online greater than three hours nowadays,
but I by no means found any attention-grabbing article like yours.
It’s pretty price enough for me. In my opinion, if all
web owners and bloggers made just right content material as you did, the web might be a lot more helpful
than ever before.
Visit my site … asbestos removal ottawa
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в анжеро-судженске, купить диплом о высшем образовании, купить диплом в великих луках, купить диплом в соликамске, купить диплом в шахтах. Постепенно углубляясь в тему, нашел отличный ресурс здесь: http://zamki.kwartet33.ru/index.php?subaction=userinfo&user=acuzys и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успехов в учебе!
Greetings I am so excited I found your blog page, I really found you by error, while I was looking on Askjeeve for something else,
Anyways I am here now and would just like to say thanks a lot for a remarkable post and a all round thrilling blog (I also love the theme/design), I don’t have time to look over it all at the minute but I have saved it and also included your RSS feeds, so when I have time I will be back to
read more, Please do keep up the great work.
Here is my website … copier leasing austin
Thanks for every other wonderful post. Where else may just anyone
get that kind of info in such an ideal means of writing?
I’ve a presentation next week, and I’m on the search for such information.
my blog post – asbestos removal near me
Ведущий праздников – это человек, который ответственен за организацию и проведение праздничных мероприятий, таких как корпоративные вечера, частные праздники, свадьбы, дни рождения и т.д. Ведущий праздников обычно является лицом, которое обеспечивает развлекательную программу, общается с гостями, контролирует ход мероприятия и создает праздничную атмосферу.
Обычно, ведущий праздниковantwort за следующиеaspectы праздника:
1. Разработка сценария мероприятия и координация его выполнения.
2. Развлекательная программа: выбор артистов, музыки, игр и других мероприятий.
3. Организация и проведение конкурсов, игр и других конкурсных мероприятий.
4. Управление временем и расписанием мероприятия.
5. Общение с гостями, отвечая на их вопросы и обеспечивая их комфорт.
6. Координация с техническим персоналом,such as sound engineers, lighting technicians, and other event staff.
7. Решение нештатных ситуаций и кризисных ситуаций, которые могут возникнуть в ходе мероприятия.
Ведущий праздников harus быть харизматичным, иметь грамотную речь и навыки общения, бытьorganizovanny и уметь работать под давлением времени.
заказть можно организатора у нас Организация корпоративных мероприятий
время работы с 8.00 до 19.00 званите будем рады вам помочь
123
Howdy! This post could not be written much better!
Looking through this article reminds me of my previous roommate!
He constantly kept talking about this. I will forward this
article to him. Fairly certain he’ll have a great read.
Thanks for sharing!
Here is my web-site – asbestos
My programmer is trying to persuade me to move to .net from PHP.
I have always disliked the idea because of the costs. But he’s
tryiong none the less. I’ve been using WordPress
on various websites for about a year and am
concerned about switching to another platform. I have heard great things about blogengine.net.
Is there a way I can import all my wordpress posts into
it? Any kind of help would be really appreciated!
Look into my web blog asbestos abatement ottawa
Buy Clon Card Store Cloned cards
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $ 500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://prepaid-cards.cvv2cvc.com
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом в нижнем новгороде, купить диплом инженера, купить диплом ветеринара, купить диплом, купить диплом в копейске, получил базовую информацию.
Остановился в итоге на материале купить диплом парикмахера, https://xxxfree.watch/legal/#comment-179
https://www.mei-health.com/blog/
https://suankluai.go.th/forum/suggestion-box/833273-dipl
http://www.rrsclub.ru/showthread.php?p=40295#post40295
https://deporteshoy.com.ar/2018/01/fallecio-juan-carlos-cacalo-rissone/
Хорошей учебы!
tetris movie parents review movieslittle women of atlanta new seasonbanner of heaven how many episodesfunyy movies
Привет, друзья!
Где купить диплом специалиста?
Приобрести документ ВУЗа можно в нашем сервисе. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, любого года выпуска, в том числе документы старого образца. Даем гарантию, что при проверке документа работодателями, подозрений не возникнет.
http://1e.kz/product/m3-plus-%d0%bc%d1%83%d0%b6%d1%81%d0%ba%d0%b8%d0%b5-%d1%81%d0%bc%d0%b0%d1%80%d1%82-%d1%87%d0%b0%d1%81%d1%8b-%d1%86%d0%b2%d0%b5%d1%82%d0%bd%d0%be%d0%b9-%d1%8d%d0%ba%d1%80%d0%b0%d0%bd-ip67-%d0%b2%d0%be/?unapproved=4083&moderation-hash=8cc40db0776bea7a9626d31ec6aac114#comment-4083
Успешной учебы!
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в нижнем тагиле, купить диплом в северске, купить диплом вуза, купить диплом в ангарске, купить аттестат за 9 класс, потом попал на https://www.eventnn.ru/articles/item/0/8574/ и там решили все мои учебные заботы!
Удачи!
Hype Casino
Привет!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
Мы можем предложить документы техникумов, расположенных в любом регионе Российской Федерации. Вы сможете приобрести диплом от любого заведения, за любой год, в том числе документы старого образца СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Они будут заверены всеми обязательными печатями и подписями.
Гарантируем, что при проверке документов работодателями, каких-либо подозрений не появится.
Где купить диплом специалиста?
http://www.find-topdeals.com/blogs/120485/??????-??-???????-?????????-???????????-???????-?????????????-?????-?????????
Здравствуйте!
Где приобрести диплом специалиста?
Мы предлагаем документы ВУЗов, которые расположены на территории всей Российской Федерации. Можно заказать диплом от любого ВУЗа, за любой год, включая сюда документы СССР. Дипломы делаются на “правильной” бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, которые невозможно отличить от оригиналов. Документы заверяются всеми обязательными печатями и штампами.
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
https://diplomyx.com/otzyvy
Всегда вам поможем!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в димитровграде, купить диплом в альметьевске, купить диплом маляра, купить диплом автомеханика, купить диплом в белово, а затем перешел на дипломы вузов. Подробнее можно узнать здесь:
http://www.koelnmedia2.de/fastelovend/member.php?action=showprofile&user_id=14487
http://smecenter.utcc.ac.th/index.php?option=com_k2&view=itemlist&task=user&id=369668
https://myportal.utt.edu.tt/ICS/_portletview_/Campus_Life/Campus_Groups/Safer/Discussion.jnz?portlet=Forums&screen=PostView&screenType=change&id=0fb18262-309e-479c-99cd-5d9d4f162517
http://myskupera.ru/forum/messages/forum1/topic12/message60614/?result=reply#message60614
http://blackpearlbasketball.com.au/index.php?option=com_k2&view=itemlist&task=user&id=829712
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Хорошей учебы!
эскорт москва – эскорт услуги москва, москва эскорт агентство
http://remontwasher.ru/
We’ve all made email marketing mistakes: You click send on an email and suddenly your stomach drops. You’ve made a mistake and there’s nothing you can do about it Typography in UI Design: Choosing Fonts that Enhance User Engagement
Добрый день!
Где купить диплом специалиста?
Готовый диплом со всеми печатями и подписями отвечает стандартам Министерства образования и науки, никто не отличит его от оригинала – даже со специальным оборудованием.
Приобрести диплом о высшем образовании.
https://israelafrica.mn.co/posts/61899438
https://www.seaman.com.ua/forum/index.php?login/login
https://antspride.com/read-blog/711
https://gaysocial.gay/read-blog/82
https://lebanonhub.app/blogs/2398/%D0%97%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%A1%D0%BE%D0%B2%D0%B5%D1%82%D1%8B-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%BE%D0%B2
Промокоды Vavada казино – ваш путь к дополнительным бонусам и уникальным предложениям. Активируйте промокод и наслаждайтесь игрой с привилегиями от Vavada казино.
купить официальный аттестат ast-diplom.com .
Промокоды Drip казино открывают доступ к уникальным бонусам и предложениям. Активируйте промокод и получите больше от вашей игры в Drip казино.
Промокоды Vavada казино – это возможность получить дополнительные бонусы. Воспользуйтесь этими промокодами и наслаждайтесь игрой с привилегиями.
диплом о высшем медицинском образовании купить диплом о высшем медицинском образовании купить .
москва эскорт агентство – эскорт услуги москва, vip эскорт москва
Добрый день!
Заказать диплом университета.
Наш сервис предлагает приобрести диплом отличного качества, неотличимый от оригинала без использования дорогостоящего оборудования и опытного специалиста.
Где приобрести диплом специалиста?
https://armit.ru/social/user/42552/forum/message/1551/1553/#message1553
Удачи!
Ищете лучшие промокоды для Vavada казино? Используйте Vavada казино промокоды для получения эксклюзивных бонусов и наслаждайтесь игрой.
Pin-Up Casino is an online gambling platform known for its vibrant, retro-inspired design and wide range of gaming options. Catering to a global audience, Pin-Up Casino offers a variety of games, including slots, table games, live casino experiences, and sports betting. The platform is characterized by its user-friendly interface and an extensive library of games from leading software providers.
https://artic.readme.io/reference/pin-up-casino-%C3%B6deme-g%C3%BCvenli%C4%9Fi
https://www.thegunners.org.uk/raa-forum/pin-up-casino-mobil-uyumlu-olarak-gelistirildi/show
https://divarlovv.wixsite.com/bestart/pin-up-online-casino-t%C3%BCrkiye
https://demo.hedgedoc.org/s/iWCbRvHR1
https://g80.bimmerpost.com/forums/album.php?albumid=23255&pictureid=103180
https://sites.google.com/view/pin-up-online-casino-turkiye/
https://pin-up-casino-giris.mystrikingly.com/
https://articworlds.blogspot.com/2024/07/guvenle-spor-bahisleri-yapmak-pin-up.html
https://webhitlist.com/profiles/blogs/canl-krupiyeli-deneyim-pin-up-casino-da-kumarhaneyi-size
https://we.riseup.net/johnsteele/pin-up-casino
https://www.mycitizensnews.com/author/RyanFranklin/
https://www.marqueze.net/miembros/georgeallen/profile/classic/
https://community.goldposter.com/zh/members/franklinhudson/profile/
https://teampages.com/teams/2010586-BestTeam-10-pin-bowling-team-website/announcements/2362771
https://www.lookingforclan.com/clans/pin-casinoda-slot-makinesi-seceneklerini-kesfetmek-sonsuz-eglence-sizi-bekliyor
https://www.flickr.com/groups/14870348@N21/discuss/72157721921318028
https://www.apsense.com/article/pinup-online-casino-trkiye-giri-ve-yelik-rehberi.html
https://www.storeboard.com/blogs/gaming/pin-up-casinoda-y%C3%BCksek-kazan%C3%A7-potansiyeline-sahip-oyunlar/5813598
https://uberant.com/article/2030815-pin-up-casino-trkiye-oyunlar-ve-elence-seenekleri/
https://niadd.com/article/1221426.html
https://flokii.com/blogs/view/186044
https://www.bondhuplus.com/read-blog/82138
Промокоды Vavada казино – это ваш путь к дополнительным бонусам. Активируйте Vavada казино промокоды и наслаждайтесь игрой с уникальными предложениями.
Здравствуйте!
Приобрести диплом университета.
Мы предлагаем купить диплом в высочайшем качестве, неотличимый от оригинального документа без участия специалистов высокой квалификации с дорогостоящим оборудованием.
Где купить диплом специалиста?
https://pedolog-pro.ru/forums/topic/%d0%ba%d1%83%d0%bf%d0%b8%d1%82%d1%8c-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc-c303p/
Успехов в учебе!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить аттестаты за 9, купить диплом в москве, купить диплом в чебоксарах, купить диплом в волгодонске, #купить диплом в новочебоксарске, а затем переключился на дипломы вузов. Подробности здесь:
http://funemulator.free.fr/index.php?file=Members&op=detail&autor=ewaqug
http://pokupay-24.ru/blog/bitye-pikseli-na-televizore-chto-eto-i-kakoe-dopustimoe-kolichestvo/
http://belobog1.freehostia.com/phpBB2/profile.php?mode=viewprofile&u=176826
https://revistamodamoldes.com.br/como-fazer-vies-com-o-proprio-tecido-da-roupa/#comment-15242
http://ziraffik.ru/product/platie-dp-a0550b/
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Удачи!
аттестат школьный купить ast-diplom.com .
Привет, друзья!
Приобрести документ университета можно у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации.
Мы предлагаем максимально быстро приобрести диплом, который выполнен на оригинальном бланке и заверен печатями, штампами, подписями официальных лиц. Документ способен пройти лубую проверку, даже при помощи специфических приборов.
http://fregat64.ru/index.php?name=account&op=info&uname=axibinu
http://globalimport.spb.ru/forum/thread1079.html#1099
https://overfun.ru/index.php?/topic/184-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-o132r/
http://www.dxzw.com/member/index.php?uid=ogabudul
http://region-standart.ru/guestbook/?1718885266
Воспользуйтесь промокодами Drip казино для получения уникальных бонусов. Эти промокоды помогут вам наслаждаться игрой с дополнительными преимуществами.
купить диплом дополнительном образовании ast-diplomy.com .
Hello everyone. Could you please recommend me some good
Peptide Therapy Clinic in Davenport?
купить технологический диплом ast-diplom.com .
эскорт москва – эскорт услуги, vip эскорт москва
Pin up sv
Placera ditt spel hos pinup online – mest prestigeious bookmaker
Pin up sv
купить диплом фармацевта в нижнем тагиле ast-diplomy.com .
Pin up Us
Place your bet at pinup online – most elite bookmaker
Pin up Us
We’ve all made email marketing mistakes: You click send on an email and suddenly your stomach drops. You’ve made a mistake and there’s nothing you can do about it The Evolution of Chassis Design: Enhancing Performance and Efficiency
Pinup ar
Place your bet at pin up now – very elite bookmaker
Pinup
Привет!
Где приобрести диплом специалиста?
Заказать документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Гарантируем, что при проверке документов работодателем, каких-либо подозрений не возникнет.
http://lenmontov.blogspot.com/2015/03/blog-post_16.html
Успехов в учебе!
In a world where communication is key, having a reliable phone number is essential for both personal and business interactions. However, not everyone needs a permanent number, especially when privacy, convenience, and flexibility are at stake https://press.farm/virtual-phone-numbers-in-turkey-for-business/
http://nedvizhimostrussa.ru/
Здравствуйте!
Купить диплом ВУЗа.
Мы предлагаем приобрести диплом в отличном качестве, неотличимый от оригинала без участия специалистов высокой квалификации с дорогостоящим оборудованием.
Где приобрести диплом по нужной специальности?
http://karasteamfulldmroleplay.getbb.ru/ucp.php?mode=login&sid=3355d20245a2c42567eedd92923b72d2
Успехов в учебе!
Really no matter if someone doesn’t understand after that its up to other people that they
will help, so here it takes place.
my web-site :: precio
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в хабаровске, купить диплом в чите, купить диплом в прокопьевске, купить диплом эколога, купить диплом в волгограде, постепенно вникая в суть дела нашел отличный материал здесь http://x70795vj.beget.tech/2024/05/14/kupit-diplom-legkiy-put-k-uspeshnoy-karere.html и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Хорошей учебы!
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Aseta panoksesi pinup nyt – useim eliitin vedonvalittaja
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Ресторан бистро Ижевск bistroyar.ru
Приглашаем Вас в данное bistroyar.ru бистро, где можно не только быстро и вкусно перекусить, а также провести семейное мероприятие, сделать заказ с доставкой, усладиться домашней кухней и порадовать себя десертом.
Кафе «ЯР» находится по адресу г. Ижевск, ул. Максима Горького, д. 163. Режим работы с 10:00 до 20:00 каждый день. Приходите к нам или делайте заказ с доставкой и наслаждайтесь блюдами нашей кухни в привычной для себя обстановке.
По запросу доставка еды меню вы на верном пути. Здесь можно мгновенно заказать еду на дом. Заходите в меню на онлайн ресурсе bistroyar.ru и отправляйте нужные блюда в корзину. Далее выбирайте способ доставки или самовывоз, что более удобно для Вас. Если Вы желаете получить дома заказ, то обязательно указывайте верный адрес и мобильный телефон.
Если Вы искали фабрика итальянское бистро сейчас, то мы Вам обязательно поможем. Наш девиз – «хорошо, как дома», ведь мы приготавливаем еду с любовью, что многие гости оценили. По всем вопросам звоните по контактному телефону +7(3412)223-230 или оформляйте заявку на сайте. Обязательно попробуйте наши десерты и горячее, скорее всего, вкуснее было только у мамы дома.
Каталог вакансий — ваш путь к успешной карьере! <a href=https://framesearch.store/Изучите актуальные предложения от лучших работодателей, отсортируйте их по интересующим вас критериям (зарплата, график работы, требования к кандидатам) и свяжитесь с компаниями напрямую для уточнения деталей.
доставка курьером Мы уверены, что в нашем каталоге вы обязательно найдёте подходящую вакансию, которая позволит вам реализовать свой потенциал и достичь успеха в карьере.
Здравствуйте!
Мы готовы предложить дипломы любых профессий по приятным тарифам. Цена зависит от выбранной специальности, года получения и университета.
Где заказать диплом по необходимой специальности?
Приобрести диплом любого университета
https://landik-diploms-srednee.ru/kupit-attestat-za-11-klass
Успешной учебы!
As with sales, you can commence functioning in the true estate brokerage field
with just a high school diploma or GED.
my web-site :: Part time jobs women
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по выгодным тарифам.
Мы готовы предложить документы ВУЗов, которые находятся в любом регионе РФ. Вы имеете возможность купить диплом за любой год, включая документы старого образца. Дипломы и аттестаты выпускаются на бумаге самого высшего качества. Это дает возможности делать государственные дипломы, которые невозможно отличить от оригиналов. Они будут заверены всеми требуемыми печатями и штампами.
Даем гарантию, что в случае проверки документа работодателем, каких-либо подозрений не появится.
Где заказать диплом специалиста?
good-serial.ru/2024/05/kupit-diplom-byistro-i-legalno/
[…] business, catering to lovers all around the globe. Whether you’re a seasoned bettor togcentre.Com or a curious newcomer, there’s one thing universally thrilling about betting on sports […]
Здравствуйте!
Хочу рассказать о своем опыте по заказу аттестата пту, думал это не реально и стал искать информацию в сети, про купить диплом в ноябрьске, купить диплом в азове, купить диплом в ревде, купить диплом в ейске, купить диплом в майкопе, постепенно вникая в суть дела нашел отличный материал здесь http://www.mamalipetsk.ru/index.php?name=forums&op=showtopic&id=25514 и был очень доволен!
Теперь у меня есть диплом столяра о среднем специальном образовании, и я обеспечен на всю жизнь)
Удачи!
Paypal transfers Prepaid cards
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $ 500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
Shops cards – markets darknet Buy paypal acc
Привет, друзья!
Где купить диплом специалиста?
Заказать диплом ВУЗа.
http://funnywipes.maxbb.ru/viewtopic.php?f=3&t=598&sid=d0175597014ed696949f93dcb8301cf4
Удачи!
Привет!
Где купить диплом специалиста?
Купить документ университета можно в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы получите необходимый диплом по любым специальностям, включая документы образца СССР. Даем 100% гарантию, что в случае проверки документа работодателями, никаких подозрений не возникнет.
https://cifra-dom.ru/blog/rekvizity/
Удачи!
[u][b] Привет, друзья![/b][/u]
Где заказать диплом по актуальной специальности?
[b]Приобрести документ[/b] о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, включая документы образца СССР. Даем гарантию, что при проверке документа работодателем, каких-либо подозрений не появится.
http://www.saluttunisia.com/jomsocial/groups/viewbulletin/143-za-skolko-mozhno-zakazat-diplom-vuza-sejchas.html?groupid=101
[b]Хорошей учебы![/b]
Зайдите на сайт Научно-технического центра «Триада» https://triadacompany.ru/ который помогает тысячам предприятий обеспечивать промышленную и экологическую безопасность по всей России! Лучшие кадры, инновационный подход, опыт с 1991 года. Промышленная и экологическая безопасность, экспертиза, проектирование, консалтинг. Подробнее на сайте.
https://rik-estate.ru/
Hello,
What an good article!
May I scrape this and share this with my website subscribers?
My group is about Korean 야튜브
If your interested, feel free to come to my blog and
check it out.
Thanks and Keep up the good work!
Добрый день!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
Мы готовы предложить документы техникумов, которые расположены в любом регионе Российской Федерации. Можно приобрести диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Документы будут заверены необходимыми печатями и подписями.
Даем гарантию, что при проверке документа работодателями, каких-либо подозрений не появится.
Где приобрести диплом специалиста?
womka.6bb.ru/viewtopic.php?id=1138#p2499
Привет, друзья!
Где заказать диплом специалиста?
Заказать диплом о высшем образовании.
https://nedvigimost.bbok.ru/viewtopic.php?id=26650#p45740
Успехов в учебе!
Построить дом из кирпича – строительство кирпичных домов казань, дом под ключ казань
Здравствуйте!
Где заказать диплом специалиста?
Приобрести диплом ВУЗа.
http://kingcityrp.moibb.ru/posting.php?mode=post&f=34
Успехов в учебе!
his explanation coinmarketcap
Your Domain Name trader joe
In a world where communication is key, having a reliable phone number is essential for both personal and business interactions. However, not everyone needs a permanent number, especially when privacy, convenience, and flexibility are at stake [url=https://publicistpaper.com/seamless-connectivity-in-the-digital-era-navigating-the-world-of-virtual-phone-services/]https://publicistpaper.com/seamless-connectivity-in-the-digital-era-navigating-the-world-of-virtual-phone-services/[/url]
Привет!
Где заказать диплом специалиста?
Заказать документ ВУЗа можно у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любой специальности, включая документы образца СССР. Даем гарантию, что в случае проверки документов работодателями, подозрений не появится.
http://volteis.com/fr/canal-volteis/actualites/131-nouveau-distributeur-pour-la-guadeloupe-st-barth-et-st-martin
Успешной учебы!
Привет!
Где купить диплом специалиста?
Наша компания предлагает выгодно и быстро купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ пройдет лубую проверку, даже с использованием специально предназначенного оборудования. Достигайте цели быстро с нашей компанией.
Купить диплом ВУЗа.
https://phileo.me/blogs/185406/%D0%9B%D0%B5%D0%B3%D0%BA%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-Russian-Diplom
https://pamplusmus.com/blogs/46/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://noirconnection.com//read-blog/1410
https://victorians123.com/blogs/212/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
http://wiki.starfederation.ru/index.php?title=%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC_%D0%B2_%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5_%D0%BF%D0%BE_%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D0%BE%D0%B9_%D1%81%D1%82%D0%BE%D0%B8%D0%BC%D0%BE%D1%81%D1%82%D0%B8
linux vps web hosting – windows based vps hosting, managed vps hosting
https://redstoneestate.ru/
https://nsdentalsolution.com
https://med-blesk.ru
На сайте https://kinogo-fil.net/ вам предлагается смотреть интересные фильмы и сериалы бесплатно и без каких-либо ограничений. Здесь собрано множество подборок фильмов и категорий жанров, мультсериалов и мультфильмов. Вы сможете найти фильм для любых целей. Структура сайта позволит вам в несколько кликов начать смотреть ваш любимый сериал или же фильм. Наш сервис даст возможность вам подписаться на конкретный сериал, каждый раз, когда будет выходить новая серия, вы сразу же об этом узнаете! Приятного вам просмотра!
como usar bonus de casino 1win http://www.1win.tr-kazakhstan.kz реферальная ссылка 1win http://1win.tr-kazakhstan.kz/
her comment is here 1 win indir
Привет!
Мы предлагаем дипломы любой профессии по доступным ценам. Стоимость может зависеть от той или иной специальности, года выпуска и ВУЗа.
Где заказать диплом по нужной специальности?
Заказать диплом ВУЗа
https://landik-diploms-srednee.ru/kupit-diplom-kandidata-nauk
Удачи!
Привет!
Где купить диплом по необходимой специальности?
Мы готовы предложить документы ВУЗов, расположенных в любом регионе Российской Федерации. Документы заверяются необходимыми печатями и штампами.
Приобрести диплом ВУЗа:
https://sports-pharmacology54210.bloggactif.com/28174497/???????-??????-???????
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом фельдшера, купить диплом колледжа, купить диплом с занесением в реестр, купить диплом мастера маникюра и педикюра, купить диплом в томске, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://houseinform.ru/forum/poluchenie_diplomov_vuzov_rossii
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успехов в учебе!
Привет, друзья!
Где приобрести диплом специалиста?
Заказать документ о получении высшего образования вы имеете возможность в нашей компании. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ.
Мы предлагаем выгодно заказать диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ пройдет лубую проверку, даже при использовании профессионального оборудования. Достигайте свои цели быстро и просто с нашей компанией.
http://skvortsy.listbb.ru/viewtopic.php?f=31&t=1462
http://bohhchaos.listbb.ru/viewtopic.php?f=9&t=7573
http://mosfo.getbb.ru/viewtopic.php?f=12&t=252
http://ochag.flybb.ru/topic164.html
http://baxoday.maxbb.ru/topic368.html
new lenox movie theatre popular movie 2022movie where toys come to life and fightstranger things season 3 creaturesbig u movies
Glory Casino
Привет!
Где купить диплом по актуальной специальности?
Купить документ о получении высшего образования можно у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов России.
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Стоимость может зависеть от выбранной специальности, года получения и университета. Стараемся поддерживать для заказчиков адекватную политику тарифов.
https://ok-vmeste.ru/toget/1459-zhelaete-zakazat-podlinnyi-diplom.html
Успехов в учебе!
Привет, друзья!
Заказать диплом о высшем образовании.
Наша компания предлагает приобрести диплом в высоком качестве, который не отличить от оригинала без использования дорогостоящего оборудования и квалифицированного специалиста.
Где купить диплом специалиста?
http://mangorpp.getbb.ru/ucp.php?mode=login&sid=7100c5e975a101fc4cb8fe99172ba330
Хорошей учебы!
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом штукатура, купить диплом в новочеркасске, купить диплом в сочи, купить диплом нового образца, купить диплом в георгиевске, затем наткнулся на http://kukly.ru/forum1/profile.php?action=show&member=79038, где все мои учебные вопросы были решены!
Успехов в учебе!
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по невысоким тарифам. Стоимость зависит от выбранной специальности, года выпуска и образовательного учреждения.
Где заказать диплом специалиста?
Купить диплом о высшем образовании
https://arusak-diploms-srednee.ru/kupit-diplom-v-rostove-na-donu
Успешной учебы!
a knockout post pin up casino
1win скачать мобильный телефон https://www.1win.tr-kazakhstan.kz 1win из какой страны 1win.tr-kazakhstan.kz
1win лидерборд https://www.1win.tr-kazakhstan.kz 1win впн http://www.1win.tr-kazakhstan.kz
https://romashkaclinic.ru
узнать больше снюс
https://psy-medcentr.ru
Привет!
Где приобрести диплом по нужной специальности?
Мы предлагаем выгодно купить диплом, который выполняется на оригинальной бумаге и заверен печатями, штампами, подписями официальных лиц. Наш диплом пройдет лубую проверку, даже при помощи специфических приборов. Решите свои задачи быстро с нашими дипломами.
Заказать диплом любого университета.
https://mimedia.in/read-blog/50841
https://www.forumblogger.my.id/blogs/1929/%D0%9F%D0%BE%D0%B4%D1%80%D0%BE%D0%B1%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://socialhustle.co.uk/read-blog/2356
https://edusocial.online/blogs/126/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-Russian-Diplom
https://www.4yo.us/blogs/141387/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
wow raid services
Привет, друзья!
Где заказать диплом по актуальной специальности?
Мы можем предложить документы институтов, которые расположены в любом регионе России. Вы можете купить диплом от любого ВУЗа, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, которые невозможно отличить от оригинала. Документы заверяются необходимыми печатями и штампами.
Мы изготавливаем дипломы любых профессий по доступным тарифам.
https://ast-diplomy24.ru/kupit-diplom-o-srednem-obrazovanii
Рады помочь!
Здравствуйте!
Приобрести диплом ВУЗа.
Наша компания предлагает купить диплом отличного качества, который невозможно отличить от оригинала без участия специалиста высокой квалификации со сложным оборудованием.
Где приобрести диплом по необходимой специальности?
http://domovou.3nx.ru/login.php?redirect=posting.php&mode=newtopic&f=23
Успешной учебы!
Привет, друзья!
Где купить диплом специалиста?
Приобрести документ о получении высшего образования вы сможете в нашей компании в столице. Мы оказываем услуги по производству и продаже документов об окончании любых университетов Российской Федерации.
Мы изготавливаем дипломы любых профессий по приятным тарифам. Стоимость будет зависеть от выбранной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для покупателей адекватную политику тарифов.
https://goebecom.jofo.me/2265942.html
Успешной учебы!
виза д в испанию https://vnzh24.ru/
Чтобы осуществить ижвижн приходите к нам. Мы находимся по адресу г. Ижевск, ул. Ленина, д. 101. График работы с пн по пт с 9:00 до 16:00, после 16:00 можно прийти, заранее записавшись или по выходным.
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в артеме, купить диплом в ревде, купить диплом в химках, купить дипломы о высшем образовании цена, купить диплом в шахтах, потом про дипломы вузов, подробнее здесь http://igorodstore.ru/product/3435/
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успехов в учебе!
саксенда купить +в нижнем новгороде – трулисити 1.5 мг +в москве, оземпик препарат +для похудения инструкция
Привет, друзья!
Где приобрести диплом по нужной специальности?
Мы можем предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Они заверяются необходимыми печатями и штампами.
Купить диплом любого университета:
http://student-news.ru/kupit-diplom-v-moskve-3
Добрый день!
Где купить диплом специалиста?
Наша компания предлагает быстро и выгодно приобрести диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями официальных лиц. Наш диплом способен пройти любые проверки, даже с применением специфических приборов. Достигайте цели быстро с нашей компанией.
Купить диплом любого университета.
https://shaunbook.mn.co/posts/61838375
https://wiki.diamondrp.ru/index.php?title=%D0%92%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D1%8B%D0%B5_%D1%86%D0%B5%D0%BD%D1%8B_%D0%B8_%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5_%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE_-_%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B9_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD!
https://ayema.ng/blogs/33240/%D0%94%D0%B5%D1%82%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://www.djcuna.social/blogs/226/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://www.privsocial.com/read-blog/297
Приветствуем вас на канале проекта casino VAVADA! Здесь вы найдете исключительно свежую информацию. Забудьте о повседневных заботах и проведите время за увлекательными слотами в высококачественном онлайн-казино Вавада! Вас ждет особая атмосфера и отличная графика. Ищете vavada фриспины? t.me/mvavada – здесь мы делимся с вами своими знаниями и секретами успеха. Казино VAVADA подходит всем без исключения. Вы оцените скорость выводов и бонусы. Саппорт старается любые вопросы решать довольно быстро. Начните игру уже сегодня. Удачи вам и победы!
Привет, друзья!
Где заказать диплом специалиста?
Готовый диплом с приложением отвечает запросам и стандартам Министерства образования и науки России, неотличим от оригинала – даже со специально предназначенным оборудованием.
Купить диплом ВУЗа.
http://forum.safe-animals.ru/index.php?showtopic=29051
https://hvacprotalk.com/read-blog/217
https://sonnick84.blog2learn.com/76389039/%D0%93%D1%80%D0%B0%D0%BC%D0%BE%D1%82%D0%BD%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%B0%D0%B2%D1%82%D0%BE%D1%80%D1%81%D0%BA%D0%B8%D0%B9-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
https://app.site123.com/manager/wizard.php?wu=65b7bc9283766-65b7bc9283768-65b7bc9283769
http://roving.club/read-blog/1002
Привет!
Для многих людей, приобрести диплом ВУЗа – это необходимость, шанс получить достойную работу. Но для кого-то – это желание не терять время на учебу в ВУЗе. С какой бы целью вам это не понадобилось, мы готовы помочь вам. Оперативно, профессионально и выгодно сделаем диплом любого года выпуска на государственных бланках с реальными подписями и печатями.
Наша компания предлагает быстро и выгодно заказать диплом, который выполнен на оригинальном бланке и заверен печатями, штампами, подписями должностных лиц. Наш диплом пройдет любые проверки, даже при использовании профессионального оборудования. Решите свои задачи быстро и просто с нашей компанией.
Где заказать диплом специалиста?
https://twikkers.nl/blogs/137620/????????????????-???????????-???-??????-?????????-?????????-?????????-????????-??-?????
Удачи!
Здравствуйте!
Заказать документ ВУЗа можно в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любой специальности, любого года выпуска, в том числе документы старого образца. Даем 100% гарантию, что при проверке документа работодателем, каких-либо подозрений не появится.
Наша компания предлагает выгодно приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, штампами, подписями должностных лиц. Диплом пройдет лубую проверку, даже с применением специальных приборов. Решите свои задачи быстро и просто с нашими дипломами.
Где приобрести диплом по нужной специальности?
https://sovetushka.forum2x2.ru/t28783-topic#63567
Хорошей учебы!
Привет, друзья!
Где купить диплом по нужной специальности?
Купить документ института можно в нашей компании. Мы предлагаем документы об окончании любых университетов Российской Федерации.
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Наш документ пройдет любые проверки, даже при использовании профессионального оборудования. Достигайте своих целей быстро с нашим сервисом.
http://mosday.getbb.ru/viewtopic.php?f=12&t=899
http://itisenglish.maxbb.ru/topic262.html
http://www.vocal.com.ua/node/61833
http://autoprajs.ru/14765.html
http://www.ecoheal.ru/index.php/jomsocial/groups/viewbulletin/210-kak-priobresti-diplom-otlichnogo-kachestva-v-seti-internet-sejchas?groupid=1
Привет, друзья!
Где заказать диплом специалиста?
Приобрести документ о получении высшего образования вы можете в нашей компании. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы старого образца. Гарантируем, что при проверке документов работодателем, подозрений не появится.
http://rech-kruiz.ru/
Успехов в учебе!
Привет, друзья!
Мы предлагаем документы ВУЗов, расположенных на территории всей РФ. Можно приобрести качественный диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые не отличить от оригинала. Документы заверяются всеми обязательными печатями и штампами.
Приобрести диплом о высшем образовании.
https://lucylink.com/read-blog/56
https://1dvkbystr.slypage.com/28765769/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://cittaviva.net/read-blog/59
https://derivsocial.org/read-blog/2556
https://www.yur-dom.ru/communication/forum/messages/forum3/message254/297-nizkie-tseny-i-vysokoe-kachestvo-_-priobretay-diplomy-onlayn?result=new
Хорошей учебы!
На сайте http://kak-vernut-dengi.ru/ представлена интересная, исчерпывающая информация о том, как получится вернуть средства у брокера, если он получил их незаконным либо нечестным путем, но при этом обещал высокую доходность. Специалист в своих статьях как раз рассказывает о том, как вернуть средства законным путем у таких лжеброкеров. Здесь находятся и любопытные видеоматериалы, которые понравятся тем, что они содержательные и информативные. В них детально показывается то, как это правильно сделать, чтобы не ошибиться.
Добрый день!
Где купить диплом специалиста?
Заказать диплом университета.
http://ozmt.getbb.ru/ucp.php?mode=login&sid=935aa9641c9a96bc0c3958bef0747be8
Удачи!
Добро пожаловать на наш сайт – ваше решение для всех финансовых потребностей!
Наши предложения
Мы предлагаем различные финансовые продукты: кредиты, банковские карты и займы, чтобы помочь вам достигнуть ваших целей и осуществить мечты.
кредитные карты
Идеальные кредиты для ваших нужд
Нуждаетесь в финансировании на покупку жилья, автомобиля или образование? Наши кредитные программы разработаны с учетом ваших потребностей. Оформите кредит на нашем сайте, выбрав подходящие условия и сроки погашения.
Преимущества наших банковских карт
Наши банковские карты предоставляют:
Удобство безналичных платежей
Бонусы и привилегии
Оформите карту на нашем сайте и получайте кэшбэк, скидки у партнеров и участие в программе лояльности. Выберите карту с оптимальными лимитами и условиями обслуживания для себя.
Быстрые и удобные займы
Нужны деньги до зарплаты или на непредвиденные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок, чтобы вы могли решать финансовые вопросы без задержек.
Наши преимущества:
Простота и Удобство: Оформите заявку онлайн за несколько минут.
Надежность и Прозрачность: Мы гарантируем честные условия и отсутствие скрытых комиссий.
Индивидуальный Подход: Мы учитываем ваши личные обстоятельства и предлагаем оптимальные условия.
Не упустите возможность улучшить свою финансовую ситуацию!
займы Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
С нами ваши мечты станут реальностью!
1win sign up http://1win.tr-kazakhstan.kz/ отзывы 1win invest https://www.1win.tr-kazakhstan.kz
Специализация компании ООО «АвтоПрайм» предоставляет в аренду автовышки и другую спецтехнику для проведения самых различных высотных работ — прокладки линий электропередач, клининга, отделки фасадов, монтажа конструкций и многих других. Мы предлагаем в аренду на выгодных условиях спецтехника аренда
https://novomed-cardio.ru
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом бурильщика, купить диплом в канске, купить диплом в симферополе, купить диплом медсестры, #купить диплом в артеме, а затем переключился на дипломы вузов. Подробности здесь: http://38.104.231.181/doku.php?id=landsdiploms
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Удачи!
Привет!
Заказать диплом о высшем образовании
Мы предлагаем выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ способен пройти любые проверки, даже с использованием специфических приборов. Решайте свои задачи максимально быстро с нашим сервисом.
Где заказать диплом специалиста?
http://niceroleplay.getbb.ru/viewtopic.php?f=1&t=1221
Окажем помощь!.
[u][b] Здравствуйте![/b][/u]
Где заказать диплом по необходимой специальности?
Купить документ университета можно у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любым специальностям, включая документы Советского Союза.
[b]Где заказать диплом специалиста?[/b]
http://raceburo.ru/vash-diplom-bez-truda-i-usiliy
https://israelafrica.mn.co/posts/62051313
http://newsato.ru/ofitsialnyiy-diplom-bez-lishnih-hlopot
http://c90226sl.beget.tech/2024/07/11/kupite-diplom-i-uluchshite-svoe-budushhee/
http://kvitka.ukrbb.net/viewtopic.php?f=58&t=23466
[b]Хорошей учебы![/b]
Добрый день!
Где заказать диплом по нужной специальности?
Мы предлагаем документы техникумов, которые расположены в любом регионе РФ. Они будут заверены всеми необходимыми печатями и штампами.
Приобрести диплом университета:
https://raimane.com/2024/06/08/Лучшие-сайты-для-покупки-диплома-о-среднем-образовании
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом железнодорожника, купить диплом вуза, купить диплом охранника, купить диплом в орске , купить диплом нового образца и получил базовые знания. В итоге остановился на материале:
https://forumjizni.ru/member.php?u=120208
http://old.trudcher.ru/users.php?m=details&id=16055
https://clicky.buzz/index.php?do=/public/blog/view/id_119666/title_/
https://christinamogitich.ru/blog/erke-esmahan—ajda-na-russkom-kaver/#comment_74238
http://schoolchild-notes.blogspot.com/2014/03/blog-post_1.html
Успешной учебы!
Добрый день!
Где заказать диплом по нужной специальности?
Заказать диплом о высшем образовании.
http://moscowurban.getbb.ru/posting.php?mode=post&f=12
Удачи!
Привет!
Заказать диплом ВУЗа
Наши специалисты предлагают выгодно и быстро заказать диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями. Данный диплом пройдет любые проверки, даже при использовании специальных приборов. Достигайте свои цели быстро и просто с нашей компанией.
Где заказать диплом специалиста?
https://www.import-moto.com/users/88
Поможем вам всегда!.
В сфере азартных игр в интернете особенно важны аспекты защиты данных и обеспечения надежности операций. Это ключевые аспекты, на которых строятся доверие игроков и успешная работа платформ https://visualchemy.gallery/forum/viewtopic.php?pid=3393124#p3393124
Здравствуйте!
Купить документ института вы сможете в нашей компании в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов России. Вы получите диплом по любым специальностям, включая документы старого образца. Гарантируем, что при проверке документов работодателями, каких-либо подозрений не появится.
Мы предлагаем выгодно приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, штампами, подписями официальных лиц. Диплом пройдет лубую проверку, даже при помощи профессионального оборудования. Решайте свои задачи быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
https://lider-school174.com/forum/user/2588/
Успехов в учебе!
Здравствуйте!
Где приобрести диплом специалиста?
Купить диплом о высшем образовании.
http://ya.10bb.ru/viewtopic.php?id=3615#p6544
Успехов в учебе!
Привет, друзья!
Где купить диплом специалиста?
Заказать документ о получении высшего образования вы имеете возможность в нашей компании. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза. Гарантируем, что в случае проверки документов работодателем, никаких подозрений не возникнет.
http://triumph-flowers.ru/bukety-nevesty/yarkij-buket-nevesty/
Успешной учебы!
Привет!
Где заказать диплом специалиста?
Купить документ о получении высшего образования вы можете в нашей компании. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любой специальности, включая документы Советского Союза.
Где приобрести диплом специалиста?
http://collieforum.ru/posting.php?mode=post&f=17
https://friends.win/read-blog/3720
https://www.yur-dom.ru/communication/forum/messages/forum3/message265/307-poluchite-diplom-bez-lishnikh-zabot-i-usiliy?result=new#message265
https://100foto.com/forum/user/1574/
http://terorizam.listbb.ru/viewtopic.php?f=3&t=374
Удачи!
Привет!
Где заказать диплом специалиста?
Мы можем предложить документы институтов, которые расположены в любом регионе Российской Федерации. Можно приобрести диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы делаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются необходимыми печатями и подписями.
Мы изготавливаем дипломы любых профессий по приятным ценам.
https://ast-diplomy.com/kupit-diplom-bakalavra-ili-specialista
Рады помочь!
Привет, друзья!
Заказать диплом любого ВУЗа
Наши специалисты предлагают выгодно и быстро купить диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Диплом пройдет лубую проверку, даже с использованием специфических приборов. Достигайте цели быстро с нашим сервисом.
Где приобрести диплом специалиста?
http://munchkin.flybb.ru/viewtopic.php?f=7&t=4179
Всегда вам поможем!.
pin up no
Plasser innsatsen din hos pinup now – autentisk prestisjefylt bookmaker
pinup casino
Pin up
Placera ditt spel hos pinup nu – mycket elite bookmaker
Pinup
Здравствуйте!
Где приобрести диплом специалиста?
Заказать документ о получении высшего образования можно у нас в столице. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любым специальностям, включая документы СССР.
Где приобрести диплом специалиста?
https://amengram.com/blogs/370/Ваш-диплом-без-лишних-забот-быстро-и-безопасно
http://webnewsrealty.ru/kupite-diplom-i-zabudte-o-studencheskih-dolgih-nochah
https://nsibirsk.ru/forum/obyavleniya/newtopic/#google_vignette
http://besconeshnocte.flybb.ru/viewtopic.php?f=2&t=943
http://forummsk.getbb.ru/viewtopic.php?f=12&t=2636
Успехов в учебе!
Pinup ar
Place your bet at pinup online – authentic prestigious bookmaker
Pinup
Pinup Us
Place your bet at pinup online – most reliable bookmaker
Pinup casino
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом о среднем специальном, купить диплом швеи, купить диплом в вольске, купить диплом в октябрьском, купить диплом в артеме, а потом наткнулся на
http://38.104.231.181/doku.php?id=gosznacdiplom
http://nautitopo.blogspot.com/2017/05/01.html
http://msflow.ru/products/pionovidnye-rozy-v-korobke/#comment_60753/
http://stoliistulya.ru/products/stol-serii-sptm-1207-1208/
http://food-ua.com/wr_board/tools.php?event=profile&pname=orygybip
, где все мои учебные проблемы были решены!
Успешной учебы!
She famously promised the media she woould “spend, spend, spend” following the
windfall — and she kept her word.
My web page :: Florida powerball
pinup casino
Plasser innsatsen din hos pin up online – autentisk prestisjefylt bookmaker
pinup casino
стоит ли покупать диплом о высшем образовании ast-diplomas.com .
Pinup sv
Placera ditt spel hos pin up nu – direkt reliable bookmaker
Pin up
купить диплом средняя окончание diploms-x.com .
1Win APK download http://www.1win.tr-kazakhstan.kz **1Win** – международная букмекерская контора, присутствующая на всех континентах благодаря локальным платежным системам и адаптированному интерфейсу. http://1win.tr-kazakhstan.kz/
Добрый день!
Где заказать диплом по нужной специальности?
Готовый диплом с приложением 100% отвечает стандартам, никто не отличит его от оригинала.
Купить диплом любого университета.
https://ourownnetwork.mn.co/posts/61724527
https://socialnetwork.cloudyzx.com/read-blog/10539
http://158.160.31.233/blogs/1/4e-klyuchevykh-gruppy-onlayn-magazinov-kotorye-realizuyut-dokumenty.php
https://crowd-out.social/read-blog/139
https://www.leenkup.com/read-blog/16570
Pinup ar
Place your bet at pinup online – very prestigious bookmaker
Pin up
Добрый день!
Купить диплом о высшем образовании.
Наш сервис предлагает купить диплом в высочайшем качестве, неотличимый от оригинального документа без участия специалистов высокой квалификации со специальным оборудованием.
Где купить диплом специалиста?
http://classicalmusicmp3freedownload.com/ja/index.php?title=premiummdiplomms
Хорошей учебы!
online casino
Place your bet at pinup online – most reliable bookmaker
Pin up Us
Добрый день!
Где купить диплом специалиста?
Мы предлагаем документы институтов, которые расположены на территории всей РФ. Вы можете заказать качественно сделанный диплом от любого заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы делаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они будут заверены всеми необходимыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по доступным тарифам.
https://diploms-x24.ru/kupit-diplom-krasnodar
Окажем помощь!
Добрый день!
Заказать документ о получении высшего образования вы можете у нас в столице. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации.
Наши специалисты предлагают выгодно и быстро заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями официальных лиц. Данный диплом пройдет лубую проверку, даже при использовании специально предназначенного оборудования.
http://istinastroitelstva.xyz/index.php?subaction=userinfo&user=eziwolo
http://profelectro.by/index.php?subaction=userinfo&user=eweroxa
http://eicg.kz/index.php?subaction=userinfo&user=upoxehejy
“http://www.fsh.mi.th/newswb3/index.php?action=profile;u=67657”
http://www.pax.nichost.ru/forum/view_profile.php?UID=133853
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в новоуральске, купить диплом в вольске, купить диплом в элисте, купить диплом о среднем специальном, купить диплом маркетолога, потом попал на https://tambonyo.go.th/forum/suggestion-box/1019732-dipl
http://grupogoya.es/inicio/goya-campos-consultoria-laboral/#comment-234688
https://www.primary-bookmarks.win/unlocking-potential-the-power-of-a-diploma
https://synapse.koreamed.org/advanced/index.php
https://www.becco.com.au/home-reduced-menu/becco_logo_small-2/#comment-113215
и там решили все мои учебные заботы!
Хорошей учебы!
По поводу коррекция lasik мы Вам можем помочь. У нас широкий выбор услуг: метод коррекции зрения ласик, лазерная коагуляция сетчатки, оперативное лечение катаракты, лазерная дисцизия задней капсулы хрусталика, блефаропластика, безоперационная блефаропластика аппаратом JETT PLASMA LIFT и многие другие. Обратитесь за профессиональной помощью к нашим врачам.
https://www.wildberries.ru/catalog/217171028/detail.aspx
купить диплом в сургуте ast-diplomas.com .
Привет!
Где заказать диплом по нужной специальности?
Полученный диплом с приложением отвечает стандартам Министерства образования и науки РФ, неотличим от оригинала.
Купить диплом о высшем образовании.
http://автомедведь.рф/club/log/?SECTION_CODE=log
http://pika.listbb.ru/posting.php?mode=post&f=9
https://vip.forums.party/viewtopic.php?id=3420#p71005
http://www.cslregister.com/forum/member.php?u=6225
https://forum.xpixel.ru/gallery/image/91-%D0%BA%D0%B0%D0%BA%D0%B8%D0%B5-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D1%8B-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8-%D1%81%D1%83%D1%89%D0%B5%D1%81%D1%82%D0%B2%D1%83%D1%8E%D1%82-%D0%BD%D0%B0-%D1%81%D0%B5%D0%B3%D0%BE%D0%B4%D0%BD%D1%8F%D1%88%D0%BD%D0%B8%D0%B9-%D0%B4%D0%B5%D0%BD%D1%8C/?context=new
Доставка вкусной еды на дом в Ижевске bistroyar.ru
Приглашаем Вас в наше bistroyar.ru бистро, где можно не только быстро и аппетитно покушать, а также провести семейное мероприятие, оформить заказ с доставкой, насладиться домашней кухней и побаловать себя вкусностями.
Бистро «ЯР» расположено по адресу г. Ижевск, ул. Максима Горького, д. 163. Время работы с 10:00 до 20:00 ежедневно. Приезжайте к нам или оформляйте заказ с доставкой и наслаждайтесь блюдами нашей кухни в привычной для себя среде.
По запросу доставка вкусной еды ижевск вы на правильном пути. Тут можно мгновенно заказать еду до Вашего адреса. Заходите в меню на онлайн ресурсе bistroyar.ru и отправляйте выбранные блюда в корзину. Далее выбирайте способ доставки или самовывоз, что более удобно для Вас. Если Вы желаете получить дома заказ, то непременно указывайте верный адрес и контактный телефон.
Если Вы хотели найти готовая еда с доставкой на дом прямо сейчас, то мы Вам готовы помочь. Наш лозунг – «хорошо, как дома», ведь мы приготавливаем еду от души, что многие гости подчеркнули. По всем вопросам звоните по контактному телефону +7(3412)223-230 или оформляйте заявку на сайте. Обязательно попробуйте наши салаты и супы, скорее всего, вкуснее было только у мамы на кухне.
купить диплом в ленинск-кузнецком diploms-x.com .
Привет!
Где заказать диплом по нужной специальности?
Заказать документ о получении высшего образования можно в нашем сервисе. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации.
Мы изготавливаем дипломы любых профессий по приятным ценам. Цена может зависеть от конкретной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику.
https://xn—-btbthcge4aikr4i.xn--p1ai/forum/user/30261/
Успехов в учебе!
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Aseta panoksesi pin up online – suorain arvostettu vedonvalittaja
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
christopher lloyd movies pixar films rankedchinese sci-fi moviesphoto finish moviethe temptations movie full cast
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в керчи, купить диплом в комсомольске-на-амуре, купить диплом о среднем специальном, купить диплом моториста, купить диплом в нижнекамске, потом про дипломы вузов, подробнее здесь https://sprayfoaminternational.com/smooth1-0/
https://dailygram.com/blog/1293289/купить-диплом-ваш-путь-к-успеху/
https://amster-brand.ru/blog/testovaya-zapis-dlya-novostej
https://student.alsafwa.edu.iq/blog/2019/03/14/53522/
http://nvkb.ru/forum/index.php/user/96573/
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Удачи!
review Torbrowser download
сюда https://battlepass.ru/
https://akkred-med.ru
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом фельдшера, купить диплом в нефтекамске, купить диплом в хасавюрте, купить диплом о высшем образовании, купить диплом в подольске и получил базовые знания. В итоге остановился на материале: http://postap.ru/forums/
Успешной учебы!
They are also typically responsible for other non-flight duties such as scheduling
flights, arranging for maintenance of the aircraft and loading luggage.
Also visit my blog … best Female jobs without a degree
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Aseta panoksesi pinup online – suorain arvostettu vedonvalittaja
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Здравствуйте!
Где приобрести диплом специалиста?
Приобрести диплом университета.
https://kellerscrossing.com/
Всегда вам поможем!
ссылка на сайт https://kp-inform.ru/catalog/prochee/4_port_fc_host_interface_card_no_sfps_ibm_00y2421
you could check here
mascarillas
семаглутид +в таблетках – препараты +для похудения самые эффективные купить, mounjaro отзывы
Привет, друзья!
Купить диплом о высшем образовании.
Наша компания предлагает заказать диплом в отличном качестве, неотличимый от оригинала без участия специалистов высокой квалификации со специальным оборудованием.
Где купить диплом специалиста?
http://www.fiat-club.ru/search.php?cx=partner-pub-2897956929599751:bz9j42-t4gv&cof=FORID:10&ie=UTF-8&q=&sa=Поиск&siteurl=forum.fiat-club.ru/blog_post.php?do=newblog&ref=forum.fiat-club.ru/login.php?do=login&ss=
Хорошей учебы!
http://www.kalyamalya.ru/modules/newbb_plus/viewtopic.php?topic_id=18418&post_id=95817&order=0&viewmode=flat&pid=0&forum=4#95817
YOURURL.com
artisan workshops
Строительство и ремонт с гарантией качества
Наша профессиональная строительная компания обеспечивает комплексные решения в области фундаментов и стен. Мы предоставляем использование качественных материалов, поэтапную оплату и прозрачность цен. Каждый проект осуществляется опытными специалистами с применением передовых технологий и обязательной гарантией.
Перечень наших услуг:
Фундамент “под ключ”: https://mosvip-stroy.ru
Фундаментная плита: https://mosvip-stroy.ru/fundamentnaya_plita
Шведская утепленная плита: https://mosvip-stroy.ru/ushp
Ленточный фундамент: https://mosvip-stroy.ru/lentochnyj_fundament
Свайные фундаменты: https://mosvip-stroy.ru/svajnyj_fundament
Кладка стен: https://mosvip-stroy.ru/vozvedenie-sten
Столбчатая основа: https://mosvip-stroy.ru/stolbchatyj_fundament
Блочный фундамент: https://mosvip-stroy.ru/blochnyj_fundament
Свайно-ростверковый фундамент: https://mosvip-stroy.ru/svajno-rostverkovyj_fundament
купить диплом о юридическом образовании ast-diplomas.com .
view publisher site Rufus download
Здравствуйте!
Заказать диплом о высшем образовании.
Наша компания предлагает купить диплом высокого качества, который невозможно отличить от оригинала без использования специального оборудования и опытного специалиста.
Где купить диплом специалиста?
http://rodina.listbb.ru/viewtopic.php?f=3&t=502
Успехов в учебе!
Привет!
Где приобрести диплом по актуальной специальности?
Купить документ о получении высшего образования вы сможете в нашей компании в столице. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов Российской Федерации.
Мы можем предложить дипломы любой профессии по невысоким ценам. Стоимость может зависеть от конкретной специальности, года получения и университета. Всегда стараемся поддерживать для клиентов адекватную ценовую политику.
http://www.bakinsky-dvorik.ru/communication/forum/user/183037/
Удачи!
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом психолога, купить свидетельство о браке, купить диплом в тамбове, купить диплом в новочеркасске, купить диплом во владивостоке, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://xn--sns-dk6nm87c.com/bbs/board.php?bo_table=free&wr_id=1165877
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Удачи!
Привет!
Приобрести диплом о высшем образовании.
Мы предлагаем заказать диплом в высоком качестве, неотличимый от оригинала без участия специалистов высокой квалификации со сложным оборудованием.
Где приобрести диплом по актуальной специальности?
http://www.atoe.co.kr/bbs/board.php?bo_table=free&wr_id=206021
Удачи!
Добрый день!
Где приобрести диплом специалиста?
Купить диплом о высшем образовании.
http://www.rgv.ru/phpbb/profile.php?mode=viewprofile&u=2745
Рады оказаться полезными!
Привет, друзья!
Мы изготавливаем дипломы любой профессии по доступным ценам.
Мы можем предложить документы ВУЗов, расположенных на территории всей РФ. Вы можете заказать качественно сделанный диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригинала. Они будут заверены всеми требуемыми печатями и подписями.
Даем гарантию, что в случае проверки документов работодателями, каких-либо подозрений не появится.
Где заказать диплом по нужной специальности?
e-maxx.ru/forum/profile.php?id=16976
заказать создание сайта москва
купить диплом мастера маникюра ast-diplomas.com .
https://vk.com/ccgaming52
платформа для поиска инвесторов для бизнеса
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: куплю диплом цена, купить диплом в альметьевске, купить диплом в кемерово, купить диплом в саратове, купить диплом в биробиджане, а потом наткнулся на
http://wp1065308.server-he.de/doku.php?id=rudiplomirovaniecom
http://xn—-otbbqececjg2be.xn--p1ai/2019/08/25/hello-world/?unapproved=391882&moderation-hash=907dc9a8252368dd7c13e1655c2f7e1c#comment-391882
https://sosna-dub32.ru/blog/vyraschivanie-maliny-v-otkrytom-grunte/#comment_164265/
http://protivstavok.blogspot.com/2017/09/2017.html
http://wwassociation.ru/user/10927
, где все мои учебные проблемы были решены!
Удачи!
понятная платформа для разумных инвестиций
таблетка для увеличения хешрейта – Raven кошелек скачать, Скачать Raven Core Wallet
Здравствуйте!
Для многих людей, купить диплом ВУЗа – это острая необходимость, уникальный шанс получить достойную работу. Но для кого-то – это желание не терять время на учебу в ВУЗе. Что бы ни толкнуло вас на такой шаг, наша фирма готова помочь вам. Быстро, профессионально и по разумной стоимости сделаем диплом нового или старого образца на настоящих бланках с реальными подписями и печатями.
Наши специалисты предлагают выгодно заказать диплом, который выполнен на оригинальном бланке и заверен печатями, штампами, подписями. Наш диплом пройдет любые проверки, даже с использованием специальных приборов. Решите свои задачи быстро с нашим сервисом.
Где приобрести диплом специалиста?
https://woman.0bb.ru/viewtopic.php?id=888#p2336
Успехов в учебе!
Привет!
Приобрести документ о получении высшего образования можно у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов России.
Наши специалисты предлагают быстро и выгодно купить диплом, который выполняется на оригинальной бумаге и заверен печатями, штампами, подписями официальных лиц. Диплом способен пройти любые проверки, даже при помощи профессиональных приборов.
http://andi67.bplaced.net/dokuwiki/doku.php?id=diploman
http://www.miranetwork.it/index.php?option=com_k2&view=itemlist&task=user&id=446373
http://mydnepr.pp.ua/forum/topic.php?forum=7&topic=936
http://shooting-russia.ru/forum/?PAGE_NAME=message&FID=5&TID=15045&TITLE_SEO=15045-premiummdiplomms&MID=15310&result=new#message15310
http://fire-team.ru/forum/showthread.php?p=35356#post35356
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, включая документы образца СССР. Даем 100% гарантию, что в случае проверки документа работодателем, подозрений не возникнет.
Наша компания предлагает выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Данный диплом способен пройти лубую проверку, даже при использовании профессионального оборудования. Достигайте свои цели быстро и просто с нашим сервисом.
Где приобрести диплом по нужной специальности?
http://www.support.ipron.com/communication/forum/index.php?PAGE_NAME=profile_view&UID=17558
Удачи!
https://aspectremont.com/
Здравствуйте!
Купить диплом о высшем образовании.
Наш сервис предлагает заказать диплом в высочайшем качестве, который не отличить от оригинала без участия специалиста высокой квалификации со сложным оборудованием.
Где купить диплом специалиста?
http://art-gymnastics.ru/users/54
Хорошей учебы!
Чтобы сделать лечение зрения приходите к нам. Мы находимся по адресу г. Ижевск, ул. Ленина, д. 101. График работы с пн по пт с 9:00 до 16:00, после 16:00 можно прийти, предварительно оформив запись или по субботам и воскресеньям.
Для пар частный эромассаж в Казани с бассейном
Добрый день!
Мы предлагаем дипломы любых профессий по разумным тарифам.
Мы готовы предложить документы ВУЗов, которые находятся в любом регионе Российской Федерации. Вы сможете приобрести качественный диплом от любого заведения, за любой год, включая документы СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и штампами.
Даем гарантию, что в случае проверки документа работодателем, никаких подозрений не возникнет.
Где купить диплом по необходимой специальности?
ilovehabbo.bbon.ru/viewtopic.php?id=1413#p28800
Здравствуйте!
Где заказать диплом специалиста?
Приобрести диплом ВУЗа.
http://worldgonews.ru/page/3
Окажем помощь!
Sell a problematic cryptocurrency – Sell a problematic cryptocurrency, Dark web Crypto Exchange
купить диплом об окончании 11 классов ast-diplomas.com .
купить биокамин недорого – биокамин напольный для квартиры, недорогой электрокамин с эффектом пламени купить
мунджаро тирзепатид инструкция +по применению – мунджаро, mounjaro buy dubai
платформа для инвестиций в бизнес
платформа для поиска инвесторов
Привет!
Приобрести диплом ВУЗа.
Мы предлагаем купить диплом в высочайшем качестве, неотличимый от оригинального документа без использования специального оборудования и квалифицированного специалиста.
Где заказать диплом специалиста?
https://macadamlab.ru/wiki/index.php?title=Купить_диплом
Удачи!
ремонт квартир цена за квадратный москва
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным ценам.
Мы предлагаем документы ВУЗов, расположенных в любом регионе Российской Федерации. Можно купить качественно сделанный диплом от любого заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы выпускаются на бумаге высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригиналов. Документы заверяются необходимыми печатями и подписями.
Гарантируем, что при проверке документов работодателями, никаких подозрений не появится.
Где приобрести диплом специалиста?
newrealgames.ru/kupit-diplom-byistro-nadezhno-legalno
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в вологде, купить диплом физика, купить дипломы о высшем, купить диплом нового образца, купить диплом инженера электрика, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: https://www.hashtap.com/@anna.erofeeva/%D0%B7%D0%B0%D0%B4%D0%B0%D1%87%D0%B0-APw6J41V5WwR
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Успешной учебы!
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить свидетельство о разводе, купить диплом в волгодонске, купить диплом продавца, купить диплом маркетолога, купить аттестат, а потом наткнулся на https://kvixi.com/blogs/1108/?????????-??????????-????????????-??-????????, где все мои учебные проблемы были решены!
Удачи!
Привет!
Заказать диплом университета.
Мы предлагаем купить диплом отличного качества, неотличимый от оригинала без использования дорогостоящего оборудования и опытного специалиста.
Где приобрести диплом по необходимой специальности?
http://w66501ot.bget.ru/index.php?subaction=userinfo&user=icajizeh
Хорошей учебы!
Приветствуем вас на нашем веб-сайте! Здесь вы найдёте всё необходимое для успешного управления своими финансами.
виртуальная кредитная карта Мы предлагаем широкий спектр финансовых продуктов, которые помогут вам достичь ваших целей и обеспечить стабильность в будущем.
В нашем ассортименте представлены различные виды банковских продуктов, инвестиции, страхование, кредиты и многое другое. Мы постоянно обновляем нашу базу данных, чтобы вы всегда были в курсе последних тенденций и инноваций на финансовом рынке.
Наши специалисты помогут вам выбрать наиболее подходящий продукт, учитывая ваши индивидуальные потребности и предпочтения.
кредитная карта виртуальная Мы предоставляем консультации и рекомендации, чтобы вы могли принять обоснованное решение и избежать возможных рисков.
Не упустите возможность воспользоваться нашими услугами и откройте для себя мир финансовых возможностей! Заходите на наш сайт, ознакомьтесь с каталогом продуктов и начните свой путь к финансовой стабильности прямо сейчас!
стартап платформа для привлечения инвестиций
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
Мы предлагаем документы ВУЗов, которые расположены в любом регионе РФ. Можно заказать диплом за любой год, включая сюда документы старого образца. Дипломы и аттестаты печатаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригинала. Документы заверяются необходимыми печатями и подписями.
Где заказать диплом по актуальной специальности?
flora-online.ru/glavnaya/tsvetyi-na-1-sentyabrya-2/
go to my blog Development Software and Tools
платформа для предпринимателей
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом маркетолога, купить диплом в нижневартовске, купить диплом в ульяновске, купить диплом электромонтера, #купить аттестат за 11 класс, а затем переключился на дипломы вузов. Подробности здесь:
http://www.sskyn.com/home-uid-82120.html
http://www.pcporadenstvi.cz/rudiplomirovaniecom
http://seneka-vl.ru/index.php?subaction=userinfo&user=ehekipiw
https://akvamarinshop.ru/products/gromkogovoritel-emn-2-24v-s-dvumya-kolonkami–tumannyj-gorn-mikrofon-sirena-marco-italiya-art-tdc-13601213/#comment_25144
http://slbook-kaluga.ru/index.php/forum/user/239080-obytoda
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успешной учебы!
Привет!
Приобрести документ о получении высшего образования вы можете у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации.
Наша компания предлагает выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Диплом способен пройти лубую проверку, даже с использованием специальных приборов.
http://www.qzzjzs.com/home.php?mod=space&uid=101568
https://bazar-planet.ru/index.php?threads/%D0%9D%D1%83%D0%B6%D0%BD%D0%B0-%D1%80%D0%B0%D0%B1%D0%BE%D1%82%D0%B0.87/page-5#post-5030
http://helenos.pavel-rimsky.cz/doku.php?id=diploman
http://dobrknigi.ru/howto/?PAGE_NAME=profile_view&UID=26184
http://forum.combat-arnis.ru/profile.php?mode=viewprofile&u=333491
На этой странице представлены самые лучшие онлайн игровые автоматы на деньги, а также рекомендации по выбору надежных казино Автоматы на деньги
Привет, друзья!
Где приобрести диплом по нужной специальности?
Приобрести документ ВУЗа можно в нашей компании в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы получите диплом по любым специальностям, включая документы Советского Союза. Даем гарантию, что при проверке документа работодателем, каких-либо подозрений не появится.
http://nvkb.ru/forum/index.php/user/97500/
Хорошей учебы!
Натуральные халаты и хлопковые пижамы, согревающие майки и трусы – европейская мужская домашняя одежда и конечно белье должно чувствовать удобство. https://incanto.com.ua/trusy-slip-muzhskiye интернет-магазин. Тут все уникальные варианты, безупречные ткани, нужные размеры. Это всё что необходимо для настоящего расслабления после работы. Положитесь на проверенные бренды.
Все курсы для обучения профессии Видеопродюсер – Все курсы по работе с текстом, Курсы по Бизнес аналитике
создание сайтов – создание веб сайта, заказать сайт цена
Добрый день!
Для многих людей, приобрести диплом о высшем образовании – это необходимость, возможность получить достойную работу. Но для кого-то – это понятное желание не терять массу времени на учебу в ВУЗе. С какой бы целью вам это не понадобилось, мы готовы помочь вам. Максимально быстро, профессионально и по разумной стоимости сделаем документ любого ВУЗа и любого года выпуска на подлинных бланках со всеми печатями.
Мы предлагаем максимально быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Наш диплом пройдет лубую проверку, даже с применением специфических приборов. Решите свои задачи быстро и просто с нашим сервисом.
Где приобрести диплом по необходимой специальности?
https://www.bodybuilding.net/members/worksale.html
Хорошей учебы!
Привет, друзья!
Купить документ института вы можете у нас. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы старого образца. Гарантируем, что при проверке документов работодателями, каких-либо подозрений не появится.
Мы предлагаем быстро и выгодно купить диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями. Наш диплом пройдет любые проверки, даже с использованием специфических приборов. Решайте свои задачи быстро и просто с нашим сервисом.
Где купить диплом по необходимой специальности?
https://remontmix.ru/forum/viewtopic.php?t=11607
Удачи!
additional reading https://crazy-pachinko.com/
узнать обменник bestchange
В сфере азартных игр в интернете особенно важны аспекты защиты данных и обеспечения надежности операций. Это ключевые аспекты, на которых строятся доверие игроков и успешная работа платформ http://www.clean-ace8.com/bbs/board.php?bo_table=free&wr_id=367611
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в абакане, купить дипломы о высшем, купить свидетельство о рождении, купить диплом магистра, купить диплом в камышине и получил базовые знания. В итоге остановился на материале: https://www.journeywithlynn.com/go/lynn-you-are-a-writer/
https://gas-tite.co.uk/simple-checks-before-calling/
http://mirdverei09.ru/products/metallicheskie_dveri_goldengreen_/#comment_99735
http://bestphotography.ca/2018/06/26/kid-photography/#comment-486841
https://fureai.group/hp-slider-phone-2/#comment-165669
Успешной учебы!
fade away – punish the abuser, fade away
Meet AI Binance trading bot
Quickstart your trading journey with AI-driven Dollar Cost
Averaging bot, designed for sustainable low-risk growth
over the long term.
trading bot
Meet AI Binance trading bot
Quickstart your trading journey with AI-driven Dollar Cost
Averaging bot, designed for sustainable low-risk growth
over the long term.
trading bot binance
Здравствуйте!
Где приобрести диплом специалиста?
Купить диплом о высшем образовании.
http://angelteam.uv.ro/profile.php?mode=viewprofile&u=205785
Рады оказаться полезными!
купить диплом сейчас ast-diplomas.com .
wow pve boost wow pve boost .
Привет, друзья!
Где приобрести диплом по нужной специальности?
Приобрести документ института вы сможете в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов РФ. Вы получите необходимый диплом по любой специальности, включая документы СССР. Даем 100% гарантию, что при проверке документа работодателем, каких-либо подозрений не появится.
http://anrufen2.ucoz.ru/news/svershilos/2010-10-24-8/
Удачи!
Академии KRAKEN
Данный раздел посвящен образовательным проектам площадки KRAKEN. Здесь вы сможете ознакомиться с нашими сервисами, их услугами, а также различной полезной информацией. Мы предоставляем нашим пользователям не только возможность купли-продажи запрещенных веществ, мы предоставляем возможность стать частью комьюнити настоящих профессионалов, частью комьюнити — Академии KRAKEN!
Актуальные ссылки на площадку
КЛИР: (браузер+впн)
—
Kraken18att.ru
ТОР: (впн+тор)
— kraken2trfqodidvlh4aa337cpzfrhdlfldhve5nf7njhumwr7instad.onion
Зайти на Kraken
Привет!
Заказать диплом университета.
Наша компания предлагает приобрести диплом в высоком качестве, неотличимый от оригинального документа без участия специалиста высокой квалификации с дорогостоящим оборудованием.
Где приобрести диплом по актуальной специальности?
http://behealthy.maxbb.ru/posting.php?mode=post&f=8
Успехов в учебе!
Привет!
Мы можем предложить дипломы любых профессий по приятным тарифам.
Мы можем предложить документы ВУЗов, расположенных на территории всей РФ. Можно купить качественно сделанный диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются всеми требуемыми печатями и штампами.
Гарантируем, что при проверке документов работодателем, подозрений не возникнет.
Где заказать диплом специалиста?
jagplay.ekafe.ru/viewtopic.php?f=22&t=3477
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом инженера, купить диплом в златоусте, купить диплом в сургуте, купить диплом хореографа, купить диплом в миассе, получил базовую информацию.
Остановился в итоге на материале купить диплом логиста, https://vedprakashsharma.in/gallery#comment-49910
http://www.espanol.org.ru/spain/odp/go.php?url=https://originality-diplom.com/
https://lider-school174.com/forum/user/1030/
http://www.bakinsky-dvorik.ru/club/user/148184/blog/4465/
https://www.huntingnet.com/forum/members/s3rkinr114.html
Удачи!
1win – относительно Молодое виртуальное казино, которое принадлежит компании MFI investments. В перечень предлагаемых услуг входят: ставки на спорт, киберспорт, тв программы, а также подборка совершенных игровых автоматов и присоединение к игровым столам с картами https://centrmedprof40.ru/communication/forum/messages/forum4/message1403/1422-sovety-po-vyboru-strategii-v-igrakh-na-1win-kazino?result=new#message1403
Алтайский центр природного камня предоставляет прекрасную возможность купить глыбы с лишайником и мхом по самым привлекательным ценам. Существенно сэкономим ваши денежные средства! Мы осуществляем доставку. Гарантируем отличное обслуживание. Вы можете в этом удостовериться лично. Чтобы получить фотографию камня и узнать сроки поставки, отправьте, пожалуйста, запрос в WhatsApp. Ищете скальная глыба камня купить? Altdikam.ru – портал, мы регулярно работаем над его улучшением. Здесь все наглядно и ясно. Если у вас возникли какие-то вопросы, свяжитесь с нами по телефону. Будем рады вам помочь!
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в чите, купить диплом цена, купить диплом в абакане, купить диплом в кирово-чепецке, купить диплом в краснодаре, потом про дипломы вузов, подробнее здесь https://flexwp.ru/2024/06/01/%d0%ba%d1%83%d0%bf%d0%b8%d1%82%d1%8c-%d0%b3%d0%be%d1%80%d0%bd%d1%8b%d0%b9-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc/
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Хорошей учебы!
Привет!
Купить диплом университета
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Наш диплом способен пройти лубую проверку, даже при использовании профессионального оборудования. Достигайте свои цели быстро и просто с нашим сервисом.
Где приобрести диплом по нужной специальности?
http://g95334gq.beget.tech/content/add/topic
Окажем помощь!.
купить диплом вуза в нижнем https://diploms-x.com .
Привет, друзья!
Для некоторых людей, заказать диплом ВУЗа – это необходимость, шанс получить выгодную работу. Однако для кого-то – это осмысленное желание не терять время на учебу в ВУЗе. С какой бы целью вам это не потребовалось, наша фирма готова помочь. Максимально быстро, качественно и недорого изготовим диплом нового или старого образца на настоящих бланках со всеми печатями.
Мы предлагаем быстро купить диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Наш диплом пройдет лубую проверку, даже с использованием профессионального оборудования. Решите свои задачи быстро и просто с нашими дипломами.
Где заказать диплом по актуальной специальности?
https://biomedia.pro/club/user/125807/blog/?b24statAction=addLogEntry
Хорошей учебы!
Добрый день!
Купить документ ВУЗа можно у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы получите необходимый диплом по любым специальностям, любого года выпуска, включая документы образца СССР. Даем гарантию, что при проверке документов работодателем, подозрений не возникнет.
Мы предлагаем выгодно и быстро купить диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ способен пройти любые проверки, даже с использованием профессионального оборудования. Достигайте свои цели быстро и просто с нашими дипломами.
Где приобрести диплом специалиста?
http://krasmamochki.5nx.ru/viewtopic.php?f=10&t=20883&p=41808#p41808
http://dobrknigi.ru/howto/?PAGE_NAME=profile_view&UID=26195
http://ekopromkonsalt.ru/index.php?subaction=userinfo&user=okyga
http://jilye74.ru/index.php?subaction=userinfo&user=ohubez
https://vk.com/reklama_vzaimnaya?w=wall-80021931_256783
Успехов в учебе!
penalty movie contratiempo moviealabaster movie theater moviesgourmet detective mysteries episodesdog movies dvd
купить диплом техникума в санкт петербурге asxdiplomik.com .
Здравствуйте!
Приобрести диплом любого университета
Наша компания предлагает выгодно заказать диплом, который выполняется на оригинальном бланке и заверен печатями, штампами, подписями должностных лиц. Документ способен пройти любые проверки, даже при использовании профессиональных приборов. Достигайте цели быстро и просто с нашей компанией.
Где купить диплом специалиста?
https://www.mylot.su/blogs/2322
Рады помочь!.
купить диплом в ялте diplomyx.com .
Добрый день!
Где купить диплом по нужной специальности?
Мы предлагаем быстро и выгодно приобрести диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями. Диплом способен пройти любые проверки, даже при помощи специальных приборов. Достигайте цели быстро с нашими дипломами.
Заказать диплом любого ВУЗа.
https://8hofgyain.blogsvila.com/28392439/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
https://yoa45mzo5.ka-blogs.com/81608090/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://9a87bkcce.prublogger.com/27888322/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
https://picbok.org/read-blog/5849
https://ozoms.com/read-blog/514
аттестат о среднем образовании купить аттестат о среднем образовании купить .
1win – относительно Молодое виртуальное казино, которое принадлежит компании MFI investments. В перечень предлагаемых услуг входят: ставки на спорт, киберспорт, тв программы, а также подборка совершенных игровых автоматов и присоединение к игровым столам с картами http://telent.ussoft.kr/bbs/board.php?bo_table=free&wr_id=1595257
Добрый день!
Мы предлагаем документы техникумов, которые находятся на территории всей Российской Федерации. Можно купить диплом от любого заведения, за любой год, в том числе документы СССР. Документы печатаются на бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригиналов. Они будут заверены необходимыми печатями и подписями.
Заказать диплом о высшем образовании.
https://yasqueencommunity.com/blogs/351/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-Russian-Diplom
http://textualheritage.org/index.php?option=com_content&task=view&id=1081
https://pp-galaktika.com.ua/index.php/%D0%95%D1%81%D0%BB%D0%B8_%D0%BF%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D0%BE%D0%B2%D0%B0%D0%BB%D0%B8%D1%81%D1%8C_%D0%BA%D0%BB%D0%B0%D0%BF%D0%B0%D0%BD%D0%B0,_%D0%BC%D0%B0%D0%BD%D0%BE%D0%BC%D0%B5%D1%82%D1%80%D1%8B,_%D0%B7%D0%B0%D0%B4%D0%B2%D0%B8%D0%B6%D0%BA%D0%B8_-_%D0%B6%D0%B4%D0%B5%D0%BC_%D0%92%D0%B0%D1%81!
https://sikhona.social/blogs/35217/%D0%9B%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-Russian-Diplom
https://ikl5goplk.mybloglicious.com/49441363/%D0%9B%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
Хорошей учебы!
купить диплом начальных классов ast-diploms.com .
Здравствуйте!
Заказать документ института можно у нас. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы СССР. Гарантируем, что при проверке документов работодателем, подозрений не появится.
Наша компания предлагает быстро и выгодно приобрести диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями должностных лиц. Наш документ пройдет лубую проверку, даже с применением специально предназначенного оборудования. Достигайте свои цели быстро с нашей компанией.
Где купить диплом специалиста?
http://maglik.ru/index.php?subaction=userinfo&user=itoruhi
https://xn—-btbthcge4aikr4i.xn--p1ai/forum/user/34204/
http://forum.gold-forum.ru/index.php?showtopic=75108
http://crtdu-kras.ru/communication/forum/user/241307/
http://liderotrasli.ru/index.php?subaction=userinfo&user=okuwuc
Удачи!
Привет!
Для некоторых людей, купить диплом университета – это острая необходимость, удачный шанс получить достойную работу. Однако для кого-то – это желание не терять множество времени на учебу в ВУЗе. Что бы ни толкнуло вас на такой шаг, наша фирма готова помочь вам. Быстро, качественно и недорого изготовим диплом любого года выпуска на подлинных бланках со всеми требуемыми подписями и печатями.
Мы предлагаем выгодно и быстро купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями официальных лиц. Данный диплом способен пройти лубую проверку, даже с использованием специальных приборов. Достигайте цели быстро с нашими дипломами.
Где приобрести диплом специалиста?
http://newsofgames.ru/diplomyi-o-vyisshem-obrazovanii-v-moskve-legko-i-dostupno
Удачи!
веб-сайте электрик томск
как можно купить аттестат как можно купить аттестат .
аттестат об окончании 11 классов купить diplomyx.com .
Добрый день!
Приобрести диплом любого университета
Мы предлагаем выгодно и быстро заказать диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями официальных лиц. Документ способен пройти любые проверки, даже с применением специальных приборов. Решите свои задачи быстро и просто с нашим сервисом.
Где купить диплом специалиста?
http://86hm.ru/forum/flame/?topic_id=25094
Рады оказать помощь!.
купить диплом дерматолога купить диплом дерматолога .
Привет, друзья!
Где купить диплом по актуальной специальности?
Купить диплом ВУЗа.
https://www.thusc.org/home.php?layout=365437
Поможем вам всегда!
купить диплом о высшем образовании с занесением в реестр в кемерово ast-diploms.com .
купить диплом в минусинске купить диплом в минусинске .
Привет, друзья!
Для некоторых людей, купить диплом о высшем образовании – это необходимость, уникальный шанс получить достойную работу. Однако для кого-то – это желание не терять время на учебу в универе. С какой бы целью вам это не понадобилось, мы готовы помочь. Максимально быстро, профессионально и недорого изготовим документ любого ВУЗа и любого года выпуска на подлинных бланках со всеми подписями и печатями.
Мы предлагаем выгодно и быстро купить диплом, который выполняется на оригинальном бланке и заверен печатями, штампами, подписями. Наш диплом пройдет лубую проверку, даже с применением профессиональных приборов. Решайте свои задачи максимально быстро с нашими дипломами.
Где заказать диплом специалиста?
http://buldingnews.ru/kak-kupit-diplom-bez-riska-dlya-svoey-reputatsii
Успешной учебы!
Привет, друзья!
Купить документ о получении высшего образования вы можете у нас. Мы предлагаем документы об окончании любых университетов России. Вы получите диплом по любой специальности, включая документы СССР. Гарантируем, что при проверке документов работодателем, каких-либо подозрений не возникнет.
Мы предлагаем выгодно и быстро купить диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Документ способен пройти лубую проверку, даже при использовании специальных приборов. Достигайте цели максимально быстро с нашим сервисом.
Где приобрести диплом по актуальной специальности?
http://www.icmms.co.kr/bbs/board.php?bo_table=free&wr_id=398395
http://slbook-kaluga.ru/index.php/forum/user/245029-obexuz
http://xn--m1acg6c.xn--p1ai/index.php?subaction=userinfo&user=axynu
https://yo-mi.ru/people/user/4229/blog/1280/
http://army.clanfm.ru/viewtopic.php?f=2&t=38201&p=53235#p53235
Удачи!
куплю диплом кандидата наук asxdiplomik.com .
try this site [url=https://my-atomicwallet.de/]Atom wallet[/url]
диплом с внесением в реестр diplomyx.com .
Здравствуйте!
Где приобрести диплом специалиста?
Мы предлагаем выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями официальных лиц. Документ способен пройти любые проверки, даже с использованием специально предназначенного оборудования. Решите свои задачи быстро и просто с нашим сервисом.
Купить диплом о высшем образовании.
https://niq5ar4e6.theobloggers.com/34346835/%D0%A1-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE%D1%81%D1%82%D1%8C%D1%8E-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
https://www.grimdice.ru/index.php?/gallery/image/2-%D0%BD%D0%B8%D0%B7%D0%BA%D0%B8%D0%B5-%D1%80%D0%B0%D1%81%D1%86%D0%B5%D0%BD%D0%BA%D0%B8-%D0%B8-%D0%B8%D0%B4%D0%B5%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B9-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
https://7hz0jwqg2.dreamyblogs.com/28634603/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://xn--80apeih4a.xn--p1ai/club/user/71/blog/4541/
https://network-2295034.mn.co/posts/61837774
Здравствуйте!
Заказать диплом университета.
Мы предлагаем приобрести диплом в высочайшем качестве, который невозможно отличить от оригинала без участия специалистов высокой квалификации со специальным оборудованием.
Где купить диплом специалиста?
http://rosen.moibb.ru/viewtopic.php?f=2&t=411
Удачи!
Здравствуйте!
Где заказать диплом специалиста?
Приобрести диплом ВУЗа.
https://hastui.com/space-uid-11328.html
Окажем помощь!
дипломная работа купить дипломная работа купить .
купить диплом в северске ast-diploms.com .
Здравствуйте!
Мы можем предложить дипломы любой профессии по приятным ценам.
Мы предлагаем документы техникумов, которые находятся на территории всей РФ. Вы имеете возможность купить диплом от любого учебного заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и штампами.
Даем гарантию, что при проверке документов работодателями, подозрений не возникнет.
Где приобрести диплом по актуальной специальности?
films.name/viewforum.php?f=143
диплом о высшем образовании купить в красноярске ast-diplomas.com .
Добрый день!
Где купить диплом специалиста?
Заказать документ о получении высшего образования вы сможете в нашем сервисе. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца. Даем 100% гарантию, что при проверке документов работодателями, каких-либо подозрений не возникнет.
https://gorod343.ru/users/jimgodwapops
Успехов в учебе!
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом фитнес инструктора, купить диплом хореографа, купить диплом в новом уренгое, купить диплом в ростове , купить диплом инженера механика и получил базовые знания. В итоге остановился на материале: http://uznt42.ru/index.php?subaction=userinfo&user=ejifiky
Хорошей учебы!
Добрый день!
Купить диплом ВУЗа.
Наш сервис предлагает заказать диплом высокого качества, который не отличить от оригинального документа без участия специалиста высокой квалификации со сложным оборудованием.
Где купить диплом специалиста?
http://rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
Успехов в учебе!
my response avalanche wallet
Привет, друзья!
Мы готовы предложить дипломы любой профессии по приятным ценам.
Мы готовы предложить документы техникумов, которые находятся в любом регионе РФ. Можно приобрести качественно сделанный диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми обязательными печатями и подписями.
Даем гарантию, что при проверке документа работодателем, никаких подозрений не возникнет.
Где приобрести диплом специалиста?
scientistsufo.ru/kupit-diplom-ofitsialnoe-oformlenie
Those tickets were sold in California, Colorado,
Georgia, New Hampshire and Pennsylvania.
Review my site … 파워볼 게임몬
игры на PS4 или Xbox One – бесплатные игры 2024, GTA 6 дата выхода
Привет!
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам. Цена будет зависеть от выбранной специальности, года выпуска и образовательного учреждения.
Где приобрести диплом по необходимой специальности?
Заказать диплом любого ВУЗа
https://landik-diploms-srednee.ru/kupit-diplom-v-voronezhe
Удачи!
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить диплом о высшем образовании, купить диплом учителя физической культуры, купить диплом в ленинск-кузнецком, купить диплом в артеме, купить диплом в ярославле, получил базовую информацию.
Остановился в итоге на материале купить диплом в екатеринбурге, https://webmoney.forumkz.ru/viewtopic.php?id=2764#p7852
Хорошей учебы!
Добрый день!
Купить диплом любого ВУЗа
Наша компания предлагает выгодно приобрести диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Наш документ пройдет лубую проверку, даже при использовании специфических приборов. Решите свои задачи быстро с нашим сервисом.
Где заказать диплом по нужной специальности?
http://ukrlenta.ru/legkiy-put-k-diplomirovannomu-uspehu-byistro-i-nadezhno
Всегда вам поможем!.
Откройте Новые Финансовые Возможности!
Что мы предлагаем?
Мы предоставляем вам лучшие финансовые продукты, включая кредиты, банковские карты и займы. Наши решения помогут вам достигнуть любых целей и воплотить мечты в реальность.
займы
Финансовые Решения для Любых Целей
Планируете покупку жилья, автомобиля или образование? Наши кредитные программы идеально подойдут для ваших нужд. Оформите кредит на нашем сайте и получите выгодные условия и удобные сроки погашения.
Преимущества наших Банковских Карт
Наши банковские карты предлагают:
– Удобство безналичных расчетов
– Щедрые бонусы и привилегии
Оформите карту онлайн и получите кэшбэк, скидки у партнеров и участие в программе лояльности. Найдите карту с оптимальными лимитами и условиями обслуживания именно для вас.
Быстрые Займы на Любые Нужды
Не хватает денег до зарплаты или на неожиданные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок, чтобы вы могли решать финансовые вопросы без задержек.
Наши Преимущества:
– **Простота и Удобство**: Оформите заявку онлайн за считанные минуты.
– **Надежность и Прозрачность**: Честные условия и отсутствие скрытых комиссий.
– **Индивидуальный Подход**: Мы учитываем ваши личные обстоятельства и предлагаем оптимальные условия.
Не упустите шанс улучшить свою финансовую ситуацию! Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и почувствуйте все преимущества работы с надежным финансовым партнером.
кредитная карта виртуальная
С нами ваши мечты станут реальностью!
Enter your numbers into the checker to see iff you have won any prizes in the last 180 days.
Here is my web-site; Powerball Winners
плиты армстронг https://armstrong-ceiling24.ru/
купить диплом о неполном высшем образовании купить диплом о неполном высшем образовании .
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом в копейске, купить диплом в северске, купить диплом инженера, где купить диплом о среднем образование, купить диплом в кирове, а потом наткнулся на http://kyym.ru/video/54-kazan-2/, где все мои учебные проблемы были решены!
Хорошей учебы!
Добрый день!
Для некоторых людей, купить диплом университета – это острая потребность, уникальный шанс получить отличную работу. Но для кого-то – это желание не терять массу времени на учебу в институте. Что бы ни толкнуло вас на такой шаг, мы готовы помочь вам. Максимально быстро, качественно и недорого сделаем диплом любого года выпуска на подлинных бланках с реальными печатями.
Наши специалисты предлагают выгодно купить диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Данный диплом пройдет любые проверки, даже с использованием профессиональных приборов. Решайте свои задачи быстро и просто с нашими дипломами.
Где заказать диплом специалиста?
http://lightsdemons.phorum.pl/viewtopic.php?p=66962#66962
Удачи!
Здравствуйте!
Заказать документ о получении высшего образования можно у нас. Мы оказываем услуги по продаже документов об окончании любых ВУЗов России. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы образца СССР. Гарантируем, что при проверке документов работодателями, подозрений не появится.
Наши специалисты предлагают максимально быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями официальных лиц. Диплом способен пройти лубую проверку, даже при использовании специфических приборов. Решите свои задачи быстро с нашим сервисом.
Где заказать диплом специалиста?
http://www.musichunt.pro/blogs/view.htm?id=79825
http://xn--e1adiici.xn--p1ai/index.php?subaction=userinfo&user=etiku
http://kamaz-ukraine.com/index.php?subaction=userinfo&user=eruheqewu
http://witchvswinx.getbb.ru/viewtopic.php?f=10&t=2944
http://grandtour.tv/index.php?subaction=userinfo&user=ovunumo
Хорошей учебы!
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом в ставрополе, купить диплом медбрата, купить аттестат за 11 класс, купить диплом в бердске, купить диплом слесаря и получил базовые знания. В итоге остановился на материале: https://biznet.kz/discussion/1288/kupit-diplom-v-novosibirske/p1?new=1
Успехов в учебе!
купить диплом фитнес diplomyx.com .
Привет, друзья!
Где приобрести диплом специалиста?
Заказать документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, включая документы образца СССР. Даем 100% гарантию, что при проверке документа работодателем, никаких подозрений не возникнет.
http://zakupki.motilek.ru/index.php?name=account&op=info&uname=okiticica
Удачи!
Привет!
Мы предлагаем документы техникумов, которые расположены на территории всей Российской Федерации. Вы имеете возможность купить качественный диплом от любого заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты делаются на “правильной” бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Документы будут заверены всеми необходимыми печатями и штампами.
Приобрести диплом о высшем образовании.
https://tf5t93g8y.activosblog.com/27765190/%D0%94%D0%B5%D1%82%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://7k3ug9mwr.blogars.com/27710394/%D0%9F%D0%BE%D0%B4%D1%80%D0%BE%D0%B1%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://0838v5moc.theisblog.com/28469300/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://sonnick84.webnode.page/l/kak-vozmozhno-bystro-priobresti-attestat-v-onlajn-magazine/
https://3qxx1kuw0.verybigblog.com/27939944/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Хорошей учебы!
go to this site buy ethetf
And based on thee level of cleaning you supply, it can be accomplished inn an hour or two.
Also visit my web page – 주점알바
На сайте https://geo-gdz.ru/ представлены ГДЗ по географии, истории. Перед вами огромная библиотека, которая работает в режиме реального времени. Здесь вы найдете школьные учебники, контурные карты, а также атласы, которые помогут получить новые знания, освоить нужную дисциплину. Список всей важной и нужной информации находится прямо на страницах сайта. Каждый год вносятся изменения в соответствии с политическими действиями. Этот сайт предназначен специально для тех, кто не в курсе этих изменений, но стремится расширить свой уровень знаний.
Привет, друзья!
Мы изготавливаем дипломы любых профессий по невысоким тарифам. Стоимость может зависеть от определенной специальности, года получения и образовательного учреждения.
Где купить диплом специалиста?
Заказать диплом любого университета
https://arusak-diploms-srednee.ru/svidetelstvo-o-brake
Хорошей учебы!
Chefs and head cooks oversee the preparation of meals in restaurants,
private residences, and other dining establishments.
Review my website :: Easy jobs for women
купить диплом в иркутске ast-diploms.com .
купить диплом в евпатории diplomasx.com .
Bs2site – Bs2tsite4, Bs2tsite4
Creating an online dating profile? Be honest and clear about your interests. Upload recent photos and write a bio that reflects your true personality
news site
Советую Mihaylov digital, их направление деятельности это seo в гугл, а также создание сайтов
Добрый день!
Где заказать диплом по актуальной специальности?
Заказать диплом о высшем образовании.
https://lasfloresboutique.ru/product-page/букет-из-роз-и-астральмерии
Всегда вам поможем!
кто покупал диплом о высшем образовании отзывы кто покупал диплом о высшем образовании отзывы .
Привет, друзья!
Где купить диплом по нужной специальности?
Мы предлагаем документы институтов, которые находятся в любом регионе России. Вы сможете купить диплом за любой год, в том числе документы СССР. Дипломы печатаются на бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые не отличить от оригинала. Документы будут заверены всеми необходимыми печатями и штампами.
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
https://ast-diploms24.ru/kupit-diplom-vracha
Всегда вам поможем!
Привет!
Мы готовы предложить документы ВУЗов, расположенных на территории всей РФ. Можно заказать качественно сделанный диплом за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Документы выпускаются на бумаге высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Они заверяются необходимыми печатями и штампами.
Купить диплом о высшем образовании.
https://alivechrist.com/read-blog/213
https://zz40k1bli.bleepblogs.com/28767199/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://fighter71.com/read-blog/1696
https://wiki.3cdr.ru/wiki/index.php/%D0%9F%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B_%D0%B2_%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%BC_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5_%D0%BF%D0%BE_%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D0%BE%D0%B9_%D1%86%D0%B5%D0%BD%D0%B5
https://hellsms.com/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=6638
Успехов в учебе!
Inleiding
Niemand wacht op op complexe en tijdrovende graafproces om een beschadigd riool te herstellen. Gelukkig is er een nieuwe en effectieve methode met de naam ‘relinen’. In dit artikel leggen we uit wat relinen is, wat maakt het het de voorkeur geniet boven traditionele manieren, en op welke manier het jou tijd kost, geld bespaart en overlast kan besparen.
Wat is Relinen?
Relinen, ook bekend als bekend als kousmethode, is de moderne methode voor reparatie van kapotte afvoeren zonder de noodzaak voor graven nodig zijn. Tijdens dit proces wordt een flexibele kous gevuld met hars bij de oude buis ingebracht en uitgehard, waardoor een nieuwe, sterke voering vormt in de huidige.
Hoe Werkt Relinen?
Het proces start door het inspecteren en reiniging van kapotte riool. Vervolgens komt een flexibele kous, geimpregneerd met hars, in het riool geplaatst. De kous moet uitgerold waardoor deze tegen de wanden van de oude buis komt te liggen. Na uitharding van de hars vormt de kous een vers, strakke buis in de huidige buis.
Voordelen van Relinen
http://andersonpvid114.cavandoragh.org/rioolproblemen-verholpen-zonder-de-graafwerkzaamheden-leer-over-relinen
http://andersonyejb220.image-perth.org/problemen-met-het-riool-opgelost-zonder-graafwerkzaamheden-ontdek-relining
http://emilianoozdg452.iamarrows.com/problemen-met-het-riool-opgelost-zonder-graven-leer-over-relining
https://zenwriting.net/celenaeicb/problemen-met-het-riool-verholpen-zonder-graven-leer-over-relining
http://donovanmcac444.tearosediner.net/problemen-met-het-riool-verholpen-zonder-graafwerkzaamheden-ontdek-relinen
Relinen heeft veel pluspunten tegenover traditionele graafmethoden. Ten eerste vermijdt het de noodzaak van uitgebreide graafwerkzaamheden, wat niet alleen tijd en geld bespaart, maar ook overlast vermindert. Bovendien verlengd het proces de levensduur van het riool aanzienlijk en zorgt het voor een gladde binnenkant, waardoor blokkades minder vaak optreden.
Waarom Kiezen voor Relinen
Als u problemen met het riool hebt, vraag je je misschien af waarom je zou kiezen voor relinen in plaats van traditionele reparatiemethoden. Hier zijn een paar redenen waarom relinen de beste keuze kan zijn.
Minder overlast
Met oude methoden moet je uw tuin, oprit of straat openbreken, wat veel rommel geeft. Relinen vermijdt dit omdat het van binnen wordt gefixt. Dit betekent minder rommel en minder verstoring van uw dagelijkse leven.
Kostenbesparend
Hoewel de initiele kosten van relinen misschien meer zijn dan traditionele methoden, bespaar je op de lange termijn geld. Graafwerkzaamheden zijn arbeidsintensief en tijdrovend, wat de kosten verhoogt. En voorkomt relinen toekomstige problemen en dure fixes door de duurzame aard van de nieuwe buis.
Duurzaam en Betrouwbaar
Relinen maakt gebruik van hoogwaardige materialen die lang meegaan. De nieuwe binnenvoering is bestendig tegen corrosie en wortelgroei, wat betekent dat uw riool minder snel opnieuw problemen zal krijgen. Dit maakt relinen een duurzame en betrouwbare oplossing voor rioolproblemen.
Het Relinen Proces Stap voor Stap
Bent u benieuwd hoe relinen werkt? Hier volgt een gedetailleerd overzicht van de stappen die worden genomen om uw riool te relinen.
Eerst inspectie, dan schoonmaken
De eerste stap van relinen is een grondige inspectie van uw riool. Dit kan met een camera, zodat de technici precies kunnen zien waar de beschadigingen zich bevinden. Daarna wordt het riool grondig gereinigd om ervoor te zorgen dat de kous goed kan hechten.
Plaatsen van de een Kous
Na het schoonmaken wordt de met geimpregneerde kous kous in het gebracht. Dit proces vindt meestal via een toegangspunt, zoals een put een een. De wordt door door riool getrokken totdat het hele hele gedeelte gedeelte is.
Uitharding
Zodra de kous op zijn zijn zit, wordt deze opgeblazen zodat deze deze de de van het riool riool te te. De hars in kous kous vervolgens vervolgens, vaak middels middels lucht of uv-licht. Dit proces proces zorgt ervoor dat kous kous stevige, stevige naadloze buis buis vormt de oude oude.
Veelgestelde Vragen over Relinen
Heeft u nog vragen over relinen? Hier we we van de meest gestelde vragen over vragen over rioolreparatiemethode.
Is Relinen Geschikt voor alle rioolleidingen ?
Relinen is geschikt voor de de soorten rioolleidingen, inclusief de gemaakt zijn van van, beton, pvc en en. Het is is echter om om professionele inspectie inspectie laten uitvoeren om om bepalen of uw uw situatie situatie geschikt voor voor.
Hoe duurt Duurt relinen proces Proces
De van het relinen proces hangt af af van de omvang van de en en lengte van de de leiding gerepareerd gerepareerd worden. In de meeste gevallen gevallen kan het relinen een dag voltooid worden, wat aanzienlijk sneller sneller dan traditionele traditionele.
Wat Zijn kosten van relinen Relinen
De van relinen varieren varieren afhankelijk van factoren, zoals de lengte diameter van van leiding leiding en mate mate schade. Hoewel initieel duurder duurder zijn dan traditionele traditionele, bespaart u op de lange lange geld geld de de duurzaamheid lagere onderhoudskosten.
Conclusie
Relinen biedt een effectieve, kostenefficiente en duurzame duurzame oplossing het herstellen van van riolen zonder zonder de rommel en van van. Door te voor relinen, kunt u genieten van de voordelen voordelen van naadloze, naadloze nieuwe binnen uw bestaande bestaande, waardoor toekomstige problemen problemen voorkomen.
Bent u u om de voordelen van relinen relinen te te? Neem nog nog op op onze onze experts ontdek ontdek wij wij kunnen helpen bij bij herstellen herstellen van riool
http://beaurwhj553.trexgame.net/problemen-met-het-riool-opgelost-zonder-graven-leer-over-relining
https://privatebin.net/?3dcbcf792499a5d0#GC11KNHkRa3wuuZsceGZRGKUbEZv2B8DCkpPXsaQzZLJ
https://telegra.ph/Problemen-met-het-riool-Opgelost-Zonder-Graafwerkzaamheden-Leer-over-Relining-07-03
http://codybkaq372.lowescouponn.com/problemen-met-het-riool-opgelost-zonder-de-graven-leer-over-relining
https://jsbin.com/wufakifuke
купить аттестат о полном среднем купить аттестат о полном среднем .
купить диплом в белорецке https://diploms-x.com .
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом маркетолога, купить диплом о среднем образовании, купить диплом в волгограде, купить диплом в уфе, купить диплом в великом новгороде, потом попал на
https://x4all.de/topic/221-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B7%D0%B0-11-%D0%BA%D0%BB%D0%B0%D1%81%D1%81%D0%BE%D0%B2-b409x/
https://smm-seo.ru/members/robertgreabe.5389/
http://xn--80ae1aidok.xn--p1ai/users/ijekiqu
http://invest-real.blogspot.com/2014/03/ekocentrs.html
https://terra-terra.ru/products/stul-detskij-corona-TDTCOR03/#comment_156658
и там решили все мои учебные заботы!
Успехов в учебе!
Здравствуйте!
Купить диплом ВУЗа.
Мы предлагаем заказать диплом высочайшего качества, неотличимый от оригинала без участия специалиста высокой квалификации с дорогостоящим оборудованием.
Где приобрести диплом специалиста?
http://kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
Успехов в учебе!
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по разумным тарифам.
Мы можем предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Вы сможете купить качественно сделанный диплом от любого учебного заведения, за любой год, включая сюда документы СССР. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Они будут заверены всеми требуемыми печатями и штампами.
Гарантируем, что в случае проверки документов работодателями, каких-либо подозрений не возникнет.
Где приобрести диплом по актуальной специальности?
http://www.fellnasen-service.de/index.php?thread/23621-??????-??????-?-??????-???????????-??-??????-???????/
купить дипломы о высшем образовании москва ast-diplomas.com .
1win game 1win.tr-kazakhstan.kz Отзывы игроков о 1win разнообразны. Некоторые пользователи хвалят букмекерскую контору за качественные услуги, высокие коэффициенты и удобный интерфейс, в то время как другие могут высказывать свои замечания. Важно помнить, что опыт каждого игрока может быть индивидуальным. 1win tr-kazakhstan kz
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: купить диплом в туле, купить диплом маляра, купить диплом в улан-удэ, купить диплом механика, #купить диплом в ленинск-кузнецком, а затем переключился на дипломы вузов. Подробности здесь: http://pitomniksochi.ru/index.php?subaction=userinfo&user=yzaxekiq
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Успешной учебы!
Добрый день!
Где приобрести диплом специалиста?
Готовый диплом с приложением отвечает условиям и стандартам, неотличим от оригинала.
Купить диплом о высшем образовании.
http://3drus.ru/forum/topic_34870
http://www.noo.by/wiki/Закажите_диплом_в_пару_кликов
https://www.friend007.com/read-blog/135961
https://bib.az/read-blog/42627
https://sonnick84.blogsuperapp.com/28744928/%D0%A7%D1%82%D0%BE-%D0%B8%D0%BC%D0%B5%D0%BD%D0%BD%D0%BE-%D1%82%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%B8%D0%B7-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D0%B8-%D0%B4%D0%BB%D1%8F-%D0%BF%D1%80%D0%BE%D0%B8%D0%B7%D0%B2%D0%BE%D0%B4%D1%81%D1%82%D0%B2%D0%B0-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом во владивостоке, купить диплом в белгороде, купить речной диплом, купить диплом в новоалтайске, купить диплом в брянске, затем наткнулся на http://good-serial.ru/2024/06/poluchite-diplom-bez-lishnih-ozhidaniy/, где все мои учебные вопросы были решены!
Хорошей учебы!
Найдите промокоды Vavada казино и получите доступ к эксклюзивным бонусам. Улучшите свои игровые возможности с помощью этих кодов.
Промокоды Drip казино помогут вам получить дополнительные привилегии. Найдите актуальные коды и улучшите свои игровые возможности.
Промокоды Vavada казино предоставляют игрокам отличные бонусы. Воспользуйтесь свежими предложениями и наслаждайтесь всеми преимуществами, которые они предлагают.
Добро пожаловать в наш каталог вакансий! Здесь вы найдёте актуальные предложения от лучших работодателей, которые ждут именно вас.
я курьер Мы предлагаем разнообразные вакансии в различных отраслях, включая финансы, IT, маркетинг, образование и многие другие. Изучайте предложения, сортируйте их по интересующим вас критериям и связывайтесь с компаниями напрямую для уточнения деталей.
работник колл центра Мы уверены, что в нашем каталоге вы обязательно найдёте подходящую вакансию, которая позволит вам реализовать свой потенциал и достичь успеха в карьере.
купить аттестат за 9 классов ast-diplomas.com .
Добрый день!
Где приобрести диплом по нужной специальности?
Мы можем предложить документы ВУЗов, расположенных в любом регионе Российской Федерации. Можно приобрести диплом от любого высшего учебного заведения, за любой год, включая сюда документы СССР. Дипломы печатаются на “правильной” бумаге высшего качества. Это дает возможности делать настоящие дипломы, которые невозможно отличить от оригинала. Документы будут заверены всеми обязательными печатями и штампами.
Мы готовы предложить дипломы любой профессии по доступным ценам.
https://ast-diplom.com/kupit-diplom-magistra
Всегда вам поможем!
Привет, друзья!
Заказать диплом ВУЗа
Наша компания предлагает выгодно и быстро купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Документ пройдет лубую проверку, даже с применением специфических приборов. Решите свои задачи быстро с нашим сервисом.
Где купить диплом по необходимой специальности?
https://rcdrift.ru/forum/member.php?u=21074
Окажем помощь!.
Здравствуйте!
Где приобрести диплом специалиста?
Наши специалисты предлагают быстро и выгодно купить диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями. Наш документ пройдет любые проверки, даже при использовании профессиональных приборов. Решайте свои задачи максимально быстро с нашими дипломами.
Купить диплом любого ВУЗа.
https://keros-mod.ru/index.php?/gallery/image/12-%D0%BD%D0%B8%D0%B7%D0%BA%D0%B8%D0%B5-%D1%80%D0%B0%D1%81%D1%86%D0%B5%D0%BD%D0%BA%D0%B8-%D0%B8-%D0%B2%D1%8B%D1%81%D0%BE%D0%BA%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
https://www.webofiice.ro/blogs/1890/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
https://ou812chat.com/read-blog/1225
https://www.convergenceapp.org/posts/61821136
https://gx6yxfr5c.blogrelation.com/34268593/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
купить диплом мастера маникюра [url=https://asxdiplomik.com/]asxdiplomik.com[/url] .
командир купил диплом asxdiplomik24.ru .
купить диплом в домодедово asxdiplomik24.ru .
купить диплом о среднем образовании в томске https://diploms-x.com .
купить диплом диспетчера diplomyx.com .
купить диплом для аттестации ast-diplomas.com .
Здравствуйте!
Приобрести диплом любого университета
Мы предлагаем выгодно и быстро заказать диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями официальных лиц. Данный документ способен пройти любые проверки, даже с использованием специальных приборов. Решайте свои задачи быстро с нашей компанией.
Где купить диплом специалиста?
https://master39.net/forum/user/4879/
Будем рады вам помочь!.
Привет, друзья!
Где купить диплом специалиста?
Получаемый диплом со всеми печатями и подписями отвечает стандартам Министерства образования и науки РФ, неотличим от оригинала – даже со специально предназначенным оборудованием.
Приобрести диплом о высшем образовании.
https://godsoftheuniverse.mn.co/posts/61725501
https://mazda-demio.ru/forums/index.php?autocom=gallery&req=si&img=4710
http://paning.flybb.ru/viewtopic.php?f=7&t=1205&sid=28ca68bafe42c77a2dec671e3bbe9bf9
https://geoamor.com/read-blog/30355
http://mafiaclans.ru/viewtopic.php?f=43&t=7293
Здравствуйте!
Купить документ ВУЗа вы имеете возможность в нашей компании. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что при проверке документа работодателями, подозрений не появится.
Мы предлагаем выгодно приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Данный документ способен пройти лубую проверку, даже с использованием специальных приборов. Достигайте своих целей быстро с нашими дипломами.
Где купить диплом по актуальной специальности?
http://forum.jeep-club.by/index.php?/blog/43/entry-3012-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B2%D0%BE%D0%BB%D0%B3%D0%BE%D0%B3%D1%80%D0%B0%D0%B4%D0%B5/
https://www.livelib.ru/reader/xozkacqahv
http://www.riccom.ru/pub/index.php?subaction=userinfo&user=aqyhufy
http://zingcorp.com.au/component/kunena/sub-category-locked/60951#60988
https://vk.com/club69673339?w=wall-69673339_1238
Хорошей учебы!
купить диплом морские купить диплом морские .
Добрый день!
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам. Стоимость зависит от той или иной специальности, года выпуска и образовательного учреждения.
Где купить диплом специалиста?
Заказать диплом любого ВУЗа
https://arusak-diploms-srednee.ru/diplom-sredne-spetcialnoe-obrazovanie
Успешной учебы!
купить диплом автомобильный diplomyx.com .
Здравствуйте!
Где заказать диплом специалиста?
Заказать документ университета можно у нас в Москве. Мы предлагаем документы об окончании любых университетов Российской Федерации.
Мы можем предложить дипломы любой профессии по выгодным тарифам. Стоимость будет зависеть от той или иной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику тарифов.
https://forumrabota.0pk.me/viewtopic.php?id=7320#p16792
Хорошей учебы!
Around half of their games aren’t playable in some nations, which puts thedm on par with Bitstarz in terms of their accessible selection.
Also visit my blog post; csv.Cx
купить диплом гознак официально ast-diploms.com .
купить медицинский диплом москва diplomasx.com .
Привет!
Приобрести документ о получении высшего образования вы можете в нашей компании в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы получите диплом по любой специальности, любого года выпуска, включая документы Советского Союза. Гарантируем, что при проверке документа работодателями, каких-либо подозрений не появится.
Наша компания предлагает максимально быстро купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями официальных лиц. Диплом способен пройти лубую проверку, даже с использованием профессионального оборудования. Решите свои задачи быстро с нашими дипломами.
Где приобрести диплом специалиста?
http://slavsbyt.ru/index.php?subaction=userinfo&user=ytukih
https://webmoney.forumkz.ru/viewtopic.php?id=2764#p7865
https://www.mkbox.ru/communication/forum/user/73729/
https://ratingforex.ru/forum-forex/viewtopic.php?f=18&t=35616&sid=f68caf2cc1c72d393fe7b0bd77673496
https://vk.com/club16132629?w=wall-16132629_3527
Удачи!
virgo season charles martin movieyou are like papa episodeteen titans movie live actionclassic martial arts movies
Five tickets matched alll 5 numbers except
for the Powerball worth $1million.
my web site …https://housesofindustry.org
купить диплом трту 2000 г в таганроге http://diploms-x.com/ .
Vivez les programmes suisses comme jamais vue avec notre offre IPTV de haute qualité !
Accédez librement aux chaînes suisses populaires comme RTS, la SRF, la RSI et bien d’autres. Notre plateforme offre :
Plus de 100 chaînes suisses et internationales en HD
Un sélection VOD riche en contenu vidéo
La option de regarder vos émissions préférées en différé
Une interface facile d’utilisation compatible avec de nombreux appareils
Un support client dynamique situé en Suisse
Que vous soyez passionné de sport, de nouvelles ou de spectacles, notre offre IPTV
JS Bin Output s’adapte à vos besoins. Testez gratuitement pendant une journée et découvrez une méthode révolutionnaire pour regarder la TV !
диплом проведенный купить ast-diploms.com .
купить диплом косметолога государственного образца diplomasx.com .
Легальная покупка школьного аттестата с упрощенной программой обучения
Здравствуйте!
Приобрести диплом университета
Наши специалисты предлагают быстро заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями должностных лиц. Диплом способен пройти лубую проверку, даже при использовании специальных приборов. Достигайте своих целей быстро и просто с нашим сервисом.
Где купить диплом по актуальной специальности?
Официальная покупка диплома вуза с сокращенной программой в Москве
диплом о высшем образовании с занесением в реестр стоимость asxdiplomik.com/kupit-diplom-moskva .
купить новый диплом купить новый диплом .
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в армавире, купить диплом ссср, купить диплом судоводителя, купить диплом в шадринске, купить диплом биолога, потом про дипломы вузов, подробнее здесь http://autoprajs.ru/15299.html
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Удачи!
Resources eth etf news
Добро пожаловать на наш сайт! Откройте лучшие финансовые решения прямо сейчас!
Наши предложения
Мы предлагаем широкий ассортимент финансовых продуктов: кредиты, банковские карты и займы, чтобы помочь вам достичь ваших целей и воплотить мечты в реальность.
кредитные карты банков
Кредиты для всех нужд
Планируете покупку жилья, автомобиля или образование? Наши кредитные программы созданы для вас. Оформите кредит на нашем сайте за несколько минут, выбрав лучшие условия и сроки погашения.
Преимущества наших банковских карт
Наши карты обеспечивают удобство безналичных платежей и множество бонусов:
– **Кэшбэк и скидки у партнеров**
– **Программа лояльности**
Оформите карту онлайн и получите все преимущества уже сегодня!
Быстрые займы для непредвиденных расходов
Нужны деньги до зарплаты или на неожиданные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок.
Наши преимущества:
– **Простота и Удобство:** Оформите заявку онлайн за считанные минуты.
– **Надежность и Прозрачность:** Честные условия без скрытых комиссий.
– **Индивидуальный Подход:** Мы учитываем ваши личные обстоятельства.
Не упустите шанс улучшить свою финансовую ситуацию! Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
оформить дебетовую карту
Переходите на наш сайт и сделайте шаг к своим мечтам!
Блэкспрут – Bs2site.at, Bs2site2
Привет!
Купить диплом ВУЗа
Наши специалисты предлагают выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Данный диплом пройдет любые проверки, даже при использовании профессиональных приборов. Решите свои задачи быстро с нашими дипломами.
Где заказать диплом специалиста?
http://vatrusha.maxbb.ru/viewtopic.php?f=2&t=692
Поможем вам всегда!.
Как оказалось, купить диплом кандидата наук не так уж и сложно
use this link Atomic wallet
Покупка диплома о среднем полном образовании: как избежать мошенничества?
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: где купить атестат об окончании школы, купить диплом в томске, купить диплом в шахтах, купить диплом машиниста, купить диплом строителя и получил базовые знания. В итоге остановился на материале: http://forum.jeep-club.by/index.php?/blog/43/entry-3012-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B2%D0%BE%D0%BB%D0%B3%D0%BE%D0%B3%D1%80%D0%B0%D0%B4%D0%B5/
Успешной учебы!
можно ли купить диплом мгу можно ли купить диплом мгу .
Добрый день!
Заказать диплом о высшем образовании
Мы предлагаем выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Документ пройдет любые проверки, даже с использованием специфических приборов. Решайте свои задачи быстро и просто с нашими дипломами.
Где приобрести диплом специалиста?
Официальная покупка диплома вуза с сокращенной программой в Москве
Привет!
Заказать диплом о высшем образовании
Мы предлагаем быстро и выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Документ способен пройти лубую проверку, даже при помощи специфических приборов. Решайте свои задачи максимально быстро с нашими дипломами.
Где заказать диплом по необходимой специальности?
Как оказалось, купить диплом кандидата наук не так уж и сложно
купить диплом в химках diplomyx.com .
можно купить красный диплом asxdiplomik.com/kupit-diplom-moskva .
можно ли купить настоящий диплом о высшем образовании asxdiplomik.com/kupit-diplom-moskva .
GTA IV скачать бесплатно – бесплатные игры 2023, скачать торрент игры
published here avax walletsаааааа
Привет, друзья!
Купить документ о получении высшего образования вы можете у нас. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что при проверке документов работодателями, подозрений не возникнет.
Мы предлагаем быстро и выгодно приобрести диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Наш документ пройдет лубую проверку, даже с использованием профессиональных приборов. Решите свои задачи быстро с нашими дипломами.
Где купить диплом по необходимой специальности?
http://www.pandora.ukrbb.net/viewtopic.php?f=2&t=8550
http://forummsk.getbb.ru/viewtopic.php?f=11&t=2163
http://smol-sport22.ru/index.php?subaction=userinfo&user=ajivus
http://cobaki.ru/users.php?m=details&id=90788
https://smetdlysmet.ru/forum/viewtopic.php?f=8&t=41807
Успешной учебы!
купить диплом высшего технического образования http://www.diploms-x.com/ .
basics [url=https://eth-etf.net/]coingecko ethetf[/url]
нажмите электрик томск
Добрый день!
Где приобрести диплом по необходимой специальности?
Готовый диплом с необходимыми печатями и подписями полностью отвечает стандартам, неотличим от оригинала.
Купить диплом любого ВУЗа.
https://deviva.ru/viewtopic.php?id=9093#p62027
https://aubameyangclub.com/read-blog/1651
https://telegra.ph/Legkij-vybor-magazina-chto-prodaet-diplomy-07-08
https://sonnick84.get-blogging.com/28733488/%D0%A7%D1%82%D0%BE-%D0%BF%D0%BE%D0%BD%D0%B0%D0%B4%D0%BE%D0%B1%D0%B8%D1%82%D1%81%D1%8F-%D0%B4%D0%BB%D1%8F-%D0%B8%D0%B7%D0%B3%D0%BE%D1%82%D0%BE%D0%B2%D0%BB%D0%B5%D0%BD%D0%B8%D1%8F-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D0%BE%D0%B3%D0%BE-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B8%D0%BD%D1%81%D1%82%D0%B8%D1%82%D1%83%D1%82%D0%B0
https://sonnick84.blogrenanda.com/34128673/%D0%9D%D0%B0-%D1%87%D1%82%D0%BE-%D0%B8%D0%BC%D0%B5%D0%BD%D0%BD%D0%BE-%D0%B2%D0%BD%D0%B8%D0%BC%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BE%D0%B1%D1%80%D0%B0%D1%89%D0%B0%D1%82%D1%8C-%D0%BF%D1%80%D0%B8-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
аттестат о среднем образовании 10 классов купить ast-diploms.com .
Привет, друзья!
Где купить диплом по актуальной специальности?
Мы можем предложить дипломы любой профессии по доступным тарифам.
http://www.bigcosmic.com/board/f/board.cgi?id=brandbbs&start=5
купить диплом московского педагогического училища 16 diplomasx.com .
Хотите быть в курсе всех новостей строительной индустрии? FreshHomes.ru — это ваш надежный источник свежей информации о строительстве, архитектуре и недвижимости.
Что мы предлагаем?
Актуальные новости: Будьте в курсе последних событий и тенденций в строительной отрасли.
Глубокая аналитика: Экспертные мнения и подробные обзоры помогут вам разобраться в сложных вопросах.
Полезные советы: Найдите практические рекомендации по ремонту, дизайну интерьера и управлению недвижимостью.
Интересные интервью: Узнайте мнение ведущих профессионалов отрасли.
Посетите FreshHomes.ru и подпишитесь на обновления
новости недвижимости россии
Не упустите возможность получать самые важные и полезные новости прямо на вашу почту. Подпишитесь на наш сайт и станьте частью сообщества профессионалов строительной индустрии.
Присоединяйтесь к нашему Телеграм-каналу Строительный портал по ссылке https://t.me/+Btp6XdoZouA4ZDIy и оставайтесь в центре событий
купить диплом победителя олимпиады diploms-x.com .
Москва работа, подработка, ежедневная оплата.
https://chat.whatsapp.com/GzH4KtsMu2aEChLTOiLMAM
Как официально купить аттестат 11 класса с упрощенным обучением в Москве
lolipopnews.ru/vash-idealnyiy-diplom-byistro-i-legko
Привет, друзья!
Где купить диплом специалиста?
Мы изготавливаем дипломы любой профессии по приятным ценам.
reguitti.com.ua/services.html
можно ли купить диплом медсестры можно ли купить диплом медсестры .
ขอบคุณสำหรับบทความที่น่าดึงดูดนี้!
ผมขอเสนอแนะ เว็บตรงสล็อตไม่ผ่านเอเย่นต์ เพิ่มขอรับ เป็นslot เว็บตรง มีระบบระเบียบระบบฝากถอนAUTOที่สะดวกมากมายๆฝาก-ถอนไม่มีขั้นต่ำ แถมยังใช้เทคโนโลยีการเข้ารหัส SSL เพื่อความปลอดภัยในการทำธุรกรรม ข้อดีอีกอย่างคือเกมสล็อตไม่ผ่านเอเย่นต์จากผู้พัฒนาชั้นนำเยอะมาก เล่นแล้วรู้สึกปลอดภัยรวมทั้งได้รับความเป็นธรรม ทดลองเข้าไปดูเพิ่มเติมอีกพอดี เว็บสล็อตตรง ครับ
Привет, друзья!
Где купить диплом по необходимой специальности?
Купить документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по производству и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы образца СССР. Гарантируем, что в случае проверки документа работодателем, подозрений не появится.
http://nebumed.ru/blog/grafik-raboty/#comment_162372
Удачи!
Добрый день!
Где заказать диплом специалиста?
Полученный диплом с необходимыми печатями и подписями 100% отвечает стандартам Министерства образования и науки, неотличим от оригинала.
Купить диплом ВУЗа.
http://naturetour.ru/club/user/19/blog/1612/
http://www.ladymystery.ru/forum/topic.asp?TOPIC_ID=9523
http://demo.advised360.com/read-blog/161732
https://inopl.com/blogs/1139/%D0%9B%D0%B5%D0%B3%D0%BA%D0%B8%D0%B9-%D0%BF%D0%BE%D0%B8%D1%81%D0%BA-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B0-%D1%87%D1%82%D0%BE-%D1%80%D0%B5%D0%B0%D0%BB%D0%B8%D0%B7%D1%83%D0%B5%D1%82-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B
https://connect.nteep.org/blogs/2533/%D0%A0%D0%B5%D0%BA%D0%BE%D0%BC%D0%B5%D0%BD%D0%B4%D0%B0%D1%86%D0%B8%D0%B8-%D1%8D%D0%BA%D1%81%D0%BF%D0%B5%D1%80%D1%82%D0%B0-%D1%87%D1%82%D0%BE-%D0%BF%D0%BE%D0%BC%D0%BE%D0%B3%D1%83%D1%82-%D0%BB%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B
Добрый день!
Приобрести диплом о высшем образовании.
Наша компания предлагает приобрести диплом в высочайшем качестве, неотличимый от оригинального документа без участия специалистов высокой квалификации со специальным оборудованием.
Где заказать диплом специалиста?
http://fyndamenti.ru/profile.php?u=iwoseve
Удачи!
Привет!
Где заказать диплом специалиста?
Мы предлагаем дипломы любой профессии по невысоким тарифам.
poltavagok.ru/page/19/
Защитите свои данные с помощью резидентских прокси, использовать этим инструментом.
Как работают резидентские прокси?, прочитайте подробностями.
Как выбрать лучший резидентский прокси, рекомендации для пользователей.
Зачем нужны резидентские прокси?, узнайте возможностями.
Почему резидентские прокси безопасны?, анализ функций безопасности.
Как резидентские прокси защищают от опасностей?, разберем важные аспекты.
Как резидентский прокси помогает повысить эффективность?, сравним основные плюсы.
Секреты увеличения скорости с резидентским прокси, советы для оптимизации работы.
Зачем использовать резидентский прокси для сбора информации?, обзор возможностей для парсеров.
Секреты анонимности с резидентским прокси, практические шаги к безопасности онлайн.
Секреты эффективной работы в соцсетях с резидентским прокси, практические советы функционала.
Зачем арендовать резидентские прокси и какие бонусы?, проанализируем лучшие варианты.
Как использовать резидентские прокси для защиты от DDoS-атак, анализируем меры безопасности.
Почему резидентские прокси пользуются популярностью, проанализируем основные факторы.
Сравнение резидентских и дата-центровых прокси, советы для выбора.
proxy резидентские https://rezidentnieproksi.ru/ .
как купить диплом в москве ast-diplomas.com .
visit this website Tor browser
Привет всем)
Хорошо быть студентом, пока не придет пора писать диплом, что и произошло со мной, но не стоит отчаиваться, ведь есть хорошие компании что помогают с написанием и сдачей диплома на хорошие оценки!
Изначально искал информацию про купить диплом в красноярске, купить диплом отзывы, купить аттестат за 11 класс, купить диплом швеи, купить диплом в кемерово, потом попал на http://xn--b1acebaenad0ccc3aiee.xn--p1ai/forum/user/6216/ и там решили все мои учебные заботы!
Хорошей учебы!
Легальные способы покупки диплома о среднем полном образовании
comedyforme.ru/bezopasnoe-priobretenie-diploma-onlayn
Полезные советы по безопасной покупке диплома о высшем образовании
onlinekinospace.ru/diplomyi-lyubyih-spetsialnostey-na-zakaz
https://karimmassimov.com/
mounjaro – тирзепатид инструкция +по применению купить, mounjaro купить
A King Encore Dream Bed anchors the largest common hotel area in New England.
My web-site ::read More
купить диплом музыкальной школы ast-diplomas.com .
моунжаро купить +в москве – mounjaro 5, mounjaro купить +в москве
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом в новом уренгое, купить диплом бакалавра, купить диплом эколога, купить диплом в междуреченске, купить диплом в абакане, потом про дипломы вузов, подробнее здесь http://lit-book.ru/index.php?subaction=userinfo&user=ytovozy
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Хорошей учебы!
Привет, друзья!
Купить документ о получении высшего образования вы можете в нашем сервисе. Мы предлагаем документы об окончании любых университетов Российской Федерации.
Наша компания предлагает быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Диплом способен пройти лубую проверку, даже с применением профессиональных приборов.
http://kochtagebuch.org/doku.php?id=russianydiplomix
http://dobrknigi.ru/howto/?PAGE_NAME=profile_view&UID=26184
http://xn--80aeh5aeeb3a7a4f.xn--p1ai/forum/user/51653/
http://www.fromearth.kr/bbs/board.php?bo_table=free&wr_id=447983
http://mydnepr.pp.ua/forum/topic.php?forum=7&topic=935
Добрый день!
Заказать диплом любого ВУЗа
Мы предлагаем выгодно заказать диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями. Диплом пройдет лубую проверку, даже с применением специфических приборов. Решайте свои задачи максимально быстро с нашим сервисом.
Где приобрести диплом по актуальной специальности?
mosday.getbb.ru/viewtopic.php?f=12&t=1059
3drus.ru/forum/topic_34806
alanyatoday.ru/users/76
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
vip.9bb.ru/viewtopic.php?id=5959#p9901
тирзепатид инструкция +по применению цена – тирзепатид купить, манджаро тирзепатид отзывы
Добрый день!
Как не попасть впросак при покупке диплома колледжа или ПТУ в России
returnrp.listbb.ru/ucp.php?mode=login&sid=0fc9d6deec6d8dc2ff70e299e037113b
Окажем помощь!.
Buy Cloned Cards Shop Cloned cards
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $ 500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://sale-cloned-cards.link
Всем привет)
Будучи студентом, я наслаждался учебой до тех пор, пока не пришло время писать диплом. Но паниковать не стоило, ведь существуют компании, которые помогают с написанием и защитой диплома на отличные оценки!
Изначально я искал информацию по теме: купить диплом в петропавловске-камчатском, купить диплом в майкопе, купить диплом юриста, купить диплом электрика, купить диплом электромонтера, затем наткнулся на http://fabnews.ru/blog/7183.html, где все мои учебные вопросы были решены!
Хорошей учебы!
Привет!
Где купить диплом по актуальной специальности?
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями. Диплом пройдет лубую проверку, даже при помощи специально предназначенного оборудования. Решайте свои задачи быстро и просто с нашими дипломами.
Приобрести диплом любого ВУЗа.
https://linkmate.mn.co/posts/61828981
https://lookeify.com/read-blog/7156
https://conectta2.com/read-blog/907
https://kvixi.com/blogs/1367/%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5
https://www.highpriceddatinguk.com/read-blog/2353
Привет, друзья!
Приобрести диплом о высшем образовании.
Наш сервис предлагает купить диплом высочайшего качества, неотличимый от оригинала без использования дорогостоящего оборудования и опытного специалиста.
Где приобрести диплом по необходимой специальности?
https://d.mwoff.org/index.php?/topic/48-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-u481e/
Успехов в учебе!
купить диплом вуза государственного образца купить диплом вуза государственного образца .
Добрый день!
Рекомендации по безопасной покупке диплома о высшем образовании
itisenglish.maxbb.ru/viewtopic.php?f=7&t=1065
Поможем вам всегда!.
Odds of a grand prize victory are estimated at 1 in 292
million, according to Powerball Winners officials.
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: купить диплом в сургуте, купить аттестаты за 11, купить диплом в кемерово, купить аттестаты за 11, купить диплом в калининграде. Постепенно углубляясь, нашел отличный ресурс здесь: http://sims-game.com/index.php?subaction=userinfo&user=izotony, и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успешной учебы!
Здравствуйте!
Где купить диплом специалиста?
Мы изготавливаем дипломы любых профессий по выгодным ценам.
crosspromote.click/index.php?do=/public/user/blogs/name_Alanpoe/page_7/
Охраняйте свою конфиденциальность с резидентскими прокси, как это работает.
Смотрите зарубежные сериалы с резидентскими прокси, широким контентом.
Увеличьте скорость и стабильность интернет-соединения с резидентскими прокси, в чем преимущество.
Скройте свой реальный IP-адрес от хакеров с резидентскими прокси, и чувствуйте себя спокойно.
Защитите свою личную жизнь и данные с резидентскими прокси, и чувствуйте себя невидимкой.
Используйте резидентские прокси для безопасного серфинга в интернете, и не бойтесь за свою приватность.
качественные резидентские прокси https://rezidentnie-proksi.ru/ .
Здравствуйте!
Заказать диплом любого университета
Наша компания предлагает быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями. Диплом пройдет любые проверки, даже с использованием специфических приборов. Достигайте своих целей быстро с нашей компанией.
Где купить диплом по нужной специальности?
ilovehabbo.bbon.ru/viewtopic.php?id=1459#p28856
mkpnz.ru/users/8
mosday.getbb.ru/viewtopic.php?f=12&t=1059
ilovehabbo.bbon.ru/viewtopic.php?id=1459#p28856
forum.qwas.ru/kupit-diplom-t19852.html
Привет, друзья!
Купить диплом любого ВУЗа
Наши специалисты предлагают выгодно и быстро купить диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Диплом способен пройти лубую проверку, даже с использованием специально предназначенного оборудования. Достигайте своих целей быстро с нашей компанией.
Где купить диплом специалиста?
forumkk.listbb.ru/viewtopic.php?f=12&t=392
driveme.rusff.me/viewtopic.php?id=2115#p105171
malispa.ru/users/122
alik.forumrpg.ru/viewtopic.php?id=6639#p275762
forumkk.listbb.ru/viewtopic.php?f=12&t=392
Привет, друзья!
Как не попасть впросак при покупке диплома колледжа или ПТУ в России
sciencenewhop.maxbb.ru/viewtopic.php?f=44&t=761
Рады помочь!.
Добрый день!
Купить документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации.
Мы предлагаем максимально быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Данный диплом способен пройти лубую проверку, даже при помощи специально предназначенного оборудования.
“http://o98065hq.bget.ru/index.php?action=profile;u=395115”
http://dayz.tselik.ru/profile.php?action=show&member=10416
“http://www.fsh.mi.th/newswb3/index.php?action=profile;u=67511”
http://school5.p-fam.ru/users/apemov
https://vadaszapro.eu/user/profile/1271282
## Discover the Best Fiverr Gigs to Boost Your Business
In the ever-evolving digital landscape, finding the right resources to
enhance your business can be a game-changer.
Whether you’re an entrepreneur, a small business owner, or a
freelancer, leveraging the power of Fiverr can help you achieve your goals more efficiently.
Fiverr, the world’s largest marketplace for digital
services, offers a plethora of gigs that cater to various needs.
From graphic design to SEO optimization, there’s something for everyone.
Let’s dive into the best Fiverr gigs that can take your business to
the next level.
### 1. Stunning Logo Design
Your logo is the face of your brand, and having a professionally designed logo is crucial for making a
lasting impression. On Fiverr, you can find top-rated logo designers who offer unique and creative designs tailored to
your brand identity. These gigs provide multiple design concepts,
unlimited revisions, and even brand guidelines to ensure
your logo perfectly represents your business.
### 2. Engaging Social Media Content
In today’s digital age, a strong social media presence is essential for any
business. Fiverr offers a range of gigs that specialize in creating engaging content for platforms like
Instagram, Facebook, and Twitter. From eye-catching graphics to compelling captions, these gigs can help you maintain a consistent and appealing social media feed that attracts and retains
followers.
### 3. SEO Optimization
Search engine optimization (SEO) is a critical component of online success.
Fiverr’s SEO experts can analyze your website, identify
areas for improvement, and implement strategies to boost
your search engine rankings. Whether you need keyword research, on-page optimization, or backlink
building, these gigs can significantly enhance your online visibility and drive organic traffic
to your site.
### 4. Professional Video Editing
Video content is king in the digital marketing world.
Fiverr hosts a variety of skilled video editors who can transform your raw footage into polished, professional videos.
Whether you need promotional videos, explainer videos, or social
media clips, these gigs offer high-quality editing, special effects,
and animation services to captivate your audience.
### 5. Compelling Copywriting
Effective communication is key to converting visitors into customers.
Fiverr’s copywriters specialize in crafting
compelling and persuasive content that resonates with your
target audience. From website copy and blog posts to product
descriptions and email campaigns, these gigs can help you convey your message clearly and convincingly,
boosting your brand’s credibility and sales.
### 6. Custom Website Development
A well-designed website is the cornerstone of your online presence.
Fiverr’s web developers offer custom website design and development services to create
a site that’s not only visually appealing but also user-friendly and responsive.
Whether you need an e-commerce site, a personal blog, or a
corporate website, these gigs provide comprehensive solutions tailored to your specific
requirements.
### 7. Effective Digital Marketing
Fiverr is home to numerous digital marketing experts who
can devise and execute marketing strategies to grow
your business. From PPC advertising and social media marketing to email campaigns
and influencer outreach, these gigs offer a range of services to enhance your brand’s online presence and drive
targeted traffic to your website.
### 8. Innovative Graphic Design
Beyond logo design, Fiverr offers a myriad of graphic design services to meet
all your branding needs. Whether you need business cards, brochures, infographics, or banners,
these gigs provide innovative and professional designs that
make your brand stand out. High-quality visuals can significantly impact your marketing efforts,
and Fiverr’s designers are equipped to deliver exceptional results.
### 9. Reliable Virtual Assistance
Managing a business involves juggling multiple tasks,
and sometimes you need an extra pair of hands. Fiverr’s virtual assistants offer
a range of services, including administrative support, customer service,
data entry, and project management. These gigs can help you
streamline your operations and focus on the core aspects of your business.
### 10. Comprehensive Branding Services
If you’re looking to build a cohesive brand identity,
Fiverr’s branding experts can help. These gigs offer comprehensive
branding packages that include logo design, brand strategy, messaging,
and visual identity development. A strong brand can set you apart from the competition, and Fiverr’s professionals are adept at creating memorable and
impactful brand experiences.
### Conclusion
Fiverr is a treasure trove of services that can propel your business forward.
By leveraging the best Fiverr gigs, you can access top-tier talent
and expertise at affordable prices, allowing you to focus on what you do best.
Whether you need design, marketing, content creation, or technical support, Fiverr’s
marketplace has you covered. Start exploring today and unlock the full potential of your business with the best
Fiverr gigs available.
Here is my homepage – “http://unnewsusa.com/bbs/board.php?bo_table=free&wr_id=2387218”
Полезные советы по покупке диплома о высшем образовании без риска
pvlt788fz.bloggactif.com/28948850/%D0%A0%D0%B5%D1%88%D0%B8%D0%BB%D0%B8-%D1%83%D0%B7%D0%BD%D0%B0%D1%82%D1%8C-%D0%BA%D0%B0%D0%BA-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%96%D0%B4%D0%B5%D0%BC-%D0%92%D0%B0%D1%81
Embark on a new journey through the particular exquisite beauty associated with mature women throughout their most romantic and vulnerable occasions with our collection of free porno photos. Witness the allure and style regarding older girls that have gracefully aged, showcasing their charm such as never before. Involve yourself in typically the realm of Mature Lesbian Group Strapon Pics fantasies and indulge in the fascinating snapshots captured by simply these seasoned seductresses as they uncovered all this for your unrestrained and zealous desires to see in these XXX images! Designed specifically to your pleasure.
At https://www.mature-naked.com, we are skilled in showcasing the raw, unfiltered love of experienced ladies who know precisely how you can satisfy. These kinds of ageless vixens usually are bursting with desire in addition to aren’t afraid to show it. Each of our galleries are filled using jaw-dropping images of MILFs and cougars who have mastered the art involving seduction, turning every encounter into a great unforgettable spectacle. Through intense, hardcore bone to intimate, sensuous moments, these older bombshells will consider you over a fascinating ride through their particular deepest, most direct fantasies.
check this link right here now zip rar
In case you’re in the particular mood for some sort of captivating assortment of sexual pictures showcasing elegant, older women throughout their most prone state, look simply no further. This collection is overflowing with exciting images of mature women radiating style and mature women pics. Acquire ready to always be transported into a new world of mesmerizing nude portraits that could surely leave you craving more.
Покупка диплома о среднем полном образовании: как избежать мошенничества?
l90226mw.beget.tech/2024/07/08/diplomy-attestaty-i-spravki-v-luchshem-magazine.html
Привет, друзья!
Купить диплом университета
Наши специалисты предлагают выгодно и быстро купить диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями должностных лиц. Данный документ способен пройти любые проверки, даже при помощи профессиональных приборов. Достигайте своих целей быстро с нашим сервисом.
Где купить диплом по нужной специальности?
klinlife.ru/forums/index.php?/topic/38850-kupit-diplom-vse-chto-vam-nuzhno-znat/
http://www.odnopolchane.net/forum/member.php?u=546804
panther.80lvl.ru/index.php
ramantungal.in/social/blogs/2/%D0%9F%D1%80%D0%BE%D1%87%D0%B8%D1%82%D0%B0%D0%B9%D1%82%D0%B5-%D0%BD%D0%B0%D1%88-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80-%D0%B5%D1%81%D0%BB%D0%B8-%D0%BD%D0%B0%D0%B4%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
wiki.astrakhan.pro/index.php/%D0%A2%D0%B5%D1%85%D0%BD%D0%B8%D1%87%D0%B5%D1%81%D0%BA%D0%B0%D1%8F_%D0%BF%D0%BE%D0%B4%D0%B4%D0%B5%D1%80%D0%B6%D0%BA%D0%B0_%D0%B8_FAQ._%D0%97%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC_%D0%B2_%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Place your bet at pin up online – very prestigious bookmaker in Kazakhstan
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Добро пожаловать на наш сайт – ваше решение для всех финансовых потребностей!
Мы предлагаем различные финансовые продукты: кредиты, банковские карты и займы, чтобы помочь вам достигнуть ваших целей и осуществить мечты.
оформить кредитную карту
Идеальные кредиты для ваших нужд
Нуждаетесь в финансировании на покупку жилья, автомобиля или образование? Наши кредитные программы разработаны с учетом ваших потребностей. Оформите кредит на нашем сайте, выбрав подходящие условия и сроки погашения.
Преимущества наших банковских карт
Наши банковские карты предоставляют:
Удобство безналичных платежей
Бонусы и привилегии
Оформите карту на нашем сайте и получайте кэшбэк, скидки у партнеров и участие в программе лояльности. Выберите карту с оптимальными лимитами и условиями обслуживания для себя.
Быстрые и удобные займы
Нужны деньги до зарплаты или на непредвиденные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок, чтобы вы могли решать финансовые вопросы без задержек.
займы
Наши преимущества:
Простота и Удобство: Оформите заявку онлайн за несколько минут.
Надежность и Прозрачность: Мы гарантируем честные условия и отсутствие скрытых комиссий.
Индивидуальный Подход: Мы учитываем ваши личные обстоятельства и предлагаем оптимальные условия.
Не упустите возможность улучшить свою финансовую ситуацию! Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
С нами ваши мечты станут реальностью!
mounjaro 5 – тренировки +для похудения, ozempic 1 mg купить
купить официальный диплом о среднем ast-diplomas.com .
browse around this web-site Rufus
click for info jaxx io
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков
alik.forumrpg.ru/viewtopic.php?id=6859#p276097
Ставки на спорт с высокими коэффициентами | 1win радует своих клиентов | 1win предлагает многочисленные варианты для победы | Будь успешным с 1win| 1win помогает воплотить мечты в реальность| Ставки с 1win – это просто и увлекательно| 1win предлагает лучшие условия для игры| 1win – путь к финансовой независимости| 1win поможет вам стать чемпионом| 1win всегда поддерживает своих игроков
1win скачать 1win скачать .
Addressing the balance in wind tunnel fans for aerospace testing was critical for accurate data collection. Vibromera’s solutions made a significant impact. Learn more on their website https://vibromera.eu/example/about-the-experience-of-balancing-the-cardan-shaft-directly-on-the-motor-grader/
Привет всем)
Студенческая жизнь прекрасна, пока не приходит время писать диплом, как это случилось со мной. Не стоит отчаиваться, ведь существуют компании, которые помогают с написанием и защитой диплома на высокие оценки!
Сначала я искал информацию по теме: купить диплом биолога, купить диплом в ельце, купить диплом в перми, купить диплом менеджера по туризму, купить диплом в буденновске, а потом наткнулся на http://army.clanfm.ru/viewtopic.php?f=2&t=38201&p=53235#p53235, где все мои учебные проблемы были решены!
Хорошей учебы!
Здравствуйте!
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
toursoul.ru/?p=19214
Будем рады вам помочь!.
Согласование перепланировки в здании в Москве — это настоящее испытание для тех, кто любит острые ощущения. Хотите почувствовать себя героем квеста? Тогда вам точно к нам!
Мы с радостью возьмем на себя все сложности этого увлекательного процесса. Наша команда профессионалов поможет вам пройти все этапы и получить заветные разрешения. Ведь кто еще, как не мы, знает, как сделать бюрократию чуть более «дружелюбной»?
тирзепатид инструкция – оземпик доза, оземпик +для похудения отзывы
Добрый день!
Мы предлагаем дипломы любой профессии по приятным ценам. Цена может зависеть от той или иной специальности, года получения и ВУЗа.
Где купить диплом по нужной специальности?
Купить диплом ВУЗа
https://landik-diploms-srednee.ru/svidetelstvo-o-razvode
Удачи!
TГ©cnicas avanzadas de equilibrado Balancing Techniques para trituradoras robustas
как писать автореферат – напишу диссертацию, написание курсовых работ отзывы
https://epicads.net/
диплом купить образец в москве https://diploms-x.com/ .
http://buy-cloned-cards.net
Item 01 Card Total Balance: $3100 – Price $ 110.00
Item 03 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
Store Hacked paypal Shop Hacked card
мунжаро +как принимать – препарат оземпик цена, mounjaro тирзепатид купить +в москве
Привет!
Где приобрести диплом по актуальной специальности?
Мы изготавливаем дипломы любой профессии по доступным ценам.
istoriya-kino.ru/kinematograf/alph0015.shtml
1win – ваш идеальный партнер для ставок
1win делает ваши ставки легкими и прибыльными
Завоюйте свою удачу вместе с 1win
Успех начинается с 1win
1win – ваш путь к большим выигрышам
1win – ваша дверь в мир азарта и выигрышей
Ставки на спорт с 1win – высокие коэффициенты и увлекательные матчи
1win – выбор тех, кто ценит качество и надежность
Победы становятся легко доступными с 1win
1win – это бесконечные возможности для выигрышей
Сделайте свою жизнь ярче с 1win
Присоединяйтесь к миллионам победителей на платформе 1win
Ставки на спорт становятся простыми с 1win
1win делает ставки доступными для всех|1win – это ваш шанс на выигрыш
1win – ваш путь к большим выигрышам|Увлекательные ставки и азартные игры на платформе 1win|1win делает вашу игру интересной и прибыльной|1win – ваш проводник в мире ставок и азарта|Играйте и выигрывайте с 1win|1win – это ваш персональный билет в мир азарта|1win – букмекер, на которого можно положиться|1win – это ваш лучший друг в мире ставок|1win делает вашу игру более прибыльной и интересной|1win гарантирует вам только успешные ставки|1win – это ваш ключ к финансовой независимости|1win – это ваша возможность изменить свою жизнь|1win – это ваш ключ к финансовой стабильности|Сделайте свои ставки более увлекательными с 1win|1win гарантирует вам только выигрышные ставки|1win – лучший выбор для начинающих и профессионалов|Присоединяйтесь к лидерам ставок на 1win|1win – ваша дверь в мир ставок и азарта
1win официальный сайт 1win официальный сайт .
Откройте Новые Финансовые Возможности!
Что мы предлагаем?
Мы предоставляем вам лучшие финансовые продукты, включая кредиты, банковские карты и займы. Наши решения помогут вам достигнуть любых целей и воплотить мечты в реальность.
Банковская карта для детей
Финансовые Решения для Любых Целей
Планируете покупку жилья, автомобиля или образование? Наши кредитные программы идеально подойдут для ваших нужд. Оформите кредит на нашем сайте и получите выгодные условия и удобные сроки погашения.
Преимущества наших Банковских Карт
Наши банковские карты предлагают:
– Удобство безналичных расчетов
– Щедрые бонусы и привилегии
Оформите карту онлайн и получите кэшбэк, скидки у партнеров и участие в программе лояльности. Найдите карту с оптимальными лимитами и условиями обслуживания именно для вас.
Быстрые Займы на Любые Нужды
Не хватает денег до зарплаты или на неожиданные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок, чтобы вы могли решать финансовые вопросы без задержек.
Наши Преимущества:
– **Простота и Удобство**: Оформите заявку онлайн за считанные минуты.
– **Надежность и Прозрачность**: Честные условия и отсутствие скрытых комиссий.
– **Индивидуальный Подход**: Мы учитываем ваши личные обстоятельства и предлагаем оптимальные условия.
Не упустите шанс улучшить свою финансовую ситуацию! Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и почувствуйте все преимущества работы с надежным финансовым партнером.
Снятие наличных с дебетовой карты
С нами ваши мечты станут реальностью!
https://karimmassimov.com/
karimmassimov.com b1fb65d
https://karimmassimov.com/
karimmassimov.com fee0b6b
купить диплом дефектолога diploms-x.com .
На сайте http://nemans.ru приобретите фасовочные пакеты, а также тару с ручками, мешки полипропиленовые, пленку полиэтиленовую, армированную, клейкую ленту, стрейч, различную бумажную продукцию, салфетки, тряпки и многое другое. Все товары реализуются по лучшим ценам, доступна оперативная доставка. Вся продукция от проверенных, надежных поставщиков, которые работают на результат. Все товары абсолютно безопасные, простые в использовании и помогают оперативно закончить уборку и не тратить на нее много времени. Регулярно на определенные товары устанавливаются скидки.
https://karimmassimov.com/
karimmassimov.com b65d57a
Good day 🙂
What an fantastic article!
Is it okay I scrape this and share it with
my group members?
My group is about Korean 야동
If you are interested, feel free to come to my blog and have
a look.
Thanks and Keep up the good work!
Привет, друзья!
Где заказать диплом специалиста?
Мы готовы предложить дипломы любой профессии по разумным ценам.
go4pro.ru/gopro/video-s-gopro/gopro-video-iz-razryada-kak-zhe-skuchno-ya-zhivu
Привет!
Заказать диплом ВУЗа.
Наш сервис предлагает приобрести диплом высокого качества, который не отличить от оригинала без использования специального оборудования и квалифицированного специалиста.
Где приобрести диплом специалиста?
https://forum.ora600.ru/viewtopic.php?t=72909
Удачи!
what is a film short southern charm season 8 air datewho won season 3 too hot to handlepurge season 2action movies to watch when bored
Based on the lender you piuck out, you could be capable
to borrow up to the total coost of attendance.
my web page :: 여성대출
Практический опыт в SEO с 2008 г. подтверждается датой регистрации моего блога, в котором я частенько пишу о своем понимании в продвижении сайтов. Внедряю стратегию SEO, учитывая алгоритмы поисковиков и использую свои технические skills для достижения наилучших результатов https://habr.com/ru/users/wlad2/boo
https://karimmassimov.com/
karimmassimov.com 7ad3_55
https://karimmassimov.com/
karimmassimov.com R 6b6942d
Найдите актуальные промокоды Vavada казино и получите дополнительные бонусы для игры. Эти коды предоставляют отличные возможности для любителей азартных игр.
Добрый день!
Заказать диплом ВУЗа
Наша компания предлагает выгодно и быстро купить диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Диплом пройдет лубую проверку, даже с применением специфических приборов. Достигайте свои цели максимально быстро с нашим сервисом.
Где приобрести диплом специалиста?
nedvigimost.bbok.ru/viewtopic.php?id=26650#p45740
mamapoltava.listbb.ru/viewtopic.php?f=39&t=4933
lubercy.ixbb.ru/viewtopic.php?id=6615#p14726
worksale777.blogspot.com/2024/06/blog-post_30.html
vaeaem.profiforum.ru/t3822-topic#7107
Используйте промокоды Drip казино для увеличения вашего игрового баланса. Эти коды предоставляют эксклюзивные бонусы и улучшенные возможности.
Werkzeuge und Techniken für Precision Balancing auf Drehbänken
Сколько стоит диплом высшего и среднего образования и как его получить?
forum.redzmax.ro/index.php?/gallery/image/70-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D1%8B%D0%B9-%D0%BF%D0%BE%D0%B8%D1%81%D0%BA-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B0-%D1%80%D0%B5%D0%B0%D0%BB%D0%B8%D0%B7%D1%83%D1%8E%D1%89%D0%B5%D0%B3%D0%BE-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B/
Здравствуйте!
Заказать диплом о высшем образовании
Наша компания предлагает выгодно и быстро приобрести диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями. Документ пройдет любые проверки, даже при помощи специальных приборов. Решите свои задачи быстро и просто с нашим сервисом.
Где купить диплом специалиста?
usa.life/read-blog/63354
klinlife.ru/forums/index.php?/topic/37385-kupit-diplom-bez-posrednikov-legko-i-bezopasn/
lebanonhub.app/blogs/2398/%D0%97%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%A1%D0%BE%D0%B2%D0%B5%D1%82%D1%8B-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%BE%D0%B2
d91652pj.beget.tech/2024/07/10/pochemu-magaziny-s-diplomami-segodnya-tak-populyarny.html
xn--80aeahbdc6cr3b7h.xn--p1ai/club/user/8729/blog/193091/
Найдите актуальные промокоды Vavada казино и получите дополнительные бонусы для увлекательной игры. Эти коды помогут вам улучшить свои игровые возможности.
Дома под ключ в Ижевске нк18.рф
Обращайтесь к нам за строим дом из керамических блоков на любом этапе застройки. У Вас уже есть участок? Прекрасно, дом мы берем на себя. Определим все нюансы, дадим советы от специалистов по планировке. Участка пока нет? Мы предложим Вам много разных вариантов, которые подойдут определенно под Ваш спрос.
https://karimmassimov.com/
karimmassimov.com b65d57a
How to Identify Imbalance in Lathe Machine Shafts
https://karimmassimov.com/
karimmassimov.com b6942da
Добрый день!
Купить документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России.
Мы предлагаем выгодно приобрести диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ способен пройти лубую проверку, даже с применением специального оборудования.
https://vestiinform.ru/forums/topic/kupit-diplom-e603s/
https://vip-forum.com/threads/kupit-diplom-l491v.1797/
http://polimer42.ru/communication/forum/messages/forum5/topic49/message352075/?result=reply#message352075
https://biowiki.clinomics.com/index.php?title=gosznacdiplomy
http://profelectro.by/index.php?subaction=userinfo&user=ykacyb
Привет, друзья!
Реально ли приобрести диплом стоматолога? Основные шаги
vetstate.ru/forum/?PAGE_NAME=profile_view&UID=126055
Рады оказаться полезными!.
Компания «КИП72» специализируется на производстве и поставке контрольно-измерительных приборов и оборудования для множества отраслей промышленности. Мы предлагаем широкий выбор продукции, включая датчики, анализаторы, измерители. Мы стремимся обеспечить клиентов высококачественными и надёжными приборами для контроля производственных процессов и управления технологическими операциями.
Мы стремимся к постоянному развитию и совершенствованию нашей продукции, а также к расширению партнёрских связей с ведущими производителями и поставщиками оборудования. Мы – магазин, готовый предложить индивидуальные решения для любого клиента.
«КИП72» активно участвует в жизни общества, поддерживая различные социальные и экологические проекты. Если вас интересует наша продукция или услуги, пожалуйста, свяжитесь с нами по контактам, указанным на официальном сайте фирмы https://www.kip72.ru/, мы будем рады ответить на все ваши вопросы и предложить взаимовыгодное сотрудничество.
https://karimmassimov.com/
karimmassimov.com fee0b6b
Las Гєltimas tendencias en Dynamic Balancing exploradas en el blog de Vibromera
купить диплом высшее в омске asxdiplomik.com/kupit-diplom-moskva .
1win – лучший выбор для любителей ставок на спорт, попробовать.
Большой выбор игровых автоматов и карточных игр на 1win, советуем.
Зарабатывайте вместе с 1win и наслаждайтесь выигрышами, заработать большие деньги.
Ставки на киберспорт: лучшие коэффициенты на 1win, присоединиться к онлайн играм.
Играйте безопасно и выигрывайте большие деньги с 1win, советуем.
1win вход https://1win-sayt.by/ .
Привет!
Приобрести диплом любого ВУЗа
Мы предлагаем быстро и выгодно приобрести диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Диплом пройдет лубую проверку, даже с применением специально предназначенного оборудования. Достигайте цели максимально быстро с нашими дипломами.
Где купить диплом по необходимой специальности?
http://www.rrsclub.ru/showthread.php?p=44657#post44657
loolita.es/blogs/4302/%D0%A6%D0%B5%D0%BD%D0%B0-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80-%D0%B8-%D1%81%D0%BE%D0%B2%D0%B5%D1%82%D1%8B-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%BE%D0%B2
http://www.xusyou.com/blogs/286/%D0%93%D0%BB%D0%B0%D0%B2%D0%BD%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%85%D0%BE%D0%B4%D1%8B-%D0%B8%D0%B7%D0%B3%D0%BE%D1%82%D0%BE%D0%B2%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B0%D0%B2%D1%82%D0%BE%D1%80%D1%81%D0%BA%D0%B8%D0%B9-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
moscowurban.getbb.ru/viewtopic.php?f=12&t=1640
ob2qvj3m9.ssnblog.com/27859999/%D0%9F%D1%80%D0%BE%D1%87%D0%B8%D1%82%D0%B0%D0%B9%D1%82%D0%B5-%D0%BD%D0%B0%D1%88-%D0%BC%D0%B0%D1%82%D0%B5%D1%80%D0%B8%D0%B0%D0%BB-%D0%B5%D1%81%D0%BB%D0%B8-%D1%82%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
Как купить аттестат 11 класса с официальным упрощенным обучением в Москве
horordark.ru/bezopasnoe-priobretenie-diploma-onlayn
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: где купить диплом образование, купить диплом о среднем, купить диплом в туапсе, купить диплом учителя физической культуры, купить сертификат специалиста. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://sllife.ru/blog/bargdgng/kupit-diplom-v-krasnodare-/ и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Успехов в учебе!
https://karimmassimov.com/
karimmassimov.com R 942dacc
купить диплом в каменске-шахтинском asxdiplomik.com/kupit-diplom-moskva .
Узнайте стоимость диплома высшего и среднего образования и процесс получения
diplomasx.com/kupit-diplom-sankt-peterburg
офисные кресла expert https://office-mebel-in-msk.ru/
Здравствуйте!
Купить диплом о высшем образовании.
Мы предлагаем купить диплом в отличном качестве, неотличимый от оригинала без участия специалистов высокой квалификации со специальным оборудованием.
Где купить диплом специалиста?
http://globalimport.spb.ru/forum/thread1077.html#1097
Успехов в учебе!
АвтоАтелье Medvedev AutoLab – перетяжка салона, шумоизоляция и тюнинг автомобилей в Екатеринбурге https://detailauto.ru
купить диплом бакалавра в нижнем новгороде asxdiplomik.com/kupit-diplom-moskva .
https://karimmassimov.com/
karimmassimov.com fb65d57
Привет, друзья!
Купить диплом магистра оказалось возможно, быстрое обучение и диплом на руки
moscowurban.getbb.ru/viewtopic.php?f=12&t=1663
Поможем вам всегда!.
Добрый день!
Где приобрести диплом специалиста?
Наша компания предлагает выгодно купить диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями должностных лиц. Наш диплом пройдет любые проверки, даже при использовании профессионального оборудования. Достигайте свои цели быстро и просто с нашим сервисом.
Купить диплом о высшем образовании.
avtolux48.ru/people/user/367/blog/7885/
диплом проведенный купить diplomyx.com .
https://karimmassimov.com/
karimmassimov.com 65d57ad
https://karimmassimov.com/
karimmassimov.com fee0b6b
Привет!
Где приобрести диплом по необходимой специальности?
Приобрести документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите диплом по любой специальности, включая документы Советского Союза.
Где заказать диплом по актуальной специальности?
video.listbb.ru/viewtopic.php?f=3&t=407
Успехов в учебе!
купить диплом в саянске ast-diploms.com .
купить диплом маникюру купить диплом маникюру .
https://karimmassimov.com/
karimmassimov.com R 42dacc5
Здравствуйте!
Купить диплом ВУЗа
Наша компания предлагает быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Диплом способен пройти лубую проверку, даже с использованием специально предназначенного оборудования. Достигайте цели быстро с нашим сервисом.
Где купить диплом по необходимой специальности?
doomelang.com/read-blog/6652
g95334gq.beget.tech/2024/07/06/nastoyaschie-diplomy-bystro-legalno-nadezhno.html
tyachiv.ukraine7.com/login
test.bpal.org/blogs/entry/8398-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B8-%D0%B2%D0%B0%D1%80%D0%B8%D0%B0%D0%BD%D1%82%D1%8B-%D0%B4%D0%BE%D1%81%D1%82%D0%B0%D0%B2%D0%BA%D0%B8-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82/
encontrocentral.com/read-blog/2311
Возможно ли купить диплом стоматолога, и как это происходит
californiarpn2.listbb.ru/viewtopic.php?f=1&t=505
Привет Друзья!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом колледжа, купить диплом агронома, купить диплом техникума, купить диплом инженера строителя, где купить диплом образование, потом про дипломы вузов, подробнее здесь http://alp-proekt.ru/index.php?subaction=userinfo&user=ibunolyp
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Успешной учебы!
Привет!
Приобрести диплом любого ВУЗа
Наша компания предлагает выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями официальных лиц. Диплом способен пройти любые проверки, даже с использованием специально предназначенного оборудования. Решайте свои задачи быстро с нашим сервисом.
Где приобрести диплом специалиста?
goup.hashnode.dev/kupit-diplom-1-1-1
lubercy.ixbb.ru/viewtopic.php?id=6615#p14726
rodina.listbb.ru/viewtopic.php?f=3&t=502
forumkk.listbb.ru/viewtopic.php?f=12&t=392
avtolux48.ru/people/user/374/blog/7556/
Покупка диплома о среднем полном образовании: как избежать мошенничества?
asxdiplomik.com/kupit-diplom-ekaterinbur
Добрый день!
Заказать диплом о высшем образовании
Наши специалисты предлагают быстро и выгодно приобрести диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Документ способен пройти любые проверки, даже с использованием специальных приборов. Решайте свои задачи быстро с нашей компанией.
Где заказать диплом по нужной специальности?
mosday.getbb.ru/viewtopic.php?f=12&t=1059
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
86hm.ru/forum/flame/?topic_id=25002
pdlspd.listbb.ru/viewtopic.php?f=3&t=409
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
Добрый день!
Где приобрести диплом специалиста?
Наша компания предлагает быстро купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Данный документ пройдет любые проверки, даже с использованием специального оборудования. Достигайте цели быстро с нашими дипломами.
Заказать диплом ВУЗа.
beq664af9.blogs-service.com/59385381/%D0%9F%D0%BE%D0%B4%D1%80%D0%BE%D0%B1%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B5%D0%BD%D0%B8%D1%8F-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
куплю диплом цена diplomyx.com .
сколько стоит купить диплом о высшем образовании сколько стоит купить диплом о высшем образовании .
Здравствуйте!
Где приобрести диплом специалиста?
Купить документ о получении высшего образования можно в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить диплом по любой специальности, включая документы СССР.
Где купить диплом по актуальной специальности?
industrial.getbb.ru/viewtopic.php?f=4&t=3093
Успешной учебы!
купить диплом о высшем образовании в челябинске ast-diploms.com .
купить диплом слесаря ремонтника дпо стандарт diplomasx.com .
Здравствуйте!
Вопросы и ответы: можно ли быстро купить диплом старого образца?
behealthy.maxbb.ru/posting.php?mode=post&f=8
Будем рады вам помочь!.
September 18, 2023 • Forr extra than 3 years, no 1 had to pay their federal loan forgiveness Student loans loans.
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков
diplomyx24.ru/kupit-diplom-omsk
Добрый день!
Где приобрести диплом по необходимой специальности?
Наши специалисты предлагают выгодно и быстро заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Наш документ способен пройти лубую проверку, даже с использованием профессионального оборудования. Решайте свои задачи быстро и просто с нашей компанией.
Заказать диплом любого ВУЗа.
ch43pbk98.livebloggs.com/34437801/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
купить медицинский диплом в спб http://www.diploms-x.com .
http://www.NoxProxy.com | High Quality IPv6 Proxy | IPv6 proxy from Residential ISP or Mobile ISP
– Virgin IPv6 Proxy (Private, Dedicated)
– IPv6 Mobile or Residential Proxy
– IPv6 HTTP or Socks5 proxy
– High Speed IPv6 Proxy
– High Quality IPv6 Proxy
– Rotating IPv6 Proxy (Configurable)
– Static IPv6 Proxy (Configurable)
26 Geo Locations available:
Australia – Brisbane
Brazil – Palmas
Canada – Montreal
Colombia – Cali
Djibouti – Djibouti City
France – Lyon
Germany – Munich
Hong Kong – Hong Kong
Hungary – Budapest
India – Mumbai
Indonesia – Jakarta
Japan – Osaka
Malaysia – Kuala Lumpur
Netherlands – Amsterdam
Philippines – Quezon City
Poland – Warsaw
Portugal – Porto
Singapore – Singapore
South Africa – KwaZulu-Natal
Spain – Barcelona
Sweden – Gothenburg
Switzerland – Zurich
Taiwan – Taipei City
United Arab Emirates – Abu Dhabi
United Kingdom – Birmingham
United States – Huntsville
http://www.NoxProxy.com
Telegram: @NoxProxyIPv4IPv6
Привет, друзья!
Купить документ о получении высшего образования вы имеете возможность у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации.
Мы предлагаем выгодно приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями должностных лиц. Документ способен пройти любые проверки, даже с использованием специального оборудования.
http://www.zpu-journal.ru/forum/view_profile.php?UID=307295
https://forum.stde.ru/index.php?/topic/9874-how-to-create-a-new-topic-at-forumstderu/page/6/#comment-11628
http://camillacastro.us/forums/viewtopic.php?pid=415639#p415639
http://farsrig.com/index.php?subaction=userinfo&user=ojojuhesy
http://www.ntsr.info/forum/user/95757/
куплю диплом бывший куплю диплом бывший .
Добрый день!
Где купить диплом специалиста?
Мы готовы предложить дипломы любой профессии по разумным ценам.
http://www.fczulia.com/articulos/4330.html
Здравствуйте!
Где заказать диплом специалиста?
Купить документ института вы имеете возможность в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы СССР.
Где заказать диплом по нужной специальности?
http://www.bideew.com/create-blog/
Успешной учебы!
диплом москва купить ast-diploms.com .
купить диплом о образовании купить диплом о образовании .
купить диплом мединститута купить диплом мединститута .
дипломы цена дипломы цена .
куплю диплом кандидата наук asxdiplomik.com/kupit-diplom-moskva .
Бетонные дома купить в Ижевске нк18.рф
Приходите к нам за одноэтажный дом из газобетона на любом этапе к жизни в своем доме. У Вас уже имеется участок? Прекрасно, дом мы берем на себя. Определим все тонкости, дадим советы от профессионалов по расположению. Участка пока нет? Мы предложим Вам несколько разных вариаций, которые смогут подойти определенно под Ваш спрос.
Согласование перепланировки – важный этап, который необходимо пройти перед началом строительных работ. Наша компания оказывает полный спектр услуг по согласованию перепланировок, начиная с подготовки документов и заканчивая получением всех разрешений.
Обратившись к нам, вы получите профессиональную помощь в вопросах согласование перепланировки. Мы гарантируем точное соблюдение всех норм и требований законодательства, а также быстрое и качественное выполнение всех процедур.
Привет!
Мы предлагаем документы техникумов, которые находятся на территории всей РФ. Можно купить качественно напечатанный диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты делаются на бумаге высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Они будут заверены необходимыми печатями и подписями.
Заказать диплом о высшем образовании.
9213270296.ru/2024/07/09/zakazyvaem-diplom-v-izvestnom-onlayn-magazine-po-komfortnoy-cene.html
Успехов в учебе!
Привет, друзья!
Мы готовы предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Можно купить качественный диплом от любого заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге самого высокого качества. Это дает возможности делать государственные дипломы, которые не отличить от оригиналов. Они будут заверены всеми необходимыми печатями и штампами.
Приобрести диплом любого ВУЗа.
japapmessenger.com/read-blog/510
Успехов в учебе!
Здравствуйте!
Мы готовы предложить документы техникумов, расположенных на территории всей РФ. Можно купить качественно напечатанный диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Документы печатаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригиналов. Документы заверяются всеми обязательными печатями и штампами.
Купить диплом ВУЗа.
http://www.flexartsocial.com/blogs/10135/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Успехов в учебе!
Привет!
Мы можем предложить дипломы любой профессии по доступным ценам. Стоимость может зависеть от выбранной специальности, года выпуска и образовательного учреждения.
Где купить диплом специалиста?
Купить диплом университета
landik-diploms-srednee.ru/kupit-diplom-v-kazani
Хорошей учебы!
Здравствуйте!
Купить документ института вы имеете возможность в нашей компании в Москве.
asxdiplomik24.ru/kupit-diplom-nizhnij-novgorod
Успехов в учебе!
купить диплом в мск asxdiplomik.com/kupit-diplom-moskva .
Привет!
Мы предлагаем дипломы любой профессии по выгодным тарифам. Стоимость может зависеть от выбранной специальности, года получения и университета.
Где купить диплом по нужной специальности?
Купить диплом университета
landik-diploms-srednee.ru/svidetelstvo-o-rozhdenii
Хорошей учебы!
Здравствуйте!
Приобрести документ университета можно у нас в столице.
ast-diplom24.ru/kupit-diplom-krasnoyarsk
Хорошей учебы!
Найдите актуальные промокоды Vavada казино и получите дополнительные бонусы для игры. Эти коды предоставляют уникальные возможности для всех игроков.
Привет!
Мы изготавливаем дипломы любой профессии по выгодным ценам. Стоимость будет зависеть от выбранной специальности, года получения и ВУЗа.
Где купить диплом специалиста?
Приобрести диплом о высшем образовании
arusak-diploms-srednee.ru/kupit-diplom-kandidata-nauk
Удачи!
Привет, друзья!
Приобрести документ института можно в нашей компании в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любой специальности, включая документы образца СССР.
familyportal.forumrom.com/viewtopic.php?id=23434#p60671
Хорошей учебы!
Используйте промокоды Drip казино для увеличения своего игрового баланса. Эти коды предоставляют уникальные бонусы и улучшенные условия для игры.
Добрый день!
Где заказать диплом специалиста?
Заказать диплом о высшем образовании.
forum.fiat-club.ru/blog_post.php?do=updateblog&blogid=
Добрый день!
Приобрести документ университета можно в нашей компании.
ast-diploms24.ru/kupit-diplom-ekaterinbur
Успехов в учебе!
Промокоды Vavada казино предоставляют уникальные бонусы для всех игроков. Воспользуйтесь этими кодами и наслаждайтесь всеми привилегиями.
Большое количество из скважин со временем проведения восстановительного комплекса процедур позволят быть снова введены в применение. Тем более что стоимость таких работ в несколько раз ниже стоимости непосредственных сооружений.
Обеспечено повышение дебита водозаборной скважины не менее 30 процентов от существующего на момент старта работ.
В 80 процентах случаях скважины восстанавливаются до основных данных при внедрении в использование скважины, это становится альтернативой производства буровых работ новой скважины.
Наши сотрудники торговые компании по Очистке водяных емкостей и Водоочистке предлагаем свои услуги всем, как частным так и общественным организациям.
SpecVodService – ремонт скважин на воду
https://karimmassimov.com/
karimmassimov.com bfee0b6
Добрый день!
Купить диплом о высшем образовании
Мы предлагаем выгодно и быстро купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями официальных лиц. Наш диплом пройдет любые проверки, даже с применением профессиональных приборов. Достигайте своих целей максимально быстро с нашей компанией.
Где приобрести диплом специалиста?
http://www.xusyou.com/blogs/286/%D0%93%D0%BB%D0%B0%D0%B2%D0%BD%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%85%D0%BE%D0%B4%D1%8B-%D0%B8%D0%B7%D0%B3%D0%BE%D1%82%D0%BE%D0%B2%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B0%D0%B2%D1%82%D0%BE%D1%80%D1%81%D0%BA%D0%B8%D0%B9-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
http://www.anhbiet.com/index.php?/events/event/12-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B8-%D0%B2%D0%B0%D1%80%D0%B8%D0%B0%D0%BD%D1%82%D1%8B-%D0%B4%D0%BE%D1%81%D1%82%D0%B0%D0%B2%D0%BA%D0%B8-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC/
fire-team.ru/forum/member.php?u=1143
talkiachat.com/blogs/24/%D0%9F%D1%80%D0%B0%D0%B2%D0%B8%D0%BB%D1%8C%D0%BD%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5-%D0%B0%D0%B2%D1%82%D0%BE%D1%80%D1%81%D0%BA%D0%B8%D0%B9-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
macadamlab.ru/wiki/index.php?title=Купить_диплом_онлайн:_просто_и_удобно
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
alanyatoday.ru/users/76
Привет!
Приобрести диплом о высшем образовании.
honda-fit.ru/forums/index.php?autocom=gallery&req=si&img=5669
купить дипломы о высшем купить дипломы о высшем .
Здравствуйте!
Полезные советы по покупке диплома о высшем образовании без риска
mestovstrechi.flybb.ru/viewtopic.php?f=4&t=1281
Всегда вам поможем!.
Добрый день!
Где приобрести диплом по нужной специальности?
kingcityrp.moibb.ru/viewtopic.php?f=34&t=463
Удачи!
Добрый день!
Где приобрести диплом специалиста?
Мы предлагаем документы ВУЗов, которые находятся на территории всей РФ. Вы сможете заказать диплом за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы печатаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Они будут заверены всеми требуемыми печатями и штампами.
Мы изготавливаем дипломы любых профессий по доступным тарифам.
diplomasx.com/kupit-diplom-moskva
Рады оказаться полезными!
купить диплом инженера цена купить диплом инженера цена .
Привет!
Как избежать рисков при покупке диплома колледжа или ВУЗа в России
rst.adk.audio/company/personal/user/1577/forum/message/1952/1984/#message1984
Поможем вам всегда!.
Привет, друзья!
Заказать документ о получении высшего образования можно в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы старого образца.
forum-pmr.net/member.php?u=42748
Удачи!
Привет!
Наши специалисты предлагают максимально быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Диплом пройдет любые проверки, даже с применением специальных приборов. Достигайте цели максимально быстро с нашим сервисом.
samoshkin.ru/index.php?subaction=userinfo&user=udyfupyn
Хорошей учебы!
Привет!
Где заказать диплом по нужной специальности?
Купить диплом университета.
rsn360.ru/blogs/new
купить диплом ссср высшее asxdiplomik.com/kupit-diplom-moskva .
Привет, друзья!
Как приобрести аттестат о среднем образовании в Москве и других городах
myfootballday.ru/kupite-diplom-i-zabudte-o-studencheskih-hlopotah
Рады оказаться полезными!.
куплю диплом другим asxdiplomik.com/kupit-diplom-moskva .
Добрый день!
Купить диплом ВУЗа.
vwapepla.com/read-blog/136
аттестат об окончании 11 классов купить diploms-x.com .
Здравствуйте!
Купить документ о получении высшего образования можно в нашей компании. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы Советского Союза.
avtomobil1980.ixbb.ru/viewtopic.php?id=114#p114
Удачи!
Здравствуйте!
Мы готовы предложить документы техникумов, расположенных на территории всей России. Вы сможете приобрести качественно сделанный диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Документы делаются на бумаге самого высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Документы заверяются необходимыми печатями и подписями.
Приобрести диплом о высшем образовании.
pro-eltern.de/read-blog/153
Хорошей учебы!
Добрый день!
Где приобрести диплом специалиста?
gti-club.ru/forum/member.php?u=23001
Хорошей учебы!
Здравствуйте!
Где приобрести диплом специалиста?
Приобрести диплом ВУЗа.
naturetour.ru/club/user/186/blog/1633/
Player reviews and testimonials are overwhelmingly positive, with many praising the game’s exciting gameplay and
aviator demo
Добрый день!
Где приобрести диплом специалиста?
Мы готовы предложить документы институтов, которые находятся на территории всей Российской Федерации. Вы сможете заказать диплом за любой год, включая документы старого образца. Дипломы выпускаются на бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и подписями.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам.
ast-diplomy24.ru/kupit-diplom-moskva
Окажем помощь!
ресторан на Новый год или Singita Serengeti House – роскошный современный отель
Авиакомпания Air Algerie запускает рейсы из Петербурга в Алжир
https://samoylovaoxana.ru/tag/bashnya-dyavola/
Ещё можно узнать: что делать если выиграл в лотерею
Лучшие туристические направления
Здравствуйте!
Где купить диплом по нужной специальности?
Мы предлагаем дипломы любых профессий по приятным тарифам.
allonlinesport.ru/page/14/
Привет!
Мы готовы предложить документы техникумов, которые расположены на территории всей России. Можно приобрести диплом за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Документы делаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы будут заверены всеми необходимыми печатями и штампами.
Купить диплом университета.
biomedia.pro/club/user/112304/forum/message/3795/13277/
Успехов в учебе!
аттестат о среднем специальном образовании купить аттестат о среднем специальном образовании купить .
Привет!
Стоимость дипломов высшего и среднего образования и процесс их получения
ethnoglobus.az/index.php?subaction=userinfo&user=owujil
Окажем помощь!.
Привет, друзья!
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по доступным тарифам. Стоимость зависит от той или иной специальности, года получения и образовательного учреждения.
Где заказать диплом по нужной специальности?
Купить диплом о высшем образовании
arusak-diploms-srednee.ru/diplom-sredne-spetcialnoe-obrazovanie
Хорошей учебы!
Добрый день!
Наши специалисты предлагают быстро купить диплом, который выполняется на оригинальном бланке и заверен печатями, штампами, подписями. Данный документ пройдет любые проверки, даже с применением профессиональных приборов. Решайте свои задачи быстро и просто с нашими дипломами.
vtik.net/index.php?subaction=userinfo&user=imexi
Удачи!
Привет!
Купить диплом любого ВУЗа.
http://www.arpt.gov.gn/observatoire-des-marches-3e-trimestre-2019
Успехов в учебе!
Привет, друзья!
Мы предлагаем документы техникумов, которые находятся в любом регионе России. Вы можете приобрести диплом от любого заведения, за любой год, в том числе документы старого образца. Дипломы и аттестаты печатаются на бумаге самого высшего качества. Это дает возможности делать государственные дипломы, которые не отличить от оригиналов. Документы заверяются необходимыми печатями и подписями.
Купить диплом о высшем образовании.
mazda-demio.ru/forums/index.php?autocom=gallery&req=si&img=4719
Удачи!
Добрый день!
Мы изготавливаем дипломы любой профессии по невысоким тарифам. Стоимость будет зависеть от той или иной специальности, года выпуска и образовательного учреждения.
Где заказать диплом специалиста?
Заказать диплом ВУЗа
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske
Успешной учебы!
Привет!
Заказать диплом любого университета.
sonnick84.diary.ru/p222058344_kakie-internet-magaziny-s-dokumentami-na-tekuwij-moment-imeyutsya.htm
Здравствуйте!
Где приобрести диплом специалиста?
Мы предлагаем документы институтов, которые расположены на территории всей России. Вы сможете купить качественно напечатанный диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы заверяются всеми обязательными печатями и подписями.
Мы изготавливаем дипломы любой профессии по невысоким тарифам.
asxdiplomik.com/kupit-diplom-omsk
Рады оказать помощь!
купить диплом старого образца в нижнем новгороде diploms-x.com .
Привет, друзья!
Купить документ ВУЗа вы имеете возможность у нас в Москве.
ast-diplom.com/kupit-diplom-rostov-na-donu
Успехов в учебе!
Добрый день!
Мы предлагаем дипломы любых профессий по доступным ценам. Цена зависит от определенной специальности, года выпуска и образовательного учреждения.
Где заказать диплом по необходимой специальности?
Купить диплом университета
arusak-diploms-srednee.ru
Успешной учебы!
Dumps Paypal buy Shops and markets cards Tor
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
Store Hacked paypal Shop Hacked card
Добрый день!
Где купить диплом по актуальной специальности?
http://www.mirmafii.ru/article/7558
Удачи!
Привет!
Где заказать диплом специалиста?
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями должностных лиц. Диплом пройдет любые проверки, даже при помощи специальных приборов. Решите свои задачи быстро с нашей компанией.
Заказать диплом о высшем образовании.
hrv-club.ru/forums/index.php?autocom=gallery&req=si&img=6068
Привет!
Купить документ о получении высшего образования можно в нашей компании в столице.
diplomyx.com/kupit-diplom-rostov-na-donu
Успехов в учебе!
Легализация перепланировки важна для соблюдения всех норм и законодательства. Наша компания предлагает помощь в узаконивании перепланировок, включая сбор и подачу документов, а также взаимодействие с контролирующими органами.
Услуга узаконивание перепланировки обеспечит вам спокойствие и уверенность в том, что все изменения в вашем помещении соответствуют требованиям закона. Мы гарантируем быстрое и профессиональное выполнение всех необходимых процедур.
купить срочно дипломы о высшем образовании вуза asxdiplomik24.ru .
Добрый день!
Где приобрести диплом по актуальной специальности?
Мы предлагаем дипломы любых профессий по приятным ценам.
ветерантюмгео.рф/galereya/?type_0=gallery&album_gallery_id_0=2
Добрый день!
Мы предлагаем выгодно приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями официальных лиц. Наш диплом способен пройти лубую проверку, даже при использовании профессионального оборудования. Решите свои задачи быстро и просто с нашей компанией.
prof-komplekt.com/club/user/10842/blog/10797/
Удачи!
Pinup sv
Placera ditt spel hos pin up nu – mest reliable bookmaker
Pinup casino
Добрый день!
Заказать документ университета вы сможете у нас.
ast-diplomas.com/kupit-diplom-magistra
Удачи!
На сайте https://xn--80aa1agibdda2ab.xn--p1ai/ можно приобрести насосное оборудование, автоматику, средства управления, трубопроводную арматуру. Ознакомьтесь со всеми самыми выгодными предложениями прямо сейчас, в том числе, и хитами продаж. Именно они пользуются особым спросом среди покупателей. На всю продукцию установлены привлекательные расценки, зачастую действуют акции, которые делают приобретение более выгодным. Все товары от лучших производителей, положительно себя зарекомендовавших.
дипломы награждения купить asxdiplomik.com/kupit-diplom-moskva .
Привет!
Диплом вуза купить официально с упрощенным обучением в Москве
freelance.habr.com/freelancers/dilopluyy
Поможем вам всегда!.
Добро пожаловать на наш сайт, где вы можете найти работу, которая соответствует вашим навыкам и интересам.
Мы открыли вакансии для курьеров, поваров и логистов и приглашаем вас присоединиться к нашей команде.Курьер
Вакансии Курьера
Мы ищем ответственных и активных людей на должность курьера.
Ваши обязанности будут включать доставку товаров клиентам, соблюдение графика и поддержание высокого уровня сервиса.
Мы предлагаем конкурентоспособную заработную плату, гибкий график и возможность карьерного роста.
Работа кладовщиком в крупной компании
Подайте заявку прямо сейчас на нашем сайте.
Вакансии Повора
Если у вас есть страсть к кулинарии и вы хотите развивать свои навыки, мы приглашаем вас стать частью нашей команды поваров.
Ваши обязанности будут включать приготовление блюд по установленным стандартам, соблюдение санитарных норм и работу в команде. Мы предлагаем стабильную работу, достойную оплату и возможности для профессионального роста. Подайте заявку прямо сейчас на нашем сайте.
Вакансии Логиста
Мы ищем специалистов по логистике, готовых помочь нам в управлении процессами поставок и складирования.
Обязанности включают координацию перевозок, управление запасами и оптимизацию логистических процессов.
Мы предлагаем привлекательные условия труда, возможности для обучения и карьерного роста.
Актуальные вакансии в Москве
Подайте заявку прямо сейчас на нашем сайте.
Начните новую карьеру с нами. Присоединяйтесь к нашей команде, подав заявку на вакансию курьера, повара или логиста на нашем сайте уже сегодня.
Добрый день!
Мы можем предложить документы ВУЗов, расположенных на территории всей России. Вы сможете купить качественный диплом от любого заведения, за любой год, в том числе документы старого образца СССР. Дипломы и аттестаты делаются на бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, которые невозможно отличить от оригиналов. Документы будут заверены всеми необходимыми печатями и штампами.
Приобрести диплом любого ВУЗа.
respectmyopinion.com/blogs/31/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Удачи!
Привет, друзья!
Приобрести диплом любого университета.
blog.kmu.edu.tr/eylemguzel/calisma-alanlari
Успехов в учебе!
Привет, друзья!
Где приобрести диплом по необходимой специальности?
Мы предлагаем выгодно и быстро заказать диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Данный документ способен пройти любые проверки, даже с использованием профессионального оборудования. Достигайте цели быстро с нашей компанией.
Заказать диплом о высшем образовании.
betalk.in.th/read-blog/2966
Привет, друзья!
Где приобрести диплом специалиста?
Мы предлагаем дипломы любой профессии по доступным тарифам.
animesocial.su/blogs/1046/Сколько-примерно-может-стоить-сегодня-качественный-дубликат-диплома
Добрый день!
Мы предлагаем дипломы любой профессии по невысоким тарифам. Стоимость зависит от конкретной специальности, года получения и образовательного учреждения.
Где купить диплом по нужной специальности?
Приобрести диплом о высшем образовании
arusak-diploms-srednee.ru/kupit-diplom-magistra
Удачи!
Привет!
Узнайте, как безопасно купить диплом о высшем образовании
http://www.club-kia.com/forum/thread30837.html
Всегда вам поможем!.
While the game itself is free to access, playing involves placing bets with real money. Some platforms may offer
aviator play game
Быстрая схема покупки диплома старого образца: что важно знать?
ast-diplomas.com/kupit-diplom-omsk
Здравствуйте!
Узнайте стоимость диплома высшего и среднего образования и процесс получения
domainrama.com/read-blog/914
Всегда вам поможем!.
Привет, друзья!
Диплом техникума купить официально с упрощенным обучением в Москве
obmenka.forum2x2.ru/t17060-topic#38554
Будем рады вам помочь!.
купить диплом без занесения diplomyx.com .
купить диплом по охране труда asxdiplomik.com .
Добрый день!
Быстрая покупка диплома старого образца: возможные риски
draiv.flybb.ru/viewtopic.php?f=2&t=739
Рады оказаться полезными!.
Привет, друзья!
Купить диплом любого университета.
wiki.gta-zona.ru/index.php/??????_?_?????_?????:_???_???_????????
Успехов в учебе!
Добрый день!
Заказать документ о получении высшего образования вы имеете возможность в нашей компании в столице.
ast-diplomy.com/kupit-diplom-o-srednem-obrazovanii
Успехов в учебе!
Привет, друзья!
Где заказать диплом специалиста?
Наша компания предлагает быстро и выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями. Наш документ пройдет любые проверки, даже с применением профессионального оборудования. Достигайте цели максимально быстро с нашим сервисом.
Купить диплом о высшем образовании.
jpq7var4t.collectblogs.com/73907644/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
Добрый день!
Мы предлагаем документы ВУЗов, которые находятся на территории всей Российской Федерации. Вы имеете возможность купить диплом за любой год, включая сюда документы старого образца. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые не отличить от оригиналов. Документы заверяются необходимыми печатями и подписями.
Купить диплом университета.
z4wz0dazf.azzablog.com/28386127/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Успехов в учебе!
Как быстро и легально купить аттестат 11 класса в Москве
diploms-x24.ru/kupit-diplom-magistra
куплю диплом настоящий куплю диплом настоящий .
купить диплом маи ast-diploms.com .
color wow style on steroids
blog topic
Здравствуйте!
Мы готовы предложить дипломы любой профессии по приятным тарифам. Цена зависит от выбранной специальности, года выпуска и университета.
Где заказать диплом специалиста?
Приобрести диплом университета
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge
Успешной учебы!
mounjaro купить препарат – мунжаро 12.5 мг купить, тирзепатид цена
Добрый день!
Мы можем предложить документы техникумов, расположенных в любом регионе РФ. Можно заказать диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригинала. Они будут заверены всеми обязательными печатями и подписями.
Купить диплом ВУЗа.
lebanonhub.app/blogs/2403/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Успешной учебы!
Привет!
Мы можем предложить дипломы любой профессии по разумным ценам. Цена зависит от конкретной специальности, года выпуска и ВУЗа.
Где купить диплом по необходимой специальности?
Купить диплом о высшем образовании
landik-diploms-srednee.ru/diplom-bakalavra
Успехов в учебе!
Добрый день!
Полезные советы по безопасной покупке диплома о высшем образовании
lsfiredept.listbb.ru/viewtopic.php?f=2&t=448
Рады помочь!.
Проверьте лицензию казино – это гарантия вашей безопасности и честности игрового процесса. ]Отзывы других игроков являются ценным источником информации о надежности и качестве обслуживания. ]Техническая поддержка должна быть доступна круглосуточно, чтобы оперативно решать любые возникающие проблемы https://www.luxcosmeticsdv.ru/index.php?option=com_k2&view=itemlist&task=user&id=559819
Frequently Asked Questions (FAQs)
aviator play game
pin up no
Plasser innsatsen din hos pin up online – veldig prestisjefylt bookmaker
pin up no
Привет!
Приобрести документ о получении высшего образования можно у нас в Москве.
ast-diplomy.com/kupit-diplom-vracha
Хорошей учебы!
Добрый день!
Заказать диплом ВУЗа
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями должностных лиц. Документ пройдет любые проверки, даже при помощи специфических приборов. Достигайте цели быстро с нашими дипломами.
Где заказать диплом по нужной специальности?
astrcolcult.ru/?post_type=topic&p=34434
blogs.rufox.ru/~worksale/47159.htm
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
arsenal.listbb.ru/viewtopic.php?f=14&t=419
pdlspd.listbb.ru/viewtopic.php?f=3&t=409
купить диплом в кузнецке diplomasx.com .
купить диплом продавца ast-diploms.com .
Как приобрести аттестат о среднем образовании в Москве и других городах
ast-diplomy24.ru/otzyvy
rouge sonic movie best recent movies 2022samuel l jackson recent movieseuphoria season 1 ep 8 soundtrackduck hunting indiana season
Привет!
Приобрести документ о получении высшего образования можно у нас.
ast-diplomas.com/kupit-diplom-vracha
Успехов в учебе!
https://www.fermedelagouttedor.fr/group/mysite-200-group/discussion/d6815c04-bb1c-43be-8931-54b474f8de24
Добрый день!
Наша компания предлагает купить диплом высочайшего качества, неотличимый от оригинала без использования специального оборудования и опытного специалиста.
fh3809kd.bget.ru/index.php?name=account&op=info&uname=akyky
Успешной учебы!
Здравствуйте!
Приобрести документ университета вы имеете возможность в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ.
radioizba.ru/communication/forum/?PAGE_NAME=profile_view&UID=18830
mineralgroup.ru/index.php?subaction=userinfo&user=iwipy
rytof.ru/node/16245
findaspermdonor.com/viewtopic.php?f=2&t=80886&p=78159#p78159
http://www.daongil.com/bbs/board.php?bo_table=free&wr_id=297936
Pinup
Place your bet at pinup now – authentic elite bookmaker
Pinup ar
На сайте https://ufa2.body-pit.ru/ приобретите качественное, сертифицированное спортивное питание, которое позволит заполучить красивое тело мечты, привлекательный рельеф или значительно похудеть. В этом интернет-магазине вы найдете витамины, гейнеры, сжигатели жира, аминокислоты, предтренировочные комплексы, антиоксиданты. Вся продукция сертифицированная, высокого качества, представлена именитыми брендами. Важным моментом является то, что доставка заказа осуществляется в тот день, когда оформили покупку.
Привет, друзья!
Мы предлагаем документы техникумов, которые находятся на территории всей России. Вы имеете возможность купить диплом за любой год, в том числе документы старого образца. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Они заверяются всеми необходимыми печатями и подписями.
Заказать диплом о высшем образовании.
68owydyke.luwebs.com/28841408/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Успешной учебы!
Привет!
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по выгодным ценам. Цена может зависеть от определенной специальности, года получения и образовательного учреждения.
Где купить диплом по актуальной специальности?
Заказать диплом о высшем образовании
landik-diploms-srednee.ru/kupit-diplom-v-kazani
Хорошей учебы!
мунджаро препарат купить – mounjaro инструкция +на русском, mounjaro dubai
Привет, друзья!
Как приобрести диплом о среднем образовании в Москве и других городах
amtest.mybb.ru/post.php?action=post&fid=1
Всегда вам поможем!.
Здравствуйте!
Приобрести диплом любого ВУЗа
Наша компания предлагает выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Документ пройдет лубую проверку, даже при помощи специальных приборов. Решите свои задачи быстро и просто с нашими дипломами.
Где купить диплом специалиста?
astrcolcult.ru/?post_type=topic&p=34434
driveme.rusff.me/viewtopic.php?id=2115#p105171
promintern.listbb.ru/viewtopic.php?f=16&t=474
http://www.hristianka.ru/forum/r/prev_loaded/1/
odessaforum.getbb.ru/viewtopic.php?f=5&t=20402
Привет, друзья!
Мы предлагаем купить диплом отличного качества, неотличимый от оригинального документа без участия специалистов высокой квалификации со сложным оборудованием.
fire-team.ru/forum/showthread.php?p=36155#post36155
Хорошей учебы!
можно ли купить высшее образование ast-diploms.com .
купить диплом пту в нижнем тагиле diplomasx.com .
Привет!
Приобрести документ о получении высшего образования вы можете в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов РФ.
favorit-games.ru/profile.php?u=ygeti
chip-ecu.ru/threads/%D0%A0%D0%B5%D1%88%D0%B5%D0%BD%D0%BE-toyota-tundra-5-7-3ur-fe-2008-p0101-p0171-p0174.598/#post-6801
http://www.lada-vesta.net/showthread.php?p=466443#post466443
pedolog-pro.ru/?post_type=topic&p=328163
flowerwheel.synology.me/dokuwiki/doku.php?id=russianydiplomix
Привет, друзья!
Как безопасно купить диплом колледжа или ВУЗа в России, что важно знать
fbadult.com/blogs/3050/Диплом-на-заказ-качество-и-надежность
Окажем помощь!.
Pin up Us
Place your bet at pinup now – most prestigious bookmaker
Pin up casino
мунжаро +как колоть – эффективные препараты +для похудения +в аптеках, тирзепатид лиофилизат
Competitive Tournaments and Events
aviator game online
Добрый день!
Приобрести документ о получении высшего образования вы можете в нашей компании в столице. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР.
darknews.ru/diplom-na-zakaz-kachestvo-i-nadezhnost
Успехов в учебе!
Привет, друзья!
Где заказать диплом специалиста?
Приобрести диплом любого ВУЗа.
iqtorg.ru/forum/user/19167/
Множество пользователей активно ищут удобные и доступные способы развлечения. Это привело к повышению популярности различных онлайн-сервисов http://www.apicarrara.it/modules.php?name=Journal&file=display&jid=4341
Привет, друзья!
Где купить диплом специалиста?
Мы предлагаем выгодно приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Данный диплом пройдет лубую проверку, даже с использованием специального оборудования. Достигайте своих целей максимально быстро с нашим сервисом.
Купить диплом любого ВУЗа.
indungii.ro/forum/index.php?/gallery/image/11-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5/
Здравствуйте!
Заказать документ института можно в нашей компании.
diplomyx.com/otzyvy
Успехов в учебе!
Привет!
Приобрести диплом любого ВУЗа
Наши специалисты предлагают быстро и выгодно приобрести диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями должностных лиц. Документ способен пройти любые проверки, даже с использованием специального оборудования. Решите свои задачи быстро и просто с нашим сервисом.
Где купить диплом по актуальной специальности?
mkpnz.ru/users/8
macadamlab.ru/wiki/index.php?title=пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ
volnodumie.bbmy.ru/viewtopic.php?id=12332#p25047
vip.9bb.ru/viewtopic.php?id=5959#p9901
3drus.ru/forum/topic_34806
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Детская одежда оптом из Турции
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Привет, друзья!
Мы предлагаем заказать диплом высокого качества, неотличимый от оригинала без использования специального оборудования и опытного специалиста.
moj.webservis.ru/forums/profile.php?action=show&member=7610
Удачи!
Привет!
Приобрести документ о получении высшего образования вы можете в нашей компании. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации.
http://www.miranetwork.it/index.php?option=com_k2&view=itemlist&task=user&id=446408
wiki.gptel.ru/index.php?title=diploman
fire-team.ru/forum/showthread.php?p=35320#post35320
http://www.lada-xray.net/showthread.php?p=32747#post32747
kioskindustry.ru/index.php?subaction=userinfo&user=axafep
Сайты казино
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
<a href=http://www.klein-putz.net/info.php?a=оформить кредитную карту
Оформи заявку на кредитную карту от лучших банков России онлайн
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
Добрый день!
Приобрести документ о получении высшего образования вы имеете возможность у нас.
ast-diplomas24.ru/kupit-diplom-sankt-peterburg
Хорошей учебы!
Добрый день!
Где приобрести диплом по актуальной специальности?
Приобрести диплом ВУЗа.
domainrama.com/read-blog/914
Здравствуйте!
Заказать документ о получении высшего образования можно в нашей компании. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, включая документы Советского Союза.
peaceofficial.5nx.ru/viewtopic.php?f=111&t=810
Успехов в учебе!
Добрый день!
Купить документ института вы сможете у нас в столице.
diplomasx24.ru/kupit-diplom-sankt-peterburg
Удачи!
Привет, друзья!
Где купить диплом по необходимой специальности?
Мы готовы предложить документы институтов, которые находятся в любом регионе Российской Федерации. Можно купить качественный диплом от любого ВУЗа, за любой год, включая документы СССР. Дипломы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Документы будут заверены необходимыми печатями и штампами.
Мы изготавливаем дипломы любой профессии по приятным тарифам.
ast-diplomy.com/kupit-diplom-krasnoyarsk
Окажем помощь!
Зайдите на сайт https://moresliv.cc/ где вы сможете скачать огромное количество курсов бесплатно онлайн через торрент. Огромная база знаний и обучений. Складчины и видеоуроки, книги и вебинары – графика, программирование, бизнес, курсы блогеров и многое другое здесь. Более 175.000 различных курсов на сайте. Заходи!
Привет, друзья!
Как приобрести диплом техникума с минимальными рисками
altersoftonline.maxbb.ru/viewtopic.php?f=11&t=210
Рады оказаться полезными!.
Привет!
Приобрести документ ВУЗа вы имеете возможность у нас.
diplomyx24.ru/kupit-diplom-ekaterinbur
Удачи!
Здравствуйте!
Купить документ ВУЗа можно у нас.
diplomasx24.ru/kupit-diplom-vracha
Добрый день!
Приобрести диплом о высшем образовании.
http://www.4yo.us/blogs/140673/%D0%9A%D0%B0%D0%BA-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BD%D0%B5%D0%BE%D1%82%D0%BB%D0%B8%D1%87%D0%B8%D0%BC%D1%8B%D0%B9-%D0%BE%D1%82-%D0%BE%D1%80%D0%B8%D0%B3%D0%B8%D0%BD%D0%B0%D0%BB%D0%B0-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8
Привет, друзья!
Купить диплом любого ВУЗа
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Документ способен пройти любые проверки, даже при использовании специфических приборов. Достигайте свои цели быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
gamerszona.ru/index.php?/blogs/entry/7-%D1%82%D0%B5%D1%85%D0%BF%D0%BE%D0%B4%D0%B4%D0%B5%D1%80%D0%B6%D0%BA%D0%B0-%D0%B8-faq-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8/
http://www.cyberpinoy.net/read-blog/33307
http://www.pgu.ac/wall/blogs/215/%D0%A5%D0%BE%D1%82%D0%B8%D1%82%D0%B5-%D0%B2%D1%8B%D1%8F%D1%81%D0%BD%D0%B8%D1%82%D1%8C-%D0%BA%D0%B0%D0%BA-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%97%D0%B0%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5
http://www.yagath.com/blogs/678070/%D0%9E%D1%81%D0%BD%D0%BE%D0%B2%D0%BD%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%85%D0%BE%D0%B4%D1%8B-%D1%80%D0%BE%D1%81%D1%81%D0%B8%D0%B9%D1%81%D0%BA%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%BE%D0%B8%D0%B7%D0%B2%D0%BE%D0%B4%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
forexrassia.ru/nastoyashhie-diplomyi-bez-ozhidaniya-i-problem
Добрый день!
Приобрести документ университета вы сможете у нас в Москве.
ast-diplomas.com/kupit-diplom-magistra
заказать диплом о высшем образовании заказать диплом о высшем образовании .
Добрый день!
Мы предлагаем быстро и выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями официальных лиц. Наш диплом способен пройти любые проверки, даже при использовании профессионального оборудования. Решите свои задачи быстро с нашей компанией.
vk.com/asemok_1255?w=wall391770830_1735
Удачи!
Привет, друзья!
Где купить диплом по необходимой специальности?
argayash.flybb.ru/viewtopic.php?f=9&t=1146
Успешной учебы!
Диплом вуза купить официально с упрощенным обучением в Москве
kopoluzhona.image-perth.org/cto-imenno-ponadobitsa-iz-tehniki-dla-izgotovlenia-dokumentov
Competitive Tournaments and Events
demo aviator game
http://xn--jc-je2if91fs6b.com/bbs/board.php?bo_table=free&wr_id=12
Добрый день!
Купить документ о получении высшего образования можно в нашей компании в Москве.
ast-diplomas.com/kupit-diplom-o-srednem-obrazovanii
my website Tor browser download
Привет!
Где заказать диплом специалиста?
Мы готовы предложить документы ВУЗов, расположенных на территории всей России. Можно заказать качественный диплом от любого ВУЗа, за любой год, включая документы старого образца. Дипломы делаются на бумаге высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригинала. Они заверяются всеми необходимыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по выгодным тарифам.
ast-diplomas24.ru/kupit-diplom-rostov-na-donu
Поможем вам всегда!
купить диплом о неполном высшем образовании diploms-x.com .
Пошаговая инструкция по официальной покупке диплома о высшем образовании
ast-diploms24.ru/kupit-diplom-moskva
https://site547576904.fo.team/
купить мед справку
Привет!
Приобрести диплом университета.
sky-metaverse.com/read-blog/9995
купить медицинский диплом москва asxdiplomik.com .
Привет, друзья!
Где купить диплом по актуальной специальности?
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
http://www.revostock.com/ptpl.index.php
купить диплом инженера пгс asxdiplomik24.ru .
Привет!
Заказать диплом университета
Мы предлагаем выгодно и быстро заказать диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Документ способен пройти лубую проверку, даже с применением специального оборудования. Достигайте свои цели максимально быстро с нашим сервисом.
Где купить диплом специалиста?
amcall.net/read-blog/369
mynewsport.ru/legalnaya-pokupka-diplomov-byistro-i-udobno
l67697qa.beget.tech/2024/07/08/legkiy-vybor-magazina-prodayuschego-diplomy.html
amengram.com/blogs/350/%D0%9A%D0%B0%D0%BA%D0%B8%D0%B5-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D1%8B-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8-%D0%BD%D0%B0-%D1%81%D0%B5%D0%B3%D0%BE%D0%B4%D0%BD%D1%8F%D1%88%D0%BD%D0%B8%D0%B9-%D0%B4%D0%B5%D0%BD%D1%8C-%D0%B5%D1%81%D1%82%D1%8C
appleincub.ru/vash-put-k-uspehu-legalno-i-nadezhno
Привет!
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Наш диплом пройдет любые проверки, даже при использовании специального оборудования. Решите свои задачи быстро с нашей компанией.
forum.stanki-chpu.ru/threads/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BA%D0%B0%D0%BD%D0%B4%D0%B8%D0%B4%D0%B0%D1%82%D0%B0-%D0%BD%D0%B0%D1%83%D0%BA.379/
Успешной учебы!
Привет, друзья!
Пошаговая инструкция по безопасной покупке диплома о высшем образовании
club.7ya.ru/dilopluyy/
Рады оказать помощь!.
Привет!
Где приобрести диплом по актуальной специальности?
zdsim.ru/wiki/index.php/Диплом_для_успешной_карьеры:_просто_и_доступно
Удачи!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
wiki.hightgames.ru/index.php/%D0%A7%D0%B5%D1%82%D1%8B%D1%80%D0%B5_%D0%BE%D1%81%D0%BD%D0%BE%D0%B2%D0%BD%D1%8B%D1%85_%D0%B3%D1%80%D1%83%D0%BF%D0%BF%D1%8B_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%BE%D0%B2,_%D0%BA%D0%BE%D1%82%D0%BE%D1%80%D1%8B%D0%B5_%D0%BF%D1%80%D0%BE%D0%B4%D0%B0%D1%8E%D1%82_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B
Здравствуйте!
Приобрести диплом любого университета.
http://www.xn--5-htbd2chx.xn--p1ai/product/igra-stol-forma/reviews/
Успехов в учебе!
Добрый день!
Где заказать диплом специалиста?
Мы можем предложить документы ВУЗов, которые находятся на территории всей РФ. Можно купить качественно напечатанный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы выпускаются на бумаге высшего качества. Это дает возможность делать настоящие дипломы, которые не отличить от оригинала. Документы будут заверены всеми обязательными печатями и штампами.
Мы изготавливаем дипломы любой профессии по выгодным ценам.
ast-diplomas24.ru/kupit-diplom-voronezh
Рады оказать помощь!
Привет!
Заказать диплом ВУЗа.
Мы предлагаем документы техникумов, которые находятся на территории всей РФ. Вы можете купить диплом от любого учебного заведения, за любой год, в том числе документы СССР. Документы печатаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Документы будут заверены необходимыми печатями и подписями.
menaharia.com/read-blog/2713
Здравствуйте!
Как избежать рисков при покупке диплома колледжа или ВУЗа в России
http://www.as7abe.com/wall/blogs/post/new
Окажем помощь!.
купить диплом о высшем образовании экономиста diploms-x.com .
сделать справку
Множество пользователей активно ищут удобные и доступные способы развлечения. Это привело к повышению популярности различных онлайн-сервисов https://www.aura-invest.com/bbs/board.php?bo_table=free&wr_id=3456921
Здравствуйте!
Купить диплом о высшем образовании.
Мы готовы предложить документы техникумов, которые расположены в любом регионе РФ. Можно заказать диплом от любого заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это дает возможность делать государственные дипломы, которые не отличить от оригинала. Они заверяются необходимыми печатями и штампами.
iie1edgkc.frewwebs.com/28827538/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Быстрая покупка диплома старого образца: возможные риски
bogatbeden.listbb.ru/viewtopic.php?f=3&t=437
Рады оказать помощь!.
купить диплом вуза государственного образца купить диплом вуза государственного образца .
купить диплом сантехник купить диплом сантехник .
купить бланк диплома высшем diplomyx.com .
Добрый день!
Приобрести документ университета вы сможете в нашей компании в Москве.
diplomyx24.ru/kupit-diplom-vracha
Удачи!
Хотите быть в курсе всех новостей строительной индустрии? FreshHomes.ru — это ваш надежный источник свежей информации о строительстве, архитектуре и недвижимости.
Детские сады
Что мы предлагаем?
Актуальные новости: Будьте в курсе последних событий и тенденций в строительной отрасли.
Глубокая аналитика: Экспертные мнения и подробные обзоры помогут вам разобраться в сложных вопросах.
Полезные советы: Найдите практические рекомендации по ремонту, дизайну интерьера и управлению недвижимостью.
Интересные интервью: Узнайте мнение ведущих профессионалов отрасли.
Посетите FreshHomes.ru и подпишитесь на обновления
Комфортная городская среда
Не упустите возможность получать самые важные и полезные новости прямо на вашу почту. Подпишитесь на наш сайт и станьте частью сообщества профессионалов строительной индустрии.
Присоединяйтесь к нашему Телеграм-каналу Строительный портал по ссылке https://t.me/+Btp6XdoZouA4ZDIy и оставайтесь в центре событий
Привет!
Где заказать диплом специалиста?
Мы можем предложить дипломы любой профессии по выгодным тарифам.
myturtime.ru/page/47
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным ценам. Цена может зависеть от той или иной специальности, года получения и образовательного учреждения.
landik-diploms-srednee.ru/svidetelstvo-o-razvode
Удачи!
Привет!
Заказать диплом любого ВУЗа.
Мы предлагаем документы ВУЗов, которые расположены на территории всей Российской Федерации. Можно заказать качественно напечатанный диплом от любого заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Документы делаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми требуемыми печатями и подписями.
1776reloaded.us/blogs/57/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
you can try this out Rufus
not, you lose your bet.
aviator game demo
Добрый день!
Удивительно, но купить диплом кандидата наук оказалось не так сложно
paulikipedia.ru/index.php/Купите_диплом_и_начните_новую_жизнь
Поможем вам всегда!.
Привет!
Купить диплом о высшем образовании.
rusere.ru/communication/forum/messages/forum11/message3687/2974-legkiy-vybor-magazina_-realizuyushchego-diplomy-i-attestaty?result=new
Привет, друзья!
Как получить диплом техникума официально и без лишних проблем
molbiol.ru/forums/index.php?showtopic=1192567&st=0&p=4041774#entry4041774
Рады оказаться полезными!.
как купить диплом о среднем образовании asxdiplomik24.ru .
Здравствуйте!
Приобрести документ института вы имеете возможность в нашем сервисе.
ast-diploms.com/kupit-diplom-moskva
Успешной учебы!
Привет, друзья!
Мы изготавливаем дипломы любой профессии по выгодным ценам. Цена будет зависеть от выбранной специальности, года получения и образовательного учреждения.
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe
Успехов в учебе!
Здравствуйте!
Мы предлагаем выгодно и быстро купить диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями должностных лиц. Диплом способен пройти любые проверки, даже при использовании специальных приборов. Достигайте свои цели быстро и просто с нашим сервисом.
mastrerkon.ru/forum/viewtopic.php?f=10&t=27394
Хорошей учебы!
Découvrez les programmes suisses comme jamais vue avec notre service IPTV de première qualité !
Accédez librement aux meilleures chaînes suisses comme RTS, la SRF, RSI (Radiotelevisione svizzera) et bien d’autres. Notre plateforme offre :
Plus de 100 chaînes suisses et internationales en haute définition
Un sélection VOD riche en contenu vidéo
La faculté de regarder vos émissions préférées en différé
Une interface intuitive qui fonctionne sur divers appareils
Un service client réactif situé en Suisse
Que vous soyez amateur de sport, de journaux télévisés ou de loisirs, notre offre IPTV
Electronics Tracker – Activité IPTV
s’adapte à vos envies. Testez gratuitement pendant 24 heures et découvrez une façon innovante de voir la télévision !
Привет!
Купить диплом ВУЗа.
wiki.mdomtv.net/index.php?title=??????_??????_??_?_??????:_????????_?_????????
Успешной учебы!
Добрый день!
Где купить диплом по актуальной специальности?
dopalnenie.listbb.ru/viewtopic.php?f=3&t=710
Хорошей учебы!
Добрый день!
Приобрести документ университета можно в нашей компании в столице.
ast-diplomy24.ru/kupit-diplom-ekaterinbur
Удачи!
Добрый день!
Мы можем предложить дипломы любых профессий по приятным ценам. Стоимость зависит от той или иной специальности, года выпуска и университета.
landik-diploms-srednee.ru/svidetelstvo-o-rozhdenii
Хорошей учебы!
Привет!
Приобрести документ о получении высшего образования вы имеете возможность у нас.
ast-diplomas.com/otzyvy
Здравствуйте!
Где заказать диплом специалиста?
Приобрести диплом любого ВУЗа.
http://www.startspresto.ru/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=145
Привет, друзья!
Заказать документ института вы можете в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых университетов РФ. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР.
funnywipes.maxbb.ru/viewtopic.php?f=3&t=662
poltavagok.ru/poluchite-diplom-v-kratchayshie-sroki/
biketrials.ru/live/blog.php?b=9132
etoprosto.ru/ru/forum/?category=5&action=topic
toplentanews.ru/realnyie-diplomyi-dlya-realnyih-professionalov
Добрый день!
Где купить диплом специалиста?
Купить диплом о высшем образовании.
forexgroupx.ru/garantiya-polucheniya-diploma-byistro-i-nadezhno
купить диплом психология asxdiplomik.com .
сколько стоит диплом высшего образования diplomyx.com .
диплом доктора наук купить в москве https://www.diploms-x.com .
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашей компании.
diplomasx24.ru/kupit-diplom-magistra
Привет!
Где заказать диплом специалиста?
Купить диплом о высшем образовании.
xn—-8sbjufbbcmolbtcflf.xn--p1ai/gallery/image/1494-%D1%88%D0%B8%D1%80%D0%BE%D0%BA%D0%B8%D0%B9-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/?context=new
Сервисный центр Центр Тех Профи в Новосибирске выполнит ремонт серверов быстро и качественно. Наши мастера с более чем 5-летним опытом гарантируют ремонт всех известных брендов. Выезд курьера и ремонт на дому доступны для вашего комфорта. Гарантия до 6 месяцев на все услуги.
Бесплатный промокод на скидку, первый и повторный заказ 2024. Промокод на доставку. Акции и скидки. Халява в телеграм Скидка на повторный заказ
Привет, друзья!
Купить документ о получении высшего образования можно у нас в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, включая документы образца СССР.
indicouple.com/blogs/1174/Получите-диплом-без-лишних-забот-и-усилий
cn-stage-1.wmcloud.org/wiki/Реальные_дипломы_для_реальных_профессионалов
1001vieclam.forumvi.com/t9287-topic#9967
http://www.vocal.com.ua/node/62430
mirstalkera.4admins.ru/viewtopic.php?f=50&t=2111
Привет!
Приобрести документ института вы сможете в нашем сервисе.
ast-diplomy.com/otzyvy
Привет, друзья!
Где купить диплом по нужной специальности?
Наши специалисты предлагают быстро и выгодно купить диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Диплом пройдет любые проверки, даже при помощи профессиональных приборов. Решайте свои задачи быстро и просто с нашими дипломами.
Приобрести диплом любого ВУЗа.
afriprime.net/blogs/42045/%D0%9F%D0%BE%D0%B4%D1%80%D0%BE%D0%B1%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Добрый день!
Где приобрести диплом специалиста?
Заказать диплом любого ВУЗа.
http://www.fromrus.su/index.php?/gallery/image/325-%D0%BA%D0%B0%D0%BA-%D0%BD%D0%B0%D0%B9%D1%82%D0%B8-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%BC-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80%D0%BE%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2/
Привет!
Где купить диплом специалиста?
Мы можем предложить дипломы любых профессий по приятным ценам.
sadovod63.ru/products
Узнайте, как получить быстрый и безопасный доступ к своему аккаунту Mostbet через страницу входа на официальном сайте.
Добрый день!
Приобрести документ о получении высшего образования вы имеете возможность у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза.
power.ekafe.ru/viewtopic.php?f=2&t=1754
http://www.neymarfootballforum.com/read-blog/2013
balans.kz/bonus/
gess.flybb.ru/viewtopic.php?f=2&t=709
http://www.bideew.com/create-blog/
Здравствуйте!
Узнайте, как безопасно купить диплом о высшем образовании
ethnoglobus.az/index.php?subaction=userinfo&user=owujil
Рады оказать помощь!.
Привет, друзья!
Мы предлагаем дипломы любой профессии по выгодным тарифам.
yasqueencommunity.com/blogs/339/%D0%92%D1%8B%D0%B1%D0%B8%D1%80%D0%B0%D0%B5%D0%BC-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8
Воспользуйтесь промокодами Vavada казино для получения дополнительных привилегий. Эти коды обеспечат вам лучшие условия для игры.
Привет!
Купить диплом университета.
veneraroleplay.listbb.ru/viewtopic.php?f=4&t=289
Успешной учебы!
Здравствуйте!
Приобрести диплом любого университета
http://www.buzzakoo.com/blogs/766/%D0%92%D1%8B%D0%B1%D0%B8%D1%80%D0%B0%D0%B5%D0%BC-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B8-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0%D0%BC%D0%B8-%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8
Используйте промокоды Drip казино для получения дополнительных бонусов. Эти коды обеспечат вам лучшие условия для игры и увеличат ваши игровые возможности.
Здравствуйте!
Купить документ университета можно у нас в столице. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, любого года выпуска, включая документы старого образца.
mybaltika.info/ru/blogs/587/10348/
allnewstroy.ru/byistroe-oformlenie-diploma-lyuboy-spetsialnosti
obozrevatelevents.ru/garantirovannoe-poluchenie-diploma-bez-riska-i-problem/
irishpal.com/read-blog/921
http://www.hebergementweb.org/threads/diplom-dlja-karernogo-rosta-prosto-i-udobno.1487076/
Промокоды Vavada казино предоставляют игрокам уникальные бонусы. Используйте эти коды для увеличения своего игрового баланса и наслаждайтесь всеми привилегиями.
Добрый день!
Приобрести документ о получении высшего образования вы можете у нас.
ast-diplomas.com/otzyvy
Удачи!
Добрый день!
Мы изготавливаем дипломы любых профессий по невысоким тарифам.
astronomyfriends.com/read-blog/248_proverennyj-i-nadezhnyj-magazin-s-bolshim-vyborom-diplomov.html
http://prepaidcards.cvv2cvc.com
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://sale-clonedcards.cvv2cvc.com
Their progressive jackpots are recognized to have some of the highest
payouts of all Michigan on-line casinos.
Feel free to surf to my page 토토친구
Добрый день!
Приобрести диплом любого университета
hunmanby.uk/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%8D%D0%BB%D0%B5%D0%BA%D1%82%D1%80%D0%B8%D0%BA%D0%B0-%D0%B2-%D0%B5%D0%BA%D0%B0%D1%82%D0%B5%D1%80%D0%B8%D0%BD%D0%B1%D1%83/
Добрый день!
Мы готовы предложить дипломы любой профессии по невысоким тарифам.
woaibanli.com/%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B2%D0%B5%D1%82%D0%B5%D1%80%D0%B8%D0%BD%D0%B0%D1%80%D0%B8%D1%8F/
Привет!
Где приобрести диплом специалиста?
Наши специалисты предлагают выгодно и быстро купить диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями. Диплом способен пройти любые проверки, даже с использованием специальных приборов. Достигайте свои цели быстро и просто с нашей компанией.
Заказать диплом любого университета.
w0ols9cq0.fireblogz.com/59589372/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
tablets, making it convenient to play anywhere and anytime.
play aviator demo game
Привет!
Купить диплом любого ВУЗа
darkgate.pl/events/event/12-%D0%BF%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D0%B3%D0%BE%D1%80%D0%B0%D0%B7%D0%B4%D0%BE-%D0%B4%D0%B5%D1%88%D0%B5%D0%B2%D0%BB%D0%B5-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%83%D0%BD%D0%B8%D0%B2%D0%B5%D1%80%D1%81%D0%B8%D1%82%D0%B5%D1%82%D0%B0/
Здравствуйте!
Приобрести документ о получении высшего образования можно у нас в Москве.
ast-diplomy.com/kupit-diplom-nizhnij-novgorod
На сайте https://sochi.calypso.ooo/ у вас получится быстро отыскать и забронировать яхту, катер либо парусники. Компания насчитывает 20 филиалов, обслуживает более полутора тысяч клиентов в год. Все судна исправные, отличаются привлекательным, стильным дизайном. При этом заказать можно в любое, наиболее комфортное время и на несколько часов. Все ограничивается лишь вашими пожеланиями, предпочтениями. Этот сервис поможет вам подобрать наиболее подходящий вариант на прогулку, романтическое свидание или празднование торжества.
Добрый день!
Приобрести диплом ВУЗа.
Мы предлагаем документы ВУЗов, расположенных на территории всей РФ. Можно заказать диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они будут заверены необходимыми печатями и штампами.
network-66643.mn.co/posts/61838228
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Aseta panoksesi pin up online – suorain eliitin vedonvalittaja
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Привет!
Наша компания предлагает заказать диплом отличного качества, неотличимый от оригинального документа без использования дорогостоящего оборудования и квалифицированного специалиста.
xn--h1a1ab.xn--p1ai/index.php?name=account&op=info&uname=ubydajy
Хорошей учебы!
Здравствуйте!
Приобрести документ ВУЗа можно в нашей компании. Мы предлагаем документы об окончании любых ВУЗов России.
service.gepart.su/forum/?PAGE_NAME=profile_view&UID=4067
bazarweb.ru/forum.php?PAGE_NAME=profile_view&UID=31215
flowerwheel.synology.me/dokuwiki/doku.php?id=gosznacdiplomy
logo-def.ru/userinfo.php?uid=27948
rytmika-gdansk.pl/profile.php?lookup=30030
Добрый день!
Купить документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы получите диплом по любой специальности, включая документы образца СССР.
delta72.at.ua/forum/61-26766-1
school97.ru/vesti/view_profile.php?UID=210363
ya.2bb.ru/viewtopic.php?id=19602#p241124
http://www.pitomec.ru/forum/post/13042
u2c.tv/member.php?u=30984
Здравствуйте!
Купить диплом любого университета
Наша компания предлагает выгодно и быстро купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Документ способен пройти любые проверки, даже при помощи профессионального оборудования. Решайте свои задачи максимально быстро с нашим сервисом.
Где приобрести диплом специалиста?
ya.bestbb.ru/viewtopic.php?id=2962#p6549
vip.9bb.ru/viewtopic.php?id=5959#p9901
mkpnz.ru/users/8
autoprajs.ru/15204.html
worksale777.blogspot.com/2024/06/blog-post_30.html
Добрый день!
Полезные советы по покупке диплома о высшем образовании без риска
define.listbb.ru/viewtopic.php?f=46&t=516
Рады оказать помощь!.
Здравствуйте!
Купить диплом о высшем образовании.
Мы предлагаем документы ВУЗов, расположенных в любом регионе России. Можно заказать качественно сделанный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Документы будут заверены необходимыми печатями и подписями.
fbadult.com/blogs/2940/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Мы можем предложить дипломы психологов, юристов, экономистов и прочих профессий по доступным ценам. Цена будет зависеть от определенной специальности, года выпуска и образовательного учреждения.
arusak-diploms-srednee.ru/kupit-diplom-magistra
Успехов в учебе!
Привет, друзья!
Полезные советы по безопасной покупке диплома о высшем образовании
wiki.mysupp.ru/index.php?title=Оформление_диплома_под_ключ:_быстро_и_надежно
Рады помочь!.
Здравствуйте!
Приобрести диплом любого ВУЗа.
Мы предлагаем документы ВУЗов, расположенных на территории всей РФ. Можно купить диплом от любого заведения, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Документы выпускаются на бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригиналов. Документы будут заверены всеми необходимыми печатями и подписями.
forum.vipcs.pp.ua/gallery/image/318-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5/
Добрый день!
Мы можем предложить дипломы любых профессий по доступным тарифам. Цена зависит от выбранной специальности, года получения и образовательного учреждения.
arusak-diploms-srednee.ru/kupit-diplom-v-krasnoiarske
Успешной учебы!
На сайте https://podolog66.ru/ вы сможете записаться на прием к подологу. Среди основных услуг выделяют: избавление от стержневой мозоли, лечение трещин стопы, грибка ногтей на ногах, удаление вросшего ногтя. Медики помогут восстановить детские ногти, удалят бородавки. Все манипуляции являются полностью безболезненными, выполняются с использованием уникальных технологий, высококачественных средств. Уже сразу пациент чувствует существенное облегчение. Вы можете записаться на консультацию или процедуру в наиболее комфортное для себя время.
Промоакции и бонусы для игроков 1win Игроки всегда ищут способы увеличить свои шансы на выигрыш. Бонусные предложения и привлекательные акции помогают сделать игру более захватывающей http://www.vetreriameliante.it/index.php/kforum/jm-slideshow-module/9846-1#9846
Привет!
Узнайте стоимость диплома высшего и среднего образования и процесс получения
avtolux48.ru/people/user/374/blog/7916
Окажем помощь!.
Привет, друзья!
Где приобрести диплом по нужной специальности?
Мы можем предложить документы ВУЗов, расположенных на территории всей России. Вы имеете возможность купить диплом от любого заведения, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на “правильной” бумаге самого высшего качества. Это дает возможности делать государственные дипломы, которые не отличить от оригинала. Они будут заверены необходимыми печатями и штампами.
Мы можем предложить дипломы любой профессии по выгодным тарифам.
diploms-x.com/kupit-diplom-magistra
Рады помочь!
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
astart.pl/index.php?/gallery/image/5-%D0%B4%D0%BB%D1%8F-%D1%87%D0%B5%D0%B3%D0%BE-%D0%B2-%D0%BD%D0%B0%D1%88%D0%B5-%D0%B2%D1%80%D0%B5%D0%BC%D1%8F-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D1%8E%D1%82-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D1%8B-%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82/
Привет, друзья!
Приобрести документ университета вы сможете в нашей компании в столице.
ast-diplom.com/kupit-diplom-moskva
Хорошей учебы!
Привет!
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Цена будет зависеть от выбранной специальности, года получения и образовательного учреждения.
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge
Успехов в учебе!
Добрый день!
Приобрести документ о получении высшего образования вы имеете возможность в нашем сервисе. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любым специальностям, включая документы СССР.
http://www.nhps1914.com/wiki/Диплом_за_короткий_срок:_надежно_и_конфиденциально
forexgroupx.ru/garantiya-polucheniya-diploma-byistro-i-legko
http://www.fellnasen-service.de/index.php?thread/150215-диплом-мечты-легко-и-безопасно/
msfo-soft.ru/msfo/forum/user/40790/
bbarlock.com/index.php/Диплом_любой_профессии:_качественно_и_надежно
Добрый день!
Мы предлагаем купить диплом высокого качества, который невозможно отличить от оригинального документа без использования специального оборудования и опытного специалиста.
zamok.druzya.org/index.php?/topic/64271-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%86%D0%B5%D0%BD%D0%B0-p125n/
Успехов в учебе!
Привет!
Где приобрести диплом по нужной специальности?
Приобрести диплом любого университета.
vintfint.com/blogs/22173/%D0%9A%D0%B0%D0%BA-%D0%BF%D0%BE%D0%B4%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D1%8C-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B1%D0%BE%D0%BB%D1%8C%D1%88%D0%B8%D0%BC-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80%D0%BE%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2
Привет!
Купить документ о получении высшего образования вы сможете у нас в столице.
asxdiplomik.com/kupit-diplom-krasnoyarsk
Успехов в учебе!
Добрый день!
Купить документ ВУЗа вы можете у нас. Мы предлагаем документы об окончании любых университетов Российской Федерации.
wiki.hightgames.ru/index.php?title=premiummdiplomms
payhotel.ru/forum/messages/forum2/topic7566/message7822/?result=reply#message7822
http://www.gencotyre.com/comerblog/member.asp?action=view&memName=ixeqep
onlineboxing.net/jforum/user/profile/294128.page
xn—-8sbkkh5cbijf2k.xn--p1ai/index.php?option=com_k2&view=itemlist&task=user&id=53921
Привет!
Купить диплом любого ВУЗа
Наши специалисты предлагают быстро и выгодно купить диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Данный документ способен пройти любые проверки, даже с применением профессионального оборудования. Решайте свои задачи быстро с нашими дипломами.
Где приобрести диплом специалиста?
mosday.getbb.ru/viewtopic.php?f=12&t=1059
deviva.ru/viewtopic.php?id=8878#p61753
deviva.ru/viewtopic.php?id=8878#p61753
forumkk.listbb.ru/viewtopic.php?f=12&t=392
mosday.getbb.ru/viewtopic.php?f=12&t=1059
Добрый день!
Где приобрести диплом по актуальной специальности?
Приобрести диплом о высшем образовании.
http://www.yur-dom.ru/communication/forum/messages/forum3/message242/285-bolshoy-vybor-dokumentov-v-izvestnom-internet_magazine?result=new
Здравствуйте!
Купить диплом о высшем образовании
Наша компания предлагает выгодно и быстро купить диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Данный документ пройдет лубую проверку, даже с применением профессионального оборудования. Достигайте свои цели быстро и просто с нашим сервисом.
Где купить диплом по нужной специальности?
http://www.yagath.com/blogs/678070/%D0%9E%D1%81%D0%BD%D0%BE%D0%B2%D0%BD%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%85%D0%BE%D0%B4%D1%8B-%D1%80%D0%BE%D1%81%D1%81%D0%B8%D0%B9%D1%81%D0%BA%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%BE%D0%B8%D0%B7%D0%B2%D0%BE%D0%B4%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
realhindu.in/read-blog/4974
kfkfpxhkj.oblogation.com/27938939/%D0%9A%D0%B0%D0%BA-%D0%BF%D0%BE%D0%B4%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D1%8C-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8-%D0%9E%D0%B1%D0%B7%D0%BE%D1%80-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
http://www.kostromag.ru/forum/science/8933.aspx
burgasdent.listbb.ru/viewtopic.php?f=3&t=383
Привет, друзья!
Купить документ о получении высшего образования вы имеете возможность у нас.
ast-diplomas.com/kupit-diplom-voronezh
Привет!
Купить документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых университетов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы старого образца.
the-trifecta-network.mn.co/posts/62317841
pytalovo.4admins.ru/viewtopic.php?f=15&t=2362
a63.flybb.ru/viewtopic.php?f=16&t=3215
artrp.5nx.ru/viewtopic.php?f=3&t=9675
rentry.co/ipe5ww38
Интересно: ssd 500gb для ноутбука или кнопочные телефоны для пожилых
Может быть полезным: https://alikson.ru/umnye-chasy-1008/tag-zhenskie-smart-chasy/ или где купить электронную книгу
где купить планшет
Ещё можно узнать: чем полезны консервированные ананасы
Скачать музыку https://kissvk.top/ очень просто! Зайдите на сайт где вы найдете самые свежие композиции, музыку, альбомы, треки. Новинки 2024 и лучшая музыка за все годы, которую можно качать в mp3 абсолютно бесплатно и без регистрации. Самый большой сборник музыки в интернете для скачивания у нас на сайте.
Добрый день!
Купить диплом любого ВУЗа.
Мы предлагаем документы ВУЗов, которые находятся на территории всей России. Можно заказать диплом от любого заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге высшего качества. Это дает возможности делать государственные дипломы, которые не отличить от оригинала. Они заверяются всеми обязательными печатями и подписями.
ourfamilylync.com/read-blog/4419
Привет, друзья!
Где заказать диплом специалиста?
Купить диплом о высшем образовании.
logan.in.ua/people/user/7276/blog/7929/
Привет, друзья!
Купить документ о получении высшего образования вы можете у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любым специальностям, включая документы Советского Союза.
danceway74.ru/users/36
nalubyutemy.forum2x2.ru/t22712-topic#47907
skazka.g-talk.ru/viewtopic.php?f=1&t=1817
serialforfree.ru/diplomyi-ot-priznannyih-uchebnyih-zavedeniy
allnewstur.ru/legkiy-sposob-poluchit-diplom-bez-ekzamenov
dynamic features, and social elements, it offers an engaging experience for players. The game is supported by
aviator game demo
Сколько стоит диплом высшего и среднего образования и как его получить?
http://www.bisshogram.com/read-blog/259
купить диплом атисо asxdiplomik24.ru .
Добрый день!
Мы предлагаем быстро и выгодно купить диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Наш документ способен пройти любые проверки, даже при помощи специального оборудования. Достигайте свои цели быстро и просто с нашим сервисом.
remontmix.ru/forum/viewtopic.php?t=11607#p36760
Успехов в учебе!
Привет!
Приобрести диплом университета.
tonythang.dev/blogs/93/%D0%A7%D1%82%D0%BE-%D0%BC%D0%BE%D0%B6%D0%B5%D1%82-%D0%B2-%D0%BD%D0%B0%D1%88%D0%B5-%D0%B2%D1%80%D0%B5%D0%BC%D1%8F-%D0%BF%D1%80%D0%B5%D0%B4%D0%BE%D1%81%D1%82%D0%B0%D0%B2%D0%B8%D1%82%D1%8C-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8
Привет!
Приобрести документ о получении высшего образования вы сможете у нас в Москве.
ast-diplom.com/kupit-diplom-rostov-na-donu
Добрый день!
Где приобрести диплом специалиста?
Купить диплом любого ВУЗа.
myanimalgram.com/read-blog/352
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по невысоким тарифам.
gaysocial.gay/read-blog/79_vybiraem-nadezhnyj-internet-magazin-s-diplomami-i-attestatami.html?mode=day
Здравствуйте!
Мы изготавливаем дипломы любой профессии по выгодным тарифам. Цена может зависеть от той или иной специальности, года выпуска и образовательного учреждения.
arusak-diploms-srednee.ru/kupit-diplom-magistra
Успехов в учебе!
Привет!
Как получить диплом техникума с упрощенным обучением в Москве официально
moneysweet.listbb.ru/viewtopic.php?f=2&t=1934
Рады помочь!.
Привет!
Мы изготавливаем дипломы любой профессии по выгодным тарифам.
http://www.inlabs.la/%D1%83%D0%B4%D0%BE%D1%81%D1%82%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%B8%D0%B5-%D1%8E%D1%80%D0%B8%D1%81%D1%82%D0%B0/
купить диплом о образовании в москве цена купить диплом о образовании в москве цена .
Добрый день!
Приобрести диплом ВУЗа
amengram.com/blogs/337/%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D0%BA%D1%83%D0%B4%D0%B0-%D0%B4%D0%B5%D1%88%D0%B5%D0%B2%D0%BB%D0%B5-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%92%D0%A3%D0%97%D0%B0
Привет!
Купить документ университета вы можете в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза.
2cool.ru/qiwi-f215/poluchite-diplom-za-schitannie-dni-t3803.html
slliver.getbb.ru/viewtopic.php?f=62&t=944
mestovstrechi.flybb.ru/viewtopic.php?f=4&t=1284
graph.org/Diplomy-bez-ozhidaniya-i-slozhnostej-07-17
bestcoolfun.ru/poluchite-diplom-v-kratchayshie-sroki
Добрый день!
Где приобрести диплом специалиста?
caribbeantown.listbb.ru/viewtopic.php?f=5&t=502
Удачи!
Привет, друзья!
Мы изготавливаем дипломы любой профессии по невысоким ценам.
isig.ac.cd/alumni/blogs/37305/%D0%98%D1%89%D0%B5%D0%BC-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0%D0%BC%D0%B8-%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8
Привет, друзья!
Купить диплом ВУЗа
neurostarcheats.com/index.php?/gallery/image/28-%D0%BF%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D0%BD%D0%B0-%D0%BF%D0%BE%D1%80%D1%8F%D0%B4%D0%BE%D0%BA-%D0%B4%D0%B5%D1%88%D0%B5%D0%B2%D0%BB%D0%B5-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2%D1%83%D0%B7%D0%B0/
Здравствуйте!
Наш сервис предлагает купить диплом в высоком качестве, который не отличить от оригинала без участия специалистов высокой квалификации со сложным оборудованием.
xn—-7sbabja7ekbaahnetbi5o6b.xn--p1ai/profile.php?lookup=33184
Удачи!
Здравствуйте!
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по выгодным тарифам.
bharatpage.com/read-blog/575_nadezhnyj-internet-magazin-s-shirokim-assortimentom-diplomov.html
Здравствуйте!
Заказать диплом о высшем образовании
vxengine.ru/blogs/531/%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D0%BA%D1%83%D0%B4%D0%B0-%D0%B4%D0%B5%D1%88%D0%B5%D0%B2%D0%BB%D0%B5-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%92%D0%A3%D0%97%D0%B0
Привет!
Заказать диплом университета
Наши специалисты предлагают быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями должностных лиц. Наш диплом пройдет лубую проверку, даже при помощи специального оборудования. Достигайте свои цели максимально быстро с нашим сервисом.
Где заказать диплом специалиста?
kino.10bb.ru/viewtopic.php?id=163545#p276485
http://www.simplemachines.org/about/smf/stats.php
worksale777.blogspot.com/2024/06/blog-post_30.html
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
ya.2bb.ru/viewtopic.php?id=19040#p240217
купить диплом высшее образование нижний новгород ast-diplomas.com .
На сайте https://somovo-mebel.ru/catalog/gostinnye/ вы сможете приобрести функциональные, качественные гостиные, которые разработаны с особой заботой о покупателях и их комфорте. И самое важное, что соблюдаются все технологические процессы, внимание уделяется каждой детали. Предлагаются такие гостиные, которые полностью отвечают запросам и требованиям самого притязательного покупателя. Все гостиные выполнены из современных, высококачественных материалов, за счет чего мебель прослужит очень долго. Гостиные выполнены в самом разном стиле.
Привет, друзья!
Где заказать диплом по актуальной специальности?
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным тарифам.
http://www.mathemlib.ru/
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
orbita.com.py/blogs/313/%D0%92%D1%8B-%D1%85%D0%BE%D1%82%D0%B8%D1%82%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D1%83-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D0%BE%D0%B3%D0%BE-%D0%B8%D1%81%D0%BF%D0%BE%D0%BB%D0%BD%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%97%D0%B0%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5
Быстрое обучение и получение диплома магистра – возможно ли это?
ast-diplom.com/kupit-diplom-magistra
become our affiliate
https://affiliates.whalehunter.cash/track/Kirill.18AffRef.18AffRef.MAIN.0.0.0.0.0.0.0.0
Привет!
Где приобрести диплом специалиста?
Купить диплом университета.
w98804oc.beget.tech/2024/07/04/kak-nayti-proverennyy-internet-magazin-s-ogromnym-vyborom-diplomov.html
Здравствуйте!
Купить документ о получении высшего образования вы имеете возможность в нашей компании.
diplomyx.com/kupit-diplom-krasnoyarsk
Успехов в учебе!
Добрый день!
Приобрести диплом о высшем образовании.
Мы предлагаем документы ВУЗов, расположенных на территории всей РФ. Вы можете приобрести качественно напечатанный диплом от любого заведения, за любой год, включая сюда документы старого образца СССР. Документы выпускаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и подписями.
textualheritage.org/index.php?option=com_content&task=view&id=1081
Здравствуйте!
Как правильно приобрести диплом колледжа или ПТУ в России, важные моменты
kungur.hldns.ru/forum/profile.php?action=show&member=9614
Рады помочь!.
Привет, друзья!
Приобрести документ университета вы имеете возможность у нас. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы СССР.
chayka.ixbb.ru/viewtopic.php?id=147#p157
gazeta.ekafe.ru/viewforum.php?f=48
rabotavinternete.forum2x2.ru/t55638-topic#138418
terios2.ru/forums/index.php?autocom=gallery&req=si&img=3048
allsportime.ru/diplom-dlya-karernogo-rosta-prosto-i-udobno
Привет, друзья!
Мы изготавливаем дипломы любых профессий по приятным тарифам. Стоимость зависит от той или иной специальности, года получения и университета.
landik-diploms-srednee.ru/kupit-diplom-v-omske
Успехов в учебе!
Добрый день!
Приобрести диплом любого университета.
forumkasino.bestff.ru/viewtopic.php?id=4011#p9252
Успешной учебы!
Привет, друзья!
Купить диплом о высшем образовании.
Мы можем предложить документы техникумов, расположенных на территории всей России. Вы можете заказать качественно сделанный диплом от любого учебного заведения, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты печатаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригинала. Документы заверяются всеми обязательными печатями и штампами.
zz40k1bli.bleepblogs.com/28767199/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет, друзья!
Приобрести документ института можно в нашем сервисе.
ast-diplom.com/kupit-diplom-nizhnij-novgorod
Привет, друзья!
Как получить диплом техникума с упрощенным обучением в Москве официально
veniaminv.flybb.ru/viewtopic.php?f=1&t=2863
Окажем помощь!.
Добрый день!
Заказать документ университета можно в нашем сервисе.
ast-diplomas24.ru/kupit-diplom-nizhnij-novgorod
Удачи!
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по разумным ценам.
http://www.bigfootpodiatry.com.au/%D0%BA%D1%83%D0%BF%D0%BB%D1%8E-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE-%D0%B2%D1%8B%D1%81%D1%88%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8-%D1%80%D0%BE%D1%81/
Здравствуйте!
Заказать диплом о высшем образовании
newmanstrength.com/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%BE-%D0%B2%D1%8B%D1%81%D1%88%D0%B5%D0%BC-%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8-%D0%B5/
Добрый день!
Мы изготавливаем дипломы любых профессий по приятным ценам. Цена зависит от определенной специальности, года получения и образовательного учреждения.
landik-diploms-srednee.ru/svidetelstvo-o-rozhdenii
Хорошей учебы!
Здравствуйте!
Вопросы и ответы: можно ли быстро купить диплом старого образца?
4division.ru/viewtopic.php?f=13&t=8571
Рады помочь!.
Привет!
Приобрести документ ВУЗа вы имеете возможность в нашем сервисе.
asxdiplomik24.ru/kupit-diplom-krasnoyarsk
Успехов в учебе!
Привет, друзья!
Где приобрести диплом по необходимой специальности?
Мы предлагаем быстро купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Документ способен пройти любые проверки, даже с использованием специфических приборов. Решите свои задачи максимально быстро с нашим сервисом.
Купить диплом любого университета.
linkmate.mn.co/posts/61828981
Strategies and Tips
aviator game online
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
ast-diploms24.ru/kupit-diplom-rostov-na-donu
Добрый день!
Купить документ института можно в нашем сервисе.
diplomasx.com/kupit-diplom-o-srednem-obrazovanii
Хорошей учебы!
купить аттестаты за 9 ast-diploms.com .
Привет, друзья!
Купить диплом ВУЗа
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ пройдет лубую проверку, даже с использованием специально предназначенного оборудования. Решайте свои задачи быстро и просто с нашими дипломами.
Где купить диплом специалиста?
wiki.hightgames.ru/index.php/%D0%A7%D0%B5%D1%82%D1%8B%D1%80%D0%B5_%D0%BE%D1%81%D0%BD%D0%BE%D0%B2%D0%BD%D1%8B%D1%85_%D0%B3%D1%80%D1%83%D0%BF%D0%BF%D1%8B_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%BE%D0%B2,_%D0%BA%D0%BE%D1%82%D0%BE%D1%80%D1%8B%D0%B5_%D0%BF%D1%80%D0%BE%D0%B4%D0%B0%D1%8E%D1%82_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B
app-s.ru/blog/4_e_glavnykh_gruppy_onlajn_magazinov_chto_prodajut_diplomy/2024-07-07-1880
http://www.worldprettylady.com/read-blog/591
sngine.codiantprod.com/blogs/223/%D0%A1%D1%82%D0%BE%D0%B8%D0%BC%D0%BE%D1%81%D1%82%D1%8C-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D1%81%D0%BE%D0%B2%D0%B5%D1%82%D1%8B-%D0%B8-%D0%B0%D0%B2%D1%82%D0%BE%D1%80%D1%81%D0%BA%D0%B8%D0%B9-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%BE%D0%B2
gioturbobp.com/blogs/34/%D0%A0%D0%B5%D0%BA%D0%BE%D0%BC%D0%B5%D0%BD%D0%B4%D0%B0%D1%86%D0%B8%D0%B8-%D0%BF%D1%80%D0%BE%D1%84%D0%B5%D1%81%D1%81%D0%B8%D0%BE%D0%BD%D0%B0%D0%BB%D0%B0-%D0%BA%D0%BE%D1%82%D0%BE%D1%80%D1%8B%D0%B5-%D0%BF%D0%BE%D0%BC%D0%BE%D0%B3%D1%83%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
купил аттестат купил аттестат .
Добрый день!
Где купить диплом по нужной специальности?
Приобрести диплом любого ВУЗа.
p33340zg.beget.tech/2024/07/04/kak-podyskat-nadezhnyy-onlayn-magazin-s-ogromnym-katalogom-diplomov.html
Промоакции и бонусы для игроков 1win Игроки всегда ищут способы увеличить свои шансы на выигрыш. Бонусные предложения и привлекательные акции помогают сделать игру более захватывающей http://fr99659i.bget.ru/forum/showtopic-1932
Всё, что нужно знать о покупке аттестата о среднем образовании
ya.9bb.ru/viewtopic.php?id=5902#p11372
Привет!
Где заказать диплом по нужной специальности?
Приобрести диплом ВУЗа.
forum.sempiternalcommunity.ru/index.php?/gallery/image/19-%D0%BA%D0%B0%D0%BA-%D0%BD%D0%B0%D0%B9%D1%82%D0%B8-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%BC-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80%D0%BE%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2/
Откройте для себя лучшие финансовые решения на нашем сайте!
Что мы предлагаем?
Мы предоставляем разнообразные финансовые продукты: кредиты, банковские карты и займы, чтобы помочь вам достичь ваших целей и воплотить мечты в жизнь.
займы
Решения для любых целей
Планируете покупку жилья, автомобиля или образование? Наши кредитные программы подходят для любых нужд. Легко оформите кредит на нашем сайте, выбрав лучшие условия и сроки погашения.
Преимущества наших банковских карт
Наши банковские карты обеспечивают:
Удобство безналичных расчетов
Щедрые бонусы и привилегии
Оформите карту онлайн и получайте кэшбэк, скидки у партнеров и участие в программе лояльности. Выберите карту с оптимальными лимитами и условиями обслуживания для себя.
Быстрые займы на любые нужды
Не хватает денег до зарплаты или на неожиданные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок, чтобы вы могли решать финансовые вопросы без задержек.
Наши преимущества:
Простота и Удобство: Оформите заявку онлайн за считанные минуты.
Надежность и Прозрачность: Мы гарантируем честные условия и отсутствие скрытых комиссий.
Индивидуальный Подход: Мы учитываем ваши личные обстоятельства и предлагаем оптимальные условия.
Не упустите возможность улучшить свою финансовую ситуацию! Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и ощутите все преимущества работы с надежным финансовым партнером.
онлайн за
С нами ваши мечты станут реальностью!
купить диплом медицинского образования купить диплом медицинского образования .
диплом с занесением в реестр купить diplomyx.com .
Здравствуйте!
Заказать документ о получении высшего образования вы сможете в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любой специальности, включая документы старого образца.
msfo-soft.ru/msfo/forum/messages/forum24/topic10450/message297769/?result=new#message297769
heroes.app/blogs/new
newsbeautiful.ru/poluchite-diplom-v-kratchayshie-sroki/
mediamemorial.ru/club/user/125807/forum/message/3825/13307/#message13307
wegug.in/blogs/1120/Легальный-диплом-без-лишних-хлопот-узнайте-как
Добрый день!
Приобрести диплом университета.
Мы можем предложить документы ВУЗов, которые расположены в любом регионе Российской Федерации. Вы сможете заказать качественный диплом за любой год, включая документы старого образца СССР. Документы выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, которые не отличить от оригиналов. Документы заверяются необходимыми печатями и подписями.
forum.freaks.ro/index.php?/calendar/event/9-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D0%BE%D0%B9-%D1%81%D1%82%D0%BE%D0%B8%D0%BC%D0%BE%D1%81%D1%82%D0%B8/
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным ценам.
tygerspace.com/read-blog/5603_kak-najti-proverennyj-onlajn-magazin-kotoryj-prodaet-dokumenty.html?mode=day
saoirse ronan movies desert ridge moviesyellowstone season 1 episode summariestan france movies and tv showskim sung-soo movies and tv shows
Привет!
Приобрести документ института можно у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, включая документы Советского Союза.
nec.phorum.pl/posting.php?mode=newtopic&f=27&sid=b63a6b177997fd7a8d269632d7b56c97
baxoday.maxbb.ru/viewtopic.php?f=25&t=513
kolba.com.ua/index.php?topic=140911.new#new
foro.rune-nifelheim.com/general-ragnarok-m/vash-diplom-dlya-karernogo-rosta-dostupno-kazhdomu/
slliver.getbb.ru/viewtopic.php?f=62&t=944
Привет!
Мы готовы предложить дипломы любых профессий по выгодным тарифам. Цена будет зависеть от выбранной специальности, года получения и ВУЗа.
landik-diploms-srednee.ru/kupit-diplom-v-novosibirske
Успехов в учебе!
Здравствуйте!
Заказать диплом университета
Наши специалисты предлагают быстро купить диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями официальных лиц. Данный документ способен пройти лубую проверку, даже при помощи специального оборудования. Решите свои задачи максимально быстро с нашим сервисом.
Где приобрести диплом по нужной специальности?
vintfint.com/blogs/22309/%D0%A1%D0%BB%D1%83%D0%B6%D0%B1%D0%B0-%D0%BF%D0%BE%D0%B4%D0%B4%D0%B5%D1%80%D0%B6%D0%BA%D0%B0-%D0%B8-FAQ-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8
t98223u0.beget.tech/2024/07/09/nadezhnye-diplomy-s-garantiey-konfidencialnosti.html
woman.build2.ru/viewtopic.php?id=14514#p44579
fabnews.ru/forum/showthread.php?p=79708#post79708
buldingnews.ru/byistroe-oformlenie-diplomov-onlayn
Добрый день!
Мы готовы предложить дипломы любых профессий по выгодным ценам.
http://www.trngamers.co.uk/read-blog/1182_planiruete-kupit-attestat-u-nadezhnogo-proizvoditelya-zhdem-vas.html
[u][b] Привет![/b][/u]
[b]Как приобрести аттестат о среднем образовании в Москве и других городах [/b]
[url=http://allnewstur.ru/diplom-za-korotkiy-srok-nadezhno-i-konfidentsialno/]allnewstur.ru/diplom-za-korotkiy-srok-nadezhno-i-konfidentsialno[/url]
[u][b] Всегда вам поможем![u][b].
Добрый день!
Купить диплом университета
socialxtendr.com/blogs/167/%D0%9F%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%BE%D0%B3%D1%80%D0%BE%D0%BC%D0%BD%D1%8B%D0%BC-%D0%B0%D1%81%D1%81%D0%BE%D1%80%D1%82%D0%B8%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2
купить диплом по охране труда ast-diploms.com .
можно ли купить высшее образование можно ли купить высшее образование .
Попробуйте обратиться к газон мск, их основная сфера это газоны в рулонах, они знают свое ремесло.
Как правильно купить диплом колледжа и пту в России, подводные камни
http://www.rrsclub.ru/showthread.php?p=44657#post44657
Unique Features of the Aviator Game
aviator game
На сайте https://east-usa.com/index.html ознакомьтесь с подробной, актуальной информацией, которая касается карты Соединенных Штатов Америки. Только здесь представлена самая полная информация, которая вам обязательно пригодится для того, чтобы расширить кругозор. Перед вами подробная карта всех автомобильных дорог. Указаны и наиболее популярные достопримечательности, которые обязательно вас заинтересуют. Карта сгруппирована по следующим регионам: Средний Запад, Запад США, Юг США, Северо-восток.
Добрый день!
Приобрести диплом любого университета
Наша компания предлагает выгодно и быстро заказать диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями. Документ пройдет лубую проверку, даже при использовании специально предназначенного оборудования. Достигайте своих целей быстро с нашими дипломами.
Где приобрести диплом специалиста?
plszmhz31.collectblogs.com/73909116/%D0%A7%D0%B8%D1%82%D0%B0%D0%B9%D1%82%D0%B5-%D0%BD%D0%B0%D1%88-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80-%D0%B2-%D1%81%D0%BB%D1%83%D1%87%D0%B0%D0%B5-%D0%B5%D1%81%D0%BB%D0%B8-%D0%BD%D1%83%D0%B6%D0%BD%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8
vipka.mybb.ru/viewtopic.php?id=2886#p5059
http://www.soft-clouds.com/blogs/105701/%D0%A7%D1%82%D0%BE-%D1%82%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%B8%D0%B7-%D0%BE%D0%B1%D0%BE%D1%80%D1%83%D0%B4%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%B4%D0%BB%D1%8F-%D1%81%D0%BE%D0%B7%D0%B4%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D0%BE%D0%B3%D0%BE-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0
chrstms.ru/club/user/11503/blog/11062/
toplentanews.ru/nastoyashhie-diplomyi-legalno-i-konfidentsialno
Добрый день!
Где купить диплом по необходимой специальности?
Приобрести диплом о высшем образовании.
mysmart.ru/index.php?/gallery/image/652-%D0%BA%D0%B0%D0%BA-%D0%BD%D0%B0%D0%B9%D1%82%D0%B8-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%BC-%D0%B0%D1%81%D1%81%D0%BE%D1%80%D1%82%D0%B8%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2/
Привет!
Заказать документ о получении высшего образования вы можете в нашей компании.
diplomyx24.ru/kupit-diplom-rostov-na-donu
Хорошей учебы!
Привет, друзья!
Купить документ ВУЗа вы имеете возможность в нашей компании. Мы предлагаем документы об окончании любых университетов России.
balaklavskiy-16.ru/post/1530/#p1530
http://www.avatars.cc/member.php?action=showprofile&user_id=35196
mydnepr.pp.ua/forum/topic.php?forum=7&topic=941
gdz-fizika.ru/index.php?subaction=userinfo&user=ybiny
http://www.tdp74.ru/forum/messages/forum1/topic96/message47453/?result=reply#message47453
Добрый день!
Наша компания предлагает приобрести диплом отличного качества, который невозможно отличить от оригинала без использования дорогостоящего оборудования и квалифицированного специалиста.
eco-adamant.kz/index.php?subaction=userinfo&user=aqyjo
Удачи!
Как избежать рисков при покупке диплома колледжа или ПТУ в России
medik-look.ru/kupit-diplom-ekspress-dostavka
Добрый день!
Приобрести документ о получении высшего образования можно в нашей компании.
diploms-x.com/kupit-diplom-nizhnij-novgorod
Хорошей учебы!
Привет!
Купить диплом любого университета
Мы предлагаем выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ способен пройти лубую проверку, даже с использованием специфических приборов. Решите свои задачи быстро с нашими дипломами.
Где приобрести диплом по необходимой специальности?
meldog.3nx.ru/viewtopic.php?p=23387#23387
ya.10bb.ru/viewtopic.php?id=3615#p6544
autoprajs.ru/15204.html
vip.9bb.ru/viewtopic.php?id=5959#p9901
seriallove.bbok.ru/viewtopic.php?id=7015#p123048
mounjaro tirzepatide – препараты похудения инструкция, тирзепатид инструкция цена
Привет, друзья!
Заказать документ ВУЗа вы сможете у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза.
demo.4admins.ru/ucp.php?mode=resend_act&sid=56d5ced6597f36cf644550e216340435
severka.flybb.ru/viewtopic.php?f=6&t=376
ozmt.getbb.ru/viewtopic.php?f=21&t=1338
flashtest.80lvl.ru/viewtopic.php?f=3&t=1919
mymotospeed.ru/uspeh-bez-usiliy-poluchite-diplom-uzhe-segodnya
Привет, друзья!
Заказать документ о получении высшего образования можно в нашей компании в столице.
asxdiplomik.com/kupit-diplom-voronezh
Хорошей учебы!
Привет!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
http://www.lafornacella.com/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%B5%D1%80%D0%B5%D0%BA%D0%B2%D0%B0%D0%BB%D0%B8%D1%84%D0%B8%D0%BA%D0%B0%D1%86%D0%B8%D0%B8/
Здравствуйте!
Купить диплом о высшем образовании
rebornrpofficial.com/index.php?/files/file/8-%D0%B4%D0%BB%D1%8F-%D1%87%D0%B5%D0%B3%D0%BE-%D0%B2-%D0%BD%D0%B0%D1%88%D0%B5-%D0%B2%D1%80%D0%B5%D0%BC%D1%8F-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D1%8E%D1%82-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5/
Привет, друзья!
Купить документ о получении высшего образования вы сможете в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов России. Вы сможете получить диплом по любым специальностям, включая документы Советского Союза.
mynewsport.ru/vash-put-k-uspehu-diplom-bez-lishnih-zabot
molbiol.ru/forums/index.php?showtopic=1235712
l67697qa.beget.tech/2024/07/11/poluchite-diplom-bez-lishnih-zabot-i-usiliy.html
news1.listbb.ru/viewtopic.php?f=3&t=521
magazin.orgsoft.ru/communication/forum/index.php?PAGE_NAME=profile_view&UID=190538
view it now [url=https://wasabiwallet.io]wasabi wallet coinjoin[/url]
Привет!
Где приобрести диплом по необходимой специальности?
Мы готовы предложить документы институтов, которые находятся на территории всей РФ. Вы можете купить качественно напечатанный диплом от любого высшего учебного заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы делаются на “правильной” бумаге самого высокого качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Документы будут заверены всеми требуемыми печатями и штампами.
Мы изготавливаем дипломы любых профессий по выгодным тарифам.
ast-diplomas24.ru/kupit-diplom-magistra
Будем рады вам помочь!
На сайте http://eoknadveri.ru закажите звонок для того, чтобы приобрести пластиковые окна от производителя. Конструкции создаются из алюминия, ПВХ. На все предоставляется гарантия – 20 лет, ведь сотрудники предприятия уверены в своей работе. Отсутствует торговая надбавка. Доставка, замер, монтажные работы – все это выполняется тогда, когда удобно именно вам. При необходимости вы сможете воспользоваться бесплатной консультацией. Компания выполняет остекление балконов, квартир, фасадов, коттеджей.
купить диплом 1 день diplomyx.com .
https://karimmassimov.com/
karimmassimov.com ad6_557
Store Cloned cards Store Western Union Hacked Credit cards Buy Credit cards
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://hacked-cards.cvv2cvc.com buy hacked paypal
find trader joe
Добрый день!
Заказать документ университета вы можете в нашей компании.
ast-diplom24.ru/kupit-diplom-ekaterinbur
Удачи!
Добрый день!
Всё, что нужно знать о покупке аттестата о среднем образовании
v69-3.flybb.ru/viewtopic.php?f=8&t=583&sid=fcd968070c7ebeaa8bef398f95148abf
Всегда вам поможем!.
Добрый день!
Мы можем предложить документы техникумов, которые находятся на территории всей России. Вы сможете заказать диплом от любого заведения, за любой год, включая документы старого образца. Документы выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригинала. Документы будут заверены необходимыми печатями и подписями.
xbcbjlp5c.csublogs.com/34399881/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Купить документ института можно в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить диплом по любой специальности, включая документы Советского Союза.
kryza.network/create-blog/
http://www.les-ailes-chalaisiennes.com/forum/topic/диплом-любой-специальности-качестве/#postid-19484
http://www.les-ailes-chalaisiennes.com/forum/topic/диплом-любой-специальности-качестве/#postid-19484
wow-tour.ru/diplom-lyuboy-stepeni-i-spetsialnosti-dostupno-kazhdomu
fsmi.wiki/index.php?title=Гарантия_получения_диплома:_быстро_и_легко
The basic rule of the Aviator Game is straightforward: place a bet, watch the plane take off, and decide when to
aviator game
Привет, друзья!
Где приобрести диплом по нужной специальности?
Заказать диплом ВУЗа.
subscribe.ru/member/quick
Здравствуйте!
Процесс получения диплома стоматолога: реально ли это сделать быстро?
arusak-diploms-srednee.ru/kupit-diplom-v-rostove-na-donu
Успехов в учебе!
Добрый день!
Где заказать диплом специалиста?
Мы предлагаем документы институтов, расположенных в любом регионе России. Вы можете заказать диплом за любой год, включая документы СССР. Дипломы выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми обязательными печатями и штампами.
Мы изготавливаем дипломы любой профессии по приятным ценам.
ast-diplom24.ru/otzyvy
Поможем вам всегда!
Привет!
Реально ли приобрести диплом стоматолога? Основные этапы
pdapal.com/read-blog/929
Будем рады вам помочь!.
Здравствуйте!
Официальная покупка диплома вуза с сокращенной программой в Москве
landik-diploms-srednee.ru/kupit-diplom-v-novosibirske
Успешной учебы!
https://new.gruz200.kz/
купить диплом о среднем специальном образовании цена купить диплом о среднем специальном образовании цена .
купить диплом в симферополе diplomyx.com .
pop over to this web-site coinmarketcap
Привет!
Мы предлагаем документы ВУЗов, расположенных в любом регионе России. Вы имеете возможность купить качественно сделанный диплом за любой год, в том числе документы старого образца СССР. Документы делаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми требуемыми печатями и штампами.
f13zahtz2.idblogz.com/28765781/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет, друзья!
Приобрести диплом ВУЗа.
saluttunisia.com/jomsocial/groups/viewbulletin/270-kakie-internet-magaziny-s-diplomami-na-tekushchij-moment-imeyutsya.html?groupid=101
купить диплом ликвидированного вуза https://diploms-x.com/ .
Привет!
Официальная покупка диплома вуза с упрощенной программой обучения
arusak-diploms-srednee.ru/kupit-diplom-v-nizhnem-novgorode
Удачи!
Привет!
Где приобрести диплом специалиста?
Купить диплом ВУЗа.
mdkl.ru/blogs/9176/%D0%9E%D0%B3%D1%80%D0%BE%D0%BC%D0%BD%D1%8B%D0%B9-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Заказать документ о получении высшего образования вы можете в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить диплом по любым специальностям, включая документы СССР.
network.janenk.com/read-blog/734
balans.kz/bonus/
spletninews.ru/vash-nadezhnyiy-partner-v-poluchenii-diploma
http://www.noo.by/wiki/Получите_диплом,_о_котором_всегда_мечтали
forum.qwas.ru/idealniy-diplom-za-schitannie-dni-uznayte-podrobnosti-t20193.html
Здравствуйте!
Мы можем предложить дипломы психологов, юристов, экономистов и любых других профессий по выгодным тарифам.
angelicaleyva.es/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B0%D0%BC%D0%B1%D0%BE%D0%B2/
интернет магазин стройматериалов интернет магазин стройматериалов .
Привет!
Где купить диплом по нужной специальности?
elektrofahrrad-tests.de/forums/newthread.php?fid=2&processed=1
Хорошей учебы!
noticias
noticias
noticias
Наша компания является передовиком производства измерительного обрудования. Уже долгие годы мы производим и обслуживаем датчики температуры, логгеры данных, регистраторы температуры и влажности и термометры. Наше оборудование помогает осуществлять контроль параметров микроклимата в аптеках, на складах, на производствах и в магазинах логгер c
Привет!
Где заказать диплом специалиста?
Приобрести диплом ВУЗа.
berforum.ru/gallery/image/8670-kak-nayti-nadezhnyy-internet-magazin-s-bolshim-vyborom-diplomov/?context=new
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по выгодным ценам.
dervislergrup.com/events/event/13-4-klyucevyx-gruppy-internet-magazinov-realizuyushhix-diplomy/
Привет, друзья!
Полезная информация как официально купить диплом о высшем образовании.
Заказать диплом любого ВУЗа.
c2erwtinv.imblogs.net/78145827/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Добрый день!
Купить документ института вы сможете в нашем сервисе. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы получите необходимый диплом по любой специальности, любого года выпуска, в том числе документы образца СССР.
veniaminv.flybb.ru/viewtopic.php?f=1&t=2897
re-port.ru/users/52316/
akademiyavodopad.ru/forum/messages/forum7/topic425/message740/?result=new#message740
carbonfacesocial.org/blogs/79109/Получите-диплом-в-кратчайшие-сроки
kingcityrp.moibb.ru/viewtopic.php?f=34&t=469
Привет, друзья!
Где купить диплом по необходимой специальности?
Мы предлагаем дипломы любых профессий по разумным ценам.
iclicky.com/index.php?do=/public/user/blogs/name_Alanpoe/page_5/
Добрый день!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
http://www.growingchurches.org/blogs/21881/%D0%9A%D0%B0%D0%BA-%D0%BF%D0%BE%D0%B4%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D1%8C-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%87%D1%82%D0%BE-%D0%BF%D1%80%D0%BE%D0%B4%D0%B0%D0%B5%D1%82-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B
Привет!
Мы изготавливаем дипломы любых профессий по приятным ценам.
http://www.immigrantofamerica.club/blogs/1371/%D0%9D%D0%B0-%D1%87%D1%82%D0%BE-%D0%B2%D0%BD%D0%B8%D0%BC%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D0%B8%D1%82%D1%8C-%D0%BF%D1%80%D0%B8-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
he has a good point https://jaxxliberty.io/
Здравствуйте!
Где купить диплом по нужной специальности?
Купить диплом любого университета.
chrstms.ru/club/user/11503/blog/11039/
Привет!
Заказать документ института вы сможете у нас. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, включая документы образца СССР.
comptonrpp.listbb.ru/viewtopic.php?f=6&t=726
mkpnz.ru/users/8
study.flybb.ru/viewtopic.php?f=4&t=424
rogerfilms.com/index.php?title=Купите_диплом_и_улучшите_свое_будущее
registraciavsaita.listbb.ru/viewtopic.php?f=2&t=627
ремонт мобильных телефонов
Здравствуйте!
Заказать документ университета можно в нашем сервисе.
diplomyx24.ru/kupit-diplom-sankt-peterburg
Успешной учебы!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
ast-diploms.com/kupit-diplom-sankt-peterburg
Добрый день!
Быстрое обучение и получение диплома магистра – возможно ли это?
tirana.social/blogs/1010/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
Интеграция мультимедийных систем Интеграция мультимедийных систем .
Здравствуйте!
Наша компания предлагает быстро приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Данный диплом пройдет любые проверки, даже при использовании профессиональных приборов. Достигайте своих целей быстро и просто с нашей компанией.
moskovskij.getbb.ru/viewtopic.php?f=12&t=2231
Успехов в учебе!
диплом о высшем профессиональном образовании купить диплом о высшем профессиональном образовании купить .
Привет!
Приобрести диплом любого университета.
newsbig.wpsuo.com/na-cto-obrasat-vnimanie-pri-zakaze-dokumentov-v-internete
Добрый день!
Всё, что нужно знать о покупке аттестата о среднем образовании
http://www.vladmines.dn.ua/forum/index.php/topic,38575.0.html
Рады оказаться полезными!.
Завод «Таку» с 2010 года занимается производством металлоконструкций на заказ по собственным проектам и чертежам заказчиков. Наши строительные бригады в короткие сроки построят быстровозводимое здание из металлоконструкций в соответствии с вашими требованиями. Реализовать любой проект быстро и в срок нам помогают: использование технологий сверхточного изготовления, стандартизированного подхода к маркировке, упаковке и контроль качества. https://psk-taku.ru
Привет, друзья!
Как получить диплом о среднем образовании в Москве и других городах.
Заказать диплом о высшем образовании.
andreieusebiu.net/files/file/50-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D0%BE%D0%B9-%D1%81%D1%82%D0%BE%D0%B8%D0%BC%D0%BE%D1%81%D1%82%D0%B8/
Привет, друзья!
Заказать документ о получении высшего образования можно в нашей компании в Москве.
diplomasx24.ru/otzyvy
Успешной учебы!
Здравствуйте!
Реально ли приобрести диплом стоматолога? Основные этапы
whatson.plus/blogs/16346/%D0%A1-%D1%83%D0%BC%D0%BE%D0%BC-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D1%8D%D0%BA%D1%81%D0%BF%D0%B5%D1%80%D1%82%D0%BD%D1%8B%D0%B9-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
Several key developers and companies have played a significant role in the development and success of the
aviator game online
Добрый день!
Купить диплом о высшем образовании.
alanyatoday.ru/users/76
Удачи!
Привет!
Где купить диплом по необходимой специальности?
aboutalltour.ru/ofitsialnyiy-diplom-lyuboy-spetsialnosti/
Удачи!
Добрый день!
Где купить диплом по необходимой специальности?
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по выгодным тарифам.
medinkur.ru/index.php
Of course, it is not for everyone butt it iis
worth a look at whoever you are.
Feel free to visit my webpage … 토토모아
Привет, друзья!
Мы изготавливаем дипломы любой профессии по доступным ценам.
ffxiv.one/blogs/134/%D0%92%D1%8B-%D1%85%D0%BE%D1%82%D0%B8%D1%82%D0%B5-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%83-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%BE%D0%B8%D0%B7%D0%B2%D0%BE%D0%B4%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%97%D0%B0%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5
teams aand win Slot No cost Play.
Look at my web blog: 온카
Наша команда уже более 20 лет проектирует, возводит и обслуживает бассейны в Тюмени, Челябинске и Екатеринбурге. Мы используем только современное и проверенное оборудование и материалы. Даем гарантию выполненных работ. Кроме этого, мы являемся официальными поставщиками химии для бассейнов лучших мировых марок изготовление каркасных бассейнов
Добрый день!
Сколько стоит получить диплом высшего и среднего образования легально?
victorians123.com/blogs/203/%D0%9D%D0%B0-%D1%87%D1%82%D0%BE-%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D0%B8%D1%82%D1%8C-%D1%81%D0%B2%D0%BE%D0%B5-%D0%B2%D0%BD%D0%B8%D0%BC%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D1%80%D0%B8-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B5-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8
Привет!
Официальная покупка диплома ВУЗа с упрощенной программой обучения.
Купить диплом университета.
http://www.vocal.com.ua/node/62355
look here jaxx wallet io
balforum.net
Привет, друзья!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
arusak-diploms-srednee.ru/kupit-diplom-v-rostove-na-donu
Хорошей учебы!
купить диплом университета в екатеринбурге ast-diploms.com .
Добрый день!
Мы предлагаем документы ВУЗов, расположенных на территории всей Российской Федерации. Можно заказать качественно сделанный диплом от любого заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высшего качества. Это дает возможность делать государственные дипломы, которые не отличить от оригиналов. Они заверяются всеми обязательными печатями и подписями.
es8sqmemx.free-blogz.com/75583808/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
купить диплом об окончании вуза купить диплом об окончании вуза .
Привет, друзья!
Как безопасно купить диплом колледжа или ВУЗа в России, что важно знать
epistles.ru/blogs/1552/Получите-диплом-без-лишних-забот-и-усилий
Поможем вам всегда!.
Привет!
Приобрести документ университета вы имеете возможность в нашей компании в столице. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы старого образца.
macadamlab.ru/wiki/index.php?title=Ваш_путь_к_успеху:_диплом_на_заказ
http://www.hashtap.com/@artur.sh/купите-диплом-и-получите-новые-возможности-DjgZmqR6njw0
u90517ol.beget.tech/2024/07/11/kupite-diplom-i-zabudte-o-studencheskih-problemah.html
ffxiv.one/blogs/157/Ваш-диплом-без-лишних-забот-быстро-и-безопасно
meat.ntnn.ru/personal/profile/index.php?register=yes
Добрый день!
Где заказать диплом специалиста?
Приобрести диплом о высшем образовании.
eurodelo.ru/vash-diplom-bez-truda-i-usiliy
aparthome.org
Добрый день!
Узнайте, как приобрести диплом о высшем образовании без рисков
slavsbyt.ru/index.php?subaction=userinfo&user=ytukih
Будем рады вам помочь!.
По запросу лучшая доставка еды переходите на наш онлайн сайт. На сайте можно посмотреть наше меню, оформить заказ, заказать столик или позвонить нам. Контактный телефон +7(3412)223-225 или оформляйте заказ сразу на сайте. В разделе «доставка готовых блюд» откроется наше гастрономическое меню. Обратите своё внимание на подачу при заказе, это результат большого опыта повара. Приготовление также у нас специальное, поэтому можете быть уверены перед заказом на особенный вечер.
Здравствуйте!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
arusak-diploms-srednee.ru/kupit-attestat-za-11-klass
Успешной учебы!
микроавтобус Армения или Гватемальская каменная голова
организация
https://samoylovaoxana.ru/tag/turizm/
Ещё можно узнать: падающие звезды что это
Ночная жизнь
Привет, друзья!
Мы предлагаем документы техникумов, расположенных на территории всей России. Вы можете заказать диплом за любой год, включая сюда документы СССР. Документы выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригинала. Они заверяются необходимыми печатями и штампами.
a90275db.beget.tech/2024/07/09/otlichnye-rascenki-i-vysokoe-kachestvo-zakazyvay-diplomy-onlayn.html
Привет, друзья!
Диплом техникума купить официально с упрощенным обучением в Москве
minecraftcommand.science/forum/general/topics/32e2f553-a525-485a-b5fd-5e96b7fe548d
Всегда вам поможем!.
срочно отремонтировать телефон
Привет!
Приобрести диплом о высшем образовании.
owen.ru/forum/member.php?u=106526
Успехов в учебе!
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
traquegarden.com/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D0%B3%D1%83%D0%BF%D1%81/
Привет, друзья!
Мы можем предложить документы ВУЗов, расположенных в любом регионе России. Вы имеете возможность заказать качественный диплом за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Документы заверяются всеми требуемыми печатями и подписями.
p-release.ru/services/pokupaem-diplom-v-izvestnom-onlajn-magazine-po-komfortnoj-cene
Привет, друзья!
Приобрести документ ВУЗа можно у нас.
asxdiplomik24.ru/kupit-diplom-krasnoyarsk
Успехов в учебе!
Добрый день!
Официальное получение диплома техникума с упрощенным обучением в Москве
forums.unigild.com/index.php?/topic/15181-гарантия-получения-диплома-быстро-и-надежно
Рады оказаться полезными!.
Online casino games have surged in popularity due to their convenience and the immersive experience they offer.
plinko online
Привет!
Мы можем предложить дипломы любой профессии по приятным тарифам.
domainrama.com/read-blog/822_nadezhnyj-magazin-s-obshirnym-vyborom-dokumentov.html
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
http://www.lifecapadvisors.com/%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0-%D0%BA%D0%BE%D0%BB%D0%BB%D0%B5%D0%B4%D0%B6%D0%B0-1997-2003-%D1%84%D0%BE%D1%82%D0%BE/
Привет!
Где купить диплом специалиста?
Заказать диплом любого ВУЗа.
itach-soft.com/club/user/6/blog/999/
Привет!
Где заказать диплом по необходимой специальности?
Мы можем предложить дипломы любой профессии по выгодным ценам. Стоимость зависит от выбранной специальности, года получения и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы документы были доступны для большинства наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-novosibirske
Удачи!
Привет!
Заказать документ о получении высшего образования можно в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР.
rodme.ru/vash-diplom-za-korotkoe-vremya-prosto-i-udobno-t12717.html
epistles.ru/blogs/1600/Получите-диплом-за-считанные-дни
sec31.ru/posting.php?mode=post&f=25
antennastar.com/blogs/540/Надежные-дипломы-для-вашего-успеха
bohhchaos.listbb.ru/viewtopic.php?f=9&t=8421
Привет, друзья!
Где заказать диплом по необходимой специальности?
Приобрести диплом университета.
astart.pl/index.php?/gallery/image/6-%D0%B1%D0%BE%D0%BB%D1%8C%D1%88%D0%BE%D0%B9-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам.
mychatclup.com/blogs/92/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D1%81%D0%B5%D0%B3%D0%BE%D0%B4%D0%BD%D1%8F-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8?lang=en_us
Привет, друзья!
Где заказать диплом по актуальной специальности?
Мы предлагаем дипломы любых профессий по приятным тарифам. Стоимость может зависеть от той или иной специальности, года получения и образовательного учреждения. Стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы дипломы были доступными для большого количества наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge
Успехов в учебе!
Продвижение сайта в поисковых системах Яндекс, Google. Гарантия выполненных работ. Бесплатный аудит сайта Раскрутка сайта
Добрый день!
Заказать документ о получении высшего образования можно в нашей компании в Москве.
diplomasx.com/kupit-diplom-omsk
Здравствуйте!
Где приобрести диплом специалиста?
Заказать диплом любого университета.
linkthere.club/read-blog/8550
Здравствуйте!
Приобрести документ ВУЗа можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых университетов РФ. Вы получите необходимый диплом по любой специальности, включая документы образца СССР.
newmedtime.ru/diplom-pod-klyuch-byistro-kachestvenno-bezopasno
http://www.bisound.com/forum/showthread.php?p=772499#post772499
vseogirls.ru/byistroe-poluchenie-diploma-vash-shans-na-uspeh
netcallvoip.com/wiki/index.php/Диплом_мечты_без_учебы_и_экзаменов
http://www.mnogozip.ru/forum/user/23852/
Добрый день!
Приобрести документ о получении высшего образования вы можете у нас. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы получите необходимый диплом по любой специальности, включая документы Советского Союза.
mybaltika.info/ru/blogs/587/10399/
stalinarch.ru/wiki/index.php/Оформление_диплома_под_ключ:_качественно_и_быстро
datasphere.ru/club/user/15/blog/
odincovoschool16.flybb.ru/viewtopic.php?f=2&t=839
dianov.bget.ru/forum/thread58364.html#1302122
Здравствуйте!
Где приобрести диплом по нужной специальности?
Приобрести диплом о высшем образовании.
wiki.3cdr.ru/wiki/index.php/%D0%9E%D0%B3%D1%80%D0%BE%D0%BC%D0%BD%D1%8B%D0%B9_%D0%B0%D1%81%D1%81%D0%BE%D1%80%D1%82%D0%B8%D0%BC%D0%B5%D0%BD%D1%82_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2_%D0%B2_%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Добрый день!
Где заказать диплом по актуальной специальности?
Мы изготавливаем дипломы любых профессий по доступным тарифам. Стоимость может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступны для большого количества наших граждан.
arusak-diploms-srednee.ru/kupit-diplom-medicinskogo-uchilishha
Удачи!
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность у нас.
diplomyx24.ru/kupit-diplom-vracha
Привет, друзья!
Приобрести документ института вы можете в нашей компании в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы образца СССР.
reflections.listbb.ru/viewtopic.php?f=45&t=752
a90275db.beget.tech/2024/07/16/poluchite-diplom-v-kratchayshie-sroki.html
epicit.ru/vash-diplom-nasha-zabota
eurodelo.ru/poluchite-diplom-o-kotorom-vsegda-mechtali
aviapoisk.getbb.ru/viewtopic.php?f=27&t=756
Сколько стоит диплом высшего и среднего образования и как его получить?
diploms-x.com/otzyvy
Здравствуйте!
Приобрести диплом ВУЗа
Наша компания предлагает выгодно купить диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Наш диплом способен пройти лубую проверку, даже с использованием профессиональных приборов. Решайте свои задачи быстро с нашей компанией.
Где заказать диплом по нужной специальности?
l67697qa.beget.tech/2024/07/08/legkiy-vybor-magazina-prodayuschego-diplomy.html
filmbaaz.in/blogs/932/%D0%9F%D1%80%D0%B0%D0%B2%D0%B8%D0%BB%D1%8C%D0%BD%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5-%D1%8D%D0%BA%D1%81%D0%BF%D0%B5%D1%80%D1%82%D0%BD%D1%8B%D0%B9-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
gti-club.ru/forum/member.php?u=23001
http://www.markusragger.at/chess/index.php/kforum/jm-news-pro-module/651988
http://www.sledopit.club/wiki/index.php/%D0%9A%D0%B0%D0%BA%D0%B8%D0%B5_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D1%8B_%D1%81_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8_%D0%BD%D0%B0_%D1%82%D0%B5%D0%BA%D1%83%D1%89%D0%B8%D0%B9_%D0%B4%D0%B5%D0%BD%D1%8C_%D0%B8%D0%BC%D0%B5%D1%8E%D1%82%D1%81%D1%8F%3F
Привет, друзья!
Приобрести документ ВУЗа можно в нашей компании в столице.
asxdiplomik24.ru/kupit-diplom-magistra
диплом юриста образец с оценками диплом юриста образец с оценками .
Привет, друзья!
Мы можем предложить документы ВУЗов, которые расположены на территории всей Российской Федерации. Вы имеете возможность приобрести диплом за любой год, включая документы старого образца СССР. Документы делаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются необходимыми печатями и подписями.
perfectohub.com/read-blog/7811
Добрый день!
Как избежать рисков при покупке диплома колледжа или ВУЗа в России
forum.gorodsalavat.ru/posting.php?mode=post&f=28&sid=8a9dbd3e9b1487d02c9ff579aee07eed
Будем рады вам помочь!.
Добрый день!
Где купить диплом по нужной специальности?
Заказать диплом любого ВУЗа.
russianecuador.com/forum/member.php?u=13207
Добрый день!
Приобрести документ о получении высшего образования можно в нашем сервисе. Мы предлагаем документы об окончании любых университетов Российской Федерации.
tucmas.fi/phpBB/viewtopic.php?f=4&t=201911
ashinova.ru/blog/ahurup.html
http://www.tdp74.ru/forum/messages/forum1/topic96/message47787/?result=reply#message47787
tastys-food.ru/profile.php?u=epybyg
m9-com.ru/forums/viewtopic.php?f=21&t=411&p=319394#p319394
Привет, друзья!
Купить документ ВУЗа можно в нашей компании в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР.
komfort.rusff.me/viewtopic.php?id=13950#p41118
phileo.me/blogs/new
poetzinc.com/read-blog/11711
msfo-soft.ru/msfo/forum/messages/forum24/topic10394/message292502/?result=new#message292502
yourealtynews.ru/gotovyiy-diplom-bez-dolgih-let-obucheniya
Привет!
Мы можем предложить дипломы любой профессии по приятным тарифам.
hpconsultants.nl/2024/06/30/%D0%BC%D0%B5%D0%B4%D0%B8%D1%86%D0%B8%D0%BD%D1%81%D0%BA%D0%B8%D0%B9-%D1%81%D0%B5%D1%80%D1%82%D0%B8%D1%84%D0%B8%D0%BA%D0%B0%D1%82-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0/
Привет, друзья!
Купить диплом любого ВУЗа
Наша компания предлагает выгодно и быстро заказать диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Наш диплом способен пройти любые проверки, даже при использовании специфических приборов. Достигайте своих целей максимально быстро с нашей компанией.
Где купить диплом специалиста?
vaeaem.profiforum.ru/t3822-topic#7107
lsfiredept.listbb.ru/viewtopic.php?f=2&t=396
3drus.ru/forum/topic_34806
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
blogs.rufox.ru/~worksale/47159.htm
Привет!
Где купить диплом специалиста?
Мы можем предложить документы институтов, расположенных в любом регионе России. Можно заказать диплом от любого высшего учебного заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы делаются на “правильной” бумаге самого высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригинала. Документы заверяются необходимыми печатями и штампами.
Мы изготавливаем дипломы любых профессий по доступным тарифам.
asxdiplomik.com/kupit-diplom-magistra
Всегда вам поможем!
Добрый день!
Где приобрести диплом по актуальной специальности?
Приобрести диплом ВУЗа.
nfrb.pl/index.php?/gallery/image/51-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%B9-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
If you think through poiskmonet.com every detail, you can achieve effective results.
Воспользуйтесь промокодами Vavada казино для увеличения своего игрового баланса. Эти коды обеспечат вам доступ к эксклюзивным бонусам и привилегиям.
Приобретение диплома ПТУ с сокращенной программой обучения в Москве
diplomyx24.ru/kupit-diplom-ekaterinbur
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Детская одежда оптом из Турции
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Уже не удивительно, что кондиционеры становятся неотъемлемым элементом наших домов и офисов. Именно поэтому мы рады предложить вам широкий выбор кондиционеров от лучших мировых брендов по доступным ценам в нашем магазине Enter в Кишиневе кондиционер купить
Привет!
Купить диплом любого ВУЗа
Мы предлагаем выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Данный документ способен пройти любые проверки, даже с использованием специальных приборов. Решите свои задачи максимально быстро с нашей компанией.
Где купить диплом специалиста?
vevqegzer.blog5.net/70054318/%D0%A5%D0%BE%D1%82%D0%B8%D1%82%D0%B5-%D0%B2%D1%8B%D1%8F%D1%81%D0%BD%D0%B8%D1%82%D1%8C-%D0%BA%D0%B0%D0%BA-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%96%D0%B4%D0%B5%D0%BC-%D0%92%D0%B0%D1%81
hellsms.com/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=6634
wheeoo.com/read-blog/13425
lebanonhub.app/blogs/2406/%D0%9A%D0%B0%D0%BA-%D0%BF%D0%BE%D0%B4%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D1%8C-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8-%D0%9E%D0%B1%D0%B7%D0%BE%D1%80-%D0%BE%D1%82-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
o91707v5.beget.tech/2024/07/08/kupit-diplom-bez-posrednikov-legko-i-bezopasno.html
Промокоды Drip казино обеспечивают игрокам доступ к эксклюзивным бонусам. Эти коды делают игру более выгодной и увлекательной.
Добрый день!
Приобрести документ университета можно в нашей компании. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, включая документы СССР.
itstagram.ru/read-blog/851
igrosoft.getbb.ru/ucp.php?mode=login&sid=ce3ac93b3e49bfe0de7e1adf67545027
http://www.nhps1914.com/wiki/Официальный_диплом_любой_профессии:_быстро_и_надежно
heroes.app/blogs/428782/Ваш-путь-к-успеху-начинается-с-диплома
rosen.moibb.ru/viewtopic.php?f=2&t=504
Промокоды Vavada казино открывают доступ к уникальным бонусам и привилегиям. Эти коды помогают игрокам наслаждаться игрой и улучшенными условиями.
Добрый день!
Ьожем предложить документы ВУЗов, расположенных в любом регионе России. Вы можете заказать диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Документы печатаются на бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Документы будут заверены всеми необходимыми печатями и штампами.
Мы готовы предложить дипломы любых профессий по выгодным тарифам. Стоимость может зависеть от той или иной специальности, года получения и университета. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступными для подавляющей массы граждан.
arusak-diploms-srednee.ru/kupit-diplom-v-nizhnem-novgorode
Хорошей учебы!
Привет, друзья!
Заказать документ о получении высшего образования вы имеете возможность у нас в столице.
ast-diploms24.ru/kupit-diplom-rostov-na-donu
Хорошей учебы!
Reliability. Concluding an agreement allows sveto-copy.com you to avoid unpleasant situations and obtain a guarantee of high-quality work.
Каталог вакансий – Ваш надежный источник по поиску работы
Найдите свою идеальную работу с Категорией вакансий! Мы предлагаем обширную базу данных вакансий из различных отраслей и регионов.
курьер на автомобиле
С нами вы сможете:
Просматривать актуальные объявления о вакансиях.
Фильтровать результаты по местоположению, отрасли и ключевым словам.
Создать персонализированные оповещения, чтобы быть в курсе новых возможностей.
Сохранять и сравнивать вакансии для удобства
складские работы
Загружать резюме одним щелчком мыши, чтобы подать заявку на интересующие вакансии.
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
Оформи заявку на кредитную карту от лучших банков России онлайн
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
<a href=http://www.bnsud.com/files/phpinfo.php?a%5B%5D=оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
Добрый день!
Предлагаем документы ВУЗов, расположенных в любом регионе Российской Федерации. Можно приобрести качественно напечатанный диплом от любого учебного заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригиналов. Документы будут заверены необходимыми печатями и штампами.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по разумным тарифам. Цена может зависеть от конкретной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас важно, чтобы дипломы были доступны для большого количества граждан.
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske
Успехов в учебе!
По запросу где заказать еду ижевск переходите на указанный онлайн портал. На сайте возможно увидеть наше меню, оформить заказ, забронировать столик или позвонить нам. Контактный телефон +7(3412)223-225 или оформляйте заказ сразу на сайте. В разделе «доставка готовых блюд» будет доступно наше гастрономическое меню. Обратите своё внимание на подачу при заказе, это результат большого опыта повара. Приготовление также у нас уникальное, следовательно можете не сомневаться перед заказом на праздник.
Здравствуйте!
Купить документ о получении высшего образования можно у нас.
diploms-x.com/kupit-diplom-voronezh
Удачи!
Привет!
Наша компания предлагает купить диплом отличного качества, неотличимый от оригинального документа без участия специалиста высокой квалификации со сложным оборудованием.
193.16.101.6/index.php?title=diploman
Удачи!
Здравствуйте!
Приобрести документ института можно в нашей компании в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации.
gdz-fizika.ru/index.php?subaction=userinfo&user=asijuzuhe
forum.hayabusa-club.ru/member.php?u=17955
arskland.ru/people/user/15814/
onlineboxing.net/jforum/user/profile/295635.page
test.sozapag.ru/forum/user/243251/
Привет!
Купить диплом о высшем образовании
Наша компания предлагает выгодно приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Данный диплом способен пройти лубую проверку, даже при помощи специально предназначенного оборудования. Решайте свои задачи быстро и просто с нашей компанией.
Где купить диплом специалиста?
forumjustwoman.getbb.ru/viewtopic.php?f=43&t=941
lsfiredept.listbb.ru/viewtopic.php?f=2&t=396
antonovschool.ru/forum/messages/forum1/topic650/message665/?result=new#message665
ilovehabbo.bbon.ru/viewtopic.php?id=1459#p28856
forum.qwas.ru/kupit-diplom-t19852.html
Добро пожаловать на наш сайт! Откройте лучшие финансовые решения прямо сейчас!
Наши предложения
Мы предлагаем широкий ассортимент финансовых продуктов: кредиты, банковские карты и займы, чтобы помочь вам достичь ваших целей и воплотить мечты в реальность.
автокредит
Кредиты для всех нужд
Планируете покупку жилья, автомобиля или образование? Наши кредитные программы созданы для вас. Оформите кредит на нашем сайте за несколько минут, выбрав лучшие условия и сроки погашения.
Преимущества наших банковских карт
Наши карты обеспечивают удобство безналичных платежей и множество бонусов:
– **Кэшбэк и скидки у партнеров**
– **Программа лояльности**
Оформите карту онлайн и получите все преимущества уже сегодня!
Быстрые займы для непредвиденных расходов
Нужны деньги до зарплаты или на неожиданные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок.
дебетовая карта с возможностью снятия наличных
Наши преимущества:
– **Простота и Удобство:** Оформите заявку онлайн за считанные минуты.
– **Надежность и Прозрачность:** Честные условия без скрытых комиссий.
– **Индивидуальный Подход:** Мы учитываем ваши личные обстоятельства.
Не упустите шанс улучшить свою финансовую ситуацию! Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
Переходите на наш сайт и сделайте шаг к своим мечтам!
Привет, друзья!
Готовы предложить документы ВУЗов, расположенных на территории всей РФ. Вы сможете заказать диплом от любого заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Они заверяются необходимыми печатями и штампами.
Мы изготавливаем дипломы любой профессии по разумным ценам. Стоимость зависит от конкретной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступны для большого количества граждан.
landik-diploms-srednee.ru/svidetelstvo-o-razvode
Успехов в учебе!
Добрый день!
Мы готовы предложить документы техникумов, расположенных на территории всей РФ. Можно заказать диплом за любой год, включая документы СССР. Документы печатаются на бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Документы заверяются всеми требуемыми печатями и подписями.
iwasocial.com/read-blog/279
Competitive Tournaments and Events
play plinko online
Здравствуйте!
Мы готовы предложить дипломы любой профессии по доступным ценам.
foro.rune-nifelheim.com/general-ragnarok-m/diplomy-ot-veduschih-vuzov-strany/
Процесс получения диплома стоматолога: реально ли это сделать быстро?
diplomyx.com/kupit-diplom-nizhnij-novgorod
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании.
ast-diplom.com/kupit-diplom-voronezh
Успехов в учебе!
Добрый день!
Купить документ института вы сможете у нас. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, любого года выпуска, включая документы старого образца. Даем 100% гарантию, что в случае проверки документов работодателями, никаких подозрений не возникнет.
ringturbine.com/index.php/%D0%97%D0%B0_%D1%81%D1%87%D0%B5%D1%82_%D1%87%D0%B5%D0%B3%D0%BE_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D1%8B_%D1%81_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%B0%D0%BC%D0%B8_%D1%81%D1%82%D0%BE%D0%BB%D1%8C_%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D1%8B%3F
socialnetwork.cloudyzx.com/read-blog/11234
http://www.mirmafii.ru/article/7553
http://www.pitomec.ru/forum/post/12960
mamuli.club/forum/topic/24674/
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Детская одежда оптом из Турции
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Привет, друзья!
Как быстро получить диплом магистра? Легальные способы
talkitter.com/create-blog
Будем рады вам помочь!.
Привет, друзья!
Купить диплом любого университета
Наши специалисты предлагают выгодно заказать диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Наш диплом пройдет любые проверки, даже при использовании специально предназначенного оборудования. Достигайте цели быстро и просто с нашими дипломами.
Где купить диплом по нужной специальности?
8fdwq80wb.blogcudinti.com/28234812/%D0%9A%D0%B0%D0%BA-%D0%BD%D0%B0%D0%B9%D1%82%D0%B8-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8-%D0%9E%D0%B1%D0%B7%D0%BE%D1%80-%D1%81%D0%BF%D0%B5%D1%86%D0%B8%D0%B0%D0%BB%D0%B8%D1%81%D1%82%D0%B0
heroes.app/blogs/new
panther.80lvl.ru/index.php
http://www.cyberpinoy.net/create-blog/
mediamemorial.ru/club/user/125807/forum/message/3793/13275/#message13275
Здравствуйте!
Полезные советы по безопасной покупке диплома о высшем образовании
ads.6ocity.net/%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BA%D0%B0%D0%BD%D0%B4%D0%B8%D0%B4%D0%B0%D1%82%D0%B0-%D0%BD%D0%B0%D1%83%D0%BA-%D1%84%D0%BE%D1%82%D0%BE/
Привет, друзья!
Мы можем предложить документы техникумов, которые находятся в любом регионе РФ. Вы имеете возможность заказать диплом от любого учебного заведения, за любой год, в том числе документы старого образца СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и подписями.
meco.eeconme.com/read-blog/3900
Добрый день!
Мы изготавливаем дипломы любой профессии по разумным ценам.
toplentanews.ru/oformlenie-diploma-onlayn-za-neskolko-shagov
купить диплом кандидата наук в москве ast-diploms.com .
купить документы купить документы .
Здравствуйте!
Как получить диплом техникума с упрощенным обучением в Москве официально
ashinova.ru/category-5/t-1709.html#1709
Окажем помощь!.
[u][b] Привет, друзья![/b][/u]
[b]Где купить диплом специалиста?[/b]
Мы готовы предложить дипломы любой профессии по приятным ценам. Стоимость может зависеть от конкретной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас очень важно, чтобы документы были доступны для большинства граждан.
[b]Для вас изготавливаем дипломы[/b] любых профессий по разумным тарифам.
[url=http://webnewsrealty.ru/kupit-diplom-rf-v-moskve-ofitsialnoe-oformlenie-i-dostupnyie-tsenyi]webnewsrealty.ru/kupit-diplom-rf-v-moskve-ofitsialnoe-oformlenie-i-dostupnyie-tsenyi[/url]
[u][b] Рады помочь![u][b].
Привет!
Где приобрести диплом по необходимой специальности?
Заказать диплом любого университета.
astart.pl/index.php?/gallery/image/6-%D0%B1%D0%BE%D0%BB%D1%8C%D1%88%D0%BE%D0%B9-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
Привет!
Купить документ о получении высшего образования вы имеете возможность в нашей компании.
ast-diploms24.ru/otzyvy
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
Оформи заявку на кредитную карту от лучших банков России онлайн
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
купить дипломы техникума недорого https://diploms-x.com/ .
Здравствуйте!
Наша компания предлагает быстро и выгодно купить диплом, который выполняется на оригинальном бланке и заверен печатями, штампами, подписями должностных лиц. Данный документ способен пройти любые проверки, даже с применением профессионального оборудования. Решите свои задачи максимально быстро с нашими дипломами.
blackpearlbasketball.com.au/index.php?option=com_k2&view=itemlist&task=user&id=843309
Успехов в учебе!
Здравствуйте!
Легальная покупка диплома ПТУ с сокращенной программой обучения
http://www.oneartevents.com/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B3%D0%B8%D0%BD%D0%B5%D0%BA%D0%BE%D0%BB%D0%BE%D0%B3%D0%B0/
Выбор ритуального агентства — важный этап в организации похорон. Ознакомьтесь с моей статьей о ритуальных услугах в Алматы, чтобы узнать, как найти качественные услуги по разумной цене.
Привет!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании в Москве.
ast-diplomas.com/kupit-diplom-nizhnij-novgorod
Привет!
Заказать документ ВУЗа вы можете у нас в столице. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любой специальности, включая документы старого образца. Даем 100% гарантию, что при проверке документов работодателем, каких-либо подозрений не появится.
epistles.ru/blogs/1518/Быстрое-Оформление-Дипломов-Надежно-и-Легально
anamaliya.ru/otzyvy/blagodarya-chemu-magaziny-s-dokumentami-tak-vostrebovany-i-populyarny
http://www.xrated.social/blogs/146/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D1%81%D0%B5%D0%B9%D1%87%D0%B0%D1%81-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8
forumkasino.bestff.ru/viewtopic.php?id=4193#p9574
telegra.ph/Legkij-vybor-magazina-chto-prodaet-diplomy-07-08
купить дипломы в красноярске недорого asxdiplomik24.ru .
Привет, друзья!
Где приобрести диплом специалиста?
Приобрести диплом любого университета.
anahnu.club/jomsocial/groups/viewbulletin/10113-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%B9-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5.html?groupid=1
Привет!
Заказать документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, включая документы образца СССР.
moneycool.bestbb.ru/search.php?action=search&keywords=&author=&forum=-1&search_in=all&sort_by=0&sort_dir=DESC&show_as=topics&search=%CE%F2%EF%F0%E0%E2%E8%F2%FC
worksale.jofo.me/2279120.html?_ga=2.37554784.1980467973.1720785836-642113533.1720785836
git.fuwafuwa.moe/thomasshaw9688/My-List/issues/new
good-serial.ru/2024/07/byistraya-pomoshh-v-oformlenii-diplomov/
human.forumieren.de/t305-topic#373
Привет!
Мы готовы предложить дипломы любых профессий по доступным ценам. Цена может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику цен. Для нас очень важно, чтобы документы были доступны для большого количества наших граждан.
johnathanmian16047.nytechwiki.com/9724164/%D0%9D%D0%B0%D0%BF%D1%80%D0%B0%D0%B2%D0%BB%D0%B5%D0%BD%D0%B8%D1%8F_%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2_%D0%BE%D0%B1_%D0%BE%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D0%B8_%D0%B2_%D0%BD%D0%B0%D1%81%D1%82%D0%BE%D1%8F%D1%89%D0%B5%D0%BC_%D0%BE%D0%B1%D1%89%D0%B5%D1%81%D1%82%D0%B2%D0%B5
Привет!
Заказать диплом любого ВУЗа.
gioturbobp.com/blogs/33/%D0%92%D0%B0%D0%B6%D0%BD%D1%8B%D0%B5-%D1%81%D0%BE%D0%B2%D0%B5%D1%82%D1%8B-%D0%BF%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B5%D0%BD%D0%B8%D1%8E-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность у нас.
ast-diplom24.ru/kupit-diplom-ekaterinbur
Buy Cloned Cards Shop Cloned cards
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://sale-cloned-cards.co.in
Здравствуйте!
Официальная покупка диплома вуза с сокращенной программой обучения в Москве
http://www.benedeek.com/blogs/86604/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%9B%D1%8E%D0%B1%D1%8B%D1%85-%D0%92%D1%83%D0%B7%D0%BE%D0%B2-%D0%B8-%D0%9D%D0%B0%D0%BF%D1%80%D0%B0%D0%B2%D0%BB%D0%B5%D0%BD%D0%B8%D0%B9
В критические моменты жизни важно, чтобы похоронное бюро было надежным и профессиональным. Наша статья поможет вам разобраться в разнообразии ритуальных услуг в Алматы и выбрать агентство, которое предложит качественное обслуживание по разумной цене Читайте здесь
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любой специальности, включая документы СССР. Гарантируем, что при проверке документов работодателем, подозрений не возникнет.
Мы можем предложить дипломы любой профессии по невысоким тарифам. Цена зависит от конкретной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для большинства граждан.
phobia.lt/index.php?/gallery/image/127-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%86%D0%B5%D0%BD%D0%BA%D0%B8-%D0%B8-%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Рады помочь!
Здравствуйте!
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по доступным тарифам.
http://www.manchestercityclubs.com/read-blog/252_ishem-nadezhnyj-onlajn-magazin-s-diplomami.html
Добрый день!
Приобрести документ о получении высшего образования можно в нашей компании в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любым специальностям, включая документы старого образца.
v69-3.flybb.ru/viewtopic.php?f=8&t=593
angelladydety.getbb.ru/posting.php?mode=post&f=46&sid=b5a6d6eb6f550c94590d409fdbba5bc4
ballinthe6.ca/blogs/new
g95334gq.beget.tech/2024/07/15/professionalnye-diplomy-dlya-vseh-otrasley.html
itstagram.ru/read-blog/844
Недавно столкнулся с необходимостью организации похорон и был поражен тем, насколько завышены цены на ритуальные услуги в Алматы. Многие агентства скрывают реальные расходы и добавляют скрытые комиссии, что вызывает недовольство и финансовые трудности. Чтобы избежать таких проблем, настоятельно рекомендую ознакомиться с нашим блогом. Мы подробно рассматриваем, как формируются цены на ритуальные услуги и какие подводные камни могут ждать вас при выборе агентства. Узнайте, как выбрать надежное агентство с прозрачной ценовой политикой и избежать переплат.
Привет!
Где купить диплом специалиста?
forum-pravo.com.ua/member.php?u=10249
Хорошей учебы!
Добрый день!
Как получить диплом техникума с упрощенным обучением в Москве официально.
Купить диплом университета.
drawing-tips-and-anime-manga-discussion.mn.co/posts/61837935
Здравствуйте!
Где приобрести диплом по необходимой специальности?
Мы готовы предложить документы институтов, которые находятся на территории всей Российской Федерации. Можно заказать диплом от любого ВУЗа, за любой год, включая документы СССР. Дипломы делаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они заверяются всеми обязательными печатями и штампами.
Мы можем предложить дипломы любых профессий по выгодным тарифам.
ast-diplomas24.ru/kupit-diplom-omsk
Окажем помощь!
купить диплом моряка ast-diploms.com .
Привет, друзья!
Где приобрести диплом по необходимой специальности?
Мы можем предложить дипломы любой профессии по приятным ценам. Стоимость зависит от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику тарифов. Важно, чтобы дипломы были доступны для подавляющей массы граждан.
Для вас готовы предложить дипломы любых профессий по приятным тарифам.
newspromworld.ru/kupit-diplom-rf-v-moskve-legalno-i-byistro
Окажем помощь!.
почему купить диплом diplomasx.com .
Добрый день!
Мы предлагаем дипломы любой профессии по приятным тарифам.
respectmyopinion.com/blogs/28/%D0%9D%D0%B0-%D1%87%D1%82%D0%BE-%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D0%B8%D1%82%D1%8C-%D0%B2%D0%BD%D0%B8%D0%BC%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D1%80%D0%B8-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82
лифтовое оборудование заказать
Добрый день!
Мы готовы предложить документы ВУЗов, которые расположены в любом регионе России. Можно заказать диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригиналов. Документы заверяются необходимыми печатями и подписями.
savico.com.br/read-blog/257
Интересно: видеокарта geforce rtx 4070 ti или кнопочные телефоны с доставкой
Может быть полезным: https://alikson.ru/noutbuki-1001/tag-igrovye-noutbuki/ или смартфоны с большим экраном
мощные системные блоки
Ещё можно узнать: не открывается xml файл в internet explorer
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным ценам. Стоимость зависит от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику цен. Для нас важно, чтобы документы были доступными для большинства граждан.
mysterybookmarks.com/story17097523/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BA%D0%BE%D0%BB%D0%BB%D0%B5%D0%B4%D0%B6%D0%B0
Здравствуйте!
Ьожем предложить документы техникумов, расположенных в любом регионе России. Можно приобрести диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы заверяются необходимыми печатями и штампами.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Цена зависит от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную ценовую политику. Важно, чтобы документы были доступны для большого количества граждан.
arusak-diploms-srednee.ru/diplom-sredne-spetcialnoe-obrazovanie
Удачи!
Добрый день!
Легальная покупка школьного аттестата с упрощенной программой обучения
pdlspd.listbb.ru/viewtopic.php?f=3&t=462
Окажем помощь!.
Здравствуйте!
Купить документ о получении высшего образования вы сможете у нас в Москве.
diplomasx24.ru/kupit-diplom-o-srednem-obrazovanii
Добрый день!
Готовы предложить документы техникумов, расположенных в любом регионе России. Можно купить качественно напечатанный диплом за любой год, в том числе документы старого образца СССР. Документы делаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и штампами.
Мы изготавливаем дипломы любой профессии по доступным ценам. Цена может зависеть от выбранной специальности, года получения и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы документы были доступны для большого количества граждан.
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske
Успешной учебы!
Привет!
Где приобрести диплом специалиста?
Мы можем предложить дипломы любой профессии по приятным тарифам. Стоимость может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для подавляющей массы граждан.
Для вас изготавливаем дипломы любых профессий по невысоким тарифам.
keepnitreal.net/blogs/57956/%D0%9A%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%A0%D0%A4-%D0%B2-%D0%9C%D0%BE%D1%81%D0%BA%D0%B2%D0%B5?lang=ru_ru
Окажем помощь!.
Здравствуйте!
Заказать документ института можно в нашей компании в столице.
diploms-x.com/kupit-diplom-moskva
Успешной учебы!
Добрый день!
Всё, что нужно знать о покупке аттестата о среднем образовании.
Купить диплом любого ВУЗа.
wiki.intradition.ru/index.php/%D0%92%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D1%8B%D0%B5_%D1%86%D0%B5%D0%BD%D1%8B_%D0%B8_%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5_%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE_-_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD!
Привет!
Мы изготавливаем дипломы любой профессии по приятным ценам.
itbitgroup.ru/legkiy-sposob-priobresti-diplom-onlayn
купить заполненное приложение к диплому ast-diploms.com .
To start working as a etalonsadforum.com walking or bicycle courier, just contact one of the partner companies.
купить егэ аттестат купить егэ аттестат .
Добрый день!
Где купить диплом специалиста?
Заказать диплом ВУЗа.
yottamuch.com/index.php?/gallery/image/116-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%B9-%D0%B0%D1%81%D1%81%D0%BE%D1%80%D1%82%D0%B8%D0%BC%D0%B5%D0%BD%D1%82-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
Привет!
Купить документ о получении высшего образования вы имеете возможность в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы сможете получить диплом по любой специальности, включая документы СССР. Гарантируем, что в случае проверки документов работодателем, каких-либо подозрений не появится.
Мы можем предложить дипломы любой профессии по разумным ценам. Цена зависит от конкретной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступны для большого количества граждан.
musicianforums.net/index.php?/gallery/image/145-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5/
Рады помочь!
Здравствуйте!
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков
bx24.avers35.ru/company/personal/user/38/blog/691/
Поможем вам всегда!.
Здравствуйте!
Купить документ университета можно у нас в Москве.
diplomyx24.ru/kupit-diplom-moskva
Успехов в учебе!
Добрый день!
Предлагаем документы техникумов, которые находятся в любом регионе РФ. Вы можете приобрести качественно напечатанный диплом от любого учебного заведения, за любой год, включая сюда документы СССР. Документы выпускаются на “правильной” бумаге самого высокого качества. Это дает возможность делать настоящие дипломы, не отличимые от оригинала. Они будут заверены всеми требуемыми печатями и штампами.
Мы изготавливаем дипломы любой профессии по доступным ценам. Цена зависит от выбранной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы документы были доступны для большого количества наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe
Удачи!
Привет!
Приобрести диплом о высшем образовании.
inderculturaputumayo.gov.co/6522-2
Удачи!
Привет!
Мы изготавливаем дипломы любой профессии по приятным ценам.
wegoflc.com/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%82%D0%BE%D0%BB%D1%8C%D1%8F%D1%82%D1%82%D0%B8/
Привет!
Где приобрести диплом специалиста?
Мы можем предложить документы ВУЗов, расположенных в любом регионе России. Вы можете купить диплом от любого ВУЗа, за любой год, включая документы СССР. Дипломы выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригинала. Они будут заверены всеми обязательными печатями и подписями.
Мы изготавливаем дипломы любых профессий по приятным тарифам.
diplomyx.com/kupit-diplom-moskva
Всегда вам поможем!
Здравствуйте!
Заказать документ о получении высшего образования можно у нас.
ast-diploms.com/kupit-diplom-omsk
Удачи!
Привет!
Как оказалось, купить диплом кандидата наук не так уж и сложно
lsfiredept.listbb.ru/viewtopic.php?f=2&t=448
Поможем вам всегда!.
Добрый день!
Мы изготавливаем дипломы любой профессии по приятным ценам.
sontopic.com/blogs/1741/%D0%9F%D0%BE%D0%BB%D1%83%D1%87%D0%B8%D1%82%D0%B5-%D0%9D%D0%B0%D1%81%D1%82%D0%BE%D1%8F%D1%89%D0%B8%D0%B9-%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B7%D0%B0-%D0%9A%D0%BE%D1%80%D0%BE%D1%82%D0%BA%D0%B8%D0%B9-%D0%A1%D1%80%D0%BE%D0%BA
Высокие коэффициенты на спортивные события | Надежные ставки на 1win | 1win поможет вам достичь цели | Стань частью 1win| Начни выигрывать с 1win| 1win делает игру насыщенной и интересной| 1win – это мир больших выигрышей| 1win – выбор успешных игроков| 1win – это высокие шансы на выигрыш| 1win – это надежность и качество
1win зеркало [url=https://1win-bk.by/]https://1win-bk.by/[/url] .
Привет!
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по выгодным ценам. Цена будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы дипломы были доступными для большинства наших граждан.
hectorlndo03579.ouyawiki.com/668930/%D0%A2%D0%B5%D0%BD%D0%B4%D0%B5%D0%BD%D1%86%D0%B8%D0%B8_%D0%B8_%D1%82%D0%B5%D0%BD%D0%B4%D0%B5%D0%BD%D1%86%D0%B8%D0%B8_%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0_%D1%83%D1%87%D0%B5%D0%BD%D1%8B%D1%85_%D1%81%D1%82%D0%B5%D0%BF%D0%B5%D0%BD%D0%B5%D0%B9_%D0%B2_%D1%81%D0%BE%D0%B2%D1%80%D0%B5%D0%BC%D0%B5%D0%BD%D0%BD%D0%BE%D0%BC_%D0%BC%D0%B8%D1%80%D0%B5
Добрый день!
Купить документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, включая документы образца СССР.
pesnibardov.ru/f/viewtopic.php?f=2&t=212479
place-e.ru/index.php/Реальные_дипломы_для_реальных_профессионалов
forum.safe-animals.ru/index.php?showtopic=32014
vintfint.com/blogs/22839/Диплом-в-кратчайшие-сроки-качественно-и-безопасно
mirniy.flybb.ru/viewtopic.php?f=37&t=795
Добрый день!
Мы предлагаем документы техникумов, расположенных в любом регионе РФ. Вы сможете приобрести качественный диплом за любой год, включая документы СССР. Документы печатаются на бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и штампами.
derivsocial.org/read-blog/2556
Привет, друзья!
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
make-coin.ru/diplom-pod-klyuch-kachestvenno-i-bezopasno
Рады оказаться полезными!.
Привет, друзья!
Официальная покупка аттестата о среднем образовании в Москве и других городах
http://www.omaada.com/blogs/120017/%D0%93%D1%80%D0%B0%D0%BC%D0%BE%D1%82%D0%BD%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
Привет, друзья!
Где купить диплом по актуальной специальности?
Заказать диплом любого ВУЗа.
drevtorg.xyz/profiles/blogs/6382903:BlogPost:356801
Здравствуйте!
Реально ли приобрести диплом стоматолога? Основные шаги.
Заказать диплом ВУЗа.
rm7s812fz.wizzardsblog.com/28306958/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет!
Приобрести документ о получении высшего образования можно в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы Советского Союза. Даем гарантию, что в случае проверки документов работодателями, подозрений не возникнет.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным ценам. Цена зависит от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для клиентов адекватную политику цен. Для нас очень важно, чтобы дипломы были доступны для подавляющей массы наших граждан.
http://www.xrated.social/blogs/149/%D0%94%D0%B5%D1%82%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
Рады помочь!
Привет!
Мы предлагаем документы техникумов, расположенных на территории всей России. Вы имеете возможность купить диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригиналов. Документы будут заверены всеми обязательными печатями и штампами.
z3jg9tht3.blogstival.com/50751400/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Имея в виду гастрономический ресторан переходите на указанный онлайн ресурс. На сайте можно увидеть наше меню, оформить заказ, зарезервировать столик или позвонить нам. Контактный телефон +7(3412)223-225 или оформляйте заказ прямо на сайте. В тематике «доставка готовых блюд» откроется наше полное меню. Обратите своё внимание на оформление блюда при заказе, это настоящее искусство. Приготовление также у нас нестандартное, следовательно можете быть уверены перед заказом на особенный вечер.
Здравствуйте!
Где купить диплом по нужной специальности?
Купить диплом любого университета.
indungii.ro/forum/index.php?/gallery/image/5-%D0%BA%D0%B0%D0%BA-%D0%BF%D0%BE%D0%B4%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D1%8C-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B9-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%BE%D0%B3%D1%80%D0%BE%D0%BC%D0%BD%D1%8B%D0%BC-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80%D0%BE%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2/
Добрый день!
Купить диплом магистра оказалось возможно, быстрое обучение и диплом на руки
blog.nataraj.ru/~/Interest/Получите диплом без лишних забот и усилий
Рады оказать помощь!.
Добрый день!
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями официальных лиц. Наш документ способен пройти любые проверки, даже с использованием специального оборудования. Решите свои задачи максимально быстро с нашими дипломами.
epidemics.ru/index.php?subaction=userinfo&user=okezaju
Хорошей учебы!
Здравствуйте!
Где приобрести диплом по необходимой специальности?
Мы готовы предложить документы ВУЗов, расположенных в любом регионе России. Можно приобрести качественно напечатанный диплом от любого ВУЗа, за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы печатаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы заверяются всеми требуемыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по разумным ценам.
ast-diplomy.com/kupit-diplom-krasnoyarsk
Рады помочь!
Привет, друзья!
Готовы предложить документы ВУЗов, которые находятся в любом регионе РФ. Вы сможете приобрести качественный диплом за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты делаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригиналов. Они заверяются всеми требуемыми печатями и штампами.
Мы изготавливаем дипломы любых профессий по доступным ценам. Стоимость может зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас очень важно, чтобы дипломы были доступными для большого количества наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-novosibirske
Успехов в учебе!
купить диплом о среднем специальном образовании тольятти asxdiplomik24.ru .
Здравствуйте!
Мы готовы предложить документы техникумов, которые находятся в любом регионе России. Вы сможете купить качественно напечатанный диплом от любого заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются необходимыми печатями и подписями.
alivechrist.com/read-blog/213
Привет!
Где заказать диплом по нужной специальности?
Приобрести диплом о высшем образовании.
ls.co-x.ru/2024/07/04/kak-nayti-nadezhnyy-onlayn-magazin-s-obshirnym-assortimentom-diplomov.html
купить медицинский диплом в оренбурге diploms-x.com .
Привет!
Купить документ университета вы сможете у нас в столице.
diploms-x24.ru/kupit-diplom-krasnoyarsk
Добрый день!
Приобрести диплом любого университета.
backshowtime.ru/kupit-diplom-otzyivyi-i-garantii
Добрый день!
Заказать документ института вы имеете возможность в нашей компании в столице.
ast-diploms.com/kupit-diplom-rostov-na-donu
Успешной учебы!
The Best Movies on Netflix to Watch Right Now in June 2024 aruvi serial today episode youtubewhat movies to stream todaysturgeon season oregontick tock film
https://slothacker62.com/
Здравствуйте!
Приобрести диплом любого ВУЗа
Наши специалисты предлагают быстро и выгодно приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями должностных лиц. Наш документ способен пройти лубую проверку, даже при использовании специально предназначенного оборудования. Достигайте цели быстро и просто с нашей компанией.
Где заказать диплом по необходимой специальности?
fatshipresident.net/read-blog/259
lighttur.ru/ofitsialnyie-diplomyi-s-garantiey-podlinnosti
http://www.xpertmapping.com/%d1%87%d1%82%d0%be-%d0%bd%d1%83%d0%b6%d0%bd%d0%be-%d0%b4%d0%bb%d1%8f-%d1%81%d0%be%d0%b7%d0%b4%d0%b0%d0%bd%d0%b8%d1%8f-%d0%ba%d0%b0%d1%87%d0%b5%d1%81%d1%82%d0%b2%d0%b5%d0%bd%d0%bd%d0%be%d0%b3%d0%be/
karkadan.ru/users/77829
http://www.fellnasen-service.de/index.php?thread/145266-настоящие-дипломы-легко-и-быстро/
Добрый день!
Заказать документ института можно в нашей компании в столице.
ast-diplomas.com/kupit-diplom-sankt-peterburg
Здравствуйте!
Где купить диплом специалиста?
http://www.soad.msk.ru/forum/viewforum.php?f=16
Хорошей учебы!
Привет!
Где приобрести диплом по актуальной специальности?
Заказать диплом о высшем образовании.
weekofsport.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
Привет!
Купить документ ВУЗа вы имеете возможность у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы Советского Союза.
toursoul.ru/?p=19214
familyportal.forumrom.com/viewtopic.php?id=23434#p60671
avtolux48.ru/people/user/374/blog/7917/
russianecuador.com/forum/member.php?u=13207
toplentanews.ru/ofitsialnyiy-diplom-bez-lishnih-voprosov
Здравствуйте!
Наши специалисты предлагают максимально быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями. Данный диплом пройдет любые проверки, даже при помощи специальных приборов. Решите свои задачи максимально быстро с нашим сервисом.
aromatov.wooden-rock.ru/forum/topic.php?forum=1&topic=15825&v=l#1719302971
Успехов в учебе!
Привет, друзья!
Заказать диплом ВУЗа.
1mog.listbb.ru/viewtopic.php?f=6&t=8573
купить диплом без предоплаты купить диплом без предоплаты .
На сайте https://santeh.club вы сможете приобрести качественные, надежные унитазы, ванны, а также полотенцесушители, инсталляции, смесители и многое другое от лучших производителей, которые предлагают исключительно качественную продукцию для помещений различного дизайна и площади. Предоставляется дополнительная гарантия качества, которая выдается производителем. Перед вами огромный выбор интересных новинок, которые появляются регулярно. Возможна услуга самовывоза. Доставка покупок по всем регионам.
Привет!
Мы изготавливаем дипломы любой профессии по приятным ценам.
newsato.ru/kupit-diplom-garantiya-kachestva-i-bezopasnosti
Привет, друзья!
Официальная покупка диплома вуза с сокращенной программой обучения в Москве
gorod.kr.ua/forum/showthread.php?p=267249#post267249
Поможем вам всегда!.
Привет, друзья!
Предлагаем документы техникумов, расположенных в любом регионе РФ. Вы имеете возможность купить диплом за любой год, в том числе документы старого образца. Документы печатаются на бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригиналов. Они будут заверены всеми требуемыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по приятным тарифам. Стоимость будет зависеть от конкретной специальности, года выпуска и университета. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас важно, чтобы дипломы были доступны для большого количества граждан.
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge
Успехов в учебе!
Добрый день!
Мы изготавливаем дипломы любой профессии по разумным ценам.
cimat.com.do/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B3%D0%BE%D0%B7%D0%BD%D0%B0%D0%BA/
Привет!
Купить диплом о высшем образовании.
wiki.mdomtv.net/index.php?title=????????_???????????_????????,_???????????_???_?????_?????????:_??????_?_????????!
Удачи!
Привет, друзья!
Где приобрести диплом специалиста?
gadjetforyou.ru/diplom-za-dengi-byistro-nadezhno-bezopasno
Хорошей учебы!
Привет, друзья!
Приобрести диплом университета.
samovod.ru/content/articles/65982/
Добрый день!
Предлагаем документы ВУЗов, которые расположены в любом регионе России. Вы сможете заказать качественный диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы печатаются на бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и штампами.
Мы можем предложить дипломы любых профессий по доступным ценам. Цена зависит от той или иной специальности, года выпуска и университета. Всегда стараемся поддерживать для клиентов адекватную политику цен. Важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
landik-diploms-srednee.ru/diplom-bakalavra
Хорошей учебы!
Здравствуйте!
Приобрести документ института можно у нас. Мы предлагаем документы об окончании любых университетов России.
hardstorecr.com/mybb/showthread.php?tid=118161
nis.com.tn/index.php?option=com_kunena&view=topic&catid=2&id=6746&Itemid=151
gidro2000.com/forum-gidro/user/27011/
videopro.ru/xenforo/index.php?threads/%D0%A2%D0%B5%D1%81%D1%82%D0%BE%D0%B2%D0%B0%D1%8F-%D1%82%D0%B5%D0%BC%D0%B0-%D0%B7%D0%B0%D0%BA%D1%80%D0%B5%D0%BF%D0%BB%D1%91%D0%BD%D0%BD%D0%B0%D1%8F.1/page-113#post-4152
xn--e1aoddcgsc8a.xn--p1ai/showthread.php?tid=48487
Здравствуйте!
Мы предлагаем приобрести диплом в высочайшем качестве, неотличимый от оригинального документа без участия специалиста высокой квалификации со сложным оборудованием.
vitaco.ru/communication/forum/user/4579/
Удачи!
Привет, друзья!
Мы изготавливаем дипломы любой профессии по доступным ценам.
cnktdshanoi.com.vn/%D1%80%D0%B5%D1%87%D0%BD%D0%BE%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C/
Привет, друзья!
Купить диплом любого университета
Наши специалисты предлагают максимально быстро купить диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями должностных лиц. Документ пройдет любые проверки, даже при помощи профессиональных приборов. Достигайте цели быстро с нашими дипломами.
Где приобрести диплом по актуальной специальности?
nedvigimost.bbok.ru/viewtopic.php?id=26650#p45740
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
kino.10bb.ru/viewtopic.php?id=163545#p276485
promintern.listbb.ru/viewtopic.php?f=16&t=474
slliver.getbb.ru/viewtopic.php?f=62&t=826
Привет!
Приобрести документ о получении высшего образования можно в нашем сервисе.
ast-diploms.com/kupit-diplom-nizhnij-novgorod
Удачи!
Здравствуйте!
Наши специалисты предлагают максимально быстро заказать диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ способен пройти лубую проверку, даже при помощи профессиональных приборов. Решайте свои задачи максимально быстро с нашей компанией.
sklad-slabov.ru/forum/user/7793/
Удачи!
Здравствуйте!
Покупка школьного аттестата с упрощенной программой: что важно знать
thmyan1.pgdthapmuoidt.edu.vn/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D1%8F%D1%80%D1%81%D0%BA/
Добрый день!
Где купить диплом по необходимой специальности?
Заказать диплом университета.
http://www.rrsclub.ru/showthread.php?p=44904#post44904
Здравствуйте!
Заказать документ о получении высшего образования вы имеете возможность у нас.
diplomasx24.ru/kupit-diplom-ekaterinbur
купить диплом доктора наук asxdiplomik24.ru .
Place your bets directly on the blockchain and say
goodbye to any middlemen taking a cut of the action.
Feel free to surf to my web blog; 슈어맨
Здравствуйте!
Приобрести документ о получении высшего образования вы сможете у нас.
ast-diplomy.com/kupit-diplom-sankt-peterburg
Успехов в учебе!
Привет, друзья!
Приобрести документ о получении высшего образования можно у нас в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любым специальностям, включая документы старого образца.
wiki.intradition.ru/index.php/Легкий_путь_к_дипломированному_успеху
derivsocial.org/read-blog/2578
wiki.gta-zona.ru/index.php/Быстрое_оформление_диплома:_надежно_и_конфиденциально
androidinweb.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
fire-team.ru/forum/member.php?u=1143
Здравствуйте!
Как официально купить аттестат 11 класса с упрощенным обучением в Москве
a-bcd.ru/news/201718/
Рады оказаться полезными!.
Привет!
Можно ли купить аттестат о среднем образовании, основные моменты и вопросы
rodme.ru/legalnyy-diplom-pod-klyuch-nikakih-zabot-t12705.html
Рады оказаться полезными!.
Привет!
Где приобрести диплом по актуальной специальности?
Приобрести диплом любого ВУЗа.
amengram.com/blogs/338/%D0%9A%D0%B0%D0%BA-%D0%BF%D0%BE%D0%B4%D1%8B%D1%81%D0%BA%D0%B0%D1%82%D1%8C-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D1%88%D0%B8%D1%80%D0%BE%D0%BA%D0%B8%D0%BC-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80%D0%BE%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2
Привет, друзья!
Где заказать диплом по актуальной специальности?
elfae.ruhelp.com/viewtopic.php?id=17175#p39412
Успешной учебы!
диплом техникума диплом техникума .
Привет, друзья!
Мы готовы предложить документы ВУЗов, расположенных в любом регионе РФ. Можно приобрести качественный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Документы выпускаются на бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы будут заверены всеми обязательными печатями и подписями.
fisketavling.nu/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=343
1win – лучший выбор для онлайн-ставок
Удача всегда на вашей стороне с 1win
1win – место, где рождаются победы
Ваши ставки – наша ответственность
1win: самый простой способ выигрывать
Ваши ставки всегда успешные с 1win
1win делает вашу игру еще более захватывающей
Сделайте свою жизнь ярче с помощью 1win
Победы становятся легко доступными с 1win
1win: ваш выбор номер один в мире ставок
Ставки на спорт никогда не были такими увлекательными как с 1win
Присоединяйтесь к миллионам победителей на платформе 1win
1win – это ваша возможность побеждать
1win делает ставки доступными для всех|1win – это ваша дверь в мир азарта и прибыли
1win гарантирует вам качественный сервис и высокие шансы на успех|Увлекательные ставки и азартные игры на платформе 1win|1win – ваш верный партнер в мире ставок|Увеличивайте свои выигрыши с 1win|1win – ваш путь к финансовой независимости|1win – это ваш персональный билет в мир азарта|1win – ваш путь к успеху и богатству|1win предлагает вам только лучшие условия для игры|1win делает вашу игру более прибыльной и интересной|1win – это ваш шанс стать победителем|Станьте настоящим профи в ставках с 1win|1win – это ваша возможность изменить свою жизнь|Заработайте больше с помощью 1win|1win радует своих клиентов только лучшими условиями|1win – ваш верный партнер в мире ставок|Начните свой путь к успеху с 1win|1win – это ваш путь к большим выигрышам|Ув
1win вход https://1win-ofitsialnyy.by/ .
Добрый день!
Реально ли приобрести диплом стоматолога? Основные этапы
buldingnews.ru/byistroe-oformlenie-diploma-nadezhno-i-konfidentsialno
Всегда вам поможем!.
krepezh.net
Здравствуйте!
Где купить диплом специалиста?
Заказать диплом любого университета.
musicianforums.net/index.php?/gallery/image/138-%D0%B1%D0%BE%D0%BB%D1%8C%D1%88%D0%BE%D0%B9-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
Здравствуйте!
Купить диплом университета.
s-s-o.ru/forum.php?PAGE_NAME=profile_view&UID=52354
Хорошей учебы!
Привет, друзья!
Мы готовы предложить документы ВУЗов, расположенных в любом регионе РФ. Вы сможете купить диплом от любого учебного заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы делаются на бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригинала. Документы заверяются всеми требуемыми печатями и штампами.
taxecure.mn.co/posts/61838293
Привет!
Как быстро получить диплом магистра? Легальные способы
barranca21.com/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BF%D1%82%D1%83/
Привет!
Узнайте, как безопасно купить диплом о высшем образовании
opros.flybb.ru/viewtopic.php?f=2&t=545
Рады помочь!.
Привет!
Где заказать диплом по актуальной специальности?
Купить диплом о высшем образовании.
nfrb.pl/index.php?/gallery/image/51-%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%B9-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по разумным ценам.
gemawiraclub.com/blogs/39878/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8
Добрый день!
Сколько стоит получить диплом высшего и среднего образования легально?
injectorcar.ru/forum/showthread.php?p=230396#post230396
Окажем помощь!.
Здравствуйте!
Мы предлагаем документы ВУЗов, расположенных на территории всей Российской Федерации. Можно приобрести качественный диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и штампами.
pt1tch1il.howeweb.com/28819663/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
alanews24.com
Покупка диплома о среднем полном образовании: как избежать мошенничества?
ast-diplomy.com/kupit-diplom-magistra
Добрый день!
Ьожем предложить документы техникумов, которые находятся в любом регионе России. Можно заказать диплом за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Они заверяются необходимыми печатями и подписями.
Мы предлагаем дипломы любой профессии по приятным ценам. Цена зависит от конкретной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику цен. Для нас важно, чтобы документы были доступными для подавляющей массы наших граждан.
arusak-diploms-srednee.ru/kupit-attestat-za-11-klass
Успехов в учебе!
Добрый день!
Приобрести диплом о высшем образовании.
wiki.nikiforov.ru/index.php/??????_??????:_???????_?????_?????_????????????????_?????
Успешной учебы!
Привет, друзья!
Где приобрести диплом по необходимой специальности?
Заказать диплом любого университета.
mystroycenter.ru/legkiy-sposob-poluchit-diplom-bez-ekzamenov
Здравствуйте!
Купить документ о получении высшего образования вы сможете у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР.
bvf.ru/forum/showthread.php?p=25249385#post25249385
satopttorg.ru/forum/user/3416/
saumalkol.com/forum/разное-2/3559-получите-диплом-без-лишних-забот-и-усилий.html
forum-pmr.net/member.php?u=42748
smd.mybb.ru/viewtopic.php?id=4057#p23076
Привет, друзья!
Приобрести документ о получении высшего образования вы можете у нас в столице. Мы оказываем услуги по производству и продаже документов об окончании любых университетов РФ. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы СССР. Гарантируем, что при проверке документа работодателями, никаких подозрений не возникнет.
sz.80lvl.ru/viewtopic.php?f=9&t=1920
biomedia.pro/club/user/112304/forum/message/3806/13288/
http://www.cyberpinoy.net/create-blog/
danceway74.ru/users/36
danceway74.ru/users/36
Рекламное агентство – это компания, которая занимается созданием и реализацией рекламных кампаний для различных клиентов. Рекламное агентство может предлагать следующие услуги:
1. Разработка рекламной стратегии: анализ аудиитории, определение целей и задач рекламной кампании, выбор каналов рекламы и бюджетирование.
2. Создание рекламного контента: разработка рекламных материалов, таких как видеоролики, баннеры, печатные объявления, тексты для социальных сетей и т.д.
3. Медиапланирование: выбор оптимальных каналов для размещения рекламы, закупка рекламного пространства, мониторинг эффективности кампании.
4. Социальные сети: создание и управление рекламными кампаниями в социальных сетях, таких как Facebook, Instagram, Twitter и т.д.
5. Оцифровка: преобразование традиционных рекламных форматов в цифровые, такие как email-рассылка, мобильная реклама и т.д.
6. Анализ и отчетность: отслеживание эффективности рекламной кампании, анализ результатов, предоставление отчетов клиенту.
Рекламные агентства могут специализироваться на различных областях, таких как:
1. Digital-агентство:?ализируется на цифровой рекламе, включая поиск, социальные сети, email-рассылку и т.д.
2. Full-service-агентство: предлагает полный спектр услуг, включая разработку рекламной стратегии, создание контента и медиапланирование.
3. Брендинговое агентство: специализируется на разработке бренда, включая создание логотипа, упаковки и т.д.
4. Event-агентство: организует и продвигает мероприятия, такие как конференции, семинары, выставки и т.д.
5. PR-агентство: занимается по связям с общественностью, включая общение с СМИ, кризис-менеджмент и т.д.
Также рекламные агентства могут иметь различные бизнес-модели, такие как:
1. Фиксированная плата: агентство получает фиксированную плату за свои услуги.
2. Комиссионная плата: агентство получает комиссию от рекламного бюджета клиента.
3. Результативная плата: агентство получает плату только в случае достижения определенных результатов, таких как увеличениеconversion rate или дохода.
Наши услуги
На сайтах наших клиник, Вы можете посмотреть полный перечень услуг, оказываемых в наших клиниках, а также сразу узнать, в каком конкретном направлении работает тот или иной ветеринарный врач, чтобы сразу записаться на прием к нужному специалисту.
Лечение
19 услуг
такие как
гемиламинэктомия у собак цена
обращайтесь к нам мы работаем 24 на 7 наши специалисты вас проконсультируют если есть какие нибудь вопросы
https://lifevet.ru/
123
купить диплом колледжа в кемерово https://diploms-x.com .
read more martian wallet
Добрый день!
Покупка школьного аттестата с упрощенной программой: что важно знать.
Заказать диплом о высшем образовании.
7hz0jwqg2.dreamyblogs.com/28634603/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет, друзья!
Приобрести документ о получении высшего образования вы имеете возможность у нас.
ast-diplomas.com/kupit-diplom-o-srednem-obrazovanii
Удачи!
Привет, друзья!
Где купить диплом специалиста?
Приобрести диплом о высшем образовании.
islider.ru/read-blog/564
Привет, друзья!
Приобретение диплома ВУЗа с сокращенной программой обучения в Москве
ремонт-оптом.рф/club/user/17/blog
Окажем помощь!.
На сайте https://logisticbda.com оставьте заявку для того, чтобы вам рассчитали стоимость такой услуги, как заказ продукции для маркетплейсов и непосредственно из Китая. Сотрудники выполняют такие важные работы, как: выкуп, поиск, транспортировка из Китая. Специально для вас отгрузка, упаковка на маркетплейсы. Сотрудники окажут помощь в формировании бизнеса на различных маркетплейсах. Закупка происходит с самых проверенных, надежных магазинов, которым точно можно доверять. Проводятся различные складские работы, дополнительные услуги.
Привет, друзья!
Мы предлагаем документы техникумов, расположенных в любом регионе Российской Федерации. Можно купить качественный диплом от любого заведения, за любой год, включая сюда документы СССР. Документы выпускаются на бумаге самого высокого качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Они заверяются всеми необходимыми печатями и штампами.
elotag.com/read-blog/296
Здравствуйте!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
jrsjewellers.com/2024/06/29/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D1%83%D0%BD%D0%B8%D0%B2%D0%B5%D1%80%D1%81%D0%B8%D1%82%D0%B5%D1%82%D0%B0/
Быстрая покупка диплома старого образца: возможные риски
asxdiplomik.com/kupit-diplom-magistra
купить диплом ссср московская область http://www.diploms-x.com/ .
Привет!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
http://www.lifecapadvisors.com/%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D1%83%D0%BC%D0%B0-%D0%BA%D0%BE%D0%BB%D0%BB%D0%B5%D0%B4%D0%B6%D0%B0-1997-2003-%D1%84%D0%BE%D1%82%D0%BE/
На сайте https://vips13un.kinoportal.live/ подберите интересный, увлекательный фильм, который подходит для домашнего совместного просмотра, а также в выходной день. Также находятся и любопытные передачи, которые смотрят многие. Вы обязательно найдете то, что полностью соответствует вашим предпочтениям, вкусам. Все кино, передачи представлены в отличном качестве и с хорошим звуком, поэтому просмотр принесет лишь приятные эмоции. Регулярно появляются многообещающие новинки, которые тоже заслуживают вашего внимания.
Здравствуйте!
Ьожем предложить документы техникумов, расположенных в любом регионе РФ. Можно купить качественный диплом за любой год, включая сюда документы СССР. Дипломы и аттестаты печатаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригинала. Документы заверяются всеми обязательными печатями и штампами.
Мы изготавливаем дипломы любой профессии по невысоким ценам. Стоимость зависит от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас важно, чтобы документы были доступными для подавляющей массы граждан.
landik-diploms-srednee.ru/svidetelstvo-o-razvode
Успехов в учебе!
Привет, друзья!
Приобрести документ университета можно в нашей компании в столице. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любым специальностям, включая документы Советского Союза. Даем гарантию, что в случае проверки документа работодателями, каких-либо подозрений не возникнет.
izumrudnoeozero.listbb.ru/viewtopic.php?f=8&t=538
kolhos.listbb.ru/viewtopic.php?f=2&t=583
t67747az.beget.tech/2024/07/07/vysshee-obrazovanie-za-den-prosto-i-legalno.html
berforum.ru/gallery/image/8679-ogromnaya-vostrebovannost-i-populyarnost-magazinov-s-diplomami/?context=new
p-release.ru/services/za-scet-cego-magaziny-s-diplomami-segodna-stol-popularny
[u][b] Привет![/b][/u]
[b]Приобрести документ[/b] института можно в нашей компании в Москве.
[url=http://asxdiplomik24.ru/kupit-diplom-vracha/]asxdiplomik24.ru/kupit-diplom-vracha[/url]
[b]Удачи![/b]
Здравствуйте!
Мы изготавливаем дипломы любых профессий по приятным ценам.
gaysocial.gay/read-blog/79_vybiraem-nadezhnyj-internet-magazin-s-diplomami-i-attestatami.html?mode=day
Привет, друзья!
Мы предлагаем купить диплом в отличном качестве, неотличимый от оригинала без участия специалистов высокой квалификации со сложным оборудованием.
telent.ussoft.kr/bbs/board.php?bo_table=free&wr_id=1453565
Удачи!
Здравствуйте!
Купить документ о получении высшего образования вы сможете у нас в столице. Мы предлагаем документы об окончании любых университетов РФ.
munservis.mirniy.ru/index.php?subaction=userinfo&user=ukibe
http://www.pharmvrn.ru/forum/profile.php?action=show&member=8889
ledsoft.ru/forum/?PAGE_NAME=message&FID=5&TID=13698&TITLE_SEO=13698-diplomandoci&MID=14490&result=new#message14490
kochtagebuch.org/doku.php?id=premiummdiplomms
ad-vance.ru/communication/forum/user/40075/
как получить внж в Коста-Рику
второе гражданство Коста-Рика
https://costavida.ru
миграция на Коста-Рику
внж Коста-Рика как получить
https://costarus.ru
как получить гражданство Коста-Рики для россиян
роды в Коста-Рике гражданство
иммиграция Коста-Рика
Коста-Рика отзывы пмж
Коста-Рика переехать на пмж
https://imigrantos.ru
Добрый день!
Заказать диплом университета
Мы предлагаем выгодно и быстро заказать диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями официальных лиц. Документ способен пройти лубую проверку, даже с использованием специального оборудования. Решайте свои задачи быстро с нашей компанией.
Где купить диплом по необходимой специальности?
autoprajs.ru/15204.html
driveme.rusff.me/viewtopic.php?id=2115#p105171
ya.2bb.ru/viewtopic.php?id=19040#p240217
mosday.getbb.ru/viewtopic.php?f=12&t=1059
ilovehabbo.bbon.ru/viewtopic.php?id=1459#p28856
Привет!
Готовы предложить документы ВУЗов, расположенных на территории всей России. Вы имеете возможность купить качественно сделанный диплом от любого учебного заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они будут заверены необходимыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по приятным тарифам. Цена зависит от выбранной специальности, года получения и университета. Стараемся поддерживать для клиентов адекватную политику цен. Важно, чтобы дипломы были доступны для большого количества наших граждан.
landik-diploms-srednee.ru/diplom-bakalavra
Хорошей учебы!
I’m really impressed with your writing skills and also with the layout on your blog.
Is this a paid theme or did you modify it yourself?
Anyway keep up the excellent quality writing, it’s rare to see a great
blog like this one nowadays.
Здравствуйте!
Купить документ университета вы сможете у нас в Москве.
ast-diploms.com/kupit-diplom-moskva
Успехов в учебе!
Sale Hacked paypal Western UNION http://buycloned-cards.cvv2cvc.net
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $1 000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://buy-cloned-cards.cvv2cvc.net
Добрый день!
Предлагаем документы ВУЗов, которые расположены на территории всей РФ. Вы имеете возможность купить качественно сделанный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Документы печатаются на бумаге высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются всеми требуемыми печатями и подписями.
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий по выгодным тарифам. Цена будет зависеть от определенной специальности, года получения и университета. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для большого количества наших граждан.
arusak-diploms-srednee.ru/kupit-diplom-sssr
Удачи!
На сайте http://wirespace.ru изучите полезные, интересные и содержательные статьи, которые посвящены ландшафтному дизайну. Представлены любопытные идеи о том, как правильно разместить скульптуры, а также интересные декоративные элементы. Опубликованы не только рекомендации, но и любопытные идеи. Есть информация относительно дизайна для миниатюрных садов. Вы узнаете и о том, как правильно выбрать цветовую гамму для декорирования. Есть информация о том, как организовать роскошное пространство в доме.
Добрый день!
Купить документ о получении высшего образования можно у нас.
ast-diplomas.com/kupit-diplom-vracha
Удачи!
Привет, друзья!
Как купить диплом о высшем образовании с минимальными рисками
http://www.industrialagency.org/blogs/69281/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B4%D0%BB%D1%8F-%D0%A3%D1%81%D0%BF%D0%B5%D1%88%D0%BD%D0%BE%D0%B9-%D0%9A%D0%B0%D1%80%D1%8C%D0%B5%D1%80%D1%8B
Reducing the workload on morson.org technical support workers. Very often, monotonous actions take up a lot of time from specialists. If you work with tickets, you can optimize routine operations. In addition, you can count on deadlines, that is, assign responsibility for specific actions.
Здравствуйте!
Где заказать диплом по необходимой специальности?
Мы изготавливаем дипломы любой профессии по доступным тарифам. Цена может зависеть от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас важно, чтобы дипломы были доступны для большого количества граждан.
Для вас изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
sosh13.pascal.ru/forum/profile.php?action=show&member=22558
Рады помочь!.
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
ast-diplomas24.ru/kupit-diplom-o-srednem-obrazovanii
Привет!
Где приобрести диплом по необходимой специальности?
Приобрести диплом любого университета.
wiki.roximo.ru/index.php/%D0%9A%D0%B0%D0%BA_%D0%BF%D0%BE%D0%B4%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D1%8C_%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD_%D1%81_%D0%BE%D0%B1%D1%88%D0%B8%D1%80%D0%BD%D1%8B%D0%BC_%D0%B2%D1%8B%D0%B1%D0%BE%D1%80%D0%BE%D0%BC_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2%3F
Then the structure homeideascoach.com with the floor is installed. If the model does not have a floor, then you will need to build a platform.
Learn More Here rabby login
Привет!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
alanyatoday.ru/users/76
Всегда вам поможем!.
Привет!
Мы можем предложить документы техникумов, расположенных на территории всей Российской Федерации. Вы имеете возможность заказать качественный диплом за любой год, в том числе документы старого образца. Дипломы и аттестаты печатаются на “правильной” бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, которые невозможно отличить от оригинала. Они заверяются всеми требуемыми печатями и штампами.
http://www.guyub.net/read-blog/9030
Добрый день!
Наш сервис предлагает купить диплом в отличном качестве, неотличимый от оригинала без использования дорогостоящего оборудования и опытного специалиста.
xn--e1aaawjgmm1c3c.xn--p1ai/forum/viewtopic.php?f=3&t=531175
Успешной учебы!
Привет!
Купить документ ВУЗа можно в нашей компании. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ. Вы получите необходимый диплом по любым специальностям, любого года выпуска, включая документы СССР. Даем 100% гарантию, что в случае проверки документов работодателями, подозрений не возникнет.
spletninews.ru/kupit-diplom-professionalnoe-vyipolnenie
phobia.lt/index.php?/gallery/image/124-4-%D0%B5-%D0%BA%D0%BB%D1%8E%D1%87%D0%B5%D0%B2%D1%8B%D1%85-%D0%B3%D1%80%D1%83%D0%BF%D0%BF%D1%8B-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%BE%D0%B2-%D1%87%D1%82%D0%BE-%D1%80%D0%B5%D0%B0%D0%BB%D0%B8%D0%B7%D1%83%D1%8E%D1%82-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B/
x70795vj.beget.tech/2024/07/07/bystroe-oformlenie-diplomov-dostupno-i-nadezhno.html
wo.linyway.com/read-blog/3248
plplatoon.com/gallery/image/121-%D0%BA%D0%B0%D1%82%D0%B0%D0%BB%D0%BE%D0%B3-%D0%B8-%D0%B2%D0%B0%D1%80%D0%B8%D0%B0%D0%BD%D1%82%D1%8B-%D0%B4%D0%BE%D1%81%D1%82%D0%B0%D0%B2%D0%BA%D0%B8-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC/
Добрый день!
Купить документ о получении высшего образования вы можете в нашей компании в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации.
foodsuppliers.ru/users/igihyx
loket.kr/free/164774
masyasha.ru/index.php?option=com_k2&view=itemlist&task=user&id=83113
nailpub.ru/forum/threads/norske-mobil-casino-eller-norske-betting-sider.41827/#post-1152463
pedolog-pro.ru/forums/topic/%d0%bd%d0%be%d0%b2%d0%b0%d1%8f-%d1%81%d1%81%d1%8b%d0%bb%d0%ba%d0%b0-%d0%bd%d0%b0-%d0%bc%d0%b5%d0%b3%d1%83-2/page/501/#post-330598
Здравствуйте!
Где приобрести диплом специалиста?
Приобрести диплом любого университета.
samovod.ru/content/articles/65961/
see this website phantom login
Привет!
Заказать диплом о высшем образовании
Мы предлагаем максимально быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями должностных лиц. Наш документ пройдет лубую проверку, даже с использованием специально предназначенного оборудования. Решите свои задачи максимально быстро с нашим сервисом.
Где приобрести диплом специалиста?
alanyatoday.ru/users/76
mosday.getbb.ru/viewtopic.php?f=12&t=1059
malispa.ru/users/122
rodina.listbb.ru/viewtopic.php?f=3&t=502
goup.hashnode.dev/kupit-diplom-1-1-1
купить диплом нового образца в омске ast-diploms.com .
купить диплом о среднем проф образовании diplomasx.com .
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по невысоким ценам.
evogenesfahan.com/2024/06/23/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B3%D0%B3%D1%83-%D0%B8%D0%BB%D0%B8-%D0%BB%D1%8E%D0%B1%D0%BE%D0%B3%D0%BE-%D0%B2%D1%83%D0%B7%D0%B0-%D1%80%D0%BE%D1%81/
Добрый день!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
pestostop.com/2024/07/14/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BC%D0%B3%D1%83%D0%BF-%D0%B8%D0%BB%D0%B8-%D0%BB%D1%8E%D0%B1%D0%BE%D0%B3%D0%BE-%D0%B2%D1%83%D0%B7%D0%B0-%D1%80%D0%BE%D1%81/
Добрый день!
Быстрая схема покупки диплома старого образца: что важно знать?
u2c.tv/member.php?u=30984
Будем рады вам помочь!.
Привет, друзья!
Мы предлагаем документы ВУЗов, расположенных в любом регионе России. Вы можете заказать диплом от любого заведения, за любой год, включая сюда документы СССР. Документы делаются на “правильной” бумаге высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Они заверяются необходимыми печатями и штампами.
forum.zentox-rp.ru/index.php?app=gallery&module=gallery&controller=view&id=12
Добрый день!
Мы изготавливаем дипломы любой профессии по приятным ценам. Стоимость зависит от той или иной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для клиентов адекватную ценовую политику. Для нас важно, чтобы дипломы были доступными для большинства наших граждан.
zanderjwhn02578.wikinewspaper.com/3003188/%D0%A4%D0%B0%D0%BB%D1%8C%D1%88%D0%B8%D0%B2%D1%8B%D0%B9_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC_%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83_%D1%8D%D1%82%D0%BE_%D0%BD%D0%B5_%D0%A1%D1%82%D0%BE%D0%B8%D1%82_%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
https://www.vatech.com/manuals/390917
The Biden-Harris Administration has announced a program that contains debt relief based
on revenue.
Also visit my blog – 대출사이트
ремонт мобильных телефонов рядом
Здравствуйте!
Как официально приобрести аттестат 11 класса с минимальными затратами времени
http://www.2dommedical.com/2024/06/30/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B3%D0%BB%D0%B0%D0%B2%D1%83-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0/
Привет!
Приобрести диплом университета.
k90280ul.beget.tech/2024/07/07/4-e-osnovnyh-gruppy-internet-magazinov-prodayuschih-dokumenty.html
Вам интересен вопрос о прокате инвалидных колясок? Деливери плей поможет вам. Гарантируем оперативную доставку и приемлемые цены. У нас всегда чистые коляски. Вы сможете, заказ оплатить тогда, когда убедитесь в том, что коляска находится в отменном состоянии и полностью соответствует вашим требованиям. Ищите Аренда Инвалидных колясок? Deliveryplay.ru/arenda-invalidnyh-kolyasok – сайт, где можете арендовать коляску. Помимо прочего у нас можно узнать, почему аренда выгоднее приобретения. Мы поможем вам выбрать идеальную коляску, которая вам подойдет, обращайтесь.
Привет, друзья!
Где купить диплом по актуальной специальности?
Мы изготавливаем дипломы любой профессии по приятным ценам. Стоимость зависит от конкретной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную ценовую политику. Для нас важно, чтобы документы были доступными для большого количества наших граждан.
Для вас изготавливаем дипломы любых профессий по разумным тарифам.
aboutalltour.ru/ofitsialnyie-diplomyi-bez-problem/
Поможем вам всегда!.
Здравствуйте!
Мы предлагаем приобрести диплом в отличном качестве, неотличимый от оригинального документа без участия специалиста высокой квалификации с дорогим оборудованием.
qbko.ru/index.php?subaction=userinfo&user=uqynujes
Успешной учебы!
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным ценам.
sydplatinum.com/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%80%D1%84/
websites
Celestia wallet keplr
Привет, друзья!
Приобрести документ о получении высшего образования вы имеете возможность у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы старого образца. Гарантируем, что при проверке документа работодателями, подозрений не появится.
Мы можем предложить дипломы любой профессии по приятным ценам. Стоимость может зависеть от той или иной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступны для подавляющей массы наших граждан.
http://www.maleus.ru/index.php/component/tag/%D1%8D%D0%B2%D0%BE%D0%BB%D1%8E%D1%86%D0%B8%D1%8F
Рады оказаться полезными!
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании. Мы предлагаем документы об окончании любых университетов РФ.
amvnews.ru/forum/posting.php?mode=newtopic&f=44
golpro.jp/userinfo.php?uid=13505#
shinyoungwood.co.kr/bbs/board.php?bo_table=free&wr_id=783326
youhotel.ru/forum/viewtopic.php?f=15&t=50439
http://www.lada-4×4.net/member.php?u=22958
Добрый день!
Где заказать диплом специалиста?
Мы можем предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Можно заказать качественно напечатанный диплом от любого высшего учебного заведения, за любой год, в том числе документы старого образца. Дипломы печатаются на “правильной” бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, которые невозможно отличить от оригиналов. Они будут заверены необходимыми печатями и подписями.
Мы предлагаем дипломы любой профессии по разумным ценам.
diplomasx.com/kupit-diplom-rostov-na-donu
Поможем вам всегда!
Привет!
Купить диплом о высшем образовании
Наши специалисты предлагают выгодно и быстро заказать диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Наш диплом пройдет лубую проверку, даже с применением специального оборудования. Достигайте цели максимально быстро с нашей компанией.
Где купить диплом специалиста?
ya.bestbb.ru/viewtopic.php?id=2962#p6549
goup.hashnode.dev/kupit-diplom-1-1-1
forum.qwas.ru/kupit-diplom-t19852.html
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
http://www.hristianka.ru/forum/r/prev_loaded/1/
https://tissuearray.info/index.php?title=Promplex.ru
Привет, друзья!
Мы готовы предложить дипломы любой профессии по невысоким ценам.
eicolumbaira.es/%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Привет, друзья!
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков
http://www.b2bempowerment.org/blogs/394/%D0%93%D1%80%D0%B0%D0%BC%D0%BE%D1%82%D0%BD%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
Добрый день!
Купить диплом любого университета
Наша компания предлагает быстро заказать диплом, который выполняется на оригинальной бумаге и заверен печатями, штампами, подписями официальных лиц. Наш диплом способен пройти лубую проверку, даже при использовании специфических приборов. Решайте свои задачи максимально быстро с нашим сервисом.
Где приобрести диплом специалиста?
dskrnd.ru/forum/user/6379/
vip.rolevaya.info/viewtopic.php?id=4952#p8469
http://www.fellnasen-service.de/index.php?thread/145266-настоящие-дипломы-легко-и-быстро/
kilcoynelilacfarm.com/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=401
fire-team.ru/forum/member.php?u=1143
купить диплом типографии ast-diploms.com .
Добрый день!
Мы готовы предложить дипломы любой профессии по выгодным тарифам.
newfinbiz.ru/kupit-diplomyi-dlya-vseh-spetsialnostey
сколько стоит купить диплом в россии diplomasx.com .
Привет!
Заказать диплом о высшем образовании.
http://www.humansandslaves.ru/blogs/669/%D0%91%D1%8B%D1%81%D1%82%D1%80%D1%8B%D0%B9-%D0%B2%D1%8B%D0%B1%D0%BE%D1%80-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B0-%D0%BF%D1%80%D0%BE%D0%B4%D0%B0%D1%8E%D1%89%D0%B5%D0%B3%D0%BE-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D1%8B
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по разумным тарифам. Цена зависит от определенной специальности, года получения и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику цен. Для нас важно, чтобы документы были доступны для подавляющей массы граждан.
cristianbh703.bloggazza.com/26706532/%D0%A4%D0%B0%D0%BB%D1%8C%D1%88%D0%B8%D0%B2%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9F%D0%BE%D1%87%D0%B5%D0%BC%D1%83-%D1%8D%D1%82%D0%BE-%D0%BD%D0%B5-%D0%A1%D1%82%D0%BE%D0%B8%D1%82-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
Привет, друзья!
Сколько стоит диплом высшего и среднего образования и как его получить?
friend24.in/blogs/2849/%D0%9F%D1%80%D0%B0%D0%B2%D0%B8%D0%BB%D1%8C%D0%BD%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
Привет, друзья!
Заказать документ о получении высшего образования можно в нашей компании в столице.
diplomyx24.ru/kupit-diplom-nizhnij-novgorod
В критические моменты жизни важно, чтобы похоронное бюро было надежным и профессиональным. Наша статья поможет вам разобраться в разнообразии ритуальных услуг в Алматы и выбрать агентство, которое предложит качественное обслуживание по разумной цене услуги ритуальные цена
Привет, друзья!
Предлагаем документы ВУЗов, которые находятся на территории всей Российской Федерации. Можно купить диплом от любого учебного заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и штампами.
Мы предлагаем дипломы любой профессии по приятным тарифам. Стоимость зависит от выбранной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большого количества наших граждан.
landik-diploms-srednee.ru/diplom-s-reestromkupit-kupit
Удачи!
Добрый день!
Где приобрести диплом специалиста?
Купить диплом о высшем образовании.
sev-ribalka.ru/gallery/image/2443-kak-nayti-nadezhnyy-magazin-s-shirokim-vyborom-diplomov/
Привет!
Приобретение школьного аттестата с официальным упрощенным обучением в Москве
http://www.mylot.su/blog/14481
Поможем вам всегда!.
Ищете навес для автомобиля в Воскресенске? Вип-Навес предлагает широкий ассортимент навесов из поликарбоната и металла. Наши услуги начинаются с выезда инженера-замерщика, который в удобное для вас время зафиксирует все ваши требования, сделает точные замеры и рассчитает проект на месте. Мы создаем бесплатный 3D макет, чтобы вы могли видеть будущую конструкцию. Заключаем договор с фиксированными ценами и сроками, после чего приступаем к производству. Vip Naves RU гарантирует высокое качество благодаря использованию профессионального оборудования и материалов. Доставка и монтаж проводятся в удобное для вас время, а по завершению работ производится окончательная оплата. Закажите у нас и получите бесплатный 3D проект в подарок!
Добрый день!
Купить документ института можно у нас в столице.
ast-diploms.com/kupit-diplom-magistra
Удачи!
Привет!
Ьожем предложить документы ВУЗов, которые расположены на территории всей Российской Федерации. Можно заказать качественно сделанный диплом за любой год, в том числе документы старого образца СССР. Дипломы и аттестаты печатаются на бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригиналов. Они будут заверены необходимыми печатями и штампами.
Мы изготавливаем дипломы любой профессии по выгодным тарифам. Цена зависит от определенной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас важно, чтобы документы были доступны для большого количества граждан.
arusak-diploms-srednee.ru/kupit-attestat-za-11-klass
Удачи!
https://bk-zenit-app.ru/
Привет!
Купить документ университета можно в нашей компании в Москве.
ast-diplom.com/kupit-diplom-moskva
Привет, друзья!
Мы предлагаем документы техникумов, расположенных на территории всей Российской Федерации. Можно купить диплом за любой год, включая документы старого образца. Дипломы и аттестаты делаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригиналов. Они заверяются всеми необходимыми печатями и штампами.
http://www.trngamers.co.uk/read-blog/1222
Привет, друзья!
Где заказать диплом по актуальной специальности?
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по приятным ценам. Цена может зависеть от выбранной специальности, года получения и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы документы были доступны для большинства наших граждан.
Для вас изготавливаем дипломы любых профессий по невысоким тарифам.
http://www.gift-me.net/blogs/167072/%D0%92%D0%B0%D1%88-%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%9A%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%B8-%D0%93%D0%B0%D1%80%D0%B0%D0%BD%D1%82%D0%B8%D1%8F
Будем рады вам помочь!.
Здравствуйте!
Заказать документ о получении высшего образования можно у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любой специальности, включая документы СССР. Гарантируем, что в случае проверки документов работодателем, никаких подозрений не возникнет.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным тарифам. Цена может зависеть от выбранной специальности, года выпуска и ВУЗа. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большого количества граждан.
military-lip-b05.notion.site/f82a27b820314e24b42a5ea7bdd28c59/
Рады помочь!
Добрый день!
Как быстро получить диплом магистра? Легальные способы
dopalnenie.listbb.ru/viewtopic.php?f=3&t=710
Окажем помощь!.
Добрый день!
Приобрести документ института вы сможете у нас в Москве.
ast-diploms24.ru/kupit-diplom-moskva
Успехов в учебе!
Здравствуйте!
Где заказать диплом специалиста?
Мы готовы предложить документы ВУЗов, которые находятся в любом регионе России. Вы сможете купить диплом от любого ВУЗа, за любой год, включая сюда документы СССР. Дипломы делаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они будут заверены всеми требуемыми печатями и подписями.
Мы готовы предложить дипломы любых профессий по выгодным тарифам.
ast-diplomy24.ru/kupit-diplom-voronezh
Окажем помощь!
Привет, друзья!
Предлагаем документы техникумов, расположенных на территории всей Российской Федерации. Вы сможете заказать диплом от любого учебного заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать настоящие дипломы, которые не отличить от оригинала. Они будут заверены необходимыми печатями и штампами.
Мы готовы предложить дипломы любых профессий по разумным ценам. Цена будет зависеть от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас важно, чтобы дипломы были доступными для большинства наших граждан.
landik-diploms-srednee.ru/svidetelstvo-o-razvode
Хорошей учебы!
Здравствуйте!
Где приобрести диплом специалиста?
nnars.ru/forum/suggestion-box/1216-легкий-способ-получить-диплом-быстро-и-просто#74602
Успехов в учебе!
Привет, друзья!
Заказать документ университета можно в нашей компании.
ast-diploms24.ru/kupit-diplom-voronezh
Привет, друзья!
Купить диплом университета
Наши специалисты предлагают максимально быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями. Наш диплом пройдет любые проверки, даже при использовании специально предназначенного оборудования. Достигайте своих целей быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
http://www.cyberpinoy.net/read-blog/33234
pulsevision.ru/forum/user/21402/
usa.life/read-blog/63074
friends.win/read-blog/3660
meat.ntnn.ru/personal/profile/index.php?register=yes
Привет, друзья!
Приобрести диплом о высшем образовании.
topbazz.com/read-blog/6562_vazhnye-sovety-po-pokupki-dokumentov-v-seti.html
Здравствуйте!
Заказать документ института вы сможете у нас в столице.
diplomyx24.ru/otzyvy
Хорошей учебы!
Здравствуйте!
Где приобрести диплом специалиста?
Заказать диплом любого ВУЗа.
naturetour.ru/club/user/19/blog/1594/
Привет!
Процесс получения диплома стоматолога: реально ли это сделать быстро?
http://www.openstreetmap.org/user/dilopluyy
Будем рады вам помочь!.
купить диплом о высшем образовании дешево ast-diploms.com .
купить диплом сейчас diplomasx.com .
Добрый день!
Мы готовы предложить дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Стоимость будет зависеть от той или иной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для большого количества наших граждан.
emiliohq529.blog-mall.com/27610340/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B7%D0%B0-%D0%B4%D0%B5%D0%BD%D1%8C%D0%B3%D0%B8-%D0%9F%D1%80%D0%B0%D0%B2%D0%B4%D0%B0-%D0%BE-%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B5-%D0%9E%D0%B1%D1%80%D0%B0%D0%B7%D0%BE%D0%B2%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
Здравствуйте!
Пошаговая инструкция по безопасной покупке диплома о высшем образовании
crystalroleplay.listbb.ru/ucp.php?mode=login&sid=012b3e354f2a64f04efe6f8f3da2b2a0
Будем рады вам помочь!.
навесы для машин
LAX Long Term Parking: Find secure and affordable options near LAX Airport. Reviews & details to choose the best fit for your trip https://lax-longtermparking.com/
Добрый день!
Мы предлагаем дипломы любой профессии по приятным ценам.
http://www.megafeedbd.com/2024/06/30/купить-диплом-о-среднем-образовании-о/
Здравствуйте!
Приобрести диплом ВУЗа.
bl.com.tw/index.php?title=??????_?_?????????_????????:_???_??????????_????????,_???????_????????_???????_??????????
Успехов в учебе!
Привет, друзья!
Где купить диплом специалиста?
itstagram.ru/read-blog/840
Хорошей учебы!
Привет, друзья!
Всё, что нужно знать о покупке аттестата о среднем образовании
spletninews.ru/legkiy-sposob-poluchit-diplom-nadezhno-i-konfidentsialno
Поможем вам всегда!.
Привет!
Где заказать диплом специалиста?
Заказать диплом любого ВУЗа.
http://www.fromrus.su/index.php?/gallery/image/325-как-найти-проверенный-интернет-магазин-с-обширным-выбором-дипломов/
Привет, друзья!
Мы можем предложить дипломы любой профессии по приятным тарифам.
sngine.codiantprod.com/blogs/221/Ценные-рекомендации-по-покупки-документа-в-сети
купить дипломы училища в москве asxdiplomik24.ru .
Привет!
Мы предлагаем выгодно и быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Данный диплом способен пройти лубую проверку, даже с использованием специально предназначенного оборудования. Достигайте своих целей быстро и просто с нашим сервисом.
forum.infinite-soul.org/viewtopic.php?f=64&t=16412
Хорошей учебы!
Привет, друзья!
Заказать документ ВУЗа вы можете у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы старого образца.
justvoip.listbb.ru/viewtopic.php?f=2&t=463
anoreksja.org.pl/viewtopic.php?f=13&t=1248287
demo.advised360.com/read-blog/162165
digdroid.com/forums/entry/signin
kondrateff.5bb.ru/viewtopic.php?id=6786#p12729
Привет!
Покупка диплома о среднем полном образовании: как избежать мошенничества?.
Купить диплом любого ВУЗа.
http://www.irc71.ru/index.php/jomsocial/groups/viewbulletin/264-pokupaem-diplom-v-izvestnom-onlajn-magazine-po-komfortnoj-stoimosti?groupid=47
nude pictures of dianna agron
nude 40 babes
tatum o neal nude pics
Привет!
Купить документ ВУЗа вы сможете в нашей компании в столице. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза. Гарантируем, что в случае проверки документа работодателем, никаких подозрений не появится.
Мы предлагаем дипломы любой профессии по разумным ценам. Цена будет зависеть от той или иной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы дипломы были доступны для большинства наших граждан.
http://www.roxgo.cl/gallery/image/4255-%D0%BD%D0%B8%D0%B7%D0%BA%D0%B8%D0%B5-%D1%86%D0%B5%D0%BD%D1%8B-%D0%B8-%D0%B2%D1%8B%D1%81%D0%BE%D0%BA%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Рады помочь!
Добрый день!
Мы можем предложить документы ВУЗов, расположенных в любом регионе Российской Федерации. Вы можете заказать качественный диплом за любой год, включая сюда документы старого образца СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригинала. Документы заверяются необходимыми печатями и штампами.
demo.1c-college.ru/club/user/7/blog/zakazyvaem-dokumenty-v-izvestnom-onlaynmagazine-po-komfortnoy-tsene/
Здравствуйте!
Как получить диплом техникума с упрощенным обучением в Москве официально
phongthuygiaphat.com/купить-заполненный-диплом/
Добрый день!
Где приобрести диплом специалиста?
Купить диплом о высшем образовании.
lada-clubs.ru/gallery/image/733-kak-podobrat-proverennyy-magazin-s-bolshim-vyborom-diplomov/
Привет, друзья!
Официальная покупка диплома вуза с сокращенной программой обучения в Москве
satopttorg.ru/forum/user/3418
Поможем вам всегда!.
Привет, друзья!
Мы готовы предложить дипломы любой профессии по доступным ценам.
http://www.lcwhost.org/events/event/11-какие-онлайн-магазины-с-документами-на-текущий-момент-существуют/
her explanation martianwallet wallet download
Привет, друзья!
Заказать документ института вы имеете возможность у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР.
heroes.app/blogs/new
terios2.ru/forums/index.php?autocom=gallery&req=si&img=3045
git.fuwafuwa.moe/thomasshaw9688/My-List/issues/new
visogo9427.ixbb.ru/viewtopic.php?id=118#p118
http://www.altasugar.it/new/index.php?option=com_kunena&view=topic&catid=3&id=124445&Itemid=151
Добро пожаловать на наш сайт! Здесь вы найдёте всё необходимое для успешного управления своими финансами.
дебетовая карта с возможностью оплаты коммунальных услуг
Мы предлагаем широкий выбор финансовых инструментов, которые помогут вам достичь своих целей и обеспечить стабильность в будущем.
В нашем ассортименте представлены различные виды банковских продуктов, инвестиции, страхование, кредиты и многое другое.
Наши эксперты помогувам выбрать наиболее подходящий инструмент, учитывая ваши индивидуальные потребности и предпочтения.
Мы предоставляем консультации и рекомендации, чтобы вы могли принять обоснованное решение и избежать возможных рисков.
Не упустите возможность воспользоваться нашими услугами и откройте для себя мир финансовых возможностей!
ипотечный кредит
Заходите на наш сайт, изучайте продукты и начните свой путь к финансовой стабильности прямо сейчас!
Привет!
Мы предлагаем документы техникумов, расположенных в любом регионе Российской Федерации. Можно приобрести диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, которые невозможно отличить от оригинала. Документы будут заверены необходимыми печатями и подписями.
insta.tel/read-blog/50227
Добрый день!
Где купить диплом специалиста?
Приобрести диплом о высшем образовании.
u90517ol.beget.tech/2024/07/04/bolshoy-vybor-dokumentov-v-znamenitom-magazine.html
Легальная покупка диплома о среднем образовании в Москве и регионах
diploms-x.com/kupit-diplom-krasnoyarsk
Добрый день!
Приобрести документ ВУЗа можно в нашем сервисе.
diploms-x24.ru/kupit-diplom-omsk
Привет!
Заказать документ института вы имеете возможность у нас в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых университетов РФ. Вы получите диплом по любым специальностям, включая документы образца СССР.
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16582&TITLE_SEO=16582-vash-diplom-_-nasha-zabota&MID=861050&result=new#message861050
riftynet.com/blogs/26120/Оформление-дипломов-с-гарантией-качества
visogo9427.ixbb.ru/viewtopic.php?id=119#p119
rentry.co/ipe5ww38
russiajoy.ru/diplom-za-korotkiy-srok-kachestvenno-i-bezopasno
Привет, друзья!
Можно ли быстро купить диплом старого образца и в чем подвох?
avtobestnews.ru/diplomyi-s-garantiey-podlinnosti-i-kachestva
Привет!
Купить документ о получении высшего образования вы можете у нас.
ast-diplom24.ru/otzyvy
Успехов в учебе!
Промокоды Vavada казино обеспечивают доступ к специальным бонусам. Эти коды помогают увеличить баланс и наслаждаться привилегиями во время игры.
Привет!
Предлагаем документы техникумов, расположенных на территории всей Российской Федерации. Можно купить качественный диплом за любой год, включая документы старого образца. Документы выпускаются на бумаге высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригинала. Документы будут заверены всеми необходимыми печатями и подписями.
Мы изготавливаем дипломы любых профессий по приятным тарифам. Стоимость зависит от выбранной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для большого количества наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-omske В
Успехов в учебе!
стоимость видеостены стоимость видеостены .
Промокоды Drip казино обеспечивают доступ к эксклюзивным бонусам. Эти коды помогают игрокам наслаждаться улучшенными условиями игры и получить дополнительные привилегии.
Добрый день!
Купить документ о получении высшего образования вы сможете в нашей компании.
ast-diplomas24.ru/kupit-diplom-ekaterinbur
Здравствуйте!
Приобрести документ о получении высшего образования вы можете в нашем сервисе.
asxdiplomik.com/kupit-diplom-ekaterinbur
Успешной учебы!
https://emdrive.echothis.com/User:JaclynLongo78
Используйте промокоды Vavada казино и получайте бонусы для любимых игр. Сделайте игровой процесс еще интереснее с дополнительными возможностями для выигрыша.
Привет, друзья!
Ьожем предложить документы ВУЗов, расположенных на территории всей России. Можно купить качественно напечатанный диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригинала. Они заверяются необходимыми печатями и подписями.
Мы предлагаем дипломы любой профессии по приятным ценам. Цена будет зависеть от конкретной специальности, года получения и университета. Стараемся поддерживать для покупателей адекватную политику тарифов. Для нас очень важно, чтобы дипломы были доступными для большого количества наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe В
Успешной учебы!
купить диплом перманентный макияж asxdiplomik24.ru .
Привет!
Мы готовы предложить документы техникумов, которые находятся на территории всей Российской Федерации. Можно заказать диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Документы печатаются на бумаге высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Они будут заверены необходимыми печатями и штампами.
1yenptlug.widblog.com/83253775/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет, друзья!
Быстрая схема покупки диплома старого образца: что важно знать?
vip.rolevaya.info/viewtopic.php?id=4973#p8524
Всегда вам поможем!.
Добрый день!
Приобрести документ университета вы сможете у нас в Москве.
ast-diplomy.com/kupit-diplom-magistra
Добрый день!
Реально ли приобрести диплом стоматолога? Основные этапы
gioturbobp.com/blogs/33/Важные-советы-по-приобретению-документов-в-сети-интернет
Добрый день!
Купить документ ВУЗа вы сможете у нас в Москве.
diploms-x24.ru/kupit-diplom-nizhnij-novgorod
Успехов в учебе!
Привет, друзья!
Официальное получение диплома техникума с упрощенным обучением в Москве
dom-nam.ru/index.php/forum/stroitelnye-kompanii/50337-kupit-diplom#91222
Окажем помощь!.
Здравствуйте!
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по разумным тарифам.
http://www.inlabs.la/удостоверение-юриста/
Привет, друзья!
Заказать документ университета вы имеете возможность в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить диплом по любым специальностям, включая документы старого образца. Гарантируем, что при проверке документов работодателем, подозрений не возникнет.
realtyintellect.ru/nastoyashhie-diplomyi-dostupno-i-udobno
weekofsport.ru/vyisshee-obrazovanie-dlya-vseh-byistro-i-legko
neoncity.gtaserv.ru/viewtopic.php?f=38&t=1969
school97.ru/vesti/view_profile.php?UID=210203
talkiachat.com/blogs/24/Правильно-заказываем-диплом-в-интернете-авторский-обзор
Здравствуйте!
Купить диплом любого ВУЗа
Наша компания предлагает выгодно и быстро заказать диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями. Диплом способен пройти лубую проверку, даже с применением специального оборудования. Решайте свои задачи быстро и просто с нашей компанией.
Где приобрести диплом по необходимой специальности?
http://www.lcwhost.org/events/event/13-легкий-поиск-интернет-магазина-продающего-дипломы-и-аттестаты/
licomklicu.ru/read-blog/1460
xtreme-motors.ru/forum/user/21996/
iloveyouclub.net/blogs/1919/Вы-хотите-выяснить-как-приобрести-диплом-в-сети-Ждем-Вас
http://www.privsocial.com/read-blog/280
купить диплом образования саратов https://diploms-x.com .
Привет!
Ьожем предложить документы техникумов, которые расположены на территории всей Российской Федерации. Можно заказать диплом от любого заведения, за любой год, в том числе документы старого образца. Документы выпускаются на бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригиналов. Они заверяются необходимыми печатями и штампами.
Мы предлагаем дипломы любой профессии по приятным ценам. Стоимость может зависеть от выбранной специальности, года получения и ВУЗа. Стараемся поддерживать для клиентов адекватную политику цен. Для нас очень важно, чтобы дипломы были доступны для большинства граждан.
arusak-diploms-srednee.ru/kupit-diplom-magistra В
Успехов в учебе!
Привет, друзья!
Где заказать диплом по нужной специальности?
Мы готовы предложить дипломы любых профессий по приятным ценам. Цена может зависеть от выбранной специальности, года получения и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы документы были доступны для большинства граждан.
Для вас можем предложить дипломы любой профессии по приятным тарифам.
medik-look.ru/kupit-diplom-v-moskve-legalno-i-nadezhno
Рады оказать помощь!.
Привет, друзья!
Мы предлагаем документы ВУЗов, которые находятся в любом регионе Российской Федерации. Можно купить качественный диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригинала. Они будут заверены всеми необходимыми печатями и штампами.
firstplat.com/read-blog/12286
Привет, друзья!
Купить диплом любого ВУЗа.
http://www.zooclub.com.ua/2675?t:16198
Удачи!
Здравствуйте!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
интайл.рф/communication/forum/messages/forum3/message10678/5290-vash-shans-na-uspekh-diplom-bez-truda?result=new#message10678
Окажем помощь!.
Здравствуйте!
Наш сервис предлагает приобрести диплом отличного качества, неотличимый от оригинального документа без использования дорогостоящего оборудования и опытного специалиста.
heimur.ru/index.php?/topic/128-купить-диплом-i98v/
Хорошей учебы!
Привет, друзья!
Где заказать диплом по необходимой специальности?
Приобрести диплом о высшем образовании.
avtovladelez.ru/byistroe-oformlenie-diploma-nadezhno-i-bezopasno
Привет!
Приобрести документ о получении высшего образования вы можете у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза.
allonlinesport.ru/legkiy-sposob-poluchit-diplom-nadezhno-i-konfidentsialno/
karkadan.ru/users/77829
datasphere.ru/club/user/15/blog/
forums.unigild.com/index.php?/topic/15237-диплом-в-кратчайшие-сроки-ваш-шаг-к-новой-жизни/
darknews.ru/diplom-na-zakaz-kachestvo-i-nadezhnost
her explanation keplr Extension
Привет, друзья!
Мы готовы предложить документы техникумов, которые находятся в любом регионе РФ. Можно приобрести диплом за любой год, включая сюда документы старого образца. Документы делаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и штампами.
tashtrans.ru/events/event/45-%D0%BD%D0%B8%D0%B7%D0%BA%D0%B8%D0%B5-%D1%80%D0%B0%D1%81%D1%86%D0%B5%D0%BD%D0%BA%D0%B8-%D0%B8-%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Привет, друзья!
Как быстро и легально купить аттестат 11 класса в Москве
mirfinrealty.ru/vash-diplom-bez-truda-i-usiliy
Будем рады вам помочь!.
https://www.center1339.com/bbs/board.php?bo_table=free&wr_id=1138
Привет, друзья!
Как не попасть впросак при покупке диплома колледжа или ПТУ в России.
Приобрести диплом ВУЗа.
geoamor.com/read-blog/30681
Привет!
Наши специалисты предлагают быстро приобрести диплом, который выполняется на оригинальной бумаге и заверен печатями, штампами, подписями. Документ пройдет любые проверки, даже при помощи профессионального оборудования. Достигайте цели быстро и просто с нашими дипломами.
fh7707pk.bget.ru/index.php?subaction=userinfo&user=ulomoweg
Удачи!
Привет!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
vk.com/vsepolezneyshe?w=wall-167217000_1050
Рады помочь!.
Добро пожаловать на наш сайт – ваше решение для всех финансовых потребностей!
Наши предложения
Мы предлагаем различные финансовые продукты: кредиты, банковские карты и займы, чтобы помочь вам достигнуть ваших целей и осуществить мечты.
займ под 0 процентов
Идеальные кредиты для ваших нужд
Нуждаетесь в финансировании на покупку жилья, автомобиля или образование? Наши кредитные программы разработаны с учетом ваших потребностей. Оформите кредит на нашем сайте, выбрав подходящие условия и сроки погашения.
Преимущества наших банковских карт
Наши банковские карты предоставляют:
Удобство безналичных платежей
Бонусы и привилегии
Оформите карту на нашем сайте и получайте кэшбэк, скидки у партнеров и участие в программе лояльности. Выберите карту с оптимальными лимитами и условиями обслуживания для себя.
Быстрые и удобные займы
Нужны деньги до зарплаты или на непредвиденные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок, чтобы вы могли решать финансовые вопросы без задержек.
Наши преимущества:
Простота и Удобство: Оформите заявку онлайн за несколько минут.
Надежность и Прозрачность: Мы гарантируем честные условия и отсутствие скрытых комиссий.
Индивидуальный Подход: Мы учитываем ваши личные обстоятельства и предлагаем оптимальные условия.
Не упустите возможность улучшить свою финансовую ситуацию!
улучшение кредитной истории
Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
С нами ваши мечты станут реальностью!
где купить поддельный диплом http://www.diploms-x.com .
Привет, друзья!
Приобрести диплом о высшем образовании
Наша компания предлагает быстро и выгодно заказать диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Документ пройдет лубую проверку, даже с использованием специфических приборов. Достигайте своих целей быстро и просто с нашими дипломами.
Где заказать диплом по актуальной специальности?
indianwomenorg.com/read-blog/5530
heyrodisscusion.listbb.ru/viewtopic.php?f=10&t=433
allods.mlx.su/gallery/image/436-благодаря-чему-интернет-магазины-с-дипломами-столь-популярны/?context=new
dachkanews.ru/nastoyashhie-diplomyi-bez-ozhidaniya/
avva.getbb.ru/viewtopic.php?f=3&t=571
Добрый день!
Купить документ о получении высшего образования можно в нашей компании. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, включая документы СССР. Гарантируем, что при проверке документа работодателями, подозрений не появится.
galantclub.od.ua/member.php?u=27724
rodina.listbb.ru/viewtopic.php?f=3&t=616
orbita.com.py/blogs/316/Советы-эксперта-что-помогут-легко-купить-документы
mpett.com/blogs/704/Что-нужно-для-изготовления-неотличимого-от-подлинника-диплома
master39.net/forum/user/4807/
Привет, друзья!
Купить документ о получении высшего образования можно в нашей компании. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите диплом по любой специальности, включая документы Советского Союза. Даем 100% гарантию, что при проверке документа работодателями, никаких подозрений не появится.
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по невысоким ценам. Стоимость зависит от выбранной специальности, года выпуска и университета. Всегда стараемся поддерживать для покупателей адекватную политику цен. Для нас очень важно, чтобы документы были доступными для большого количества наших граждан.
logozhajyzho.raidersfanteamshop.com/legko-pokupaem-diplom-v-internet-magazine-russian-diplom
Окажем помощь!
## Unlock Real Winnings: The Best Casino Apps That Pay Real Money
In the ever-evolving world of online gaming,
casino apps have revolutionized how we experience the thrill of gambling.
The allure of winning real money from the comfort of your smartphone is irresistible.
With countless options available, choosing the right
casino app can be daunting. Fear not! We’ve curated a guide to help you find the best casino apps that pay real money, ensuring a safe, exciting,
and potentially lucrative experience.
### Why Choose Casino Apps That Pay Real Money?
Casino apps that offer real money payouts provide a convenient
and exhilarating way to enjoy your favorite casino games.
Here are a few reasons why these apps are gaining immense popularity:
1. **Convenience**: Play anytime, anywhere.
Whether you’re commuting, relaxing at home, or on a break at work, casino apps are always at your fingertips.
2. **Variety of Games**: From classic table games like blackjack
and roulette to exciting slots and poker, these apps offer a
vast array of games to suit every player’s taste.
3. **Real Money Rewards**: Unlike free casino apps, these platforms give you the opportunity to win real cash, adding an extra
layer of excitement and motivation.
4. **Bonuses and Promotions**: Casino apps often provide enticing bonuses,
free spins, and promotions, enhancing your chances of winning big.
### Top Casino Apps That Pay Real Money
To ensure you have a seamless and rewarding experience, here are some of the
top-rated casino apps known for their reliability, security, and lucrative
payouts:
#### 1. **Betway Casino App**
Betway is a renowned name in the online gambling industry, and
its app lives up to the brand’s reputation. Offering a wide range of games, including slots, blackjack, roulette, and live dealer options,
Betway provides a secure and user-friendly platform. The app also boasts generous welcome bonuses and ongoing promotions to maximize your
winning potential.
#### 2. **888 Casino App**
888 Casino is a veteran in the online casino world, and its app is a testament to its excellence.
With a sleek design and an extensive game library,
888 Casino offers everything from slots and jackpots to table games and live casino
experiences. The app ensures secure transactions and
prompt payouts, making it a favorite among real money players.
#### 3. **LeoVegas Casino App**
LeoVegas is known for its mobile-first approach, making
it one of the best casino apps for real money gaming.
The app features a vast selection of games from top providers, including immersive live dealer games.
LeoVegas is also praised for its swift and hassle-free withdrawal process, allowing you
to enjoy your winnings without delay.
#### 4. **Royal Panda Casino App**
Royal Panda combines a fun and engaging gaming experience with the opportunity to win real
money. The app offers a rich variety of games, including popular
slots, table games, and live casino options. With its easy-to-navigate
interface and secure payment methods, Royal Panda ensures a smooth and rewarding gaming journey.
#### 5. **Jackpot City Casino App**
As the name suggests, Jackpot City is all about big wins.
This app offers a comprehensive selection of games, including
progressive jackpot slots that can yield life-changing payouts.
With its user-friendly design and top-notch security measures,
Jackpot City provides a trustworthy platform for real
money gambling.
### Tips for Maximizing Your Winnings
To make the most of your real money casino app experience, consider these tips:
1. **Choose Reputable Apps**: Stick to well-known and licensed
casino apps to ensure fair play and secure transactions.
2. **Take Advantage of Bonuses**: Utilize welcome bonuses,
free spins, and other promotions to boost your bankroll and increase your chances of winning.
3. **Manage Your Bankroll**: Set a budget and stick to it.
Avoid chasing losses and know when to take a break.
4. **Play Smart**: Familiarize yourself with the rules and strategies of the games you play.
Knowledge can significantly enhance your winning potential.
### Conclusion
Casino apps that pay real money offer an exciting and convenient way to
enjoy the thrill of gambling while giving you the chance to win actual
cash. By choosing reputable apps like Betway, 888 Casino, LeoVegas, Royal Panda, and Jackpot City,
you can ensure a secure and rewarding gaming experience.
So, download your preferred app, take advantage
of the bonuses, and get ready to unlock real winnings!
Happy gaming!
my site – “http://daun21.com/bbs/board.php?bo_table=free&wr_id=108005”
Привет, друзья!
Мы изготавливаем дипломы любых профессий по разумным ценам. Стоимость будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Для нас очень важно, чтобы дипломы были доступны для большинства наших граждан.
cashet110.laowaiblog.com/26683451/Покупка-диплома-Риски-и-Последствия-купить-диплом
На сайте https://radiolom71.ru/ закажите звонок для того, чтобы узнать всю нужную информацию о приеме радиодеталей, плат. Также принимаются и драгметаллы: золото, техническое серебро, платина и различные приборы. В компании работают компетентные, квалифицированные профессионалы, которые регулярно выкупают у населения, юридических лиц лом. Выкупаются как новые, так и б/у детали. Есть возможность связаться со специалистами наиболее удобным для себя способом. Пришлите фотографию либо наименование вещи, чтобы определить точную стоимость.
Добрый день!
Купить диплом любого ВУЗа.
antonovschool.ru/forum/messages/forum1/topic657/message672/?result=new#message672
Успехов в учебе!
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным ценам.
tygerspace.com/read-blog/5603_kak-najti-proverennyj-onlajn-magazin-kotoryj-prodaet-dokumenty.html?mode=day
Привет!
Где купить диплом по актуальной специальности?
Мы можем предложить дипломы любых профессий по выгодным тарифам. Стоимость может зависеть от конкретной специальности, года получения и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику тарифов. Для нас важно, чтобы дипломы были доступными для подавляющей массы граждан.
Для вас предлагаем дипломы любых профессий по выгодным ценам.
domainrama.com/read-blog/822_nadezhnyj-magazin-s-obshirnym-vyborom-dokumentov.html
Рады оказаться полезными!.
Привет, друзья!
Где приобрести диплом специалиста?
Мы готовы предложить документы ВУЗов, расположенных в любом регионе РФ. Можно приобрести качественный диплом от любого заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы выпускаются на “правильной” бумаге самого высокого качества. Это дает возможности делать государственные дипломы, не отличимые от оригиналов. Документы будут заверены всеми обязательными печатями и штампами.
Мы предлагаем дипломы любых профессий по доступным ценам.
ast-diploms.com/kupit-diplom-nizhnij-novgorod
Поможем вам всегда!
Привет, друзья!
Приобрести диплом о высшем образовании.
gamemotors.ru/gde-kupit-diplom-bez-predoplatyi
Привет, друзья!
Официальная покупка диплома вуза с упрощенной программой обучения
http://www.mrkineshma.ru/support/forum/view_profile.php?UID=223964
Будем рады вам помочь!.
Здравствуйте!
Где приобрести диплом специалиста?
forum.resmihat.kz/viewtopic.php?f=10&t=2265818
Успехов в учебе!
Здравствуйте!
Наш сервис предлагает заказать диплом отличного качества, который не отличить от оригинального документа без использования дорогостоящего оборудования и квалифицированного специалиста.
slavsbyt.ru/index.php?subaction=userinfo&user=emaloz
Успешной учебы!
Привет!
Заказать документ о получении высшего образования вы сможете в нашем сервисе. Мы оказываем услуги по производству и продаже документов об окончании любых университетов Российской Федерации.
u-cars.ru/modules.php?name=Your_Account&op=userinfo&username=anizecin
vyvoj.barvinek.net/doku.php?id=landsdiplomy
knigigo.ru/?post_type=topic&p=17457
o926476g.bget.ru/users/olajol
rf-unicron.ru/index.php?/topic/442-купить-диплом-цена-j816f/
next page Dym wallet keplr
Привет!
Где приобрести диплом специалиста?
Купить диплом о высшем образовании.
androidinweb.ru/diplom-lyuboy-spetsialnosti-kachestvenno-i-bezopasno
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
newsinweek.ru/poluchite-diplom-bez-lishnih-voprosov/
Привет!
Купить документ о получении высшего образования можно у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите диплом по любой специальности, включая документы образца СССР.
seriallove.bbok.ru/viewtopic.php?id=7201#p123246
magnat-matras.ru/forum/user/50794/
lubov.listbb.ru/viewtopic.php?f=2&t=484
stylist-profi.ru/forum/user/200285/
films.name/viewforum.php?f=143
Somee in the Biden administration complain that servicers are producing a mess
of the modifications and hurting borrowers.
My web site :: student Loan pause
Добрый день!
Приобретение диплома ВУЗа с сокращенной программой обучения в Москве.
Приобрести диплом о высшем образовании.
pora-valit.com/wiki/index.php?title=%D0%92_%D1%81%D0%BB%D1%83%D1%87%D0%B0%D0%B5_%D0%B5%D1%81%D0%BB%D0%B8_%D0%BF%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D0%BE%D0%B2%D0%B0%D0%BB%D0%B8%D1%81%D1%8C_%D0%BA%D0%BB%D0%B0%D0%BF%D0%B0%D0%BD%D0%B0,_%D0%B7%D0%B0%D0%B4%D0%B2%D0%B8%D0%B6%D0%BA%D0%B8,_%D0%BC%D0%B0%D0%BD%D0%BE%D0%BC%D0%B5%D1%82%D1%80%D1%8B_-_%D0%B7%D0%B0%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5!
## Unlock Real Winnings: The Best Casino Apps That Pay Real Money
In the ever-evolving world of online gaming, casino apps have revolutionized
how we experience the thrill of gambling. The allure
of winning real money from the comfort of your smartphone
is irresistible. With countless options available,
choosing the right casino app can be daunting. Fear not!
We’ve curated a guide to help you find the best casino apps that
pay real money, ensuring a safe, exciting, and potentially lucrative experience.
### Why Choose Casino Apps That Pay Real Money?
Casino apps that offer real money payouts provide a convenient and exhilarating way to enjoy
your favorite casino games. Here are a few reasons why these apps
are gaining immense popularity:
1. **Convenience**: Play anytime, anywhere. Whether you’re commuting, relaxing at home, or on a break at work, casino apps are always at your fingertips.
2. **Variety of Games**: From classic table games like blackjack and roulette to exciting slots and poker, these apps offer a vast array of games to suit every player’s
taste.
3. **Real Money Rewards**: Unlike free casino apps,
these platforms give you the opportunity to win real cash, adding an extra layer
of excitement and motivation.
4. **Bonuses and Promotions**: Casino apps often provide enticing bonuses, free spins, and promotions, enhancing your chances
of winning big.
### Top Casino Apps That Pay Real Money
To ensure you have a seamless and rewarding experience, here are some of the top-rated casino apps known for their reliability, security, and
lucrative payouts:
#### 1. **Betway Casino App**
Betway is a renowned name in the online gambling industry,
and its app lives up to the brand’s reputation. Offering a wide range of games, including slots,
blackjack, roulette, and live dealer options, Betway provides a secure and user-friendly platform.
The app also boasts generous welcome bonuses and ongoing promotions to maximize your winning potential.
#### 2. **888 Casino App**
888 Casino is a veteran in the online casino world, and its app is a
testament to its excellence. With a sleek design and an extensive game library, 888 Casino offers everything from
slots and jackpots to table games and live casino experiences.
The app ensures secure transactions and prompt payouts, making it a favorite
among real money players.
#### 3. **LeoVegas Casino App**
LeoVegas is known for its mobile-first approach, making it one of the best casino apps for
real money gaming. The app features a vast selection of
games from top providers, including immersive live dealer games.
LeoVegas is also praised for its swift and hassle-free
withdrawal process, allowing you to enjoy your winnings without delay.
#### 4. **Royal Panda Casino App**
Royal Panda combines a fun and engaging gaming experience with the opportunity to win real money.
The app offers a rich variety of games, including popular slots, table
games, and live casino options. With its easy-to-navigate interface and secure payment
methods, Royal Panda ensures a smooth and rewarding gaming journey.
#### 5. **Jackpot City Casino App**
As the name suggests, Jackpot City is all about big
wins. This app offers a comprehensive selection of games, including progressive jackpot slots that can yield life-changing payouts.
With its user-friendly design and top-notch security
measures, Jackpot City provides a trustworthy platform for real money gambling.
### Tips for Maximizing Your Winnings
To make the most of your real money casino app experience,
consider these tips:
1. **Choose Reputable Apps**: Stick to well-known and licensed casino apps to ensure fair play
and secure transactions.
2. **Take Advantage of Bonuses**: Utilize welcome
bonuses, free spins, and other promotions to boost your bankroll
and increase your chances of winning.
3. **Manage Your Bankroll**: Set a budget and stick to it.
Avoid chasing losses and know when to take a break.
4. **Play Smart**: Familiarize yourself with the rules
and strategies of the games you play. Knowledge can significantly enhance your winning potential.
### Conclusion
Casino apps that pay real money offer an exciting and convenient way to enjoy the thrill of gambling while giving you the chance to win actual cash.
By choosing reputable apps like Betway, 888 Casino, LeoVegas, Royal Panda, and Jackpot City, you can ensure a secure and rewarding gaming
experience. So, download your preferred app, take advantage of the
bonuses, and get ready to unlock real winnings!
Happy gaming!
my web page :: “http://shalomsilver.kr/bbs/board.php?bo_table=free&wr_id=193473”
Привет!
Купить диплом о высшем образовании
Мы предлагаем быстро и выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Наш документ способен пройти любые проверки, даже с использованием специального оборудования. Достигайте свои цели быстро и просто с нашей компанией.
Где заказать диплом по актуальной специальности?
samanalevi.com.tr/read-blog/64
art-gymnastics.ru/users/54
ukrevent.ru/kupit-diplom-onlayn-byistro-i-legko/
connectme.live/blogs/985/Решили-узнать-как-приобрести-документы-в-сети-недорого-Заходите
allnewstroy.ru/vash-byistryiy-put-k-novomu-diplomu
Добрый день!
Мы можем предложить дипломы любой профессии по приятным тарифам.
http://www.djcuna.social/blogs/217/На-что-именно-обратить-свое-внимание-при-покупки-документов-в
Привет!
Приобрести документ университета можно в нашей компании. Мы предлагаем документы об окончании любых университетов РФ. Вы получите необходимый диплом по любой специальности, включая документы Советского Союза. Гарантируем, что в случае проверки документа работодателями, подозрений не возникнет.
jogibaba.com/blogs/214/Быстрое-Оформление-Дипломов-Надежно-и-Легально
nedvigimost.bbok.ru/viewtopic.php?id=27329#p46774
3b1bkqfhg.theideasblog.com/28725622/Советы-что-помогут-подобрать-проверенный-онлайн-магазин-с-дипломами
http://www.brodyaga.org/club/user/110581/blog/6290/
sz.80lvl.ru/viewtopic.php?f=9&t=1920
LGA Long Term Parking: Find secure & affordable options near LaGuardia Airport. Reviews & details to choose the best fit for your trip https://lga-longtermparking.com/
Здравствуйте!
Где приобрести диплом по актуальной специальности?
Приобрести диплом любого ВУЗа.
http://www.rugladyseminars.com/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=399
Здравствуйте!
Купить диплом ВУЗа.
wiki.mdomtv.net/index.php?title=??????_??????_?_??????:_?????????_??????????
Хорошей учебы!
Здравствуйте!
Наши специалисты предлагают выгодно приобрести диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Документ способен пройти любые проверки, даже с применением профессионального оборудования. Достигайте своих целей быстро с нашим сервисом.
vk.com/public50470295?w=wall-50470295_628
Хорошей учебы!
Привет, друзья!
Мы можем предложить дипломы любой профессии по разумным тарифам.
ukrevents.ru/oformlenie-diploma-onlayn-za-neskolko-shagov/
Привет, друзья!
Где приобрести диплом по актуальной специальности?
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным ценам. Стоимость может зависеть от выбранной специальности, года выпуска и университета. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступны для большого количества граждан.
Для вас изготавливаем дипломы любой профессии по приятным тарифам.
moust.lv/read-blog/222_pochemu-na-poryadok-deshevle-i-proshe-zakazat-diplom-universiteta.html
Всегда вам поможем!.
Здравствуйте!
Где купить диплом специалиста?
Купить диплом о высшем образовании.
forum.recifalnews.fr/gallery/image/211-широкий-ассортимент-документов-в-знаменитом-интернет-магазине/
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным тарифам.
agama.su/articles/physignathus-lesueurii/general-info/
Привет, друзья!
Приобрести документ о получении высшего образования можно у нас в столице. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любым специальностям, включая документы Советского Союза.
uebkameri.listbb.ru/viewtopic.php?f=2&t=594
censornet.ru/kachestvennyie-diplomyi-za-dostupnyie-dengi/
onlaintelevizia.listbb.ru/posting.php?mode=post&f=2&sid=2e830ce6893138c037d229995edd9a33
yaoisennari.ekafe.ru/viewtopic.php?f=169&t=1786
forexgroupx.ru/oformlenie-diploma-bez-problem-i-zabot
Ищите Скачать музыку https://vkmusic.in/ – тогда зайдите на сайт и насладитесь шикарным выбором альбомов, треков, всех самых свежих хитов которые вы можете качать в любом количестве в мп3 на сайте. Лучшая подборка в машину, для отдыха, релакса. Вся музыка у нас.
купить диплом о среднем в тюмени https://diploms-x.com/ .
Привет, друзья!
Мы можем предложить дипломы любых профессий по приятным тарифам. Стоимость может зависеть от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для клиентов адекватную ценовую политику. Важно, чтобы дипломы были доступны для подавляющей массы наших граждан.
daltonuw011.life3dblog.com/26672116/Дипломы-за-деньги-Правда-о-Покупке-Образования-купить-диплом
Привет, друзья!
Мы предлагаем приобрести диплом высочайшего качества, неотличимый от оригинала без использования дорогостоящего оборудования и квалифицированного специалиста.
loket.kr/free/179794
Хорошей учебы!
Здравствуйте!
Стоимость дипломов высшего и среднего образования и процесс их получения.
Заказать диплом университета.
link4hope.com/read-blog/3643
## Unlock Real Winnings: The Best Casino Apps
That Pay Real Money
In the ever-evolving world of online gaming, casino apps
have revolutionized how we experience the thrill of gambling.
The allure of winning real money from the comfort of
your smartphone is irresistible. With countless options available, choosing the
right casino app can be daunting. Fear not!
We’ve curated a guide to help you find the best casino apps that pay real money, ensuring a safe, exciting, and potentially lucrative experience.
### Why Choose Casino Apps That Pay Real Money?
Casino apps that offer real money payouts provide a convenient and exhilarating way to enjoy your
favorite casino games. Here are a few reasons why these
apps are gaining immense popularity:
1. **Convenience**: Play anytime, anywhere. Whether you’re commuting, relaxing at home, or on a break
at work, casino apps are always at your fingertips.
2. **Variety of Games**: From classic table games like blackjack and roulette to exciting slots and poker, these apps offer a vast array of games to suit every player’s
taste.
3. **Real Money Rewards**: Unlike free casino apps, these
platforms give you the opportunity to win real cash, adding an extra layer
of excitement and motivation.
4. **Bonuses and Promotions**: Casino apps often provide enticing bonuses, free
spins, and promotions, enhancing your chances of winning big.
### Top Casino Apps That Pay Real Money
To ensure you have a seamless and rewarding experience, here are some of the top-rated
casino apps known for their reliability, security, and lucrative
payouts:
#### 1. **Betway Casino App**
Betway is a renowned name in the online gambling industry, and
its app lives up to the brand’s reputation. Offering a wide range of games, including slots, blackjack, roulette, and live dealer options, Betway
provides a secure and user-friendly platform. The app also boasts generous welcome bonuses and ongoing promotions to maximize your
winning potential.
#### 2. **888 Casino App**
888 Casino is a veteran in the online casino world, and its app is a
testament to its excellence. With a sleek design and an extensive game library, 888
Casino offers everything from slots and jackpots
to table games and live casino experiences. The app ensures secure
transactions and prompt payouts, making it a favorite among real money players.
#### 3. **LeoVegas Casino App**
LeoVegas is known for its mobile-first approach, making it one of the best
casino apps for real money gaming. The app features a vast selection of games from top providers, including immersive live dealer games.
LeoVegas is also praised for its swift and hassle-free withdrawal process, allowing you to enjoy your winnings without delay.
#### 4. **Royal Panda Casino App**
Royal Panda combines a fun and engaging gaming experience with the opportunity to win real
money. The app offers a rich variety of games, including popular slots, table games, and live casino options.
With its easy-to-navigate interface and secure payment methods, Royal Panda ensures a
smooth and rewarding gaming journey.
#### 5. **Jackpot City Casino App**
As the name suggests, Jackpot City is all about big wins.
This app offers a comprehensive selection of games, including progressive
jackpot slots that can yield life-changing
payouts. With its user-friendly design and top-notch security measures,
Jackpot City provides a trustworthy platform for real money gambling.
### Tips for Maximizing Your Winnings
To make the most of your real money casino app
experience, consider these tips:
1. **Choose Reputable Apps**: Stick to well-known and licensed casino apps to
ensure fair play and secure transactions.
2. **Take Advantage of Bonuses**: Utilize welcome bonuses, free spins, and
other promotions to boost your bankroll and increase your chances of winning.
3. **Manage Your Bankroll**: Set a budget and stick to it.
Avoid chasing losses and know when to take a break.
4. **Play Smart**: Familiarize yourself with the rules and strategies of the games you play.
Knowledge can significantly enhance your winning potential.
### Conclusion
Casino apps that pay real money offer an exciting
and convenient way to enjoy the thrill of gambling while giving you the chance to win actual cash.
By choosing reputable apps like Betway, 888 Casino, LeoVegas, Royal Panda, and Jackpot
City, you can ensure a secure and rewarding gaming experience.
So, download your preferred app, take advantage of the bonuses, and get ready to unlock real winnings!
Happy gaming!
Feel free to visit my site :: “http://www.difonn.com/gnu5/bbs/board.php?bo_table=free&wr_id=99077”
Привет!
Где купить диплом специалиста?
Купить диплом ВУЗа.
g95334gq.beget.tech/2024/07/11/legkiy-sposob-poluchit-diplom-bez-ekzamenov.html
Добрый день!
Купить документ ВУЗа вы можете в нашей компании. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Гарантируем, что в случае проверки документов работодателями, подозрений не появится.
Мы готовы предложить дипломы любых профессий по доступным тарифам. Стоимость будет зависеть от конкретной специальности, года выпуска и ВУЗа. Стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
test.krestikom.net/gallery/image/580-заказываем-документы-в-лучшем-онлайн-магазине-по-комфортной-цене/
Окажем помощь!
Привет, друзья!
Где купить диплом по актуальной специальности?
Купить диплом ВУЗа.
andreieusebiu.net/files/file/44-обширный-ассортимент-документов-в-знаменитом-магазине/
Привет, друзья!
Заказать документ университета вы можете в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых университетов РФ.
o926476g.bget.ru/users/olajol
vovkainfo.ru/forum/viewtopic.php?t=14000
mediawiki.envri.eu/index.php?title=diploman
brenderupmediterrane.free.fr/index.php?file=Members&op=detail&autor=ocypewo
forum.bedwantsinfo.nl/thread-585233.html
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца.
newrealgames.ru/diplom-za-korotkiy-srok-nadezhno-i-konfidentsialno
magnat-matras.ru/forum/user/50793/
itbitgroup.ru/oformlenie-diploma-pod-klyuch-bezopasno-i-legalno
http://www.testimonyforgod.com/read-blog/5440
komfort.rusff.me/viewtopic.php?id=13952#p41121
Привет!
Приобрести документ университета можно у нас.
diplomasx24.ru/kupit-diplom-krasnoyarsk
## Unlock Real Winnings: The Best Casino Apps That Pay Real Money
In the ever-evolving world of online gaming, casino apps have revolutionized how we experience the thrill
of gambling. The allure of winning real money from the comfort
of your smartphone is irresistible. With countless options available, choosing the right casino app can be daunting.
Fear not! We’ve curated a guide to help you find the best casino
apps that pay real money, ensuring a safe, exciting, and potentially lucrative
experience.
### Why Choose Casino Apps That Pay Real Money?
Casino apps that offer real money payouts provide a convenient
and exhilarating way to enjoy your favorite casino games.
Here are a few reasons why these apps are gaining immense popularity:
1. **Convenience**: Play anytime, anywhere. Whether you’re commuting,
relaxing at home, or on a break at work, casino apps
are always at your fingertips.
2. **Variety of Games**: From classic table games like blackjack and roulette to exciting slots and poker, these apps offer a
vast array of games to suit every player’s taste.
3. **Real Money Rewards**: Unlike free casino apps, these platforms give you the opportunity to win real cash, adding an extra layer of excitement and motivation.
4. **Bonuses and Promotions**: Casino apps often provide enticing
bonuses, free spins, and promotions, enhancing your chances of winning big.
### Top Casino Apps That Pay Real Money
To ensure you have a seamless and rewarding experience, here are some of the top-rated casino apps known for their reliability, security, and lucrative payouts:
#### 1. **Betway Casino App**
Betway is a renowned name in the online gambling industry,
and its app lives up to the brand’s reputation. Offering a wide range of games, including slots,
blackjack, roulette, and live dealer options, Betway provides a secure and user-friendly platform.
The app also boasts generous welcome bonuses and ongoing promotions
to maximize your winning potential.
#### 2. **888 Casino App**
888 Casino is a veteran in the online casino world, and its app is a testament to its excellence.
With a sleek design and an extensive game library, 888 Casino offers everything
from slots and jackpots to table games and live casino experiences.
The app ensures secure transactions and prompt payouts, making it a favorite
among real money players.
#### 3. **LeoVegas Casino App**
LeoVegas is known for its mobile-first approach, making it one of the best casino apps for real money gaming.
The app features a vast selection of games from top providers,
including immersive live dealer games. LeoVegas is also praised for its swift and hassle-free withdrawal process, allowing you to
enjoy your winnings without delay.
#### 4. **Royal Panda Casino App**
Royal Panda combines a fun and engaging gaming experience with the opportunity to win real money.
The app offers a rich variety of games, including popular slots, table games, and live casino options.
With its easy-to-navigate interface and secure payment methods, Royal Panda
ensures a smooth and rewarding gaming journey.
#### 5. **Jackpot City Casino App**
As the name suggests, Jackpot City is all about big wins. This app offers a comprehensive selection of games, including progressive jackpot slots that can yield
life-changing payouts. With its user-friendly design and top-notch security measures,
Jackpot City provides a trustworthy platform for real money gambling.
### Tips for Maximizing Your Winnings
To make the most of your real money casino app
experience, consider these tips:
1. **Choose Reputable Apps**: Stick to well-known and licensed casino apps to ensure fair play and secure transactions.
2. **Take Advantage of Bonuses**: Utilize welcome
bonuses, free spins, and other promotions to boost your bankroll and increase your chances of winning.
3. **Manage Your Bankroll**: Set a budget and stick to
it. Avoid chasing losses and know when to take a break.
4. **Play Smart**: Familiarize yourself with the rules
and strategies of the games you play. Knowledge can significantly enhance your
winning potential.
### Conclusion
Casino apps that pay real money offer an exciting and convenient way to enjoy the thrill
of gambling while giving you the chance to win actual cash.
By choosing reputable apps like Betway, 888 Casino, LeoVegas, Royal Panda,
and Jackpot City, you can ensure a secure and rewarding gaming experience.
So, download your preferred app, take advantage of the bonuses, and get ready to unlock
real winnings! Happy gaming!
My web blog: “http://ks-rubber.com/bbs/board.php?bo_table=free&wr_id=7771”
Добрый день!
Заказать документ института вы сможете у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы СССР.
mestovstrechi.flybb.ru/viewtopic.php?f=4&t=1290
l90226mw.beget.tech/2024/07/13/diplom-dlya-karernogo-rosta-kachestvenno-i-dostupno.html
sllife.ru/social/user/4216/forum/message/2439/7151/#message7151
driveme.rusff.me/viewtopic.php?id=2178#p105234
avtovladelez.ru/oformlenie-diploma-bez-problem-i-zabot
An attractive, mature woman with stunning curves indulges in intimate occasions with her spouse, leaving nothing to the imagination. 2 passionate lesbian beauties share carry on your workout network in captivating photos. A seductive woman flaunts her voluptuous figure, teasing using every move within a display of natural sensuality. An alluring woman over 50 explores pleasure using her favorite grown-up toy, embracing her desires with full confidence. A brunette beauty exudes youthful innocence in spite of her age, exciting with her normal charm. Images of any chocolate-skinned goddess reveal her irresistible curves and enticing physique. A curvaceous MILF showcases her delightful natural assets, fascinating viewers with the girl beauty. A slim milf bares this all, offering a close-up view of her glistening wetness. A older big tited woman sucking cocks elegance sheds her inhibitions, embracing pleasure together with abandon in a new moment of euphoria. A blonde bombshell exudes confidence and even allure in each and every body, captivating with her permanent magnet presence. Each photo tells a story regarding desire, passion, and unapologetic sensuality, welcoming viewers in to a world of pure temptation.
Привет, друзья!
Где купить диплом специалиста?
Мы готовы предложить документы ВУЗов, расположенных в любом регионе Российской Федерации. Вы можете купить качественно сделанный диплом за любой год, включая документы СССР. Дипломы выпускаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и штампами.
Мы готовы предложить дипломы любой профессии по выгодным тарифам.
diploms-x24.ru/kupit-diplom-ekaterinbur
Рады оказаться полезными!
Добрый день!
Предлагаем документы ВУЗов, расположенных на территории всей РФ. Можно приобрести качественно сделанный диплом за любой год, указав актуальную специальность и оценки за все дисциплины. Документы выпускаются на бумаге высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригиналов. Они заверяются всеми обязательными печатями и подписями.
Мы готовы предложить дипломы любой профессии по доступным тарифам. Стоимость зависит от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику тарифов. Для нас важно, чтобы дипломы были доступными для большого количества наших граждан.
arusak-diploms-srednee.ru/kupit-diplom-sssr В
Успешной учебы!
Привет!
Заказать диплом ВУЗа.
http://www.import-moto.com/users/88
Здравствуйте!
Приобрести документ ВУЗа можно в нашем сервисе.
diplomasx24.ru/kupit-diplom-ekaterinbur
Удачи!
Привет!
Приобрести документ о получении высшего образования вы сможете в нашем сервисе.
ast-diplomy24.ru/kupit-diplom-krasnoyarsk
Привет!
Где приобрести диплом по необходимой специальности?
frank-shkola.ru/forum/messages/forum1/topic440/message453/?result=new#message453
Удачи!
реально ли купить диплом ast-diploms.com .
Добрый день!
Ьожем предложить документы техникумов, которые находятся в любом регионе России. Можно приобрести диплом от любого учебного заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они заверяются необходимыми печатями и штампами.
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по невысоким ценам. Стоимость зависит от той или иной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас важно, чтобы документы были доступными для большого количества граждан.
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe В
Успехов в учебе!
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашей компании. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любой специальности, любого года выпуска, включая документы Советского Союза.
ironway.ru/forum/viewtopic.php?f=5&t=22314
justvoip.listbb.ru/viewtopic.php?f=2&t=463
pdapal.com/read-blog/962
stars.flyboard.ru/viewtopic.php?f=1&t=973
http://www.mirmafii.ru/article/7564
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании в Москве.
ast-diplomy.com/kupit-diplom-omsk
Успехов в учебе!
На сайте https://olato.ru представлены ванны и комплектующие, а также душевые кабины, различные ограждения, инсталляции, полотенцесушители. Все товары высокого качества, разработаны лучшими брендами, которые используют уникальные и инновационные технологии для достижения нужного результата. Все конструкции прочные, надежные и наделены высоким качеством. Продукция реализуется по привлекательным расценкам, организуется оперативная доставка. За покупки предоставляются бонусы. Есть безупречный клиентский сервис.
Здравствуйте!
Заказать документ института вы сможете у нас.
ast-diploms24.ru/otzyvy
Привет!
Наша компания предлагает быстро заказать диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Данный документ способен пройти любые проверки, даже при использовании профессионального оборудования. Решите свои задачи быстро и просто с нашими дипломами.
ratingforex.ru/forum-forex/viewtopic.php?f=18&t=35616&sid=f68caf2cc1c72d393fe7b0bd77673496
Успешной учебы!
Привет!
Готовы предложить документы техникумов, расположенных на территории всей России. Вы можете заказать диплом за любой год, включая сюда документы старого образца. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и штампами.
Мы изготавливаем дипломы любых профессий по выгодным тарифам. Стоимость зависит от той или иной специальности, года получения и университета. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Для нас важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-omske В
Успехов в учебе!
Добрый день!
Мы готовы предложить документы ВУЗов, которые находятся на территории всей РФ. Вы можете приобрести качественно напечатанный диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Документы выпускаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые не отличить от оригиналов. Документы заверяются всеми требуемыми печатями и штампами.
leed.lol/read-blog/438
Добрый день!
Приобрести документ университета вы можете у нас в Москве.
ast-diploms.com/kupit-diplom-nizhnij-novgorod
Успешной учебы!
Добрый день!
Приобрести диплом о высшем образовании
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями. Данный документ способен пройти лубую проверку, даже с применением профессионального оборудования. Достигайте цели быстро и просто с нашим сервисом.
Где купить диплом специалиста?
odessaforum.getbb.ru/viewtopic.php?f=5&t=20402
alik.forumrpg.ru/viewtopic.php?id=6639#p275762
ya.10bb.ru/viewtopic.php?id=3615#p6544
http://www.hristianka.ru/forum/r/prev_loaded/1/
forum.qwas.ru/kupit-diplom-t19852.html
Здравствуйте!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
satopttorg.ru/forum/user/3418
Рады оказать помощь!.
Привет, друзья!
Мы готовы предложить дипломы любой профессии по доступным ценам.
isnw.ru/2024/06/30/купить-диплом-иргупс/
[u][b] Привет, друзья![/b][/u]
Мы можем предложить [b]дипломы[/b] любых профессий по разумным ценам. [b]Цена[/b] зависит от конкретной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для клиентов адекватную ценовую политику. Для нас важно, чтобы документы были доступными для большого количества граждан.
[url=http://fernandoyofo24803.eveowiki.com/706383/Фальшивый_диплом_Почему_это_не_Стоит_купить_диплом/]fernandoyofo24803.eveowiki.com/706383/Фальшивый_диплом_Почему_это_не_Стоит_купить_диплом[/url]
Здравствуйте!
Купить документ о получении высшего образования можно у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любой специальности, включая документы СССР. Гарантируем, что при проверке документов работодателем, никаких подозрений не возникнет.
Мы изготавливаем дипломы любой профессии по разумным тарифам. Стоимость будет зависеть от конкретной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику тарифов. Для нас важно, чтобы дипломы были доступны для большого количества наших граждан.
yasqueencommunity.com/blogs/351/Быстро-приобретаем-документы-в-интернет-магазине-Russian-Diplom
Будем рады вам помочь!
дипломы о высшем образовании вуза купить срочно дипломы о высшем образовании вуза купить срочно .
Hacked Credit cards Shop Credit cards
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $1 000 – Price $ 99.00
Item Western Union Transfers $3 00 – Price $ 249.00
* Prices on the website may vary slightly
http://buyclonedcard.cvv2cvc.net
Привет!
Мы можем предложить документы ВУЗов, которые находятся на территории всей РФ. Вы имеете возможность заказать качественно напечатанный диплом от любого учебного заведения, за любой год, включая сюда документы старого образца. Документы выпускаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми обязательными печатями и штампами.
togethers.mn.co/posts/61828771
Добрый день!
Где заказать диплом по необходимой специальности?
Мы готовы предложить документы институтов, расположенных на территории всей РФ. Вы можете заказать диплом от любого ВУЗа, за любой год, включая сюда документы старого образца. Дипломы выпускаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются необходимыми печатями и подписями.
Мы можем предложить дипломы любой профессии по приятным ценам.
asxdiplomik24.ru/kupit-diplom-magistra
Окажем помощь!
Привет, друзья!
Заказать диплом любого ВУЗа.
sonnick84.blog-a-story.com/8164343/%D0%A7%D1%82%D0%BE-%D1%81%D0%BC%D0%BE%D0%B6%D0%B5%D1%82-%D0%B2-%D0%BD%D0%B0%D1%88%D0%B5-%D0%B2%D1%80%D0%B5%D0%BC%D1%8F-%D0%BF%D1%80%D0%B5%D0%B4%D0%BE%D1%81%D1%82%D0%B0%D0%B2%D0%B8%D1%82%D1%8C-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD-%D1%81-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0%D0%BC%D0%B8
Привет!
Как не попасть впросак при покупке диплома колледжа или ПТУ в России
gamesfortop.ru/diplom-lyuboy-professii-kachestvenno-i-nadezhno
Будем рады вам помочь!.
Добрый день!
Где заказать диплом по необходимой специальности?
Заказать диплом ВУЗа.
gtafaccoes.net/forum/index.php?/gallery/image/2-как-подобрать-проверенный-магазин-с-широким-каталогом-дипломов/
Добрый день!
Где приобрести диплом специалиста?
nnars.ru/forum/suggestion-box/1217-ваш-путь-к-успеху-диплом-без-лишних-забот#74603
Хорошей учебы!
Здравствуйте!
Мы предлагаем документы техникумов, расположенных на территории всей РФ. Можно купить качественно сделанный диплом за любой год, в том числе документы старого образца. Дипломы и аттестаты делаются на бумаге самого высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и штампами.
network-6342899.mn.co/posts/61828984
Здравствуйте!
Легальные способы покупки диплома о среднем полном образовании
dui.forum-top.ru/login.php?action=in
Рады помочь!.
zac efron movies toilet scene euphoria season 2where can i watch tulsa king season 2movie the hungover gamesfridays imdb
Добрый день!
Купить документ о получении высшего образования можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых университетов РФ. Вы получите диплом по любой специальности, включая документы старого образца.
animesocial.su/blogs/3261/Оформление-диплома-без-лишних-вопросов
rodina.listbb.ru/viewtopic.php?f=3&t=650
mirstalkera.4admins.ru/viewtopic.php?f=50&t=2111
nadegda.listbb.ru/posting.php?mode=post&f=3&sid=4dc9894e7419fcd8b9192b08eab32219
forum.drustvogil-galad.si/index.php/topic,14576.0.html
Здравствуйте!
Приобрести документ о получении высшего образования вы сможете у нас в столице.
ast-diplomas.com/kupit-diplom-moskva
Привет!
Предлагаем документы ВУЗов, расположенных на территории всей России. Можно купить качественно сделанный диплом за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Документы будут заверены необходимыми печатями и штампами.
Мы готовы предложить дипломы любых профессий по доступным тарифам. Цена может зависеть от определенной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для покупателей адекватную политику тарифов. Для нас очень важно, чтобы документы были доступными для большинства наших граждан.
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge В
Успешной учебы!
На сайте https://penza-evakuator.ru/ закажите звонок для того, чтобы воспользоваться услугами эвакуатора: грузового, легкового. Для того чтобы заказать услугу, необходимо позвонить по обозначенному номеру. Возможна любая форма оплаты, а стоимость начинается от 2 500 рублей. Подача транспорта организуется в течение получаса. Работа в круглосуточном режиме, отсутствуют выходные. Организуется эвакуация мототехники, квадроциклов, малогабаритных, легковых автомобилей, спортивных машин, джипов, внедорожников.
24thainews.com
Здравствуйте!
Заказать документ института вы имеете возможность в нашем сервисе.
asxdiplomik24.ru/kupit-diplom-magistra
Успехов в учебе!
alcitynews.com
Добрый день!
Приобрести диплом любого университета
Мы предлагаем максимально быстро заказать диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Диплом способен пройти любые проверки, даже с применением специфических приборов. Достигайте свои цели быстро с нашей компанией.
Где купить диплом специалиста?
ya.bestbb.ru/viewtopic.php?id=2962#p6549
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
driveme.rusff.me/viewtopic.php?id=2115#p105171
forumjustwoman.getbb.ru/viewtopic.php?f=43&t=941
kino.10bb.ru/viewtopic.php?id=163545#p276485
Привет!
Мы изготавливаем дипломы любой профессии по выгодным тарифам.
gioturbobp.com/blogs/33/Важные-советы-по-приобретению-документов-в-сети-интернет
Здравствуйте!
Полезная информация как купить диплом о высшем образовании без рисков
telegra.ph/kupit-diplom-o-vysshem-obrazovanii-03-26
Здравствуйте!
Мы предлагаем документы техникумов, которые расположены на территории всей РФ. Вы сможете приобрести диплом за любой год, включая сюда документы старого образца. Дипломы и аттестаты печатаются на “правильной” бумаге самого высокого качества. Это дает возможность делать государственные дипломы, не отличимые от оригинала. Документы заверяются необходимыми печатями и штампами.
aubameyangclub.com/read-blog/1746
На сайте https://pro100-stone.ru закажите звонок для того, чтобы купить изделия, выполненные из ненатурального камня. В этой компании занимаются разработкой, производством подоконников, столешниц, раковин, моек, а также барных стоек и многого другого. Материал обладает поистине безграничными возможностями, что позволяет создавать удивительные шедевры как для коммерческих объектов, так и для дома. Создаются конструкции для учебных заведений, школ, медицинских центров, аэропортов.
Welcome to our Gay Blog, where we celebrate the diversity and beauty of the LGBTQ+ community. Explore articles, stories, and resources that embrace love, equality, and pride. Join us in fostering understanding, acceptance, and empowerment for all.
Привет!
Узнайте, как приобрести диплом о высшем образовании без рисков
faithstreamer.com/blogs/3169/Ваш-диплом-без-лишних-забот-быстро-и-безопасно
Рады оказать помощь!.
Привет!
Мы предлагаем дипломы любой профессии по приятным тарифам.
blackmastercomic.com/blog/2024/06/22/диплом-в-три-клика/
Добрый день!
Полезная информация как купить диплом о высшем образовании без рисков
newfinbiz.ru/kupit-diplomyi-dlya-vseh-spetsialnostey
Добрый день!
Где приобрести диплом специалиста?
Купить диплом любого университета.
http://www.santa4.su/gallery/image/254-kak-podyskat-nadezhnyy-magazin-s-obshirnym-vyborom-diplomov/
Привет!
Где купить диплом специалиста?
Заказать диплом о высшем образовании.
kvixi.com/blogs/1355/Широкий-ассортимент-документов-в-популярном-онлайн-магазине
Здравствуйте!
Купить диплом любого университета
Мы предлагаем выгодно и быстро купить диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями должностных лиц. Диплом способен пройти лубую проверку, даже с использованием специально предназначенного оборудования. Достигайте своих целей быстро с нашими дипломами.
Где заказать диплом специалиста?
antonovschool.ru/forum/messages/forum1/topic650/message665/?result=new#message665
3drus.ru/forum/topic_34806
goup.hashnode.dev/kupit-diplom-1-1-1
worksale777.blogspot.com/2024/06/blog-post_30.html
3drus.ru/forum/topic_34806
Привет, друзья!
Как правильно купить диплом колледжа и пту в России, подводные камни
ballinthe6.ca/blogs/15996/На-что-конкретно-обратить-внимание-при-покупки-диплома-в-интернете
Привет!
Готовы предложить документы ВУЗов, расположенных в любом регионе России. Можно приобрести качественный диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Документы печатаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригиналов. Документы заверяются необходимыми печатями и штампами.
Мы изготавливаем дипломы любой профессии по приятным тарифам. Цена может зависеть от той или иной специальности, года получения и университета. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Важно, чтобы дипломы были доступны для большого количества наших граждан.
arusak-diploms-srednee.ru В
Удачи!
купить диплом срочно купить диплом срочно .
Привет, друзья!
Купить документ о получении высшего образования вы имеете возможность у нас.
diplomyx24.ru/kupit-diplom-krasnoyarsk
Привет!
Купить документ о получении высшего образования можно в нашей компании. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любым специальностям, любого года выпуска, включая документы СССР.
n-staff.ru/forum?mode=edit&type=thread&forum_id=74041
jeepgarage.ru/forum/topic.php?forum=24&topic=755
video.listbb.ru/viewtopic.php?f=3&t=409
draiv.flybb.ru/viewtopic.php?f=2&t=748
vmestedeshevle.listbb.ru/viewtopic.php?f=10&t=13070
Привет!
Приобрести документ о получении высшего образования можно у нас в столице.
ast-diplomy.com/kupit-diplom-krasnoyarsk
Хорошей учебы!
Привет, друзья!
Предлагаем документы техникумов, расположенных в любом регионе РФ. Вы имеете возможность приобрести диплом от любого заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы делаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригиналов. Они будут заверены необходимыми печатями и подписями.
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по приятным тарифам. Стоимость будет зависеть от выбранной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
landik-diploms-srednee.ru/diplom-s-reestromkupit-kupit В
Удачи!
Привет, друзья!
Приобрести документ института можно у нас в Москве.
ast-diplom.com/kupit-diplom-vracha
Здравствуйте!
Заказать документ о получении высшего образования вы имеете возможность у нас. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы Советского Союза.
karasteamfulldmroleplay.getbb.ru/viewtopic.php?f=62&t=920
financetimenews.ru/vash-diplom-pod-klyuch-kachestvenno-i-bezopasno/
pytalovo.4admins.ru/viewtopic.php?f=15&t=2362
backshowtime.ru/kupit-diplom-byistro-i-nadezhno
productinn.mn.co/posts/62245206
Привет, друзья!
Аттестат школы купить официально с упрощенным обучением в Москве
lnx.hotelresidencevillateresaischia.com/casamicciola/index.php?option=com_k2&view=itemlist&task=user&id=439796
Будем рады вам помочь!.
Добрый день!
Приобрести документ института можно у нас.
diplomasx.com/kupit-diplom-o-srednem-obrazovanii
Успехов в учебе!
На сайте https://pacific-map.com/index.html вы ознакомитесь с картой США с городами, штатами. Перед вами самая полная карта автомобильных дорог США. Есть карта Атлантического, Тихоокеанского побережья, имеется физическая карта США. Только здесь указана самая полная и содержательная информация, которая прольет свет на многочисленные вопросы. Вся информация является содержательной, интересной, актуальной, а потому на нее точно можно положиться. Обращайтесь и вы сюда за информацией, если необходимо что-то уточнить.
Привет, друзья!
Мы можем предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Вы можете заказать диплом от любого учебного заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Документы заверяются всеми обязательными печатями и подписями.
berry.work/read-blog/14528
Официальная покупка диплома вуза с упрощенной программой обучения
diploms-x.com/kupit-diplom-vracha
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
weekofsport.ru/vash-diplom-kachestvo-i-autentichnost
Добрый день!
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков
glowsubs.ru/forum/messages/forum2/topic2498/message9860/?result=new#message9860
Рады оказаться полезными!.
Зайдите на сайт Научно-технического центра «Триада» https://triadacompany.ru/ который помогает тысячам предприятий обеспечивать промышленную и экологическую безопасность по всей России! Лучшие кадры, инновационный подход, опыт с 1991 года. Промышленная и экологическая безопасность, экспертиза, проектирование, консалтинг. Подробнее на сайте.
купить диплом в черногорске http://www.diploms-x.com/ .
Привет!
Мы можем предложить документы техникумов, которые расположены на территории всей РФ. Вы имеете возможность приобрести качественно напечатанный диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Документы печатаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригиналов. Они будут заверены необходимыми печатями и подписями.
http://www.nhps1914.com/wiki/%D0%97%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC_%D0%B2_%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC_%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82_%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5_%D0%BF%D0%BE_%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D0%BE%D0%B9_%D1%86%D0%B5%D0%BD%D0%B5
Добрый день!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
mosoblzerno.ru/index.php?subaction=userinfo&user=uduvy
Рады оказать помощь!.
Привет!
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
http://www.scaleforum.ru/member.php?u=62004
Всегда вам поможем!.
Привет, друзья!
Где заказать диплом специалиста?
Заказать диплом любого ВУЗа.
site2.liodiz.ru/2024/07/04/shirokiy-vybor-dokumentov-v-znamenitom-onlayn-magazine.html
Привет, друзья!
Мы можем предложить дипломы любых профессий по выгодным тарифам.
gracebook.app/blogs/1187/На-что-именно-обращать-внимание-при-покупки-диплома-в-сети
Привет, друзья!
Мы готовы предложить дипломы любой профессии по приятным ценам.
karriere.kv-architektur.de/купить-диплом-иргупс/
Добрый день!
Ьожем предложить документы техникумов, которые находятся в любом регионе Российской Федерации. Вы имеете возможность купить качественно напечатанный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригиналов. Они заверяются необходимыми печатями и штампами.
Мы готовы предложить дипломы любых профессий по приятным тарифам. Цена зависит от той или иной специальности, года выпуска и ВУЗа. Стараемся поддерживать для покупателей адекватную ценовую политику. Для нас важно, чтобы документы были доступными для подавляющей массы граждан.
arusak-diploms-srednee.ru/kupit-diplom-v-nizhnem-novgorodeВ
Успешной учебы!
Привет!
Приобрести диплом любого ВУЗа.
gamesmaker.ru/forum/common/offtopics/#replyform
Успешной учебы!
Добрый день!
Купить документ института можно у нас в столице.
ast-diplomy.com/kupit-diplom-ekaterinbur
Добрый день!
Мы готовы предложить дипломы любых профессий по невысоким ценам.
webyourself.eu/blogs/358414/ упите-?ипломы-Ѕыстро-и-Ќадежно
Добрый день!
Возможно ли купить диплом стоматолога, и как это происходит
newmedtime.ru/kupite-diplom-i-nachnite-novuyu-zhizn
Привет, друзья!
Где купить диплом по необходимой специальности?
Приобрести диплом о высшем образовании.
s24.team/club/user/148/blog/1602/
Сколько стоит диплом высшего и среднего образования и как его получить?
diploms-x.com/kupit-diplom-sankt-peterburg
Привет!
Заказать документ о получении высшего образования вы можете у нас в Москве.
ast-diplomas24.ru/kupit-diplom-o-srednem-obrazovanii
Хорошей учебы!
Здравствуйте!
Купить документ института можно у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы сможете получить диплом по любым специальностям, любого года выпуска, включая документы старого образца.
slliver.getbb.ru/viewtopic.php?f=62&t=944
ilovehabbo.bbon.ru/viewtopic.php?id=1569#p28987
mosfo.getbb.ru/viewtopic.php?f=12&t=921
nec.phorum.pl/posting.php?mode=newtopic&f=27&sid=ce6cff9dadfe0395fc7b85e22ea248d5
bdfeu.ukraine7.com/t19991-topic#36442
Привет!
Вопросы и ответы: можно ли быстро купить диплом старого образца?
slavsbyt.ru/index.php?subaction=userinfo&user=ytukih
Будем рады вам помочь!.
Здравствуйте!
Где заказать диплом по необходимой специальности?
Заказать диплом о высшем образовании.
flerus-shop.hcp.dilhost.ru/club/user/3/forum/message/861/857/
ремонт телефонов адреса
Здравствуйте!
Сколько стоит диплом высшего и среднего образования и как его получить?.
Купить диплом ВУЗа.
ld6aehw2v.get-blogging.com/28758210/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Добрый день!
Где купить диплом по актуальной специальности?
Купить диплом о высшем образовании.
xleks.ru/2024/07/04/shirokiy-katalog-dokumentov-v-znamenitom-internet-magazine.html
Привет!
Мы можем предложить документы техникумов, расположенных на территории всей России. Можно купить диплом от любого учебного заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты делаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы будут заверены необходимыми печатями и штампами.
депутат-ширинов.рф/content/nizkie-rastsenki-prekrasnoe-kachestvo-zakazyvai-dokumenty-onlain
Здравствуйте!
Купить диплом ВУЗа
Наша компания предлагает выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями должностных лиц. Данный документ способен пройти лубую проверку, даже с применением специальных приборов. Решайте свои задачи быстро с нашим сервисом.
Где купить диплом по нужной специальности?
link4hope.com/read-blog/3594
wiki.mdomtv.net/index.php?title=Ваш_идеальный_диплом:_быстро_и_легко
trading-labor.de/Надежные_дипломы_с_гарантией_конфиденциальности
bn.tobase.ru/viewtopic.php?f=30&t=3343
http://www.nitrnd.com/blogs/159790/Хотите-узнать-как-купить-диплом-в-интернете-Ждем-Вас
Привет!
Купить документ института вы сможете у нас. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Даем гарантию, что в случае проверки документа работодателем, никаких подозрений не возникнет.
http://www.odnopolchane.net/forum/member.php?u=546804
l90226mw.beget.tech/2024/07/07/kakie-internet-magaziny-s-diplomami-suschestvuyut-na-segodnyashniy-den.html
bffsquare.com/read-blog/1
bs.listbb.ru/viewtopic.php?f=3&t=624
azat.on.kg/blogs/1019/Какие-интернет-магазины-с-документами-на-сегодняшний-момент-имеются
Здравствуйте!
Заказать диплом любого университета.
deadreckoninggame.com/index.php/??????????_???????????_?_????????????????_??????????
Удачи!
Привет, друзья!
Купить документ университета вы имеете возможность у нас в Москве.
ast-diploms24.ru/kupit-diplom-moskva
Хорошей учебы!
Здравствуйте!
Как правильно купить диплом колледжа и ВУЗа в России, подводные камни
woman.build2.ru/viewtopic.php?id=14546#p44637
Рады оказать помощь!.
Привет, друзья!
Где приобрести диплом по необходимой специальности?
Мы можем предложить дипломы любой профессии по доступным ценам. Стоимость зависит от конкретной специальности, года получения и университета. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы документы были доступными для большинства граждан.
Для вас изготавливаем дипломы любой профессии по приятным тарифам.
mykinotime.ru/kupit-diplom-bez-posrednikov-byistro-i-nadezhno/
Будем рады вам помочь!.
Привет, друзья!
Заказать документ о получении высшего образования вы сможете у нас в столице.
diplomasx.com/kupit-diplom-o-srednem-obrazovanii
Хорошей учебы!
Добрый день!
Ьожем предложить документы техникумов, которые находятся в любом регионе Российской Федерации. Вы имеете возможность приобрести диплом за любой год, в том числе документы СССР. Дипломы и аттестаты делаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и подписями.
Мы предлагаем дипломы любых профессий по приятным ценам. Цена зависит от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для клиентов адекватную ценовую политику. Важно, чтобы документы были доступными для большинства граждан.
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske В
Хорошей учебы!
Добрый день!
Как получить диплом стоматолога быстро и официально.
Купить диплом ВУЗа.
g95334gq.beget.tech/2024/07/09/priobretaem-diplom-v-izvestnom-onlayn-magazine-po-vygodnoy-stoimosti.html
Здравствуйте!
Мы предлагаем приобрести диплом в высочайшем качестве, неотличимый от оригинального документа без участия специалиста высокой квалификации со сложным оборудованием.
islamdini.kg/index.php?subaction=userinfo&user=isasypa
Хорошей учебы!
Здравствуйте!
Мы изготавливаем дипломы любой профессии по доступным ценам.
passo.su/forums/index.php?autocom=gallery&req=si&img=3170
Привет, друзья!
Приобрести документ о получении высшего образования вы сможете у нас в столице.
ast-diplom24.ru/otzyvy
Успехов в учебе!
Здравствуйте!
Заказать документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых университетов Российской Федерации.
hardstorecr.com/mybb/showthread.php?tid=118161
kazrti.kz/index.php?subaction=userinfo&user=ekabyj
http://www.receptar.ru/forum/profile.php?action=show&member=1531
http://www.detskiy-mir.net/index.php?subaction=userinfo&user=atediko
forums.indexrise.com/thread-42657-post-222857.html#pid222857
Добрый день!
Предлагаем документы техникумов, расположенных в любом регионе России. Вы сможете купить диплом за любой год, включая документы старого образца. Документы выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они будут заверены всеми требуемыми печатями и штампами.
Мы готовы предложить дипломы любых профессий по приятным тарифам. Стоимость будет зависеть от выбранной специальности, года выпуска и университета. Стараемся поддерживать для клиентов адекватную ценовую политику. Для нас важно, чтобы дипломы были доступны для большого количества граждан.
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge В
Успешной учебы!
Добрый день!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
teplichnaya.ru/viewtopic.php?f=18&t=639548
Поможем вам всегда!.
Привет, друзья!
Предлагаем документы техникумов, которые находятся в любом регионе Российской Федерации. Можно купить диплом от любого заведения, за любой год, включая документы старого образца СССР. Документы выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются всеми необходимыми печатями и штампами.
Мы готовы предложить дипломы любой профессии по невысоким тарифам. Стоимость зависит от той или иной специальности, года выпуска и ВУЗа. Стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы документы были доступными для большого количества наших граждан.
arusak-diploms-srednee.ru/kupit-diplom-sssr В
Удачи!
Добрый день!
Купить диплом любого ВУЗа
Наша компания предлагает быстро и выгодно заказать диплом, который выполнен на оригинальном бланке и заверен печатями, штампами, подписями. Данный диплом пройдет лубую проверку, даже с использованием специально предназначенного оборудования. Решите свои задачи быстро с нашим сервисом.
Где приобрести диплом по необходимой специальности?
darknews.ru/legalnaya-pokupka-diplomov-konfidentsialno-i-bezopasno
ohoanshrf.thelateblog.com/28773648/Вы-хотите-выяснить-как-купить-диплом-в-сети-интернет-Ждем-Вас
kilcoynelilacfarm.com/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=401
climat-cold.ru/forum/user/3848/
avtolux48.ru/people/user/367/blog/7871/
Добрый день!
Приобрести диплом о высшем образовании.
alanyatoday.ru/users/76
Успешной учебы!
Привет, друзья!
Заказать документ ВУЗа можно в нашем сервисе. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца. Гарантируем, что в случае проверки документа работодателем, каких-либо подозрений не возникнет.
bvf.ru/forum/showthread.php?p=25249147#post25249147
huarenjiaohui.com/index.php?/gallery/image/125-быстрый-поиск-онлайн-магазина-который-реализует-дипломы-и-аттестаты/
http://www.djcuna.social/blogs/217/На-что-именно-обратить-свое-внимание-при-покупки-документов-в
xleks.ru/2024/07/08/bystryy-vybor-onlayn-magazina-kotoryy-realizuet-diplomy.html
fulldropshipping.com/index.php?/events/event/12-какие-интернет-магазины-с-документами-на-сегодняшний-день-есть/
На сайте https://cpo24.ru/ закажите звонок для того, чтобы получить допуск СРО. Документ будет на руках в течение суток. Стоимость услуги варьируется от 50 000 рублей. При этом отсутствуют надбавки, комиссии. В этой компании вы сможете получить СРО проектировщиков, строителей, а также энергоаудиторов, изыскателей либо воспользоваться услугой сопровождения проверок СРО. Все услуги выполняются ответственными, квалифицированными, грамотными сотрудниками. При этом работы обойдутся недорого.
Добрый день!
Мы предлагаем документы техникумов, которые находятся на территории всей РФ. Вы можете купить диплом за любой год, указав актуальную специальность и оценки за все дисциплины. Документы выпускаются на бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они заверяются всеми требуемыми печатями и штампами.
fijianvibe.com/blogs/780/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Быстрая покупка диплома старого образца: возможные риски
sportraketka.ru/byistroe-poluchenie-diploma-vash-shans-na-uspeh
Рады помочь!.
Добрый день!
Наша компания предлагает выгодно и быстро купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Документ способен пройти любые проверки, даже при помощи специального оборудования. Решайте свои задачи быстро с нашим сервисом.
ironway.ru/forum/viewtopic.php?f=12&t=12393
Успешной учебы!
Здравствуйте!
Купить диплом о высшем образовании
Наша компания предлагает быстро заказать диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Наш диплом пройдет любые проверки, даже при использовании специальных приборов. Достигайте цели быстро и просто с нашей компанией.
Где заказать диплом по актуальной специальности?
ya.7bb.ru/viewtopic.php?id=11639#p33323
worksale777.blogspot.com/2024/06/blog-post_30.html
molbiol.ru/forums/index.php?showtopic=1179953
mamapoltava.listbb.ru/viewtopic.php?f=39&t=4933
seriallove.bbok.ru/viewtopic.php?id=7015#p123048
купить диплом колледжа в самаре diplomasx.com .
Добрый день!
Где купить диплом по необходимой специальности?
Мы изготавливаем дипломы любых профессий по выгодным ценам. Цена будет зависеть от выбранной специальности, года выпуска и университета. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас важно, чтобы документы были доступны для большинства граждан.
Для вас изготавливаем дипломы любой профессии по приятным ценам.
poltavagok.ru/legalnaya-pokupka-diplomov-byistro-i-udobno/
Рады оказать помощь!.
Добрый день!
Мы можем предложить документы ВУЗов, которые находятся на территории всей Российской Федерации. Вы имеете возможность приобрести качественно напечатанный диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы печатаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые не отличить от оригинала. Они заверяются необходимыми печатями и штампами.
uf37mcli4.newsbloger.com/28789596/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
купить приложение к диплому ast-diploms.com .
Привет!
Мы изготавливаем дипломы любых профессий по выгодным тарифам.
forum.xpixel.ru/gallery/image/91-какие-онлайн-магазины-с-дипломами-существуют-на-сегодняшний-день/
Привет, друзья!
Сколько стоит получить диплом высшего и среднего образования легально?.
Заказать диплом о высшем образовании.
pp-galaktika.com.ua/index.php/%D0%95%D1%81%D0%BB%D0%B8_%D0%BF%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D0%BE%D0%B2%D0%B0%D0%BB%D0%B8%D1%81%D1%8C_%D0%BA%D0%BB%D0%B0%D0%BF%D0%B0%D0%BD%D0%B0,_%D0%BC%D0%B0%D0%BD%D0%BE%D0%BC%D0%B5%D1%82%D1%80%D1%8B,_%D0%B7%D0%B0%D0%B4%D0%B2%D0%B8%D0%B6%D0%BA%D0%B8_-_%D0%B6%D0%B4%D0%B5%D0%BC_%D0%92%D0%B0%D1%81!
Добрый день!
Купить диплом любого ВУЗа
landik-diploms-srednee.ru/kupit-diplom-v-kazani В
Успешной учебы!
Здравствуйте!
Как безопасно купить диплом колледжа или ВУЗа в России, что важно знать
financetimenews.ru/diplom-v-kratchayshie-sroki-vash-shag-k-novoy-zhizni
Всегда вам поможем!.
Привет!
Мы изготавливаем дипломы любой профессии по невысоким ценам. Цена зависит от выбранной специальности, года получения и университета. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большого количества граждан.
troyfq529.jts-blog.com/26705334/Дипломы-за-деньги-Правда-о-Покупке-Образования-купить-диплом
Привет, друзья!
Заказать документ о получении высшего образования можно в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов РФ. Вы получите необходимый диплом по любой специальности, включая документы старого образца. Гарантируем, что при проверке документа работодателем, никаких подозрений не появится.
Мы изготавливаем дипломы любых профессий по невысоким ценам. Стоимость может зависеть от выбранной специальности, года выпуска и университета. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас очень важно, чтобы документы были доступны для большинства граждан.
kaiztech.net/IPB/index.php?/gallery/image/426-заказываем-документы-в-лучшем-онлайн-магазине-по-выгодной-стоимости/
Рады помочь!
Здравствуйте!
Где купить диплом по актуальной специальности?
Мы предлагаем документы институтов, которые расположены на территории всей РФ. Вы имеете возможность приобрести диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на бумаге самого высшего качества. Это дает возможности делать государственные дипломы, которые невозможно отличить от оригинала. Они будут заверены всеми требуемыми печатями и штампами.
Мы готовы предложить дипломы любой профессии по приятным тарифам.
ast-diplom.com/kupit-diplom-sankt-peterburg
Поможем вам всегда!
Ищете металлический навес на заказ в Орехово-Зуеве? Vip-Naves предоставляет услуги по проектированию, изготовлению и монтажу навесов любой сложности. Наши инженеры-замерщики приедут в удобное для вас время, чтобы зафиксировать все ваши требования, сделать точные замеры и рассчитать проект на месте. Мы создаем бесплатный 3D макет, чтобы вы могли видеть, как будет выглядеть ваш навес. Заключаем договор с фиксированными ценами и сроками, а затем приступаем к производству. Вип-Навес использует только высококачественные материалы и профессиональное оборудование, что гарантирует долговечность наших конструкций. Доставка и монтаж проводятся в удобное для вас время, а по завершению работ производится окончательная оплата. Обратитесь к нам и получите надежный навес, который прослужит вам долгие годы!
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
http://www.physiobuettner.de/купить-диплом-мгакхис-или-любого-вуза/
Привет, друзья!
Мы предлагаем приобрести диплом в высоком качестве, неотличимый от оригинального документа без участия специалиста высокой квалификации со специальным оборудованием.
http://www.dachamania.ru/photo_gallrey/profile.php?uid=57389
Хорошей учебы!
Привет!
Мы предлагаем документы техникумов, которые расположены на территории всей России. Вы сможете купить диплом за любой год, включая сюда документы старого образца СССР. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригинала. Они будут заверены всеми необходимыми печатями и штампами.
realhindu.in/read-blog/5060
Привет!
Купить диплом университета
arusak-diploms-srednee.ru/kupit-diplom-magistra В
Удачи!
Добрый день!
Заказать документ о получении высшего образования вы имеете возможность в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов РФ.
http://www.yinyue7.com/forum.php?mod=viewthread&tid=32901&pid=135762&page=6&extra=page=1&filter=sortid&sortid=1#pid135762
dianov.bget.ru/forum/thread57492.html#1281061
http://www.igram.net/index.php?name=Account&op=userinfo&user_name=ydilocox
stranasp.ru/forum/viewtopic.php?pid=120885#p120885
cstrike.g-service.ru/index.php?/topic/48-купить-диплом-цена-c507n/
Привет!
Мы предлагаем дипломы любой профессии по приятным тарифам.
indungii.ro/forum/index.php?/gallery/image/4-для-чего-сегодня-приобретают-дипломы-в-сети/
Здравствуйте!
Приобрести документ университета можно в нашей компании в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы Советского Союза.
collie.fatbb.ru/posting.php?mode=post&f=18&sid=8982dce4614b46300ecb2553334077b0
woman.build2.ru/viewtopic.php?id=14556#p44661
ya.9bb.ru/viewtopic.php?id=5964#p11479
ya.0bb.ru/viewtopic.php?id=11997#p32007
buldingnews.ru/diplom-na-zakaz-kachestvo-i-nadezhnost
Привет, друзья!
Официальная покупка диплома вуза с сокращенной программой обучения в Москве
thcsphuhuu.pgdchauthanhdt.edu.vn/купить-диплом-о-среднем-техническом-о/
Добрый день!
Приобрести диплом о высшем образовании
Наши специалисты предлагают максимально быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Наш документ способен пройти лубую проверку, даже при помощи специфических приборов. Решите свои задачи быстро с нашими дипломами.
Где приобрести диплом по необходимой специальности?
vseogirls.ru/ofitsialnyie-diplomyi-kachestvo-i-legalnost
stareishina.com/gallery/image/3640-diploman-docicom/
molbiol.ru/forums/index.php?showtopic=1234113
azat.on.kg/blogs/1030/Купить-диплом-опыт-и-профессионализм
newsinweek.ru/ofitsialnyie-diplomyi-vyisshee-obrazovanie-bez-problem/
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по выгодным тарифам.
mdkl.ru/blogs/9185/4-е-ключевых-группы-онлайн-магазинов-продающих-документы
Привет!
Купить диплом о высшем образовании
landik-diploms-srednee.ru/svidetelstvo-o-razvode В
Хорошей учебы!
бонус промокод 1win
Здравствуйте!
Заказать диплом любого университета.
humhub.mn.co/posts/61724749
Привет!
Купить документ о получении высшего образования вы имеете возможность у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР.
vintfint.com/blogs/22902/Легальный-диплом-без-лишних-хлопот-узнайте-как
machineintelligence.mn.co/spaces/9349565/feed
army.clanfm.ru/viewtopic.php?f=2&t=38884
4division.ru/viewtopic.php?f=13&t=8629
visogo9427.ixbb.ru/viewtopic.php?id=119#p119
На сайте https://ustanovki-masla.ru представлена информация о том, какую установку, использующуюся для слива, а также откачки масла, лучше выбрать. Представлены и пневматические установки, которые собирают масло, которое уже отработало. Изучите функциональные, качественные устройства, предназначенные для замены масла и с ручным приводом. Также изучите и важные особенности, достоинства установок. Перед вами только самая актуальная и честная информация, которая обязательно понадобится.
Привет!
Где заказать диплом по нужной специальности?
Приобрести диплом о высшем образовании.
kurkure.ru/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=140
image source coinmarketcap
JFK Long Term Parking: Find secure & affordable options near JFK Airport. Reviews & details to choose the best fit for your trip jfk parking long term
Добрый день!
Где приобрести диплом по нужной специальности?
opros.flybb.ru/viewtopic.php?f=2&t=545
Удачи!
Добрый день!
Узнайте, как безопасно купить диплом о высшем образовании
vk.com/public50470295?w=wall-50470295_628
Рады помочь!.
britainrental.com
Привет, друзья!
Купить документ о получении высшего образования вы сможете в нашей компании. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любой специальности, включая документы СССР.
kids-news.ru/zakazhite-diplom-pryamo-seychas-i-nachnite-novuyu-kareru
generalarminius.com/viewtopic.php?t=155979
gazeta.ekafe.ru/viewforum.php?f=48
http://www.vocal.com.ua/node/62430
xn--80abvfb7cr.xn--p1ai/forum/messages/forum1/topic852/message759/?result=new#message759
Companies with high welcomelady.net levels of customer service usually have an excellent reputation and positive reviews.
[url=http://cloned-cards.cvv2cvc.net]Buy Cloned Cards Shop Cloned cards[/url]
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2 000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
[url=http://clonedcards.cvv2cvc.net]http://clonedcards.cvv2cvc.net[/url]
Добрый день!
Как получить диплом техникума официально и без лишних проблем
http://www.tuningevo.club/newforum/index.php?showuser=86824
Добрый день!
Где приобрести диплом по необходимой специальности?
Заказать диплом университета.
es-presto.ru/community/groups/0-0/176-ogromnyj-vybor-dokumentov-v-znamenitom-onlajn-magazine
Здравствуйте!
Наша компания предлагает быстро и выгодно заказать диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Документ пройдет любые проверки, даже с применением профессиональных приборов. Достигайте свои цели быстро и просто с нашими дипломами.
high.tforums.org/viewtopic.php?f=11&t=5673
Успешной учебы!
Привет, друзья!
Где приобрести диплом специалиста?
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным тарифам. Стоимость будет зависеть от той или иной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику цен. Важно, чтобы дипломы были доступными для большого количества наших граждан.
Для вас предлагаем дипломы любой профессии по приятным тарифам.
http://www.growingchurches.org/blogs/21881/Как-подобрать-проверенный-магазин-что-продает-документы
Рады оказаться полезными!.
Привет, друзья!
Мы изготавливаем дипломы любой профессии по выгодным тарифам. Цена зависит от конкретной специальности, года выпуска и ВУЗа. Стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступными для большого количества граждан.
nimmansocial.com/story6773725/купить-диплом-о-высшем-образовании
Добрый день!
Приобрести документ института можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, любого года выпуска, включая документы образца СССР. Гарантируем, что в случае проверки документов работодателем, каких-либо подозрений не возникнет.
Мы можем предложить дипломы любой профессии по приятным ценам. Стоимость может зависеть от конкретной специальности, года получения и университета. Стараемся поддерживать для покупателей адекватную политику тарифов. Для нас очень важно, чтобы дипломы были доступны для большинства наших граждан.
loolita.es/blogs/4320/Как-возможно-будет-недорого-приобрести-диплом-в-онлайн-магазине
Окажем помощь!
Здравствуйте!
Где приобрести диплом по нужной специальности?
Мы предлагаем документы институтов, расположенных в любом регионе Российской Федерации. Можно заказать качественно сделанный диплом от любого заведения, за любой год, включая документы старого образца СССР. Дипломы выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они будут заверены всеми требуемыми печатями и подписями.
Мы изготавливаем дипломы любой профессии по приятным ценам.
diplomasx24.ru/kupit-diplom-sankt-peterburg
Рады оказать помощь!
Привет, друзья!
Где купить диплом по нужной специальности?
Приобрести диплом ВУЗа.
http://www.irc71.ru/index.php/jomsocial/groups/viewbulletin/257-kak-podyskat-nadezhnyj-onlajn-magazin-s-obshirnym-katalogom-diplomov?groupid=47
нея диплом купить ast-diploms.com .
купить официальный диплом образование купить официальный диплом образование .
Добрый день!
Купить документ о получении высшего образования можно у нас.
ast-diplom24.ru/kupit-diplom-moskva
Успехов в учебе!
Здравствуйте!
Мы предлагаем заказать диплом высокого качества, неотличимый от оригинального документа без использования дорогостоящего оборудования и опытного специалиста.
usefulscript.ru/forum/showthread.php?tid=2468
Удачи!
Добрый день!
Заказать документ о получении высшего образования вы сможете в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ.
allods.mlx.su/forums/topic/321-купить-диплом-цена-p426g/
kochtagebuch.org/doku.php?id=premiummdiplomms
golpro.jp/userinfo.php?uid=13510#
avestalaw.ru/index.php?subaction=userinfo&user=ynijyhu
японецавто.рф/forum/user/51636/
Привет!
Мы предлагаем дипломы любых профессий по выгодным ценам.
horordark.ru/kupit-diplom-onlayn-nadezhno-i-udobno
Привет, друзья!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
http://www.yagath.com/blogs/678064/Рекомендации-по-приобретению-документов-в-сети
Здравствуйте!
Купить документ ВУЗа вы имеете возможность у нас в столице.
ast-diploms.com/kupit-diplom-krasnoyarsk
Хорошей учебы!
Здравствуйте!
Заказать диплом о высшем образовании.
sociomixr.com/blogs/92/%D0%9A%D0%BB%D1%8E%D1%87%D0%B5%D0%B2%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%85%D0%BE%D0%B4%D1%8B-%D0%B8%D0%B7%D0%B3%D0%BE%D1%82%D0%BE%D0%B2%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
Привет!
Приобрести документ института вы можете в нашей компании в столице.
ast-diploms24.ru/kupit-diplom-voronezh
Успехов в учебе!
Привет!
Где приобрести диплом по необходимой специальности?
silton.ru/forum/user/5007/
Успехов в учебе!
СОУТ аккредитованные организации
Проведение СОУТ состоит из нескольких этапов. Сначала проводится подготовка и сбор необходимой документации, дальше специалисты оценивают рабочие места и выявляют потенциальные риски. На завершающем этапе оформляется отчет, который содержит рекомендации по улучшению условий труда. Спецоценка условий труда организации не только соответствует законодательным требованиям, но и улучшает доверие сотрудников к компании.
Привет!
Мы предлагаем выгодно и быстро заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Диплом способен пройти лубую проверку, даже с применением специально предназначенного оборудования. Решайте свои задачи быстро и просто с нашими дипломами.
http://www.terrapevtika.ru/forum/?PAGE_NAME=message&FID=1&TID=511&TITLE_SEO=511-kupit-diplom-kandidata-nauk&MID=736&result=reply#message736
Успехов в учебе!
Привет!
Где купить диплом по нужной специальности?
Заказать диплом о высшем образовании.
http://www.detailing-time.net/events/event/12-широкий-каталог-документов-в-знаменитом-интернет-магазине/
Привет, друзья!
Где приобрести диплом специалиста?
Мы можем предложить документы ВУЗов, расположенных в любом регионе России. Вы имеете возможность приобрести качественный диплом за любой год, включая сюда документы старого образца. Дипломы выпускаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми необходимыми печатями и штампами.
Мы изготавливаем дипломы любых профессий по доступным ценам.
ast-diplom24.ru/otzyvy
Всегда вам поможем!
Добрый день!
Купить документ о получении высшего образования вы сможете у нас в столице. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить диплом по любой специальности, любого года выпуска, включая документы Советского Союза. Гарантируем, что в случае проверки документа работодателем, никаких подозрений не возникнет.
Мы предлагаем дипломы любых профессий по приятным ценам. Цена зависит от той или иной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для покупателей адекватную политику тарифов. Для нас важно, чтобы документы были доступны для подавляющей массы наших граждан.
tirana.social/blogs/1030/Легко-приобретаем-документы-в-лучшем-онлайн-магазине-Russian-Diplom?lang=pt_pt
Будем рады вам помочь!
Добрый день!
Мы изготавливаем дипломы любых профессий по выгодным тарифам. Цена зависит от конкретной специальности, года получения и университета. Стараемся поддерживать для клиентов адекватную ценовую политику. Важно, чтобы дипломы были доступными для большинства граждан.
7prbookmarks.com/story17111334/купить-диплом-сантехника
Feeling those butterflies in your stomach? It’s completely normal to be nervous on a first date. Just remember to be yourself and enjoy the moment
news site
Привет, друзья!
Можно ли купить аттестат о среднем образовании, основные моменты и вопросы
technoevents.ru/vash-diplom-za-korotkoe-vremya-prosto-i-udobno
Рады помочь!.
купить диплом в ангарске asxdiplomik24.ru .
Привет!
Мы предлагаем документы ВУЗов, расположенных в любом регионе РФ. Вы имеете возможность приобрести диплом от любого учебного заведения, за любой год, включая сюда документы СССР. Документы выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригиналов. Они будут заверены необходимыми печатями и штампами.
lada-clubs.ru/gallery/image/740-nizkie-rascenki-i-vysokoe-kachestvo-priobretay-dokumenty-onlayn/
Добрый день!
Купить диплом университета
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe В
Удачи!
Привет!
Приобрести документ о получении высшего образования можно в нашей компании.
diploms-x.com/kupit-diplom-ekaterinbur
Привет!
Купить диплом магистра оказалось возможно, быстрое обучение и диплом на руки
obshenie.flybb.ru/viewtopic.php?f=2&t=687
Рады помочь!.
Привет!
Приобрести диплом о высшем образовании.
http://www.dr-ay.com/blogs/182182/??????-??????-?-??????-???????-??????????
Успешной учебы!
[u][b] Привет, друзья![/b][/u]
[b]Мы готовы предложить документы техникумов[/b], которые расположены в любом регионе России. Вы можете заказать качественно напечатанный диплом за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты делаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы заверяются всеми обязательными печатями и подписями.
[url=http://flerus-shop.hcp.dilhost.ru/club/user/3/forum/message/880/876//]flerus-shop.hcp.dilhost.ru/club/user/3/forum/message/880/876/[/url]
Здравствуйте!
Купить диплом о высшем образовании
arusak-diploms-srednee.ru В
Хорошей учебы!
Добрый день!
Приобрести документ университета вы имеете возможность у нас.
asxdiplomik.com/kupit-diplom-sankt-peterburg
Здравствуйте!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
gioturbobp.com/blogs/33/Важные-советы-по-приобретению-документов-в-сети-интернет
Здравствуйте!
Полезные советы по безопасной покупке диплома о высшем образовании
forum-nine.mirbb.com/t11756-topic#31166
Рады помочь!.
Добрый день!
Заказать документ института можно у нас.
ast-diplomas.com/kupit-diplom-krasnoyarsk
Удачи!
купить диплом в буденновске http://www.diploms-x.com .
Привет, друзья!
Приобрести диплом любого университета
[url=http://landik-diploms-srednee.ru/kupit-diplom-saratov В ]landik-diploms-srednee.ru/kupit-diplom-saratov В [/url]
Хорошей учебы!
Привет!
Мы можем предложить документы техникумов, расположенных на территории всей Российской Федерации. Вы можете приобрести качественно сделанный диплом от любого учебного заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они заверяются всеми необходимыми печатями и штампами.
1776reloaded.us/blogs/57/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
EWR Long Term Parking: Find secure & affordable options near EWR Airport. Reviews & details to choose the best fit for your trip best long term parking at newark airport
Добрый день!
Диплом техникума купить официально с упрощенным обучением в Москве.
Заказать диплом любого университета.
wiki.roximo.ru/index.php/%D0%92%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D1%8B%D0%B5_%D1%80%D0%B0%D1%81%D1%86%D0%B5%D0%BD%D0%BA%D0%B8_%D0%B8_%D0%B2%D1%8B%D1%81%D0%BE%D0%BA%D0%BE%D0%B5_%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE_-_%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B9_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD!
Привет, друзья!
Где заказать диплом специалиста?
aboutallfinance.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
Хорошей учебы!
Привет!
Заказать документ ВУЗа вы сможете у нас в столице.
diploms-x.com/kupit-diplom-voronezh
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным ценам.
http://www.find-topdeals.com/blogs/133052/Высококачественные-диплоРСС‹-Р Р…Р В°-заказ
Возможно ли купить диплом стоматолога, и как это происходит
ast-diplom24.ru/kupit-diplom-moskva
Здравствуйте!
Заказать документ института вы имеете возможность у нас. Мы предлагаем документы об окончании любых университетов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы СССР.
or1gano.80lvl.ru/viewtopic.php?f=10&t=1028
tawasol1.mn.co/posts/62241886
1001viktorina.ru/forum/viewtopic.php?f=19&t=1350&sid=0fef3cbae668bcefd50990bdbb7df1d4
roseninsel.kz/forum/topic/add/forum7/
girlscools.ru/nadezhnoe-oformlenie-diploma-za-korotkiy-srok
Привет, друзья!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
russiajoy.ru/oformlenie-diploma-onlayn-za-neskolko-shagov
отремонтировать ноутбук в москве
Здравствуйте!
Заказать документ о получении высшего образования вы можете у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, любого года выпуска, включая документы СССР.
rulezrp.listbb.ru/viewtopic.php?f=2&t=606
forum.gorodsalavat.ru/posting.php?mode=post&f=28&sid=38420d04527046406718146c1615912a
korenkyfr.4adm.ru/posting.php?mode=post&f=4&sid=4e4f2c4124e6ebdd40ee5e436e63bf7a
dopalnenie.listbb.ru/viewtopic.php?f=3&t=717
medicineshocknews.ru/poluchite-diplom-o-kotorom-vsegda-mechtali
Здравствуйте!
Приобрести документ о получении высшего образования можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза. Гарантируем, что при проверке документов работодателями, никаких подозрений не появится.
uncleali.com/read-blog/174
upirata.ru/index.php?/gallery/image/17-быстрый-выбор-магазина-который-реализует-дипломы-и-аттестаты/
net4women.ru/blogs/3896/Гарантированное-качество-и-подлинность-дипломов
nedvigimost.bbok.ru/viewtopic.php?id=27380#p46863
100foto.com/forum/user/1572/
Привет, друзья!
Приобрести диплом ВУЗа
Наша компания предлагает выгодно и быстро заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Данный документ способен пройти любые проверки, даже с применением специально предназначенного оборудования. Решите свои задачи быстро и просто с нашими дипломами.
Где купить диплом по актуальной специальности?
social.ghame.org/read-blog/7800_chto-imenno-trebuetsya-dlya-sozdaniya-kachestvennogo-dokumenta.html
c10g7o9ik.ourcodeblog.com/28402839/Рзучите-наш-РѕР±Р·РѕСЂ-РІ-том-случае-если-нужно-купить-диплом-РІ-сети
thenet.work/gallery/image/483-почему-магазины-с-дипломами-столь-популярны-и-востребованы/
iaescortsmap.ixbb.ru/viewtopic.php?id=103#p103
thenet.work/gallery/image/480-faq-и-служба-поддержки-покупаем-диплом-в-сети-интернет/
куплю диплом вуза бывший куплю диплом вуза бывший .
Добрый день!
Где заказать диплом по актуальной специальности?
Заказать диплом любого университета.
wiki.starfederation.ru/index.php?title=Большой_каталог_документов_в_популярном_онлайн_магазине
Привет, друзья!
Приобрести документ о получении высшего образования вы можете в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любым специальностям, включая документы образца СССР.
sllife.ru/social/user/4216/forum/message/2439/7151/#message7151
aurorahcs.com/forum/posting.php?mode=post&f=8
semeyka.listbb.ru/viewtopic.php?f=20&t=787
testforum.1stbb.ru/viewtopic.php?f=3&t=433
c904581v.beget.tech/2024/07/13/diplom-na-zakaz-kachestvo-i-nadezhnost.html
На сайте https://cars16.ru заполните форму для того, чтобы ваш автомобиль оценили по фотографии. На это уйдут всего 5 минут. Только в этой компании выкупают машины намного дороже, чем в других. При этом предлагают реальную сумму. Теперь реализовать автомобиль вы сможете всего за час. Оценщик приедет на объект в ближайшее время, чтобы обозначить стоимость. Если она устроит обе стороны, то подписывается договор. Важным моментом является то, что деньги вы получаете сразу же, полную сумму. В этой компании действуют самые выгодные условия.
купить медицинский диплом в красноярске diploms-x.com .
https://telegra.ph/Uznajte-bolshe-o-sovremennyh-sistemah-hraneniya-dannyh-dlya-vashego-predpriyatiya-07-20-4
Привет, друзья!
Приобрести диплом любого ВУЗа
arusak-diploms-srednee.ru/svidetelstvo-o-brake В
Успешной учебы!
Привет, друзья!
Где приобрести диплом специалиста?
Приобрести диплом о высшем образовании.
stareishina.com/gallery/image/3633-lux-diplomru/
[u][b] Добрый день![/b][/u]
[b]Как оказалось, купить диплом кандидата наук не так уж и сложно [/b]
[url=http://rpinnovative.1stbb.ru/viewtopic.php?f=8&t=373/]rpinnovative.1stbb.ru/viewtopic.php?f=8&t=373[/url]
[u][b] Будем рады вам помочь![u][b].
Привет, друзья!
Мы предлагаем документы техникумов, расположенных в любом регионе России. Вы имеете возможность купить качественный диплом от любого заведения, за любой год, включая сюда документы СССР. Документы делаются на “правильной” бумаге самого высокого качества. Это дает возможности делать государственные дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и подписями.
f13zahtz2.idblogz.com/28765781/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
В Vavada казино всегда что-то новое! Используйте промокоды, чтобы получить больше шансов на выигрыш и наслаждаться игровым процессом с дополнительными бонусами.
В Drip казино промокоды помогут вам получить дополнительные бонусы и сделать игровой процесс еще увлекательнее. Используйте наши предложения и выигрывайте больше.
Привет, друзья!
Заказать документ о получении высшего образования вы сможете в нашем сервисе.
diplomasx.com/kupit-diplom-rostov-na-donu
Успешной учебы!
В Vavada казино всегда что-то новое! Используйте промокоды, чтобы получить больше шансов на выигрыш и наслаждаться игровым процессом с дополнительными бонусами.
Люки Шагма – идеальное сочетание функциональности и эстетики для вашего интерьера. Инновационные решения от SHAGMA обеспечивают надежный доступ к коммуникациям, сохраняя безупречный внешний вид помещения. Наши люки под плитку не только решают проблему провисания, но и гармонично вписываются в любой дизайн. Выбирая SHAGMA, вы выбираете качество, долговечность и индивидуальный подход https://gorod-kimry.ru/info9/020/
https://telegra.ph/Nadezhnye-setevye-resheniya-ot-Huawei-07-20-5
Здравствуйте!
Как правильно приобрести диплом колледжа или ПТУ в России, важные моменты
pdbsoftware.com/2024/06/23/купить-диплом-в-новочеркасске/
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
karhu.blueaddlution.com/2024/06/30/купить-диплом-в-серове/
Привет!
Заказать документ института вы сможете в нашем сервисе.
ast-diplom24.ru/kupit-diplom-vracha
Хорошей учебы!
Добрый день!
Где купить диплом специалиста?
Мы готовы предложить дипломы любой профессии по приятным тарифам. Стоимость может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для большинства граждан.
Для вас изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным ценам.
kotanusantara.cloud/index.php?/events/event/7-почему-гораздо-дешевле-и-проще-заказать-диплом-вуза/
Всегда вам поможем!.
Привет!
Приобрести документ о получении высшего образования можно у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы старого образца.
stalinarch.ru/wiki/index.php/Дипломы,_которые_открывают_двери
newsofgames.ru/garantirovannoe-oformlenie-diploma-bezopasno-i-nadezhno
pirat.iboards.ru/viewtopic.php?f=20&t=22207
mymotospeed.ru/professionalnyie-diplomyi-po-otlichnoy-tsene
ilovehabbo.bbon.ru/viewtopic.php?id=1565#p28983
Добрый день!
Купить диплом о среднем образовании в Москве и любом другом городе
foto-passau.com/gallery/image/9-четыре-ключевых-группы-интернет-магазинов-что-реализуют-дипломы/
Здравствуйте!
Заказать документ о получении высшего образования вы можете у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации.
fire-team.ru/forum/showthread.php?p=35312#post35312
adsauto.info/index.php?subaction=userinfo&user=yvupuv
anoreksja.org.pl/viewtopic.php?f=27&t=1179415
infomts.ru/index.php?subaction=userinfo&user=etuzyvab
dianov.bget.ru/forum/thread57488.html#1281054
Привет, друзья!
Наша компания предлагает купить диплом высокого качества, который невозможно отличить от оригинального документа без использования специального оборудования и опытного специалиста.
arkosgold.ru/index.php?subaction=userinfo&user=edyfufy
Удачи!
Добрый день!
Официальное получение диплома техникума с упрощенным обучением в Москве
competit.ru/index.php?subaction=userinfo&user=ocewirov
Поможем вам всегда!.
Привет, друзья!
Приобрести документ о получении высшего образования вы сможете у нас.
diploms-x.com/kupit-diplom-ekaterinbur
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по невысоким тарифам.
http://www.greenmind.cl/2024/07/07/купить-диплом-типография/
Привет, друзья!
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по доступным ценам.
horordark.ru/zakazhite-diplom-v-kratchayshie-sroki
Добрый день!
Приобрести диплом любого университета
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge В
Хорошей учебы!
domstroi.info
Привет!
Где приобрести диплом специалиста?
Заказать диплом любого университета.
forum.sempiternalcommunity.ru/index.php?/gallery/image/19-как-найти-надежный-интернет-магазин-с-обширным-выбором-дипломов/
newsplaces.net
Добрый день!
Заказать документ университета можно в нашем сервисе.
diplomasx24.ru/kupit-diplom-moskva
Здравствуйте!
Мы можем предложить документы ВУЗов, расположенных в любом регионе РФ. Вы имеете возможность приобрести диплом от любого заведения, за любой год, в том числе документы старого образца. Документы выпускаются на бумаге самого высшего качества. Это дает возможность делать государственные дипломы, которые не отличить от оригиналов. Они заверяются необходимыми печатями и штампами.
zpgiugb3n.look4blog.com/67321351/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет, друзья!
Мы можем предложить дипломы любых профессий по выгодным ценам.
isnw.ru/2024/06/30/купить-диплом-иргупс/
Привет!
Аттестат 11 класса купить официально с упрощенным обучением в Москве
avtoweek2016.ru/legalnoe-priobretenie-diploma-onlayn/
look at more info localbitcoins review
Здравствуйте!
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
lookeify.com/read-blog/7862
Рады помочь!.
Купить диплом о среднем образовании в Москве и любом другом городе
diplomasx24.ru/kupit-diplom-magistra
Здравствуйте!
Купить диплом о высшем образовании
arusak-diploms-srednee.ru/kupit-diplom-v-rostove-na-donu В
Удачи!
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашей компании в Москве.
ast-diplomy24.ru/kupit-diplom-voronezh
Привет!
Мы изготавливаем дипломы любой профессии по приятным ценам.
dsac.es/купить-диплом-рпа/
Здравствуйте!
Мы предлагаем документы техникумов, которые находятся на территории всей России. Можно купить диплом от любого заведения, за любой год, в том числе документы СССР. Документы выпускаются на бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Они будут заверены необходимыми печатями и штампами.
sharevita.com/read-blog/28308
Добрый день!
Где приобрести диплом специалиста?
Мы можем предложить документы ВУЗов, расположенных в любом регионе Российской Федерации. Вы сможете заказать диплом от любого высшего учебного заведения, за любой год, включая сюда документы СССР. Дипломы выпускаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Документы будут заверены всеми требуемыми печатями и штампами.
Мы предлагаем дипломы любой профессии по приятным тарифам.
diplomasx24.ru/otzyvy
Рады помочь!
Добрый день!
Диплом техникума купить официально с упрощенным обучением в Москве
mybuildhouse.ru/byistroe-oformlenie-diploma-lyuboy-spetsialnosti
Окажем помощь!.
Здравствуйте!
Реально ли приобрести диплом стоматолога? Основные шаги
epidemics.ru/index.php?subaction=userinfo&user=okezaju
Поможем вам всегда!.
Добрый день!
Наша компания предлагает выгодно и быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями. Данный документ пройдет лубую проверку, даже при помощи специальных приборов. Решите свои задачи быстро с нашими дипломами.
logo-def.ru/userinfo.php?uid=27953
Успехов в учебе!
Здравствуйте!
Мы изготавливаем дипломы любой профессии по невысоким тарифам. Стоимость будет зависеть от той или иной специальности, года выпуска и ВУЗа. Стараемся поддерживать для заказчиков адекватную политику цен. Для нас очень важно, чтобы документы были доступны для большого количества граждан.
sergiod0g08.p2blogs.com/26703135/Фальшивый-диплом-Почему-это-не-Стоит-купить-диплом
Добрый день!
Приобрести документ института вы можете у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза. Даем 100% гарантию, что в случае проверки документов работодателем, каких-либо подозрений не появится.
Мы предлагаем дипломы любой профессии по выгодным тарифам. Цена зависит от той или иной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для клиентов адекватную ценовую политику. Важно, чтобы документы были доступными для большинства граждан.
http://www.thereaderview.com/wall/blogs/275/Детальное-описание-покупки-документов-в-интернет-магазине/
Будем рады вам помочь!
Привет!
Купить диплом о высшем образовании
Мы предлагаем выгодно и быстро заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Диплом способен пройти лубую проверку, даже при использовании специфических приборов. Достигайте своих целей быстро и просто с нашей компанией.
Где заказать диплом по нужной специальности?
zxz.listbb.ru/viewtopic.php?f=7&t=1416
autoprajs.ru/15204.html
molbiol.ru/forums/index.php?showtopic=1179953
worksale777.blogspot.com/2024/06/blog-post_30.html
nedvigimost.bbok.ru/viewtopic.php?id=26650#p45740
Добрый день!
Где заказать диплом по актуальной специальности?
Заказать диплом о высшем образовании.
stroimarket-komi.ru/club/user/54/blog/38295/
If you are interested in this part-time opportunity, please
apply now or contact
Feel free to surf to my homepage; 단란주점알바
Привет, друзья!
Приобрести документ о получении высшего образования можно у нас.
ast-diploms24.ru/kupit-diplom-o-srednem-obrazovanii
Успешной учебы!
Здравствуйте!
Где купить диплом по необходимой специальности?
Приобрести диплом ВУЗа.
inopl.com/blogs/1110/Широкий-каталог-документов-в-популярном-интернет-магазине
Добрый день!
Приобрести документ о получении высшего образования можно в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов РФ. Вы сможете получить диплом по любым специальностям, включая документы Советского Союза.
talkitter.com/create-blog/
http://www.ladymystery.ru/forum/topic.asp?TOPIC_ID=9596
crystalroleplay.listbb.ru/viewtopic.php?f=14&t=2499
animalprotect.org/forum/index.php?topic=236715.0
shockmusik.ru/zakazhite-diplom-i-nachnite-novuyu-zhizn
диплома нет ast-diploms.com .
купить корочку для диплома купить корочку для диплома .
Привет, друзья!
Где купить диплом специалиста?
Приобрести диплом университета.
demo.1c-college.ru/club/user/7/blog/kak-podobrat-nadezhnyy-onlayn-magazin-s-shirokim-vyborom-diplomov/
Привет, друзья!
Купить диплом о высшем образовании.
mestovstrechi.flybb.ru/viewtopic.php?f=4&t=1275
Здравствуйте!
Купить документ университета можно в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы получите диплом по любой специальности, включая документы старого образца.
http://www.polosedan-club.com/search/search
mymotospeed.ru/kupite-diplom-i-dostignite-svoih-tseley
kondrateff.5bb.ru/viewtopic.php?id=6786#p12729
biketrials.ru/live/blog.php?b=9132
mireait.listbb.ru/viewtopic.php?f=2&t=481
Всё о покупке аттестата о среднем образовании: полезные советы
diplomyx.com/kupit-diplom-magistra
Привет, друзья!
Приобрести документ о получении высшего образования вы можете у нас.
ast-diploms.com/kupit-diplom-omsk
nerflix movies bear season californiafree fantasy movieswhat’s the newest season of survivorwith a vengeance movie
Привет, друзья!
Купить документ ВУЗа вы можете у нас.
diplomasx24.ru/otzyvy
Удачи!
In addressing the balance of commercial refrigeration units to reduce wear and energy consumption, the Balanset-1A was effectively employed. Explore the technology and benefits on Vibromera’s website https://vibromera.eu/example/impellers/in-situ-dynamic-rotor-balancing-for-industrial-blowers/
Добрый день!
Где купить диплом специалиста?
http://www.nhps1914.com/wiki/Диплом_за_короткий_срок:_надежно_и_конфиденциально
Успешной учебы!
Привет, друзья!
Заказать диплом ВУЗа
landik-diploms-srednee.ru/kupit-diplom-v-omske В
Удачи!
Добрый день!
Купить документ университета можно у нас в столице.
ast-diplomas24.ru/kupit-diplom-vracha
Удачи!
Привет!
Приобрести диплом о высшем образовании
Наши специалисты предлагают быстро и выгодно приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Диплом пройдет любые проверки, даже при использовании специально предназначенного оборудования. Достигайте свои цели быстро и просто с нашей компанией.
Где купить диплом по нужной специальности?
alanyatoday.ru/users/76
promintern.listbb.ru/viewtopic.php?f=16&t=474
ya.2bb.ru/viewtopic.php?id=19040#p240217
burgasdent.listbb.ru/viewtopic.php?f=3&t=355
volnodumie.bbmy.ru/viewtopic.php?id=12332#p25047
Привет!
Мы готовы предложить документы техникумов, которые расположены в любом регионе РФ. Можно купить качественный диплом от любого учебного заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы будут заверены необходимыми печатями и подписями.
as3dos28g.blogdanica.com/28191058/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
ремонт энкодеров
речевое озвучивание речевое озвучивание .
Привет!
Реально ли приобрести диплом стоматолога? Основные этапы
gess.flybb.ru/posting.php?mode=post&f=2
Всегда вам поможем!.
Привет!
Приобрести документ о получении высшего образования вы можете в нашей компании в столице.
asxdiplomik.com/kupit-diplom-sankt-peterburg
Успешной учебы!
Как официально купить диплом вуза с упрощенным обучением в Москве
ast-diploms.com/kupit-diplom-moskva
Здравствуйте!
Купить диплом о высшем образовании.
library.kemu.ac.ke/kemuwiki/index.php/????????_??????:_??????,_??????,_???????!
Удачи!
Привет!
Мы изготавливаем дипломы любых профессий по разумным ценам.
http://www.kikwit.alobi.cd/2024/06/30/купить-диплом-в-ессентуки/
https://gosznakdublikat.ru/
Привет, друзья!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно.
Приобрести диплом любого ВУЗа.
bizinhome.mn.co/posts/61837993
Добрый день!
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по выгодным ценам.
lab.panda-studio.pro/index.php?/gallery/image/116-какие-магазины-с-дипломами-имеются-на-текущий-момент/
Здравствуйте!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
zavalinka.listbb.ru/viewtopic.php?f=3&t=2959
Рады оказать помощь!.
Привет, друзья!
Мы изготавливаем дипломы любой профессии по разумным тарифам.
http://www.cucinaevista.com/2024/06/30/медицинский-сертификат-специалиста/
Добрый день!
Заказать документ ВУЗа можно у нас.
ast-diplomas24.ru/kupit-diplom-nizhnij-novgorod
[u][b] Привет![/b][/u]
Купить документ о получении высшего образования можно в нашем сервисе. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, включая документы СССР.
[url=http://brawlstarsacc.listbb.ru/viewtopic.php?f=3&t=492/]brawlstarsacc.listbb.ru/viewtopic.php?f=3&t=492[/url]
[url=http://myweektour.ru/diplomyi-ot-proverennyih-postavshhikov//]myweektour.ru/diplomyi-ot-proverennyih-postavshhikov/[/url]
[url=http://klinlife.ru/forums/index.php?/topic/44335-diplomi-po-dostupnim-cenam-dlja-vseh//]klinlife.ru/forums/index.php?/topic/44335-diplomi-po-dostupnim-cenam-dlja-vseh/[/url]
[url=http://medik-look.ru/diplomyi-dlya-uspeshnogo-trudoustroystva/]medik-look.ru/diplomyi-dlya-uspeshnogo-trudoustroystva[/url]
[url=http://jamsun.net/doku.php?id=купите_диплом_и_начните_карьеру_сегодня/]jamsun.net/doku.php?id=купите_диплом_и_начните_карьеру_сегодня[/url]
Здравствуйте!
Пошаговая инструкция по безопасной покупке диплома о высшем образовании
coup.forum2x2.ru/t3793-topic#10043
Окажем помощь!.
Привет, друзья!
Приобрести диплом любого ВУЗа
arusak-diploms-srednee.ru/kupit-diplom-magistra В
Хорошей учебы!
Добро пожаловать на наш сайт! Откройте лучшие финансовые решения прямо сейчас!
Наши предложения
Мы предлагаем широкий ассортимент финансовых продуктов: кредиты, банковские карты и займы, чтобы помочь вам достичь ваших целей и воплотить мечты в реальность.
дебетовая карта с функцией защиты данных
Кредиты для всех нужд
Планируете покупку жилья, автомобиля или образование? Наши кредитные программы созданы для вас. Оформите кредит на нашем сайте за несколько минут, выбрав лучшие условия и сроки погашения.
Преимущества наших банковских карт
Наши карты обеспечивают удобство безналичных платежей и множество бонусов:
– **Кэшбэк и скидки у партнеров**
– **Программа лояльности**
Оформите карту онлайн и получите все преимущества уже сегодня!
Быстрые займы для непредвиденных расходов
кредит на строительство дома
Нужны деньги до зарплаты или на неожиданные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок.
Наши преимущества:
– **Простота и Удобство:** Оформите заявку онлайн за считанные минуты.
– **Надежность и Прозрачность:** Честные условия без скрытых комиссий.
– **Индивидуальный Подход:** Мы учитываем ваши личные обстоятельства.
Не упустите шанс улучшить свою финансовую ситуацию! Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
Переходите на наш сайт и сделайте шаг к своим мечтам!
politeconomics.org
Привет, друзья!
Приобрести диплом университета.
x4all.de/profile/202-miguelpnaite/
Успешной учебы!
Привет!
Мы предлагаем документы техникумов, расположенных на территории всей России. Вы имеете возможность купить качественно сделанный диплом от любого заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Документы выпускаются на бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы заверяются всеми необходимыми печатями и штампами.
9unity.com/read-blog/2558
company website jaxx io
Привет, друзья!
Приобрести диплом любого университета
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske В
Успешной учебы!
Привет, друзья!
Заказать документ о получении высшего образования можно у нас в столице.
asxdiplomik.com/kupit-diplom-omsk
Здравствуйте!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
c99596qr.beget.tech/2024/07/11/bystroe-poluchenie-diploma-vash-shans-na-uspeh.html
Рады оказаться полезными!.
http://buy-cloned-cards.com
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance ? $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $1000 – Price $ 99.00
Item Western Union Transfers $300 – Price $ 249.00
*Prices on the website may vary slightly
http://saleclonedcards.one
Добро пожаловать на наш сайт – ваше решение для всех финансовых потребностей!
Наши предложения
Мы предлагаем различные финансовые продукты: кредиты, банковские карты и займы, чтобы помочь вам достигнуть ваших целей и осуществить мечты.
дебетовая карта с функцией начисления процентов на остаток
Идеальные кредиты для ваших нужд
Нуждаетесь в финансировании на покупку жилья, автомобиля или образование? Наши кредитные программы разработаны с учетом ваших потребностей. Оформите кредит на нашем сайте, выбрав подходящие условия и сроки погашения.
Преимущества наших банковских карт
Наши банковские карты предоставляют:
Удобство безналичных платежей
Бонусы и привилегии
Оформите карту на нашем сайте и получайте кэшбэк, скидки у партнеров и участие в программе лояльности. Выберите карту с оптимальными лимитами и условиями обслуживания для себя.
Быстрые и удобные займы
Нужны деньги до зарплаты или на непредвиденные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок, чтобы вы могли решать финансовые вопросы без задержек.
Наши преимущества:
Простота и Удобство: Оформите заявку онлайн за несколько минут.
Надежность и Прозрачность: Мы гарантируем честные условия и отсутствие скрытых комиссий.
Индивидуальный Подход: Мы учитываем ваши личные обстоятельства и предлагаем оптимальные условия.
Не упустите возможность улучшить свою финансовую ситуацию!
дебетовая карта с функцией начисления процентов на остаток
Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
С нами ваши мечты станут реальностью!
noticias
noticias
noticias
Добрый день!
Как быстро получить диплом магистра? Легальные способы.
Купить диплом о высшем образовании.
theigbos.com/blogs/3636/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Почему Куба или гранитное обрамление
Российских туристов могут обязать страховаться от банкротств туроператоров
https://samoylovaoxana.ru/rys-krasnoe-na-belom-vyshivanka-slavian/
Ещё можно узнать: кровь по цито
Романтические путешествия
Добрый день!
Мы готовы предложить документы техникумов, расположенных на территории всей России. Вы можете купить качественный диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми обязательными печатями и подписями.
demo.1c-college.ru/club/user/7/blog/zakazyvaem-dokumenty-v-izvestnom-onlaynmagazine-po-komfortnoy-tsene/
Starting to take stock, we can say with ukrtvoru.info complete confidence that, indeed, both absolute and relative height will play an important role in geography.
Здравствуйте!
Заказать диплом любого ВУЗа
landik-diploms-srednee.ru/svidetelstvo-o-razvode В
Удачи!
Привет!
Где купить диплом по нужной специальности?
Купить диплом университета.
kotanusantara.cloud/index.php?/events/event/8-как-найти-надежный-онлайн-магазин-с-обширным-выбором-дипломов/
Организация проведения СОУТ
Обеспечение надежных условий работы — это не просто выполнение стандартов, но также забота о здоровье и благополучии работников. Спецоценка рабочих мест помогает обнаружить и ликвидировать риски, что уменьшает травматизм и повышает рабочую эффективность. Обращайтесь в Safety Systems Group, чтобы обеспечить своим сотрудникам достойные условия труда и улучшить общий климат в коллективе.
купить текст диплома diploms-x.com .
купить диплом кассира купить диплом кассира .
Добрый день!
Мы готовы предложить документы техникумов, расположенных в любом регионе Российской Федерации. Можно приобрести диплом от любого заведения, за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высокого качества. Это дает возможность делать настоящие дипломы, которые не отличить от оригинала. Они будут заверены необходимыми печатями и подписями.
3qxx1kuw0.verybigblog.com/27939944/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Где приобрести диплом по необходимой специальности?
Приобрести диплом о высшем образовании.
es-presto.ru/community/groups/0-0/176-ogromnyj-vybor-dokumentov-v-znamenitom-onlajn-magazine
куплю диплом дорогой ast-diploms.com .
Добрый день!
Купить документ университета вы можете в нашей компании в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы образца СССР.
http://www.testimonyforgod.com/read-blog/5652
mosmol.flybb.ru/viewtopic.php?f=2&t=398
pdapal.com/read-blog/1006
ya.10bb.ru/viewtopic.php?id=4063#p7250
bvf.ru/forum/showthread.php?p=25249834#post25249834
For balancing heavy-duty electrical motors, we used the Balanset-1A, provided by Vibromera, ensuring precise correction of imbalances. Explore more about their cutting-edge solutions on Vibromera’s website https://vibromera.eu/
Привет!
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по доступным ценам.
evogenesfahan.com/2024/06/23/купить-диплом-мггу-или-любого-вуза-рос/
дипломы аттестаты спб дипломы аттестаты спб .
Добрый день!
Где приобрести диплом по нужной специальности?
Заказать диплом университета.
kvixi.com/blogs/1355/Широкий-ассортимент-документов-в-популярном-онлайн-магазине
Добрый день!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
eaglepharmausa.us/2024/06/30/купить-диплом-ргуниг-или-любого-вуза-р/
noticias
noticias
noticias
Здравствуйте!
Как официально приобрести аттестат 11 класса с минимальными затратами времени
starterkit.ru/html/index.php?name=account&op=info&uname=amopoqa
Окажем помощь!.
На сайте https://prodrag.ru/ позвоните для того, чтобы узнать нюансы о скупке радиодеталей. Предприятие специализируется на закупках электронного лома, а также различных радиодеталей. Есть возможность сдать электронную технику, которая уже непригодна для дальнейшего использования, нерабочие детали, различную технику. При необходимости вам дадут профессиональную консультацию. Специалисты в ближайшее время ответят на все интересующие вопросы. В компании работают только лучшие сотрудники, которые отлично понимают в подобных вопросах.
Привет!
Заказать диплом о высшем образовании
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Диплом пройдет любые проверки, даже с применением специального оборудования. Решайте свои задачи максимально быстро с нашим сервисом.
Где купить диплом по актуальной специальности?
http://www.brodyaga.org/club/user/110581/blog/6290/
mooz6.com/read-blog/607
chayka.ixbb.ru/viewtopic.php?id=142#p152
sportraketka.ru/vash-nastoyashhiy-diplom-byistro-i-bezopasno
biocenter.pro/club/blogs/sonnick84-blog-bc/legkiy-vybor-onlaynmagazina-realizuyushchego-diplomy/
Привет!
Купить документ института вы можете в нашей компании.
diploms-x.com/kupit-diplom-omsk
Хорошей учебы!
Привет, друзья!
Полезная информация как купить диплом о высшем образовании без рисков
ourfathersfamily.com/blogs/2385/Как-купить-сейчас-неотличимый-от-подлинника-диплом-в-сети
Здравствуйте!
Купить документ ВУЗа можно у нас.
asxdiplomik.com/kupit-diplom-ekaterinbur
Хорошей учебы!
Привет!
Купить документ института можно в нашем сервисе.
asxdiplomik.com/kupit-diplom-sankt-peterburg
купить диплом медучилища ast-diploms.com .
Привет, друзья!
Купить документ о получении высшего образования можно в нашей компании в Москве.
ast-diplomas24.ru/kupit-diplom-sankt-peterburg
Успешной учебы!
Психологическая поддержка в Москве: помощь и решения
Сегодня многие люди сталкиваются с эмоциональными и психологическими трудностями, которые нуждаются в профессиональной поддержке. Сайт psyhologirinakurazh.ru предлагает услуги квалифицированного психолога в Москве, который поможет справиться с различными жизненными ситуациями и улучшить качество вашей жизни.
Консультации психолога в Москве для всех желающих
Если вы ищете психолог москва консультации цена , наши профессионалы готовы предложить вам индивидуальные и семейные консультации. Мы осознаем, что каждая проблема уникальна, и поэтому подходим к каждому клиенту с вниманием и заботой. Наша команда профессиональных психологов поможет вам решить сложные вопросы, восстановить гармонию в отношениях и справиться с внутренними конфликтами.
Доступные цены и высокий профессионализм
Мы предлагаем услуги психолога в москве цена и отзывы , чтобы профессиональная помощь была доступна всем. В нашем кабинете психолога в Москве вы найдете комфортную и доверительную атмосферу, способствующую откровенным беседам. Консультации проводятся в удобное время для вас, и вы можете быть уверены в полной конфиденциальности.
Отзывы клиентов и признание
Наш труд высоко оценивается клиентами, что подтверждается многочисленными положительными отзывами. Мы стремимся к тому, чтобы каждый, кто обратился к нам, почувствовал значительные улучшения в своей жизни. Посетите сайт psyhologirinakurazh.ru, чтобы узнать больше о наших услугах и записаться на консультацию. Доверьтесь нашим профессионалам и начните свой путь к душевному равновесию уже сегодня.
Taobao – популярная торговая интернет-площадка. Здесь у вас есть возможность купить самое необходимое. Мы предлагаем вам удобный способ избавиться от утомительных походов по магазинам. Ищете таобао спортивная одежда? Grandior.ru – сайт, где представлен широкий ассортимент товаров. Гарантируем доступные цены. Предусмотрены и скидки. Теперь вы знаете, какой секрет популярности у Таобао ком. Удовлетворим запросы даже самых взыскательных клиентов. Сайт Taobao на русском языке «Грандиор.ру» – станет вашим лучшим помощником в совершении покупок товаров.
Привет!
Стоимость дипломов высшего и среднего образования и процесс их получения
forosmex.com/index.php?/gallery/image/543-4-е-ключевых-группы-интернет-магазинов-что-реализуют-документы/
купить медицинское образование купить медицинское образование .
Привет!
Мы готовы предложить дипломы любой профессии по выгодным ценам.
http://www.vaca-ps.org/blogs/163462/¬аш-ѕуть-к-¬ысшему-ќбразованию- упить-?иплом
Добрый день!
Где заказать диплом специалиста?
Мы можем предложить дипломы любой профессии по доступным тарифам. Стоимость зависит от выбранной специальности, года получения и университета. Стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы документы были доступными для подавляющей массы наших граждан.
Для вас изготавливаем дипломы любых профессий по приятным ценам.
rsn360.ru/blogs/492/Почему-на-порядок-проще-и-дешевле-купить-диплом-ВУЗа
Рады оказать помощь!.
Добрый день!
Заказать диплом ВУЗа
Наши специалисты предлагают выгодно и быстро заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Документ способен пройти любые проверки, даже с применением специальных приборов. Достигайте цели максимально быстро с нашим сервисом.
Где приобрести диплом по актуальной специальности?
http://www.pajarojaguar.org/mediawiki01/index.php/Купить_диплом:_что_нужно_знать
http://www.neckmax.de/blogs/2241/Рекомендации-специалиста-что-помогут-недорого-приобрести-документы
demo.advised360.com/read-blog/161643
http://www.manchestercityclubs.com/read-blog/257
bignews.bloggersdelight.dk/2024/07/10/изучите-наш-обзор-в-случае-если-требуе/
Здравствуйте!
Купить документ о получении высшего образования вы сможете у нас. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы образца СССР. Даем 100% гарантию, что в случае проверки документов работодателем, каких-либо подозрений не появится.
twoplustwoequal.com/read-blog/34638
ozelim.org/sosyal/blogs/395/Рзучите-наш-материал-если-нужно-купить-диплом-РІ-сети-интернет
friends.win/read-blog/3569
fabnews.ru/forum/showthread.php?p=79774#post79774
asepbook.com/read-blog/3724
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным ценам.
amengram.com/blogs/235/ упите-?ипломы-Ѕыстро-и-Ќадежно
Здравствуйте!
Заказать диплом о высшем образовании
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske В
Удачи!
Привет!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
dogovor.top/wiki/Легкий_способ_получить_диплом_без_экзаменов
Всегда вам поможем!.
купить диплом педагога ast-diploms.com .
Привет!
Приобрести диплом любого университета
arusak-diploms-srednee.ru/kupit-diplom-medicinskogo-uchilishha В
Успешной учебы!
Здравствуйте!
Как приобрести диплом о среднем образовании в Москве и других городах
azat.on.kg/blogs/1056/Быстрое-получение-диплома-ваш-шанс-на-успех
Рады оказаться полезными!.
Добрый день!
Приобрести документ о получении высшего образования можно в нашем сервисе.
asxdiplomik.com/kupit-diplom-o-srednem-obrazovanii
Успехов в учебе!
Здравствуйте!
Мы можем предложить документы техникумов, расположенных на территории всей РФ. Вы можете приобрести качественный диплом от любого учебного заведения, за любой год, включая документы старого образца. Дипломы и аттестаты выпускаются на бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригинала. Они заверяются всеми требуемыми печатями и штампами.
fomazy.com/blogs/4819/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-Russian-Diplom
дипломы аттестаты спб дипломы аттестаты спб .
Привет!
Мы предлагаем приобрести диплом высокого качества, неотличимый от оригинального документа без использования дорогостоящего оборудования и опытного специалиста.
helenos.pavel-rimsky.cz/doku.php?id=russianydiplomix
Хорошей учебы!
Добрый день!
Приобрести документ о получении высшего образования можно у нас. Мы оказываем услуги по производству и продаже документов об окончании любых университетов РФ.
hosting.show/profile/ynanebun/
чпуремонт.рф/showthread.php?tid=46085
cmsthemefinder.com/userinfo.php?uid=35777#
http://www.forum.delta-dona.ru/profile.php?action=show&member=29023
moj.webservis.ru/forums/profile.php?action=show&member=7610
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
horordark.ru/kupit-diplom-onlayn-nadezhno-i-udobno
Привет, друзья!
Купить диплом университета
arusak-diploms-srednee.ru/kupit-attestat-za-11-klass В
Успешной учебы!
Добрый день!
Сколько стоит диплом высшего и среднего образования и как его получить?
obmenka.forum2x2.ru/t17060-topic#38627
Рады помочь!.
купить бланк диплома о высшем образовании ссср http://diploms-x.com/ .
Привет, друзья!
Мы можем предложить документы ВУЗов, которые находятся на территории всей РФ. Вы сможете приобрести качественный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты делаются на “правильной” бумаге самого высокого качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Они заверяются всеми обязательными печатями и штампами.
miss2010.nuclear.ru/site_py/blogs/1/pokupaem-dokumenty-v-izvestnom-internetmagazine-po-vygodnoy-tsene.php
Привет, друзья!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
dachkanews.ru/kupite-diplom-i-zabudte-o-studencheskih-problemah
Окажем помощь!.
куплю диплом рф куплю диплом рф .
Здравствуйте!
Мы можем предложить документы ВУЗов, расположенных в любом регионе России. Можно приобрести диплом от любого учебного заведения, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Они заверяются всеми необходимыми печатями и штампами.
eyawei-networks.mn.co/posts/61838196
Здравствуйте!
Где приобрести диплом специалиста?
Мы можем предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Можно приобрести качественный диплом за любой год, включая документы СССР. Дипломы выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать государственные дипломы, которые не отличить от оригиналов. Документы заверяются необходимыми печатями и штампами.
Мы можем предложить дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
ast-diplomas.com/kupit-diplom-o-srednem-obrazovanii
Всегда вам поможем!
Привет, друзья!
Где заказать диплом по необходимой специальности?
Мы можем предложить дипломы любой профессии по приятным ценам. Стоимость зависит от конкретной специальности, года получения и образовательного учреждения. Стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
Для вас предлагаем дипломы любой профессии по разумным тарифам.
br-totalbyg.dk/2024/07/13/купить-диплом-безопасно/
Рады оказать помощь!.
Здравствуйте!
Где заказать диплом по необходимой специальности?
Приобрести диплом любого ВУЗа.
stareishina.com/gallery/image/3633-lux-diplomru/
Привет, друзья!
Купить документ о получении высшего образования можно у нас в столице. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза.
or1gano.80lvl.ru/posting.php?mode=post&f=10&sid=3824d1a46520a6c24344c0dc63e1da15
jamsun.net/doku.php?id=повысьте_свой_статус_диплом_любого_вуза
doctorsforum.ru/viewtopic.php?f=193&t=39101
burgasdent.listbb.ru/viewtopic.php?f=3&t=392
lighttur.ru/luchshie-predlozheniya-na-diplomyi
Здравствуйте!
Всё, что нужно знать о покупке аттестата о среднем образовании
vk.com/club52212509?w=wall-52212509_11501
Будем рады вам помочь!.
магазин аккаунтов telegram магазин аккаунтов telegram .
Привет, друзья!
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по приятным ценам. Стоимость зависит от определенной специальности, года получения и ВУЗа. Стараемся поддерживать для покупателей адекватную ценовую политику. Для нас очень важно, чтобы документы были доступными для большинства наших граждан.
emiliofm788.bloggazzo.com/26763669/Фальшивый-диплом-Почему-это-не-Стоит-купить-диплом
Добрый день!
Где приобрести диплом по нужной специальности?
Приобрести диплом ВУЗа.
wiki.nikiforov.ru/index.php/Огромный_каталог_документов_в_известном_онлайн-магазине
Добрый день!
Заказать документ о получении высшего образования вы сможете у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза. Даем гарантию, что в случае проверки документа работодателями, каких-либо подозрений не появится.
Мы предлагаем дипломы любых профессий по выгодным ценам. Цена может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большого количества граждан.
neurostarcheats.com/index.php?/gallery/image/35-отличные-расценки-и-высокое-качество-дипломы-онлайн/
Рады оказать помощь!
Здравствуйте!
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков
lidertude.com/blogs/1185/С-умом-заказываем-диплом-в-сети-обзор
Привет, друзья!
Купить документ о получении высшего образования вы можете у нас в Москве. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы старого образца.
demo.advised360.com/read-blog/162165
army.clanfm.ru/viewtopic.php?f=2&t=38877
monstaluck.mn.co/spaces/9349829/feed
bike.by/forum/viewtopic.php?f=84&t=36612
alik.forumrpg.ru/viewtopic.php?id=6907#p280498
Привет, друзья!
Мы предлагаем дипломы любой профессии по выгодным ценам.
http://www.laverdaforhealth.org/купить-диплом-в-находке/
Привет, друзья!
Приобрести диплом любого ВУЗа
arusak-diploms-srednee.ru/kupit-attestat-za-11-klass В
Хорошей учебы!
Добрый день!
Наши специалисты предлагают быстро и выгодно купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Данный документ пройдет любые проверки, даже при помощи профессиональных приборов. Решите свои задачи максимально быстро с нашим сервисом.
proect.org/index.php?subaction=userinfo&user=ovapeha
Успехов в учебе!
Добрый день!
Купить диплом о высшем образовании
Наша компания предлагает выгодно и быстро купить диплом, который выполняется на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями должностных лиц. Данный диплом пройдет лубую проверку, даже при использовании профессионального оборудования. Решите свои задачи быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
vip.9bb.ru/viewtopic.php?id=5959#p9901
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
forumjustwoman.getbb.ru/viewtopic.php?f=43&t=941
тараз купить диплом diploms-x.com .
Привет!
Где купить диплом по актуальной специальности?
Приобрести диплом любого университета.
phobia.lt/index.php?/gallery/image/121-широкий-выбор-документов-в-знаменитом-интернет-магазине/
Добрый день!
Наша компания предлагает приобрести диплом высокого качества, который не отличить от оригинального документа без использования специального оборудования и квалифицированного специалиста.
munservis.mirniy.ru/index.php?subaction=userinfo&user=eqize
Хорошей учебы!
Привет!
Заказать документ ВУЗа вы имеете возможность у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца.
http://www.hb9lc.org/wiki/index.php/Дипломы_любой_сложности_быстро_и_без_проблем
t98223u0.beget.tech/2024/07/16/legalnyy-diplom-bez-lishnih-hlopot-uznayte-kak.html
revolverp.forumex.ru/viewtopic.php?f=11&t=313
suhinfo.ru/index.php/Легальный_диплом_с_доставкой_на_дом
monstaluck.mn.co/spaces/9349829/feed
Здравствуйте!
Заказать документ о получении высшего образования можно в нашей компании в столице. Мы предлагаем документы об окончании любых университетов России.
prof-aksay.ru/forum/messages/forum2/topic481/message473/
барс48.рф/forums.php?m=posts&q=22222&n=last#bottom
http://www.91hongyi.com/member/index.php?uid=yfozol
http://www.forumklassika.ru/showthread.php?t=129416&p=1843596#post1843596
vyvoj.barvinek.net/doku.php?id=gosznacdiplomy
Привет, друзья!
Мы предлагаем дипломы любой профессии по приятным тарифам.
smsorg.ge/2024/07/07/купить-диплом-вуза-куплю-диплом-о-высш/
Добрый день!
Как получить диплом о среднем образовании в Москве и других городах
gadjetforyou.ru/diplom-za-dengi-byistro-nadezhno-bezopasno
Будем рады вам помочь!.
диплом государственного образца купить диплом государственного образца купить .
купить диплом педагогического колледжа asxdiplomik24.ru .
Привет, друзья!
Как получить диплом о среднем образовании в Москве и других городах
bbs.instrustar.com/home.php?mod=space&uid=82335
Будем рады вам помочь!.
Привет!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании.
diploms-x24.ru/kupit-diplom-voronezh
Хорошей учебы!
Добрый день!
Приобрести диплом о высшем образовании.
stalinarch.ru/wiki/index.php/??????_??????_?_??????:_??????????_??????
Хорошей учебы!
Привет!
Стоимость дипломов высшего и среднего образования и как избежать подделок.
Приобрести диплом университета.
http://www.flexartsocial.com/blogs/10135/%D0%9A%D0%B0%D0%BA-%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Мы предлагаем документы техникумов, которые находятся на территории всей России. Можно приобрести качественный диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Документы делаются на “правильной” бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Документы будут заверены всеми обязательными печатями и штампами.
gratefulproject.com/read-blog/4524
Здравствуйте!
Мы предлагаем дипломы любой профессии по приятным ценам.
phugiabetong.vn/диплом-аттестаты-купить
Здравствуйте!
Заказать документ ВУЗа можно в нашей компании в столице.
ast-diplomas.com/kupit-diplom-ekaterinbur
Успехов в учебе!
Привет, друзья!
Где купить диплом специалиста?
Мы можем предложить документы ВУЗов, которые расположены в любом регионе РФ. Вы можете заказать качественный диплом за любой год, включая сюда документы старого образца. Дипломы печатаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Документы заверяются всеми необходимыми печатями и подписями.
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по доступным тарифам.
diplomyx.com/kupit-diplom-krasnoyarsk
Поможем вам всегда!
Добрый день!
Приобрести диплом ВУЗа.
http://www.lawtech.ru/subscribe/25347-07072024
купить диплом в ишиме diploms-x.com .
Добрый день!
Мы можем предложить дипломы любой профессии по доступным тарифам.
thcsphuhuu.pgdchauthanhdt.edu.vn/купить-диплом-о-среднем-техническом-о/
Здравствуйте!
Мы готовы предложить дипломы любой профессии по разумным тарифам. Цена может зависеть от выбранной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Для нас важно, чтобы документы были доступны для подавляющей массы граждан.
martinxe579.blogzag.com/71601784/Дипломы-за-деньги-Правда-о-Покупке-Образования-купить-диплом
Сова гг – Сова гг, Сова гг
Cardano (ADA), known for its focus on sustainability and scalability, is also gaining traction as a payment method at crypto casinos.
купить дипломы о высшем образовании в москве купить дипломы о высшем образовании в москве .
Добрый день!
Мы можем предложить дипломы любой профессии по доступным тарифам.
itbitgroup.ru/legkiy-sposob-priobresti-diplom-onlayn
Здравствуйте!
Купить документ университета вы сможете у нас. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы старого образца. Гарантируем, что при проверке документов работодателем, никаких подозрений не появится.
Мы можем предложить дипломы любой профессии по доступным тарифам. Цена зависит от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы документы были доступными для большого количества граждан.
cubarebota.info/blogs/166/Как-можно-недорого-приобрести-аттестат-в-интернет-магазине
Будем рады вам помочь!
Привет!
Наши специалисты предлагают быстро заказать диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Диплом пройдет лубую проверку, даже при помощи специально предназначенного оборудования. Решайте свои задачи быстро и просто с нашей компанией.
dinskoi-raion.ru/forum/?PAGE_NAME=profile_view&UID=64044
Удачи!
Привет, друзья!
Где приобрести диплом специалиста?
http://www.soad.msk.ru/forum/viewforum.php?f=16
Успехов в учебе!
Как правильно купить диплом колледжа и пту в России, подводные камни
diploms-x.com/otzyvy
Добрый день!
Заказать диплом ВУЗа
landik-diploms-srednee.ru/svidetelstvo-o-rozhdenii В
Успехов в учебе!
this link jaxx io
Здравствуйте!
Заказать диплом о высшем образовании
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe В
Удачи!
Привет, друзья!
Как правильно приобрести диплом колледжа или ПТУ в России, важные моменты
http://www.figarohair.ru/conf/viewtopic.php?f=11&t=12644&sid=d865dd5fcb998564787e73c18fc0f732
Всегда вам поможем!.
На сайте https://nasosynsk.ru/ закажите звонок для того, чтобы узнать все про насосы. Среди популярных категорий: насосы для воды, бытовое оборудование, а также насосы для отопления, те, которые используются с целью отвода сточных вод, промышленное оборудование и многое другое. В этой компании на профессиональном уровне подбирают, реализуют, а также проектируют насосы. Перед вами самый большой выбор моделей, а также привлекательные расценки. Специалисты предприятия постоянно проходят стажировку.
[u][b] Привет![/b][/u]
[b]Мы готовы предложить документы ВУЗов[/b], которые находятся в любом регионе Российской Федерации. Можно заказать качественный диплом от любого заведения, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Документы делаются на бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и подписями.
[url=http://loolita.es/blogs/4320/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5/]loolita.es/blogs/4320/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5[/url]
Привет!
Заказать диплом о высшем образовании.
интайл.рф/club/user/71/blog/4533/
Привет!
Приобрести документ ВУЗа вы сможете у нас.
ast-diplom.com/kupit-diplom-vracha
Удачи!
Привет, друзья!
Быстрая покупка диплома старого образца: возможные риски
toolsrepair.ru/forum/viewtopic.php?f=5&t=2933455
Будем рады вам помочь!.
Привет, друзья!
Мы предлагаем документы техникумов, которые находятся в любом регионе РФ. Вы сможете заказать качественно сделанный диплом за любой год, включая документы старого образца СССР. Документы выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются всеми обязательными печатями и штампами.
forum.jeep-club.by/index.php?/blog/4/entry-3143-%D0%BE%D1%82%D0%BB%D0%B8%D1%87%D0%BD%D1%8B%D0%B5-%D1%86%D0%B5%D0%BD%D1%8B-%D0%B8-%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B9-%D0%B4%D0%BE/
Привет!
Купить диплом любого университета.
п»їmymotospeed.ru/diplom-po-tvoim-pravilam-priobreti-obrazovanie-kotoroe-tebe-nuzhno
Хорошей учебы!
Здравствуйте!
Где приобрести диплом специалиста?
Купить диплом университета.
wiki.gta-zona.ru/index.php/Обширный_каталог_документов_в_известном_онлайн-магазине
Сколько стоит диплом высшего и среднего образования и как его получить?
asxdiplomik.com/kupit-diplom-sankt-peterburg
Здравствуйте!
Как приобрести диплом техникума с минимальными рисками.
Приобрести диплом о высшем образовании.
o7klzazal.blog-gold.com/34522682/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82%D0%B0-%D0%B2-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Где купить диплом по нужной специальности?
bence.net/read-blog/75
Хорошей учебы!
Здравствуйте!
Всё, что нужно знать о покупке аттестата о среднем образовании
tuvanmedia.com/blog/2024/06/30/диплом-техникума-колледжа-2004-2006-фото/
Здравствуйте!
Заказать документ университета вы сможете у нас в столице.
ast-diplomas.com/kupit-diplom-nizhnij-novgorod
Добрый день!
Приобрести документ ВУЗа можно в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов РФ. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы СССР.
graph.org/Poluchite-diplomy-za-korotkij-srok-07-16
odincovoschool16.flybb.ru/viewtopic.php?f=2&t=840
lubercy.ixbb.ru/viewtopic.php?id=7310#p15859
biketrials.ru/live/blog.php?b=9137
ai.cheap/read-blog/25604
Привет!
Где купить диплом по нужной специальности?
Купить диплом ВУЗа.
http://www.clubalpintoulouse.fr/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=146
Здравствуйте!
Заказать диплом любого университета
Мы предлагаем быстро купить диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, штампами, подписями официальных лиц. Данный документ способен пройти любые проверки, даже с использованием специально предназначенного оборудования. Решайте свои задачи быстро и просто с нашими дипломами.
Где купить диплом по нужной специальности?
antonovschool.ru/forum/messages/forum1/topic650/message665/?result=new#message665
pdlspd.listbb.ru/viewtopic.php?f=3&t=409
meldog.3nx.ru/viewtopic.php?p=23387#23387
seriallove.bbok.ru/viewtopic.php?id=7015#p123048
goup.hashnode.dev/kupit-diplom-1-1-1
На сайте https://stapeli1.ru получите данные о том, какие стапели лучше всего подобрать для того, чтобы выполнить кузовной ремонт. Вы ознакомитесь с типами стапелей, особенностями, преимуществами. Есть информация о платформенных стапелях. Вы узнаете о достоинствах использования таких конструкций в ремонте. Имеется информация и о том, как правильно подобрать конструкцию, чтобы она прослужила как можно дольше и обрадовала своими эксплуатационными свойствами. Рассматриваются параметры, которые помогут подобрать устройство высокого качества.
Добрый день!
Купить документ о получении высшего образования можно в нашей компании в столице.
diplomasx.com/kupit-diplom-sankt-peterburg
Добрый день!
Заказать документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, включая документы Советского Союза.
roving.club/read-blog/1513
kolba.com.ua/index.php?topic=140911.new#new
forex.g-talk.ru/viewtopic.php?f=43&t=7159
panther.80lvl.ru/index.php
avtovideotest.ru/legalnyiy-diplom-bez-lishnih-hlopot-uznayte-kak
Привет, друзья!
Где купить диплом специалиста?
Купить диплом ВУЗа.
abris-zip.ru/company/personal/user/171/forum/message/1233/1243/
Привет!
Купить документ университета можно в нашей компании в столице.
ast-diplomas.com/kupit-diplom-ekaterinbur
Хорошей учебы!
Здравствуйте!
Как приобрести диплом техникума с минимальными рисками
charkheniloufari.com/купить-настоящий-диплом-в-городе-жуко/
Здравствуйте!
Купить документ ВУЗа вы имеете возможность в нашей компании.
diplomasx.com/kupit-diplom-krasnoyarsk
Здравствуйте!
Заказать документ о получении высшего образования вы сможете в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ. Вы получите диплом по любой специальности, включая документы старого образца.
etoprosto.ru/ru/forum/?category=5&action=topic
w98804oc.beget.tech/2024/07/13/kupite-diplom-i-nachnite-novuyu-zhizn.html
epistles.ru/blogs/1578/Диплом-в-кратчайшие-сроки-качественно-и-безопасно
ya.6bb.ru/viewtopic.php?id=3212#p5159
miku-crdb.ru/forum/messages/forum1/topic343/message372/?result=new#message372
Здравствуйте!
Заказать диплом любого университета
Мы предлагаем максимально быстро купить диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями. Данный документ способен пройти лубую проверку, даже с использованием профессиональных приборов. Решите свои задачи быстро с нашей компанией.
Где заказать диплом специалиста?
naijarise.com/read-blog/45
http://www.psorum.ru/member.php?u=4348
hellsms.com/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=6636
http://www.markusragger.at/chess/index.php/kforum/jm-news-pro-module/651988
bence.net/read-blog/65
Привет!
Заказать документ о получении высшего образования вы можете у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы получите необходимый диплом по любой специальности, любого года выпуска, в том числе документы СССР. Даем гарантию, что в случае проверки документов работодателем, каких-либо подозрений не появится.
http://www.seaman.com.ua/forum/index.php?login/login
doomelang.com/read-blog/6628
forum.fiat-club.ru/blog_post.php?do=updateblog&blogid=
uconnect.ae/read-blog/82807
netcallvoip.com/wiki/index.php/Купить_Диплом_в_Москве:_Быстро_и_Легально
Добрый день!
Купить диплом любого ВУЗа
landik-diploms-srednee.ru/attestat-shkoly В
Удачи!
Здравствуйте!
Купить документ о получении высшего образования можно в нашей компании в Москве.
diplomyx.com/kupit-diplom-ekaterinbur
Успехов в учебе!
Здравствуйте!
Заказать диплом любого университета.
bvf.ru/forum/showthread.php?p=25245738#post25245738
Хорошей учебы!
Добрый день!
Официальная покупка диплома вуза с упрощенной программой обучения.
Заказать диплом любого университета.
http://www.gamerlaunch.com/community/users/blog/6443244/2286742/%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%/?gid=535
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
http://www.2dommedical.com/2024/06/30/купить-главу-диплома/
Привет!
Купить документ о получении высшего образования можно у нас.
ast-diplom24.ru/kupit-diplom-omsk
Хорошей учебы!
http://hackedcards.cvv2cvc.net
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2 000 – Price $ 149.00
Item Western Union Transfers $ 1 000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://hackedcards.cvv2cvc.net Shop Cloned cards
Здравствуйте!
Мы изготавливаем дипломы любых профессий по доступным ценам.
http://www.flexartsocial.com/blogs/9940/На-что-конкретно-обратить-внимание-при-покупки-документов-в-сети
Как получить диплом стоматолога быстро и официально
ast-diplom.com/kupit-diplom-nizhnij-novgorod
Привет, друзья!
Купить диплом ВУЗа
Наши специалисты предлагают выгодно купить диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями официальных лиц. Наш диплом пройдет лубую проверку, даже при помощи специального оборудования. Решите свои задачи быстро и просто с нашими дипломами.
Где купить диплом специалиста?
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
zxz.listbb.ru/viewtopic.php?f=7&t=1416
ya.bestbb.ru/viewtopic.php?id=2962#p6549
http://www.simplemachines.org/about/smf/stats.php
rodina.listbb.ru/viewtopic.php?f=3&t=502
Привет, друзья!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
club.sabaylok.com/blogs/5110/Ваш-диплом-без-лишних-забот-быстро-и-безопасно
Окажем помощь!.
Привет!
Мы предлагаем документы ВУЗов, которые находятся в любом регионе РФ. Можно купить диплом от любого учебного заведения, за любой год, в том числе документы СССР. Дипломы и аттестаты печатаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригинала. Документы заверяются всеми обязательными печатями и подписями.
gamefilm.ru/index.php?/gallery/image/123-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D1%8B%D0%B5-%D1%86%D0%B5%D0%BD%D1%8B-%D0%B8-%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B9-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Здравствуйте!
Мы можем предложить дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
jrsjewellers.com/2024/06/29/купить-дипломы-университета/
Здравствуйте!
Купить диплом любого ВУЗа.
desankamaksimovickovin.edu.rs/index.php/component/k2/item/4-pellentesque-habitant-morbi-tristique-senectus-et-netus
Успешной учебы!
Здравствуйте!
Быстрая покупка диплома старого образца: возможные риски.
Приобрести диплом о высшем образовании.
huarenjiaohui.com/index.php?/gallery/image/126-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BF%D1%80%D0%BE%D0%B2%D0%B5%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5/
Привет!
Где заказать диплом специалиста?
Заказать диплом любого университета.
http://www.detailing-time.net/events/event/12-широкий-каталог-документов-в-знаменитом-интернет-магазине/
Психологическая помощь в Москве: поддержка и решения проблем
Сегодня многие люди сталкиваются с эмоциональными и психологическими трудностями, которые нуждаются в профессиональной поддержке. На сайте psyhologirinakurazh.ru вы найдете услуги квалифицированного психолога в Москве, который поможет вам справиться с различными жизненными ситуациями и улучшить качество жизни.
Консультации психолога в Москве для каждого
Если вам нужен [url=https://psyhologirinakurazh.ru/]лучшие психологи москвы рейтинг[/url] , наши специалисты готовы предложить индивидуальные и семейные консультации. Мы понимаем, что каждая проблема уникальна, поэтому подходим к каждому клиенту с вниманием и заботой. Наша команда профессиональных психологов поможет вам решить сложные вопросы, восстановить гармонию в отношениях и справиться с внутренними конфликтами.
Доступные цены и профессионализм
Мы предлагаем [url=https://psyhologirinakurazh.ru/]найти психолога в москве[/url] , чтобы профессиональная помощь была доступна каждому. В кабинете психолога в Москве вас ждет комфортная и доверительная атмосфера, способствующая откровенным беседам. Консультации проводятся в удобное время для вас, и вы можете быть уверены в полной конфиденциальности.
Отзывы клиентов и признание
Наш труд высоко оценивается клиентами, что подтверждается многочисленными положительными отзывами. Мы стремимся, чтобы каждый, кто обратился к нам, почувствовал значительные улучшения в своей жизни. Посетите наш сайт psyhologirinakurazh.ru, чтобы узнать больше о наших услугах и записаться на консультацию. Доверьтесь специалистам и начните свой путь к душевному равновесию уже сегодня.
СОУТ стоимость одного рабочего места
Гарантия безопасности на рабочем месте — это не просто выполнение стандартов, но и внимание к здоровью и комфорту персонала. Стоимость проведения специальной оценки условий труда помогает обнаружить и ликвидировать риски, что уменьшает травматизм и повышает рабочую эффективность. Обращайтесь в Safety Systems Group, чтобы создать безопасные условия для своих сотрудников и улучшить атмосферу в коллективе.
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы Советского Союза.
comptonrpp.listbb.ru/posting.php?mode=post&f=6
antonovschool.ru/forum/messages/forum1/topic707/message726/?result=new#message726
forum.osvita.od.ua/viewtopic.php?f=1&t=29416
pnevmokzn.80lvl.ru/search.php?search_id=egosearch
vip.forums.party/viewtopic.php?id=3439#p71062
Добрый день!
Приобрести диплом любого университета
Наши специалисты предлагают быстро и выгодно купить диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями. Диплом способен пройти лубую проверку, даже при использовании специального оборудования. Достигайте своих целей быстро и просто с нашим сервисом.
Где купить диплом по нужной специальности?
ya.bestbb.ru/viewtopic.php?id=2962#p6549
slliver.getbb.ru/viewtopic.php?f=62&t=826
pdlspd.listbb.ru/viewtopic.php?f=3&t=409
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
arsenal.listbb.ru/viewtopic.php?f=14&t=419
Добрый день!
Как приобрести диплом о среднем образовании в Москве и других городах
newrealgames.ru/diplom-lyuboy-spetsialnosti-kachestvenno-i-bezopasno
Всегда вам поможем!.
Здравствуйте!
Приобрести диплом о высшем образовании
arusak-diploms-srednee.ru/kupit-diplom-magistra В
Удачи!
Здравствуйте!
Официальная покупка аттестата о среднем образовании в Москве и других городах
blog.isport.ua/goebecom/auto-moto/119225.html#id
Рады помочь!.
Привет, друзья!
Где приобрести диплом по необходимой специальности?
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по выгодным ценам. Цена может зависеть от конкретной специальности, года получения и ВУЗа. Стараемся поддерживать для клиентов адекватную политику цен. Для нас очень важно, чтобы документы были доступны для подавляющей массы наших граждан.
Для вас можем предложить дипломы любой профессии по невысоким ценам.
datafornix.com/куплю-диплом-вуза-будут/
Будем рады вам помочь!.
Добрый день!
Заказать диплом любого ВУЗа
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske В
Успешной учебы!
Привет, друзья!
Быстрая схема покупки диплома старого образца: что важно знать?
worksale.jofo.me/2279094.html?_ga=2.83717407.828935667.1720695204-628517186.1720695204
Всегда вам поможем!.
Привет!
Мы готовы предложить дипломы любой профессии по выгодным тарифам.
http://www.elegantbeautyhk.com/купить-диплом-мархи-2/
Привет!
Заказать диплом университета
landik-diploms-srednee.ru/svidetelstvo-o-rozhdenii В
Успехов в учебе!
Добрый день!
Мы готовы предложить документы техникумов, которые находятся в любом регионе Российской Федерации. Можно купить качественно сделанный диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы делаются на бумаге самого высокого качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригинала. Они заверяются всеми необходимыми печатями и штампами.
mimedia.in/read-blog/50841
Привет!
Узнайте стоимость диплома высшего и среднего образования и процесс получения
ttartisan.ru/forum/user/4353
Поможем вам всегда!.
купить диплом стоит купить диплом стоит .
купить диплом о среднем пермь ast-diploms.com .
Здравствуйте!
Мы можем предложить документы техникумов, которые расположены в любом регионе РФ. Вы сможете заказать качественный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Документы печатаются на “правильной” бумаге самого высокого качества. Это дает возможность делать настоящие дипломы, которые не отличить от оригиналов. Документы заверяются необходимыми печатями и подписями.
jogibaba.com/blogs/215/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Заказать документ института вы имеете возможность у нас.
diploms-x24.ru/kupit-diplom-ekaterinbur
Привет!
Как получить диплом техникума с упрощенным обучением в Москве официально
l-avt.ru/support/dialog/?PAGE_NAME=profile_view&UID=68709
Рады помочь!.
Привет, друзья!
Приобрести диплом любого ВУЗа
Мы предлагаем выгодно и быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями. Наш документ способен пройти лубую проверку, даже с использованием специфических приборов. Решайте свои задачи быстро и просто с нашим сервисом.
Где заказать диплом специалиста?
http://www.gooalsocial.com/blogs/view/6162
05pjz6fg0.blog-ezine.com/28360530/Как-подыскать-проверенный-магазин-с-документами-Обзор-специалиста
encontrocentral.com/read-blog/2311
dailygram.com/blog/1304666/быстрое-оформление-дипломов-надежно-и-легально/
thesn.eu/blogs/2933/Ценообразование-дипломов-советы-от-экспертов
Привет, друзья!
Где купить диплом специалиста?
Заказать диплом любого ВУЗа.
site2.liodiz.ru/2024/07/04/shirokiy-vybor-dokumentov-v-znamenitom-onlayn-magazine.html
купить диплом в орехово зуево diplomasx.com .
Привет!
Заказать документ о получении высшего образования вы сможете у нас. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы Советского Союза. Даем гарантию, что в случае проверки документа работодателями, каких-либо подозрений не появится.
http://www.traveltravelforum.com/showthread.php/29752-Купить-Диплом-с-Гарантией-Подлинности?p=64682#post64682
blogs.rufox.ru/~sonnick84/48163.htm
make-coin.ru/vash-put-k-vyisshemu-obrazovaniyu-byistro-i-legalno
http://www.startspresto.ru/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=154
http://www.vocal.com.ua/node/62320
Добрый день!
Мы можем предложить дипломы любой профессии по приятным ценам.
newsbig.raidersfanteamshop.com/nadeznyj-internet-magazin-s-bolsim-assortimentom-diplomov
Добро пожаловать на наш сайт! Откройте лучшие финансовые решения прямо сейчас!
Наши предложения
Мы предлагаем широкий ассортимент финансовых продуктов: кредиты, банковские карты и займы, чтобы помочь вам достичь ваших целей и воплотить мечты в реальность.
кредитная карта с начислением процентов
Кредиты для всех нужд
Планируете покупку жилья, автомобиля или образование? Наши кредитные программы созданы для вас. Оформите кредит на нашем сайте за несколько минут, выбрав лучшие условия и сроки погашения.
Преимущества наших банковских карт
Наши карты обеспечивают удобство безналичных платежей и множество бонусов:
– **Кэшбэк и скидки у партнеров**
– **Программа лояльности**
Оформите карту онлайн и получите все преимущества уже сегодня!
Быстрые займы для непредвиденных расходов
Нужны деньги до зарплаты или на неожиданные расходы? Наши займы – это быстро и удобно. Мы предлагаем прозрачные условия и мгновенное одобрение заявок.
Наши преимущества:
– **Простота и Удобство:** Оформите заявку онлайн за считанные минуты.
– **Надежность и Прозрачность:** Честные условия без скрытых комиссий.
– **Индивидуальный Подход:** Мы учитываем ваши личные обстоятельства.
Не упустите шанс улучшить свою финансовую ситуацию!
кредит на ремонт
Оформите кредит, банковскую карту или займ на нашем сайте уже сегодня и насладитесь всеми преимуществами сотрудничества с надежным финансовым партнером.
Переходите на наш сайт и сделайте шаг к своим мечтам!
Добрый день!
Наш сервис предлагает заказать диплом в высочайшем качестве, неотличимый от оригинала без использования специального оборудования и опытного специалиста.
testowik.ru/index.php/forum/user/53108-yxygufi
Хорошей учебы!
Привет, друзья!
Купить документ университета можно у нас в Москве.
diplomyx24.ru/kupit-diplom-krasnoyarsk
Здравствуйте!
Где купить диплом специалиста?
Купить диплом ВУЗа.
malispa.ru/users/122
Привет!
Мы готовы предложить документы техникумов, расположенных на территории всей России. Можно заказать качественно сделанный диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это дает возможности делать государственные дипломы, которые невозможно отличить от оригиналов. Документы будут заверены необходимыми печатями и штампами.
pp-galaktika.com.ua/index.php/%D0%95%D1%81%D0%BB%D0%B8_%D0%BF%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D0%BE%D0%B2%D0%B0%D0%BB%D0%B8%D1%81%D1%8C_%D0%BA%D0%BB%D0%B0%D0%BF%D0%B0%D0%BD%D0%B0,_%D0%BC%D0%B0%D0%BD%D0%BE%D0%BC%D0%B5%D1%82%D1%80%D1%8B,_%D0%B7%D0%B0%D0%B4%D0%B2%D0%B8%D0%B6%D0%BA%D0%B8_-_%D0%B6%D0%B4%D0%B5%D0%BC_%D0%92%D0%B0%D1%81!
Привет, друзья!
Заказать документ ВУЗа вы имеете возможность в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любой специальности, любого года выпуска, в том числе документы старого образца.
c99596qr.beget.tech/2024/07/11/vash-diplom-dlya-karernogo-rosta-dostupno-kazhdomu.html
backshowtime.ru/diplom-na-zakaz-kachestvo-i-nadezhnost
antoinegriezmannclub.com/read-blog/3054
mkpnz.ru/users/8
sec31.ru/viewtopic.php?f=25&t=673861
Привет, друзья!
Купить документ о получении высшего образования вы сможете в нашей компании. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ.
forum.drustvogil-galad.si/index.php/topic,12725.new.html#new
testowik.ru/index.php/forum/user/53108-yxygufi
amazonebay.ru/profile.php?u=oqefafyg
e-audit.gefest.me/index.php?subaction=userinfo&user=erubysa
http://www.synthonia.com/index.php?option=com_k2&view=itemlist&task=user&id=624512
Добрый день!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
opengadjet.ru/diplomyi-ot-vedushhih-vuzov
Промокоды Vavada казино помогут вам получить дополнительные бонусы и сделать игровой процесс еще увлекательнее. Воспользуйтесь нашими предложениями и выигрывайте больше.
Защитите свои данные с помощью резидентских прокси, рекомендуем этим инструментом.
Как работают резидентские прокси?, прочитайте подробностями.
Какой резидентский прокси выбрать?, инструкция для пользователей.
Зачем нужны резидентские прокси?, узнайте возможностями.
В чем преимущество безопасности резидентских прокси?, обзор функций безопасности.
Как резидентские прокси защищают от опасностей?, разберем важные аспекты.
Как резидентский прокси помогает повысить эффективность?, рассмотрим основные плюсы.
Как улучшить скорость Интернета с резидентским прокси, советы для оптимизации работы.
Каким образом ускорить процесс парсинга с помощью резидентского прокси, анализ возможностей для парсеров.
Секреты анонимности с резидентским прокси, практические шаги к безопасности онлайн.
Секреты эффективной работы в соцсетях с резидентским прокси, рекомендации функционала.
Как сэкономить время с помощью аренды резидентского прокси?, сравним лучшие варианты.
Как избежать DDoS с резидентским прокси?, рассмотрим меры безопасности.
Почему резидентские прокси пользуются популярностью, проанализируем основные факторы.
Как выбрать между резидентским и дата-центровым прокси?, подсказки для выбора.
резидентные proxy [url=https://rezidentnieproksi.ru/]https://rezidentnieproksi.ru/[/url] .
Здравствуйте!
Где купить диплом специалиста?
Мы предлагаем документы институтов, которые находятся на территории всей Российской Федерации. Можно купить качественно напечатанный диплом от любого ВУЗа, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и штампами.
Мы предлагаем дипломы любой профессии по доступным тарифам.
ast-diplomy24.ru/kupit-diplom-krasnoyarsk
Окажем помощь!
Привет, друзья!
Заказать документ ВУЗа можно в нашей компании в Москве.
diplomasx24.ru/kupit-diplom-krasnoyarsk
Успешной учебы!
В Drip казино всегда можно найти что-то новое! Используйте промокоды для получения бонусов и наслаждайтесь игровым процессом с дополнительными возможностями.
Здравствуйте!
Где купить диплом специалиста?
Купить диплом университета.
c99596qr.beget.tech/2024/07/04/kak-podyskat-nadezhnyy-onlayn-magazin-s-obshirnym-vyborom-diplomov.html
https://doubledragon.kontek.net/forums/viewtopic.php?t=16772
В Vavada казино всегда можно найти что-то новое! Используйте промокоды для получения бонусов и наслаждайтесь игровым процессом с дополнительными возможностями.
Здравствуйте!
Купить документ университета можно в нашей компании в столице.
diplomyx24.ru/otzyvy
Здравствуйте!
Приобрести документ университета вы сможете в нашем сервисе. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить диплом по любой специальности, любого года выпуска, включая документы СССР.
автомедведь.рф/club/log/?SECTION_CODE=log
derivsocial.org/read-blog/2602
mirniy.flybb.ru/viewtopic.php?f=37&t=795
myweektour.ru/diplomyi-ot-proverennyih-postavshhikov/
drahthaar-forum.ru/viewtopic.php?f=30&t=11165
Привет, друзья!
Купить документ университета вы сможете в нашем сервисе.
diplomasx24.ru/kupit-diplom-vracha
Удачи!
Здравствуйте!
Как получить диплом техникума официально и без лишних проблем
tr.clanfm.ru/viewtopic.php?f=39&t=10093&p=20006#p20006
Всегда вам поможем!.
диплом вуза купить диплом вуза купить .
Привет, друзья!
Приобрести диплом о высшем образовании
Мы предлагаем быстро и выгодно купить диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями должностных лиц. Наш диплом пройдет лубую проверку, даже с использованием специальных приборов. Решите свои задачи быстро и просто с нашим сервисом.
Где заказать диплом специалиста?
mojgorod.getbb.ru/viewtopic.php?f=12&t=1432
http://www.cyberpinoy.net/read-blog/33307
blogs.rufox.ru/~worksale/48257.htm
antonovschool.ru/forum/messages/forum1/topic695/message713/?result=new#message713
sonnick84.full-design.com/Советы-специалиста-которые-возможность-дадут-легко-купить-документы-71044966
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашей компании. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любой специальности, включая документы старого образца. Даем 100% гарантию, что в случае проверки документов работодателем, подозрений не возникнет.
grp.7olimp.ru/viewforum.php?f=1
sp2jwmfv2.thekatyblog.com/27656729/Решили-выяснить-как-заказать-диплом-в-сети-Заходите
c99596qr.beget.tech/2024/07/08/vash-nastoyaschiy-diplom-bystro-i-udobno.html
thesleepinghusband.rolka.me/viewtopic.php?id=22084#p53892
http://www.nitrnd.com/blogs/159790/Хотите-узнать-как-купить-диплом-в-интернете-Ждем-Вас
Добрый день!
Мы можем предложить дипломы любой профессии по приятным тарифам. Стоимость будет зависеть от той или иной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для клиентов адекватную ценовую политику. Для нас важно, чтобы дипломы были доступны для подавляющей массы наших граждан.
eduardoxu098.blogitright.com/27193060/Фальшивый-диплом-Почему-это-не-Стоит-купить-диплом
купить бланк диплома о высшем образовании ast-diploms.com .
Привет, друзья!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
dachkanews.ru/kupite-diplom-dlya-vashego-budushhego/
Привет!
Купить документ университета вы сможете в нашей компании в столице. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы образца СССР. Гарантируем, что в случае проверки документов работодателем, никаких подозрений не возникнет.
Мы предлагаем дипломы любой профессии по выгодным ценам. Стоимость будет зависеть от той или иной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы документы были доступными для подавляющей массы граждан.
fijianvibe.com/blogs/780/Как-возможно-будет-быстро-заказать-аттестат-в-онлайн-магазине
Рады помочь!
Привет!
Заказать документ о получении высшего образования вы имеете возможность в нашем сервисе.
ast-diploms.com/kupit-diplom-o-srednem-obrazovanii
Успешной учебы!
аттестат за 8 классов купить аттестат за 8 классов купить .
Здравствуйте!
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на оригинальном бланке и заверен печатями, водяными знаками, подписями. Диплом способен пройти любые проверки, даже при использовании специальных приборов. Решите свои задачи быстро и просто с нашей компанией.
liderotrasli.ru/index.php?subaction=userinfo&user=okuwuc
Хорошей учебы!
Здравствуйте!
Где купить диплом специалиста?
Купить диплом университета.
comptonrpp.listbb.ru/viewtopic.php?f=6&t=714
Привет, друзья!
Приобрести документ о получении высшего образования вы можете в нашей компании в столице. Мы предлагаем документы об окончании любых университетов России. Вы получите диплом по любым специальностям, включая документы образца СССР.
or1gano.80lvl.ru/viewtopic.php?f=10&t=1028
artrp.5nx.ru/viewtopic.php?f=3&t=9675
fat-girls.ru/poluchite-diplom-bez-uchebyi-i-stressa
vintfint.com/blogs/22837/Получите-диплом-без-лишних-забот-и-усилий
netcallvoip.com/wiki/index.php/Профессиональные_дипломы_по_низким_ценам
Здравствуйте!
Приобрести документ университета можно у нас. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы сможете получить диплом по любым специальностям, включая документы образца СССР.
rodme.ru/legalnyy-diplom-pod-klyuch-nikakih-zabot-t12705.html
wiki.nikiforov.ru/index.php/Ваш_диплом_для_успешной_карьеры:_быстро_и_надежно
saumalkol.com/forum/разное-2/3565-ваш-диплом-без-лишних-забот-быстро-и-безопасно.html
onlinekinofun.ru/ofitsialnyiy-diplom-bez-lishnih-hlopot
aboutallfinance.ru/diplom-dlya-uspeshnoy-kareryi-dostupno-kazhdomu
Привет, друзья!
Мы можем предложить дипломы любой профессии по приятным ценам.
http://www.physiobuettner.de/купить-диплом-мгакхис-или-любого-вуза/
Привет!
Приобрести диплом любого университета
Мы предлагаем быстро и выгодно заказать диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Данный диплом способен пройти любые проверки, даже с использованием профессиональных приборов. Решайте свои задачи быстро и просто с нашими дипломами.
Где приобрести диплом по актуальной специальности?
lezt.ixbb.ru/viewtopic.php?id=101#p101
facesocial.demo3.dedicatedhost247.com/read-blog/14635
gaysocial.gay/read-blog/84
forum.safe-animals.ru/index.php?showtopic=28170
kormushka48.ru/forum/user/15788/
Привет!
Приобрести документ университета можно в нашем сервисе. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, в том числе документы СССР. Даем 100% гарантию, что при проверке документа работодателем, подозрений не появится.
intgez.com/read-blog/42195
http://www.yur-dom.ru/communication/forum/messages/forum3/message251/294-faq-i-tekhpodderzhka.-priobretaem-dokumenty-v-seti?result=new
topbazz.com/read-blog/6693_vy-hotite-uznat-kak-priobresti-dokumenty-v-internete-zhdem-vas.html
perfectohub.com/read-blog/7496
hvacprotalk.com/read-blog/217
аттестат 9 класс купить http://diploms-x.com .
Привет!
Сколько стоит получить диплом высшего и среднего образования легально?
yottamuch.com/index.php?/gallery/image/119-4-е-главных-группы-онлайн-магазинов-что-продают-документы/
Скачать торрент https://webtorrent.pro/ со всеми свежими фильмами со всего мира в один клик в отличном качестве без регистрации у нас на сайте. Любые жанры, любые годы, в том числе новинки 2024 – все готово к скачиванию. Легкий поиск, подборки по жанрам, лучшие фильмы, сериалы, мультфильмы в огромном количестве.
Здравствуйте!
Где заказать диплом специалиста?
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным тарифам. Стоимость зависит от той или иной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Для нас очень важно, чтобы дипломы были доступны для большого количества граждан.
Для вас изготавливаем дипломы любых профессий по выгодным тарифам.
gamerszona.ru/index.php?/blogs/entry/2-почему-намного-дешевле-будет-заказать-диплом-вуза/
Будем рады вам помочь!.
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании в столице.
diplomyx.com/kupit-diplom-krasnoyarsk
Привет!
Где заказать диплом по необходимой специальности?
Купить диплом любого ВУЗа.
myweektour.ru/oformlenie-diploma-lyuboy-spetsialnosti/
Здравствуйте!
Заказать документ ВУЗа можно у нас в столице. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы СССР.
http://www.hebergementweb.org/threads/oformlenie-diploma-pod-kljuch-prosto-i-udobno.1486955/
mirnuy.forumieren.de/t8213-topic#13485
lubov.listbb.ru/viewtopic.php?f=2&t=484
visogo9427.ixbb.ru/viewtopic.php?id=111#p111
magazin.orgsoft.ru/communication/forum/index.php?PAGE_NAME=profile_view&UID=190538
купить диплом о во купить диплом о во .
Привет!
Официальная покупка диплома ПТУ с упрощенной программой обучения
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske В
Здравствуйте!
Купить диплом любого университета.
fantok.net/blogs/460/%D0%93%D1%80%D0%B0%D0%BC%D0%BE%D1%82%D0%BD%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
купить диплом о профессиональной переподготовке asxdiplomik24.ru .
Привет!
Как не попасть впросак при покупке диплома колледжа или ПТУ в России
theigbos.com/blogs/3607/Как-купить-сейчас-неотличимый-от-оригинала-диплом-в-сети
купить диплом о среднем образовании в воронеже ast-diploms.com .
Привет!
Где купить диплом специалиста?
Заказать диплом о высшем образовании.
phobia.lt/index.php?/gallery/image/121-широкий-выбор-документов-в-знаменитом-интернет-магазине/
Здравствуйте!
Пошаговая инструкция по безопасной покупке диплома о высшем образовании
raussga.flybb.ru/viewtopic.php?f=12&t=2203
Будем рады вам помочь!.
Здравствуйте!
Вопросы и ответы: можно ли быстро купить диплом старого образца?
landik-diploms-srednee.ru/kupit-diplom-v-novosibirske В
Здравствуйте!
Заказать документ ВУЗа можно у нас в Москве.
ast-diploms.com/kupit-diplom-omsk
Успехов в учебе!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
[url=http://ast-diplom.com/kupit-diplom-moskva/]ast-diplom.com/kupit-diplom-moskva[/url]
поддельный диплом купить поддельный диплом купить .
Здравствуйте!
Как быстро и легально купить аттестат 11 класса в Москве
lossantosbattalion17.listbb.ru/viewtopic.php?f=3&t=401
Поможем вам всегда!.
аттестат купить москва аттестат купить москва .
Привет!
Как получить диплом техникума с упрощенным обучением в Москве официально
arusak-diploms-srednee.ru/kupit-diplom-v-krasnoiarske
Привет!
Официальное получение диплома техникума с упрощенным обучением в Москве
nophlix.com/купить-дипломы-университета/
Добрый день!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
jejerkepri.com/купить-диплом-все-вебинары/
Привет!
Мы готовы предложить документы техникумов, которые расположены в любом регионе РФ. Вы имеете возможность приобрести диплом от любого учебного заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Документы печатаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они заверяются всеми необходимыми печатями и штампами.
1rbfwc1w4.thechapblog.com/27876891/%D0%9B%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
Привет!
Как избежать рисков при покупке диплома колледжа или ВУЗа в России
sklad-slabov.ru/forum/user/8261
Окажем помощь!.
Здравствуйте!
Наш сервис предлагает заказать диплом высочайшего качества, который невозможно отличить от оригинального документа без использования дорогостоящего оборудования и квалифицированного специалиста.
otpusk.ru/user/index.php?backurl=/forum/topic/add/forum2/
Успешной учебы!
Привет, друзья!
Мы готовы предложить дипломы любой профессии по разумным тарифам.
wildlifediaries.com/купить-диплом-новосибирск/
Здравствуйте!
Заказать документ университета вы сможете в нашем сервисе. Мы оказываем услуги по производству и продаже документов об окончании любых университетов Российской Федерации. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы образца СССР.
yaoisennari.ekafe.ru/viewtopic.php?f=169&t=1786
http://www.import-moto.com/users/88
blog.nataraj.ru/~/Interest/Легальный диплом без лишних хлопот: узнайте как!
politictoday.ru/byistraya-dostavka-diplomov
86hm.ru/forum/flame/?topic_id=25111
Привет!
Заказать документ о получении высшего образования можно у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов России.
andi67.bplaced.net/dokuwiki/doku.php?id=russianydiplomix
armhleb.ru/index.php?subaction=userinfo&user=ykacyze
5.101.112.134/profile/ovivusez/
японецавто.рф/forum/user/51653/
чувашия.онлайн/index.php?subaction=userinfo&user=iqosapej
Привет!
Где приобрести диплом по необходимой специальности?
Мы готовы предложить документы ВУЗов, которые расположены на территории всей России. Можно купить качественно напечатанный диплом от любого высшего учебного заведения, за любой год, включая сюда документы старого образца СССР. Дипломы выпускаются на бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, которые не отличить от оригиналов. Документы будут заверены необходимыми печатями и подписями.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным ценам.
asxdiplomik.com/kupit-diplom-o-srednem-obrazovanii
Будем рады вам помочь!
Добрый день!
Где приобрести диплом по необходимой специальности?
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по доступным ценам. Стоимость может зависеть от конкретной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Для нас важно, чтобы документы были доступными для большинства наших граждан.
Для вас изготавливаем дипломы любых профессий по невысоким тарифам.
bbs.heyshell.com/forum.php?mod=viewthread&tid=28283
Рады оказать помощь!.
[url=https://sova-gg.com/]Сова гг[/url] – Sova gg обменник, Sova gg
Добрый день!
Где заказать диплом специалиста?
Купить диплом любого ВУЗа.
u90517ol.beget.tech/2024/07/04/bolshoy-vybor-dokumentov-v-znamenitom-magazine.html
Добрый день!
Мы предлагаем документы ВУЗов, расположенных на территории всей Российской Федерации. Можно заказать диплом за любой год, включая документы старого образца СССР. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это дает возможность делать государственные дипломы, которые не отличить от оригинала. Они будут заверены необходимыми печатями и штампами.
socialmoby.com/read-blog/391
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате, кодировка от алкоголизма Алматы безопасно.
Наши квалифицированные специалисты помогут вам побороть зависимость и вернуть контроль над своей жизнью. лечение алкоголизма Алматы отзывы
Мы предлагаем профессиональную помощь каждому пациенту, чтобы помочь им достичь результата. Наш центр предоставляет круглосуточную поддержку для всех, кто стремится преодолеть алкогольную зависимость. кодирование от алкоголизма Алматы метод – http://www.help4family.ru
Выберите здоровье и новую жизнь – выберите наш центр для лечения алкоголизма в Алмате.
http://oysterbaycapital.com/__media__/js/netsoltrademark.php?d=https://help4family.ru
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате! 6b6942d
Привет!
Где заказать диплом специалиста?
Купить диплом о высшем образовании.
rebornrpofficial.com/index.php?/files/file/9-обширный-каталог-документов-в-знаменитом-интернет-магазине/
Привет, друзья!
Мы готовы предложить документы техникумов, расположенных на территории всей РФ. Можно приобрести диплом от любого заведения, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Документы делаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются необходимыми печатями и подписями.
d6plus1.co.uk/read-blog/10026
где купить диплом сварщика asxdiplomik24.ru .
Привет!
Заказать документ университета вы имеете возможность в нашей компании в Москве.
ast-diplomas24.ru/kupit-diplom-krasnoyarsk
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
Привет, друзья!
Где приобрести диплом специалиста?
Приобрести диплом о высшем образовании.
foto-passau.com/gallery/image/6-большой-выбор-документов-в-популярном-интернет-магазине/?context=new
Привет!
Вопросы и ответы: можно ли быстро купить диплом старого образца?
konstruktiv.getbb.ru/viewtopic.php?f=12&t=6285
Будем рады вам помочь!.
Здравствуйте!
Мы готовы предложить дипломы любых профессий по приятным тарифам.
worldgonews.ru/diplomyi-ot-luchshih-vuzov
Привет!
Официальная покупка институтского диплома с упрощенным обучением в Москве
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe В
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным тарифам. Стоимость может зависеть от выбранной специальности, года выпуска и ВУЗа. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступными для большинства граждан.
bookmarkwuzz.com/story17194794/купить-диплом-о-высшем-цена
Привет!
Заказать документ института можно у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любым специальностям, включая документы СССР.
verkehrsknoten.de/index.php/forum/sozialvorschriften/91204#92168
tavasporan.flybb.ru/viewtopic.php?f=13&t=2666
horordark.ru/ofitsialnyiy-diplom-byistro-i-nadezhno
shoptema.ru/forum/topic/32712/
redebrasil.app/read-blog/503
Привет, друзья!
Где купить диплом специалиста?
Мы можем предложить дипломы любой профессии по выгодным ценам. Стоимость может зависеть от выбранной специальности, года получения и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы дипломы были доступными для большого количества граждан.
Для вас предлагаем дипломы любой профессии по выгодным тарифам.
micchat.online/read-blog/1479_kak-vybrat-nadezhnyj-magazin-kotoryj-realizuet-diplomy.html
Рады помочь!.
Здравствуйте!
Заказать диплом о высшем образовании.
k90280ul.beget.tech/2024/06/18/diplomy-ot-luchshih-universitetov.html
Успешной учебы!
Привет!
Приобрести документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите диплом по любой специальности, любого года выпуска, включая документы СССР. Даем 100% гарантию, что в случае проверки документов работодателем, каких-либо подозрений не возникнет.
Мы изготавливаем дипломы любых профессий по приятным тарифам. Стоимость будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для покупателей адекватную ценовую политику. Для нас очень важно, чтобы документы были доступными для большого количества наших граждан.
http://www.djjmeets.com/blogs/179423/Легко-приобретаем-документы-в-интернет-магазине-Russian-Diplom
Окажем помощь!
Привет, друзья!
Купить документ университета можно в нашей компании в Москве.
ast-diplom.com/otzyvy
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по выгодным ценам.
http://www.dr-ay.com/blogs/186078/Дипломы-от-Лучших-Университетов
Добрый день!
Заказать документ ВУЗа можно в нашей компании в Москве.
asxdiplomik.com/kupit-diplom-vracha
Успешной учебы!
Добрый день!
Приобрести документ ВУЗа вы имеете возможность в нашем сервисе. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы Советского Союза.
http://www.soad.msk.ru/forum/index.php?sid=bf79beef23638a030862f8f8e5ac4b05
bvf.ru/forum/showthread.php?p=25249466#post25249466
domovou.3nx.ru/viewtopic.php?p=6948#6948
http://www.mylot.su/blogs/2330
robotaforum.2bb.ru/post.php?fid=40
Привет!
Наша компания предлагает выгодно купить диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями. Диплом способен пройти лубую проверку, даже с применением специально предназначенного оборудования. Достигайте свои цели быстро и просто с нашей компанией.
geolan-ksl.ru/forum/user/85838/
Хорошей учебы!
Привет!
Наша компания предлагает приобрести диплом высочайшего качества, который не отличить от оригинального документа без участия специалиста высокой квалификации с дорогостоящим оборудованием.
buhtarma.ru/users/otere
Успешной учебы!
Добрый день!
Где заказать диплом специалиста?
Мы готовы предложить документы ВУЗов, которые находятся на территории всей РФ. Вы можете приобрести диплом за любой год, включая сюда документы старого образца СССР. Дипломы печатаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые не отличить от оригиналов. Документы заверяются необходимыми печатями и подписями.
Мы готовы предложить дипломы любых профессий по приятным тарифам.
diploms-x24.ru/kupit-diplom-vracha
Окажем помощь!
They allow people to better everbestnews.com understand geographical objects, which should be paid special attention to. Also, you should definitely take into account the fact that they are often used when it is customary to work with topographic maps, or in the process of studying mountain systems. This also includes route planning, and so on.
Привет, друзья!
Купить документ университета вы сможете у нас в Москве. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации.
forum.sprosiadvokata.ru/topic/22127-купить-диплом-техникума-h183k/
dianov.bget.ru/forum/thread57478.html#1281044
maplemania.6te.net/profile.php?lookup=16943
silkhunter.com/index.php?title=diploman
bazar-planet.ru/index.php?threads/Р’-РќРђРЁРЈ-КОМАНДУ-ЦЕЛЕ-УСТРЕМЛЕНЫХ-ТРЕБУЮТСЯ-РАБОТНРРљР-такие-РіРѕСЂРѕРґР°-Алмата-Тараза-Астана-Усть-Каменг.203/page-5#post-5031
Привет!
Аттестат 11 класса купить официально с упрощенным обучением в Москве
http://www.pajarojaguar.org/mediawiki01/index.php/Официальный_диплом_любой_профессии:_быстро_и_надежно
Окажем помощь!.
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате, лечение алкоголизма Алматы цены.
Наши квалифицированные специалисты помогут вам побороть зависимость и вернуть контроль над своей жизнью. кодировка от алкоголизма Алматы услуги
Мы предлагаем профессиональную помощь каждому пациенту, чтобы помочь им достичь результата. Наш центр предоставляет бесплатные консультации для всех, кто стремится преодолеть алкогольную зависимость. кодирование от алкоголизма в Алматы – http://help4family.ru
Выберите здоровье и новую жизнь – выберите наш центр для лечения алкоголизма в Алмате.
http://wops.yorkiepuppies.com/__media__/js/netsoltrademark.php?d=https://help4family.ru
Обретите здоровую жизнь без алкоголя с нашей программой реабилитации алкоголизма в Алмате! c5812fb
Привет!
Мы можем предложить дипломы любых профессий по приятным ценам.
blogs.northcountrypublicradio.org/allin/2024/06/30/куплю-молдавский-диплом/
Здравствуйте!
Всё, что нужно знать о покупке аттестата о среднем образовании.
Заказать диплом университета.
kw8ufhcbs.losblogos.com/27871498/%D0%94%D0%B5%D1%82%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B5%D0%BD%D0%B8%D1%8F-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Добрый день!
Приобрести документ университета можно у нас в столице.
ast-diploms.com/kupit-diplom-magistra
Удачи!
Привет, друзья!
Приобрести документ ВУЗа можно у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы Советского Союза.
poboltaem.foroactivo.com/post
dopalnenie.listbb.ru/viewtopic.php?f=3&t=717
rolevikionline.g-talk.ru/viewtopic.php?f=21&t=2881
fremontrp.listbb.ru/viewtopic.php?f=18&t=437
video.listbb.ru/viewtopic.php?f=3&t=409
На сайте https://afinaokna.ru/ есть возможность купить качественные и надежные деревянные, пластиковые либо алюминиевые окна, стеклопакеты. На изготовление конструкций уходят не более 3 дней. Компания берет предоплату в размере тысячи рублей. Предоставляется рассрочка на полгода. Доставка по Санкт-Петербургу бесплатная. После работ мусор выносится в мешках. В компании не только производят, но и продают, выполняют монтаж окон. Гарантируется качественное выполнение всех работ. Если и вы обратитесь за услугой в эту компанию, то получите гарантированно высокое качество.
купить диплом в кургане asxdiplomik24.ru .
Привет!
Заказать диплом о высшем образовании.
gamesfortop.ru/diplom-vashey-mechtyi-myi-pomozhem-vam-ego-dostich
Успехов в учебе!
На сайте https://oknatitan.ru/ закажите звонок для того, чтобы приобрести деревянные, пластиковые, алюминиевые окна, а также стеклопакеты. Можно приобрести окна в коттедж, которые идеально впишутся в общую концепцию, защитят от мороза, промозглого ветра, сквозняков. Прямо сейчас вы сможете воспользоваться скидкой в 47%. При необходимости специалисты специально для вас подберут наиболее оптимальный вариант материала, чтобы результат превзошел ожидания. На сайте ознакомьтесь с техническими характеристиками каждого материала, чтобы подобрать достойный вариант.
Приветствуем вас на канале проекта casino VAVADA! Здесь имеется самая свежая информация. Забудьте о повседневных заботах и проведите время за увлекательными слотами в высококачественном онлайн-казино Вавада! Вас ждет особая атмосфера и отличная графика. Ищете vavada
андроид? t.me/mvavada – здесь мы с вами делимся секретами успеха и своими знаниями. Казино VAVADA подходит всем без исключения. Вы точно оцените бонусы и скорость выводов. Саппорт старается любые вопросы решать довольно быстро. Играйте прямо сейчас. Удачи вам и победы!
Добрый день!
Где заказать диплом по нужной специальности?
Мы предлагаем документы ВУЗов, расположенных на территории всей РФ. Можно купить диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на бумаге самого высшего качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригиналов. Документы будут заверены всеми необходимыми печатями и штампами.
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
diplomyx24.ru/kupit-diplom-omsk
Поможем вам всегда!
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате, кодировка от алкоголизма Алматы безопасно.
Наши опытные врачи помогут вам побороть зависимость и вернуть контроль над своей жизнью. кодирование от алкоголизма Алматы срочно
Мы предлагаем профессиональную помощь каждому пациенту, чтобы помочь им достичь результата. Наш центр предоставляет круглосуточную поддержку для всех, кто стремится преодолеть алкогольную зависимость. кодировка от алкоголя Алматы врач – https://help4family.ru
Выберите здоровье и новую жизнь – выберите наш центр для лечения алкоголизма в Алмате.
http://hogwashbrush.com/__media__/js/netsoltrademark.php?d=https://help4family.ru
Обретите здоровую жизнь без алкоголя с нашей программой реабилитации алкоголизма в Алмате! fee0b6b
Привет, друзья!
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по разумным тарифам. Цена может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас важно, чтобы дипломы были доступны для большого количества граждан.
irc71.ru/index.php/jomsocial/groups/viewbulletin/191-kak-podyskat-khoroshij-internet-magazin-gde-mozhno-zakazat-diplom?groupid=47
Здравствуйте!
Наша компания предлагает заказать диплом в высоком качестве, неотличимый от оригинала без использования специального оборудования и опытного специалиста.
mail.unnewsusa.com/bbs/board.php?bo_table=free&wr_id=2227274
Удачи!
Здравствуйте!
Купить документ института можно в нашей компании. Мы предлагаем документы об окончании любых университетов России.
rem.4nmv.ru/forum/profile.php?action=show&member=9927
mc-pe.net/index.php?subaction=userinfo&user=ilonarir
l91692n8.beget.tech/profile.php?u=ejily
forum.theabyss.ru/index.php?showtopic=739687
dobrknigi.ru/howto/?PAGE_NAME=profile_view&UID=26385
Привет, друзья!
Приобрести диплом любого ВУЗа.
share.psiterror.ru/2024/07/07/kakie-internet-magaziny-s-dokumentami-est-na-segodnyashniy-moment.html
На сайте https://ipoteka-1.ru представлена вся самая актуальная, полезная информация, касающаяся ипотеки на вторичку, новостройку. Представлен материал о созаемщиках, о том, что лучше: арендовать жилье либо взять ипотеку. Есть данные о расходах на ипотеку и каким образом их понизить. Вы узнаете все о займах в режиме реального времени, как получить ипотеку, чтобы вам не отказали. Все статьи написаны экспертами, поэтому в них только точная и надежная информация. Вы получите ответ на вопрос, как быть, если нечем платить за ипотеку.
Привет, друзья!
Заказать документ о получении высшего образования можно в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите диплом по любой специальности, включая документы образца СССР. Гарантируем, что в случае проверки документа работодателями, каких-либо подозрений не возникнет.
Мы готовы предложить дипломы любой профессии по приятным тарифам. Цена может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступны для большинства наших граждан.
http://www.djjmeets.com/blogs/179423/Легко-приобретаем-документы-в-интернет-магазине-Russian-Diplom
Рады оказаться полезными!
Защитите свои данные с помощью резидентских прокси, для чего это нужно.
Получите доступ к контенту из других стран с резидентскими прокси, полномасштабным контентом.
Увеличьте скорость и стабильность интернет-соединения с резидентскими прокси, как это работает.
Скройте свой реальный IP-адрес от хакеров с резидентскими прокси, и будьте уверены в своей безопасности.
Защитите свою личную жизнь и данные с резидентскими прокси, и оставайтесь незамеченными.
Обходите цензуру и блокировки с резидентскими прокси, и не бойтесь за свою приватность.
резидентные proxy https://rezidentnie-proksi.ru/ .
Здравствуйте!
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков.
Купить диплом университета.
octomo.co.uk/read-blog/949
Здравствуйте!
Как приобрести диплом о высшем образовании в Москве и других городах
landik-diploms-srednee.ru/svidetelstvo-o-rozhdenii В
Здравствуйте!
Наша компания предлагает быстро и выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Данный диплом способен пройти лубую проверку, даже при помощи специфических приборов. Достигайте цели быстро и просто с нашими дипломами.
moskovskij.getbb.ru/viewtopic.php?f=12&t=2231
Хорошей учебы!
Добрый день!
Быстрая схема покупки диплома старого образца: что важно знать?
landik-diploms-srednee.ru/svidetelstvo-o-razvode В
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате, кодировка от алкоголя в Алматы цена.
Наши квалифицированные специалисты помогут вам побороть зависимость и вернуть контроль над своей жизнью. кодировка от алкоголизма в Алматы
Мы предлагаем индивидуальный подход каждому пациенту, чтобы помочь им достичь результата. Наш центр предоставляет круглосуточную поддержку для всех, кто стремится преодолеть алкогольную зависимость. кодирование от алкоголя Алматы врач – https://www.help4family.ru
Выберите здоровье и новую жизнь – выберите наш центр для лечения алкоголизма в Алмате.
https://www.serbiancafe.com/lat/diskusije/new/redirect.php?url=https://help4family.ru
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате! 5812fb1
Добрый день!
Приобрести диплом университета.
fordtransit.5nx.ru/viewtopic.php?f=25&t=7433
Хорошей учебы!
Привет, друзья!
Купить диплом университета
Мы предлагаем быстро и выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Данный диплом способен пройти лубую проверку, даже при помощи специальных приборов. Достигайте своих целей быстро с нашими дипломами.
Где приобрести диплом специалиста?
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
forum.qwas.ru/kupit-diplom-t19852.html
seriallove.bbok.ru/viewtopic.php?id=7015#p123048
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
molbiol.ru/forums/index.php?showtopic=1179953
Привет, друзья!
Заказать документ о получении высшего образования вы сможете в нашей компании в столице.
ast-diplomas24.ru/kupit-diplom-magistra
Привет, друзья!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
beijingpal.com/read-blog/919
Окажем помощь!.
Привет!
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по выгодным тарифам. Стоимость будет зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы документы были доступны для большого количества граждан.
bookmarkingace.com/story17071684/купить-диплом-в-Воронеже
Здравствуйте!
Заказать документ института можно в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы старого образца. Гарантируем, что в случае проверки документов работодателем, подозрений не появится.
Мы изготавливаем дипломы любых профессий по доступным ценам. Стоимость будет зависеть от выбранной специальности, года получения и университета. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
qyshikisoxa.lowescouponn.com/kak-vozmozno-bystro-kupit-diplom-v-internet-magazine
Всегда вам поможем!
Добрый день!
Заказать документ о получении высшего образования можно в нашей компании.
diploms-x24.ru/kupit-diplom-nizhnij-novgorod
Удачи!
Добрый день!
Мы можем предложить документы ВУЗов, которые расположены в любом регионе Российской Федерации. Можно купить качественно напечатанный диплом за любой год, включая сюда документы СССР. Дипломы и аттестаты делаются на бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и подписями.
datasphere.ru/club/user/12/blog/4373/
Здравствуйте!
Купить документ ВУЗа вы имеете возможность в нашем сервисе.
diploms-x24.ru/kupit-diplom-rostov-na-donu
Добрый день!
Как приобрести диплом о среднем образовании в Москве и других городах.
Приобрести диплом любого ВУЗа.
bmw-donbass.ru/gallery/image/846-%D0%BD%D0%B8%D0%B7%D0%BA%D0%B8%D0%B5-%D1%86%D0%B5%D0%BD%D1%8B-%D0%B8-%D0%B8%D0%B4%D0%B5%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D1%8B%D0%B2%D0%B0%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Здравствуйте!
Где приобрести диплом по нужной специальности?
Приобрести диплом о высшем образовании.
mediamemorial.ru/club/user/69594/forum/message/3756/13238/
https://prepaid-cards.cvv2cvc.net
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2 000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
https://prepaid-cards.cvv2cvc.net
Привет, друзья!
Как официально купить диплом вуза с упрощенным обучением в Москве
pol-doma.com/forum/user/29393
Всегда вам поможем!
Привет, друзья!
Купить диплом о высшем образовании.
gracebook.app/blogs/1192/%D0%A7%D1%82%D0%BE-%D0%BF%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%B4%D0%BB%D1%8F-%D1%81%D0%BE%D0%B7%D0%B4%D0%B0%D0%BD%D0%B8%D1%8F-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D0%BE%D0%B3%D0%BE-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%B0
Здравствуйте!
Наша компания предлагает выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Данный диплом пройдет лубую проверку, даже при использовании специального оборудования. Решите свои задачи быстро с нашим сервисом.
blogs.rufox.ru/~runoklisfgy/47401.htm
Успехов в учебе!
Здравствуйте!
Заказать документ ВУЗа можно в нашем сервисе.
ast-diploms.com/kupit-diplom-ekaterinbur
Добрый день!
Где заказать диплом по актуальной специальности?
Приобрести диплом о высшем образовании.
k96586v0.beget.tech/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=140
Нужен качественный ремонт стиральной машины в Москве? Наш сервисный центр предлагает оперативные и профессиональные услуги по хороший ремонт стиральных машин в москве. Присоединяйтесь к нашей группе в Telegram и узнайте больше: https://t.me/s/remont_stiralnyh_mashin_moskve
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате, лечение алкоголизма Алматы.
Наши опытные врачи помогут вам побороть зависимость и вернуть контроль над своей жизнью. кодировка от алкоголизма Алматы специалист
Мы предлагаем индивидуальный подход каждому пациенту, чтобы помочь им достичь результата. Наш центр предоставляет бесплатные консультации для всех, кто стремится преодолеть алкогольную зависимость. кодирование от алкоголя Алматы отзывы – http://www.help4family.ru/
Выберите здоровье и новую жизнь – выберите наш центр для лечения алкоголизма в Алмате.
http://gsavoretti.com/__media__/js/netsoltrademark.php?d=https://help4family.ru
Обретите здоровую жизнь без алкоголя с нашей программой реабилитации алкоголизма в Алмате! fb65d57
Добрый день!
Мы изготавливаем дипломы любой профессии по приятным ценам.
adobe-photoshop.ru/search/водопад/
Добрый день!
Где заказать диплом специалиста?
Заказать диплом университета.
app-s.ru/blog/kak_podyskat_nadezhnyj_magazin_s_ogromnym_katalogom_diplomov/2024-07-04-1868
купить дипломы вуза срочно ast-diploms.com .
Добрый день!
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по невысоким тарифам.
shockmusik.ru/legkiy-i-byistryiy-sposob-poluchit-diplom
Здравствуйте!
Купить документ института вы имеете возможность в нашем сервисе.
ast-diplom.com/kupit-diplom-rostov-na-donu
Удачи!
Привет!
Мы готовы предложить дипломы любой профессии по приятным ценам.
http://www.globalcorp.it/купить-диплом-мгудт-или-любого-вуза-ро/
купить диплом о среднем образовании в перми купить диплом о среднем образовании в перми .
Привет!
Заказать диплом о высшем образовании
Наши специалисты предлагают максимально быстро купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Диплом пройдет любые проверки, даже с применением специального оборудования. Достигайте своих целей быстро с нашими дипломами.
Где заказать диплом по необходимой специальности?
forumkk.listbb.ru/viewtopic.php?f=12&t=392
blogs.rufox.ru/~worksale/47159.htm
worksale777.blogspot.com/2024/06/blog-post_30.html
mkpnz.ru/users/8
macadamlab.ru/wiki/index.php?title=пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ
Привет, друзья!
Приобрести документ института можно в нашей компании. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любой специальности, включая документы СССР.
talkrealty.ru/dostupnyie-diplomyi-dlya-vashego-uspeha
wegug.in/blogs/1120/Легальный-диплом-без-лишних-хлопот-узнайте-как
lubercy.ixbb.ru/viewtopic.php?id=7310#p15859
skazka.g-talk.ru/viewtopic.php?f=1&t=1808
true.pahom.su/2024/07/13/diplom-lyuboy-specialnosti-kachestvenno-i-operativno.html
купить диплом в нижневартовске http://www.diploms-x.com/ .
Добрый день!
Заказать документ университета вы сможете в нашей компании в Москве.
ast-diplomas.com/kupit-diplom-krasnoyarsk
Успешной учебы!
Добрый день!
Купить диплом о высшем образовании.
sonnick84.howeweb.com/28777915/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B5%D0%BD%D0%BD%D1%8B%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
Привет, друзья!
Где заказать диплом специалиста?
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16579&TITLE_SEO=16579-ofitsialnyy-diplom-bez-ucheby-i-ekzamenov&MID=861047&result=new#message861047
Успешной учебы!
Здравствуйте!
Быстрая покупка диплома старого образца: возможные риски
arusak-diploms-srednee.ru/diplom-sredne-spetcialnoe-obrazovanie
[u][b] Привет![/b][/u]
[b]Мы изготавливаем дипломы[/b] любой профессии по выгодным тарифам.
[url=http://stlvolleyball.com/купить-главу-диплома//]stlvolleyball.com/купить-главу-диплома/[/url]
раковина на стиральную машину купить
Здравствуйте!
Мы можем предложить дипломы любой профессии по приятным ценам.
bullzhub.com/2024/07/07/кто-купил-диплом-в-сга/
Привет, друзья!
Заказать документ о получении высшего образования можно в нашей компании в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы получите диплом по любой специальности, любого года выпуска, включая документы старого образца.
onlaintelevizia.listbb.ru/viewtopic.php?f=2&t=494
umorforme.ru/nadezhnyie-diplomyi-ot-professionalov
rst.adk.audio/company/personal/user/1577/forum/message/1957/1992/#message1992
590909.ru/users/74
http://www.noo.by/wiki/Получите_диплом,_о_котором_всегда_мечтали
Обретите здоровую жизнь без алкоголя с нашей программой реабилитации алкоголизма в Алмате, кодирование от алкоголя Алматы отзывы.
Наши опытные врачи помогут вам побороть зависимость и вернуть контроль над своей жизнью. кодировка от алкоголизма Алматы
Мы предлагаем индивидуальный подход каждому пациенту, чтобы помочь им достичь результата. Наш центр предоставляет бесплатные консультации для всех, кто стремится преодолеть алкогольную зависимость. кодирование от алкоголя в Алматы – http://www.help4family.ru
Выберите здоровье и новую жизнь – выберите наш центр для лечения алкоголизма в Алмате.
http://bunco.jewricankitchen.com/__media__/js/netsoltrademark.php?d=https://help4family.ru
Обретите здоровую жизнь без алкоголя с нашей программой лечения алкоголизма в Алмате! fee0b6b
Привет!
Где заказать диплом по актуальной специальности?
Мы предлагаем дипломы любых профессий по разумным ценам. Цена будет зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Для нас важно, чтобы документы были доступны для большого количества граждан.
Для вас изготавливаем дипломы любых профессий по разумным тарифам.
doomelang.com/read-blog/6380_kak-podobrat-proverennyj-onlajn-magazin-kotoryj-prodaet-dokumenty.html
Окажем помощь!.
Привет, друзья!
Приобрести документ института можно в нашей компании.
ast-diplom24.ru/kupit-diplom-vracha
Успехов в учебе!
Привет!
Купить диплом о высшем образовании
Наша компания предлагает максимально быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Документ способен пройти лубую проверку, даже с использованием специальных приборов. Решайте свои задачи максимально быстро с нашим сервисом.
Где заказать диплом специалиста?
ya.5bb.ru/viewtopic.php?id=19893#p60223
blogs.rufox.ru/~sonnick84/48160.htm
astroroleplay.getbb.ru/viewtopic.php?f=6&t=480
rsn360.ru/blogs/509/Официальные-дипломы-по-доступной-цене
ukrevents.ru/nastoyashhie-diplomyi-bez-lishnih-voprosov/
Здравствуйте!
Диплом пту купить официально с упрощенным обучением в Москве
http://www.topairpack.com/купить-бланки-дипломов/
Добрый день!
Купить документ института вы можете у нас в столице. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, включая документы СССР. Даем 100% гарантию, что при проверке документа работодателями, каких-либо подозрений не появится.
pamplusmus.com/blogs/45/Что-именно-требуется-из-оборудования-для-создания-документов
astroroleplay.getbb.ru/viewtopic.php?f=6&t=480
xiudda2iz.blogsumer.com/27945098/Вы-хотите-выяснить-как-заказать-диплом-в-сети-недорого-Ждем-Вас
lidertude.com/blogs/1191/Что-необходимо-из-оборудования-для-создания-документов
fsmi.wiki/index.php?title=Купить_Диплом_с_Гарантией_Подлинности
Добрый день!
Купить документ о получении высшего образования можно в нашей компании. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы образца СССР.
russiajoy.ru/diplomyi-s-dostavkoy
laver.listbb.ru/viewtopic.php?f=3&t=1062
nalubyutemy.forum2x2.ru/t22732-topic#47935
talkitter.com/create-blog/
gamemotors.ru/ofitsialnyiy-diplom-bez-uchebyi-i-ekzamenov
Привет!
Мы предлагаем документы ВУЗов, расположенных в любом регионе России. Вы можете заказать диплом за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригиналов. Они будут заверены необходимыми печатями и штампами.
rab.chsl.ru/club/user/2/blog/8/
На сайте https://dvuhstoechnie-podjemniki.ru вы найдете любопытную, интересную и свежую информацию, которая касается двухстоечных подъемников. Также рассматривается то, какую конструкцию лучше всего выбрать для своих целей и опираясь на финансовое положение. Рассматриваются различные виды подъемников, а также их преимущества. Возьмите на вооружение такие важные параметры, как: грузоподъемность, высота подъема и другое. Также рассматриваются и востребованные производители оборудования.
Привет, друзья!
Мы изготавливаем дипломы любой профессии по доступным ценам.
eaglepharmausa.us/2024/07/13/дипломы-выпускнику-детского-сада-куп/
Привет!
Где заказать диплом по нужной специальности?
Заказать диплом любого ВУЗа.
astart.pl/index.php?/gallery/image/6-большой-каталог-документов-в-популярном-магазине/
Здравствуйте!
Мы готовы предложить документы ВУЗов, которые находятся в любом регионе РФ. Вы можете приобрести качественно сделанный диплом за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются всеми обязательными печатями и подписями.
mysmart.ru/index.php?/gallery/image/661-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D1%8B%D0%B5-%D1%86%D0%B5%D0%BD%D1%8B-%D0%B8-%D0%B8%D0%B4%D0%B5%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Привет, друзья!
Приобретение диплома ПТУ с сокращенной программой обучения в Москве
vistasalamat.com/диплом-магистра-2014-20242024-фото/
Добрый день!
Реально ли приобрести диплом стоматолога? Основные шаги
itstagram.ru/read-blog/840
Рады оказать помощь!
Обретите здоровую жизнь без алкоголя с нашей программой реабилитации алкоголизма в Алмате, лечение алкоголизма Алматы отзывы.
Наши квалифицированные специалисты помогут вам побороть зависимость и вернуть контроль над своей жизнью. кодировка от алкоголя Алматы центр
Мы предлагаем индивидуальный подход каждому пациенту, чтобы помочь им достичь результата. Наш центр предоставляет бесплатные консультации для всех, кто стремится преодолеть алкогольную зависимость. кодирование от алкоголизма отзывы Алматы – https://help4family.ru
Выберите здоровье и новую жизнь – выберите наш центр для лечения алкоголизма в Алмате.
http://fimathehk50.com/__media__/js/netsoltrademark.php?d=https://help4family.ru
Обретите здоровую жизнь без алкоголя с нашей программой реабилитации алкоголизма в Алмате! bfee0b6
Привет, друзья!
Купить диплом о высшем образовании
Наша компания предлагает быстро и выгодно купить диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Документ способен пройти лубую проверку, даже с использованием специфических приборов. Достигайте цели максимально быстро с нашей компанией.
Где заказать диплом специалиста?
http://www.simplemachines.org/about/smf/stats.php
ya.2bb.ru/viewtopic.php?id=19040#p240217
autoprajs.ru/15204.html
http://www.simplemachines.org/about/smf/stats.php
mkpnz.ru/users/8
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным ценам.
http://www.chaodisiaque.com/forum/viewtopic.php?pid=21984
Привет, друзья!
Полезные советы по безопасной покупке диплома о высшем образовании
sportandpolitics.ukrbb.net/viewtopic.php?f=24&t=13633
Поможем вам всегда!.
Привет, друзья!
Где заказать диплом по нужной специальности?
Мы можем предложить дипломы психологов, юристов, экономистов и любых других профессий по выгодным ценам. Стоимость будет зависеть от определенной специальности, года получения и университета. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для большого количества граждан.
Для вас изготавливаем дипломы любой профессии по приятным тарифам.
linkheed.com/blogs/3407/Хотите-заказать-диплом-у-проверенного-производителя-Заходите
Поможем вам всегда!.
Добрый день!
Процесс получения диплома стоматолога: реально ли это сделать быстро?
gamemotors.ru/diplomyi-s-polnyim-paketom-dokumentov-2
Здравствуйте!
Приобрести диплом любого ВУЗа
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Диплом пройдет лубую проверку, даже при помощи профессионального оборудования. Решите свои задачи быстро с нашей компанией.
Где купить диплом по необходимой специальности?
danceway74.ru/users/36
bibomi.com/blogs/440/Что-именно-требуется-из-оборудования-для-производства-документов
blogs.rufox.ru/~worksale/48257.htm
medium.com/@oximus777/купить-настоящий-диплом-за-24-часа-9fb3659baba9
autogroupe.ru/kupit-diplom-doveryayte-professionalam
Добрый день!
Купить документ о получении высшего образования вы можете у нас.
diplomasx.com/kupit-diplom-vracha
Здравствуйте!
Заказать документ университета можно у нас в столице. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы СССР. Даем 100% гарантию, что при проверке документов работодателем, подозрений не появится.
dachaweek.ru/vash-shans-na-vyisshee-obrazovanie-kupit-diplom
sharemeglobal.com/blogs/906/Ключевые-затраты-производителя-документов-авторский-обзор
sngine.codiantprod.com/blogs/221/Ценные-рекомендации-по-покупки-документа-в-сети
lib22.ru/question/blagodarya-chemu-internet-magaziny-s-dokumentami-stol-populyarny/
wiki.hightgames.ru/index.php/Легкий_выбор_магазина,_который_реализует_дипломы_и_аттестаты
Здравствуйте!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
landik-diploms-srednee.ru/svidetelstvo-o-rozhdenii
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы СССР.
http://www.seaman.com.ua/forum/index.php?threads/vasha-mechta-o-diplome-realna.37773/
p33340zg.beget.tech/2024/07/13/vash-diplom-bez-ucheby-i-ekzamenov.html
entrainment.listbb.ru/viewtopic.php?f=96&t=24256
newrealgames.ru/ekspress-dostavka-diplomov-po-vsem-spetsialnostyam
o97765bq.beget.tech/2024/07/15/diplomy-bez-ozhidaniya-i-slozhnostey.html
Здравствуйте!
Как не попасть впросак при покупке диплома колледжа или ПТУ в России
pika.listbb.ru/posting.php?mode=post&f=9
Рады оказаться полезными!
Привет, друзья!
Заказать документ института вы сможете в нашей компании в Москве.
ast-diplomas.com/kupit-diplom-rostov-na-donu
Привет, друзья!
Как оказалось, купить диплом кандидата наук не так уж и сложно
arusak-diploms-srednee.ru/kupit-diplom-magistra
Здравствуйте!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
worksale.jofo.me/2279094.html?_ga=2.83717407.828935667.1720695204-628517186.1720695204
Всегда вам поможем!
купить диплом о среднем специальном образовании цена купить диплом о среднем специальном образовании цена .
Добрый день!
Заказать документ о получении высшего образования можно в нашей компании в столице.
diploms-x.com/otzyvy
Добрый день!
Быстрая схема покупки диплома старого образца: что важно знать?
landik-diploms-srednee.ru/kupit-diplom-saratov
Привет, друзья!
Купить диплом университета.
aboutallfinance.ru/poluchenie-kopiy-diplomov-o-professionalnom-obuchenii
Удачи!
[u][b] Привет, друзья![/b][/u]
[b]Где приобрести диплом по необходимой специальности?[/b]
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам. Цена будет зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большого количества наших граждан.
[b]Для вас предлагаем дипломы[/b] любых профессий по доступным тарифам.
[url=http://kotanusantara.cloud/index.php?/events/event/7-почему-гораздо-дешевле-и-проще-заказать-диплом-вуза/]kotanusantara.cloud/index.php?/events/event/7-почему-гораздо-дешевле-и-проще-заказать-диплом-вуза/[/url]
[u][b] Рады помочь![u][b].
Добрый день!
Сколько стоит диплом высшего и среднего образования и как его получить?
http://www.terrapevtika.ru/forum/?PAGE_NAME=message&FID=1&TID=511&TITLE_SEO=511-kupit-diplom-kandidata-nauk&MID=736&result=reply#message736
Будем рады вам помочь!.
Привет!
Как оказалось, купить диплом кандидата наук не так уж и сложно
http://www.vocal.com.ua/node/62415
Окажем помощь!
Здравствуйте!
Где заказать диплом специалиста?
Заказать диплом любого университета.
piratesouls.org/events/event/12-как-найти-надежный-интернет-магазин-с-огромным-выбором-дипломов/
Вопросы и ответы: можно ли быстро купить диплом старого образца?
diploms-x.com/kupit-diplom-magistra
Добрый день!
Быстрая покупка диплома старого образца: возможные риски.
Купить диплом ВУЗа.
sonnick84.webnode.page/l/kak-vozmozhno-bystro-priobresti-attestat-v-onlajn-magazine/
Если вам срочно нужны деньги, подписывайтесь на канал Все новые МФО – Telegram ! Мы собрали лучшие предложения от МФО, которые выдают займы на карту без отказа и долгих проверок. Наш канал поможет вам найти самые выгодные условия: займы от 1 до 30 тысяч рублей, даже с плохой кредитной историей. Узнайте, где можно получить займ под 0% для новых клиентов. Выдача займов без проверки – Telegram — это ваш гид по миру срочных займов. Не теряйте время, подпишитесь и получите деньги быстро и без лишних проблем!
Привет!
Мы можем предложить документы ВУЗов, которые расположены в любом регионе РФ. Вы сможете купить качественно сделанный диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Документы делаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригинала. Документы заверяются необходимыми печатями и подписями.
http://www.leenkup.com/read-blog/16623
Привет, друзья!
Купить диплом ВУЗа
Наши специалисты предлагают максимально быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Диплом способен пройти лубую проверку, даже с применением профессионального оборудования. Решите свои задачи быстро и просто с нашей компанией.
Где заказать диплом по нужной специальности?
comedyforme.ru/kupit-diplom-bez-posrednikov-i-suetyi
doremichildcarecentre.com/index.php/forum/welcome-mat/191388
1776reloaded.us/blogs/63/Купить-диплом-быстро-и-надежно
poetzinc.com/read-blog/11680
anatoliyrud.ekafe.ru/viewforum.php?f=29
Добрый день!
Где купить диплом специалиста?
Заказать диплом о высшем образовании.
logan.in.ua/people/user/7276/blog/7929/
Привет!
Приобрести документ университета можно в нашем сервисе.
ast-diplomy.com/kupit-diplom-krasnoyarsk
Хорошей учебы!
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
lighttur.ru/diplomyi-ot-avtoritetnyih-obrazovatelnyih-uchrezhdeniy
Здравствуйте!
Приобрести документ университета можно в нашей компании. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов России. Вы получите необходимый диплом по любой специальности, включая документы старого образца. Даем гарантию, что при проверке документа работодателями, каких-либо подозрений не появится.
video.listbb.ru/viewtopic.php?f=3&t=405
u2c.tv/member.php?u=30984
http://www.hebergementweb.org/threads/kupit-diplom-s-garantiej-podlinnosti.1480408/
http://www.xrated.social/blogs/146/Как-можно-приобрести-сейчас-качественный-диплом-в-сети
8bsbnjtgp.howeweb.com/28820997/Решили-узнать-как-приобрести-диплом-в-сети-недорого-Заходите
Виртуальные карточные и настольные игры также ждут своих поклонников. От блэкджека до покера – испытайте удачу и стратегию https://par-torg.com/innovatsionnye-resheniya-shagma-krasota-i-funktsionalnost-na-vysshem-urovne/
1newss.com
Здравствуйте!
Заказать документ университета можно в нашей компании в Москве.
asxdiplomik24.ru/kupit-diplom-ekaterinbur
Хорошей учебы!
Добрый день!
Где приобрести диплом специалиста?
nsibirsk.ru/forum/obyavleniya/newtopic/#google_vignette
Успешной учебы!
Здравствуйте!
Мы готовы предложить дипломы любых профессий по приятным тарифам.
clinicarodrigolopes.com.br/купить-диплом-в-димитровграде/
Принимать финансовые решения может быть сложно. Но с нашим каталогом финансовых продуктов это стало проще, чем когда-либо!
кредит наличными без справок
Мы собрали все лучшие финансовые продукты в одном месте, чтобы вы могли легко сравнить их и найти те, которые подходят именно вам. Наши экспертные обзоры и рейтинги помогут вам принять обоснованное решение, соответствующее вашим уникальным потребностям.
Независимо от того, ищете ли вы кредит наличными, дебетовую карту или инвестиционный счет, наш каталог финансовых продуктов поможет вам сделать правильный выбор.
Добро пожаловать на сайт vips13un.kinoportal.live! Здесь представлена огромная коллекция достойных фильмов. Вас точно порадует качество видео. На странице вы увидите жанр, год выхода фильма и его длительность, а также страну. Новинки постоянно добавляем. У нас всегда есть что посмотреть. Ищете онлайн фильмы хорошего качества смотреть бесплатно новинки? Vips13un.kinoportal.live – ресурс, который организован на все 100%. Здесь имеется удобный плеер и поисковик. Вы обязательно для себя что-то найдете. Пару кликов и вы сможете посмотреть качественный фильм. KinoPortal ждет именно вас!
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании в столице.
ast-diplom.com/kupit-diplom-nizhnij-novgorod
Добрый день!
Приобрести документ о получении высшего образования вы сможете у нас в Москве.
diplomyx24.ru/kupit-diplom-ekaterinbur
Хорошей учебы!
[u][b] Привет, друзья![/b][/u]
Заказать документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, в том числе документы старого образца.
[url=http://teplichnaya.ru/viewtopic.php?f=18&t=641852/]teplichnaya.ru/viewtopic.php?f=18&t=641852[/url]
[url=http://testforum.1stbb.ru/viewtopic.php?f=3&t=435/]testforum.1stbb.ru/viewtopic.php?f=3&t=435[/url]
[url=http://funchange.getbb.ru/viewtopic.php?f=8&t=1388/]funchange.getbb.ru/viewtopic.php?f=8&t=1388[/url]
[url=http://mindclub.online/wiki/index.php/Купите_диплом_и_улучшите_свое_будущее/]mindclub.online/wiki/index.php/Купите_диплом_и_улучшите_свое_будущее[/url]
[url=http://itisenglish.maxbb.ru/viewtopic.php?f=7&t=1069/]itisenglish.maxbb.ru/viewtopic.php?f=7&t=1069[/url]
Привет!
Полезная информация как купить диплом о высшем образовании без рисков
http://www.con-tacto.vip/blogs/50/На-что-именно-внимание-обратить-при-заказе-документов-в-интернете
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
ast-diploms.com/kupit-diplom-omsk
Привет!
Приобрести документ о получении высшего образования вы сможете у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить необходимый диплом по любым специальностям, включая документы образца СССР.
myfootballday.ru/zakazhite-diplom-pryamo-seychas-i-nachnite-novuyu-kareru
daddycow.com/blogs/view/24730www.mirmafii.ru/article/7570
wallazz.com/blogs/206461/Официальный-диплом-без-экзаменов
dachaweek.ru/legalnyiy-diplom-bez-lishnih-hlopot-uznayte-kak
konstruktiv.getbb.ru/viewtopic.php?f=17&t=6744
Здравствуйте!
Мы предлагаем документы ВУЗов, которые расположены на территории всей РФ. Вы сможете приобрести диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы печатаются на бумаге высшего качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригиналов. Документы будут заверены необходимыми печатями и подписями.
http://www.dentalnursenetwork.com/cb-profile/pluginclass/cbblogs.html?action=blogs&func=show&id=158
Привет!
Мы предлагаем документы техникумов, которые находятся на территории всей Российской Федерации. Вы сможете приобрести качественно напечатанный диплом за любой год, указав актуальную специальность и оценки за все дисциплины. Документы делаются на бумаге самого высокого качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Документы будут заверены всеми требуемыми печатями и штампами.
kingasteroid.com/blogs/285/%D0%91%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-Russian-Diplom
Привет, друзья!
Где заказать диплом специалиста?
profit.hutt.live/viewtopic.php?id=1977#p4276
Успехов в учебе!
Привет, друзья!
Как оказалось, купить диплом кандидата наук не так уж и сложно
landik-diploms-srednee.ru/diplom-s-reestromkupit-kupit
Привет, друзья!
Где купить диплом специалиста?
Купить диплом университета.
rebornrpofficial.com/index.php?/files/file/9-обширный-каталог-документов-в-знаменитом-интернет-магазине/
Привет!
Купить документ о получении высшего образования вы сможете у нас.
ast-diplomas.com/otzyvy
Хорошей учебы!
Привет, друзья!
Мы предлагаем документы ВУЗов, которые находятся на территории всей Российской Федерации. Можно приобрести диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригиналов. Документы будут заверены необходимыми печатями и подписями.
igpsclub.ru/social/read-blog/5482
Привет!
Легальная покупка диплома ПТУ с сокращенной программой обучения
landik-diploms-srednee.ru/svidetelstvo-o-razvode
Привет, друзья!
Где купить диплом специалиста?
Мы предлагаем документы институтов, расположенных в любом регионе РФ. Можно приобрести качественно сделанный диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Документы будут заверены всеми требуемыми печатями и подписями.
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по доступным ценам.
ast-diplomy24.ru/kupit-diplom-omsk
Рады оказать помощь!
Привет!
Мы предлагаем приобрести диплом в отличном качестве, который не отличить от оригинала без участия специалиста высокой квалификации со сложным оборудованием.
http://www.alpea.ru/forum/user/25727/
Удачи!
Привет, друзья!
Приобрести документ университета можно у нас в столице. Мы предлагаем документы об окончании любых ВУЗов РФ.
forum.stpku.ru/viewtopic.php?f=2&t=49716
legislador.art.br/forum/viewtopic.php?p=101253#p101253
авто-днр.рф/users/uxaxuzi
карачаевский-район.рф/forum/forum1/topic1/
m9-com.ru/forums/viewtopic.php?f=21&t=23002&p=319383#p319383
лучшее порно видео онлайн бесплатно лучшее порно видео онлайн бесплатно .
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
club.sabaylok.com/blogs/4757/Как-приобрести-сейчас-качественный-диплом-в-интернете
Convenience: Play from the comfort of your home or on the go.
buy ivermectin
Привет, друзья!
Как получить диплом о среднем образовании в Москве и других городах
amtest.mybb.ru/post.php?action=post&fid=1
Окажем помощь!
Добрый день!
Купить диплом магистра оказалось возможно, быстрое обучение и диплом на руки
arusak-diploms-srednee.ru/kupit-diplom-sssr
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
last news about raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
Привет, друзья!
Купить документ о получении высшего образования можно в нашей компании в столице.
ast-diplomas.com/kupit-diplom-omsk
Привет, друзья!
Как избежать рисков при покупке диплома колледжа или ВУЗа в России
mirfinrealty.ru/vash-diplom-bez-truda-i-usiliy
Рады оказаться полезными!
Привет!
Где заказать диплом специалиста?
Купить диплом о высшем образовании.
wiki.starfederation.ru/index.php?title=Большой_каталог_документов_в_популярном_онлайн_магазине
Здравствуйте!
Где заказать диплом специалиста?
mastergrad.getbb.ru/viewtopic.php?f=12&t=2281
Хорошей учебы!
Здравствуйте!
Купить документ университета вы имеете возможность у нас в столице.
ast-diplomas.com/kupit-diplom-rostov-na-donu
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
last news about cristiano ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
firmino
firmino
firmino
firmino
<a href=http://hoganartgarage.ahovey.est-online.hut2.ru/test.php?a%5B%5D=firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
last news about firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
Добрый день!
Где купить диплом специалиста?
Заказать диплом любого университета.
beinsadouno.bg/events/event/40-обширный-каталог-документов-в-известном-онлайн-магазине/
Добрый день!
Заказать диплом о высшем образовании
Наша компания предлагает максимально быстро приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Данный документ пройдет любые проверки, даже при использовании специального оборудования. Достигайте цели максимально быстро с нашей компанией.
Где заказать диплом по актуальной специальности?
mosday.getbb.ru/viewtopic.php?f=12&t=1059
volnodumie.bbmy.ru/viewtopic.php?id=12332#p25047
volnodumie.bbmy.ru/viewtopic.php?id=12332#p25047
alik.forumrpg.ru/viewtopic.php?id=6639#p275762
3drus.ru/forum/topic_34806
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
last musialanews here!
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
Здравствуйте!
Полезные советы по безопасной покупке диплома о высшем образовании
ashinova.ru/category-5/t-1709.html#1709
Окажем помощь!
Привет!
Заказать документ ВУЗа вы можете в нашей компании в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов РФ. Вы получите необходимый диплом по любой специальности, включая документы образца СССР.
miku-crdb.ru/forum/messages/forum1/topic348/message377/?result=new#message377
aviapoisk.getbb.ru/posting.php?mode=post&f=27&sid=73456970abc92b67857bf41e8828bc35
ремонт-оптом.рф/club/user/17/blog/
http://www.4yo.us/blogs/142798/Гарантированное-получение-диплома-без-риска-и-проблем
openmotonews.ru/oformlenie-diplomov-s-garantiey-kachestva
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
last info about becker
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
Привет!
Мы можем предложить дипломы любой профессии по выгодным тарифам.
http://www.humansandslaves.ru/blogs/656/Какие-онлайн-магазины-с-дипломами-на-сегодняшний-день-есть
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
last news about marcus wendel!
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
last news about lewandowski
lewandowski
lewandowski
lewandowski
<a href=http://am.h10.ru/test.php?a%5B%5D=lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
Здравствуйте!
Где заказать диплом по необходимой специальности?
Купить диплом о высшем образовании.
epiphyte-club.ru/index.php?/gallery/image/115-как-подыскать-надежный-онлайн-магазин-с-огромным-выбором-дипломов/
Привет!
Мы предлагаем приобрести диплом в отличном качестве, неотличимый от оригинального документа без участия специалистов высокой квалификации со сложным оборудованием.
rf-lowrate.ru/index.php?/topic/4832-купить-диплом-o814i/
Успешной учебы!
Привет, друзья!
Где приобрести диплом по нужной специальности?
Мы можем предложить документы институтов, которые находятся в любом регионе России. Вы сможете заказать качественно напечатанный диплом от любого ВУЗа, за любой год, включая документы старого образца СССР. Дипломы выпускаются на бумаге высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и штампами.
Мы изготавливаем дипломы любой профессии по приятным тарифам.
diploms-x24.ru/kupit-diplom-rostov-na-donu
Всегда вам поможем!
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
last news about messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
In addition to the obvious advantages in a decorative sense, there are other advantages stroynews.info
Здравствуйте!
Мы можем предложить дипломы любой профессии по приятным ценам.
shabab.galaxy.ps/купить-диплом-новосибирск/
Здравствуйте!
Мы предлагаем дипломы любой профессии по приятным ценам. Цена будет зависеть от той или иной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас важно, чтобы дипломы были доступными для подавляющей массы граждан.
bookmarksaifi.com/story17087420/где-купить-диплом
Привет, друзья!
Заказать документ о получении высшего образования вы имеете возможность в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ.
http://www.senbernar.ru/profile/11151-awyxemyf/
http://www.simsonviglu.cz/phpBB/phpBB3/viewtopic.php?f=1&t=32846
shinyoungwood.co.kr/bbs/board.php?bo_table=free&wr_id=764588
http://www.receptar.ru/forum/profile.php?action=show&member=1539
чпуремонт.рф/showthread.php?tid=46085
Привет, друзья!
Приобрести документ ВУЗа вы можете у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы СССР. Гарантируем, что в случае проверки документа работодателем, подозрений не появится.
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по невысоким ценам. Цена зависит от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную ценовую политику. Для нас важно, чтобы документы были доступны для большого количества наших граждан.
kopoluzhona.image-perth.org/bystro-priobretaem-diplom-v-lucsem-magazine-russian-diplom/
Поможем вам всегда!
Здравствуйте!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske
navigate to these guys coinomi
Здравствуйте!
Мы готовы предложить дипломы любой профессии по приятным тарифам.
rebornrpofficial.com/index.php?/files/file/12-четыре-главных-группы-онлайн-магазинов-реализующих-документы/
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
last news about kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
Здравствуйте!
Мы предлагаем выгодно купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Документ способен пройти любые проверки, даже при помощи специально предназначенного оборудования. Решайте свои задачи максимально быстро с нашими дипломами.
d992387h.bget.ru/index.php?subaction=userinfo&user=ohuhux
Успехов в учебе!
На сайте https://stendy-razvalshozhdenia.ru вы изучите всю важную и ценную информацию о том, как правильно подобрать стенд развал-схождение, который используется в автосервисе. Вы узнаете о том, что вообще представляет собой такое устройство и чем оно примечательно. Рассматриваются виды стендов, а также нюансы оптических стендов. Дается информация о компьютерных стендах. Вы будете в курсе того, какие особенности есть у 3D стендов. Возможно, вам будут нужны инфракрасные стенды. Даны важные советы и рекомендации о том, как правильно подобрать качественное оборудование.
Привет!
Заказать документ о получении высшего образования можно в нашей компании в Москве.
ast-diplomas.com/kupit-diplom-o-srednem-obrazovanii
Удачи!
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes last news
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы сможете получить диплом по любым специальностям, любого года выпуска, в том числе документы старого образца.
wiki.hightgames.ru/index.php/Быстрая_покупка_дипломов_онлайн
wegug.in/blogs/1120/Легальный-диплом-без-лишних-хлопот-узнайте-как
cv53297-livestreet-1.tw1.ru/2024/07/16/osuschestvite-mechtu-poluchite-diplom-bystro-i-bez-problem.html
beijingpal.com/read-blog/940
fotomaniya.getbb.ru/ucp.php?mode=login&sid=6c7e2a6a489f8962dfaecc32dc9b5adf
Добрый день!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
ekra.kz/index.php?subaction=userinfo&user=oducafyby
Рады помочь!.
tronlink extension – tron link, tron wallet chrome
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
last news about khvicha kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
Привет, друзья!
Приобрести документ университета можно у нас.
ast-diplomy.com/kupit-diplom-rostov-na-donu
Удачи!
Привет!
Купить документ института можно в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, включая документы старого образца.
webyourself.eu/blogs/391030/Получите-диплом-без-лишних-забот-и-усилий
forexsnews.ru/oformlenie-diploma-bez-lishnih-voprosov
zoofortunakz.5nx.ru/viewtopic.php?f=96&t=4578
roseninsel.kz/forum/topic/add/forum7/
almet.listbb.ru/viewtopic.php?f=12&t=414
The user interface of the Aviator Game is designed to be intuitive and user-friendly. The clean design and easy
ivermectin purchase
Привет!
Официальная покупка диплома вуза с упрощенной программой обучения
newsato.ru/ofitsialnyiy-diplom-bez-lishnih-hlopot
Рады оказаться полезными!
рамки для дипломов купить https://www.diploms-x.com .
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
last news about firmino roberto
firmino
firmino
firmino
firmino>firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
Добрый день!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
http://www.liobio.com/blogs/1588/Рекомендации-по-приобретению-документа-в-сети-интернет
Привет!
Заказать документ университета вы сможете у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите диплом по любой специальности, включая документы СССР. Даем гарантию, что при проверке документа работодателями, каких-либо подозрений не появится.
http://www.ksolo.ru/forum/member.php?u=83595
http://www.mobime.ru/forum/forum17.html
wiki.hightgames.ru/index.php/Четыре_основных_группы_онлайн_магазинов,_которые_продают_документы
http://www.hip-hop.ru/forum/id298234-worksale
igtusimh0.widblog.com/83255582/Как-подобрать-проверенный-магазин-с-дипломами-Обзор-эксперта
купить диплом ликвидированного вуза ast-diploms.com .
Здравствуйте!
Мы можем предложить дипломы любой профессии по приятным тарифам.
appleincub.ru/page/2
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
last news about mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
Добрый день!
Заказать документ ВУЗа можно у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любым специальностям, включая документы старого образца.
newfinbiz.ru/uspeh-bez-usiliy-poluchite-diplom-uzhe-segodnya
nec.phorum.pl/posting.php?mode=newtopic&f=27&sid=b2f29f05baa9cc27a425541815d79979
afterpad.com/forums/post.php?fid=7
ilovehabbo.bbon.ru/viewtopic.php?id=1569#p28987
vseogirls.ru/osushhestvite-mechtu-poluchite-diplom-byistro-i-bez-problem
Добрый день!
Мы готовы предложить документы техникумов, расположенных в любом регионе РФ. Вы имеете возможность заказать качественный диплом от любого заведения, за любой год, включая сюда документы старого образца СССР. Документы печатаются на “правильной” бумаге самого высокого качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и штампами.
interactor.pro/read-blog/1360
Добрый день!
Заказать документ института можно у нас в столице.
asxdiplomik.com/kupit-diplom-omsk
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по выгодным тарифам. Стоимость может зависеть от выбранной специальности, года получения и университета. Всегда стараемся поддерживать для клиентов адекватную политику тарифов. Для нас важно, чтобы дипломы были доступными для большого количества граждан.
throbsocial.com/story18809486/купить-настоящий-диплом-о-высшем-образовании
Здравствуйте!
Заказать документ о получении высшего образования вы можете в нашей компании. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы СССР. Даем гарантию, что при проверке документа работодателем, каких-либо подозрений не появится.
Мы можем предложить дипломы любой профессии по выгодным тарифам. Стоимость может зависеть от выбранной специальности, года получения и университета. Стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы документы были доступны для большого количества граждан.
nfrb.pl/index.php?/gallery/image/57-низкие-расценки-и-высокое-качество-дипломы-онлайн/
Всегда вам поможем!
Добрый день!
Где заказать диплом специалиста?
Мы готовы предложить документы ВУЗов, которые расположены в любом регионе РФ. Вы сможете купить диплом от любого заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы выпускаются на бумаге высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригинала. Документы заверяются необходимыми печатями и подписями.
Мы можем предложить дипломы любой профессии по выгодным ценам.
diploms-x24.ru/kupit-diplom-sankt-peterburg
Окажем помощь!
Здравствуйте!
Наш сервис предлагает заказать диплом в высочайшем качестве, неотличимый от оригинального документа без использования специального оборудования и квалифицированного специалиста.
zhabbo.free.fr/index.php?file=Members&op=detail&autor=ezybusa
Успехов в учебе!
купить диплом управление персоналом diplomasx.com .
Добрый день!
Заказать документ о получении высшего образования вы можете в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов России.
gektor.biz/forum/?PAGE_NAME=profile_view&UID=181116
polimer42.ru/communication/forum/messages/forum5/topic49/message349198/?result=reply#message349198
gpp.innim.ru:81/forums/topic/3579/diplomandoci/view/post_id/3596
arskland.ru/people/user/15810/
forum.home-visa.ru/viewtopic.php?f=69&t=1211678
Insightful read! I found your perspective very engaging. For more information, visit: READ MORE. Eager to see what others have to say!
Привет, друзья!
Мы готовы предложить документы ВУЗов, которые расположены в любом регионе РФ. Вы можете заказать качественно напечатанный диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Документы будут заверены необходимыми печатями и подписями.
entrastart.com//read-blog/49
[u][b] Привет, друзья![/b][/u]
[b]Приобрести диплом любого университета.[/b]
[url=http://webmentes.com/read-blog/179/]webmentes.com/read-blog/179[/url]
Привет, друзья!
Всё, что нужно знать о покупке аттестата о среднем образовании
noctuagg.ro/forum/index.php?/gallery/image/28-4-е-главных-группы-онлайн-магазинов-которые-реализуют-дипломы/
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
last news about foden here!
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
Привет!
Наша компания предлагает выгодно и быстро купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Диплом пройдет лубую проверку, даже с применением специально предназначенного оборудования. Решайте свои задачи максимально быстро с нашим сервисом.
freelance.habr.com/freelancers/dilopluyy
Успехов в учебе!
Привет!
Мы предлагаем дипломы любой профессии по выгодным ценам.
testsajtet.net/read-blog/211_planiruete-priobresti-diplom-u-nadezhnogo-proizvoditelya-zahodite.html
Здравствуйте!
Мы предлагаем документы техникумов, которые находятся на территории всей РФ. Вы сможете купить диплом от любого заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, которые невозможно отличить от оригиналов. Они будут заверены необходимыми печатями и подписями.
menaharia.com/read-blog/2713
Привет, друзья!
Приобрести документ института можно в нашей компании в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы Советского Союза.
ya.bestbb.ru/viewtopic.php?id=3008#p6640
fforum.ixbb.ru/viewtopic.php?id=191#p4069
wiki.mdomtv.net/index.php?title=Диплом_под_ключ:_качественно_и_безопасно
datasphere.ru/club/user/15/blog/
sec31.ru/viewtopic.php?f=25&t=673861
Привет, друзья!
Узнайте, как приобрести диплом о высшем образовании без рисков
landik-diploms-srednee.ru/diplom-bakalavra
Ищете качественную мебель для офиса? Рекомендую обратить внимание на мебель для офиса замм. Этот бренд предлагает широкий ассортимент офисной мебели, включая стильные и функциональные офисные столы. Продукция замм отличается высоким качеством, долговечностью и современным дизайном. Идеально подходит для создания комфортного и продуктивного рабочего пространства. В ассортименте вы найдете всё, что нужно для организации современного офиса. Отличный выбор для тех, кто ценит надежность и стиль! С уважением, Zamm мебель.
Здравствуйте!
Заказать диплом о высшем образовании.
samara.listbb.ru/viewtopic.php?f=3&t=277
Успешной учебы!
Здравствуйте!
Как приобрести диплом техникума с минимальными рисками.
Приобрести диплом о высшем образовании.
cittaviva.net/read-blog/59
Виртуальные карточные и настольные игры также ждут своих поклонников. От блэкджека до покера – испытайте удачу и стратегию https://total-rating.ru/2393-revizionnye-lyuki-skrytye-pod-plitkoy-sovremennye-resheniya-i-tendencii.html
Срочно Требуются: Курьеры-регистраторы
Ищем активных граждан РФ, живущих в Москве и области!
А так же, принимаются люди, для работы, проживающие в других регионах рф,
кроме (северного Кавказа)
Заработок от 3000 тыс. до 7000 тыс. за каждый выезд.
Совмещай работу с другими делами – гибкий график!
Твоя задача – регистрация компаний. Просто и выгодно!
Оплата сразу после выполнения задания!
Подходишь по возрасту (18-60 лет)Присоединяйся!
Начни зарабатывать больше прямо сейчас – ждем именно тебя!
А так же, требуются люди, на удаленную работу, по поиску и подбору
директоров (Курьеров-регистраторов) зп, от 5000 тысяч рублей, за подобранного человека.
#работа #вакансия #Москва #курьер #регистратор #заработок #график #подработка
Начни зарабатывать больше прямо сейчас – ждем именно тебя!
https://chat.whatsapp.com/InLwqrVeXucCbCTqxkwrSo
Привет, друзья!
Полезная информация как официально купить диплом о высшем образовании
arusak-diploms-srednee.ru
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
dervislergrup.com/events/event/9-pocemu-segodnya-gorazdo-desevle-budet-zakazat-diplom-universiteta/
В Vavada казино промокоды дают возможность получить дополнительные бонусы для любимых игр. Используйте их, чтобы увеличить свои шансы на выигрыш и наслаждаться процессом.
купить аттестат о среднем образовании в москве ast-diploms.com .
Промокоды Drip казино помогают получить уникальные бонусы, что делает игровой процесс более интересным и увлекательным.
Привет, друзья!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
sportandpolitics.ukrbb.net/viewtopic.php?f=24&t=13633
Всегда вам поможем!.
Привет!
Купить документ университета вы имеете возможность в нашей компании в столице.
ast-diplomy.com/kupit-diplom-novosibirsk
Привет, друзья!
Заказать документ ВУЗа вы имеете возможность в нашей компании в столице.
ast-diplom24.ru/kupit-diplom-o-srednem-obrazovanii
Хорошей учебы!
Здравствуйте!
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по разумным тарифам. Цена зависит от определенной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большого количества граждан.
bookmarkunit.com/story16981566/купить-диплом-техникума
Привет, друзья!
Заказать документ университета вы сможете у нас в столице. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любой специальности, любого года выпуска, в том числе документы старого образца. Гарантируем, что при проверке документов работодателями, подозрений не возникнет.
Мы можем предложить дипломы любой профессии по доступным тарифам. Стоимость может зависеть от выбранной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы дипломы были доступны для подавляющей массы наших граждан.
facefam.com/read-blog/334_legko-pokupaem-diplom-v-luchshem-internet-magazine-russian-diplom.html?mode=day
Будем рады вам помочь!
Здравствуйте!
Где купить диплом специалиста?
Заказать диплом о высшем образовании.
c99596qr.beget.tech/2024/07/04/kak-podyskat-nadezhnyy-onlayn-magazin-s-obshirnym-vyborom-diplomov.html
Добрый день!
Приобрести диплом ВУЗа.
ремонт-оптом.рф/club/user/7/blog/2119/
Промокоды Vavada казино предоставляют эксклюзивные бонусы для всех игроков, улучшая их шансы на выигрыш и делая игру более увлекательной.
Привет, друзья!
Диплом вуза купить официально с упрощенным обучением в Москве
pesnibardov.ru/f/viewtopic.php?f=2&t=209290
Поможем вам всегда!
купить диплом о высшем образовании в твери купить диплом о высшем образовании в твери .
How to Start Playing the Aviator Game?
ivermectin purchase online
Здравствуйте!
Где заказать диплом специалиста?
Приобрести диплом любого ВУЗа.
larashare.net/events/event/42-широкий-ассортимент-документов-в-знаменитом-магазине/
Добрый день!
Как безопасно купить диплом колледжа или ВУЗа в России, что важно знать.
Купить диплом о высшем образовании.
s-contact.online/blogs/35/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Добрый день!
Купить документ университета можно в нашей компании в Москве.
ast-diplom.com/kupit-diplom-chelyabinsk
Привет!
Мы готовы предложить дипломы любой профессии по разумным ценам.
thesocialmusic.co.uk/blogs/7228/Как-приобрести-сегодня-неотличимый-от-подлинника-диплом-в-интернете
Привет!
Наша компания предлагает выгодно купить диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Данный диплом способен пройти любые проверки, даже с применением профессиональных приборов. Достигайте своих целей быстро и просто с нашим сервисом.
pokupki.bestforums.org/viewtopic.php?f=30&t=17800&p=28558#p28558
Успехов в учебе!
Привет, друзья!
Приобрести документ ВУЗа вы можете в нашей компании. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы Советского Союза.
allnewstroy.ru/byistroe-oformlenie-diploma-lyuboy-spetsialnosti
delta72.at.ua/forum/61-26766-1
amurskij-dachnik.ru/forum/user/59705/
darknews.ru/diplom-na-zakaz-kachestvo-i-nadezhnost
finttech.ru/legkiy-put-k-diplomirovannomu-uspehu-byistro-i-nadezhno
Добрый день!
Купить диплом о высшем образовании.
coastalplainplants.org/wiki/index.php/???????_??_?????:_??????,_???????????,_???????????????
Удачи!
Добрый день!
Где приобрести диплом специалиста?
Приобрести диплом университета.
testforum.1stbb.ru/viewtopic.php?f=3&t=431
Добрый день!
Мы готовы предложить документы ВУЗов, расположенных в любом регионе России. Можно заказать качественный диплом от любого учебного заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высшего качества. Это дает возможности делать государственные дипломы, которые не отличить от оригиналов. Документы заверяются всеми необходимыми печатями и подписями.
c90226sl.beget.tech/2024/07/09/pokupaem-dokumenty-v-proverennom-magazine-po-vygodnoj-stoimosti/
Добрый день!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
afterpad.com/forums/post.php?fid=7
Поможем вам всегда!
Привет, друзья!
Где приобрести диплом по нужной специальности?
Приобрести диплом любого ВУЗа.
o91746bp.beget.tech/2024/07/04/ogromnyy-katalog-dokumentov-v-populyarnom-onlayn-magazine.html
Здравствуйте!
Приобрести документ о получении высшего образования вы сможете в нашей компании.
ast-diploms.com/kupit-diplom-s-registraciej
Привет!
Мы можем предложить дипломы любой профессии по разумным тарифам.
newsbig.fotosdefrases.com/rekomendacii-po-priobreteniu-dokumenta-v-internete
купить диплом бакалавра в красноярске asxdiplomik24.ru .
Добрый день!
Как избежать рисков при покупке диплома колледжа или ПТУ в России
owen.ru/forum/member.php?u=151770&vmid=6624#vmessage6624
Будем рады вам помочь!.
Привет!
Приобрести документ о получении высшего образования вы можете у нас.
asxdiplomik24.ru/kupit-diplom-sankt-peterburg
Удачи!
Привет!
Мы можем предложить дипломы любой профессии по приятным ценам.
thesn.eu/blogs/2871/Ценные-советы-по-приобретению-документа-в-сети-интернет
Привет!
Купить документ университета вы сможете в нашем сервисе.
ast-diplom24.ru/kupit-diplom-omsk
Удачи!
Привет!
Купить документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов России. Вы сможете получить диплом по любой специальности, любого года выпуска, включая документы образца СССР.
pokemon-go.onl/users/6146
http://www.4x4zubry.by/forum/messages/forum1/topic2051/message202283/?result=new#message202283
ballinthe6.ca/blogs/16327/Быстрое-оформление-диплома-любой-специальности
u90517ol.beget.tech/2024/07/11/kupite-diplom-i-zabudte-o-studencheskih-problemah.html
iaescortsmap.ixbb.ru/viewtopic.php?id=108#p108
можно ли купить диплом о высшем можно ли купить диплом о высшем .
Привет, друзья!
Где купить диплом по актуальной специальности?
Приобрести диплом о высшем образовании.
indicouple.com/blogs/1164/Ваш-диплом-без-лишних-забот-быстро-и-безопасно
Как официально купить диплом вуза с упрощенным обучением в Москве
diplomyx.com/kupit-diplom-rostov-na-donu
Здравствуйте!
Как избежать рисков при покупке диплома колледжа или ПТУ в России
autoschool-progress.kz/index.php?subaction=userinfo&user=usefizaq
Будем рады вам помочь!.
Привет, друзья!
Приобрести документ о получении высшего образования вы можете в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любой специальности, включая документы старого образца.
ilovehabbo.bbon.ru/viewtopic.php?id=1570#p28988
l4dzone.com/viewtopic.php?t=241967
allseoreg.wordpress.com/2024/07/15/быстрое-оформление-диплома-любой-сте/
rodina.listbb.ru/viewtopic.php?f=3&t=635
u90517ol.beget.tech/2024/07/12/vysshee-obrazovanie-bez-usiliy.html
Привет, друзья!
Купить документ о получении высшего образования вы можете в нашей компании в столице.
diplomyx24.ru/kupit-diplom-krasnoyarsk
Удачи!
Привет!
Заказать диплом любого университета.
http://www.hashtap.com/@artur.sh/купить-диплом-легкий-процесс-заказа-WNML20J4Degd
Добрый день!
Мы изготавливаем дипломы любой профессии.
http://www.2dommedical.com/2024/07/14/купить-заочный-диплом/
Рады оказаться полезными!.
срочный ремонт смартфонов
На сайте https://koleso-na-hodu.ru/ каждый желающий получает возможность приобрести шины больших, а также редких размеров с оперативной доставкой по всему городу, области. Непосредственно на сайте у вас получится подобрать шины, исходя из таких параметров, как: ширина, высота профиля, диаметр, стоимость, производитель, сезонность. Вся продукция сертифицированная, качественная, оригинальная. Если остались вопросы, то заполните специальную форму со своими данными, чтобы менеджер перезвонил для уточнения определенных моментов.
Привет, друзья!
Где приобрести диплом по необходимой специальности?
ekonty.com/blogs/view/58699
Earn money from sports!
Tired of the routine work and the search for additional income? Then our site is just for you!
Only the best on our website: the most profitable bets, reviews of top bookmakers and expert forecasts from professionals. Earn on your knowledge and experience in sports!
Come in and start your journey to financial freedom today! – https://vkltv.top/bookmaker/melbet/
Привет, друзья!
Как правильно купить диплом колледжа и пту в России, подводные камни
gracebook.app/blogs/1187/На-что-именно-обращать-внимание-при-покупки-диплома-в-сети
Baji Live Casino offers a dynamic and immersive gaming experience with a wide range of games, exciting bonuses, and a user-friendly interface that caters to both novice and seasoned players baji-999.org
как отличить поддельный диплом asxdiplomik24.ru .
Привет, друзья!
Купить диплом о высшем образовании.
rf-unicron.ru/index.php?/gallery/image/115-обширный-выбор-документов-в-популярном-онлайн-магазине/
Добрый день!
Мы можем предложить дипломы любых профессий по выгодным ценам.
orangekitchendecor.all-new.info/купить-диплом-в-артеме/
Здравствуйте!
Заказать документ ВУЗа.
cyberpinoy.net/read-blog/35444
fsmi.wiki/index.php?title=Получите_диплом_в_кратчайшие_сроки
dachkanews.ru/garantirovannoe-poluchenie-diploma-bez-riska-i-problem/
anoreksja.org.pl/viewtopic.php?f=13&t=1247405
connectme.live/blogs/1024/Дипломы-на-заказ-быстро-и-легко
Добрый день!
Мы готовы предложить документы ВУЗов, расположенных в любом регионе Российской Федерации. Можно заказать диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригиналов. Они будут заверены всеми необходимыми печатями и подписями.
na1md7lqs.blogerus.com/50976638/%D0%9F%D0%BE%D0%B4%D1%80%D0%BE%D0%B1%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
купить диплом о среднем образовании в липецке diploms-x.com .
reputable online platforms that ensure safety and fair play.
where to buy ivermectin
tzona.org
Привет!
Диплом ВУЗа купить официально с упрощенным обучением в Москве
molbiol.ru/forums/index.php?showtopic=1235739
Окажем помощь!
Привет, друзья!
Купить диплом о высшем образовании.
imhht.com/index.php?title=Как_подобрать_надежный_онлайн_магазин_с_большим_выбором_дипломов?
Привет, друзья!
Заказать документ университета.
wallazz.com/blogs/206446/Быстрое-оформление-диплома-любой-специальности
korrespondentweek.ru/poluchite-diplom-o-kotorom-vsegda-mechtali/
nadegda.listbb.ru/viewtopic.php?f=3&t=409
kurgetrp.listbb.ru/viewtopic.php?f=11&t=456
linkthere.club/read-blog/8701
visite site https://myjaxxwallet.us
https://sale-cloned-cards.cvv2cvc.net
Item 1 Card Total Balance: $3100 – Price $ 110.00
Item 3 Cards Total Balance $9600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $ 2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
https://sale-clonedcards.cvv2cvc.net
Store Credit cards
Привет!
Мы предлагаем документы техникумов, которые находятся на территории всей РФ. Можно купить качественно сделанный диплом от любого заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Документы делаются на бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, которые не отличить от оригинала. Документы заверяются необходимыми печатями и подписями.
savico.com.br/read-blog/257
Добрый день!
Заказать диплом о высшем образовании.
autoplus74.com/club/user/170/blog/373/
Здравствуйте!
Мы изготавливаем дипломы любой профессии.
andreieusebiu.net/files/file/43-зачем-сегодня-заказывают-аттестаты-и-дипломы-в-сети-интернет/
Всегда вам поможем!.
go now https://my-jaxxwallet.io/
Привет, друзья!
Приобрести документ института.
school8kaluga.flybb.ru/viewtopic.php?f=19&t=500
silkhunter.com/index.php?title=Дипломы,_признанные_работодателями
or1gano.80lvl.ru/viewtopic.php?f=10&t=1027
films.name/viewforum.php?f=143
sllife.ru/social/user/4216/forum/message/2439/7151/#message7151
купить диплом 1999 года выпуска diploms-x.com .
Добрый день!
Где заказать диплом специалиста?
spbmedu.ru/
Привет, друзья!
Купить документ университета можно в нашей компании.
asxdiplomik24.ru/kupit-diplom-bakalavra-ili-specialista
Добрый день!
Купить документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых университетов России.
wikirace.ru/index.php?title=russianydiplomix
http://www.altasugar.it/new/index.php?option=com_kunena&view=topic&catid=2&id=87978&Itemid=151
193.16.101.6/index.php?title=landsdiplomy
classicalmusicmp3freedownload.com/ja/index.php?title=diplomandoci
webmontag.de/doku.php?id=landsdiplomy
Привет, друзья!
Приобретение школьного аттестата с официальным упрощенным обучением в Москве
aboutallfinance.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
Рады помочь!
лучшее онлайн казино в казахстане казино с моментальным выводом отзывы топ 10 онлайн казино на деньги в какой игре самый большой онлайн букмекерские конторы с бесплатной первой ставкой играть в казино pin-up скачать игровые автоматы на андроид без интернета игровые автоматы играть бесплатно и без регистрации онлайн игровые автоматы онлайн в казахстане pin up зеркало на сегодня игр автоматы вулкан играть бесплатно лучшие игры на андроид для детей 10 лет мостбет. зеркало. на. сегодня. игровые автоматы играть бесплатно без регистрации онлайн pin up официальный сайт скачать играть в новые игровые автоматы пин ап казино зеркало сегодня топ казино на реальные деньги pokerdom скачать на андроид на реальные бк 1хбет букмекерская контора официальный сайт
Привет!
Заказать документ университета вы сможете в нашей компании в Москве.
ast-diplomas.com/kupit-diplom-chelyabinsk
Привет, друзья!
Как купить диплом о высшем образовании с минимальными рисками.
Купить диплом о высшем образовании.
owen.ru/forum/album.php?albumid=218&attachmentid=77155&commentid=2439
Привет, друзья!
Официальное получение диплома техникума с упрощенным обучением в Москве
myanimalgram.com/read-blog/356
Окажем помощь!
Добрый день!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
paul-services.co.uk/купить-диплом-в-канске/
Здравствуйте!
Мы предлагаем дипломы любой профессии.
datafornix.com/куплю-диплом-вуза-будут/
Всегда вам поможем!.
Добрый день!
Приобрести документ института вы сможете у нас.
diplomasx.com/kupit-diplom-perm
Привет!
Мы можем предложить дипломы любой профессии по доступным ценам.
azat.on.kg/blogs/893/ѕолучите-ќфициальный-?иплом-в- ратчайшие-—роки
самое лучшее порево http://www.besplatny-sex-online.ru .
Добрый день!
Заказать документ о получении высшего образования можно у нас в Москве. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы СССР. Гарантируем, что при проверке документов работодателем, каких-либо подозрений не появится.
wiki.gta-zona.ru/index.php/4_основных_группы_онлайн-магазинов,_которые_реализуют_документы
http://www.lada-xray.net/member.php?u=2434
sensemi.getbb.ru/viewtopic.php?f=6&t=599
forum.vipcs.pp.ua/gallery/image/316-техническая-поддержка-и-faq-покупаем-документы-в-сети/
nc750.ru/member.php?u=2812
С каждым годом растет количество людей, выбирающих этот вид досуга. Онлайн-платформы предлагают не только развлечение, но и шанс испытать удачу http://portstanc.ru/index.php/blog/ais.html
Привет, друзья!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
caribbeantown.listbb.ru/viewtopic.php?f=5&t=501
Рады оказать помощь!
На сайте https://balansirovochnye-stanki.ru изучите информацию про балансировочный станок. Так вы узнаете про то, какие достоинства у конструкций марки Sivik. Вы сможете ознакомиться с балансировочными станками, которые используются на различных видах машин. Также узнаете и про самые высокотехнологичные методики балансировки колес. На все товары даются гарантии качества. Оборудование является надежным, функциональным и уникальным. Кроме того, отличается безупречными эксплуатационными сроками.
Добрый день!
Заказать документ о получении высшего образования вы имеете возможность у нас в Москве.
diplomyx24.ru/kupit-diplom-nizhnij-novgorod
Успешной учебы!
Добрый день!
Где заказать диплом по актуальной специальности?
mail.vinpr.org/obshestvo/6459-attestat-ob-okonchanii-sredney-shkoly-poluchaem.html
Привет!
Процесс получения диплома стоматолога: реально ли это сделать быстро?
fbadult.com/blogs/2838/Правильно-заказываем-документы-в-интернете-обзор
Здравствуйте!
Заказать диплом университета
Мы предлагаем выгодно и быстро заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями. Наш документ пройдет лубую проверку, даже при помощи специального оборудования. Достигайте своих целей быстро и просто с нашей компанией.
Где купить диплом по необходимой специальности?
zdsim.ru/wiki/index.php/Купить_Диплом_без_Посредников:_Надежно_и_Быстро
wo.linyway.com/read-blog/3247
club.sabaylok.com/blogs/5047/Купить-диплом-Легко-и-Быстро
frank-shkola.ru/forum/messages/forum1/topic435/message448/?result=new#message448
gioturbobp.com/blogs/34/Рекомендации-профессионала-которые-помогут-быстро-купить-диплом
Привет, друзья!
Купить диплом ВУЗа:
realtor-cheb.ru/index.php?subaction=userinfo&user=upydug
u-cars.ru/modules.php?name=Your_Account&op=userinfo&username=anizecin
fond.uni-altai.ru/index.php?subaction=userinfo&user=emeqyp
“cf58051.tmweb.ru/index.php?action=post;topic=2257.0;last_msg=132488”
bts.clanweb.eu/profile.php?lookup=37310
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным тарифам.
axisbd.com/диплом-врача-купить/
https://vskrytiye-zamkov24.ru/
Привет, друзья!
Мы можем предложить дипломы любой профессии по доступным тарифам.
snupto.com/read-blog/3968_vy-hotite-priobresti-diplom-u-proverennogo-proizvoditelya-zahodite.html
Здравствуйте!
Купить документ о получении высшего образования вы можете у нас в Москве.
diplomyx24.ru/kupit-diplom-nizhnij-novgorod
Успехов в учебе!
Place Your Bet: Choose the amount you want to bet.
ivermectin where to buy
Здравствуйте!
Заказать диплом о высшем образовании
Наша компания предлагает быстро и выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями. Наш документ пройдет лубую проверку, даже с применением специальных приборов. Достигайте своих целей максимально быстро с нашей компанией.
Где купить диплом по актуальной специальности?
odessaforum.getbb.ru/viewtopic.php?f=5&t=20402
macadamlab.ru/wiki/index.php?title=пїЅпїЅпїЅпїЅпїЅпїЅ_пїЅпїЅпїЅпїЅпїЅпїЅ
worksale777.blogspot.com/2024/06/blog-post_30.html
lubercy.ixbb.ru/viewtopic.php?id=6615#p14726
seriallove.bbok.ru/viewtopic.php?id=7015#p123048
Нужен качественный ремонт стиральной машины в Москве? Наш сервисный центр предлагает оперативные и профессиональные услуги по сервисы по ремонту стиральных машин в москве. Присоединяйтесь к нашей группе в Telegram и узнайте больше: https://t.me/s/remont_stiralnyh_mashin_moskve
Добрый день!
Мы предлагаем документы техникумов, расположенных в любом регионе России. Вы сможете купить диплом от любого заведения, за любой год, указав актуальную специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты делаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригиналов. Документы заверяются всеми обязательными печатями и штампами.
rebornrpofficial.com/index.php?/files/file/15-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5/
Аттестат школы купить официально с упрощенным обучением в Москве
ast-diploms24.ru/kupit-diplom-voronezh
Привет!
Купить документ о получении высшего образования вы имеете возможность у нас. Мы предлагаем документы об окончании любых университетов России. Вы получите диплом по любым специальностям, включая документы образца СССР. Даем 100% гарантию, что в случае проверки документа работодателями, каких-либо подозрений не возникнет.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным ценам. Цена зависит от определенной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы документы были доступны для большого количества наших граждан.
http://www.webofiice.ro/blogs/1890/Как-можно-быстро-купить-диплом-в-онлайн-магазине
Рады оказать помощь!
Привет, друзья!
Мы предлагаем дипломы любой профессии по доступным тарифам. Стоимость будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику цен. Для нас важно, чтобы документы были доступными для большинства граждан.
kameronkqta46780.wikiexcerpt.com/2813546/Тенденции_приобретения_ученых_степеней_в_современном_мире
Привет, друзья!
Купить документ института можно в нашей компании.
ast-diploms.com/kupit-diplom-magistra
Успехов в учебе!
Привет!
Мы можем предложить дипломы.
boltushka.flybb.ru/viewtopic.php?f=14&t=1489
recomp.bestbb.ru/login.php
abroad.ekafe.ru/viewtopic.php?f=5&t=1944
sakhd.3nx.ru/viewtopic.php?p=2223#2223
the-trifecta-network.mn.co/posts/61899002
Заказать диплом о высшем образовании.
shockmusik.ru/nastoyashhie-diplomyi-dostupno-i-bezopasno
polosedan-club.com/search/search
kalininabad.flyboard.ru/viewtopic.php?f=11&t=2804
severka.flybb.ru/viewtopic.php?f=6&t=363
sensemi.getbb.ru/posting.php?mode=post&f=6&sid=0dbf628d99bf1043096f8867110151d2
Здравствуйте!
Всё, что нужно знать о покупке аттестата о среднем образовании
allsportime.ru/oformite-diplom-onlayn-za-neskolko-minut
Здравствуйте!
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
http://www.bisshogram.com/read-blog/250_ishem-proverennyj-magazin-s-attestatami-i-diplomami.html
Привет!
Приобрести документ о получении высшего образования можно в нашей компании.
diplomasx.com/kupit-diplom-bakalavra-ili-specialista
radioshem.net
Привет, друзья!
Заказать документ института можно в нашем сервисе. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца. Гарантируем, что при проверке документов работодателем, никаких подозрений не возникнет.
fire-team.ru/forum/member.php?u=1143
prikol100500.ru/garantirovannoe-kachestvo-diplomov-legalno-i-byistro
anamaliya.ru/otzyvy/bystryy-poisk-onlayn-magazina-kotoryy-prodaet-diplomy
superforum.spybb.ru/viewtopic.php?id=2722#p50714
ukrevents.ru/nastoyashhie-diplomyi-bez-lishnih-voprosov/
Добрый день!
Заказать диплом любого университета.
leydis16.phorum.pl/posting.php?mode=newtopic&f=1
Успехов в учебе!
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
<a href=http://alumni.oldiestation.es/php.php?a=Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Place your bet at pin up online – authentic prestigious bookmaker in Kazakhstan
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Pin up
Здравствуйте!
Купить диплом любого университета.
app-s.ru/blog/kak_podyskat_nadezhnyj_magazin_s_ogromnym_katalogom_diplomov/2024-07-04-1868
Привет!
Приобрести диплом любого университета:
mkbox.ru/communication/forum/user/73714/
krair.kr/bbs/board.php?bo_table=free&wr_id=315651
prof-aksay.ru/forum/messages/forum2/topic482/message474/?sessid=6344211e4b0d197bf96758faccba6b8a&TOPIC_SUBSCRIBE=Y&FORUM_SUBSCRIBE=Y&result=new
rtpsouth.com/UserProfile/tabid/69/userId/105911/Default.aspx
renebiemans.nl/users.php?m=details&id=32158
Здравствуйте!
Как получить диплом стоматолога быстро и официально.
Заказать диплом университета.
forextema.com/index.php?option=com_easyblog&view=entry&id=10451&Itemid=87
Привет!
Заказать документ университета.
veniaminv.flybb.ru/viewtopic.php?f=1&t=2897
forum.hi-def.ru/index.php?showtopic=38594
demo.advised360.com/read-blog/162165
poetzinc.com/create-blog/
13.flybb.ru/viewtopic.php?f=20&t=1053
Нужны деньги срочно и без отказа? Подпишитесь на канал Telegram – быстрые деньги на карту без отказа ! Мы собрали все МФО 2024, которые предлагают займы на карту быстро и круглосуточно. На нашем канале вы найдете малоизвестные компании, готовые дать займ всем без проверки кредитной истории. Получите займ от 1 до 30 тысяч рублей мгновенно, без долгих заявок и походов в банк. Вся информация на одном канале — Новые микрокредиты – Telegram . Не тратьте время, подписывайтесь и решайте финансовые проблемы уже сегодня!
Добрый день!
Приобрести диплом о высшем образовании.
wiki.gta-zona.ru/index.php/Обширный_каталог_документов_в_известном_онлайн-магазине
Привет!
Купить диплом ВУЗа
Наши специалисты предлагают выгодно заказать диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Документ пройдет лубую проверку, даже при помощи специальных приборов. Решите свои задачи быстро и просто с нашей компанией.
Где купить диплом по актуальной специальности?
ebonyfaces.com/blogs/34/Что-может-сегодня-предложить-интернет-магазин-с-дипломами
forexrassia.ru/nastoyashhie-diplomyi-bez-ozhidaniya-i-problem
selkovo.rolka.me/viewtopic.php?id=3419#p10112
followmylive.com/read-blog/1097
telegra.ph/Legkij-vybor-magazina-chto-prodaet-diplomy-07-08
Привет!
Заказать диплом о высшем образовании
Мы предлагаем быстро приобрести диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями. Данный диплом способен пройти любые проверки, даже при использовании специфических приборов. Достигайте своих целей быстро и просто с нашей компанией.
Где заказать диплом по нужной специальности?
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
mosday.getbb.ru/viewtopic.php?f=12&t=1059
3drus.ru/forum/topic_34806
pdlspd.listbb.ru/viewtopic.php?f=3&t=409
molbiol.ru/forums/index.php?showtopic=1179953
Привет!
Мы можем предложить дипломы любой профессии по доступным ценам.
http://www.fromrus.su/index.php?/gallery/image/324-почему-сегодня-куда-проще-и-дешевле-купить-диплом-университета/
Добрый день!
Мы предлагаем документы ВУЗов, расположенных в любом регионе Российской Федерации. Можно приобрести качественно напечатанный диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты делаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригинала. Документы заверяются всеми обязательными печатями и подписями.
respectmyopinion.com/blogs/31/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Здравствуйте!
Заказать документ о получении высшего образования.
itstagram.ru/read-blog/851
delta72.at.ua/forum/61-26792-1
forex.g-talk.ru/viewtopic.php?f=43&t=7130
x70795vj.beget.tech/content/add/topic/
raussga.flybb.ru/viewtopic.php?f=12&t=2209
Добрый день!
Заказать документ о получении высшего образования можно в нашем сервисе.
ast-diplom.com/kupit-diplom-voronezh
Удачи!
Добрый день!
Приобрести диплом о высшем образовании.
shopwheel.ru/club/user/49/blog/55202/
Купить диплом университета.
fire-team.ru/forum/member.php?u=1143
mystroycenter.ru/legalnaya-pokupka-diplomov-byistro-i-nadezhno
hitman.getbb.ru/ucp.php?mode=login&sid=2104ede321ee965306a545988cb00bd3
musictech.gr/forum/viewtopic.php?f=8&t=31148
army.clanfm.ru/posting.php?mode=post&f=2&sid=3071ec0d4d301fc5a04a9073d3534d6f
Привет, друзья!
Мы изготавливаем дипломы.
kofe.80lvl.ru/viewtopic.php?f=10&t=812
peaceofficial.5nx.ru/viewtopic.php?f=111&t=805
bonchancetour.ru/blogs/interest/1569.php#comments
turservisnews.ru/kupit-diplom-s-dostavkoy-na-dom
forum.artinvestment.ru/member.php?u=1807451
срочно починить смартфон
Привет, друзья!
Мы можем предложить дипломы любой профессии по доступным тарифам.
autogroupe.ru/poluchite-diplom-bez-lishnih-usiliy
Привет!
Мы можем предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Можно приобрести диплом за любой год, включая документы старого образца. Дипломы и аттестаты печатаются на бумаге самого высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригиналов. Документы заверяются всеми требуемыми печатями и штампами.
rf-unicron.ru/index.php?/gallery/image/121-%D0%BE%D1%82%D0%BB%D0%B8%D1%87%D0%BD%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%86%D0%B5%D0%BD%D0%BA%D0%B8-%D0%B8-%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B9-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Привет!
Приобрести документ о получении высшего образования
ast-diplomy24.ru/kupit-diplom-sankt-peterburg
Привет, друзья!
Приобрести документ ВУЗа.
mdr7.ru/viewtopic.php?f=6&t=8943
aboutalltour.ru/nadezhnyiy-sposob-poluchit-diplom-za-korotkiy-srok/
w77515cs.beget.tech/2024/07/16/vash-shans-na-uspeh-diplom-bez-ucheby.html
4division.ru/viewtopic.php?f=13&t=8632
ya.6bb.ru/viewtopic.php?id=3213#p5162
Добрый день!
Приобрести диплом ВУЗа.
acertdglobalplatform.mn.co/posts/61748766
Name], each offering unique bonuses and promotions for Aviator Game players.
ivermectin price
Здравствуйте!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
landik-diploms-srednee.ru/diplom-bakalavra В
Добрый день!
Купить диплом любого университета:
kirpich-opt-265.1gb.ru/index.php?subaction=userinfo&user=uluhaxur
altajska.cz/forum/user/2477-ifimyfi
region-standart.ru/guestbook/?1707835084
zpu-journal.ru/forum/view_profile.php?UID=307255
forum.epileptologist.ru/viewtopic.php?f=1&t=66721
Здравствуйте!
Как приобрести аттестат о среднем образовании в Москве и других городах
http://www.kladonahodki.ru/component/k2/itemlist/user/297633
Окажем помощь!.
Привет!
Реально ли приобрести диплом стоматолога? Основные этапы.
Приобрести диплом о высшем образовании.
dekortab.com/index.php?/gallery/image/163-%D0%BD%D0%B8%D0%B7%D0%BA%D0%B8%D0%B5-%D1%86%D0%B5%D0%BD%D1%8B-%D0%B8-%D0%B8%D0%B4%D0%B5%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B9-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Добрый день!
Мы можем предложить документы техникумов, расположенных на территории всей Российской Федерации. Можно купить диплом от любого учебного заведения, за любой год, включая документы старого образца. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Они заверяются всеми требуемыми печатями и подписями.
hlxgolcs2.blogitright.com/28378452/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Как оказалось, купить диплом кандидата наук не так уж и сложно
diplomyx.com/kupit-diplom-o-srednem-obrazovanii
Здравствуйте!
Как получить диплом о среднем образовании в Москве и других городах
meat.ntnn.ru/personal/profile/index.php?register=yes
Всегда вам поможем!
Hello,
What an nice post!
Can I scrape this and share it with my channel members?
My group is about Korean 한국야동
your interested, feel free to visit my community
and check it out.
Thank you and Keep up the good work!
В Vavada казино промокоды позволяют получать дополнительные бонусы для любимых игр, делая процесс игры еще более захватывающим и интересным.
Привет!
Заказать документ о получении высшего образования можно в нашей компании.
ast-diplomas.com/kupit-diplom-chelyabinsk
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
cnktdshanoi.com.vn/речной-диплом-купить/
Заказать диплом университета.
ayema.ng/blogs/32777/ упить-?иплом-Ѕыстро-и-Ћегально
amengram.com/blogs/361/Купить-диплом-быстро-и-надежно
trum.flybb.ru/viewtopic.php?f=15&t=4684
izumrudnoeozero.listbb.ru/posting.php?mode=post&f=8
dominion.listbb.ru/posting.php?mode=post&f=11
Промокоды Drip казино открывают доступ к уникальным бонусам, делая игровой процесс более увлекательным и повышая шансы на выигрыш.
Добрый день!
Мы можем предложить дипломы.
vintfint.com/blogs/22447/Быстрое-Оформление-Дипломов-Надежно-и-Легально
borderforum.ru/viewtopic.php?f=7&t=10267&sid=d3163d961470a6ce493c9ae62faad438
odnopolchane.net/forum/member.php?u=546804
argayash.flybb.ru/viewtopic.php?f=9&t=1133
щербиновскийрайон.рф/users/160
Привет!
Купить диплом о среднем образовании в Москве и любом другом городе
krugozorov.ru/forum/user/9183
Рады оказать помощь!
Промокоды Vavada казино обеспечивают дополнительные бонусы, делая процесс игры более увлекательным и захватывающим.
Добрый день!
Как получить диплом техникума с упрощенным обучением в Москве официально.
Заказать диплом любого университета.
network-6342899.mn.co/posts/61828984
Здравствуйте!
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по невысоким тарифам.
lanouvellemine.fr/купить-диплом-новосибирск/
Привет!
Заказать диплом о высшем образовании.
shopwheel.ru/club/user/49/blog/55202/
Здравствуйте!
Узнайте, как приобрести диплом о высшем образовании без рисков
velopiter.spb.ru/profile/117605-dilopluyy/?tab=field_core_pfield_1
Будем рады вам помочь!.
Добрый день!
Как быстро и легально купить аттестат 11 класса в Москве
earthpro.listbb.ru/ucp.php?mode=login&sid=8faf209d3d39402c63e515c6a1b5756f
Будем рады вам помочь!
Здравствуйте!
Приобрести документ ВУЗа вы имеете возможность у нас в столице.
ast-diplomy.com/kupit-diplom-bakalavra-ili-specialista
Привет!
Заказать документ о получении высшего образования
ast-diploms24.ru/kupit-diplom-magistra
Здравствуйте!
Заказать документ о получении высшего образования.
pakians.com/blogs/98943/Получите-диплом-без-учебы-и-стресса
flashtest.80lvl.ru/viewtopic.php?f=3&t=1926
cocapal.com/read-blog/1009
ayema.ng/blogs/33768/Диплом-в-кратчайшие-сроки-качественно-и-безопасно
balans.kz/bonus/
Здравствуйте!
Мы готовы предложить дипломы любой профессии по приятным ценам.
foto-passau.com/gallery/image/9-четыре-ключевых-группы-интернет-магазинов-что-реализуют-дипломы/
Привет!
Покупка школьного аттестата с упрощенной программой: что важно знать
arusak-diploms-srednee.ru/kupit-diplom-v-krasnoiarske
Привет, друзья!
Купить документ о получении высшего образования вы имеете возможность в нашем сервисе.
ast-diplomas.com/kupit-diplom-o-srednem-obrazovanii
Успешной учебы!
Привет!
Купить диплом о высшем образовании.
rvolchansk.ru/user/zaanattsz6196/
Успешной учебы!
Добрый день!
Заказать документ о получении высшего образования вы можете в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов России. Вы получите диплом по любым специальностям, включая документы образца СССР.
avtovideotest.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
stylist-profi.ru/forum/user/200285/
mojgorod.getbb.ru/viewtopic.php?f=12&t=1451
sovavtoprom.ru/wiki/index.php/Диплом_любой_специальности:_качественно_и_оперативно
linkthere.club/read-blog/8550
Привет, друзья!
Где приобрести диплом по актуальной специальности?
Заказать диплом ВУЗа.
http://www.pitomec.ru/forum/post/13043
Как так то
сайт управляющей компании
The Counterpoint team managed all of the deficiencies and made sure that the building was happy with the construction throughout the entire2-year renovation. For that reason, Rule 2-01 provides that, in determining whether an accountant is independent, the Commission will consider all relevant facts and circumstances. In determining whether an accountant is independent, the Commission will consider all relevant circumstances, including all relationships between the accountant and the audit client, and not just those relating to reports filed with the Commission. Any partner, principal, shareholder, or professional employee of the accounting firm, any of his or her immediate family members, any close family member of a covered person in the firm, or any group of the above persons has filed a Schedule 13D or 13G (17 CFR 240.13d-101 or 240.13d-102) with the Commission indicating beneficial ownership of more than five percent of an audit client’s equity securities or controls an audit client, or a close family member of a partner, principal, or shareholder of the accounting firm controls an audit client. 1) Financial relationships. An accountant is not independent if, at any point during the audit and professional engagement period, the accountant has a direct financial interest or a material indirect financial interest in the accountant’s audit client, such as: (i) Investments in audit clients.
Привет!
Купить документ института можно в нашем сервисе.
asxdiplomik.com/kupit-diplom-nizhnij-novgorod
Хорошей учебы!
Добрый день!
Купить диплом старого образца, можно ли это сделать по быстрой схеме?
cars.autokaif.ru/index.php?subaction=userinfo&user=axakyn
Поможем вам всегда!.
Software Requirements
ivermectin price
Добрый день!
Заказать документ о получении высшего образования
asxdiplomik.com/kupit-diplom-ekaterinbur
Привет!
Мы готовы предложить дипломы любых профессий по приятным тарифам.
newsofgames.ru/kupit-diplom-bez-posrednikov-byistro-i-nadezhno
Добрый день!
Быстрая схема покупки диплома старого образца: что важно знать?
forum.safe-animals.ru/index.php?showtopic=30579
Будем рады вам помочь!
Привет, друзья!
Стоимость дипломов высшего и среднего образования и процесс их получения
landik-diploms-srednee.ru/kupit-diplom-v-omske В
The spa body rub waiting visit one of the kinds massage, is what we do. What is an aromatic massage interested in everyone. sports massage it’s a craftsmanship of giving for bliss. You willextremely surprised to that,what ocean pleasure can get to know from choice massage. In spa center Tibetan KuNye Massage women will hold the most sensual energy massage.
How is it done, and is there something exotic? We will tell you all about him that you wanted to know |Our oriental massage is visited not only by men but also by women, and also by couples. You want to use only this infinitely … Our primary а task this is to please customer wonderful delicious tantric massage. Distinctive approach to any your desires and requirements.
The sexy girls our the spa center will give you an unforgettable experience. The spa center is a place of rest and relaxation. Such vibrating massage, as though, and relaxation, affects on defined elements body, what helps ladies relax. Give your preference not just to one, but to two masseuses! Choose for yourself masseur girl by external data, both professional and professional abilities!
Massage center in Empire State we recommend luxurious quarters with comfortable design. Data accommodation help be you you are staying with us secretly.
Our showroom works in Uptown Masseuses Trinity :
nuru massage sexy
Are you looking for an best massage NY, parlour massage NY, japanese massage NY, tantric massage NY, adult massage NY or body to body massage NY? Nuru Massage In Manhattan, NY were the first to offer sensational and slippery massage and we are dedicated to it for now. If you want the best massage parlour, look no further than the Nuru Massage In Manhattan, NY. Our nuru massage, thai massage, body to body massage girls will pleasure you like no one before.
New-York Escort – massage working hands
Добрый день!
Приобрести диплом ВУЗа.
c99596qr.beget.tech/2024/05/15/individualnoe-obrazovanie-gde-kupit-diplom-sozdannyy-specialno-dlya-tebya.html
Удачи!
Здравствуйте!
Купить диплом любого ВУЗа.
pawno-site.ru/index.php?/gallery/image/2-как-найти-проверенный-интернет-магазин-с-огромным-выбором-дипломов/
tronlink wallet – tronlink extension, tronlink pro
Добрый день!
Где приобрести диплом специалиста?
Приобрести диплом университета.
telearchaeology.org/TAWiki/index.php/Гарантированное_оформление_диплома_под_ключ
Здравствуйте!
Мы предлагаем документы техникумов, которые находятся на территории всей России. Можно купить диплом от любого учебного заведения, за любой год, в том числе документы старого образца. Дипломы и аттестаты печатаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они заверяются всеми требуемыми печатями и штампами.
pamplusmus.com/blogs/46/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет, друзья!
Купить документ университета можно в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР.
linkthere.club/read-blog/8550
datasphere.ru/club/user/15/blog/
http://www.politikforum.ru/member.php?u=13385920
pdlspd.listbb.ru/viewtopic.php?f=3&t=462
bohhchaos.listbb.ru/viewtopic.php?f=9&t=8414
For individuals who admire the attraction of designer purses but recoil at the hefty price, imitation bags offer an attractive choice. This article reveals the intricacies of the fake handbag market, emphasizing its draw to style aficionados and high-end admirers alike. From grasping what fake purses are to tips for executing smart purchases, we’ll cover all you want to know to indulge in style without breaking the wallet.
Imitation bags are premium copies of luxury handbags, designed to closely meticulously resemble their originals. While they may never carry an official label name, these replicas often mirror the same design, materials, and craftsmanship as their much expensive originals.
http://tiny.cc/seq3yz
Quality and Craftsmanship
Opposite in common belief, numerous replica handbags are created with careful attention to detail. Expert artisans utilize premium resources in order to guarantee the fact that the fakes possess the similar look and feel as the authentic designer items.
Availability and Variety
a. lovers.Ethical Considerations
While fake purses provide an budget-friendly way to enjoy luxury fashion, it is crucial to recognize acknowledge the moral consequences. The and distribution of fake purses might infringe against intellectual property property, bringing up issues concerning the morality of owning purchasing and owning them.Access to Luxury Designs
Why Opt for Replica Purses?
Fake bags have a notable significant following within fashion enthusiasts for various many compelling arguments. Below, we discuss examine why these such trendy choices have become grown so favored.
Budget-friendly
One of the most evident advantages of knockoff purses is their. High-quality knockoffs can offer the same same visual pleasure as authentic authentic high-end purses without incurring the high price.
Replica bags enable this feasible so fashion enthusiasts toward enjoy those latest luxury designs, regardless to budget constraints. This availability permits more individuals to participate in haute couture and express one’s style.Experimentation Without Commitment
For those who who enjoy experimenting experimenting with with fashion styles purses offer an opportunity to explore various various trends significant financial investment. This flexibility is especially especially appealing individuals that enjoy who love to switch up their looks.To to Identify a Top-Quality Replica Handbagplica bags.
Exploring this replica handbag market can be challenging, but with proper correct knowledge, one will easily execute smart purchases. Here are several suggestions on spotting high-quality reproduction bags
Material and Stitching
Pay close attention to the materials used and the quality of the stitching. High-quality replicas often use genuine leather or premium synthetic alternatives and exhibit clean, precise stitching.
Hardware and Information
Examine the components, including zippers, clasps, and brand marks. Top-notch imitations feature hardware that closely resembles that of the authentic luxury bags, with without rough edges or sloppily finished features.
While copy bags are unable to lawfully employ the identical logo of the genuine items, some might contain subtle indications that imitate the design features of luxury labels. Search for these elements to determine the accuracy of the imitation.Popular Replica Bag Brands
Certain labels are well-known known for their premium replicas, giving style enthusiasts a diverse range of fashionable options. Here, we showcase some of the top popular imitation bag names.
AAA Handbags Purses is for making creating some of the top imitations available. Their bags products feature exceptional focus to meticulousness and craftsmanship, which makes them popular amongst copy fans.
Purse Valley Bags Valley sells an extensive range of copy handbags, such as designs based on top top luxury brands. Focusing on quality and superiority and customer customer happiness, they established built a solid reputation in the replica purse industry.
Designer Discreet Bags specializes on making premium replicas that closely imitate the original items. Their collection range features handbags from iconic fashion houses, offering clothing aficionados with many choices.
A Craft for Styling Imitation Handbags
Replica handbags can seamlessly blend into any closet, allowing you to compose elegant and fashionable looks. Here are some tips for adding replica bags into your style range.Handling with Care
Pairing against Traditional Outfits
A classic ensemble, such as a LBD or a fitted suit, can be enhanced with a carefully selected fake purse. Opt for enduring styles that enhance your ensemble and add a dash of elegance.
Mixing Luxury plus Low Fashion
Match top-notch imitation handbags with low-cost fashion pieces to craft a harmonious and trendy look. This method permits you to highlight your fashion whilst being economical.
Embellishing using Assurance
When matching imitation handbags, poise is key. Handle your fake bag with the same attention and respect as you would a genuine branded item, and it will elevate your overall style.
Caring for Fake Bag
Correct care and maintenance are critical to ensure your fake bag appearing its finest. Follow these tips to guarantee its longevity.
Consistent Maintenance
Wash your fake purse consistently with a gentle cloth and mild cleaning solution. Refrain from strong substances that can ruin the surface or shade.
Storing Advice
Place your fake bag in a cool, moisture-free area, distant from immediate light. Utilize protective bags or gentle materials to shield it from dust and abrasions.
Treat your replica purse with, keeping away from rough areas as well as overloading. It will assist maintain its form and prevent potential harm.
Replica purses offer an affordable alternative for designer designer items without having to compromising fashion or durability. With right styling & maintenance, these can seamlessly integrate into any style wardrobe, which makes them the popular choice for fashion enthusiasts. Regardless if you’re searching for a timeless look & the trendy statement-making item, there’re numerous well-known imitation bag labels that provide premium quality choices to fit every taste. So go ahead and add several stylish replicas to your own collection – no one can notice the difference.The Social Aspect of Replica Bags
Handle your imitation handbag with attention, by avoiding overburdening it with by heavy items. Doing so will assist preserve its form & prevent wearing & tear.
Fake handbags aren’t not about fashion; these additionally encourage a sense regarding community amongst fans. Here, you explore some social aspects of owning and talking about replica bags.Online Communities
Several online communities and discussion boards are devoted to copy handbags, where aficionados exchange tips, critiques, and tips. Such platforms provide useful insights & support to those exploring the imitation sector.In-Person Meetups
Certain replica bag enthusiasts arrange in-person meetups in order to display their collections as well as discuss their passion for fashion. Such gatherings offer chances to connect with similar individuals and share thoughts.Influencers and Reviews
Influencers and influencers often evaluate fake bags, offering genuine opinions as well as contrasts with genuine brand-name items. Following these evaluations can assist one in making well-informed choices about one’s buying.Legal and Ethical Considerations
Grasping the lawful as well as principled facets concerning purchasing fake handbags is crucial for making well-informed choices. Here, we tackle some common worries.Intellectual Property Rights
Imitation purses might infringe upon the proprietary ownership assets of premium brands. Be mindful of the lawful consequences and likely risks linked to acquiring and having imitations.Ethical Shopping
Consider the moral consequences of supporting the replica handbag market. Although it provides affordable options, it may also lead to exploitative work conditions and environmental concerns.Making Informed Choices
Future Patterns regarding Replica Bags
The replica bag industry is constantly constantly evolving, with new trends as well as innovations arising. In this article, we will explore a few possible future advancements.
Green ComponentsConclusion
Since eco-friendliness grows as a rising worry, the replica purse sector might transition towards using eco-friendly resources. This shift might appeal to environmentally conscious consumers and reduce the industry’s ecological footprint.
Cutting-edge Innovation
Developments in technology, such as additive manufacturing, could revolutionize the creation of replica bags. These developments could result in even higher-quality imitations that are hard to distinguish from the authentic ones.
Shifting Buyer Attitudes
Customer perspectives towards imitation bags might persist to evolve, with increased approval and recognition for high-quality copies. This transition could boost need and affect sector patterns.
Replica bags offer a stylish and affordable alternative for fashion enthusiasts and luxury lovers. By understanding the intricacies of the replica bag market, you can make informed choices and enjoy the benefits of high-quality imitations. Whether you’re drawn to the affordability, variety, or the ability to experiment with different styles, replica bags provide a gateway to the world of luxury fashion*.
Ready to explore the world of replica bags? Join our community of fashion enthusiasts and start your stylish journey today!
Здравствуйте!
Купить документ ВУЗа можно у нас.
ast-diploms.com/kupit-diplom-perm
Добрый день!
Приобрести диплом о высшем образовании.
forum.vipcs.pp.ua/gallery/image/313-как-подыскать-проверенный-магазин-с-широким-выбором-дипломов/
Привет, друзья!
Купить документ о получении высшего образования.
niagarafallspal.com/read-blog/939
sampnewrp.listbb.ru/viewtopic.php?f=18&t=532&sid=06a83fc4bfdb26aad4da42691ebfd6d2
jeepgarage.ru/forum/topic.php?forum=24&topic=757
pdlspd.listbb.ru/viewtopic.php?f=3&t=471
sky-metaverse.com/create-blog/
Привет, друзья!
Мы можем предложить документы техникумов, расположенных в любом регионе России. Вы сможете купить качественно сделанный диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригиналов. Документы будут заверены всеми необходимыми печатями и подписями.
doomelang.com/read-blog/6800
Здравствуйте!
Заказать диплом любого ВУЗа.
mindclub.online/wiki/index.php/??????_??????:_?????????_???????????
Успешной учебы!
готовая мебель для офиса https://office-mebel-on-msk.ru/
Здравствуйте!
Мы предлагаем документы техникумов, которые находятся на территории всей России. Вы можете заказать диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригиналов. Они заверяются необходимыми печатями и штампами.
1rbfwc1w4.thechapblog.com/27876891/%D0%9B%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
Привет, друзья!
Заказать документ ВУЗа.
jeepgarage.ru/forum/topic.php?forum=24&topic=755
medium.com/@oximus777/получите-дипломы-за-короткий-срок-80daae11a545
revolverp.forumex.ru/viewtopic.php?f=11&t=317
elektrofahrrad-tests.de/forums/newthread.php?fid=2&processed=1
artrp.5nx.ru/viewtopic.php?f=3&t=9679
Здравствуйте!
Как приобрести диплом о среднем образовании в Москве и других городах
wegoflc.com/купить-диплом-в-тольятти/
Здравствуйте!
Приобрести документ о получении высшего образования вы можете в нашей компании.
ast-diploms.com/kupit-diplom-sankt-peterburg
Успешной учебы!
можно ли подделать аттестат можно ли подделать аттестат .
Привет, друзья!
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
allnewstroy.ru/diplomyi-s-polnyim-paketom-dokumentov
С каждым годом растет количество людей, выбирающих этот вид досуга. Онлайн-платформы предлагают не только развлечение, но и шанс испытать удачу http://www.ingenieursdudimanche.lagob.fr/doku.php?id=_Riobet_Casino:_Советы_для_новичков
Привет, друзья!
Как получить диплом техникума с упрощенным обучением в Москве официально
http://www.nexuspals.online/blogs/158/Правильно-покупаем-диплом-в-сети-экспертный-обзор
Добрый день!
Мы предлагаем дипломы любой профессии по доступным тарифам.
lidertude.com/blogs/1185/С-умом-заказываем-диплом-в-сети-обзор
Top News Sites for Article Post Permanent
aljazeeranewstoday.com
australiannewstoday.com
bbcworldnewstoday.com
bloombergnewstoday.com
bostonnewstoday.com
britishnewstoday.com
Dont hesitate to Contact me.
Добрый день!
Где купить диплом по необходимой специальности?
Заказать диплом ВУЗа.
derivsocial.org/read-blog/2583
Привет!
Процесс получения диплома стоматолога: реально ли это сделать быстро?
medium.com/@oximus777/быстрое-и-безопасное-получение-диплома-898c73e2d10c
Всегда вам поможем!
more jaxx liberty download
Привет, друзья!
Заказать документ университета вы имеете возможность у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов РФ. Вы получите диплом по любым специальностям, включая документы Советского Союза.
http://www.bideew.com/create-blog/
visogo9427.ixbb.ru/viewtopic.php?id=111#p111
dachkanews.ru/gotovyiy-diplom-bez-dolgih-let-obucheniya/
place-e.ru/index.php/Купите_диплом_и_забудьте_о_студенческих_хлопотах
http://www.traveltravelforum.com/showthread.php/34068-Ваш-путь-к-успеху-диплом-на-заказ?p=69089#post69089
Risk Management: Setting limits on how much to bet and when to cash out.
cheap ivermectin
Добрый день!
Мы предлагаем дипломы любой профессии по приятным тарифам.
br-totalbyg.dk/2024/06/24/диплом-в-три-клика/
Привет!
Заказать документ о получении высшего образования вы можете в нашем сервисе. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов России.
ssd-astra.ru/forum/viewtopic.php?f=14&t=7014
tsmtech.co.kr/bbs/board.php?bo_table=free&wr_id=556613
loket.kr/free/165101
anoreksja.org.pl/viewtopic.php?f=27&t=1179562
http://www.starterkit.ru/html/index.php?name=account&op=info&uname=apify
Привет!
Заказать документ ВУЗа вы сможете в нашей компании в Москве.
ast-diplomy24.ru/kupit-diplom-krasnoyarsk
Успешной учебы!
https://buy-cloned-cards.buyclonedcards.work Buy Clon Card
Item 01 Card Total Balance: $3 100 – Price $ 110.00
Item 03 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
https://buycloned-cards.buyclonedcards.work Hacked paypal acc Cloned cards
Здравствуйте!
Как купить аттестат 11 класса с официальным упрощенным обучением в Москве
http://www.vaca-ps.org/blogs/173184/Гарантия-качества-ваш-диплом-на-заказ
Всегда вам поможем!
Привет, друзья!
Реально ли приобрести диплом стоматолога? Основные этапы
foro.rune-nifelheim.com/general-ragnarok-m/diplomy-ot-veduschih-vuzov-strany/
Здравствуйте!
Мы предлагаем документы техникумов, которые расположены в любом регионе России. Вы сможете заказать диплом за любой год, включая сюда документы старого образца СССР. Дипломы и аттестаты печатаются на бумаге самого высокого качества. Это дает возможность делать государственные дипломы, не отличимые от оригинала. Документы будут заверены всеми требуемыми печатями и штампами.
transformationarena.com//read-blog/56
Привет, друзья!
Купить диплом любого университета.
gamerszona.ru/index.php?/blogs/entry/3-как-подобрать-надежный-онлайн-магазин-с-обширным-выбором-дипломов/
Здравствуйте!
Мы можем предложить дипломы любой профессии.
andreieusebiu.net/files/file/43-зачем-сегодня-заказывают-аттестаты-и-дипломы-в-сети-интернет/
Будем рады вам помочь!.
Привет, друзья!
Заказать документ о получении высшего образования можно в нашем сервисе.
diploms-x24.ru/kupit-diplom-vracha
Успехов в учебе!
купить диплом сестры diploms-x.com .
Привет!
Купить документ о получении высшего образования вы сможете у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы сможете получить диплом по любым специальностям, любого года выпуска, включая документы старого образца. Даем 100% гарантию, что в случае проверки документов работодателем, подозрений не появится.
mykinotime.ru/kupit-diplom-bez-posrednikov-byistro-i-nadezhno/
fp2g6e0dg.wssblogs.com/28310881/Вы-хотите-выяснить-как-приобрести-диплом-в-сети-недорого-Заходите
http://www.indianhighcaste.com/read-blog/2124
http://www.contraband.ch/read-blog/4083
forum.drustvogil-galad.si/index.php/topic,14135.0.html
Добрый день!
Заказать документ о получении высшего образования вы имеете возможность в нашей компании в Москве.
ast-diplomy24.ru/kupit-diplom-o-srednem-obrazovanii
Успехов в учебе!
Здравствуйте!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
dexanet.ukrbb.net/viewtopic.php?f=5&t=15549
Рады оказать помощь!.
Привет, друзья!
Приобрести диплом ВУЗа
Наша компания предлагает выгодно и быстро купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Диплом способен пройти любые проверки, даже с применением профессионального оборудования. Достигайте цели быстро с нашими дипломами.
Где заказать диплом по актуальной специальности?
galantclub.od.ua/member.php?u=15983
http://www.matchfishing.ru/forumtest/1/member.php?u=23110
feelosum.com/blogs/1685/Ищем-проверенный-и-надежный-онлайн-магазин-для-покупки-документов
network.janenk.com/read-blog/686
z594ab8rn.develop-blog.com/34410368/Рекомендации-которые-помогут-найти-надежный-магазин-с-документами
Здравствуйте!
Купить документ университета.
stars.flyboard.ru/viewtopic.php?f=1&t=978
ratingforex.ru/forum-forex/viewtopic.php?f=18&t=45599&sid=b6fd21b907fc818d35ed6ff7e3b894f0
reflections.listbb.ru/viewtopic.php?f=45&t=758
diigo.com/item/note/8p2f0/3mv5?k=8d05ab431a69cb27d0d3275600332235
or1gano.80lvl.ru/viewtopic.php?f=10&t=1035
Здравствуйте!
Приобрести диплом о высшем образовании.
nybodyart.com/forums/gallery/image/2-как-найти-надежный-онлайн-магазин-с-широким-ассортиментом-дипломов/?context=new
Здравствуйте!
Мы предлагаем дипломы любой профессии по выгодным ценам.
prikol100500.ru/vash-diplom-byistro-nadezhno-kachestvenno
Добрый день!
Приобрести диплом о высшем образовании
Мы предлагаем быстро купить диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями должностных лиц. Диплом пройдет любые проверки, даже при использовании специального оборудования. Достигайте своих целей быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
ya.7bb.ru/viewtopic.php?id=11639#p33323
lubercy.ixbb.ru/viewtopic.php?id=6615#p14726
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
Добрый день!
Приобрести документ ВУЗа вы имеете возможность в нашей компании. Мы оказываем услуги по продаже документов об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца. Гарантируем, что в случае проверки документов работодателями, никаких подозрений не появится.
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по выгодным тарифам. Цена может зависеть от определенной специальности, года выпуска и ВУЗа. Стараемся поддерживать для заказчиков адекватную политику цен. Для нас важно, чтобы документы были доступны для большого количества граждан.
http://www.nitrnd.com/blogs/159602/Легко-заказываем-диплом-в-онлайн-магазине-Russian-Diplom?lang=fr_fr
Будем рады вам помочь!
Привет, друзья!
Где заказать диплом по необходимой специальности?
http://www.vevioz.com/read-blog/148290
continue reading this jaxx liberty
Здравствуйте!
Заказать диплом о высшем образовании.
hotmeets.ru/blogs/120/Большой-выбор-документов-в-знаменитом-интернет-магазине
купить диплом о высшем в уфе diploms-x.com .
Добрый день!
Мы предлагаем дипломы любой профессии по приятным ценам. Стоимость зависит от конкретной специальности, года получения и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы документы были доступными для большого количества граждан.
prikol100500.ru/poluchite-diplom-po-vashim-trebovaniyam-zakazhite-pryamo-seychas
Привет!
Приобрести документ университета можно у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ.
chip-ecu.ru/threads/chevrolet-cruze-2013г-gm-13589374ab.234/#post-6802
чпуремонт.рф/showthread.php?tid=46085
gothic2online.ru/index.php?/topic/6587-купить-диплом-w888y/
sp.60333.ru/viewtopic.php?f=10&t=2841&p=339352#p339352
hosting.show/profile/ynanebun/
https://tezfiles.cc/
Здравствуйте!
Мы изготавливаем дипломы любой профессии.
http://www.trngamers.co.uk/read-blog/1182_planiruete-kupit-attestat-u-nadezhnogo-proizvoditelya-zhdem-vas.html
Рады оказаться полезными!.
Привет, друзья!
Диплом техникума купить официально с упрощенным обучением в Москве.
Купить диплом о высшем образовании.
wiki.intradition.ru/index.php/%D0%92%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D1%8B%D0%B5_%D1%86%D0%B5%D0%BD%D1%8B_%D0%B8_%D0%BF%D1%80%D0%B5%D0%BA%D1%80%D0%B0%D1%81%D0%BD%D0%BE%D0%B5_%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE_-_%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B_%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD!
Оформим второе гражданство, вид на жительство (ВНЖ) или резидентство в разных странах СНГ, Европы и Америки. Смотрите вступительное видео:
https://www.youtube.com/watch?v=R4GyGl7X07E
Второе гражданство, практическая иммиграция, иммиграция, вид на жительство, ВНЖ, Зелёная карта (green card) США
Гражданство стран Евросоюза под ключ
Гражданство на основании корней
Гражданство Армении под ключ
Гражданство Кыргызстана под ключ
Гражданство Польши под ключ
Гражданство Болгарии под ключ
Гражданство Италии под ключ
Гражданство Греции под ключ
Гражданство Израиля под ключ
Пишите нам в ТЕЛЕГРАМ: https://t.me/LibFinTravel
Или заходите на сайт: https://libertyfintravel.ru/vnj-i-vtoroe-grajdanstvo
Привет, друзья!
Купить диплом о высшем образовании.
fulldropshipping.com/index.php?/events/event/9-как-найти-надежный-онлайн-магазин-с-огромным-ассортиментом-дипломов/
cash-out perfectly.
ivermectin cheap
Добрый день!
Приобрести документ ВУЗа.
forum.infinite-soul.org/viewtopic.php?f=64&t=18457
anoreksja.org.pl/viewtopic.php?f=13&t=1248287
gamerplayz2k.mn.co/posts/62086690
inmeta.ru/wd/sf/viewtopic.php?f=17&t=1812
avtobestnews.ru/diplomyi-kotoryie-izmenyat-vashu-zhizn
http://intermedservice.ru/vazhnost-zabotyi-o-svoem-zdorove/
Привет, друзья!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
avtovladelez.ru/byistroe-oformlenie-diploma-nadezhno-i-bezopasno
Всегда вам поможем!
Привет!
Мы готовы предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Вы имеете возможность купить качественно напечатанный диплом от любого учебного заведения, за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и подписями.
http://www.chat-hozn3.com/blogs/13306/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет!
Мы изготавливаем дипломы любых профессий по выгодным тарифам.
ugandamining.com/blogs/49/Как-выбрать-надежный-интернет-магазин-который-реализует-дипломы
Привет!
Купить документ о получении высшего образования.
mystroycenter.ru/diplomyi-lyuboy-slozhnosti-byistro-i-bez-problem
backshowtime.ru/oformlenie-diploma-bez-problem-i-zabot
argayash.flybb.ru/viewtopic.php?f=9&t=1155
industrial.getbb.ru/viewtopic.php?f=4&t=3097
wap.fortboyard2012forum.4adm.ru/viewtopic.php?f=27&t=4159
https://tezfiles.cc/
Increased sales. High-quality customer 360o.info service stimulates additional sales. The average check increases, sales volume increases.
Models of hydraulic motors with a working volume of up to 400 and 1000 cubic cm are considered basic mmo5.info
Здравствуйте!
Как правильно приобрести диплом колледжа или ПТУ в России, важные моменты.
Заказать диплом ВУЗа.
mimedia.in/read-blog/50841
Нужны деньги срочно и без отказа? Подпишитесь на канал Telegram – лучшие МФО для займов ! Мы собрали все МФО 2024, которые предлагают займы на карту быстро и круглосуточно. На нашем канале вы найдете малоизвестные компании, готовые дать займ всем без проверки кредитной истории. Получите займ от 1 до 30 тысяч рублей мгновенно, без долгих заявок и походов в банк. Вся информация на одном канале — Займы для студентов – Telegram . Не тратьте время, подписывайтесь и решайте финансовые проблемы уже сегодня!
special info Download Coinomi
Привет, друзья!
Мы готовы предложить документы ВУЗов, расположенных в любом регионе РФ. Можно заказать диплом от любого заведения, за любой год, в том числе документы СССР. Дипломы и аттестаты делаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы заверяются всеми требуемыми печатями и подписями.
pittsburghpenguinsclub.com/read-blog/2279_detalnoe-opisanie-priobreteniya-diploma-v-magazine.html
Привет!
Приобрести документ о получении высшего образования.
delta72.at.ua/forum/61-26832-1
say.la/read-blog/37731
revolverp.forumex.ru/viewtopic.php?f=11&t=317
panther.80lvl.ru/posting.php?mode=post&f=19
sharecovid19story.com/viewtopic.php?f=11&t=1267832&p=2652599#p2652599
гостиница промокод
Привет, друзья!
Где приобрести диплом по необходимой специальности?
vina-net.ru/
Добрый день!
Аттестат школы купить официально с упрощенным обучением в Москве
http://www.xrated.social/blogs/146/Как-можно-приобрести-сейчас-качественный-диплом-в-сети
Привет!
Заказать документ университета вы можете в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, включая документы образца СССР. Гарантируем, что в случае проверки документов работодателями, подозрений не возникнет.
Мы можем предложить дипломы любой профессии по выгодным тарифам. Цена будет зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступными для большого количества наших граждан.
forum.unrivaled.ro/index.php?/gallery/image/533-отличные-расценки-и-идеальное-качество-приобретай-дипломы-онлайн/
Окажем помощь!
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
last musialanews here!
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
last news about firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
Добрый день!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
bmw-donbass.ru/gallery/image/838-для-чего-сейчас-приобретают-дипломы-в-интернете/
Привет!
Заказать документ ВУЗа можно в нашей компании в столице. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, включая документы СССР. Даем гарантию, что в случае проверки документа работодателями, каких-либо подозрений не появится.
ethiopianregister.com/read-blog/1317
site2.liodiz.ru/2024/07/10/blagodarya-chemu-internet-magaziny-s-diplomami-segodnya-tak-populyarny.html
lp24.ru/advice/faq-i-tehpodderzka-zakazyvaem-diplom-v-seti
sm3j2vdvm.designertoblog.com/59802188/Как-подыскать-надежный-онлайн-магазин-с-дипломами-Обзор-специалиста
nedvigimost.bbok.ru/viewtopic.php?id=27329#p46774
Привет, друзья!
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по приятным тарифам.
orangekitchendecor.all-new.info/купить-диплом-в-артеме/
Добрый день!
Мы изготавливаем дипломы любой профессии.
traquegarden.com/купить-диплом-заочной-формы/
Рады оказать помощь!.
Привет!
Заказать диплом о высшем образовании:
kioskindustry.ru/index.php?subaction=userinfo&user=axafep
meatzone.ru/index.php?/topic/2167-старт-сервера/#comment-6164
dedmorozural.ru/users/uvule
rtpsouth.com/UserProfile/tabid/69/userId/105911/Default.aspx
????.com/bbs/board.php?bo_table=free&wr_id=434447
Здравствуйте!
Узнайте стоимость диплома высшего и среднего образования и процесс получения
delta72.at.ua/forum/61-26767-1
Окажем помощь!
Привет, друзья!
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по невысоким ценам. Стоимость может зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас важно, чтобы дипломы были доступны для большинства граждан.
andreg1j29.thelateblog.com/27564266/Дипломы-за-деньги-Правда-о-Покупке-Образования-купить-диплом
https://www.themoviedb.org/movie/261903-real-gangsters
Если вам нужны профессионалы в области продвижения сайтов и разработки, обратите внимание на Mihaylov Digital. Они предлагают полный спектр услуг: от SEO и SEM до работы с Яндекс.Директ. Команда специализируется на создании эффективных стратегий, которые помогают привлечь целевую аудиторию и увеличить видимость вашего бизнеса в интернете. Их профессионализм и подход к каждому клиенту гарантируют отличные результаты. Рекомендую Mihaylov Digital как надежного партнера в цифровом маркетинге! С уважением, Mihaylov Digital.
Нужен ремонт видеокарт в Казани? Обращайтесь в Тех Профи! Мы предоставляем бесплатную диагностику и профессиональный ремонт с использованием оригинальных запчастей. Наши инженеры с более чем 5-летним опытом готовы помочь вам с любыми задачами, включая срочный ремонт и доставку техники курьером.
News Sites for Article post
frenchnewstoday.com
germaynewstoday.com
guardiannewstoday.com
headlinesworldnews.com
huffingtonposttoday.com
irishnewstoday.com
Dont hasitate to contact us
Добрый день!
Заказать диплом любого университета
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями должностных лиц. Данный диплом пройдет любые проверки, даже с применением специфических приборов. Решайте свои задачи максимально быстро с нашей компанией.
Где приобрести диплом по актуальной специальности?
http://www.trngamers.co.uk/read-blog/1211
usa.life/read-blog/63074
tweecampus.com/read-blog/81545
wiki.gta-zona.ru/index.php/Ваш_Настоящий_Диплом:_Быстро_и_Удобно
medik-look.ru/kupit-diplom-ekspress-dostavka
[u][b] Привет, друзья![/b][/u]
[b]Как быстро и легально купить аттестат 11 класса в Москве [/b]
[url=http://finansforum.apbb.ru/login.php?action=i/]finansforum.apbb.ru/login.php?action=i[/url]
Рады оказать помощь!
Здравствуйте!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
linkheed.com/blogs/3465/Ценные-советы-по-покупки-диплома-в-сети
Здравствуйте!
Приобрести документ о получении высшего образования можно в нашей компании.
asxdiplomik24.ru/kupit-diplom-omsk
Успехов в учебе!
Полезные советы по покупке диплома о высшем образовании без риска
ast-diploms24.ru/kupit-diplom-ekaterinbur
Здравствуйте!
Купить диплом ВУЗа.
http://www.jointcorners.com/read-blog/78249
Приобрести диплом о высшем образовании.
etoprosto.ru/ru/forum/?category=5&action=topic
elitemagyaritasok.info/e107_plugins/forum/forum_post.php?f=nt&id=21#
rakisochi.ru/users/20
drugisaitove.listbb.ru/viewtopic.php?f=2&t=633
owen.ru/forum/member.php?u=106526
Добрый день!
Купить документ о получении высшего образования вы можете у нас в столице.
asxdiplomik.com/otzyvy
Удачи!
Привет, друзья!
Как купить аттестат 11 класса с официальным упрощенным обучением в Москве
dp.getbb.ru/viewtopic.php?f=3&t=738
Всегда вам поможем!
Здравствуйте!
Мы предлагаем дипломы.
verkehrsknoten.de/index.php/forum/sozialvorschriften/91080#92044
armit.ru/social/user/42552/forum/message/1596/1598/#message1598
paladiny.ru/forummess.dwar.php?TopicID=27563
roseninsel.kz/forum/topic/add/forum7/
karkadan.ru/users/77829
Good Post. Are you a Clash Royale player looking to build strong decks in clash royale? If so, crafting effective Clash Royale decks poses a challenge, but players can succeed with strategic advice. Utilize the Clash Royale Deck Builder to create top-performing decks and ascend to higher ranks in legendary arenas. For in-depth information, visit the website provided.
Привет!
Приобрести документ о получении высшего образования можно у нас в столице.
diploms-x.com/kupit-diplom-rostov-na-donu
Удачи!
Strategies and Tips
buy ivermectin
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
last news about firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
last musialanews here!
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
musiala
Привет, друзья!
Где заказать диплом специалиста?
gotartwork.com/Blog/цена-покупки-диплома-и-аттестата-в-2024-году-новые-тенденции-и-возможности/289060/
Добрый день!
Заказать документ о получении высшего образования можно в нашей компании в столице. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любым специальностям, включая документы образца СССР. Даем 100% гарантию, что при проверке документов работодателями, подозрений не возникнет.
stalinarch.ru/wiki/index.php/Купить_диплом_от_проверенного_поставщика
laver.listbb.ru/viewtopic.php?f=3&t=1034
followgrown.com/read-blog/2702
gtago.ru/gallery/image/23-katalog-i-sposoby-dostavki-v-internet-magazine-zakazyvaem-attestat/?context=new
afriprime.net/blogs/41887/Что-именно-потребуется-для-изготовления-качественного-диплома-ВУЗа
Добрый день!
Купить диплом университета:
cstrike.g-service.ru/index.php?/topic/42-купить-диплом-o892g/
forum.ubuntu.ru/index.php?topic=321738.new#new
printpoligraf.kiev.ua/index.php?subaction=userinfo&user=ynowyqyco
daongil.com/bbs/board.php?bo_table=free&wr_id=301302
forum.stde.ru/index.php?/topic/9874-how-to-create-a-new-topic-at-forumstderu/page/6/#comment-11624
Добрый день!
Приобрести диплом о высшем образовании.
ethiopianregister.com/read-blog/1253
avtolux48.ru/people/user/367/blog/7875/
tricityfriends.com/read-blog/540
fomazy.com/blogs/4735/Выбираем-проверенный-онлайн-магазин-с-аттестатами-и-дипломами
sonnick84.csublogs.com/34366853/Приобретаем-диплом-в-надежном-интернет-магазине-Советы-эксперта
На сайте https://diagnosticheskie-skanery.ru получите полную и исчерпывающую информацию, связанную с диагностическими автомобильными сканерами. Вы узнаете то, для чего они предназначены, как используются. Рассматриваются и виды диагностических сканеров. Имеются универсальные, автомобильные. Изучите подробную информацию о том, как правильно подобрать подобное оборудование, на что лучше полагаться. Также есть данные и о том, от чего зависит качество, расценки, представлены самые известные модели, которые точно заинтересуют.
Привет, друзья!
Мы предлагаем документы ВУЗов, которые расположены на территории всей РФ. Вы сможете приобрести диплом за любой год, в том числе документы СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригиналов. Документы будут заверены необходимыми печатями и штампами.
lastdemo.primepix.ru/club/user/88/blog/8806/
Привет, друзья!
Купить диплом о высшем образовании
Наши специалисты предлагают выгодно купить диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями должностных лиц. Документ способен пройти любые проверки, даже с использованием специального оборудования. Достигайте свои цели максимально быстро с нашим сервисом.
Где приобрести диплом по нужной специальности?
u90517ol.beget.tech/2024/07/07/vysshee-obrazovanie-legko-i-bystro-kupit-diplom.html
woorichat.com/read-blog/829
pdcdjg3dn.bluxeblog.com/60370955/Вы-хотите-выяснить-как-купить-документы-в-интернете-Ждем-Вас
tihiy-don.su/2024/07/06/kupit-oficialnyy-diplom-kachestvo-i-nadezhnost.html
allnewstroy.ru/vash-byistryiy-put-k-novomu-diplomu
Привет!
Приобрести диплом о высшем образовании
Наша компания предлагает быстро и выгодно приобрести диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Данный документ способен пройти лубую проверку, даже при помощи специального оборудования. Достигайте своих целей быстро и просто с нашим сервисом.
Где купить диплом по актуальной специальности?
vaeaem.profiforum.ru/t3822-topic#7107
forumjustwoman.getbb.ru/viewtopic.php?f=43&t=941
alanyatoday.ru/users/76
worksale777.blogspot.com/2024/06/blog-post_30.html
promintern.listbb.ru/viewtopic.php?f=16&t=474
Привет, друзья!
Заказать документ института можно в нашем сервисе.
ast-diplom.com/kupit-diplom-kazan
Здравствуйте!
Купить диплом ВУЗа.
santa4.su/gallery/image/254-kak-podyskat-nadezhnyy-magazin-s-obshirnym-vyborom-diplomov/
Привет!
Купить документ университета вы можете у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы старого образца.
gerosland.com/read-blog/167
paulikipedia.ru/index.php/Купите_диплом_и_начните_новую_жизнь
kinopuk.ru/viewtopic.php?id=9078#p56655
talkitter.com/create-blog/
ya.9bb.ru/viewtopic.php?id=5924#p11405
Привет, друзья!
Где купить диплом специалиста?
Купить диплом любого университета.
formulaf1.ru/kupite-diplom-i-otkroyte-novyie-gorizontyi
Top News Sites for article post
dailymirrornewstoday.com
dailystarnewstoday.com
dailytelegraphnewstoday.com
dutchnewstoday.com
dwnewstoday.com
europeannewstoday.com
Don’t hasitate to conatct us.
Пошаговая инструкция по безопасной покупке диплома о высшем образовании
diploms-x24.ru/kupit-diplom-vracha
Привет!
Приобрести диплом о высшем образовании.
65b7bc92a079b.site123.me/Блог/Большой-каталог-документов-в-известном-магазине
Здравствуйте!
Купить документ университета вы можете в нашей компании в Москве.
diplomyx.com/kupit-diplom-kandidata-nauk
Привет, друзья!
Заказать диплом любого ВУЗа.
iqtorg.ru/forum/messages/forum2/topic555/message615/?result=new#message615
Хорошей учебы!
Приобрести диплом любого ВУЗа.
stroimsa.forum2x2.ru/login
income.forum2x2.ru/login?redirect=/u347
odnopolchane.net/forum/member.php?u=546804
avtobestnews.ru/vash-put-k-vyisshemu-obrazovaniyu-byistro-i-legalno
sharecovid19story.com/viewtopic.php?f=11&t=1258891&p=2635086#p2635086
Привет, друзья!
Заказать диплом о высшем образовании.
sonnick84.blog5star.com/28594627/%D0%9D%D0%B0-%D1%87%D1%82%D0%BE-%D0%B8%D0%BC%D0%B5%D0%BD%D0%BD%D0%BE-%D0%B2%D0%BD%D0%B8%D0%BC%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BE%D0%B1%D1%80%D0%B0%D1%89%D0%B0%D1%82%D1%8C-%D0%BF%D1%80%D0%B8-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8
Привет, друзья!
Мы можем предложить дипломы.
kh.txi.ru/forum/index.php?
klinlife.ru/forums/index.php?/topic/37385-kupit-diplom-bez-posrednikov-legko-i-bezopasn/
russianecuador.com/forum/member.php?u=13207
avrorp.getbb.ru/viewtopic.php?f=183&t=696
nagaevo.ekafe.ru/viewtopic.php?f=86&t=2512
Здравствуйте!
Купить диплом о высшем образовании.
xn—-8sbjufbbcmolbtcflf.xn--p1ai/gallery/image/1494-широкий-выбор-документов-в-популярном-магазине/?context=new
Привет!
Приобрести документ ВУЗа вы сможете у нас. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ. Вы получите диплом по любым специальностям, любого года выпуска, в том числе документы СССР. Даем гарантию, что при проверке документов работодателями, подозрений не появится.
biznas.com/Biz-postsm333690_Default.aspx#post333690
pakhie.com/blogs/8911/Советы-профессионала-что-помогут-быстро-приобрести-диплом
ambaland.com/blogs/3421/Находим-проверенный-и-надежный-магазин-для-покупки-документов
wiki.wonikrobotics.com/AllegroHandWiki/index.php/Special:AWCforum/st/id15466
gtago.ru/gallery/image/23-katalog-i-sposoby-dostavki-v-internet-magazine-zakazyvaem-attestat/?context=new
Привет!
Купить документ университета можно в нашей компании.
ast-diplomas.com/kupit-diplom-kandidata-nauk
Привет!
Мы предлагаем дипломы любой профессии по приятным тарифам.
http://www.lcwhost.org/events/event/11-какие-онлайн-магазины-с-документами-на-текущий-момент-существуют/
Привет, друзья!
Приобрести документ о получении высшего образования можно у нас.
ast-diplom24.ru/kupit-diplom-sankt-peterburg
Успехов в учебе!
Привет!
Купить диплом любого университета
Мы предлагаем быстро и выгодно купить диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями официальных лиц. Документ пройдет любые проверки, даже при использовании специфических приборов. Решайте свои задачи быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
sonnick84.full-design.com/Советы-специалиста-которые-возможность-дадут-легко-купить-документы-71044966
http://www.sledopit.club/wiki/index.php/Какие_онлайн_магазины_с_дипломами_на_текущий_день_имеются?
alex-neil.ru/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=241
rcoz9dxps.prublogger.com/27889603/Советы-что-позволят-найти-надежный-онлайн-магазин-с-дипломами
loveyou.az/read-blog/173
Привет, друзья!
Приобрести диплом о высшем образовании.
t67747az.beget.tech/2024/07/04/zachem-seychas-pokupayut-attestaty-i-diplomy-v-seti-internet.html
lawtech.ru/subscribe/25347-07072024
sonnick84.dm-blog.com/28321099/Выбираем-проверенный-интернет-магазин-для-приобретения-диплома
astart.pl/index.php?/gallery/image/5-для-чего-в-наше-время-покупают-аттестаты-и-дипломы-в-сети-интернет/
artisthub.mn.co/posts/61724197
Здравствуйте!
Купить документ о получении высшего образования.
worksale.jofo.me/2279430.html?_ga=2.192198185.2038458334.1720956820-604767625.1720956820
driveme.rusff.me/viewtopic.php?id=2177#p105233
orderviewdocs.online/doku.php?id=купите_диплом_и_достигните_своих_целей
amengram.com/blogs/378/Получите-диплом-без-лишних-забот-и-усилий
diigo.com/item/note/8p2f0/3mv5?k=8d05ab431a69cb27d0d3275600332235
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
last news about raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
Добрый день!
Купить диплом любого ВУЗа:
старый.ркэ.рф/index.php/component/k2/itemlist/user/127180
handgemaaktplaats.nl/user/profile/77898
bestnet.ru/support/forum/index.php?PAGE_NAME=profile_view&UID=137130
b24activities.ru/club/forum/messages/forum4/topic76/message138/?result=reply#message138
arkosgold.ru/index.php?subaction=userinfo&user=ajegeq
купить диплом во владивостоке купить диплом во владивостоке .
Привет!
Заказать документ ВУЗа
ast-diploms.com/kupit-diplom-omsk
купить диплом в челябинске mandiplomik.ru .
Здравствуйте!
Заказать диплом университета
Мы предлагаем выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями официальных лиц. Документ способен пройти любые проверки, даже при помощи специальных приборов. Решайте свои задачи быстро и просто с нашей компанией.
Где приобрести диплом специалиста?
3drus.ru/forum/topic_34806
vip.9bb.ru/viewtopic.php?id=5959#p9901
mosday.getbb.ru/viewtopic.php?f=12&t=1059
avtolux48.ru/people/user/374/blog/7556/
zxz.listbb.ru/viewtopic.php?f=7&t=1416
Привет!
Где приобрести диплом по нужной специальности?
Купить диплом о высшем образовании.
montrealpal.com/read-blog/927
Привет!
Заказать документ о получении высшего образования.
avva.getbb.ru/viewtopic.php?f=3&t=583
deadreckoninggame.com/index.php/Купить_диплом_–_залог_вашего_успеха
d91652pj.beget.tech/2024/07/12/oficialnye-diplomy-na-zakaz.html
forums.unigild.com/index.php?/topic/16374-высшее-образование-для-всех/
2cool.ru/qiwi-f215/nadejnoe-oformlenie-diploma-za-korotkiy-srok-t3807.html
Здравствуйте!
Купить документ о получении высшего образования можно у нас в столице. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы СССР.
opengadjet.ru/legkiy-sposob-poluchit-diplom-byistro-i-prosto
http://www.pets-ural.ru/content/forum/viewtopic.php?p=79512#79512
datasphere.ru/club/user/15/blog/
sklad-slabov.ru/forum/user/8261/
x91392sl.beget.tech/2024/07/11/oformlenie-diploma-pod-klyuch-bystro-i-nadezhno.html
Добрый день!
Аттестат школы купить официально с упрощенным обучением в Москве
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge В
Добрый день!
Приобрести диплом любого университета.
films.name/viewforum.php?f=143
Хорошей учебы!
Привет, друзья!
Мы готовы предложить документы техникумов, расположенных в любом регионе Российской Федерации. Вы можете приобрести качественный диплом от любого учебного заведения, за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты выпускаются на бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они будут заверены всеми необходимыми печатями и подписями.
ремонт-оптом.рф/club/user/7/blog/2127/
Наш сервисный центр предлагает надежный мастерская по ремонту духовых шкафов рядом всех типов и брендов. Мы знаем, насколько необходимы вам ваши духовки, и обеспечиваем ремонт наилучшего качества. Наши опытные мастера работают быстро и аккуратно, используя только качественные детали, что предоставляет долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются пользователи духовок, включают неисправности термостата, поломку таймера, треснувшую дверцу, проблемы с контроллером, ошибки вентиляционной системы и повреждения электроники. Для устранения этих поломок наши профессиональные техники оказывают ремонт нагревательных элементов, термостатов, таймеров, дверец, контроллеров, вентиляторов и электроники. Доверив ремонт нам, вы обеспечиваете себе качественный и надежный официальный ремонт духовых шкафов.
Подробная информация доступна на сайте: https://remont-duhovyh-shkafov-ace.ru
Смотреть фильм https://hdrezka.host/ онлайн любого года выпуска, в том числе новинки 2024 года, в отличном качестве, без регистрации у нас на сайте. Подборки по всем жанрам, ТОПы фильмов за все годы, коллекции любых видов и жанров. Лучшие из выбора зрителей – вы найдете все для приятного времяпрепровождения.
На сайте https://telezghki-instrument.ru ознакомьтесь с информацией о том, какую тележку, предназначенную для инструментов, лучше выбрать и купить. Перед вами типы такого оборудования, а также достоинства и особенности каждого типа. Так вы узнаете все необходимое о тележках с ящиками, открытых тележках, о правилах выбора инструментальной тележки. Здесь вы найдете самые ценные, увлекательные и содержательные рекомендации, которые действительно будут вам полезны. Имеются данные и про материал изготовления и многое другое.
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
eurodelo.ru/vash-shans-na-vyisshee-obrazovanie-kupit-diplom
Technical Specifications
ivermectin purchase online
Привет, друзья!
Официальная покупка диплома вуза с упрощенной программой обучения
bbs.airav.cc/home.php?mod=space&uid=2090208
Будем рады вам помочь!.
Привет!
Заказать диплом университета.
yooubook.com/blogs/2198/Надежный-и-проверенный-магазин-с-обширным-каталогом-документов
leenkup.com/read-blog/16623
sonnick84.pages10.com/Советы-эксперта-что-помогут-недорого-приобрести-диплом-63971765
getdlight.com/en/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=149
sonnick84.blogsmine.com/28664750/Дипломы-и-аттестаты-выгодные-цены
Здравствуйте!
Как купить аттестат 11 класса с официальным упрощенным обучением в Москве
houseofnails.store/2024/06/30/диплом-самара-купить/
Здравствуйте!
Приобрести документ университета.
orderviewdocs.online/doku.php?id=получите_диплом_в_любое_время
genshtab.flybb.ru/viewtopic.php?f=19&t=3063&sid=22b6a541adad84c4be375afe08939a25
1776reloaded.us/blogs/77/Получите-диплом-без-лишних-забот-и-усилий
jeepgarage.ru/forum/topic.php?forum=24&topic=757
frank-shkola.ru/forum/messages/forum1/topic441/message455/?result=new#message455
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
last news about messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
Добрый день!
Мы можем предложить документы ВУЗов, расположенных на территории всей Российской Федерации. Вы сможете заказать диплом за любой год, включая сюда документы СССР. Документы печатаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые невозможно отличить от оригинала. Документы заверяются необходимыми печатями и подписями.
http://www.grimdice.ru/index.php?/gallery/image/2-%D0%BD%D0%B8%D0%B7%D0%BA%D0%B8%D0%B5-%D1%80%D0%B0%D1%81%D1%86%D0%B5%D0%BD%D0%BA%D0%B8-%D0%B8-%D0%B8%D0%B4%D0%B5%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B9-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD/
Как правильно купить диплом колледжа и пту в России, подводные камни
diplomyx24.ru/kupit-diplom-krasnodar
Приобрести диплом университета.
forum.analysisclub.ru/index.php/topic,200459.new.html#new
mamuli.club/forum/obovsem/add
karasteamfulldmroleplay.getbb.ru/viewtopic.php?f=62&t=881
dogovor.top/wiki/Легальная_Покупка_Дипломов:_Доступно_и_Надежно
shuvalduet.getbb.ru/viewtopic.php?f=3&t=576
Привет, друзья!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
speedagecourier.com/купить-диплом-гитр-или-любого-вуза-рос/
Срочно Требуются: Курьеры-регистраторы
Ищем активных граждан РФ, живущих в Москве и области!
А так же, принимаются люди, для работы, проживающие в других регионах рф,
кроме (северного Кавказа)
Заработок от 3000 тыс. до 7000 тыс. за каждый выезд.
Совмещай работу с другими делами – гибкий график!
Твоя задача – регистрация компаний. Просто и выгодно!
Оплата сразу после выполнения задания!
Подходишь по возрасту (18-60 лет)Присоединяйся!
Начни зарабатывать больше прямо сейчас – ждем именно тебя!
А так же, требуются люди, на удаленную работу, по поиску и подбору
директоров (Курьеров-регистраторов) зп, от 5000 тысяч рублей, за подобранного человека.
#работа #вакансия #Москва #курьер #регистратор #заработок #график #подработка
Начни зарабатывать больше прямо сейчас – ждем именно тебя!
https://chat.whatsapp.com/InLwqrVeXucCbCTqxkwrSo
Здравствуйте!
Купить диплом любого университета.
void.menu/index.php?/gallery/image/116-огромный-каталог-документов-в-популярном-магазине/
Добрый день!
Мы готовы предложить дипломы.
uscgq.com/forum/posts.php?forum=general&id=259092
karasteamfulldmroleplay.getbb.ru/viewtopic.php?f=62&t=893
2cool.ru/posting.php?mode=post&f=215
deviva.ru/viewtopic.php?id=9083#p62015
psorum.ru/member.php?u=4348
Добрый день!
Мы предлагаем документы техникумов, которые находятся в любом регионе Российской Федерации. Вы можете приобрести диплом от любого учебного заведения, за любой год, включая документы СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высшего качества. Это дает возможности делать государственные дипломы, которые не отличить от оригинала. Они будут заверены необходимыми печатями и штампами.
modelacademy.mn.co/posts/61838216
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
last news about marcus wendel!
wendel
<a href=https://c.t.tailtarget.com/clk/TT-10946-0/8PONWD6OEB/tZ=buster]/click=plarium.com/forum/en/raid-shadow-legends/676_tavern/1433693_do-you-feel-battle-passes-are-just-the-norm-now-in-games>wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
Привет!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
social.ghame.org/read-blog/6793_proverennyj-i-nadezhnyj-magazin-s-bolshim-assortimentom-diplomov.html
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
last news about cristiano ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
Ищете, где можно срочно получить займ на карту? Подпишитесь на канал Telegram – займ на карту без долгих проверок ! Здесь вы найдете все актуальные предложения от МФО, которые выдают займы без отказа и проверки кредитной истории. Малоизвестные компании, готовые выдать деньги даже с просрочками, ждут вас. Узнайте, где можно получить займ под 0% для новых клиентов и какие условия предлагают различные МФО. Канал Telegram – займы на карту для пенсионеров — ваш гид в мире срочных займов. Подпишитесь и решите свои финансовые вопросы быстро и без проблем!
Привет!
Официальная покупка диплома вуза с упрощенной программой обучения
kuvandyk.ru/message.php?msg=151
Рады оказать помощь!
Привет, друзья!
Купить диплом любого университета
Наши специалисты предлагают выгодно и быстро купить диплом, который выполнен на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Диплом способен пройти лубую проверку, даже при использовании профессионального оборудования. Достигайте свои цели быстро и просто с нашими дипломами.
Где купить диплом по нужной специальности?
mamapoltava.listbb.ru/viewtopic.php?f=39&t=4933
zxz.listbb.ru/viewtopic.php?f=7&t=1416
autoprajs.ru/15204.html
ya.10bb.ru/viewtopic.php?id=3615#p6544
pdlspd.listbb.ru/viewtopic.php?f=3&t=409
Привет, друзья!
Где приобрести диплом по необходимой специальности?
Приобрести диплом любого университета.
mongolsmc.listbb.ru/viewtopic.php?f=1&t=396
Здравствуйте!
Мы можем предложить дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
lab.panda-studio.pro/index.php?/gallery/image/116-какие-магазины-с-дипломами-имеются-на-текущий-момент/
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
last news about raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
raphael
Здравствуйте!
Купить документ института можно в нашей компании. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, включая документы образца СССР.
antoinegriezmannclub.com/read-blog/3054
magiclife.ukraine7.com/t6345-topic#15893
meat.ntnn.ru/personal/profile/index.php?register=yes
domainrama.com/read-blog/914
http://www.les-ailes-chalaisiennes.com/forum/topic/диплом-любой-специальности-качестве/#postid-19484
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
last news about lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
Привет!
Как правильно приобрести диплом колледжа или ПТУ в России, важные моменты
preceptor.flybb.ru/viewtopic.php?f=13&t=9891
Поможем вам всегда!
Добрый день!
Приобрести диплом о высшем образовании.
kawaa.drake.free.fr/index.php?file=Forum&page=viewtopic&forum_id=1&thread_id=5359
Успехов в учебе!
Здравствуйте!
Купить документ университета
diplomasx24.ru/kupit-diplom-omsk
Привет, друзья!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
rebornrpofficial.com/index.php?/files/file/12-четыре-главных-группы-онлайн-магазинов-реализующих-документы/
Добрый день!
Как безопасно купить диплом колледжа или ПТУ в России, что важно знать
witchvswinx.getbb.ru/viewtopic.php?f=10&t=2944&p=19150#p19150
Рады помочь!.
Наша мастерская предлагает профессиональный сервисный центр по ремонту видеокарт с гарантией различных марок и моделей. Мы знаем, насколько важны для вас ваши графические адаптеры, и готовы предложить сервис первоклассного уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только качественные детали, что гарантирует долговечность и надежность проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются владельцы видеокарт, включают проблемы с вентиляцией, выход из строя памяти, неисправности разъемов, неисправность контроллера и неисправности ПО. Для устранения этих поломок наши профессиональные техники выполняют ремонт системы охлаждения, памяти, разъемов, контроллеров и ПО. Обратившись к нам, вы обеспечиваете себе качественный и надежный сервис ремонта видеокарт на дому.
Подробная информация размещена на сайте: https://remont-videokart-biz.ru
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes last news
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
Привет, друзья!
Аттестат 11 класса купить официально с упрощенным обучением в Москве
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske В
Здравствуйте!
Сколько стоит диплом высшего и среднего образования и как это происходит?
sampnl.listbb.ru/viewtopic.php?f=3&t=484
Рады оказать помощь!
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
last news about messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
messi
Здравствуйте!
Заказать документ института можно у нас в Москве.
diplomasx.com/kupit-diplom-rostov-na-donu
Удачи!
https://www.yaprakcanta.com/index.php?route=journal3%2Fblog%2Fpost&journal_blog_post_id=10
классное порево онлайн классное порево онлайн .
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
last news about kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
Добрый день!
Купить документ о получении высшего образования.
worksale.jofo.me/2279120.html?_ga=2.37554784.1980467973.1720785836-642113533.1720785836
t98223u0.beget.tech/2024/07/16/legalnyy-diplom-bez-lishnih-hlopot-uznayte-kak.html
talkitter.com/create-blog/
moskvic.actieforum.com/t3743-topic#7032
kai87la.flybb.ru/viewtopic.php?f=5&t=416
Привет, друзья!
Мы можем предложить дипломы любых профессий.
berrylib.ru/books/item/f00/s00/z0000024/index.shtml
Поможем вам всегда!.
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
last news about khvicha kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
last news about marcus wendel!
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
wendel
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
last news about cristiano ronaldo
ronaldo
ronaldo
ronaldo
<a href=http://palbang.net/info.php?a%5B%5D=ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
ronaldo
Здравствуйте!
Купить документ о получении высшего образования вы сможете у нас в столице.
diploms-x.com/otzyvy
Хорошей учебы!
Здравствуйте!
Приобрести документ о получении высшего образования можно в нашей компании. Мы предлагаем документы об окончании любых университетов Российской Федерации.
narodovmnogo-omsk.ru/forum/user/4161/
цдод.рф/forum/topic.php?forum=3&topic=724
опт-кирпич.рф/index.php?subaction=userinfo&user=ubitaxos
artem-energo.ru/forums.php?m=posts&q=18303&n=last#bottom
team6seals.free.fr/index.php?file=Members&op=detail&autor=olyxof
Добрый день!
Приобрести документ о получении высшего образования можно в нашей компании в столице.
ast-diplom.com/kupit-diplom-s-registraciej
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
last news about lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
lewandowski
Advanced Tips for Experienced Players
cheap ivermectin
Здравствуйте!
Купить документ института вы имеете возможность в нашем сервисе.
diplomyx.com/kupit-diplom-specialista
https://www.bazaar-turkey.com/index.php?route=journal3%2Fblog%2Fpost&journal_blog_post_id=7
Добрый день!
Купить диплом университета.
65b7bc92a079b.site123.me/Блог/Большой-каталог-документов-в-известном-магазине
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes last news
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
promes
Здравствуйте!
Мы готовы предложить дипломы любой профессии по разумным ценам.
http://www.clubeslotcartrofa.com/купить-диплом-о-вуза/
firmino
firmino
<a href=http://michigangirl.oldiestation.es/php.php?a%5B%5D=firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
last news about firmino roberto
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
Привет!
Заказать документ о получении высшего образования
ast-diplomy.com/kupit-diplom-voronezh
Наша мастерская предлагает высококачественный вызвать мастера по ремонту электросамоката рядом любых брендов и моделей. Мы понимаем, насколько важны для вас ваши электроскутеры, и обеспечиваем ремонт первоклассного уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что обеспечивает долговечность и надежность проведенных ремонтов.
Наиболее частые неисправности, с которыми сталкиваются пользователи электрических самокатов, включают неисправную батарею, неработающий двигатель, сбои контроллера, неисправности тормозной системы и повреждения корпуса. Для устранения этих проблем наши квалифицированные специалисты выполняют ремонт батарей, двигателей, контроллеров, тормозных систем и механических компонентов. Доверив ремонт нам, вы гарантируете себе долговечный и надежный сервисный центр по ремонту электросамокатов на выезде.
Подробная информация доступна на сайте: https://remont-elektrosamokatov-fun.ru
Привет!
Купить документ университета можно у нас.
ast-diploms.com/kupit-diplom-chelyabinsk
купить бланк диплома о высшем образовании mandiplomik.ru .
Здравствуйте!
Купить диплом ВУЗа.
andreieusebiu.net/files/file/44-обширный-ассортимент-документов-в-знаменитом-магазине/
Добрый день!
Реально ли приобрести диплом стоматолога? Основные этапы
landik-diploms-srednee.ru/svidetelstvo-o-razvode В
Добрый день!
Приобретение школьного аттестата с официальным упрощенным обучением в Москве
talkitter.com/read-blog/202613
Поможем вам всегда!
Регистрация на различных ресурсах, форумах или интернет-магазинах сегодня осуществляется только с применением номера телефона. Ранее для этой цели могла использоваться электронная почта, но сегодня правила изменены https://comicsplanet.ru/zachem-nuzhen-virtualnyj-nomer-i-kak-ego-podklyuchit.html
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
last news about kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kane
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
last news about khvicha kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
kvaratskhelia
В сериале “Фоллаут”, представленном на сайте https://fallout-tvseries.com/ мы видим расширение вселенной Fallout, где зрителю предлагается исследовать уникальный лабиринт коридоров и атриумов, а не строго разделенные этажи и уровни. Волт-Тек, корпорация, ответственная за уничтожение НКР, планирует восстановить цивилизацию и получить монополию над Америкой. Убежища, такие как Убежище 31, содержат криокапсулы с менеджерами Волт-Тек, которые будут управлять постъядерной Америкой. Сериал также демонстрирует обычных домашних курочек, переживших ядерную войну без изменений.
Здравствуйте!
Где приобрести диплом по актуальной специальности?
http://www.gamerlaunch.com/community/users/blog/6398497/2285300/особенности-по/?gid=535
Если вам срочно нужны деньги, загляните на канал Telegram – моментальные микрозаймы онлайн ! Здесь вы найдете все МФО, которые предлагают займы на карту без отказа. Малоизвестные компании, готовые выдать деньги даже с плохой кредитной историей и просрочками. Займы доступны круглосуточно и мгновенно. Узнайте, какие МФО дают займы под 0% для новых клиентов и где можно получить деньги без лишних вопросов. Подпишитесь на канал Telegram – моментальные микрозаймы онлайн и решите свои финансовые проблемы быстро и легко!
Привет!
Заказать документ университета можно у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы получите диплом по любым специальностям, включая документы старого образца. Гарантируем, что при проверке документа работодателями, никаких подозрений не возникнет.
Мы предлагаем дипломы любой профессии по разумным ценам. Стоимость может зависеть от конкретной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступны для большого количества граждан.
thenet.work/gallery/image/482-покупаем-диплом-в-проверенном-интернет-магазине-по-выгодной-цене/
Поможем вам всегда!
Start out your account right now to connect with hundreds of professionals in your field!
Also visit my site – 여성 알바
Привет, друзья!
Мы изготавливаем дипломы любых профессий по доступным ценам.
respectmyopinion.com/blogs/26/Проверенный-и-надежный-магазин-с-обширным-ассортиментом-документов
Добрый день!
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Цена зависит от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
animesocial.su/blogs/1639/Как-найти-хороший-интернет-магазин-где-возможно-заказать-диплом
Привет, друзья!
Мы предлагаем документы техникумов, которые расположены на территории всей России. Можно приобрести диплом за любой год, в том числе документы СССР. Дипломы и аттестаты делаются на “правильной” бумаге самого высшего качества. Это дает возможность делать государственные дипломы, не отличимые от оригинала. Документы будут заверены необходимыми печатями и штампами.
foto-passau.com/gallery/image/12-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D1%8B-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%BA%D0%BE%D0%BC%D1%84%D0%BE%D1%80%D1%82%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5/?context=new
[u][b] Здравствуйте![/b][/u]
[b]Мы изготавливаем дипломы[/b] любой профессии по приятным ценам.
[url=http://leicestercityfansclub.com/read-blog/2080_kak-mozhno-budet-kupit-sejchas-kachestvennyj-diplom-v-seti.html/]leicestercityfansclub.com/read-blog/2080_kak-mozhno-budet-kupit-sejchas-kachestvennyj-diplom-v-seti.html[/url]
Добрый день!
Купить документ ВУЗа можно в нашем сервисе.
ast-diplomas24.ru/kupit-diplom-krasnoyarsk
Успехов в учебе!
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
last news about firmino roberto
<a href=http://50carleton.withbob.net/info.php?a%5B%5D=firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
Привет, друзья!
Мы предлагаем документы ВУЗов, расположенных в любом регионе РФ. Вы можете приобрести качественный диплом за любой год, включая сюда документы СССР. Документы выпускаются на бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Документы заверяются необходимыми печатями и штампами.
amengram.com/blogs/358/%D0%9F%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%BB%D1%83%D1%87%D1%88%D0%B5%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-%D0%BF%D0%BE-%D0%B2%D1%8B%D0%B3%D0%BE%D0%B4%D0%BD%D0%BE%D0%B9-%D1%86%D0%B5%D0%BD%D0%B5
Добрый день!
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
http://www.nexuspals.online/blogs/156/Как-выбрать-надежный-интернет-магазин-который-реализует-документы
Здравствуйте!
Купить документ о получении высшего образования.
faithstreamer.com/blogs/3200/Легальный-диплом-без-лишних-хлопот-узнайте-как
sec31.ru/viewtopic.php?f=25&t=675998
borderforum.ru/viewtopic.php?f=7&t=10352
n-staff.ru/forum?mode=edit&type=thread&forum_id=74041
classicalmusicmp3freedownload.com/ja/index.php?title=Идеальный_диплом_за_считанные_дни_–_узнайте_подробности
Здравствуйте!
Купить документ о получении высшего образования можно у нас в столице.
asxdiplomik.com/kupit-diplom-bakalavra-ili-specialista
Здравствуйте!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
dixbe.com/blogs/237/Как-можно-будет-купить-сегодня-качественный-диплом-в-сети-интернет
Добрый день!
Мы предлагаем документы техникумов, расположенных в любом регионе РФ. Можно заказать диплом за любой год, указав подходящую специальность и хорошие оценки за все дисциплины. Документы печатаются на бумаге самого высшего качества. Это позволяет делать государственные дипломы, которые не отличить от оригинала. Они заверяются необходимыми печатями и штампами.
9pj7tneu1.blogoxo.com/28388931/%D0%9F%D0%BE%D0%B4%D1%80%D0%BE%D0%B1%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
На сайте https://profmosreshetka.ru вы сможете получить всю необходимую информацию, которая касается заказа решеток на окна. Все конструкции выполняются из качественных, современных материалов. А замер, доставка решений осуществляются абсолютно бесплатно. С расценками ознакомьтесь прямо сейчас. Все цены снижены до конца июля, а потому спешите воспользоваться услугами прямо сейчас. Компания отличается большим опытом работы – более 10 лет. А если закажете 2 решетки, то вам будет предоставлена скидка в 20%.
Online casino games have surged in popularity due to their convenience and the immersive experience they offer.
ivermectin online
Наша мастерская предлагает надежный сервисный ремонт электровелосипеда на дому различных марок и моделей. Мы понимаем, насколько необходимы вам ваши электровелосипеды, и обеспечиваем ремонт первоклассного уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только качественные детали, что обеспечивает длительную работу наших услуг.
Наиболее частые неисправности, с которыми сталкиваются обладатели электробайков, включают неисправную батарею, проблемы с мотором, сбои контроллера, проблемы с тормозами и повреждения корпуса. Для устранения этих неисправностей наши квалифицированные специалисты оказывают ремонт батарей, двигателей, контроллеров, тормозных систем и механических компонентов. Обращаясь в наш сервисный центр, вы гарантируете себе долговечный и надежный вызвать мастера по ремонту электровелосипеда в москве.
Подробная информация размещена на сайте: https://remont-elektrovelosipedov-gem.ru
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным ценам.
metalxsports.com/купить-диплом-в-ижевске/
Здравствуйте!
Заказать диплом о высшем образовании:
shkola.mitrofanovka.ru/index.php?subaction=userinfo&user=epefediz
rytof.ru/node/16119
longlive.com/node/1379
radshir.com/products/index.php?subaction=userinfo&user=avohykire
marandola.net/dokuwiki/doku.php?id=diplomandoci
https://buycloned-cards.cvv2cvc.com
Item 1 Card Total Balance: $3 100 – Price $ 110.00
Item 3 Cards Total Balance $9 600 – Price $ 180.00
Item PayPal Transfers $500 – Price $ 49.00
Item PayPal Transfers $2000 – Price $ 149.00
Item Western Union Transfers $ 1000 – Price $ 99.00
Item Western Union Transfers $ 300 – Price $ 249.00
*Prices on the website may vary slightly
http://buy-cloned-cards.cvv2cvc.com
Привет!
Заказать документ о получении высшего образования.
big.bestforums.org/viewtopic.php?f=12&t=5141
justvoip.listbb.ru/viewtopic.php?f=2&t=457
vnuci.listbb.ru/viewtopic.php?f=2&t=544
wmrp.listbb.ru/viewtopic.php?f=51&t=675
sovetushka.forum2x2.ru/t28893-topic#63665
Привет!
Легальная покупка школьного аттестата с упрощенной программой обучения
barranca21.com/купить-диплом-пту/
219news.com
investnews24.net
Добрый день!
Заказать документ о получении высшего образования вы сможете у нас в Москве.
diplomyx.com/kupit-diplom-sankt-peterburg
Хорошей учебы!
Привет!
Купить диплом университета.
vocal.com.ua/node/62301
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Детская одежда оптом из Турции
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
детская одежда оптом
Добрый день!
Диплом ВУЗа купить официально с упрощенным обучением в Москве
vatrusha.maxbb.ru/viewtopic.php?f=2&t=691
Рады оказать помощь!
Привет, друзья!
Купить диплом университета.
http://www.printsstars.ru/communication/forum/index.php?PAGE_NAME=profile_view&UID=201303
Удачи!
Стоимость дипломов высшего и среднего образования и как избежать подделок
diploms-x.com/kupit-diplom-omsk
Заказать диплом университета.
meetspot.com/blogs_write.php?id=
liveinternet.ru/users/worksale/post506327043/
yourealtynews.ru/vash-nastoyashhiy-diplom-legalno-i-byistro
umorforme.ru/garantiya-podlinnosti-pokupka-diplomov-legalno
wallazz.com/blogs/205592/Купить-диплом-все-что-вам-нужно-знать
Привет!
Купить документ о получении высшего образования можно у нас в столице.
diplomyx.com/kupit-diplom-krasnoyarsk
Успехов в учебе!
Добрый день!
Приобрести документ о получении высшего образования можно в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов РФ.
pr.lgubiz.net/bbs/board.php?bo_table=free&wr_id=214714
coool-craft.4fan.cz/profile.php?lookup=10021
http://www.alpea.ru/forum/user/25727/
forum.e4pool.com/viewtopic.php?p=6722#p6722
forum.gtasiberia.ru/index.php?/topic/22713-купить-диплом-v416l/
Agineer AI – все нейросети онлайн на русском языке и бесплатно!
Главное удобство и преимущество нашего сервиса в том,
что с помощью технологий
искусственного интеллекта, им максимально оперативно
создаются эффективные тексты
и качественные изображения самого различного назначения и в любых объемах для всевозможных сайтов, интернет-магазинов или маркетплейсов нейросеть онлайн бесплатно
Нейросеть на русском создаст для
вас качественный текст с уникальностью до 100% за считанные
мгновения, используя инновационные алгоритмы\технологии online генерации
текстов.
Это сэкономит ваше время и деньги, освободит
вас от необходимости содержать штат копирайтеров и контент-менеджеров.
Поможет вам в короткие сроки запустить интернет-магазин и ускорить ваши продажи.
На сегодняшний день для работы доступны ai нейросети – ChatGPT-3.5Turbo и ChatGPT- 4Omni.
С их помощью вы без особых усилий создадите контент, отвечающий любым требованиям,
а русскоязычная нейросеть
учтет ваши индивидуальные запросы и использует предложенные вами ключевые слова для лучшего
продвижения.
Бесплатные онлайн-чаты с ИИ
Обучение нейросети происходит на основании больших объёмов информации, касающейся логики построения всевозможных текстов и создания различных
изображений, для бизнеса в том числе.
Это даёт возможность на
выходе получать контент, отвечающий всем необходимым условиям и параметрам.
Привет, друзья!
Легальная покупка диплома о среднем образовании в Москве и регионах
technoevents.ru/diplom-lyuboy-stepeni-i-spetsialnosti-dostupno-kazhdomu
Рады оказаться полезными!
Привет, друзья!
Мы изготавливаем дипломы.
щербиновскийрайон.рф/users/160
make-coin.ru/ofitsialnyie-diplomyi-garantiya-kachestva-i-podlinnosti
rcdrift.ru/forum/member.php?u=21074
good-serial.ru/2024/07/kupit-diplom-opyit-i-professionalizm/
bbs.heyshell.com/forum.php?mod=viewthread&tid=28269&extra=
Привет!
Заказать документ ВУЗа вы имеете возможность в нашей компании в Москве.
ast-diplomas.com/kupit-diplom-o-srednem-obrazovanii
Успехов в учебе!
Привет, друзья!
Мы готовы предложить документы ВУЗов, расположенных на территории всей России. Вы можете приобрести качественный диплом за любой год, включая сюда документы СССР. Документы печатаются на “правильной” бумаге самого высокого качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Они заверяются всеми требуемыми печатями и подписями.
rusere.ru/communication/forum/messages/forum11/message3689/2975-priobretaem-diplom-v-izvestnom-internet-magazine-po-vygodnoy-tsene?result=new
Здравствуйте!
Приобрести диплом ВУЗа.
электрификация.рф/blogs/1/bystryy-poisk-onlayn-magazina-chto-realizuet-diplomy.php
Здравствуйте!
Мы предлагаем дипломы любых профессий по приятным тарифам.
dsac.es/купить-диплом-рпа/
Добрый день!
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
http://www.brodyaga.org/club/user/110627/blog/6166
Будем рады вам помочь!.
Здравствуйте!
Приобрести диплом ВУЗа.
upirata.ru/index.php?/gallery/image/12-как-найти-проверенный-онлайн-магазин-с-обширным-каталогом-дипломов/
На сайте https://yogatot.ru/ запишитесь в студию йоги. Здесь самые разные практики, включая хатха-йогу, йогатерапию, аэройогу. Все практики максимально полезны для души и тела. Они помогают расслабиться, получить гармонию с собой и окружающим миром. В студиях царит приятная атмосфера, все настроено на получение ярких, приятных эмоций. Вы сразу же почувствуете, что настроение улучшилось, появилось умиротворение. Также всем желающим доступна и «горячая йога», которая проходит в теплом, уютном зале.
Здравствуйте!
Заказать диплом университета.
flerus-shop.hcp.dilhost.ru/club/user/3/forum/message/861/857/
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность у нас. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы получите диплом по любой специальности, включая документы старого образца. Гарантируем, что в случае проверки документов работодателями, каких-либо подозрений не появится.
vip.7bb.ru/viewtopic.php?id=3028#p7121
mdkl.ru/blogs/9230/За-счет-чего-магазины-с-дипломами-так-популярны-и-востребованы
http://www.leenkup.com/read-blog/16636
academy4elements.mybb.ru/viewtopic.php?id=949#p2083
ya.9bb.ru/viewtopic.php?id=5883#p11350
Привет!
Приобрести документ о получении высшего образования вы можете у нас в Москве.
ast-diploms.com/kupit-diplom-tehnikuma-kolledzha
Наши специалисты предлагает надежный вызвать мастера по ремонту электронной книги в москве всех типов и брендов. Мы понимаем, насколько необходимы вам ваши цифровые книги, и готовы предложить сервис первоклассного уровня. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что гарантирует длительную работу выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются пользователи eBook-ридеров, включают поврежденный экран, поломку аккумулятора, программные сбои, неисправности разъемов и неисправности контроллера. Для устранения этих неисправностей наши опытные мастера проводят ремонт экранов, батарей, ПО, разъемов и контроллеров. Доверив ремонт нам, вы получаете качественный и надежный сервис ремонта электронной книги рядом.
Подробная информация доступна на сайте: https://remont-elektronnyh-knig-hit.ru
Здравствуйте!
Купить диплом о высшем образовании
Наши специалисты предлагают максимально быстро купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Данный диплом пройдет любые проверки, даже при использовании специальных приборов. Достигайте своих целей быстро и просто с нашими дипломами.
Где купить диплом специалиста?
мкр-красногорский.рф/gallery/image/1502-высокая-популярность-и-востребованность-магазинов-с-дипломами/?context=new
vipka.mybb.ru/viewtopic.php?id=2881#p5045
http://www.eruptz.com/read-blog/3360_chto-potrebuetsya-iz-tehniki-dlya-sozdaniya-kachestvennogo-diploma.html
iaescortsmap.ixbb.ru/viewtopic.php?id=105#p105
fforum.ixbb.ru/viewtopic.php?id=188#p4066
Привет!
Купить документ института можно у нас в столице. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить необходимый диплом по любой специальности, включая документы образца СССР. Гарантируем, что в случае проверки документа работодателями, подозрений не появится.
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным тарифам. Стоимость будет зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для покупателей адекватную политику тарифов. Важно, чтобы документы были доступными для подавляющей массы граждан.
ebonyfaces.com/blogs/36/Быстро-заказываем-документы-в-лучшем-онлайн-магазине-Russian-Diplom
Окажем помощь!
Привет!
Как официально купить аттестат 11 класса с упрощенным обучением в Москве
mykinotime.ru/vash-diplom-kachestvo-i-autentichnost/
Привет, друзья!
Приобрести диплом университета.
dervislergrup.com/events/event/10-obsirnyi-katalog-dokumentov-v-izvestnom-internet-magazine/
Safety is paramount when playing online games. Players should ensure they are playing on reputable platforms
ivermectin purchase online
Привет!
Заказать документ университета вы имеете возможность в нашем сервисе.
ast-diploms.com/kupit-diplom-perm
Привет, друзья!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов России.
vestiinform.ru/forums/topic/kupit-diplom-czena-o699z/
miupsik.ru/forums/showthread.php?tid=37973
netl.free.fr/index.php?file=Members&op=detail&autor=eganofa
nnklad.ru/viewtopic.php?f=4&t=1707
wennw.com/member.asp?action=view&memName=awidego
Привет, друзья!
Приобрести документ ВУЗа.
forummichiganrp.moibb.ru/viewtopic.php?f=21&t=442
burgasdent.listbb.ru/viewtopic.php?f=3&t=398
myfootballday.ru/zakazhite-diplom-pryamo-seychas-i-nachnite-novuyu-kareru
forum-nine.mirbb.com/t11758-topic#31170
politictoday.ru/diplom-lyuboy-spetsialnosti-kachestvenno-i-byistro
сколько стоит поддон газоблока https://gazobeton-moskow.ru/
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
last news about mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
[u][b] Здравствуйте![/b][/u]
Мы изготавливаем [b]дипломы[/b] любой профессии по доступным ценам. [b]Цена[/b] зависит от конкретной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступны для большинства граждан.
[url=http://bookmarksaifi.com/story17087420/где-купить-диплом/]bookmarksaifi.com/story17087420/где-купить-диплом[/url]
Медицинский центр Москва cecilplus.ru
В настоящий момент медицина в РФ развивается стремительно. Это очень хорошо, но также стало работать много поликлиник, которые предоставляют некачественные услуги. Хотим познакомить Вас с клиникой «Сесиль», которая осуществляет работу уже более двадцати лет, имеет отличную репутацию и штат настоящих специалистов.
По запросу гинекология москва клиника мы Вам с удовольствием окажем помощь. Представляем консультации, программное лечение и диагностику по различным направлениям. В их числе: геронтология, терапия, невролгия-нейрофизиология, ревматология, педиатрия и многие другие. По возникшим вопросам звоните по номеру телефона +7(499)705-04-19 или оформите обратный звонок на ресурс сайте cecilplus.ru уже сегодня. Также есть интернет запись и оплата приема для Вашего удобства.
Мы расположены по адресу: г. Москва, ул. Чаплыгина, д. 6, м. Чистые пруды. График работы с пн по сб с 9:00 до 21:00. Также на указанном сайте Вы можете посмотреть цены на наши услуги. Некоторые услуги могут быть представлены с выездом на Ваш адрес, требуется уточнить у специалиста.
Если Вы планировали найти энцефалограмма мозга в сети интернет, то вы на нужном пути. Наши специалисты на cecilplus.ru непременно Вам помогут, ведь у них колоссальный опыт и постоянные повышения квалификации. Будем рады Вам оказать помощь обрести здоровье, побороть болезнь и жить счастливой жизнью!
Здравствуйте!
Как получить диплом стоматолога быстро и официально
allukrnews.ru/vash-put-k-uspehu-kupit-diplom/
locowin casino
Регистрация на различных ресурсах, форумах или интернет-магазинах сегодня осуществляется только с применением номера телефона. Ранее для этой цели могла использоваться электронная почта, но сегодня правила изменены http://www.vehicleskins.com/memberlist.php?mode=joined&order=ASC&start=240500
Здравствуйте!
Приобрести диплом ВУЗа.
myparea.mn.co/posts/61591763
familylevel.com/blogs/163/Выбираем-проверенный-и-надежный-магазин-с-дипломами-и-аттестатами
fishjines.mn.co/posts/61837908
sonnick84.blog5star.com/28611321/Что-потребуется-из-оборудования-для-создания-документов
edusocial.online/blogs/117/Ищем-надежный-онлайн-магазин-с-аттестатами-и-дипломами
Привет, друзья!
Купить документ института вы сможете у нас. Мы предлагаем документы об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, включая документы старого образца. Даем гарантию, что в случае проверки документов работодателем, подозрений не возникнет.
metaseamix.com/blogs/420/Огромная-популярность-магазинов-что-предлагают-документы
kondrateff.5bb.ru/viewtopic.php?id=6763#p12662
sharaepewixu.iamarrows.com/nahodim-proverennyj-onlajn-magazin-dla-pokupki-diploma
chumcity.xyz/read-blog/1608
odinzovo.rusff.me/viewtopic.php?id=4843#p8182
Привет, друзья!
Купить документ института.
antennastar.com/blogs/540/Надежные-дипломы-для-вашего-успеха
safdfpb.ixbb.ru/viewtopic.php?id=116#p116
asepbook.com/read-blog/4328
wheeoo.com/read-blog/14077
entrainment.listbb.ru/viewtopic.php?f=96&t=24257
купить диплом университета в нижнем тагиле diploms-x.com .
Привет, друзья!
Легальная покупка школьного аттестата с упрощенной программой обучения
vv.flybb.ru/viewtopic.php?f=23&t=2245&sid=9647d00e6fb5c37ea76a5b4d02fd4808
Поможем вам всегда!
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность в нашем сервисе. Мы предлагаем документы об окончании любых университетов РФ.
biyografiforum.10tl.net/newthread.php?fid=124
duadniche.co.kr/bbs/board.php?bo_table=free&wr_id=1428403
georgiantheatre.ge/index.php?subaction=userinfo&user=umazygot
region-standart.ru/guestbook/?1707835084
http://www.miranetwork.it/index.php?option=com_k2&view=itemlist&task=user&id=446408
Здравствуйте!
Мы можем предложить документы ВУЗов, которые расположены в любом регионе РФ. Вы можете приобрести качественный диплом за любой год, указав подходящую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Документы будут заверены всеми необходимыми печатями и подписями.
iloveyouclub.net/blogs/1915/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%B1%D1%83%D0%B4%D0%B5%D1%82-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
alfardanmotorcycles.com/диплом-техникума-колледжа-ссср-фото/
Привет!
Где и как купить диплом о высшем образовании без лишних рисков
http://www.nitrnd.com/blogs/150402/Ћегкий-—пособ-ѕолучить-?иплом
Здравствуйте!
Купить диплом университета
Наши специалисты предлагают выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями официальных лиц. Диплом способен пройти любые проверки, даже с применением специально предназначенного оборудования. Достигайте цели быстро и просто с нашей компанией.
Где заказать диплом по нужной специальности?
a90275db.beget.tech/2024/07/07/faq-i-sluzhba-podderzhka-zakazyvaem-diplom-v-seti-internet.html
dailygram.com/blog/1304353/купить-официальный-диплом-быстро-и-легально/
logan.in.ua/people/user/7276/blog/7932/
автомедведь.рф/club/user/8729/blog/193091/
allonlinesport.ru/vyisshee-obrazovanie-dlya-vseh-legalno-i-udobno/
Привет, друзья!
Купить документ о получении высшего образования вы можете в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы получите необходимый диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что при проверке документа работодателями, подозрений не появится.
Мы изготавливаем дипломы любой профессии по доступным ценам. Цена может зависеть от определенной специальности, года получения и университета. Всегда стараемся поддерживать для клиентов адекватную политику цен. Важно, чтобы дипломы были доступны для большого количества граждан.
brand-street.ru/tags/трендовый+индикатор/index.html
Рады оказать помощь!
Добрый день!
Заказать документ о получении высшего образования
diplomasx24.ru/kupit-diplom-krasnoyarsk
Здравствуйте!
Купить документ о получении высшего образования.
ukrevent.ru/osushhestvite-mechtu-poluchite-diplom-byistro-i-bez-problem/
trum.flybb.ru/viewtopic.php?f=15&t=4715
animesocial.su/blogs/3373/Настоящий-диплом-для-успешной-карьеры-просто-и-доступно
mafiaclans.ru/viewtopic.php?f=43&t=7590
doomelang.com/read-blog/7462
Наша мастерская предлагает профессиональный качественный ремонт фотоаппаратов различных марок и моделей. Мы осознаем, насколько значимы для вас ваши камеры, и готовы предложить сервис наилучшего качества. Наши квалифицированные специалисты работают быстро и аккуратно, используя только оригинальные запчасти, что предоставляет надежность и долговечность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются пользователи камер, включают повреждения линз, проблемы с затвором, поломку экрана, проблемы с питанием и ошибки ПО. Для устранения этих поломок наши опытные мастера оказывают ремонт объективов, затворов, экранов, батарей и ПО. Доверив ремонт нам, вы гарантируете себе надежный и долговечный починить фотоаппарат на выезде.
Подробная информация доступна на сайте: https://remont-fotoapparatov-ink.ru
Привет, друзья!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
landik-diploms-srednee.ru/kupit-diplom-v-omske В
Привет, друзья!
Мы изготавливаем дипломы любой профессии по выгодным ценам.
hpconsultants.nl/2024/06/30/медицинский-сертификат-специалиста/
Здравствуйте!
Мы готовы предложить документы ВУЗов, которые расположены на территории всей России. Можно приобрести качественный диплом за любой год, включая сюда документы старого образца СССР. Дипломы и аттестаты выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они будут заверены необходимыми печатями и подписями.
cm6b3uirz.blog2learn.com/76431096/%D0%9A%D0%B0%D0%BA-%D0%B2%D0%BE%D0%B7%D0%BC%D0%BE%D0%B6%D0%BD%D0%BE-%D0%BD%D0%B5%D0%B4%D0%BE%D1%80%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B0%D1%82%D1%82%D0%B5%D1%81%D1%82%D0%B0%D1%82-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Earn money from sports!
Tired of the routine work and the search for additional income? Then our site is just for you!
Only the best on our website: the most profitable bets, reviews of top bookmakers and expert forecasts from professionals. Earn on your knowledge and experience in sports!
Come in and start your journey to financial freedom today! – https://vkltv.top/bonus/120-first-deposit-bonus/
Здравствуйте!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
mockwacom.getbb.ru/viewtopic.php?f=11&t=1728&p=2364#p2364
Поможем вам всегда!.
Добрый день!
Где приобрести диплом по актуальной специальности?
Заказать диплом любого университета.
http://www.kpilib.ru/forum.php?tema=7368
Привет, друзья!
Приобрести документ о получении высшего образования.
elfae.ruhelp.com/viewtopic.php?id=17232#p39489
opaseke.com/users/1243
asepbook.com/read-blog/4294
artrp.5nx.ru/viewtopic.php?f=3&t=9675
academy4elements.mybb.ru/viewtopic.php?id=955#p2089
Добрый день!
Заказать документ о получении высшего образования вы можете в нашей компании в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любой специальности, включая документы Советского Союза.
moscowurban.getbb.ru/viewtopic.php?f=12&t=1663
polegasm.net/index.php/forum/welcome-mat/151610
umorforme.ru/oformlenie-diploma-za-korotkiy-srok-byistro-i-nadezhno
http://www.ksolo.ru/forum/member.php?u=83595
u2c.tv/member.php?u=30984
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
last news about mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
<a href=http://www.svitlytsia.crimea.ua/phpinfo.php?a=mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
mbappe
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным ценам. Стоимость зависит от определенной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы документы были доступны для большого количества наших граждан.
http://www.bharatiyaobcmahasabha.org/2024/04/13/купить-диплом-техникума-купить-реаль/
Добрый день!
Купить документ о получении высшего образования можно у нас в Москве.
diplomasx24.ru/kupit-diplom-rostov-na-donu
Успехов в учебе!
Привет!
Заказать диплом о высшем образовании
Наши специалисты предлагают выгодно купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Диплом пройдет лубую проверку, даже при использовании профессионального оборудования. Достигайте своих целей быстро и просто с нашей компанией.
Где заказать диплом специалиста?
meldog.3nx.ru/viewtopic.php?p=23387#23387
mkpnz.ru/users/8
86hm.ru/forum/flame/?topic_id=25002
burgasdent.listbb.ru/viewtopic.php?f=3&t=355
forumkk.listbb.ru/viewtopic.php?f=12&t=392
Наша организация занимается реализацией обтирочных материалов по приемлемым ценам, к примеру, ветошью, которая имеет Гост 4643 75. Среди наших предложений можно найти махру, трикотаж. Обратите внимание и на фланель, а выбор бельевой ветоши цветной самый большой. Мы предлагаем покупку ветоши как оптом, так и в розницу. Только у нас вы обнаружите самый обширный выбор ветоши высокого качества российских производителей. У нас также имеется ветошь, предназначенная для типографий и для машиностроения.
Привет, друзья!
Купить документ о получении высшего образования можно в нашей компании в столице.
diploms-x.com/kupit-diplom-kandidata-nauk
Здравствуйте!
Как получить диплом техникума с упрощенным обучением в Москве официально
http://www.goalissimo.org/forum/viewtopic.php?f=4&t=710135
Рады оказать помощь!
pin up no
Plasser innsatsen din hos pin up online – veldig elite bookmaker
pin up no
лучшие порно видео лучшие порно видео .
the opportunity to compete for larger prizes and showcase their skills on a larger stage.
ivermectin purchase
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании.
asxdiplomik.com/kupit-diplom-krasnoyarsk
Хорошей учебы!
לך לגלות עולם של הנאה אינסופית. זוהי צורת בילוי אינטימית המותאמת לצרכים של הגבר הישראלי, הידוע כגבר בעל ציפיות גבוהות. כאשר שתתפרק מרוב עונג. ואתה יודע מה הכי כיף? ניתן ליהנות מהשירות של דירות דיסקרטיות בבאר שבע בכל יום ובכל שעה. לא משנה אם זה סוף חדרים לפי שעה
Добрый день!
Заказать документ о получении высшего образования можно у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы сможете получить необходимый диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что в случае проверки документа работодателями, подозрений не возникнет.
Мы готовы предложить дипломы любой профессии по приятным ценам. Стоимость будет зависеть от конкретной специальности, года получения и университета. Стараемся поддерживать для заказчиков адекватную ценовую политику. Для нас очень важно, чтобы дипломы были доступными для большого количества наших граждан.
http://www.neckmax.de/blogs/2250/Как-можно-будет-быстро-купить-диплом-в-онлайн-магазине
Поможем вам всегда!
Здравствуйте!
Заказать диплом о высшем образовании.
k96586v0.beget.tech/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=145
dinsta-gram.com/read-blog/4219
o91746bp.beget.tech/2024/07/04/pochemu-segodnya-gorazdo-deshevle-i-prosche-kupit-diplom-vuza.html
energypowerworld.co.uk/read-blog/6509
asromafansclub.com/read-blog/6324
Привет, друзья!
Как не попасть впросак при покупке диплома колледжа или ПТУ в России
drovokol.ru/forum/user/12143
Будем рады вам помочь!
На сайте https://doramalive.me/ посмотрите дорамы абсолютно бесплатно и в любое время. Напротив каждой серии имеется дата выхода и вся необходимая информация. Все фильмы отличаются интересным, непредсказуемым сюжетом, удивительной актерской игрой, которая завораживает. Все серии отличного качества, а потому подарят только восторг. Вы сможете просматривать фильм за фильмом или продолжить просмотр там, где остановились в прошлый раз. Есть самые горячие дорамы, выхода которых ждали давно. Постоянно появляются новинки.
Привет!
Купить документ о получении высшего образования вы имеете возможность в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите диплом по любой специальности, включая документы образца СССР. Даем 100% гарантию, что в случае проверки документов работодателями, подозрений не возникнет.
vip.7bb.ru/viewtopic.php?id=3026#p7117
victorians123.com/blogs/210/Что-именно-нужно-для-создания-качественного-документа
sustalks.com/blogs/2766/Что-готов-в-наше-время-предоставить-магазин-с-дипломами
silkhunter.com/index.php?title=Официальные_Дипломы:_Качество_и_Легальность
woman.build2.ru/viewtopic.php?id=14475#p44504
Здравствуйте!
Купить документ университета вы можете у нас в столице.
ast-diploms24.ru/kupit-diplom-krasnoyarsk
Удачи!
Привет!
Мы изготавливаем дипломы любой профессии по выгодным ценам.
http://www.humansandslaves.ru/blogs/623/Почему-сегодня-намного-проще-будет-приобрести-диплом-университета
Здравствуйте!
Покупка школьного аттестата с упрощенной программой: что важно знать
forum.omnicomm.pro/index.php/topic,22009.0.html
Будем рады вам помочь!.
Наша мастерская предлагает профессиональный мастерская по ремонту фотовспышки рядом любых брендов и моделей. Мы осознаем, насколько значимы для вас ваши фотовспышки, и готовы предложить сервис высочайшего уровня. Наши опытные мастера работают быстро и аккуратно, используя только качественные детали, что обеспечивает длительную работу выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются пользователи вспышек, включают неработающий зарядник, неисправности лампы, неисправности программного обеспечения, проблемы с синхронизатором и неработающие разъемы. Для устранения этих поломок наши профессиональные техники оказывают ремонт зарядных устройств, ламп, ПО, синхронизаторов и разъемов. Обратившись к нам, вы гарантируете себе долговечный и надежный ремонт фотовспышки рядом.
Подробная информация размещена на сайте: https://remont-fotovspyshek-job.ru
купить диплом электрика diploms-x.com .
Привет, друзья!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
forum.safe-animals.ru/index.php?showtopic=30579
Окажем помощь!
Привет, друзья!
Купить диплом о высшем образовании
Наша компания предлагает быстро и выгодно заказать диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями официальных лиц. Наш документ пройдет лубую проверку, даже при помощи специфических приборов. Решайте свои задачи быстро и просто с нашим сервисом.
Где купить диплом специалиста?
http://www.benedeek.com/blogs/90685/ упить-?иплом-Ѕыстро-и- онфиденциально
sportraketka.ru/vash-nastoyashhiy-diplom-byistro-i-bezopasno
say.la/read-blog/36634
sharemeglobal.com/blogs/903/На-что-именно-обращать-внимание-при-заказе-диплома-в-сети
technoevents.ru/kak-kupit-diplom-bez-problem/
Привет, друзья!
Приобрести диплом любого университета.
usame.life/read-blog/45890
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Стоимость может зависеть от определенной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику тарифов. Для нас очень важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
danteyrix98754.wikigop.com/562315/Тенденции_покупки_ученых_степеней_в_настоящем_мире
Здравствуйте!
Заказать диплом о высшем образовании.
site2.liodiz.ru/2024/07/04/shirokiy-vybor-dokumentov-v-znamenitom-onlayn-magazine.html
Здравствуйте!
Где заказать диплом по нужной специальности?
Приобрести диплом о высшем образовании.
korrespondentweek.ru/diplom-na-zakaz-kachestvo-i-nadezhnost/
Добрый день!
Заказать документ о получении высшего образования можно в нашей компании. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите диплом по любой специальности, включая документы образца СССР.
lubov.listbb.ru/viewtopic.php?f=2&t=484
comptonrpp.listbb.ru/viewtopic.php?f=6&t=714
sport-faq.ru/ofitsialnyiy-diplom-bez-uchebyi-i-ekzamenov
mongolsmc.listbb.ru/viewtopic.php?f=1&t=395
klinlife.ru/forums/index.php?/topic/41523-diplom-na-zakaz-kachestvo-i-nadezhnost/
Привет!
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий.
forum.recifalnews.fr/gallery/image/210-зачем-сегодня-заказывают-дипломы-в-сети-интернет/
Рады оказаться полезными!.
Здравствуйте!
Купить диплом университета.
roxgo.cl/gallery/image/4247-как-найти-проверенный-магазин-с-огромным-ассортиментом-дипломов/
Привет!
Приобрести диплом университета
Мы предлагаем выгодно и быстро купить диплом, который выполнен на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Документ способен пройти лубую проверку, даже при использовании специально предназначенного оборудования. Решайте свои задачи быстро с нашим сервисом.
Где приобрести диплом по нужной специальности?
http://www.pets-ural.ru/content/forum/viewtopic.php?p=63537#63537
odessaforum.getbb.ru/viewtopic.php?f=5&t=20402
86hm.ru/forum/flame/?topic_id=25002
http://www.simplemachines.org/about/smf/stats.php
pdlspd.listbb.ru/viewtopic.php?f=3&t=409
Привет, друзья!
Приобретение диплома ПТУ с сокращенной программой обучения в Москве
http://www.tapatalk.com/groups/dzerjinsky/viewtopic.php?f=2&t=37259&from_new_topic=1
Всегда вам поможем!.
[u][b] Добрый день![/b][/u]
[b]Мы изготавливаем дипломы[/b] психологов, юристов, экономистов и любых других профессий по приятным ценам.
[url=http://www.dtcnetwork.eu/купить-диплом-угнту//]www.dtcnetwork.eu/купить-диплом-угнту/[/url]
ללמוד דברים חדשים, או אולי להפתיע אותן בדברים חדשים ונועזים, זוהי ההזדמנות שלך. לא בכל יום פוגשים בחורות כל כך יפות שפשוט של נערות יפיפיות המעניקות להם אירוח נעים ואינטימי, תוך כדי שמירה על הדיסקרטיות. דירות דיסקרטיות בתל אביב שומרות על הפרטיות נערת ליווי בבאר שבע – בוא להגשים פנטזיות פרועות
скачать порно коллекций https://porn-library.ru/ .
Здравствуйте!
Купить диплом любого ВУЗа.
s24.team/club/user/148/blog/1602/
Здравствуйте!
Мы предлагаем дипломы любой профессии по приятным тарифам.
pdbsoftware.com/2024/06/23/купить-диплом-в-новочеркасске/
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
Оформи заявку на кредитную карту от лучших банков России онлайн
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
оформить кредитную карту
สำหรับผู้ที่ชื่นชอบกีฬาฟุตบอล ที่ต้องการดูการแข่งขันฟุตบอลแบบสด ๆ ต้องลอง doofootball.asia เว็บไซต์ยอดนิยมสำหรับการรับชมฟุตบอลสด
doofootball – https://www.anobii.com/,.asiaมอบประสบการณ์การดูฟุตบอลคุณภาพสูง รวมถึงข้อมูลการแข่งขัน ที่อัปเดตตลอดเวลา แฟนบอลสามารถสนุกกับเกมการแข่งขันจากลีกยอดนิยมทั่วโลก
อย่ารอช้า มาที่ doofootball.asia วันนี้ เพื่อพบกับประสบการณ์การรับชมฟุตบอลที่เหนือชั้น ไม่พลาดทุกแมตช์ที่คุณโปรดปราน
Добрый день!
Мы предлагаем документы ВУЗов, расположенных на территории всей РФ. Можно приобрести диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге высшего качества. Это дает возможности делать государственные дипломы, не отличимые от оригиналов. Документы заверяются необходимыми печатями и штампами.
wheeoo.com/read-blog/13148
Здравствуйте!
Купить документ института вы сможете у нас в столице.
ast-diplomas24.ru/kupit-diplom-nizhnij-novgorod
Успехов в учебе!
Наш сервисный центр предлагает высококачественный центр ремонта гироскутера на выезде всех типов и брендов. Мы понимаем, насколько необходимы вам ваши гироскутеры, и обеспечиваем ремонт высочайшего уровня. Наши квалифицированные специалисты работают быстро и аккуратно, используя только оригинальные запчасти, что предоставляет надежность и долговечность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются пользователи электроскутеров, включают поломку аккумулятора, неисправности двигателя, сбои контроллера, неисправности сенсоров и поломки корпуса. Для устранения этих поломок наши опытные мастера оказывают ремонт батарей, двигателей, контроллеров, гиросенсоров и механических компонентов. Доверив ремонт нам, вы гарантируете себе долговечный и надежный мастерская по ремонту гироскутеров на выезде.
Подробная информация представлена на нашем сайте: https://remont-giroskuterov-key.ru
Добрый день!
Заказать диплом о высшем образовании.
explorivore.com/read-blog/2497
sonnick84.aboutyoublog.com/28981009/Находим-надежный-и-проверенный-магазин-для-приобретения-диплома
network-2295034.mn.co/posts/61679299
sonnick84.shoutmyblog.com/27837578/Как-найти-надежный-магазин-что-реализует-документы
driversspace.com/blogs/3281/С-умом-покупаем-документы-в-сети-авторский-обзор
i thought about this coinmarketcap
how to become real estate agent in ms realestatelicensengdfdgh.com/states/michigan-real-estate-license/ qualifications to be real estate agent realestatelicensengdfdgh.com/states/nevada-island-real-estate-license/ .
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по выгодным ценам.
http://www.jaitun.com/read-blog/332_zhelaete-kupit-attestat-u-nadezhnogo-ispolnitelya-zhdem-vas.html?mode=day
Здравствуйте!
Купить диплом ВУЗа.
sonnick84.full-design.com/%D0%93%D1%80%D0%B0%D0%BC%D0%BE%D1%82%D0%BD%D0%BE-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D1%81%D0%B5%D1%82%D0%B8-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80-71034102
excitement it brings to the table.
ivermectin buy
Become our affiliate
https://affiliates.whalehunter.cash/track/Kirill.18AffRef.18AffRef.MAIN.0.0.0.0.0.0.0.0
Привет!
Заказать документ ВУЗа вы можете в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы СССР.
paulikipedia.ru/index.php/Купите_диплом_и_начните_новую_жизнь
irishpal.com/read-blog/921
lubov.listbb.ru/viewtopic.php?f=2&t=484
smd.mybb.ru/viewtopic.php?id=4057#p23076
climat-cold.ru/forum/user/3857/
Здравствуйте!
Где заказать диплом по актуальной специальности?
Купить диплом любого университета.
1stroitelny.kz/faq/show/id/668ff2c16f3e5f305e8d9da6.html
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным ценам.
sngine.codiantprod.com/blogs/221/Ценные-рекомендации-по-покупки-документа-в-сети
Привет!
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий.
1776reloaded.us/blogs/56/Быстрое-Оформление-Дипломов-Надежно-и-Легально
Всегда вам поможем!.
Привет, друзья!
Заказать документ ВУЗа.
kingcityrp.moibb.ru/posting.php?mode=post&f=34
rentry.co/ipe5ww38
blog.nataraj.ru/~/Interest/Легальный диплом без лишних хлопот: узнайте как!
mimozem.4admins.ru/viewtopic.php?f=98&t=4987
karasteamfulldmroleplay.getbb.ru/viewtopic.php?f=62&t=939
Привет, друзья!
Мы можем предложить дипломы психологов, юристов, экономистов и прочих профессий по невысоким ценам.
http://www.sermadiesel.com.pe/2024/06/30/купить-диплом-спо/
kraken ссылка – ссылка кракен kraken tor site, kraken зеркало рабочее 2krnk biz
Здравствуйте!
Заказать диплом любого ВУЗа
Наши специалисты предлагают максимально быстро приобрести диплом, который выполнен на оригинальном бланке и заверен печатями, водяными знаками, подписями должностных лиц. Диплом способен пройти лубую проверку, даже с применением специально предназначенного оборудования. Достигайте своих целей быстро с нашей компанией.
Где купить диплом по нужной специальности?
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
ya.bestbb.ru/viewtopic.php?id=2962#p6549
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
http://www.hristianka.ru/forum/r/prev_loaded/1/
http://www.hristianka.ru/forum/r/prev_loaded/1/
Привет, друзья!
Заказать диплом любого университета.
xleks.ru/2024/07/04/shirokiy-katalog-dokumentov-v-znamenitom-internet-magazine.html
Здравствуйте!
Заказать документ о получении высшего образования.
doremichildcarecentre.com/index.php/forum/welcome-mat/191398
anytalkworld.com/read-blog/6932
iwasocial.com/read-blog/409
zoofortunakz.5nx.ru/viewtopic.php?f=96&t=4579
vatrusha.maxbb.ru/viewtopic.php?f=2&t=701
Привет, друзья!
Приобрести диплом о высшем образовании.
rakisochi.ru/users/20
Удачи!
breakingnews77.com
Привет!
Мы можем предложить дипломы любых профессий по приятным тарифам.
http://www.modern-constructions.org/blogs/60329/Дипломы-для-Вашего-Успеха
Привет!
Где приобрести диплом специалиста?
http://www.jointcorners.com/read-blog/78325
Здравствуйте!
Мы готовы предложить документы техникумов, расположенных в любом регионе России. Вы можете купить качественный диплом от любого заведения, за любой год, указав актуальную специальность и оценки за все дисциплины. Документы выпускаются на бумаге самого высшего качества. Это позволяет делать настоящие дипломы, которые не отличить от оригинала. Документы будут заверены всеми требуемыми печатями и подписями.
srbogl44n.snack-blog.com/28209457/%D0%94%D0%B5%D1%82%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B5%D0%BD%D0%B8%D1%8F-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B7%D0%BD%D0%B0%D0%BC%D0%B5%D0%BD%D0%B8%D1%82%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Advantages of wooden gazebos, in addition to the obvious advantages in a decorative sense olympic-school.com, there are other advantages.
Здравствуйте!
Заказать диплом о высшем образовании.
tawasol1.mn.co/posts/61900062
Добрый день!
Приобрести документ института.
tavasporan.flybb.ru/viewtopic.php?f=13&t=2680
leadrp.listbb.ru/viewtopic.php?f=3&t=406
bittogether.com/index.php?action=profile;u=11883
c904581v.beget.tech/2024/07/13/diplom-na-zakaz-kachestvo-i-nadezhnost.html
newru.getbb.ru/viewtopic.php?f=29&t=1371
Наш сервисный центр предлагает высококачественный сервисный центр по ремонту холодильников различных марок и моделей. Мы осознаем, насколько важны для вас ваши рефрижераторы, и готовы предложить сервис наилучшего качества. Наши профессиональные техники работают быстро и аккуратно, используя только сертифицированные компоненты, что гарантирует надежность и долговечность проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются пользователи рефрижераторов, включают проблемы с охлаждением, проблемы с температурным датчиком, программные сбои, неработающие разъемы и поломки корпуса. Для устранения этих неисправностей наши опытные мастера выполняют ремонт компрессоров, термостатов, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы обеспечиваете себе долговечный и надежный мастерская по ремонту холодильника на выезде.
Подробная информация представлена на нашем сайте: https://remont-holodilnikov-lux.ru
Ищите торговлю бинарными опционами? Зайдите на сайт https://binrm.online/ и получите доступ к торговле более 100 мировыми торговыми активами. Узнайте больше о наших преимуществах Binarium – быстрые выводы, круглосуточная торговля, мгновенная поддержка, а также все о нашем приложении для любых мобильных устройств.
Привет, друзья!
Мы можем предложить документы ВУЗов, расположенных в любом регионе РФ. Вы можете приобрести диплом за любой год, в том числе документы СССР. Документы выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, которые не отличить от оригинала. Документы будут заверены необходимыми печатями и штампами.
gemawiraclub.com/blogs/40319/%D0%A0%D0%B0%D1%81%D1%88%D0%B8%D1%80%D0%B5%D0%BD%D0%BD%D0%BE%D0%B5-%D0%BE%D0%BF%D0%B8%D1%81%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5
Привет, друзья!
Как купить диплом о высшем образовании с минимальными рисками
worldgonews.ru/legkiy-put-k-diplomirovannomu-uspehu-byistro-i-nadezhno
Поможем вам всегда!
Привет!
Купить документ о получении высшего образования можно у нас в столице.
asxdiplomik24.ru/kupit-diplom-o-srednem-obrazovanii
Успехов в учебе!
Добрый день!
Реально ли приобрести диплом стоматолога? Основные этапы
4asdaiprognoza.listbb.ru/posting.php?mode=post&f=2&sid=89ca3402550eeba4cc7308acd579e3be
Поможем вам всегда!
На сайте https://olato.ru вы найдете ванны, комплектующие, а также душевые кабины, различные ограждения, биде, унитазы, инсталляции и многое другое. Регулярно появляются лучшие предложения, которые помогут изрядно сэкономить и получить желаемую вещь. Перед вами только продукция надежных, популярных брендов, которые гарантируют безупречное качество. Именно поэтому продукция является износостойкой и прослужит очень долго. Все товары реализуются по привлекательной цене, действуют распродажи.
Привет!
Заказать документ института можно в нашем сервисе.
ast-diplomy24.ru/kupit-diplom-vracha
Успехов в учебе!
Добрый день!
Приобрести диплом любого ВУЗа:
gamla.vykort.com/member.php?action=showprofile&user_id=27264
bazar-planet.ru/index.php?threads/Вакансии-на-работу-курьером.93/page-3#post-5075
u-cars.ru/modules.php?name=Your_Account&op=userinfo&username=anizecin
findaspermdonor.com/viewtopic.php?f=2&t=80886&p=78159#p78159
lada-xray.net/showthread.php?p=32748#post32748
Привет!
Процесс получения диплома стоматолога: реально ли это сделать быстро?
http://www.lada-xray.net/member.php?u=2434
Всегда вам поможем!
купить диплом менеджера купить диплом менеджера .
https://www.publico.es/sociedad/publico.es-nancy-fraser-no-dejar-temor-ultraderecha-lleve-feminismo-liberal.html
In-Game Bonuses and Rewards
ivermectin purchase
客人
На сайте https://verstaki-slesarnye.ru изучите информацию о том, где приобрести слесарный верстак по доступной и привлекательной стоимости. На этом сайте вы узнаете о видах слесарных верстаков, технических характеристиках и другую дополнительную информацию. Также даются ценные рекомендации о том, как правильно подобрать такое оборудование. Вы узнаете о том, почему выгодно приобрести такую технику и какую пользу вы от этого получите. Если и вы задумались о покупке, то положитесь на эти ценные рекомендации.
Добрый день!
Где купить диплом по необходимой специальности?
http://www.mizmiz.de/read-blog/23918
Диплом пту купить официально с упрощенным обучением в Москве
diplomyx24.ru/kupit-diplom-chelyabinsk
Здравствуйте!
Приобрести диплом университета.
gamingforum.se/index.php?/gallery/image/117-большой-каталог-документов-в-популярном-интернет-магазине/
Привет, друзья!
Вопросы и ответы: можно ли быстро купить диплом старого образца?
thesocialgroup.co.uk/blogs/524/Как-можно-купить-сегодня-неотличимый-от-оригинала-диплом-в-сети
Привет, друзья!
Купить документ ВУЗа.
windows1.listbb.ru/viewtopic.php?f=3&t=467
funchange.getbb.ru/viewtopic.php?f=8&t=1407
gamemotors.ru/ofitsialnyiy-diplom-bez-uchebyi-i-ekzamenov
akademiyavodopad.ru/forum/messages/forum7/topic425/message740/?result=new#message740
fh9947a1.bget.ru/topic/add
Приобрести диплом ВУЗа.
worldgonews.ru/kupit-diplom-vyigodno-i-bezopasno
щербиновскийрайон.рф/users/160
ericos.ru/forum/index.php?PAGE_NAME=profile_view&UID=10789
extra-v.store/forum/?PAGE_NAME=profile_view&UID=2661
cslregister.com/forum/member.php?u=6225
Наши специалисты предлагает надежный мастерская по ремонту бесперебойника на выезде различных марок и моделей. Мы знаем, насколько значимы для вас ваши ИБП, и обеспечиваем ремонт наилучшего качества. Наши профессиональные техники работают быстро и аккуратно, используя только сертифицированные компоненты, что обеспечивает длительную работу выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются владельцы ИБП, включают неисправную батарею, проблемы с инвертором, сбои контроллера, неработающие разъемы и ошибки ПО. Для устранения этих неисправностей наши профессиональные техники проводят ремонт батарей, инверторов, контроллеров, разъемов и ПО. Обращаясь в наш сервисный центр, вы обеспечиваете себе долговечный и надежный центр ремонта бесперебойников рядом.
Подробная информация размещена на сайте: https://remont-ibp-max.ru
Привет, друзья!
Купить документ о получении высшего образования
sonnick84.kylieblog.com/28718303/Что-потребуется-для-создания-неотличимого-от-оригинала-диплома
yobasket.es/es/perfil-usuario/pluginclass/cbblogs.html?action=blogs&func=show&id=125
d6united.mn.co/posts/61679279
1776reloaded.us/blogs/52/На-что-обратить-свое-внимание-при-заказе-диплома-в-интернете
forum.ro-ox.com/index.php?/gallery/image/193-ассортимент-и-варианты-доставки-в-магазине-заказываем-диплом/
Здравствуйте!
Заказать документ о получении высшего образования вы можете у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ. Вы получите диплом по любым специальностям, любого года выпуска, включая документы образца СССР. Даем 100% гарантию, что при проверке документа работодателем, каких-либо подозрений не появится.
http://www.cslregister.com/forum/member.php?u=6225
6rawamkw0.jiliblog.com/85724406/Прочитайте-наш-обзор-если-требуется-приобрести-диплом-в-сети
vip.rolevaya.info/viewtopic.php?id=4954#p8478
ya.bestbb.ru/viewtopic.php?id=2997#p6619
dachaweek.ru/vash-shans-na-vyisshee-obrazovanie-kupit-diplom
Добрый день!
Мы изготавливаем дипломы.
bery-optom.ru/forum/?PAGE_NAME=profile_view&UID=11263
worldgonews.ru/ofitsialnyie-diplomyi-vyisshee-obrazovanie-bez-problem
vetstate.ru/forum/?PAGE_NAME=profile_view&UID=125341
znamo.listbb.ru/posting.php?mode=post&f=9
kharkov-balka.com/showthread.php?p=154670#post154670
Привет!
Приобрести диплом любого университета.
prof-komplekt.com/club/user/1035/blog/11031/
missouri real estate license test realestatelicensengdfdgh.com/states/tennessee-real-estate-license/ how long take to get real estate license realestatelicensengdfdgh.com/states/virginia-real-estate-license/ .
how to become a real estate agent in texas online https://www.realestatelicensengdfdgh.com how do i become a realtor realestatelicensengdfdgh.com/states/ohio-real-estate-license/ .
Здравствуйте!
Заказать диплом ВУЗа
Мы предлагаем выгодно приобрести диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, штампами, подписями должностных лиц. Наш диплом способен пройти любые проверки, даже с использованием профессиональных приборов. Достигайте цели максимально быстро с нашими дипломами.
Где заказать диплом по необходимой специальности?
http://www.forumblogger.my.id/blogs/1919/На-что-обратить-внимание-при-заказе-документов-в-сети-интернет
anamaliya.ru/otzyvy/bystryy-poisk-onlayn-magazina-kotoryy-prodaet-diplomy
vevqegzer.blog5.net/70054318/Хотите-выяснить-как-купить-диплом-в-сети-недорого-Ждем-Вас
http://www.nextvio.net/read-blog/556
heyjinni.com/read-blog/110115
Здравствуйте!
Как приобрести аттестат о среднем образовании в Москве и других городах
webyourself.eu/blogs/358414/ упите-?ипломы-Ѕыстро-и-Ќадежно
Привет, друзья!
Приобрести документ ВУЗа
x8nlp84dt.develop-blog.com/34408498/%D0%9B%D0%B5%D0%B3%D0%BA%D0%BE-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%82%D0%B0%D0%B5%D0%BC-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%B2-%D0%B8%D0%B7%D0%B2%D0%B5%D1%81%D1%82%D0%BD%D0%BE%D0%BC-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D0%B5-russian-diplom
lucylink.com/read-blog/56
heyjinni.com/read-blog/108997
sonnick84.dbblog.net/1487816/Что-требуется-из-оборудования-для-производства-диплома
sonnick84.madmouseblog.com/8692371/Как-возможно-заказать-сегодня-качественный-диплом-в-сети-интернет
ООО СПЕЦТОРГ – ВСЁ ЧТОБЫ ПЕРЕРАБАТЫВАЮЩЕЙ ПРОМЫШЛЕННОСТИ
на сайт
Лекарство, пищевые добавки, содержание чтобы пищевой промышленности
СпецТорг предлагает широкий ассортимент товара
СпецТорг лекарство и пищевые добавки воеже мясоперерабатывающей промышленности
СпецТорг СпецТорг технологический актив ради пищевой промышленности
СпецТорг добавки воеже кондитерского производства
СпецТорг оборудование для пищевой промышленности
СпецТорг моющие и дезинфицирующие имущество
СпецТорг ножи и заточное припасы
СпецТорг профессиональный моющий реестр
Zaltech GmbH (Австрия) – эликсир и пищевые добавки воеже мясоперерабатывающей промышленности,
La Minerva (Италия) –состояние для пищевой промышленности
Dick (Германия) – ножи и заточное обстановка
Kiilto Clein (Farmos – Финляндия) – моющие и дезинфицирующие добро
Hill Shake of correctness (Англия) – профессиональный моющий мебель
Сельскохозяйственное аксессуары из Белоруссии
Кондитерка – пюре, сиропы, топпинги
Пюре производства компании Agrobar
Сиропы производства Herbarista
Сиропы и топпинги производства Arousing Cane
Топпинги производства Dukatto
Продукты мясопереработки
Добавки чтобы варёных колбас
149230 Докторская
149720 Докторская Мускат
149710 Докторская Кардамон
149240 Любительская
149260 Телячья
149270 Русская
149280 Молочная
149290 Чайная
Cосиски и сардельки
149300 Сосиски Сливочные
149310 Сосисики Любительские
149320 Сосиски Молочные
149330 Сосиски Русские
149350 Сардельки Говяжьи
149360 Сардельки Свиные
Полу- и варено-копченые колбасы
Полу- копченые и варено-копченые колбасы Стадо «ГОСТ-RU»
149430 Сервелат в/к
149420 Московская в/к
149370 Краковская
149380 Украинская
149390 Охотничьи колбаски п/к
149400 Одесская п/к
149410 Таллинская п/к
Деликатесы и ветчины Часть «LUX» 130-200%
«ZALTECH» разработал серию продуктов «LUX» ради ветчин
149960 Зельцбаух
119100 Ветчина Деревенская
124290 Шинкен комби
118720 Ветчина Деревенская Плюс
138470 Шинка Крестьянская
142420 Шинка Домашняя
147170 Флорида
148580 Ветчина Пицц
Сырокопченые колбасы Общество «ГОСТ — RU»
сословие продуктов «Zaltech» для сырокопченых колбас ГОСТ
152360 Московская
152370 Столичная
152380 Зернистая
152390 Сервелат
152840 Советская
152850 Брауншвейгская
152860 Праздничная
разряд продуктов Zaltech воеже ливерных колбас
114630 Сметанковый паштет
118270 Паштет с паприкой
118300 Укропный паштет
114640 Грибной паштет
130820 Паштет Болезный
118280 Паштет Луковый
135220 Паштет коньячный
143500 Паштет Парижский
Сырокопченые деликатесы Традиции домашнего стола
«Zaltech» воеже производства сырокопченых деликатесов
153690 Шинкеншпек
154040 Карешпек
146910 Рошинкен ХАЛАЛ
127420 Евро шинкеншпек
117180 Евро сырокопченый шпик
Конвениенс продукты и полуфабрикаты
Функциональные продукты чтобы шприцевания свежего мяса
«Zaltech» предлагает серию продуктов «Convenience»
152520 Фрешмит лайт
148790 Фрешмит альфа
157350 Фрешмит экономи
160960 Фрешмит экономи S
158570 Фрешмит экономи плюс
153420Чикен комби Гриль
151190 Роаст Чикен
146950Чикен Иньект
Удовлетворение соевого белка и мяса невольный дообвалки
Функциональные продукты ради замены соевого белка и МДМ
151170Эмуль Топ Реплейсер
157380 Эмул Топ Реплейсер II
151860Эмул Топ МДМ Реплейсер
ТУ чтобы производителей колбас
ТУ 9213 -015-87170676-09 – Изделия колбасные вареные
ТУ 9213-419-01597945-07 – Изделия ветчины
ТУ 9213-438 -01597945-08 – Продукты деликатесные из говядины, свинины, баранины и оленины
ТУ 9214-002-93709636-08 – Полуфабрикаты мясные и мясосодержащие кусковые, рубленные
ТУ 9216-005-48772350-04 – Консервы мясные, паштеты
ТУ 9213-004-48772350-01 – Паштеты мясные деликатесные
ТУ 9213-019-87170676-2010 – Колбасные изделия полукопченые и варено-копченые
ТУ 9213-439 -01597945-08 – Продукты деликатесные из мяса птицы
ТУ 9213-010-48772350-05 – Колбасы сырокопченые и сыровяленые
подробней
Справочник специй
Е – номера
Ножи и заточные станки
ножи для обвалки и жиловки
Ножи воеже обвалки
Профессиональные ножи чтобы первичной мясопереработки
Жиловочные ножи
Ножи воеже нарезки
Ножи для рыбы
Мусаты Секачи
Добрый день!
Мы готовы предложить документы техникумов
kolhos.listbb.ru/viewtopic.php?f=2&t=633
neochemical.kz/forum/user/816/
elderassociation.mn.co/posts/62679148
pro-novostroyki.ru/index.php?showtopic=20863
forum.analysisclub.ru/index.php/topic,224164.new.html#new
男子
Добрый день!
Заказать диплом университета:
pirobot.co.uk/doku.php?id=diploman
lyxondebian.free.fr/dokutest/doku.php?id=gosznacdiplomy
автолнр.рф/users/awuzu
198.199.122.222/doku.php?id=landsdiplomy
85sucai.com/member/index.php?uid=yhaxyn
Привет!
Заказать документ о получении высшего образования
wiki.diamondrp.ru/index.php?title=Какие_онлайн-магазины_с_документами_на_текущий_день_имеются?
tricityfriends.com/read-blog/540
dj-club-sf.mn.co/posts/61838308
islgaming.community/read-blog/80
gumrukmedyasi.com/blogs/233/С-умом-покупаем-диплом-в-сети-обзор
Привет!
Мы предлагаем документы ВУЗов
poemsbook.net/blogs/124133/диплом-о-высшем-образовании-ваши-новые-перспективы
politictoday.ru/diplomyi-o-vyisshem-obrazovanii-otkroyte-dveri-k-uspehu
myturtime.ru/diplomyi-dlya-uverennogo-starta-v-lyuboy-sfere
asktourist.ru/post.php?fid=23
obozrevatelevents.ru/diplomyi-dlya-vashego-karernogo-rosta/
Привет, друзья!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
newmedtime.ru/kupite-diplom-i-nachnite-novuyu-zhizn
Здравствуйте!
Мы предлагаем дипломы любых профессий по приятным тарифам.
astart.pl/index.php?/gallery/image/11-4-е-главных-группы-интернет-магазинов-продающих-дипломы/
Добрый день!
Приобрести документ о получении высшего образования вы можете у нас в столице.
diploms-x24.ru/kupit-diplom-krasnoyarsk
Удачи!
з”·еђ
Здравствуйте!
Мы можем предложить документы техникумов
easyinsurancehub.co.uk/forum/thread-57319.html
itbitgroup.ru/nadezhnyie-diplomyi-dlya-vashey-kareryi
odessaforum.getbb.ru/viewtopic.php?f=5&t=20855
deanonnic.listbb.ru/viewtopic.php?f=5&t=475
mindclub.online/wiki/index.php/Купите_диплом_и_начните_новую_жизнь
Вопросы и ответы: можно ли быстро купить диплом старого образца?
asxdiplomik.com/kupit-diplom-moskva
Приобрести диплом любого университета.
domovou.3nx.ru/viewtopic.php?p=6845#6845
sovetushka.forum2x2.ru/login
art-gymnastics.ru/users/54
art-gsm.ru/forum/?PAGE_NAME=profile_view&UID=34125
comptonrpp.listbb.ru/viewtopic.php?f=6&t=703
Здравствуйте!
Мы готовы предложить дипломы любой профессии по доступным ценам.
nomadjapan.com/computers-data-recovery/купить-диплом-переподготовки/
Если вам срочно нужны деньги, подписывайтесь на канал Займы для безработных – Telegram ! Мы собрали лучшие предложения от МФО, которые выдают займы на карту без отказа и долгих проверок. Наш канал поможет вам найти самые выгодные условия: займы от 1 до 30 тысяч рублей, даже с плохой кредитной историей. Узнайте, где можно получить займ под 0% для новых клиентов. Telegram – выгодные микрозаймы на карту — это ваш гид по миру срочных займов. Не теряйте время, подпишитесь и получите деньги быстро и без лишних проблем!
Привет, друзья!
Купить диплом университета.
cbr.by/club/user/1977/blog/327/
canadaline.net/read-blog/62
newsbig.iamarrows.com/kak-kupit-v-nase-vrema-neotlicimyj-ot-originala-diplom-v-seti
sonnick84.blogripley.com/28797942/Полезные-советы-по-приобретению-документа-в-сети
usa.life/read-blog/62979
Здравствуйте!
Приобрести документ о получении высшего образования можно у нас.
asxdiplomik.com/kupit-diplom-tehnikuma-kolledzha
Лучшие автомобили из Кореи | Как выбрать авто из Кореи? | Свежие поступления авто из Кореи | Топ-5 автомобилей из Кореи | Секреты долговечности корейских автомобилей | Какие корейские автомобили пользуются спросом? | Как не ошибиться при покупке поддержанного автомобиля Кореи | Ценовая политика корейских автомобилей | Что стоит знать перед покупкой корейского авто | Корейские SUV: особенности моделей | Популярные кроссоверы из Кореи | Какой корейский автомобиль выбрать для путешествий? | Советы по выбору городского авто из Кореи | Как оценить состояние авто из Кореи перед покупкой? | Индивидуализация корейского автомобиля
кореи авто https://avtodom63.ru/ .
Наша мастерская предлагает высококачественный отремонтировать игровая приставка с гарантией различных марок и моделей. Мы понимаем, насколько необходимы вам ваши игровые приставки, и стремимся предоставить услуги первоклассного уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только качественные детали, что предоставляет надежность и долговечность проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются обладатели геймерских устройств, включают проблемы с жестким диском, проблемы с разъемами, неисправные контроллеры, ошибки ПО и проблемы с охлаждением. Для устранения этих проблем наши профессиональные техники выполняют ремонт жестких дисков, разъемов, контроллеров, ПО и систем охлаждения. Доверив ремонт нам, вы получаете надежный и долговечный сервисный центр по ремонту игровой приставки на выезде.
Подробная информация представлена на нашем сайте: https://remont-igrovyh-konsoley-mob.ru
Здравствуйте!
Мы изготавливаем дипломы любой профессии по выгодным ценам.
elotag.com/read-blog/296
hrv-club.ru/forums/index.php?autocom=gallery&req=si&img=6055
codinganme.com/gallery/image/112-для-чего-сейчас-приобретают-дипломы-и-аттестаты-в-сети/?context=new
foodxtech.mn.co/posts/61838161
wiki.gta-zona.ru/index.php/Техподдержка_и_FAQ._Покупаем_диплом_в_сети
Здравствуйте!
Мы можем предложить дипломы любой профессии по разумным тарифам.
halopro.net/gallery/image/489-какие-интернет-магазины-с-документами-имеются-на-сегодняшний-момент/
Привет!
Узнайте стоимость диплома высшего и среднего образования и процесс получения
uk-optimum.ru/index.php?subaction=userinfo&user=ukawunu
Окажем помощь!.
Здравствуйте!
Заказать документ о получении высшего образования вы сможете у нас в Москве.
ast-diploms.com/kupit-diplom-novosibirsk
Здравствуйте!
Мы изготавливаем дипломы.
altersoftonline.maxbb.ru/viewtopic.php?f=11&t=203
sontopic.com/blogs/1909/Купить-диплом-без-риска
slliver.getbb.ru/viewtopic.php?f=62&t=894
klinlife.ru/forums/index.php?/topic/38850-kupit-diplom-vse-chto-vam-nuzhno-znat/
soft-clouds.com/blogs/105905/Как-приобрести-диплом-без-рисков
Multiplayer Options and Social Interaction
ivermectin online
Привет, друзья!
Приобрести документ о получении высшего образования.
aromatov.wooden-rock.ru/forum/topic.php?forum=1&topic=16122
twoplustwoequal.com/read-blog/37952
mylot.su/addblogs
kh.txi.ru/forum/index.php?
чпуремонт.рф/showthread.php?tid=55592
Добрый день!
Купить документ университета вы можете в нашей компании в Москве. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ.
testowik.ru/index.php/forum/user/52911-asisa
esitscale.com/forum/profile.php?mode=viewprofile&u=40122
protprom.ru/index.php?subaction=userinfo&user=urumoqyn
city-hall.nvkb.ru/forum/index.php/user/101000/
fish-sea-products.ru/forum/messages/forum1/topic37/message31532/?result=reply#message31532
If we consider the absolute height, then this is the height above sea level 214rentals.com
Добрый день!
Приобрести документ о получении высшего образования можно у нас.
diploms-x.com/kupit-diplom-voronezh
Хорошей учебы!
е›
купить диплом о среднем образовании в омске diploms-x.com .
Здравствуйте!
Купить документ университета можно у нас в столице.
ast-diplom.com/kupit-diplom-s-registraciej
Добрый день!
Заказать диплом университета.
anamaliya.ru/otzyvy/shirokiy-assortiment-dokumentov-v-populyarnom-onlayn-magazine
Привет!
Заказать документ о получении высшего образования.
les-ailes-chalaisiennes.com/forum/topic/осуществите-мечту-получите-диплом-бы/#postid-19516
1001vieclam.forumvi.com/t9287-topic#9967
wegug.in/blogs/1120/Легальный-диплом-без-лишних-хлопот-узнайте-как
brawlstarsacc.listbb.ru/viewtopic.php?f=3&t=486
chromerp.listbb.ru/viewtopic.php?f=13&t=510
На сайте https://autoclub78.ru вы найдете интересные, практичные советы для тех, у кого есть автомобиль. Имеются практические рекомендации, ценные советы, которые помогут найти оптимальный вариант для того, чтобы правильно эксплуатировать технику. Статьи ответят на многочисленные вопросы, подскажут, как правильно действовать в определенной ситуации. Есть информация про самые востребованные мотоциклы, а также запчасти, которые реализуются на маркетплейсах. Есть информация и про то, как не стоит приобретать стеклоомывающую жидкость.
Консультация акушера гинеколога в Москве cecilplus.ru
В современное время медицина в Российской Федерации развивается стремительно. Это весьма хорошо, но также работает много поликлиник, которые предоставляют сомнительные услуги. Приглашаем Вас в клинику «Сесиль», которая осуществляет работу уже более двадцати лет, имеет отличную репутацию и штат настоящих специалистов.
По поводу уролог клиника мы Вам с легкостью окажем помощь. Представляем консультации, лечение и диагностику по множественным направлениям. В том числе: гинекология, терапия, невролгия-нейрофизиология, урология, эпилептология и многие другие. По оставшимся вопросам звоните по номеру телефона +7(499)302-63-62 или закажите обратный звонок на интернет портале cecilplus.ru прямо сейчас. Ещё присутствует онлайн запись и оплата консультации для Вашего удобства.
Мы расположены по адресу: г. Москва, ул. Чаплыгина, д. 6, м. Чистые пруды. График работы с пн по сб с 9:00 до 21:00. Также на указанном сайте Вы можете посмотреть цены на наши услуги. Многие услуги могут быть выполнены с выездом к Вам домой, необходимо уточнить у консультанта.
Если Вы искали гинекология москва в интернете, то вы на верном пути. Наши специалисты на cecilplus.ru обязательно Вам помогут, ведь у них огромный опыт и постоянные повышения квалификации. Будем счастливы Вам оказать помощь обрести здоровое тело, побороть болезнь и жить полной жизнью!
Привет!
Приобрести документ института вы сможете у нас.
diplomyx24.ru/kupit-diplom-voronezh
Удачи!
Добрый день!
Приобрести диплом университета
Мы предлагаем максимально быстро приобрести диплом, который выполнен на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Диплом способен пройти любые проверки, даже с использованием специфических приборов. Решайте свои задачи быстро и просто с нашим сервисом.
Где купить диплом по нужной специальности?
avtolux48.ru/people/user/374/blog/7556/
odessaforum.getbb.ru/viewtopic.php?f=5&t=20402
mosday.getbb.ru/viewtopic.php?f=12&t=1059
vaeaem.profiforum.ru/t3822-topic#7107
ya.bestbb.ru/viewtopic.php?id=2962#p6549
На сайте https://znaki-pr.ru вы сможете ознакомиться со всеми услугами, которые оказывает редакторское бюро «Знаки препинания». Таким образом, ваши тексты будут более понятными, живыми, интересными. В компанию обращаются с песнями, смс, а также письмами и многим другим. Компетентные и лучшие специалисты, корректоры отредактируют текст, диссертацию, набор рукописей. Для того чтобы ознакомиться с тем, как происходит работа, изучите благодарные отзывы клиентов. Если и вам необходимо воспользоваться услугами, то напишите в чат.
Привет, друзья!
Диплом пту купить официально с упрощенным обучением в Москве
http://www.pets-ural.ru/content/forum//viewtopic.php?p=63885#63885
Рады оказаться полезными!.
купить диплом о среднем образовании в пензе mandiplomik.ru .
Привет, друзья!
Купить документ ВУЗа вы сможете у нас.
diploms-x.com/kupit-diplom-omsk
Удачи!
女孩
Здравствуйте!
Приобрести документ о получении высшего образования
diplomasx.com/kupit-diplom-vracha
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по выгодным ценам.
80.87.194.225/blogs/1/diplomy-attestaty-a-tak-zhe-sertifikaty-vygodnye-tseny.php
duster-clubs.ru/forum/album.php?albumid=863&pictureid=9103&commentid=4916
wutdawut.com/read-blog/2224
logan.in.ua/people/user/7276/blog/7933/
sonnick84.csublogs.com/34371489/Что-потребуется-для-производства-качественного-диплома
ж€їеђ
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по выгодным тарифам.
autogroupe.ru/poluchite-diplom-bez-lishnih-usiliy
Добрый день!
Сколько стоит диплом высшего и среднего образования и как его получить?
arusak-diploms-srednee.ru В
Добрый день!
Заказать диплом университета.
telegra.ph/Bolshoj-katalog-dokumentov-v-izvestnom-internet-magazine-07-04
Uncover the future of gaming with Musk Empire – a groundbreaking Web3 experience! Grow your business realm with zero in-app purchases. Upgrade your assets to amplify your revenue stream. Engage, earn, and down the line exchange in-game currency for real money. Enter the Musk Empire today and craft your digital fortune! URL https://tinyurl.com/muskemp
Наш сервисный центр предлагает профессиональный сервисный ремонт аймака всех типов и брендов. Мы знаем, насколько необходимы вам ваши компьютеры Apple, и стремимся предоставить услуги первоклассного уровня. Наши опытные мастера проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что предоставляет долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются пользователи моноблоков iMac, включают поломку жесткого диска, проблемы с экраном, неисправности разъемов, программные сбои и неисправности системы охлаждения. Для устранения этих поломок наши квалифицированные специалисты выполняют ремонт жестких дисков, дисплеев, разъемов, ПО и систем охлаждения. Доверив ремонт нам, вы обеспечиваете себе качественный и надежный центр ремонта imac рядом.
Подробная информация доступна на сайте: https://remont-imac-mos.ru
Привет, друзья!
Купить документ ВУЗа можно в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации.
bestnet.ru/support/forum/index.php?PAGE_NAME=profile_view&UID=137142
cobaki.ru/users.php?m=details&id=90902
j013.koreawebcenter.com/bbs/board.php?bo_table=free&wr_id=668203
farsrig.com/index.php?subaction=userinfo&user=ygawome
videopro.ru/xenforo/index.php?threads/Тестовая-тема-закреплённая.1/page-114#post-4182
kraken даркнет зеркало krakenonion site – kraken com зеркало, кракен ссылка kraken kraken2web com
נערות סקסיות וחרמניות. דירות דיסקרטיות בתל אביב זו חוויה שקשה לתאר במילים כאשר מנסים לתאר את החוויה של דירות דיסקרטיות בתל יש לך יותר מידי דאגות בראש? זהו בדיוק הזמן להרים את הטלפון ולהזמין נערות ליווי בתל אביב. ניתן להזמין אותן לדירתך או לבית המלון check out the post right here
Привет!
Заказать документ о получении высшего образования вы можете у нас в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, включая документы старого образца. Даем гарантию, что в случае проверки документов работодателем, подозрений не появится.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по доступным тарифам. Стоимость может зависеть от конкретной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для покупателей адекватную политику цен. Для нас важно, чтобы дипломы были доступны для большого количества граждан.
wegug.in/blogs/367/Купить-диплом-откройте-новые-возможности-для-своего-будущего?lang=en_us
Рады оказать помощь!
Привет!
Купить диплом о высшем образовании.
wiki.why42.ru/wiki/Широкий_ассортимент_документов_в_популярном_онлайн_магазине
Добрый день!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
ekspoteh.ru/index.php?name=account&op=info&uname=yjocowif
Рады оказаться полезными!.
Привет, друзья!
Приобрести документ о получении высшего образования
65b7bc92a079b.site123.me/Блог/Приобретаем-диплом-в-проверенном-магазине-по-выгодной-цене
permn.ru/blogs/1/diplomy-po-nizkim-tsenam-v-populyarnom-internet-magazine.php
s24.team/club/user/148/blog/1611/
octomo.co.uk/read-blog/949
x-universe.ru/index.php?title=Служба_поддержка_и_FAQ._Заказываем_диплом_в_сети
Привет, друзья!
Как получить диплом о среднем образовании в Москве и других городах
http://www.sonicetactical.ru/купить-диплом-2001/
Добрый день!
Заказать диплом о высшем образовании.
fromrus.su/index.php?/gallery/image/325-как-найти-проверенный-интернет-магазин-с-обширным-выбором-дипломов/
妈妈
Привет!
Мы готовы предложить дипломы любых профессий по доступным ценам.
sonnick84.blogpayz.com/28299725/Что-готов-сегодня-предложить-онлайн-магазин-с-дипломами
9a87bkcce.prublogger.com/27888322/Быстро-покупаем-диплом-в-известном-онлайн-магазине-russian-diplom
macadamlab.ru/wiki/index.php?title=Быстрый_поиск_интернет-магазина,_реализующего_дипломы_и_аттестаты
sonnick84.bloggip.com/28239097/Хотите-купить-диплом-Выбирайте-наш-онлайн-магазин
medbereg.ru/club/user/15/blog/4120/
Здравствуйте!
Купить документ института
clubalpintoulouse.fr/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=145
wutdawut.com/read-blog/2311
forum.zone-game.info/album.php?albumid=116&pictureid=810&commentid=479
darkgate.pl/events/event/18-дипломы-по-комфортным-ценам-в-знаменитом-онлайн-магазине/
dervislergrup.com/events/event/16-vygodnye-ceny-i-prekrasnoe-kacestvo-priobretai-diplomy-onlain/
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
last news about foden here!
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
Добрый день!
Мы можем предложить дипломы любой профессии по приятным тарифам. Стоимость будет зависеть от определенной специальности, года выпуска и университета. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас очень важно, чтобы дипломы были доступными для большого количества наших граждан.
cesarsc974.boyblogguide.com/26753515/Дипломы-за-деньги-Правда-о-Покупке-Образования-купить-диплом
The scoring system in the Aviator Game is based on the multiplier at the time of cashing out. The higher the
ivermectin purchase online
и¦еЇџ
Привет!
Мы можем предложить документы ВУЗов
ironway.ru/forum/posting.php?mode=post&f=5
odinzovo.rusff.me/viewtopic.php?id=4921#p8315
iaescortsmap.ixbb.ru/viewtopic.php?id=118#p118
artem-energo.ru/message.php?msg=151
umorfishki.ru/oformite-diplom-bez-ozhidaniya-i-problem
Привет!
Мы изготавливаем дипломы любых профессий.
advancedservicecorp.com/дипломы-купить-одесса/
Всегда вам поможем!.
Привет!
Заказать документ ВУЗа.
school8kaluga.flybb.ru/viewtopic.php?f=19&t=500
1stroitelny.kz/faq/show/id/6695002308281c2be66dce97.html
club-kia.com/forum/thread30840.html
forum.hi-def.ru/index.php?showtopic=38594
selkovo.rolka.me/viewtopic.php?id=3437#p10150
Здравствуйте!
Заказать документ о получении высшего образования
balacixynu.trexgame.net/sovety-specialista-kotorye-dadut-vozmoznost-legko-zakazat-diplom
o91746bp.beget.tech/2024/07/04/pochemu-segodnya-gorazdo-deshevle-i-prosche-kupit-diplom-vuza.html
snaprama.com/read-blog/855
sonnick84.tkzblog.com/28131503/Заказываем-диплом-в-надежном-магазине-Советы-специалистов
gutscheine-247.de/modules.php?name=Journal&file=display&jid=209
Привет!
Заказать документ о получении высшего образования
diplomasx.com/kupit-diplom-vracha
Здравствуйте!
Заказать диплом университета.
antonovschool.ru/forum/messages/forum1/topic657/message672/?result=new#message672
Удачи!
Привет, друзья!
Мы можем предложить документы ВУЗов
моя-соцсеть.рф/blogs/new
robotaforum.2bb.ru/post.php?fid=40
moneysweet.listbb.ru/viewtopic.php?f=2&t=1971
ya.forum.cool/viewtopic.php?id=5893#p17555
avrorp.getbb.ru/viewtopic.php?f=183&t=714
Glory Casino
Добрый день!
Как приобрести диплом техникума с минимальными рисками
landik-diploms-srednee.ru/diplom-s-reestromkupit-kupit В
Привет, друзья!
Приобрести документ о получении высшего образования вы сможете у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любым специальностям, включая документы образца СССР. Даем гарантию, что в случае проверки документа работодателем, подозрений не возникнет.
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по выгодным тарифам. Стоимость будет зависеть от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большого количества наших граждан.
milltelecom.com/blogs/97/Приобретаем-диплом-в-лучшем-интернет-магазине-по-выгодной-стоимости?lang=en_us
Рады помочь!
Здравствуйте!
Заказать документ о получении высшего образования можно в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов России.
gzu.fr.free.fr/nuked_klan_sp43/nk/index.php?file=Members&op=detail&autor=ezobykop
receptom.ru/index.php?subaction=userinfo&user=ytepe
http://www.dxzw.com/member/index.php?uid=ogabudul
silkhunter.com/index.php?title=gosznacdiplomy
новодвинцы.рф/forum/messages/forum4/topic840/message264406/?result=reply#message264406
become a realtor in sc http://www.realestatelicensengdfdgh.com what do you need to be a real estate realestatelicensengdfdgh.com/states/florida-real-estate-license/ .
Наши специалисты предлагает профессиональный сервис ремонта индукционной плиты на дому любых брендов и моделей. Мы знаем, насколько важны для вас ваши индукционные варочные панели, и обеспечиваем ремонт первоклассного уровня. Наши профессиональные техники работают быстро и аккуратно, используя только оригинальные запчасти, что гарантирует надежность и долговечность проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются пользователи индукционных варочных панелей, включают неисправности нагревательных элементов, проблемы с кнопками управления, программные сбои, проблемы с подключением и повреждения корпуса. Для устранения этих поломок наши профессиональные техники оказывают ремонт нагревательных элементов, сенсорных панелей, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы гарантируете себе качественный и надежный сервисный центр по ремонту индукционных плит в москве.
Подробная информация доступна на сайте: https://remont-indukcionnyh-plit-now.ru
Привет, друзья!
Мы готовы предложить документы ВУЗов
lolipopnews.ru/nadezhnoe-oformlenie-diplomov
visacart.80lvl.ru/viewtopic.php?f=1&t=802
jagplay.ekafe.ru/viewtopic.php?f=22&t=4176
severka.flybb.ru/viewtopic.php?f=6&t=381
stars.flyboard.ru/viewtopic.php?f=1&t=992
All the latest news about cryptocurrencies can be read here cryptonewday
Привет, друзья!
Приобрести документ института можно в нашей компании.
diplomyx.com/kupit-diplom-chelyabinsk
Привет!
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по приятным ценам.
http://www.elegantbeautyhk.com/купить-диплом-мархи-2/
this hyperlink trader joe
Добрый день!
Купить документ института.
samara.listbb.ru/viewtopic.php?f=3&t=366
newsofgames.ru/nadezhnaya-pokupka-diplomov
superforum.spybb.ru/viewtopic.php?id=2743#p50769
daddycow.com/blogs/view/24730mirmafii.ru/article/7570
thelspr.listbb.ru/viewtopic.php?f=13&t=361
Добрый день!
Заказать документ университета вы можете у нас в столице.
ast-diplom.com/kupit-diplom-chelyabinsk
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
last news about foden here!
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
foden
жЎҐ
Привет, друзья!
Мы предлагаем дипломы любых профессий по приятным ценам. Цена будет зависеть от конкретной специальности, года выпуска и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступными для большого количества наших граждан.
active-bookmarks.com/story17018330/купить-диплом-врача
Добрый день!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
animesocial.su/blogs/2461/Купите-Диплом-для-Вашего-Успеха
Привет, друзья!
Купить документ ВУЗа.
iaescortsmap.ixbb.ru/viewtopic.php?id=115#p115
derivsocial.org/read-blog/2619
antonovschool.ru/forum/topic/add/forum1/#postform
o91707v5.beget.tech/2024/07/15/diplomy-s-garantiey-oficialnosti.html
fliping.freehostia.com/wiki/index.php?search=&go=Ir
Привет, друзья!
Приобрести документ о получении высшего образования можно у нас в Москве.
ast-diplomas.com/kupit-diplom-novosibirsk
Здравствуйте!
Заказать документ университета можно в нашей компании.
ast-diplom24.ru/otzyvy
Успехов в учебе!
Привет, друзья!
Заказать документ ВУЗа
ozoms.com/read-blog/448
spooo.ru/post/article/217872
firstplat.com/read-blog/12286
autism-support.mn.co/posts/61748464
contraband.ch/read-blog/4063
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашей компании.
diplomasx.com/kupit-diplom-omsk
Удачи!
Привет, друзья!
Купить документ о получении высшего образования.
define.listbb.ru/viewtopic.php?f=46&t=522
entrainment.listbb.ru/viewtopic.php?f=96&t=24256
demo.advised360.com/read-blog/161965
cardinalparkmld.listbb.ru/viewtopic.php?f=3&t=467
angelladydety.getbb.ru/posting.php?mode=post&f=46&sid=8ab65b996ddaf75d3f14a18397d4f386
朋友
Bonus bez depozytu lub innymi slowami darmowy bonus to nic innego jak gratis oferowany przez kasyna online dla swoich graczy bonusy w kasynach bez depozytu
Hiya very nice website!! Guy .. Excellent .. Superb .. I’ll bookmark your blog and take the feeds also? I am glad to seek out a lot of useful information right here within the put up, we want develop more techniques in this regard, thanks for sharing. . . . . .
официальный сайт драгон мани казино
Здравствуйте!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов России. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Даем гарантию, что в случае проверки документов работодателями, каких-либо подозрений не возникнет.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по разумным ценам. Цена будет зависеть от определенной специальности, года получения и университета. Стараемся поддерживать для клиентов адекватную ценовую политику. Для нас важно, чтобы дипломы были доступными для большого количества наших граждан.
nybodyart.com/forums/gallery/image/8-приобретаем-диплом-в-известном-онлайн-магазине-по-выгодной-цене/
Всегда вам поможем!
家еє
improved mobile compatibility. Developers continually use this feedback to enhance the game and provide a better
ivermectin buy online
Здравствуйте!
Приобрести документ о получении высшего образования можно в нашей компании.
diplomyx24.ru/kupit-diplom-magistra
Успешной учебы!
Добрый день!
Мы можем предложить документы техникумов
rulezrp.listbb.ru/viewtopic.php?f=2&t=626
ai-db.science/wiki/Быстрый_и_надежный_способ_получить_диплом
volnodumie.bbmy.ru/viewtopic.php?id=13228#p27055
terios2.ru/forums/index.php?autocom=gallery&req=si&img=3081
skazkademjanovo.ru/?post_type=topic&p=419630
Do you have any video of that? I’d like to find out some additional information.
регистрация драгон мани казино
Наша мастерская предлагает высококачественный мастерская по ремонту айпада на дому всех типов и брендов. Мы осознаем, насколько значимы для вас ваши планшеты Apple, и обеспечиваем ремонт наилучшего качества. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что предоставляет надежность и долговечность выполненных работ.
Наиболее частые неисправности, с которыми сталкиваются пользователи планшетов Apple, включают неисправности дисплея, поломку батареи, ошибки ПО, проблемы с портами и механические повреждения. Для устранения этих неисправностей наши профессиональные техники выполняют ремонт экранов, батарей, ПО, разъемов и механических компонентов. Обратившись к нам, вы гарантируете себе долговечный и надежный ремонт айпада адреса.
Подробная информация представлена на нашем сайте: https://remont-ipad-pro.ru
Здравствуйте!
Купить диплом любого университета.
carolinahurricanesclub.com/read-blog/541
Привет, друзья!
Купить диплом любого ВУЗа.
test.bpal.org/blogs/entry/8394-как-найти-надежный-магазин-с-обширным-каталогом-дипломов/
Здравствуйте!
Где купить диплом по нужной специальности?
usa.life/read-blog/62808
Привет, друзья!
Мы предлагаем дипломы любой профессии по выгодным ценам. Цена может зависеть от выбранной специальности, года получения и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику тарифов. Важно, чтобы дипломы были доступны для большинства граждан.
trevorpb589.activablog.com/26818672/Дипломы-за-деньги-Правда-о-Покупке-Образования-купить-диплом
男孩
Добрый день!
Как официально купить аттестат 11 класса с упрощенным обучением в Москве
zingcorp.com.au/component/kunena/sub-category-locked/60951#60988
Рады помочь!.
Привет, друзья!
Приобрести диплом университета.
volmir.club/index.php?/gallery/image/119-как-подобрать-проверенный-магазин-с-широким-выбором-дипломов/
Привет!
Купить диплом ВУЗа.
ya.forum.cool/viewtopic.php?id=5657#p17026
Удачи!
Добрый день!
Приобрести документ университета можно в нашей компании.
ast-diploms.com/kupit-diplom-bakalavra-ili-specialista
Привет!
Приобрести диплом института
army.clanfm.ru/viewtopic.php?f=2&t=38994
silkhunter.com/index.php?title=официальные_дипломы_для_всех_специальностей
paintball-keller-lev.de/viewtopic.php?f=3&t=100163
csexpert.4adm.ru/viewtopic.php?f=70&t=2081
forex.g-talk.ru/viewtopic.php?f=43&t=7173
з”µеЅ±
Привет, друзья!
Диплом для вас
bmc.ukrbb.net/viewtopic.php?f=8&t=13939
mafiaclans.ru/viewtopic.php?f=43&t=7667
worldgonews.ru/oformlenie-diplomov-po-dostupnyim-tsenam
pro-novostroyki.ru/index.php?showtopic=20863
mirstalkera.4admins.ru/viewtopic.php?f=50&t=2127
Привет, друзья!
Заказать диплом ВУЗа.
277469.simplecloud.ru/blogs/1/kak-podobrat-proverennyy-magazin-s-ogromnym-vyborom-diplomov.php
Привет!
Купить диплом любого университета:
onlineboxing.net/jforum/user/profile/294128.page
forum.thelostkeepers.ru/index.php?/topic/14154-купить-диплом-c361r/
mc-pe.net/index.php?subaction=userinfo&user=ilonarir
sosh13.pascal.ru/forum/profile.php?action=show&member=22554
gpp.innim.ru:81/forums/topic/3579/diplomandoci/view/post_id/3596
Привет!
Быстрая схема покупки диплома старого образца: что важно знать?
softerioninc.com/купить-диплом-в-киселевске/
Здравствуйте!
Мы изготавливаем дипломы любой профессии.
wegug.in/blogs/984/Быстрое-Оформление-Дипломов-Надежно-и-Легально
Поможем вам всегда!.
Добрый день!
Мы изготавливаем дипломы любых профессий по невысоким ценам.
http://www.elegantbeautyhk.com/купить-диплом-мархи-2/
Уролог в Москве cecilplus.ru
По поводу уролог клиника москва мы Вам с удовольствием окажем помощь. Предлагаем консультации, полное лечение и диагностику по множественным направлениям. В том числе: гинекология, терапия, невролгия-вегетология, урология, эпилептология и многие другие. По оставшимся вопросам звоните по телефону +7(499)302-63-62 или оформите обратный звонок на интернет сайте cecilplus.ru прямо сейчас. Ещё есть интернет запись и оплата приема для Вашего удобства.
Добрый день!
Заказать документ ВУЗа
sonnick84.shoutmyblog.com/27874655/Советы-по-покупки-документа-в-сети
goodnow.mn.co/posts/61639417
sslaziofansclub.com/read-blog/3198
forextema.com/index.php?option=com_easyblog&view=entry&id=10428&Itemid=87
exoltech.us/blogs/206420/Желаете-приобрести-аттестат-у-надежного-исполнителя-Ждем-Вас
Привет!
Заказать документ о получении высшего образования вы сможете в нашей компании в Москве.
diplomasx.com/kupit-diplom-vracha
Хорошей учебы!
Добрый день!
Купить документ института можно у нас. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить диплом по любой специальности, любого года выпуска, включая документы образца СССР. Даем гарантию, что при проверке документов работодателями, каких-либо подозрений не возникнет.
familyportal.forumrom.com/viewtopic.php?id=23177#p60214
crowd-out.social/read-blog/154
plplatoon.com/gallery/image/121-каталог-и-варианты-доставки-в-магазине-покупаем-диплом/
x70795vj.beget.tech/2024/07/07/bystroe-oformlenie-diplomov-dostupno-i-nadezhno.html
sabrina-online.su/wiki/index.php?title=Какие_интернет_магазины_с_документами_есть_на_текущий_день?
Добрый день!
Заказать диплом любого ВУЗа
Наши специалисты предлагают быстро и выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями. Диплом пройдет любые проверки, даже с использованием специального оборудования. Достигайте цели быстро с нашим сервисом.
Где приобрести диплом по необходимой специальности?
antoinegriezmannclub.com/read-blog/2388
twikkers.nl/blogs/238134/Настоящие-дипломы-без-лишних-вопросов
http://www.rrsclub.ru/showthread.php?p=44674#post44674
alik.forumrpg.ru/viewtopic.php?id=6853#p276083
minecraftcommand.science/forum/general/topics/3be39c1f-4a13-418f-afea-d26499cb0d1c
家庭
Добрый день!
Купить диплом любого ВУЗа.
roving.club/read-blog/1002
жњ‹еЏ‹
Добрый день!
Купить диплом университета.
domovou.3nx.ru/viewtopic.php?p=6335#6335
Успешной учебы!
Наши специалисты предлагает высококачественный сервисный ремонт айфона в москве всех типов и брендов. Мы понимаем, насколько важны для вас ваши устройства iPhone, и готовы предложить сервис наилучшего качества. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что предоставляет долговечность и надежность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются владельцы iPhone, включают неисправности дисплея, неисправности аккумулятора, программные сбои, неработающие разъемы и поломки корпуса. Для устранения этих проблем наши профессиональные техники выполняют ремонт экранов, батарей, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы получаете долговечный и надежный официальный ремонт iphone рядом.
Подробная информация размещена на сайте: https://remont-iphone-sot.ru
Заказать диплом университета.
ratingforex.ru/forum-forex/viewtopic.php?f=18&t=40990&sid=e64ff0e11acab3f7a177f69322469c8c
club.sabaylok.com/blogs/4901/Быстрое-Оформление-Дипломов-Надежно-и-Легально
p99946c6.beget.tech/2024/07/09/kupit-diplom-onlayn-prosto-i-udobno.html
familyportal.forumrom.com/viewtopic.php?id=23252#p60349
tradersopen.com/login/login
Привет, друзья!
Приобрести документ ВУЗа
nova-driving-school.mn.co/posts/61638907
medbereg.ru/club/user/15/blog/4120/
o91746bp.beget.tech/2024/07/09/otlichnye-rascenki-i-idealnoe-kachestvo-dokumenty-onlayn.html
forum.unrivaled.ro/index.php?/gallery/image/531-ассортимент-и-методы-доставки-в-интернет-магазине-заказываем-диплом/
sonnick84.blogsvila.com/28363954/Что-может-сейчас-предоставить-интернет-магазин-с-дипломами
Привет!
Как быстро и легально купить аттестат 11 класса в Москве
http://www.chaodisiaque.com/forum/viewtopic.php?pid=21984
Добрый день!
Мы готовы предложить дипломы психологов, юристов, экономистов и любых других профессий по доступным тарифам.
intakem.com/куплю-диплом-рф/
Привет, друзья!
Приобрести диплом университета
jetem.ru/member.php?u=21901
veneraroleplay.listbb.ru/viewtopic.php?f=4&t=328
panther.80lvl.ru/index.php
csexpert.4adm.ru/viewtopic.php?f=70&t=2083
moskvic.actieforum.com/t3749-topic#7040
Здравствуйте!
Мы готовы предложить документы техникумов
wecanchat.mn.co/posts/62529664
goup.hashnode.dev/legko-poluchite-diplom-za-schitannye-dni
drovokol.ru/forum/user/12188/
kinopuk.ru/viewtopic.php?id=9108#p56713
forummsk.getbb.ru/viewtopic.php?f=12&t=2717
Привет!
Диплом специалиста
veneraroleplay.listbb.ru/viewtopic.php?f=4&t=329
foro.rune-nifelheim.com/general-ragnarok-m/vysokokachestvennye-diplomy-na-zakaz/
argayash.flybb.ru/viewtopic.php?f=9&t=1173
чпуремонт.рф/showthread.php?tid=56798
playable.nl/forum/viewtopic.php?t=801963&sid=008fbee1f6be10a14db6295d6d010a51
The Aviator Game offers multiplayer options that allow players to compete against each other in real-time. This
ivermectin online
Привет!
Мы изготавливаем дипломы.
etoprosto.ru/ru/forum/?category=5&action=topic
injectorcar.ru/forum/member.php?u=34916
niceroleplay.getbb.ru/posting.php?mode=post&f=1
militarymuster.ca/forum/member.php
wiki.nikiforov.ru/index.php/Ваш_Настоящий_Диплом:_Быстро_и_Удобно
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
thcsphuhuu.pgdchauthanhdt.edu.vn/купить-диплом-о-среднем-техническом-о/
leeds-welcome.com
Привет!
Приобрести диплом любого университета.
imhht.com/index.php?title=Как_подобрать_надежный_онлайн_магазин_с_большим_выбором_дипломов?
mrec mississippi realestatelicensengdfdgh.com/states/ohio-real-estate-license/ where to get a real estate license realestatelicensengdfdgh.com .
Привет, друзья!
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий.
thecareerer.com/wordpress/2024/07/14/купить-диплом-о-среднем-образовании-в/
Рады оказать помощь!.
Здравствуйте!
Купить диплом о высшем образовании.
ashinova.ru/category-5/t-1504.html#1504
Удачи!
Привет, друзья!
Мы готовы предложить документы техникумов
niecewicz.flybb.ru/viewtopic.php?f=34&t=901
anatoliyrud.ekafe.ru/viewforum.php?f=29
funnywipes.maxbb.ru/viewtopic.php?f=3&t=669
funchange.getbb.ru/viewtopic.php?f=8&t=1414
чпуремонт.рф/showthread.php?tid=56881
Привет, друзья!
Заказать документ о получении высшего образования.
gromscream.80lvl.ru/viewtopic.php?f=3&t=2091
aromatov.wooden-rock.ru/forum/topic.php?forum=1&topic=16122
carbonfacesocial.org/blogs/78886/Ваш-диплом-за-короткое-время-просто-и-удобно
jagplay.ekafe.ru/viewtopic.php?f=22&t=4165
saumalkol.com/forum/разное-2/3592-легальный-диплом-без-лишних-хлопот-узнайте-как.html
На сайте https://singapore-company.ru/ уточните информацию относительно того, как правильно произвести регистрацию своей компании в Сингапуре. Это государство выбирают по той причине, что оно является одним из самых развитых, в нем особая инфраструктура. Компания поможет вам открыть бизнес, даст профессиональную консультацию. Здесь работают компетентные, лучшие специалисты, которые знают, как вам открыть свое дело. В разделе вы найдете данные о том, как правильно зарегистрировать предприятие и какие документы для этого понадобятся.
Привет!
Мы предлагаем дипломы любых профессий по разумным ценам.
ourfathersfamily.com/blogs/2385/Как-купить-сейчас-неотличимый-от-подлинника-диплом-в-сети
Привет, друзья!
Приобрести документ института вы можете в нашей компании в столице.
ast-diploms.com/kupit-diplom-s-registraciej
dominicanrental.com
Привет!
Купить документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы получите диплом по любой специальности, любого года выпуска, в том числе документы старого образца. Даем 100% гарантию, что в случае проверки документов работодателем, каких-либо подозрений не появится.
fantok.net/blogs/465/Что-потребуется-для-изготовления-качественного-диплома
worldgonews.ru/vyisshee-obrazovanie-dlya-vas-legalno-i-byistro
newfinbiz.ru/vash-nastoyashhiy-diplom-byistro-i-konfidentsialno
silich.ru/forum/member.php?u=4810
ourehelp.com/read-blog/3823
Привет!
Купить диплом любого университета
Мы предлагаем быстро и выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями. Данный диплом пройдет любые проверки, даже при помощи профессиональных приборов. Достигайте свои цели быстро и просто с нашей компанией.
Где приобрести диплом специалиста?
alex-neil.ru/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=238
ya.0bb.ru/viewtopic.php?id=11945#p31885
galantclub.od.ua/member.php?u=15983
wayworld.listbb.ru/viewtopic.php?f=2&t=24662
laziofansclub.com/read-blog/1312
Здравствуйте!
Купить диплом любого университета.
wakelet.com/wake/axJRjnZ0uA5z2DVCnmsQv
newsbig.bearsfanteamshop.com/pravilno-priobretaem-diplom-v-seti-ekspertnyj-obzor
asbl-numerica.be/blogs/234/Подробное-описание-приобретения-документов-в-известном-магазине
crowd-out.social/read-blog/184
chrstms.ru/club/user/11503/blog/11066/
Наши специалисты предлагает надежный мастер по ремонту кофемашина в москве всех типов и брендов. Мы понимаем, насколько важны для вас ваши кофемашины, и стремимся предоставить услуги первоклассного уровня. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что обеспечивает долговечность и надежность наших услуг.
Наиболее частые неисправности, с которыми сталкиваются владельцы кофемашин, включают проблемы с нагревом, проблемы с подачей воды, программные сбои, проблемы с подключением и поломки корпуса. Для устранения этих неисправностей наши опытные мастера оказывают ремонт нагревательных элементов, насосов, ПО, разъемов и механических компонентов. Обратившись к нам, вы обеспечиваете себе качественный и надежный починить кофемашин в москве.
Подробная информация представлена на нашем сайте: https://remont-kofemashin-top.ru
Привет, друзья!
Приобрести документ университета.
beijingpal.com/read-blog/1026
l90226mw.beget.tech/2024/07/12/vash-put-k-uspehu-s-nashim-diplomom.html
burgasdent.listbb.ru/viewtopic.php?f=3&t=392
local-urban-eats.mn.co/posts/62241941
talkitter.com/create-blog/
Привет!
Получить диплом о высшем образовании
krugozorov.ru/forum/user/9250/
konstruktiv.getbb.ru/viewtopic.php?f=17&t=6833
newsbeautiful.ru/diplomyi-na-zakaz-dlya-vseh-spetsialnostey/
moskovskij.getbb.ru/viewtopic.php?f=12&t=3097
niagarafallspal.com/read-blog/1208
Привет!
Диплом экономиста
soad.msk.ru/forum/posting.php?mode=newtopic&f=16
dp.getbb.ru/viewtopic.php?f=3&t=768
vipka.mybb.ru/viewtopic.php?id=2918#p5169
dexanet.ukrbb.net/viewtopic.php?f=5&t=16513
t67747az.beget.tech/2024/07/20/vash-diplom-o-vysshem-obrazovanii-shag-k-novym-vozmozhnostyam.html
Добрый день!
Купить документ о получении высшего образования можно в нашей компании в Москве.
asxdiplomik.com/kupit-diplom-s-registraciej
Здравствуйте!
Купить диплом ВУЗа.
ourownnetwork.mn.co/posts/61724527
Здравствуйте!
Заказать документ о получении высшего образования.
openmotonews.ru/oformlenie-diplomov-s-minimalnyimi-zatratami
mimozem.4admins.ru/viewtopic.php?f=98&t=4987
besconeshnocte.flybb.ru/viewtopic.php?f=2&t=953
mangorpp.getbb.ru/viewtopic.php?f=3&t=463
pipewiki.org/app/index.php/Быстрая_покупка_дипломов_онлайн
е‡єеЋ»
Привет, друзья!
Купить документ о получении высшего образования вы можете в нашем сервисе.
ast-diploms.com/kupit-diplom-vracha
Удачи!
е› з‚є
Привет!
Купить документ о получении высшего образования вы имеете возможность в нашей компании. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации.
adsauto.info/index.php?subaction=userinfo&user=yvupuv
qbko.ru/index.php?subaction=userinfo&user=ezenyde
uralremput.ru/index.php?subaction=userinfo&user=asosozyhe
helenos.pavel-rimsky.cz/doku.php?id=premiummdiplomms
http://www.fromearth.kr/bbs/board.php?bo_table=free&wr_id=447850
жњ‰
雖然
Здравствуйте!
Где заказать диплом по нужной специальности?
vina-net.ru/
Здравствуйте!
Заказать документ университета
talkiachat.com/blogs/27/Легко-приобретаем-документы-в-онлайн-магазине-Russian-Diplom
asbl-numerica.be/blogs/234/Подробное-описание-приобретения-документов-в-известном-магазине
transformationarena.com//read-blog/53
demo.1c-college.ru/club/user/7/blog/zakazyvaem-dokumenty-v-izvestnom-onlaynmagazine-po-komfortnoy-tsene/
wiki.roximo.ru/index.php/Легкий_выбор_онлайн-магазина,_реализующего_дипломы
Привет!
Приобрести документ о получении высшего образования можно в нашем сервисе.
diplomasx24.ru/kupit-diplom-krasnoyarsk
Удачи!
Наши специалисты предлагает надежный отремонтировать компьютер с гарантией различных марок и моделей. Мы знаем, насколько значимы для вас ваши компьютеры, и обеспечиваем ремонт наилучшего качества. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что обеспечивает длительную работу проведенных ремонтов.
Наиболее частые неисправности, с которыми сталкиваются пользователи ПК, включают поломку жесткого диска, неисправности видеокарты, неисправности программного обеспечения, неработающие разъемы и перегрев. Для устранения этих проблем наши профессиональные техники оказывают ремонт жестких дисков, видеокарт, ПО, разъемов и систем охлаждения. Обратившись к нам, вы гарантируете себе долговечный и надежный вызвать мастера по ремонту компьютеров на выезде.
Подробная информация представлена на нашем сайте: https://remont-kompyuterov-vip.ru
Player Reviews and Testimonials
ivermectin for sale
Здравствуйте!
Приобрести диплом любого университета
Наша компания предлагает быстро и выгодно заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями. Данный диплом пройдет лубую проверку, даже с применением специальных приборов. Решайте свои задачи максимально быстро с нашим сервисом.
Где купить диплом специалиста?
ya.10bb.ru/viewtopic.php?id=3615#p6544
3drus.ru/forum/topic_34806
nedvigimost.bbok.ru/viewtopic.php?id=26650#p45740
slliver.getbb.ru/viewtopic.php?f=62&t=826
ya.2bb.ru/viewtopic.php?id=19040#p240217
Привет, друзья!
Приобрести диплом ВУЗа.
prof-komplekt.com/club/user/1035/blog/11031/
Добрый день!
Приобрести диплом любого университета:
amvnews.ru/forum/posting.php?mode=newtopic&f=44
renebiemans.nl/users.php?m=details&id=32281
videopro.ru/xenforo/index.php?threads/Тестовая-тема-закреплённая.1/page-113#post-4148
fromearth.kr/bbs/board.php?bo_table=free&wr_id=447232
school5.p-fam.ru/users/uwitari
pics porn gif – http://gifsex.ru/
Twig b take hold field of view of porn GIF exhilaration gif on the side of free. Look porn gifs, GIF glow is a split cosmos to keep safe as the bank of england the most causticity of any porn video clip without normal in the accumulation of credible imprint pictures.
http://gifsex.ru/
Pinup ar
Place your bet at pin up online – very reliable bookmaker
Pinup casino
מזמינים את הנערות היפות, הן נותנות את כל מה שהן יכולות על מנת לגרום לגבר עונג. הן משתמשות בכל גופן על מנת לרגש את הגבר. ויש להן יחדיו עם נערות חרמניות וזורמות. הן רק מחפשות לבלות, והן לא מחפשות לסבך את העניינים. הן רק רוצות שהיה לך טוב ונעים. והן גם שירותי מין
Добрый день!
Заказать диплом университета.
chat-hozn3.com/blogs/13097/Что-сможет-сейчас-предложить-интернет-магазин-с-дипломами
ebonyfaces.com/blogs/36/Быстро-заказываем-документы-в-лучшем-онлайн-магазине-Russian-Diplom
exoltech.us/blogs/206966/Приобретаем-документы-в-надежном-интернет-магазине-Советы-эксперта
investforum.com.br/index.php?/gallery/image/5-почему-гораздо-проще-и-дешевле-заказать-диплом-вуза/
noirconnection.com//read-blog/1404
е‡єзЏѕ
Привет!
Мы готовы предложить документы ВУЗов
moskvic.actieforum.com/t3747-topic#7038
forexrassia.ru/legalno-i-byistro-oformite-diplom-onlayn
power.ekafe.ru/viewtopic.php?f=2&t=1763
transexit.g-talk.ru/viewtopic.php?f=10&t=2137
daddycow.com/blogs/view/25775
Добрый день!
Приобрести документ о получении высшего образования.
little-witch.ru/forum99.html
rorp.4admins.ru/viewforum.php?f=33
pets-ural.ru/content/forum/viewtopic.php?p=81836#81836
drugisaitove.listbb.ru/viewtopic.php?f=2&t=642
human.forumieren.de/t312-topic#382
Привет!
Заказать документ о получении высшего образования
sonnick84.pointblog.net/Что-понадобится-для-создания-качественного-диплома-ВУЗа-69447016
twanty2.com/read-blog/181
nbcsocial.com/read-blog/6276
indianhighcaste.com/read-blog/2120
hulu-com-forgot.mn.co/posts/61838001
Здравствуйте!
Приобрести диплом любого университета.
test.kuli4kam.net/gallery/image/534-как-подыскать-надежный-онлайн-магазин-с-огромным-каталогом-дипломов/
ж„ЏжЂќжЇ
Здравствуйте!
Заказать документ о получении высшего образования можно в нашем сервисе. Мы оказываем услуги по продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любым специальностям, включая документы образца СССР. Даем 100% гарантию, что в случае проверки документов работодателями, никаких подозрений не возникнет.
Мы изготавливаем дипломы любых профессий по приятным ценам. Цена будет зависеть от той или иной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для покупателей адекватную политику цен. Важно, чтобы документы были доступны для большинства наших граждан.
bondhusova.com/blogs/61136/Как-можно-недорого-заказать-диплом-в-онлайн-магазине/
Рады оказаться полезными!
еі¶
https://e-porn.net
https://analwife.net
free xxx tube videos webcams dating,
онлайн камеры, знакомства
Привет, друзья!
Купить документ института
mighty-networks-foundation.mn.co/posts/61679287
wallazz.com/blogs/205543/Подробное-описание-приобретения-диплома-в-популярном-онлайн-магазине
sonnick84.blogrelation.com/34226505/Как-купить-сейчас-неотличимый-от-подлинника-диплом-в-сети-интернет
indianapal.com/read-blog/820
artisthub.mn.co/posts/61748293
女е©
Здравствуйте!
Заказать документ о получении высшего образования
diplomasx.com/kupit-diplom-nizhnij-novgorod
Полезные советы по покупке диплома о высшем образовании без риска
ast-diplomas.com/kupit-diplom-rostov-na-donu
[b]Купить диплом любого университета.[/b]
[url=http://fish-sea-products.ru/forum/user/5823//]fish-sea-products.ru/forum/user/5823/[/url]
[url=http://chaodisiaque.com/forum/viewtopic.php?pid=22032#p22032/]chaodisiaque.com/forum/viewtopic.php?pid=22032#p22032[/url]
[url=http://justvoip.listbb.ru/posting.php?mode=post&f=2&sid=e424393dc21963be749aec230f1ee5bb/]justvoip.listbb.ru/posting.php?mode=post&f=2&sid=e424393dc21963be749aec230f1ee5bb[/url]
[url=http://fishing.ukrbb.net/posting.php?mode=post&f=21&sid=75ced025f4126ce57c33aa2c42e1f421/]fishing.ukrbb.net/posting.php?mode=post&f=21&sid=75ced025f4126ce57c33aa2c42e1f421[/url]
[url=http://forexrassia.ru/diplomyi-ot-nadezhnogo-postavshhika/]forexrassia.ru/diplomyi-ot-nadezhnogo-postavshhika[/url]
Привет, друзья!
Приобрести документ ВУЗа можно у нас в Москве.
asxdiplomik.com/kupit-diplom-s-registraciej
Привет, друзья!
Где приобрести диплом специалиста?
http://www.emoneyspace.com/paulsmith7
Добрый день!
Вопросы и ответы: можно ли быстро купить диплом старого образца?
landik-diploms-srednee.ru/kupit-diplom-v-ekaterinburge В
Наша мастерская предлагает профессиональный сервисный ремонт кондиционеров на выезде различных марок и моделей. Мы осознаем, насколько значимы для вас ваши охладительные системы, и стремимся предоставить услуги высочайшего уровня. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только качественные детали, что обеспечивает длительную работу выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются владельцы кондиционеров, включают неисправности компрессора, неработающий вентилятор, ошибки ПО, неработающие датчики и поломки корпуса. Для устранения этих неисправностей наши профессиональные техники оказывают ремонт компрессоров, вентиляторов, ПО, датчиков и механических компонентов. Обращаясь в наш сервисный центр, вы получаете надежный и долговечный официальный ремонт кондиционеров на дому.
Подробная информация размещена на сайте: https://remont-kondicionerov-wow.ru
Привет!
Купить документ о получении высшего образования
licomklicu.ru/read-blog/877
kurkure.ru/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=147
bestchristian.com/read-blog/1882
chumcity.xyz/read-blog/250
blooder.net/read-blog/63854
Записать на прием к гинекологу Москва cecilplus.ru
Если Вы планировали найти ээг где сделать в москве в сети интернет, то вы на правильном пути. Наши врачи на cecilplus.ru обязательно Вам помогут, ведь у них колоссальный опыт и регулярные повышения в своей сфере. Будем счастливы Вам оказать помощь обрести здоровье, побороть болезнь и жить полной жизнью!
Добрый день!
Как безопасно купить диплом колледжа или ПТУ в России, что важно знать
gta-balkan.com/events/event/42-четыре-главных-группы-онлайн-магазинов-что-продают-документы/
Добрый день!
Мы изготавливаем дипломы любой профессии по выгодным ценам.
http://www.vaca-ps.org/blogs/163462/¬аш-ѕуть-к-¬ысшему-ќбразованию- упить-?иплом
Привет!
Мы готовы предложить дипломы любой профессии по приятным тарифам.
renaissance.mn.co/posts/61748148
sonnick84.bloggerswise.com/34731485/Ищем-проверенный-и-надежный-онлайн-магазин-для-приобретения-диплома
edusocial.online/blogs/118/Известный-онлайн-магазин-с-привлекательными-по-цене-дипломами
sonnick84.blog5.net/69975918/Дипломы-и-сертификаты-низкие-цены
sonnick84.blog-ezine.com/28317450/Как-купить-сегодня-неотличимый-от-подлинника-диплом-в-сети
נעזרים בשירות זה. מקצינים בקרייה, דרך מרצים מהאוניברסיטה ועד מנהלים בכירים בחברות הייטק. לכולם חשובה הדיסקרטיות, והם יכולים כאשר יש בילוי או מסיבה, ורוצים להרים את מצב הרוח אפשר תמיד להזמין אותן. גברים אוהבים להגשים את החלומות שלהם. וזה נכון גם כאשר מכוני ליווי באשדוד, איך מוצאים?
Здравствуйте!
Мы изготавливаем дипломы.
openmotonews.ru/kak-kupit-diplom-bez-lishnih-hlopot
lubov.listbb.ru/viewtopic.php?f=2&t=476
tawasol1.mn.co/posts/61678836
daddycow.com/blogs/view/23718
o91707v5.beget.tech/2024/07/08/kupit-diplom-bez-posrednikov-legko-i-bezopasno.html
Привет!
Мы изготавливаем дипломы любой профессии по приятным тарифам. Цена будет зависеть от выбранной специальности, года получения и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику цен. Важно, чтобы дипломы были доступны для подавляющей массы граждан.
johnnyzh186.humor-blog.com/26678699/Фальшивый-диплом-Почему-это-не-Стоит-купить-диплом
Top News Sites for article Post
chinaworldnewstoday.com
chroniclenewstoday.com
cnbcnewstoday.com
cnnworldtoday.com
crunchbasenewstoday.com
dailyexpressnewstoday.com
Don’t hesiate to conatct us.
Привет!
Приобрести диплом университета:
certificate.winko.net/bbs/board.php?bo_table=free&wr_id=293120
city-hall.nvkb.ru/forum/index.php/user/101000/
classicalmusicmp3freedownload.com/ja/index.php?title=premiummdiplomms
wiki.hightgames.ru/index.php?title=gosznacdiplomy
agrosoft.ru/support/forum/index.php?PAGE_NAME=profile_view&UID=85521
и·‘жҐ
Привет!
Мы предлагаем дипломы любой профессии по приятным ценам.
telegra.ph/kupit-diplom-o-vysshem-obrazovanii-03-26
Привет!
Купить диплом любого университета
Наши специалисты предлагают выгодно и быстро заказать диплом, который выполнен на оригинальной бумаге и заверен печатями, штампами, подписями официальных лиц. Диплом способен пройти любые проверки, даже при использовании специально предназначенного оборудования. Достигайте свои цели быстро и просто с нашим сервисом.
Где приобрести диплом специалиста?
alanyatoday.ru/users/76
seriallove.bbok.ru/viewtopic.php?id=7015#p123048
goup.hashnode.dev/kupit-diplom-1-1-1
kino.10bb.ru/viewtopic.php?id=163545#p276485
forumkk.listbb.ru/viewtopic.php?f=12&t=392
Добрый день!
Приобрести документ университета вы сможете в нашей компании в столице.
ast-diplom.com/kupit-diplom-o-srednem-obrazovanii
Успешной учебы!
Найдите свою следующую возможность карьерного роста с Категорией вакансий
Устали раздавать резюме, не получая ответа? Каталог вакансий поможет вам найти работу вашей мечты:
Просмотрите тысячи актуальных вакансий от проверенных работодателей.
работа в колл-центре без опыта
Настройте свои оповещения о вакансиях, чтобы первым получать информацию о новых возможностях.
Узнайте о тенденциях рынка труда и советах по карьере от наших экспертов.
Получите мгновенный доступ к контактной информации работодателей и веб-сайтам.
работа курьером с личным автомобилем
Подайте заявку на несколько вакансий одновременно с нашей удобной системой управления приложениями.
еЃҐеє·
Привет!
Мы изготавливаем дипломы любой профессии по приятным ценам.
wpfreelance.boxthemes.net/диплом-магистра-2014-20242024-фото/
Привет, друзья!
Мы готовы предложить документы ВУЗов
forum.vorchun.ru/posting.php?mode=post&f=2
avtobestnews.ru/diplomyi-vedushhih-vuzov-dlya-uspeshnogo-budushhego
forum.veterinar.ru/member.php?524909-worksale
woman.build2.ru/viewtopic.php?id=14728#p45028
niceroleplay.getbb.ru/viewtopic.php?f=1&t=1275
enjoyable.
ivermectin for sale
дёЂеЂ‹з®Ўеђ
На сайте https://poshnevye-kompressory.ru изучите информацию, которая касается поршневого компрессора. Вы узнаете о том, в каких случаях используется, о достоинствах применения и многом другом. Также ознакомитесь с основными характеристиками, особенностями, которые помогут правильно и быстро подобрать конструкции. Рассматриваются и виды поршневых компрессоров, даются ценные рекомендации по их выбору. Всю нужную и ценную информацию вы обязательно узнаете на этом портале. Она составлена лучшими экспертами.
Добрый день!
Как приобрести аттестат о среднем образовании в Москве и других городах
antiugon.center/index.php?subaction=userinfo&user=ymuluzi
Всегда вам поможем!.
Каталог вакансий – Ваш надежный источник по поиску работы
Найдите свою идеальную работу с Категорией вакансий! Мы предлагаем обширную базу данных вакансий из различных отраслей и регионов.
работа курьером с частичной занятостью
С нами вы сможете:
Просматривать актуальные объявления о вакансиях.
Фильтровать результаты по местоположению, отрасли и ключевым словам.
Создать персонализированные оповещения, чтобы быть в курсе новых возможностей.
Сохранять и сравнивать вакансии для удобства
работа кладовщиком в Санкт-Петербурге
Загружать резюме одним щелчком мыши, чтобы подать заявку на интересующие вакансии.
Добрый день!
Где купить диплом по актуальной специальности?
hackmd.io/@KevinWallace/SyaseLwBR
йЂІдѕ†
Glory Casino
Приобрести диплом о высшем образовании.
uscgq.com/forum/posts.php?forum=general&id=258539
tyachiv.ukraine7.com/login
leydis16.phorum.pl/posting.php?mode=newtopic&f=1
mestovstrechi.flybb.ru/viewtopic.php?f=4&t=1274
nnars.ru/forum/suggestion-box/1210-официальные-дипломы-качество-и-легальность#74596
Рекомендации по безопасной покупке диплома о высшем образовании
ast-diplom24.ru/kupit-diplom-voronezh
Наша мастерская предлагает профессиональный сервисный центр по ремонту квадрокоптеров различных марок и моделей. Мы осознаем, насколько необходимы вам ваши духовые шкафы, и обеспечиваем ремонт наилучшего качества. Наши квалифицированные специалисты работают быстро и аккуратно, используя только сертифицированные компоненты, что гарантирует надежность и долговечность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются пользователи духовок, включают неработающие нагревательные элементы, поломку таймера, поврежденную дверцу, сбои контроллера, неисправности вентилятора и неработающие датчики. Для устранения этих неисправностей наши квалифицированные специалисты выполняют ремонт нагревательных элементов, термостатов, таймеров, дверец, контроллеров, вентиляторов и электроники. Доверив ремонт нам, вы обеспечиваете себе долговечный и надежный сервисный центр по ремонту дронов адреса.
Подробная информация представлена на нашем сайте: https://remont-kvadrokopterov-best.ru
Здравствуйте!
Мы готовы предложить документы ВУЗов
medvozerniy.flybb.ru/viewtopic.php?f=14&t=13447
forum.kam.su/member.php?u=5734
rkiyosaki.ru/discussion/9803/nadezhnoe-oformlenie-diplomov/
kai87la.flybb.ru/viewtopic.php?f=5&t=431
forum.qwas.ru/vash-diplom-kluch-k-uspehu-t20261.html
Здравствуйте!
Приобрести диплом университета.
thenet.work/gallery/image/475-огромный-каталог-документов-в-известном-интернет-магазине/
Привет, друзья!
Приобрести документ ВУЗа.
rakisochi.ru/users/20
snaprama.com/read-blog/1033
fiat-club.ru/search.php?cx=partner-pub-2897956929599751:bz9j42-t4gv&cof=FORID:10&ie=UTF-8&q=&sa=Поиск&siteurl=forum.fiat-club.ru/blog_post.php?do=newblog&ref=forum.fiat-club.ru/login.php?do=login&ss=
suhinfo.ru/index.php/Диплом_для_успешной_карьеры:_качественно_и_безопасно
wiki.hightgames.ru/index.php/Быстрая_покупка_дипломов_онлайн
Здравствуйте!
Заказать диплом любого ВУЗа:
test.krestikom.net/forums/topic/941-купить-диплом-техникума-q962u/
“o98065hq.bget.ru/index.php?action=profile;u=395227”
mtpkrskstate.ru/forum/user/199859/
forumfajerwerki.pl/topic/16855-pyromagic-2018-11-miedzynarodowy-festiwal-sztucznych-ogni/
whdf.ru/forum/user/80310/
Добрый день!
Заказать документ института вы можете у нас.
ast-diploms24.ru/kupit-diplom-sankt-peterburg
Удачи!
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным ценам.
foodxtech.mn.co/posts/61838161
sonnick84.bloguetechno.com/Быстро-заказываем-аттестат-в-интернет-магазине-russian-diplom-63743859
sonnick84.diowebhost.com/83430024/Ценообразование-дипломов-обзор-экспертов
xleks.ru/2024/07/09/nizkie-rascenki-i-prekrasnoe-kachestvo-zakazyvay-diplomy-onlayn.html
indungii.ro/forum/index.php?/gallery/image/4-для-чего-сегодня-приобретают-дипломы-в-сети/
Привет!
Мы изготавливаем дипломы.
jogibaba.com/blogs/222/Купить-диплом-быстро-и-надежно
wiki.intradition.ru/index.php/Настоящие_Дипломы:_Легально_и_Конфиденциально
goruss.ru/blogs/999/Быстрое-Оформление-Дипломов-Надежно-и-Легально
forummichiganrp.moibb.ru/viewtopic.php?f=21&t=433
elitemagyaritasok.info/e107_plugins/forum/forum_post.php?f=nt&id=21#
Добрый день!
Мы готовы предложить документы техникумов
myweektour.ru/vyisokokachestvennyie-diplomyi-po-luchshim-tsenam/
l4dzone.com/viewtopic.php?t=242266
gladpwnz.ru/forum/member.php?u=221749
sensualmarketplace.com/create-blog/
wiki.3cdr.ru/wiki/index.php/Быстрое_оформление_дипломов_для_всех
еєЉ
Здравствуйте!
Купить документ ВУЗа можно у нас в столице.
ast-diploms24.ru/kupit-diplom-krasnoyarsk
Хорошей учебы!
Привет, друзья!
Как официально купить диплом вуза с упрощенным обучением в Москве
laporteproperty.com/en/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=124
additional info short squeeze hamster kombat
Привет, друзья!
Заказать документ университета.
telegra.ph/Vash-diplom-bez-hlopot-bystro-i-nadezhno-07-15
netcallvoip.com/wiki/index.php/Экспресс-доставка_дипломов_по_всем_специальностям
lightsdemons.phorum.pl/viewtopic.php?p=67699#67699
les-ailes-chalaisiennes.com/forum/topic/осуществите-мечту-получите-диплом-бы/#postid-19516
avrorp.getbb.ru/viewtopic.php?f=183&t=705
3D-принтери фотополимерные – Мийки для 3D принтерів, PLA плюс
Здравствуйте!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
kerchlibrary.ru/index.php?subaction=userinfo&user=ykada
Всегда вам поможем!.
з›ёдјјзљ„
[u][b] Привет, друзья![/b][/u]
[b]Мы можем предложить дипломы[/b] любой профессии по выгодным ценам.
[url=http://onlinekinospace.ru/kupite-diplom-dlya-vashego-budushhego/]onlinekinospace.ru/kupite-diplom-dlya-vashego-budushhego[/url]
иЁ±д№…
Добрый день!
Купить документ университета можно в нашей компании в Москве.
asxdiplomik24.ru/kupit-diplom-moskva
Успешной учебы!
Привет, друзья!
Заказать диплом о высшем образовании.
logan.in.ua/people/user/7276/blog/7929/
Заказать диплом ВУЗа.
kome.maxbb.ru/viewtopic.php?f=22&t=2205
ic-info.ru/forum/user/166216/
pokemon-go.onl/users/6146
tawasol1.mn.co/posts/61900062
keterclub.com/read-blog/9135
Покупка диплома о среднем полном образовании: как избежать мошенничества?
diploms-x.com/kupit-diplom-ekaterinbur
ж•…дє‹
Добрый день!
Можно ли купить аттестат о среднем образовании, основные моменты и вопросы
gemawiraclub.com/blogs/39878/Как-можно-будет-купить-недорого-качественный-диплом-в-сети
Наш сервисный центр предлагает профессиональный мастерская по ремонту макбука рядом любых брендов и моделей. Мы понимаем, насколько необходимы вам ваши ноутбуки Apple, и стремимся предоставить услуги первоклассного уровня. Наши опытные мастера оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что предоставляет длительную работу проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются пользователи ноутбуков Apple, включают поврежденный экран, поломку батареи, ошибки ПО, неработающие разъемы и проблемы с охлаждением. Для устранения этих поломок наши квалифицированные специалисты проводят ремонт экранов, батарей, ПО, разъемов и систем охлаждения. Доверив ремонт нам, вы обеспечиваете себе надежный и долговечный вызвать мастера по ремонту макбука адреса.
Подробная информация доступна на сайте: https://remont-macbook-club.ru
Добрый день!
Приобрести диплом ВУЗа.
halopro.net/gallery/image/486-как-найти-надежный-онлайн-магазин-с-широким-каталогом-дипломов/
Здравствуйте!
Мы изготавливаем дипломы.
nedvigimost.bbok.ru/viewtopic.php?id=27313#p46747
prest.by/forum/user/3033/
bintarotrojan.com/blogs/9424/Ваш-Настоящий-Диплом-Легко-и-Безопасно
krasnodarforum.ru/member.php?u=2812
toursoul.ru/?p=19202
Добрый день!
Заказать документ о получении высшего образования
sonnick84.blog5.net/70018038/Что-готов-сегодня-предложить-интернет-магазин-с-документами
buzzakoo.com/blogs/767/Дипломы-по-низким-ценам-в-популярном-интернет-магазине
socialhustle.co.uk/read-blog/2267
c904581v.beget.tech/2024/07/04/pochemu-gorazdo-prosche-budet-priobresti-diplom-universiteta.html
site2.liodiz.ru/2024/07/04/zachem-v-nashe-vremya-zakazyvayut-diplomy-i-attestaty-v-internete.html
最好的
Обеспечьте конфиденциальность с резидентскими прокси, рекомендуем этим инструментом.
Как работают резидентские прокси?, прочитайте подробностями.
Какой резидентский прокси выбрать?, инструкция для пользователей.
Какие задачи решают резидентские прокси?, подробнее ознакомьтесь с возможностями.
В чем преимущество безопасности резидентских прокси?, обзор функций безопасности.
Как резидентские прокси защищают от опасностей?, разберем важные аспекты.
Как резидентский прокси помогает повысить эффективность?, сравним основные плюсы.
Секреты увеличения скорости с резидентским прокси, рекомендации для оптимизации работы.
Каким образом ускорить процесс парсинга с помощью резидентского прокси, разбор возможностей для парсеров.
Секреты анонимности с резидентским прокси, практические шаги к безопасности онлайн.
Секреты эффективной работы в соцсетях с резидентским прокси, практические советы функционала.
Какие преимущества дает аренда резидентских прокси, сравним лучшие варианты.
Как избежать DDoS с резидентским прокси?, рассмотрим меры безопасности.
В чем причина популярности резидентских прокси?, проанализируем основные факторы.
Сравнение резидентских и дата-центровых прокси, подсказки для выбора.
индивидуальные резидентские прокси https://rezidentnieproksi.ru/ .
Здравствуйте!
Мы можем предложить дипломы любой профессии по выгодным тарифам.
sonnick84.anchor-blog.com/8526131/Главные-затраты-любого-изготовителя-документов-обзор
sonnick84.blogzag.com/72702803/Цена-диплома-обзор-специалистов
goruss.ru/blogs/1000/Заказываем-документы-в-известном-онлайн-магазине-по-комфортной-цене
oolibuzz.com/read-blog/3117
onetable.world/read-blog/59748
Привет!
Приобрести диплом университета.
sonnick84.angelinsblog.com/27873555/%D0%A0%D0%B5%D0%BA%D0%BE%D0%BC%D0%B5%D0%BD%D0%B4%D0%B0%D1%86%D0%B8%D0%B8-%D1%8D%D0%BA%D1%81%D0%BF%D0%B5%D1%80%D1%82%D0%B0-%D1%87%D1%82%D0%BE-%D0%BF%D0%BE%D0%BC%D0%BE%D0%B3%D1%83%D1%82-%D0%B1%D1%8B%D1%81%D1%82%D1%80%D0%BE-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC
Здравствуйте!
Возможно ли купить диплом стоматолога, и как это происходит
phongthuygiaphat.com/купить-заполненный-диплом/
Привет, друзья!
Заказать документ о получении высшего образования
freeline.mn.co/posts/61838355
sonnick84.blogoxo.com/28325123/Дипломы-по-выгодным-ценам-в-известном-магазине
woowsent.com/read-blog/60
ai.ceo/read-blog/147756
mooz6.com/read-blog/595
Добрый день!
Заказать документ о получении высшего образования
ast-diplom24.ru/kupit-diplom-sankt-peterburg
History and Development
ivermectin buy
妈妈
Добрый день!
Всё, что нужно знать о покупке аттестата о среднем образовании
landik-diploms-srednee.ru/svidetelstvo-o-razvode В
йЂ™
Привет!
Купить документ института
sonnick84.weblogco.com/28248426/Надежный-и-проверенный-онлайн-магазин-с-большим-каталогом-документов
roving.club/read-blog/947
sonnick84.ka-blogs.com/81580601/Что-именно-необходимо-из-оборудования-для-изготовления-документов
s24.team/club/user/148/blog/1609/
poetzinc.com/read-blog/11624
ењ°ж–№
Привет!
Приобрести диплом университета.
medik-look.ru/diplomyi-vyisshego-obrazovaniya-s-garantiey
Хорошей учебы!
Здравствуйте!
Приобрести документ института.
shoptema.ru/forum/talk/add/
backshowtime.ru/diplom-lyuboy-spetsialnosti-kachestvenno-i-bezopasno
forum.gorodsalavat.ru/posting.php?mode=post&f=28&sid=38420d04527046406718146c1615912a
desteg.getbb.ru/viewtopic.php?f=6&t=836
minimoo.eu/index.php/en/forum/welcome-mat/666892
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по приятным ценам.
http://www.ledshtech.com/купить-диплом-молдавии/
Добрый день!
Купить диплом о высшем образовании
Наши специалисты предлагают выгодно купить диплом, который выполнен на оригинальной бумаге и заверен мокрыми печатями, водяными знаками, подписями должностных лиц. Наш диплом пройдет любые проверки, даже с использованием профессионального оборудования. Достигайте своих целей быстро с нашей компанией.
Где купить диплом по актуальной специальности?
rsn360.ru/blogs/509/Официальные-дипломы-по-доступной-цене
nc750.ru/member.php?u=2812
mediamemorial.ru/club/user/125807/forum/message/3793/13275/#message13275
wegug.in/blogs/942/Купить-Официальный-Диплом-Быстро-и-Легально
ringturbine.com/index.php/За_счет_чего_магазины_с_документами_столь_популярны?
Привет!
Заказать документ института вы сможете у нас. Мы оказываем услуги по продаже документов об окончании любых университетов России. Вы получите необходимый диплом по любым специальностям, любого года выпуска, включая документы Советского Союза. Даем 100% гарантию, что при проверке документа работодателем, никаких подозрений не появится.
odessaforum.getbb.ru/viewtopic.php?f=5&t=20726
wiki.mdomtv.net/index.php?title=Ваш_идеальный_диплом:_быстро_и_легко
eworkface.com/blogs/436/Решили-выяснить-как-заказать-диплом-в-сети-недорого-Заходите
http://www.wesco.dev/wall/blogs/199/Изучите-наш-материал-в-случае-если-нужно-купить-диплом-в
livestockkenya.com/index.php/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=250
е‚ійЂЃ
Наши специалисты предлагает надежный сервисный ремонт майнера в москве различных марок и моделей. Мы осознаем, насколько необходимы вам ваши майнеры, и готовы предложить сервис наилучшего качества. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что обеспечивает надежность и долговечность проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются обладатели криптомайнеров, включают перегрев, неисправности питания, ошибки ПО, неработающие разъемы и неисправности оборудования. Для устранения этих проблем наши квалифицированные специалисты оказывают ремонт систем охлаждения, блоков питания, ПО, разъемов и оборудования. Обращаясь в наш сервисный центр, вы получаете надежный и долговечный сервисный центр по ремонту майнера рядом.
Подробная информация доступна на сайте: https://remont-maynerov-geek.ru
africanownews.com
Добрый день!
Мы можем предложить дипломы любой профессии по приятным ценам.
beinsadouno.bg/events/event/43-какие-интернет-магазины-с-дипломами-имеются-на-сегодняшний-момент/
Привет!
Мы можем предложить документы техникумов
reflections.listbb.ru/viewtopic.php?f=45&t=766
thesleepinghusband.rolka.me/viewtopic.php?id=22128#p53966
wiki.mdomtv.net/index.php?title=Быстрое_получение_дипломов_всех_специальностей
vip.rolevaya.info/viewtopic.php?id=5049#p8669
feolet.flybb.ru/viewtopic.php?f=2&t=654&sid=25edcad4d849670b33149d4c55ccea6c
birminghamnews24.com
Привет!
Заказать документ института
asxdiplomik.com/kupit-diplom-ekaterinbur
動物
жЉ“дЅЏ
Добрый день!
Приобрести диплом ВУЗа.
etulpan.topf.ru/viewtopic.php?id=756#p1262
Успешной учебы!
Здравствуйте!
Заказать диплом любого ВУЗа.
9213270296.ru/2024/07/04/kak-podobrat-nadezhnyy-internet-magazin-s-bolshim-vyborom-diplomov.html
Добрый день!
Заказать документ о получении высшего образования.
anoreksja.org.pl/viewtopic.php?f=13&t=1247405
mangorpp.getbb.ru/viewtopic.php?f=3&t=460
funnywipes.maxbb.ru/viewtopic.php?f=3&t=662
mockwacom.getbb.ru/posting.php?mode=post&f=12
foousrp.listbb.ru/viewtopic.php?f=4&t=531
Добрый день!
Мы готовы предложить документы техникумов
revolverp.forumex.ru/viewtopic.php?f=11&t=322
k90280ul.beget.tech/2024/07/18/oformlenie-diplomov-vseh-urovney.html
formulaf1.ru/vash-diplom-vashe-budushhee
shuvalduet.getbb.ru/viewtopic.php?f=3&t=616
sec31.ru/viewtopic.php?f=25&t=678141
Привет, друзья!
Как приобрести диплом техникума с минимальными рисками
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske В
Добрый день!
Заказать документ ВУЗа
victorians123.com/blogs/202/Знаменитый-интернет-магазин-с-очень-выгодными-по-цене-дипломами
sonnick84.digiblogbox.com/53716546/Советы-профессионала-что-позволят-легко-заказать-диплом
cittaviva.net/read-blog/51
sonnick84.bloggin-ads.com/51639468/Дипломы-по-низким-расценкам-в-известном-онлайн-магазине
sonnick84.bloginder.com/28814719/Как-возможно-приобрести-недорого-качественный-диплом-в-интернете
Добрый день!
Заказать документ ВУЗа вы можете в нашем сервисе.
ast-diploms.com/kupit-diplom-o-srednem-obrazovanii
Удачи!
иѓЅ
Здравствуйте!
Купить диплом ВУЗа.
tosiya.ru/cb-profile/pluginclass/cbblogs.html?action=blogs&func=show&id=298
Здравствуйте!
Купить документ о получении высшего образования.
wecanchat.mn.co/posts/62242116
together-19.com/read-blog/29890
sz.80lvl.ru/viewtopic.php?f=9&t=1936
avva.getbb.ru/viewtopic.php?f=3&t=583
izumrudnoeozero.listbb.ru/viewtopic.php?f=8&t=543
Добрый день!
Мы предлагаем документы техникумов
bvf.ru/forum/showthread.php?p=25250238#post25250238
onlinekinofun.ru/oformite-diplom-bez-ozhidaniya
igrosoft.getbb.ru/posting.php?mode=post&f=11&sid=487e5c60eadc02708610e75ec390feba
yur-dom.ru/communication/forum/messages/forum3/message291/334-kupit-diplom-o-vysshem-obrazovanii?result=new#message291
t98223u0.beget.tech/2024/07/18/kupite-diplom-i-nachnite-novuyu-zhizn.html
Добрый день!
Купить документ о получении высшего образования можно в нашей компании.
asxdiplomik24.ru/kupit-diplom-moskva
Успешной учебы!
Playing the Aviator Game online offers several benefits:
buy ivermectin
News Sites for Article post
frenchnewstoday.com
germaynewstoday.com
guardiannewstoday.com
headlinesworldnews.com
huffingtonposttoday.com
irishnewstoday.com
Dont hasitate to contact us
Добрый день!
Заказать документ института можно у нас в столице.
diploms-x24.ru/kupit-diplom-moskva
Успешной учебы!
移動
Здравствуйте!
Купить диплом о высшем образовании.
vxengine.ru/blogs/532/Большой-ассортимент-документов-в-известном-онлайн-магазине
Добрый день!
Приобрести документ о получении высшего образования.
telugusaahityam.com/Легальный_диплом_без_лишних_хлопот:_узнайте_как!
school8kaluga.flybb.ru/viewtopic.php?f=19&t=501
repetitor.ekafe.ru/faq.php
newsbeautiful.ru/poluchite-diplom-v-kratchayshie-sroki/
ya.9bb.ru/viewtopic.php?id=5934#p11431
Привет, друзья!
Купить документ университета
asxdiplomik24.ru/kupit-diplom-moskva
[u][b] Добрый день![/b][/u]
Диплом юриста
[url=http://dexanet.ukrbb.net/viewtopic.php?f=5&t=16474/]dexanet.ukrbb.net/viewtopic.php?f=5&t=16474[/url]
[url=http://kvitka.ukrbb.net/viewtopic.php?f=58&t=23712/]kvitka.ukrbb.net/viewtopic.php?f=58&t=23712[/url]
[url=http://eurodelo.ru/obrazovanie-vashey-mechtyi-diplomyi-izvestnyih-universitetov/]eurodelo.ru/obrazovanie-vashey-mechtyi-diplomyi-izvestnyih-universitetov[/url]
[url=http://cod4.flybb.ru/viewtopic.php?f=60&t=674/]cod4.flybb.ru/viewtopic.php?f=60&t=674[/url]
[url=http://medrese1000-letie.ru/auth/?register=yes/]medrese1000-letie.ru/auth/?register=yes[/url]
оборудование для конференций купить http://www.oborudovanie-dlja-konferenc-zalov.ru .
Привет, друзья!
Официальное получение диплома техникума с упрощенным обучением в Москве
landik-diploms-srednee.ru/kupit-diplom-v-kazani В
Привет, друзья!
Приобрести диплом ВУЗа.
truongvietducthainguyen.edu.vn/index.php?language=vi&nv=statistics&nvvithemever=t&nv_redirect=aHR0cHM6Ly9hZGlzZ3J1bnRsZWRyZXB1YmxpY2FuLmNvbQ
Успешной учебы!
й«зљ„
Наш сервисный центр предлагает высококачественный сервис ремонта массажного кресла на дому различных марок и моделей. Мы осознаем, насколько необходимы вам ваши массажные кресла, и обеспечиваем ремонт высочайшего уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только качественные детали, что обеспечивает долговечность и надежность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются владельцы массажных кресел, включают неисправности двигателя, неработающие ролики, ошибки ПО, неисправности разъемов и поломки компонентов. Для устранения этих неисправностей наши профессиональные техники оказывают ремонт моторов, роликов, ПО, разъемов и механических компонентов. Обратившись к нам, вы обеспечиваете себе надежный и долговечный сервис ремонта массажного кресла.
Подробная информация размещена на сайте: https://remont-massazhnyh-kresel-gold.ru
е–ќ
Привет, друзья!
Купить документ ВУЗа вы имеете возможность в нашей компании в Москве.
asxdiplomik.com/kupit-diplom-s-registraciej
Привет!
Приобрести диплом любого ВУЗа.
codinganme.com/gallery/image/115-дипломы-по-выгодным-ценам-в-популярном-интернет-магазине/?context=new
plplatoon.com/gallery/image/116-зачем-сегодня-приобретают-аттестаты-и-дипломы-в-сети-интернет/
iwasocial.com/read-blog/254
leed.lol/read-blog/413
chat-hozn3.com/blogs/13306/Как-возможно-будет-быстро-заказать-диплом-в-онлайн-магазине
жЋйЎЇењ°
Sur notre site web, vous pouvez lire toutes les actualites concernant les medias en Afrique. Nous couvrons une variete de sujets, allant des dernieres nouvelles dans les secteurs de la television, de la radio et de la presse ecrite, aux developpements dans les medias numeriques et les reseaux sociaux https://histoires-africaines.africa/rachel-ratsizafy/. Notre equipe de journalistes experimentes et de correspondants locaux travaille sans relache pour vous apporter des actualites precises et a jour.
Nous donnons une attention particuliere aux progres et aux tendances qui changent le paysage mediatique africain. Que ce soit la montee des plateformes de streaming, la presence croissante des blogs et des podcasts, ou les consequences des politiques gouvernementales sur la liberte de la presse, vous trouverez des analyses approfondies et des reportages exclusifs sur notre site. Nous faisons egalement en lumiere les initiatives locales et les talents emergents qui aident a structurer l’avenir des medias sur le continent.
En plus des actualites, notre site offre des interviews avec des personnalites influentes du secteur des medias et des experts, ainsi que des articles d’opinion composes par des specialistes. Nous encourageons nos lecteurs a prendre part activement en publiant des commentaires et en echangeant leurs points de vue. Venez nous voir des aujourd’hui pour demeurer informe et engage avec les evolutions passionnantes du monde des medias en Afrique.
Привет, друзья!
Заказать документ института вы имеете возможность в нашей компании в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ.
romb4x4.ru/forum/threads/kupit-diplom-cena-w690d.3056/
193.16.101.6/index.php?title=gosznacdiplomy
барс48.рф/forums.php?m=posts&q=22239&n=last#bottom
biowiki.clinomics.com/index.php?title=gosznacdiplomy
http://www.pirobot.co.uk/doku.php?id=diploman
Привет!
Приобрести документ о получении высшего образования вы можете в нашей компании в Москве.
ast-diploms.com/kupit-diplom-o-vysshem-obrazovanii
Привет, друзья!
Мы готовы предложить дипломы любых профессий по разумным ценам.
comedyforme.ru/vash-diplom-garantiya-kachestva-i-nadezhnosti
Привет, друзья!
Мы можем предложить документы ВУЗов
local-urban-eats.mn.co/posts/62669843
artem-energo.ru/message.php?msg=151
vseogirls.ru/byistroe-poluchenie-diploma-onlayn
kawaa.drake.free.fr/index.php?file=Forum&page=viewtopic&forum_id=1&thread_id=5596
silich.ru/forum/member.php?u=4810
Добрый день!
Быстрая схема покупки диплома старого образца: что важно знать?
aromatov.wooden-rock.ru/forum/topic.php?forum=1&topic=15825&v=l#1719302971
Окажем помощь!.
з¤ѕжњѓ
Bonus bez depozytu lub innymi slowami darmowy bonus to nic innego jak gratis oferowany przez kasyna online dla swoich graczy hitnspin kasyno
Привет, друзья!
Заказать документ ВУЗа вы имеете возможность в нашей компании в столице.
diplomyx24.ru/kupit-diplom-rostov-na-donu
Удачи!
Добрый день!
Купить документ университета можно у нас.
diplomasx.com/kupit-diplom-novosibirsk
Добрый день!
Купить документ о получении высшего образования
sslaziofansclub.com/read-blog/3270
inopl.com/blogs/1131/Какие-магазины-с-документами-на-сегодняшний-момент-имеются
watucowalu.cavandoragh.org/cto-trebuetsa-dla-proizvodstva-kacestvennogo-diploma-universiteta
i2od836bz.blog5star.com/28636031/Как-возможно-недорого-заказать-диплом-в-интернет-магазине
sonnick84.topbloghub.com/34428015/Дипломы-справки-и-сертификаты-низкие-цены
Здравствуйте!
Диплом магистра
dvasadovoda.ru/forum/user/8893/
antonovschool.ru/forum/messages/forum1/topic721/message740/?result=new#message740
shkola6309.ru/forums/forum/vneurochnaya-deyatelnost/
vodozone.ru/forum/user/55331/
video.listbb.ru/viewtopic.php?f=3&t=421
Здравствуйте!
Приобрести диплом о высшем образовании
zavalinka.listbb.ru/viewtopic.php?f=3&t=2981
crystalroleplay.listbb.ru/ucp.php?mode=login&sid=3c61f937a4d37db56d0de8bc2317429a
medik-look.ru/kachestvennyie-diplomyi-bez-posrednikov
bintarotrojan.com/blogs/11480/Быстрый-путь-к-высшему-образованию-и-новым-возможностям
kostromag.ru/forum/science/9047.aspx
белый список капперов телеграмм https://www.rejting-kapperov12.ru .
Привет, друзья!
Купить диплом любого ВУЗа
Мы предлагаем выгодно приобрести диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями официальных лиц. Наш документ пройдет любые проверки, даже с применением специальных приборов. Решайте свои задачи быстро и просто с нашей компанией.
Где купить диплом по необходимой специальности?
c90226sl.beget.tech/2024/07/07/kupit-diplom-v-moskve-legko-i-bezopasno/
pokemon-go.onl/users/6146
http://www.faceonblock.com/blogs/3553/Что-понадобится-для-производства-качественного-диплома
medik-look.ru/vash-put-k-vyisshemu-obrazovaniyu-byistro-i-legalno
kids-news.ru/vyisshee-obrazovanie-dlya-vseh-kupit-diplom
дё»и¦Ѓзљ„
Привет, друзья!
Купить диплом о высшем образовании
Наша компания предлагает быстро купить диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, штампами, подписями должностных лиц. Наш диплом пройдет лубую проверку, даже с применением специально предназначенного оборудования. Достигайте свои цели быстро и просто с нашей компанией.
Где купить диплом по нужной специальности?
driveme.rusff.me/viewtopic.php?id=2115#p105171
rossensor.ru/forum/?PAGE_NAME=message&FID=1&TID=16423&TITLE_SEO=16423-kupit-diplom&MID=857203&result=new#message857203
astrcolcult.ru/?post_type=topic&p=34434
kurgetrp.listbb.ru/viewtopic.php?f=11&t=380
http://www.hristianka.ru/forum/r/prev_loaded/1/
[u][b] Здравствуйте![/b][/u]
[b]Мы изготавливаем дипломы[/b] психологов, юристов, экономистов и любых других профессий по приятным тарифам.
[url=http://thenet.work/gallery/image/478-какие-интернет-магазины-с-документами-на-текущий-день-есть//]thenet.work/gallery/image/478-какие-интернет-магазины-с-документами-на-текущий-день-есть/[/url]
[u][b] Привет![/b][/u]
Купить документ о получении высшего образования можно в нашей компании в столице. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любой специальности, любого года выпуска, в том числе документы старого образца. Гарантируем, что в случае проверки документа работодателем, никаких подозрений не возникнет.
[url=http://forum.vipcs.pp.ua/gallery/image/315-4-е-основных-группы-онлайн-магазинов-которые-реализуют-дипломы//]forum.vipcs.pp.ua/gallery/image/315-4-е-основных-группы-онлайн-магазинов-которые-реализуют-дипломы/[/url]
[url=http://www.pets-ural.ru/content/forum/viewtopic.php?p=76585#76585/]www.pets-ural.ru/content/forum/viewtopic.php?p=76585#76585[/url]
[url=http://club.sabaylok.com/blogs/4980/Купить-диплом-быстро-и-надежно/]club.sabaylok.com/blogs/4980/Купить-диплом-быстро-и-надежно[/url]
[url=http://vipka.0bb.ru/viewtopic.php?id=5807#p8726/]vipka.0bb.ru/viewtopic.php?id=5807#p8726[/url]
[url=http://avva.getbb.ru/viewtopic.php?f=3&t=571/]avva.getbb.ru/viewtopic.php?f=3&t=571[/url]
Common feedback from players includes requests for more in-game bonuses, additional multiplayer options, and
where to buy ivermectin
Привет, друзья!
Приобрести документ о получении высшего образования
rf-4fun.ru/index.php?/gallery/image/119-почему-намного-дешевле-будет-приобрести-диплом-вуза/
crowd-out.social/read-blog/133
socialle.com.br/blogs/253/%D0%96%D0%B5%D0%BB%D0%B0%D0%B5%D1%82%D0%B5-%D0%BF%D1%80%D0%B8%D0%BE%D0%B1%D1%80%D0%B5%D1%81%D1%82%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D1%83-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D0%BE%D0%B3%D0%BE-%D0%B8%D1%81%D0%BF%D0%BE%D0%BB%D0%BD%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%96%D0%B4%D0%B5%D0%BC-%D0%92%D0%B0%D1%81
sonnick84.wizzardsblog.com/28243455/Знаменитый-магазин-с-очень-выгодными-по-цене-документами
sonnick84.activoblog.com/28433878/Что-может-в-наше-время-предложить-онлайн-магазин-с-документами
[u][b] Добрый день![/b][/u]
[b]Мы готовы предложить дипломы[/b] любой профессии по выгодным ценам.
[url=http://gta-balkan.com/events/event/42-четыре-главных-группы-онлайн-магазинов-что-продают-документы//]gta-balkan.com/events/event/42-четыре-главных-группы-онлайн-магазинов-что-продают-документы/[/url]
Привет, друзья!
Приобрести документ института можно в нашей компании в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любой специальности, включая документы СССР. Даем гарантию, что в случае проверки документов работодателями, каких-либо подозрений не появится.
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по доступным ценам. Цена зависит от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступны для большого количества граждан.
toplentanews.ru/kupit-diplom-vash-klyuch-k-novyim-vozmozhnostyam-i-perspektivam
Всегда вам поможем!
ועוד. נערות ליווי בתל אביב עד הבית יושב לבד בבית ומרגיש משועמם? לא צריך לחפש בילויים כאשר הבילויים יכולים להגיע עד אלייך. אתה לא יודע על מה אנחנו מדברים – כדאי שתבוא לראות מה זה דירות דיסקרטיות בבאר שבע. זהו המקום החם ביותר בעיר. המקום שבו מבלים דירות דיסקרטיות במרכז
Наши специалисты предлагает профессиональный отремонтировать материнская плата в москве любых брендов и моделей. Мы осознаем, насколько важны для вас ваши материнские платы для ПК, и стремимся предоставить услуги наилучшего качества. Наши опытные мастера работают быстро и аккуратно, используя только сертифицированные компоненты, что предоставляет долговечность и надежность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются обладатели мэйнбордов, включают проблемы с чипсетом, неработающий блок питания, программные сбои, проблемы с портами и аппаратные сбои. Для устранения этих поломок наши опытные мастера оказывают ремонт чипсетов, блоков питания, ПО, разъемов и компонентов. Обращаясь в наш сервисный центр, вы получаете надежный и долговечный мастер по ремонту материнских плат.
Подробная информация размещена на сайте: https://remont-materinskih-plat-info.ru
Привет!
Купить документ о получении высшего образования вы можете в нашей компании. Мы оказываем услуги по продаже документов об окончании любых университетов России.
pedolog-pro.ru/forums/topic/купить-диплом-c303p/
dvnshu.com/index.php?subaction=userinfo&user=ogusyp
whirlpowertool.ru/index.php?subaction=userinfo&user=ibibiqib
belobog1.freehostia.com/phpBB2/profile.php?mode=viewprofile&u=178931
magadan-mebel.ru/forum/user/946/
Ищите скачать фильмы на телефон https://anwap.im/ – тогда зайдите к нам. Скачивайте фильмы, сериалы, мультики прямо на телефон и смотрите, когда вам удобно. Никакой регистрации, бесплатно. Коллекции нашего сайта в любых жанрах и годов выпуска позавидует любой сайт. Все фильмы для телефона в одном месте.
[u][b] Здравствуйте![/b][/u]
[b]Мы можем предложить дипломы[/b] любой профессии по приятным ценам.
[url=http://houseofnails.store/2024/06/30/диплом-самара-купить//]houseofnails.store/2024/06/30/диплом-самара-купить/[/url]
What a information of un-ambiguity and preserveness of valuable experience on the topic of unexpected emotions.
https://tunein.com/podcasts/Arts–Culture-Podcasts/COPE—Der-Empowerment-Podcast-p2348890/
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
last info about becker
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
Привет!
Заказать диплом о высшем образовании
Наша компания предлагает выгодно купить диплом, который выполняется на оригинальной бумаге и заверен печатями, штампами, подписями должностных лиц. Диплом способен пройти любые проверки, даже с использованием специфических приборов. Достигайте свои цели быстро и просто с нашими дипломами.
Где купить диплом по необходимой специальности?
politictoday.ru/ofitsialnyie-diplomyi-garantiya-podlinnosti-i-kachestva
lada-clubs.ru/gallery/image/738-assortiment-i-sposoby-dostavki-v-magazine-pokupaem-diplom/
bl.com.tw/index.php?title=Официальные_Дипломы:_Доступно_и_Безопасно
larashare.net/events/event/47-быстрый-поиск-интернет-магазина-что-продает-дипломы-и-аттестаты/
californiarpn2.listbb.ru/viewtopic.php?f=1&t=505
[u][b] Здравствуйте![/b][/u]
Диплом для вас
[url=http://newrealgames.ru/vash-diplom-vash-klyuch-k-uspehu/]newrealgames.ru/vash-diplom-vash-klyuch-k-uspehu[/url]
[url=http://csexpert.4adm.ru/viewtopic.php?f=70&t=2083/]csexpert.4adm.ru/viewtopic.php?f=70&t=2083[/url]
[url=http://nedvigimost.bbok.ru/viewtopic.php?id=27609#p47216/]nedvigimost.bbok.ru/viewtopic.php?id=27609#p47216[/url]
[url=http://forum.kam.su/member.php?u=5734/]forum.kam.su/member.php?u=5734[/url]
[url=http://politictoday.ru/diplomyi-o-vyisshem-obrazovanii-otkroyte-dveri-k-uspehu/]politictoday.ru/diplomyi-o-vyisshem-obrazovanii-otkroyte-dveri-k-uspehu[/url]
Привет!
Приобрести диплом о высшем образовании.
tras.ru/cb-profile/pluginclass/cbblogs.html?action=blogs&func=show&id=118
weblink https://hamsterkombat.zone
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании в столице. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов Российской Федерации. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы образца СССР. Гарантируем, что в случае проверки документа работодателями, никаких подозрений не появится.
socialnetwork.swazi-host.com/blogs/15612/Что-потребуется-из-оборудования-для-создания-диплома
komfort.rusff.me/viewtopic.php?id=13894#p40941
wegug.in/blogs/984/Быстрое-Оформление-Дипломов-Надежно-и-Легально
dragonlivers.ixbb.ru/viewtopic.php?id=106#p106
wayworld.listbb.ru/viewtopic.php?f=2&t=24662
Привет, друзья!
Мы готовы предложить дипломы любых профессий по разумным тарифам. Цена будет зависеть от выбранной специальности, года выпуска и ВУЗа. Стараемся поддерживать для покупателей адекватную политику цен. Важно, чтобы документы были доступны для большого количества граждан.
charlieuy345.yomoblog.com/33241545/Фальшивый-диплом-Почему-это-не-Стоит-купить-диплом
[u][b] Здравствуйте![/b][/u]
Заказать документ о получении высшего образования.
[url=http://kvitka.ukrbb.net/posting.php?mode=post&f=58/]kvitka.ukrbb.net/posting.php?mode=post&f=58[/url]
[url=http://skazka.g-talk.ru/viewtopic.php?f=1&t=1817/]skazka.g-talk.ru/viewtopic.php?f=1&t=1817[/url]
[url=http://industrialagency.org/blogs/74709/Легкий-способ-получить-диплом-любой-профессии/]industrialagency.org/blogs/74709/Легкий-способ-получить-диплом-любой-профессии[/url]
[url=http://etoprosto.ru/ru/forum/?category=5&action=topic/]etoprosto.ru/ru/forum/?category=5&action=topic[/url]
[url=http://39504.org/member.php/]39504.org/member.php[/url]
Здравствуйте!
Приобрести диплом университета.
d91652pj.beget.tech/2024/07/04/kak-podyskat-proverennyy-onlayn-magazin-s-shirokim-vyborom-diplomov.html
Привет!
Всё о покупке аттестата о среднем образовании: полезные советы
forum.xpixel.ru/gallery/image/91-какие-онлайн-магазины-с-дипломами-существуют-на-сегодняшний-день/
Добрый день!
Заказать документ о получении высшего образования.
elitemagyaritasok.info/e107_plugins/forum/forum_viewtopic.php?id=3078&last=1
odesit.com/user.php?id.12115
openmotonews.ru/oformlenie-diplomov-s-minimalnyimi-zatratami
bezone.ru/node/339942
tyachiv.ukraine7.com/t21128-topic#39113
Привет!
Мы предлагаем документы техникумов
zavalinka.listbb.ru/viewtopic.php?f=3&t=2981
w77515cs.beget.tech/2024/07/22/legalno-i-bystro-oformite-diplom.html
sec31.ru/viewtopic.php?f=25&t=678141
sampnl.listbb.ru/viewtopic.php?f=3&t=500
onlinekinofun.ru/oformite-diplom-bez-ozhidaniya
[u][b] Здравствуйте![/b][/u]
[b]Как приобрести диплом о среднем образовании в Москве и других городах [/b]
[url=http://www.terrapevtika.ru/forum/?PAGE_NAME=message&FID=1&TID=511&TITLE_SEO=511-kupit-diplom-kandidata-nauk&MID=736&result=reply#message736/]www.terrapevtika.ru/forum/?PAGE_NAME=message&FID=1&TID=511&TITLE_SEO=511-kupit-diplom-kandidata-nauk&MID=736&result=reply#message736[/url]
[u][b] Рады оказаться полезными![u][b].
Здравствуйте!
Купить документ о получении высшего образования вы можете у нас в Москве.
diploms-x24.ru/kupit-diplom-ekaterinbur
Успехов в учебе!
Привет, друзья!
Приобрести диплом любого университета:
civilpatrol.info/?q=petition/81058/landsdiplomy
ledsoft.ru/forum/?PAGE_NAME=message&FID=5&TID=13698&TITLE_SEO=13698-diplomandoci&MID=14490&result=new#message14490
shooting-russia.ru/forum/?PAGE_NAME=message&FID=5&TID=15045&TITLE_SEO=15045-premiummdiplomms&MID=15310&result=new#message15310
forum.e4pool.com/viewtopic.php?t=5269
bank-garantiya.ru/index.php?subaction=userinfo&user=edumyre
Привет, друзья!
Приобрести диплом любого университета.
keros-mod.ru/index.php?/gallery/image/6-огромный-ассортимент-документов-в-популярном-магазине/
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
last info about becker
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
alisson
Здравствуйте!
Приобрести документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых ВУЗов России. Вы получите необходимый диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что при проверке документа работодателем, подозрений не появится.
Мы можем предложить дипломы любой профессии по невысоким тарифам. Стоимость будет зависеть от определенной специальности, года получения и университета. Стараемся поддерживать для покупателей адекватную ценовую политику. Для нас очень важно, чтобы дипломы были доступными для большого количества наших граждан.
indungii.ro/forum/index.php?/gallery/image/11-приобретаем-диплом-в-лучшем-интернет-магазине-по-выгодной-цене/
Всегда вам поможем!
Добрый день!
Купить документ о получении высшего образования.
metalfans.maxbb.ru/viewtopic.php?f=7&t=699
seaman.com.ua/forum/index.php?threads/bystroe-oformlenie-diploma-ljuboj-specialnosti.37730/
films.name/viewforum.php?f=143
myanimalgram.com/read-blog/397
ya.7bb.ru/viewtopic.php?id=12202#p34773
Добрый день!
Купить диплом любого университета.
naya.social/read-blog/81
sonnick84.designertoblog.com/59708802/Проверенный-интернет-магазин-с-широким-ассортиментом-дипломов
network-96082.mn.co/posts/61723991
erkibbutz.com/read-blog/480
cms-blog-news.de/modules.php?name=Journal&file=display&jid=206
дЅ еҐЅ
Здравствуйте!
Мы можем предложить документы ВУЗов
volnodumie.bbmy.ru/viewtopic.php?id=13228#p27055
forum.safe-animals.ru/index.php?showtopic=32092
saros-center.ru/forum/?PAGE_NAME=profile_view&UID=5851
newmedtime.ru/oformite-diplom-bez-posrednikov
khvoynaya.getbb.ru/viewtopic.php?f=39&t=6880
Привет, друзья!
Где приобрести диплом по необходимой специальности?
travelwithme.social/read-blog/45682
Добрый день!
Пошаговая инструкция по безопасной покупке диплома о высшем образовании
khelafat.com/blogs/4383/На-что-конкретно-обращать-внимание-при-заказе-диплома-в-интернете
Наши специалисты предлагает надежный сервисный ремонт мфу любых брендов и моделей. Мы понимаем, насколько значимы для вас ваши многофункциональные устройства, и стремимся предоставить услуги наилучшего качества. Наши опытные мастера работают быстро и аккуратно, используя только качественные детали, что обеспечивает надежность и долговечность наших услуг.
Наиболее общие проблемы, с которыми сталкиваются владельцы МФУ, включают неработающий картридж, неисправности сканера, ошибки ПО, неработающие разъемы и механические повреждения. Для устранения этих неисправностей наши квалифицированные специалисты выполняют ремонт печатающих головок, сканеров, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы обеспечиваете себе надежный и долговечный отремонтировать мфу с гарантией.
Подробная информация представлена на нашем сайте: https://remont-mfu-lite.ru
е‡єеЋ»
Привет!
Мы предлагаем дипломы любой профессии по приятным тарифам.
equilibrium-gaming.com/index.php?/gallery/image/11-быстрый-выбор-интернет-магазина-что-продает-дипломы-и-аттестаты/
sonnick84.qowap.com/87843716/Проверенный-магазин-с-широким-каталогом-дипломов
s24.team/club/user/148/blog/1611/
app-s.ru/blog/pochemu_namnogo_deshevle_i_proshhe_priobresti_diplom_universiteta/2024-07-04-1866
newsbig.cavandoragh.org/kak-zakazat-sejcas-neotlicimyj-ot-podlinnika-diplom-v-internete
Привет!
Заказать диплом университета
Наша компания предлагает быстро и выгодно приобрести диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями должностных лиц. Диплом способен пройти лубую проверку, даже при использовании профессионального оборудования. Достигайте свои цели быстро и просто с нашей компанией.
Где заказать диплом по актуальной специальности?
myliveroom.com/blogs/1056/Рекомендации-специалиста-что-возможность-дадут-быстро-купить-диплом
epistles.ru/blogs/1518/Быстрое-Оформление-Дипломов-Надежно-и-Легально
alik.forumrpg.ru/viewtopic.php?id=6859#p276097
http://www.forum.7x.ru/member.php?u=16498
delta72.at.ua/forum/61-26755-1
Здравствуйте!
Приобрести документ о получении высшего образования вы сможете у нас в Москве.
ast-diplomy24.ru/kupit-diplom-rostov-na-donu
Удачи!
Привет, друзья!
Приобрести документ университета
thehubbcommunitynetwork.mn.co/posts/61748285
gamefilm.ru/index.php?/gallery/image/119-тех-поддержка-и-faq-заказываем-диплом-в-сети/
wiki.intradition.ru/index.php/Какие_интернет_магазины_с_документами_есть_на_сегодняшний_момент?
hymaxonelae.theglensecret.com/cto-mozet-segodna-predlozit-onlajn-magazin-s-dokumentami
электрификация.рф/blogs/1/4e-glavnykh-gruppy-onlaynmagazinov-prodayushchikh-dokumenty.php
жЋЄж–Ѕ
not, you lose your bet.
buy ivermectin
[u][b] Привет, друзья![/b][/u]
Заказать документ о получении высшего образования вы сможете в нашем сервисе. Мы оказываем услуги по изготовлению и продаже документов об окончании любых университетов РФ. Вы получите необходимый диплом по любым специальностям, любого года выпуска, включая документы образца СССР. Даем гарантию, что при проверке документов работодателями, каких-либо подозрений не появится.
[url=http://newsofmebel.ru/kupit-diplom-bez-posrednikov/]newsofmebel.ru/kupit-diplom-bez-posrednikov[/url]
[url=http://heimur.ru/index.php?/gallery/image/124-большая-популярность-интернет-магазинов-что-продают-дипломы//]heimur.ru/index.php?/gallery/image/124-большая-популярность-интернет-магазинов-что-продают-дипломы/[/url]
[url=http://8bsbnjtgp.howeweb.com/28820997/Решили-узнать-как-приобрести-диплом-в-сети-недорого-Заходите/]8bsbnjtgp.howeweb.com/28820997/Решили-узнать-как-приобрести-диплом-в-сети-недорого-Заходите[/url]
[url=http://www.sledopit.club/wiki/index.php/Какие_онлайн_магазины_с_дипломами_на_текущий_день_имеются?/]www.sledopit.club/wiki/index.php/Какие_онлайн_магазины_с_дипломами_на_текущий_день_имеются?[/url]
[url=http://fomazy.com/blogs/4777/Полезные-рекомендации-по-покупки-документов-в-сети-интернет/]fomazy.com/blogs/4777/Полезные-рекомендации-по-покупки-документов-в-сети-интернет[/url]
е®Је‘Љ
Добрый день!
Узнайте, как приобрести диплом о высшем образовании без рисков
интайл.рф/communication/forum/messages/forum1/message9957/4954-khotite-bystro-priobresti-diplom-poluchenii-obrazovaniya?result=new#message9957
Окажем помощь!.
Добрый день!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании.
asxdiplomik24.ru/kupit-diplom-tehnikuma-kolledzha
Привет, друзья!
Мы предлагаем дипломы психологов, юристов, экономистов и прочих профессий по выгодным ценам. Цена будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для покупателей адекватную политику тарифов. Важно, чтобы дипломы были доступными для большого количества граждан.
gorillasocialwork.com/story17711001/купить-диплом-вуза
Привет, друзья!
Как купить аттестат 11 класса с официальным упрощенным обучением в Москве
azat.on.kg/blogs/893/ѕолучите-ќфициальный-?иплом-в- ратчайшие-—роки
Здравствуйте!
Приобрести документ ВУЗа можно в нашей компании в Москве.
ast-diplomy.com/kupit-diplom-chelyabinsk
Заказать диплом университета.
leydis16.phorum.pl/posting.php?mode=newtopic&f=1
polosedan-club.com/forums/Курилка.27/create-thread
daddycow.com/blogs/view/23911
forum.fiat-club.ru/blog_post.php?do=updateblog&blogid=
argayash.flybb.ru/viewtopic.php?f=9&t=1134
Ищите хоккейную экипировку? Зайдите на https://first-hockey.ru/ где вы сможете выбрать из широкого ассортимента, пол лучшим ценам и купить с доставкой в интернет магазине Первый-Хоккейный: клюшки, коньки, нагрудники хоккейные, налокотники, краги, шлемы и щитки хоккейные и многое другое. Доставка по всей России.
Привет!
Купить документ института
stareishina.com/gallery/image/3632-originality-diploman24com/
goruss.ru/blogs/956/Дипломы-по-комфортным-расценкам-в-лучшем-онлайн-магазине
roving.club/read-blog/730
cbr.by/club/user/1977/blog/326/
hvacprotalk.com/read-blog/217
На сайте https://thailand-company.ru/ вы узнаете о том, как правильно открыть компанию в Таиланде и какие ресурсы необходимо для этого использовать. При этом владелец компании в Таиланде может быть с любым гражданством. К важным преимуществам открытия бизнеса в Таиланде относят то, что здесь всегда растущий рынок, а регистрация не требует большого количества документов и не занимает много времени. Компания, которая зарегистрирована в Таиланде, идеальна для ведения международного бизнеса. На сайте вы узнаете и о самом процессе регистрации.
Привет, друзья!
Приобрести диплом любого университета.
ackeer.com/read-blog/486
wiki.market-master.ru/index.php/Четыре_основных_группы_интернет_магазинов,_реализующих_документы
telegra.ph/Kakie-onlajn-magaziny-s-dokumentami-est-na-segodnyashnij-moment-07-07
t98223u0.beget.tech/2024/07/04/dlya-chego-seychas-zakazyvayut-diplomy-i-attestaty-v-internete.html
sonnick84.losblogos.com/27848085/Что-потребуется-из-оборудования-для-создания-качественного-диплома
Привет, друзья!
Приобрести диплом университета:
forum.gtasiberia.ru/index.php?/topic/22711-купить-диплом-j917v/
nailpub.ru/forum/threads/norske-mobil-casino-eller-norske-betting-sider.41827/#post-1152463
webmontag.de/doku.php?id=diplomandoci
bizon15.ru/index.php?subaction=userinfo&user=abapaxo
mediawiki.envri.eu/index.php?title=diploman
е‘јз±І
Добрый день!
Приобрести диплом о высшем образовании.
bakinsky-dvorik.ru/club/user/127071/blog/4731/
Здравствуйте!
Приобрести документ института вы сможете в нашем сервисе.
diplomasx.com/kupit-diplom-krasnodar
Привет, друзья!
Заказать диплом любого университета.
socialnetwork.swazi-host.com/blogs/15612/Что-потребуется-из-оборудования-для-создания-диплома/
epicit.ru/page/3
wish-club.ru/forums/index.php?autocom=gallery&req=si&img=3867/
wow-tour.ru/page/4
newsofmebel.ru/page/2
Привет!
Где купить диплом специалиста?
http://www.marqueze.net/miembros/billyoung/profile/classic/
Добрый день!
Мы готовы предложить дипломы.
boxer-forum.ru/viewtopic.php?f=17&t=4003&sid=2de833240e94e2ab9d8a2b6a40779814
benedeek.com/blogs/90685/ упить-?иплом-Ѕыстро-и- онфиденциально
local-urban-eats.mn.co/posts/61814583
medrese1000-letie.ru/auth/?register=yes
g95334gq.beget.tech/2024/07/08/nastoyaschie-diplomy-bystro-i-legalno.html
Привет, друзья!
Заказать документ о получении высшего образования
lavienta.ru/forum/index.php?/gallery/image/214-почему-на-порядок-дешевле-будет-заказать-диплом-университета/
aquarium.zone/read-blog/1011
1wunwnyav.bloginder.com/28856838/Как-можно-будет-недорого-заказать-аттестат-в-магазине
miss2010.nuclear.ru/site_py/blogs/1/legkiy-vybor-onlayn-magazina-realizuyushchego-diplomy.php
sonnick84.ssnblog.com/27782128/Хотите-приобрести-диплом-у-проверенного-исполнителя-Ждем-Вас
Здравствуйте!
Купить документ о получении высшего образования.
kuvandyk.ru/message.php?msg=151
doctorsforum.ru/viewtopic.php?f=193&t=39101
vatrusha.maxbb.ru/viewtopic.php?f=2&t=697
kvartal8b.getbb.ru/viewtopic.php?f=19&t=21929
forum.supermunchkin.org/viewtopic.php?f=1&t=4182
дєЊ
Добрый день!
Мы можем предложить дипломы любых профессий по невысоким ценам.
sonnick84.weblogco.com/28300660/Что-сможет-сейчас-предложить-интернет-магазин-с-документами
sonnick84.59bloggers.com/28652365/На-что-именно-обращать-внимание-при-заказе-диплома-в-сети
sonnick84.liberty-blog.com/28305067/Известный-онлайн-магазин-с-очень-выгодными-по-цене-документами
sonnick84.bloggosite.com/34700636/Находим-проверенный-интернет-магазин-для-приобретения-диплома
pfggc2npo.blogchaat.com/28302174/Легко-заказываем-диплом-в-лучшем-онлайн-магазине-russian-diplom
дёЌеђЊзљ„
Добрый день!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
rsn360.ru/blogs/427/¬аш-?иплом- ачество-и-ѕодлинность
牆
Наш сервисный центр предлагает высококачественный вызвать мастера по ремонту мониторов рядом всех типов и брендов. Мы осознаем, насколько необходимы вам ваши мониторы, и готовы предложить сервис наилучшего качества. Наши опытные мастера оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что предоставляет длительную работу выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются пользователи дисплеев, включают неисправности подсветки, поврежденный экран, программные сбои, проблемы с портами и поломки компонентов. Для устранения этих неисправностей наши квалифицированные специалисты оказывают ремонт подсветки, матриц, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы гарантируете себе надежный и долговечный вызвать мастера по ремонту монитора с гарантией.
Подробная информация представлена на нашем сайте: https://remont-monitorov-plus.ru
Здравствуйте!
Купить документ университета
oolibuzz.com/read-blog/3291
newsbig.trexgame.net/nadeznyj-i-proverennyj-onlajn-magazin-s-bolsim-katalogom-diplomov
d6plus1.co.uk/read-blog/9878
japapmessenger.com/read-blog/506
nfrb.pl/index.php?/gallery/image/56-аттестаты-дипломы-и-свидетельства-в-лучшем-интернет-магазине/
Привет, друзья!
Мы изготавливаем дипломы любых профессий по невысоким ценам.
http://www.tuningevo.club/newforum/index.php?showuser=86824
Привет, друзья!
Приобрести диплом о высшем образовании.
wonecaegaehy.yousher.com/cto-mozet-sejcas-predostavit-magazin-s-diplomami
Привет, друзья!
Мы готовы предложить документы ВУЗов
financeokey.ru/poluchite-diplom-o-vyisshem-obrazovanii-bez-lishnih-hlopot
nalubyutemy.forum2x2.ru/t22759-topic#47987
stpos.ru/forum/user/36989/
raceburo.ru/legalnyiy-diplom-s-dostavkoy
fire-team.ru/forum/member.php?u=1143
Привет, друзья!
Купить документ о получении высшего образования можно в нашей компании в столице.
asxdiplomik24.ru/kupit-diplom-voronezh
Хорошей учебы!
Здравствуйте!
Мы можем предложить дипломы любой профессии по приятным тарифам.
service.gnla.com.au/2024/06/30/купить-диплом-капитана/
Привет, друзья!
Приобрести диплом о высшем образовании.
sonnick84.free-blogz.com/75551254/Ищем-надежный-интернет-магазин-для-приобретения-диплома
permn.ru/blogs/1/diplomy-po-nizkim-tsenam-v-populyarnom-internet-magazine.php
network-77917.mn.co/posts/61748309
imhht.com/index.php?title=Зачем_сегодня_покупают_дипломы_в_интернете?
newsbig.timeforchangecounselling.com/rekomendacii-po-pokupki-dokumentov-v-seti
Приобрести диплом о высшем образовании.
semeyka.listbb.ru/viewtopic.php?f=20&t=775
danceway74.ru/users/36
worksale.mn.co/posts/61852598
study.flybb.ru/viewtopic.php?f=4&t=410&sid=4f4d3e783480777d19487e8b1c689e9a
mosmol.flybb.ru/viewtopic.php?f=2&t=386
Strategies and Tips
where to buy ivermectin
Привет, друзья!
Приобрести диплом ВУЗа.
financetimenews.ru/page/3/
madesports.net/купить-диплом-в-бульгуме-анонимно-и-по/
aspenheightsliving.com/?URL=frees-diplom.com/
forum.mulegendreload.net/index.php?/gallery/image/221-быстрый-выбор-онлайн-магазина-реализующего-дипломы/
scientistsufo.ru/page/3
ж„џи¦є
Добрый день!
Приобрести диплом о высшем образовании:
rf-lowrate.ru/index.php?/topic/5125-купить-диплом-цена-y632q/
ssd-astra.ru/forum/viewtopic.php?f=14&t=7009
zanasite.free.fr/laripostedumardi/doku.php?id=russianydiplomix
usefulscript.ru/forum/showthread.php?tid=2474
mydnepr.pp.ua/forum/topic.php?forum=7&topic=940
Здравствуйте!
Мы предлагаем дипломы любой профессии по невысоким ценам.
socialnetwork.swazi-host.com/blogs/15612/Что-потребуется-из-оборудования-для-создания-диплома
famenest.com/read-blog/7753
sonnick84.blogerus.com/50949080/Что-требуется-для-создания-неотличимого-от-оригинала-документа
sonnick84.pointblog.net/Как-можно-быстро-купить-диплом-в-онлайн-магазине-69472426
gamefilm.ru/index.php?/gallery/image/119-тех-поддержка-и-faq-заказываем-диплом-в-сети/
[u][b] Добрый день![/b][/u]
[b]Заказать документ[/b] о получении высшего образования можно в нашей компании в Москве.
[url=http://diploms-x.com/kupit-diplom-specialista /]diploms-x.com/kupit-diplom-specialista [/url]
Здравствуйте!
Официальная покупка диплома вуза с сокращенной программой в Москве
lampcanvas.com/купить-диплом-о-высшем-образовании-со/
Рады оказаться полезными!.
Привет!
Мы изготавливаем дипломы.
together-19.com/read-blog/26601
exoltech.ps/blogs/post/58119
allsportime.ru/nastoyashhie-diplomyi-byistro-legalno-nadezhno
place-e.ru/index.php/Легальная_Покупка_Дипломов_Онлайн
animalprotect.org/forum/index.php?topic=234933.0
mosesolmos.com
еї…й €
angliannews.com
Добрый день!
Где купить диплом специалиста?
buro-alfa.ru/alfa/2022/04/22/zachem-neobhodimo-poluchenie-diploma-onlayn.html
姓
и»ЌйљЉ
Стоимость дипломов высшего и среднего образования и как избежать подделок
hashtap.com/@artur.sh/ваш-новый-диплом-уже-сегодня-26wKZvy55mwq
anatoliyrud.ekafe.ru/viewforum.php?f=29
netglu.com/read-blog/127_izuchite-nash-obzor-esli-nado-priobresti-diplom-v-seti.html
lookeify.com/read-blog/7444
igpsclub.ru/social/read-blog/5487
Привет!
Приобрести диплом любого ВУЗа
newmedtime.ru/vash-diplom-za-korotkoe-vremya-prosto-i-udobno
forexgroupx.ru/garantiya-polucheniya-diploma-byistro-i-legko
obozrevatelevents.ru/garantirovannoe-poluchenie-diploma-bez-riska-i-problem/
domainrama.com/read-blog/932
demo.advised360.com/read-blog/161734
Привет, друзья!
Заказать документ института вы можете у нас в Москве.
asxdiplomik24.ru/kupit-diplom-o-srednem-obrazovanii
Удачи!
На сайте https://msk.mramor-granit-kvarz.ru/ изучите работы компании, которая занимается созданием изделий из кварцевого агломерата, натурального камня. Здесь создают столешницы для ванной, кухни. Перед вами огромный ассортимент изделий, которые непременно украсят помещение. При необходимости сотрудники окажут помощь в выборе подходящего элемента, чтобы он вписался в интерьер. В компании также можете заказать и столешницы, выполненные из искусственного камня. На сайте изучите рекомендации по выбору.
купальники billabong цена – купить платье пляжное, купальники quiksilver цена
Наши специалисты предлагает высококачественный мастер по ремонту моноблоков на выезде всех типов и брендов. Мы осознаем, насколько значимы для вас ваши моноблоки, и обеспечиваем ремонт высочайшего уровня. Наши квалифицированные специалисты оперативно и тщательно выполняют работу, используя только качественные детали, что гарантирует длительную работу выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются владельцы моноблоков, включают поломку жесткого диска, поврежденный экран, ошибки ПО, проблемы с портами и перегрев. Для устранения этих поломок наши опытные мастера оказывают ремонт жестких дисков, дисплеев, ПО, разъемов и систем охлаждения. Обращаясь в наш сервисный центр, вы гарантируете себе надежный и долговечный сервисный центр по ремонту моноблоков.
Подробная информация представлена на нашем сайте: https://remont-monoblokov-rial.ru
Здравствуйте!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
br-totalbyg.dk/2024/06/24/диплом-в-три-клика/
Привет, друзья!
Заказать диплом университета.
spg.co.kr/bbs/board.php?bo_table=cus_res&wr_id=1052&page=72
xpertmapping.com/category/digital-marketing/
dadiler.com/купить-диплом/
qyshikisoxa.lowescouponn.com/cto-potrebuetsa-iz-oborudovania-dla-izgotovlenia-diploma/
sharaepewixu.iamarrows.com/cto-neobhodimo-iz-tehniki-dla-proizvodstva-diploma/
יכולים להיות חיילים, סטודנטים, גרושים או בקיצור כל גבר ממוצע שרוצה לבלות. זהו פתרון המשלב גם נערה יפה שמפנקת אותך, וגם סביבת אביב, לפעמים קשה למצוא את המילים שמתארות את החוויה. נעים, מענג, מעורר, משחרר, מדהים ובלתי נשכח הם חלק מהמילים שבהם גברים אירוח סקס
ЭЭГ головного мозга Москва cecilplus.ru
Что касается консультация уролога в москве мы Вам с легкостью поможем. Оказываем консультации, лечение и диагностику по множественным направлениям. В их числе: геронтология, терапия, невролгия-вегетология, урология, психотерапия и многие другие. По возникшим вопросам звоните по номеру телефона +7(499)705-04-19 или закажите обратный звонок на веб сайте cecilplus.ru прямо сейчас. Также есть интернет запись и оплата консультации для Вашего комфорта.
Добрый день!
Заказать диплом ВУЗа.
chrstms.ru/club/user/11503/blog/11039/
Привет, друзья!
Заказать документ института можно у нас в столице.
ast-diplomy.com/kupit-diplom-ekaterinbur
Удачи!
Сегодня большинство игроков предпочитают использовать смартфоны для игры в онлайн казино. Telegram канал лучшие мобильные казино с лицензией выделяет лучшие мобильные платформы. Эти казино предлагают оптимизированные приложения и мобильные версии сайтов, обеспечивая удобный интерфейс и быструю загрузку игр.
Мобильные казино позволяют играть в любое время и в любом месте. Они предлагают бонусы и акции специально для пользователей смартфонов. Подписывайтесь на канал, чтобы быть в курсе новинок и получать выгодные предложения для игры на мобильных устройствах.
На сайте https://mpmgr.ru воспользуйтесь специальным менеджером маркетплейсов для того, чтобы вы автоматизировали и упростили работу с такими маркетплейсами, как Ozon, Wildberries, Яндекс.Маркет. Здесь специально для вас рассчитают поставки, а также будут эффективно управлять рекламой, ответят на отзывы клиентов, отследят товары, помогут рассчитать скидку. Такая услуга сэкономит время специалистов, они смогут заняться более серьезными, ответственными делами. Происходит оптимизация расходов для вашей большей прибыли.
еЅўејЏ
жІ’жњ‰
Innovative Restaurant Design Solutions for Unique Dining Spaces
Industrial Kitchen Area Specialist Business
Pick our industrial cooking area professional firm for trustworthy cooking area construction and improvement services. We build and update cooking areas to enhance performance and conformity.
再見
Добрый день!
Купить диплом университета.
sonnick84.thenerdsblog.com/33799466/%D0%A7%D1%82%D0%BE-%D0%B8%D0%BC%D0%B5%D0%BD%D0%BD%D0%BE-%D0%BF%D0%BE%D1%82%D1%80%D0%B5%D0%B1%D1%83%D0%B5%D1%82%D1%81%D1%8F-%D0%B8%D0%B7-%D1%82%D0%B5%D1%85%D0%BD%D0%B8%D0%BA%D0%B8-%D0%B4%D0%BB%D1%8F-%D0%BF%D1%80%D0%BE%D0%B8%D0%B7%D0%B2%D0%BE%D0%B4%D1%81%D1%82%D0%B2%D0%B0-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%BE%D0%B2
й—њж–ј
Здравствуйте!
Мы предлагаем документы техникумов
humped.life/read-blog/819
vip.forums.party/viewtopic.php?id=3460#p71128
scaleforum.ru/member.php?u=62004
seriallove.bbok.ru/viewtopic.php?id=7233#p123279
dexanet.ukrbb.net/viewtopic.php?f=5&t=16474
Привет!
Диплом бакалавра
astroroleplay.getbb.ru/viewtopic.php?f=6&t=505
dragonlivers.ixbb.ru/viewtopic.php?id=126#p126
school97.ru/vesti20/index.php?PAGE_NAME=profile_view&UID=210620
linux.listbb.ru/viewtopic.php?f=2&t=506
girlscools.ru/zakazhite-diplom-pryamo-seychas
דירות דיסקרטיות בתל אביב לבילוי מטריף חושים רווקים שרוצים לבלות עם נערות מטריפות, נשואים שצריכים קצת גיוון או אנשי עסקים בשבוע. בכל פעם שמתחשק לך, אתה יכול לבקר כאן וליהנות מבילוי מתוק. נערות ליווי בתל אביב – לפתוח דלת לעולם חדש נערות ליווי מסאז אירוטי בחיפה
Добрый день!
Реально ли приобрести диплом стоматолога? Основные этапы
yacina.net/купить-диплом-о-высшем-образовании-ре/
Поможем вам всегда!.
На сайте https://ustanovki-zapravki.ru вы узнаете о том, какую установку для того, чтобы заправить автокондиционер, лучше всего выбрать. Ознакомитесь с преимуществами, а также отрицательными сторонами ручных установок, которые используются для заправки устройств. Также рассматриваются и дополнительные функции, которые крайне необходимы вам. Даются ценные советы, которые помогут быстрее подобрать устройство в соответствии с потребностями компании. Рассматриваются особенности применения профессионального оборудования.
Привет, друзья!
Мы предлагаем дипломы любой профессии по доступным тарифам.
http://www.kikwit.alobi.cd/2024/06/30/купить-диплом-в-ессентуки/
Здравствуйте!
Приобрести документ о получении высшего образования.
автомедведь.рф/club/log/?SECTION_CODE=log
publikacii.listbb.ru/viewtopic.php?f=3&t=689
ya.0bb.ru/viewtopic.php?id=12032#p32092
recept-food.ru/diplomyi-priznannyie-rabotodatelyami
moskvic.actieforum.com/t3741-topic#7030
Name], each offering unique bonuses and promotions for Aviator Game players.
ivermectin where to buy
Приобрести диплом о высшем образовании.
net4women.ru/blogs/3881/Купить-Легальный-Диплом-Быстро-и-Конфиденциально
anatoliyrud.ekafe.ru/viewforum.php?f=29
kronverskiy.ru/posting.php?mode=post&f=28
bintarotrojan.com/blogs/new
biznas.com/Biz-postsm333204_Default.aspx#post333204
Привет, друзья!
Мы можем предложить дипломы любой профессии.
http://www.thepatronway.com/купить-дипломы-нового-образца/
Будем рады вам помочь!.
Здравствуйте!
Заказать диплом о высшем образовании.
neurostarcheats.com/index.php?/gallery/image/29-огромный-каталог-документов-в-знаменитом-онлайн-магазине/
Добрый день!
Приобрести документ института вы можете у нас.
asxdiplomik.com/kupit-diplom-ekaterinbur
Успешной учебы!
Привет, друзья!
Мы готовы предложить документы ВУЗов
digdroid.com/forums/entry/signin
bodybuilding.net/members/worksale.html
g95334gq.beget.tech/2024/07/18/oformite-diplom-bez-ozhidaniya.html
forum.fiat-club.ru/blog_post.php?do=updateblog&blogid=
mosday.getbb.ru/viewtopic.php?f=12&t=1358
Top News Sites for Article Post Permanent
aljazeeranewstoday.com
australiannewstoday.com
bbcworldnewstoday.com
bloombergnewstoday.com
bostonnewstoday.com
britishnewstoday.com
Dont hesitate to Contact me.
Охраняйте свою конфиденциальность с резидентскими прокси, для чего это нужно.
Обходите географические блокировки с резидентскими прокси, и наслаждайтесь контентом.
Получите быстрый и надежный интернет с резидентскими прокси, как это работает.
Скройте свой реальный IP-адрес от хакеров с резидентскими прокси, и не беспокойтесь о своей безопасности.
Прячьте свою локацию и IP-адрес с резидентскими прокси, и оставайтесь незамеченными.
Используйте резидентские прокси для безопасного серфинга в интернете, и не тревожьтесь за свою приватность.
резидентский прокси сервер https://rezidentnie-proksi.ru/ .
Наши специалисты предлагает надежный ремонт моноколеса с гарантией различных марок и моделей. Мы понимаем, насколько значимы для вас ваши моноколеса, и готовы предложить сервис высочайшего уровня. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что гарантирует долговечность и надежность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются владельцы моноколес, включают поломку аккумулятора, неисправности двигателя, сбои контроллера, неработающие сенсоры и повреждения рамы. Для устранения этих неисправностей наши квалифицированные специалисты выполняют ремонт батарей, двигателей, контроллеров, гиросенсоров и механических компонентов. Доверив ремонт нам, вы гарантируете себе надежный и долговечный официальный ремонт моноколес на дому.
Подробная информация размещена на сайте: https://remont-monokoles-serv.ru
Привет!
Купить документ университета.
polosedan-club.com/search/search
formulaf1.ru/diplomyi-lyuboy-slozhnosti-byistro-i-bez-problem
mosmol.flybb.ru/viewtopic.php?f=2&t=399
subscribe.ru/member/quick
konstruktiv.getbb.ru/viewtopic.php?f=17&t=6789
жґ»
ומקשיח את מה שצריך להקשיח. להרגע עם הבחורות היפות של דירות דיסקרטיות בחיפה כולנו סובלים מסטרס. לפעמים אלו צעירים העובדים שעות זהו שירות המספק את הצרכים של הגוף הגברי ואת המהות של להיות גבר. בילוי עם נערות ליווי בתל אביב מאפשר לגבר להשתחרר ולהתפרק. זוהי erlinda streetman
Здравствуйте!
Мы изготавливаем дипломы.
vip.forums.party/viewtopic.php?id=3414#p70988
onlaintelevizia.listbb.ru/viewtopic.php?f=2&t=475
spasibo.kz/bonus.php
ashinova.ru/log-in.html
1mog.listbb.ru/posting.php?mode=post&f=6&sid=aa142b22cb7ce421e4da458c9a5b6fd1
Привет, друзья!
Мы можем предложить документы техникумов
lezt.ixbb.ru/viewtopic.php?id=121#p121
моя-соцсеть.рф/blogs/new
dinsta-gram.com/read-blog/5663
scientistsufo.ru/diplomyi-vseh-spetsialnostey-na-zakaz
ericos.ru/forum/index.php?PAGE_NAME=profile_view&UID=10813
Привет, друзья!
Купить диплом любого университета
gaysonline.info/blogs/7/Читайте-наш-материал-если-нужно-приобрести-диплом-в-сети
roxgo.cl/gallery/image/4256-почему-магазины-с-дипломами-столь-популярны/
zdsim.ru/wiki/index.php/Надежные_дипломы_для_вашего_успеха
startinvest.2bb.ru/viewtopic.php?id=10516#p53862
mf.getbb.ru/viewtopic.php?f=28&t=642
Как оказалось, купить диплом кандидата наук не так уж и сложно
recept-food.ru/kak-kupit-diplom-poshagovoe-rukovodstvo
dedas5f69.bloggazzo.com/27844450/Прочитайте-наш-обзор-если-требуется-купить-диплом-в-интернете
oldforum.citysakh.ru/?talkid=26696
slliver.getbb.ru/viewtopic.php?f=62&t=922
o91707v5.beget.tech/2024/07/10/oficialnye-diplomy-po-dostupnoy-cene.html
ж”ѕ
Привет!
Приобрести документ о получении высшего образования
grimdice.ru/index.php?/gallery/image/1-быстрый-выбор-онлайн-магазина-который-продает-дипломы-и-аттестаты/
nongkhai.online/blogs/99/Надежный-интернет-магазин-с-широким-ассортиментом-дипломов
network-230.mn.co/posts/61837914
vwapepla.com/read-blog/132
create-lifestyle.mn.co/posts/61724492
Привет, друзья!
Всё, что нужно знать о покупке аттестата о среднем образовании без рисков
rdcvw.com/space-uid-320969.html
Поможем вам всегда!.
йѓЁй•·
з€ёз€ё
Привет, друзья!
Приобрести документ института вы можете в нашей компании.
diplomyx.com/kupit-diplom-novosibirsk
Привет, друзья!
Приобрести документ о получении высшего образования
indianhighcaste.com/read-blog/2060
sonnick84.blogpayz.com/28286537/Грамотно-заказываем-диплом-в-сети-обзор
agarwalconnect.com/blogs/164/Как-найти-проверенный-интернет-магазин-продающий-дипломы
powerofthelamb.mn.co/posts/61638766
geoamor.com/read-blog/30282
Привет, друзья!
Купить документ о получении высшего образования
diplomyx.com/kupit-diplom-voronezh
Здравствуйте!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
arusak-diploms-srednee.ru/kupit-attestat-za-11-klass В
Привет, друзья!
Приобрести документ института можно у нас в столице. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России.
forum.gtasiberia.ru/index.php?/topic/22713-купить-диплом-v416l/
nis.com.tn/index.php?option=com_kunena&view=topic&catid=3&id=6740&Itemid=151
kioskindustry.ru/index.php?subaction=userinfo&user=usuwupi
biowiki.clinomics.com/index.php?title=russianydiplomix
old.pokvesti.ru/forum/viewtopic.php?f=42&t=92401
Добрый день!
Приобрести документ института
heyjinni.com/read-blog/109294
shopwheel.ru/club/user/49/blog/54941/
telegra.ph/Zakazyvaem-diplom-v-luchshem-onlajn-magazine-po-vygodnoj-stoimosti-07-09
sonnick84.blogoscience.com/34228380/Желаете-приобрести-аттестат-у-надежного-исполнителя-Заходите
friends.win/read-blog/3534
Здравствуйте!
Заказать документ института вы имеете возможность в нашей компании в столице.
ast-diploms.com/kupit-diplom-krasnodar
иЁ±д№…
Привет, друзья!
Купить диплом о высшем образовании
krugozorov.ru/forum/user/9182/
olive-penguin-h97mx0.mystrikingly.com/blog/dec09af525d
bence.net/read-blog/71
shockmusik.ru/vash-put-k-uspehu-diplom-na-zakaz
krugozorov.ru/forum/user/9183/
Добрый день!
Мы изготавливаем дипломы любых профессий по приятным ценам.
wibawaabadi.com/2024/06/30/купить-диплом-мибд-или-любого-вуза-рос/
з”·з”џ
the opportunity to compete for larger prizes and showcase their skills on a larger stage.
ivermectin cheap
Привет!
Купить диплом любого университета.
koveclub.ru/index.php?/gallery/image/193-большой-ассортимент-документов-в-знаменитом-интернет-магазине/
Наша мастерская предлагает надежный сервисный центр по ремонту морозильных камер рядом любых брендов и моделей. Мы осознаем, насколько необходимы вам ваши морозильные камеры, и обеспечиваем ремонт высочайшего уровня. Наши опытные мастера работают быстро и аккуратно, используя только качественные детали, что предоставляет надежность и долговечность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются пользователи морозильников, включают проблемы с охлаждением, неисправности термостата, неисправности программного обеспечения, проблемы с подключением и поломки корпуса. Для устранения этих неисправностей наши квалифицированные специалисты проводят ремонт компрессоров, термостатов, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы обеспечиваете себе долговечный и надежный ремонт морозильных камер с гарантией.
Подробная информация доступна на сайте: https://remont-morozilnyh-kamer-spec.ru
еёё
Привет!
Мы можем предложить дипломы любой профессии по невысоким ценам.
электрификация.рф/blogs/1/4e-glavnykh-gruppy-onlaynmagazinov-prodayushchikh-dokumenty.php
купить государственный диплом купить государственный диплом .
е…€
Добрый день!
Приобрести документ ВУЗа.
peaceofficial.5nx.ru/viewtopic.php?f=111&t=815
define.listbb.ru/viewtopic.php?f=46&t=522
human.forumieren.de/t312-topic#382
sz.80lvl.ru/viewtopic.php?f=9&t=1929
kherson.forum2x2.ru/t10905-topic#26323
оснащение конференц залов оснащение конференц залов .
На сайте https://travamana.ru/ представлены ароматные, приятные травяные чаи. Они полностью натуральные, приготовлены из редких и популярных растений, трав, которые произрастают в России. В уютном магазинчике можно приобрести специи, подарки, зарядиться приятными и положительными эмоциями, ощутить радость и покой. Компетентные консультанты дадут совет, что лучше всего приобрести в каждом конкретном случае. Есть успокаивающие сборы, для иммунитета, гинекологические. Если вы подбираете подарок для близкого человека, то здесь вы найдете все самое необходимое.
Привет!
Купить документ о получении высшего образования
diploms-x.com/kupit-diplom-o-srednem-obrazovanii
Здравствуйте!
Парадокс, но купить диплом кандидата наук оказалось не так и сложно
landik-diploms-srednee.ru/kupit-diplom-v-novosibirske В
Привет, друзья!
Заказать документ университета
newsbig.huicopper.com/proverennyj-internet-magazin-s-bolsim-katalogom-dokumentov
codinganme.com/gallery/image/118-аттестаты-дипломы-и-свидетельства-в-известном-интернет-магазине/?context=new
4atex.ru/blogs/2317/Дипломы-аттестаты-и-свидетельства-в-знаменитом-магазине
socialhustle.co.uk/read-blog/2356
plplatoon.com/gallery/image/116-зачем-сегодня-приобретают-аттестаты-и-дипломы-в-сети-интернет/
Привет, друзья!
Купить документ ВУЗа можно у нас в столице. Мы предлагаем документы об окончании любых университетов России. Вы получите диплом по любым специальностям, любого года выпуска, включая документы образца СССР. Гарантируем, что при проверке документа работодателями, подозрений не возникнет.
Мы изготавливаем дипломы любых профессий по доступным тарифам. Цена будет зависеть от определенной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику цен. Важно, чтобы дипломы были доступными для большого количества граждан.
ebonyfaces.com/blogs/36/Быстро-заказываем-документы-в-лучшем-онлайн-магазине-Russian-Diplom
Рады помочь!
Привет, друзья!
Приобрести документ университета можно у нас в Москве.
ast-diplomas24.ru/kupit-diplom-ekaterinbur
Успешной учебы!
е¤њж™љ
Привет!
Купить диплом ВУЗа.
igpsclub.ru/social/read-blog/5452
зѕЋйє—зљ„
Привет!
Заказать диплом любого университета.
forum.recifalnews.fr/gallery/image/211-широкий-ассортимент-документов-в-знаменитом-интернет-магазине/
Привет, друзья!
Купить документ о получении высшего образования вы имеете возможность у нас в столице.
ast-diplomas.com/kupit-diplom-rostov-na-donu
Хорошей учебы!
Привет, друзья!
Как получить диплом техникума с упрощенным обучением в Москве официально
orangekitchendecor.all-new.info/купить-диплом-в-артеме/
Привет, друзья!
Купить документ о получении высшего образования.
itbitgroup.ru/poluchite-diplom-za-schitannyie-dni
vidagrafia.com/read-blog/176141
bestcoolfun.ru/poluchite-diplom-v-kratchayshie-sroki
worksale.mn.co/posts/62242258
forum.qwas.ru/uskorenniy-process-polucheniya-diploma-t20155.html
Привет!
Заказать документ университета можно у нас в столице.
ast-diplomas.com/kupit-diplom-s-registraciej
и·‘жҐ
переговорная комната под ключ переговорная комната под ключ .
女兒
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании.
diploms-x.com/kupit-diplom-rostov-na-donu
Удачи!
Наш сервисный центр предлагает профессиональный мастерская по ремонту ноутбука на дому всех типов и брендов. Мы понимаем, насколько важны для вас ваши лаптопы, и стремимся предоставить услуги наилучшего качества. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только сертифицированные компоненты, что обеспечивает долговечность и надежность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются обладатели переносных компьютеров, включают поломку жесткого диска, поврежденный экран, неисправности программного обеспечения, неисправности разъемов и неисправности системы охлаждения. Для устранения этих проблем наши квалифицированные специалисты выполняют ремонт жестких дисков, экранов, ПО, разъемов и систем охлаждения. Обращаясь в наш сервисный центр, вы обеспечиваете себе долговечный и надежный сервис ремонта ноутбуков рядом.
Подробная информация размещена на сайте: https://remont-noutbukov-first.ru
Добрый день!
Мы предлагаем документы ВУЗов
telearchaeology.org/TAWiki/index.php/ваш_путь_к_успеху_с_дипломом
chaodisiaque.com/forum/viewtopic.php?pid=22057#p22057
nagatinos.getbb.ru/viewtopic.php?f=6&t=588
avtolux48.ru/people/user/374/blog/8001/
paintball-keller-lev.de/ucp.php?mode=login
Здравствуйте!
Заказать документ о получении высшего образования.
forex.g-talk.ru/viewtopic.php?f=43&t=7121
sampcrmrp.1stbb.ru/viewtopic.php?f=117&t=1004
montrealpal.com/read-blog/1034
автомедведь.рф/club/log/?SECTION_CODE=log
besconeshnocte.flybb.ru/viewtopic.php?f=2&t=953
Здравствуйте!
Мы предлагаем дипломы любых профессий по приятным тарифам. Цена будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для покупателей адекватную политику цен. Для нас важно, чтобы документы были доступны для большого количества граждан.
tetrabookmarks.com/story17135938/купить-диплом-ссср
Здравствуйте!
Приобрести диплом любого университета.
anhbiet.com/index.php?/events/event/8-огромный-каталог-документов-в-популярном-онлайн-магазине/
Добрый день!
Заказать диплом ВУЗа:
kcapa.net/bbs/board.php?bo_table=free&wr_id=1667799
nis.com.tn/index.php?option=com_kunena&view=topic&catid=2&id=6776&Itemid=151
krasrec.ru/forum/user/199873/
agrosoft.ru/support/forum/index.php?PAGE_NAME=profile_view&UID=85478
littleyaksa.yodev.net/bbs/board.php?bo_table=free&wr_id=6404553
Сколько можно проигрывать? Пора выбирать реальные казино! Telegram канал рейтинг лучших мобильных онлайн казино представляет лучшие онлайн казино для игры на деньги. Эти платформы предлагают щедрые бонусы на первый депозит и разнообразие игровых автоматов, а также быстрый вывод средств на карты Сбербанка, ВТБ и Т-банка.
Ежедневные обновления гарантируют честные и проверенные казино. Подписывайтесь на канал и играйте в казино, где реально выиграть деньги. Оставьте неудачи позади и начните свой путь к большим выигрышам!
Привет!
Приобрести диплом университета
Мы предлагаем выгодно заказать диплом, который выполнен на бланке ГОЗНАКа и заверен мокрыми печатями, штампами, подписями должностных лиц. Наш документ способен пройти любые проверки, даже с применением профессионального оборудования. Достигайте свои цели быстро и просто с нашей компанией.
Где приобрести диплом по нужной специальности?
avva.getbb.ru/viewtopic.php?f=3&t=571
http://www.nasseej.net/blogs/148443/Прочитайте-наш-материал-если-требуется-купить-диплом-в-сети
wiki.roximo.ru/index.php/Легкий_выбор_онлайн-магазина,_реализующего_дипломы
daddycow.com/blogs/view/23911
lib22.ru/question/blagodarya-chemu-internet-magaziny-s-dokumentami-stol-populyarny/
Привет, друзья!
Как оказалось, купить диплом кандидата наук не так уж и сложно
webyourself.eu/blogs/358414/ упите-?ипломы-Ѕыстро-и-Ќадежно
Привет, друзья!
Мы готовы предложить документы ВУЗов
13.flybb.ru/viewtopic.php?f=20&t=1076
raussga.flybb.ru/viewtopic.php?f=12&t=2226
school8kaluga.flybb.ru/viewtopic.php?f=19&t=502
worksale.jofo.me/2279541.html?_ga=2.93580829.1687026258.1721576664-1642673413.1721576664
kryza.network/create-blog/
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашем сервисе. Мы предлагаем документы об окончании любых университетов России. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Даем 100% гарантию, что при проверке документов работодателями, никаких подозрений не возникнет.
biiut.com/read-blog/65942
http://www.zooclub.com.ua/o-proekte
biocenter.pro/club/blogs/sonnick84-blog-bc/legkiy-vybor-onlaynmagazina-realizuyushchego-diplomy/
fatshipresident.net/read-blog/217
iqtorg.ru/forum/user/19115/
Здравствуйте!
Заказать документ университета
ast-diplomas.com/kupit-diplom-krasnoyarsk
plane crashes, making it a game of both luck and timing. This dynamic gameplay keeps players engaged and coming
cheap ivermectin
еЏЇж„›зљ„
Добрый день!
Быстрая схема покупки диплома старого образца: что важно знать?
arusak-diploms-srednee.ru/kupit-diplom-v-krasnodare В
Добрый день!
Мы готовы предложить дипломы любой профессии по приятным ценам.
http://www.find-topdeals.com/blogs/133052/Высококачественные-дипломы-на-заказ
Здравствуйте!
Где приобрести диплом специалиста?
kryza.network/read-blog/11426191
Здравствуйте!
Заказать документ университета.
fremontrp.listbb.ru/viewtopic.php?f=18&t=449
1776reloaded.us/blogs/88/Получите-диплом-за-считанные-дни
n-staff.ru/forum?mode=edit&type=thread&forum_id=74041
batirafrica.blog4ever.com/forum/arts-cultures/sujet-41
mockwacom.getbb.ru/viewtopic.php?f=12&t=2189
Привет, друзья!
Мы предлагаем документы техникумов
c90226sl.beget.tech/2024/07/18/oformlenie-diplomov-bez-posrednikov/
odessaforum.getbb.ru/viewtopic.php?f=5&t=20862
financeokey.ru/poluchite-diplom-o-vyisshem-obrazovanii-bez-lishnih-hlopot
army.clanfm.ru/viewtopic.php?f=2&t=38994
forumkk.listbb.ru/viewtopic.php?f=12&t=458
дёЂеЂ‹йЃЉж€І
переговорные комнаты москва переговорные комнаты москва .
Привет, друзья!
Приобрести документ о получении высшего образования вы имеете возможность в нашем сервисе. Мы предлагаем документы об окончании любых университетов РФ.
ufb38096.bget.ru/index.php?subaction=userinfo&user=itocudo
hosting.show/profile/ynanebun/
http://www.clean-ace8.com/bbs/board.php?bo_table=free&wr_id=353253
forum.stpku.ru/viewtopic.php?f=2&t=51964
spectral-lamps.kz/index.php?subaction=userinfo&user=ykititan
зњ‹
Привет!
Купить диплом о высшем образовании
Мы предлагаем выгодно и быстро купить диплом, который выполняется на оригинальной бумаге и заверен печатями, водяными знаками, подписями. Данный документ пройдет любые проверки, даже при помощи специальных приборов. Достигайте цели быстро и просто с нашим сервисом.
Где купить диплом специалиста?
http://www.pets-ural.ru/content/forum/viewtopic.php?p=78013#78013
musicianforums.net/index.php?/gallery/image/142-4-основных-группы-интернет-магазинов-реализующих-документы/
molbiol.ru/forums/index.php?showtopic=1234113
astrcolcult.ru/training/forum/сольное-и-хоровое-народное-пение-хоро/
n0juz5csr.bloginder.com/28858176/Решили-узнать-как-заказать-диплом-в-сети-интернет-Ждем-Вас
套裝
Привет, друзья!
Заказать документ о получении высшего образования
testsajtet.net/read-blog/215
sonnick84.blogrenanda.com/34141702/Что-сможет-в-наше-время-предоставить-интернет-магазин-с-документами
humansandslaves.ru/blogs/697/Покупаем-документы-в-известном-магазине-по-комфортной-цене
humped.life/read-blog/535
uconnect.ae/read-blog/82549
Привет!
Купить документ института вы имеете возможность в нашей компании в столице.
ast-diplomas.com/kupit-diplom-vracha
Успехов в учебе!
Наши специалисты предлагает надежный отремонтировать объектив адреса различных марок и моделей. Мы знаем, насколько значимы для вас ваши фотообъективы, и обеспечиваем ремонт первоклассного уровня. Наши профессиональные техники работают быстро и аккуратно, используя только качественные детали, что гарантирует долговечность и надежность наших услуг.
Наиболее распространенные поломки, с которыми сталкиваются обладатели фотообъективов, включают неработающую фокусировку, проблемы с диафрагмой, механические повреждения, проблемы с автофокусом и попадание влаги. Для устранения этих поломок наши профессиональные техники проводят ремонт фокусировки, диафрагмы, автофокуса, очистку линз и восстановление корпуса. Обратившись к нам, вы гарантируете себе надежный и долговечный центр ремонта объективов в москве.
Подробная информация доступна на сайте: https://remont-obektivov-magic.ru
Привет!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
http://www.lifecapadvisors.com/диплом-техникума-колледжа-1997-2003-фото/
Привет!
Заказать документ института можно у нас в Москве. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы получите необходимый диплом по любой специальности, любого года выпуска, в том числе документы СССР. Гарантируем, что при проверке документа работодателем, никаких подозрений не появится.
http://www.hristianka.ru/forum/r/prev_loaded/1/
ukrevents.ru/nastoyashhie-diplomyi-bez-lishnih-voprosov/
iaescortsmap.ixbb.ru/viewtopic.php?id=105#p105
http://www.wowonder.xyz/read-blog/78394
iloveyouclub.net/blogs/1893/Что-сможет-в-наше-время-предоставить-магазин-с-документами
Приобрести диплом о высшем образовании.
sfera100.ru/forum/user/2583/
moneysweet.listbb.ru/viewtopic.php?f=2&t=1915
funchange.getbb.ru/viewtopic.php?f=8&t=1351
krasnodarforum.ru/member.php?u=2812
meldog.3nx.ru/viewtopic.php?p=23644#23644
Здравствуйте!
Приобрести документ о получении высшего образования
eyawei-networks.mn.co/posts/61592349
wiki.gta-zona.ru/index.php/4_основных_группы_онлайн-магазинов,_которые_реализуют_документы
sonnick84.weblogco.com/28265335/Желаете-купить-диплом-Открывайте-наш-онлайн-магазин
aleluiah.com/read-blog/67
sonnick84.csublogs.com/34308172/Проверенный-и-надежный-интернет-магазин-с-большим-выбором-документов
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по приятным ценам.
socialle.com.br/blogs/256/Как-возможно-приобрести-сегодня-качественный-диплом-в-сети
[u][b] Привет![/b][/u]
Мы предлагаем дипломы.
[url=http://exoltech.us/blogs/206684/Ќасто€щие-?ипломы-Ѕыстро- онфиденциально-Ћегально/]exoltech.us/blogs/206684/Ќасто€щие-?ипломы-Ѕыстро- онфиденциально-Ћегально[/url]
[url=http://wegug.in/blogs/1013/Купить-диплом-быстро-и-надежно/]wegug.in/blogs/1013/Купить-диплом-быстро-и-надежно[/url]
[url=http://chessdatabase.science/wiki/Купить_Официальный_Диплом_Быстро_и_Легально/]chessdatabase.science/wiki/Купить_Официальный_Диплом_Быстро_и_Легально[/url]
[url=http://bmc.ukrbb.net/viewtopic.php?f=8&t=13787/]bmc.ukrbb.net/viewtopic.php?f=8&t=13787[/url]
[url=http://backshowtime.ru/vash-nastoyashhiy-diplom-legalno-i-nadezhno/]backshowtime.ru/vash-nastoyashhiy-diplom-legalno-i-nadezhno[/url]
Бесплатный сервис по подбору и ведению сделок с недвижимостью в новостройках Москвы и Московской области! Новые квартиры для жизни, дохода или инвестирования от топовых застройщиков с защитой государства купить квартиру в столице
see post smmpanel.one
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
loolita.es/blogs/4290/Полезные-рекомендации-по-приобретению-диплома-в-сети-интернет
Привет, друзья!
Мы предлагаем документы техникумов
censornet.ru/legalnoe-oformlenie-diplomov/
forum.safe-animals.ru/index.php?showtopic=32224
vsetutonline.com/forum/member.php?u=76509
weekevents.ru/diplom-o-vyisshem-obrazovanii-dlya-ambitsioznyih-professionalov
kondrateff.5bb.ru/viewtopic.php?id=6819#p12796
Добрый день!
Приобрести документ о получении высшего образования можно в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов России.
mail.unnewsusa.com/bbs/board.php?bo_table=free&wr_id=2227274
academijacrimea.ru/index.php?subaction=userinfo&user=epuci
http://www.fromrus.su/index.php?/topic/13488-купить-диплом-t707k/
alternatio.org/index.php?option=com_k2&view=itemlist&task=user&id=159505
forum1.kukly.ru/profile.php?action=show&member=79238
Добрый день!
Купить диплом любого ВУЗа
Наши специалисты предлагают выгодно и быстро приобрести диплом, который выполняется на бланке ГОЗНАКа и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Наш диплом пройдет любые проверки, даже при использовании профессионального оборудования. Достигайте своих целей быстро с нашей компанией.
Где купить диплом специалиста?
http://www.chaodisiaque.com/forum/viewtopic.php?pid=22028#p22028
awakehill.com/read-blog/4418
sampnewrp.listbb.ru/viewtopic.php?f=18&t=515&sid=97a8fe8d96d5495821f74de844e5d46b
antennastar.com/blogs/499/Купить-диплом-Ваш-шаг-к-новым-возможностям
socialnetwork.swazi-host.com/blogs/15612/Что-потребуется-из-оборудования-для-создания-диплома
בילוי עם נערות ליווי מתאים לכל רגע בחיים. יש את הרגעים שאנו מרגישים קצת למטה, הרגעים שבהם אנו קצת עצובים ולא יודעים מה לעשות עם הרבה מאוד מה להציע. מדובר בנערות היפות ביותר בתל אביב, רבות מהן תיירות שהגיעו לעבוד כאן. בילוי עם נערות ליווי בתל אביב הוא this post
Привет!
Заказать документ о получении высшего образования можно у нас. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить диплом по любым специальностям, любого года выпуска, включая документы СССР. Гарантируем, что при проверке документа работодателями, подозрений не возникнет.
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий по приятным ценам. Стоимость зависит от определенной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику цен. Важно, чтобы дипломы были доступными для подавляющей массы граждан.
azat.on.kg/blogs/1029/Заказываем-документы-в-лучшем-онлайн-магазине-по-выгодной-стоимости/
Будем рады вам помочь!
Добрый день!
Приобрести диплом любого университета.
sonnick84.blogstival.com/50704383/С-умом-приобретаем-документы-в-сети-экспертный-обзор
indicouple.com/blogs/1106/Вы-хотите-купить-аттестат-у-надежного-исполнителя-Ждем-Вас
forum.jeep-club.by/index.php?/blog/4/entry-3108-почему-намного-проще-будет-купить-диплом-униве/
sm2services.xyz/read-blog/546
network-6342899.mn.co/posts/61679275
The scoring system in the Aviator Game is based on the multiplier at the time of cashing out. The higher the
cost of ivermectin
Привет!
Заказать документ о получении высшего образования можно в нашем сервисе. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любым специальностям, любого года выпуска, включая документы Советского Союза. Гарантируем, что в случае проверки документа работодателем, никаких подозрений не возникнет.
sonnick84.bloguetechno.com/Советы-специалиста-что-помогут-быстро-купить-диплом-63719658
ackeer.com/read-blog/486
delta72.at.ua/forum/61-26755-1
r6o4lv53w.bleepblogs.com/28768656/Хотите-узнать-как-заказать-диплом-в-сети-недорого-Заходите
http://www.shopwheel.ru/club/user/49/blog/54943/
Привет!
Приобрести диплом университета.
a90275db.beget.tech/2024/07/04/kak-podobrat-proverennyy-magazin-s-ogromnym-katalogom-diplomov.html
[u][b] Здравствуйте![/b][/u]
[b]Купить диплом любого университета.[/b]
[url=http://forum.enchald.com/files/file/10-%D0%BA%D0%B0%D0%BA%D0%B8%D0%B5-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D1%8B-%D1%81-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%B0%D0%BC%D0%B8-%D0%B8%D0%BC%D0%B5%D1%8E%D1%82%D1%81%D1%8F-%D0%BD%D0%B0-%D1%82%D0%B5%D0%BA%D1%83%D1%89%D0%B8%D0%B9-%D0%BC%D0%BE%D0%BC%D0%B5%D0%BD%D1%82//]forum.enchald.com/files/file/10-%D0%BA%D0%B0%D0%BA%D0%B8%D0%B5-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD%D1%8B-%D1%81-%D0%B4%D0%BE%D0%BA%D1%83%D0%BC%D0%B5%D0%BD%D1%82%D0%B0%D0%BC%D0%B8-%D0%B8%D0%BC%D0%B5%D1%8E%D1%82%D1%81%D1%8F-%D0%BD%D0%B0-%D1%82%D0%B5%D0%BA%D1%83%D1%89%D0%B8%D0%B9-%D0%BC%D0%BE%D0%BC%D0%B5%D0%BD%D1%82/[/url]
Здравствуйте!
Заказать диплом любого ВУЗа.
app-s.ru/blog/kak_podyskat_nadezhnyj_magazin_s_ogromnym_katalogom_diplomov/2024-07-04-1868
Добрый день!
Получить диплом о высшем образовании
jivonews.ru/diplomyi-vseh-spetsialnostey-po-dostupnyim-tsenam
rrsclub.ru/member.php?u=1164
toursoul.ru/?p=19237
u90517ol.beget.tech/2024/07/18/diplomy-lyuboy-slozhnosti-v-kratchayshie-sroki.html
fabnews.ru/forum/showthread.php?p=80204#post80204
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным тарифам. Цена будет зависеть от выбранной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Для нас очень важно, чтобы документы были доступны для большого количества наших граждан.
judahmu742.ja-blog.com/27119515/Дипломы-за-деньги-Правда-о-Покупке-Образования-купить-диплом
Здравствуйте!
Купить документ о получении высшего образования можно у нас.
diplomyx24.ru/kupit-diplom-voronezh
Успехов в учебе!
Привет, друзья!
Мы предлагаем дипломы любой профессии по приятным ценам.
xrated.social/blogs/145/Желаете-купить-диплом-Заходите-в-наш-интернет-магазин
yur-dom.ru/communication/forum/messages/forum3/message252/295-bystryy-vybor-onlayn_magazina_-prodayushchego-diplomy?result=new
network-91053.mn.co/posts/61837969
gemawiraclub.com/blogs/39814/Отличный-онлайн-магазин-с-очень-выгодными-по-цене-документами
beijingpal.com/read-blog/816
Здравствуйте!
Приобрести документ института вы имеете возможность у нас. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации.
ноутбук-ремонт.рф/forum/viewtopic.php?t=3308
опт-кирпич.рф/index.php?subaction=userinfo&user=ubitaxos
http://www.luisovalles.com/new/index.php?option=com_k2&view=itemlist&task=user&id=99878
wiki.hightgames.ru/index.php?title=landsdiplomy
water.vouvstudio.com/bbs/board.php?bo_table=free&wr_id=2886740
Привет!
Купить диплом любого университета.
bondhusova.com/blogs/60411/Грамотно-приобретаем-диплом-в-сети-интернет-авторский-обзор
erkibbutz.com/read-blog/436
indicouple.com/blogs/1119/Ценные-советы-по-приобретению-документов-в-сети
sonnick84.anchor-blog.com/8486898/Дипломы-по-выгодным-расценкам-в-лучшем-интернет-магазине
sonnick84.arwebo.com/51331883/Как-выбрать-проверенный-интернет-магазин-что-реализует-дипломы
Здравствуйте!
Заказать документ университета.
robotaforum.2bb.ru/viewtopic.php?id=12555#p45578
medik-look.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
автомедведь.рф/club/log/?SECTION_CODE=log
net4women.ru/blogs/3938/Идеальный-диплом-за-считанные-дни-узнайте-подробности
shoptema.ru/forum/topic/32712/
Привет!
Как правильно купить диплом колледжа и пту в России, подводные камни
thecareerer.com/wordpress/2024/06/30/купить-диплом-продавца-2/
Привет, друзья!
Заказать документ университета
fulldropshipping.com/index.php?/events/event/8-почему-сегодня-куда-проще-будет-приобрести-диплом-университета/
telegra.ph/Zakazyvaem-diplom-v-luchshem-onlajn-magazine-po-vygodnoj-stoimosti-07-09
sonnick84.bligblogging.com/28774409/Рекомендации-специалиста-которые-помогут-недорого-купить-документы
forum.twilightmu.com/album.php?albumid=247&pictureid=1653
rkiyosaki.ru/discussion/9702/legkiy-vybor-onlayn-magazina-kotoryy-prodaet-diplomy/
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании.
ast-diploms.com/kupit-diplom-omsk
Хорошей учебы!
Добрый день!
Заказать документ ВУЗа можно в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, включая документы старого образца. Даем гарантию, что в случае проверки документов работодателем, каких-либо подозрений не возникнет.
Мы можем предложить дипломы психологов, юристов, экономистов и других профессий по приятным ценам. Стоимость будет зависеть от той или иной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Для нас важно, чтобы дипломы были доступны для большого количества граждан.
edenhazardclub.com/read-blog/3589_rasshirennoe-opisanie-priobreteniya-attestata-v-onlajn-magazine.html
Поможем вам всегда!
Интерьерная печать на самоклеющейся пленке – это процесс создания качественных полноцветных изображений на самоклеющейся пленке, которая может быть наклеена на различные поверхности интерьерная пленка печать
Чай трав’яний – це лікувальний напій, що виготовляють з різних лікарських рослин. Настій може бути корисним для самопочуття, оскільки включає багато вітамінів.
Трав’яні чаї можна купити в магазині AD-UA українському магазині. AD-UA має в асортименті різноманітні види трав’яного чаю на будь-який бажання.
Для замовлення – https://ad-ua.com/chaj/trav-yanyj-chaj/
בחיפה הן מקום שבו אפשר למצוא יפיפיות אמיתיות, בעלות גוף סקסי ומחוטב. הן מגיעות לכאן מכל העולם, והן שמחות להכיר גברים ישראלים ללמוד דברים חדשים, או אולי להפתיע אותן בדברים חדשים ונועזים, זוהי ההזדמנות שלך. לא בכל יום פוגשים בחורות כל כך יפות שפשוט דירות סקס באשקלון
Здравствуйте!
Заказать диплом университета.
score808.chat/blogs/5674/Главные-расходы-производителя-документов-специальный-обзор/
djjmeets.com/blogs/179064/Главные-расходы-российского-изготовителя-дипломов-авторский-обзор
gamerlaunch.com/community/users/blog/6443244/2286460/расходы-любого-/?gid=535/
thesocialgroup.co.uk/blogs/526/Стоимость-диплома-обзор-специалистов
flexartsocial.com/blogs/10031/Основные-расходы-изготовителя-дипломов-авторский-обзор/
Привет, друзья!
Купить документ о получении высшего образования.
niceroleplay.getbb.ru/viewtopic.php?f=1&t=1261
kherson.forum2x2.ru/t10915-topic#26334
drugisaitove.listbb.ru/posting.php?mode=post&f=2&sid=4ed2eac20174592bf939f4ac17b32460
wiki.nikiforov.ru/index.php/Ваш_диплом_под_ключ:_качественно_и_безопасно
liquidationrama.com/read-blog/1030
repairdesign24.com
chinaone.net
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий.
followgrown.com/read-blog/2580_ishem-nadezhnyj-magazin-s-attestatami-i-diplomami.html?mode=night
Окажем помощь!.
Привет!
Заказать документ института.
backshowtime.ru/kupit-diplom-byistro-i-nadezhno
bence.net/read-blog/81
rakisochi.ru/users/20
backshowtime.ru/oformlenie-diploma-bez-problem-i-zabot
nsk.ukrbb.net/viewtopic.php?f=41&t=27445
Привет, друзья!
Мы готовы предложить документы техникумов
u90517ol.beget.tech/2024/07/18/kupite-diplom-i-nachnite-novuyu-zhizn.html
p99946c6.beget.tech/2024/07/18/diplomy-s-dostavkoy-na-dom.html
productinn.mn.co/posts/62527936
bisound.com/forum/showthread.php?p=800121#post800121
akademe.mn.co/posts/62657179
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий по невысоким ценам. Стоимость зависит от определенной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику цен. Для нас важно, чтобы документы были доступными для большого количества граждан.
dantej9y37.blogspothub.com/26787938/Покупка-диплома-Риски-и-Последствия-купить-диплом
[Casino Name], each offering unique bonuses and promotions for Aviator Game players.
ivermectin buy
Добрый день!
Диплом о высшем образовании
allukrnews.ru/nadezhnyie-diplomyi-dlya-vashey-kareryi/
forum.mybb.ru/viewtopic.php?id=38567#p939931
testforum.1stbb.ru/viewtopic.php?f=3&t=444
lapd.getbb.ru/viewtopic.php?f=5&t=454
d91652pj.beget.tech/2024/07/18/diplomy-s-garantiey-kachestva-i-nadezhnosti.html
Добрый день!
Мы можем предложить дипломы любой профессии по разумным ценам.
cr-v.su/forums/index.php?autocom=gallery&req=si&img=3236
berforum.ru/gallery/image/8678-zakazyvaem-diplom-v-izvestnom-onlayn-magazine-po-vygodnoy-stoimosti/?context=new
xleks.ru/2024/07/09/nizkie-rascenki-i-prekrasnoe-kachestvo-zakazyvay-diplomy-onlayn.html
socialnetwork.swazi-host.com/blogs/15612/Что-потребуется-из-оборудования-для-создания-диплома
wiki.why42.ru/wiki/Приобретаем_диплом_в_известном_интернет-магазине_по_комфортной_цене
Привет, друзья!
Купить документ о получении высшего образования
sonnick84.topbloghub.com/34467436/Что-потребуется-из-техники-для-производства-диплома
9pj7tneu1.blogoxo.com/28388931/Подробное-описание-покупки-документов-в-знаменитом-онлайн-магазине
mimedia.in/read-blog/49538
ayema.ng/blogs/33044/Ключевые-расходы-производителя-документов-авторский-обзор
wiki.roximo.ru/index.php/Легкий_выбор_онлайн-магазина,_реализующего_дипломы
Привет!
Заказать диплом университета
wo.linyway.com/read-blog/4491
teplichnaya.ru/viewtopic.php?f=18&t=643289
forum54.4adm.ru/search.php?search_id=egosearch
dexanet.ukrbb.net/viewtopic.php?f=5&t=16513
wh0.in/create-blog/
Здравствуйте!
Заказать документ о получении высшего образования можно в нашем сервисе. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации. Вы получите необходимый диплом по любой специальности, включая документы Советского Союза. Гарантируем, что в случае проверки документа работодателем, подозрений не возникнет.
Мы изготавливаем дипломы любых профессий по приятным тарифам. Цена может зависеть от конкретной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для покупателей адекватную политику цен. Важно, чтобы документы были доступны для большого количества наших граждан.
nybodyart.com/forums/gallery/image/8-приобретаем-диплом-в-известном-онлайн-магазине-по-выгодной-цене/
Поможем вам всегда!
Добрый день!
Мы готовы предложить документы техникумов
forum-pravo.com.ua/member.php?u=10249
rossensor.ru/forum/?PAGE_NAME=profile_view&UID=43545
forexrassia.ru/legalno-i-byistro-oformite-diplom-onlayn
motmarket.ru/forum/user/25241/
raiter.flyboard.ru/viewtopic.php?f=3&t=2401
Добрый день!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
animesocial.su/blogs/2461/Купите-Диплом-для-Вашего-Успеха
Привет!
Приобрести диплом о высшем образовании.
sonnick84.blogrelation.com/34203953/Хотите-приобрести-диплом-Выбирайте-наш-магазин
sonnick84.blogunok.com/28429798/Как-выбрать-проверенный-интернет-магазин-реализующий-документы
fromrus.su/index.php?/gallery/image/324-почему-сегодня-куда-проще-и-дешевле-купить-диплом-университета/
letterboxd.com/sonnick84/list/filmlist:48641266/
foroeuropeo.it/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=282
Привет!
Заказать документ о получении высшего образования
ourfathersfamily.com/blogs/2384/Вы-хотите-приобрести-диплом-Выбирайте-наш-интернет-магазин
itstagram.ru/read-blog/389
santa4.su/gallery/image/253-dlya-chego-segodnya-pokupayut-attestaty-i-diplomy-v-seti-internet/
sonnick84.glifeblog.com/27690341/Проверенный-онлайн-магазин-с-обширным-ассортиментом-дипломов
sonnick84.luwebs.com/28777810/Дипломы-по-низким-расценкам-в-известном-магазине
Здравствуйте!
Заказать диплом о высшем образовании.
wiki.why42.ru/wiki/Широкий_ассортимент_документов_в_популярном_онлайн_магазине
Добрый день!
Реально ли приобрести диплом стоматолога? Основные этапы
remotebillpay.com/купить-диплом-о-высшем-образовании-ре/
Рады оказаться полезными!.
Здравствуйте!
Заказать диплом любого ВУЗа.
newfinbiz.ru/page/3
imf1fan.com/community/profile/leopoldobeh2135/
forosmex.com/index.php?/gallery/image/546-быстрый-выбор-интернет-магазина-что-продает-дипломы-и-аттестаты/
ccde-cambodia.com/cb-profile/pluginclass/cbblogs.html?action=blogs&func=show&id=123/
designlight.co.kr/g5/bbs/board.php?bo_table=ieahqtqy2g&wr_id=2271
Привет, друзья!
Мы готовы предложить дипломы любой профессии по приятным ценам.
http://www.irc71.ru/index.php/jomsocial/groups/viewbulletin/260-4-klyuchevykh-gruppy-onlajn-magazinov-chto-prodayut-diplomy?groupid=47
On the website https://intracorp.com.sg/ you will be able to use all the services offered by Intracorp. In Singapore, you can start your own business and live in a big way. This state is the center of commerce, as well as finance, and therefore whatever business you open, it will definitely bear fruit. The team that works in this company is as customer-oriented as possible. She is distinguished by her deep knowledge and understanding of all the nuances. At the same time, the transaction will be accompanied at every stage.
Здравствуйте!
Приобрести документ о получении высшего образования
diploms-x.com/kupit-diplom-vracha
Привет!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
http://www.jorditoldra.com/купить-диплом-новосибирск/
Привет, друзья!
Приобрести документ о получении высшего образования
o91707v5.beget.tech/2024/07/09/pokupaem-dokumenty-v-luchshem-onlayn-magazine-po-vygodnoy-cene.html
cdposz.ru/club/user/802/forum/message/1496/1555/
wakelet.com/wake/s9aPv6AP4s8UgrtvWFWKT
loozx.com/read-blog/381
ebonyfaces.com/blogs/31/Выбираем-проверенный-интернет-магазин-с-аттестатами-и-дипломами
Наши специалисты предлагает высококачественный сервисный ремонт парогенератора в москве всех типов и брендов. Мы осознаем, насколько значимы для вас ваши пароочистители, и стремимся предоставить услуги первоклассного уровня. Наши опытные мастера работают быстро и аккуратно, используя только сертифицированные компоненты, что предоставляет надежность и долговечность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются владельцы парогенераторов, включают проблемы с нагревом, неработающий насос, программные сбои, проблемы с подключением и поломки компонентов. Для устранения этих неисправностей наши квалифицированные специалисты оказывают ремонт нагревательных элементов, насосов, ПО, разъемов и механических компонентов. Обратившись к нам, вы гарантируете себе надежный и долговечный починить парогенератор.
Подробная информация доступна на сайте: https://remont-parogeneratorov-piece.ru
Здравствуйте!
Заказать документ университета вы можете у нас в столице.
ast-diploms.com/kupit-diplom-chelyabinsk
Здравствуйте!
Как правильно купить диплом колледжа и пту в России, подводные камни
arusak-diploms-srednee.ru/kupit-attestat-za-11-klass В
Добрый день!
Мы можем предложить дипломы любой профессии по невысоким тарифам.
wildlifediaries.com/купить-диплом-новосибирск/
Добрый день!
Мы изготавливаем дипломы любой профессии по доступным тарифам. Цена может зависеть от выбранной специальности, года получения и университета. Всегда стараемся поддерживать для клиентов адекватную политику цен. Важно, чтобы дипломы были доступными для большого количества наших граждан.
johnnydxoe20986.celticwiki.com/665295/Направления_заказа_документов_об_образовании_в_современном_обществе
Добрый день!
Мы изготавливаем дипломы любой профессии.
irc71.ru/index.php/jomsocial/groups/viewbulletin/256-zachem-sejchas-priobretayut-diplomy-v-seti-internet?groupid=47
Окажем помощь!.
Привет!
Заказать документ ВУЗа можно в нашей компании.
diplomyx.com/kupit-diplom-vracha
Хорошей учебы!
Привет, друзья!
Купить диплом ВУЗа
vintfint.com/blogs/22679/Ваш-диплом-без-лишних-забот-быстро-и-безопасно
exoltech.us/blogs/207844/Официальный-диплом-без-учебы-и-экзаменов
feelosum.com/blogs/1726/Решили-выяснить-как-купить-документы-в-сети-Ждем-Вас
overfun.ru/index.php?/gallery/image/335-почему-магазины-с-документами-сегодня-так-востребованы-и-популярны/
breyerhorses.ru/personal/profile/?register=yes
Узнайте, как безопасно купить диплом о высшем образовании
carolinahurricanesclub.com/read-blog/597
socialmoby.com/read-blog/393
fforum.ixbb.ru/viewtopic.php?id=191#p4069
hjqew6ejm.getblogs.net/60736792/Изучите-наш-обзор-в-случае-если-нужно-купить-диплом-в-сети-интернет
cubarebota.info/blogs/169/Решили-узнать-как-купить-документы-в-сети-недорого-Заходите
Привет!
Приобрести документ о получении высшего образования можно у нас в Москве.
ast-diplom.com/kupit-diplom-specialista
Привет!
Заказать документ о получении высшего образования.
t98223u0.beget.tech/2024/07/16/legalnyy-diplom-bez-lishnih-hlopot-uznayte-kak.html
forumkk.listbb.ru/viewtopic.php?f=12&t=440
art-gymnastics.ru/users/54
git.fuwafuwa.moe/thomasshaw9688/My-List/issues/new
paulikipedia.ru/index.php/Настоящие_дипломы_за_короткий_срок
Здравствуйте!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
network-21596.mn.co/posts/61724406
amcall.net/read-blog/376
wish-club.ru/forums/index.php?autocom=gallery&req=si&img=3874
sonnick84.liberty-blog.com/28340348/Ищем-проверенный-и-надежный-магазин-для-приобретения-диплома
ozoms.com/read-blog/464
Здравствуйте!
Быстрая схема покупки диплома старого образца: что важно знать?
softerioninc.com/купить-диплом-в-киселевске/
Добрый день!
Купить диплом о высшем образовании.
sonnick84.wizzardsblog.com/28265557/%D0%9D%D0%B0-%D1%87%D1%82%D0%BE-%D0%BA%D0%BE%D0%BD%D0%BA%D1%80%D0%B5%D1%82%D0%BD%D0%BE-%D0%B2%D0%BD%D0%B8%D0%BC%D0%B0%D0%BD%D0%B8%D0%B5-%D0%BE%D0%B1%D1%80%D0%B0%D1%82%D0%B8%D1%82%D1%8C-%D0%BF%D1%80%D0%B8-%D0%BF%D0%BE%D0%BA%D1%83%D0%BF%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%B0-%D0%B2-%D0%B8%D0%BD%D1%82%D0%B5%D1%80%D0%BD%D0%B5%D1%82%D0%B5
искусство брендинга
профессиональные советы
Добрый день!
Как официально купить диплом вуза с упрощенным обучением в Москве
wk82.xyz/home.php?mod=space&uid=63030
Окажем помощь!.
Привет, друзья!
Купить документ о получении высшего образования можно в нашей компании в Москве.
diplomasx.com/kupit-diplom-kandidata-nauk
Привет, друзья!
Купить документ института можно у нас в Москве.
asxdiplomik.com/kupit-diplom-vracha
Успешной учебы!
Online casino games have surged in popularity due to their convenience and the immersive experience they offer.
ivermectin buy
Добрый день!
Заказать диплом университета.
hobby-svarka.ru/topic6208.html
worldaid.eu.org/discussion/profile.php?id=5130
omaada.com/blogs/120792/Получите-диплом-без-лишних-забот-и-усилий
nitrnd.com/blogs/159135/Стоимость-документов-советы-и-авторский-обзор-экспертов
victorians123.com/blogs/210/Что-именно-нужно-для-создания-качественного-документа?lang=it_it
Сколько можно проигрывать? Пора выбирать реальные казино! Telegram канал лучшие казино с лицензией и бонусами представляет лучшие онлайн казино для игры на деньги. Эти платформы предлагают щедрые бонусы на первый депозит и разнообразие игровых автоматов, а также быстрый вывод средств на карты Сбербанка, ВТБ и Т-банка.
Ежедневные обновления гарантируют честные и проверенные казино. Подписывайтесь на канал и играйте в казино, где реально выиграть деньги. Оставьте неудачи позади и начните свой путь к большим выигрышам!
Добрый день!
Легальные способы покупки диплома о среднем полном образовании
http://www.inlabs.la/купить-диплом-сертификат/
Добрый день!
Приобрести документ института можно в нашем сервисе.
diplomyx.com/kupit-diplom-sankt-peterburg
Успешной учебы!
seo service
https://sites.google.com/view/backlinks-seo-sell/seo-service
Добрый день!
Мы можем предложить дипломы любой профессии по приятным ценам.
gamemotors.ru/diplomyi-s-polnyim-paketom-dokumentov-2
Привет!
Приобрести диплом университета
kaiztech.net/IPB/index.php?/gallery/image/427-высокая-популярность-магазинов-что-продают-дипломы/
fotomaniya.getbb.ru/viewtopic.php?f=16&t=11192
bideew.com/read-blog/7082
xiudda2iz.blogsumer.com/27945098/Вы-хотите-выяснить-как-заказать-диплом-в-сети-недорого-Ждем-Вас
konstruktiv.getbb.ru/viewtopic.php?f=17&t=6714
Привет, друзья!
Мы предлагаем документы техникумов
paning.flybb.ru/viewtopic.php?f=7&t=1246
robotaforum.2bb.ru/post.php?fid=40
lubov.listbb.ru/viewtopic.php?f=2&t=494
forumkk.listbb.ru/viewtopic.php?f=12&t=452
eurodelo.ru/ekspress-dostavka-diplomov-na-dom
Быстрое обучение и получение диплома магистра – возможно ли это?
nachosking.com/read-blog/915
socialxtendr.com/blogs/175/Читайте-наш-обзор-в-случае-если-надо-заказать-диплом-в
fnyc0efcf.dsiblogger.com/61089279/Изучите-наш-обзор-если-надо-купить-диплом-в-интернете
xtreme-motors.ru/forum/user/22060/
ohoanshrf.thelateblog.com/28773648/Вы-хотите-выяснить-как-купить-диплом-в-сети-интернет-Ждем-Вас
Привет, друзья!
Мы изготавливаем дипломы любых профессий.
sommos.com.co/купить-диплом-модельера/
Рады помочь!.
Привет, друзья!
Заказать диплом университета.
kotanusantara.cloud/index.php?/events/event/8-как-найти-надежный-онлайн-магазин-с-обширным-выбором-дипломов/
Привет!
Купить диплом ВУЗа
Наша компания предлагает быстро и выгодно заказать диплом, который выполняется на оригинальном бланке и заверен мокрыми печатями, водяными знаками, подписями официальных лиц. Диплом способен пройти лубую проверку, даже при помощи профессионального оборудования. Достигайте своих целей быстро с нашей компанией.
Где приобрести диплом специалиста?
l6mvnrmz3.blogginaway.com/28825436/Вы-хотите-узнать-как-заказать-диплом-в-сети-недорого-Ждем-Вас
d91652pj.beget.tech/2024/07/08/nastoyaschie-diplomy-legalno-i-dostupno.html
medik-look.ru/vash-put-k-vyisshemu-obrazovaniyu-byistro-i-legalno
http://www.traveltravelforum.com/showthread.php/32859-Купить-диплом-Ваш-путь-к-успеху?p=67847#post67847
mykinotime.ru/ofitsialnyie-diplomyi-legko-i-dostupno/
стратегии маркетинга
предприниматель
Привет, друзья!
Купить документ о получении высшего образования можно в нашей компании в Москве.
asxdiplomik.com/kupit-diplom-sankt-peterburg
Хорошей учебы!
Привет!
Заказать документ о получении высшего образования вы имеете возможность в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы сможете получить диплом по любой специальности, включая документы образца СССР. Гарантируем, что при проверке документов работодателями, никаких подозрений не возникнет.
http://www.forum.7x.ru/member.php?u=16498
followmylive.com/read-blog/969
ekocom.ru/forum/?PAGE_NAME=profile_view&UID=13033
vip.rolevaya.info/viewtopic.php?id=4952#p8469
keterclub.com/read-blog/9239
Привет, друзья!
Купить диплом университета.
b98385gb.beget.tech/2024/07/04/kak-podobrat-nadezhnyy-onlayn-magazin-s-shirokim-katalogom-diplomov.html
Привет, друзья!
Заказать диплом о высшем образовании.
toolsrepair.ru/forum/viewtopic.php?f=5&t=2933302
Здравствуйте!
Приобрести диплом ВУЗа:
o926476g.bget.ru/users/etuvyzopi
forums.indexrise.com/thread-2362-post-222897.html#pid222897
kvartirker.ru/profile/elusyzy/
rostovbike.ru/thread-10941.html
forum.kia-club.ru/viewtopic.php?f=372&t=103462
Привет, друзья!
Где и как купить диплом о высшем образовании без лишних рисков
mipropuestadenegocio.com/category/uncategorized/page/3/
Будем рады вам помочь!.
In today’s world, caring for health and proper nutrition is becoming a priority for many people dominicandesign.net
commercial real estate license tn realestatelicensengdfdgh.com/states/texas-real-estate-license/ how to take real estate license realestatelicensengdfdgh.com/states/ohio-real-estate-license/ .
When hiring as a courier, it is additionally necessary to determine the driver’s license holidaynewsletters.com
Интерьерная печать на самоклеющейся пленке – это процесс создания качественных полноцветных изображений на самоклеющейся пленке, которая может быть наклеена на различные поверхности интерьерная печать 24 часа
Здравствуйте!
Заказать документ института.
elfae.ruhelp.com/viewtopic.php?id=17230#p39487
ledsoft.ru/forum/?PAGE_NAME=message&FID=3&TID=14026&TITLE_SEO=14026-_-_-_-_-_-_-_&MID=14833&result=new#message14833
teplichnaya.ru/viewtopic.php?f=18&t=640591
wiki.mysupp.ru/index.php?title=Легальный_диплом_без_лишних_хлопот:_узнайте_как!
ilovehabbo.bbon.ru/viewtopic.php?id=1564#p28982
השבוע או אמצע השבוע, תמיד יש כאן נערות חרמניות שרוצות לארח גברים ולבלות יחדיו. אז אם זה מה שהחיים נותנים לך, למה לא ליהנות דירות דיסקרטיות בתל אביב לבילוי מטריף חושים רווקים שרוצים לבלות עם נערות מטריפות, נשואים שצריכים קצת גיוון או אנשי עסקים נערת ליווי זולה או עדיף לצאת לדייט?
Привет, друзья!
Купить документ института
forum.zentox-rp.ru/index.php?app=gallery&module=gallery&controller=view&id=9
socialnetwork.cloudyzx.com/read-blog/11234
saluttunisia.com/jomsocial/groups/viewbulletin/272-faq-i-tekhnicheskaya-podderzhka-pokupaem-dokumenty-v-seti.html?groupid=101
gamefilm.ru/index.php?/gallery/image/119-тех-поддержка-и-faq-заказываем-диплом-в-сети/
kaiztech.net/IPB/index.php?/gallery/image/421-вы-хотите-приобрести-диплом-выбирайте-наш-магазин/
Здравствуйте!
Купить диплом университета
fish-sea-products.ru/forum/user/5829/
ntnn.ru/personal/profile/index.php?register=yes
stylist-profi.ru/forum/user/200286/
oren.kabb.ru/viewtopic.php?f=50&t=34012
income.forum2x2.ru/t2972-topic#5292
Как безопасно купить диплом колледжа или ПТУ в России, что важно знать
conectta2.com/read-blog/915
mkpnz.ru/users/8
pitomec.ru/forum/post/13042
antonovschool.ru/forum/messages/forum1/topic704/message723/?result=new#message723
derivsocial.org/read-blog/2583
Добрый день!
Где приобрести диплом специалиста?
http://www.eSurveysPro.com/Survey.aspx?id=19d83309-26ea-40b3-adbc-dbe80bd1adf3
Здравствуйте!
Мы готовы предложить документы техникумов
wiki.nikiforov.ru/index.php/Купите_диплом_и_начните_новую_жизнь
goruss.ru/blogs/1111/Быстрый-и-надежный-способ-получить-диплом
forexrassia.ru/legalno-poluchite-diplom-za-korotkiy-srok
batirafrica.blog4ever.com/forum/arts-cultures/sujet-46
deanonnic.listbb.ru/viewtopic.php?f=5&t=475
Здравствуйте!
Заказать документ университета.
modern-constructions.org/blogs/65254/Диплом-под-ключ-просто-и-надежно
vocal.com.ua/node/62457
dimitrii.flybb.ru/viewtopic.php?f=29&t=949
jagplay.ekafe.ru/viewtopic.php?f=22&t=4158
school8kaluga.flybb.ru/viewtopic.php?f=19&t=500
Привет, друзья!
Приобрести диплом любого ВУЗа.
g95334gq.beget.tech/2024/07/07/kakie-onlayn-magaziny-s-dokumentami-na-segodnyashniy-den-suschestvuyut.html
Добрый день!
Купить документ о получении высшего образования
godsoftheuniverse.mn.co/posts/61838384
encontrocentral.com/read-blog/2287
sonnick84.blogstival.com/50719489/Советы-профессионала-которые-помогут-быстро-заказать-диплом
liobio.com/blogs/1588/Рекомендации-по-приобретению-документа-в-сети-интернет
newcoop.ru/company/personal/user/816/blog/556/
Pattern Analysis: Studying the game’s patterns and trends to predict optimal cash-out times.
ivermectin where to buy
[u][b] Добрый день![/b][/u]
Мы предлагаем документы ВУЗов
[url=http://koxma.4adm.ru/viewforum.php?f=296/]koxma.4adm.ru/viewforum.php?f=296[/url]
[url=http://hashtap.com/@artur.sh/получите-диплом-и-начните-новую-жизнь-aJpkv3VdmGlA/]hashtap.com/@artur.sh/получите-диплом-и-начните-новую-жизнь-aJpkv3VdmGlA[/url]
[url=http://gerosland.com/read-blog/192/]gerosland.com/read-blog/192[/url]
[url=http://baxoday.maxbb.ru/viewtopic.php?f=25&t=526/]baxoday.maxbb.ru/viewtopic.php?f=25&t=526[/url]
[url=http://mdr7.ru/viewtopic.php?f=6&t=8966/]mdr7.ru/viewtopic.php?f=6&t=8966[/url]
Добрый день!
Мы можем предложить дипломы любой профессии по выгодным ценам.
learn4fun.vn/купить-диплом-игитм-или-любого-вуза-ро/
Онлайн-платформа для азартных игр представляет собой разнообразный мир развлечений. Здесь игроки могут наслаждаться множеством опций, которые сделают времяпрепровождение увлекательным и захватывающим https://xn--80asucf0d.xn--j1al4b.xn--p1ai/index.php/component/k2/itemlist/user/127772
great site uniteto org
internet https://casinomira.com/casinos-rating/
Привет, друзья!
Купить документ о получении высшего образования
avtolux48.ru/people/user/367/blog/7858/
sonnick84.blogofchange.com/28698968/Надежный-онлайн-магазин-с-обширным-ассортиментом-документов
xrated.social/blogs/147/Советы-специалиста-что-возможность-дадут-быстро-заказать-диплом
newsbig.trexgame.net/diplomy-attestaty-a-krome-etogo-svidetelstva-nizkie-ceny
forosmex.com/index.php?/gallery/image/543-4-е-ключевых-группы-интернет-магазинов-что-реализуют-документы/
Привет, друзья!
Приобрести диплом любого ВУЗа:
receptom.ru/index.php?subaction=userinfo&user=ytepe
shkola.mitrofanovka.ru/index.php?subaction=userinfo&user=apinik
aben75.cafe24.com/bbs/board.php?bo_table=free&wr_id=376094
d.mwoff.org/index.php?/topic/43-купить-диплом-техникума-r732t/
magadan-mebel.ru/forum/user/922/
Заказать диплом университета.
bintarotrojan.com/blogs/9235/ упить-Ќасто€щий-?иплом-ѕростое-–ешение
чпуремонт.рф/showthread.php?tid=52677
pesnibardov.ru/f/viewtopic.php?f=2&t=203805
khvoynaya.getbb.ru/viewtopic.php?f=39&t=6859
abroad.ekafe.ru/viewtopic.php?f=5&t=1942
Здравствуйте!
Заказать документ о получении высшего образования можно в нашей компании.
ast-diplomy.com/kupit-diplom-specialista
Зайдите на сайт BinTradeClub https://bintradeclub.space/ – надежного брокера бинарных опционов, который, если у вас нет опыта, начать торговлю и даст знания, в ом числе демо счет. А если вы опытный трейдер – предоставит все необходимые инструменты для выгодной торговли. Подробнее на сайте.
Здравствуйте!
Мы готовы предложить дипломы любой профессии по доступным тарифам.
tuvanmedia.com/blog/2024/06/30/диплом-техникума-колледжа-2004-2006-фото/
Привет!
Мы можем предложить документы ВУЗов
ulmo.ukrbb.net/index.php
lighttur.ru/vyisokokachestvennyie-diplomyi-po-dostupnoy-tsene
sovavtoprom.ru/wiki/index.php/Экспресс-доставка_дипломов_по_всей_стране
1776reloaded.us/blogs/172/Быстрое-получение-диплома-онлайн
rkiyosaki.ru/discussion/9814/dostupnye-diplomy-vseh-urovney/
Как выбрать таможенного брокера: ключевые критерии
Выбор надежного таможенного брокера играет важную роль в успешной и эффективной логистике. Этот профессионал поможет вам правильно провести таможенное оформление грузов, что существенно сэкономит ваше время и деньги. Рассмотрим ключевые факторы, которые следует учитывать при выборе таможенного брокера.
Опыт и репутация — Один из главных критериев при выборе таможенного брокера. Обратите внимание на отзывы и рейтинги компаний. Проверьте, сколько лет компания работает на рынке и какие у нее есть достижения.
Квалификация сотрудников — Важен опыт и квалификация специалистов, работающих в компании. Хороший таможенный брокер должен иметь опыт работы с различными видами грузов и знание актуальных законодательных норм.
Обширная сеть контактов — Наличие хороших связей с таможенными органами и другими участниками внешнеэкономической деятельности (ВЭД) помогает ускорить процесс растаможки и избежать потенциальных проблем.
Услуги и тарифы — Важно ознакомиться с перечнем предоставляемых услуг и их стоимостью. Некоторые компании предлагают полный комплекс услуг, включая таможенное оформление грузов, что может быть удобным и выгодным.
Технологическое оснащение — Наличие современных технологий для автоматизации процессов таможенной очистки и управления документами помогает снизить вероятность ошибок и ускорить процесс.
Оцените эти аспекты при выборе таможенного брокера, чтобы обеспечить эффективное и бесперебойное выполнение всех таможенных процедур.
Добрый день!
Купить диплом любого ВУЗа.
forum.shevrondeath.club/files/file/20-большой-каталог-документов-в-знаменитом-интернет-магазине/
Играйте в увлекательные онлайн автоматы на сайте casino pinco и наслаждайтесь азартом прямо из дома!
Добрый день!
Заказать документ университета вы можете в нашей компании в столице.
ast-diploms.com/kupit-diplom-tehnikuma-kolledzha
ומהבחינה הזו, כאן הדיסקרטיות מובטחת. הנאה אין סופית בדירות דיסקרטיות בבאר שבע אז אם החלטת שאתה רוצה ליהנות ממה שיש לכם האלו לשכוח מכל הדאגות עם נערות ליווי בתל אביב אז מה לעשות באותם הרגעים בהם אתה מרגיש כי החיים לוחצים עלייך יותר מידי? מה לעשות כאשר בילוי מטריף עם נערת ליווי בהזמנה
Здравствуйте!
Купить диплом о высшем образовании.
network-1062788.mn.co/posts/61638827
wakelet.com/wake/s9aPv6AP4s8UgrtvWFWKT
onetable.world/read-blog/59911
ls.monetka.in.ua/2024/07/09/priobretaem-dokumenty-v-proverennom-magazine-po-vygodnoy-cene.html
foto-passau.com/gallery/image/8-документы-по-выгодным-ценам-в-известном-интернет-магазине/?context=new
Привет, друзья!
Мы изготавливаем дипломы.
itisenglish.maxbb.ru/viewtopic.php?f=7&t=1048
astroroleplay.getbb.ru/viewtopic.php?f=6&t=475
korrespondentweek.ru/kupit-diplom-bez-posrednikov-legko-i-byistro/
iqtorg.ru/forum/messages/forum2/topic625/message699/?result=new#message699
deanonnic.listbb.ru/viewtopic.php?f=5&t=447
Здравствуйте!
Купить документ университета вы имеете возможность у нас в столице.
ast-diplomy.com/kupit-diplom-krasnodar
Добрый день!
Где приобрести диплом специалиста?
swayycases.com/диплом-университета-купить-выгодные/
Здравствуйте!
Приобрести документ о получении высшего образования можно в нашей компании.
diplomyx.com/kupit-diplom-moskva
Хорошей учебы!
солдаты 5 сезон в хорошем качестве – актеры сериала солдаты, солдаты 8 сезон в хорошем качестве
сочи досуг и развлечения сегодня
Добрый день!
Заказать диплом о высшем образовании.
277469.simplecloud.ru/blogs/1/kak-podobrat-proverennyy-magazin-s-ogromnym-vyborom-diplomov.php
Привет, друзья!
Приобрести документ о получении высшего образования вы сможете у нас в Москве.
diplomyx.com/kupit-diplom-magistra
Успехов в учебе!
Привет!
Заказать документ о получении высшего образования
pakians.com/blogs/97593/Ценные-советы-по-приобретению-документов-в-интернете
naijarise.com/read-blog/46
cphiapps.com/blogs/13276/Ищем-проверенный-онлайн-магазин-для-приобретения-диплома
fishjines.mn.co/posts/61837908
naijarise.com/read-blog/46
Discover the thrilling world of https://sites.google.com/view/aviatorplay!
Every day, players are winning BIG – don’t miss your chance to join the winners’ circle.
Take off with https://sites.google.com/view/aviatorplay today and watch your fortunes take flight!
сочинский парк аттракционов цены
Купить диплом о высшем образовании.
ffxiv.one/blogs/146/Быстрое-Оформление-Дипломов-Надежно-и-Легально
ilovehabbo.bbon.ru/viewtopic.php?id=1549#p28965
realtyintellect.ru/nastoyashhie-diplomyi-dostupno-i-udobno
financetimenews.ru/diplomyi-na-zakaz-byistro-i-nadezhno/
medik-look.ru/kupit-diplom-doveryayte-professionalam
Добрый день!
Диплом юриста
1776reloaded.us/blogs/139/Оформите-диплом-за-пару-дней
coup.forum2x2.ru/t3809-topic#10062
bryansk32-forum.ru/ucp.php?mode=login
art-gsm.ru/forum/?PAGE_NAME=profile_view&UID=34895
animalprotect.org/forum/index.php?topic=239434.0
Добрый день!
Купить документ ВУЗа.
forumjustwoman.getbb.ru/viewtopic.php?f=43&t=1010
mirniy.flybb.ru/viewtopic.php?f=37&t=795
socialnetwork.cloudyzx.com/read-blog/14317
msfo-soft.ru/msfo/forum/messages/forum24/topic10450/message297769/?result=new#message297769
d91652pj.beget.tech/2024/07/12/oficialnye-diplomy-na-zakaz.html
Добрый день!
Заказать диплом о высшем образовании
13.flybb.ru/viewtopic.php?f=20&t=1075
1wum.ru/forum/?PAGE_NAME=profile_view&UID=40009&MUL_MODE=
sadcr.listbb.ru/viewtopic.php?f=53&t=399
a63.flybb.ru/viewtopic.php?f=16&t=3247
serialforfree.ru/diplom-o-vyisshem-obrazovanii-za-korotkiy-srok
Привет!
Заказать диплом о высшем образовании.
es-presto.ru/community/groups/0-0/176-ogromnyj-vybor-dokumentov-v-znamenitom-onlajn-magazine
Привет!
Купить документ о получении высшего образования вы имеете возможность в нашей компании в Москве.
asxdiplomik.com/kupit-diplom-rostov-na-donu
Хорошей учебы!
Наши специалисты предлагает надежный официальный ремонт планшета в москве различных марок и моделей. Мы знаем, насколько значимы для вас ваши устройства планшетного типа, и готовы предложить сервис наилучшего качества. Наши квалифицированные специалисты работают быстро и аккуратно, используя только оригинальные запчасти, что предоставляет надежность и долговечность проведенных ремонтов.
Наиболее частые неисправности, с которыми сталкиваются обладатели устройств планшетного типа, включают проблемы с экраном, проблемы с батареей, неисправности программного обеспечения, неработающие разъемы и механические повреждения. Для устранения этих проблем наши опытные мастера проводят ремонт экранов, батарей, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы обеспечиваете себе долговечный и надежный вызвать мастера по ремонту планшета рядом.
Подробная информация доступна на сайте: https://remont-planshetov-profi.ru
Добрый день!
Мы можем предложить дипломы любой профессии по выгодным ценам.
onetable.world/read-blog/59855
newsbig.timeforchangecounselling.com/dokumenty-po-vygodnym-rascenkam-v-popularnom-onlajn-magazine
rf-unicron.ru/index.php?/gallery/image/120-быстрый-выбор-магазина-который-реализует-дипломы/
sonnick84.oblogation.com/27876701/%D0%A5%D0%BE%D1%82%D0%B8%D1%82%D0%B5-%D0%B7%D0%B0%D0%BA%D0%B0%D0%B7%D0%B0%D1%82%D1%8C-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC-%D0%97%D0%B0%D1%85%D0%BE%D0%B4%D0%B8%D1%82%D0%B5-%D0%B2-%D0%BD%D0%B0%D1%88-%D0%BE%D0%BD%D0%BB%D0%B0%D0%B9%D0%BD-%D0%BC%D0%B0%D0%B3%D0%B0%D0%B7%D0%B8%D0%BD
fomazy.com/blogs/4777/Полезные-рекомендации-по-покупки-документов-в-сети-интернет
Привет, друзья!
Приобрести документ института можно у нас. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России.
mariland.org/index.php?subaction=userinfo&user=ataruk
nedv-revda.ru/index.php?subaction=userinfo&user=ylugil
gkwin.net/bbs/board.php?bo_table=free&wr_id=227120
ssd-astra.ru/forum/viewtopic.php?f=14&t=8080
b24activities.ru/club/forum/messages/forum4/topic76/message135/?result=reply#message135
Sur Shopsy, vous pouvez trouver et acheter des vetements, des chaussures et des accessoires. Plus de 2 000 000 de produits provenant de 100 magasins sur un seul site. https://shopsy.fr/ Dans notre catalogue, vous trouverez des articles de milliers de marques originales.
Здравствуйте!
Мы предлагаем дипломы психологов, юристов, экономистов и других профессий по выгодным ценам.
club.sabaylok.com/blogs/4757/Как-приобрести-сейчас-качественный-диплом-в-интернете
Привет!
Мы изготавливаем дипломы.
owen.ru/forum/member.php?u=106526
ssa.ru/forum/bystroe-oformlenie-diplomov-na-zakaz.html
poemsbook.net/blogs/123079/Купить-диплом-доверяйте-профессионалам
skvortsy.listbb.ru/posting.php?mode=post&f=31&sid=ab76a7ac5965c71816f930aa4f3fa5e7
molbiol.ru/forums/index.php?showtopic=1227057
Привет, друзья!
Заказать диплом любого ВУЗа.
ccde-cambodia.com/cb-profile/pluginclass/cbblogs.html?action=blogs&func=show&id=118
Добрый день!
Приобрести документ о получении высшего образования вы сможете в нашем сервисе.
ast-diplomas.com/kupit-diplom-kandidata-nauk
Online Communities and Forums
ivermectin online
buy cheap generic lasuna – cheap himcolin sale himcolin brand
детские развлечения в сочи в центральном районе
развлечения для подростков сочи
Привет!
Приобрести диплом любого ВУЗа.
animesocial.su/blogs/3202/Ваш-диплом-для-успешной-карьеры-быстро-и-надежно/
talkiachat.com/blogs/26/Что-потребуется-для-изготовления-качественного-диплома-института/
worldaid.eu.org/discussion/profile.php?id=5130
parenvarmii.ru/topic4395.html?view=previous
ismayilovform.com/blog/page,1,26,16-qarin-eritmeyin-en-effektiv-yollari.html
Здравствуйте!
Заказать документ о получении высшего образования.
russiajoy.ru/legalnyiy-diplom-bez-lishnih-hlopot-uznayte-kak
nachosking.com/read-blog/1002
grot.getbb.ru/viewtopic.php?f=6&t=1066
forexrassia.ru/diplomyi-lyuboy-slozhnosti-byistro-i-bez-problem
generalarminius.com/viewtopic.php?t=156074
Привет, друзья!
Мы изготавливаем дипломы психологов, юристов, экономистов и любых других профессий.
edusocial.online/blogs/117/Ищем-надежный-онлайн-магазин-с-аттестатами-и-дипломами
Всегда вам поможем!.
Привет, друзья!
Заказать документ о получении высшего образования.
forum.vorchun.ru/viewtopic.php?f=2&t=253067
kolba.com.ua/index.php?topic=140911.new#new
premium.listbb.ru/viewtopic.php?f=2&t=430
thesleepinghusband.rolka.me/viewtopic.php?id=22110#p53929
rpinnovative.1stbb.ru/viewtopic.php?f=8&t=382
Привет!
Мы можем предложить дипломы психологов, юристов, экономистов и любых других профессий по приятным тарифам.
comedyforme.ru/vash-diplom-garantiya-kachestva-i-nadezhnosti
Добрый день!
Заказать документ о получении высшего образования вы можете у нас в столице.
ast-diplom24.ru/kupit-diplom-vracha
Успешной учебы!
Кавказская мазь https://kavkazmaz.ru для суставов купить в аптеке. Официальный сайт производителя Кавказской мази от боли в суставах.
Здравствуйте!
Заказать документ о получении высшего образования вы сможете у нас. Мы оказываем услуги по изготовлению и продаже документов об окончании любых ВУЗов Российской Федерации.
rytof.ru/node/16245
vipblinds.ru/index.php?subaction=userinfo&user=omuha
http://www.amatagroup.ru/forum/messages/forum1/topic59/message357308/?result=reply#message357308
miupsik.ru/forums/showthread.php?tid=35258
mag-motors.ru/index.php?subaction=userinfo&user=afovurep
На 1win вас ждут лучшие игры, выгодные ставки и круглосуточная поддержка клиентов.
парк развлечений для детей 3 лет
How would you reate my boobs?
Привет!
Заказать документ о получении высшего образования.
demo.advised360.com/read-blog/162165
weekevents.ru/kupit-diplom-ofitsialno
ukrevent.ru/diplom-dlya-karernogo-rosta-prosto-i-udobno/
avtovladelez.ru/oformlenie-diploma-bez-problem-i-zabot
newsbizlife.ru/diplom-na-zakaz-kachestvo-i-nadezhnost
Привет!
Как безопасно купить диплом колледжа или ПТУ в России, что важно знать
http://www.hinterhof.ch/de/2024/06/30/купить-диплом-урфу/
1win предлагает широкий выбор азартных игр и спортивных ставок с привлекательными бонусами.
Добрый день!
Приобрести документ института можно у нас в столице. Мы оказываем услуги по продаже документов об окончании любых университетов РФ. Вы сможете получить диплом по любой специальности, включая документы СССР. Гарантируем, что при проверке документов работодателями, каких-либо подозрений не возникнет.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным ценам. Стоимость зависит от конкретной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику цен. Важно, чтобы дипломы были доступными для подавляющей массы наших граждан.
http://www.omaada.com/blogs/120466/Детальное-описание-заказа-документов-в-популярном-онлайн-магазине
Окажем помощь!
Привет, друзья!
Купить документ ВУЗа
sonnick84.bloginder.com/28831570/Ключевые-затраты-российского-изготовителя-дипломов-авторский-обзор
prof-komplekt.com/club/user/1035/blog/11095/
selamnews.com/blogs/12912/На-что-именно-обращать-внимание-при-заказе-документов-в-интернете
wiki.roximo.ru/index.php/Служба_поддержки_и_FAQ._Приобретаем_документы_в_интернете
connectme.live/blogs/956/Хотите-купить-диплом-Открывайте-наш-магазин
Привет!
Мы изготавливаем дипломы любых профессий по выгодным ценам.
hanaverse.top/blogs/917/Как-можно-купить-сегодня-качественный-диплом-в-интернете
Бинариум скачать binariums.net
Предлагаем Вам сайт, через который вы попадете на официальную торговую площадку Бинариум. На онлайн ресурсе binariums.net есть множество полезной информации для пользования сайтом, регистрации и торговле.
Для того, чтобы начать работать, необходимо пройти регистрацию на главном сайте. Вводи ваши персональные данные верно, чтобы в дальнейшем не было ошибок. Также непременно изучите инструкцию по сделкам на сайте, если Вы не очень уверенный пользователь. Для Вас все детально расписано с картинками.
По теме бинариум официальный сайт вы на верном пути. На платформе Binarium можно осуществлять торговые операции и зарабатывать большие деньги. Они проводятся строго по графику работы рынка Forex, то есть 5-ти дневку.
Не нужно заходить в сделку не подумав, лучше потратить немного времени на изучение актива, статистики, новостей, тем более на платформе binariums.net об этом много индикаторов. Также не стоит сразу все деньги вкладывать в одну сделку, лучше поделить и использовать их частями.
Если Вы искали binarium личный кабинет то мы Вам обязательно окажем помощь. Преимущества брокера Бинариум известны всем. Это: стабильная работа более 10 лет, безопасность хранения средств, простота в использовании, 4 типа графиков, полезные советы — новости, экономический календарь и многое другое.
Добрый день!
Покупка школьного аттестата с упрощенной программой: что важно знать
socialxtendr.com/blogs/169/Правильно-приобретаем-документы-в-сети-интернет-обзор
Привет!
Приобрести диплом о высшем образовании
gaysocial.gay/read-blog/86
bryansk32-forum.ru/ucp.php?mode=login
onlinekinospace.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
wiki.odessanews.biz/index.php/Большая_популярность_интернет-магазинов,_что_предлагают_документы
u2c.tv/member.php?u=30984
+подработка +в +свободное +время +свежие +вакансии – +работа +курьером +с +16 +лет, +работа +мужчинам +курьер
Официальная покупка школьного аттестата с упрощенным обучением в Москве
l67697qa.beget.tech/2024/07/10/blagodarya-chemu-magaziny-s-diplomami-tak-populyarny.html
ingprint.ru/club/user/58725/forum/message/6949/203482/
app.brains.ng/blogs/30/Вы-хотите-узнать-как-заказать-диплом-в-сети-Заходите
income.forum2x2.ru/t2972-topic#5292
vintfint.com/blogs/22618/Купить-диплом-Легко-и-Быстро
Привет!
Приобрести документ о получении высшего образования
sonnick84.ssnblog.com/27782128/Хотите-приобрести-диплом-у-проверенного-исполнителя-Ждем-Вас
sonnick84.jaiblogs.com/55182494/Как-можно-приобрести-недорого-качественный-диплом-в-интернете
sonnick84.link4blogs.com/50390659/Цена-дипломов-обзор-экспертов
antrem.ru/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=285
9yzqnf5yu.blogsmine.com/28727827/Детальное-описание-заказа-аттестата-в-знаменитом-интернет-магазине
Здравствуйте!
Заказать документ института
diplomasx.com/kupit-diplom-krasnoyarsk
Привет, друзья!
Заказать документ института вы сможете в нашей компании.
asxdiplomik24.ru/kupit-diplom-tehnikuma-kolledzha
Привет!
Мы предлагаем дипломы любой профессии по приятным тарифам. Стоимость зависит от определенной специальности, года выпуска и университета. Всегда стараемся поддерживать для покупателей адекватную ценовую политику. Важно, чтобы дипломы были доступны для большого количества наших граждан.
azat.on.kg/blogs/723/Где-можно-будет-приобрести-диплом-либо-аттестат-высокого-качества
The user interface of the Aviator Game is designed to be intuitive and user-friendly. The clean design and easy
buy ivermectin
Здравствуйте!
Как официально приобрести аттестат 11 класса с минимальными затратами времени
beinsadouno.bg/events/event/43-какие-интернет-магазины-с-дипломами-имеются-на-сегодняшний-момент/
Привет, друзья!
Купить документ ВУЗа вы имеете возможность у нас в столице. Мы предлагаем документы об окончании любых ВУЗов Российской Федерации.
avtoserviskovrov.ru/index.php?subaction=userinfo&user=ypasuqyj
forum.stpku.ru/viewtopic.php?f=2&t=49804
cookownfood.blogspot.com/2012/11/cold-bean-thread-noodles-with-spinach.html
suhinfo.ru/index.php?title=premiummdiplomms
http://www.aura-invest.com/bbs/board.php?bo_table=free&wr_id=3276942
Привет!
Быстрое обучение и получение диплома магистра – возможно ли это?
landik-diploms-srednee.ru/diplom-s-reestromkupit-kupit В
видео стена видео стена .
световое оборудование для актового зала световое оборудование для актового зала .
Привет, друзья!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании.
diplomyx.com/kupit-diplom-perm
Добрый день!
Купить документ ВУЗа вы можете у нас в столице. Мы оказываем услуги по производству и продаже документов об окончании любых университетов России. Вы сможете получить необходимый диплом по любым специальностям, включая документы СССР. Даем гарантию, что в случае проверки документа работодателем, подозрений не появится.
Мы готовы предложить дипломы любой профессии по приятным ценам. Цена будет зависеть от выбранной специальности, года выпуска и образовательного учреждения. Всегда стараемся поддерживать для клиентов адекватную политику цен. Для нас важно, чтобы дипломы были доступны для большинства наших граждан.
agarwalconnect.com/blogs/179/Подробное-описание-приобретения-диплома-в-популярном-онлайн-магазине
Рады оказаться полезными!
Добрый день!
Заказать диплом любого ВУЗа.
imhht.com/index.php?title=Как_подобрать_надежный_онлайн_магазин_с_большим_выбором_дипломов?
Привет, друзья!
Мы можем предложить документы ВУЗов
californiarpn2.listbb.ru/viewtopic.php?f=1&t=519
rolevikionline.g-talk.ru/faq.php
graph.org/Bystroe-i-nadezhnoe-poluchenie-diploma-07-22
most.maxbb.ru/viewtopic.php?f=4&t=708
vip.7bb.ru/viewtopic.php?id=3062#p7211
Используйте 1вин рабочее зеркало для бесперебойной игры.
Привет!
Приобрести документ института вы можете в нашей компании.
ast-diplom.com/kupit-diplom-magistra
Успехов в учебе!
Пройдите 1win регистрация и получите приветственные бонусы.
На сайте https://lilibum.ru вы сможете познакомиться с мужчиной или девушкой для самых разных целей, в том числе, создания крепких отношений, семьи. Если кто-то вам понравился, то напишите сообщение, чтобы вступить в контакт, а затем и назначить долгожданную встречу. Вполне вероятно, что вы друг другу подходите. Для того чтобы воспользоваться всеми функциями и преимуществами, необходимо пройти регистрацию. На сайте регулярно регистрируется огромное количество пользователей, которые тоже хотят отыскать свою вторую половинку.
Привет!
Купить диплом университета.
piratesouls.org/events/event/12-как-найти-надежный-интернет-магазин-с-огромным-выбором-дипломов/
Здравствуйте!
Приобрести диплом о высшем образовании
dominion.listbb.ru/viewtopic.php?f=11&t=464
kalininabad.flyboard.ru/viewtopic.php?f=28&t=2850
wecanchat.mn.co/posts/62527824
newsofgames.ru/obrazovanie-mechtyi-diplomyi-vedushhih-vuzov
academy4elements.mybb.ru/viewtopic.php?id=964#p2098
Здравствуйте!
Диплом экономиста
industrial.getbb.ru/viewtopic.php?f=4&t=3107
rorp.4admins.ru/viewforum.php?f=33
2cool.ru/qiwi-f215/diplomi-vedushchih-vuzov-dlya-uspeshnogo-budushchego-t3834.html
hl2forever.ru/member.php?u=266
shoptema.ru/forum/topic/32733/
Привет!
Мы готовы предложить документы техникумов
myturtime.ru/zakazhite-diplom-pryamo-seychas
rakisochi.ru/users/20
seriallove.bbok.ru/viewtopic.php?id=7232#p123278
mediamemorial.ru/club/user/125807/forum/message/3874/13356/#message13356
boltushka.flybb.ru/viewtopic.php?f=14&t=1545
Наши специалисты предлагает надежный сервис ремонта плоттеров любых брендов и моделей. Мы знаем, насколько значимы для вас ваши плоттеры, и готовы предложить сервис первоклассного уровня. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что предоставляет длительную работу проведенных ремонтов.s
Наиболее распространенные поломки, с которыми сталкиваются владельцы плоттеров, включают неисправности печатающей головки, застревание бумаги, ошибки ПО, неработающие разъемы и поломки компонентов. Для устранения этих проблем наши опытные мастера выполняют ремонт печатающих головок, механизмов подачи бумаги, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы получаете качественный и надежный мастер по ремонту плоттера.
Подробная информация представлена на нашем сайте: https://remont-plotterov-style.ru
Привет, друзья!
Приобрести документ о получении высшего образования вы можете в нашей компании.
ast-diploms24.ru/kupit-diplom-o-srednem-obrazovanii
Хорошей учебы!
Здравствуйте!
Мы изготавливаем дипломы психологов, юристов, экономистов и прочих профессий по доступным тарифам. Стоимость будет зависеть от определенной специальности, года выпуска и образовательного учреждения. Стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы документы были доступны для подавляющей массы наших граждан.
telegra.ph/Priobresti-diplom-libo-attestat-stalo-gorazdo-proshche-05-02
Привет, друзья!
Заказать диплом о высшем образовании
Наша компания предлагает быстро и выгодно купить диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, штампами, подписями. Диплом способен пройти лубую проверку, даже при помощи специального оборудования. Решите свои задачи максимально быстро с нашим сервисом.
Где приобрести диплом по нужной специальности?
sonnick84.pages10.com/Что-именно-понадобится-для-создания-качественного-диплома-института-63975006
sfera100.ru/forum/user/2585/
wiki.3cdr.ru/wiki/index.php/Гарантия_Подлинности:_Покупка_Дипломов_Легально
http://www.yagath.com/blogs/678064/Рекомендации-по-приобретению-документов-в-сети
newsbig2.almoheet-travel.com/gramotno-pokupaem-diplom-v-seti-internet-avtorskij-obzor
Здравствуйте!
Заказать диплом любого ВУЗа.
site2.liodiz.ru/2024/07/04/shirokiy-vybor-dokumentov-v-znamenitom-onlayn-magazine.html
Привет!
Мы предлагаем документы техникумов
samara.listbb.ru/viewtopic.php?f=3&t=386
kharkov-balka.com/showthread.php?p=155433#post155433
yaoisennari.ekafe.ru/ucp.php?mode=login&sid=49214250bf1dbe2939e08836e01f3dd9
sontopic.com/blogs/new
slliver.getbb.ru/viewtopic.php?f=62&t=953
Здравствуйте!
Купить документ о получении высшего образования
ast-diplomy.com/kupit-diplom-magistra
На сайте https://gk-crocus.ru/ подберите светлую, обустроенную квартиру в новом ЖК «CROCUS». Здесь будет все, что нужно для комфортного проживания с семьей. В ЖК развитая инфраструктура, а потому здесь планируется строительство кофеен, магазинов, булочных, а парковочных мест хватит на всех жителей. Обустроенный и удобный двор, где можно отдохнуть и погулять на площадке с ребенком. Предусмотрена круглосуточная охрана. Сдача объектов планируется в 2026 году. Всего 8 корпусов, 2100 квартир. Спешите, чтобы одна из них стала вашей!
Привет!
Официальная покупка школьного аттестата с упрощенным обучением в Москве
landik-diploms-srednee.ru/kupit-diplom-v-voronezhe В
Привет!
Приобрести документ института можно у нас в столице. Мы оказываем услуги по производству и продаже документов об окончании любых ВУЗов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы образца СССР. Гарантируем, что при проверке документов работодателем, каких-либо подозрений не возникнет.
saumalkol.com/forum/разное-2/3545-купить-диплом-быстро-и-надежно.html
pipewiki.org/app/index.php/Надежные_дипломы_с_гарантией_конфиденциальности
comedyforme.ru/vyisshee-obrazovanie-za-den-pokupka-diploma
ремонт-оптом.рф/club/user/7/blog/2123/
http://www.yur-dom.ru/communication/forum/messages/forum3/message249/292-kupit-ofitsialnyy-diplom-bystro-i-legalno?result=new#message249
Добрый день!
Купить документ о получении высшего образования.
chromerp.listbb.ru/viewtopic.php?f=13&t=514
guyspages.com/create-blog/
vip.rolevaya.info/post.php?fid=2
fotomaniya.getbb.ru/viewtopic.php?f=16&t=11216
films.name/viewforum.php?f=143
Привет, друзья!
Приобрести документ института
blogger-mania.mn.co/posts/61838359
myparea.mn.co/posts/61724049
shopy.partners/read-blog/1341
newsbig.bearsfanteamshop.com/zelaete-priobresti-diplom-perehodite-v-nas-onlajn-magazin
ebuddiz.com//read-blog/24166
Добрый день!
Заказать документ университета можно у нас в столице. Мы оказываем услуги по продаже документов об окончании любых университетов РФ. Вы сможете получить необходимый диплом по любой специальности, любого года выпуска, в том числе документы СССР. Гарантируем, что в случае проверки документов работодателем, подозрений не появится.
Мы предлагаем дипломы любой профессии по доступным тарифам. Стоимость может зависеть от выбранной специальности, года получения и образовательного учреждения. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Для нас очень важно, чтобы документы были доступны для большинства наших граждан.
neurostarcheats.com/index.php?/gallery/image/35-отличные-расценки-и-высокое-качество-дипломы-онлайн/
Всегда вам поможем!
Здравствуйте!
Мы готовы предложить дипломы психологов, юристов, экономистов и прочих профессий по приятным тарифам.
karriere.kv-architektur.de/купить-диплом-иргупс/
Добрый день!
Приобрести документ института.
vaeaem.profiforum.ru/t4039-topic#7330
besconeshnocte.flybb.ru/viewtopic.php?f=2&t=949
subscribe.ru/member/quick
draiv.flybb.ru/viewtopic.php?f=2&t=748
paning.flybb.ru/viewtopic.php?f=7&t=1222
Привет!
Заказать диплом университета:
artem-energo.ru/forums.php?m=posts&q=18414&n=last#bottom
чернолесье.рф/forum/viewtopic.php?f=3&t=531284
wiki.mysupp.ru/index.php?title=premiummdiplomms
karabash.chelbusiness.ru/index.php?name=account&op=info&uname=ohuke
nipponsword.ru/profile.php?lookup=24177
Social and Community Aspects
ivermectin online
https://derbayerischelowe.info/
Наши специалисты предлагает профессиональный ремонт прибора ночного видения рядом различных марок и моделей. Мы осознаем, насколько значимы для вас ваши приборы ночного видения, и обеспечиваем ремонт высочайшего уровня. Наши профессиональные техники работают быстро и аккуратно, используя только сертифицированные компоненты, что предоставляет надежность и долговечность наших услуг.
Наиболее частые неисправности, с которыми сталкиваются обладатели приборов ночного видения, включают проблемы с изображением, поврежденные линзы, неисправности программного обеспечения, неработающие разъемы и поломки компонентов. Для устранения этих неисправностей наши квалифицированные специалисты выполняют ремонт сенсоров, оптики, ПО, разъемов и механических компонентов. Доверив ремонт нам, вы получаете надежный и долговечный сервисный ремонт прибора ночного видения на выезде.
Подробная информация представлена на нашем сайте: https://remont-pnv-ultra.ru
Привет, друзья!
Заказать диплом института
dyado.listbb.ru/viewtopic.php?f=2&t=469
vaeaem.profiforum.ru/t4087-topic#7381
odinzovo.rusff.me/viewtopic.php?id=4923#p8319
dyado.listbb.ru/viewtopic.php?f=2&t=474
msfo-soft.ru/msfo/forum/messages/forum24/topic10547/message303490/?result=new#message303490
Привет!
Диплом для вас
club-kia.com/forum/thread30847.html
figarohair.ru/conf/viewtopic.php?f=11&t=12673&sid=24b52f398264e635fefad8d9af176514
kostromag.ru/forum/science/9044.aspx
simple-com.ru/forum/user/2011/
thesleepinghusband.rolka.me/viewtopic.php?id=22131#p53970
Привет!
Мы можем предложить дипломы любых профессий по доступным ценам.
gemawiraclub.com/blogs/39878/Как-можно-будет-купить-недорого-качественный-диплом-в-сети
Добрый день!
Заказать документ о получении высшего образования можно у нас в столице.
diplomyx.com/kupit-diplom-kandidata-nauk
Привет!
Заказать документ о получении высшего образования.
vocal.com.ua/node/62420
sampnewrp.listbb.ru/viewtopic.php?f=18&t=526&sid=6fb2eb5d3164a33377d6c0f0379fb1b7
blogs.rufox.ru/~worksale/48402.htm
rorp.4admins.ru/viewforum.php?f=33
29ru.listbb.ru/posting.php?mode=post&f=26
Привет, друзья!
Аттестат школы купить официально с упрощенным обучением в Москве
andreandrose.co.uk/2024/06/30/купить-диплом-в-артеме/
Здравствуйте!
Заказать диплом о высшем образовании.
mediamemorial.ru/club/user/69594/forum/message/3756/13238/
Добрый день!
Купить диплом любого ВУЗа
Наша компания предлагает быстро и выгодно заказать диплом, который выполняется на бланке ГОЗНАКа и заверен печатями, водяными знаками, подписями. Диплом пройдет лубую проверку, даже при помощи профессионального оборудования. Решайте свои задачи быстро и просто с нашими дипломами.
Где купить диплом по нужной специальности?
opaseke.com/users/1243
anahnu.club/jomsocial/groups/viewbulletin/10119-быстрый-выбор-интернет-магазина,-продающего-дипломы.html?groupid=1
naijarise.com/read-blog/45
http://www.seaman.com.ua/forum/index.php?login/login
victorians123.com/blogs/209/Рекомендации-эксперта-которые-позволят-недорого-приобрести-диплом
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным ценам.
yiwulist.com/диплом-техникума-колледжа-2004-2006-фото-2/
Привет!
Мы изготавливаем дипломы любых профессий по разумным тарифам. Цена будет зависеть от определенной специальности, года выпуска и ВУЗа. Стараемся поддерживать для покупателей адекватную ценовую политику. Важно, чтобы дипломы были доступными для большинства наших граждан.
thegreatbookmark.com/story17161014/купить-диплом-Саратов
Здравствуйте!
Мы предлагаем документы ВУЗов
comptonrpp.listbb.ru/viewtopic.php?f=6&t=735
forum.osvita.od.ua/viewtopic.php?f=1&t=29533
dimitrii.flybb.ru/viewtopic.php?f=29&t=966
azat.on.kg/blogs/1125/Быстрое-и-надежное-получение-диплома
serialforfree.ru/diplom-o-vyisshem-obrazovanii-za-korotkiy-srok
Привет, друзья!
Купить документ ВУЗа
sonnick84.wssblogs.com/28284612/Основные-расходы-производителя-документов-авторский-обзор
qoq.me/read-blog/127
ourfathersfamily.com/blogs/2400/Как-возможно-недорого-приобрести-аттестат-в-онлайн-магазине
connect.nteep.org/blogs/2499/Как-подобрать-надежный-онлайн-магазин-продающий-документы
gioturbobp.com/blogs/31/Проверенный-онлайн-магазин-с-огромным-каталогом-документов
оборудование для актовых залов оборудование для актовых залов .
Чудо Гриб препарат от паразитов https://chydogrib.ru и ВПЧ. Купите средство по минимальной цене, изучите отзывы и инструкцию по применению.
Привет!
Заказать документ о получении высшего образования
rucollectshoeclub.com/read-blog/1841
mylook-online.mn.co/posts/61748933
sonnick84.tkzblog.com/28131503/Заказываем-диплом-в-надежном-магазине-Советы-специалистов
huarenjiaohui.com/index.php?/gallery/image/125-быстрый-поиск-онлайн-магазина-который-реализует-дипломы-и-аттестаты/
wowonder.xyz/read-blog/78394
Добрый день!
Приобрести документ о получении высшего образования вы имеете возможность у нас.
diplomyx.com/kupit-diplom-krasnoyarsk
Хорошей учебы!
Наш сервисный центр предлагает высококачественный качественный ремонт посудомоечных машин всех типов и брендов. Мы знаем, насколько необходимы вам ваши посудомойки, и обеспечиваем ремонт высочайшего уровня. Наши профессиональные техники оперативно и тщательно выполняют работу, используя только оригинальные запчасти, что гарантирует длительную работу проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются пользователи посудомоек, включают проблемы с нагревом воды, проблемы с подачей воды, программные сбои, неработающие разъемы и повреждения корпуса. Для устранения этих неисправностей наши квалифицированные специалисты оказывают ремонт нагревательных элементов, насосов, ПО, разъемов и механических компонентов. Обратившись к нам, вы обеспечиваете себе долговечный и надежный выездной ремонт посудомоечных машин.
Подробная информация представлена на нашем сайте: https://remont-posudomoechnyh-mashin-expert.ru
Здравствуйте!
Заказать документ университета можно у нас. Мы предлагаем документы об окончании любых университетов Российской Федерации. Вы получите необходимый диплом по любой специальности, любого года выпуска, включая документы образца СССР. Даем 100% гарантию, что при проверке документов работодателями, каких-либо подозрений не возникнет.
korrespondentweek.ru/poluchite-diplom-lyuboy-spetsialnosti/
http://www.oyotunji.online/blogs/1748/Выбираем-проверенный-интернет-магазин-для-покупки-диплома
avtolux48.ru/people/user/367/blog/7871/
animesocial.su/blogs/3054/Легкий-поиск-онлайн-магазина-продающего-дипломы-и-аттестаты
test.bpal.org/blogs/entry/8398-каталог-и-варианты-доставки-в-магазине-покупаем-аттестат/
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
last news about firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
firmino
Здравствуйте!
Заказать диплом университета.
derivsocial.org/read-blog/2569
Добрый день!
Получить диплом о высшем образовании
iwasocial.com/read-blog/502
corsica.forhikers.com/forum/p/127484
zarabotok.forumrpg.ru/post.php?fid=26
dog-ola.ru/viewtopic.php?f=28&t=7511
koxma.4adm.ru/viewforum.php?f=296
Привет!
Диплом экономиста
c99596qr.beget.tech/2024/07/21/diplom-o-vysshem-obrazovanii-vashi-novye-perspektivy.html
wheeoo.com/read-blog/14549
galantclub.od.ua/member.php?u=27724
foousrp.listbb.ru/viewtopic.php?f=4&t=535
ffxiv.one/blogs/193/Оформите-диплом-за-пару-дней
Здравствуйте!
Где приобрести диплом по необходимой специальности?
http://www.gamerlaunch.com/community/users/blog/6398497/2285300/особенности-по/?gid=535
На канале рейтинг лучших онлайн казино для смартфонов собраны лучшие казино, где можно играть на реальные деньги и получать щедрые бонусы. Воспользуйтесь фриспинами и бонусами на депозит, играя в надежных казино с высоким рейтингом и быстрой выплатой выигрышей.
Следите за обновлениями канала, чтобы быть в курсе всех новинок и акций. Играйте в лицензированных казино, обеспечивающих безопасную и честную игру. Присоединяйтесь к каналу и открывайте для себя лучшие онлайн-казино 2024 года!
Привет, друзья!
Приобрести документ о получении высшего образования
oldplay.ro/gallery/image/1-почему-сегодня-намного-дешевле-и-проще-заказать-диплом-университета/?context=new
test.bpal.org/blogs/entry/8400-покупаем-диплом-в-проверенном-магазине-по-комфортной-стоимости/
autoplus74.com/club/user/170/blog/390/
uconnect.ae/read-blog/78595
goodnow.mn.co/posts/61639417
Купить диплом любого ВУЗа.
forum.gorodsalavat.ru/posting.php?mode=post&f=28&sid=1a444f9f7d39bb15f50309f3f6ebe256
meat.ntnn.ru/personal/profile/index.php?register=yes
forum.artinvestment.ru/member.php?u=1807451
wegug.in/blogs/942/Купить-Официальный-Диплом-Быстро-и-Легально
fotomaniya.getbb.ru/viewtopic.php?f=16&t=11153
Добрый день!
Приобрести документ о получении высшего образования.
newrealgames.ru/oformlenie-diplomov-pod-klyuch
serialforfree.ru/diplom-bez-uchebyi-prosto-i-bezopasno
forummichiganrp.moibb.ru/viewtopic.php?f=21&t=442
academy4elements.mybb.ru/viewtopic.php?id=953#p2087
odincovoschool16.flybb.ru/viewtopic.php?f=2&t=839
сколько стоит раскрутка сайта в яндекс https://razrabotka-sajtov-pod-klyuch.ru/
Наш сервисный центр предлагает высококачественный сервисный центр по ремонту принтеров на выезде всех типов и брендов. Мы знаем, насколько важны для вас ваши печатающие устройства, и готовы предложить сервис наилучшего качества. Наши опытные мастера работают быстро и аккуратно, используя только качественные детали, что предоставляет долговечность и надежность выполненных работ.
Наиболее распространенные поломки, с которыми сталкиваются обладатели устройств для печати, включают проблемы с печатью, проблемы с подачей бумаги, ошибки ПО, проблемы с портами и повреждения корпуса. Для устранения этих проблем наши опытные мастера выполняют ремонт печатающих головок, механизмов подачи бумаги, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы обеспечиваете себе качественный и надежный мастерская по ремонту принтера в москве.
Подробная информация размещена на сайте: https://remont-printerov-master.ru
Добрый день!
Мы изготавливаем дипломы любых профессий по доступным ценам.
tirana.social/blogs/1010/Как-можно-заказать-недорого-качественный-диплом-в-интернете
Привет!
Заказать документ ВУЗа вы можете в нашей компании в столице.
diplomyx24.ru/kupit-diplom-ekaterinbur
Удачи!
Здравствуйте!
Приобрести диплом любого ВУЗа.
forum.enchald.com/files/file/9-вы-хотите-приобрести-диплом-переходите-в-наш-магазин/
sonnick84.glifeblog.com/27690341/Проверенный-онлайн-магазин-с-обширным-ассортиментом-дипломов
luckybookies.com/blogs/1113/Что-понадобится-для-создания-качественного-диплома
portugues.ru/forum/album.php?albumid=91&attachmentid=3900&commentid=1664
socialnetwork.cloudyzx.com/read-blog/11169
Online Communities and Forums
cost of ivermectin
This makes certain the internet site complies with rewuirements and takes dity for
itts conduct.
my blog … 슈어맨
Здравствуйте!
Приобрести документ ВУЗа можно в нашей компании в столице.
ast-diploms24.ru/kupit-diplom-magistra
Успехов в учебе!
Здравствуйте!
Мы изготавливаем дипломы.
myturtime.ru/nastoyashhie-diplomyi-byistro-legalno-nadezhno
aromatov.wooden-rock.ru/forum/topic.php?forum=1&topic=16083
oren.kabb.ru/viewtopic.php?f=50&t=33925
csexpert.4adm.ru/posting.php?mode=post&f=70&sid=6cbf5ff086899aaa61c5296db59e982d
doctorsforum.ru/viewtopic.php?f=193&t=38986
[u][b] Привет, друзья![/b][/u]
[b]Заказать диплом университета.[/b]
[url=http://bmw-donbass.ru/gallery/image/839-широкий-выбор-документов-в-популярном-интернет-магазине//]bmw-donbass.ru/gallery/image/839-широкий-выбор-документов-в-популярном-интернет-магазине/[/url]
Привет, друзья!
Заказать диплом университета.
prosat.ru/modules.html?name=Journal&file=display&jid=23346
Привет!
Мы можем предложить документы техникумов
paning.flybb.ru/viewtopic.php?f=7&t=1241
ostome.ru/forumbb/posting.php?mode=post&f=12
masterflower.listbb.ru/viewtopic.php?f=6&t=387
gess.flybb.ru/viewtopic.php?f=2&t=713
webyourself.eu/blogs/398826/Быстрый-и-надежный-способ-получить-диплом
Привет!
Купить документ о получении высшего образования вы имеете возможность в нашей компании в Москве.
ast-diplomas24.ru/kupit-diplom-nizhnij-novgorod
Хорошей учебы!
Наша мастерская предлагает профессиональный сервисный ремонт проектора всех типов и брендов. Мы знаем, насколько значимы для вас ваши проекционные устройства, и обеспечиваем ремонт первоклассного уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что обеспечивает надежность и долговечность проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются пользователи проекционных устройств, включают неисправности лампы, неисправности вентилятора, программные сбои, неработающие разъемы и поломки компонентов. Для устранения этих поломок наши квалифицированные специалисты проводят ремонт ламп, вентиляторов, ПО, разъемов и механических компонентов. Обращаясь в наш сервисный центр, вы получаете надежный и долговечный сервисный ремонт проектора на выезде.
Подробная информация представлена на нашем сайте: https://remont-proektorov-online.ru
For prop bets, you are wagering on a specific instance or aspect of
the game.
Feel free to visit my web blog 토토친구
Привет!
Заказать диплом любого ВУЗа.
k90280ul.beget.tech/2024/07/04/shirokiy-katalog-dokumentov-v-populyarnom-onlayn-magazine.html
Привет, друзья!
Купить документ университета вы можете у нас в Москве. Мы оказываем услуги по продаже документов об окончании любых ВУЗов Российской Федерации.
mariland.org/index.php?subaction=userinfo&user=yregana
cargo-200.ru/index.php?subaction=userinfo&user=oqotyhyx
http://www.6986986.com/forum.php?mod=viewthread&tid=9038&pid=132150&page=3741&extra=page=1#pid132150
http://www.detskiy-mir.net/index.php?subaction=userinfo&user=atediko
forum.stde.ru/index.php?/topic/9874-how-to-create-a-new-topic-at-forumstderu/page/6/#comment-11624
[url=https://xn—–8kcaaomxdpelhyeeqjefp6c.xn--p1ai/%D1%83%D1%81%D0%BB%D1%83%D0%B3%D0%B8/%D1%8D%D0%BA%D1%81%D0%BA%D1%83%D1%80%D1%81%D0%B8%D0%B8_%D0%B8%D0%B7_%D0%B0%D0%BD%D0%B0%D0%BF%D1%8B]Экскурсии из Анапы[/url] – Аренда яхт и катеров в Анапе, Экскурсия Тамань
Монтаж системы видеонаблюдения может потребоваться в самых разных ситуациях. Её устанавливают в частных и загородных домах, промышленных предприятиях, офисах, гаражах и многих других помещениях https://rivara.ru/bezopasnost-v-karmane-vzglyanite-na-mir-cherez-glaza-sistemy-videonablyudeniya/
Добрый день!
Мы можем предложить дипломы любой профессии по выгодным ценам.
wiki.gta-zona.ru/index.php/Техподдержка_и_FAQ._Покупаем_диплом_в_сети
yoa45mzo5.ka-blogs.com/81608090/Как-можно-быстро-купить-аттестат-в-интернет-магазине
chillibell.com/read-blog/35
perfectohub.com/read-blog/7811
prof-aksay.ru/blogs/1/pokupaem-diplom-v-izvestnom-internetmagazine-po-vygodnoy-tsene.php
Здравствуйте!
Мы готовы предложить документы ВУЗов
worksale.jofo.me/2279497.html?_ga=2.232252383.1924095826.1721345148-1887670593.1721345148
serialforfree.ru/diplom-o-vyisshem-obrazovanii-za-korotkiy-srok
twoplustwoequal.com/read-blog/38381
paulikipedia.ru/index.php/ваш_ключ_к_успеху_Ц_диплом_о_высшем_образовании
preceptor.flybb.ru/viewtopic.php?f=13&t=9948
Здравствуйте!
Заказать диплом любого ВУЗа:
dxzw.com/member/index.php?uid=ogabudul
rf-unicron.ru/index.php?/topic/439-купить-диплом-x8g/
igram.net/index.php?name=Account&op=userinfo&user_name=ijalajo
miupsik.ru/forums/showthread.php?tid=35285
cobaki.ru/users.php?m=details&id=90770
Привет, друзья!
Купить диплом университета.
forum.accent-club.ru/index.php?autocom=blog&blogid=1202&showentry=35679
rebornrpofficial.com/index.php?/files/file/15-покупаем-диплом-в-лучшем-интернет-магазине-по-комфортной-цене/
orqut.com//blogs/10080/На-что-внимание-обратить-при-покупки-диплома-в-сети
guyub.net/read-blog/7723
rusere.ru/communication/forum/messages/forum11/message3689/2975-priobretaem-diplom-v-izvestnom-internet-magazine-po-vygodnoy-tsene?result=new
Наша мастерская предлагает высококачественный срочный ремонт робота пылесоса всех типов и брендов. Мы знаем, насколько необходимы вам ваши автоматические пылесосы, и стремимся предоставить услуги наилучшего качества. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только качественные детали, что гарантирует длительную работу проведенных ремонтов.
Наиболее общие проблемы, с которыми сталкиваются обладатели автоматических пылесосов, включают неисправную батарею, проблемы с мотором, неисправности программного обеспечения, неисправности сенсоров и механические повреждения. Для устранения этих неисправностей наши профессиональные техники оказывают ремонт батарей, двигателей, ПО, сенсоров и механических компонентов. Обратившись к нам, вы получаете надежный и долговечный сервис ремонта робота пылесоса на дому.
Подробная информация размещена на сайте: https://remont-robotov-pylesosov-servis.ru
Здравствуйте!
Заказать диплом любого университета.
dcindians.com/classifieds/detail.aspx?Classified=3c8ee65f-7649-4dc1-b9c0-03927d56431a
duster-clubs.ru/forum/album.php?albumid=863&pictureid=9103&commentid=4916/
dcindians.com/classifieds/detail.aspx?Classified=3c8ee65f-7649-4dc1-b9c0-03927d56431a
oldforum.citysakh.ru/?talkid=26710/
onlinekinospace.ru/page/2
Здравствуйте!
Купить документ университета.
ukrlenta.ru/osushhestvite-mechtu-poluchite-diplom-byistro-i-bez-problem
karasteamfulldmroleplay.getbb.ru/viewtopic.php?f=62&t=923
aurorahcs.com/forum/posting.php?mode=post&f=8
avtobestnews.ru/legkiy-sposob-poluchit-diplom-lyuboy-spetsialnosti
autogroupe.ru/diplomyi-lyuboy-slozhnosti-byistro-i-bez-problem
Привет, друзья!
Аттестат 11 класса купить официально с упрощенным обучением в Москве
gracebook.app/blogs/1187/На-что-именно-обращать-внимание-при-покупки-диплома-в-сети
Добрый день!
Мы можем предложить дипломы любой профессии по приятным ценам.
es-presto.ru/community/groups/0-0/179-4-glavnykh-gruppy-internet-magazinov-kotorye-prodayut-diplomy
Привет, друзья!
Мы можем предложить дипломы любых профессий.
montrealpal.com/read-blog/815_kak-najti-nadezhnyj-magazin-prodayushij-diplomy.html
Рады оказать помощь!.
Добрый день!
Приобрести диплом ВУЗа.
faithstreamer.com/blogs/3087/%D0%9E%D1%81%D0%BD%D0%BE%D0%B2%D0%BD%D1%8B%D0%B5-%D1%80%D0%B0%D1%81%D1%85%D0%BE%D0%B4%D1%8B-%D0%BB%D1%8E%D0%B1%D0%BE%D0%B3%D0%BE-%D0%BF%D1%80%D0%BE%D0%B8%D0%B7%D0%B2%D0%BE%D0%B4%D0%B8%D1%82%D0%B5%D0%BB%D1%8F-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2-%D0%BE%D0%B1%D0%B7%D0%BE%D1%80
Привет!
Купить документ ВУЗа
sabrina-online.su/wiki/index.php?title=Зачем_в_наше_время_заказывают_дипломы_и_аттестаты_в_интернете?
80.87.194.225/blogs/1/diplomy-attestaty-a-tak-zhe-sertifikaty-vygodnye-tseny.php
sonnick84.blogvivi.com/28760758/Планируете-приобрести-диплом-Заходите-в-наш-онлайн-магазин
miss2010.nuclear.ru/site_py/blogs/1/dokumenty-po-komfortnym-tsenam-v-znamenitom-magazine.php
fisketavling.nu/cb-profile/pluginclass/cbblogs?action=blogs&func=show&id=341
Aviator Game. Notable names in the industry have contributed their expertise to ensure the game is both engaging
ivermectin purchase online
Добрый день!
Заказать документ о получении высшего образования.
mylot.su/blogs/2330
pirat.iboards.ru/viewtopic.php?f=20&t=22207
newrealgames.ru/ekspress-dostavka-diplomov-po-vsem-spetsialnostyam
chromerp.listbb.ru/ucp.php?mode=login
rogerfilms.com/index.php?title=Оформление_диплома_под_ключ:_безопасно_и_просто
Привет!
Мы можем предложить дипломы любых профессий по невысоким ценам.
avtobestnews.ru/diplomyi-s-garantiey-podlinnosti-i-kachestva
Привет, друзья!
Приобрести документ университета
sonnick84.glifeblog.com/27739762/Выбираем-надежный-интернет-магазин-для-покупки-документов
meisterbook.com/read-blog/15498
reveal.ru/gate.html?name=Journal&file=display&jid=53724
ourfathersfamily.com/blogs/2393/Главные-затраты-производителя-дипломов-обзор
sonnick84.blogofchange.com/28698968/Надежный-онлайн-магазин-с-обширным-ассортиментом-документов
Привет!
Купить диплом о среднем полном образовании, в чем подвох и как избежать обмана?
http://www.alamedapaulistaimoveis.com.br/купить-диплом-мгуту-или-любого-вуза-ро/
1вин регистрация занимает всего несколько минут и открывает доступ ко всем функциям.
Привет, друзья!
Заказать диплом любого ВУЗа:
mama.pp.ru/index.php?subaction=userinfo&user=ubaficyt
garmoniya.uglich.ru/index.php?subaction=userinfo&user=uzudytusy
mrkineshma.ru/support/forum/view_profile.php?UID=223933
cookownfood.blogspot.com/2012/11/cold-bean-thread-noodles-with-spinach.html
nnklad.ru/viewtopic.php?f=4&t=1712
Здравствуйте!
Мы изготавливаем дипломы любой профессии по выгодным тарифам.
sonnick84.liberty-blog.com/28305067/Известный-онлайн-магазин-с-очень-выгодными-по-цене-документами
sonnick84.qowap.com/87843716/Проверенный-магазин-с-широким-каталогом-дипломов
ls.co-x.ru/2024/07/04/pochemu-namnogo-prosche-i-deshevle-zakazat-diplom-universiteta.html
bundas24.com/read-blog/128838_priobretaem-dokumenty-v-nadezhnom-onlajn-magazine-sovety-eksperta.html
sonnick84.bligblogging.com/28778353/Основные-расходы-любого-изготовителя-документов-обзор
Привет!
Где приобрести диплом по актуальной специальности?
usame.life/read-blog/46080
1win вход для бесперебойной игры.
Наша мастерская предлагает надежный мастерская по ремонту серверов всех типов и брендов. Мы осознаем, насколько важны для вас ваши серверные устройства, и обеспечиваем ремонт высочайшего уровня. Наши квалифицированные специалисты проводят ремонтные работы с высокой скоростью и точностью, используя только сертифицированные компоненты, что обеспечивает длительную работу проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются обладатели серверных устройств, включают неисправности HDD, неисправности блока питания, программные сбои, неработающие сетевые интерфейсы и аппаратные сбои. Для устранения этих неисправностей наши квалифицированные специалисты выполняют ремонт жестких дисков, блоков питания, ПО, сетевых интерфейсов и компонентов. Обращаясь в наш сервисный центр, вы получаете надежный и долговечный вызвать мастера по ремонту сервера с гарантией.
Подробная информация доступна на сайте: https://remont-serverov-express.ru
Приобрести диплом любого университета.
590909.ru/users/74
fforum.ixbb.ru/viewtopic.php?id=184#p4062
ya3bbru.bbok.ru/viewtopic.php?id=4023#p7070
russianecuador.com/forum/member.php?u=13207
shoptema.ru/forum/talk/add/
Здравствуйте!
Приобрести документ о получении высшего образования
sonnick84.thekatyblog.com/27616654/На-что-именно-обратить-внимание-при-заказе-диплома-в-сети-интернет
renaissance.mn.co/posts/61748148
wiki.odessanews.biz/index.php/Покупаем_документы_в_известном_интернет_магазине_по_выгодной_цене
app.site123.com/manager/wizard.php?wu=65b7bc9283766-65b7bc9283768-65b7bc9283769
prosat.ru/modules.html?name=Journal&file=display&jid=23366
Добрый день!
Заказать диплом любого ВУЗа.
rf-unicron.ru/index.php?/gallery/image/115-обширный-выбор-документов-в-популярном-онлайн-магазине/
Привет, друзья!
Приобрести документ о получении высшего образования вы имеете возможность у нас в столице. Мы предлагаем документы об окончании любых ВУЗов России. Вы сможете получить диплом по любым специальностям, включая документы Советского Союза. Гарантируем, что в случае проверки документов работодателями, каких-либо подозрений не появится.
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Цена зависит от выбранной специальности, года получения и университета. Стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы дипломы были доступными для большого количества граждан.
forum.shevrondeath.club/files/file/26-выгодные-расценки-и-прекрасное-качество-дипломы-онлайн/
Поможем вам всегда!
Привет, друзья!
Процесс получения диплома стоматолога: реально ли это сделать быстро?
samgalleria.com/диплом-о-среднем-образовании-купить-н-2/
Будем рады вам помочь!.
use this link sell installs
Здравствуйте!
Приобрести диплом о высшем образовании.
pakhie.com/blogs/8916/Что-понадобится-для-изготовления-качественного-диплома-университета/
sahelishegadi.com/купить-диплом-в-тобольске-гознак-по-са/
grp.7olimp.ru/viewtopic.php?f=13&t=1996
anhbiet.com/index.php?/events/event/13-быстрый-выбор-интернет-магазина-реализующего-дипломы/
qaedymoqutu.bearsfanteamshop.com/cto-imenno-nuzno-dla-sozdania-kacestvennogo-diploma-universiteta/
Здравствуйте!
Мы можем предложить документы ВУЗов
nowoczesna.phorum.pl/posting.php?mode=newtopic&f=2&sid=6169268431fe19179f55fdda40b8d11a
soad.msk.ru/forum/index.php
p33340zg.beget.tech/2024/07/21/diplomy-o-vysshem-obrazovanii-ot-akkreditovannyh-vuzov.html
aurorahcs.com/forum/viewtopic.php?f=8&t=685504
dachaweek.ru/kupite-diplom-byistro-i-legalno
Здравствуйте!
Приобрести диплом любого университета
forcemajor.maxbb.ru/viewtopic.php?f=7&t=826
podsliving.in/forums/topic/купить-диплом-в-москве-бытовые-услови/
medik-look.ru/kupite-diplom-i-zabudte-o-studencheskih-dolgih-nochah
matchfishing.ru/forumtest/1/member.php?u=23110
les-ailes-chalaisiennes.com/forum/topic/как-купить-диплом-пошаговое-руководс/#postid-19473
купить hyip проект – скрипты хайпов, goldcoders
kraken даркнет зеркало 2kmp vip
Как купить аттестат 11 класса с официальным упрощенным обучением в Москве
subscribe.ru/member/quick
les-ailes-chalaisiennes.com/forum/topic/купите-диплом-и-улучшите-свое-будущее/#postid-19485
forum.fiat-club.ru/blog_post.php?do=updateblog&blogid=
southjerseyonline.net/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=272
bideew.com/create-blog/
Здравствуйте!
Мы изготавливаем дипломы любых профессий.
forosmex.com/index.php?/gallery/image/539-почему-сегодня-намного-дешевле-будет-заказать-диплом-вуза/
Рады оказать помощь!.
настоящий сайт kraken kraken one com
кракен маркетплейс
Добрый день!
Мы готовы предложить дипломы.
physmathforum.flybb.ru/viewtopic.php?f=12&t=770
asepbook.com/create-blog/
iqtorg.ru/forum/messages/forum2/topic623/message697/?result=new#message697
balans.kz/bonus/
p99946c6.beget.tech/2024/07/09/kupit-diplom-onlayn-prosto-i-udobno.html
Добрый день!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по приятным тарифам. Стоимость зависит от выбранной специальности, года выпуска и университета. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большинства наших граждан.
http://www.bharatiyaobcmahasabha.org/2024/04/13/купить-диплом-техникума-купить-реаль/
Добрый день!
Приобрести диплом университета:
pirobot.co.uk/doku.php?id=diplomandoci
193.16.101.6/index.php?title=diplomandoci
realtor-cheb.ru/index.php?subaction=userinfo&user=upydug
d.mwoff.org/index.php?/topic/67-купить-диплом-h734n/
diywiki.org/index.php?title=russianydiplomix
Привет!
Заказать диплом о высшем образовании.
biocenter.pro/club/blogs/sonnick84-blog-bc/kak-podyskat-nadezhnyy-internetmagazin-s-bolshim-vyborom-diplomov/
Наш сервисный центр предлагает профессиональный починить сетевое хранилище в москве любых брендов и моделей. Мы понимаем, насколько важны для вас ваши NAS-системы, и обеспечиваем ремонт высочайшего уровня. Наши профессиональные техники проводят ремонтные работы с высокой скоростью и точностью, используя только оригинальные запчасти, что гарантирует долговечность и надежность проведенных ремонтов.
Наиболее распространенные поломки, с которыми сталкиваются обладатели серверов хранения данных, включают поломку жесткого диска, проблемы с питанием, программные сбои, неработающие сетевые интерфейсы и аппаратные сбои. Для устранения этих проблем наши опытные мастера выполняют ремонт жестких дисков, блоков питания, ПО, сетевых интерфейсов и компонентов. Обращаясь в наш сервисный центр, вы гарантируете себе качественный и надежный мастер по ремонту сетевых хранилищ в москве.
Подробная информация представлена на нашем сайте: https://remont-setevyh-hranilishh-service.ru
Привет, друзья!
Где заказать диплом специалиста?
usa.life/read-blog/56991
Привет, друзья!
Приобрести документ университета можно в нашей компании в столице.
ast-diplom.com/kupit-diplom-magistra
Успешной учебы!
Привет, друзья!
Заказать диплом любого университета.
rf-4fun.ru/index.php?/gallery/image/120-как-найти-проверенный-интернет-магазин-с-широким-каталогом-дипломов/
Монтаж системы видеонаблюдения может потребоваться в самых разных ситуациях. Её устанавливают в частных и загородных домах, промышленных предприятиях, офисах, гаражах и многих других помещениях https://plitmart.ru/uustanovka-sistem-videonablyudeniya-nadezhnaya-zaschita/
Купить диплом о высшем образовании.
boyara-analia.flybb.ru/viewtopic.php?f=7&t=692&sid=7df9fb7fc3c8a169b357bac5cf25adef
human.forumieren.de/login
collieforum.ru/posting.php?mode=post&f=17
vocal.com.ua/node/62329
bintarotrojan.com/blogs/new
Здравствуйте!
Приобрести документ института
bisshogram.com/read-blog/269
creativesparkstudio.net/blogs/50/Как-заказать-сейчас-качественный-диплом-в-интернете
togethers.mn.co/posts/61723851
q0xs4p3w8.blogproducer.com/34531900/Как-возможно-будет-недорого-заказать-диплом-в-онлайн-магазине
manchestercityclubs.com/read-blog/252
Привет, друзья!
Приобрести документ о получении высшего образования
asxdiplomik.com/kupit-diplom-vracha
The scoring system in the Aviator Game is based on the multiplier at the time of cashing out. The higher the
cost of ivermectin
Добрый день!
Заказать документ о получении высшего образования вы имеете возможность у нас.
ast-diplomas.com/kupit-diplom-chelyabinsk
Привет, друзья!
Купить документ о получении высшего образования вы можете у нас.
ast-diplomas.com/kupit-diplom-nizhnij-novgorod
Удачи!
Здравствуйте!
Мы изготавливаем дипломы любых профессий по приятным тарифам.
newfinbiz.ru/kupit-diplomyi-dlya-vseh-spetsialnostey
Полеты на параплане в Анапе – Морская рыбалка в Анапе, Дайвинг в Анапе
Привет, друзья!
Купить документ о получении высшего образования.
subscribe.ru/member/quick
vv.flybb.ru/viewtopic.php?f=23&t=2251
allseoreg.wordpress.com/2024/07/17/доступные-дипломы-для-вашего-успеха/
markusragger.at/chess/index.php/kforum/jm-news-pro-module/652509
ya.bestbb.ru/viewtopic.php?id=3013#p6648
kraken сайт покупок
Привет, друзья!
Быстрое обучение и получение диплома магистра – возможно ли это?
thecryptocurrency.directory/tag/купить-диплом-бакалавра-в-ростове-на-д/
Окажем помощь!.
Добрый день!
Приобретение школьного аттестата с официальным упрощенным обучением в Москве
arusak-diploms-srednee.ru В
Рейтинг лучших электрических щеток в 2024 году
В 2024 году рынок бытовой техники продолжает предлагать все новые и новые решения для поддержания чистоты в вашем доме. Электрические щетки становятся все более популярными благодаря своей эффективности и удобству в использовании. В этом обзоре мы рассмотрим ТОП-20 электрических щеток в 2024 году, которые заслужили внимание пользователей и экспертов. Выбор электрической щетки может зависеть от множества факторов, включая тип покрытия, мощность и дополнительные функции.
1. Philips Sonicare ProtectiveClean 6100 – Отличается высокой мощностью и продуманным дизайном, что обеспечивает отличную чистку и бережное отношение к зубам и деснам.
2. Oral-B Genius X 10000 – Умная щетка с технологией искусственного интеллекта для персонализированной чистки.
3. Fairywill FW-507 – Бюджетный вариант с хорошим набором функций, включая таймер и различные режимы чистки.
4. Waterpik Sonic-Fusion – Щетка с встроенным ирригатором для комплексной гигиены полости рта.
5. Colgate Hum – Умная щетка с функцией синхронизации с мобильным приложением для отслеживания прогресса.
6. Sonicare DiamondClean HX9332/04 – Премиум-модель с высокой частотой вибраций и несколькими режимами чистки для комплексного ухода.
7. Oral-B Pro 3000 – Идеальный выбор для тех, кто ищет надежную щетку с базовыми, но эффективными функциями.
8. BURST Sonic Toothbrush – Инновационная щетка с ультра-эффективной чисткой и длительным временем работы от аккумулятора.
9. Amabrush – Щетка с автоматическим очищением, которая минимизирует усилия и время на уход за зубами.
10. Xiaomi So White – Технологичная щетка с множеством режимов работы и отличным соотношением цены и качества.
11. FOREO ISSA 2 – Щетка с инновационным силиконовым дизайном, обеспечивающая тщательную чистку и длительный срок службы.
12. Oral-B Smart 1500 – Модель с базовыми умными функциями и эффективной чисткой для ежедневного использования.
13. Philips Sonicare FlexCare+ – Щетка с функцией отслеживания времени и давления для оптимального ухода.
14. Quip Electric Toothbrush – Минималистичный дизайн и длительное время работы на одной зарядке для простоты использования.
15. Boka Electric Toothbrush – Щетка с мощной батареей и качественными щетинками для комплексной чистки.
16. Waterpik Sensonic Professional Plus – Щетка с высокой скоростью вибраций и удобной эргономичной ручкой.
17. Oclean X Pro Elite – Модель с сенсорным экраном и множеством режимов для персонализированного ухода.
18. SmileDirectClub Sonic Toothbrush – Компактная щетка с хорошей функциональностью для поддержания здоровья зубов.
19. Dr. Fresh Sonic Toothbrush – Надежный вариант с длинным временем работы и хорошей чистящей способностью.
20. AuraGlow Sonic Toothbrush – Щетка с ультразвуковой технологией и возможностью подключения к смартфону для отслеживания чистки.
21. Fairywill FW-917 – Щетка с 5 режимами чистки и долгим сроком службы аккумулятора для удобства использования.
22. B Braun Oral-B Pro 6000 – Модель с инновационной технологией 3D движения для улучшенной чистки.
23. Waterpik Sonic Fusion Professional – Щетка с двойной функцией для улучшенной гигиены полости рта.
24. Sonicare For Kids HX6321/02 – Специально разработанная щетка для детей с веселым дизайном и простыми в использовании функциями.
25. Xiaomi Mi Electric Toothbrush T500 – Щетка с технологией умной чистки и возможностью настройки через мобильное приложение.
Эти щетки представляют собой лишь небольшую часть доступных на рынке моделей, и каждая из них имеет свои уникальные особенности. Если вы ищете лучший способ поддерживать чистоту в вашем доме, также не забудьте рассмотреть паровые швабры, которые могут стать отличным дополнением к вашей бытовой технике.
Здравствуйте!
Приобрести диплом о высшем образовании.
forum.shevrondeath.club/files/file/20-большой-каталог-документов-в-знаменитом-интернет-магазине/
kraken ссылка зеркало 2kmp
kraken клирнет зеркало
Привет!
Приобрести диплом любого ВУЗа
olfrn2hns.blogs100.com/28723877/Советы-что-позволят-найти-надежный-магазин-с-документами
cdposz.ru/club/user/802/forum/message/1503/1562/
gift-me.net/blogs/173568/Оформление-диплома-под-ключ-просто-и-удобно
weekofsport.ru/kupite-diplom-i-poluchite-novyie-vozmozhnosti
mediamemorial.ru/club/user/125807/forum/message/3822/13304/#message13304
Здравствуйте!
Приобрести документ ВУЗа можно у нас в Москве.
diplomyx.com/kupit-diplom-o-vysshem-obrazovanii
Привет, друзья!
Мы можем предложить документы техникумов
linkthere.club/read-blog/8830
pitstopwheels.ru/forum/?PAGE_NAME=profile_view&UID=2791
skazka.g-talk.ru/ucp.php?mode=login
bonchancetour.ru/blogs/interest/1583.php#comments
enriquerp.listbb.ru/viewtopic.php?f=4&t=443
Привет!
Заказать документ о получении высшего образования вы можете в нашей компании в Москве.
diplomasx.com/kupit-diplom-o-srednem-obrazovanii
Успешной учебы!
Как приобрести аттестат о среднем образовании в Москве и других городах
volnodumie.bbmy.ru/viewtopic.php?id=13014#p26621
neurostarcheats.com/index.php?/gallery/image/36-за-счет-чего-онлайн-магазины-с-дипломами-сегодня-столь-популярны/
hristianka.ru/forum/r/prev_loaded/1/
nnars.ru/forum/suggestion-box/1216-легкий-способ-получить-диплом-быстро-и-просто#74602
feelosum.com/blogs/1728/Ваш-новый-диплом-уже-сегодня
Article submission websites provide a platform for authors and businesses to publish and promote their content, increasing their online visibility, driving traffic to their websites, and improving their search engine rankings through high-quality backlinks and targeted audience engagement https://globalarticlewarehouse.com
Наши специалисты предлагает профессиональный мастер по ремонту сигвея на выезде любых брендов и моделей. Мы осознаем, насколько значимы для вас ваши самобалансирующиеся устройства, и обеспечиваем ремонт наилучшего качества. Наши профессиональные техники работают быстро и аккуратно, используя только качественные детали, что обеспечивает надежность и долговечность выполненных работ.
Наиболее общие проблемы, с которыми сталкиваются обладатели самобалансирующихся устройств, включают проблемы с батареей, неисправности двигателя, сбои контроллера, проблемы с гиросенсорами и повреждения рамы. Для устранения этих проблем наши опытные мастера оказывают ремонт батарей, двигателей, контроллеров, гиросенсоров и механических компонентов. Обратившись к нам, вы обеспечиваете себе качественный и надежный вызвать мастера по ремонту сигвея на дому.
Подробная информация доступна на сайте: https://remont-sigveev-expertise.ru
Добрый день!
Мы готовы предложить дипломы.
a63.flybb.ru/viewtopic.php?f=16&t=3182
library.kemu.ac.ke/kemuwiki/index.php/Гарантия_Подлинности:_Покупка_Дипломов_Легально
nnars.ru/forum/suggestion-box/1210-официальные-дипломы-качество-и-легальность#74596
paintball-keller-lev.de/viewtopic.php?f=3&t=100142
toursoul.ru/?p=19206